Appendix 1. Standardised data collection tool used to assess documentation of chest drain insertion.
|
|
|
- Andrea Jordan
- 5 years ago
- Views:
Transcription
1 Appendix 1. Standardised data collection tool used to assess documentation of chest drain insertion. Case number: Pre-procedure Date recorded: Yes No Time recorded: Yes No Indication for drain recorded: Yes No Specific indication for drain: Documented who made decision for drain insertion Yes N Specialty of decision maker: ACU Respiratory Other Level of decision maker: Consultant SpR SHO Record of clotting checked: Yes No Record of platelets checked: Yes No Record of up to date / recent CXR: Yes No Pre-medication recorded: Yes No Nature of pre-medication: If no pre-medication, reason documented: Yes No Nature of reason: Patient consent recorded: Yes No Nature of consent: Written Verbal Information leaflet given recorded: Yes No Procedure Location of drain insertion: Bedside Theatre Procedure room Other Bedside ultrasonography: Yes No Ultrasonography + marked in radiology: Yes No CT guided Yes No Site of drain insertion recorded: Yes No Site of drain insertion: 2% chlorhexidine / antiseptic use recorded: Yes No Mask use recorded: Yes No Gown use recorded: Yes No Sterile drapes use recorded: Yes No Local anaesthetic use recorded: Yes No Volume of local anaesthetic used recorded: Yes No Volume: Drain size recorded: Yes No Size: Length drain inserted to recorded: Yes No Length: Method drain secured recorded: Yes No Method: Post-procedure What drained recorded: Yes No What drained: Serous Turbid Blood stained Purulent Other Initial volume drained recorded: Yes No Volume: Complications recorded: Yes No Nature of complications: Post-procedure advice recorded: Yes No Nature of advice: Chest drain observation sheet: Yes No Pain score during insertion recorded: Yes No Pain: Record of post-drain CXR request: Yes No Record of post-drain CXR interpretation: Yes No Results of post-drain CXR: Investigations any aspirated samples sent for recorded: Yes No Investigations requested: Microbiology Biochemistry Cytology Other Grade of practitioner recorded: Yes No Grade of practitioner: F1/ F2 SHO SpR Consultant
2 Appendix 2. Final Chest Drain Care Bundle
3 Appendix 3. Final Pleural Procedures Guidance Pleural Procedures Guidelines INDEX: Guideline Overview Training in Pleural Procedures Indications for Pleural Procedures Use of Ultrasonography Location and Timing of Procedure Patient Consent Pre-medication and Anaesthesia Aseptic Technique Patient Position Pleural Aspiration Chest Drain Insertion Recognition and Management of Drain Complications References
4 Guidance Overview 1. Introduction Safe and appropriate use of pleural procedures by skilled and experienced operators remains a key recommendation of the British Thoracic Society (BTS) 1 following national work on significant concerns raised by the National Patient Safety Agency (NPSA) 2. This guidance is primarily based British Thoracic Society for management of pleural diseases 1, which can be found at 2. Policy Scope This policy applies to all medical staff who perform pleural aspirations and chest drain insertion, and to all nursing staff who manage patients with chest drains. 3. Policy Aims The aim of this policy is to ensure safe and effective pleural aspiration, chest drain insertion and appropriate management of patients who undergo these procedures. 4. Roles and Responsibilities Consultants and senior members of the nursing staff team are responsible for ensuring this guidance is implanted within their individual departments. It is the duty and responsibility of all medical and nursing personnel to ensure they work within this guidance.
5 Training in Pleural Procedures 1. Achieving Competence for Trainees For trainees who have not yet achieved the relevant competencies, pleural aspiration and chest drain insertion should be performed under the direct guidance of a doctor who has adequate training and experience with the relevant procedure and available equipment. 2. Competencies for Independent Pleural Aspiration or Drain Insertion The number of procedures required to achieve competency will vary between individuals. However it is anticipated that most trainees would need to have performed at least 5-10 procedures to develop the skills needed to be signed off as independent practitioners. Competence in pleural procedures must be evidenced by DOPS stating independence. Those who are already fully competent in pleural aspiration and chest drain insertion should be able to demonstrate that competence is being actively maintained. The difficulty of pleural procedures depends on many factors such as effusion size or location and body habitus. It is paramount that all clinicians, whatever their level of experience, seek senior help whenever they are uncertain whether a pleural procedure is indicated or whether it can be performed safely. 3. Further Training The respiratory team can be contacted by those who wish to obtain these competencies in pleural aspiration and / or chest drain insertion (GRH: henry.steer@glos.nhs.uk; CGH: Mark.Slade@glos.nhs.uk). For trainees within the Emergency Department, the primary point of contact for those wishing to achieve these competencies should be an Emergency Department Consultant with adequate training and experience with the relevant procedure (helen.mansfield@glos.nhs.uk).
