Endovascular Treatment of Gastrointestinal Bleeding
|
|
|
- Bethany Briggs
- 5 years ago
- Views:
Transcription
1 Health Topics for Tokyoites Juntendo Medical Journal (3), Endovascular Treatment of Gastrointestinal Bleeding AKIHIKO SHIRAISHI * *Department of Radiology, Juntendo University Faculty of Medicine, Tokyo, Japan Acute gastrointestinal (GI) bleeding is a common medical emergency that varies from minor to potentially life-threatening bleeding. Endoscopy is a first-line diagnostic procedure for both upper and lower GI bleeding. Therapeutic options for the treatment of acute GI bleeding include conservative management, therapeutic endoscopy, transcatheter embolization, and surgery. Transcatheter embolization and surgery are both options for recurrent GI bleeding when therapeutic endoscopy fails; however, both options are associated with several complications and the risk of rebleeding. The choice of management depends upon the status of the patient. Emergency surgery is typically associated with high rates of morbidity and death. Recently, superselective transcatheter embolization has become a safer procedure and is now widely used for the management of acute GI bleeding. This review article describes the role of interventional radiology in the management of acute GI bleeding. Key words: endovascular treatment, transarterial embolization, GI bleeding Introduction Acute gastrointestinal (GI) bleeding is a common medical emergency that varies from minor, self-limited bleeding to potentially life-threatening bleeding 1). The bleeding site can be located anywhere along the GI tract, making determination of its precise location challenging. Patients with upper GI bleeding usually present with hematemesis or melena and the bleeding point is proximal to the ligament of Treitz, whereas those with lower GI bleeding usually present with melena or hematochezia and the bleeding point is distal to the ligament of Treitz. Endoscopy is a first-line diagnostic procedure with 100% sensitivity for diagnosing upper GI bleeding; however, it has only 60% sensitivity for diagnosing lower GI bleeding. Therapeutic options for the treatment of acute GI bleeding include conservative management, therapeutic endoscopy, transcatheter embolization, and surgery 2) 3). Transcatheter embolization and surgery are both options for recurrent GI bleeding when therapeutic endoscopy fails; however, both options are associated with several complications and the risk of rebleeding. The choice of management depends upon the status of the patient (e.g., the degree of hemodynamic instability or hypotension, or whether there is a need for resuscitation). Emergency surgery is typically associated with high rates of morbidity and death 4)-6). However, recent technical improvements in superselective transcatheter embolization have increased the procedureʼs safety and it is now widely used for the management of acute GI bleeding 7). This review article describes role of interventional radiology in the emergent management of acute GI bleeding. Upper GI bleeding Upper GI bleeding is defined as bleeding originating from the distal esophagus, the stomach, or the duodenum (i.e., proximal to the ligament of Treitz). The most common cause of upper GI bleeding is peptic ulcer disease, but the differential diagnosis is diverse and includes benign and malignant tumors, ischemia, gastritis, arteriovenous malformations, Akihiko Shiraishi Department of Radiology, Juntendo University Faculty of Medicine Hongo, Bunkyo-ku, Tokyo , Japan TEL: asiraisi@juntendo.ac.jp 35th Health Topics for Tokyoites: The Cutting Edge of Intravascular Treatment Held on Feb. 21, 2015 Received Mar. 17,
2 Juntendo Medical Journal 61 (3), 2015 Mallory-Weiss tears, trauma such as Dieulafoyʼs lesion, and iatrogenic causes. Upper GI bleeding is a potentially fatal condition, so immediate management and accurate diagnosis of both the location and etiology of the bleed is necessary. The primary diagnostic procedure for upper GI bleeding is endoscopy, which has high sensitivity and specificity for locating and identifying bleeding lesions in the upper GI tract. Once a bleeding lesion has been identified, therapeutic endoscopy techniques such as thermal coagulation or hemoclip placement can be used to achieve acute hemostasis. Endoscopic management achieves hemostasis in the majority of patients, but 10% to 30% of patients experience rebleeding, for a variety of reasons 8) 9). When hemostasis is not achieved with endoscopic management, other options include surgery and transarterial embolization. Surgery has long been the standard of care, but with the development of interventional radiology, an increasing number of patients are now referred for embolotherapy 10). Transarterial embolization may prevent unnecessary resection of the upper GI tract and should be considered as an alternative to surgery. Lower GI bleeding Lower GI bleeding is defined as bleeding originating from a source distal to the ligament of Treitz. Approximately 80% of all lower GI bleeding comes from a colorectal source and 5% to 10% from a small bowel source; 10% to 15% is classed as blood of upper GI tract origin. The source of small bowel bleeding is more likely than that of colorectal bleeding to be obscure or occult 11) 12). The most common cause of lower GI bleeding is colonic diverticula. The differential diagnosis includes colitis or enteritis, anorectal anomalies (hemorrhoids, proctitis), tumors, arteriovenous malformation or angiodysplasia, and post-polypectomy bleeding. Therapeutic colonoscopy is currently a first-line intervention for colonic bleeding. Colonoscopy is the diagnostic modality of choice in patients with lower GI bleeding, but therapeutic endoscopy may also be successful in a limited number of patients 13)-17). Therapeutic colonoscopy fails in approximately 32% of cases because of the presence of stool or blood clots, or because of technical difficulties such as the time required to prepare patients 18). Further disadvantages include the fact that small bowel bleeding cannot be accessed via colonoscopy 19) and that colonoscopy is relatively ineffective when performed without bowel preparation in patients with marked bleeding 20) 21). If the bleeding cannot be stopped with therapeutic colonoscopy, transarterial embolization is the next line of therapy for controlling hemostasis. As with upper GI bleeding, transarterial embolization is now a first-line therapy for patients with severe lower GI bleeding 22). The efficacy of transarterial embolization in treating acute GI bleeding when medical or endoscopic techniques are insufficient has been shown in several large studies 23) 24). In both upper and lower GI bleeding, surgery is now typically reserved as a last-line treatment for patients whose bleeding has failed to respond to previous treatments. Angiography and embolization In angiography, access to the blood vessels is usually gained via transfemoral catheterization with a 4- or 5-Fr catheter and sheath. Diagnostic visceral arteriography, which consists of angiography of the celiac trunk, superior mesenteric artery, and inferior mesenteric artery, is performed to investigate a suspicious vascular region, and a microcatheter is then inserted coaxially for superselective cannulation of the bleeding artery. In upper GI bleeding, the source of the bleeding is usually identified by means of endoscopy. Therefore, angiography is most often performed only as a precursor to transcatheter embolotherapy. Angiograms are considered positive when they show either a direct angiographic sign of active GI bleeding (i.e., extravasation of contrast medium) or an indirect angiographic sign of bleeding (e. g., pseudoaneurysm). For embolization, an appropriate catheter position is selected, and transcatheter vessel occlusion is performed with an embolic material. Embolizations are performed as selectively as possible, with the catheter advanced as close to the site of bleeding as technically feasible. The aim is to achieve proximal and distal control of the bleeding lesion (embolization of both the inflow and outflow vessels) to minimize the risk of 243
