Hypothermia & Local Cold Injuries
|
|
|
- Hester Boone
- 5 years ago
- Views:
Transcription
1 Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital and hospital treatment of hypothermia Discuss pre-hospital and hospital treatment of local cold injuries Radiation Heat transferred from one structure to another without heating air Sunshine on a cold, winter day Convection Heat transferred to air around body or structure Infra-red thermogram of body heat Significant of heat loss with air movement Types of heat loss Thermoregulation Evaporation Heat transferred to water molecules then evaporate Sweating when exercising Significant of heat loss with air movement Conduction Heat transferred directly between bodies or structures Patient laying on a cold, tile floor for hours Up to 35 X greater loss in water compared to air Normal temp 98.6 F Normal range = 96.9 to 99.9 F Normal temperature required for body s chemical reactions to function Core temperature variations Lower in the morning Higher in the early afternoon Higher in women during some parts of menstrual cycle 1
2 Thermoregulation Peripheral thermoreceptors Entire outer surface of body More in upper torso Fewer in lower torso Fewer still in lower limbs Sends signals to hypothalmus Central thermoreceptors in: Abdominal organs Spinal cord Hypothalamus All provide temperature input to hypothalamus Thermoregulation Hypothalamus Integrates input from both peripheral and central inputs Maintains core temperature Core temp = sweating Core temp = cold response Vascular response Vasoconstriction Shunts blood from cold areas Preserves core temperature Ability to constrict affected by sunburn for up to one week Drop in blood pressure with immersion rescue Thermoregulation Evaporation suppressed Metabolic response Increase REQUIRED to maintain core temperature Metabolic rate will by 4% for every of 1 F in core Metabolic response Glucose stores mobilized, then quickly depleted if not replenished Shivering may triple oxygen consumption Thermoregulation Neurological response Enzyme function sensitive Usually first system impaired Changed personality/behavior Poor memory or judgment Slurred speech Decreased consciousness Nerve chilling shivering Cardiovascular response myocardial O 2 consumption Cardiac output will Heart rate will and then If patient is tachycardiac with hypothermia, look for another cause 2
3 Thermoregulation Cardiovascular response Conduction more sensitive PR, QRS, QT interval increased Shivering may obscure P wave All types of arrhythmias found J wave (Osburn wave) Cardiovascular response J wave (Osburn wave) May occur in core temp 90 F Most commonly found in II/V 6 When core temps are below 77 F, may be found in V 3 & V 4 J-Wave (Osburn Wave) Thermoregulation Respiratory response Increased rate, followed by depression 5 10 breaths/minute with core temperature 86 F Chest wall loses elasticity Hypoxia increased by cold Renal response Vasoconstriction central vascular volume volume = diuresis Immersion U/O by 3.5 X Alcohol can double this!!! Thermoregulation Coagulation response Enzyme malfunction causes clotting problems Platelets become inactive Diuresis leads to hemoconcentration RBCs lose ability to deform Risk Factors Exhaustion Glucose stores exhausted No glucose for shivering Hypoglycemia decreases temperature for shivering threshold Immobilization Unable to generate heat Includes entrapment Meds affecting glucose Beta blockers Steroids Oral anti-hyperglycemics Risk Factors Alcohol Affects judgment and decision making capability May heat loss through vasodilitation, not proven Creates hypoglycemia Hypoxia Decreases regulated core temperature Inadequate clothing Simplest way to prevent Affected by: Windchill Wet clothing 3
