The New England Journal of Medicine
|
|
|
- Gwendolyn Mitchell
- 6 years ago
- Views:
Transcription
1 The New England Journal of Medicine Copyright 2001 by the Massachusetts Medical Society VOLUME 344 M AY 24, 2001 NUMBER 21 MATERNAL AND FETAL OUTCOMES OF SUBSEQUENT PREGNANCIES IN WOMEN WITH PERIPARTUM CARDIOMYOPATHY URI ELKAYAM, M.D., PADMINI P. TUMMALA, M.D., KALPANA RAO, M.D., MOHAMMED W. AKHTER, M.D., ILYAS S. KARAALP, M.D., OMAR R. WANI, M.D., AFSHAN HAMEED, M.D., ISRAEL GVIAZDA, B.S., AND AVRAHAM SHOTAN, M.D. ABSTRACT Background Peripartum cardiomyopathy is a rare but sometimes fatal form of heart failure. Little is known about the outcomes of subsequent pregnancies in women who have had the disorder. Methods Through a survey of members of the American College of Cardiology, we identified 44 women who had had peripartum cardiomyopathy and had a total of 60 subsequent pregnancies. We then reviewed the medical records of these women and interviewed the women or their physicians. Results Among the first subsequent pregnancies in the 44 women, 28 occurred in women in whom left ventricular function had returned to normal (group 1) and 16 occurred in women with persistent left ventricular dysfunction (group 2). The pregnancies were associated with a reduction in the mean (±SD) left ventricular ejection fraction both in the total cohort (from 49±12 percent to 42±13 percent, P<0.001) and in each group separately (from 56±7 percent to 49±10 percent in group 1, P=0.002 and from 36±9 percent to 32±11 percent in group 2, P=0.08). During these pregnancies, symptoms of heart failure occurred in 21 percent of the women in group 1 and 44 percent of those in group 2. The mortality rate was 0 percent in group 1 and 19 percent in group 2 (P=0.06). In addition, the frequency of premature delivery was higher in group 2 (37 percent vs. 11 percent), as was that of therapeutic abortions (25 percent vs. 4 percent). Conclusions Subsequent pregnancy in women with a history of peripartum cardiomyopathy is associated with a significant decrease in left ventricular function and can result in clinical deterioration and even death. (N Engl J Med : ) Copyright 2001 Massachusetts Medical Society. PERIPARTUM cardiomyopathy is a rare form of heart failure of unknown cause that occurs during pregnancy or during the postpartum period. 1-3 Although approximately 20 percent of women with the disorder either die or survive only because they receive cardiac transplants, the majority recover partially or completely. Although the women who recover may desire to become pregnant again, there is a concern that such pregnancies may be associated with an increased risk of recurrence of cardiomyopathy. 1-4 Information about the outcome of additional pregnancies, however, is limited. 4-8 There is therefore no consensus regarding recommendations for future pregnancies in women who have had peripartum cardiomyopathy. 3 We undertook a study to determine maternal and fetal outcomes of subsequent pregnancy among women with a history of peripartum cardiomyopathy. METHODS We obtained information about subsequent pregnancies in women who had had peripartum cardiomyopathy by sending a questionnaire in 1997 and 1998 to all members of the American College of Cardiology in the United States (approximately 15,000 persons) and to 2 members of one cardiology group in South Africa, seeking information about women with peripartum cardiomyopathy who had subsequent pregnancies. The physicians who responded were asked to obtain from their patients written informed consent to participate in the study and to release their medical records to the investigators. Data were then collected by the investigators through the review of medical records and supplemented, if necessary, by information elicited in telephone interviews of the referring physicians or the patients. The study protocol and the consent form were approved by the institutional review board of the University of Southern California. From the Section of Heart Failure, Division of Cardiology, Department of Medicine (U.E., P.P.T., K.R., M.W.A., I.S.K., O.R.W., I.G., A.S.), and the Department of Obstetrics and Gynecology (A.H.), University of Southern California School of Medicine, Los Angeles. Address reprint requests to Dr. Elkayam at the Section of Heart Failure, Division of Cardiology, University of Southern California School of Medicine, LAC/USC Medical Center, 2025 Zonal Ave., Rm. 7621, Los Angeles, CA 90033, or at elkayam@hsc.usc.edu. N Engl J Med, Vol. 344, No. 21 May 24,
2 The criteria for the diagnosis of peripartum cardiomyopathy included the development of congestive heart failure during the last six months of pregnancy or the first six months after delivery, the absence of another identifiable cause of heart failure, and evidence of depressed left ventricular function, defined as a left ventricular ejection fraction of less than 40 percent, as measured by echocardiography. Comparisons between groups were made with the use of Fisher s exact test. Comparisons of left ventricular ejection fractions were made with the use of Student s paired t-test. All statistical tests were two-sided. RESULTS Of the approximately 15,000 physicians who were contacted, 409 returned the questionnaire. On the basis of these responses, we identified 92 women with a history of peripartum cardiomyopathy who had had a subsequent pregnancy. We were able to review the clinical and echocardiographic information for 44 of these women, of whom 23 were white, 16 were black, and 5 were Hispanic. Their ages at the time of diagnosis of peripartum cardiomyopathy ranged from 19 to 39 years (mean [±SD], 29±6) parity ranged from 1 to 9 (mean, 1.9±1.5), and gravidity ranged from 1 to 10 (mean, 2.8±2.5). The diagnosis of cardiomyopathy was made before delivery in 7 women (1 woman each in the fifth, sixth, and seventh months of pregnancy, 2 women in the eighth month of pregnancy, and 2 women in the last month of pregnancy), during the first month after delivery in 28 women, and between two and six months after delivery in 9 women (2 women in the second month after delivery, 1 in the third month, 1 in the fifth month, and 5 in the sixth month after delivery). Ten women had preeclampsia, and four had a history of chronic hypertension. None of the women had severe anemia or a history of hyperthyroidism. Seven were reported to have undergone endomyocardial biopsy, and in three of these the biopsy results were reported to be positive for myocarditis. The mean interval between the pregnancy complicated by peripartum cardiomyopathy (index pregnancy) and the first subsequent pregnancy was 27±18 months, and the duration of follow-up after the index pregnancy was 90±87 months. A total of 33 of the women had one subsequent pregnancy, 6 had two subsequent pregnancies each, and 5 had three subsequent pregnancies each. At diagnosis, the mean left ventricular end-diastolic dimension, as measured by echocardiography, in the 44 women was 56±7 mm (normal range, 36 to 52), 9 the end-systolic dimension was 44±8 mm (normal range, 23 to 39), and the ejection fraction was 32±11 percent (normal range, 59±6) (Fig. 1). First Subsequent Pregnancies The mean left ventricular ejection fraction in the total cohort of 44 women was 32±11 percent at diagnosis and increased significantly to 49±12 percent before the first subsequent pregnancy (P<0.001). During the subsequent pregnancy, the mean left ventricular ejection fraction decreased to 42±13 percent (P<0.001), and the mean value was 45±13 percent a mean of 72 months after the subsequent pregnancy (Fig. 1). The normalization of ventricular function, defined as an increase in the left ventricular ejection fraction to at least 50 percent, was documented in 28 women (group 1) before their first subsequent pregnancy, whereas 16 women (group 2) had persistent left ventricular dysfunction (an ejection fraction of less than 50 percent) (Fig. 1). The mean left ventricular ejection fraction decreased in both groups during the subsequent pregnancy, from 56±7 percent to 49±10 percent in group 1 (P=0.002) and from 36±9 percent to 32±11 percent in group 2 (P=0.08). Maternal Outcome During the first subsequent pregnancy, 6 of the 28 women in group 1 (21 percent) and 7 of the 16 women in group 2 (44 percent) had symptoms of heart failure (Table 1). Twenty-one percent of the women in group 1 and 25 percent of those in group 2 had a decrease of more than 20 percent in the left ventricular ejection fraction during the first subsequent pregnancy, and 14 percent of the women in group 1 and 31 percent of those in group 2 had a decreased ejection fraction