Risk factors and functional abnormalities associated with adult onset secondary nocturnal enuresis in women
|
|
|
- Antony Winfred Ball
- 5 years ago
- Views:
Transcription
1 University of Plymouth PEARL 01 University of Plymouth Research Outputs University of Plymouth Research Outputs Risk factors and functional abnormalities associated with adult onset secondary nocturnal enuresis in women Madhu, C /nau Neurourology and Urodynamics All content in PEARL is protected by copyright law. Author manuscripts are made available in accordance with publisher policies. Please cite only the published version using the details provided on the item record or document. In the absence of an open licence (e.g. Creative Commons), permissions for further reuse of content should be sought from the publisher or author.
2 This is an accepted manuscript of an article published by Neurourology and Urodynamics available at Risk factors and functional abnormalities associated with adult onset secondary nocturnal enuresis in women Chendrimada Madhu 1 Hashim Hashim 2 Doyo Enki 3 Musaab Yaasin 4 Marcus Drake 5 1 Subspecialty Registrar in urogynaecology, Derriford Hospital, Plymouth and Bristol Urological Institute, Bristol 2 Consultant Urological Surgeon and Director of Urodynamics Unit, Bristol Urological Institute, Southmead Hospital and Honorary Senior Lecturer, University of Bristol 3 Research Fellow in Statistics, Plymouth University, Peninsula Schools of Medicine and Dentistry 4 Research Fellow in Urodynamics and Incontinence, Bristol Urological Institute, Southmead Hospital, Bristol 5 Consultant Urologist, Bristol Urological Institute, Southmead Hospital and Senior lecturer, University of Bristol Corresponding author: Dr. Chendrimada Madhu Department of Urogynaecology and the Bristol Urological Institute Southmead Hospital Bristol BS10 5NB cmadhu@nhs.net Phone: Chendrimada Madhu Protocol/project development, Data collection or management, Data analysis, Manuscript writing/editing Hashim Hashim Protocol/project development, Data collection or management, Data analysis, Manuscript writing/editing Doyo Enki Data analysis, Manuscript writing/editing Musaab Yaasin Protocol/project development, Data collection or management, Manuscript writing/editing Marcus Drake 1
3 Protocol/project development, Data collection or management, Manuscript writing/editing Word count: 2695 Abstract word count: 248 Tables: 2 Summary: This study is a review of risk factors and functional abnormalities in women (age > 1718) with adult onset secondary nocturnal enuresis Key words: Secondary nocturnal enuresis, urodynamics, smoking, antidepressants, stress incontinence, detrusor overactivity Short title: Risk factors and urodynamic findings in adult onset secondary nocturnal enuresis in women 2
4 Abstract Introduction The aim of the study is to review the bothersome lower urinary tract symptoms, risk factors and associated functional urinary abnormalities in women reporting adult onset secondary nocturnal enuresis (SNE), to help understand the pathophysiology of SNE. Methods women (age > 18) attending a single tertiary referral centre underwent a comprehensive standardized evaluation including urodynamic testing in accordance with the recommendations of the International Continence Society. Records of all patients reporting bedwetting whilst asleep were evaluated under various categories. Multiple logistic regression was fitted to identify statistically significant risk factors and urodynamic findings associated with SNE. Results The prevalence of SNE in women undergoing urodynamic testing for bothersome LUTS was 14.4% (1838). High BMI (OR= 1.47, p< 0.001), cigarette smoking (OR= 2, p< 0.001), antidepressant usage (OR= 1.8, p< 0.001), neurological conditions (OR= 2.12, p< 0.001) and previous hysterectomy (OR= 1.19, p= 0.03) were significantly associated with SNE. Women with SNE significantly complained of overactive bladder symptoms (OR= 1.65, p< 0.001) and slightly higher mean nocturia episodes (OR= 1.38, p< ). Low maximum urethral closure pressure (MUCP) (OR= 1.34, p<0.0001) and urodynamically demonstrable detrusor overactivity incontinence (DOI) (OR= 1.75, p<0.0001) were significantly associated with SNE. There was no significant association with the symptom of stress urinary incontinence (SUI) (p= 0.264), urodynamically demonstrable stress incontinence (p= 0.454) or detrusor overactivity (p= 0.231). Conclusion Adult SNE is rarely monosymptomatic and patients usually present with OAB symptoms. SNE is associated with high BMI, cigarette smoking, 3
5 antidepressant use and neurological conditions. DOI and a low MUCP seems to be the main pathophysiological mechanisms associated with SNE. Abstract: 248 words Key words: Adult secondary nocturnal enuresis, overactive bladder symptoms, detrusor overactivity incontinence, antidepressants, High BMI Tables: 2 Conflicts of interest Chendrimada Madhu Hashim Hashim Doyo Enki Musaab Yaasin Marcus Drake Funding: None 4