4 Risk Factors Spinal cord injuries Acute injury may cause spinal shock vasodilitation Lack of movement decreases heat generation by movement Age Infants Lack of ability to shiver until about 2 years of age Generate heat from brown fat Premature babies lack substantial brown fat = greater risk for hypothermia Large head size radiates heat Risk Factors Age Children Activity usually generates a substantial amount of heat Large head size radiates heat Age Elderly Decreased fat & insulation Decreased muscle mass Decreased vascular response to cold Impaired thermal perception Medication interactions Risk Factors Medical conditions Any condition that body reserves Cardiac Respiratory Diabetes Environmental acclimation Repeated exposure = risk Lack of acclimation = risk Windchill - heat loss from: Convection Evaporation Windchill Chart Risk Factors Dehydration Increase risk Better to drink cold water Physical condition ability to respond to stress Poor conditioning risk TRAUMA! Often seen with hypothermia stress response capability May be overlooked Caused by examination or treatment? Causes coagulation disorders TREAT ALL TRAUMA PATIENTS AS IF THEY ARE HYPOTHERMIC! 4
5 Patient Assessment Thermometers Mercury type More subject to error Accurate scale? Has it been shaken down? Remain in place for 3 minutes? Use electronic types Esophageal most accurate Oral temperatures Mouth MUST remained closed Affected by: Eating Smoking Fluid intake Axillary site as a last resort! Patient Assessment Mild hypothermia 96.8 F Increased blood pressure Increased muscle tone Start of shivering 95.0 F Maximum shivering Mild hypothermia 93.2 F Amnesia, poor judgment & maladaptive behaviors Painful joints Normal blood pressure Maximum respiratory response and then in heart rate Patient Assessment Mild hypothermia 91.4 F Apathy Ataxia & then in respiratory rate Cold diuresis Moderate hypothermia 89.6 F Stupor 25% in oxygen consumption 87.8 F Shivering stops 86.0 F Insulin looses effectiveness Arrhythmias begin to develop Patient Assessment Moderate hypothermia 85.2 F Progressive in: Level of consciousness Pulse Respirations Pupils dilated Paradoxical undressing Patient Assessment Severe hypothermia 82.4 F Decreased threshold for VF O 2 consumption by 50% Pulse by 50% Significant hypoventilation Patient Assessment Severe hypothermia 80.6 F Significant loss of reflexes and voluntary motion 78.8 F Loss of reflexes and response to pain Severe hypothermia 77.0 F Cerebral blood flow 33% normal Cardiac output 45% normal Pulmonary edema may develop 75.2 F - Significant hypotension & bradycardia 5
6 Patient Assessment Severe hypothermia 74.3 F No corneal reflexes 71.6 F Maximum risk of ventricular fibrillation Oxygen consumption by 75% Profound hypothermia 68.0 F Pulse 20% of normal 66.2 F Brain wave activity ceases 66.4 F - Asystole THEY AIN T DEAD UNTIL THEY ARE WARM AND DEAD! Pre-hospital Treatment Prevent further heat loss Remove from cold environment Remove wet and/or restrictive clothing If available, add wrapped heat sources to groin, neck, axilla Begin passive re-warming Wrap in layers Start with polymer sheets Add blankets/sleeping bags Cover head!!! Keep hands at sides Avoid radiant heat Pre-hospital Treatment Body to body rewarming is of no practical value. (Danzl, 2001, p. 504) Pre-hospital Treatment If conscious with adequate airway, give warmed, sweet beverages Keep in horizontal position Handle gently Prevent excess movement Establish IV/IO access Fluid challenge with D5%NS Any dextrose IV fluid Avoid LR d/t lactate Place IV bag under patient Wrap IV tubing in chemical warmer Pre-hospital Treatment Avoid massage of limbs Attach cardiac monitor Increase gain May have to use benzoin Small gauge needles through electrodes may be needed Life support issues Intubate (ET or Combitube) Avoid cuff overinflation Ventilate with 100% oxygen Warmed & humidified, if available Heat/moisture exchanger (HME) to prevent further heat losses 6
7 Pre-hospital Treatment Life support issues Assess pulses for > 1 minute If no pulse or signs of circulation, begin CPR Defibrillate up to three times for: Pulseless ventricular tachycardia Ventricular fibrillation Withhold further defibrillations Life support issues Continue CPR Withhold medications Transport to definitive care ASAP! Continue passive re-warming Consider arterial line Avoid pulmonary artery or CVP catheter into subclavian Draw labs X-rays for any trauma Insert an NG tube Insert foley catheter Begin IV therapy Use fluid warmer to deliver IVs Fluid challenge with D5%NS Any dextrose IV fluid Avoid LR d/t lactate Monitor for: Compartment syndrome Rhabdomyolysis Life support issues Intubate (ET or Combitube) Avoid cuff overinflation Ventilate with 100% oxygen Warmed & humidified, if available Heat/moisture exchanger (HME) to prevent further heat losses 7