3 Shiraishi: Endovascular treatment of gastrointestinal bleeding level of the gastroduodenal artery with the catheter pushed to the origin of the right gastroepiploic artery, and coils are introduced into the proximal gastroduodenal artery as the catheter is withdrawn. Complete embolization of the gastroduodenal artery, which includes proximal and distal embolization and exclusion of its two side branches, is the technical endpoint. Selective superior mesenteric arteriography is performed after embolization to ensure the absence of a collateral supply to the bleeding site. If extravasation is identified, superselective catheterization of the inferior pancreaticoduodenal artery and the side branch responsible for the collateral circulation is performed with a microcatheter. In the past 10 years, significant improvements in this technique have made superselective embolization a safer procedure by minimizing the risk of intestinal ischemia 26) 27). recurrent bleeding via the collateral circulation. Embolization is continued to an occlusive angiographic endpoint with no antegrade arterial blood flow in the embolized artery. Post-embolization arteriography is performed to confirm completion of the procedure. The most common embolic material used to treat upper GI bleeding is the fibered platinum microcoil, which is usually placed in the bleeding artery in a distal-to-proximal manner until angiographic extravasation of contrast medium ceases and there is complete occlusion of the bleeding vessel. Coiling the gastroduodenal artery from the celiac axis may be inadequate, as the gastroduodenal artery can then be fed via collateral branches from the superior mesenteric artery. A sandwich technique (Figure-1) has been proposed 25) in which the gastroduodenal artery is coiled in a distal-to-proximal manner. Sandwich occlusion can be used at the A C B D Figure-1 Sandwich embolization of duodenal diverticular bleeding A. Three-dimensional computed tomography (3D-CT) (volume-rendered image) demonstrating the anatomic structure of the abdomen. B. 3D-CT (multiplanar-reconstruction image) showing a branch of the pancreaticoduodenal artery projecting toward the duodenal diverticulum (arrow). C. Selective posterior-superior pancreaticoduodenal angiogram showing no active extravasation of contrast medium. D. Result of empiric coil embolization of the distal and proximal posterior-superior pancreaticoduodenal artery to prevent retrograde flow. Bleeding was controlled after embolization and no ischemic complications were observed. 244
4 Juntendo Medical Journal 61 (3), 2015 The development of finer torqueable guidewires and coaxial microcatheters, coupled with advances in digital fluoroscopic imaging, now allows for more precise vascular intervention. In a recent report, transarterial embolization for upper GI bleeding was associated with a high rate (93%) of technical success and a minimal rate of complications (9%) 25). Furthermore, a recently published international consensus recommendation considers transarterial embolization an alternative therapy for the management of upper GI bleeding in patients in whom an endoscopic hemostatic procedure has failed or in those with recurrent bleeding 28). Transarterial embolization for the treatment of lower GI bleeding was first introduced in 1974 and involved non-selective injection of autologous clot 29). In 1977, injection of Gelfoam and Oxycel was described for embolization of diverticular bleeding. Although the injection of autologous clot or gelatin sponge showed promise for achieving hemostasis, these early embolization techniques were characterized by high rates of bowel infarction 30) 31). The development of coaxial microcatheters renewed interest in using embolization to control lower GI bleeding. Using a microcatheter delivered through a 4- or 5-Fr guiding catheter, specific marginal arteries or the vasa recta near the bleeding site can be accessed for delivery of an embolic material. As this technique is superselective, the risk of bowel infarction is markedly lower than with non-selective embolic techniques or vasopressin infusion, and there is none of the systemic side effects associated with vasopressin. In addition, there is decreased risk of bleeding from collateral vessels when the embolic material is delivered close to the bleeding site 30). The most common embolic materials for lower GI bleeding, used either alone or in combination, are microcoils, polyvinyl alcohol (PVA) particles, and gelatin sponge. Microcoils are permanent embolic agents that can be placed superselectively near the site of bleeding and are readily identifiable under fluoroscopy. However, because of the small caliber of the target vessels, proper deployment of these coils can be challenging. Coils may back out of small vessels and provoke ischemia if they enter larger feeding vessels. PVA is a permanent embolic agent that is less selective than microcoils. The rationale behind flow-directed PVA embolization is that the PVA particles preferentially flow to the area of least resistance (i.e., the site of bleeding) 32). Defreyne et al. have demonstrated in 10 patients that lesions not accessible with superselective catheterization can be embolized safely with flow-directed PVA embolization 32). However, consensus on the optimal size of PVA particles for embolization in lower GI bleeding is yet to be reached. Previous reports have recommended PVA particles 300 to 500 μm in size, because an earlier animal study suggested that smaller particles may be associated with a higher risk of bowel ischemia 30) 33). B A Figure-2 Superselective embolization of colonic diverticular bleeding A. Radiopaque clips were placed via colonoscopy at the bleeding point on the distal portion of the ascending colon before angiography. Selective ileocolic artery angiogram showing intraluminal extravasation of contrast medium in the ascending colon (arrow). B. After superselective embolization of the vasa recta with gelatin sponge particles, no extravasation or bleeding was seen on angiography. 245
5 Shiraishi: Endovascular treatment of gastrointestinal bleeding The choice of embolic agent in relation to the characteristics of the bleeding vessel is important, but which embolic agent is best among coils, cyanoacrylate glue, gelatin sponge, and calibrated particles remains a matter of debate. In our department, microcoils, 1,000-μm gelatin sponge particles, and cyanoacrylate glue are used to treat acute GI bleeding. In contrast to PVA, gelatin sponge is a temporary embolic agent, allowing for vessel recanalization within a few days to weeks. A representative image of gelatin sponge embolization of colonic diverticular bleeding is shown in Figure-2. If the angiogram is negative for active bleeding, empiric embolization is performed on the basis of discussions with the referring gastroenterologist or surgeon (Figure-1). For empiric embolization, if endoscopy has demonstrated that the source of bleeding is located in the proximal stomach, the left gastric artery is selectively embolized. If endoscopy has demonstrated that the source of bleeding is in the distal stomach or duodenum, the gastroduodenal artery, right gastroepiploic artery, pancreaticoduodenal arcade, or all three, are selectively embolized. If endoscopic intervention fails to control the bleeding, radiopaque clips are positioned as a guide at the bleeding site by means of colonoscopy and transarterial embolization is performed to stop the bleeding, with deposition of the coils being guided by hemoclips placed beforehand by means of endoscopy. As a result, angiography and embolization of causative vessels in GI bleeding have been gradually accepted, and this has transformed the management of lower GI bleeding. Complications associated with endovascular treatment Complications associated with embolization include those associated with the angiography itself (e. g., hematoma, arterial thrombosis, dissection, embolism, pseudoaneurysm), as well as bowel infarction. Early transcatheter interventions involved vasopressin infusion, but a high rate of rebleeding and a high incidence of complications led to a reduction in its use. Higher rates of complication and rebleeding have been reported in patients treated with vasopressin 34). Although the first embolic techniques improved hemostasis, their utility was limited by a high incidence of bowel infarction 35)-37). It was not until the advent and development of microcatheter technology that transarterial embolization became a safe, more effective method for the management of GI bleeding. Improvements in microcatheter systems have allowed more selective delivery of embolic material closer to bleeding sites; this has bypassed the systemic side effects of vasopressin and led to lower risks of bowel infarction and bleeding from the collateral vessels. Recently, many reports have suggested that superselective embolization for the management of GI bleeding rapidly stops bleeding with minimal risk of ischemia 20) 21) 27) 38)-49). However, the risk of ischemia after embolization is increased in patients with a history of surgery within the same area 50) or when the therapeutic intervention involves embolic agents that can advance far into the vascular bed. Such agents include liquids (e. g., tissue adhesives such as cyanoacrylate) or very small particles (e.g., gelatin sponge powder or calibrated microspheres) 50)-53). Multi-detector row computed tomography In stable patients, multi-detector row computed tomography (MDCT) imaging is a useful tool for locating bleeding sites and evaluating the anatomic structure of the GI tract, thereby enabling more focused intervention. Technetium-99m red blood cell scintigraphy has a sensitivity and specificity of more than 90%; however, its limited resolution does not allow precise diagnosis. Computed tomography angiography (CTA) has also been used (sensitivity up to 86%) in the diagnosis of acute GI bleeding and can be used to precisely determine the location and etiology of the bleeding, and thereby direct further management 54). A positive MDCT angiogram can be useful to select appropriate patients for rapid targeted embolization. Visualization of active extravasation of contrast medium in the GI tract requires careful attention to technique, including the use of thin collimation, rapid contrast-medium administration, and appropriate scan timing. The additional use of multiplanar reconstructions and three-dimensional imaging is beneficial in identifying the exact source 246