6 Introduction Nocturnal enuresis (NE) is a highly bothersome lower urinary tract symptom of involuntary loss of urine occurring at sleep (Haylen et al. 2010). NE can be considered as primary (life-long) or secondary (arising after a period without bedwetting of at least one year). It can also be monosymptomatic or polysymptomatic (arising in conjunction with other symptoms). NE is common in children and at 5 years of age up to 25% of children wet the bed (Wan & Greenfield 1997). With each year of maturity the percentage of bed wetting declines by 15 percent, with 8 percent of twelve year old boys and 4 percent of 12 year old girls are enuretic, and this number at adolescent is between 1 and 3% (Thiedke 2003). Longitudinal follow up studies have suggested that 3% of adults over 20 years of age remain enuretic from childhood and are at risk of remaining enuretic for the rest of their lives (Moilanen et al. 1998; Forsythe & Redmond 1974). However, NE may develop as a new symptom in adults after achieving control for a reasonable period of time (Adult onset secondary nocturnal enuresis). Adult onset secondary nocturnal enuresis is the focus of investigation in this paper and will henceforth be referred to as SNE. The prevalence of SNE in women, especially with LUTS is not known. A large epidemiological survey from the Netherlands suggested an overall prevalence of NE at 0.5% in non-institutionalized adults aged between 18 to 64 years, with no difference in age groups or sexes (Hirasing et al. 2009). Various mechanisms including deficient vasopressin release, sleep disorders, psychosocial problems, genetic factors and anatomical bladder problems have been implicated in the pathophysiology of NE (Thiedke 2003; Hirasing et al. 2009; Yeung 2003; Wolfish 2001; Umlauf & Chasens 2003). A reduction in the bladder capacity has been suggested by some studies (C K Yeung et al. 2002), whilst this is not shown as a significant finding in other studies (Nørgaard & Djurhuus 1993). Detrusor overactivity (bladder instability) has also been implicated in the pathophysiology of NE (C K Yeung et al. 2002; Warwick & Whiteside 1979). NE in men has been suggested as a sign of a high pressure chronic urinary retention due to urethral outflow resistance, with a recommendation for investigations and treatment (SAKAMOTO & BLAIVAS 2001; Abeygunasekera & Goonesinghe 2013). Even though urodynamic 5
7 investigations have been used in the assessment of adults with NE with or without other lower urinary tract symptoms, NE is still poorly understood, making management difficult and challenging. This study is a review of findings in all women (>18 years of age) reporting nocturnal enuresis when presenting for urodynamic testing for various lower urinary tract symptoms. The study attempts to characterise specific risk factors and urodynamic findings to further our understanding of this bothersome problem in adults. The aim is to draw conclusions to recommend further research and help manage women with this distressing condition. Methodology: The study was registered with the Research and Innovation department, Southmead Hospital, Bristol. Ethical approval was also obtained from the regional research ethics committee. All patients were seen in the Department of Urodynamics (Bristol Urological Institute) at Southmead Hospital, Bristol. Patients were referred from local, regional and national centres for urodynamic assessment. All patients were sent an information leaflet regarding the urodynamic procedure along with their appointment letter. A team of doctors and specialist urodynamic nurses saw the patients. A verbal consent was obtained prior to performing the test. A complete history and a pelvic examination were done in all patients. A urine analysis was carried out to rule out any infections in all the patients. Invasive and non-invasive urodynamic tests were done in all the patients according to the recommendations of the International Continence Society (ICS). Frequency volume charts of all the patients who filled them out were analyzed, but only mean daytime frequency and nocturia episodes were entered on to the database. All the patients reporting adult onset bedwetting (SNE) were included in the study. Patients with primary nocturnal enuresis (since childhood), with no period of remission, were excluded from the study. Patients aged less than 18 years were also excluded from this study. Data including history and urodynamic findings were kept on a database maintained by the North Bristol NHS trust, Bristol. All the trust standard operating procedures and policies were followed in the collection and analysis 6
8 of the data for this study. Data was analyzed as a whole group and also considered under various associated conditions. NE was considered under primary or secondary types. Patients with primary NE were excluded from analysis. NE was also considered in patients with or without overactive bladder symptoms. NE was also considered in patients smoking cigarettes, using antidepressants and associated neurological conditions. Data from the urodynamic database was anonymized and cleaned for clarity, and then analyzed using SPSS (IBM SPSS Statistics for Windows, Version Armonk, NY: IBM Corp [DGE1]). Student s t-test was used for testing differences in the mean between two continuous variables, while a Chi-square test was used for testing associations between categorical variables. A multivariate multiple logistic regression analysis was done with all the covariates in the model to evaluate the risk factors and urodynamic findings associated with SNE. Unless specified otherwise, all tests were made at a 5% level of significance. Whenever appropriate, p-values, Odds ratios and 95% confidence intervals were computed and included in the result. Results Data from women who underwent urodynamics for various lower urinary tract symptoms during the study period (January 2000 to December 2010) were reviewed women (study group) aged over years complained of secondary nocturnal enuresis in this study, with a prevalence rate of 14.4%. The demographic details of all the patients in the study are summarized in table 1. The average age of women in the study group was 52.6 years (compared to 52.5 in the control group), which was not significant (p= 0.961). The mean parity of women with SNE was 2.4, which was the same in the control group and[dge2] this was not significant (p= 0.158). High BMI (> 30) was significantly associated with SNE in women (27.4% Vs. 19.4%; OR= 1.47, p< ). Significant proportion of women with SNE also smoked cigarettes (30.1% Vs. 15.9%; OR= 2.03, p< 0.001) and reported using anti-depressant medications (16.3% Vs. 8.5%; OR= 1.795, p< 0.001). Neurological conditions like cerebro-vascular accidents and multiple sclerosis were significantly higher in women with SNE (10.3% Vs. 5.2%; OR= 2.12, p< 0.001). Previous hysterectomy was also significantly associated with SNE 7