8 Life support issues Assess pulses for > 1 minute If no pulse or signs of circulation, begin CPR Defibrillate ONE TIME for: Pulseless ventricular tachycardia Ventricular fibrillation Withhold further defibrillations until core temperature > 86 F Life support issues Continue CPR Medications Hold until core temps > 86.0 F Administer 2 3 X normal intervals Consider thiamine if alcohol related Active re-warming required in core temps < 89.6 F Active external re-warming TRUNCAL area only! Forced, heated air Wrapped, hot packs to groin, neck, axilla Immersion not practical Active internal re-warming Use as many modes as possible for best effect Airway re-warming Heated, humidified oxygen Prevents further heat loss Heated IV infusions One L can core temp by 1.4 F Tubing can loose a lot of heat Will likely need significant volume to correct cold diuresis Naso-gastric irrigation Monitor ins and outs to assure fluid balance Intubate to maintain airway ml boluses of electrolyte solution (NS, LR) Allow 15 minute dwell Closed thoracic lavage Two tube method Anterior/posterior tubes placed Fluid instilled anterior Drained posterior After re-warming, DC anterior tube and maintain posterior tube to drainage system 8
9 Closed thoracic lavage Single tube method Single tube placed poster, with Y connector ml boluses of electrolyte solution (NS, LR) Allowed 15 minute dwell Fluid suctioned out Peritoneal lavage Large bore catheter inserted Empty bladder and stomach Up to 2 L electrolyte solution (NS, LR) instilled Allowed 20 minute dwell & then siphoned out Aggressive internal re-warming VERY effective!!! Usually only available at higher level trauma centers Multiple types Electrolyte disturbances primarily potassium Bacterial infection Alterations in immune system Primarily pneumonia, but other sites possible Significantly affected by extremes of age Complications Coagulation disturbances primarily loss and/or malfunction of platelets Possibility of local cold injuries and/or other trauma 9
10 Non-Freezing Injuries One Two Three Four Usually caused by cold and wet conditions Risk factors, same as with hypothermia Additional risk factors may make patient more vulnerable Additional risk factors Diabetes Tight, constriction clothing Tobacco use Dehydration Previous local cold injury Vascular insufficiency/disease Chilblain - Pernio Same basic cause prolonged exposure to wet and cold Chilblain = 3 12 hour exposure Pernio More than 12 hours exposure or Repeated, frequent exposure Chilblain 3 12 hour exposure Swelling & tenderness that resolves with drying May display blisters Pain with > 6 hours exposure May have deep sensitivity to foot pressure for several days Treatment Dry Gentle massage Pernio Extension of chilblain > 12 hour or repeated, frequent exposure Deep pain that persists for multiple days Partial thickness blisters Swelling Treatment Dry Elevation to help swelling NSAID such as ibuprofen Significant pain control issues Pernio Sequela Long term sensitivity to even mild cooling of limb Pain Numbness Paresthesia 10
11 Trench Foot Also known as immersion foot Prolonged exposure to: Cold Wet Tight constricting boots Reduced blood flow caused by: Vasoconstriction, leading to Tissue hypoxia and Cellular death Injuries compounded by walking on injured feet Trench Foot Symptoms appear in three phases Pre-hyperemic phase Extremity blanched & cold Patient reports cold and numb feet Balance is impaired Trench Foot Hyperemic phase Last 6 10 weeks Upon warming, feet become: Red Hot Painful Swollen Hyperemic phase 7 10 days after injury: Pain intensifies Loss of motor control & sensation Pain & numbness with warming or dependency of foot Trench Foot Hyperemic phase 7 10 days after injury: Blisters form (bloody = bad!) Black eschars form Nails slough without pain Tissue mummifies Gangrene may require premature surgery 11
