Keywords Stroke; ischemic; carotid artery stenting; microembolic brain infarcts; diffusion restriction
|
|
|
- Anna Spencer
- 5 years ago
- Views:
Transcription
1 Comparison of Clinical and Radiological Outcome of Carotid Angioplasty and Stenting after Direct Navigation Versus Exchange Methods: a Randomized Clinical Trial Mojtaba Rismanchi 1,2 and Afshin Borhani-Haghighi 1,2, * 1 Clinical Neurology Research Center, Shiraz University of Medical Sciences, Shiraz, Iran 2 Department of Neurology, Shiraz University of Medical Sciences, Shiraz, Iran Abstract Background The purpose of this study was to compare the frequency of microembolic brain infarcts after direct navigation method versus exchange method in carotid artery stenting and vertebral artery origin angioplasty. Methods and Material This is a prospective study conducted at Shiraz University of Medical Sciences in southern Iran. Consecutive patients undergoing carotid angioplasty and stenting and vertebral artery origin stenting were randomly assigned into two groups with direct navigation method and exchange method. Subsequently, postprocedural magnetic resonance imaging (MRI) including diffusion weighted imaging and apparent diffusion coefficient were obtained within the first 24 hours after completion of the procedure. Results In total, 89 patients were recruited (67% male, mean age: 72 years). Cases comprised of 38 left internal carotid arteries (ICAs), 38 right ICAs, 6 left vertebral artery origin, and 7 right vertebral artery origin. Forty patients underwent exchange method, while 49 underwent direct navigation method. There was only one clinical stroke that occurred in exchange method group. Fifteen patients (37.5%) in exchange group and 23 patients (46.9%) in direct navigation group developed diffusion restricted lesions. In exchange group, 13 patients (32.5%) had at least one diffusion restricted lesion ipsilateral to the target vessel, and three patients (7.5%) had at least one diffusion restricted lesion contralateral to the target vessel. In direct navigation group, these measures were 19 (38.8%) and 9 (18.4%). However, no statistically significant intergroup differences were observed. The only significant difference was bilateral infarct percentile, which was more common in the direct navigation method (0.032). Conclusion Diffusion restricted lesions were more common in the direct navigation method, both ipsilateral and contralateral to the target vessel, and in both carotid and vertebral artery study subgroups. However, differences were not statistically significant. Keywords Stroke; ischemic; carotid artery stenting; microembolic brain infarcts; diffusion restriction Introduction Stroke is a worldwide critical health problem [1]. Large arterial stenosis is one of the treatable causes of ischemic stroke [2]. Carotid artery stenting (CAS) and vertebral artery origin stenting (VAOS) have been increasingly applied as an alternative to invasive carotid endarterectomy (CEA) in cases with cervical artery stenosis [3,4]. Nonetheless, transient ischemic attack (TIA), ischemic strokes, intracerebral hemorrhage (ICH), myocardial infarction, hemodynamic depression, and death are the most serious complications of these procedures [5]. Micro embolic brain infarcts have been considered as a major concern for CAS and their detrimental effects Vol. 9, No. 6, pp. XX XX. Published December, All Rights Reserved by JVIN. Unauthorized reproduction of this article is prohibited Address correspondence to: Afshin Borhani-Haghighi. *Corresponding Author: Afshin Borhani-Haghighi MD, Department of Neurology, Namazi Hospital, Shiraz, Iran. Tel/Fax: neuro.ab@gmail.com
2 2 on cognition are well-established [6]. Although usually silent, symptomatic microembolic brain infarcts are present in 2 17% of such patients [7]. Difficult aortic arch, unfavorable supra-aortic takeoff, pre- or poststenotic vascular tortuosity and acute angle between parent and offspring arteries are among the factors. These pose special challenges during the advancement of guiding catheters near carotid bifurcation, and consequently, increase the rate of symptomatic and asymptomatic brain infarcts [8]. There are two methods for advancement of guiding catheter. In direct navigation method, guiding catheter is directly engaged to supra-aortic arteries and advanced on a hydrophilic wire. Meanwhile, the exchange method is based on using a stiff wire anchored to external carotid artery (ECA) for further advancement of guiding catheter [9]. There are pros and cons regarding these techniques [10,11]. In this prospective study, the risk of postprocedural strokes and silent brain infarcts was compared between direct navigation and exchange methods. Methods and Materials Patients and settings This study was conducted from January 2016 to January 2017 at Kowsar Hospital, a major referral center for stroke patients in southern Iran, affiliated to Shiraz University of Medical Sciences (SUMS). The study consists of two subgroups. In CAS subgroup, we included symptomatic patients with ischemic stroke/tia with greater than 70% stenosis of the ipsilateral internal carotid artery (ICA), as well as asymptomatic patients with more than 80% stenosis of ICA, who were at standard or high risk for CEA. The severity of stenosis was calculated according to the North American Symptomatic CEA Trial criteria [12]. VAOS was performed for patients with greater than 70% stenosis of vertebral artery origin and contralateral occlusion, stenosis or atresia, and posterior circulation stroke or TIA, need for coronary artery bypass graft, bilateral anterior circulation disease, and ipsilateral posterior inferior cerebellar artery TIA/stroke with no other embolic source [3]. The stenosis in vertebral artery origin was verified by computed tomography angiography or magnetic resonance angiography before stenting. Patients with ICH, lacunar stroke, vasculitis, arterial dissection, and fibromuscular dysplasia were excluded. Patients with Modified Ranking Scale of equal or greater than 3 after a stroke were also excluded. The trial was approved by Medical Ethics for Researches and Institutional Review Board ( ) affiliated to SUMS. Each patient was individually informed about the process of experiment and a written informed consent was obtained. Patients were pretreated with clopidogrel 75 mg/day and aspirin 80 mg/day. During the procedure, the patients received heparin 80 units/kg of body weight after successful femoral artery puncture to maintain an activated clotting time longer than 250 seconds. Patients were randomly assigned into direct navigation method or exchanging method using block randomization. In direct navigation method, 7F right Judkins guiding catheter, Zenyte (Asahi Intecc, Aichi, Japan) or Launcher (Medtronic, MN, USA) was used to engage supra-aortic arteries and advanced on a hydrophilic wire (Glidewire, Terumo, NJ, USA). The guiding catheter was parked close to common carotid artery (CCA) bifurcation or vertebral artery origin. In exchanging technique, a 5F diagnostic catheter (Glidecath JB1, Terumo, NJ, USA) was advanced into the ipsilateral ECA or superior carotid artery (SCA) using a hydrophilic wire. Afterward, the hydrophilic wire was withdrawn and substituted with a stiff (0.038, 260 cm) wire (Emerald, Cordis, Baar, Switzerland). Next, the 5F catheter was also withdrawn and a 7F guiding catheter was advanced (as