Glossary of ESRD Terms
|
|
|
- Pauline Arabella Allison
- 5 years ago
- Views:
Transcription
1 Glossary of ESRD Terms ACCESS: A means to reach the bloodstream, In hemodialysis, fistulas, grafts, catheters, and vascular accesses are used. Access to the peritoneal cavity for peritoneal dialysis is through a peritoneal catheter. ACCESS ANEURYSM: A thinned, bulging, pulsating area on a fistula or graft. Aneurysms can be caused by repeated puncture of an access in one spot. The trauma and stenosis can increase pressure that weakens the access wall and can cause rupture. ACCESS FLOW: The blood flow through a vascular access. Transonic flow/dilution sensors record the ultrasound velocity of the arterial and venous blood lines. This provides a measure of changes in arterial and venous saline concentration when a bolus of saline is introduced in the venous blood line. Under Transonic s proprietary Krivitski Method, this bolus travels through the reversed blood lines and into the patient s vascular access where it mixes with access flow. The Krivitski indicator dilution algorithm automatically calculate vascular access flow. ACUTE RENAL FAILURE: A condition in which the kidneys suddenly stop functioning. In many cases, kidneys can recover. ACUTE TUBULAR NECROSIS (ATN): Reversible kidney damage resulting in delayed kidney function after a kidney transplant. ADEQUACY, DIALYSIS: The amount of dialysis to prevent uremic symptoms. In hemodialysis this is measured by Kt/V or URR. In peritoneal dialysis, this is measured by KT/V and creatinine clearance. AF/CO: ACCESS FLOW TO CARDIAC OUTPUT RATIO: The AF/CO value is the percentage ratio of the patient s access flow to the patient s cardiac output. For example an AF/CO value of 22% would mean that 22% of the patient s cardiac output is being shunted through the patient s access. However, when access flow exceeds 25% of cardiac output, a potential cardiac problem may exist. ALBUMIN: One of a class of proteins in the blood. A reduced level of albumin may be a sign of inadequate protein intake in the diet. HDGlossaryofTerms(DL-9-tn)RevC2017USltr ALLOGRAFT: An organ or tissue transplant from one human to another. ANEMIA: A common condition in patients with kidney disease when they have not enough red blood cells (RBC) in the blood to carry oxygen. Often referred to as low blood, anemia causes weakness and fatigue. ANGIOPLASTY: The inflation of a balloon inside a narrowing blood vessel. The inflation of the balloon makes the vessel opening bigger and allows for more blood flow. ANURIA: A condition in which a person stops producing urine. ARTERIAL LINE: The tube carrying blood from the body into the artificial kidney. ARTERIOGRAM, RENAL: An X-ray involving the injection of dye into the main artery supplying the kidney. It is used to determine if the blood vessels to the kidney are normal. ARTERIOVENOUS FISTULA (AV FIS- TULA): Surgical connection of an artery directly to a vein in patients who need hemodialysis. As the AV fistula matures, it grows thicker, allowing repeated needle insertions required for hemodialysis. ARTERY: A blood vessel that carries blood away from the heart and to the body. ARTIFICIAL KIDNEY: Another name for dialyzer. ASCITES: Fluid retained in the abdominal cavity. BANDING: A procedure to reduce flow in a high flow fistula by reducing the diameter of the fistula. BATH: Another name for dialysate fluid, which is a self-cleaning salt solution. Inside the dialyzer, waste products will flow from the blood into the dialysate and are then washed away. BILATERAL NEPHRECTOMY: Removal of both kidneys. BLOOD FLOW RATE (BFR OR QB): The amount of blood passing through the artificial kidney (dialyzer) each minute. This is determined by the speed at which the pump is set. Page 1 BLOOD LEAK: The dialyzer fibers or membrane develop a small break or tear allowing blood to leak into the dialysate. BLOOD PUMP: A pump that is used to bring blood from the patient and push it through the artificial kidney or dialyzer and back to the body. BLOOD UREA NITROGEN BUN: A waste product, or toxin, that appears in the blood as protein from digested food. BUN levels are a measure of how well the kidneys are functioning as well as adequacy of dialysis and nutritional status. A high BUN indicates that the kidneys are not removing enough waste. BLOODLINES: The arterial line and venous line used in hemodialysis. BRUIT: The sound of blood moving through a fistula or graft that indicates the access is working. Bruits can also be heard from an artery and may indicate a blockage. CALIBRATION: (not to be misused as a synonym for validation) In Situ: adjustment or correction made to a measurement device for errors produced under actual conditions of use by comparing the measurement with a known standard. In Vivo: adjustment or correction made to a measurement device during use in a living body. CANNULATION: The process of inserting a needle into the graft or fistula. CARDIAC INDEX: Cardiac Index is cardiac output divided by estimated Body Surface Area (BSA). The Transonic Flow-QC Cardiac Output Program automatically calculates CI using the patient s body height and weight. A primary criterion of cardiac adequacy, CI is useful in comparing different sized patients. Normal CI values for the general population range from 2.5 to 4.2 L/min/m 2. Cardiac Indexes from 6-8 L/min/m 2 may indicate high access flow. A low CI (< 2 L/min/m 2 ) at the beginning of a hemodialysis session indicates significant deterioration of cardiac function. A decrease in CI during the hemodialysis session indi-
2 cates potential cardiac problems, inadequate dry weight estimation, and/or inadequate medication prescription. CARDIAC OUTPUT: The amount of blood which the heart pumps in one heart beat. The Transonic Flow-QC Hemodialysis Monitor measures cardiac output through a bolus of saline quickly injected into the venous blood line where its concentration is measured by a Transonic flow/dilution sensor. This bolus is carried by the venous blood stream in the heart, where it is diluted (mixed) into the full cardiac flow. A portion of this diluted saline returns to the shunt, where it is removed by the arterial blood line, and its saline concentration is measured by the second Transonic flow/dilution sensor. Classic dilution equations are used to calculate Cardiac Output from the changes in indicator concentration between the venous and arterial line. CARDIOPULMONARY RECIRCULATION (CPR): Is the condition when blood that flows back into the heart and lungs. CPR can be measured with the Transonic Monitor and can be separated from vascular access recirculation. This enables a true measurement of zero percent recirculation( through the access) a reality. CATHETER: A tube inserted through the skin into a blood vessel or body cavity to draw out blood or body fluids, or to put in fluid. In hemodialysis, a catheter is a vein can be used to create a temporary or longterm dialysis access. In peritoneal dialysis, a catheter is used to put dialysis solution into the abdominal cavity and to drain it out again. CENTERS FOR MEDICARE & MEDICAID SERVICES (CMS), an agency of the U.S. Department of Health and Human Services (DHHS). CENTRAL BLOOD VOLUME (CBV) AND CENTRAL BLOOD VOLUME INDEX (CBVI) Central Blood Volume (CBV) is defined as the volume of blood in the heart, lungs, and the great vessels. Normal values range from L. CBVI is found by dividing CBV by the patient s weight (typical range, ml/kg). Maintenance of CBV is thought to be a factor in blood pressure regulation. CBV decreases during hemodialysis are similar to CO, and probably precede CO. 10 When CBV is depleted, hypotensive episodes may occur. Therefore, monitoring CBV repeatedly during ultrafiltration may indicate how fast a patient can be dialyzed without hypovolemic collapse. Baseline values for each parameter, their change during the hemodialysis treatment, as well as their changes over time provide valuable clinical information to the nephrologist and hemodialysis staff. CENTRAL VENOUS STENOSIS: Narrowing of the central veins in the body that can make the arm on that side unsuitable for a vascular access. CHRONIC RENAL FAILURE (CRF): Slow and progressive loss of kidney function over several years, often resulting in End Stage Renal Disease. CIRCLE OF CARE: A phrase coined by Transonic to describe the entire treatment process that a patient undergoing hemodialysis could experience. Includes intraoperative placement of a fistula or graft by a surgeon during which