6 1. Pleural Effusions 1a. Diagnostic Aspirations Indications for Pleural Procedures Pleural aspiration of up to 50ml of fluid is utilised for diagnostic evaluation of unilateral pleural effusions. 1b. Therapeutic Aspirations Therapeutic aspiration of up to 1.5L of fluid is usually sufficient to relieve acute breathlessness in patients with pleural effusions. It should be considered first line in patients who do not have suspected pleural infection and do not need a drain for other reasons see below. Therapeutic pleural aspiration is also preferable out of hours when chest drain insertion is best avoided unless necessary. 1c. Chest Drain Insertion Chest drain should be inserted in the following instances: Empyema and complicated parapneumonic effusions Traumatic haemo/pneumothorax During surgery in certain instances (VATS, thoracotomy, oesophagectomy, cardiac surgery) Malignant effusions for the purpose of talc pleurodesis 2. Pneumothorax 2a. Pleural Aspiration Minimally symptomatic patients with small (<2cm at level of hilum) primary pneumothoraces can be initially managed with observation alone. Aspiration should be considered first line in symptomatic patients with spontaneous primary pneumothorax of any size 1. No more than 2.5L of air should be aspirated before reassessment with CXR. 2b. Chest Drain Insertion Chest drains should be inserted for patients with pneumothorax in the following situations: In any ventilated patient
7 In tension pneumothorax after initial needle decompression Persistent or recurrent pneumothorax after initial aspiration Secondary pneumothorax Traumatic pneumothorax Bilateral pneumothoraces Some clinicians favour initial small bore ( 12F) chest drain insertion over aspiration in patients with a large/complete spontaneous primary pneumothorax. A pneumothorax in a patient over 50 with a significant smoking history should be treated as a secondary pneumothorax.
8 1. Bedside Ultrasonography Use of Ultrasonography BTS guidelines strongly recommend that all chest drains and pleural aspirations for the purposes of draining fluid be carried out under bedside ultrasound guidance by a suitably trained practitioner. This has been demonstrated to give greater likelihood of success as well as minimising the risk of adverse events and complications 1. Ultrasound is recommended especially in the case of white out to ensure that the opacified lung field is truly fluid and not consolidated/collapsed lung. If no suitably trained US operator is immediately available pleural procedures should be delayed until an ultrasound can be performed. The occasions when pleural drainage cannot be deferred for a few hours to obtain an ultrasound are rare (eg trauma), and in all other circumstances ultrasound guidance should be considered mandatory. Ultrasound is of no practical use in guiding pleural procedures for pneumothorax. 2. X-marks-the-spot Departmental Ultrasonography If X-marks-the-spot ultrasound guidance is to be used, the person who is to perform the procedure should accompany the patient to the radiology department and perform the procedure there under the ultrasound guidance. Reliance on a previously marked spot is not recommended as the technique has poor accuracy. The complication rate for X-marks-the-spot with later, separate insertion is equivalent to that of using no ultrasound guidance 1.
9 Location and Timing of Procedure 1. Location 1a. Generalities Both pleural aspiration and chest drain insertion should be performed in a clean area using full aseptic technique 1. Equipment for monitoring should be available. This includes pulse oximetry, blood pressure measurement and access to ECG. 1b. Designated Procedure Room A designated clean procedure room is preferable for aspiration or drain insertion. This should be used whenever possible unless the clinical situation demands otherwise, or a suitable alternative area exists, eg ED resus. 1c. Patient Bedside Bedside aspiration or drain insertion should only be performed where no procedure room is available. Adequate care must be taken to ensure there is sufficient space for both the procedure and appropriately sterile field. 2. Timing Pleural aspiration and chest drain insertion should be avoided outside of normal working hours unless absolutely necessary 1. This is because the complication rate has been demonstrated to be higher at these times, especially at night 1. There may be occasions where the clinical situation requires an out-of-hours pleural procedure to be performed. Out of hours pleural aspiration is preferable to chest drain. The circumstances where this may be appropriate are detailed in Section 3: Indications for Pleural Procedures.
10 Patient Consent 1. Nature of Consent Patients should be fully consented as to the risks and benefits of their pleural procedure. For pleural aspiration, documented verbal consent is adequate. For chest drain insertion, consent should be written consent except in a clinical emergency. 2. Risks of Pleural Procedures 2a. Risks of Pleural Aspirations Pain Failure of procedure Pneumothorax (about 3% with ultrasound guidance, 5-15% without ultrasound guidance) Visceral injury, haemothorax, pleural infection (rare) 2b. Risks of Chest Drain Insertion Pain Pneumothorax (5%) Bleeding / haemothorax (2%) Intrapleural infection (2%) Drain dislodgement or blockage (15%) Organ puncture (rare) Failure of procedure
11 1. Pre-medication Pre-medication and Anaesthesia 1a. Pre-medication for Pleural Aspiration Pre-medication is not routinely indicated for pleural aspiration. 1b. Pre-medication for Chest Drain Insertion Chest drain insertion is a painful procedure 1,3. As such, pre-medication with an opioid or anxiolytic agent should be strongly considered. If sedation is given, this should be in line with current guidance for conscious sedation 4 with appropriate monitoring. 2. Use of Local Anaesthesia 1% lidocaine should be infiltrated into the skin, periosteum and pleura prior to carrying out therapeutic pleural aspiration or chest drain insertion. For diagnostic pleural aspiration the needle size used to infiltrate lignocaine to the pleura is the same size as the aspiration needle and therefore the use of lignocaine may not reduce discomfort. It is thought that the volume of lidocaine given rather than the total dose is more important in achieving adequate analgesia as this helps achieve adequate spread of anaesthesia 1. For this reason 1% lidocaine is preferred to stronger formulations. Both lidocaine strength and volume given should be documented post-procedure.