12 Trench Foot Post-hyperemic phase Swelling, pain & numbness Cold sensitivity Neurological damage will affect balance and mobility Treatment Dry & elevate feet to heart level Pain control issues significant Minor injuries can produce significant problems in later life = Cold sensitivity Frostbite Damage occurs in four phases Pre-freeze phase tissue cools Freeze-thaw phase ice crystals from in tissue Freeze-thaw phase Extra cellular ice crystals Caused by slow cooling Cellular dehydration Intra-cellular electrolyte concentration Break down of cellular walls Frostbite Freeze-thaw phase Intra-cellular ice crystals Caused by fast cooling Breakdown of cell walls Breakdown of cell proteins Cells rupture Vascular stasis phase Plasma leaks into tissue Emboli showers to small blood vessels Late ischemic phase Thrombosis formation Ischemia Tissue death Frostbite Initial classification VERY difficult Superficial frost bite First degree Numbness White, firm plaque at site Edema forms on re-warming 1 st Degree Frostbite of Ear 12
13 Frostbite Superficial frostbite Second degree As with First degree Blisters filled with clear fluid Deep frostbite Third degree As with Second degree Blisters filled with bloody fluid 4 & 5 Weeks After Frostbite Frostbite Deep frostbite Fourth degree Full thickness damage Tissue may appear mummified 24 Hours after Frostbite 6 Weeks Later 13
14 Frostbite Initial or presenting symptoms Numbness with SIGNFICANT pain on re-warming Tissue changes as described above Tissue may appear mottled blue or frozen Symptoms on re-warming Redness Sensation returns until blisters form Sensory loss persistent Blisters form within 6 24 hours Frostbite Edema forms within 3 hours and may last 5 days Pain EXTREME on re-warming Becomes throbbing May have burning sensation Electric current-like shock Eschars of black tissue form in 9 15 days Mummification and lines of demarcation form in days Frostbite Prognostic signs Favorable Sensation to pinprick Normal color and warmth Large, clear blisters Appear early Extend to tips of digits Prognostic signs Unfavorable Small, dark blisters Appear late Do NOT extend to tips of digits Absence of edema Cyanosis that does not blanch Frostbite All but the most minor frostbite cases should be admitted to the hospital. (McCauley, p. 187) Pre- Assess and treat: Hypothermia Dehydration Trauma Handle gently!! If < 2 hours from definitive care, do NOT re-warm Remove wet/restrictive clothing Keep away from dry heat sources (fires, car heaters) Pad and splint extremity Leave blisters intact Elevate to level of heart Pre- Prohibit use of: Tobacco Alcohol Provide rapid transport to definitive care If > 2 hours from definitive care: Rapid re-warming with water After re-warming, treat as above DO NOT ALLOW INJURY TO BE RE-EXPOSED TO COLD!!! 14
15 Pre- Rapid re-warming in water 104 to 108 F for 30 minutes Continue until tissue becomes pliable and red Active motion helpful Massage contraindicated!!!! Favorable signs on re-warming Rapid return of skin warmth and sensation Redness Unfavorable signs on re-warming Skin that continues to be: Pale Cold Numb Blister management AVOID betadine White blisters Represents superficial injury Debride to remove inflammatory mediators Aloe vera ointment every 6 hours Blister management Red blisters Sub-dermal injury Aspirate fluid Leave blisters intact to prevent conversion to full-thickness Aloe vera ointment every 6 hours Medications Ibuprofen, 400 mg Q12 hours Tetanus anti-toxin, if needed Penicillin Pentoxifylline blood viscosity RBC flexibility Pain control Morphine drip or PCA Fentanyl drip or PCA Avoid Demerol may cause neurological complications Long term therapy Physical therapy maintains mobility Occupational therapy maintains functional ability Long term therapy Surgical intervention usually held until: Tissue declares viability may take months Tissue infection Amputation for Gangrene 15
