Pharmacology: Heart Failure
|
|
|
- Ralf Knight
- 6 years ago
- Views:
Transcription
1 Pharmacology: Heart Failure PHPP 515 (IT I) Fall 2014 Monday, Oct. 13 3:00 4:50 PM Dr. Jacobs Required Reading (via Access Pharmacy) Katzung: Chapters 13 Recommended Reading (via Access Pharmacy) Goodman and Gilman: Chapter 28 1
2 Lecture Outline: Heart Failure Overview Cardiac Output: (Heart rate, Preload, Contractility, Afterload) Hormonal and Sympathetic Activity in HF HF Drugs Diuretics RAA system inhibitors Beta blockers Vasodilators Inotropic agents (chronic and acute) 2
3 PULMONARY VASCULATURE RV Cardiac Output Basic Concepts LV failure: Pulmonary Edema Pulmonary Return RV failure: Peripheral Edema RV Systemic Venous Return SYSTEMIC LV LV Cardiac Output DIASTOLIC HF: Ventricles LESS COMPLIANT SYSTOLIC HF: Ventricles LESS CONTRACTILE 3
4 1. HEART RATE FOUR FACTORS DETERMINE CO: 1. Heart rate (HR) 2. Preload 3. Contractility 4. Afterload Basic Concepts CARDIAC OUTPUT (CO = SV x HR) Stroke Volume x Heart Rate Or, the amount of blood pumped in 1 min (units = liters/min) Influence Stroke Volume (SV) Taken independently (not considering effects of HR on other cardiovascular factors) heart rate will proportionally cardiac output. 4
5 Basic Concepts 2. PRELOAD PRELOAD = STRESS on the walls at the END OF DIASTOLE (just before ventricular contraction). At this time, the ventricles are at their greatest stretch. For the RIGHT ventricle, preload is proportional to central venous pressure (CVP), which is the same as Right ventricular end diastolic pressure (RV EDP). Normal CVP is around 3 8 mmhg. For the LEFT ventricle, preload is also known as left ventricular end diastolic pressure (LV EDP). An estimate of this value is provided by measuring pulmonary capillary wedge pressure (PCWP). Normal LV EDP is around 6 12 mmhg. END DIASTOLE 5
6 Basic Concepts 2. PRELOAD It is easiest to visualize the effect of preload on cardiac output (via SV) by looking at only the DIASTOLIC filling part of the P V Loop (GREEN LINE) Pressure END SYSTOLE Ventricles emptying (systole) Cardiac Pressure Volume Loop SV END DIASTOLE Ventricles filling (diastole) Volume 6
7 2. PRELOAD Basic Concepts During filling there is no muscle contraction. The rise in pressure during filling is relative to the COMPLIANCE of the ventricles (i.e. stretchiness ) Pressure Ventricles filling (diastole) while muscle relaxed SV Volume 7
8 2. PRELOAD Basic Concepts Preload is proportional to end diastolic pressure (EDP) If you Preload, then you Stroke Volume (SV) For RV, preload is increased by CVP For LV, preload is increased by PCWP Pressure Effect of Preload on Stroke Volume Higher SV Normal SV Volume 8
9 2. PRELOAD Basic Concepts In DIASTOLIC HF (red line) the heart is STIFFER (less compliant) So if you keep end diastolic pressure (EDP) the same, then SV in Diastolic HF. Pressure Low SV Diastolic HF Leftward Shift in Diastolic PV Curve (caused by reduced compliance) Same EDP Normal SV Volume 9
10 2. PRELOAD Basic Concepts To COMPENSATE for the SV in diastolic HF, the body will Preload. How does it do this? By Venous Pressure (water retention, edema) Pressure Preload Increased SV SV Higher EDP (w/ edema) Diastolic HF is typically associated withelevated preload, which helps to compensate for less heart compliance Volume 10
11 2. PRELOAD Pressure Basic Concepts In DIASTOLIC HF, the heart still contracts strongly but on a SMALLER VOLUME and is less compliant (less stretchy) END SYSTOLE SV END DIASTOLE Reduced End Diastolic Volume Volume 11
12 3. CONTRACTILITY Basic Concepts This is FORCE generated by the ventricles during systole. This is affected by various factors, including preload More Preload = More Contractility This is the FRANK STARLING LAW of the heart Frank (German) Starling (English) 12
13 3. CONTRACTILITY Basic Concepts The FRANK STARLING LAW simply states: Preload (i.e. EDV) causes Contractility (up to a point) How? Let s re visit cardiac muscle contraction Sarcomere Z line M line Sarcomere I band A band 13
14 3. CONTRACTILITY Basic Concepts Few myosin heads touching actin, ALSO: too crowded! Partially Stretched (more pre load) More myosin heads touching actin, less crowded 14
15 3. CONTRACTILITY Basic Concepts Fully stretched (even more pre load) Optimal # of myosin heads touching actin Over Stretched (too much!) 15
16 3. CONTRACTILITY Stroke Volume Basic Concepts Frank Starling Law = heart s intrinsic way of matching cardiac output to venous return. more preload (i.e. Venous Return) = more SV (i.e. Cardiac Output) Frank Starling Curve End Diastolic Volume (EDV) 16
17 3. CONTRACTILITY Basic Concepts Relationship of BLOOD VOLUME to cardiac contractility Stroke Volume Underloaded Dehydration Shock (sepsis) Apex Overloaded (CONGESTION) RIGHT VENTRICLE FAILURE Peripheral edema, ascites LEFT VENTRICLE FAILURE Pulmonary edema, dyspnea Frank Starling Curve End Diastolic Volume (EDV) 17
18 3. CONTRACTILITY Stroke Volume Basic Concepts Normal Apex A. In SYSTOLIC HF the ventricles are less contractile, so are less effective at ejecting blood at a given EDV Systolic Heart Failure B. SV in HF is also WORSENED by the increased preload (cardiac stretch) caused by edema (because CO < venous return) End Diastolic Volume (EDV) 18
19 3. CONTRACTILITY Basic Concepts In CHRONIC SYSTOLIC HF you have higher preload (giving you EDV), but the pressure it can generate and the volume it can expel are both lower ( EDV, overall SV) Pressure Reduced Peak Systolic Pressure SV Smaller Pulse Pressure Elevated Preload Higher End Systolic Volume Higher End Diastolic Volume Volume 19
20 4. AFTERLOAD Basic Concepts This is PEAK STRESS in the ventricles during SYSTOLE (i.e. ventricular contraction) It can be thought of as the stress encountered by ventricular myofibrils as they contract against the volume of blood in the heart. AFTERLOAD is proportional to PEAK SYSTOLIC PRESSURE (similar to how preload is proportional to end diastolic pressure) END SYSTOLE 20