9 (36% Vs. 30.3%; OR= 1.19, p= 0.032). Menopausal status was not significantly associated with SNE (p=0.638). Important LUTS and urodynamic findings are summarized in table 2. The mean daytime frequency in women with SNE was 8.3 (SD= 3.4), which was slightly higher compared to 7.95 in the control group (OR= 0.97, p= 0.03). The mean nocturia episode was 1.76 (SD = 2.8) in women with SNE compared to 1.26 in the control group, which was statistically highly significant (OR= 1.38, p < 0.001). Significant proportion of women with SNE reported overactive bladder (OAB) symptoms (82.6% Vs. 62.6%; OR= 1.65, p< 0.001). Stress incontinence was not a significant symptom reported at history taking (p= 0.264). At uroflowmetry, a significant proportion of women with SNE (8.1% Vs. 7.1%) had significant post-void residual volume of urine of > 150 ml, (OR = 1.6, p< 0.001). The mean residual volume of urine retained, in women with significant PVR (> 150 ml) was ml compared to ml in the control group, which was significant (p= 0.001). The average flow rate was slightly lesser in the SNE group (21.1 ml/s Vs ml/s, p= 0.017). Women with SNE had a significantly lower cystometric capacity (219.2 ml Vs ml, p < 0.001). 41.1% of women with SNE had low maximum urethral closure pressures compared to 37.9% in the control group, which was statistically significant (OR= 1.34, p< 0.001). Detrusor overactivity was seen in 55.8% of the study group (compared to 40.3% in the control) but this was not statistically significant (p= 0.231). Detrusor overactivity incontinence was demonstrable in 22.9% of women in the study group (22.9% Vs. 12.4%; OR= 1.75, p< 0.001), which was statistically highly significant. Neither a symptom of SUI (p= 0.264) nor a urodynamic finding of UDSI (p= 0.454) were significantly associated with SNE. A combination of UDSI with DOI (mixed UI) was highly significant (37.3% Vs. 21.5%; OR= 1.64, p < 0.001). 8
10 Discussion SNE is a common condition reported by adult women presenting with bothersome LUTS. SNE is significantly associated with overactive bladder symptoms and urinary incontinence. High BMI, cigarette smoking, antidepressant usage were the most significant risk factors associated with SNE. Neurological conditions and pervious hysterectomy were also significantly associated with SNE. Detrusor overactivity incontinence and a low MUCP were the most common associated urodynamic findings. A prevalence of 14.4% of SNE in women presenting with bothersome LUTS for urodynamic testing suggests a high prevalence of this poorly studied condition. Epidemiological studies in adult population quote a prevalence rate of around 3% in adult population (Moilanen et al. 1998; Forsythe & Redmond 1974). A large epidemiological survey suggested an overall prevalence of SNE at 0.5% in non-institutionalized adults (18 64 years) (Hirasing et al. 2009). A study based on a database review of 3000 patients of adult onset nocturnal enuresis without daytime incontinence quoted a prevalence rate of 0.02% (Schäfer et al. 2002). Our study was based on a large database of adult women who presented with various lower urinary tract symptoms indicating a higher prevalence of SNE in adult women with LUTS. It is an indication of the polysymptomatic nature of the problem. It may also be an indication of how women respond to other LUTS in association with SNE, which also reflects their healthcare seeking behavior. Majority of patients in our study complained of overactive bladder symptoms (OR= 1.65) [DGE3]and nocturia (OR= 1.38) [DGE4]was a significant association with SNE. SNE is a nighttime problem; it is possible that women get up more often to ensure that they empty their bladder to avoid SNE episodes. Nocturnal polyuria and abnormal diurnal rhythm of plasma vasopressin are suggested as possible mechanisms for NE (Kamperis et al. 2006; Rittig et al. 1989), which could explain this finding. The database however, did not provide data on nighttime voided volumes and hence we were unable to analyze this data further. DO was more prevalent with SNE but this was not statistically significant. DOI (OR= 2.16) was the most significant urodynamic 9
11 findings demonstrated in women with SNE, which suggests a dysfunction of the bladder detrusor as an important mechanism in the pathophysiology of SNE. Detrusor overactivity has been reported in other studies as one of the predominant urodynamic finding and an important factor in the pathophysiology of NE (Wadie 2004; Foldspang & Mommsen 1994). A genetic inheritance of SNE with associated DO has also been proposed (Chiozza et al. 1998). Current evidence is conflicting on the role of reduced bladder capacity in the pathophysiology of nocturnal enuresis (Ciftci et al. 2012; Kamperis et al. 2006; Lin et al. 2004). The mean maximum cystometric capacity was slightly lower in women with SNE in our study (mean difference of 53.3, p< 0.001), which does indicate a lower bladder capacity as a possible factor in the pathogenesis of NE. A low MUCP was an independent risk factor associated with SNE and was significantly low in the study group, also suggesting a possible role in the etiopathogenesis of SNE. High