above) on the anchored stiff wire in the CCA or SCA for the purpose of stenting. Distal embolic protection devices such as Filter EZ (Boston scientific, Marlborough, MA, USA) or Spider X (Medtronic, MN, USA) were used for carotid stenting. Self-expanding stents such as Wallstent (Boston scientific) or Cristalloideale (Medtronic, MN, USA) were used for carotid stenting. For VAOS, balloon-mounted drug eluted stents were deployed without protection device. Pre- and/or postdilation were performed in suitable cases. Postdilation was done with the same balloon to flare the proximal part of the stent in SCA. Coronary stents such as Orsiro (Biotronick, Bülach, Switzerland), Xience (Abbott, Chicago, IL, USA), or Promus (Boston Scientific, Marlborough, ma, USA) were used for VAOS. All patients were followed up over the next several days and were thoroughly evaluated by the interventionist neurologist for any potential ischemic or hemorrhagic stroke and any other peri- and postprocedural complications immediately after the procedure, as well as on days 1, 7, and 30. Data collection Postprocedural magnetic resonance imaging (MRI) was taken within the first 24 hours after completion of the
3 Rismanchi and Borhani-Haghighi 3 procedure using Simens MR 1.5 Tesla machine. The studied MRI sequences included mm slice thickness axial diffusion weighted imaging (DWI), and apparent diffusion coefficient (ADC) with TR/TE: 100/1000, flip angle: 90. Maximum spatial gradient of 3.3 Tesla/meter and a maximum whole body averaged specific absorption rate of 2.0 W/kg for 15 min of MRI were considered for all procedures. In order to determine any new ischemic lesion during the trial time window and to differentiate them from old ones, only lesions with diffusion restriction (hyperintense in DWI and hypointense in ADC) were recognized as to be relevant to the outcome interpretation. Presence or absence of new lesions, number of lesions, the largest existing diameter of a lesion, accumulated lesion surface area, and the average surface area (accumulated lesion surface area/ number of lesions) were measured. Location (cortical versus subcortical) and laterality (ipsilateral versus contralateral to the target vessel) were also recorded. In order to measure the lesion surface area, two perpendicular lesion diameters matched with the largest diameter of lesions were measured by means of computerized tools from Infinite PACS software (Infinite Healthcare, Seoul, South Korea), assuming elliptical geometry of cerebral infarctive lesion studied in the literature [12]. In an attempt to ensure acuity of the results, images were studied by two independent neuroradiologists who were blinded to the patients clinical status and grouping, and discrepancies were later reviewed and reconciled. Outcome definition Primary clinical outcome was defined as development of any new stroke event after CAS or VAOS. Secondary clinical outcomes were ischemic stroke ipsilateral or contralateral to the target vessel. All clinical outcomes in one month were ascertained. Primary radiologic outcome was the presence of any DWI restricted lesion, while the presence of DWI restricted lesions ipsilateral or contralateral to the target vessel, number of these lesions and surface area of the lesions were considered as the secondary radiologic outcomes. Statistical analysis Data were analyzed using the Statistical Package for the Social Sciences version 16.0 (SPSS Inc., Chicago, IL, USA). Continuous values are presented as mean ± SD and categorical variables as frequency and percentage. Fisher s exact test or Student s t-test were used when appropriate. Results In this randomized trial study, 89 patients were recruited (67% male, age: ± 8.1). Thirty-eight LICA, 38 RICA, 6 LVAO, and 7 RVAO were stented. Regarding major risk factors of atherosclerosis, 69 (77.5%), 39 (43.8%), 35 (39.3%), and 31 (34.8%) of patients had hypertension, hyperlipidemia, smoking and diabetes mellitus, respectively. Preprocedural stenosis and residual stenosis were 78.6% ± 17.8% and 17.8% ± 14.6%. Seventy-four percent of all lesions were ulcerated and 48% calcified. In total, 40 patients underwent exchange method and 49 patients underwent direct navigation method. After the stenting procedures, 38 patients (42.7%) had diffusion restricted lesions. In DWI+ patients, on average each patient had 1.7 ± 2.7 lesions. Largest lesion diameter, accumulated lesion surface area, and average surface area were 10.8 ± 7.5, 99.2 ± 217, and ± 211, respectively. In these patients, 15.7% of lesions were cortical and 84.3% were subcortical. Meanwhile, 77.2% of lesions were ipsilateral and 22.8% were contralateral to the target vessels. Percentage of DWI + patients, number of lesions, lesion surface area, average surface area, largest lesion diameter, percentage of cortical infarcts, and percentage of contralateral infarct were not significantly different between direct navigation method and exchange method (Table 1). The percentile of contralateral, ipsilateral, and bilateral infarct was defined as the percentage of patients with at least one infarct in the corresponding areas. Ipsilateral infarct percentile and contralateral infarct percentile were not significantly different between the two methods. Bilateral infarct percentile was observed in one patient in exchange method (2.5%), and eight patients in direct navigation method (16.39%). This difference was statistically significant (P = 0.032). CAS subgroup Seventy-six patients were assigned in the CAS subgroup (67.1% male, age: 72.6 ± 8); 38 LICA and 38 RICA were stented. EPD was used in 64 (84.2%) of patients. Also, predilation was performed in 30 (39.5%) patients and postdilation in 64 (84.2%) patients. There was no significant difference between two groups regarding mean age, gender, major risk factors of atherosclerosis, hemoglobin concentration, platelet count and
4 4 Table 1. Comparison of MRI derived factors describing microinfarcts in the general population CAS + VAOS(N = 89) Direct navigation method N = 49 Exchange method N = 40 P value Percent of DWI + patients 61.22% 47.5% 0.14 Number of lesions (n) 1.89 ± ± Lesion surface area (mm 2 ) ± ± Average surface area (mm 2 ) ± ± Largest lesion diameter (mm 2 ) 11.5 ± ± Cortical infarct (%) 15.9% 15.47% 0.95 Contralateral infarct (%) 33.5% 16.66% 0.19 Contralateral infarct percentile 22.5% (N = 11) 10% (N = 4) 0.10 Ipsilateral infarct percentile 55% (N = 27) 40%(N = 16) 0.11 Bilateral infarct percentile 16.39% (N = 8) 2.5% (N = 1) The percentage of contralateral infarcts indicates the ratio of infarct numbers contralateral to the target stented vessel in the form of percentage. The percentile of contralateral, ipsilateral, and bilateral infarct indicates the number of patients with at least one infarct in the corresponding areas. Table 2. Comparison of MRI derived factors describing microinfarcts in CAS study subgroup CAS(N = 76) Direct navigation method N = 43 Exchange method N = 33 P value Percent of DWI + patients 65.11% (N = 28) 57.57% (N = 19) 0.33 Number of lesions (n) 2 ± ± Lesion surface area (mm 2 ) ± ± Average surface area (mm 2 ) ± ± Largest lesion diameter (mm 2 ) ± ± Cortical infarct (%) 10% 19.6% 0.16 Contralateral infarct (%) 30.35% 16.66% 0.28 Contralateral infarct percentile 21% (N = 9) 12.12% (N = 4) 0.23 ipsilateral infarct percentile 60.5% (N = 26) 48.5% (N = 16) 0.20 Bilateral infarct percentile 16.3% (N = 7) 3% (N = 1) The percent of contralateral infarcts indicates the ratio of infarct numbers contralateral to the target stented vessel in the form of percentage. The percentile of contralateral, ipsilateral, and bilateral infarcts indicates the number of patients with at least one infarct in the corresponding areas. creatinine level, mean pre-procedural stenosis, lesion ulceration, lesion calcification, mean residual stenosis, procedural time and rate of pre-dilation, post-dilation, and EPD usage (all P values >0.05). In this subgroup, 33 patients (46%) had diffusion restricted lesions, while 79% of the lesions were ipsilateral and 21% were contralateral to the target carotid. There was only one clinical stroke, which occurred after LICA stenting by direct navigation method in occipital lobe ipsilateral to the stented carotid artery. Due to inconsiderable number of clinical strokes, statistical comparison was not possible. In patients with exchange method, 19 patients (57.57%) developed diffusion restricted lesions. Meanwhile, 28 patients (65.11%) were DWI+ in the direct navigation method group. There was no statistically significant difference between these groups (P = 0.33). Table 2 shows there was no statistically significant difference between the two groups regarding the presence of diffusion restricted lesions, number of lesions, the largest lesion diameter, the accumulated lesion surface area, and the average surface area. Considering the laterality to target vessel, in exchange method 16 patients (48.5%) had at least one diffusion restricted lesion ipsilateral to the target vessel and four patients (12.12%) had at least one diffusion restricted lesion contralateral to the target vessel, and one patient in both ipsilateral and contralateral areas (3%). In direct navigation method, these measures were 26 (60.5%), 9 (21%), and 7 (16.3%), respectively. The differences between the two groups were not significant (Table 1). The mean number of contralateral lesions in exchange method was 0.4 ± 0.9 (16.6% of total lesions), and in direct navigation method 1.2 ± 1.9 (30.3% of total lesions). This difference was not significant (P = 0.13). VAOS subgroup In VAO subgroup, 13 patients (69.2% male, age: 69 ± 8.3) were assigned amongst which 6 LVAO, and 7 RVAO were stented. In the exchange method group (N = 7), no infarcts were detected after stenting. While there were two patients with new infarcts after the procedure (33%) in the direct navigation group, but was not statistically significant (P = 0.19). The comparison of other factors derived from DWI studies was not possible due to lack of new infarction in the exchange method group. Table 3 shows DWI derived microinfarct features in this study subgroup. A total of 60% of the lesions (three out of five total lesions) were contralateral to the targeted vessel in the VAOS study subgroup. All the lesions had occurred after
5 Rismanchi and Borhani-Haghighi 5 Table 3. Comparison of MRI derived factors describing microinfarcts in vertebral stenting study subgroup VAOS(N = 13) Direct method N = 6 Exchange method N = 7 P value Percent of DWI + patients 33% (N = 2) 0% (N = 0) 0.19 Number of lesions (n) 0.83 ± 1.32 NA - Lesion surface area (mm 2 ) 48 ± 15 NA - Average surface area (mm 2 ) 21 ± 12 NA - Largest lesion diameter (mm 2 ) 9.2 ± 4.5 NA - Cortical infarct (mm 2 ) 33% NA - Contralateral infarct (mm 2 ) 60% NA - Contralateral infarct (mm 2 ) 33% (N = 2) NA - ipsilateral infarct percentile 16% (N = 1) NA - Bilateral infarct percentile 16% (N = 1) NA - The percent of contralateral infarcts indicates the ratio of infarct numbers contralateral to the target stented vessel in the form of percentage. The percentile of contralateral, ipsilateral and bilateral infarct indicates the number of patients with at least one infarct in the corresponding areas. Due to the absence of microembolic signals in the exchange method, statistical analysis could not be performed. LVAO stenting in direct navigation method, even though considerable, was not possible to be analyzed statistically. Discussion The biggest drawback in endovascular treatments of cervicocephalic large arterial disease is higher rate of minor strokes in comparison with CEA [13]. The frequency of microembolic infarcts after CAS is reported to be 20 55% [6]. Although the rate of symptomatic presentation of these infarcts ranges 2 17%, their detrimental effects on cognition are well established [6,7]. Any technical modification that can decrease the rate of postprocedural symptomatic or asymptomatic brain infarcts is encouraged to be employed by the interventionists. In the current study, diffusion restricted lesions were more common in the direct navigation method both ipsilateral and contralateral to the target vessel and in both carotid and vertebral artery study subgroups, but the differences were not statistically significant. The only significant difference was bilateral infarct percentile, which was more common in direct navigation method. Although exchange method may facilitate the advancement of guiding catheter on an ECA-anchored stiff wire, it lengthens the procedure, and in turn increases the risk of embolization due to the application of a thrombogenic wire [14]. Retrograde embolization through ECA to brain was also presumed [14]. Some interventionists have used guiding sheath instead of guiding catheter [9], yet its disadvantages are the increase in procedural time, the risk of parent artery dissection and anatomical bifurcation change. We randomized our patients regardless of vessel anatomy. However, some interventionists advocate this factor in patient selection. Exchange method is favorable in treatment of patients with tortuous or aneurismal aorta, elongated aortic arch, poor angulation of innominate, LCCA or LSCA or tortuosity of CCAs or SCAs. Occlusion or severe stenoses of ECA or SCA after VAO are indications for direct navigation method [15 17]. The presence of diffusion restricted lesions contralateral to the target vessel is generally due to embolization from arch of aorta. The presence of atheromatous plaques and particularly thrombus in the arch of aorta increase the risk of embolization during CAS. The arch of aorta CT angiography or trans-esophageal echocardiography might be useful in patient selection for CAS [17]. Complex aortic arch anatomy is associated with increased risk of embolic lesions [15] and clinical complications [16]. The most important shortcoming of our study was loss of volumetric evaluation of the DWI lesions. Although the presence or absence of lesions, number of lesions, and largest lesion diameter can be obtained with nonvolumetric method (naked-eye method), accumulated or average surface area could have been evaluated, and we used volumetric assessment. Acknowledgment This work was extracted from the thesis project for the specialty degree in neurology by Mojtaba Rismanchi MD. The authors would like to appreciate the Office of Vice Chancellor of Research at SUMS for their financial support of this study (grant No# ). We also want to thank Mr. Mojtaba Neydavoudi and Mr. Zarei for their assistance. The authors wish to thank Mr. H. Argasi at the Research Consultation Center at SUMS for his invaluable assistance in editing this manuscript. References 1. Borhani-Haghighi A, et al. Hospital mortality associated with stroke in southern Iran. Iran. J Med Sci 2013;38(4):314.
