April Clinical Focus Topic URINARY FREQUENCY
|
|
|
- Jocelin Robbins
- 5 years ago
- Views:
Transcription
1 April Clinical Focus Topic URINARY FREQUENCY This month I am focusing on a topic that may seem a little boring. But I would like to look at it from a less common perspective.urinary Frequency and its relationship to voiding dysfunction. ************************************************** Both the ICS and IUGA define urinary frequency as the complaint by a patient who considers that he/she voids too often by the day Abrams 2002, Haylen et al 2010 We have all obviously had numerous patients present complaining of urinary frequency. They often indicate that their bladder rules their life and that they need to void every hour (or sometimes even more). The difficult part is that whilst numerous patients present with this complaint, we know that the actual cause of urinary frequency can be markedly different from patient to patient. Unless we accurately determine the cause of the patient s urinary frequency, it will be difficult to implement the most effective treatment. The most commonly identified causes of urinary frequency include: 1. Excessive fluid intake ie drinking 4-5L/day (especially all the Gen Y s carrying their water bottles!) 2. Habit ie the person is simply voiding frequently out of habit, not because they need to 3. Secondary to Urgency ie the person experiences abnormal sensory signalling in the LUT When excessive fluid intake is found to be the cause of urinary frequency the management is usually quite simple. We first would discuss with the patient about possible reasons for such a high fluid intake ie do they always feel thirsty or is it just habit? If they regularly feel an unusually high thirst, we would first encourage a medical review in case there is another undiagnosed condition influencing their thirst. In contrast, if their high fluid intake appears to simply be habit, or, as I am finding more and more a belief that 4L is good for them - then re-education about appropriate fluid intake will probably suffice. In terms of reason number 2 above - habit, occasionally I find that when people complete their bladder diary for me (especially one where I ask them to specifically document how strong an urge they felt before each void) they come back for their follow up having realized for themselves that their frequency is purely habit. In this scenario, I find that they usually come back having fixed themselves saying I realized that I was going when I really didn t need to, so I ve just started holding on longer. Then we have frequency that occurs because the person has symptomatic urgency. Those of you who have attended the OAB course would remember that we spent a lot of time talking about the concept of urgency. WHTA, Newsletter April 2012 Page 1
2 Urgency is now regarded as not only symptomatically, but also physiologically different from just having a strong urge to void. It is a form of sensory dysfunction that can have multiple causes, and is therefore not regarded as within the normal spectrum of bladder sensations that should occur during the bladder storage phase. It is an abnormal sensation caused by some form of anatomical/physiological dysfunction. In people who suffer from urgency there is no doubt they often subsequently develop a pattern of voiding frequently. This tends to be a secondary behaviour due to the urgency rather than a primary dysfunction in its own right. When a person suffers from sudden onset urgency episodes, the only way we will realistically improve their frequency is to first normalise their bladder sensation. NOTE: In this scenario we aim to improve the urgency which should then improve the frequency.. we don t try to improve the frequency to reduce the urgency! To do this we may give urgency suppression strategies to manage the urgency when it occurs (eg toe curling, PFC, perineal pressure, counting backwards etc etc), but we also employ a range of strategies such as reduction of bladder sensation irritants, alteration to patterns of fluid consumption, bladder retraining / bladder drills, inhibitory electrical stim, and possibly discussion with their GP/gynae/urologist regarding the prescription of anticholinergics/muscarinics or vaginal oestrogen. But what about other causes of urinary frequency?? CLINICAL EXAMPLE: A 55yo female presents to your clinic with urinary frequency of 12 voids per day and 3/night that she finds extremely bothersome. She has a fluid intake of 2.4L per day with an average voided volume of 200mls. She indicates that she doesn t experience urgency prior to voiding, but does experience a strong desire to void that would be uncomfortable to continue holding, even though when she voids she often only passes mls. It is my experience that this is the type of clinical scenario where we as physios can very quickly jump to the urgency techniques described previously (ie urge suppression, try to hold on, electrical stim to inhibit detrusor overactivity etc). It is also the scenario where I find that doctors often jump to anticholinergics / antimuscarinics. However.. is this the best management strategy??? I remember when I was in high school and I had a maths teacher explain that we can t assume that the relationship between two variables are always going to be bi-directional. What do I mean by this??? Well, the really nice example my teacher gave was: All females are human, but not all humans are female I think this is the theory I try to remember with urgency and frequency. Suffering from sensations of urgency will often cause a person to void frequently, but voiding frequently isn t always caused by a sensation of urgency WHTA, Newsletter April 2012 Page 2