21 4. AFTERLOAD Stroke Volume Basic Concepts increasing afterload will decrease stroke volume Afterload Curve Afterload (peak systolic stress) 21
22 4. AFTERLOAD Stroke Volume Basic Concepts With SYSTOLIC HF, for a given afterload (i.e. pulmonary artery or aortic pressure) the stroke volume is reduced (the heart can t push as strongly against that pressure) Systolic Heart Failure Normal Afterload Curve Afterload (peak systolic stress) 22
23 4. AFTERLOAD LaPlace Equation = Pr 2w Basic Concepts r w = Stress (afterload) P = systolic pressure* r = ventricular diameter w= wall thickness *For R Ventricle, P = pulmonary artery pressure *For L Ventricle, P = aortic pressure 23
24 4. AFTERLOAD Pr = 2w Basic Concepts High Systolic BP and Ventricular Dilation MAY CONTRIBUTE to HF and will affect the AFTERLOAD in the ventricles. HOW? HIGH SYSTOLIC PRESSURE (P) = HIGHER Afterload ( ) DILATED HEART (r) = HIGHER Afterload ( ) seen in 1/3 of HF The heart may COMPENSATE by wall thickness (w) through cardiac HYPERTROPHY because: THICKER VENTRICLE WALL (w) = Afterload ( ) which should CO......BUT this doesn t really help for long because cardiac hypertrophy eventually causes REDUCED CHAMBER COMPLIANCE, causing Preload which causes CO 24
25 Basic Concepts CO = SV x HR Stroke Volume, SV = EDV ESV CO = (EDV ESV) x HR EDV ESV SV PRELOAD affects End Diastolic Volume (EDV) Preload means EDV means SV means CO 25
26 Basic Concepts CO = (EDV ESV) x HR Contractility and Afterload affect End Systolic Volume (ESV) Contractility (force) EDV ESV SV Afterload (pulmonary artery or aortic pressure) Contractility means ESV means SV means CO Afterload means ESV means SV means CO 26
27 Heart Failure Hormonal Activation in HF CO Renal Perfusion CO CVP (preload) (blood volume) Na +, H 2 O uptake JGA Renin Angiotensinogen Angiotensin I Aldosterone Principal Cells (distal tubule, collecting ducts) + ACE Angiotensin II Adrenal cortex 27
28 Heart Failure Hormonal Activation in HF CO Renal Perfusion CO JGA Angiotensinogen Renin Angiotensin I Afterload (arterial BP) + ACE Angiotensin II arteriole vasoconstriction 28
29 Heart Failure Sympathetic Activation in HF CO Arterial Baroreceptor Firing Cranial nerve IX Sympathetic activity (NE) Inotropy EPI, NE Adrenal Stimulation Vasoconstriction SVR (Afterload) CVP (Preload) Cardiac Remodeling (Hypertrophy) Vagal activity Chronotropy (HR) (parasympathetic, ACh) 29
30 Inotropy Vent. Compliance HF is a Complex Web Renin CO SNS (NE, EPI) Inotropy HR Angiotensin I Afterload CO Angiotensin II Vasoconstriction CVP Aldosterone Na +, H 2 O retention Preload 30
31 Inotropic Agents Inotropy Vent. Compliance Drug Therapy for HF Renin CO SNS (NE, EPI) Inotropy Renin inhibitors blockers HR Angiotensin I Afterload ACE inhibitors Vasodilators CO Angiotensin II AT 1 antagonists (ARB) Vasoconstriction CVP Aldosterone Na +, H 2 O retention Preload K+ sparing diuretics Loop and Thiazide diuretics 31
32 In summary, to CO (CO = SV x HR), we can: I. HR Chronotropic drugs (catecholamines) II. Drug Therapy for HF SV a. PRELOAD see next page Diuretics RAA system inhibitors b. AFTERLOAD Vasodilators RAA system inhibitors blockers c. CONTRACTILITY Inotropic agents 32
33 Drug Therapy for HF Why Decrease Preload? Stroke Volume Normal Apex Treated Systolic Heart Failure EDV In a normal person, decreasing preload will REDUCE SV But in a person with HF, decreasing preload INCREASES or MINIMALLY AFFECTS SV because they often are AT OR NEAR the right side of the Frank Starling Curve 33
34 Stroke Volume Drug Therapy for HF Over Treated Apex Systolic Heart Failure EDV CO RAA activation Afterload Cardiac Remodeling Worsening of HF CAUTION: TOO MUCH DIURESIS (or too quickly) can lead to volume reduction and ACTIVATION of RAA system! 34
35 DIURETICS Drug Therapy for HF LOOP DIURETUCS [the mainstay of CHF therapy] Furosemide (Lasix ) Bumetanide (Bumex ) Torsemide (Demadex ) Ethacrynic Acid (Edecrin ) Choice drugs underlined THIAZIDE DIURETICS [can be added on for refractory CHF, refer to diuretics pharmacology lectures Dr. Connelly] Chlorothiazide (Diuril ) Chlorothalidone (Hygroton ) Metolazone (Zaroxolyn ) K + SPARING DIURETICS [discussed later in this lecture] Amiloride Triamterene (Dyrenium ) Spironolactone (Diuril ) Eplerenone (Aldactone ) 35
36 LOOP DIURETICS Capillary blood Drug Therapy for HF Loop of Henle Ascending Limb 2Cl K + 3 Na + Na + 2 K + K + Tubular Lumen Site of Action: Na K Cl cotransporter (NKCC2) CAUSE LOSS OF: Na + (H 2 O) Cl K + Most powerful diuretics. Why? About 25% of the filtered sodium re uptake happens here. 36
37 LOOP DIURETICS Drug Therapy for HF Administration: ORAL (maintenance), IV (decompendated) Oral Bioavailability: Furosemide 40 70% (variable absorption) Bumetanide >80% Torsemide 80 90% Ethacrynic Acid: ~100% Drug absorption may be REDUCED by edema in the gut wall Protein binding: All are HIGHLY protein bound (>90%) They reach their site of action (luminal surface of ascending Loop of Henle) after secretion of the free drug from the plasma into the proximal tubule. 37
38 LOOP DIURETICS Half lifes: Furosemide: h Bumetanide: h Torsemide: 3.5 h Ethacrynic acid: 2 4 h Drug Therapy for HF Duration: ORAL: 4 6 h (typical), except ethacrynic acid (12 h) IV: 2 3 h (although often given by continuous admin) 38
39 LOOP DIURETICS Route of Elimination: Drug Therapy for HF Furosemide and Bumetanide Urinary excretion (slower elimination with renal disease) Torsemide Hepatic metabolism (slower in hepatic disease, cirrhosis) Mainly by CYP2C9 Only 20% excreted in urine as parent drug Ethacrynic acid Urinary AND Biliary excretion (as cysteine conjugate) 39