6 6 2. Borhani-Haghighi A, et al. Large-vessel stenosis in the patients with ischemic stroke in Iran: prevalence, pattern, and risk factors. J Vasc Interv Neurol 2015;8(1): Borhani-Haghighi AB, et al. Vertebral artery origin stenosis and its treatment. J Stroke Cerebrovasc Dis 2011;20(4): Borhani-Haghighi A, et al. Demographic and technical risk factors of 30-day stroke, myocardial infarction, and/or death in standardand high-risk patients who underwent carotid angioplasty and stenting. Interv Neurol 2014;3(3 4): Borhani-Haghighi A, et al. The prevalence and factors contributing to hemodynamic depression in patients undergoing carotid angioplasty and stenting. J Vasc Interv Neurol 2015;8(4):5. 6. Bendszus M, Stoll G. Silent cerebral ischaemia: hidden fingerprints of invasive medical procedures. Lancet Neurol 2006;5(4): Maggio P, et al. Diffusion-weighted lesions after carotid artery stenting are associated with cognitive impairment. J Neurol Sci 2013;328(1): Harrigan MR, Deveikis JP. Intracranial cerebrovascular occlusive disease. Handbook of cerebrovascular disease and neurointerventional technique Springer2013: Gupta K, et al. A modified technique for carotid cannulation via the transfemoral approach, during angioplasty and stent placement. Tex Heart Inst J 2008;35(3): Morris P. Practical neuroangiography Lippincott Williams & Wilkins Vitek JJ, et al. Carotid artery stenting: technical considerations. Am J Neuroradiol 2000;21(9): Sims JR, et al. ABC/2 for rapid clinical estimate of infarct, perfusion, and mismatch volumes. Neurology 2009;72(24): Brott TG, et al. Stenting versus endarterectomy for treatment of carotid-artery stenosis. N Engl J Med 2010;363(1): Al-Mubarak N, et al. Effect of the distal-balloon protection system on microembolization during carotid stenting. Circulation 2001;104(17): Bijuklic K, et al. Risk factors for cerebral embolization after carotid artery stenting with embolic protection. Circ Cardiovasc Interv 2013;6(3): Burzotta F, et al. Clinical and procedural impact of aortic arch anatomic variants in carotid stenting procedures. Catheter Cardiovasc Interv 2015;86(3): Szikra P, et al. Aortic arch and common carotid artery plaques with soft components pose a substantial risk of cerebral embolization during carotid stenting. Interv Neuroradiol 2016;22(4):
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Carotid Artery Stenting (CAS) Pathophysiology. Technical Considerations. Plaque characteristics: relevant concepts. CAS and CEA
 Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent
 The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent 6 month data Piotr Musialek, MD DPhil FESC Jagiellonian University Dept. of Cardiac & Vascular Diseases John
The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent 6 month data Piotr Musialek, MD DPhil FESC Jagiellonian University Dept. of Cardiac & Vascular Diseases John
Endovascular treatment for pseudoocclusion of the internal carotid artery
 Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
New concepts for filter protection during CAS: double filtration. Alberto Cremonesi MD, FESC
 New concepts for filter protection during CAS: double filtration Alberto Cremonesi MD, FESC First Experience with the PALADIN Carotid Post-Dilation Balloon with Integrated Embolic Protection Alberto Cremonesi
New concepts for filter protection during CAS: double filtration Alberto Cremonesi MD, FESC First Experience with the PALADIN Carotid Post-Dilation Balloon with Integrated Embolic Protection Alberto Cremonesi
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Why I m afraid of occlusive devices
 Why I m afraid of occlusive devices Cannes 28.06.2008 Carlo Cernetti Cardiology Department Mirano (Venice) MEET 2008 CANNES I HAVE NOT FINACIAL INTEREST/ARRANGEMENT OR AFFILIATION CONFLICT Obstructive
Why I m afraid of occlusive devices Cannes 28.06.2008 Carlo Cernetti Cardiology Department Mirano (Venice) MEET 2008 CANNES I HAVE NOT FINACIAL INTEREST/ARRANGEMENT OR AFFILIATION CONFLICT Obstructive
The variation of carotid origin, the divergent orientation of common carotid (frequent posterior and left to right direction of right common as
 1 Introduction The access to the common carotid during carotid stenting is very challenging and is responsible of a significant number of embolic complications in the ipsilateral but also in the contralateral
1 Introduction The access to the common carotid during carotid stenting is very challenging and is responsible of a significant number of embolic complications in the ipsilateral but also in the contralateral
Assessment of the procedural etiology of stroke resulting from carotid artery stenting
 Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Managing Carotid Access from Straight - Forward to Complex Bernhard Reimers Cardiology Dept. Mirano Italy
 Managing Carotid Access from Straight - Forward to Complex Bernhard Reimers Cardiology Dept. Mirano Italy Cerebrovascular Interventions Disclosure Statement of Financial Interest I, Bernhard Reimers DO
Managing Carotid Access from Straight - Forward to Complex Bernhard Reimers Cardiology Dept. Mirano Italy Cerebrovascular Interventions Disclosure Statement of Financial Interest I, Bernhard Reimers DO
Carotid Stenting and Surgery in 2016 in Russia
 Carotid Stenting and Surgery in 2016 in Russia Novosibirsk research institute of circulation pathology named by Meshalkin, Novosibirsk, Russia Starodubtsev V., Karpenko A., Ignatenko P. Annually in Russia
