There exists little controversy regarding the clinical
|
|
|
- Francine Poole
- 6 years ago
- Views:
Transcription
1 Pressure-Sensing Guidewire Analysis in RAS Adapting this coronary-based technology to optimize functional renal artery revascularization could have significant clinical implications. BY DAVID E. ALLIE, MD; CHRIS J. HEBERT, RT, RCIS; AND CRAIG M. WALKER, MD There exists little controversy regarding the clinical benefits of renal artery (RA) PTA/stenting in hemodynamically significant renal artery stenosis (RAS) in several patient subsets, including (1) those with poorly controlled hypertension on multiple antihypertensive medications or those who are intolerant of medications; (2) patients with ischemic nephropathy for preservation of renal function in the patient demonstrating deteriorating renal function and/or renal size; or (3) patients with coronary ischemia, angina, congestive heart failure, or flash pulmonary edema exacerbated by RAS or renovascular hypertension. 1-4 Unfortunately, RA PTA/stenting has shown no objective clinical benefit in 30% to 40% of patients. 5,6 Therefore, there is significant controversy in several other aspects of RAS treatment, including (1) the definition and identification of a hemodynamically or physiologically (functional) significant RAS; (2) treatment in unilateral or bilateral moderate (50%-70%) RAS; and (3) any treatment recommendation in RA in-stent restenosis (ISR). 5-8 Several reports have documented a decline in renal function after PTA/stenting and high ISR rates (12%-29%), further leading to controversy in treating any RAS patient This will continue to be true for ad hoc renal interventions performed during drive-by cardiac catheterization until outcomes are predictable, improved, and complications minimized Meticulous technique and use of distal protection devices to reduce cholesterol and atherosclerotic emboli, and contrast-induced nephrotoxicity, are important issues related to best outcomes, but there is little consensus on the optimal methods of identifying significant RAS and no consensus correlating anatomic RAS to hemodynamic or physiological (functional) revascularization in RAS. Figure 1. Regulation of blood flow in a normal and an atherosclerotic RA. In the normal RA, the vessel and microvascular vessels dilate with papaverine provocation to meet metabolic demands. In the diseased vessel, during rest, there is a drop in pressure ( P) across the stenosis. During provocation, the RA constricts, the P across the stenosis increases, and the microcirculation has limited capacity for dilatation. The increase of blood flow is inadequate to meet the increased metabolic demands. An FFRren model would be reduced (FFRren = 0.40). 14 I ENDOVASCULAR TODAY I OCTOBER 2004
2 CURRENT RAS ASSESSMENT Conventional angiography with or without digital subtraction angiography (CADSA) is still considered the gold standard, but it is well known that CADSA has significant limitations. 14,15 Multidetector CT angiography (MDCTA) may prove to be more sensitive than CADSA in detecting anatomic RAS, but it is not widely available at this time and provides no functional information. 16 Discrete ostial lesions and complex, especially oblique, RA ostial origins are common and add to the difficulty in identifying and quantifying RAS. Patients with RA ISR are increasingly returning for evaluation and treatment, and again, there currently exists no consensus treatment or guidelines regarding diagnosis or repeat revascularization. 10,17,18 Translesional systolic pressure gradients (TSPG) have recently been advocated by Rundback et al as a standard guideline for reporting RA revascularization in clinical trials, but limitations have been identified with TSPG determinations with 4-F to 6-F end-hole catheters and the threshold values. 15,19 There is no consensus as to the exact degree of RAS or minimal TSPG justifying revascularization, and neither CADSA nor TSPG provide physiological RAS information. 14,15 Radionuclide scans, renal vein renin assays, captopril renography, and duplex ultrasound resistive index have been advocated as methods to physiologically assess RAS, but all have significant limitations. Additionally, these methods are infrequently used as physiological or functional measures of RAS and therefore are rarely used for decision making in RA revascularization THE PRESSUREWIRE AND FRACTIONAL FLOW RESERVE It is becoming increasingly incumbent upon clinicians to identify and document objective indications for treatment based on both anatomic and physiologic parameters and have data to support treatment and predict outcomes. With significant controversy still surrounding RA PTA/stent- A B C Figure 2. Schematic of the RADI PressureWire (RADI Medical Inc., Uppsla, Sweden). Note the 31-cm flexible tip and the 3-cm radiopaque soft tip distal to the 1.8-mm sensor (A). Magnification of the fiberoptic pressure sensor. The element modulates an optical reflection with pressure-induced elastic movements using an emitting diode in the control unit as a light source (B). The RADIAnalyzer demonstrating a 0.71 FFRmyo (C). 16 I ENDOVASCULAR TODAY I OCTOBER 2004
3 Figure 3. PressureWire TSPG analysis; the guiding catheter is engaged at the RA ostia to facilitate the PressureWire translesional placement (A). The guide catheter is pulled back into the aorta demonstrating a 30-mm Hg peak-to-peak systolic gradient (B). Re-engagement of the guide catheter into RA, avoiding crossing the lesion, followed by RA papaverine injection (C). The guide catheter is immediately pulled back into the aorta demonstrating a 70-mm Hg peak-to-peak systolic after papaverine provocation gradient (D). ing, no other vascular territory would benefit more from a method or tool that would allow functional revascularization decision making than RAS, much like functional assessment for coronary artery disease in the cath lab. The PressureWire is such a tool that allows acquisition of pressure signals on a.014-inch coronary angioplasty guidewire, eliminating false gradients due to large catheters. Use of the PressureWire and physiologic measurements have been found to be beneficial in percutaneous coronary intervention (PCI) in identifying ischemic (functional) lesions, optimizing stent deployment, and in predicting and improving outcomes There are limited data describing the use of the PressureWire in peripheral vascular disease and no validated data reporting the utility in determining the fractional flow reserve (FFR) in RAS (FFRren) Reports by Pijls, Bech, DeBruyne, and Kern have eloquently described the concept of myocardial FFR (FFRmyo) as an accurate, safe, simple, cost-effective, and lesion-specific invasive index of the functional severity of a coronary artery stenosis that is not affected by the microcirculation or hemodynamic variability. 24,26-28 Using reasonable clinical assumptions, we have investigated the use of the FFR concept analogously in indexing the functional severity of RAS. The FFR is defined as the maximal blood flow in the presence of a stenosis divided by the theoretical maximum flow without a stenosis; therefore, a normal value (ratio) is 1.0. The FFR does not directly measure blood flow, but it is the transtenotic pressure across a stenosis measured at peak blood flow after administration of an arteriolar vasodilator and indexed for the aortic driving pressure. Several key concepts are that a stenotic lesion obstructs flow only if a pressure gradient develops across the stenosis with maximal hyperemic arteriolar and microvascular dilation. If there is no pressure gradient, the lesion is not the site of a functional obstruction and PTA/stenting cannot physiologically improve blood flow. Because flow can be expressed as the ratio of aortic driving pressure to resistance (Rmin), maximal attainable blood flow through the end organ equals the ratio of perfusion pressure (PP) across the end organ (distal RA pressure minus renal venous pressure) and the Rmin. This assumption has been proven true for the heart but remains uninvestigated for the kidney. Using this analogous assumption for the kidney, if there is no RAS, the PP across the RAS/kidney equals Pa Pv, where Pa = mean aortic pressure and Pv = venous pressure. In RAS, the PP across the kidney has decreased to Pd Pv, where Pd = hyperemic RA pressure distal to the lesion. Therefore, FFR = (Pd Pv) Rmin (Pa Pv) Rmin and, because at maximum RA vasodilation, R is constant and minimal, the Rmin cancel resulting in: FFR = (Pd Pv) (Pa Pv) Because Pv is minimal and not increased, the FFR is further simplified: FFR = Pd Pa when Pd and Pa are measured simultaneously by a guiding catheter and pressure sensing guidewire after maximum vasodilatation (Figure 1). THE BENEFITS OF FFRMYO IN PCI: A POTENTIAL IN RAS Multiple reports have validated the utilization of FFRmyo, including benefits in identifying functional severity of coronary stenosis, identifying ischemic culprit lesions, facilitating decision making in multivessel coronary artery disease, assessment of intermediate lesions, optimization of PCI stent deployment and outcomes, and in assessing left main disease, ostial lesions, bifurcations, and serial stenosis. Pijls et al demonstrated an FFR <0.75 (the mean pressure distal to the stenotic lesion or <75% of the mean aortic pressure) correlated with functional stenosis and inducible ischemia on exercise testing, thallium scans, and stress echocardiograms. 23 Pijls et al also showed that successful PCI in patients with FFR <0.75 relieved symptoms, improved functional class, and reversed ischemia on postprocedural functional stress testing and that PCI in intermediate lesions with FFRmyo >0.75 and worse outcomes than medical therapy OCTOBER 2004 I ENDOVASCULAR TODAY I 17