6 Juntendo Medical Journal 61 (3), 2015 of the bleeding. Although further studies are needed to address which course of action is best when bowel preparation cannot be performed, CTA may be useful in this situation for identifying the bleeding site 55). Conclusion Improvements in catheter technology, the development of more compatible embolization agents, and the expansion of embolization techniques have resulted in the increased use of angiography and embolization for the treatment of both upper and lower GI bleeding. Transcatheter embolization therapy for the treatment of acute GI bleeding is a safe procedure with high rates of technical and clinical success, but it should be reserved as a treatment option for patients who have failed endoscopic and medical management. MDCT imaging is a useful tool for identifying the bleeding site and evaluating the anatomic structure of the GI tract in stable patients. Close working relationships among interventional radiologists, gastroenterologists, and diagnostic radiologists are necessary for optimal management of patients with GI bleeding. References 1) Charbonnet P, Toman J, Buhler L, et al: Treatment of gastrointestinal hemorrhage. Abdom Imaging, 2005; 30: ) Cherian MP, Mehta P, Kalyanpur TM, Hedgire SS, Narsinghpura KS: Arterial interventions in gastrointestinal bleeding. Semin Intervent Radiol, 2009; 26: ) Sheth R, Someshwar V, Warawdekar G: Treatment of acute lower gastrointestinal hemorrhage by superselective transcatheter embolization. Indian J Gastroenterol, 2006; 25: ) Rozycki GS, Tremblay L, Feliciano DV, et al: Three hundred consecutive emergent celiotomies in general surgery patients. Ann Surg, 2002; 235: ) Pennoyer WP, Vignati PV, Cohen JL: Management of angiogram positive lower gastrointestinal hemorrhage: long term follow-up of non-operative treatments. Int J Colorectal Dis, 1996; 11: ) Schuetz A, Jauch KW: Lower gastrointestinal bleeding: therapeutic strategies, surgical techniques and results. Langenbecks Arch Surg, 2001; 386: ) Mirsadraee S, Tirukonda P, Nicholson A, Everett SM, McPherson SJ: Embolization for non-variceal upper gastrointestinal tract haemorrhage: a systematic review. Clin Radiol, 2011; 66: ) Bjorkman DJ, Zaman A, Fennerty MB, Lieberman D, Disario JA, Guest-Warnick G: Urgent vs. elective endoscopy for acute non-variceal upper GI-bleeding: an effectiveness study. Gastrointest Endosc, 2004; 60: ) Church NI, Palmer KR: Diagnostic and therapeutic endoscopy. Curr Opin Gastroenterol, 1999; 15: ) Yap FY, Omene BO, Patel MN, et al: Transcatheter embolotherapy for gastrointestinal bleeding: a single center review of safety, efficacy, and clinical outcomes. Dig Dis Sci, 2013; 58: ) DeBarros J, Rosas L, Cohen J, Vignati P, Sardella W, Hallisey M: The changing paradigm for the treatment of colonic hemorrhage: superselective angiographic embolization. Dis Colon Rectum, 2002; 45: ) Lewis BS: Small intestinal bleeding. Gastroenterol Clin North Am, 1994; 23: ) Jenson DM, Machicado GA, Jutabha R, Kovacs TO: Urgentcolonoscopy for the diagnosis and treatment of severe diverticular hemorrhage. N Engl J Med, 2000; 342: ) Zuccaro G: Management of the adult patient with acute lower gastrointestinal bleeding. Am J Gastroenterol, 1998; 93: ) Angtuaco TL, Reddy SK, Drapkin S, Harrell LE, Howden CW: The utility of urgent colonoscopy in the evaluation of acute lower gastrointestinal tract bleeding: a 2-year experience from a single center. Am J Gastroenterol, 2001; 96: ) Bloomfield RD, Rockey DC, Shetzline MA: Endoscopic therapy of acute diverticular hemorrhage. Am J Gastroenterol, 2001; 96: ) Eisen GM, Dominitz JA, Faigel D, et al; American Society for Gastrointestinal Endoscopy. Standards of Practice Committee: an annotated algorithmic approach to acute lower gastrointestinal bleeding. Gastrointest Endosc, 2001; 53: ) Zuckerman GR, Prakash C: Acute lower intestinal bleeding. Part I: clinical presentation and diagnosis. Gastrointest Endosc, 1998; 48: ) Fisher L, Krinsky ML, Anderson MA, et al: The role of endoscopy in the management of obscure GI bleeding. Gastrointestinal Endoscopy, 2010; 72: ) Funaki B, Kostelic JK, Lorenz J, et al: Superselective microcoil embolization of colonic hemorrhage. Am J Roentgenol, 2001; 177: ) Funaki B: Superselective embolization of lower gastrointestinal hemorrhage: a new paradigm. Abdom Imaging, 2004; 29: ) Barkun AN, Bardou M, Kuipers EJ, et al: International consensus recommendations on the management of patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med, 2010; 152: ) Weldon DT, Burke SJ, Sun S, Mimura H, Golzarian J: Interventional management of lower gastrointestinal bleeding. Eur Radiol, 2008; 18: ) Mirsadraee S, Tirukonda P, Nicholson A, Everett SM, McPherson SJ: Embolization for non-variceal upper gastrointestinal tract haemorrhage: a systematic review. Clin Radiol, 2011; 66: ) Loffroy R, Rao P, Ota S, De Lin M, Kwak BK, Geschwind JF: Embolization of acute nonvariceal upper gastrointestinal hemorrhage resistant to endoscopic treatment results and predictors of recurrent bleeding. Cardiovasc Intervent Radiol, 2010; 33: ) Nussbaum M, Baum S, Blakemore W, Finkelstein A: Demonstration of intra-abdominal bleeding by selective arteriography. J Am Med Assoc, 1965; 191:
7 Shiraishi: Endovascular treatment of gastrointestinal bleeding 27) Luchtefeld MA, Senagore AJ, Szomstein M, Fedeson B, Van Erp J, Rupp S: Evaluation of transarterial embolization for lower gastrointestinal bleeding. Dis Colon Rectum, 2000; 43: ) Angle JF, Siddiqi NH, Wallace MJ, et al: Quality improvement guidelines for percutaneous transcatheter embolization: society of interventional radiology standards of practice committee. J Vasc IntervRadiol, 2010; 21: ) Bookstein JJ, Chlosta EM, Foley D, Walter JF: Trancatheter hemostasis of gastrointestinal bleeding using modified autologouos clot. Radiology, 1974; 113: ) Darcy M: Embolization for lower GI bleeding. In: Golzarian J, et al, eds. Vascular Embolotherapy. Berlin, Heidelberg, New York: Springer, 2006: ) Darcy M: Treatment of lower gastrointestinal bleeding: vasopressin infusion versus embolization. J Vasc Interv Radiol, 2003; 14: ) Defreyne L, Vanlangenhove P, De Vos M, et al: Embolization as a first approach with endoscopically unmanageable acute nonvariceal gastrointestinal hemorrhage. Radiology, 2001; 218: ) Kusano S, Murata K, Ohuchi H, Motohashi O, Atari H: Low-dose particulate polyvinyl alcohol embolization in massive small artery intestinal hemorrhage: experimental and clinical results. Invest Radiol, 1987; 22: ) Miller M Jr, Smith TP: Angiographic diagnosis and endovascular management of nonvariceal gastrointestinal hemorrhage. Gastroenterol Clin North Am, 2005; 34: ) Belaiche J, Louis E, Dʼ Haens G, et al: Acute lower gastrointestinal bleeding in Crohnʼs disease: characteristics of a unique series of 34 patients. Am J Gastroenterol, 1999; 94: ) Robert JH, Sachar DB, Aufses AH: Management of severe hemorrhage in ulcerative colitis. Am J Surg, 1990; 159: ) Zuckerman GR, Prakash C: Acute lower gastrointestinal bleeding: etiology, therapy and outcomes. Gastrointest Endosc, 1999; 49: ) Ledermann HP, Schoch E, Jost R, Zollikofer CL: Embolization of the vasa recta in acute lower gastrointestinal hemorrhage: a report of five cases. Cardiovasc Intervent Radiol, 1999; 22: ) Gordon RL, Ahl KL, Kerlan RK, et al: Selective arterial embolization for the control of lower gastrointestinal bleeding. Am J Surg, 1997; 174: ) Nicholson AA, Ettles DF, Hartley JE, et al: Transcatheter coil embolotherapy: a safe and effective option for major colonic hemorrhage. Gut, 1998; 43: ) Bandi R, Shetty PC, Sharma RP, Burke TH, Burke MW, Kastan D: Superselective arterial embolization for the treatment of lower gastrointestinal hemorrhage. J Vasc IntervRadiol, 2001; 12: ) DeBarros J, Rosas L, Cohen J, Vignati P, Sardella W, Hallisey M: The changing paradigm for the treatment of colonic hemorrhage. Dis Colon Rectum, 2002; 45: ) Gady CJ, Reynolds CH, Blum A: Selective arterial embolization for control of lower gastrointestinal bleeding: recommendations for a clinical management pathway. Curr Surg, 2003; 60: ) Kuo WT, Lee DE, Saad WE, Patel N, Sahler LG, Waldman DL: Superselective microcoil embolization for the treatment of lower gastrointestinal hemorrhage. J Vasc IntervRadiol, 2003; 14: ) dʼothee BJ, Surapaneni P, Rabkin D, Nasser I, Clouse M: Microcoil embolization for acute lower gastrointestinal bleeding. Cardiovasc Intervent Radiol, 2006; 29: ) Ahmed TM, Cowley JB, Robinson G, et al: Long term follow-up of transcatheter coil embolotherapy for major colonic hemorrhage. Colorectal