Carotid Stenting and Surgery in 2016 in Russia Novosibirsk research institute of circulation pathology named by Meshalkin, Novosibirsk, Russia Starodubtsev V., Karpenko A., Ignatenko P. Annually in Russia
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Carotid Artery Stenting
 Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Algorithmic selection of emboli protection device during the procedure of carotid artery stunting
 Algorithmic selection of emboli protection device during the procedure of carotid artery stunting Yasuhiro Kawabata, Tetsuya Tsukahara, Shunichi Fukuda, Tomokazu Aoki, Satoru Kawarazaki Department of Neurosurgery,
Algorithmic selection of emboli protection device during the procedure of carotid artery stunting Yasuhiro Kawabata, Tetsuya Tsukahara, Shunichi Fukuda, Tomokazu Aoki, Satoru Kawarazaki Department of Neurosurgery,
Issam D. Moussa, MD. Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, FL
 Carotid Technologies and Protection Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, FL Disclosure Statement
Carotid Technologies and Protection Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, FL Disclosure Statement
Carotid Artery Stenting
 Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease
 AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Limitations of Other Embolic Protection Devices - Filters. Carotid Stenting with Flow Reversal. Limitations of Distal Occlusion
 Carotid Stenting with Flow Reversal Marc Schermerhorn, MD Division of Vascular and Endovascular Surgery Beth Israel Deaconess Center Boston, MA Limitations of Other Embolic Protection Devices - Filters
Carotid Stenting with Flow Reversal Marc Schermerhorn, MD Division of Vascular and Endovascular Surgery Beth Israel Deaconess Center Boston, MA Limitations of Other Embolic Protection Devices - Filters
Carotid Artery Revascularization: Current Strategies. Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014
 Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion
 Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR study
 Comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR study (RADial access for CARotide artery stenting) Zoltán Ruzsa MD PhD et al. TCT 2013 Disclosure Statement of Financial
Comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR study (RADial access for CARotide artery stenting) Zoltán Ruzsa MD PhD et al. TCT 2013 Disclosure Statement of Financial
Techniques for Carotid Interventon
 Techniques for Carotid Interventon Jay S. Yadav MD Cleveland, Ohio Disclosures Inventor of Angioguard; fixed and recurring payments from JNJ Advisor: JNJ, Guidant Understand the Patient What is the Cause
Techniques for Carotid Interventon Jay S. Yadav MD Cleveland, Ohio Disclosures Inventor of Angioguard; fixed and recurring payments from JNJ Advisor: JNJ, Guidant Understand the Patient What is the Cause
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Extracranial Carotid Artery Stenting With or Without Distal Protection Device
 Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
CAROTID ARTERY STENTING TECHNICALS ASPECTS. Symposium Abbott Vascular CANNES MEET 2008 Drs V PIRET, P BERGERON
 CAROTID ARTERY STENTING TECHNICALS ASPECTS Symposium Abbott Vascular CANNES MEET 2008 Drs V PIRET, P BERGERON POINTS TO DISCUSS TO CAS INDICATIONS CONTRA INDICATIONS ANATOMICAL CONSIDERATION TECHNICS CAS
CAROTID ARTERY STENTING TECHNICALS ASPECTS Symposium Abbott Vascular CANNES MEET 2008 Drs V PIRET, P BERGERON POINTS TO DISCUSS TO CAS INDICATIONS CONTRA INDICATIONS ANATOMICAL CONSIDERATION TECHNICS CAS
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
Although CAS is increasingly used to treat extracranial carotid
 ORIGINAL RESEARCH H.J. Kim H.J. Lee J.H. Yang I.S. Yeo J.S. Yi I.W. Lee S.B. Lee S.Y. Ryu J.K. Kim P.S. Yang The Influence of Carotid Artery Catheterization Technique on the Incidence of Thromboembolism
ORIGINAL RESEARCH H.J. Kim H.J. Lee J.H. Yang I.S. Yeo J.S. Yi I.W. Lee S.B. Lee S.Y. Ryu J.K. Kim P.S. Yang The Influence of Carotid Artery Catheterization Technique on the Incidence of Thromboembolism
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Carlo Setacci Chief Department of Surgery Vascular and Endovascular Unit University of Siena
 Which carotid procedures are required to grade the stroke risk? Carlo Setacci Chief Department of Surgery Vascular and Endovascular Unit University of Siena Faculty disclosure Carlo Setacci I have no financial
Which carotid procedures are required to grade the stroke risk? Carlo Setacci Chief Department of Surgery Vascular and Endovascular Unit University of Siena Faculty disclosure Carlo Setacci I have no financial
Treatment Considerations for Carotid Artery Stenosis. Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery
 Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
My Indications are based on anatomy
 Update in Carotid Artery Stenting &Stroke Management How to choose the best therapy? My Indications are based on anatomy Max Amor M.D max-amor@wanadoo.fr C.Breton,Z.Chati,G.Ethevenot,J.Lemoine,J.P.Simon
Update in Carotid Artery Stenting &Stroke Management How to choose the best therapy? My Indications are based on anatomy Max Amor M.D max-amor@wanadoo.fr C.Breton,Z.Chati,G.Ethevenot,J.Lemoine,J.P.Simon
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
Copyright HMP Communications