4 A B C D E F Figure 4. An RA ISR case demonstrating use of the PressureWire. An 80% to 90% right RA ISR lesion by CADSA (A). A 70-mm Hg peak-to-peak PressureWire TSPG after papaverine provocation (B). A 2-mm eccentric excimer laser probe begins 4-quadrant atheroablation (C). Low-pressure PTA after laser (D). Postlaser PTA PressureWire TSPG confirms obliteration (<5 mm Hg) of the gradient (E). Postprocedural CADSA results (F). alone. 23 Hanekamp et al compared quantitative coronary angiography, intravascular ultrasound (IVUS), and FFR to assess optimal PCI stent deployment in 81 patients paired with IVUS and quantitative coronary assessment. 25 A concordance was found between FFR/IVUS, IVUS/QCA, and FFR/QCA of 91%, 48%, and 46%, respectively, therefore proposing FFR as a rapid and cheaper alternative to IVUS for optimizing stent deployment and outcomes. Pijls et al analyzed FFR-facilitated, post-pci outcomes at 6 months and found that FFR was a strong predictor of outcomes, with event rates of 4.9%, 6.2%, 20.3%, and 29.5%, in the post-pci FFR group >0.85, 0.90 to 0.95, 0.80 to 0.90, and <0.80, respectively (P >.001). 26 In a randomized trial, Bech et al determined the appropriateness of PCI in patients with moderate coronary artery disease who did not have documented inducible ischemia and who were referred for PCI. An FFR of < or >0.75 identified those patients who benefited from PCI (<0.75 before and >0.75 after PCI) and proved patients with FFR >0.75 could be safely treated medically. 27 Utilizing the proven concepts with the PressureWire in PCI, and considering the recognized limitations with renal PTA/stent, we began a PressureWire safety and feasibility analysis in treating 89 patients with RAS. This analysis in RAS included a comparison between traditional 4-F TSPG, PressureWireobtained TSPG, FFRren, percent stenosis by MDCTA and CADSA, and an analysis of our clinical decision making in the cath lab based on this anatomic and functional information. STUDY METHODOLOGY/TECHNIQUE The.014-inch RADI PressureWire is a high-fidelity, solidstate, electronic.014-inch pressure-sensing, coronary angioplasty guidewire with wire characteristics comparable to a conventional high-torque, floppy angioplasty guidewire (Figure 2). The pressure sensor is located 3 cm proximal from the wire tip, allowing ample room for wire manipulation without requiring repeated wire tip crossing. For our RAS TSPG analysis and PressureWire functional analysis, the PressureWire is introduced through a 4-F catheter, and is calibrated and advanced into the RA. The lesion is crossed positioning the sensor distal to the stenosis. The guiding catheter tip is placed 5 mm to 10 mm into the aorta (away from the renal ostium) and the sensor tip is placed 3 mm to 5 mm distal to the lesion. A resting PressureWire TSPG is first analyzed with the signal RADI analyzer by recording the peak-to-peak systolic pressure difference between the pressure sensor located distal to the lesion and the guiding catheter tip placed well into the aorta. The 4-F guiding catheter is then placed across the lesion and a traditional pull-back, peak-to-peak systolic TSPG is recorded as the catheter is pulled back 5 mm to 10 mm into the aorta (Figure 3). We used papaverine as our provocative (hyperemic vaso- 18 I ENDOVASCULAR TODAY I OCTOBER 2004
5 CRITERIA FOR RAS: FUNCTIONAL ASSESSMENT OF THE RENAL ARTERY STENOSIS By Morton J. Kern, MD How can one conclusively demonstrate that renal artery stenting is necessary and that the procedure is justified for its risks and clinical benefits to the patient subsets of poorly controlled hypertension despite multiple medications, stabilization of deteriorating renal function and renal size, and prevention of episodic severe pulmonary edema in patients with coexisting coronary artery disease and hypertension? Which degree of renal stenosis is important, by which measurement and, most of all, how can this approach be best quantified? The answers to these questions spark controversy because poor results occur in 30% to 40% of patients after renal artery stenting who have no demonstrable clinical benefit. Did the procedure fail or was the procedure unnecessary? We describe the issues with regard to the definition and identification of physiologically functional significant renal artery stenosis and highlight the application of transstenotic pressure measurements and their role in identifying those renal stenoses thought to be functionally significant lesions. The fundamental problem with all angiographic definitions of arterial lesion severity is that for an eccentric orifice (which comprise the majority of all angiographic stenoses) the two-dimensional geometry fails to translate into a representative physiologic response (ie, a severe narrowing does not always have a severe pressure gradient). This disparity between angiographic percent stenosis and true physiologic stenosis is well understood from the coronary artery literature, especially with the wide appreciation of the findings of intravascular ultrasound imaging. A large discrepancy between the angiographic percent diameter stenosis and the IVUS-identified lumen cross-sectional area has been repeatedly identified. Moreover, the physiologic importance of angiographic lesions is widely disparate as evidenced not only by stress testing results but also for hemodynamic assessments. For coronary stenoses, some severe lesions have no evidence of flow impairment by resistance or pressure gradient, whereas other more modest narrowings have a significant physiologic impact. The same issue applies to the renal artery and its attendant stenosis with angiographic difficulties arising, especially in the ostial regions of these vessels. For ostial lesions in coronary arteries, a significant variance between physiologic findings and the percent diameter stenosis is reported. The physiology of the renal artery stenosis differs from that of coronary artery stenosis in that a significant coronary stenosis has a predominant diastolic gradient, whereas the renal artery has a systolic pressure gradient (as do all peripheral arterial stenoses). For the kidney, peak systolic pressure differences between the perfusion head in the aorta and the distal recipient bed in the kidney probably play more of a role because there is equilibration of the diastolic pressures. The differences between the mean arterial pressure values may be minimal even at maximal flow, but peak systolic perfusion pressure may be a more sensitive indicator than in the coronary bed. A modest or mild systolic translesional pressure loss may indicate a significant renal perfusion deficit. Because the physiology of the kidney differs from that of the heart in both the phasic nature of the pressure difference and in the resistance bed responses to common vasodilators, the FFR concept for the renal arteries has not yet been adequately defined. Moreover, even if the FFR concept is applied, the best hyperemic stimuli to assess the microcirculation of the renal bed remain unknown. Finally, with regard to the best measurement of translesional gradients and the hemodynamic criteria, all previous studies have used small catheters (at least 4 F or larger). The difference between a 4-F catheter and a.014-inch pressure guidewire gradient is significant and consistent. The absence of a pressure gradient with a 4-F catheter certainly would be a pressure gradient of 0 with the guidewire, but the converse is not true. A modest or even important gradient with the 4-F catheter can also be a gradient of 0 with the.014-inch pressure wire. The use of pressure gradients based on catheter measurements has led to the assumption that treatment of renal artery stenosis with such gradients was either ineffective or unsuccessful instead of realizing that stenting a true low- or no-gradient stenosis was not necessary and thus no clinical difference would be seen or expected. The importance of the functional assessment of renal arteries prior to revascularization will improve outcome, provide accurate assessment of the endpoint of the intervention, identify suboptimal stent deployment in some conditions, and will identify additional angiographic anomalies, which may or may not be physiologically significant. The documentation of the outcome and quantitation of the indications to treat the renal artery stenosis will provide the best clinical outcomes and reshape our current activity in this field. Morton J. Kern, MD, is Professor of Medicine, Director Cardiac Catheterization Lab, St. Louis University, St. Louis, Missouri. Dr. Kern amy be reached at (314) ; kernm@slu.edu. 1. Zaiee A, Parham WA, Hermann SC, et al. Lack of relation between imaging and physiology in ostial coronary artery narrowing. Am J Cardiol. 2004;93: I ENDOVASCULAR TODAY I OCTOBER 2004
6 dialation) agent because it is known as a potent peripheral arterial vasodilator. To date, there are no published data using papaverine in RAS or intra-arterial RA injection. In our initial experience, we used 30 mg of papaverine because it was a familiar surgical dose used safely in the OR (internal mammary artery preparation during CABG, intra-arterial SFA, or popliteal artery injection during thromboembolectomy). Recently, we have found a 20-mg papaverine injection to be effective, and this is now our routine provocation dose for PressureWire TSPG and FFRren. The RA injection is made as a rapid hand-held 20-mg injection of papaverine in 10 ml of saline. The renal ostia is engaged with the guiding catheter, and we avoid totally crossing the lesion to minimize catheter manipulation at the ostia and lesion. The catheter is immediately pulled back into the aorta for PressureWire TSPG determination because the papaverine response occurs within 5 to 15 seconds. DeBruyne has also found 20 mg of papaverine to be equivalent to adenosine (40 µg/kg per min) for FFRmyo. 33 There was no difference in clinical response between 20 mg and 30 mg of papaverine intra-arterial injection. Mixing papaverine and heparin must be avoided to eliminate precipitation. For FFRren analysis, baseline Pa and Pd measurements are obtained and recorded by the RADI analyzer. RA vasodilatation is performed by an intra-arterial injection of 20 mg of papaverine. Simultaneous phasic and mean aortic and distal RA pressures are monitored and FFRren is calculated as the ratio of Pd/Pa at maximal hyperemic vasodilation. If renal revascularization is performed, a postprocedural Pressurewire TSPG and FFRren is performed (as described previously) and recorded. Questionnaire and Decision Making A simple questionnaire was completed in our 89 RAS cases by the treating clinician assessing the influence of this information on immediate procedural decision making comparing the actual procedure performed with the clinician s best-predicted planned procedure. The clinician was first asked the best prediction of the treatment (stent or no stent) before the PressureWire analysis. The clinician was then asked (A) Did the TSPG or FFRren significantly influence procedure decision making? (yes/no). And, if yes, (B) stenting? (yes/no) or no stenting? (yes/no). Twenty-nine of 89 (32.5%) reported, yes, this information significantly influenced decision making. Nineteen of 89 (21.3 %) reported stented or added a stent, in cases in which they did not predict a stent would be used. A significant procedural decision-making change was seen most often in patients with a moderate RAS identified on MDCTA or during a previous CADSA in which the RAS was estimated to be 50% to 70%. In these 19 patients, the clinician performed RA PTA/stenting in lesions believed to be significant only after papaverine provocation and a TSPG was found to be >20 mm Hg. In five cases, a >10 mm Hg TSPG found immediately after PTA/stent occurred and resulted