urethral closure pressure suggestive of obstruction was not noted in our cases, which is in contrast to some studies suggesting retention with outflow obstruction (C K Yeung et al. 2004). A smaller bladder with detrusor dysfunction and a low MUCP may suggest a possible mechanism of adult bed-wetting. A significant proportion of women with SNE did not complain of stress incontinence, and UDSI was not a significant association noted, which indicates that stress incontinence is unlikely to have a role in SNE. Cigarette smoking is associated with overactive bladder symptoms and detrusor overactivity (Tampakoudis et al. 1995; Dallosso et al. 2003). Smoking was a significant finding associated with SNE in our study (OR= 2.26). Nicotine, a nicotinic acetylcholine receptors (nachrs) agonist, has a role in the modulation of neurotransmitter release in both the central and peripheral nervous systems resulting in detrusor contractile responses (Masuda et al. 2006). It is however difficult to establish a causal role of smoking based on this study. Obesity is a known risk factor for both stress and UUI[DGE5] (Mayo & Burns 1990; Whiteside & Arnold 1975; Chung Kwong Yeung et al. 2002). Even though the mechanism is not fully understood on its role in UUI, obesity may cause chronic strain, stretching and weakening the muscles, nerves and other pelvic floor structures (Subak et al. 2009). Obesity 10
12 may also have an affect on the nerve conduction velocities, affecting neuronal control of the urinary bladder and contribute to DOI and in turn SNE (Miscio et al. 2005). Some of these mechanisms explain the significant association of a high BMI with SNE in the study group. Even though we have not used any objective tools to measure depression, 16.3% of our patients reported using antidepressants (OR= 2.1, p<0.001). This data could be an indication of a higher association of depression with nocturnal enuresis or may indicate a higher antidepressant usage in women with SNE. It is difficult to establish a causal relationship based on the data from our study. It is known that NE is associated with depression and low selfesteem in adults (Chung Kwong Yeung et al. 2004). NE might be associated with hypnotic medications (Vural et al. 2007). Antidepressants may also interfere with arousal mechanisms at night, which may lead to nocturnal enuresis (Neveus 2003). Disorders of sleep and arousal have been implicated in the pathophysiology of NE (Umlauf & Chasens 2003; Wolfish 2001). No information could be drawn from the database to evaluate arousal and sleep to explain this finding further. However, the association of antidepressant with SNE indicates a possible neurological basis for the occurrence SNE. The integrity of the central nervous system, nervous control of the bladder and the arousal system of the central nervous system are crucial for maintenance of nighttime bladder function (Fowler et al. 2008). A tenth of all our cases with nocturnal enuresis developed secondary nocturnal enuresis in association with a neurological pathology, which indicates a disruption in the neuronal pathways controlling the bladder. Damage to the neuronal circuits either at the brain or spinal cord results in unmasking of primitive voiding reflexes and trigger detrusor overactivity and incontinence (de Groat 1997). This may also explain the higher incidence of detrusor overactivity in these cases and explain the associated SNE. This study is an evaluation of urodynamic findings of individuals complaining of SNE with or without other lower urinary tract symptoms. SNE alone was not the primary focus of the urodynamic testing in many of the cases, but was 11
13 routinely questioned at history taking. Cystometric tests were done in all cases as per ICS recommendations, which provide valuable data for interpretation and understanding of SNE. All the patients in the study were awake and the test results are an indirect reflection of a problem, which occurs at sleep. Urodynamic assessments were conducted at daytime when the subjects were awake and hence the findings must be interpreted as only associations. Treatment received and outcomes of treatment were also not available from the database and it is also not helped by the fact that some of the cases were referred from other centres for urodynamic testing only. These factors do limit further correlation of the urodynamic findings to patient symptoms and outcomes of treatment. Further long-term longitudinal studies exploring OAB symptoms and NE are needed to understand symptoms emergence and etiopathogenesis of SNE. Conclusion Patients with adult SNE usually present with OAB symptoms. High BMI, cigarette smoking, antidepressant use and neurological conditions are significant risk factors associated with SNE. A low bladder capacity, detrusor overactivity incontinence and Low MUCP are the most significant urodynamic findings associated with SNE. Further studies are needed to evaluate the importance of these findings on treatment outcomes of patients with NE. References: Abeygunasekera, A.M. & Goonesinghe, S.K., Nocturnal Enuresis in Adults. Current Bladder Dysfunction Reports, 8, pp Caldwell, P.H.Y., Deshpande, A. V & Gontard, A. Von, Management of nocturnal enuresis. BMJ: British Medical Journal, 347 :f6259. Chiozza, M.L. et al., An Italian epidemiological multicentre study of nocturnal enuresis. British journal of urology, 81 Suppl 3, pp Ciftci, H. et al., The Relations between Enuresis in Childhood and Nocturnal Polyuria Syndrome in Adult Life. International neurourology journal, 16(1), pp