3 As we all know, Bladder Capacity refers to the total volume of urine that the bladder can hold. It is largely determined by the compliance of the bladder wall, or in other words, the ability of the bladder wall to expand so as to hold increasing volumes of urine. Obviously, a bladder wall that can only stretch to accommodate 200mls is going to result in a much greater daily frequency than a bladder that can stretch to a capacity of 600mls. Anatomically we know that as the collagen content of the bladder increases, the compliance commonly decreases. In addition, collagen content often increases if the bladder has a denervation injury for a period of time. When we ask our patients to perform a bladder diary, we are attempting to approximate the capacity of the bladder and it s sensory patterning (if we perform a sensation related bladder diary). However, if we consider the situation where a patient may have a high post-void residual (PVR), the volumes listed on their bladder diary will obviously give a false impression of the patient s true bladder capacity. The bladder diary output isn t really reflective of the full Bladder Capacity, it is only reflective of Functional Bladder Capacity. eg Functional Bladder Capacity: A bladder may be able to expand to hold a normal 500mls, but if every time the person voids they leave a 200ml residual, their functional capacity (the amount of urine production the bladder can receive from the kidneys before reaching capacity) is only going to be 300mls. Why am I going on about this so much??? The problem is What if the only reason a woman has frequency is because she has a voiding dysfunction with a residual of mls that is reducing her functional bladder capacity?? It could be that putting her on antimuscarinics or treating her with inhibitory stim may increase her residual to 300mls (due to decreased detrusor contractility from the antimuscarinic), which would then reducing her functional capacity further and worsen her urinary frequency. Incomplete bladder emptying is a cause of urinary frequency that I find urologists working with men commonly consider due to the high post void residuals associated with an enlarged prostate. However, I personally tend to find it is commonly overlooked in females. Research Update Overactive Bladder Symptoms and Voiding Dysfunction in Neurologically Normal Women Espuna-Pons M, Cardozo L, Chapple C, Sievert K, Kerrebroeack P and Kirby M. Neurourology & Urodynamics 20120, March, Vol 31, pp In March 2012 Espuna-Pons et al published a nice review article on post-void residuals, voiding dysfunction and urinary frequency in women. They began the research paper by summarising some evidence for voiding dysfunction in the female population. They mentioned studies such as: - the EPIC study by Irwin et al 2006, which was an international random sample of persons > 18years which found voiding dysfunction in 19.5% of women; the EpiLUTS study which was a cross-sectional study in the United States, United Kingdom and Sweden that found combined voiding and storage symptoms in 14.9% of women, and combined voiding, storage and post-micturition symptoms in WHTA, Newsletter April 2012 Page 3
4 26.3% of women; and also the study by Lukacz et al 2007 which found that the overall prevalence of PVR >100mls in women presenting with pelvic floor disorders was 11%. Therefore, whilst symptoms such as detrusor overactivity, stress incontinence and urgency are all obviously a lot more common than high post-void residuals in women, high PVRs do exist, and in those women where they occur, they can be a significant cause of urinary frequency due to reduced functional capacity. I think that the primary issue for us as physiotherapists is working out whether incomplete bladder emptying could be a cause of our patient s urinary frequency. If it is, we don t want to suggest treatments aimed at reducing voiding ability (eg inhibitory stim or discussion with GP regarding antimuscarinics), rather we need to assist our patients to void to completion. But how do we determine whether this is the issue?? Espuna-Pons et al indicate that the two main ways high PVR is usually diagnosed is by manual palpation of the bladder post void (which they also acknowledge is quite inaccurate), bladder scan (which not all health professionals have access to) or by post void catheterisation (which involves a high UTI risk). They then spent a large amount of time reviewing whether high PVR can be accurately identified by the subjective history. Interesting articles they cited included: 1. Al-Shahrani et al 2005 who found that voiding symptoms alone (eg sensation of incomplete emptying, hesitancy, straining to void) were poor at identifying women with high PVR. This is probably not surprising considering that the normal bladder does not pick up bladder filling until ~150mls. Therefore, if the residual is only 120mls, it is likely that the person will not realise they are incompletely emptying. 