12 Aseptic Technique 1. Aseptic Technique for Pleural Aspirations Pleural aspiration should be carried out in a clean area using full aseptic technique. For full aseptic technique, this requires 1 : Sterile gloves/gown Sterile field Sterile dressing Skin sterilising preparations such as iodine or chlorhexidine in alcohol 2. Aseptic Technique for Chest Drain Insertion Chest drains should likewise be inserted in a clean area using full aseptic technique. This clean area should ideally be separate from the main ward area. To achieve adequate aseptic technique, this requires 1 : Sterile gloves Sterile gown Sterile field Sterile drapes Mask Skin sterilising preparations such as chlorhexidine in alcohol Additional sterile equipment required: sterile gauze swabs, selection of syringes and needles, scalpel and blade, suture (0 or 1-0 silk), guide wire and dilators for Seldinger technique, chest tube, connecting tubing, closed drainage system including sterile water for underwater seal
13 Patient Position 1. Patient Position There are two usual positions for a patient to be sat for a pleural procedure. Upright position whilst leaning forwards with arms resting on a table or bed (image A) 1 Lying on the bed whilst slightly rotated with the arm on the side of the lesion behind the patient s head (image B) 1 Providing there is sufficient depth of fluid visible on ultrasound, an alternative is with the patient lying flat in the lateral position with arms up in front of the face 2. Site of Needle Insertion The site of needle insertion should ideally be within the triangle of safety (image C) 1 to minimise the risk to underlying structures and reduce the risk of visible scarring. Alternatively, the 2 nd intercostal space in the mid-clavicular line may be used in the case of pneumothorax. The triangle of safety is bordered by the lateral edge of latissimus dorsi, the lateral border of pectoralis major and superior to the 5 th intercostal space. A posterior approach may be used for drainage of fluid under ultrasound guidance. However, inserting the needle more posteriorly gives greater risk of damage to the intercostal artery. For this reason it is important that the site is located lateral to the angle of the rib posteriorly (at least 10cm from spine) (figure D). C D
14 Pleural Aspiration It is not the aim of this guidance to provide a step-by-step walkthrough guide to performing pleural aspiration but rather to cover the important safety points for the procedure. Therefore: Ultrasound guidance for all fluid aspirates is strongly advised Ensure adequate patient position Use small-bore needle to reduce risk of complications Insert needle above superior border of rib to avoid neurovascular bundle For diagnostic aspirations, 20-50ml of fluid is sufficient For therapeutic aspirations: - After confirming depth of the pleural space using initial needle aspiration the cannula should be advanced into the chest whilst aspirating continuously until the pleura is breached and air or fluid is withdrawn - Attach the cannula to a three-way tap to enable easy expulsion of fluid or air - Stop when no more air / fluid can be withdrawn or 1.5L has been withdrawn or until the patient develops symptoms of cough / chest discomfort Post-procedure Care After aspiration has been carried out, there are several steps to consider. A simple clean dressing should be immediately applied to the site of aspiration Follow-up chest radiograph is not indicated if the patient has had a simple, uncomplicated diagnostic tap. For diagnostic aspirates, the samples should be sent for: - Biochemistry (protein, lactate dehydrogenase, glucose) - Microbiology (M,C&S +/- acid-fast bacilli) in blood culture bottles - Cytology - ph if suspected pleural infection (into heparinised blood gas syringe. Must not be put through a gas machine if purulent) - Other tests may be indicated as discussed with respiratory team
15 1. Size of Chest Drain Chest Drain Insertion Small-bore chest drains (12-18 French) inserted with the Seldinger technique should be used as first line therapy for 1 : Pneumothoraces Pleural effusions Pleural infection / empyema Large-bore chest drains inserted with blunt dissection require a different set of competencies. These should be considered for: Haemothorax / Trauma Where risk of lung perforation exists with Seldinger needle technique (e.g. lung edge close/tethered to chest wall) Where there is worsening surgical emphysema despite small bore drain. 2. Important Points from Procedure It is not the aim of this guidance to provide a step-by-step walkthrough for inserting chest drains. Instead, it aims to cover the important safety points for the procedure. Therefore when inserting chest drains: Written consent for all chest drains should be obtained Direct ultrasound guidance is strongly recommended for pleural effusions Ensure adequate patient position and analgesia Should be carried out with full aseptic technique (including gown, sterile drapes, mask, sterile field, sterile gloves) Insert drain above superior border of rib to avoid neurovascular bundle Before fully inserting the drain, fluid (or air in the case of pneumothorax) from the site of drain insertion should be obtained. If no fluid can be drained, the procedure should be abandoned Drains should be inserted with the Seldinger technique It is imperative that the wire is not left inside the chest cavity
16 Drains should never be inserted with substantial force The dilator should not be inserted further than 1cm beyond the depth from skin to pleural space. The marker on the dilator should be set to the correct depth needed to access the pleural space, as determined by the introducer needle. 3. Securing Chest Drains A common complication of drain insertion is accidental removal due to insufficient securing methods. Chest drains should be secured with a combination of 1 : Stout non-absorbable (0 1.0 silk) suture that gathers adequate skin and subcutaneous tissue. A stitch under the skin 0.5cm from the drain exit site should be secured then the threads should be tied around the drain multiple times next to the skin to ensure that the drain can neither move forwards nor backwards. A clear dressing over the drain site It is good practice to secure the drainage tubing to the abdomen at a second point to take the direct weight off the chest drain fixing. 4. Post-procedure Care After a chest-drain has been inserted, there are several aspects to post-procedure care that must be carried out, documented and communicated to the nursing staff and/or patient. These include: Keep the bucket below hip level Complete record for chest drain insertion (utilising Trust chest drain proforma) Post-procedure radiograph for all successful or failed chest drain attempts Rate of drainage for pleural effusions / empyema / haemothorax: - A maximum of 1.5L should be drained in the first hour after chest drain insertion to reduce the risk of re-expansion pulmonary oedema. Drainage should be ceased immediately if the patient begins to cough. It can be cautiously restarted 1 hour later if the coughing ceases with cessation of drainage. - A suitable regime for rate of drainage should be provided by the doctor inserting the drain a recommended regime would be drain 1-1.5L, clamp for 4 hour, drain 1L, clamp for 4 hour then repeat
17 Prophylactic Fragmin can be given after drain insertion, providing there are no bleeding complications or haemothorax. Clamping chest drains: - A bubbling chest drain should NEVER be clamped - Clamping drains in the case of pneumothorax, once bubbling has ceased and the lung is fully re-inflated on CXR, should be done under the direct guidance of respiratory registrar or consultant only. In the case of empyema, regular flushes (2-4 times per day) with 10-20ml of normal saline should be prescribed on the drug chart to reduce the likelihood of drain blockage. Suction may occasionally be used. This should be under the guidance of a respiratory registrar or consultant. This should be high volume low pressure thoracic suction Nursed on a ward familiar with the management and monitoring of chest drains (generally respiratory ward except in exceptional circumstances) Chest drains should be checked daily for signs of wound infection, drainage volumes, swinging & bubbling, and for loose connections which can allow air into the drain and produce bubbling even when the air leak from the lung has ceased.