16 Complications VERY sensitive to cold re-injury during recovery Long term sensitivity to cold & cold injuries for life Changes in skin color Joint stiffness & pain on movement Sacred Heart Medical Center and Children s Hospital Michael W. Day, RN, MSN, CCRN Daymw@shmc.org Fax Materials to: Renee Anderson (fax) (d) andersr@inhs.org 16
Hypothermia & Local Cold Injuries
 Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital
Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
By: M.A Jafari MD EM Specialist Shahid Sadoughi Hospital
 By: M.A Jafari MD EM Specialist Shahid Sadoughi Hospital Cold weather was an important factor in second world war. Factors Influencing the Likelihood of Cold Injuries Temperature, Cold acclimatization,
By: M.A Jafari MD EM Specialist Shahid Sadoughi Hospital Cold weather was an important factor in second world war. Factors Influencing the Likelihood of Cold Injuries Temperature, Cold acclimatization,
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
Cold Injuries: An Update on Hypothermia and Frostbite
 Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Hypothermia. d. Severe Hypothermia - core temperature degrees and below (immediately life threatening)
 Hypothermia 1. Hypothermia - "a decrease in the core body temperature to a level at which normal muscular and cerebral functions are impaired." - Medicine for Mountaineering 2. Conditions Leading to Hypothermia
Hypothermia 1. Hypothermia - "a decrease in the core body temperature to a level at which normal muscular and cerebral functions are impaired." - Medicine for Mountaineering 2. Conditions Leading to Hypothermia
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Cold Injuries: Frostbite and Hypothermia. Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University
 Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
Temperature Extremes
 Temperature Extremes A SAFETY TALK FOR DISCUSSION LEADERS This safety talk is designed for discussion leaders to use in preparing safety meetings. Set a specific time and date for your safety meeting.
Temperature Extremes A SAFETY TALK FOR DISCUSSION LEADERS This safety talk is designed for discussion leaders to use in preparing safety meetings. Set a specific time and date for your safety meeting.
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
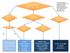 Suspected Hypothermia Temp
Suspected Hypothermia Temp
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded)
 People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
2. A drop in core temperature induced thermogenesis. A drop in core temperature initiates:
 Get Adobe Flash player Introduction to Cold: Only in rare instances do people exercise at very low body temperatures (Brooks, 2009). Due to the combination of increased metabolism duirng exercise and the
Get Adobe Flash player Introduction to Cold: Only in rare instances do people exercise at very low body temperatures (Brooks, 2009). Due to the combination of increased metabolism duirng exercise and the
CHAIN OF COMMAND: THE FOLLOWING CHAIN OF COMMAND WILL OCCUR:
 LEWISVILLE ISD COLD WEATHER POLICY Cold exposure can be uncomfortable, impair performance and even become life threatening. Conditions created by cold exposure include frostbite and hypothermia. Wind chill
LEWISVILLE ISD COLD WEATHER POLICY Cold exposure can be uncomfortable, impair performance and even become life threatening. Conditions created by cold exposure include frostbite and hypothermia. Wind chill
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
Skin and Temperature Management following Spinal Cord Injury. North West Regional Spinal Injuries Centre Southport & Ormskirk NHS Trust
 Skin and Temperature Management following Spinal Cord Injury Functions of the skin The skin is the largest organ of the integumentary system The skin is the interface with the environment and plays an
Skin and Temperature Management following Spinal Cord Injury Functions of the skin The skin is the largest organ of the integumentary system The skin is the interface with the environment and plays an
THERMOREGULATION 05 JUNE 2013
 THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
Humans are physiologically tropical - so we need to adapt our behaviour to survive in cold.