Dis, 2010; 12: ) Mensel B, Kuhn JP, Kraft M, et al: Selective microcoil embolization of arterial gastrointestinal bleeding in the acute situation: outcome, complications, and factors affecting treatment success. Eur J Gastroenterol Hepatol, 2012; 24: ) Teng HC, Liang HL, Lin YH, et al: The efficacy and long-term outcome of microcoil embolotherapy for acute lower gastrointestinal bleeding. Korean J Radiol, 2013; 14: ) Adusumilli S, Gosselink MP, Ctercteko G, et al: The efficacy of selective arterial embolization in the management of colonic bleeding. Tech Coloproctol, 2014; 18: ) Shapiro N, Brandt L, Sprayregan S, Mitsudo S, Glotzer P: Duodenal infarction after therapeutic Gelfoam embolization of a bleeding duodenal ulcer. Gastroenterology, 1981; 80: ) Rosch J, Keller FS, Kozak B, Niles N, Dotter CT: Gelfoam powder embolization of the left gastric artery in treatment of massive small-vessel gastric bleeding. Radiology, 1984; 151: ) Walsh RM, Anain P, Geisinger M, et al: Role of angiography and embolization for massive gastroduodenal hemorrhage. J Gastrointest Surg, 1999; 3: ) Loffroy R, Guiu B, Cercueil JP, Krausé D: Endovascular therapeutic embolisation: an overview of occluding agents and their effects on embolised tissues. Curr Vasc Pharmacol, 2009; 7: ) Chua AE, Ridley LJ: Diagnostic accuracy of CT angiography in acute gastrointestinal bleeding. J Med Imaging Radiat Oncol, 2008, 52: ) Duchat F, Soyer P, Boudiaf M, et al: Multi-detector row CT of patients with acute intestinal bleeding: a new perspective using multiplanar and MIP reformations from submillimeter isotropic voxels. Abdom Imaging, 2010; 35:
Superselective Microcoil Embolization of Colonic Hemorrhage
 Brian Funaki 1 Jonathan K. Kostelic 2 Jonathan Lorenz 1 Thuong Van Ha 1 Doris L. Yip 1 Jordan D. Rosenblum 1 Jeffrey A. Leef 1 Christopher Straus 1 George X. Zaleski 3 Received January 24, 2001; accepted
Brian Funaki 1 Jonathan K. Kostelic 2 Jonathan Lorenz 1 Thuong Van Ha 1 Doris L. Yip 1 Jordan D. Rosenblum 1 Jeffrey A. Leef 1 Christopher Straus 1 George X. Zaleski 3 Received January 24, 2001; accepted
Refractory Bleeding: Role of Angiographic Intervention
 Session III UGS-III: Endoscopic Hemostasis for Nonvariceal Bleeding Refractory Bleeding: Role of Angiographic Intervention Ji Hoon Shin, M.D. Department of Radiology, Asan Medical Center, University of
Session III UGS-III: Endoscopic Hemostasis for Nonvariceal Bleeding Refractory Bleeding: Role of Angiographic Intervention Ji Hoon Shin, M.D. Department of Radiology, Asan Medical Center, University of
Superselective Embolization for Lower Gastrointestinal Hemorrhage: An Institutional Review Over 7 Years
 World J Surg (2008) 32:2707 275 DOI 0.007/s00268-008-9759-6 Superselective Embolization for Lower Gastrointestinal Hemorrhage: An Institutional Review Over 7 Years Ker-Kan Tan Æ Daniel Wong Æ Richard Sim
World J Surg (2008) 32:2707 275 DOI 0.007/s00268-008-9759-6 Superselective Embolization for Lower Gastrointestinal Hemorrhage: An Institutional Review Over 7 Years Ker-Kan Tan Æ Daniel Wong Æ Richard Sim
Role of radiology in colo-rectal bleedings. Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE
 Role of radiology in colo-rectal bleedings Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE Epidemiology Lower GI bleeding accounts for 20-25% of all GI bleeding Annual incidence in USA :21-27/100000 Longstreth
Role of radiology in colo-rectal bleedings Alban DENYS MD FCIRSE EBIR CHUV LAUSANNE Epidemiology Lower GI bleeding accounts for 20-25% of all GI bleeding Annual incidence in USA :21-27/100000 Longstreth
Percutaneous Transarterial Embolization of Pseudoaneurysm Secondary to Pancreatitis: a case report
 Chin J Radiol 2003; 28: 347-351 347 Percutaneous Transarterial Embolization of Pseudoaneurysm Secondary to Pancreatitis: a case report HSIN-YI LAI YUNG-FANG CHEN HSEIN-JAR CHIANG WU-CHUNG SHEN Department
Chin J Radiol 2003; 28: 347-351 347 Percutaneous Transarterial Embolization of Pseudoaneurysm Secondary to Pancreatitis: a case report HSIN-YI LAI YUNG-FANG CHEN HSEIN-JAR CHIANG WU-CHUNG SHEN Department
Gastro-Intestinal Bleeding- Interventional Radiology turning off the tap. Simon McPherson, Vascular Interventional Radiologist, Leeds
 Gastro-Intestinal Bleeding- Interventional Radiology turning off the tap Simon McPherson, Vascular Interventional Radiologist, Leeds Scale UK 100,000 /year Commonest Vascular IR on-call 75% UGIB 65% NVUGIB
Gastro-Intestinal Bleeding- Interventional Radiology turning off the tap Simon McPherson, Vascular Interventional Radiologist, Leeds Scale UK 100,000 /year Commonest Vascular IR on-call 75% UGIB 65% NVUGIB
The Efficacy and Long-Term Outcome of Microcoil Embolotherapy for Acute Lower Gastrointestinal Bleeding
 Original Article Intervention http://dx.doi.org/10.3348/kjr.2013.14.2.259 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2013;14(2):259-268 The Efficacy and Long-Term Outcome of Microcoil Embolotherapy
Original Article Intervention http://dx.doi.org/10.3348/kjr.2013.14.2.259 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2013;14(2):259-268 The Efficacy and Long-Term Outcome of Microcoil Embolotherapy
Definitive Surgical Treatment When Endoscopy Fails. Erik Peltz D.O. Resident Debate February 26 th 2007 University of Colorado Dept.
 Nonvariceal Gastrointestinal Hemorrhage: Definitive Surgical Treatment When Endoscopy Fails Erik Peltz D.O. Resident Debate February 26 th 2007 University of Colorado Dept. Surgery Non-Variceal Upper GI
Nonvariceal Gastrointestinal Hemorrhage: Definitive Surgical Treatment When Endoscopy Fails Erik Peltz D.O. Resident Debate February 26 th 2007 University of Colorado Dept. Surgery Non-Variceal Upper GI
Imaging of upper and lower gastrointestinal bleeding: An update for the radiologist
 Imaging of upper and lower gastrointestinal bleeding: An update for the radiologist Poster No.: C-3149 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular Authors: S. Leong, H. Sara, F. Oisin,
Imaging of upper and lower gastrointestinal bleeding: An update for the radiologist Poster No.: C-3149 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular Authors: S. Leong, H. Sara, F. Oisin,
GEST 2016: Case-Based Discussion: GI Bleeding of Arterial Origin
 GEST 2016: Case-Based Discussion: GI Bleeding of Arterial Origin Presented by: Mubin I. Syed, MD, FACR, FSIR Clinical Associate Professor of the Radiological Sciences Wright State University School of
GEST 2016: Case-Based Discussion: GI Bleeding of Arterial Origin Presented by: Mubin I. Syed, MD, FACR, FSIR Clinical Associate Professor of the Radiological Sciences Wright State University School of
6 Embolization for Lower GI Bleeding
 Embolization for Lower GI Bleeding 73 6 Embolization for Lower GI Bleeding Michael Darcy CONTENTS 6.1 Introduction 73 6.2 Physiopathology 73 6.2.1 Underlying Principles 73 6.2.2 Type of Lesion 74 6.3 Clinical
Embolization for Lower GI Bleeding 73 6 Embolization for Lower GI Bleeding Michael Darcy CONTENTS 6.1 Introduction 73 6.2 Physiopathology 73 6.2.1 Underlying Principles 73 6.2.2 Type of Lesion 74 6.3 Clinical
When to Scope in Lower GI Bleeding: It Must Be Done Now. Lisa L. Strate, MD, MPH Assistant Professor of Medicine University of Washington, Seattle, WA
 When to Scope in Lower GI Bleeding: It Must Be Done Now Lisa L. Strate, MD, MPH Assistant Professor of Medicine University of Washington, Seattle, WA Outline Epidemiology Overview of available tests Urgent
When to Scope in Lower GI Bleeding: It Must Be Done Now Lisa L. Strate, MD, MPH Assistant Professor of Medicine University of Washington, Seattle, WA Outline Epidemiology Overview of available tests Urgent
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Management of Lower Gastrointestinal Bleeding. Patrick Lau Department of Surgery Kwong Wah Hospital
 Management of Lower Gastrointestinal Bleeding Patrick Lau Department of Surgery Kwong Wah Hospital Lower Gastrointestinal bleeding The challenge Account for 20% of gastrointestinal bleeding 80% stopped
Management of Lower Gastrointestinal Bleeding Patrick Lau Department of Surgery Kwong Wah Hospital Lower Gastrointestinal bleeding The challenge Account for 20% of gastrointestinal bleeding 80% stopped
Angiographically Negative Acute Arterial Upper and Lower Gastrointestinal Bleeding: Incidence, Predictive Factors, and Clinical Outcomes
 Angiographically Negative Acute Arterial Upper and Lower Gastrointestinal Bleeding: Incidence, Predictive Factors, and Clinical Outcomes Jin Hyoung Kim, MD 1 Ji Hoon Shin, MD 1 Hyun-Ki Yoon, MD 1 Eun Young
Angiographically Negative Acute Arterial Upper and Lower Gastrointestinal Bleeding: Incidence, Predictive Factors, and Clinical Outcomes Jin Hyoung Kim, MD 1 Ji Hoon Shin, MD 1 Hyun-Ki Yoon, MD 1 Eun Young
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Lower GI bleeding. Aliu Sanni, MD Long Island College Hospital 17 th June, 2010
 Lower GI bleeding Aliu Sanni, MD Long Island College Hospital 17 th June, 2010 Case Presentation CC: Hematochezia HPI: 28yr old male presents with 1 day episode of bloody stools. Denies any abdominal pain.