an intraoperative measurement with transit-time ultrasound technology is used, hemodialysis surveillance with the Transonic Hemodialysis Monitor using ultrasound dilution technology and finally, access intervention via angioplasty using the HVT100 Endovascular Flowmeter and ReoCath Flow Catheter using thermal dilution technology or surgical revision with intraoperative transit-time ultrasound measurments. CLOTTING TIME: The time it takes for blood to clot. CONDUCTIVITY: The measure of ions in a solution. A conductivity meter measures the chemical composition of dialysate by measuring the dialysate s ability to conduct an electrical current. If the conductivity of dialysate is not correct, an alarm will go off, and the dialysate is bypassed to the drain. This means that the dialysate will not come in contact with the patient s blood. CONGESTIVE HEART FAILURE: A condition in which a weakened heart does not pump blood effectively, resulting in retention of excess fluid in the lungs which make breathing difficult. CREATININE: A waste product released from the muscles of the body. Creatinine is normally removed form the blood by the kidneys. Page 2 CREATININE CLEARANCE: A test that measures how well the kidneys remove creatinine from the blood. A decreased creatinine clearance reading means decreased function of the kidneys. CROSS-MATCHING: A test used to establish blood compatibility before transfusion and transplant. DASS: Dialysis Access Induced Steal Syndrome DECLOTTING: Removal of a blood clot so fluid can flow through a blood vessel or tube, such as a dialysis access. DELIVERED BLOOD FLOW: During hemodialysis matched flow/dilution sensors, clipped onto the arterial and venous dialysis lines, continuously measure the actually blood flow delivered to the patient. Comparison of this reading displayed on the Hemodialysis Monitor with the pump flow setting (i.e., the flow the pump tries to deliver) provides an opportunity to identify and correct dialysis delivery problems. DIABETIC NEPHROPATHY: Kidney disease caused by diabetes mellitus (high blood sugar). DIABETIC NEUROPATHY: Nerve damage caused by diabetes mellitus. DIABETIC RETINOPATHY: Eye disease caused by diabetes mellitus that may result in reduced vision or blindness. DIALYSATE/DIALYSATE FLUID: The solution used to remove excess fluids and waste products from the blood. DIALYSATE FLOW RATE (DFR) OR QD: The rate at which dialysate fluid moves through the dialyzer. DIALYSIS: The artificial process of cleaning wastes from the blood with special equipment when kidneys fail. DIALYZER: An artificial kidney used with a hemodialysis machine. The dialyzer has two compartments separated by a membrane. One section holds dialysate fluid and the other holds the patient s blood. Waste products and fluid travel from the blood into the dialysate fluid, across the dialyzer membrane, and then are disposed. DISEQUILIBRIUM SYNDROME: A term used to describe a condition which may result from dialysis therapy, most commonly in patients new to dialysis.
3 Some symptoms may be headache, cramps, nausea, or vomiting. DRILL: Distal Revascularization-interval Ligation, a procedure to reduce high flow fistulas by reducing inflow into the fistula. DRY PACK: A dialyzer that has not been pre-processed for first use of hemodialysis. DRY WEIGHT (IDEAL OR TARGET WEIGHT): The weight at which all excess fluids have been removed. DWELL TIME: In peritoneal dialysis, the amount of time that dialysate fluid remains in the patient s abdominal cavity during an exchange. EDEMA: Swelling caused by too much fluid in the body. ELECTROLYTES: Salts in the body fluids including sodium, potassium, magnesium and chloride. The kidneys control the amount of these electrolytes in the body. When the kidneys fail, electrolytes get out of balance, possibly causing serious health problems. Dialysis can help correct this problem. END STAGE RENAL DISEASE (ESRD): Any irreversible kidney disease that requires dialysis therapy or kidney transplant in order to live. The term end-stage means that the renal disease is permanent and irreversible, and not that the person s condition is terminal. ESRD SEAMLESS CARE ORGANIZA- TIONS (ESCO): a partnership among groups of health care providers and suppliers including Medicare certified dialysis facilities, nephrologists and other Medicare enrolled providers and suppliers located in a contiguous geographical area. Through the ESCO model, these partners are able to work together to enhance patientcentered care, improve communication and coordination of care and access to services. In addition, these partners test a new payment model and care delivery method specifically for Medicare beneficiaries with ESRD. ERYTHROPOIETIN: A hormone which stimulates the body to produce red blood cells. With renal failure, the kidney can t produce this hormone, resulting in anemia. EXCHANGE: In peritoneal dialysis, the draining is used dialysate fluid solution from the abdomen, followed by refilling with a fresh bag of solution. EXIT SITE: The site at which the catheter exits the body. FEMORAL CATHETER: A temporary catheter placed in the femoral vein in the groin. FERRITIN: The amount of iron stored in the body. FIRST-USE SYNDROME: Symptoms that may occur after starting hemodialysis with a dry pack or dialyzer that has not been pre-processed for first use of hemodialysis. Symptoms may include chest pain, back pain, nervousness, and itching. FISTULA: (AV Fistula): Surgical connection of an artery directly to a vein in patients who need hemodialysis. As the AV fistula matures, it grows thicker, allowing repeated needle insertions required for hemodialysis. FISTULA FIRST/CATHETERLAST: A national vascular access improvement initiative to increase the number of fistulas in the US and decrease the number of catheters. FISTULOGRAM: An X-ray, using dye, to evaluate the blood flow through a fistula. Performed in the Radiology Department of a hospital, the procedure can detect problems such as a clot or narrowing in the fistula. Early detection and treatment of problems with a fistula can improve its performance and limit future complications. FLOWMETRY: Measurement of flow parameters. FLOW/DILUTION SENSOR: A device which measures volume of a liquid passing through tubing by flow/dilution technology. Fluid Overload: Excess sodium (salt) and fluid retained in the body between dialysis treatments;,may cause shortness of breath and swelling. FLUID RESTRICTION: The amount of fluid a patient is allowed to drink in a 24-hour period to avoid adding extra weight that would cause fluid overload and undue stress to the heart. FOLIC ACID: A vitamin necessary for red blood cell protection. Page 3 GLOMERULONEPHRITIS: Also called Bright s Disease or Nephritis. It is an inflammation of the glomeruli. It usually affects both kidneys and generally first occurs in early childhood. Recovery from the acute form may take one year. Those with the chronic form suffer low, progressive damage which may ultimately lead to ESRD. GLOMERULUS (GLOMERULI PL.): A tiny site of looping blood vessels in the kidney where the blood is filtered. GRAFT: In hemodialysis, a vascular access surgically created using a synthetic tube to connect an artery to a vein. In transplantation, a graft is the transplanted organ or tissue. HAIDI: Hemodialysis Access-Induced Distal Ischemia HEMATOCRIT: A measure that tells how many red blood cells are present in a blood sample. Low hematocrit suggests anemia or increased blood loss. HEMODIALYSIS: The use of a machine to clean wastes from the blood after the kidneys have failed. The blood is circulated through tubes to a dialyzer, which removes wastes and extra fluid. The cleaned blood then flows through another set of tubes back into the body. HEMOGLOBIN: The substance in red blood cells that carries oxygen around the body. Low hemoglobin suggests anemia or increased blood loss. HYPERGLYCEMIA: Too high a level of glucose (sugar) in the blood; a sign that diabetes is out of control. HYPERKALEMIA: A high level of potassium in the blood; can cause irregular heartbeat and, if severe, cardiac arrest. HYPOGLYCEMIA: Low blood sugar. INFILTRATION: The leakage of a substance into body tissues. In hemodialysis patients, infiltration of blood into the tissues surrounding the access can occur if the needle punctures the back of the vessel wall or is partially dislodged from the access. INTERNAL JUGULAR CATHETER (IJ): A temporary dialysis catheter that is placed in the internal jugular vein of the neck.