at the last follow-up. None of the women in group 1 died during or after the first subsequent pregnancy three of the women in group 2 (19 percent) died after the first subsequent pregnancy. Two of the women died suddenly (one died two months after the subsequent pregnancy and the other two years after the subsequent pregnancy), and one woman died of progressive heart failure two months after the subsequent pregnancy. Outcome of Pregnancies That Were Not Terminated Because the early interruption of pregnancy may prevent complications in the pregnant woman, we separately evaluated the outcome of the 35 first subsequent pregnancies that were not terminated. In the 35 women who did not have abortions, the mean ejection fraction decreased by 14 percent (from 49±12 percent to 42±14 percent, P<0.001), as compared with a decrease of only 7 percent in the 9 women who had abortions (from 46±13 percent to 43±11 percent, P=0.20). The mean decrease in the left ventricular ejection fraction was 8 percent in the 23 women in group 1 who did not have abortions (P<0.01) and 5 percent in the 12 women in group 2 who did not have abortions (P<0.05). Among the women who did not have abortions, a greater proportion of those in group 2 than of those in group 1 had symptoms of heart failure, a decrease in the ejection fraction of more than 20 percent during the subsequent pregnancy, or a decreased ejection fraction at last followup (Table 1). There were no deaths in group 1, but three women in this subgroup of group 2 died N Engl J Med, Vol. 344, No. 21 May 24,
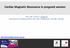
3 THE OUTCOMES OF SUBSEQUENT PREGNANCIES IN WOMEN WITH PERIPARTUM CARDIOMYOPATHY Percentage of Women ±11 All women Group 1 Group 2 34±11 28±12 49±12 56±7 36±9 42±13 49±10 32±11 45±13 52±9 36± IndexŁ Pregnancy PostpartumŁ Follow-up SubsequentŁ Pregnancy LastŁ Follow-up Figure 1. Mean (±SD) Left Ventricular Ejection Fraction in 44 Women at the Time of the Diagnosis of Peripartum Cardiomyopathy (Index Pregnancy), at Postpartum Follow-up, during the First Subsequent Pregnancy, and at the Last Follow-up a Mean of 72 Months after the First Subsequent Pregnancy. Group 1 included all the women with a left ventricular ejection fraction of 50 percent or higher before subsequent pregnancies, and group 2 included all those with a left ventricular ejection fraction of less than 50 percent before subsequent pregnancies. For the total cohort (all women), P<0.001 for the comparison between postpartum follow-up and the index pregnancy, P<0.001 for the comparison between subsequent pregnancy and postpartum follow up, and P=0.06 for the comparison between last follow-up and subsequent pregnancy. For group 1, P<0.001 for the comparison between postpartum follow-up and the index pregnancy, P=0.002 for the comparison between subsequent pregnancy and postpartum follow-up, and P=0.06 for the comparison between last followup and subsequent pregnancy. For group 2, P=0.05 for the comparison between postpartum follow-up and the index pregnancy and P=0.08 for the comparison between subsequent pregnancy and postpartum follow-up. Fetal Outcome Among the 35 women who had a subsequent pregnancy and did not have an abortion, 21 had a normal vaginal delivery, and 14 delivered by cesarean section. Premature delivery (defined as delivery at less than 37 weeks gestation) occurred in three women (13 percent of the subgroup) in group 1 (at 30, 32, and 36 weeks) and in six women (50 percent of the subgroup) in group 2 (two women at 30 weeks, one at 34 weeks, one at 35 weeks, and two at 36 weeks). There was no perinatal mortality. Of the nine abortions, five were therapeutic one of these occurred in group 1 (4 percent of the first subsequent pregnancies) and the other four in group 2 (25 percent of the first subsequent pregnancies). Additional Pregnancies Eleven of the women had 16 additional pregnancies. Of the women in group 1, five women had one additional pregnancy each and four women had two additional pregnancies each of those in group 2, one TABLE 1. INCIDENCE OF MATERNAL COMPLICATIONS DURING GROUP THE FIRST SUBSEQUENT PREGNANCY IN WOMEN WHO HAD HAD PERIPARTUM CARDIOMYOPATHY.* NO. OF WOMEN SYMPTOMS OF HEART FAILURE >20% DECREASE IN LVEF DECREASED LVEF AT FOLLOW-UP no. of women (%) DEATH All women 44 Group (21) 6 (21) 4 (14) 0 Group (44) 4 (25) 5 (31) 3 (19) Women who did not 35 have abortions Group (26) 4 (17) 2 (9) 0 Group (50) 4 (33) 5 (42) 3 (25) *Group 1 consisted of women with recovered left ventricular function, defined as a left ventricular ejection fraction (LVEF) of 50 percent or higher, before the subsequent pregnancy group 2 consisted of women with persistent left ventricular dysfunction (an LVEF of less than 50 percent). P=0.06 for the comparison with group 1. P=0.05 for the comparison with group 1. N Engl J Med, Vol. 344, No. 21 May 24,
4 woman had one additional pregnancy, and one woman had two additional pregnancies. None of these women were reported to have symptoms of heart failure during these later pregnancies. One woman who had no change in the left ventricular ejection fraction during her first subsequent pregnancy had a substantial decrease in the ejection fraction from 55 percent to 40 percent during her second subsequent pregnancy, and the decreased ejection fraction persisted at three months of follow-up. DISCUSSION Determination of the risk associated with subsequent pregnancies in women with a history of peripartum cardiomyopathy has obvious clinical implications. This study demonstrates that in women who have had peripartum cardiomyopathy, subsequent pregnancies may be associated with deleterious fetal and maternal outcomes such as premature delivery and maternal cardiac dysfunction, including symptomatic heart failure and even death. We found the outcomes of subsequent pregnancies to be poor, not only in women with persistent left ventricular dysfunction after the initial diagnosis of peripartum cardiomyopathy, but also, in contrast to the results of a small study conducted by Sutton et al., 6 in women whose left ventricular function returned to normal after the initial pregnancy complicated by peripartum cardiomyopathy. When pregnancies that were ended by abortion were excluded, the risk of unfavorable maternal and fetal outcome was even higher, especially in the women who had had persistent left ventricular dysfunction (group 2). Of the 44 women we studied, 3 (7 percent) died during a mean follow-up period of more than seven years all of those who died had had persistent left ventricular dysfunction after their first episode of peripartum cardiomyopathy. Two of the deaths occurred soon after delivery, but the third death occurred suddenly four years after the initial diagnosis and two years after the subsequent pregnancy. The lower mortality rate in the present study than in previous reports 5,9 may be due to differences in the study subjects, criteria for diagnosis, or treatments to the high rate of abortions (20 percent), which could have prevented the deterioration of cardiac function as well as other complications and death or simply to reporting bias. The possibility that the diagnosis and treatment of heart failure have improved in recent years is supported by a recent finding of less than 10 percent mortality over 4.4 years among 51 women with peripartum cardiomyopathy diagnosed between 1982 and The exact mechanism of recurrent depression of cardiac function associated with subsequent pregnancy in women who have had peripartum cardiomyopathy is not clear. The persistence of such dysfunction in some of the women suggests a reactivation of the underlying idiopathic process responsible for the initial cardiomyopathy. Unmasked subclinical myocardial dysfunction may also be related to clinical worsening with subsequent pregnancies. Lampert et al. 11 reported reduced contractile reserve in women with peripartum cardiomyopathy even after the apparent recovery of left ventricular function. In addition, a transient decrease in myocardial contractility during the second and third trimesters of pregnancy and the early postpartum period has been described. 12 Such a change in myocardial performance is normally compensated for by a change in loading conditions during normal pregnancy, but it may unmask decreased contractile reserve in women with peripartum cardiomyopathy. The data for this study were collected by a retrospective survey that was completely dependent on the responses of physicians and patients. Data collected in this way can be strongly influenced by ascertainment bias, selection bias, and recall bias, and they are likely to be incomplete. In addition, our echocardiographic data were based on the interpretations of individual physicians as contained in the patients records. Although we studied more women than did previous investigators, the numbers of women in the two groups, and especially in the subgroups, were small. In spite of these limitations, the findings are strongly supported by a previous survey that we conducted. 