18 1. Bleeding 1a. Recognition Recognition and Management of Drain Complications It is not uncommon for a small amount of bleeding during drain insertion however this should quickly stop. Bruising/swelling around drain insertion site. Frank blood draining from the drain which quickly clots (unless known haemothorax). This can be difficult at times to distinguish from heavily blood stained effusion however these should not clot. Signs and symptoms of shock. This may develop several hours after the procedure. Increasing dyspnoea post drain insertion and CXR showing no change or increasing effusion size. Bleeding can rarely be a complication of drain removal. This occurs when a vessel is penetrated during drain insertion but is then tamponaded by the drain until it is removed. 1b. Management Check urgent haemoglobin, coagulation, cross match Obtain good intravenous access. Apply continuous pressure to the intercostal space at the site of pleural intervention. This can be very effective in compressing the bleeding vessel and slowing the rate of blood loss. Significant bleeds will require resuscitation of the patient and urgent discussion with the thoracic surgeons. 2. Surgical Emphysema 2a. Recognition Occurs when air is trapped under the skin, is usually associated with pneumothorax. Subcutaneous swelling, which in extreme circumstances can extend up to involve the face and neck. In this circumstance it has the potential to cause airway compromise and restrict drainage from the jugular veins. Crepitus on palpation CXR showing radiolucent streaks throughout the subcutaneous tissue and muscle. 2b. Management
19 Ensure that any pneumothorax present is being appropriately managed with a functioning chest drain and the drain is not kinked. Check that proximal drainage holes are not in subcutaneous tissue. Management is usually conservative and the air should reabsorb on its own over time, however patients should be closely monitored especially if the emphysema is extending. If airway compromise is suspected urgent senior anaesthetic assistance is required. A blunt dissection, wide bore drain may be required if progressive surgical emphysema despite narrow bore drain or if pneumothorax is not large enough to insert Seldinger drain safely. In rare cases skin incision +/- subcutaneous drain to allow the release of air can be considered only after discussion with a respiratory or ITU consultant. 3. Pneumothorax 3a. Recognition Small pneumothoraces are relatively common complication of chest drain insertion and will be noted on CXR. Consider if the patient is at risk of trapped lung, which is due to the lung being fixed and unable to expand once pleural fluid is drained. This is especially common in mesothelioma but can also occur in other malignant effusions and in empyema. 3b. Management Ensure that the drain is correctly positioned and swinging (fluid in drainage tubing moves with respiration) a swinging drain means that it is functioning. Check the connections and underwater seal Discuss with respiratory team 4. Secondary Infection 4a. Recognition Risk of infection increases the longer the drain is in situ. Cloudy pleural fluid, pain, infection round drain exit site. Clinical signs of sepsis 4b. Management Aspirate some pleural fluid and send for MC&S and culture. Discuss with microbiology and respiratory. 5. Pain 5a. Recognition Pain is common post drain insertion and is managed with regular analgesia, including opiates if necessary.
20 Chest pain and discomfort can also result from negative intrapleural pressure during fluid removal. This can indicate an underlying trapped lung and can be accompanied by vasovagal responses. 5b. Management Check for other complications, including haemorrhage. If pain due to rapid fluid drainage is suspected, turn the drain off and leave it off for 2 hours or until the pain has completely settled. Analgesia 6. Drain Blockage If the drain is no longer swinging or draining any fluid this can be an indication that it is blocked. Flushing the drain with 20mls of normal saline is usually sufficient to relieve any blockage. 7. Drain Dislodgement This occurs when a drain has not been adequately sutured in place. The drain should never be advanced again due to risk of infection but can be pulled back slightly and resutured if drain is in too far. Consider removing the drain.
21 References (1) Pleural procedures and thoracic ultrasound; British Thoracic Society pleural disease guideline BTS Guidance. Thorax 2010; 65 (suppl 2); ii61-ii76. (2) NPSA Alert. (3) Chest tube insertion: a prospective evaluation of pain management. Luketich JD, Kiss M, Hershey J, et al. Clinical Journal of Pain 1998(14): 152e4. (4) Implementing and ensuring safe sedation practice for healthcare procedures in adults. Academy of Medical Royal Colleges. London: Academy of Medical Royal Colleges, 2001.