4 Glossary of ESRD Terms Cont. INTRAVENOUS: Within a vein. IRON DEFICIENCY: lack of enough available iron to produce red blood cells. KDOQI OR NKFDOQI GUIDELINES: Kidney Disease Outcomes Quality Initiative (NKF KDOQI) guidelines for dialysis care including Hemodialysis Adequacy, Vascular Access and Cardiovascular Disease in Dialysis Patients. ( KIDNEY FAILURE: Loss of kidney function. KIDNEY TRANSPLANTATION: The replacement of a diseased kidney with a healthy one. KIDNEYS: Two bean-shaped organs located on either side of the spine, just above the waist. The rid the body of waste materials and maintain fluid balance through the making or urine. KRIVITSKI METHOD : A way to measure vascular access flow directly, pioneered by Nikolai Krivitski PhD, DSc by reversing the dilaysis bloodlines at their needle connections and injection a volume of innocuous saline into the venous port. Kt/V: A measurement of how much urea is being removed form the body during dialysis. The measurement takes into account the efficiency of the dialyzer, the treatment time, and the total amount of urea in the body. LIPID: A term for fat. The body stores fat as energy for future use. When the body needs energy, it can break down the lipids into fatty acids and burn them like glucose (sugar). MEMBRANE: A thin sheet or layer of tissue that lines a cavity or separates two parts of the body. A membrane can act as a filter, allowing some particles to pass from one part of the body to another while keeping others where the are. The artificial membrane in a dialyzer filters waste products from the blood. MILLER BANDING: Minimally Invasive Limited Ligation Endoluminal-Assisted Revision: Method of endovascular banding of a high flow access using an endoluminal balloon as a sizing dowel to shrink a fistula s inner diameter to an exact size. MODALITY: Methods of treatment for kidney failure. Modalities for ESRD include transplant, hemodialysis and peritoneal dialysis. NEEDLE GAUGE: Refers to the size of the needle. The larger the number, the smaller the size of the needle. NEGATIVE PRESSURE: The method of removing extra water and salt from the blood by creating pressure inside the blood compartment of the dialyzer, allowing the process of ultrafiltration to take place. NEPHROLOGIST: A medical doctor who treats patients with kidney problems or hypertension. The head of a dialysis care team. NEPHRON: A tiny part of the kidneys. each kidney is made up of about one million nephrons, which are the working units, removing waste and extra fluids from the blood. NATIONAL KIDNEY FOUNDATION (NKF): An advocacy organization for persons with kidney disease OCCLUDE: Obstructed or blocked flow in a blood vessel, graft or catheter. OSMOSIS: Passing fluid through a semipermeable membrane from a solution with low solute concentration to a solution with a higher solute concentration until there is an equal concentration of fluid on both sides of the membrane. QUALITY INCENTIVE PROGRAM (QIP): An incentive program administered by CMS to promote high-quality services in outpatient dialysis facilities treating patients with End-Stage Renal Disease (ESRD). Known as pay-for-performance or value-based purchasing (VBP) programs, the program changes the way CMS pays for the treatment of patients with ESRD by linking a portion of payment directly to facilities performance on quality of care measures. PAI: Proximalization of Arterial Inflow, a procedure that converts the arterial supply of an AV access to a more proximal artery with higher capacity. PALPATE: To examine by touching. PATENT: Unblocked flow of blood in a blood vessel, graft, or catheter. PERCUTANEOUS TRANSLUMINAL ANGIOPLASTY OR ANGIOPLASTY: The inflation of a balloon inside a narrowing blood vessel. The inflation Page 4 of the balloon makes the vessel opening bigger and allows for more blood flow. PERFUSION MACHINE: A machine that keeps a donor kidney in the best possible condition outside the body until such time as it can be transplanted into a recipient. PERIPHERAL RESISTANCE (PR): Total Peripheral Resistance is the average resistance to systemic blood flow and is approximated as Mean Arterial Pressure divided by Cardiac Output. If pressures are measured in mmhg, PR will be in units of mmhg/l/min. Normal values range from mmhg/l/min. Peripheral Resistance is the Holy Grail of people studying hypertension We all measure pressure but what we really want to know is peripheral resistance. We cannot measure this in the outpatient but now we can measure it in hemodialysis patients. Patients diagnosed with diabetes may have substantially higher PR. Because CO generally decreases during hemodialysis and pressure is maintained, PR will increase during hemodialysis for most patients. Dr. Depner suggests that patients whose PR does not increase during treatment may have fluid overload. The Depner study correlated an increased 1-year mortality risk with a failure of PR to increase in response to the stress of hemodialysis, combined with higher initial PR and lower initial CO. PRIMING: Filling and rinsing the bloodlines and the dialyzer with a solution of saline. PROCESS OF CARE: a phrase used to describe work flow through a dialysis clinic. RECIRCULATION: Is the condition when blood that flows back into the arterial line through the vascular access without circulating through the patient s circulatory system. Recirculation is also measured with the Transonic Monitor. Saline is introduced into the venous blood line. If any of this saline reaches the arterial blood line immediately after its release into the venous blood line, it must have traversed the vascular access in reversed direction ( recirculation ).