Lower GI bleeding Aliu Sanni, MD Long Island College Hospital 17 th June, 2010 Case Presentation CC: Hematochezia HPI: 28yr old male presents with 1 day episode of bloody stools. Denies any abdominal pain.
Lower GI bleeding Management DR EHSANI PROFESSOR IN GASTROENTEROLOGY AND HEPATOLOGY
 Lower GI bleeding Management DR EHSANI PROFESSOR IN GASTROENTEROLOGY AND HEPATOLOGY 15 FEB 2018 Sources Sources Sources Initial evaluation History Physical examination Laboratory evaluation Obtained at
Lower GI bleeding Management DR EHSANI PROFESSOR IN GASTROENTEROLOGY AND HEPATOLOGY 15 FEB 2018 Sources Sources Sources Initial evaluation History Physical examination Laboratory evaluation Obtained at
Renal Artery Embolization in Post Traumatic Vascular Lesions
 Med. J. Cairo Univ., VoL 81, No. 2, March: 69-73, 2013 www.medicaljournalofcairouniversity.com Renal Artery Embolization in Post Traumatic Vascular Lesions IHAB I. ALI, M.D.*; HESHAM BADAWY, M.D.**; AMR
Med. J. Cairo Univ., VoL 81, No. 2, March: 69-73, 2013 www.medicaljournalofcairouniversity.com Renal Artery Embolization in Post Traumatic Vascular Lesions IHAB I. ALI, M.D.*; HESHAM BADAWY, M.D.**; AMR
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment
 Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
MASSIVE GASTROINTESTINAL HAEMORRHAGE: THE RADIOLOGIST'S ROLE IN DIAGNOSIS AND MANAGEMENT
 MASSIVE GASTROINTESTINAL HAEMORRHAGE: THE RADIOLOGIST'S ROLE IN DIAGNOSIS AND MANAGEMENT K.P. Tan H.K. Boey SYNOPSIS Massive gastrointestinal haemorrhage is a life -threatening condition. Angiography can
MASSIVE GASTROINTESTINAL HAEMORRHAGE: THE RADIOLOGIST'S ROLE IN DIAGNOSIS AND MANAGEMENT K.P. Tan H.K. Boey SYNOPSIS Massive gastrointestinal haemorrhage is a life -threatening condition. Angiography can
COPYRIGHTED MATERIAL. 1 Approach to the patient with gross gastrointestinal bleeding. Grace H. Elta, Mimi Takami
 1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
Renal Artery Embolization for the Treatment of Renal Artery Pseudoaneurysm Following Partial Nephrectomy
 The Ochsner Journal 13:259 263, 2013 Ó Academic Division of Ochsner Clinic Foundation Renal Artery Embolization for the Treatment of Renal Artery Pseudoaneurysm Following Partial Nephrectomy Cara Irwine,
The Ochsner Journal 13:259 263, 2013 Ó Academic Division of Ochsner Clinic Foundation Renal Artery Embolization for the Treatment of Renal Artery Pseudoaneurysm Following Partial Nephrectomy Cara Irwine,
Clinical Management of Obscure- Overt Gastrointestinal Bleeding. Presented by Dr. 張瀚文
 Clinical Management of Obscure- Overt Gastrointestinal Bleeding Presented by Dr. 張瀚文 Definition Obscure: : hard to understand; not clear. Overt: : public; not secret. Occult: : hidden from the knowledge
Clinical Management of Obscure- Overt Gastrointestinal Bleeding Presented by Dr. 張瀚文 Definition Obscure: : hard to understand; not clear. Overt: : public; not secret. Occult: : hidden from the knowledge
N-butyl Cyanoacrylate Embolotherapy for Acute Gastroduodenal Ulcer Bleeding 1
 N-butyl Cyanoacrylate Embolotherapy for Acute Gastroduodenal Ulcer Bleeding 1 Young Ho Choi, M.D., Ji-hoon Kim, M.D., Young Hwan Koh, M.D., Daehee Han, M.D., Joo Hee Cha, M.D., Chang Kyu Seong, M.D., Chi
N-butyl Cyanoacrylate Embolotherapy for Acute Gastroduodenal Ulcer Bleeding 1 Young Ho Choi, M.D., Ji-hoon Kim, M.D., Young Hwan Koh, M.D., Daehee Han, M.D., Joo Hee Cha, M.D., Chang Kyu Seong, M.D., Chi
Interventional radiology in gastrointestinal hemorrhage When and how we do it!
 Interventional radiology in gastrointestinal hemorrhage When and how we do it! Poster No.: C-1221 Congress: ECR 2014 Type: Educational Exhibit Authors: H. Nunes Correia, J. F. Costa, P. Donato, A. Gil
Interventional radiology in gastrointestinal hemorrhage When and how we do it! Poster No.: C-1221 Congress: ECR 2014 Type: Educational Exhibit Authors: H. Nunes Correia, J. F. Costa, P. Donato, A. Gil
Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the Uterus with Fibroids
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the
The gastroduodenal artery: Radiological anatomy, imaging and endovascular intervention
 The gastroduodenal artery: Radiological anatomy, imaging and endovascular intervention Poster No.: C-2049 Congress: ECR 2010 Type: Educational Exhibit Topic: Interventional Radiology Authors: R. D. White,
The gastroduodenal artery: Radiological anatomy, imaging and endovascular intervention Poster No.: C-2049 Congress: ECR 2010 Type: Educational Exhibit Topic: Interventional Radiology Authors: R. D. White,
Emergency Surgery Course Graz, March UPPER GI BLEEDING. Carlos Mesquita Coimbra
 UPPER GI BLEEDING Carlos Mesquita Coimbra Aim Causes Management Problem Above angle of Treitz Common emergency 1-2/1000 pts 10% rebleeed 1% angioembolization 20% over 60
UPPER GI BLEEDING Carlos Mesquita Coimbra Aim Causes Management Problem Above angle of Treitz Common emergency 1-2/1000 pts 10% rebleeed 1% angioembolization 20% over 60
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Occult bleeding of small bowel: endovascular embolization and literature review
 Journal of Digestive Diseases 2009; 10; 152 156 doi: 10.1111/j.1751-2980.2009.00379.x Occult bleeding of small bowel: endovascular embolization and literature review XXX Case Embolization AH CASE Blackwell
Journal of Digestive Diseases 2009; 10; 152 156 doi: 10.1111/j.1751-2980.2009.00379.x Occult bleeding of small bowel: endovascular embolization and literature review XXX Case Embolization AH CASE Blackwell
Endoscopic Examination for Duodenal Ulcer Bleeding during Transcatheter Arterial Embolization: Analysis of Two Cases
 Tokai J Exp Clin Med., Vol. 34, No. 4, pp. 156-163, 2009 Endoscopic Examination for Duodenal Ulcer Bleeding during Transcatheter Arterial Embolization: Analysis of Two Cases Ryuzo DEGUCHI *1, Toshiyuki
Tokai J Exp Clin Med., Vol. 34, No. 4, pp. 156-163, 2009 Endoscopic Examination for Duodenal Ulcer Bleeding during Transcatheter Arterial Embolization: Analysis of Two Cases Ryuzo DEGUCHI *1, Toshiyuki
The Role of Colonoscopy and Radiological Procedures in the Management of Acute Lower Intestinal Bleeding
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:333 343 STATE OF THE ART The Role of Colonoscopy and Radiological Procedures in the Management of Acute Lower Intestinal Bleeding LISA L. STRATE and CHRISTOPHER
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:333 343 STATE OF THE ART The Role of Colonoscopy and Radiological Procedures in the Management of Acute Lower Intestinal Bleeding LISA L. STRATE and CHRISTOPHER
GASTROINESTINAL BLEEDING. Dr.Ammar I. Abdul-Latif
 GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
Hemobilia and Occult Cystic Artery Stump Bleeding after a Laparoscopic Cholecystectomy: Endovascular Treatment with N-butyl Cyanoacrylate
 132) Prague Medical Report / Vol. 112 (2011) No. 2, p. 132 136 Hemobilia and Occult Cystic Artery Stump Bleeding after a Laparoscopic Cholecystectomy: Endovascular Treatment with N-butyl Cyanoacrylate
132) Prague Medical Report / Vol. 112 (2011) No. 2, p. 132 136 Hemobilia and Occult Cystic Artery Stump Bleeding after a Laparoscopic Cholecystectomy: Endovascular Treatment with N-butyl Cyanoacrylate
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Role of Imaging & Endovascular Intervention in Acute Non-Variceal Gastrointestinal Bleeding
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Role of Imaging & Endovascular Intervention in Acute Non-Variceal Gastrointestinal Bleeding
Rectal bleeding represents approximately 9% to 10% of all
 BRIEF COMMUNICATION Catheter-directed middle hemorrhoidal artery embolization for life-threatening rectal bleeding Mubin I Syed MD 1, Najeeb Chaudhry MD 1, Azim Shaikh MD 1, Kamal Morar MD 1, Kumar Mukerjee
BRIEF COMMUNICATION Catheter-directed middle hemorrhoidal artery embolization for life-threatening rectal bleeding Mubin I Syed MD 1, Najeeb Chaudhry MD 1, Azim Shaikh MD 1, Kamal Morar MD 1, Kumar Mukerjee
Research Article Super-Selective Mesenteric Embolization Provides Effective Control of Lower GI Bleeding
 Hindawi Radiology Research and Practice Volume 2017, Article ID 1074804, 5 pages https://doi.org/10.1155/2017/1074804 Research Article Super-Selective Mesenteric Embolization Provides Effective Control
Hindawi Radiology Research and Practice Volume 2017, Article ID 1074804, 5 pages https://doi.org/10.1155/2017/1074804 Research Article Super-Selective Mesenteric Embolization Provides Effective Control
Small-Bowel Bleeding With Laparoscopic Resection Guided by Microcoil Placement
 CASE REPORT Small-Bowel Bleeding With Laparoscopic Resection Guided by Microcoil Placement Andrew Dobradin, MD, PhD, Jennifer Suzanne Henson, BS, Alberto Mansilla, MD, Charlene LePane, DO University of