Trust Guidelines. Title: Guidelines for chest drain insertion
 Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Comment / Changes / Approval. Initial version for consultation
 Document Control Title Pleural Procedures Guidelines Author Respiratory Consultant Directorate Medicine Date Version Issued 0.1 Aug 2011 0.2 Sep 2011 0.3 Sep 2011 0.4 Oct 2011 1.0 Oct 2011 Status Draft
Document Control Title Pleural Procedures Guidelines Author Respiratory Consultant Directorate Medicine Date Version Issued 0.1 Aug 2011 0.2 Sep 2011 0.3 Sep 2011 0.4 Oct 2011 1.0 Oct 2011 Status Draft
North West London Trauma Network. Management of Chest Drains
 North West London Trauma Network Management of Chest Drains Contents Introduction... 2 What is a chest drain?... 2 Indications for insertion:... 2 Insertion of drain:... 3 Equipment:... 3 Procedure...
North West London Trauma Network Management of Chest Drains Contents Introduction... 2 What is a chest drain?... 2 Indications for insertion:... 2 Insertion of drain:... 3 Equipment:... 3 Procedure...
CHEST DRAIN PROTOCOL
 CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
(SKILLS/HANDS-ON) Chest Tubes. Rebecca Carman, MSN, ACNP-BC. Amanda Shumway, PA-C. Thomas W. White, MD, FACS, CNSC
 (SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
(SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Critical Care Monitoring. Indications. Pleural Space. Chest Drainage. Chest Drainage. Potential space. Contains fluid lubricant
 Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003
 BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003 GRADING OF PRIMARY LITERATURE(The Bibliographies) Ia Meta-analysis analysis of randomised trials Ib Randomised controlled trial IIa Well
BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003 GRADING OF PRIMARY LITERATURE(The Bibliographies) Ia Meta-analysis analysis of randomised trials Ib Randomised controlled trial IIa Well
Pleural Effusion. Exudative pleural effusion - Involve an increase in capillary permeability and impaired pleural fluid resorption
 Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Pleural procedures and thoracic ultrasound: British Thoracic Society pleural disease guideline 2010
 < Supplementary appendices 1-4 are published online only. To view these files please visit the journal online (http://thorax. bmj.com). 1 Wellcome Trust Clinical Research Facility, Southampton General
< Supplementary appendices 1-4 are published online only. To view these files please visit the journal online (http://thorax. bmj.com). 1 Wellcome Trust Clinical Research Facility, Southampton General
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Chest Tube Thoracostomy
 Chest Tube Thoracostomy INTRODUCTION A chest tube thoracostomy is commonly done in the ED to evacuate an abnormal accumulation of fluid (blood, empyema) or air from the pleural space under an elective,
Chest Tube Thoracostomy INTRODUCTION A chest tube thoracostomy is commonly done in the ED to evacuate an abnormal accumulation of fluid (blood, empyema) or air from the pleural space under an elective,
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
Central Venous Line Insertion
 Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
relieve pressure on the lungs treat symptoms such as shortness of breath and pain determine the cause of excess fluid in the pleural space.
 Scan for mobile link. Thoracentesis Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions, a condition in which the space between the lungs and the inside of the
Scan for mobile link. Thoracentesis Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions, a condition in which the space between the lungs and the inside of the
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Information for Patients
 Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
ASEPT -System ASEPT Pleural/Peritoneal. ASEPT Drainage Kits (600 ml + 1,200 ml) Accessories. Quality and Experience
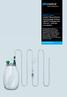
 Quality and Experience ASEPT -System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 1,200 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Quality and Experience ASEPT -System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 1,200 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury
 Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
ASEPT System ASEPT Pleural/Peritoneal. ASEPT Drainage Kits (600 ml ml) Accessories. Quality and Experience
 Quality and Experience ASEPT System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 000 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Quality and Experience ASEPT System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 000 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Standard Operational Procedure. Drainage of Malignant Ascites (Abdominal Paracentesis)
 Standard Operational Procedure Drainage of Malignant Ascites (Abdominal Paracentesis) Background Cancers that involve the peritoneum can cause fluid to build up within the abdominal cavity. This is most
Standard Operational Procedure Drainage of Malignant Ascites (Abdominal Paracentesis) Background Cancers that involve the peritoneum can cause fluid to build up within the abdominal cavity. This is most
Supplementary Online Content
 Supplementary Online Content Rahman NM, Pepperell J, Rehal S, et al. Effect of opioids vs NSAIDs and larger vs smaller chest tube size on pain control and pleurodesis efficacy among patients with malignant
Supplementary Online Content Rahman NM, Pepperell J, Rehal S, et al. Effect of opioids vs NSAIDs and larger vs smaller chest tube size on pain control and pleurodesis efficacy among patients with malignant
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Insertion of a totally implantable vascular access device (TIVAD)
 Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Nephrostomy. Radiology Department. Patient information leaflet
 Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Procedures/Risks:central venous catheter
 Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Nephrostomy. Radiology
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Nephrostomy Radiology This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Nephrostomy Radiology This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and
Insertion of a Haemodialysis Catheter
 Insertion of a Haemodialysis Catheter Exceptional healthcare, personally delivered Introduction This leaflet is about the procedure required to put in a temporary dialysis catheter. It is intended to give