5 The % amount of recirculation is accurately calculated from the ratio of arterial to venous saline concentration registered between the two Transonic flow/dilution sensors. RENAL: Pertaining to the kidneys. RUDI: Revision Using Distal Inflow, a procedure to reduce high flow fistulas by reducing moving inflow into the fistula into a more distal site. SALINE: A salt solution containing sodium and chloride. SHUNT: Another word for fistula or graft. SOLUTE: A substance dissolved in another substance. STEAL SYNDROME: Occurs when a fistula or graft steals too much blood away from the distal (farthest from center of body) part of the arm usually the hand. STENOSIS: The narrowing of a blood vessel which can lead to a clot. SUBCLAVIAN/SUBCLAVIAN VEIN: Means beneath the clavicle (collarbone). The subclavian vein is a large vein behind the collarbone which is sometimes used for hemodialysis. SUBCLAVIAN CATHETER: A catheter placed in the subclavian vein. SUTURE: The material used to surgically close a wound or join tissues. TENCKHOFF CATHETER: A type of catheter used in peritoneal dialysis. THE DIALYSIS FACILITY COMPARE (DFC) STAR PROGRAM: The Dialysis Facility Compare (DFC) Star Program is a rating system developed by Medicare that assigns 1 to 5 stars to dialysis facilities by comparing the health of the patients in their clinics to the patients in other dialysis facilities across the country. It is intended to help a patient find and compare dialysis facilities in his or her local area THRILL: The buzzing sensation that can be felt by touching a fistula or graft. This indicates that the access is working. THROMBUS: A clot formed in a blood vessel. TISSUE TYPING: A laboratory test done on your blood to find the degree of matching between a potential donated kidney and the patient waiting for transplant. TOXINS: Waste products, harmful to the body, that accumulate in the blood of ESRD patients. TRANSPLANT: Replacement of a diseased organ with a healthy one. TRENDELENBURG POSITION: A body position in which the head is placed at 45 degrees with the legs up (feet above the head). This position helps when a person has hypotension. TUNNELED CUFFED CATHETER: A dialysis catheter that is inserted into a blood vessel through a tunnel created under the patient s skin. Inside the tunnel tract, surround tissue grows into an attached cuff to help stabilize the catheter and provide a physical barrier to bacteria. ULTRAFILTRATION: The process of removing excess water from the blood during dialysis. ULTRASOUND: A technology that bounces safe, painless sound waves off organs to create an image of their structure. ULTRASOUND INDICATOR DILUTION: a technology pioneered by Transonic which unites dilution and ultrasonic transit time to measure the changes that occur in the velocity of a liquid when diluted with isotonic saline; measures recirculation, access flow and cardiac output during hemodialysis. UREMIA OR UREMIC SYNDROME: Changes in the body caused by the build-up of waste products in the blood when the kidneys fail to function. URETER: The tube that carries urine from the kidney to the bladder. Urea: A waste product found in the blood and caused by the normal breakdown of protein in the body. urea is normally removed form the blood by the kidneys and then excreted as urine. UREA REDUCTION RATIO (URR): A blood test that compares the amount of blood urea nitrogen (BUN) before and after dialysis to measure the effectiveness of the dialysis prescription. VASCULAR ACCESS FLOW: Transonic flow/ dilution sensors also record the ultrasound velocity of the arterial and venous blood lines. This provides a measure of changes in arterial and venous saline concentration when a bolus of saline is introduced in the venous blood line. Under Transonic s proprietary Krivitski Method, this bolus travels through the reversed blood lines and into the patient s vascular access where it mixes with access flow. The Krivitski indicator dilution algorithm automatically calculate vascular access flow. VAMP : A vascular access monitoring program created by L. Spergel, MD, to improve patient outcomes by lengthening the life of the vascular access through routine monitoring and surveillance. VASCULITIS: Inflammation of the wall of blood vessels. VEIN: A blood vessel that carries blood toward the heart. VENOUS LINE: The tube that carries blood beck into the body from the artificial kidney machine. Page 5
ONLINE HEMODIALYSIS TRAINING SESSION 1
 ONLINE HEMODIALYSIS TRAINING SESSION 1 This document is a supplement to the Online Training. Do not reproduce. Copyright Dialysis4Career. All Rights Reserved. The Renal System - A highly sophisticated
ONLINE HEMODIALYSIS TRAINING SESSION 1 This document is a supplement to the Online Training. Do not reproduce. Copyright Dialysis4Career. All Rights Reserved. The Renal System - A highly sophisticated
Definitions. You & Your New Transplant ` 38
 Definitions Acute Short, relatively severe Analgesic Pain medicine Anemia A low number of red blood cells Anesthetic Medication that dulls sensation in order to reduce pain Acute Tubular Necrosis (ATN)
Definitions Acute Short, relatively severe Analgesic Pain medicine Anemia A low number of red blood cells Anesthetic Medication that dulls sensation in order to reduce pain Acute Tubular Necrosis (ATN)
HEALTHYSTART TRAINING MANUAL. Living well with Kidney Disease
 HEALTHYSTART TRAINING MANUAL Living well with Kidney Disease KIDNEY DISEASE CAN AFFECT ANYONE! 1 HEALTHYSTART PROGRAMME HEALTHYSTART is a lifestyle management programme to assist you to remain healthy
HEALTHYSTART TRAINING MANUAL Living well with Kidney Disease KIDNEY DISEASE CAN AFFECT ANYONE! 1 HEALTHYSTART PROGRAMME HEALTHYSTART is a lifestyle management programme to assist you to remain healthy
Fundamentals of DIALYSIS
 Fundamentals of DIALYSIS Knowing Your Kidneys Healthy Kidneys are the body s cleaning crew These are twin bean shaped organs, of the size of fist They make up a filter system for the blood & reabsorb almost
Fundamentals of DIALYSIS Knowing Your Kidneys Healthy Kidneys are the body s cleaning crew These are twin bean shaped organs, of the size of fist They make up a filter system for the blood & reabsorb almost
Treatment Options Not Not access
 Treatment Options Treatment options for Chronic Kidney Disease (CKD) CKD is a permanent condition. Treatment will: Help the patient feel better Not cure the disease Not make the kidneys start working again
Treatment Options Treatment options for Chronic Kidney Disease (CKD) CKD is a permanent condition. Treatment will: Help the patient feel better Not cure the disease Not make the kidneys start working again
What Your Kidneys Do
 UW MEDICINE PATIENT EDUCATION What Your Kidneys Do And what happens with kidney disease Class Goals 1. Understand what kidneys do. 2. Understand symptoms of uremia. 3. Know the common causes of kidney
UW MEDICINE PATIENT EDUCATION What Your Kidneys Do And what happens with kidney disease Class Goals 1. Understand what kidneys do. 2. Understand symptoms of uremia. 3. Know the common causes of kidney
Nursing Care of the Dialysis Patient. Adrian Hordon, MSN, RN
 Nursing Care of the Dialysis Patient Adrian Hordon, MSN, RN Understand principles of hemodialysis Recognize different access ports Identify side effects and complications Discuss nursing care for pre and
Nursing Care of the Dialysis Patient Adrian Hordon, MSN, RN Understand principles of hemodialysis Recognize different access ports Identify side effects and complications Discuss nursing care for pre and
What Your Kidneys Do and What Happens When They Fail
 Patient Education Chapter 2 Page 1 What Your Kidneys Do and What Happens When They Fail Objectives: 1. Understand basic kidney functions. 2. Understand symptoms of uremia and some treatments used for it.
Patient Education Chapter 2 Page 1 What Your Kidneys Do and What Happens When They Fail Objectives: 1. Understand basic kidney functions. 2. Understand symptoms of uremia and some treatments used for it.
CARE OF YOUR FISTULA
 CARE OF YOUR FISTULA 1 . What is a fistula? An arteriovenous fistula, or AVF, is a vessel that is formed by joining a vein to an artery in your arm during an operation to form an accessible blood vessel
CARE OF YOUR FISTULA 1 . What is a fistula? An arteriovenous fistula, or AVF, is a vessel that is formed by joining a vein to an artery in your arm during an operation to form an accessible blood vessel
Patient Education Kidney Early Education Program (KEEP) Chapter 2 bjectives: Overview 1. Understand what kidneys do. 2. Understand symptoms
 Patient Education (KEEP) Chapter 2 What Your Kidneys Do And what happens when they fail Objectives: 1. Understand what kidneys do. 2. Understand symptoms of uremia and some ways to treat it. 3. Know the
Patient Education (KEEP) Chapter 2 What Your Kidneys Do And what happens when they fail Objectives: 1. Understand what kidneys do. 2. Understand symptoms of uremia and some ways to treat it. 3. Know the
AV Fistula for Dialysis
 AV Fistula for Dialysis Introduction Before starting regular hemodialysis sessions, you must first prepare a vascular access. A vascular access is the site on your body where blood is removed and returned
AV Fistula for Dialysis Introduction Before starting regular hemodialysis sessions, you must first prepare a vascular access. A vascular access is the site on your body where blood is removed and returned
Chapter 12. Excretion and the Interaction of Systems
 Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Kidney Decisions Aid
 Kidney Decisions Aid A G U I D E F O R P E O P L E W H O H A V E, O R K N O W S O M E O N E, W I T H C H R O N I C K I D N E Y D I S E A S E, A N D T O A I D I N T H E D E C I S I O N A B O U T W H I C
Kidney Decisions Aid A G U I D E F O R P E O P L E W H O H A V E, O R K N O W S O M E O N E, W I T H C H R O N I C K I D N E Y D I S E A S E, A N D T O A I D I N T H E D E C I S I O N A B O U T W H I C
Make an appointment with your doctor if you have any signs or symptoms of acute kidney failure.