40 LOOP DIURETICS Drug Therapy for HF Adverse Effects: Furosemide, Bumetanide and Torsemide have sulfonylurea moieties. They can cause hypersensitivity reactions in sensitive patients. Ethacrynic Acid is NOT a sulfonylurea. However, ethacrynic acid is MORE likely to cause ototoxicity All loop diuretics can cause K+ wasting (hypokalemia): muscle weakness, fatigue, severe cramps constipation hyperglycemia, hyperlipidemia (low insulin) abnormal heart rhythms Too aggressive therapy can lead to circulatory volume reduction (and lower CO) which may be mistaken for worsening of heart function 40
41 LOOP DIURETICS Drug Interactions: Drug Therapy for HF NSAIDs (aspirin, ibuprofen, etc.) These block prostaglandin biosynthesis (COX 1, COX 2). Prostaglandins vasodilate afferent arterioles and increase intra glomerular pressure. Therefore, NSAIDs can decrease GFR. ACE inhibitors (captopril, enalapril, lisinopril, etc.), AND AT 1 antagonists (azilsartan, losartan, valsartan, etc.) AT II receptor (AT 1 ) vasoconstricts efferent arterioles and increases intra glomerular pressure. Therefore, ACE I and ARBs can decrease GFR. Negative interactions typically short lived, occurs during initiation of drug therapy or dose escalations. 41
42 LOOP DIURETICS Loop Diuretic Resistance: Drug Therapy for HF Caused by compensatory renal Na + reabsorption ( GFR leading to activation of RAA system). Reduction in dosing intervals or adding/switching diuretic class can sometimes overcome resistance. 42
43 THIAZIDE DIURETICS Capillary blood Drug Therapy for HF Early Distal Tubule Cl 3 Na + Na + Tubular Lumen Site of Action: NaCl Symporter (SLC12A3) CAUSE LOSS OF: 2 K + Na + (H 2 O) K + Cl K + (indirect) 43
44 K+ SPARING DIURETICS Drug Therapy for HF Spironolactone, Eplerenone (Aldosterone antagonists) Capillary blood Late Distal Tubule + Collecting Ducts Tubular Lumen Site of Action: Aldosterone (mineralcorticoid) Receptor, MR 3 Na + MR CAUSE LOSS OF: Na + Na + Na+ (H 2 O) 2 K + 44
45 K+ SPARING DIURETICS Drug Therapy for HF Amiloride, Triamterene (Na + channel blockers) Capillary blood Late Distal Tubule + Collecting Ducts Tubular Lumen CAUSE LOSS OF: 3 Na + Na + Na + Na+ (H 2 O) 2 K + Site of Action: Sodium channel 45
46 K+ SPARING DIURETICS Administration: ALL ORAL Drug Therapy for HF Oral Bioavailability: Amiloride: 15 25% (poor absorption) Triamterene: 50% (poor absorption) Spironolactone: around 70% (variable, increased by food) Eplerenone: 70% Metabolism: Amiloride: NOT metabolized Triamterene: hepatic (CYP1A2 to active metabolite) Spironolactone: hepatic (to active metabolites: canrenone and 7 alpha spirolactone) Eplerenone: hepatic (CYP3A4 to inactive metabolites) AVOID strong CYP3A4 inhibitors (e.g. ritnoanvir, ketoconazole, itraconazole, clarithromycin) 46
47 K+ SPARING DIURETICS Drug Therapy for HF Half lives: Amiloride: 6 9 hr Triamterene: 1 2 hr (metabolite: 3 hr) Spironolactone: 1.5 hr (metabolites: 7 23 hr) Eplerenone: 4 6 hr Excretion: Urine and feces 47
48 K+ SPARING DIURETICS Drug Therapy for HF Adverse effects: Hyperkalemia (esp. if taking K + supplements) Electrolyte/fluid loss (reduction in CO) Spironolactone, Endocrine effects: Gynecomastia Breast tenderness Sexual dysfunction (endocrine effects not as severe with eplerenone b/c it is more selective for the aldosterone (mineralcorticoid) receptor vs. sex hormone receptors MR > AR, ER, PR) 48
49 Stroke Volume Drug Therapy for HF RAA INHIBITORS (ACE inhibitors, Renin inhibitors, AT 1 antagonists) Normal Apex Treated Systolic Heart Failure EDV Inhibition of the RAA system causes natiuresis (Na + loss) and diuresis (water loss) which decreases preload (and lowers EDV) This helps get rid of edema and may also improve cardiac output 49
50 Drug Therapy for HF RAA INHIBITORS (ACE inhibitors, Renin inhibitors, AT 1 antagonists) Stroke Volume Treated Normal Systolic Heart Failure Afterload Inhibition of the RAA system also causes arteriolar vasorelaxation (decreasing arterial BP and afterload, thus increasing CO) 50
51 Drug Therapy for HF RAA INHIBITORS ACE inhibitors Benazepril* (Lotensin ) Captopril (Capoten ) Enalapril (Vasotec ) Fosinopril (Monopril ) Lisinopril (Prinivil, Zestril ) Moexipril (Univasc ) Perindopril* (Aceon ) Quinapril (Accupril ) Ramipril (Altace ) Trandolapril (Mavik ) Renin inhibitors Aliskiren (Tekturna ) AT 1 antagonists Azilsartan (Edarbi ) Candesartan (Atacand ) Eprosartan (Teveten ) Irebesartan (Avapro ) Losartan* (Cozaar ) Olmesartan (Benicar ) Telmisartan (Micardis ) Valsartan (Diovan ) HF indications in blue Choice drugs underlined * = Off label for HF 51
52 Drug Therapy for HF RAA INHIBITORS: ACE inhibitors Angiotensin I Angiotensin II Vasoconstriction (endothelin, TxA 2 ) + ACE ACE inhibitors Inactive peptides Bradykinin Vasorelaxation (NO, EDHF, PGI 2 ) arterioles (resistance arteries) Effect of drug: Systemic vascular resistance ( BP) 52
53 Drug Therapy for HF RAA INHIBITORS: ACE inhibitors Angiotensin I Angiotensin II + ACE ACE inhibitors Adrenal glands (zona glomerulosa) Aldosterone Sodium and water reabsorption Effect of drug: Natriuresis, Diuresis 53
54 Drug Therapy for HF RAA INHIBITORS: ACE inhibitors Administration: ORAL Oral Bioavailability: Variable Low (<40%): Benazepril, Fosinopril, Lisinopril Caused by poor absorption Good (50 95%): other ACE I Effect of Food: Food INHIBITS captopril absorption by 30 40% take at least 1 hr before meals 54
55 Drug Therapy for HF RAA INHIBITORS: ACE inhibitors Metabolism: prodrug Almost all ACE I are prodrugs (rapid hydrolysis to active metabolites) But, Captopril and Lisinopril are NOT prodrugs Esterase active metabolite Excretion: Some renal Some renal and fecal Heart Failure Accumulation: Some ACE I have been shown to accumulate in patients with heart failure (due to lower CO and renal perfusion), take caution: Lisinopril, Perindopril, Quinapril Because these agents are eliminated 100% by kidneys (also take caution in other causes of renal impairment) 55
56 Drug Therapy for HF RAA INHIBITORS: ACE inhibitors Adverse Effects: Dry Cough (caused by bradykinin) Hypotension Hyperkalemia Renal function deterioration Angioedema (rare) Contraindicated in pregnancy 56