Insertion of a Haemodialysis Catheter Exceptional healthcare, personally delivered Introduction This leaflet is about the procedure required to put in a temporary dialysis catheter. It is intended to give
LESSON ASSIGNMENT. Emergency Surgical Procedures. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Emergency Surgical Procedures. LESSON ASSIGNMENT Paragraphs 3-1 through 3-6. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify the steps in
LESSON ASSIGNMENT LESSON 3 Emergency Surgical Procedures. LESSON ASSIGNMENT Paragraphs 3-1 through 3-6. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify the steps in
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS
 Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Having a radiologically inserted gastrostomy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
Transjugular liver biopsy
 Transjugular liver biopsy Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a transjugular liver biopsy. It explains what is involved and the possible
Transjugular liver biopsy Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a transjugular liver biopsy. It explains what is involved and the possible
Sterile Technique & IJ/Femoral Return Demonstration
 Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Antegrade ureteric stent insertion Patient information
 Antegrade ureteric stent insertion Patient information This leaflet tells you about having antegrade ureteric stenting. It explains what is involved and what the possible risks are. It is not meant to
Antegrade ureteric stent insertion Patient information This leaflet tells you about having antegrade ureteric stenting. It explains what is involved and what the possible risks are. It is not meant to
Skin tunnelled dialysis catheter (Tesio ) insertion
 Skin tunnelled dialysis catheter (Tesio ) insertion This leaflet explains more about Tesio insertion, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
Skin tunnelled dialysis catheter (Tesio ) insertion This leaflet explains more about Tesio insertion, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
Superior vena cava stent
 Radiology department Superior vena cava stent Introduction This leaflet tells you about the procedure known as superior vena cava (SVC) stent insertion. It explains what is involved and what the benefits
Radiology department Superior vena cava stent Introduction This leaflet tells you about the procedure known as superior vena cava (SVC) stent insertion. It explains what is involved and what the benefits
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Having a diagnostic catheter angiogram
 Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Peripherally Inserted Central Catheter (PICC) Booklet
 Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
2. Indications Infusion of hyperosmolar medication, e.g. TPN. Administration of vasoactive/irritant drugs.
 Policy and Procedure for Insertion and care of Peripherally Inserted Central Catheters by Neonatal Staff (see Ch 8 TPN) 1. Introduction The peripherally inserted central catheter (PICC) is an intravenous
Policy and Procedure for Insertion and care of Peripherally Inserted Central Catheters by Neonatal Staff (see Ch 8 TPN) 1. Introduction The peripherally inserted central catheter (PICC) is an intravenous
INTERCOSTAL CATHETER (ICC) & UNDERWATER SEAL DRAINAGE (UWSD) Self-Directed Learning Package
 INTERCOSTAL CATHETER (ICC) & UNDERWATER SEAL DRAINAGE (UWSD) Self-Directed Learning Package Name: Belmore ID: Date: Intercostal Catheters and UWSD Updated 27/11/2010 Page 1 of 22 TABLE OF CONTENTS INTRODUCTION...
INTERCOSTAL CATHETER (ICC) & UNDERWATER SEAL DRAINAGE (UWSD) Self-Directed Learning Package Name: Belmore ID: Date: Intercostal Catheters and UWSD Updated 27/11/2010 Page 1 of 22 TABLE OF CONTENTS INTRODUCTION...
Needle biopsy of lung or pleura (lining of the lung) (guided by ultrasound or CT scanner)
 Needle biopsy of lung or pleura (guided by ultrasound or CT scanner) Turnberg Building Respiratory Medicine 0161 206 4039 Page 1 of 6 Document for issue as handout. Unique Identifier: MED23(18). Review
Needle biopsy of lung or pleura (guided by ultrasound or CT scanner) Turnberg Building Respiratory Medicine 0161 206 4039 Page 1 of 6 Document for issue as handout. Unique Identifier: MED23(18). Review
Identification of Factors Affecting Complications of Chest Drains in Menoufiya University Hospital
 Journal of American Science, ;7(9) Identification of Factors Affecting Complications of Chest Drains in Menoufiya University Hospital Neama Ali Riad and * Amina Ebrahim Badawy Medical-Surgical Nursing,
Journal of American Science, ;7(9) Identification of Factors Affecting Complications of Chest Drains in Menoufiya University Hospital Neama Ali Riad and * Amina Ebrahim Badawy Medical-Surgical Nursing,
Lung Investigation Service Patient Information Leaflet
 Thoracoscopy Lung Investigation Service Patient Information Leaflet Introduction The purpose of this leaflet is to answer any questions you may have about having a thoracoscopy. If you are unsure of anything,
Thoracoscopy Lung Investigation Service Patient Information Leaflet Introduction The purpose of this leaflet is to answer any questions you may have about having a thoracoscopy. If you are unsure of anything,
CHEST INJURIES. Jacek Piątkowski M.D., Ph. D.
 CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
Paravertebral policy. The Acute pain Management Dept, UCLH
 UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
Pneumothorax and Chest Tube Problems
 Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Title of Guideline (must include the word Guideline (not. Guidelines. Contact Name and Job Title (author)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Date of submission Date on which guideline must be
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Date of submission Date on which guideline must be
INFORMATION FOR PATIENTS AND FAMILIES. CT guided lung biopsy (under local anaesthetic)
 INFORMATION FOR PATIENTS AND FAMILIES CT guided lung biopsy (under local anaesthetic) This leaflet provides information about the test you are due to have. It should replace the discussions you have with
INFORMATION FOR PATIENTS AND FAMILIES CT guided lung biopsy (under local anaesthetic) This leaflet provides information about the test you are due to have. It should replace the discussions you have with
relieve pressure on the lungs treat symptoms such as shortness of breath and pain determine the cause of excess fluid in the pleural space.