14 Dallosso, H.M. et al., The association of diet and other lifestyle factors with overactive bladder and stress incontinence: a longitudinal study in women. BJU International, 92(1), pp Foldspang, A. & Mommsen, S., Adult female urinary incontinence and childhood bedwetting. The Journal of urology, 152, pp Forsythe, W.I. & Redmond, A., Enuresis and spontaneous cure rate. Archives of disease in childhood, 49, pp Fowler, C.J., Griffiths, D. & de Groat, W.C., The neural control of micturition. Nature reviews. Neuroscience, 9, pp De Groat, W.C., A neurologic basis for the overactive bladder. Urology, 50(6), pp Haylen, B.T. et al., An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. International urogynecology journal, 21(1), pp Hirasing, R.A. et al., Enuresis Nocturna in Adults. Kamperis, K. et al., Nocturnal polyuria in monosymptomatic nocturnal enuresis refractory to desmopressin treatment. American Journal of Physiology-Renal Physiology, 291(6), pp.f1232 F1240. Lin, A.D.Y. et al., Nocturnal enuresis in older adults. JOURNAL- CHINESE MEDICAL ASSOCIATION, 67(3), pp Masuda, H. et al., Roles of peripheral and central nicotinic receptors in the micturition reflex in rats. The Journal of urology, 176(1), pp Mayo, M.E. & Burns, M.W., Urodynamic studies in children who wet. British journal of urology, 65(6), pp Miscio, G. et al., Obesity and peripheral neuropathy risk: a dangerous liaison. Journal of the peripheral nervous system : JPNS, 10(4), pp Moilanen, I. et al., A follow-up of enuresis from childhood to adolescence. British journal of urology, 81 Suppl 3, pp Neveus, T., The role of sleep and arousal in nocturnal enuresis. Acta Paediatrica, 92(10), pp Nørgaard, J.P. & Djurhuus, J.C., The pathophysiology of enuresis in children and young adults. Clinical pediatrics, Spec No, pp
15 Rittig, S. et al., Abnormal diurnal rhythm of plasma vasopressin and urinary output in patients with enuresis. The American journal of physiology, 256, pp.f664 F671. SAKAMOTO, K. & BLAIVAS, J.G., Adult onset nocturnal enuresis. The Journal of urology, 165(6), pp Schäfer, W. et al., Good urodynamic practices: Uroflowmetry, filling cystometry, and pressure flow studies**. Neurourology and urodynamics, 21(3), pp Subak, L.L., Richter, H.E. & Hunskaar, S., Obesity and urinary incontinence: epidemiology and clinical research update. The Journal of urology, 182(6 Suppl), pp.s2 7. Tampakoudis, P. et al., Cigarette smoking and urinary incontinence in women a new calculative method of estimating the exposure to smoke. European Journal of Obstetrics & Gynecology and Reproductive Biology, 63(1), pp Thiedke, C.C., Nocturnal enuresis. American Family Physician, 67, pp Umlauf, M.G. & Chasens, E.R., Sleep disordered breathing and nocturnal polyuria: Nocturia and enuresis. Sleep Medicine Reviews, 7, pp Vural, I.M. et al., Nicotine potentiates the neurogenic contractile response of rabbit bladder tissue via nicotinic acetylcholine receptors: nitric oxide and prostaglandins have no role in this process. Life sciences, 80(12), pp Wadie, B.S., Primary nocturnal enuresis persistent to adulthood, functional evaluation. Neurourology and urodynamics, 23(1), pp Wan, J. & Greenfield, S., Enuresis and common voiding abnormalities. Pediatric Clinics of North America, 44, pp Warwick, R.T. & Whiteside, G., Nocturnal enuresis. Urol Clin North Am, 6, pp Whiteside, C.G. & Arnold, E.P., Persistent primary enuresis: a urodynamic assessment. British medical journal, 1(5954), p.364. Wolfish, N.M., Sleep/arousal and enuresis subtypes. The Journal of urology, 166(6), pp Yeung, C.-K., Nocturnal enuresis (bedwetting). Current opinion in urology, 13, pp
16 Yeung, C.K. et al., Characteristics of primary nocturnal enuresis in adults: an epidemiological study. BJU international, 93(3), pp Yeung, C.K. et al., Reduction in nocturnal functional bladder capacity is a common factor in the pathogenesis of refractory nocturnal enuresis. BJU international, 90(3), pp Yeung, C.K. et al., Reduction in nocturnal functional bladder capacity is a common factor in the pathogenesis of refractory nocturnal enuresis. BJU international, 90(3), pp Yeung, C.K. et al., Urodynamic findings in adults with primary nocturnal enuresis. The Journal of urology, 171(6), pp Abbreviations used: NE Nocturnal enuresis SNE Adult onset secondary nocturnal enuresis DO Detrusor overactivity UDSI Urodynamic stress incontinence UPP Urethral pressure profile OAB Overactive bladder BMI Body mass index NAD Nothing abnormal detected ICS International continence society PVR Post-void residual volume of urine MUCP Maximum urethral closure pressure UUI? Table 1: Demographic details of women LUTS, with and without secondary NE Parameter SNE group Control group n1 (%) n2 (%) p-value Odds ratio 95% Number 1838 (14.4) (85.6) High BMI (>30) 504 (27.4) 2122 (19.4) < Smokers 554 (30.1) 1744 (15.9) < Anti-depressants 300 (16.3) 935 (8.5) < Neurological conditions 190 (10.3) 565 (5.2) < Menopausal 1157 (62.9) 6685 (61) Previous hysterectomy 662 (36) 3325 (30.3) Mean (SD) Mean (SD) Mean age 52.6 (14.9) 52.5 (13.24) Parity 2.4 (1.5) 2.4 (1.3) Table 2: 15
17 Lower Urinary tract symptoms and urodynamic findings in women, with and without secondary NE SNE group n1 (%) Control group n2 (%) P-value Odds ra Parameter Overactive Bladder (OAB) symptoms 1518 (82.6) 6863 (62.6) < Stress urinary incontinence 1510 (82.2) 9130 (83.3) Low MUCP 756 (41.1) 4158 (37.9) < Detrusor overactivity 1027 (55.8) 4415 (40.3) Detrusor Overactivity incontinence (DOI) 420 (22.9) 1321 (12.4) < UDSI 818 (44.5) 5513 (50.3) DOI + UDSI (Mixed UI) 685 (37.3) 2357 (21.5) < Mean (SD) Mean (SD) Daytime Frequency 8.3 (3.35) 7.95 (2.79) Nocturia Episodes 1.76 (1.34) 1.26 (1.17) <
University of Bristol - Explore Bristol Research. Peer reviewed version. Link to published version (if available): 10.