 CRACKCast E139 (Rosen s Ch 131) Frostbite Key concepts: Frostbite Premature termination of thawing in 37 C to 39 C (98.6 F 102.2 F) water is a common error. Reperfusion of completely frozen tissue may
CRACKCast E139 (Rosen s Ch 131) Frostbite Key concepts: Frostbite Premature termination of thawing in 37 C to 39 C (98.6 F 102.2 F) water is a common error. Reperfusion of completely frozen tissue may
11/8/2017. Notice. Road Map
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
LESSON 2. Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE?
 LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
ENVIRONMENTAL EMERGENCIES
 Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
Frostbite in January, Operate in June?
 Frostbite in January, Operate in June? Tam Pham, MD Assistant Professor, Surgery Associate Director, UW Burn Center Frozen Yang Tze River, NY Times 2009 Subclass of cold exposure injuries Non-freezing
Frostbite in January, Operate in June? Tam Pham, MD Assistant Professor, Surgery Associate Director, UW Burn Center Frozen Yang Tze River, NY Times 2009 Subclass of cold exposure injuries Non-freezing
HENRY COUNTY SCHOOL DISTRICT GUIDELINES FOR OUTDOOR EXTRACURRICULAR ACTIVITIES DURING EXTREME HOT AND HUMID WEATHER
 HENRY COUNTY SCHOOL DISTRICT GUIDELINES FOR OUTDOOR EXTRACURRICULAR ACTIVITIES DURING EXTREME HOT AND HUMID WEATHER 1. Each school shall have and use a digital psychrometer, or a similar device for measuring
HENRY COUNTY SCHOOL DISTRICT GUIDELINES FOR OUTDOOR EXTRACURRICULAR ACTIVITIES DURING EXTREME HOT AND HUMID WEATHER 1. Each school shall have and use a digital psychrometer, or a similar device for measuring
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
EmergencyKT: Management of Thermal Injury in Adult Patients
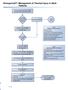 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
Thermal Injury. Thermal Injury Presentation CCFP (EM) Rounds. Topics Hypothermia. Resources Ch Tinitinelli
 Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Medical & Safety. Stay safe at Kamp Dovetail 2011
 Medical & Safety Stay safe at Kamp Dovetail 2011 Seizures Seizures are very misunderstood and may be caused by many different types of conditions, such as: Insulin shock High fevers Viral infections of
Medical & Safety Stay safe at Kamp Dovetail 2011 Seizures Seizures are very misunderstood and may be caused by many different types of conditions, such as: Insulin shock High fevers Viral infections of
Death and Postmortem Changes. Prof. Mahmoud Abd El-Nasser
 Death and Postmortem Changes BY Prof. Mahmoud Abd El-Nasser By the end oftheselecturesthestudentshouldbe: -Able to decide whether the animal is dead or not. 2-Estimation of the time passed since death.
Death and Postmortem Changes BY Prof. Mahmoud Abd El-Nasser By the end oftheselecturesthestudentshouldbe: -Able to decide whether the animal is dead or not. 2-Estimation of the time passed since death.
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Frostbite. Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department
 Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
Module Summaries: The emergency plan is a crucial part of the total sports program.
 Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Burns and Scalds. Treatment and Management. Accident and Emergency Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Drowning is a leading cause of death and loss of years of life with over 90% of cases occurring in lower- and middle-income countries.
 Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
A day at the sauna. Boardworks Ltd How does the body react to change?
 1 of 40 2 of 40 A day at the sauna 3 of 40 How does the body react to change? Saving energy? 4 of 40 Sayid has decided to save energy by staying in bed all day. How much of his energy do you think this
1 of 40 2 of 40 A day at the sauna 3 of 40 How does the body react to change? Saving energy? 4 of 40 Sayid has decided to save energy by staying in bed all day. How much of his energy do you think this
Gangrene. Introduction Gangrene is the death of tissues in your body. It happens when a part of your body loses its blood supply.