 Ocelot With Wildcat in a Complicated Superficial Femoral Artery Chronic Total Occlusion Soundos K. Moualla, MD, FACC, FSCAI; Richard R. Heuser, MD, FACC, FACP, FESC, FSCAI From Phoenix Heart Center, Phoenix,
Ocelot With Wildcat in a Complicated Superficial Femoral Artery Chronic Total Occlusion Soundos K. Moualla, MD, FACC, FSCAI; Richard R. Heuser, MD, FACC, FACP, FESC, FSCAI From Phoenix Heart Center, Phoenix,
Cerebral hyperperfusion syndrome after carotid angioplasty
 case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
Contemporary Management of Carotid Disease What We Know So Far
 Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Carotid Revascularization
 Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers
 The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
TRANSRADIAL PERIPHERAL VASCULAR INTERVENTIONS
 TRANSRADIAL PERIPHERAL VASCULAR INTERVENTIONS Cezar Staniloae NYU Heart and Vascular Institute May 27, 2015 Radial Artery is an Ideal Acess Site Easily accessible even in subjects with severe PVD Major
TRANSRADIAL PERIPHERAL VASCULAR INTERVENTIONS Cezar Staniloae NYU Heart and Vascular Institute May 27, 2015 Radial Artery is an Ideal Acess Site Easily accessible even in subjects with severe PVD Major
Prevention and Management of Vascular Complications Related to Transcatheter Aortic Valve Implantation
 Prevention and Management of Vascular Complications Related to Transcatheter Aortic Valve Implantation Marco Roffi Division of Cardiology University Hospital Geneva, Switzerland Disclosure Speaker name:...marco
Prevention and Management of Vascular Complications Related to Transcatheter Aortic Valve Implantation Marco Roffi Division of Cardiology University Hospital Geneva, Switzerland Disclosure Speaker name:...marco
Embolic Protection Devices for Transcatheter Aortic Valve Replacement
 Embolic Protection Devices for Transcatheter Aortic Valve Replacement James M. McCabe, MD Medical Director, Cardiac Cath Lab University of Washington Seattle, WA Disclosures Proctoring and honoraria for
Embolic Protection Devices for Transcatheter Aortic Valve Replacement James M. McCabe, MD Medical Director, Cardiac Cath Lab University of Washington Seattle, WA Disclosures Proctoring and honoraria for
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
CAROTID ARTERY ANGIOPLASTY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Avoiding and Managing Complications During CAS: Lessons Learned
 LINC 2019 Leipzig, Germany, Jan 22-25, 2019 Avoiding and Managing Complications During CAS: Lessons Learned Horst Sievert, Ilona Hofmann, Kolja Sievert, Laura Vaskelyte, Sameer Gafoor, Stefan Bertog, Predrag
LINC 2019 Leipzig, Germany, Jan 22-25, 2019 Avoiding and Managing Complications During CAS: Lessons Learned Horst Sievert, Ilona Hofmann, Kolja Sievert, Laura Vaskelyte, Sameer Gafoor, Stefan Bertog, Predrag
Possibilities for reducing procedural embolisation in the endovascular treatment of cervical carotid artery stenosis
 0 Possibilities for reducing procedural embolisation in the endovascular treatment of cervical carotid artery stenosis ---------------------------------------------------------------------------------------------------------
0 Possibilities for reducing procedural embolisation in the endovascular treatment of cervical carotid artery stenosis ---------------------------------------------------------------------------------------------------------
Sentinel Dual Filter Device: Technology Overview and Status of the CLEAN-TAVI Randomized Trial. Martin B. Leon, MD
 8 mins Sentinel Dual Filter Device: Technology Overview and Status of the CLEAN-TAVI Randomized Trial Martin B. Leon, MD Columbia University Medical Center Cardiovascular Research Foundation New York City
8 mins Sentinel Dual Filter Device: Technology Overview and Status of the CLEAN-TAVI Randomized Trial Martin B. Leon, MD Columbia University Medical Center Cardiovascular Research Foundation New York City
Carotid Artery Stent: Is it ready for prime time?
 2010 CATH LAB SYMPOSIUM Carotid Artery Stent: Is it ready for prime time? Luis F. Tami, MD, FACC, FSCAI Interventional Cardiology and Vascular Medicine Memorial Regional Hospital August 2010 CAE and CAS
2010 CATH LAB SYMPOSIUM Carotid Artery Stent: Is it ready for prime time? Luis F. Tami, MD, FACC, FSCAI Interventional Cardiology and Vascular Medicine Memorial Regional Hospital August 2010 CAE and CAS
Small in-stent Low Density on CT Angiography after Carotid Artery Stenting
 www.centauro.it Interventional Neuroradiology 14 (Suppl. 2): 41-46, 2008 Small in-stent Low Density on CT Angiography after Carotid Artery Stenting MIKA OKAHARA 1, HIRO KIYOSUE 2, JUNJI KASHIWAGI 1, SHINYA
www.centauro.it Interventional Neuroradiology 14 (Suppl. 2): 41-46, 2008 Small in-stent Low Density on CT Angiography after Carotid Artery Stenting MIKA OKAHARA 1, HIRO KIYOSUE 2, JUNJI KASHIWAGI 1, SHINYA
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Safety of Latest-Generation Self-expanding Stents in Patients With NASCET-Ineligible Severe Symptomatic Extracranial Internal Carotid Artery Stenosis Italo Linfante, MD; Joshua A.
ORIGINAL CONTRIBUTION Safety of Latest-Generation Self-expanding Stents in Patients With NASCET-Ineligible Severe Symptomatic Extracranial Internal Carotid Artery Stenosis Italo Linfante, MD; Joshua A.
Filters versus Occlusion Balloons during CAS Is there a clear preference?