13 That survey, which relied solely on a questionnaire filled out by physicians, provided data on 67 subsequent pregnancies in 63 women who had had peripartum cardiomyopathy and who were not included in the present study. In the survey, there were 40 women with normal left ventricular function after peripartum cardiomyopathy and 23 women with persistent left ventricular dysfunction. The women with normal left ventricular function had 43 subsequent pregnancies, of which 10 (23 percent) were associated with cardiac dysfunction one of the women in this group (2 percent) died. The women with persistent left ventricular dysfunction had 24 subsequent pregnancies, of which 13 (54 percent) were associated with cardiac dysfunction two of the women in this group (9 percent) died. The present study demonstrates an important effect of subsequent pregnancy in terms of both maternal and fetal outcome among women with a history of peripartum cardiomyopathy, especially those with persistent depression of left ventricular function. This information should be useful for decision making in cases in which women with a history of peripartum cardiomyopathy desire to become pregnant again. We are indebted to Ms. Natalia Zapadinsky and Ms. Lorine Araiza for their help in the preparation of the manuscript. REFERENCES 1. Lang RM, Lampert MB, Poppas A, Hameed A, Elkayam U. Peripartal cardiomyopathy. In: Elkayam U, Gleicher N, eds. Cardiac problems in pregnancy. 3rd ed. New York: Wiley Liss, 1998: N Engl J Med, Vol. 344, No. 21 May 24,
5 THE OUTCOMES OF SUBSEQUENT PREGNANCIES IN WOMEN WITH PERIPARTUM CARDIOMYOPATHY 2. Heider AL, Kuller JA, Strauss RA, Wells SR. Peripartum cardiomyopathy: review of the literature. Obstet Gynecol Surv : Pearson GD, Veille J-C, Rahimtoola S, et al. Peripartum cardiomyopathy: National Heart, Lung, and Blood Institute and Office of Rare Diseases (National Institutes of Health) Workshop recommendations and review. JAMA : Witlin AG, Mabie WC, Sibai BM. Peripartum cardiomyopathy: an ominous diagnosis. Am J Obstet Gynecol : Demakis JG, Rahimtoola SH, Sutton GC, et al. Natural course of peripartum cardiomyopathy. Circulation : Sutton MSJ, Cole P, Plappert M, Saltzman D, Goldhaber S. Effects of subsequent pregnancy on left ventricular function in peripartum cardiomyopathy. Am Heart J : Ceci O, Berardesca C, Caradonna F, Corsano P, Guglielmi R, Nappi L. Recurrent peripartum cardiomyopathy. Eur J Obstet Gynecol Reprod Biol : Elkayam U. Pregnancy and cardiovascular disease. In: Braunwald E, ed. Heart disease. 4th ed. Philadelphia: W.B. Saunders, 1992: Echocardiographic measurements and normal valves. In: Feigenbaum H. Echocardiography. 5th ed. Philadelphia: Lea & Febiger, 1994: Felker GM, Thompson RE, Hare JM, et al. Underlying causes and long-term survival in patients with initially unexplained cardiomyopathy. N Engl J Med : Lampert M, Weinert L, Hibbard J, Korcarz C, Lindheimer M, Lang RM. Contractile reserve in patients with peripartum cardiomyopathy and recovered left ventricular function. Am J Obstet Gynecol : Geva T, Mauer MB, Striker L, Kirshon B, Pivarnik JM. Effects of physiologic load of pregnancy on left ventricular contractility and remodeling. Am Heart J : Ostrzega E, Elkayam U. Risk of subsequent pregnancy in women with a history of peripartum cardiomyopathy: results of a survey. Circulation :Suppl I:I-333. abstract. Copyright 2001 Massachusetts Medical Society. RECEIVE THE JOURNAL S TABLE OF CONTENTS EACH WEEK BY To receive the table of contents of the New England Journal of Medicine by every Wednesday evening, you can sign up through our Web site at: N Engl J Med, Vol. 344, No. 21 May 24,
Risk of Subsequent Pregnancy in Women with a History of Peripartum Cardiomyopathy Uri Elkayam, MD
 Risk of Subsequent Pregnancy in Women with a History of Peripartum Cardiomyopathy Uri Elkayam, MD Professor of Medicine / Cardiology Professor of Obstetrics and Gynecology University of Southern California
Risk of Subsequent Pregnancy in Women with a History of Peripartum Cardiomyopathy Uri Elkayam, MD Professor of Medicine / Cardiology Professor of Obstetrics and Gynecology University of Southern California
Maternal and fetal prognosis of subsequent pregnancy in black African women with peripartum cardiomyopathy
 Yaméogo et al. BMC Cardiovascular Disorders (2018) 18:119 https://doi.org/10.1186/s12872-018-0856-7 RESEARCH ARTICLE Maternal and fetal prognosis of subsequent pregnancy in black African women with peripartum
Yaméogo et al. BMC Cardiovascular Disorders (2018) 18:119 https://doi.org/10.1186/s12872-018-0856-7 RESEARCH ARTICLE Maternal and fetal prognosis of subsequent pregnancy in black African women with peripartum
Pregnancy outcome in Peripartum Cardiomyopathy
 Abstract Pregnancy outcome in Peripartum Cardiomyopathy Anuja Bhalerao, Richa Garg Department of Obstetrics and Gynaecology NKP Salve institute of medical sciences, Nagpur,India Email: anuja_bhalerao@yahoo.com,
Abstract Pregnancy outcome in Peripartum Cardiomyopathy Anuja Bhalerao, Richa Garg Department of Obstetrics and Gynaecology NKP Salve institute of medical sciences, Nagpur,India Email: anuja_bhalerao@yahoo.com,
Reversible peripartum cardiomyopathy in a triplet pregnancy
 Reversible peripartum cardiomyopathy in a triplet pregnancy BY EDVARD GALIĆ, DARIO GULIN, KREŠIMIR KORDIĆ, BERIVOJ MIŠKOVIĆ, OLIVER VASILJ, JOZICA ŠIKIĆ Abstract Peripartum cardiomyopathy (PPCM) is a rare
Reversible peripartum cardiomyopathy in a triplet pregnancy BY EDVARD GALIĆ, DARIO GULIN, KREŠIMIR KORDIĆ, BERIVOJ MIŠKOVIĆ, OLIVER VASILJ, JOZICA ŠIKIĆ Abstract Peripartum cardiomyopathy (PPCM) is a rare
Clinical Profile and Predictors of Complications in Peripartum Cardiomyopathy
 Journal of Cardiac Failure Vol. 15 No. 8 2009 Clinical Investigations Clinical Profile and Predictors of Complications in Peripartum Cardiomyopathy SOREL GOLAND, MD, 1 KALGI MODI, MD, 2 FAHED BITAR, MD,
Journal of Cardiac Failure Vol. 15 No. 8 2009 Clinical Investigations Clinical Profile and Predictors of Complications in Peripartum Cardiomyopathy SOREL GOLAND, MD, 1 KALGI MODI, MD, 2 FAHED BITAR, MD,
Peripartum Cardiomyopathy: Clinical, Hemodynamic, Histologic and Prognostic Characteristics
 52 JACC Vol. 8, No. I Peripartum Cardiomyopathy: Clinical, Hemodynamic, Histologic and Prognostic Characteristics JOHN B. O'CONNELL, MD, FACC, MARIA ROSA COSTANZO-NORDIN, MD, RAMIAH SUBRAMANIAN, MB, MRC
52 JACC Vol. 8, No. I Peripartum Cardiomyopathy: Clinical, Hemodynamic, Histologic and Prognostic Characteristics JOHN B. O'CONNELL, MD, FACC, MARIA ROSA COSTANZO-NORDIN, MD, RAMIAH SUBRAMANIAN, MB, MRC
The Effect of Valvular Heart Diseases on Maternal and Fetal Outcome of Pregnancy Nada Salih Ameen*,Nawfal Fawzi Anwer**
 THE VALVULAR IRAQI POSTGRADUATE HEART DISEASES MEDICAL AND JOURNAL PREGNANCY The Effect of Valvular Heart Diseases on Maternal and Fetal Outcome of Pregnancy Nada Salih Ameen*,Nawfal Fawzi Anwer** ABSTRACT:
THE VALVULAR IRAQI POSTGRADUATE HEART DISEASES MEDICAL AND JOURNAL PREGNANCY The Effect of Valvular Heart Diseases on Maternal and Fetal Outcome of Pregnancy Nada Salih Ameen*,Nawfal Fawzi Anwer** ABSTRACT:
Peripartum cardiomyopathy: review and practice guidelines. Hanan ALBackr Associate Professor King Saud university, King Fahad Cardaic center -Riyadh
 Peripartum cardiomyopathy: review and practice guidelines Hanan ALBackr Associate Professor King Saud university, King Fahad Cardaic center -Riyadh Outlines Definition of PPCM Dignostic Critaria for peripartum
Peripartum cardiomyopathy: review and practice guidelines Hanan ALBackr Associate Professor King Saud university, King Fahad Cardaic center -Riyadh Outlines Definition of PPCM Dignostic Critaria for peripartum
Images in Cardiovascular Medicine
 Images in Cardiovascular Medicine Management of Severe Mitral Stenosis During Pregnancy Rebecca S. Norrad, MBBS; Omid Salehian, MSc, MD, FRCPC, FACC, FAHA A 37-year-old woman originally from Iraq was referred
Images in Cardiovascular Medicine Management of Severe Mitral Stenosis During Pregnancy Rebecca S. Norrad, MBBS; Omid Salehian, MSc, MD, FRCPC, FACC, FAHA A 37-year-old woman originally from Iraq was referred
Considerations on Phasing Out Medications In the Treatment of Peripartum Cardiomyopathy After Full Recovery James D. Fett, MD