 Acute Kidney Failure Acute kidney failure occurs when your kidneys suddenly become unable to filter waste products from your blood. When your kidneys lose their filtering ability, dangerous levels of wastes
Acute Kidney Failure Acute kidney failure occurs when your kidneys suddenly become unable to filter waste products from your blood. When your kidneys lose their filtering ability, dangerous levels of wastes
BLEEDING EMERGENCY. Always apply pressure directly over the bleeding site with your thumb or use an inverted bottle top to localise the pressure
 Bleeding between dialysis sessions is very rare and there are almost always warning signs before this happens. Warning signs include:- Infection of the fistula Bulging area, usually with shiny skin and
Bleeding between dialysis sessions is very rare and there are almost always warning signs before this happens. Warning signs include:- Infection of the fistula Bulging area, usually with shiny skin and
KIDNEY FAILURE TREATMENT OPTIONS Choosing What s Best For You
 KIDNEY FAILURE TREATMENT OPTIONS Choosing What s Best For You What Kidneys Do The kidneys are a pair of bean shaped organs located below your ribcage near the middle of your back. Kidneys play a vital
KIDNEY FAILURE TREATMENT OPTIONS Choosing What s Best For You What Kidneys Do The kidneys are a pair of bean shaped organs located below your ribcage near the middle of your back. Kidneys play a vital
KIDNEY FAILURE. What causes kidney failure People who are most at risk for kidney failure usually have one or more of the following causes:
 KIDNEY FAILURE Your kidneys are a pair of organs located toward your lower back. One kidney is on each side of your spine. They filter your blood and remove toxins from your body. Your kidneys send toxins
KIDNEY FAILURE Your kidneys are a pair of organs located toward your lower back. One kidney is on each side of your spine. They filter your blood and remove toxins from your body. Your kidneys send toxins
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Module 10 Troubleshooting Guide
 Module 10 Troubleshooting Guide Your safety and wellbeing are our priority. Issues can occur during your treatment and it is important that you recognize the symptoms. This guide will teach you how to
Module 10 Troubleshooting Guide Your safety and wellbeing are our priority. Issues can occur during your treatment and it is important that you recognize the symptoms. This guide will teach you how to
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents
 Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Understanding Your Fluid Status During Dialysis and the Crit-Line. IV Monitor
 Understanding Your Fluid Status During Dialysis and the Crit-Line IV Monitor IV 1 Understanding Your Fluid Status During Hemodialysis Welcome to understanding your fluid status during hemodialysis. This
Understanding Your Fluid Status During Dialysis and the Crit-Line IV Monitor IV 1 Understanding Your Fluid Status During Hemodialysis Welcome to understanding your fluid status during hemodialysis. This
Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HOME HEMODIALYSIS OPTIONS
 Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HOME HEMODIALYSIS OPTIONS UNDERSTANDING YOUR HOME HEMODIALYSIS OPTIONS HOW DO THE KIDNEYS FUNCTION? Most people are born with two kidneys.
Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HOME HEMODIALYSIS OPTIONS UNDERSTANDING YOUR HOME HEMODIALYSIS OPTIONS HOW DO THE KIDNEYS FUNCTION? Most people are born with two kidneys.
Renal Patient s Information Leaflet
 Renal (Haemodialysis) Unit Patient Information Renal Patient s Information Leaflet Opening hours: If you need this information in large print, easy read, on audiotape or in another language please call
Renal (Haemodialysis) Unit Patient Information Renal Patient s Information Leaflet Opening hours: If you need this information in large print, easy read, on audiotape or in another language please call
Patient Education Programme. Kidney Options Guiding you when kidneys fail
 Patient Education Programme Kidney Options Guiding you when kidneys fail About the kidneys What do healthy kidneys do? Your two kidneys work more than you realise. The kidneys remove excess body water
Patient Education Programme Kidney Options Guiding you when kidneys fail About the kidneys What do healthy kidneys do? Your two kidneys work more than you realise. The kidneys remove excess body water
UW MEDICINE PATIENT EDUCATION. Peritoneal Dialysis. A treatment option for kidney disease. There are 2 types of PD: continuous ambulatory
 UW MEDICINE PATIENT EDUCATION Peritoneal Dialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and basic principles of continuous ambulatory peritoneal dialysis (CAPD). 2.
UW MEDICINE PATIENT EDUCATION Peritoneal Dialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and basic principles of continuous ambulatory peritoneal dialysis (CAPD). 2.
Chronic Kidney Disease. Basics of CKD Terms Diagnosis Management
 Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
HIV AND CHRONIC KIDNEY DISEASE. Understanding GFR
 HIV AND CHRONIC KIDNEY DISEASE Understanding GFR in PEOPLE WITH HIV contents Introduction... 4 Chronic Kidney Disease... 5 What are kidneys and what do they do?... 5 What is glomerular filtration rate
HIV AND CHRONIC KIDNEY DISEASE Understanding GFR in PEOPLE WITH HIV contents Introduction... 4 Chronic Kidney Disease... 5 What are kidneys and what do they do?... 5 What is glomerular filtration rate
Routine Clinic Lab Studies
 Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
CHRONIC KIDNEY FAILURE
 CHRONIC KIDNEY FAILURE Overview Chronic kidney disease, also called chronic kidney failure, describes the gradual loss of kidney function. Your kidneys filter wastes and excess fluids from your blood,
CHRONIC KIDNEY FAILURE Overview Chronic kidney disease, also called chronic kidney failure, describes the gradual loss of kidney function. Your kidneys filter wastes and excess fluids from your blood,
IN-CENTER HEMODIALYSIS (HD) CLINICAL PERFORMANCE MEASURES DATA COLLECTION FORM 2006
 IN-CENTER HEMODIALYSIS (HD) CLINICAL PERFORMANCE MEASURES DATA COLLECTION FORM 2006 PATIENT IDENTIFICATION [Before completing please read instructions at the bottom of this page and on pages 5 and 6] MAKE
IN-CENTER HEMODIALYSIS (HD) CLINICAL PERFORMANCE MEASURES DATA COLLECTION FORM 2006 PATIENT IDENTIFICATION [Before completing please read instructions at the bottom of this page and on pages 5 and 6] MAKE
Haemodialysis. Overview. Preparing for haemodialysis. Links to sections in topic Other topics available on website. Fistula
 Haemodialysis This infokid topic is for parents and carers about children s kidney conditions. Visit www.infokid.org.uk to find more topics about conditions, tests & diagnosis, treatments and supporting
Haemodialysis This infokid topic is for parents and carers about children s kidney conditions. Visit www.infokid.org.uk to find more topics about conditions, tests & diagnosis, treatments and supporting
Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm.
 Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Critical Thinking. Beat the Clock!
 Critical Thinking Beat the Clock! Critical Thinking Making good choices by using information from several sources o Training o Policies and procedures o Communicating/collaborating with other dialysis
Critical Thinking Beat the Clock! Critical Thinking Making good choices by using information from several sources o Training o Policies and procedures o Communicating/collaborating with other dialysis
End-Stage Renal Disease. Anna Vinnikova, M.D. Associate Professor of Medicine Division of Nephrology
 End-Stage Renal Disease Anna Vinnikova, M.D. Associate Professor of Medicine Division of Nephrology ESRD : Life with renal replacement therapy CASE: 18 month old male with HUS develops ESRD PD complicated
End-Stage Renal Disease Anna Vinnikova, M.D. Associate Professor of Medicine Division of Nephrology ESRD : Life with renal replacement therapy CASE: 18 month old male with HUS develops ESRD PD complicated
Haemodialysis access with an arteriovenous fistula
 Haemodialysis access with an arteriovenous fistula NHS Logo here Health & care information you can trust The Information Standard Certified Member Working together for better patient information If you
Haemodialysis access with an arteriovenous fistula NHS Logo here Health & care information you can trust The Information Standard Certified Member Working together for better patient information If you
Glossary. Anesthesiologist A doctor who puts you or parts of your body to sleep during surgery.
 1-Glossary Glossary Acute rejection A type of rejection that occurs when immune cells from your body attack the transplanted organ(s). Acute rejection may occur at any time after a transplant. But it usually
1-Glossary Glossary Acute rejection A type of rejection that occurs when immune cells from your body attack the transplanted organ(s). Acute rejection may occur at any time after a transplant. But it usually
Sid Bhende MD Sentara Vascular Specialists April 28 th Dialysis Access Review: Understanding the Access Options our Patients Face
 Sid Bhende MD Sentara Vascular Specialists April 28 th 2018 Dialysis Access Review: Understanding the Access Options our Patients Face Disclosures Dialysis Background Why is it important? Outline National
Sid Bhende MD Sentara Vascular Specialists April 28 th 2018 Dialysis Access Review: Understanding the Access Options our Patients Face Disclosures Dialysis Background Why is it important? Outline National
Patient Education Transplant Services. Glossary of Terms. For a kidney/pancreas transplant
 Patient Education Glossary of Terms For a kidney/pancreas transplant Glossary of Terms Page 18-2 Antibody A protein substance made by the body s immune system in response to a foreign substance. Antibodies
Patient Education Glossary of Terms For a kidney/pancreas transplant Glossary of Terms Page 18-2 Antibody A protein substance made by the body s immune system in response to a foreign substance. Antibodies
What is renal failure?
 What is renal failure? The kidney is a very important organ, and cannot be restored to health once it fails. However, it is possible to avoid or retard the deterioration of its functionality if therapy
What is renal failure? The kidney is a very important organ, and cannot be restored to health once it fails. However, it is possible to avoid or retard the deterioration of its functionality if therapy
DIABETES AND CHRONIC KIDNEY DISEASE
 DIABETES AND CHRONIC KIDNEY DISEASE Stage 5 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
DIABETES AND CHRONIC KIDNEY DISEASE Stage 5 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
CIE Biology GCSE. 9: Transport in animals. Notes.
 CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
Urinary System. Analyze the Anatomy and Physiology of the urinary system
 Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
About Your Dialysis Treatment
 PATIENT & CAREGIVER EDUCATION About Your Dialysis Treatment This information explains dialysis at Memorial Sloan Kettering (MSK). Your Kidneys and Their Functions Your kidneys are 2 bean-shaped organs
PATIENT & CAREGIVER EDUCATION About Your Dialysis Treatment This information explains dialysis at Memorial Sloan Kettering (MSK). Your Kidneys and Their Functions Your kidneys are 2 bean-shaped organs
UW MEDICINE PATIENT EDUCATION. Hemodialysis. A treatment option for kidney disease. Treatment Options for Kidney Disease
 UW MEDICINE PATIENT EDUCATION Hemodialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and care of blood access. 2. Understand the purpose and basic principles of hemodialysis.
UW MEDICINE PATIENT EDUCATION Hemodialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and care of blood access. 2. Understand the purpose and basic principles of hemodialysis.
Understanding. Your Kidneys. Laurie Biel, RN,BSN, CNN The MGH Center For Renal Education March 28, 2016
 Understanding Your Kidneys Laurie Biel, RN,BSN, CNN The MGH Center For Renal Education March 28, 2016 Today s Discussion - The Role of your kidneys Common causes of kidney disease Treatment for kidney
Understanding Your Kidneys Laurie Biel, RN,BSN, CNN The MGH Center For Renal Education March 28, 2016 Today s Discussion - The Role of your kidneys Common causes of kidney disease Treatment for kidney
It is important to learn all you can about your access so you can take better care of yourself.
 PEP CONNECT PEP Talk Outline Topic Vascular Access P A T I E N T E D U C A T I O N P R O G R A M An adequate permanent vascular access is the key to living long and well on dialysis. There are three kinds
PEP CONNECT PEP Talk Outline Topic Vascular Access P A T I E N T E D U C A T I O N P R O G R A M An adequate permanent vascular access is the key to living long and well on dialysis. There are three kinds
Utopia Health Career Center, LLC. Do not distribute without permission.
 Introduction What is dialysis and a brief history. What laws govern dialysis treatments. How to ensure high quality care for patients. How to behave in a professional way. How to become certified. We don
Introduction What is dialysis and a brief history. What laws govern dialysis treatments. How to ensure high quality care for patients. How to behave in a professional way. How to become certified. We don
Evaluation of AVF and AVG
 Evaluation of AVF and AVG 2013 Nephrology Nursing Symposium Albuquerque Vascular Access Leading cause of hospitalization in the ESRD population Annual cost approaching $1.5 billion (USRDS, 2004) Current
Evaluation of AVF and AVG 2013 Nephrology Nursing Symposium Albuquerque Vascular Access Leading cause of hospitalization in the ESRD population Annual cost approaching $1.5 billion (USRDS, 2004) Current
There are no shortcuts to Dialysis
 There are no shortcuts to Dialysis 1 Outcomes John Sweeny Wednesday, March 21 st, 2018 (3:10 pm 4:10 pm) 2 Quality in Hemodialysis Quality Health Care is the degree to which health services increases the
There are no shortcuts to Dialysis 1 Outcomes John Sweeny Wednesday, March 21 st, 2018 (3:10 pm 4:10 pm) 2 Quality in Hemodialysis Quality Health Care is the degree to which health services increases the
Diabetes and Kidney Disease: Time to Act. Your Guide to Diabetes and Kidney Disease
 Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
Diabetes and Kidney Disease: Time to Act Your Guide to Diabetes and Kidney Disease Diabetes is fast becoming a world epidemic Diabetes is reaching epidemic proportions worldwide. Every year more people
ONLINE HEMODIALYSIS TRAINING SESSION 2
 ONLINE HEMODIALYSIS TRAINING SESSION 2 This document is a supplement to the Online Training. Do not reproduce. Copyright Dialysis4Career. All Rights Reserved. The Renal Diet Why is the renal diet important?