57 Drug Therapy for HF RAA INHIBITORS: AT 1 antagonists (Angiotensin II receptor blockers, ARBs) Arterioles (resistance arteries) Angiotensin II Adrenal glands (zona glomerulosa) Vasoconstriction (endothelin, TxA 2 ) AT 1 receptor Effect of drug: Systemic vascular resistance ( BP) AT 1 receptor Aldosterone Sodium and water reabsorption Effect of drug: Natriuresis, Diuresis 57
58 Administration: ORAL Absorption: Incomplete Oral Bioavailability: LOW Candesartan (15%) Losartan (33%) Valsartan (25%) Effect of Food: Drug Therapy for HF RAA INHIBITORS: AT 1 antagonists Drugs may be taken with or without food 58
59 Metabolism: Candesartan cilexetil is a prodrug Losartan is a prodrug Drug Therapy for HF RAA INHIBITORS: AT 1 antagonists Candesartan cilexetil Losartan Intestinal Esterase CYP2C9, 3A4 Valsartan is NOT a prodrug Candesartan (active) EXP
60 Drug Therapy for HF RAA INHIBITORS: AT 1 antagonists Half lives: Candesartan: 9 hr Losartan: 1 2 hr, EXP 3174: 6 9 hr Valsartan: 6 hr Excretion: mainly fecal Adverse Effects: Hypotension Hyperkalemia Reduced renal function Contraindicated in pregnancy 60
61 Drug Therapy for HF RAA INHIBITORS: AT 1 antagonists Another benefit of AT 1 antagonists Ventricular Hypertrophy (VH) Atrial Enlargement HF Angiotensin II AT 1 receptors Cell Enlargement Candesartan, Losartan, Valsartan Also, by reducing BP these drugs help prevent VH, since afterload also promotes cardiac remodeling 61
62 Drug Therapy for HF RAA INHIBITORS Aldosterone Breakthrough (several possible mechanisms) Angiotensinogen Tissue plasminogen activator Cathepsin G Renin Renin inhibitors Chymase Cathepsin G Angiotensin I ACE ACE inhibitors Angiotensin II Aldosterone antagonists Spironolactone Eplerenone AT 1 Receptor Aldosterone AT 1 antagonists fluid retention 62
63 BETA BLOCKERS Drug Therapy for HF Bisoprolol* (Zebeta ) Carvedilol (Coreg ) Metoprolol succinate ER (Toprol XL ) HF indications in blue Choice drugs underlined * = Off label for HF Beta blocker classes for HF: Bisoprolol, Metorpolol succinate ER: Second generation beta blockers ( 1 specific) Carvedilol: S( ) carvedilol: Nonselective beta blocker ( 1 and 2) R(+) and S( ): Selective alpha1 blocker ( 1) Effects of blocking 1: Arterial and Venous Vasodilation Reduced Inotropy (in response to endogenous catecholamines) 63
64 Drug Therapy for HF BETA BLOCKERS Beta blockers are a mixed bag of effects in HF CO Afterload SNS (NE, EPI) blockers Inotropy HR CO In the HEART: O 2 demand (good) Contraction (bad) Vasoconstriction In the ARTERIES: Afterload (good) CVP Preload In the VENOUS RETURN: Preload (good for HF patents) 64
65 BETA BLOCKERS Drug Therapy for HF Clinical trials have shown THREE blockers to benefit survival in patients with chronic HF: Bisoprolol Carvedilol Metorpolol ER 65 TRENDS in Pharmacological Sciences
66 BETA BLOCKERS Drug Therapy for HF What is the MECHANISM for the beneficial actions (survival benefits) of only these three blockers in HF? To summarize part of this report: We don t know why they work, But it s probably NOT due to their blocking effects 66
67 BETA BLOCKERS Normal Drug Therapy for HF EDV SV EF 1 = SV EDV Enlarged Ventricle EDV SV LOW EF EF 2 = SV EDV EF 2 < EF 1 In patients with dilated ventricular cardiomyopathy EF is low partly because the volume of the ventricles is abnormally large. (afterload is also high, Law of Laplace) Beta blockers have been shown to decrease chamber size (through cardiac remodeling) and help restore normal EF 67
68 BETA BLOCKERS Administration: ORAL Drug Therapy for HF Absorption: all are well absorbed, but... Oral Bioavailability: Bisoprolol (80%) 20% lost in 1 st pass to CYP3A4 Carvedilol (25%) 75% lost in 1 st pass to CYP2D6 (carvedilol ER has much higher bioavailability) Metoprolol (50%) 75% lost in 1 st pass to CYP2D6 Effect of Food: Drugs may be taken with or without food Half lifes: Bisoprolol: 9 12 hr Carvedilol: S( ): 7 10 hr, R(+): 5 9 hr Metoprolol: 3 7 hr 68
69 BETA BLOCKERS Drug Therapy for HF Adverse Effects: Bradycardia Syncope Dizziness Fatigue Masking signs of hypoglycemia (preventing rapid HR) Abrupt withdrawal/withdrawal syndrome: Acute tachycardia Hypertension Ischemia 69
70 VASODILATORS Drug Therapy for HF RAA Inhibitors have vasodilatory actions by blocking angiotensin II production (blocking vasoconstriction) ACE inhibitors (also bradykinin) AT 1 antagonists Other vasodilators also have beneficial effects for HF: ARTERIAL Vasodilators ( AFTERLOAD) Hydralazine (oral, high doses) for chronic management VENOUS Vasodilators ( PRELOAD) Nitroglycerin Sodium nitroprusside Isosorbide mono/di nitrate for acute decompensation 70
71 INOTROPIC DRUGS Drug Therapy for HF For management of chronic HF Cardiac Glycosides (digitalis glycosides) Digoxin (Digox, Lanoxin ) For acute decompensated HF with hypotension Catecholamines Dopamine Dobutamine Phosphodiesterase 3 (PDE 3) Inhibitors Inamrinone (Inocor ) Milrinone (Primacor ) 71
72 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides (OUT) Na + Ca 2+ 3 Na + Na + Na + Ca 2+ (IN) Digoxin (competes with K + for K + binding site) 2 K + Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ Ca 2+ SR = Inotopy Effect of drug: intracellular calcium levels (SR stores) 72
73 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides w/digoxin 73
74 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides Stroke Volume Normal Treated Systolic Heart Failure Effect on Frank Starling Curve Ventricular End Diastolic Volume (EDV) 74
75 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides Administration: ORAL (CHF), INJ (A Fib, rate control in HF patients) Oral Bioavailability: 60 80% (Variable hydrolysis in the stomach and metabolism by intestinal bacteria prior to absorption about 10% of population will lose 40% of the dose to gut bacteria) Effect of Food: food may cause a small decrease in bioavailability: Longer retention in stomach = more hydrolysis High fiber diet = more bacterial metabolism However, the effect is not believed to be significant enough to necessitate counselling patients Distribution: ss = 5 L/kg Half life: hr (3 5 days with renal failure) Excretion: Urine (80 90% as parent drug) 75