 Considerations on Phasing Out Medications In the Treatment of Peripartum Cardiomyopathy After Full Recovery James D. Fett, MD Co-Director, Peripartum Cardiomyopathy Network, Coordinating Center, University
Considerations on Phasing Out Medications In the Treatment of Peripartum Cardiomyopathy After Full Recovery James D. Fett, MD Co-Director, Peripartum Cardiomyopathy Network, Coordinating Center, University
Peripartum cardiomyopathy (PPCM) is a rare, potentially
 J Perinat Neonat Nurs Vol. 20, No. 4, pp. 324 332 c 2006 Lippincott Williams & Wilkins, Inc. Peripartum Cardiomyopathy Denise G. Palmer, MS, RN, CNS Peripartum cardiomyopathy is a rare and potentially
J Perinat Neonat Nurs Vol. 20, No. 4, pp. 324 332 c 2006 Lippincott Williams & Wilkins, Inc. Peripartum Cardiomyopathy Denise G. Palmer, MS, RN, CNS Peripartum cardiomyopathy is a rare and potentially
Angiogenic imbalance and residual myocardial dysfunction in women with Peripartum Cardiomyopathy and left ventricular function recovery
 Angiogenic imbalance and residual myocardial dysfunction in women with Peripartum Cardiomyopathy and left ventricular function recovery Sorel Goland¹, Adi Zalik¹, Jan Mark Weinstein³, Liaz Zilberman¹,
Angiogenic imbalance and residual myocardial dysfunction in women with Peripartum Cardiomyopathy and left ventricular function recovery Sorel Goland¹, Adi Zalik¹, Jan Mark Weinstein³, Liaz Zilberman¹,
Pregnancy in Non-Peripartum Cardiomyopathy
 Pregnancy in Non-Peripartum Cardiomyopathy Avraham Shotan, Lubov Vasilenco, Michael Shochat, Mark Kazatsker, David Blondheim, Yaniv Levi, Simcha Meisel, Alicia Vazan Heart Institute, Hillel Yaffe Medical
Pregnancy in Non-Peripartum Cardiomyopathy Avraham Shotan, Lubov Vasilenco, Michael Shochat, Mark Kazatsker, David Blondheim, Yaniv Levi, Simcha Meisel, Alicia Vazan Heart Institute, Hillel Yaffe Medical
Prevalence of thyroid disorder in pregnancy and pregnancy outcome
 Original Research Article Prevalence of thyroid disorder in pregnancy and pregnancy outcome Praveena K.R. 1, Pramod Kumar K.R. 2*, Prasuna K.R. 3, Krishna Kumar TV 4 1 Assistant Professor, Department of
Original Research Article Prevalence of thyroid disorder in pregnancy and pregnancy outcome Praveena K.R. 1, Pramod Kumar K.R. 2*, Prasuna K.R. 3, Krishna Kumar TV 4 1 Assistant Professor, Department of
EVALUATION OF PREGNANT PATIENTS WITH HEART DISEASE. Karen Stout, MD University of Washington Seattle Children s Seattle, WA
 EVALUATION OF PREGNANT PATIENTS WITH HEART DISEASE Karen Stout, MD University of Washington Seattle Children s Seattle, WA CASE PRESENTATION 24 year old woman with aortic regurgitation referred for evaluation
EVALUATION OF PREGNANT PATIENTS WITH HEART DISEASE Karen Stout, MD University of Washington Seattle Children s Seattle, WA CASE PRESENTATION 24 year old woman with aortic regurgitation referred for evaluation
Module 1: Defini3on Epidemiology of Heart Failure Pathophysiology of Heart Failure Specific Diseases causing Heart Failure and prac3cal case studies
 Program: Module 1: Defini3on Epidemiology of Heart Failure Pathophysiology of Heart Failure Specific Diseases causing Heart Failure and prac3cal case studies Module 2: Diagnosis and Inves3ga3on of HF and
Program: Module 1: Defini3on Epidemiology of Heart Failure Pathophysiology of Heart Failure Specific Diseases causing Heart Failure and prac3cal case studies Module 2: Diagnosis and Inves3ga3on of HF and
Effects of pregnancy-related hemodynamic and hormonal changes
 Information extracted from WWW.HEARTDISEASEANDPREGNANCY.COM CORONARY ARTERY DISEASE Background Coronary artery disease (CAD) is the leading cause of death worldwide in women. It has already been noted
Information extracted from WWW.HEARTDISEASEANDPREGNANCY.COM CORONARY ARTERY DISEASE Background Coronary artery disease (CAD) is the leading cause of death worldwide in women. It has already been noted
Peripartum Cardiomyopathy. Lavanya Rai Manipal
 Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Clinical Outcomes of Women with Peripartum Cardiomyopathy With and Without Preeclampsia: a Population-based Study
 Clinical Outcomes of Women with Peripartum Cardiomyopathy With and Without Preeclampsia: a Population-based Study Isabelle Malhamé, MSc Candidate in Epidemiology, McGill University Obstetric Medicine Fellow,
Clinical Outcomes of Women with Peripartum Cardiomyopathy With and Without Preeclampsia: a Population-based Study Isabelle Malhamé, MSc Candidate in Epidemiology, McGill University Obstetric Medicine Fellow,
Maternal And Fetal Outcome In Pregnancies Complicated With Maternal Cardiac Diseases: Experience At A Tertiary Care Hospital
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 19 Number 1 Maternal And Fetal Outcome In Pregnancies Complicated With Maternal Cardiac Diseases: Experience At A Tertiary Care Hospital
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 19 Number 1 Maternal And Fetal Outcome In Pregnancies Complicated With Maternal Cardiac Diseases: Experience At A Tertiary Care Hospital
CARDIOVASCULAR DISEASE ASSESSMENT IN PREGNANT AND POSTPARTUM WOMEN
 ! ASSESSMENT IN PREGNANT AND POSTPARTUM WOMEN Afshan'Hameed,'MD' 'University'of'California,'Irvine'Medical'Center' Elyse'Foster,'MD' 'University'of'California,'San'Francisco' Elliott'Main,'MD' 'California'Maternal'Quality'Care'Collaborative'
! ASSESSMENT IN PREGNANT AND POSTPARTUM WOMEN Afshan'Hameed,'MD' 'University'of'California,'Irvine'Medical'Center' Elyse'Foster,'MD' 'University'of'California,'San'Francisco' Elliott'Main,'MD' 'California'Maternal'Quality'Care'Collaborative'
Outcomes of Pregnancies at Risk for Hypertensive Complications Managed Using Impedance Cardiography
 Outcomes of Pregnancies at Risk for Hypertensive Complications Managed Using Impedance Cardiography David G. Chaffin, M.D., 1 and Denise G. Webb, RNC, BSN 2 ABSTRACT We assessed the effect of antihypertensive
Outcomes of Pregnancies at Risk for Hypertensive Complications Managed Using Impedance Cardiography David G. Chaffin, M.D., 1 and Denise G. Webb, RNC, BSN 2 ABSTRACT We assessed the effect of antihypertensive
A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH
 A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH 1* Paul Leeson, PhD, FRCP and 1 Adam J. Lewandowski, DPhil 1 Oxford Cardiovascular Clinical Research Facility, Division of Cardiovascular Medicine,
A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH 1* Paul Leeson, PhD, FRCP and 1 Adam J. Lewandowski, DPhil 1 Oxford Cardiovascular Clinical Research Facility, Division of Cardiovascular Medicine,
Susan P. D Anna MSN, APRN BC February 14, 2019
 Is there Equal Opportunity in Heart Failure?? Susan P. D Anna MSN, APRN BC February 14, 2019 Disclosures: I have no financial disclosures. I am not an expert on this topic, but see a lot of women with
Is there Equal Opportunity in Heart Failure?? Susan P. D Anna MSN, APRN BC February 14, 2019 Disclosures: I have no financial disclosures. I am not an expert on this topic, but see a lot of women with
Maternal Mortality in Women with Sickle Cell Disease. Zainab Al-Jufairi, MHPE, FRCOG* Amarjit Sandhu, MD, FRCOG*
 Bahrain Medical Bulletin, Vol. 36, No. 4, December 2014 Maternal Mortality in Women with Sickle Cell Disease Zainab Al-Jufairi, MHPE, FRCOG* Amarjit Sandhu, MD, FRCOG* Background: Sickle cell disease (SCD)
Bahrain Medical Bulletin, Vol. 36, No. 4, December 2014 Maternal Mortality in Women with Sickle Cell Disease Zainab Al-Jufairi, MHPE, FRCOG* Amarjit Sandhu, MD, FRCOG* Background: Sickle cell disease (SCD)
PREGESTATIONAL DIABETES (TYPE 1 AND 2)
 PREGESTATIONAL DIABETES (TYPE 1 AND 2) Women with diabetes prior to pregnancy need to evaluate and optimize their baseline to assure the healthiest pregnancy possible.[1] The overall prevalence of pregnant
PREGESTATIONAL DIABETES (TYPE 1 AND 2) Women with diabetes prior to pregnancy need to evaluate and optimize their baseline to assure the healthiest pregnancy possible.[1] The overall prevalence of pregnant
Different Characteristics of Peripartum Cardiomyopathy Between Patients Complicated With and Without Hypertensive Disorders
 Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGINAL ARTICLE Myocardial Disease Different Characteristics of Peripartum Cardiomyopathy Between Patients
Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGINAL ARTICLE Myocardial Disease Different Characteristics of Peripartum Cardiomyopathy Between Patients
Anesthesia with etomidate and remifentanil for cesarean section in severe peripartum cardiomyopathy
 Case Report Anesthesia with etomidate and remifentanil for cesarean section in severe peripartum cardiomyopathy Eisa Bilehjani, Amir Abbas Kianfar, Mehrnoosh Solmaz Fakhari From Department of Cardiovascular