 Scan for mobile link. Chest Interventions What are Chest Interventions? Chest interventions are minimally invasive procedures used to diagnose and treat pleural effusions, a condition in which there is
Scan for mobile link. Chest Interventions What are Chest Interventions? Chest interventions are minimally invasive procedures used to diagnose and treat pleural effusions, a condition in which there is
Diagnostic and therapeutic pleural aspiration
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient Diagnostic and therapeutic pleural aspiration affix patient label Who is this leaflet for? This leaflet
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient Diagnostic and therapeutic pleural aspiration affix patient label Who is this leaflet for? This leaflet
Inferior Vena Cava (IVC) filter insertion. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Inferior Vena Cava (IVC) filter insertion An information guide Inferior Vena Cava (IVC) Filter Insertion Introduction This leaflet tells
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Inferior Vena Cava (IVC) filter insertion An information guide Inferior Vena Cava (IVC) Filter Insertion Introduction This leaflet tells
Transjugular Liver Biopsy UHB is a no smoking Trust
 Transjugular Liver Biopsy UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction, benefits and alternatives
Transjugular Liver Biopsy UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction, benefits and alternatives
In ESH we usually see blunt chest trauma but penetrating injuries also treated here (usually as single injuries, like stab wound)
 Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
CHEST TRAUMA. Dr Naeem Zia FCPS,FACS,FRCS
 CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
Patient Information Undergoing Percutaneous Nephrostomy. Directorate of Clinical Radiology
 Patient Information Undergoing Percutaneous Nephrostomy Directorate of Clinical Radiology Introduction This leaflet tells you about the procedure known as percutaneous nephrostomy, explains what is involved
Patient Information Undergoing Percutaneous Nephrostomy Directorate of Clinical Radiology Introduction This leaflet tells you about the procedure known as percutaneous nephrostomy, explains what is involved
ASEPT. Pleural Drainage System INSTRUCTIONS FOR USE. Rx only REF LOT. STERILE EO Sterilized using ethylene oxide
 ASEPT Pleural Drainage System INSTRUCTIONS FOR USE L1171/D REV 2014-02 2 Do not reuse 2 STERILIZE Do not resterilize Store at room temperature STERILE EO Sterilized using ethylene oxide Rx only Do not
ASEPT Pleural Drainage System INSTRUCTIONS FOR USE L1171/D REV 2014-02 2 Do not reuse 2 STERILIZE Do not resterilize Store at room temperature STERILE EO Sterilized using ethylene oxide Rx only Do not
Antegrade Ureteric Stent
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Antegrade Ureteric Stent Radiology This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Antegrade Ureteric Stent Radiology This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains
PERCUTANEOUS BILIARY DRAINAGE
 PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
Understanding your HICKMAN CATHETER
 Understanding your HICKMAN CATHETER Patient Information What is the purpose of this information sheet? This information sheet has been written by patients, members of the public and health professionals.
Understanding your HICKMAN CATHETER Patient Information What is the purpose of this information sheet? This information sheet has been written by patients, members of the public and health professionals.
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Antegrade Ureteric Stent
 Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Prostate Artery Embolisation (PAE)
 Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
Service: Imaging Prostate Artery Embolisation (PAE) Exceptional healthcare, personally delivered Ask 3 Questions The team delivering your healthcare want to encourage you to become as involved as possible
PROTOCOL FOR THE INSERTION OF NON TUNNELLED DIALYSIS CENTRAL VENOUS CATHETERS
 PROTOCOL FOR THE INSERTION OF NON TUNNELLED DIALYSIS CENTRAL VENOUS CATHETERS Version 1.0 Author Vinod Mathrani, Kieron Donovan, Steve Riley, Soma Meran, Gareth Roberts, Vinod Ravindran Agreed 06/11/2015
PROTOCOL FOR THE INSERTION OF NON TUNNELLED DIALYSIS CENTRAL VENOUS CATHETERS Version 1.0 Author Vinod Mathrani, Kieron Donovan, Steve Riley, Soma Meran, Gareth Roberts, Vinod Ravindran Agreed 06/11/2015
Radiological insertion of a nephrostomy and ureteric stent. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Radiological insertion of a nephrostomy and ureteric stent An information guide Radiological Insertion of Nephrostomy and Ureteric Stent
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Radiological insertion of a nephrostomy and ureteric stent An information guide Radiological Insertion of Nephrostomy and Ureteric Stent
Cheltenham General Hospital
 Page 1 of 5 Coronary angioplasty Introduction This leaflet provides information for patients undergoing coronary angioplasty also known as PCI (Percutaneous Coronary Intervention). What is coronary artery
Page 1 of 5 Coronary angioplasty Introduction This leaflet provides information for patients undergoing coronary angioplasty also known as PCI (Percutaneous Coronary Intervention). What is coronary artery
Date: I hereby consent to and authorize Chest Medicine Associates and other individuals involved in my care to perform a thoracentesis procedure.
 Consent for Surgical and Medical Treatment Patient Name: ----------- Date: --------------- Patient Number: _ Treatment Location: Chest Medicine Associates Date of Birth: ~~ I hereby consent to and authorize
Consent for Surgical and Medical Treatment Patient Name: ----------- Date: --------------- Patient Number: _ Treatment Location: Chest Medicine Associates Date of Birth: ~~ I hereby consent to and authorize
Trust Guideline for the management of Parapneumonic Effusion in children
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
ASEPT. Pleural Drainage System INSTRUCTIONS FOR USE REF LOT STERILE EO. Manufactured for: 824 Twelfth Avenue Bethlehem, PA
 ASEPT Pleural Drainage System LS-00116-01-AB 017-11 INSTRUCTIONS FOR USE Do not reuse STERILIZE Do not resterilize 30 C Rx only 15 C REF Store at controlled room temperature 15-30 C (59-86 F) Keep away
ASEPT Pleural Drainage System LS-00116-01-AB 017-11 INSTRUCTIONS FOR USE Do not reuse STERILIZE Do not resterilize 30 C Rx only 15 C REF Store at controlled room temperature 15-30 C (59-86 F) Keep away
Central venous access devices for children with lysosomal storage disorders
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Chest Trauma.