 Madhu, C., Enki, D., Yassin, M., Drake, M., & Hashim, H. (2015). The Functional Effects of Cigarette Smoking in Women on the Lower Urinary Tract. Urologia Internationalis, 95(4), 478-482. https://doi.org/10.1159/000438928
Madhu, C., Enki, D., Yassin, M., Drake, M., & Hashim, H. (2015). The Functional Effects of Cigarette Smoking in Women on the Lower Urinary Tract. Urologia Internationalis, 95(4), 478-482. https://doi.org/10.1159/000438928
The new ICCS terminology J Urol 176, , 2006
 The new ICCS terminology J Urol 176, 314-324, 2006 The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Report from the Standardisation Committee of the International
The new ICCS terminology J Urol 176, 314-324, 2006 The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Report from the Standardisation Committee of the International
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Urodynamic findings in patient above 15 years old with primary refractory nocturnal enuresis
 Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-323X) Vol. 4(8) pp. 374-378, August, 2016 Available online http://www.meritresearchjournals.org/mms/index.htm Copyright 2016 Merit Research
Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-323X) Vol. 4(8) pp. 374-378, August, 2016 Available online http://www.meritresearchjournals.org/mms/index.htm Copyright 2016 Merit Research
Urodynamics in women. Aims of Urodynamics in women. Why do Urodynamics?
 Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Diagnostic Value of Functional Bladder Capacity, Urine Osmolality, and Daytime Storage Symptoms for Severity of Nocturnal Enuresis
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.114 Pediatric Urology Diagnostic Value of Functional Bladder Capacity, Urine Osmolality, and Daytime Storage Symptoms for Severity of Nocturnal
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.114 Pediatric Urology Diagnostic Value of Functional Bladder Capacity, Urine Osmolality, and Daytime Storage Symptoms for Severity of Nocturnal
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Table 1. International Consultation on Incontinence recommendations for frail older adults
 Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: , ISSN(Online): Vol.9, No.
 International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304, ISSN(Online): 2455-9563 Vol.9, No.5, pp 81-85, 2016 Percutaneous Electrical Stimulation for Management of Monosympatomatic
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304, ISSN(Online): 2455-9563 Vol.9, No.5, pp 81-85, 2016 Percutaneous Electrical Stimulation for Management of Monosympatomatic
Okubo, Kazutoshi; Aoki, Katsuya; Wa. Right Research, Inc. Published by Elsevie
 Title Objective patterning of uroflowmetr daytime and nighttime wetting. Kanematsu, Akihiro; Johnin, Kazuyos Author(s) Okubo, Kazutoshi; Aoki, Katsuya; Wa Yoshino, Kaoru; Tanaka, Shiro; Tani Osamu Citation
Title Objective patterning of uroflowmetr daytime and nighttime wetting. Kanematsu, Akihiro; Johnin, Kazuyos Author(s) Okubo, Kazutoshi; Aoki, Katsuya; Wa Yoshino, Kaoru; Tanaka, Shiro; Tani Osamu Citation
This article is a CME certified activity. To earn credit for this activity visit: /viewarticle/758676
 This article is a CME certified activity. To earn credit for this activity visit: /viewarticle/758676 CME Information CME Released: 02/15/2012; Valid for credit through 02/15/2013 Target Audience www.medscape.org
This article is a CME certified activity. To earn credit for this activity visit: /viewarticle/758676 CME Information CME Released: 02/15/2012; Valid for credit through 02/15/2013 Target Audience www.medscape.org
Overactive Bladder in Clinical Practice
 Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in children
 ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
ORIGINAL ARTICLE Vol. 41 (4): 739-743, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0303 Urodynamic outcome of parasacral transcutaneous electrical neural stimulation for overactive bladder in
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
LUTS after TURP: How come and how to manage? Matthias Oelke
 LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Urinary Incontinence. Vibhash Mishra Consultant Urological Surgeon Royal Free Hospital
 Urinary Incontinence Vibhash Mishra Consultant Urological Surgeon Royal Free Hospital Affects women of all ages Impacts physical, psychological & social wellbeing Impact on families & carers Costs the
Urinary Incontinence Vibhash Mishra Consultant Urological Surgeon Royal Free Hospital Affects women of all ages Impacts physical, psychological & social wellbeing Impact on families & carers Costs the
김준철 가톨릭대학교의과대학비뇨기과학교실
 비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Presented by Grace Smith CNC Latrobe Regional Hospital Continence Clinic
 Presented by Grace Smith CNC Latrobe Regional Hospital Continence Clinic Better understand the true effects of aging on the lower urinary tract / bladder Consider other factors that may contribute to urinary
Presented by Grace Smith CNC Latrobe Regional Hospital Continence Clinic Better understand the true effects of aging on the lower urinary tract / bladder Consider other factors that may contribute to urinary
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction
 Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
UK Consensus on Bladder Management in MS
 Continence Care Forum Annual Conference UK Consensus on Bladder Management in MS Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Association of British Neurologists
Continence Care Forum Annual Conference UK Consensus on Bladder Management in MS Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Association of British Neurologists
Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive Bladder
 Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
The standardization of terminology in nocturia: report from the standardization subcommittee of the International Continence Society
 Blackwell Science, LtdOxford, UK BJUBJU International1465-5101BJU International 90Supplement 3December 2002 147 STANDARDIZATION OF TERMINOLOGY P. VAN KERREBROECK et al. 10.1046/j.1464-4096.2002.147.x Original
Blackwell Science, LtdOxford, UK BJUBJU International1465-5101BJU International 90Supplement 3December 2002 147 STANDARDIZATION OF TERMINOLOGY P. VAN KERREBROECK et al. 10.1046/j.1464-4096.2002.147.x Original
Compassionate and effective management
 IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
Frequency of urinary incontinence with Pelvic organ prolapse and associated factors
 ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
April Clinical Focus Topic URINARY FREQUENCY