ONLINE HEMODIALYSIS TRAINING SESSION 2 This document is a supplement to the Online Training. Do not reproduce. Copyright Dialysis4Career. All Rights Reserved. The Renal Diet Why is the renal diet important?
CSI (Clinical Scenario Investigation): Hyperkalemia
 CSI (Clinical Scenario Investigation): Hyperkalemia Alison Thomas, RN(EC), MN, CNeph(C) Ann Jones, RN(EC), MSN, CNeph(C) Joyce Hunter, RN, Vascular Access Co-ordinator Simcoe Muskoka Regional Kidney Care
CSI (Clinical Scenario Investigation): Hyperkalemia Alison Thomas, RN(EC), MN, CNeph(C) Ann Jones, RN(EC), MSN, CNeph(C) Joyce Hunter, RN, Vascular Access Co-ordinator Simcoe Muskoka Regional Kidney Care
LIVING WITH KIDNEY DISEASE: A PATIENT MANUAL
 LIVING WITH KIDNEY DISEASE: A PATIENT MANUAL Fifth Edition, September, 2002 i Presented by The Renal Network, Inc., this manual was published under CMS contact numbers 500-00-NW09 & 500-00-NW10. Living
LIVING WITH KIDNEY DISEASE: A PATIENT MANUAL Fifth Edition, September, 2002 i Presented by The Renal Network, Inc., this manual was published under CMS contact numbers 500-00-NW09 & 500-00-NW10. Living
Excretion and Water Balance
 Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Kidney Failure. Haemodialysis
 Kidneys & Kidney Failure 2 Haemodialysis This booklet will help you to know the process of Haemodialysis in detail. It will also tell you about the disposables of Haemodialysis. In the end the advantages
Kidneys & Kidney Failure 2 Haemodialysis This booklet will help you to know the process of Haemodialysis in detail. It will also tell you about the disposables of Haemodialysis. In the end the advantages
Urinary System. Dr. Thorson
 Urinary System Dr. Thorson Lesson Objectives Upon completion of this lesson, students should be able to Define and spell the terms to learn for this chapter. Describe the purpose and function of the urinary
Urinary System Dr. Thorson Lesson Objectives Upon completion of this lesson, students should be able to Define and spell the terms to learn for this chapter. Describe the purpose and function of the urinary
Blood pressure and kidney disease
 Blood pressure and High blood pressure is the second most common cause of. Your heart pumps your blood through tubes (blood vessels) called arteries and veins. When your blood moves through the blood vessels,
Blood pressure and High blood pressure is the second most common cause of. Your heart pumps your blood through tubes (blood vessels) called arteries and veins. When your blood moves through the blood vessels,
Patient Education. Transplant Services. Benefits and. Of a kidney/pancreas transplant
 Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure
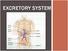 EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
HEMODIALYSIS. Nursing 246 Adapted from Lewis Chapter 47 Donna Geiger, RN, MSN, FNP
 HEMODIALYSIS Nursing 246 Adapted from Lewis Chapter 47 Donna Geiger, RN, MSN, FNP Dialysis Begun when patient s uremia can no longer be adequately managed conservatively What is uremia?? What lab test
HEMODIALYSIS Nursing 246 Adapted from Lewis Chapter 47 Donna Geiger, RN, MSN, FNP Dialysis Begun when patient s uremia can no longer be adequately managed conservatively What is uremia?? What lab test
INTRODUCTION TO HAEMODIALYSIS
 INTRODUCTION TO HAEMODIALYSIS Why do I need dialysis? What is dialysis? How does haemodialysis work? Where will I have my treatment? Will dialysis cure my kidney failure? Will dialysis keep me well? I
INTRODUCTION TO HAEMODIALYSIS Why do I need dialysis? What is dialysis? How does haemodialysis work? Where will I have my treatment? Will dialysis cure my kidney failure? Will dialysis keep me well? I
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Science 8 Chapter 12 Section 1
 Science 8 Chapter 12 Section 1 How Body Systems are Connected (pp. 436-445) System Coordination Cellular Respiration There are 4 different body systems that all play a part in the process of cellular respiration:
Science 8 Chapter 12 Section 1 How Body Systems are Connected (pp. 436-445) System Coordination Cellular Respiration There are 4 different body systems that all play a part in the process of cellular respiration:
Informed Consent for Liver Transplant Patients
 Informed Consent for Liver Transplant Patients Evaluation Process You will be evaluated with consultations, lab tests and various procedures to determine the medical appropriateness of liver transplant.
Informed Consent for Liver Transplant Patients Evaluation Process You will be evaluated with consultations, lab tests and various procedures to determine the medical appropriateness of liver transplant.
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC
 RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC GOALS Overview of renal system anatomy / physiology Discuss common medical / trauma renal issues Identify associated assessment keys GOALS Introduction
RENAL & HEMATOLOGY EMERGENCIES JEFF SIMONS B.S. F-PC GOALS Overview of renal system anatomy / physiology Discuss common medical / trauma renal issues Identify associated assessment keys GOALS Introduction
Utopia Health Career Center
 Utopia Health Career Center Magda Castaneda RN, BSN, CNN, HTC Coordinator / Instructor BONENT Approved Program Florida Board of Nursing CE Provider # 50-16333 Property of Utopia Health Career Center, LLC.
Utopia Health Career Center Magda Castaneda RN, BSN, CNN, HTC Coordinator / Instructor BONENT Approved Program Florida Board of Nursing CE Provider # 50-16333 Property of Utopia Health Career Center, LLC.
Our Commitment to Quality and Patient Safety Core Measures
 Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Heart Facts. The average adult heart beats 72 times a min 100,000 times a day 3,600,000 times a year 2.5 billion times during a lifetime.
 Circulatory System Heart Facts The average adult heart beats 72 times a min 100,000 times a day 3,600,000 times a year 2.5 billion times during a lifetime. Heart Facts Weighs 11 oz A healthy heart pumps
Circulatory System Heart Facts The average adult heart beats 72 times a min 100,000 times a day 3,600,000 times a year 2.5 billion times during a lifetime. Heart Facts Weighs 11 oz A healthy heart pumps
network of thin-walled capillaries closely surrounded by a pear-shaped epithelial membrane called the Bowman s capsule
 Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Kidney Disease and Failure. March 2018
 Kidney Disease and Failure March 2018 Objectives l State the function of the kidney l Define kidney disease l Identify tests and abnormal test results for kidney function l Recognize prevention and treatment
Kidney Disease and Failure March 2018 Objectives l State the function of the kidney l Define kidney disease l Identify tests and abnormal test results for kidney function l Recognize prevention and treatment
Chronic Kidney Disease (CKD) Stages. CHRONIC KIDNEY DISEASE Treatment Options. Incident counts & adjusted rates, by primary diagnosis Figure 2.
 Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Taking Care of Your Kidneys
 Taking Care of Your Kidneys Part A Roseville & Sacramento Medical Centers Health Promotion Department Nutritional Services Agenda Slide How your kidneys work Explaining chronic kidney disease Protecting
Taking Care of Your Kidneys Part A Roseville & Sacramento Medical Centers Health Promotion Department Nutritional Services Agenda Slide How your kidneys work Explaining chronic kidney disease Protecting
Module 7 Your Blood Work
 Module 7 Your Blood Work Every month you will need to collect a sample of your blood just before you start dialysis, and depending on your doctor s recommendation, at the end of your dialysis treatment.