CASE REPORT Small-Bowel Bleeding With Laparoscopic Resection Guided by Microcoil Placement Andrew Dobradin, MD, PhD, Jennifer Suzanne Henson, BS, Alberto Mansilla, MD, Charlene LePane, DO University of
Nonvariceal Upper Gastrointestinal Bleeding: the Usefulness of Rotational Angiography after Endoscopic Marking with a Metallic Clip
 Original Article DOI: 10.3348/kjr.2011.12.4.473 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(4):473-480 Nonvariceal Upper Gastrointestinal Bleeding: the Usefulness of Rotational Angiography
Original Article DOI: 10.3348/kjr.2011.12.4.473 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(4):473-480 Nonvariceal Upper Gastrointestinal Bleeding: the Usefulness of Rotational Angiography
An unusual source of right upper quadrant pain
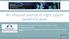 Originally Posted: Month, 00, 20xx An unusual source of right upper quadrant pain Resident(s): Ashish R. Vyas MD (PGY-V), Dominic T. Semaan M.D., J.D. (PGY-V) Attending(s): Dr. Denis Lincoln Program/Dept(s):
Originally Posted: Month, 00, 20xx An unusual source of right upper quadrant pain Resident(s): Ashish R. Vyas MD (PGY-V), Dominic T. Semaan M.D., J.D. (PGY-V) Attending(s): Dr. Denis Lincoln Program/Dept(s):
THE BLEEDING MARGINAL ULCER*
 DECEMBER, 1975 THE BLEEDING MARGINAL ULCER* ABSTRACT: CATHETERIZATION DIAGNOSIS AND THERAPY By ALFRED ROSENBAUM, M.D.,t STANLEY S. SIEGELMAN, M.D.4 and SEYMOUR SPRAYREGEN, M.D. Superior mesenteric arteriography
DECEMBER, 1975 THE BLEEDING MARGINAL ULCER* ABSTRACT: CATHETERIZATION DIAGNOSIS AND THERAPY By ALFRED ROSENBAUM, M.D.,t STANLEY S. SIEGELMAN, M.D.4 and SEYMOUR SPRAYREGEN, M.D. Superior mesenteric arteriography
Sangrado Gastrointestinal Alto Upper GI Bleeding
 Sangrado Gastrointestinal Alto Upper GI Bleeding Curso Internacional Retos Clinicos en la Gastroenterologia de Urgencias Asociacion Colombiana de Gastroenterologia 31 de Agosto, 2012 Pereira, Risaralda
Sangrado Gastrointestinal Alto Upper GI Bleeding Curso Internacional Retos Clinicos en la Gastroenterologia de Urgencias Asociacion Colombiana de Gastroenterologia 31 de Agosto, 2012 Pereira, Risaralda
Coils and plugs have emerged as the most commonly
 The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1
 Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Transcatheter Arterial Embolization of Nonvariceal Upper Gastrointestinal Bleeding with N-Butyl Cyanoacrylate
 Transcatheter Arterial Embolization of Nonvariceal Upper Gastrointestinal Bleeding with N-Butyl Cyanoacrylate Hwan Jun Jae, MD Jin Wook Chung, MD Ah Young Jung, MD Whal Lee, MD Jae Hyung Park, MD Index
Transcatheter Arterial Embolization of Nonvariceal Upper Gastrointestinal Bleeding with N-Butyl Cyanoacrylate Hwan Jun Jae, MD Jin Wook Chung, MD Ah Young Jung, MD Whal Lee, MD Jae Hyung Park, MD Index
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Oakland K, Jairath V, Uberoi R, et al. Derivation
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Oakland K, Jairath V, Uberoi R, et al. Derivation
Emergency Surgery Board Department of General Surgery Rambam Health Care Campus
 Emergency Surgery Board Department of General Surgery Rambam Health Care Campus Surgical Complications of Peptic Ulcer Disease Bleeding Case Presentation and Review of the Literature Case Presentation
Emergency Surgery Board Department of General Surgery Rambam Health Care Campus Surgical Complications of Peptic Ulcer Disease Bleeding Case Presentation and Review of the Literature Case Presentation
CHIEF COMPLAINT & HPI
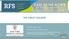 THE GREAT HOUDINI Resident: Marc Lim, MD Attending: Shekher Maddineni, MD Program/Department: Westchester Medical Center/New York Medical College/Department of Radiology CHIEF COMPLAINT & HPI Chief Complaint
THE GREAT HOUDINI Resident: Marc Lim, MD Attending: Shekher Maddineni, MD Program/Department: Westchester Medical Center/New York Medical College/Department of Radiology CHIEF COMPLAINT & HPI Chief Complaint
Quality Improvement Guidelines for Transcatheter Embolization for Acute Gastrointestinal Nonvariceal Hemorrhage
 Cardiovasc Intervent Radiol (2013) 36:608 612 DOI 10.1007/s00270-012-0462-5 CIRSE STANDARDS OF PRACTICE GUIDELINES Quality Improvement Guidelines for Transcatheter Embolization for Acute Gastrointestinal
Cardiovasc Intervent Radiol (2013) 36:608 612 DOI 10.1007/s00270-012-0462-5 CIRSE STANDARDS OF PRACTICE GUIDELINES Quality Improvement Guidelines for Transcatheter Embolization for Acute Gastrointestinal
WASSIM ABI JAOUDE, MD SUNY DOWNSTATE MEDICAL CENTER MAY 20 TH, 2010 MANAGEMENT OF ACUTE UPPER GI BLEEDING
 WASSIM ABI JAOUDE, MD SUNY DOWNSTATE MEDICAL CENTER MAY 20 TH, 2010 MANAGEMENT OF ACUTE UPPER GI BLEEDING CASE PRESENTATION 74 YO female JEHOVAH S WITNESS admitted for CHEST PAIN to telemetry on 4/26/2010
WASSIM ABI JAOUDE, MD SUNY DOWNSTATE MEDICAL CENTER MAY 20 TH, 2010 MANAGEMENT OF ACUTE UPPER GI BLEEDING CASE PRESENTATION 74 YO female JEHOVAH S WITNESS admitted for CHEST PAIN to telemetry on 4/26/2010
On-Call Upper GI Bleeding. Upper Gastrointestinal Bleeding
 On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
Management of Bleeding Gastroduodenal Ulcers
 Complications in Oesophageal and Gastric Surgery Dig Surg 2002;19:99 104 Management of Bleeding Gastroduodenal Ulcers J.J.B. van Lanschot a M. van Leerdam b O.M. van Delden c P. Fockens b Departments of
Complications in Oesophageal and Gastric Surgery Dig Surg 2002;19:99 104 Management of Bleeding Gastroduodenal Ulcers J.J.B. van Lanschot a M. van Leerdam b O.M. van Delden c P. Fockens b Departments of
Sanda et al. SpringerPlus 2014, 3:17 a SpringerOpen Journal
 Sanda et al. SpringerPlus 2014, 3:17 a SpringerOpen Journal CASE STUDY Open Access Arterial supply to the bleeding diverticulum in the ascending duodenum treated by transcatheter arterial embolization
Sanda et al. SpringerPlus 2014, 3:17 a SpringerOpen Journal CASE STUDY Open Access Arterial supply to the bleeding diverticulum in the ascending duodenum treated by transcatheter arterial embolization
Ethylene-vinyl alcohol polymer transarterial embolization in emergency peripheral active bleeding
 Ethylene-vinyl alcohol polymer transarterial embolization in emergency peripheral active bleeding Ierardi AM, Duka E, Micieli C, Carrafiello G Interventional Radiology Unit University of Insubria, Varese
Ethylene-vinyl alcohol polymer transarterial embolization in emergency peripheral active bleeding Ierardi AM, Duka E, Micieli C, Carrafiello G Interventional Radiology Unit University of Insubria, Varese
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Role of the Radiologist
 Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
25/11/ / upper G.I. bleeding sources 20/ lower G.I. bleeding sources. scaricato da 1
 U.S.L. AVEZZANO - SULMONA Ospedale SS Filippo e Nicola U.O. ENDOSCOPIA DIGESTIVA (Direttore Dott. Antonio Sedici) double-balloon balloon enteroscopy new gold standard for small-bowel imaging? A. Sedici
U.S.L. AVEZZANO - SULMONA Ospedale SS Filippo e Nicola U.O. ENDOSCOPIA DIGESTIVA (Direttore Dott. Antonio Sedici) double-balloon balloon enteroscopy new gold standard for small-bowel imaging? A. Sedici
Management of Massive Peptic Ulcer Bleeding
 Management of Massive Peptic Ulcer Bleeding Frances K.Y. Cheung, FRCS, JamesY.W. Lau, MD KEYWORDS Bleeding peptic ulcer Endoscopy Surgery Angiographic embolization In an old surgical series, massive bleeding
Management of Massive Peptic Ulcer Bleeding Frances K.Y. Cheung, FRCS, JamesY.W. Lau, MD KEYWORDS Bleeding peptic ulcer Endoscopy Surgery Angiographic embolization In an old surgical series, massive bleeding
Shou Jiang Tang, MD, FASGE. Director of Endoscopic Research Professor in Medicine
 Shou Jiang Tang, MD, FASGE Director of Endoscopic Research Professor in Medicine Through-the-scope clipping devices Over-the-scope clipping devices First reported clipping device Hayshi T, Yonezawa M,
Shou Jiang Tang, MD, FASGE Director of Endoscopic Research Professor in Medicine Through-the-scope clipping devices Over-the-scope clipping devices First reported clipping device Hayshi T, Yonezawa M,
Interventions in Visceral Artery Bleed
 Interventions in Visceral Artery Bleed Dr. Arun Gupta Consultant, Interventional Radiology Sir Ganga Ram Hospital, Delhi, India. INTRODUCTION Visceral artery aneurysms (VAAs) are rare, reported incidence
Interventions in Visceral Artery Bleed Dr. Arun Gupta Consultant, Interventional Radiology Sir Ganga Ram Hospital, Delhi, India. INTRODUCTION Visceral artery aneurysms (VAAs) are rare, reported incidence
A bleeding ulcer: What can the GP do? Gastrointestinal bleeding is a relatively common. How is UGI bleeding manifested? Who is at risk?