 Washington TCT 2005 Filters versus Occlusion Balloons during CAS Is there a clear preference? K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany Presenter Disclosure Information
Washington TCT 2005 Filters versus Occlusion Balloons during CAS Is there a clear preference? K. Mathias Department of Radiology Teaching Hospital of Dortmund - Germany Presenter Disclosure Information
Tips and Tricks for CAS T-CAR
 Tips and Tricks for CAS T-CAR H.-H. Eckstein, M. Kallmayer Department for Vascular and Endovascular Surgery, Klinikum Rechts der Isar, Technical University of Munich,, Germany Disclosures Collaborator
Tips and Tricks for CAS T-CAR H.-H. Eckstein, M. Kallmayer Department for Vascular and Endovascular Surgery, Klinikum Rechts der Isar, Technical University of Munich,, Germany Disclosures Collaborator
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Carotid Artery Stenosis
 Evidence-Based Approach to Carotid Artery Stenosis Seong-Wook Park, MD Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea Carotid Artery Stenosis Carotid
Evidence-Based Approach to Carotid Artery Stenosis Seong-Wook Park, MD Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea Carotid Artery Stenosis Carotid
Surgical Treatment of Carotid Disease
 Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston Surgical Treatment of Carotid Disease The Old, the New, and the Future
Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston Surgical Treatment of Carotid Disease The Old, the New, and the Future
Contemporary management of brachiocephalic occlusive disease. TM Sullivan Minneapolis, MN
 Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Non Atheromatous Lesions Fibromuscular Dysplasia. Rod Samuelson, MD Babak Jahromi,, MD Elad Levy, MD Adnan Siddiqui,, PhD, MD Nick Hopkins, MD
 Non Atheromatous Lesions Fibromuscular Dysplasia Rod Samuelson, MD Babak Jahromi,, MD Elad Levy, MD Adnan Siddiqui,, PhD, MD Nick Hopkins, MD Presenter Disclosure Information L. Nelson Hopkins MD FINANCIAL
Non Atheromatous Lesions Fibromuscular Dysplasia Rod Samuelson, MD Babak Jahromi,, MD Elad Levy, MD Adnan Siddiqui,, PhD, MD Nick Hopkins, MD Presenter Disclosure Information L. Nelson Hopkins MD FINANCIAL
Challenges. 1. Sizing. 2. Proximal landing zone 3. Distal landing zone 4. Access vessels 5. Spinal cord ischemia 6. Endoleak
 Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
PrOspective multicenter study of carotid artery stenting Usinng mer Stent OCEANUS study!!!
 PrOspective multicenter study of carotid artery stenting Usinng mer Stent OCEANUS study!!! Prof Piotr Pieniazek MD PhD Jagiellonian University Institute of Cardiology, John Paul II Hospital Krakow, Poland
PrOspective multicenter study of carotid artery stenting Usinng mer Stent OCEANUS study!!! Prof Piotr Pieniazek MD PhD Jagiellonian University Institute of Cardiology, John Paul II Hospital Krakow, Poland
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
William A. Gray MD System Chief of Cardiovascular Services, Main Line Health President, Lankenau Heart Institute Wynnewood, PA USA
 William A. Gray MD System Chief of Cardiovascular Services, President, Wynnewood, PA USA What are the possible causes of stroke in CAS? Operator error Technique (balloon sizing, wire misadventure, EPD
William A. Gray MD System Chief of Cardiovascular Services, President, Wynnewood, PA USA What are the possible causes of stroke in CAS? Operator error Technique (balloon sizing, wire misadventure, EPD
CardioLucca2014. Fare luce sulla scelta ottimale del trattamento nella rivascolarizzazione delle stenosi carotidee. Fabrizio Tomai
 CardioLucca2014 Fare luce sulla scelta ottimale del trattamento nella rivascolarizzazione delle stenosi carotidee Fabrizio Tomai European Hospital e Aurelia Hospital Roma Treatment of Carotid Artery Disease
CardioLucca2014 Fare luce sulla scelta ottimale del trattamento nella rivascolarizzazione delle stenosi carotidee Fabrizio Tomai European Hospital e Aurelia Hospital Roma Treatment of Carotid Artery Disease
Carotid stenosis management: CAS or CEA? Yaoguo Yang, Chen Zhong Beijing Anzhen Hospital,China
 Carotid stenosis management: CAS or CEA? Yaoguo Yang, Chen Zhong Beijing Anzhen Hospital,China Disclosure Speaker name:... I have the following potential conflicts of interest to report: Consulting Employment
Carotid stenosis management: CAS or CEA? Yaoguo Yang, Chen Zhong Beijing Anzhen Hospital,China Disclosure Speaker name:... I have the following potential conflicts of interest to report: Consulting Employment
AN EXPERIENCE WITH ANGIOPLASTY AND STENTING OF CAROTID ARTERY STENOSIS WITH EMBOLIC PROTECTION DEVICES
 Arch Iranian Med 2006; 9 (2): 138 143 Original Article AN EXPERIENCE WITH ANGIOPLASTY AND STENTING OF CAROTID ARTERY STENOSIS WITH EMBOLIC PROTECTION DEVICES Ali-Mohammad Haji-Zeinali MD *, Davood Kazemi-Saleh
Arch Iranian Med 2006; 9 (2): 138 143 Original Article AN EXPERIENCE WITH ANGIOPLASTY AND STENTING OF CAROTID ARTERY STENOSIS WITH EMBOLIC PROTECTION DEVICES Ali-Mohammad Haji-Zeinali MD *, Davood Kazemi-Saleh
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E39-E41 A Case With Successful Retrograde Stent Delivery via AC Branch for Tortuous Right Coronary Artery Yoshiki Uehara, MD, PhD, Mitsuyuki Shimizu, MD, PhD,
Case Report J INVASIVE CARDIOL 2013;25(2):E39-E41 A Case With Successful Retrograde Stent Delivery via AC Branch for Tortuous Right Coronary Artery Yoshiki Uehara, MD, PhD, Mitsuyuki Shimizu, MD, PhD,
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous Internal Carotid Artery Dissections
 Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
(EU), FACC (USA), FSCAI (USA)
 How to reduce vascular complications of TAVI Paul TL Chiam MBBS (S pore), MMed, MRCP (UK), FAMS FRCP (Edin), FESC (EU), FACC (USA), FSCAI (USA) Cardiologist Mount Elizabeth Hospital Singapore Definition
How to reduce vascular complications of TAVI Paul TL Chiam MBBS (S pore), MMed, MRCP (UK), FAMS FRCP (Edin), FESC (EU), FACC (USA), FSCAI (USA) Cardiologist Mount Elizabeth Hospital Singapore Definition
Subclavian Revascularization. Douglas E. Drachman, MD, FSCAI Division of Cardiology Vascular Medicine Section December 9, 2014
 Subclavian Revascularization Douglas E. Drachman, MD, FSCAI Division of Cardiology Vascular Medicine Section December 9, 2014 Disclosure Information Douglas E. Drachman, MD, FACC Abbott Vascular, Inc.:
Subclavian Revascularization Douglas E. Drachman, MD, FSCAI Division of Cardiology Vascular Medicine Section December 9, 2014 Disclosure Information Douglas E. Drachman, MD, FACC Abbott Vascular, Inc.:
Contemporary Carotid Imaging and Approach to Treatment: Course Notes Thursday, June 22, 2017 David M. Pelz, MD, FRCPC
 CNSF Meeting, Victoria, BC. June 2017 Contemporary Carotid Imaging and Approach to Treatment: Course Notes Thursday, June 22, 2017 David M. Pelz, MD, FRCPC A. Objectives 1. To understand the current imaging
CNSF Meeting, Victoria, BC. June 2017 Contemporary Carotid Imaging and Approach to Treatment: Course Notes Thursday, June 22, 2017 David M. Pelz, MD, FRCPC A. Objectives 1. To understand the current imaging
Technique Of Carotid Stenting Decision Making Analysis To Overcome Challenges
 Technique Of Carotid Stenting Decision Making Analysis To Overcome Challenges Subbarao Myla MD FACC Hoag Memorial Hospital Presbyterian Newport Beach, CA USA Presenter Disclosure Information Name: Subbarao
Technique Of Carotid Stenting Decision Making Analysis To Overcome Challenges Subbarao Myla MD FACC Hoag Memorial Hospital Presbyterian Newport Beach, CA USA Presenter Disclosure Information Name: Subbarao
Roadsaver the paradigm shift in carotid artery treatment. G. Torsello Münster
 Roadsaver the paradigm shift in carotid artery treatment G. Torsello Münster Disclosure Speaker name:...g. Torsello... I have the following potential conflicts of interest to report: Consulting Employment
Roadsaver the paradigm shift in carotid artery treatment G. Torsello Münster Disclosure Speaker name:...g. Torsello... I have the following potential conflicts of interest to report: Consulting Employment
Advances in the treatment of posterior cerebral circulation symptomatic disease
 Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Tailored carotid artery stenting
 Tailored carotid artery stenting is associated with a low complication rate 30-day results from the continued TARGET-CAS study in 1133 consecutive procedures. Lukasz Tekieli, Piotr Pieniazek, Piotr Musialek,
Tailored carotid artery stenting is associated with a low complication rate 30-day results from the continued TARGET-CAS study in 1133 consecutive procedures. Lukasz Tekieli, Piotr Pieniazek, Piotr Musialek,
Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
 Case Reports in Vascular Medicine Volume 2013, Article ID 207602, 4 pages http://dx.doi.org/10.1155/2013/207602 Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
Case Reports in Vascular Medicine Volume 2013, Article ID 207602, 4 pages http://dx.doi.org/10.1155/2013/207602 Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
Percutaneous Intervention for totally Occluded Coarctation Of Aorta. John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology
 Percutaneous Intervention for totally Occluded Coarctation Of Aorta John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology Background Coarctation of aorta (CoA) forms 5-7% of congenital heart diseases
Percutaneous Intervention for totally Occluded Coarctation Of Aorta John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology Background Coarctation of aorta (CoA) forms 5-7% of congenital heart diseases
Appropriate Device Selection for Endovascular Procedures
 Appropriate Device Selection for Endovascular Procedures Thomas M. Shimshak, MD Florida Hospital Heartland Medical Center Sebring, Florida Disclosures Speaker s Bureau: Abbott Vascular Boston Scientific
Appropriate Device Selection for Endovascular Procedures Thomas M. Shimshak, MD Florida Hospital Heartland Medical Center Sebring, Florida Disclosures Speaker s Bureau: Abbott Vascular Boston Scientific
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Plaque Imaging: What It Can Tell Us. Kenneth Snyder, MD, PhD L Nelson Hopkins MD FACS Elad Levy MD MBA FAHA FACS Adnan Siddiqui MD PhD
 Plaque Imaging: What It Can Tell Us Kenneth Snyder, MD, PhD L Nelson Hopkins MD FACS Elad Levy MD MBA FAHA FACS Adnan Siddiqui MD PhD Buffalo Disclosure Information FINANCIAL DISCLOSURE: Research and consultant
Plaque Imaging: What It Can Tell Us Kenneth Snyder, MD, PhD L Nelson Hopkins MD FACS Elad Levy MD MBA FAHA FACS Adnan Siddiqui MD PhD Buffalo Disclosure Information FINANCIAL DISCLOSURE: Research and consultant
Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary
 SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
Carotid Stenosis (carotid artery disease)
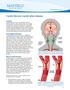 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
Octogenarians Must Be Treated With CAS
 Some Octogenarians Must Be Treated With CAS LN Hopkins, MD E Levy MD, Adnan Siddiqui,, MD, PhD Rod Samuelson MD J Mocco MD LN Hopkins, MD Potential Conflicts Consultant & research support: Boston Scientific,
Some Octogenarians Must Be Treated With CAS LN Hopkins, MD E Levy MD, Adnan Siddiqui,, MD, PhD Rod Samuelson MD J Mocco MD LN Hopkins, MD Potential Conflicts Consultant & research support: Boston Scientific,
2013 Coding Changes. Diagnostic Radiology. Nuclear Medicine
 2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
The learning curve associated with intracranial angioplasty and stenting: analysis from a single center
 Original Article Page 1 of 7 The learning curve associated with intracranial angioplasty and stenting: analysis from a single center Peiquan Zhou, Guang Zhang, Zhiyong Ji, Shancai Xu, Huaizhang Shi Department
Original Article Page 1 of 7 The learning curve associated with intracranial angioplasty and stenting: analysis from a single center Peiquan Zhou, Guang Zhang, Zhiyong Ji, Shancai Xu, Huaizhang Shi Department
Disclosures. State of the Art Management of Carotid Stenosis. NIH funding for clinical trials Consultant for Scientia Vascular and Medtronic
 State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
Stroke is the most common life-threatening neurologic disorder
 ORIGINAL RESEARCH EXTRACRANIAL VASCULAR Can Doppler Flow Parameters of Carotid Stenosis Predict the Occurrence of New Ischemic Brain Lesions Detected by Diffusion-Weighted MR Imaging after Filter-Protected
ORIGINAL RESEARCH EXTRACRANIAL VASCULAR Can Doppler Flow Parameters of Carotid Stenosis Predict the Occurrence of New Ischemic Brain Lesions Detected by Diffusion-Weighted MR Imaging after Filter-Protected
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Update on Carotid Disease
 Update on Carotid Disease L. Nelson Hopkins, MD Elad Levy, MD Adnan Siddiqui, MD,PhD Ken Snyder, MD,PhD Gates Vascular Institute LN Hopkins, MD I disclose the following financial relationship(s): President,
Update on Carotid Disease L. Nelson Hopkins, MD Elad Levy, MD Adnan Siddiqui, MD,PhD Ken Snyder, MD,PhD Gates Vascular Institute LN Hopkins, MD I disclose the following financial relationship(s): President,