in identification of three missed ostia and two underdeployed stents. Each case was corrected immediately and resulted in postprocedural TSPGs <5 mm Hg. IVUS was not routinely performed in this analysis. In 10 of 89 cases (11.2%), a stent was not deployed when resting and postprovocation TSPGs were <20 mm Hg in cases in which the CADSA or MDCTA had predicted >60% to 70% stenosis. RESULTS TSPG/FFRren Analysis There were no PressureWire or papaverine-related complications. Eighty-nine patients had 4-F catheter and PressureWire TSPG analysis with FFRren and were compared to CADSA. Additionally, 48 of 89 patients (56.4%) were compared to MDCTA. CADSA and MDCTA percent stenosis did not strongly correlate to 4-F catheter TSPG (r 2 = 0.224) but did correlate strongly with PressureWire TSPG (r 2 = 0.610). A FFRren of <0.75 did not strongly correlate with CADSA (r 2 = 0.210), MDCTA (r 2 = 0.191), or 4-F catheter TSPG (r 2 = 0.246), raising the issue that the current FFRmyo concept may be inappropriate in the renal vasculature (FFRren). To Stent? Or Not to Stent? The identification and decision to treat moderate-tointermediate angiographically significant RAS (60%-70% stenosis or 50% luminal diameter reduction) is not always straightforward considering the known limitations of CADSA, MDCTA, and TSPG. These intermediate lesions may be functionally significant. No consensus exists as to the minimal TSPG required to treat RAS, and there is a lack of data available to use as a guideline for treatment. Earlier RA PTA/stent trials accepted 5 mm Hg transcatheter TSPG to define a suboptimal/failed PTA requiring stenting. A 20 mm Hg TSPG has been recently proposed for RAS clinical trials, but this may be an arbitrary number without any physiological basis. 19 Considering the lack of a consensus RAS treatment guideline, we currently use >20 mm Hg TSPG, resting or after injection of 20 mg of papaverine, as an indication to primarily treat RAS and <5 mm Hg PressureWire TSPG post-pta/stent to define our procedural success and rule out missed lesions, dissections, or stent underdeployment. More than 30% of our cases experienced major clinical decision changes after papaverine provocation, with approximately 20% stented and 10% not stented in cases in which these treatments were not definitely planned. The PressureWire potentially helped identify those patients who have angiographically moderate but functionally significant 22 I ENDOVASCULAR TODAY I OCTOBER 2004
7 TABLE 1. POTENTIAL BENEFITS OF PRESSURE WIRE ANALYSIS AND FUNCTIONAL RENAL REVASCULARIZATION Improved accuracy in identification of RAS Identification of physiologically significant RAS Functional assessment of intermediate (50%-70%) lesions Improved treatment staging of bilateral RAS Identification of angiographically significant but physiologically nonsignificant RAS Optimizing stent deployment Identifying intraprocedural technical problems (dissections, missed ostias, residual gradients, underdeployed stents, etc.) Improved prediction of clinical outcomes with/without stenting Objective documentation of indications to treat (PTA/stent) Less contrast utilization Less fluoroscopic and radiographic exposure Identification and treatment of RA ISR lesions Decrease RA ISR rates Identify the 30%-40% of poor clinical responders after PTA/stenting Overall improved clinical outcomes RAS who would not be offered PTA/stenting who functionally need it, and therefore should receive functional benefit from PTA/stenting. Conversely, the PressureWire may have the potential to identify those patients who are not likely to clinically benefit from RA PTA/stenting, therefore not exposing them to the 12% to 29% RA ISR rates and the current 30% to 40% of RAS patients not receiving clinical benefit after RA PTA/stenting. Long-term clinical followup will be required to answer these questions. In our analysis, 12 of 89 (13.5%) had RA ISR, and identifying and treating this ISR patient population is problematic. Traditional CADSA has significant limitations in diagnosing RA ISR, but MDCTA allows improved imaging, and curved coronal imaging and flow probing software have allowed more accurate assessment in RA ISR. 16 Treatment for RA ISR is not defined with results of PTA only or restenting reporting approximately 50% restenosis rates. 17,18,30,34-36 We now use 4-quadrant excimer laser atheroablation as our treatment of choice in RA ISR patients and we now use the PressureWire to gauge the number of laser catheter passes required to achieve our goal of a TSPG of <5 mm Hg. This technique has decreased our need for aggressive repeat high-pressure PTA and the need for repeat stenting (stent sandwich) (Figure 4). We recently reported this technique in 25 RA ISR patients with a 92% procedural success rate and a 10% 6-month >50% restenosis rate as determined by duplex ultrasound. 36 Optimizing Renal Stent Deployment RA ISR has been reported in 12% to 29% of cases and is dependent on vessel size, minimal luminal diameters (MLD) or acute procedural gain after stent placement, and optimal stent deployment technique. 12 Lederman et al reported MLD after RA PTA/stent and vessel size correlated with clinical outcomes and reported RA ISR rates of 36%, 15.8%, and 6.5% for vessels <4.5 mm, 4 6 mm, and >6 mm, respectively. 12 Suboptimal stent expansion, missed ostial lesions, and unrecognized distal dissections are all implicated in increased RA restenosis rates and potentially could be identified periprocedurally by TSPG and/or FFRren, allowing for immediate correction and optimized outcomes similar to the reports in PCI by Hanekamp et al and Pijls et al. 23,25 This study has confirmed the work of Colyer et al and identified the PressureWire TSPG to be more accurate than 4-F catheter TSPG, therefore highlighting the known limitation of measuring TSPG with guiding catheters. 19 The 4-F catheter TSPG method is still advocated as a practice guideline and is used in clinical trials. 19 Although we were unable to identify a strong correlation between FFRren and TSPG, we found the PressureWire TSPG to highly correlate with CADSA and MDCTA and to be a simple and accurate means to document intraprocedure treatment decisions both before and after stenting. The >30% rate of influence on clinical decision making seen in our 89 patients is the first published data accessing intraprocedure decision making in treating RAS. We now use PressureWire analysis for decision making in treating celiac and superior mesenteric artery disease and we are investigating other utilizations in peripheral vascular disease. Similar to RAS, treating visceral arterial disease is limited by diagnostic imaging accuracy, identification of functional stenosis, and high ISR rates. 37 Limitations This small single-center study has shown the safety and feasibility of using the PressureWire in accessing RAS but has not provided clinical follow-up or demonstrated clinical efficacy and will require long-term multicenter validation. This study has not unraveled the conundrum between assessing RAS by objective imaging, TSPG, identification of functional RAS, and correlation between RAS, clinical manifestations, and outcomes. This study is, however, a first step in providing insight into optimizing functional renal revascularization. The lack of a correlation between the clinical usefulness of 24 I ENDOVASCULAR TODAY I OCTOBER 2004
8 the FFRmyo <0.75 and an analogous FFRren validation in this report should not be surprising because extrapolating experience from PCI and the coronary bed into the renal artery bed is likely not that simple, further underscoring the differences in coronary artery disease and peripheral vascular disease. This study has confirmed that pressure gradients (TSPG) obtained by PressureWire measurements are more accurate in identifying anatomic RAS than gradients obtained by catheter measurements, MDCTA, or CADSA imaging. CONCLUSION The many current limitations in assessing and treating RAS and the proven PCI benefits of FFRmyo are compelling reasons to further pursue PressureWire investigations in peripheral vascular disease and identify the keys to developing a FFRren analogous to FFRmyo. The potential benefits of FFRren in RAS, if analogous to the benefits of FFRmyo in PCI, would have significant clinical implications (Table 1). We now recommend the RADI PressureWire analysis on all RAS cases utilizing a PressureWire TSPG of >20 mm Hg (resting or after papaverine injection) as objective documentation to treat. Our goal is to achieve 5 mm Hg PressureWire gradient (resting and postprovocation) after PTA/stenting to define optimal treatment. We now rely heavily on PressureWire TSPG, not catheter gradients or angiography, in our clinical decision making during RAS treatment. It is now time to reproduce the elegant work by Pijls, DeBruyne, Bech, and Kern in PCI and FFRmyo in peripheral arterial disease, and validate an analogous renal model with a goal to provide more optimal functional revascularization in RAS and other peripheral vascular beds, including celiac, mesenteric, and infrainguinal arterial disease. David E. Allie, MD, is Director of Cardiothoracic and Endovascular Surgery at the Cardiovascular Institute of the South in Lafayette, Louisiana. He has disclosed that he holds no financial interest in any product or manufacturer mentioned herein. Dr. Allie may be reached at (800) ; David.Allie@cardio.com. Chris J. Hebert, RT, RCIS, is Director of Cardiovascular Services at the Cardiovascular Institute of the South in Lafayette, Louisiana. He has disclosed that he holds no financial interest in any product or manufacturer mentioned herein. Mr. Hebert may be reached at (800) ; Chris.Hebert@cardio.com. Craig M. Walker, MD, is Medical Director and Founder, Cardiovascular Institute of the South in Houma, Louisiana. He has disclosed that he holds no financial interest in any product or manufacturer mentioned herein. Dr. Walker may be reached at (800) ; Craig.Walker@cardio.com. 1. Bush RL, Najibi S, MacDonald MJ, et al. Endovascular revascularization of renal artery stenosis: technical and clinical results. J Vasc Surg. 2001;33: Palmaz JC. The current status of vascular intervention in ischemic nephropathy. J Vasc Intervent Radiol. 1998;9: Dorros G, Jaff M, Mathiak L, He T, for the Multicenter Registry Participant. Multicenter Palmaz stent renal artery stenosis revascularization registry report: Four-year follow-up of 1,058 successful patients. Cathet Cardiovasc Intervent. 2002;55: Henry M, Amor M, Henry I, et al. Stents in the treatment of renal artery stenosis: long-term followup. J Endovasc Surg. 1999;6: Burket M, Cooper C, Kennedy D, et al. Renal artery angioplasty and stent placement: predictors of a favorable outcome. Am Heart J. 2000;139: Harden P, MacLeod M, Rodger R, et al. Effect of renal-artery stenting on progression of renovascular renal failure. Lancet. 