 Focus on CME at the University of British Columbia A bleeding ulcer: What can the GP do? By Robert Enns, MD, FRCP Gastrointestinal bleeding is a relatively common disorder affecting thousands of Canadians
Focus on CME at the University of British Columbia A bleeding ulcer: What can the GP do? By Robert Enns, MD, FRCP Gastrointestinal bleeding is a relatively common disorder affecting thousands of Canadians
Treatment options for endoleaks: stents, embolizations and conversions
 Treatment options for endoleaks: stents, embolizations and conversions Poster No.: C-0861 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit G. Lombardi; napoli/it Arteries / Aorta, Abdomen,
Treatment options for endoleaks: stents, embolizations and conversions Poster No.: C-0861 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit G. Lombardi; napoli/it Arteries / Aorta, Abdomen,
Available online at journal homepage:
 Formosan Journal of Surgery (2012) 45, 113e117 Available online at www.sciencedirect.com journal homepage: www.e-fjs.com ORIGINAL ARTICLE Palpation of preoperatively inserted indwelling angiocatheter facilitates
Formosan Journal of Surgery (2012) 45, 113e117 Available online at www.sciencedirect.com journal homepage: www.e-fjs.com ORIGINAL ARTICLE Palpation of preoperatively inserted indwelling angiocatheter facilitates
Acute Gastrointestinal Hemorrhage: Radiologic Diagnosis and Management
 Canadian Association of Radiologists Journal 64 (2013) 90e100 Vascular and Interventional Radiology / Radiologie vasculaire et radiologie d intervention Acute Gastrointestinal Hemorrhage: Radiologic Diagnosis
Canadian Association of Radiologists Journal 64 (2013) 90e100 Vascular and Interventional Radiology / Radiologie vasculaire et radiologie d intervention Acute Gastrointestinal Hemorrhage: Radiologic Diagnosis
Role of transcatheter arterial embolization for massive bleeding from gastroduodenal ulcers
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 2009 December 21; 15(47): 5889-5897 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.15.5889 2009 The WJG Press and
Online Submissions: wjg.wjgnet.com World J Gastroenterol 2009 December 21; 15(47): 5889-5897 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.15.5889 2009 The WJG Press and
Clinical Endoscopic Parameters of Upper Gastrointestinal Bleeding Hemal Shah, 1 T. P. Manohar 2
 Original Article Clinical Endoscopic Parameters of Upper Gastrointestinal Bleeding Hemal Shah, 1 T. P. Manohar 2 1 Junior Resident 2 Associate Professor,Department of Medicine, N.K.P. Salve Institute Of
Original Article Clinical Endoscopic Parameters of Upper Gastrointestinal Bleeding Hemal Shah, 1 T. P. Manohar 2 1 Junior Resident 2 Associate Professor,Department of Medicine, N.K.P. Salve Institute Of
CT Angiography g of Lower Intestinal Bleeding
 CT Angiography g of Lower Intestinal Bleeding Jorge A. Soto, MD General concepts: Learning Objectives Clinical Importance Presentation, Location Etiologies CT Ttchniques: CT Angiography CT Enterography
CT Angiography g of Lower Intestinal Bleeding Jorge A. Soto, MD General concepts: Learning Objectives Clinical Importance Presentation, Location Etiologies CT Ttchniques: CT Angiography CT Enterography
Incidence and Management of Bleeding Complications Following Percutaneous Radiologic Gastrostomy
 Original Article http://dx.doi.org/10.3348/kjr.2012.13.2.174 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(2):174-181 Incidence and Management of Bleeding Complications Following Percutaneous
Original Article http://dx.doi.org/10.3348/kjr.2012.13.2.174 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(2):174-181 Incidence and Management of Bleeding Complications Following Percutaneous
Chin J Radiol 2005; 30:
 Chin J Radiol 2005; 30: 41-45 41 Transcatheter Arterial Embolization with N-Butyl 2-Cyanoacrylate for Ruptured Pseudoaneurysm of Gastroduodenal Artery Complicated by Traumatic Pancreatitis: report of a
Chin J Radiol 2005; 30: 41-45 41 Transcatheter Arterial Embolization with N-Butyl 2-Cyanoacrylate for Ruptured Pseudoaneurysm of Gastroduodenal Artery Complicated by Traumatic Pancreatitis: report of a
Management of Endoleaks. Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09
 Management of Endoleaks Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09 Endoleak Failure to totally exclude the abdominal aortic aneurysm (AAA) from continued perfusion and pressurization
Management of Endoleaks Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09 Endoleak Failure to totally exclude the abdominal aortic aneurysm (AAA) from continued perfusion and pressurization
Visceral Artery Aneurysms Endovascular vs. Open?