Case Report Anesthesia with etomidate and remifentanil for cesarean section in severe peripartum cardiomyopathy Eisa Bilehjani, Amir Abbas Kianfar, Mehrnoosh Solmaz Fakhari From Department of Cardiovascular
Diagnosis of Congenital Cardiac Defects Between 11 and 14 Weeks Gestation in High-Risk Patients
 Article Diagnosis of Congenital Cardiac Defects Between 11 and 14 Weeks Gestation in High-Risk Patients Zeev Weiner, MD, Abraham Lorber, MD, Eliezer Shalev, MD Objective. To examine the feasibility of
Article Diagnosis of Congenital Cardiac Defects Between 11 and 14 Weeks Gestation in High-Risk Patients Zeev Weiner, MD, Abraham Lorber, MD, Eliezer Shalev, MD Objective. To examine the feasibility of
Peripartum kardiomyopati
 Fall 3 Peripartum kardiomyopati Roman A roch 2017 01 26 2 3 Dg. PPCM Symptoms ECG, pro-bnp echocardiography 4 Peripartum cardiomyopathy: a systematic literature review Acta Obstetricia et Gynecologica
Fall 3 Peripartum kardiomyopati Roman A roch 2017 01 26 2 3 Dg. PPCM Symptoms ECG, pro-bnp echocardiography 4 Peripartum cardiomyopathy: a systematic literature review Acta Obstetricia et Gynecologica
A pregnant patient with a prosthetic valve Giacomo Boccuzzi, MD, FESC
 A pregnant patient with a prosthetic valve Giacomo Boccuzzi, MD, FESC Department of Invasive Cardiology, Ospedale San Giovanni Bosco, Turin, Italy *C.V. was born the 24th May 1980 Rheumatic fever during
A pregnant patient with a prosthetic valve Giacomo Boccuzzi, MD, FESC Department of Invasive Cardiology, Ospedale San Giovanni Bosco, Turin, Italy *C.V. was born the 24th May 1980 Rheumatic fever during
Quantitative Assessment of Fetal Ventricular Function:
 Reprinted with permission from ECHOCARDIOGRAPHY, Volume 18, No. 1, January 2001 Copyright 2001 by Futura Publishing Company, Inc., Armonk, NY 1004-0418 Quantitative Assessment of Fetal Ventricular Function:
Reprinted with permission from ECHOCARDIOGRAPHY, Volume 18, No. 1, January 2001 Copyright 2001 by Futura Publishing Company, Inc., Armonk, NY 1004-0418 Quantitative Assessment of Fetal Ventricular Function:
Objectives. Systolic Heart Failure: Definitions. Heart Failure: Historical Perspective 2/7/2009
 Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
Pregnancy outcomes in women after an arterial switch operation for transposition of the great arteries
 Pregnancy outcomes in women after an arterial switch operation for transposition of the great arteries Department of Obstetrics and Gynecology 1) Department of Pediatrics 2) National Cerebral and Cardiovascular
Pregnancy outcomes in women after an arterial switch operation for transposition of the great arteries Department of Obstetrics and Gynecology 1) Department of Pediatrics 2) National Cerebral and Cardiovascular
Diastolic Dysfunction: Hypertension to Hypertrophy to Heart Failure
 Diastolic Dysfunction: Hypertension to Hypertrophy to Heart Failure Dr. Shelley Zieroth FRCPC Assistant Professor, Cardiology, University of Manitoba Director of Cardiac Transplant and Heart Failure Clinics
Diastolic Dysfunction: Hypertension to Hypertrophy to Heart Failure Dr. Shelley Zieroth FRCPC Assistant Professor, Cardiology, University of Manitoba Director of Cardiac Transplant and Heart Failure Clinics
A lthough few studies have examined the clinical implications
 752 CARDIOVASCULAR MEDICINE Pregnancy related complications in women with hypertrophic cardiomyopathy R Thaman, A Varnava, M S Hamid, S Firoozi, B Sachdev, M Condon, J R Gimeno, R Murphy, P M Elliott,
752 CARDIOVASCULAR MEDICINE Pregnancy related complications in women with hypertrophic cardiomyopathy R Thaman, A Varnava, M S Hamid, S Firoozi, B Sachdev, M Condon, J R Gimeno, R Murphy, P M Elliott,
Pan American Heart Failure Congress (PAHF 2012) October 18 th -21 th 2012 Panama City, Panama
 Pan American Heart Failure Congress (PAHF 2012) October 18 th -21 th 2012 Panama City, Panama Congress Chairman Uri Elkayam, MD Professor of Medicine University of Southern California, Keck School of Medicine
Pan American Heart Failure Congress (PAHF 2012) October 18 th -21 th 2012 Panama City, Panama Congress Chairman Uri Elkayam, MD Professor of Medicine University of Southern California, Keck School of Medicine
Gestational Diabetes: An Update on Testing. Kimberlee A McKay, M.D. Avera Medical Group Ob/GYN
 Gestational Diabetes: An Update on Testing Kimberlee A McKay, M.D. Avera Medical Group Ob/GYN Gestational Diabetes Increased risks of: Still Birth Hydramnios Should Dystocia Prolonged Labor Preeclampsia
Gestational Diabetes: An Update on Testing Kimberlee A McKay, M.D. Avera Medical Group Ob/GYN Gestational Diabetes Increased risks of: Still Birth Hydramnios Should Dystocia Prolonged Labor Preeclampsia
Management of Heart Failure and Cardiomyopathies in Pregnancy
 Management of Heart Failure and Cardiomyopathies in Pregnancy Professor Sanjay Sharma Disclosures: None Epidemiology of Cardiac Disease In Pregnancy Cardiovascular disease in pregnancy is increasing in
Management of Heart Failure and Cardiomyopathies in Pregnancy Professor Sanjay Sharma Disclosures: None Epidemiology of Cardiac Disease In Pregnancy Cardiovascular disease in pregnancy is increasing in
Maternal Cardiac Disease In Pregnancy. August 25, 2017 PREGNANCY ECHO CONFERENCE
 Maternal Cardiac Disease In Pregnancy August 25, 2017 PREGNANCY ECHO CONFERENCE Maternal Physiology Cardiac Output = HR x SV Non-pregnant: 4.5 L/min Pregnant: 6.0 L/min Increase most acute in first 10
Maternal Cardiac Disease In Pregnancy August 25, 2017 PREGNANCY ECHO CONFERENCE Maternal Physiology Cardiac Output = HR x SV Non-pregnant: 4.5 L/min Pregnant: 6.0 L/min Increase most acute in first 10
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Vincelj, J., Sokol, I., Pevec, D., Sutlić, Ž. (2007) Infective endocarditis of aortic valve during pregnancy: A case report. International Journal of Cardiology, [Epub ahead
Središnja medicinska knjižnica Vincelj, J., Sokol, I., Pevec, D., Sutlić, Ž. (2007) Infective endocarditis of aortic valve during pregnancy: A case report. International Journal of Cardiology, [Epub ahead
Heart Failure treatment during pregnancy
 Heart Failure treatment during pregnancy Angeles Alonso García Hospital Universitario Puerta de Hierro. Majadahonda. Madrid. Spain European Society of Cardiology. Stockholm. 29 August 2010 Starting Point
Heart Failure treatment during pregnancy Angeles Alonso García Hospital Universitario Puerta de Hierro. Majadahonda. Madrid. Spain European Society of Cardiology. Stockholm. 29 August 2010 Starting Point
Cardiac Magnetic Resonance in pregnant women
 Cardiac Magnetic Resonance in pregnant women Chen SSM, Leeton L, Dennis AT Royal Women s Hospital and The University of Melbourne, Parkville, Australia alicia.dennis@thewomens.org.au Quantification of
Cardiac Magnetic Resonance in pregnant women Chen SSM, Leeton L, Dennis AT Royal Women s Hospital and The University of Melbourne, Parkville, Australia alicia.dennis@thewomens.org.au Quantification of
ISOLATED ANOMALOUS DEVELOPMENT OF MYOCARDIUM DURING FETAL LIFE: EXPERIENCE OF OUR CENTRE
 Azienda Ospedaliera Universitaria Integrata Verona ISOLATED ANOMALOUS DEVELOPMENT OF MYOCARDIUM DURING FETAL LIFE: EXPERIENCE OF OUR CENTRE C.Sandrini *, L.Rossetti *, M.Rebonato *, M.A.Prioli *, F.Bettinazzi,
Azienda Ospedaliera Universitaria Integrata Verona ISOLATED ANOMALOUS DEVELOPMENT OF MYOCARDIUM DURING FETAL LIFE: EXPERIENCE OF OUR CENTRE C.Sandrini *, L.Rossetti *, M.Rebonato *, M.A.Prioli *, F.Bettinazzi,
Sex differences in cardiovascular disease: What are we learning?
 Sex differences in cardiovascular disease: What are we learning? February 2018 Amy Sarma, MD MHS Cardiology and Advanced Echocardiography Fellow Massachusetts General Hospital 2 No disclosures 3 The scope
Sex differences in cardiovascular disease: What are we learning? February 2018 Amy Sarma, MD MHS Cardiology and Advanced Echocardiography Fellow Massachusetts General Hospital 2 No disclosures 3 The scope
Use of bromocriptine for the treatment of PPCM: are we there yet?
 Use of bromocriptine for the treatment of PPCM: are we there yet? Uri Elkayam, MD Professor of Medicine Professor of Obstetrics and Gynecology Director maternal cardiology University of Southern California
Use of bromocriptine for the treatment of PPCM: are we there yet? Uri Elkayam, MD Professor of Medicine Professor of Obstetrics and Gynecology Director maternal cardiology University of Southern California
Serum β-hcg levels between 12 to 20 weeks of gestation in prediction of. hypertensive disorders of pregnancy.