1997;349: Dorros G, Jaff M, Mathiak L, et al. A four-year follow-up of Palmaz-Schatz stent revascularization as treatment for atherosclerotic renal artery stenosis. Circulation. 1998;98: Pickering TG, Devereaux RB, James GD, et al. Recurrent pulmonary edema in hypertension due to bilateral renal artery stenosis: treatment by angioplasty or surgical revascularization. Lancet. 1998;9: Perkovic V, Thomson KR, Mitchell PJ, et al. Treatment of renovascular disease with percutaneous stent insertion: long-term outcomes. Australas Radiol. 2001;45: Shammas NW, Kapalis MJ, Dippel EJ, et al. Clinical and angiographic predictors of restenosis following renal artery stenting. J Invasive Cardiol. 2004;16: Dorros G, Jaff M, Jain A, et al. Follow-up of primary Palmaz-Schatz stent placement for atherosclerotic renal artery stenosis. Am J Cardiol. 1995;75: Lederman RJ, Mendelsohn FO, Santos R, et al. Primary renal artery stenting: characteristics and outcomes after 363 procedures. Am Heart J. 2001;142: White CJ. Renal artery disease: facts and myths. Endovasc Today. 2003;2: Roach-Singh K. Aortorenal artery translesion pressure gradients in renovascular hypertension: in search of clinical significance. Cathet Cardiovasc Intervent. 2003;59: Colyer WR, Cooper CJ, Thomas WJ, et al. Utility of a pressure-sensing guidewire to assess renal artery translesional systolic pressure gradients. Cathet Cardiovasc Intervent. 2003;59: Allie DE, Hebert CJ, Walker CM, et al. Multidetector computed tomography angiography. Endovasc Today. 2004;3(3): Mali BL, Van De Ven PJ, et al. Repeated intervention for in-stent restenosis of the renal arteries. J Vasc Intervent Radiol. 2002;13: Munneke GJ, Engelke C, Belli AM, et al. Cutting balloon angioplasty for resistant renal artery instent restenosis. J Vasc Intervent Radiol. 2002; 13: Rundback J, Sacks D, Kent K, et al. Guidelines for the reporting of renal artery revascularization in clinical trials. J Vasc Intervent Radiol. 2002;13: Radermacher J, Chavan A, Haller H, et al. Use of a Doppler ultrasonography to predict the outcome of therapy for renal-artery stenosis. N Engl J Med. 2001;344: Leung D, Hoffman U, Debatin J, et al. Magnetic resonance imaging versus duplex sonography for diagnosing renovascular disease. Hypertension. 1999;33: Bongers V, Bakker J, De Klerk J, et al. Assessment of renal artery stenosis: comparison of captopril renography and gadolinium-enhanced breath-hold MR angiography. Clin Radiol. 2000;55: Pijls NHJ, De Bruyne B, Koolen JJ, et al. Measurement of fractional flow reserve to assess the functional severity of coronary artery stenosis. N Engl J Med. 1996;334: De Bruyne B, Piljs N, Wijns W, et al. Fractional flow reserve in patients with prior myocardial infarction. Circulation. 2001;Dec: Hanekamp CE, Koolen JJ, Bonnier H, et al. Comparison of quantitative coronary angiography, intravascular ultrasound, and coronary pressure measurement to assess optimum stent deployment. Circulation. 1999;99: Piljs NHJ, Klauss V, De Bruyne B, et al. Coronary pressure measurement after stenting predicts adverse events at follow-up: a multicenter registry. Circulation. 2002;105: Bech G, De Bruyne B, Wijns W, et al. Fractional flow reserve to determine the appropriateness of angioplasty in moderate coronary stenosis: a randomized trial. Circulation. 2001;103: Kern MJ, Donohue TJ, Aguirre FV, et al. Clinical outcome of deferring angioplasty in patients with normal translesional pressure-flow velocity measurements. J Am Coll Cardiol. 1995;25: van der Hulst VP, van Baalen J, Kool LS, et al. Renal artery stenosis: endovascular flow wire study for validation of Doppler ultrasound. Radiology. 1996;200: Nahman NS, Maniqm P, Hernandez RA, et al. Renal artery pressure gradients in patients with angiographic evidence of atherosclerotic renal artery stenosis. Am J Kidney Dis. 1994;24: Privat C, Ravel A, Chirossel P, et al. Endovascular Doppler guide wire in renal arteries: correlation with angiography in 20 patients. Invest Radiol. 1999;34: Gross CM, Kramer J, Weingartner O, et al. Determination of renal arterial stenosis severity: comparison of pressure gradient and vessel diameter. Radiology. 2001;220: De Bruyne B, Pijls NHJ, Wijns W, et al. Intracoronary and intravenous (central vs. peripheral) administration of ATP and adenosine to induce maximal coronary vasodilatation [abstract]. Circulation. 1999;100(Suppl I):I Bax LM, Mali WP, Beek FJ, et al. Repeated intervention for in-stent restenosis of renal arteries. J Vasc Intervent Radiol. 2002;13: Blum U, Krumme B, Flugel P, et al. Treatment of ostial renal-artery stenosis with vascular endoprostheses after unsuccessful balloon angioplasty. N Engl J Med. 1997;336: Walker CM, Hebert CJ, Lirtzman MD, et al. Renal artery in-stent restenosis: early results with excimer laser atheroablation. Poster 17th International Congress on Endovascular Interventions, Scottsdale, Arizona, February 8-12, J Endovasc Ther. 2004; 11: I1-I47; I Matsumo AH, Angle JF, Spinosa DJ, et al. Percutaneous transluminal angioplasty and stenting in chronic mesenteric ischemia: results and long term follow-up. J Am Coll Surg. 2002;194:Suppl 1: I ENDOVASCULAR TODAY I OCTOBER 2004
Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis
 Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea Etiology Fibromuscular
Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea Etiology Fibromuscular
Fractional Flow Reserve. A physiological approach to guide complex interventions
 Fractional Flow Reserve A physiological approach to guide complex interventions What is FFR? Fractional Flow Reserve (FFR) is a lesion specific, physiological index determining the hemodynamic severity
Fractional Flow Reserve A physiological approach to guide complex interventions What is FFR? Fractional Flow Reserve (FFR) is a lesion specific, physiological index determining the hemodynamic severity
FRACTIONAL FLOW RESERVE Step-by-step measurement, Practical tips & Pitfalls
 FRACTIONAL FLOW RESERVE Step-by-step measurement, Practical tips & Pitfalls Ahmed M ElGuindy, MSc, MRCP(UK) Division of Cardiology Aswan Heart Centre 2013 Fractional Flow Reserve Essential diagnostic tool
FRACTIONAL FLOW RESERVE Step-by-step measurement, Practical tips & Pitfalls Ahmed M ElGuindy, MSc, MRCP(UK) Division of Cardiology Aswan Heart Centre 2013 Fractional Flow Reserve Essential diagnostic tool
Evaluation of Intermediate Coronary lesions: Can You Handle the Pressure? Jeffrey A Southard, MD May 4, 2013
 Evaluation of Intermediate Coronary lesions: Can You Handle the Pressure? Jeffrey A Southard, MD May 4, 2013 Disclosures Consultant- St Jude Medical Boston Scientific Speaker- Volcano Corporation Heart
Evaluation of Intermediate Coronary lesions: Can You Handle the Pressure? Jeffrey A Southard, MD May 4, 2013 Disclosures Consultant- St Jude Medical Boston Scientific Speaker- Volcano Corporation Heart
FFR Incorporating & Expanding it s use in Clinical Practice
 FFR Incorporating & Expanding it s use in Clinical Practice Suleiman Kharabsheh, MD Consultant Invasive Cardiology Assistant professor, Alfaisal Univ. KFHI - KFSHRC Concept of FFR Maximum flow down a vessel
FFR Incorporating & Expanding it s use in Clinical Practice Suleiman Kharabsheh, MD Consultant Invasive Cardiology Assistant professor, Alfaisal Univ. KFHI - KFSHRC Concept of FFR Maximum flow down a vessel
Renal artery stenosis (RAS) is a relatively common
 The Importance of Appropriate Renal Artery Stenting Considerations for diagnosis and treatment of patients with renal artery stenosis. By Massoud A. Leesar, MD, FACC, FSCAI Renal artery stenosis (RAS)
The Importance of Appropriate Renal Artery Stenting Considerations for diagnosis and treatment of patients with renal artery stenosis. By Massoud A. Leesar, MD, FACC, FSCAI Renal artery stenosis (RAS)
Anatomy is Destiny, But Physiology is Here Today
 Published on Journal of Invasive Cardiology (http://www.invasivecardiology.com) September, 2010 [1] Anatomy is Destiny, But Physiology is Here Today Thu, 9/9/10-10:54am 0 Comments Section: Commentary Issue
Published on Journal of Invasive Cardiology (http://www.invasivecardiology.com) September, 2010 [1] Anatomy is Destiny, But Physiology is Here Today Thu, 9/9/10-10:54am 0 Comments Section: Commentary Issue
Fractional Flow Reserve (FFR) --Practical Set Up Pressure Measurement --
 Fractional Flow Reserve (FFR) --Practical Set Up Pressure Measurement -- JoonHyung Doh, MD, PhD Assistant Professor, Vision21 Cardiac and Vascular Center Inje University Ilsan Paik Hospital Goyang, Korea
Fractional Flow Reserve (FFR) --Practical Set Up Pressure Measurement -- JoonHyung Doh, MD, PhD Assistant Professor, Vision21 Cardiac and Vascular Center Inje University Ilsan Paik Hospital Goyang, Korea
Dave Kettles, St Dominics Hospital East London.
 Dave Kettles, St Dominics Hospital East London. 110 x 150 Angina for a couple of months Trop T negative T wave inversion across the chest leads Not wanting to risk radial Huge struggle with femoral
Dave Kettles, St Dominics Hospital East London. 110 x 150 Angina for a couple of months Trop T negative T wave inversion across the chest leads Not wanting to risk radial Huge struggle with femoral
PCI for Renal Artery stenosis
 PCI for Renal Artery stenosis Why should we treat Renal Artery Stenosis? Natural History of RAS RAS is progressive disease Study Follow-up (months) Pts Progression N (%) Total occlusion Wollenweber Meaney
PCI for Renal Artery stenosis Why should we treat Renal Artery Stenosis? Natural History of RAS RAS is progressive disease Study Follow-up (months) Pts Progression N (%) Total occlusion Wollenweber Meaney
Life After CORAL: What Did CORAL Prove? David Paul Slovut, MD, PhD Co-director TAVR, Dir of Advanced Intervention
 Life After CORAL: What Did CORAL Prove? David Paul Slovut, MD, PhD Co-director TAVR, Dir of Advanced Intervention No Relationships to Disclose The Need for Modern Renal Trials Increased rate of RAS diagnosis
Life After CORAL: What Did CORAL Prove? David Paul Slovut, MD, PhD Co-director TAVR, Dir of Advanced Intervention No Relationships to Disclose The Need for Modern Renal Trials Increased rate of RAS diagnosis
Fractional Flow Reserve (FFR) --Practical Set Up Pressure Measurement --
 Fractional Flow Reserve (FFR) --Practical Set Up Pressure Measurement -- Joon Hyung Doh, MD, PhD Associate Professor, Division of Cardiology Inje University Ilsan Paik Hospital Goyang, Korea 목차 Fractional
Fractional Flow Reserve (FFR) --Practical Set Up Pressure Measurement -- Joon Hyung Doh, MD, PhD Associate Professor, Division of Cardiology Inje University Ilsan Paik Hospital Goyang, Korea 목차 Fractional
FRACTIONAL FLOW RESERVE USE IN THE CATH LAB BECAUSE ANGIOGRAPHY ALONE IS NOT ENOUGH!!!!!!!!