76 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides Therapeutic Window: NARROW! typical range for HF: 0.5 and 1.0 ng/ml toxicity is dose related (rare below 0.8 ng/ml) Common Adverse Effects of digoxin: Nausea, loss of appetite, diarrhea Increased urine output (caused by increased renal perfusion due to enhanced CO) not really an AE because it helps with diuresis More likely in hypokalemia (low K + ) because digoxin is more active (less competition for binding site) 76
77 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides Digitalis Toxicity (usually if >2 ng/ml) Nausea, vomiting, diarrhea, hyperkalemia Visual disturbances (yellow/green, halos) CNS: confusion, dizziness, anxiety Cardiac: arrhythmias, heart block Overdose: LD 50 = mg oral 77
78 Drug Therapy for HF INOTROPIC DRUGS: Cardiac Glycosides Toxicity/Overdose treatment: Digoxin immune FAb (DigiFab, Digibind ) For life threatening digitalis toxicity FAb (fragment, antigen binding) produced in sheep (ovine) Given by IV inj Binds to and neutralizing circulating digoxin Inactive complexes are eliminated renally Other care (supportive): Arrhythmias: magnesium, lidocaine, phenytoin Bradycardia: atropine, isoprenaline 78
79 Drug Therapy for HF INOTROPIC DRUGS: Catecholamines Dopamine (DA) and Dobutamine are inotropic catecholamines used in acute decomensated HF (low CO). Given IV. They have LESS chronotropic (HR stimulation) effects and cause LESS of an increase in myocardial O 2 consumption than isoproterenol, EPI, or NE and are more frequently used in treating HF. They also have the benefit of causing vasodilation (although, only at low doses for DA) which can GFR and Afterload. 79
80 Drug Therapy for HF INOTROPIC DRUGS: Catecholamines Dopamine: D 1 and D 2 > receptors (but also causes NE release) Strong (+) inotropy Moderate (+) chronotropy D 2 = vasodilation (low doses) Good for GFR and causing diuresis in acute CHF Vasoconstriction at high doses (hypertension, ischemia) Dobutamine: 1 and 2 > D receptors Strong (+) inotropy Moderate (+) chronotropy 2 = vasodilation Good for GFR and causing diuresis in acute CHF Less vasoconstriction than DA (less risk of hypertension) 80
81 Drug Therapy for HF INOTROPIC DRUGS: Catecholamines Dopamine, Dobutamine Gs D 1 receptor or 1 receptor EPI, NE, IsoP Ca 2+ ATP Ca 2+ (IN) AC camp PKA CONTRACTION SR Ca 2+ Stores 81
82 Drug Therapy for HF INOTROPIC DRUGS: Catecholamines Administration: IV Infusion Onset: 1 2 min (peak effect 5 10 min) Duration: < 10 min Metabolism: MAO, COMT (O methylation) Half life: 2 min Excretion: Urine (inactive metabolites) 82
83 Drug Therapy for HF INOTROPIC DRUGS: Catecholamines Adverse Effects: NOT intended for long term therapy Ventricular arrhythmias (ectopic beats) Low infusion rates: Vasodilation Possible hypotension (although, BP is usually seen because the BP lowering effect of vasodilation is offset by the increase in CO) Use carefully in hypovolemic patients (correct first) High infusion rates (esp. dopamine): Vasoconstriction Diastolic pressure Careful in patients with occlusive vascular diseases atherosclerosis arterial embolism Raynaud disease 83
84 Drug Therapy for HF INOTROPIC DRUGS: PDE3 Inhibitors Ca 2+ ATP Ca 2+ (IN) Inamrinone, Milrinone AC camp PDE3 AMP PKA CONTRACTION SR Ca 2+ Stores 84
85 Drug Therapy for HF INOTROPIC DRUGS: PDE3 Inhibitors Administration: IV bolus followed by infusion Onset: Inamrinone: 2 5 min Milrinone: 5 15 min Duration: hr Metabolism: Hepatic (glucuronidation) Half lifes: (in HF patients) Inamrinone: 6 hr Milrinone: 2.5 hr (shorter) Excretion: Urine, active tubular secretion (mostly as parent drug, consider dose reduction in patients with renal impairment) 85
86 Benefits: Drug Therapy for HF INOTROPIC DRUGS: PDE3 Inhibitors Do NOT increase heart rate (HR) or myocardial O 2 demand as much as catecholamines do (e.g. DA, IsoP, etc.) Decrease preload (filling pressures) and afterload (SVR) Enhance contractility ( CO) Adverse effects: headache, ventricular arrhythmias, chest pain Drug specific adverse effects: NOT intended for long term therapy Inamrinone: thrombocytopenia (10%) (rare with milrinone) Milrinone: vasodilation (reduced MAP), use caution in patients with marginal arterial BP and low CO. Milrinone: hypersensitivity 86
Pharmacology: Heart Failure PHPP 515 (IT-I) Fall JACOBS Monday, Oct. 14 3:00 4:50 PM
 Pharmacology: Heart Failure PHPP 515 (IT-I) Fall 2013 JACOBS Monday, Oct. 14 3:00 4:50 PM Required Reading (via Access Pharmacy) Katzung: Chapters 13 Recommended Reading (via Access Pharmacy) Goodman and
Pharmacology: Heart Failure PHPP 515 (IT-I) Fall 2013 JACOBS Monday, Oct. 14 3:00 4:50 PM Required Reading (via Access Pharmacy) Katzung: Chapters 13 Recommended Reading (via Access Pharmacy) Goodman and
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Estimated 5.7 million Americans with HF. 915, 000 new HF cases annually, HF incidence approaches
 Heart Failure: Management of a Chronic Disease Jenny Bauerly RN, CHFN, APRN-BC Heart Failure (HF) Definition A complex clinical syndrome that can result from any structural or functional cardiac disorder
Heart Failure: Management of a Chronic Disease Jenny Bauerly RN, CHFN, APRN-BC Heart Failure (HF) Definition A complex clinical syndrome that can result from any structural or functional cardiac disorder
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Drugs Used in Heart Failure. Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
1/4/18. Heart Failure Guideline Review and Update. Disclosure. Pharmacist Objectives. Pharmacy Technician Objectives. What is Heart Failure?