 Gangrene Introduction Gangrene is the death of tissues in your body. It happens when a part of your body loses its blood supply. Gangrene can happen on the surface of the body, such as on the skin. It
Gangrene Introduction Gangrene is the death of tissues in your body. It happens when a part of your body loses its blood supply. Gangrene can happen on the surface of the body, such as on the skin. It
FootHuggers Comfort Socks have been found to help people suffering with: Raynaud s Syndrome
 FootHuggers Comfort Socks have been found to help people suffering with: Raynaud s Syndrome How FootHuggers Comfort Socks help with Raynaud s Syndrome? 1. FootHuggers have no elastic. No tightness around
FootHuggers Comfort Socks have been found to help people suffering with: Raynaud s Syndrome How FootHuggers Comfort Socks help with Raynaud s Syndrome? 1. FootHuggers have no elastic. No tightness around
Note: This CareKit does not replace expert medical care. Be Prepared
 Note: This CareKit does not replace expert medical care. Be Prepared EMS #: 9-1-1 Poison Control #: 800.222.1222 Take a first aid course. Learn CPR and first aid for choking. Before you give first aid,
Note: This CareKit does not replace expert medical care. Be Prepared EMS #: 9-1-1 Poison Control #: 800.222.1222 Take a first aid course. Learn CPR and first aid for choking. Before you give first aid,
COLD INJURIES: DESCRIPTION, TREATMENT AND PREVENTION
 COLD INJURIES: DESCRIPTION, TREATMENT AND PREVENTION Presenter s Name Presenter s Command Local Contact Information Prepared by: U.S. Army Center for Health Promotion and Preventive Medicine (800) 222-9698/
COLD INJURIES: DESCRIPTION, TREATMENT AND PREVENTION Presenter s Name Presenter s Command Local Contact Information Prepared by: U.S. Army Center for Health Promotion and Preventive Medicine (800) 222-9698/
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES. Justin Astafan, EMT-P, CIC
 ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES Justin Astafan, EMT-P, CIC NYS EMT-P NYS CIC 17 years in the fire and ems profession Work both career and volunteer side Worked for commercial and notfor
ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES Justin Astafan, EMT-P, CIC NYS EMT-P NYS CIC 17 years in the fire and ems profession Work both career and volunteer side Worked for commercial and notfor
CHILL OUT! Induced Hypothermia: Challenges & Successes in the
 CHILL OUT! Induced Hypothermia: Challenges & Successes in the ICU Colleen Bell RN, BS, CCRN, Donna Brault RN, BSN, CCRN, Cathy Patnode RN, BSN, CCRN Champlain Valley Physician Hospital November 2012 Objectives
CHILL OUT! Induced Hypothermia: Challenges & Successes in the ICU Colleen Bell RN, BS, CCRN, Donna Brault RN, BSN, CCRN, Cathy Patnode RN, BSN, CCRN Champlain Valley Physician Hospital November 2012 Objectives
Chapter 12. Temperature Regulation
 Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Vital Signs and Oxygen Administration
 Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Gatorade Heat Safety Package
 Gatorade Heat Safety Package 1. The Four Downs of Heat Safety 2. Tips to Hydrate and Fuel for the Football Season 3. Preventing Heat-Related Illnesses The 4 Downs of Heat Safety Know the plays of heat
Gatorade Heat Safety Package 1. The Four Downs of Heat Safety 2. Tips to Hydrate and Fuel for the Football Season 3. Preventing Heat-Related Illnesses The 4 Downs of Heat Safety Know the plays of heat
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
SYSTEM-WIDE POLICY & PROCEDURE MANUAL. Policy Title: Hypothermia Post Cardiac Arrest Policy Number: PC-124. President & CEO Page 1 of 9
 Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Disaster Medical Operations Part 2. CERT Basic Training Unit 4
 Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Bi100 Chapter 1 Introduction to Human Anatomy and Physiology
 Bi100 Chapter 1 Introduction to Human Anatomy and Physiology Anatomy and Physiology A. Anatomy deals with the structure (morphology) of the body and its parts; in other words, what are things called? B.