 FRACTIONAL FLOW RESERVE USE IN THE CATH LAB BECAUSE ANGIOGRAPHY ALONE IS NOT ENOUGH!!!!!!!! Juan Antonio Pastor-Cervantes,M.D FSCAI, FACC Cardiovascular Institute Memorial Regional Hospital Hollywood Florida
FRACTIONAL FLOW RESERVE USE IN THE CATH LAB BECAUSE ANGIOGRAPHY ALONE IS NOT ENOUGH!!!!!!!! Juan Antonio Pastor-Cervantes,M.D FSCAI, FACC Cardiovascular Institute Memorial Regional Hospital Hollywood Florida
Coronary stenting: the appropriate use of FFR
 Coronary stenting: the appropriate use of FFR Morton J. Kern, MD Professor of Medicine Chief of Cardiology LBVA Associate Chief Cardiology University California Irvine Orange, California To treat or not
Coronary stenting: the appropriate use of FFR Morton J. Kern, MD Professor of Medicine Chief of Cardiology LBVA Associate Chief Cardiology University California Irvine Orange, California To treat or not
FFR and intravascular imaging, which of which?
 FFR and intravascular imaging, which of which? Ayman Khairy MD, PhD, FESC Associate professor of Cardiovascular Medicine Vice Director of Assiut University Hospitals Assiut, Egypt Diagnostic assessment
FFR and intravascular imaging, which of which? Ayman Khairy MD, PhD, FESC Associate professor of Cardiovascular Medicine Vice Director of Assiut University Hospitals Assiut, Egypt Diagnostic assessment
Case report. Resistance in the cath lab : the utility of hyperemic stenosis resistance in the functional assessment of coronary artery disease
 Resistance in the cath lab : the utility of hyperemic stenosis resistance in the functional assessment of coronary artery disease Kalpa De Silva, Divaka Perera Cardiovascular Division, The Rayne Institute,
Resistance in the cath lab : the utility of hyperemic stenosis resistance in the functional assessment of coronary artery disease Kalpa De Silva, Divaka Perera Cardiovascular Division, The Rayne Institute,
The fluid, dynamic interaction of multiple sequential
 Coronary Pressure Measurement to Assess the Hemodynamic Significance of Serial Stenoses Within One Coronary Artery Validation in Humans Nico H.J. Pijls, MD, PhD; Bernard De Bruyne, MD, PhD; G. Jan Willem
Coronary Pressure Measurement to Assess the Hemodynamic Significance of Serial Stenoses Within One Coronary Artery Validation in Humans Nico H.J. Pijls, MD, PhD; Bernard De Bruyne, MD, PhD; G. Jan Willem
ROLE OF CORONARY PRESSURE & FFR IN MULTIVESSEL DISEASE
 ROLE OF CORONARY PRESSURE & FFR IN MULTIVESSEL DISEASE Angioplasty Summit TCT ASIA Seoul, Korea, april 24th, 2008 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands A rather common
ROLE OF CORONARY PRESSURE & FFR IN MULTIVESSEL DISEASE Angioplasty Summit TCT ASIA Seoul, Korea, april 24th, 2008 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands A rather common
A Novel Simple Technique Using Hyperemia to Enhance Pressure Gradient Measurement of the Lower Extremity During Peripheral Intervention
 A Novel Simple Technique Using Hyperemia to Enhance Pressure Gradient Measurement of the Lower Extremity During Peripheral Intervention Issam Koleilat, MD; Bruce Gray, MD From Greenville Health System,
A Novel Simple Technique Using Hyperemia to Enhance Pressure Gradient Measurement of the Lower Extremity During Peripheral Intervention Issam Koleilat, MD; Bruce Gray, MD From Greenville Health System,
FRACTIONAL FLOW RESERVE: STANDARD OF CARE
 FRACTIONAL FLOW RESERVE: FROM INVESTIGATIONAL TOOL TO STANDARD OF CARE TCT ASIA Seoul, Korea, april 26 th, 2012 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands FRACTIONAL FLOW
FRACTIONAL FLOW RESERVE: FROM INVESTIGATIONAL TOOL TO STANDARD OF CARE TCT ASIA Seoul, Korea, april 26 th, 2012 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands FRACTIONAL FLOW
New Insight about FFR and IVUS MLA
 New Insight about FFR and IVUS MLA Can IVUS MLA Predict FFR
New Insight about FFR and IVUS MLA Can IVUS MLA Predict FFR
Evaluation of the Safety and Effectiveness of Renal Artery Stenting After Unsuccessful Balloon Angioplasty The ASPIRE-2 Study
 Journal of the American College of Cardiology Vol. 46, No. 5, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.073
Journal of the American College of Cardiology Vol. 46, No. 5, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.073
Coral Trials: A personal experience that challenges its results in patients with uncontrolled blood pressure.
 Coral Trials: A personal experience that challenges its results in patients with uncontrolled blood pressure.. Dr. Javier Ruiz Aburto, FACS, FICS Assistant Professor Ponce School of Medicine Puerto Rico
Coral Trials: A personal experience that challenges its results in patients with uncontrolled blood pressure.. Dr. Javier Ruiz Aburto, FACS, FICS Assistant Professor Ponce School of Medicine Puerto Rico
Treatment of renal artery in-stent restenosis with sirolimus-eluting stents
 Treatment of renal artery in-stent restenosis with sirolimus-eluting stents Vascular Medicine 15(1) 3 7 The Author(s) 2009 Reprints and permission: http://www. sagepub.co.uk/journalspermission.nav DOI:
Treatment of renal artery in-stent restenosis with sirolimus-eluting stents Vascular Medicine 15(1) 3 7 The Author(s) 2009 Reprints and permission: http://www. sagepub.co.uk/journalspermission.nav DOI:
Coronary Physiology and FFR. David H. Sibley MD FACC, FSCAI, FACP
 Coronary Physiology and FFR David H. Sibley MD FACC, FSCAI, FACP Braunwald s Heart Disease, 7 th Edition Control of Coronary Blood Flow 1. CFR = max flow/basal flow and decreases with increasing stenosis
Coronary Physiology and FFR David H. Sibley MD FACC, FSCAI, FACP Braunwald s Heart Disease, 7 th Edition Control of Coronary Blood Flow 1. CFR = max flow/basal flow and decreases with increasing stenosis
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Endovascular treatment of transplant renal artery stenosis based on hemodynamic assessment using a pressure wire: a case report
 Kadoya et al. BMC Cardiovascular Disorders (2018) 18:172 https://doi.org/10.1186/s12872-018-0909-y CASE REPORT Open Access Endovascular treatment of transplant renal artery stenosis based on hemodynamic
Kadoya et al. BMC Cardiovascular Disorders (2018) 18:172 https://doi.org/10.1186/s12872-018-0909-y CASE REPORT Open Access Endovascular treatment of transplant renal artery stenosis based on hemodynamic
Pressure Wire Study. Fractional Flow Reserve (FFR) Nishat Jahagirdar Principal Clinical Cardiac Physiologist Kings College Hospital
 Pressure Wire Study Fractional Flow Reserve (FFR) Nishat Jahagirdar Principal Clinical Cardiac Physiologist Kings College Hospital History Andreas Gruentzig s paper on Non operative dilation of coronaryartery
Pressure Wire Study Fractional Flow Reserve (FFR) Nishat Jahagirdar Principal Clinical Cardiac Physiologist Kings College Hospital History Andreas Gruentzig s paper on Non operative dilation of coronaryartery
Renal Artery Stenting With Embolic Protection
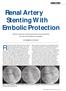 Renal Artery Stenting With Embolic Protection Embolic protection during renal stenting may be beneficial, but new device designs are necessary. BY RAJESH M. DAVE, MD Renal artery stenosis (RAS) is the
Renal Artery Stenting With Embolic Protection Embolic protection during renal stenting may be beneficial, but new device designs are necessary. BY RAJESH M. DAVE, MD Renal artery stenosis (RAS) is the
Fractional Flow Reserve: Basics, FAME 1, FAME 2. William F. Fearon, MD Associate Professor Stanford University Medical Center
 Fractional Flow Reserve: Basics, FAME 1, FAME 2 William F. Fearon, MD Associate Professor Stanford University Medical Center Conflict of Interest Advisory Board for HeartFlow Research grant from St. Jude
Fractional Flow Reserve: Basics, FAME 1, FAME 2 William F. Fearon, MD Associate Professor Stanford University Medical Center Conflict of Interest Advisory Board for HeartFlow Research grant from St. Jude
Accurate Vessel Sizing Drives Clinical Results. IVUS In the Periphery
 Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Effective Health Care
 Number 5 Effective Health Care Comparative Effectiveness of Management Strategies for Renal Artery Stenosis Executive Summary Background Renal artery stenosis (RAS) is defined as the narrowing of the lumen
Number 5 Effective Health Care Comparative Effectiveness of Management Strategies for Renal Artery Stenosis Executive Summary Background Renal artery stenosis (RAS) is defined as the narrowing of the lumen
Fractional Flow Reserve from Coronary CT Angiography (and some neat CT images)
 Fractional Flow Reserve from Coronary CT Angiography (and some neat CT images) Victor Cheng, M.D. Director, Cardiovascular CT Oklahoma Heart Institute 1 Disclosures Tornadoes scare me 2 Treating CAD Fixing
Fractional Flow Reserve from Coronary CT Angiography (and some neat CT images) Victor Cheng, M.D. Director, Cardiovascular CT Oklahoma Heart Institute 1 Disclosures Tornadoes scare me 2 Treating CAD Fixing
Debate Should we use FFR? I will say NO.