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Muthulakshmi D et al. Int J Reprod Contracept Obstet Gynecol. 2017 Aug;6(8):3347-3351 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20173263
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Muthulakshmi D et al. Int J Reprod Contracept Obstet Gynecol. 2017 Aug;6(8):3347-3351 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20173263
In , three studies described patients
 Heart 2001;85:337 341 VALVE DISEASE Should patients with asymptomatic mild or moderate aortic stenosis undergoing coronary artery bypass surgery also have valve replacement for their aortic stenosis? Shahbudin
Heart 2001;85:337 341 VALVE DISEASE Should patients with asymptomatic mild or moderate aortic stenosis undergoing coronary artery bypass surgery also have valve replacement for their aortic stenosis? Shahbudin
GSK Medicine: Study Number: Title: Rationale: Study Period: Objectives: Indication: Study Investigators/Centers: Data Source:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Course of Maternal Human Immunodeficiency Virus
 Infectious Diseases in Obstetrics and Gynecology 2:251-254 (1995) (C) 1995 Wiley-Liss, Inc. Effect of Successive Single-Gestation Pregnancies on the Course of Maternal Human Immunodeficiency Virus Disease
Infectious Diseases in Obstetrics and Gynecology 2:251-254 (1995) (C) 1995 Wiley-Liss, Inc. Effect of Successive Single-Gestation Pregnancies on the Course of Maternal Human Immunodeficiency Virus Disease
Overt and subclinical hypothyroidism among Bangladeshi pregnant women and its effect on fetomaternal outcome
 Bangladesh Med Res Counc Bull 21; : 52-57 Overt and subclinical hypothyroidism among Bangladeshi pregnant women and its effect on fetomaternal outcome Sharmeen M, Shamsunnahar A, Laita TR, Chowdhury SB
Bangladesh Med Res Counc Bull 21; : 52-57 Overt and subclinical hypothyroidism among Bangladeshi pregnant women and its effect on fetomaternal outcome Sharmeen M, Shamsunnahar A, Laita TR, Chowdhury SB
Gestational Diabetes. Gestational Diabetes:
 Gestational Diabetes Detection and Management Steven Gabbe, MD The Ohio State University Medical Center Gestational Diabetes: Detection and Management Learning Objectives: At the conclusion of this presentation,
Gestational Diabetes Detection and Management Steven Gabbe, MD The Ohio State University Medical Center Gestational Diabetes: Detection and Management Learning Objectives: At the conclusion of this presentation,
Dr.ssa Loredana Iannetta. Centro Cardiologico Monzino
 Dr.ssa Loredana Iannetta Centro Cardiologico Monzino Bicuspid aortic valve BAV is the most common congenital cardiac anomaly. Estimated incidence is 2% in general population. 4:1 male predominance. Frequency
Dr.ssa Loredana Iannetta Centro Cardiologico Monzino Bicuspid aortic valve BAV is the most common congenital cardiac anomaly. Estimated incidence is 2% in general population. 4:1 male predominance. Frequency
Acyclovir suppression to prevent recurrent genital herpes at delivery
 Infect Dis Obstet Gynecol 2002;10:71 77 Acyclovir suppression to prevent recurrent genital herpes at delivery L. L. Scott 1, L. M. Hollier 1, D. McIntire 1, P. J. Sanchez 2, G. L. Jackson 2 and G. D. Wendel,
Infect Dis Obstet Gynecol 2002;10:71 77 Acyclovir suppression to prevent recurrent genital herpes at delivery L. L. Scott 1, L. M. Hollier 1, D. McIntire 1, P. J. Sanchez 2, G. L. Jackson 2 and G. D. Wendel,
A descriptive study of the prevalence of hypothyroidism among antenatal women and foetal outcome in treated hypothyroid women
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Prasad DR et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1892-1896 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Prasad DR et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1892-1896 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
Cardiac disease in pre pr gnancy
 IN THE NAME OF GOD Cardiac disease in pregn nancy MITRAL STENOSIS 33 y/o G3L2(2c/s) GA 34 + 5 CC: LP & dyspnea PMHx: MS sinse 4 yrs ago due to Rheumatism PSHx: 2c/s DHx: metoral 50 mg q6h/ ASA/ Enoxaparin
IN THE NAME OF GOD Cardiac disease in pregn nancy MITRAL STENOSIS 33 y/o G3L2(2c/s) GA 34 + 5 CC: LP & dyspnea PMHx: MS sinse 4 yrs ago due to Rheumatism PSHx: 2c/s DHx: metoral 50 mg q6h/ ASA/ Enoxaparin
Salpingectomy for Sterilization
 Salpingectomy for Sterilization Change in Practice in a Large Integrated Health Care System 2011-2016 Journal Club November 15, 2017 Blaine Campbell, DO Salpingectomy for Sterilization: Change in Practice
Salpingectomy for Sterilization Change in Practice in a Large Integrated Health Care System 2011-2016 Journal Club November 15, 2017 Blaine Campbell, DO Salpingectomy for Sterilization: Change in Practice
PREGNANCY IN PATIENTS WITH A SYSTEMIC RV
 PREGNANCY IN PATIENTS WITH A SYSTEMIC RV Carole A. Warnes MD, FRCP Professor of Medicine, Mayo Clinic No disclosures 2013 MFMER slide-1 PREGNANCY : SYSTEMIC RV D - transposition after atrial switch procedure
PREGNANCY IN PATIENTS WITH A SYSTEMIC RV Carole A. Warnes MD, FRCP Professor of Medicine, Mayo Clinic No disclosures 2013 MFMER slide-1 PREGNANCY : SYSTEMIC RV D - transposition after atrial switch procedure
PREGNANCY AND CONGENITAL HEART DISEASE
 PREGNANCY AND CONGENITAL HEART DISEASE SIDDHARTH JADHAV M.D. Assistant Professor of Radiology E.B. Singleton Department of Pediatric Radiology Texas Children's Hospital COMMERCIAL DISCLOSURE - None Objectives
PREGNANCY AND CONGENITAL HEART DISEASE SIDDHARTH JADHAV M.D. Assistant Professor of Radiology E.B. Singleton Department of Pediatric Radiology Texas Children's Hospital COMMERCIAL DISCLOSURE - None Objectives
Peripartum Cardiomyopathy
 Peripartum Cardiomyopathy Denise Hilfiker-Kleiner Kardiologie & Angiologie MHH, Hannover Nothing to disclose Peri- or Postpartum Cardiomyopathy Peri- or postpartum cardiomyopathy (PPCM) is a disorder of
Peripartum Cardiomyopathy Denise Hilfiker-Kleiner Kardiologie & Angiologie MHH, Hannover Nothing to disclose Peri- or Postpartum Cardiomyopathy Peri- or postpartum cardiomyopathy (PPCM) is a disorder of
Acute Postpartum Pulmonary Edema: A Case Report
 Postpartum pulmonary edema 157 Acute Postpartum Pulmonary Edema: A Case Report Min-Po Ho 1, Wing-Keung Cheung 2, Kaung-Chau Tsai 1 Acute pulmonary edema after pregnancy is rare. Pulmonary emobolism, pneumonia,
Postpartum pulmonary edema 157 Acute Postpartum Pulmonary Edema: A Case Report Min-Po Ho 1, Wing-Keung Cheung 2, Kaung-Chau Tsai 1 Acute pulmonary edema after pregnancy is rare. Pulmonary emobolism, pneumonia,
The Impacts of Maternal Gestational Diabetes Mellitus (GDM) on Fetal Hearts *
 Biomed Environ Sci, 2012; 25(1): 15 22 15 Original Article The Impacts of Maternal Gestational Diabetes Mellitus (GDM) on Fetal Hearts * CHU Chen 1, GUI Yong Hao 1,#, REN Yun Yun 2, and SHI Li Ye 3 1.
Biomed Environ Sci, 2012; 25(1): 15 22 15 Original Article The Impacts of Maternal Gestational Diabetes Mellitus (GDM) on Fetal Hearts * CHU Chen 1, GUI Yong Hao 1,#, REN Yun Yun 2, and SHI Li Ye 3 1.
Maternal Outcome in Heart Disease in Pregnancy.
 RESEARCH AND REVIEWS: JOURNAL OF MEDICAL AND HEALTH SCIENCES Maternal Outcome in Heart Disease in Pregnancy. Vijaya Balasaheb Chinchawade*, Rekha G Daver, and Preeti Lewis. Govt Medical College, Miraj,
RESEARCH AND REVIEWS: JOURNAL OF MEDICAL AND HEALTH SCIENCES Maternal Outcome in Heart Disease in Pregnancy. Vijaya Balasaheb Chinchawade*, Rekha G Daver, and Preeti Lewis. Govt Medical College, Miraj,
Cardiac Resynchronization Therapy: Improving Patient Selection and Outcomes
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 899 904 DEVICE THERAPY CLINICAL DECISION MAKING Cardiac Resynchronization Therapy: Improving Patient Selection and Outcomes GURINDER S.
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 899 904 DEVICE THERAPY CLINICAL DECISION MAKING Cardiac Resynchronization Therapy: Improving Patient Selection and Outcomes GURINDER S.