 Disclosures Visceral Artery Aneurysms Endovascular vs. Open? John S. Lane III, MD Professor and Acting Chief of Vascular Surgery UC San Diego, Department of Surgery None relevant UCSF Vascular Symposium,
Disclosures Visceral Artery Aneurysms Endovascular vs. Open? John S. Lane III, MD Professor and Acting Chief of Vascular Surgery UC San Diego, Department of Surgery None relevant UCSF Vascular Symposium,
Occult and Overt GI Bleeding: Small Bowel Imaging. Outline of Talk
 Occult and Overt GI Bleeding: Small Bowel Imaging Lauren B. Gerson MD, MSc Director of Clinical Research, GI Fellowship Program California Pacific Medical Center San Francisco, CA Outline of Talk Definition
Occult and Overt GI Bleeding: Small Bowel Imaging Lauren B. Gerson MD, MSc Director of Clinical Research, GI Fellowship Program California Pacific Medical Center San Francisco, CA Outline of Talk Definition
ACG Clinical Guideline: Diagnosis and Management of Small Bowel Bleeding
 ACG Clinical Guideline: Diagnosis and Management of Small Bowel Bleeding Lauren B. Gerson, MD, MSc, FACG 1, Jeff L. Fidler 2, MD, David R. Cave, MD, PhD, FACG 3, Jonathan A. Leighton, MD, FACG 4 1 Division
ACG Clinical Guideline: Diagnosis and Management of Small Bowel Bleeding Lauren B. Gerson, MD, MSc, FACG 1, Jeff L. Fidler 2, MD, David R. Cave, MD, PhD, FACG 3, Jonathan A. Leighton, MD, FACG 4 1 Division
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms: a case report
 Chen et al. BMC Urology (2017) 17:120 DOI 10.1186/s12894-017-0311-6 CASE REPORT Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms:
Chen et al. BMC Urology (2017) 17:120 DOI 10.1186/s12894-017-0311-6 CASE REPORT Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms:
Improved risk assessment in upper GI bleeding
 EDITORIAL Improved risk assessment in upper GI bleeding Acute upper GI bleeding is the most common GI emergency, with a reported incidence in various epidemiological studies ranging from 50 to over 100
EDITORIAL Improved risk assessment in upper GI bleeding Acute upper GI bleeding is the most common GI emergency, with a reported incidence in various epidemiological studies ranging from 50 to over 100
Computed Tomography Angiography in Acute Gastrointestinal and Intra-abdominal Bleeding in Children: Preliminary Experience
 Canadian Association of Radiologists Journal 64 (2013) 345e350 Pediatric Radiology / Radiologie pediatrique Computed Tomography Angiography in Acute Gastrointestinal and Intra-abdominal Bleeding in Children:
Canadian Association of Radiologists Journal 64 (2013) 345e350 Pediatric Radiology / Radiologie pediatrique Computed Tomography Angiography in Acute Gastrointestinal and Intra-abdominal Bleeding in Children:
Evaluation and Management of Gastrointestinal Bleeding Part 2: Lower and Obscure Gastrointestinal Bleeding
 Evaluation and Management of Gastrointestinal Bleeding Part 2: Lower and Obscure Gastrointestinal Bleeding Edward Lung, MD, MPH ABSTRACT This article, the second in a 2-part series, provides information
Evaluation and Management of Gastrointestinal Bleeding Part 2: Lower and Obscure Gastrointestinal Bleeding Edward Lung, MD, MPH ABSTRACT This article, the second in a 2-part series, provides information
CrackCast Episode 30 GI Bleeding
 CrackCast Episode 30 GI Bleeding Episode overview: 1) List 5 causes of UGIB in adults and pediatrics 2) List 5 causes of LGIB in adults and pediatrics 3) Describe your management approach for severe UGIB
CrackCast Episode 30 GI Bleeding Episode overview: 1) List 5 causes of UGIB in adults and pediatrics 2) List 5 causes of LGIB in adults and pediatrics 3) Describe your management approach for severe UGIB
CT angiography: imaging findings in GI bleeding
 CT angiography: imaging findings in GI bleeding Poster No.: C-1382 Congress: ECR 2015 Type: Educational Exhibit Authors: S. DIMOULIA, P. Zampakis, A. Valsamos, G. 1 1 1 1 1 1 2 DIAMANTOPOULOU, M. PATSOURA,
CT angiography: imaging findings in GI bleeding Poster No.: C-1382 Congress: ECR 2015 Type: Educational Exhibit Authors: S. DIMOULIA, P. Zampakis, A. Valsamos, G. 1 1 1 1 1 1 2 DIAMANTOPOULOU, M. PATSOURA,
Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased
 1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome. Original Policy Date
 MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
An Evaluation of 99mTc-Labeled Red Blood Cell Scintigraphy for the Detection and Localization of Gastrointestinal Bleeding Sites
 GASTROENTEROLOGY 982 ;83 :394-8 An Evaluation of 99mTc-Labeled Red Blood Cell Scintigraphy for the Detection and Localization of Gastrointestinal Bleeding Sites JOHN A. MARKISZ, DOV FRONT, HENRY D. ROYAL,
GASTROENTEROLOGY 982 ;83 :394-8 An Evaluation of 99mTc-Labeled Red Blood Cell Scintigraphy for the Detection and Localization of Gastrointestinal Bleeding Sites JOHN A. MARKISZ, DOV FRONT, HENRY D. ROYAL,
Therapeutic barium enema for bleeding colonic diverticula: Four case series and review of the literature
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 2008 November 7; 14(41): 6413-6417 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.14.6413 2008 The WJG Press. All
Online Submissions: wjg.wjgnet.com World J Gastroenterol 2008 November 7; 14(41): 6413-6417 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.14.6413 2008 The WJG Press. All
Gastrointestinal Angiodysplasia: CT Findings
 Gastrointestinal Angiodysplasia: CT Findings Poster No.: C-1792 Congress: ECR 2012 Type: Authors: Keywords: DOI: Educational Exhibit G. Anguita Martinez, A. Fernandez Alfonso, D. C. Olivares Morello, J.
Gastrointestinal Angiodysplasia: CT Findings Poster No.: C-1792 Congress: ECR 2012 Type: Authors: Keywords: DOI: Educational Exhibit G. Anguita Martinez, A. Fernandez Alfonso, D. C. Olivares Morello, J.
caused by chronic pancreatitis
 Gut, 1983, 24, 1094-1098 Case report Embolisation of gastroduodenal artery aneurysm caused by chronic pancreatitis R V THAKKER, B GAJJAR, R A WILKINS, AND A J LEVI From Northwick Park Hospital and Clinical
Gut, 1983, 24, 1094-1098 Case report Embolisation of gastroduodenal artery aneurysm caused by chronic pancreatitis R V THAKKER, B GAJJAR, R A WILKINS, AND A J LEVI From Northwick Park Hospital and Clinical
The Occurrence of a Pseudoaneurysm of the Hepatic Artery within the Thrombosed Portal Vein of a Patient with Chronic Pancreatitis: A Case Report 1
 The Occurrence of a Pseudoaneurysm of the Hepatic Artery within the Thrombosed Portal Vein of a Patient with Chronic Pancreatitis: A Case Report 1 Eun Soo Kim, M.D., Kyung Mi Jang, M.D., Min-Jeong Kim,
The Occurrence of a Pseudoaneurysm of the Hepatic Artery within the Thrombosed Portal Vein of a Patient with Chronic Pancreatitis: A Case Report 1 Eun Soo Kim, M.D., Kyung Mi Jang, M.D., Min-Jeong Kim,
Splenic Trauma Where to Occlude and with what
 Splenic Trauma Where to Occlude and with what Trauma session, Thurday May 5, 2016 Pierre GOFFETTE St-Luc University Hospital Brussels Pierre Goffette, M.D. Consultant/Advisory Board: Covidien (Neuro) and
Splenic Trauma Where to Occlude and with what Trauma session, Thurday May 5, 2016 Pierre GOFFETTE St-Luc University Hospital Brussels Pierre Goffette, M.D. Consultant/Advisory Board: Covidien (Neuro) and
Anticoagulants are a contributing factor. Other causes are Mallory-Weiss tears, AV malformations, and malignancy and aorto-enteric fistula.
 Upper GI Bleeding EMU2018 Dr. Walter Himmel MD Incidence: In non-cirrhotics, the commonest causes are peptic ulcer disease (50%) followed by erosive gastritis. In cirrhotic patients, variceal bleeding
Upper GI Bleeding EMU2018 Dr. Walter Himmel MD Incidence: In non-cirrhotics, the commonest causes are peptic ulcer disease (50%) followed by erosive gastritis. In cirrhotic patients, variceal bleeding
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
Bleeding in the Digestive Tract
 Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Urgent Computed Tomography for Determining the Optimal Timing of Colonoscopy in Patients with Acute Lower Gastrointestinal Bleeding
 ORIGINAL ARTICLE Urgent Computed Tomography for Determining the Optimal Timing of Colonoscopy in Patients with Acute Lower Gastrointestinal Bleeding Satoko Nakatsu, Hiroshi Yasuda, Tadateru Maehata, Masahito
ORIGINAL ARTICLE Urgent Computed Tomography for Determining the Optimal Timing of Colonoscopy in Patients with Acute Lower Gastrointestinal Bleeding Satoko Nakatsu, Hiroshi Yasuda, Tadateru Maehata, Masahito
Case Report Multiple Aneurysms of the Inferior Pancreaticoduodenal Artery: A Rare Complication of Acute Pancreatitis
 Case Reports in Vascular Medicine Volume 2013, Article ID 621350, 5 pages http://dx.doi.org/10.1155/2013/621350 Case Report Multiple Aneurysms of the Inferior Pancreaticoduodenal Artery: A Rare Complication
Case Reports in Vascular Medicine Volume 2013, Article ID 621350, 5 pages http://dx.doi.org/10.1155/2013/621350 Case Report Multiple Aneurysms of the Inferior Pancreaticoduodenal Artery: A Rare Complication
Localization of Gastrointestinal Bleeding by Cinematic 99m Tc Labeled Red Blood Cell Scan
 Localization of Gastrointestinal Bleeding by Cinematic 99m Tc Labeled Red Blood Cell Scan Chia-Shang Wu 1, Chang-Chung Lin 1, Nan-Jing Peng 1, 1 Department of Nuclear Medicine, Kaohsiung Veterans General
Localization of Gastrointestinal Bleeding by Cinematic 99m Tc Labeled Red Blood Cell Scan Chia-Shang Wu 1, Chang-Chung Lin 1, Nan-Jing Peng 1, 1 Department of Nuclear Medicine, Kaohsiung Veterans General
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL
 SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