 Debate Should we use FFR? I will say NO. Hyeon-Cheol Gwon Cardiac and Vascular Center Samsung Medical Center Sungkyunkwan University School of Medicine Dr. Hyeon-Cheol Gwon Research fund from Abbott Korea
Debate Should we use FFR? I will say NO. Hyeon-Cheol Gwon Cardiac and Vascular Center Samsung Medical Center Sungkyunkwan University School of Medicine Dr. Hyeon-Cheol Gwon Research fund from Abbott Korea
Ostial Stents and Distal Embolic Protection During Renal Stenting
 Ostial Stents and Distal Embolic Protection During Renal Stenting John R. Laird, MD Professor of Medicine Director of the Vascular Center UC Davis Medical Center Limitations of Current Techniques of Renal
Ostial Stents and Distal Embolic Protection During Renal Stenting John R. Laird, MD Professor of Medicine Director of the Vascular Center UC Davis Medical Center Limitations of Current Techniques of Renal
Do stents deserve the bad press? Mark A. Tulli MD, FACC
 Do stents deserve the bad press? Mark A. Tulli MD, FACC Disclosures: None Introduction Stents don t help people. Stents are bad for patients. Heart Treatment Overused WSJ Study Finds Doctors Often Too
Do stents deserve the bad press? Mark A. Tulli MD, FACC Disclosures: None Introduction Stents don t help people. Stents are bad for patients. Heart Treatment Overused WSJ Study Finds Doctors Often Too
Vascular Imaging Original Research
 MDCT Angiography of Renal Arteries Vascular Imaging Original Research Adam D. Talenfeld 1 Ryan B. Schwope Huntley J. Alper Emil I. Cohen Robert A. Lookstein Talenfeld AD, Schwope RB, Alper HJ, Cohen EI,
MDCT Angiography of Renal Arteries Vascular Imaging Original Research Adam D. Talenfeld 1 Ryan B. Schwope Huntley J. Alper Emil I. Cohen Robert A. Lookstein Talenfeld AD, Schwope RB, Alper HJ, Cohen EI,
FFR: Tips and Tricks. A/Prof (Adj) Yeo Khung Keong, MBBS, FAMS, FACC, FSCAI National Heart Centre Singapore
 FFR: Tips and Tricks A/Prof (Adj) Yeo Khung Keong, MBBS, FAMS, FACC, FSCAI National Heart Centre Singapore Disclosures Abbott Vascular: Speaker, Proctor (MitraClip) Boston Scientific: Consultant, honorarium
FFR: Tips and Tricks A/Prof (Adj) Yeo Khung Keong, MBBS, FAMS, FACC, FSCAI National Heart Centre Singapore Disclosures Abbott Vascular: Speaker, Proctor (MitraClip) Boston Scientific: Consultant, honorarium
A Closer Look: Renal Artery Stenosis. Renal artery stenosis (RAS) is defined as a TOPICS FROM CHEP. Shawn s stenosis
 TOPICS FROM CHEP A Closer Look: Renal Artery Stenosis On behalf of the Canadian Hypertension Education Program (CHEP), Dr. Tobe gives an overview of renal artery stenosis, including the prevalence, screening
TOPICS FROM CHEP A Closer Look: Renal Artery Stenosis On behalf of the Canadian Hypertension Education Program (CHEP), Dr. Tobe gives an overview of renal artery stenosis, including the prevalence, screening
Fractional Flow Reserve: Review of the latest data
 Fractional Flow Reserve: Review of the latest data Michalis Hamilos, MD, PhD, FESC University Hospital of Heraklion Fractional Flow Reserve (FFR) Coronary angiography does not always tell the truth Most
Fractional Flow Reserve: Review of the latest data Michalis Hamilos, MD, PhD, FESC University Hospital of Heraklion Fractional Flow Reserve (FFR) Coronary angiography does not always tell the truth Most
The Utility of Atherectomy and the Jetstream Atherectomy System
 The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
Renal Artery FFR. Woo-Young Chung. Seoul National University, College of Medicine Boramae Medical Center Cardiovascular Center
 Renal Artery FFR Woo-Young Chung Seoul National University, College of Medicine Boramae Medical Center Cardiovascular Center Why renal FFR? Renal artery angioplasty (PTRA) Indication of Renal artery angioplasty
Renal Artery FFR Woo-Young Chung Seoul National University, College of Medicine Boramae Medical Center Cardiovascular Center Why renal FFR? Renal artery angioplasty (PTRA) Indication of Renal artery angioplasty
PCIs on Intermediate Lesions NCDR Cath-PCI Registry
 Practical Application Of Coronary Physiology in The Cath Lab Talal T Attar, MD, MBA, FACC PCIs on Intermediate Lesions NCDR Cath-PCI Registry Fraction of stenoses 50-70% treated with PCI without further
Practical Application Of Coronary Physiology in The Cath Lab Talal T Attar, MD, MBA, FACC PCIs on Intermediate Lesions NCDR Cath-PCI Registry Fraction of stenoses 50-70% treated with PCI without further
Effects of Increasing Doses of Intracoronary Adenosine on the Assessment of Fractional Flow Reserve
 JACC: CARDIOVASCULAR INTERVENTIONS VOL. 4, NO. 10, 2011 2011 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2011.08.004 Effects of
JACC: CARDIOVASCULAR INTERVENTIONS VOL. 4, NO. 10, 2011 2011 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2011.08.004 Effects of
Novel insights into the complexity of ischaemic heart disease derived from combined coronary pressure and flow velocity measurements van de Hoef, T.P.
 UvA-DARE (Digital Academic Repository) Novel insights into the complexity of ischaemic heart disease derived from combined coronary pressure and flow velocity measurements van de Hoef, T.P. Link to publication
UvA-DARE (Digital Academic Repository) Novel insights into the complexity of ischaemic heart disease derived from combined coronary pressure and flow velocity measurements van de Hoef, T.P. Link to publication
Renal Artery Stenting
 Renal Artery Stenting J.P. Reilly, MD, FSCAI Ochsner Medical Center Speaker s bureau: Astra Zeneca and Lilly/Diachi Sankyo Prevalence of RAS is high in cath population. Renal artery intervention can help
Renal Artery Stenting J.P. Reilly, MD, FSCAI Ochsner Medical Center Speaker s bureau: Astra Zeneca and Lilly/Diachi Sankyo Prevalence of RAS is high in cath population. Renal artery intervention can help
Ultrasound velocity criteria for renal in-stent restenosis
 Ultrasound velocity criteria for renal in-stent restenosis Yung-Wei Chi, DO, Christopher J. White, MD, Stanley Thornton, MD, and Richard V. Milani, MD, New Orleans, La Background: Renal artery stent placement
Ultrasound velocity criteria for renal in-stent restenosis Yung-Wei Chi, DO, Christopher J. White, MD, Stanley Thornton, MD, and Richard V. Milani, MD, New Orleans, La Background: Renal artery stent placement
Technical Aspects and Clinical Indications of FFR
 Technical Aspects and Clinical Indications of FFR Emanuele Barbato, MD, PhD, FESC Cardiovascular Center Aalst - OLV Clinic Aalst, Belgium Potential conflicts of interest Consulting fees and honoraria on
Technical Aspects and Clinical Indications of FFR Emanuele Barbato, MD, PhD, FESC Cardiovascular Center Aalst - OLV Clinic Aalst, Belgium Potential conflicts of interest Consulting fees and honoraria on
Fibromuscular Dysplasia (FMD) of the renal arteries Angiographic features and therapeutic options
 Fibromuscular Dysplasia (FMD) of the renal arteries Angiographic features and therapeutic options Poster No.: C-0630 Congress: ECR 2012 Type: Educational Exhibit Authors: K. I. Ringe, B. Meyer, F. Wacker,
Fibromuscular Dysplasia (FMD) of the renal arteries Angiographic features and therapeutic options Poster No.: C-0630 Congress: ECR 2012 Type: Educational Exhibit Authors: K. I. Ringe, B. Meyer, F. Wacker,
Turbo-Power. Laser atherectomy catheter. The standard. for ISR
 Turbo-Power Laser atherectomy catheter The standard for ISR Vaporize the ISR challenge In-stent restenosis (ISR) Chance of recurring 7 115,000 + /year (U.S.) 1-6 Repeated narrowing of the arteries after
Turbo-Power Laser atherectomy catheter The standard for ISR Vaporize the ISR challenge In-stent restenosis (ISR) Chance of recurring 7 115,000 + /year (U.S.) 1-6 Repeated narrowing of the arteries after
How to assess the hemodynamic importance of a renal artery stenosis. Felix Mahfoud, MD Saarland University Hospital Homburg/Saar, Germany
 How to assess the hemodynamic importance of a renal artery stenosis Felix Mahfoud, MD Saarland University Hospital Homburg/Saar, Germany How to assess renal artery stenosis severity 1. Non-invasive assessments
How to assess the hemodynamic importance of a renal artery stenosis Felix Mahfoud, MD Saarland University Hospital Homburg/Saar, Germany How to assess renal artery stenosis severity 1. Non-invasive assessments
Between Coronary Angiography and Fractional Flow Reserve
 Visual-Functional Mismatch Between Coronary Angiography and Fractional Flow Reserve Seung-Jung Park, MD., PhD. University of Ulsan, College of Medicine Asan Medical Center, Seoul, Korea Visual - Functional
Visual-Functional Mismatch Between Coronary Angiography and Fractional Flow Reserve Seung-Jung Park, MD., PhD. University of Ulsan, College of Medicine Asan Medical Center, Seoul, Korea Visual - Functional
Fractional Flow Reserve (FFR)