 April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship
April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Epidemiology of Urinary (UI) and Faecal (FI) Incontinence and Pelvic Organ Prolapse (POP)
 Committee 1 Epidemiology of Urinary (UI) and Faecal (FI) Incontinence and Pelvic Organ Prolapse (POP) Chairman I. MILSOM (Sweden) Members D. ALTMAN (Sweden), M.C. LAPITAN (The Philippines), R. NELSON (U.K),
Committee 1 Epidemiology of Urinary (UI) and Faecal (FI) Incontinence and Pelvic Organ Prolapse (POP) Chairman I. MILSOM (Sweden) Members D. ALTMAN (Sweden), M.C. LAPITAN (The Philippines), R. NELSON (U.K),
Botulinum Toxin: Applications in Urology
 Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Adrenoceptor Antagonist Tamsulosin for the Treatment of Voiding Symptoms Improves Nocturia and Sleep Quality in Women. The α 1 FEMALE UROLOGY
 The α 1 Adrenoceptor Antagonist Tamsulosin for the Treatment of Voiding Symptoms Improves Nocturia and Sleep Quality in Women Sun-Ouck Kim, Hyang Sik Choi, Dongdeuk Kwon FEMALE UROLOGY Department of Urology,
The α 1 Adrenoceptor Antagonist Tamsulosin for the Treatment of Voiding Symptoms Improves Nocturia and Sleep Quality in Women Sun-Ouck Kim, Hyang Sik Choi, Dongdeuk Kwon FEMALE UROLOGY Department of Urology,
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
SELECTED POSTER PRESENTATIONS
 SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
OAB score: A clinical model that predicts the probability of presenting overactive detrusor in the urodynamic study
 ORIGINAL ARTICLE Vol. 44 (2): 348-354, March - Abril, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0213 OAB score: A clinical model that predicts the probability of presenting overactive detrusor in the urodynamic
ORIGINAL ARTICLE Vol. 44 (2): 348-354, March - Abril, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0213 OAB score: A clinical model that predicts the probability of presenting overactive detrusor in the urodynamic
A joint venture between the Department of Uro-Neurology, Queen Square, University College London and the Neuro-Urology Promotion Committee of the ICS
 Neurogenic bladder 2-day course A joint venture between the Uro-Neurology,, University College London and the Neuro-Urology Promotion Committee of the ICS November 27 and 28, 2014 Venue: Clinical Neuroscience
Neurogenic bladder 2-day course A joint venture between the Uro-Neurology,, University College London and the Neuro-Urology Promotion Committee of the ICS November 27 and 28, 2014 Venue: Clinical Neuroscience
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Pediatric Voiding Dysfunction
 What is wrong with Kids?? Pediatric Voiding Dysfunction Pediatric Urology divided into The Lower Urinary Tract bladder, urethra The Upper Urinary Tract- kidneys and ureters The Lower Urinary Tract Storage
What is wrong with Kids?? Pediatric Voiding Dysfunction Pediatric Urology divided into The Lower Urinary Tract bladder, urethra The Upper Urinary Tract- kidneys and ureters The Lower Urinary Tract Storage
Case studies: LUTS. Case 1 history. Case 1 - questions. Case 1 - outcome. Case 2 - history. Case 1 learning point 14/07/2015 DR JON REES
 Case 1 history Case studies: LUTS DR JON REES A 49 year old male comes to see you he has had gradual deterioration of his flow over the last few years- he saw a colleague of yours 6 weeks ago who recorded
Case 1 history Case studies: LUTS DR JON REES A 49 year old male comes to see you he has had gradual deterioration of his flow over the last few years- he saw a colleague of yours 6 weeks ago who recorded
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 3Q17 July-August
 BRAND NAME Noctiva GENERIC NAME Desmopressin acetate nasal spray MANUFACTURER Serenity Pharmaceuticals DATE OF APPROVAL March 3, 2017 PRODUCT LAUNCH DATE TBD REVIEW TYPE Review type 1 (RT1): New Drug Review
BRAND NAME Noctiva GENERIC NAME Desmopressin acetate nasal spray MANUFACTURER Serenity Pharmaceuticals DATE OF APPROVAL March 3, 2017 PRODUCT LAUNCH DATE TBD REVIEW TYPE Review type 1 (RT1): New Drug Review
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
University of Bristol - Explore Bristol Research
 Drake, M., Lewis, A. L., & Lane, A. (2016). Urodynamic Testing for Men with Voiding Symptoms Considering Interventional Therapy: The Merits of a Properly Constructed Randomised Trial. European Urology,
Drake, M., Lewis, A. L., & Lane, A. (2016). Urodynamic Testing for Men with Voiding Symptoms Considering Interventional Therapy: The Merits of a Properly Constructed Randomised Trial. European Urology,
Clinical Focus Topic
 Clinical Focus Topic NOCTURIA BACKGROUND INFORMATION As we all know, nocturia (needing to wake through the night to void) is a common complaint of men and women around the world. The incidence of nocturia
Clinical Focus Topic NOCTURIA BACKGROUND INFORMATION As we all know, nocturia (needing to wake through the night to void) is a common complaint of men and women around the world. The incidence of nocturia
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Patient Information. Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE
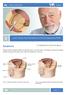 Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Information for Patients. Overactive bladder syndrome (OAB) English
 Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Telford and Wrekin Clinical Commissioning Group
 Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital
 LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
FACTORS AFFECTING VOIDING FUNCTION IN UROGYNECOLOGY PATIENTS
 ORIGINAL ARTICLE FACTORS AFFECTING VOIDING FUNCTION IN UROGYNECOLOGY PATIENTS Ling-Hong Tseng*, Ching-Chung Liang, Pei-Kwei Tsay 1, Alex C. Wang, Tsia-Shu Lo, Yi-Hao Lin Department of Obstetrics and Gynecology,
ORIGINAL ARTICLE FACTORS AFFECTING VOIDING FUNCTION IN UROGYNECOLOGY PATIENTS Ling-Hong Tseng*, Ching-Chung Liang, Pei-Kwei Tsay 1, Alex C. Wang, Tsia-Shu Lo, Yi-Hao Lin Department of Obstetrics and Gynecology,
Michael Organ PGY2 Urology Major Presentation 2011
 Michael Organ PGY2 Urology Major Presentation 2011 1 Epidemiology Pathophysiology Evaluation and Diagnosis Treatments -General -Nocturnal Polyuria -BPH -OAB Conclusion 2 Nocturia is the complaint that
Michael Organ PGY2 Urology Major Presentation 2011 1 Epidemiology Pathophysiology Evaluation and Diagnosis Treatments -General -Nocturnal Polyuria -BPH -OAB Conclusion 2 Nocturia is the complaint that
Diagnosis and Treatment of Urinary Incontinence. Urinary Incontinence
 Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Introduction. Spinal Cord Injury (SCI) Is it necessary to perform surveillance investigations for long term follow up of spinal cord injury patients?