 Chest Trauma www.fisiokinesiterapia.biz Objectives Anatomy of Thorax Main Causes of Chest Injuries S/S of Chest Injuries Different Types of Chest Injuries Treatments of Chest Injuries Anatomy of the chest
Chest Trauma www.fisiokinesiterapia.biz Objectives Anatomy of Thorax Main Causes of Chest Injuries S/S of Chest Injuries Different Types of Chest Injuries Treatments of Chest Injuries Anatomy of the chest
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Trauma CT Scanning Protocol
 Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Arterial Line Insertion Pre Reading
 PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
Southern Sudan Medical Bulletin vol 2 no 1. Box 1. CAGE questionnaire Have you ever felt you should Cut down on your drinking?
 Management of Dependence on Alcohol - 2nd Of Two Articles a Dr Eluzai Hakim, FRCP Consultant Physician, St Mary s Hospital, Newport, Isle of Wight PO30 5TG UK b Introduction The management of alcohol dependence
Management of Dependence on Alcohol - 2nd Of Two Articles a Dr Eluzai Hakim, FRCP Consultant Physician, St Mary s Hospital, Newport, Isle of Wight PO30 5TG UK b Introduction The management of alcohol dependence
Suprapubic catheter insertion in the radiology department. Information for patients Urology
 Suprapubic catheter insertion in the radiology department Information for patients Urology page 2 of 8 What is a suprapubic catheter? A suprapubic catheter is an indwelling tube that drains the bladder
Suprapubic catheter insertion in the radiology department Information for patients Urology page 2 of 8 What is a suprapubic catheter? A suprapubic catheter is an indwelling tube that drains the bladder
Arch Angiography. Exceptional healthcare, personally delivered
 Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
STANDARDIZED PROCEDURE NEONATAL / PEDIATRIC CHEST TUBE PLACEMENT (Neonatal, Pediatric)
 I. Definition To place a tube in the pleural space to decompress a tension pneumothorax or fluid accumulation in order to allow adequate lung expansion for ventilation. II. Background Information A. Setting:
I. Definition To place a tube in the pleural space to decompress a tension pneumothorax or fluid accumulation in order to allow adequate lung expansion for ventilation. II. Background Information A. Setting:
Information for patients undergoing Angiography (Angiogram) or Arteriography (Arteriogram) Patient Information
 Information for patients undergoing Angiography (Angiogram) or Arteriography (Arteriogram) Patient Information Author ID: SH Leaflet Number: X-ray 004 Version: 6 Name of Leaflet: Information for patients
Information for patients undergoing Angiography (Angiogram) or Arteriography (Arteriogram) Patient Information Author ID: SH Leaflet Number: X-ray 004 Version: 6 Name of Leaflet: Information for patients
Angiogram, angioplasty and stenting
 Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Lumbar drains. Information for patients Neurosurgery
 Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Indwelling pleural drainage system explained
 Indwelling pleural drainage system explained Respiratory Medicine Patient Information Leaflet Introduction This leaflet is about the procedure to fit an indwelling drainage system. It tells you what the
Indwelling pleural drainage system explained Respiratory Medicine Patient Information Leaflet Introduction This leaflet is about the procedure to fit an indwelling drainage system. It tells you what the
Radiology department. Vena cava filter
 Radiology department Vena cava filter Introduction This leaflet tells you about the procedure known as vena cava filter insertion. It explains what is involved and what the benefits and risks are. It may
Radiology department Vena cava filter Introduction This leaflet tells you about the procedure known as vena cava filter insertion. It explains what is involved and what the benefits and risks are. It may
National Hospital for Neurology and Neurosurgery. Muscle biopsy Centre for Neuromuscular Diseases
 National Hospital for Neurology and Neurosurgery Muscle biopsy Centre for Neuromuscular Diseases If you would like this document in another language or format or if you require the services of an interpreter
National Hospital for Neurology and Neurosurgery Muscle biopsy Centre for Neuromuscular Diseases If you would like this document in another language or format or if you require the services of an interpreter
Your Angiogram/ Angioplasty and Stenting
 Your Angiogram/ Angioplasty and Stenting Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Your Angiogram/ Angioplasty and Stenting Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Pericardiocentesis and Drainage by a Silicon Rubber Line. without Echocardiographic Guidance. Experience in 55 Consecutive Patients
 Pericardiocentesis and Drainage by a Silicon Rubber Line without Echocardiographic Guidance Experience in 55 Consecutive Patients Kunshen LIU, M.D., Wenling LIU, M.D., Xiaotao LI, M.D., Yue XIA, M.D.,
Pericardiocentesis and Drainage by a Silicon Rubber Line without Echocardiographic Guidance Experience in 55 Consecutive Patients Kunshen LIU, M.D., Wenling LIU, M.D., Xiaotao LI, M.D., Yue XIA, M.D.,
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Testicular Vein Embolisation
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Testicular Vein Embolisation Radiology This leaflet tells you about the procedure known as a testicular vein embolisation.
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Testicular Vein Embolisation Radiology This leaflet tells you about the procedure known as a testicular vein embolisation.
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