Bi100 Chapter 1 Introduction to Human Anatomy and Physiology Anatomy and Physiology A. Anatomy deals with the structure (morphology) of the body and its parts; in other words, what are things called? B.
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Objectives. Objectives. Shock. Objectives. Cardiac output. Review of Blood Flow and Perfusion. Review the components of perfusion
 Objectives Shock Review the components of perfusion Cardiac output Perfusion at the capillary level Perfusion and cellular metabolism Aerobic metabolism and energy production Objectives Identify the stages
Objectives Shock Review the components of perfusion Cardiac output Perfusion at the capillary level Perfusion and cellular metabolism Aerobic metabolism and energy production Objectives Identify the stages
MASCOUTAH LITTE INDIANS YOUTH FOOTBALL PROGRAM HEAT PREVENTION. Plan
 MASCOUTAH LITTE INDIANS YOUTH FOOTBALL PROGRAM HEAT PREVENTION Plan MASCOUTAH LITTLE INDIANS YOUTH FOOTBALL PROGRAM Heat Prevention Plan Purpose: To educate and maintain a high level of safety awareness
MASCOUTAH LITTE INDIANS YOUTH FOOTBALL PROGRAM HEAT PREVENTION Plan MASCOUTAH LITTLE INDIANS YOUTH FOOTBALL PROGRAM Heat Prevention Plan Purpose: To educate and maintain a high level of safety awareness
ENVIRONMENTAL EMERGENCIES
 SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest. Objectives: U.S. stats
 Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
The ALS Algorithm and Post Resuscitation Care
 The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
CrackCast Episode 8 Brain Resuscitation
 CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
Heat Stress Course Outline
 Heat Stress Course Outline The following outline summarizes the major points of information presented in the program. The outline can be used to review the program before conducting a classroom session,
Heat Stress Course Outline The following outline summarizes the major points of information presented in the program. The outline can be used to review the program before conducting a classroom session,
Unit 9 MODALITIES AND REHABILITATION Lecture Guide
 Unit 9 MODALITIES AND REHABILITATION Lecture Guide Therapeutic Modalities What are they? Therapeutic= Modality= Many different modalities to choose from- selection is dependant on: Smaller, slower nerve
Unit 9 MODALITIES AND REHABILITATION Lecture Guide Therapeutic Modalities What are they? Therapeutic= Modality= Many different modalities to choose from- selection is dependant on: Smaller, slower nerve
Preparing for your upcoming PALS course
 IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
THERMOREGULATION PHARMACOLOGY 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1
 THERMOREGULATION DIVISION OF PHYSIOLOGY DEPARTMENT OF ANATOMY, PHYSIOLOGY AND PHARMACOLOGY FACULTY OF VETERINARY MEDICINE IPB 2017 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1 Regulation
THERMOREGULATION DIVISION OF PHYSIOLOGY DEPARTMENT OF ANATOMY, PHYSIOLOGY AND PHARMACOLOGY FACULTY OF VETERINARY MEDICINE IPB 2017 6/21/2017 MATERI AJAR FISIOLOGI VETERINER II (TERMOREGULASI) 1 Regulation
New Therapeutic Hypothermia Techniques
 New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
(31189) Hypothermia Initiation Phase One
 Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Bleeding and Shock. Circulatory System
 Bleeding and Shock Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to body tissues Delivers
Bleeding and Shock Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to body tissues Delivers
Chapter 28. Wound Care. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
Extreme Heat: A Prevention Guide to Promote Health and Safety
 Extreme Heat: A Prevention Guide to Promote Health and Safety People suffer heat-related illness when their bodies are unable to compensate and properly cool themselves. The body normally cools itself
Extreme Heat: A Prevention Guide to Promote Health and Safety People suffer heat-related illness when their bodies are unable to compensate and properly cool themselves. The body normally cools itself
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