 Is it necessary to perform surveillance investigations for long term follow up of spinal cord injury patients? Rizwan Hamid MBBS, FRCSEd, FRCS(Urol), MD(Res) Honorary Senior Lecturer & Consultant Urologist
Is it necessary to perform surveillance investigations for long term follow up of spinal cord injury patients? Rizwan Hamid MBBS, FRCSEd, FRCS(Urol), MD(Res) Honorary Senior Lecturer & Consultant Urologist
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Paediatric update. Abstract. Background. A u s t r a l i a n a n d N e w Z e a l a n d C o n t i n e n c e J o u r n a l.
 Paediatric update The standardisation of terminology of lower urinary tract function in children and adolescents: Report from the Standardisation Committee of the International Children s Continence Society
Paediatric update The standardisation of terminology of lower urinary tract function in children and adolescents: Report from the Standardisation Committee of the International Children s Continence Society
NOCTURIA WHAT S KEEPING YOU UP AT NIGHT? Frances Stewart RN,NCA
 WHAT S KEEPING YOU UP AT NIGHT? Frances Stewart RN,NCA Objectives Be more knowledgeable in the diagnosis and treatment of nocturia Differentiate between urological causes of nocturia Select appropriate
WHAT S KEEPING YOU UP AT NIGHT? Frances Stewart RN,NCA Objectives Be more knowledgeable in the diagnosis and treatment of nocturia Differentiate between urological causes of nocturia Select appropriate
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder
 www.kjurology.org DOI:10.4111/kju.2011.52.6.396 Voiding Dysfunction Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder Young Kook Han, Won Ki Lee, Seong Ho Lee, Dae
www.kjurology.org DOI:10.4111/kju.2011.52.6.396 Voiding Dysfunction Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder Young Kook Han, Won Ki Lee, Seong Ho Lee, Dae
BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY IN CHILDREN
 0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
GUIDELINES ON URINARY INCONTINENCE
 GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Enuresis is a worldwide problem. In the western population,
 0031-3998/06/6005-0582 PEDIATRIC RESEARCH Vol. 60, No. 5, 2006 Copyright 2006 International Pediatric Research Foundation, Inc. Printed in U.S.A. In this article, the authors propose a non-invasive method
0031-3998/06/6005-0582 PEDIATRIC RESEARCH Vol. 60, No. 5, 2006 Copyright 2006 International Pediatric Research Foundation, Inc. Printed in U.S.A. In this article, the authors propose a non-invasive method
How to assess and predict success or failure of intra-detrusor injections with onabotulinumtoxina
 Reviews How to assess and predict success or failure of intra-detrusor injections with onabotulinumtoxina Mikolaj Przydacz A F, Tomasz Golabek A,E,F, Piotr Chlosta A,E,F Department of Urology, Jagiellonian
Reviews How to assess and predict success or failure of intra-detrusor injections with onabotulinumtoxina Mikolaj Przydacz A F, Tomasz Golabek A,E,F, Piotr Chlosta A,E,F Department of Urology, Jagiellonian
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Urinary incontinence: the management of urinary incontinence in women
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
INJ. Original Article INTRODUCTION. Int Neurourol J 2010;14: doi: /inj pissn eissn
 Original Article Int Neurourol J 21;14:267-271 pissn 293-4777 eissn 293-6931 International Neurourology Journal The Influence of Preoperative Bladder Outlet Obstruction on Continence and Satisfaction in
Original Article Int Neurourol J 21;14:267-271 pissn 293-4777 eissn 293-6931 International Neurourology Journal The Influence of Preoperative Bladder Outlet Obstruction on Continence and Satisfaction in
Incontinence: The silent scourge of the young and old. The International Continence Society has. In this article:
 Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Urinary incontinence and overactive bladder in the non-institutionalized Portuguese population: national survey and methodological issues
 Urinary incontinence and overactive bladder in the non-institutionalized Portuguese population: national survey and methodological issues Sofia Gonçalves Correia Porto 2008 Faculdade de Medicina da Universidade
Urinary incontinence and overactive bladder in the non-institutionalized Portuguese population: national survey and methodological issues Sofia Gonçalves Correia Porto 2008 Faculdade de Medicina da Universidade