 Non-invasive FFR using coronary CT angiography and computational fluid dyn amics predicts the hemodynamic signifi cance of coronary lesions First in man experience with CT-Flow Andrejs Erglis, Sanda Jegere,
Non-invasive FFR using coronary CT angiography and computational fluid dyn amics predicts the hemodynamic signifi cance of coronary lesions First in man experience with CT-Flow Andrejs Erglis, Sanda Jegere,
FFR in Left Main Disease
 FFR in Left Main Disease William F. Fearon, MD Associate Professor of Medicine Director, Interventional Cardiology Stanford University Medical Center Why FFR instead of IVUS? Physiologic versus anatomic
FFR in Left Main Disease William F. Fearon, MD Associate Professor of Medicine Director, Interventional Cardiology Stanford University Medical Center Why FFR instead of IVUS? Physiologic versus anatomic
NOT FOR PUBLICATION, QUOTATION, OR CITATION RESOLUTION NO. 22
 BE IT RESOLVED, Sponsored By: RESOLUTION NO. 22 that the American College of Radiology adopt the ACR SIR Practice Parameter for the Performance of Angiography, Angioplasty, and Stenting for the Diagnosis
BE IT RESOLVED, Sponsored By: RESOLUTION NO. 22 that the American College of Radiology adopt the ACR SIR Practice Parameter for the Performance of Angiography, Angioplasty, and Stenting for the Diagnosis
Why I try to avoid side branch dilatation
 Why I try to avoid side branch dilatation Hyeon-Cheol Gwon Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Why I don t kiss? I kiss! I prefer to discuss SB ballooning rather
Why I try to avoid side branch dilatation Hyeon-Cheol Gwon Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Why I don t kiss? I kiss! I prefer to discuss SB ballooning rather
Coronary Physiology the current state of play
 Coronary Physiology the current state of play Background The concept of using the trans-stenotic pressure gradient in a diseased coronary artery as a measure to guide percutaneous coronary intervention
Coronary Physiology the current state of play Background The concept of using the trans-stenotic pressure gradient in a diseased coronary artery as a measure to guide percutaneous coronary intervention
PCI for Left Anterior Descending Artery Ostial Stenosis
 PCI for Left Anterior Descending Artery Ostial Stenosis Why do you hesitate PCI for LAD ostial stenosis? LAD Ostial Lesion Limitations of PCI High elastic recoil Involvement of the distal left main coronary
PCI for Left Anterior Descending Artery Ostial Stenosis Why do you hesitate PCI for LAD ostial stenosis? LAD Ostial Lesion Limitations of PCI High elastic recoil Involvement of the distal left main coronary
PressureWire Aeris with Agile Tip Technology. Wireless FFR Functionality and Handles like a Workhorse PCI Guidewire 1
 Home» Products» All International Products» PressureWire Aeris with Agile Tip Technology PressureWire Aeris with Agile Tip Technology This device is commercially available for use in select international
Home» Products» All International Products» PressureWire Aeris with Agile Tip Technology PressureWire Aeris with Agile Tip Technology This device is commercially available for use in select international
Coronary Physiology in the Cath Lab: Beyond the Basics
 Coronary Physiology in the Cath Lab: Beyond the Basics Morton J. Kern, MD, FSCAI KEYWORDS Coronary artery disease Cardiac catheterization laboratory Translesional pressure measurement In-lab coronary physiology
Coronary Physiology in the Cath Lab: Beyond the Basics Morton J. Kern, MD, FSCAI KEYWORDS Coronary artery disease Cardiac catheterization laboratory Translesional pressure measurement In-lab coronary physiology
Value of Index of Microvascular Resistance (IMR) in Microvascular Integrity
 Value of Index of Microvascular Resistance (IMR) in Microvascular Integrity Seung-Woon Rha, Korea University Guro Hospital, Myeong-Ho Yoon, Ajou University Hospital Imaging & Physiology Summit 2009 Nov
Value of Index of Microvascular Resistance (IMR) in Microvascular Integrity Seung-Woon Rha, Korea University Guro Hospital, Myeong-Ho Yoon, Ajou University Hospital Imaging & Physiology Summit 2009 Nov
av ailab le at jou rn al h om epa g e:
 Journal of Cardiology Cases (2011) 4, e163 e167 av ailab le at www.sciencedirect.com jou rn al h om epa g e: www.elsevier.com/locate/jccase Case Report In vivo intravascular ultrasound imaging of fibromuscular
Journal of Cardiology Cases (2011) 4, e163 e167 av ailab le at www.sciencedirect.com jou rn al h om epa g e: www.elsevier.com/locate/jccase Case Report In vivo intravascular ultrasound imaging of fibromuscular
Calcium Removal and Plaque Modification in the Era of DEB and Contemporary Stenting for Femoro- Popliteal Disease
 Calcium Removal and Plaque Modification in the Era of DEB and Contemporary Stenting for Femoro- Popliteal Disease Thomas M. Shimshak, MD Heart and Vascular Center Florida Hospital Heartland Medical Center
Calcium Removal and Plaque Modification in the Era of DEB and Contemporary Stenting for Femoro- Popliteal Disease Thomas M. Shimshak, MD Heart and Vascular Center Florida Hospital Heartland Medical Center
FFR and CABG Emanuele Barbato, MD, PhD, FESC Cardiovascular Center Aalst, Belgium
 FFR and CABG Emanuele Barbato, MD, PhD, FESC Cardiovascular Center Aalst, Belgium Conflict of Interest Institutional research grants and speaker s fee from St. Jude Medical and Boston Scientic to Cardiovascular
FFR and CABG Emanuele Barbato, MD, PhD, FESC Cardiovascular Center Aalst, Belgium Conflict of Interest Institutional research grants and speaker s fee from St. Jude Medical and Boston Scientic to Cardiovascular
Renal Artery Stenosis: Insights from the CORAL Trial
 Renal Artery Stenosis: Insights from the CORAL Trial Christopher J. Cooper, M.D., FACC, FACP Dean and Senior Vice President University of Toledo, College of Medicine President, Ohio Chapter ACC State of
Renal Artery Stenosis: Insights from the CORAL Trial Christopher J. Cooper, M.D., FACC, FACP Dean and Senior Vice President University of Toledo, College of Medicine President, Ohio Chapter ACC State of
Management of In-stent Restenosis after Lower Extremity Endovascular Procedures
 Management of In-stent Restenosis after Lower Extremity Endovascular Procedures Piotr Sobieszczyk, MD Associate Director, Cardiac Catheterization Laboratory Cardiovascular Division and Vascular Medicine
Management of In-stent Restenosis after Lower Extremity Endovascular Procedures Piotr Sobieszczyk, MD Associate Director, Cardiac Catheterization Laboratory Cardiovascular Division and Vascular Medicine
Cardiac transplant related arteriopathy remains a leading
 Simultaneous Assessment of Fractional and Coronary Flow Reserves in Cardiac Transplant Recipients Physiologic Investigation for Transplant Arteriopathy (PITA Study) William F. Fearon, MD; Mamoo Nakamura,
Simultaneous Assessment of Fractional and Coronary Flow Reserves in Cardiac Transplant Recipients Physiologic Investigation for Transplant Arteriopathy (PITA Study) William F. Fearon, MD; Mamoo Nakamura,
Renal artery stenosis
 Renal artery stenosis Dr. Alexander Woywodt Consultant Renal Physician, Royal Preston Hospital Preston, 31.10.2007 Menu anatomy of the renal arteries diseases of the large renal arteries atherosclerotic
Renal artery stenosis Dr. Alexander Woywodt Consultant Renal Physician, Royal Preston Hospital Preston, 31.10.2007 Menu anatomy of the renal arteries diseases of the large renal arteries atherosclerotic
CLINICAL CONSEQUENCES OF THE
 CLINICAL CONSEQUENCES OF THE FAME STUDY TCT ASIA Seoul, Korea, april 26 th, 2012 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands GUIDELINES ESC SEPTEMBER 2010 FFR UPGRADED TO LEVEL
CLINICAL CONSEQUENCES OF THE FAME STUDY TCT ASIA Seoul, Korea, april 26 th, 2012 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands GUIDELINES ESC SEPTEMBER 2010 FFR UPGRADED TO LEVEL
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Appropriate Patient Identification For Renal Artery Intervention Remains Challenging
 Renal Intervention Herbert D. Aronow, MD, MPH, FACC, FSCAI, FSVM Director, Interventional Cardiology, Cardiovascular Institute Director, Cardiac Cath Labs, Rhode Island &The Miriam Hospitals None Disclosures
Renal Intervention Herbert D. Aronow, MD, MPH, FACC, FSCAI, FSVM Director, Interventional Cardiology, Cardiovascular Institute Director, Cardiac Cath Labs, Rhode Island &The Miriam Hospitals None Disclosures
ABSOLUTE BLOOD FLOW MEASUREMENTS: PRINCIPLES
 CORONARY PHYSIOLOGY IN THE CATHLAB: ABSOLUTE BLOOD FLOW MEASUREMENTS: PRINCIPLES Educational Training Program ESC European Heart House april 23rd - 25th 2015 Nico H. J. Pijls, MD, PhD Catharina Hospital,
CORONARY PHYSIOLOGY IN THE CATHLAB: ABSOLUTE BLOOD FLOW MEASUREMENTS: PRINCIPLES Educational Training Program ESC European Heart House april 23rd - 25th 2015 Nico H. J. Pijls, MD, PhD Catharina Hospital,
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
What do the guidelines say?