Module 7 Your Blood Work Every month you will need to collect a sample of your blood just before you start dialysis, and depending on your doctor s recommendation, at the end of your dialysis treatment.
Lower Extremity Arterial Disease
 Lower Extremity Arterial Disease Circulating the Facts About Peripheral Disease Brought to you by the Education Committee of the Society for 1 www.svnnet.org Peripheral Artery Disease (PAD) Many people
Lower Extremity Arterial Disease Circulating the Facts About Peripheral Disease Brought to you by the Education Committee of the Society for 1 www.svnnet.org Peripheral Artery Disease (PAD) Many people
The Excretory System
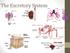 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Dialysis Event Protocol
 Dialysis Event Protocol Introduction In 2009, more than 370,000 patients were treated with maintenance hemodialysis in the United States. 1 Hemodialysis patients require a vascular access, which can be
Dialysis Event Protocol Introduction In 2009, more than 370,000 patients were treated with maintenance hemodialysis in the United States. 1 Hemodialysis patients require a vascular access, which can be
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Kidney Disease Treatment Options
 Page 1 Fact sheet The kidneys play a number of important roles in your body such as: extracting excess water to make urine (wee) controlling your blood pressure filtering waste products and toxins from
Page 1 Fact sheet The kidneys play a number of important roles in your body such as: extracting excess water to make urine (wee) controlling your blood pressure filtering waste products and toxins from
Treatment choices for someone with Stage 5 kidney disease are:
 Information for patients about advanced kidney disease Dialysis and non-dialysis treatments DOCUMENT PREPARED FOR This information is to help you understand some key issues about dialysis; it is designed
Information for patients about advanced kidney disease Dialysis and non-dialysis treatments DOCUMENT PREPARED FOR This information is to help you understand some key issues about dialysis; it is designed
Presented by UIC College of Nursing
 Presented by UIC College of Nursing Renal Disease Purpose and Objectives Background Renal disease Causes Statistics Renal disease and Hypertension Renal disease and Diabetes Types Acute renal failure Chronic
Presented by UIC College of Nursing Renal Disease Purpose and Objectives Background Renal disease Causes Statistics Renal disease and Hypertension Renal disease and Diabetes Types Acute renal failure Chronic
Your Kidney Health. Your Choices. Chronic Kidney Disease
 Your Kidney Health Your Choices Your doctor may have told you that you have chronic kidney disease (CKD or advanced kidney disease; or, you may be in kidney failure, and may have to make a decision about
Your Kidney Health Your Choices Your doctor may have told you that you have chronic kidney disease (CKD or advanced kidney disease; or, you may be in kidney failure, and may have to make a decision about
A VIDEO SERIES. living WELL. with kidney failure HOW KIDNEY FAILURE AFFECTS YOUR BODY
 A VIDEO SERIES living WELL with kidney failure HOW KIDNEY FAILURE AFFECTS YOUR BODY Contents 2 Introduction 3 What will I learn? 4 How does kidney failure affect my body? 5 How can I protect my heart
A VIDEO SERIES living WELL with kidney failure HOW KIDNEY FAILURE AFFECTS YOUR BODY Contents 2 Introduction 3 What will I learn? 4 How does kidney failure affect my body? 5 How can I protect my heart
3.4. The Circulatory System
 The Circulatory System The human circulatory system is made up of the blood, the heart, and the blood vessels. The function of the circulatory system is to transport substances around the body. It moves
The Circulatory System The human circulatory system is made up of the blood, the heart, and the blood vessels. The function of the circulatory system is to transport substances around the body. It moves
Kidney Failure: Choosing a treatment that is RIGHT FOR YOU
 Kidney Failure: Choosing a treatment that is RIGHT FOR YOU Your kidneys filter wastes from your blood and regulate other functions of your body. When your kidneys fail, you need treatment to replace the
Kidney Failure: Choosing a treatment that is RIGHT FOR YOU Your kidneys filter wastes from your blood and regulate other functions of your body. When your kidneys fail, you need treatment to replace the
Treatment Options for Kidney Failure Living with End-Stage Renal Disease
 Treatment Options for Kidney Failure Dialysis Center Living with End-Stage Renal Disease 1887_FMech_1601.indd 25 12/29/15 10:56 AM Facing Kidney Failure Your doctor has told you that you have kidney failure,
Treatment Options for Kidney Failure Dialysis Center Living with End-Stage Renal Disease 1887_FMech_1601.indd 25 12/29/15 10:56 AM Facing Kidney Failure Your doctor has told you that you have kidney failure,
Excretion: is the removal of waste products formed by metabolism, out of the body
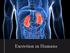 Excretion in Humans Excretion: is the removal of waste products formed by metabolism, out of the body Accumulation of wastes in the cells would affect the normal functioning of the cells By getting rid
Excretion in Humans Excretion: is the removal of waste products formed by metabolism, out of the body Accumulation of wastes in the cells would affect the normal functioning of the cells By getting rid
YOUR KIDNEYS AREN T WORKING PROPERLY.
 When you re born, everything works perfectly. Then something goes wrong and you ask: YOUR KIDNEYS AREN T WORKING PROPERLY. What does this mean? How can you stay healthy? HOW DO I DEAL WITH THIS? WHAT ROLE
When you re born, everything works perfectly. Then something goes wrong and you ask: YOUR KIDNEYS AREN T WORKING PROPERLY. What does this mean? How can you stay healthy? HOW DO I DEAL WITH THIS? WHAT ROLE
: thick middle layer; cardiac muscles : thin inner layer; endothelial lining
 1 2 3 4 Bio 1102 Lecture 5 (guided) Chapter 8: Heart & Blood Vessels Functions of Circulatory System: To carry from lungs to all cells, tissues, and organs of body To carry from digestive system to all
1 2 3 4 Bio 1102 Lecture 5 (guided) Chapter 8: Heart & Blood Vessels Functions of Circulatory System: To carry from lungs to all cells, tissues, and organs of body To carry from digestive system to all
MEDICAL EQUIPMENT II HEMODIALYSIS
 MEDICAL EQUIPMENT II - 2012 HEMODIALYSIS Lecture 1 Prof. Yasser Mostafa Kadah Hemodialysis Machines Single-patient hemodialysis machines deliver a patient s dialysis prescription by controlling blood and
MEDICAL EQUIPMENT II - 2012 HEMODIALYSIS Lecture 1 Prof. Yasser Mostafa Kadah Hemodialysis Machines Single-patient hemodialysis machines deliver a patient s dialysis prescription by controlling blood and
Atherosclerosis. Atherosclerosis happens when the blood vessels
 Atherosclerosis Atherosclerosis happens when the blood vessels that carry oxygen and nutrients from your heart to the rest of your body (arteries) become thick and stiff sometimes restricting blood flow
Atherosclerosis Atherosclerosis happens when the blood vessels that carry oxygen and nutrients from your heart to the rest of your body (arteries) become thick and stiff sometimes restricting blood flow
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
Lesson #7: Quality Assessment and Performance Improvement
 ESRD Update: Transitioning to New ESRD Conditions for Coverage Student Manual Lesson #7: Quality Assessment and Performance Improvement Learning Objectives At the conclusion of this lesson, you will be
ESRD Update: Transitioning to New ESRD Conditions for Coverage Student Manual Lesson #7: Quality Assessment and Performance Improvement Learning Objectives At the conclusion of this lesson, you will be
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