 Disclosure Heart Failure Guideline Review and Update I have had no financial relationship over the past 12 months with any commercial sponsor with a vested interest in this presentation. Natalie Beiter,
Disclosure Heart Failure Guideline Review and Update I have had no financial relationship over the past 12 months with any commercial sponsor with a vested interest in this presentation. Natalie Beiter,
Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF<40%
 Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF
Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF
Heart failure. Failure? blood supply insufficient for body needs. CHF = congestive heart failure. increased blood volume, interstitial fluid
 Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Cardiac Medications At A Glance
 Cardiac Medications At A Glance 1) Anticoagulants (Also known as Blood Thinners.) Dalteparin (Fragmin), Danaparoid (Orgaran) Enoxaparin (Lovenox) Heparin (various) Tinzaparin (Innohep) Warfarin (Coumadin)
Cardiac Medications At A Glance 1) Anticoagulants (Also known as Blood Thinners.) Dalteparin (Fragmin), Danaparoid (Orgaran) Enoxaparin (Lovenox) Heparin (various) Tinzaparin (Innohep) Warfarin (Coumadin)
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Antihypertensives. Antihypertensive Classes. RAAS Inhibitors. Renin-Angiotensin Cascade. Angiotensin Receptors. Approaches to Hypertension Treatment
 Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Medical Management of Acutely Decompensated Heart Failure. William T. Abraham, MD Director, Division of Cardiovascular Medicine
 Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
Therapeutics of Diuretics
 (Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
(Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Heart Failure CTSHP Fall Seminar
 Heart Failure CTSHP Fall Seminar Laurajo Ryan, PharmD, MSc, BCPS, CDE Pharmacist Learning Objectives Outline the pathophysiology of heart failure List triggers for decompensated heart failure Describe
Heart Failure CTSHP Fall Seminar Laurajo Ryan, PharmD, MSc, BCPS, CDE Pharmacist Learning Objectives Outline the pathophysiology of heart failure List triggers for decompensated heart failure Describe
Improving Transition of Care in Congestive Heart Failure. Mark J. Gloth, DO, MBA. Vice President, Chief Medical Officer HCR ManorCare
 Improving Transition of Care in Congestive Heart Failure Mark J. Gloth, DO, MBA. Vice President, Chief Medical Officer HCR ManorCare Heart Failure Fastest growing clinical cardiac disease in the United
Improving Transition of Care in Congestive Heart Failure Mark J. Gloth, DO, MBA. Vice President, Chief Medical Officer HCR ManorCare Heart Failure Fastest growing clinical cardiac disease in the United
CONGESTIVE CARDIAC FAILURE. Dr.T.Rajathilagam, M.D., S.R.M. Medical College
 CONGESTIVE CARDIAC FAILURE Dr.T.Rajathilagam, M.D., S.R.M. Medical College HEART FUNCTIONS Your heart is an amazing powerhouse that pumps and circulates 5 or 6 gallons of blood each minute through your
CONGESTIVE CARDIAC FAILURE Dr.T.Rajathilagam, M.D., S.R.M. Medical College HEART FUNCTIONS Your heart is an amazing powerhouse that pumps and circulates 5 or 6 gallons of blood each minute through your
sympatholytics sympatholytics sympatholytics
 sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari
![Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari](/thumbs/90/104323364.jpg) Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
Pre-discussion questions
 Amanda Bartlett, PA-C Dustin Bartlett, PA-C Andrea Applegate, PA-C Leslie Yearta Brown, NP CHF Round Table Discussion Objectives ANDREA- Discuss the definition and different categories of CHF DUSTIN- Define
Amanda Bartlett, PA-C Dustin Bartlett, PA-C Andrea Applegate, PA-C Leslie Yearta Brown, NP CHF Round Table Discussion Objectives ANDREA- Discuss the definition and different categories of CHF DUSTIN- Define
HEART FAILURE. Heart Failure in the US. Heart Failure (HF) 3/2/2014
 HEART FAILURE Martina Frost, PA-C Desert Cardiology of Tucson Northwest Medical Center March 2014 Heart Failure in the US Prevalence - ~5 million 650,000 new cases annually 300,000 deaths annually Leading
HEART FAILURE Martina Frost, PA-C Desert Cardiology of Tucson Northwest Medical Center March 2014 Heart Failure in the US Prevalence - ~5 million 650,000 new cases annually 300,000 deaths annually Leading
Low Efficacy Diuretics. Potassium sparing diuretics. Carbonic anhydrase inhibitors. Osmotic diuretics. Miscellaneous
 University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Low Efficacy Diuretics 1. Potassium sparing diuretics 2. Carbonic anhydrase inhibitors 3. Osmotic diuretics 4. Miscellaneous
University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Low Efficacy Diuretics 1. Potassium sparing diuretics 2. Carbonic anhydrase inhibitors 3. Osmotic diuretics 4. Miscellaneous
PRINCIPLES OF DIURETIC ACTIONS:
 DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
Chapter 21. Diuretic Agents. Mosby items and derived items 2008, 2002 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Drug Therapy of Heart Failure. Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014
 Drug Therapy of Heart Failure Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Drug Therapy of Heart Failure Definition of Heart Failure Causes Classifications
Drug Therapy of Heart Failure Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Drug Therapy of Heart Failure Definition of Heart Failure Causes Classifications
Disclosure Statement. Heart Failure: Refreshers and Updates. Objectives. CHF: Chronic Heart Failure. Definitions. Definitions 2/19/2018
 Disclosure Statement Heart Failure: Refreshers and Updates Tracy K. Pettinger, PharmD Clinical Associate Professor College of Pharmacy The planners and presenter of this presentation have disclosed no
Disclosure Statement Heart Failure: Refreshers and Updates Tracy K. Pettinger, PharmD Clinical Associate Professor College of Pharmacy The planners and presenter of this presentation have disclosed no
Congestive Heart Failure
 Congestive Heart Failure (CHF) Congestive Heart Failure - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@vcu.edu Heart failure:
Congestive Heart Failure (CHF) Congestive Heart Failure - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@vcu.edu Heart failure:
Images have been removed from the PowerPoint slides in this handout due to copyright restrictions.
 Heart Failure Heart Failure Introduction and History AHA 2015 Statistics About 6 million Americans 870,000 new cases each year 1 in 9 deaths related to HF Almost 1 million hospitalizations each year (cost
Heart Failure Heart Failure Introduction and History AHA 2015 Statistics About 6 million Americans 870,000 new cases each year 1 in 9 deaths related to HF Almost 1 million hospitalizations each year (cost
CONCORD INTERNAL & PULMONARY MEDICINE CONGESTIVE HEART FAILURE PROTOCOL. Douglas G. Kelling, Jr., MD & C. Gismondi-Eagan, MD, FACP
 CONCORD INTERNAL & PULMONARY MEDICINE CONGESTIVE HEART FAILURE PROTOCOL Douglas G. Kelling, Jr., MD & C. Gismondi-Eagan, MD, FACP Revised August 14, 2009 Page 1 Congestive Heart Failure Protocol Patients
CONCORD INTERNAL & PULMONARY MEDICINE CONGESTIVE HEART FAILURE PROTOCOL Douglas G. Kelling, Jr., MD & C. Gismondi-Eagan, MD, FACP Revised August 14, 2009 Page 1 Congestive Heart Failure Protocol Patients
Hypertension is also an important risk factor in the development of chronic kidney disease and heart failure.