Data from birth certificates in the United
 Chapter 36 Pregnancy in Preexisting Diabetes Thomas A. Buchanan, M.D. SUMMARY Data from birth certificates in the United States indicate that maternal diabetes complicates 2%-3% of all pregnancies, but
Chapter 36 Pregnancy in Preexisting Diabetes Thomas A. Buchanan, M.D. SUMMARY Data from birth certificates in the United States indicate that maternal diabetes complicates 2%-3% of all pregnancies, but
Cardiomyopathy. ACOI IM Board Review 2018 Martin C. Burke DO, FACOI
 Cardiomyopathy ACOI IM Board Review 2018 Martin C. Burke DO, FACOI No Disclosures Cardiomyopathies Definition: diseases of heart muscle 1980 WHO: unknown causes Not clinically relevant 1995 WHO: diseases
Cardiomyopathy ACOI IM Board Review 2018 Martin C. Burke DO, FACOI No Disclosures Cardiomyopathies Definition: diseases of heart muscle 1980 WHO: unknown causes Not clinically relevant 1995 WHO: diseases
CASE DISCUSSION. Dr JAYASREE VEERABOINA 2nd yr PG MS OBG
 CASE DISCUSSION Dr JAYASREE VEERABOINA 2nd yr PG MS OBG Normal Cardiovascular changes in Pregnancy CARDIAC OUTPUT 5 th wk -- starts 12 wks -- 30-35% 30-32 wks -- 40% During labour -- 50% After delivery
CASE DISCUSSION Dr JAYASREE VEERABOINA 2nd yr PG MS OBG Normal Cardiovascular changes in Pregnancy CARDIAC OUTPUT 5 th wk -- starts 12 wks -- 30-35% 30-32 wks -- 40% During labour -- 50% After delivery
The dos and don ts των νέων Κατευθυντηρίων Οδηγιών της Ευρωπαϊκής Καρδιολογικής Εταιρείας Για την καρδιαγγειακή νόσο στην εγκυμοσύνη
 The dos and don ts των νέων Κατευθυντηρίων Οδηγιών της Ευρωπαϊκής Καρδιολογικής Εταιρείας Για την καρδιαγγειακή νόσο στην εγκυμοσύνη Θωμάς Κ. Μακρής, MD FA, FES Συντονιστής Διευθυντής Καρδιολογικού Τμήματος
The dos and don ts των νέων Κατευθυντηρίων Οδηγιών της Ευρωπαϊκής Καρδιολογικής Εταιρείας Για την καρδιαγγειακή νόσο στην εγκυμοσύνη Θωμάς Κ. Μακρής, MD FA, FES Συντονιστής Διευθυντής Καρδιολογικού Τμήματος
Clinical study of cardiac diseases during pregnancy
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Kamat AV et al. Int J Reprod Contracept Obstet Gynecol. 2016 Mar;5(3):855-859 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Kamat AV et al. Int J Reprod Contracept Obstet Gynecol. 2016 Mar;5(3):855-859 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
Peripartum management of Rheumatic Heart Disease
 Peripartum management of Rheumatic Heart Disease Dr James Sartain Director of Anaesthesia & Perioperative Medicine Cairns & Hinterland Hospital & Health Service Talk outline Why (still) talk about RHD
Peripartum management of Rheumatic Heart Disease Dr James Sartain Director of Anaesthesia & Perioperative Medicine Cairns & Hinterland Hospital & Health Service Talk outline Why (still) talk about RHD
Imaging Cardiovascular Disease in Pregnancy
 Imaging Cardiovascular Disease in Pregnancy Karen Ordovas MD, MAS Associate Professor of Radiology and Medicine Director of Cardiac Imaging University of California San Francisco Cardiac MRI during pregnancy
Imaging Cardiovascular Disease in Pregnancy Karen Ordovas MD, MAS Associate Professor of Radiology and Medicine Director of Cardiac Imaging University of California San Francisco Cardiac MRI during pregnancy
PERIPARTUM CARDIOMYOPATHY: A CASE REPORT R. Sowjanya 1, K. Saritha 2, T. Shravya 3
 PERIPARTUM CARDIOMYOPATHY: A R. Sowjanya 1, K. Saritha 2, T. Shravya 3 HOW TO CITE THIS ARTICLE: R. Sowjanya, K. Saritha, T. Shravya. Peripartum Cardiomyopathy: A Case Report. Journal of Evolution of Medical
PERIPARTUM CARDIOMYOPATHY: A R. Sowjanya 1, K. Saritha 2, T. Shravya 3 HOW TO CITE THIS ARTICLE: R. Sowjanya, K. Saritha, T. Shravya. Peripartum Cardiomyopathy: A Case Report. Journal of Evolution of Medical
The Relationship between Random Urinary Protein-to-Creatinine Ratio and 24-hours Urine Protein in Diagnosis of Proteinuria in Mild Preeclampsia
 Received: 8/22/2004 Accepted: 4/20/2005 Original Article The Relationship between Random Urinary Protein-to-Creatinine Ratio and 24-hours Urine Protein in Diagnosis of Proteinuria in Mild Preeclampsia
Received: 8/22/2004 Accepted: 4/20/2005 Original Article The Relationship between Random Urinary Protein-to-Creatinine Ratio and 24-hours Urine Protein in Diagnosis of Proteinuria in Mild Preeclampsia
Familial Aggregation of Dilated Cardiomyopathy in Patients with Peripartum Cardiomyopathy
 Familial Aggregation of Dilated Cardiomyopathy in Patients with Peripartum Cardiomyopathy Tibazarwa K 1, Sliwa K 1, Wonkam A 2, Mayosi BM 1 1 Hatter Cardiovascular Research Institute, Department of Medicine,
Familial Aggregation of Dilated Cardiomyopathy in Patients with Peripartum Cardiomyopathy Tibazarwa K 1, Sliwa K 1, Wonkam A 2, Mayosi BM 1 1 Hatter Cardiovascular Research Institute, Department of Medicine,
Pregnancy and Heart Disease. Alexandra A Frogoudaki Adult Congenital Heart Clinic ATTIKON University Hospital
 Pregnancy and Heart Disease Alexandra A Frogoudaki Adult Congenital Heart Clinic ATTIKON University Hospital Pregnancy is not a state Hemodynamic changes During pregnancy Estrogens 1. Renin 2.
Pregnancy and Heart Disease Alexandra A Frogoudaki Adult Congenital Heart Clinic ATTIKON University Hospital Pregnancy is not a state Hemodynamic changes During pregnancy Estrogens 1. Renin 2.
First Trimester Fetal Echocardiography: Insight Into the Fetal Circulation
 First Trimester Fetal Echocardiography: Insight Into the Fetal Circulation Lisa K. Hornberger, MD Fetal & Neonatal Cardiology Program Department of Pediatrics, Division of Cardiology Department of Obstetrics
First Trimester Fetal Echocardiography: Insight Into the Fetal Circulation Lisa K. Hornberger, MD Fetal & Neonatal Cardiology Program Department of Pediatrics, Division of Cardiology Department of Obstetrics
AF Today: W. For the majority of patients with atrial. are the Options? Chris Case
 AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
Pregnancy outcome in chronic rheumatic heart disease
 J Obstet Gynecol India Vol. 59, No. 1 : January/February 2009 pg 41-46 Original Article Pregnancy outcome in chronic rheumatic heart disease Devabhaktuni Pratibha 1, Devineni Kiranmai 2, Vemuri Usha Rani
J Obstet Gynecol India Vol. 59, No. 1 : January/February 2009 pg 41-46 Original Article Pregnancy outcome in chronic rheumatic heart disease Devabhaktuni Pratibha 1, Devineni Kiranmai 2, Vemuri Usha Rani
Peripartum Cardiomypathy: A five year hospital-based analytical study
 Bahrain Medical Bulletin, Vol. 26, No. 3, September 2004 Peripartum Cardiomypathy: A five year hospital-based analytical study Khalil E Rajab, FRCOG* Abdulla A Issa, FRCOG** Objective: To review the incidence,
Bahrain Medical Bulletin, Vol. 26, No. 3, September 2004 Peripartum Cardiomypathy: A five year hospital-based analytical study Khalil E Rajab, FRCOG* Abdulla A Issa, FRCOG** Objective: To review the incidence,
AWHONN Oregon Section 2014
 AWHONN Oregon Section 2014 Carol J Harvey, MS, BSN, RNC-OB, C-EFM, CS Northside Hospital Atlanta Cherokee - Forsyth Hypertensive in Pregnancy Carol J Harvey, MS, RNC-OB, C-EFM Clinical Specialist Northside
AWHONN Oregon Section 2014 Carol J Harvey, MS, BSN, RNC-OB, C-EFM, CS Northside Hospital Atlanta Cherokee - Forsyth Hypertensive in Pregnancy Carol J Harvey, MS, RNC-OB, C-EFM Clinical Specialist Northside
A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia
 Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
CMQCC Preeclampsia Tool Kit: Hypertensive Disorders Across the Lifespan
 CMQCC Preeclampsia Tool Kit: Hypertensive Disorders Across the Lifespan Carol J Harvey, MS, BSN, RNC-OB, C-EFM, CS Northside Hospital Atlanta Cherokee - Forsyth New! Improving Health Care Response to Preeclampsia:
CMQCC Preeclampsia Tool Kit: Hypertensive Disorders Across the Lifespan Carol J Harvey, MS, BSN, RNC-OB, C-EFM, CS Northside Hospital Atlanta Cherokee - Forsyth New! Improving Health Care Response to Preeclampsia:
FETAL ECHO IN TWIN PREGNACY: MONOCHORIONIC TWINS DELHI CHILD HEART CENTER & INDRAPRASTHA APOLLO HOSPITAL NEW DELHI
 FETAL ECHO IN TWIN PREGNACY: MONOCHORIONIC TWINS DELHI CHILD HEART CENTER & INDRAPRASTHA APOLLO HOSPITAL NEW DELHI Scope of this talk Twin to Twin Transfusion TRAP Sequence Congenital Heart Defects in
FETAL ECHO IN TWIN PREGNACY: MONOCHORIONIC TWINS DELHI CHILD HEART CENTER & INDRAPRASTHA APOLLO HOSPITAL NEW DELHI Scope of this talk Twin to Twin Transfusion TRAP Sequence Congenital Heart Defects in
Isolated proteinuria in Chinese pregnant women with pre-eclampsia: Results of retrospective observational study
 Biomedical Research 2017; 28 (11): 5162-5166 ISSN 0970-938X www.biomedres.info Isolated proteinuria in Chinese pregnant women with pre-eclampsia: Results of retrospective observational study Jing Cai 1,
Biomedical Research 2017; 28 (11): 5162-5166 ISSN 0970-938X www.biomedres.info Isolated proteinuria in Chinese pregnant women with pre-eclampsia: Results of retrospective observational study Jing Cai 1,
Magnesium sulfate has an antihypertensive effect on severe pregnancy induced hypertension
 Hypertension Research In Pregnancy 11 S. Takenaka et al. ORIGINAL ARTICLE Magnesium sulfate has an antihypertensive effect on severe pregnancy induced hypertension Shin Takenaka 1, Ryu Matsuoka 2, Daisuke
Hypertension Research In Pregnancy 11 S. Takenaka et al. ORIGINAL ARTICLE Magnesium sulfate has an antihypertensive effect on severe pregnancy induced hypertension Shin Takenaka 1, Ryu Matsuoka 2, Daisuke
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy
 Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy Early diagnosis and good management of maternal thyroid dysfunction are essential to ensure minimal adverse effects on
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy Early diagnosis and good management of maternal thyroid dysfunction are essential to ensure minimal adverse effects on
A Case Report On Peripartum Cardiomyopathy
 Birdem Medical Journal Vol. 1, No. 1, July 2011 CASE REPORTS A Case Report On Peripartum Cardiomyopathy SAFDER AMB a, MIR SA b, MIAH BM c, TAMANNA RJ d, MOHIBULLAH AKM e Abstract: A 32 year-old primigravida
Birdem Medical Journal Vol. 1, No. 1, July 2011 CASE REPORTS A Case Report On Peripartum Cardiomyopathy SAFDER AMB a, MIR SA b, MIAH BM c, TAMANNA RJ d, MOHIBULLAH AKM e Abstract: A 32 year-old primigravida
Peripartum cardiomyopathy: a condition intensivists should be aware of
 Intensive Care Med (2003) 29:167 174 DOI 10.1007/s00134-002-1583-0 REVIEW Esther Beus Walther N. K. A. Mook Graham Ramsay Jan L. M. Stappers Hans W. H. M. Putten Peripartum cardiomyopathy: a condition
Intensive Care Med (2003) 29:167 174 DOI 10.1007/s00134-002-1583-0 REVIEW Esther Beus Walther N. K. A. Mook Graham Ramsay Jan L. M. Stappers Hans W. H. M. Putten Peripartum cardiomyopathy: a condition
Diabetes in Pregnancy
 Disclosure Diabetes in Pregnancy I have no conflicts of interest to disclose Jennifer Krupp, MD Maternal Fetal Medicine St. Marys Hospital/SSM Health Madison, WI Objectives Classification of Diabetes Classifications
Disclosure Diabetes in Pregnancy I have no conflicts of interest to disclose Jennifer Krupp, MD Maternal Fetal Medicine St. Marys Hospital/SSM Health Madison, WI Objectives Classification of Diabetes Classifications
Pregnancy and Heart Disease Sharon L. Roble, MD Echo Hawaii 2016
 1 Pregnancy and Heart Disease Sharon L. Roble, MD Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Cardiovascular Effects of Pregnancy Anatomic Ventricular muscle mass increases
1 Pregnancy and Heart Disease Sharon L. Roble, MD Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Cardiovascular Effects of Pregnancy Anatomic Ventricular muscle mass increases
A randomized trial of azithromycin versus amoxicillin for the treatment of Chlamydia trachomatis in pregnancy
 Infect Dis Obstet Gynecol 2001;9:197 202 A randomized trial of azithromycin versus amoxicillin for the treatment of Chlamydia trachomatis in pregnancy Jennifer Kacmar, Emily Cheh, Andrea Montagno and Jeffrey
Infect Dis Obstet Gynecol 2001;9:197 202 A randomized trial of azithromycin versus amoxicillin for the treatment of Chlamydia trachomatis in pregnancy Jennifer Kacmar, Emily Cheh, Andrea Montagno and Jeffrey
New Agents for Heart Failure: Ivabradine Jeffrey S. Borer, MD
 New Agents for Heart Failure: Ivabradine Jeffrey S. Borer, MD Professor of Medicine, Cell Biology, Radiology and Surgery Director, The Howard Gilman Institute for Heart Valve Disease and the Schiavone
New Agents for Heart Failure: Ivabradine Jeffrey S. Borer, MD Professor of Medicine, Cell Biology, Radiology and Surgery Director, The Howard Gilman Institute for Heart Valve Disease and the Schiavone
Peripartum Cardiomyopathy. Kyleah Bowder. Concordia University
 Peripartum Cardiomyopathy 1 Peripartum Cardiomyopathy Kyleah Bowder Concordia University Peripartum Cardiomyopathy 2 Cardiomyopathy is the deterioration of the myocardium in the heart. The myocardium is
Peripartum Cardiomyopathy 1 Peripartum Cardiomyopathy Kyleah Bowder Concordia University Peripartum Cardiomyopathy 2 Cardiomyopathy is the deterioration of the myocardium in the heart. The myocardium is
Peripartum cardiomyopathy: Frequency and predictors and indicators of clinical outcome
 1517 ORIGINAL ARTICLE Peripartum cardiomyopathy: Frequency and predictors and indicators of clinical outcome Shakira Perveen, 1 Jahanara Ainuddin, 2 Shazia Jabbar, 3 Khalida Soomro, 4 Arif Ali 5 Abstract
1517 ORIGINAL ARTICLE Peripartum cardiomyopathy: Frequency and predictors and indicators of clinical outcome Shakira Perveen, 1 Jahanara Ainuddin, 2 Shazia Jabbar, 3 Khalida Soomro, 4 Arif Ali 5 Abstract
Critical Care in Obstetrics: An Innovative and Integrated Model for Learning the Essentials
 Critical Care in Obstetrics: An Innovative and Integrated Model for Learning the Essentials Pregnancy and Congenital Heart Disease Case Review Heidi M. Connolly, M.D. Professor of Medicine Chair for Education
Critical Care in Obstetrics: An Innovative and Integrated Model for Learning the Essentials Pregnancy and Congenital Heart Disease Case Review Heidi M. Connolly, M.D. Professor of Medicine Chair for Education
Effect of Various Degrees of Maternal Hyperglycemia on Fetal Outcome
 ORIGINAL ARTICLE Effect of Various Degrees of Maternal Hyperglycemia on Fetal Outcome ABSTRACT Shagufta Tahir, Shaheen Zafar, Savita Thontia Objective Study design Place & Duration of study Methodology
ORIGINAL ARTICLE Effect of Various Degrees of Maternal Hyperglycemia on Fetal Outcome ABSTRACT Shagufta Tahir, Shaheen Zafar, Savita Thontia Objective Study design Place & Duration of study Methodology
Heart failure associated with pregnancy and the peripartum
 Contemporary Reviews in Cardiovascular Medicine Peripartum Cardiomyopathy Zolt Arany, MD, PhD; Uri Elkayam, MD Abstract Peripartum cardiomyopathy is a potentially life-threatening pregnancy-associated
Contemporary Reviews in Cardiovascular Medicine Peripartum Cardiomyopathy Zolt Arany, MD, PhD; Uri Elkayam, MD Abstract Peripartum cardiomyopathy is a potentially life-threatening pregnancy-associated
ESC Guidelines on the Management of Cardiovascular Diseases during Pregnancy
 ESC Guidelines on the Management of Cardiovascular Diseases during Pregnancy Task force on the management of CVD during pregnancy of the ESC Chair: Vera Regitz-Zagrosek, Charite, Berlin None DECLARATION
ESC Guidelines on the Management of Cardiovascular Diseases during Pregnancy Task force on the management of CVD during pregnancy of the ESC Chair: Vera Regitz-Zagrosek, Charite, Berlin None DECLARATION
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