 Percutaneous coronary intervention in 3-vessel disease and main stem What do the guidelines say? Nothing to disclose Dariusz Dudek Institute of Cardiology, Jagiellonian University Krakow, Poland The European
Percutaneous coronary intervention in 3-vessel disease and main stem What do the guidelines say? Nothing to disclose Dariusz Dudek Institute of Cardiology, Jagiellonian University Krakow, Poland The European
Declaration of conflict of interest. Nothing to disclose
 Declaration of conflict of interest Nothing to disclose Hong-Seok Lim, Seung-Jea Tahk, Hyoung-Mo Yang, Jin-Woo Kim, Kyoung- Woo Seo, Byoung-Joo Choi, So-Yeon Choi, Myeong-Ho Yoon, Gyo-Seung Hwang, Joon-Han
Declaration of conflict of interest Nothing to disclose Hong-Seok Lim, Seung-Jea Tahk, Hyoung-Mo Yang, Jin-Woo Kim, Kyoung- Woo Seo, Byoung-Joo Choi, So-Yeon Choi, Myeong-Ho Yoon, Gyo-Seung Hwang, Joon-Han
The Centers for Medicare & Medicaid Services
 Percutaneous Renal Revascularization and Medicare Coverage The Society of Interventional Radiology s position on the current CMS coverage of renal interventions. BY DAVID SACKS, MD, AND TIMOTHY P. MURPHY,
Percutaneous Renal Revascularization and Medicare Coverage The Society of Interventional Radiology s position on the current CMS coverage of renal interventions. BY DAVID SACKS, MD, AND TIMOTHY P. MURPHY,
Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System
 Volume 1, Issue 1 Case Report Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System Robert F. Riley * and Bill Lombardi University of Washington Medical Center, Division
Volume 1, Issue 1 Case Report Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System Robert F. Riley * and Bill Lombardi University of Washington Medical Center, Division
Aun-Yeong Chong MD, MRCP(UK), MBBS University of Ottawa Heart Institute
 Aun-Yeong Chong MD, MRCP(UK), MBBS University of Ottawa Heart Institute Cardiac Imaging Symposium Oct 2013 Invasive Coronary Artery Assessment Coronary angiography IntraVascular UltraSound (IVUS) Optical
Aun-Yeong Chong MD, MRCP(UK), MBBS University of Ottawa Heart Institute Cardiac Imaging Symposium Oct 2013 Invasive Coronary Artery Assessment Coronary angiography IntraVascular UltraSound (IVUS) Optical
Assessment of recurrent mesenteric ischemia after stenting with a pressure wire
 524852VMJ0010.1177/1358863X14524852Vascular MedicineMargiotta and Gray research-article2014 Case Report Assessment of recurrent mesenteric ischemia after stenting with a pressure wire Vascular Medicine
524852VMJ0010.1177/1358863X14524852Vascular MedicineMargiotta and Gray research-article2014 Case Report Assessment of recurrent mesenteric ischemia after stenting with a pressure wire Vascular Medicine
Intracoronary Continuous Adenosine Infusion
 Circ J 2005; 69: 908 912 Intracoronary Continuous Adenosine Infusion A Novel and Effective Way of Inducing Maximal Hyperemia for Fractional Flow Reserve Measurement Bon-Kwon Koo, MD, PhD; Cheol-Ho Kim,
Circ J 2005; 69: 908 912 Intracoronary Continuous Adenosine Infusion A Novel and Effective Way of Inducing Maximal Hyperemia for Fractional Flow Reserve Measurement Bon-Kwon Koo, MD, PhD; Cheol-Ho Kim,
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Coronary Artery Dissection Following Angioplasty Evaluated by Fractional Flow Reserve: Report of Three Cases
 J Cardiol 2001 Dec; 386: 337 342 : 3 Coronary Artery Dissection Following Angioplasty Evaluated by Fractional Flow Reserve: Report of Three Cases Kazutaka AMAYA, MD Kenji TAKAZAWA, MD, FJCC Nobuhiro TANAKA,
J Cardiol 2001 Dec; 386: 337 342 : 3 Coronary Artery Dissection Following Angioplasty Evaluated by Fractional Flow Reserve: Report of Three Cases Kazutaka AMAYA, MD Kenji TAKAZAWA, MD, FJCC Nobuhiro TANAKA,
Coronary artery disease (CAD): Fractional Flow Reserve (FFR) for Pilots Risk Assessment. B. Haaff, R. Quast
 Coronary artery disease (CAD): Fractional Flow Reserve (FFR) for Pilots Risk Assessment B. Haaff, R. Quast Aeromedical Center Germany, Stuttgart-Airport Westpfalz-Klinikum, Kaiserslautern, Germany Disclosure
Coronary artery disease (CAD): Fractional Flow Reserve (FFR) for Pilots Risk Assessment B. Haaff, R. Quast Aeromedical Center Germany, Stuttgart-Airport Westpfalz-Klinikum, Kaiserslautern, Germany Disclosure
Σεμινάριο Ομάδων Εργασίας Fractional Flow Reserve (FFR) Σε ποιούς ασθενείς; ΔΗΜΗΤΡΗΣ ΑΥΖΩΤΗΣ Επιστ. υπεύθυνος Αιμοδυναμικού Τμήματος, Βιοκλινική
 ΕΛΛΗΝΙΚΗΚΑΡΔΙΟΛΟΓΙΚΗΕΤΑΙΡΕΙΑ Σεμινάριο Ομάδων Εργασίας 2011 Fractional Flow Reserve (FFR) Σε ποιούς ασθενείς; ΔΗΜΗΤΡΗΣ ΑΥΖΩΤΗΣ Επιστ. υπεύθυνος Αιμοδυναμικού Τμήματος, Βιοκλινική GUIDELINES ON MYOCARDIAL
ΕΛΛΗΝΙΚΗΚΑΡΔΙΟΛΟΓΙΚΗΕΤΑΙΡΕΙΑ Σεμινάριο Ομάδων Εργασίας 2011 Fractional Flow Reserve (FFR) Σε ποιούς ασθενείς; ΔΗΜΗΤΡΗΣ ΑΥΖΩΤΗΣ Επιστ. υπεύθυνος Αιμοδυναμικού Τμήματος, Βιοκλινική GUIDELINES ON MYOCARDIAL
FFR in diffuse disease and serial stenoses
 FFR in diffuse disease and serial stenoses Educational Training Program ESC European Heart House Apr. 25-27 2013 Nils Witt MD PhD, Södersjukhuset, Stockholm, Sweden Single stenosis Functionally Functional
FFR in diffuse disease and serial stenoses Educational Training Program ESC European Heart House Apr. 25-27 2013 Nils Witt MD PhD, Södersjukhuset, Stockholm, Sweden Single stenosis Functionally Functional
Duplex Ultrasound of the Renal Arteries. Duplex Ultrasound. In the Beginning
 Duplex Ultrasound of the Renal Arteries DIMENSIONS IN HEART AND VASCULAR CARE 2013 PENN STATE HEART AND VASCULAR INSTITUTE ROBERT G. ATNIP MD PROFESSOR OF SURGERY AND RADIOLOGY Duplex Ultrasound Developed
Duplex Ultrasound of the Renal Arteries DIMENSIONS IN HEART AND VASCULAR CARE 2013 PENN STATE HEART AND VASCULAR INSTITUTE ROBERT G. ATNIP MD PROFESSOR OF SURGERY AND RADIOLOGY Duplex Ultrasound Developed
Functional and Anatomical Diagnosis of Coronary Artery Stenoses
 Journal of Surgical Research 150, 24 33 (2008) doi:10.1016/j.jss.2007.10.018 Functional and Anatomical Diagnosis of Coronary Artery Stenoses Abhijit Sinha Roy, Ph.D.,* Martin R. Back, M.D.,** Saeb F. Khoury,
Journal of Surgical Research 150, 24 33 (2008) doi:10.1016/j.jss.2007.10.018 Functional and Anatomical Diagnosis of Coronary Artery Stenoses Abhijit Sinha Roy, Ph.D.,* Martin R. Back, M.D.,** Saeb F. Khoury,
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Renal Artery Stenosis With Severe Hypertension: A Case Report
 CASE REPORT Renal Artery Stenosis With Severe Hypertension: A Case Report Suwaid MA ABSTRACT Background: Renal artery stenosis (RAS) is found in 77% of hypertensive patients and is responsible for 1-2%
CASE REPORT Renal Artery Stenosis With Severe Hypertension: A Case Report Suwaid MA ABSTRACT Background: Renal artery stenosis (RAS) is found in 77% of hypertensive patients and is responsible for 1-2%
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
FFR Fundamentals and Measurements
 FFR Fundamentals and Measurements Ghassan S. Kassab Thomas Linnemeier Chair Professor Biomedical Engineering, Indiana University Purdue University Indianapolis Principle of FFR Q S ( P P ) / R P max d
FFR Fundamentals and Measurements Ghassan S. Kassab Thomas Linnemeier Chair Professor Biomedical Engineering, Indiana University Purdue University Indianapolis Principle of FFR Q S ( P P ) / R P max d
Diffuse Disease and Serial Stenoses. Bernard De Bruyne Cardiovascular Center Aalst Belgium
 Diffuse Disease and Serial Stenoses Bernard De Bruyne Cardiovascular Center Aalst Belgium Atherosclerosis is a Diffuse Disease Serial Stenoses A B P a P m P d When A is isolated, hyperemic flow through
Diffuse Disease and Serial Stenoses Bernard De Bruyne Cardiovascular Center Aalst Belgium Atherosclerosis is a Diffuse Disease Serial Stenoses A B P a P m P d When A is isolated, hyperemic flow through
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
CPT Code Details
 CPT Code 93572 Details Code Descriptor Intravascular Doppler velocity and/or pressure derived coronary flow reserve measurement (coronary vessel or graft) during coronary angiography including pharmacologically
CPT Code 93572 Details Code Descriptor Intravascular Doppler velocity and/or pressure derived coronary flow reserve measurement (coronary vessel or graft) during coronary angiography including pharmacologically
CT FFR: Are you ready to totally change the way you diagnose Coronary Artery Disease?
 CT FFR: Are you ready to totally change the way you diagnose Coronary Artery Disease? Madan Mohan MD MRCP FACC CQO, Division of Cardiovascular Medicine University Hospitals Case Medical Center Assistant
CT FFR: Are you ready to totally change the way you diagnose Coronary Artery Disease? Madan Mohan MD MRCP FACC CQO, Division of Cardiovascular Medicine University Hospitals Case Medical Center Assistant
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Instantaneous Wave-Free Ratio
 Instantaneous Wave-Free Ratio Alejandro Aquino MD Interventional Cardiology Fellow Washington University in St. Louis Barnes-Jewish Hospital Instantaneous Wave-Free Ratio Alejandro Aquino MD Disclosure
Instantaneous Wave-Free Ratio Alejandro Aquino MD Interventional Cardiology Fellow Washington University in St. Louis Barnes-Jewish Hospital Instantaneous Wave-Free Ratio Alejandro Aquino MD Disclosure
Intervention: How and to which extent is technology helping us?
 Cardiological Society of India Congress 12th February 2016 Chennai, India Intervention: How and to which extent is technology helping us? SIMONE BISCAGLIA MD CARDIOVASCULAR INSTITUTE, FERRARA, ITALY Introduction
Cardiological Society of India Congress 12th February 2016 Chennai, India Intervention: How and to which extent is technology helping us? SIMONE BISCAGLIA MD CARDIOVASCULAR INSTITUTE, FERRARA, ITALY Introduction
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE A Comparison between the Instantaneous Wave-free Ratio and Resting Distal Coronary Artery Pressure/Aortic Pressure and the Fractional Flow Reserve: The Diagnostic Accuracy CanBeImprovedbytheUseofbothIndices
ORIGINAL ARTICLE A Comparison between the Instantaneous Wave-free Ratio and Resting Distal Coronary Artery Pressure/Aortic Pressure and the Fractional Flow Reserve: The Diagnostic Accuracy CanBeImprovedbytheUseofbothIndices