 Hypertension Hypertension Hypertension is defined as either a sustained systolic blood pressure of greater than 140 mm Hg or a sustained diastolic blood pressure of greater than 90 mm Hg. Hypertension
Hypertension Hypertension Hypertension is defined as either a sustained systolic blood pressure of greater than 140 mm Hg or a sustained diastolic blood pressure of greater than 90 mm Hg. Hypertension
Advanced Heart Failure Palliative Considerations DEBBY GREENLAW, ACNPC, ACHPN, CCRN INDEPENDENT CONSULTANT ACUTE CARE NURSE PRACTITIONER
 Advanced Heart Failure Palliative Considerations DEBBY GREENLAW, ACNPC, ACHPN, CCRN INDEPENDENT CONSULTANT ACUTE CARE NURSE PRACTITIONER Objectives Recognize functional limitations associated with the
Advanced Heart Failure Palliative Considerations DEBBY GREENLAW, ACNPC, ACHPN, CCRN INDEPENDENT CONSULTANT ACUTE CARE NURSE PRACTITIONER Objectives Recognize functional limitations associated with the
THE RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM
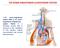 THE RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM The renin angiotensin system (RAS) or the renin angiotensin aldosterone system (RAAS) is a hormone system that is involved in the regulation of the plasma sodium
THE RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM The renin angiotensin system (RAS) or the renin angiotensin aldosterone system (RAAS) is a hormone system that is involved in the regulation of the plasma sodium
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Cardiorenal and Renocardiac Syndrome
 And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
Antihypertensive Agents
 Antihypertensive Agents Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 7, 08, presented by Ezra Levy, Pharm.D! Usual Dose,
Antihypertensive Agents Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 7, 08, presented by Ezra Levy, Pharm.D! Usual Dose,
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI
 DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
Guideline-Directed Medical Therapy
 Guideline-Directed Medical Therapy Cardiovascular Outcomes Assessment of the MitraClip Percutaneous Therapy for Heart Failure Patients with Functional Mitral Regurgitation OPTIMAL THERAPY (As defined in
Guideline-Directed Medical Therapy Cardiovascular Outcomes Assessment of the MitraClip Percutaneous Therapy for Heart Failure Patients with Functional Mitral Regurgitation OPTIMAL THERAPY (As defined in
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
M2 TEACHING UNDERSTANDING PHARMACOLOGY
 M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
DIURETICS. Assoc. Prof. Bilgen Başgut
 DIURETICS Assoc. Prof. Bilgen Başgut Classification of Diuretics The best way to classify diuretics is to look for their Site of action in the nephron A. Diuretics that inhibit transport in the Proximal
DIURETICS Assoc. Prof. Bilgen Başgut Classification of Diuretics The best way to classify diuretics is to look for their Site of action in the nephron A. Diuretics that inhibit transport in the Proximal
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
LESSON ASSIGNMENT. After completing this lesson you will be able to:
 LESSON ASSIGNMENT SUBCOURSE MD0806 LESSON 7 Therapeutics III. Antihypertensive Agents. LESSON ASSIGNMENT Paragraphs 7-1--7-12. LESSON OBJECTIVES After completing this lesson you will be able to: 7-1. From
LESSON ASSIGNMENT SUBCOURSE MD0806 LESSON 7 Therapeutics III. Antihypertensive Agents. LESSON ASSIGNMENT Paragraphs 7-1--7-12. LESSON OBJECTIVES After completing this lesson you will be able to: 7-1. From
Module 1: Evidence-based Education for Health Care Professionals
 Module 1: Evidence-based Education for Health Care Professionals Heart Failure is a HUGE Problem Prevalence Incidence Mortality Hospital Discharges Cost 1 5,300,000 660,000 284,965 1,084,000 $34.8 billion
Module 1: Evidence-based Education for Health Care Professionals Heart Failure is a HUGE Problem Prevalence Incidence Mortality Hospital Discharges Cost 1 5,300,000 660,000 284,965 1,084,000 $34.8 billion
Living with Congestive Heart Failure: A Guide to a Healthy Heart
 Living with Congestive Heart Failure: A Guide to a Healthy Heart Things to Know, Before You Go Dear Patient/Caregiver These are the things you NEED TO KNOW, BEFORE YOU GO. It is very important that you
Living with Congestive Heart Failure: A Guide to a Healthy Heart Things to Know, Before You Go Dear Patient/Caregiver These are the things you NEED TO KNOW, BEFORE YOU GO. It is very important that you
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Heart Failure Clinician Guide JANUARY 2018
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Normal Cardiac Anatomy
 Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Drugs act on Cardiovascular system (Heart Failure)
 Drugs act on Cardiovascular system (Heart Failure) Dr Laith M Abbas Al-Huseini M.B.Ch.B, M.Sc., M.Res., Ph.D. Department of Pharmacology and Therapeutics efinition and Pathophysiology Heart failure (HF)
Drugs act on Cardiovascular system (Heart Failure) Dr Laith M Abbas Al-Huseini M.B.Ch.B, M.Sc., M.Res., Ph.D. Department of Pharmacology and Therapeutics efinition and Pathophysiology Heart failure (HF)
Heart Failure Clinician Guide JANUARY 2016
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
7/21/2017. Learning Objectives. Current Cardiovascular Pharmacology. Epinephrine. Cardiotonic Agents. Epinephrine. Epinephrine. Arthur Jones, EdD, RRT
 Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Chapter 10 Worksheet Blood Pressure and Antithrombotic Agents
 Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Contemporary Management of Heart Failure. Keerthy K Narisetty, MD Comprehensive Heart Failure Management Program BHHI Primary Care Symposium
 Contemporary Management of Heart Failure Keerthy K Narisetty, MD Comprehensive Heart Failure Management Program BHHI Primary Care Symposium Disclosures I have no relevant relationships with commercial
Contemporary Management of Heart Failure Keerthy K Narisetty, MD Comprehensive Heart Failure Management Program BHHI Primary Care Symposium Disclosures I have no relevant relationships with commercial
Antihypertensives. Diagnostic category
 Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Beta 1 Beta blockers A - Propranolol,
 Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Module 1: Evidence-based Education for Health Care Professionals
 Module 1: Evidence-based Education for Health Care Professionals Heart Failure is a HUGE Problem Prevalence Incidence Mortality Hospital Discharges Cost 1 5,300,000 660,000 284,965 1,084,000 $34.8 billion
Module 1: Evidence-based Education for Health Care Professionals Heart Failure is a HUGE Problem Prevalence Incidence Mortality Hospital Discharges Cost 1 5,300,000 660,000 284,965 1,084,000 $34.8 billion
MEDICAL MANAGEMENT OF PATIENTS WITH HEART FAILURE AND REDUCED EJECTION FRACTION
 MEDICAL MANAGEMENT OF PATIENTS WITH HEART FAILURE AND REDUCED EJECTION FRACTION FRANCIS X. CELIS, D.O. OPSO FALL CONFERENCE PORTLAND, OR 16 SEPTEMBER 2017 OVERVIEW What are the ACC/AHA Stages of HF? What
MEDICAL MANAGEMENT OF PATIENTS WITH HEART FAILURE AND REDUCED EJECTION FRACTION FRANCIS X. CELIS, D.O. OPSO FALL CONFERENCE PORTLAND, OR 16 SEPTEMBER 2017 OVERVIEW What are the ACC/AHA Stages of HF? What
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
WRITER TRISTAN WALKER TABLE OF CONTENTS. The Basics of cardiac pharmacology 2007
 WRITER TRISTAN WALKER TABLE OF CONTENTS 1. WHAT ARE THE MAJOR CLASSES OF CARDIAC DRUGS?...2 2. HOW DO THEY WORK?...3 3. CONSIDERATIONS FOR THE PEDIATRIC PATIENT...7 4. SUMMARY TABLE...10 REFERENCES...14
WRITER TRISTAN WALKER TABLE OF CONTENTS 1. WHAT ARE THE MAJOR CLASSES OF CARDIAC DRUGS?...2 2. HOW DO THEY WORK?...3 3. CONSIDERATIONS FOR THE PEDIATRIC PATIENT...7 4. SUMMARY TABLE...10 REFERENCES...14
DROGAS PARA HIPERTENSION ARTERIAL JONATHAN POVEDA FERNANDEZ HSJD / 2013 FACC/FSCAI/FESC
 DROGAS PARA HIPERTENSION ARTERIAL JONATHAN POVEDA FERNANDEZ HSJD / 2013 FACC/FSCAI/FESC Pharmacotherapy of HTN Rationale for reducing arterial pressure Reduce cardiac output Reduce heart rate Reduce stroke
DROGAS PARA HIPERTENSION ARTERIAL JONATHAN POVEDA FERNANDEZ HSJD / 2013 FACC/FSCAI/FESC Pharmacotherapy of HTN Rationale for reducing arterial pressure Reduce cardiac output Reduce heart rate Reduce stroke
12.5mg, 25mg, 50mg. 25mg, 50mg. 250mg, 500mg, 250mg/5ml. 2.5mg, 5mg, 10mg. 5mg, 10mg, 20mg, 100mg. 25mg
 MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Blood Pressure P&T DATE: 9/11/2018 THERAPEUTIC CLASS: Cardiovascular Disorders REVIEW HISTORY: 5/17, 9/15, 2/13, 2/08, LOB
MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Blood Pressure P&T DATE: 9/11/2018 THERAPEUTIC CLASS: Cardiovascular Disorders REVIEW HISTORY: 5/17, 9/15, 2/13, 2/08, LOB
Heart Failure Teri Diederich, APRN April 7, Objectives. Heart Failure Statistics 3/29/2016
 Heart Failure Teri Diederich, APRN April 7, 2016 Objectives Verbalize heart failure statistics Understand cardiac anatomy and physiology Define heart failure and it s effects on cardiac anatomy Identify
Heart Failure Teri Diederich, APRN April 7, 2016 Objectives Verbalize heart failure statistics Understand cardiac anatomy and physiology Define heart failure and it s effects on cardiac anatomy Identify
HYPERTENSION IN CKD. LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL
 HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
HEART FAILURE KEEPING YOUR PATIENT AT HOME
 HEART FAILURE KEEPING YOUR PATIENT AT HOME SUZANNE FRAZIER MS, CRNP, NP-C, CHFN HEART FAILURE DISEASE MANAGEMENT COORDINATOR PENN STATE HERSHEY HEART & VASCULAR INSTITUTE IMPACT OF HEART FAILURE In 2010,
HEART FAILURE KEEPING YOUR PATIENT AT HOME SUZANNE FRAZIER MS, CRNP, NP-C, CHFN HEART FAILURE DISEASE MANAGEMENT COORDINATOR PENN STATE HERSHEY HEART & VASCULAR INSTITUTE IMPACT OF HEART FAILURE In 2010,
Hypertension (JNC-8)
 Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D.
 Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Leading Causes of Death in the U.S. Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Blood flow at rest and exercise
 Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Cardiovascular Clinical Practice Guideline Pilot Implementation
 Cardiovascular Clinical Practice Guideline Pilot Implementation Pharmacologic Management of Chronic Heart Failure Sept 15, 2004 Angela Allerman, PharmD, BCPS DoD Pharmacoeconomic Center Promoting high
Cardiovascular Clinical Practice Guideline Pilot Implementation Pharmacologic Management of Chronic Heart Failure Sept 15, 2004 Angela Allerman, PharmD, BCPS DoD Pharmacoeconomic Center Promoting high
Section 3, Lecture 2
 59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
HEART FAILURE. Heart Failure in the US. Heart Failure (HF) 10/5/2015. Martina Frost, PA-C Desert Cardiology of Tucson Northwest Medical Center
 HEART FAILURE Martina Frost, PA-C Desert Cardiology of Tucson Northwest Medical Center Heart Failure in the US Prevalence - ~5 million 650,000 new cases annually 300,000 deaths annually Leading DRG among
HEART FAILURE Martina Frost, PA-C Desert Cardiology of Tucson Northwest Medical Center Heart Failure in the US Prevalence - ~5 million 650,000 new cases annually 300,000 deaths annually Leading DRG among
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic
![Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic](/thumbs/90/103241154.jpg) Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Treatment of Congestive Heart Failure
 Treatment of Congestive Heart Failure Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 2 1 Congestive Heart Failure I Congestive heart failure (CHF) is a major contributor
Treatment of Congestive Heart Failure Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 2 1 Congestive Heart Failure I Congestive heart failure (CHF) is a major contributor
ACE Inhibitors and ARBs To Protect Your Heart? A Guide for Patients Being Treated for Stable Coronary Heart Disease
 ACE Inhibitors and ARBs To Protect Your Heart? A Guide for Patients Being Treated for Stable Coronary Heart Disease Is This Guide Right for Me? This Guide Is for You If: You have coronary heart disease,
ACE Inhibitors and ARBs To Protect Your Heart? A Guide for Patients Being Treated for Stable Coronary Heart Disease Is This Guide Right for Me? This Guide Is for You If: You have coronary heart disease,
Diuretics (Saluretics)
 Diuretics (Saluretics) Diuretics increase urine excretion mainly by reabsorption of salts and water from kidney tubules These agents are ion transport inhibitors that decrease the reabsorption of Na+ at
Diuretics (Saluretics) Diuretics increase urine excretion mainly by reabsorption of salts and water from kidney tubules These agents are ion transport inhibitors that decrease the reabsorption of Na+ at
Pharmacotherapy of Heart Failure (CHF) Inotropics and Other Agents. Edward JN Ishac, Ph.D.
 Pharmacotherapy of Heart Failure (CHF) Inotropics and Other Agents Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Pharmacotherapy of Heart Failure (CHF) Inotropics and Other Agents Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
A Guide to the Etiology, Pathophysiology, Diagnosis, and Treatment of Heart Failure. Part I: Etiology and Pathophysiology of Heart Failure
 A Guide to the Etiology, Pathophysiology, Diagnosis, and Treatment of Heart Failure Dr Badri Paudel GMC Part I: Etiology and Pathophysiology of Heart Failure Heart Failure (HF) Definition A complex clinical
A Guide to the Etiology, Pathophysiology, Diagnosis, and Treatment of Heart Failure Dr Badri Paudel GMC Part I: Etiology and Pathophysiology of Heart Failure Heart Failure (HF) Definition A complex clinical
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis.
 Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
12.5mg, 25mg, 50mg. 25mg, 50mg. 2.5mg, 5mg, 10mg. 5mg, 10mg, 20mg, 100mg. 25mg. -- $2.81 Acetazolamide (IR, 125mg, 250mg, 500mg (ER)
 MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Blood Pressure P&T DATE: 5/9/2017 THERAPEUTIC CLASS: Cardiovascular Disorders REVIEW HISTORY: 9/15, 2/13, 2/08, 5/07 LOB
MEDICATION COVERAGE POLICY PHARMACY AND THERAPEUTICS ADVISORY COMMITTEE POLICY: Blood Pressure P&T DATE: 5/9/2017 THERAPEUTIC CLASS: Cardiovascular Disorders REVIEW HISTORY: 9/15, 2/13, 2/08, 5/07 LOB
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction
 Cardio-Metabolic Franchise Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction Randy L Webb, PhD Rutgers Workshop October 21, 2016 Heart
Cardio-Metabolic Franchise Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction Randy L Webb, PhD Rutgers Workshop October 21, 2016 Heart
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Congestive Heart Failure 2015
 Definition Congestive Heart Failure 215 JP Mehegan/ Mercy Cardiology n Cardiac failure; Congestive heart failure; Chronic heart failure (synonyms) n When the heart is unable to pump sufficiently and at
Definition Congestive Heart Failure 215 JP Mehegan/ Mercy Cardiology n Cardiac failure; Congestive heart failure; Chronic heart failure (synonyms) n When the heart is unable to pump sufficiently and at
Clinical Teach-Back Cards
 Clinical Teach-Back Cards The Medicare Quality Improvement Organization for Texas TMF Health Quality Institute focuses on improving lives by improving the quality of health care through contracts with
Clinical Teach-Back Cards The Medicare Quality Improvement Organization for Texas TMF Health Quality Institute focuses on improving lives by improving the quality of health care through contracts with