2. Lowenstein et al 2008 who also found that voiding symptoms alone were not a good indicator. However, whilst this doesn t look promising, Espuna-pons et al then cited a number of interesting studies that looked at whether symptom clusters could be more reliable. The first was a study by Fitzgerald et al Fitzgerald et al found that in women with urgency/frequency or urge incontinence: 5% of patients with urgency and/or frequency have a PVR >100mls, and. 10% of patients with urgency and urge incontinence have a high PVR >100mls What Fitzgerald also found was that in patients with urgency, frequency and UUI, using a combined symptom cluster criteria of co-existing pelvic organ prolapse >/= stage 2, symptoms of voiding difficulty and absence of stress incontinence that you could predict 82% of patients who have an elevated post-void residual >100mls. WHTA, Newsletter April 2012 Page 4
5 Interestingly, Lukacz et al 2007 who also found that anterior wall or apical prolapse, a feeling of a vaginal bulge, pelvic pressure, splitting of urinary stream and the absence of stress urinary incontinence were associated with PVR >100mls when they occurred together, but only prolapse at or beyond the hymen was a significant factor on logistical regression. Finally, Milleman et al 2007, showed that 19% of women with urgency, frequency and urge incontinence had an elevated post-void residual >100mls, and that age >55years, prior incontinence surgery, history of multiple sclerosis and prolapse grade >/=stage 2 were also associated with high PVR. CLINICAL APPLICATION TIP Whilst most women with OAB (urgency and frequency symptoms) don t always have a high post void residual, there is a certain percentage that do. There seems to be a consistent theme emerging that patients who present with urinary frequency +/- urgency, who also present with symptoms of voiding dysfunction, Prolapse >/=stage 2, and minimal stress incontinence may have elevated PVR as a contributing factor to their frequency. In these circumstances it is important that we don t suggest management options that may worsen their post-void residual. So.. if we think our patient may have a high post-void residual what do we do? This is probably a very long discussion to be had for another day. The main point I hoped to get across in this newsletter is the cluster symptoms that should alert us to the high likelihood of post-void residual being a cause of urinary frequency. However. a few things I would suggest is.. In people with multiple sclerosis there is research to show that the Queen s Square suprapubic bladder stimulator is useful in reducing post-void residuals. It is about $70 to purchase and is available from Malem Pty Ltd in Queensland. Personally, I have also found the Queens square bladder stimulator helpful in some of my patient who have had damage to their bladder following gynae surgery (eg resection of endometriosis from the bladder) Constipation is known to be a significant influence on post-void residual. Improving constipation may reduce outflow obstruction through the urethra and thereby reduce residuals. Both anterior vaginal wall prolapse ( classic cystocele ) and apical prolapse (classic Uterine Prolapse) is associated with residual. Whilst we can easily get into a habit of telling patients to lean slightly WHTA, Newsletter April 2012 Page 5
6 forward to assist bladder emptying, in the case of uterine prolapse this may result in even greater urethral closure pressure due to the uterus compressing the urethra against the pubis. In this case, some women will void better leaning backwards. Finally, in the tweets this month I gave links to the various research projects that have looked at the concept of hovering regarding voiding function. Whilst we all have historically told our patients not to hover (including myself) I would encourage you to have a read over those (the links are available at the end of the newsletter). WHTA, Newsletter April 2012 Page 6
Women s Health Training Associates
 Newsletter April 2012 Opening Letter from Taryn Dear Colleagues, Welcome to the second newsletter of 2012. Hopefully all of you will find something useful in the following pages that may benefit your clinical
Newsletter April 2012 Opening Letter from Taryn Dear Colleagues, Welcome to the second newsletter of 2012. Hopefully all of you will find something useful in the following pages that may benefit your clinical
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Coping with urges and leaks?
 OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
URINARY INCONTINENCE FOR FALLS PREVENTION. by Susan Elms P.T. Elms Physiotherapy
 URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
SPECIAL EDITION: Men s Health
 SPECIAL EDITION: Men s Health 1 Heart Health If you re like most Americans, heart health might be something you don t think about very often. You should. The risk of heart disease increases with age and
SPECIAL EDITION: Men s Health 1 Heart Health If you re like most Americans, heart health might be something you don t think about very often. You should. The risk of heart disease increases with age and
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Managing Female Urinary Incontinence Within Primary Care
 Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Clinical Focus Topic
 Clinical Focus Topic NOCTURIA BACKGROUND INFORMATION As we all know, nocturia (needing to wake through the night to void) is a common complaint of men and women around the world. The incidence of nocturia
Clinical Focus Topic NOCTURIA BACKGROUND INFORMATION As we all know, nocturia (needing to wake through the night to void) is a common complaint of men and women around the world. The incidence of nocturia
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Overactive bladder. Information for patients from Urogynaecology
 Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Patient Information. Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE
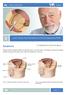 Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
How does interstitial cystitis begin?
 Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
INCONTINENCE AND OTHER UROLOGICAL DILEMMAS DR. ANNA LAWRENCE UROLOGIST AUCKLAND HOSPITAL 161 UROLOGY
 INCONTINENCE AND OTHER UROLOGICAL DILEMMAS DR. ANNA LAWRENCE UROLOGIST AUCKLAND HOSPITAL 161 UROLOGY COVERING INCONTINENCE BE ON JUST NAPPIES CATHETERS TYPES AVAILABLE AND WHEN TO USE THEM JJ STENTS???
INCONTINENCE AND OTHER UROLOGICAL DILEMMAS DR. ANNA LAWRENCE UROLOGIST AUCKLAND HOSPITAL 161 UROLOGY COVERING INCONTINENCE BE ON JUST NAPPIES CATHETERS TYPES AVAILABLE AND WHEN TO USE THEM JJ STENTS???
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Voiding Dysfunction Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU.
 Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises
 MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
Stress incontinence -- occurs during certain activities like coughing, sneezing, laughing, or exercise.
 Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
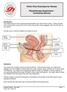 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Management of Incontinence and Pelvic Floor Disorders
 Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital
 LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
LUTS A plea for a holistic approach. HUBERT GALLAGHER, MCh; FRCSI, FRCSI(Urol) Head of Urology Beacon Hospital LUTS- Classification Men LUTS can be divided into: Storage Voiding Frequency Nocturia Urgency
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Incontinence: The silent scourge of the young and old. The International Continence Society has. In this article:
 Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Urinary Incontinence? - gør dig ikke skakmat...
 Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Overactive Bladder Syndrome
 Page 1 of 5 Overactive Bladder Syndrome Overactive bladder syndrome is common. Symptoms include an urgent feeling to go to the toilet, going to the toilet frequently, and sometimes leaking urine before
Page 1 of 5 Overactive Bladder Syndrome Overactive bladder syndrome is common. Symptoms include an urgent feeling to go to the toilet, going to the toilet frequently, and sometimes leaking urine before
Latest Treatments for a Leaky Bladder None
 Latest Treatments for a Leaky Bladder None Financial Disclosures Jeremiah McNamara, MD, OBGYN Boulder Women s Care 303-500-1947 Boulder Women s Care Agenda: Prolapse & Urinary Incontinence The Pelvic Floor
Latest Treatments for a Leaky Bladder None Financial Disclosures Jeremiah McNamara, MD, OBGYN Boulder Women s Care 303-500-1947 Boulder Women s Care Agenda: Prolapse & Urinary Incontinence The Pelvic Floor
Bladder and Bowel Symptoms Troubleshooting Tips
 Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Information for Patients. Overactive bladder syndrome (OAB) English
 Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Urinary Incontinence. a problem for many
 Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Presented by Grace Smith CNC Latrobe Regional Hospital Continence Clinic
 Presented by Grace Smith CNC Latrobe Regional Hospital Continence Clinic Better understand the true effects of aging on the lower urinary tract / bladder Consider other factors that may contribute to urinary
Presented by Grace Smith CNC Latrobe Regional Hospital Continence Clinic Better understand the true effects of aging on the lower urinary tract / bladder Consider other factors that may contribute to urinary
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
CLINICIAN INTERVIEW SPECIFIC FACTORS OF NOCTURIA: A SPECIALIST PERSPECTIVE. An interview with Eric S. Rovner, MD
 SPECIFIC FACTORS OF NOCTURIA: A SPECIALIST PERSPECTIVE An interview with Eric S. Rovner, MD Eric S. Rovner, MD, is Associate Professor of Urology at the Medical University of South Carolina in Charleston.
SPECIFIC FACTORS OF NOCTURIA: A SPECIALIST PERSPECTIVE An interview with Eric S. Rovner, MD Eric S. Rovner, MD, is Associate Professor of Urology at the Medical University of South Carolina in Charleston.
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Table 1. International Consultation on Incontinence recommendations for frail older adults
 Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Y0028_2726_0 File&Use Bladder Control Does Matter
 Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Daily Mail Date: 29 th September ,707,200 unique monthly users
 Daily Mail Date: 29 th September 2014 65,707,200 unique monthly users The bladder problem no one wants to talk about that's blighting 7m lives Lucy Elkins 29 th September 2014 On the face of it Hilary
Daily Mail Date: 29 th September 2014 65,707,200 unique monthly users The bladder problem no one wants to talk about that's blighting 7m lives Lucy Elkins 29 th September 2014 On the face of it Hilary
Management of LUTS. Simon Woodhams February 2012
 Management of LUTS Simon Woodhams February 2012 The management of lower urinary tract symptoms (LUTS) in men Implementing NICE guidance May 2010 NICE clinical guideline 97 Background Lower urinary tract
Management of LUTS Simon Woodhams February 2012 The management of lower urinary tract symptoms (LUTS) in men Implementing NICE guidance May 2010 NICE clinical guideline 97 Background Lower urinary tract
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd
 Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd Segment 1 What is continence? Incontinence is not a but a sign of What organs are involved? and Urine incontinence
Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd Segment 1 What is continence? Incontinence is not a but a sign of What organs are involved? and Urine incontinence
ICD-10 Common Codes for Pelvic Rehab Providers
 ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
Bladder Cancer Knowing the Risks and Warning Signs. Part II: Warning Signs
 Bladder Cancer Knowing the Risks and Warning Signs Part II: Warning Signs May 8, 2018 Presented by: is the Director of Urologic Oncology at MedStar Washington Hospital Center and an Assistant Professor
Bladder Cancer Knowing the Risks and Warning Signs Part II: Warning Signs May 8, 2018 Presented by: is the Director of Urologic Oncology at MedStar Washington Hospital Center and an Assistant Professor
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Continence. Who cares and does it matter? Dr Carl Hanger Geriatrician, CDHB SI Alliance Stroke Education Day 2/11/17
 Continence. Who cares and does it matter? Dr Carl Hanger Geriatrician, CDHB SI Alliance Stroke Education Day 2/11/17 1500 pages, leading stroke experts Does it Matter? Definitely! Patient Dignity / QOL
Continence. Who cares and does it matter? Dr Carl Hanger Geriatrician, CDHB SI Alliance Stroke Education Day 2/11/17 1500 pages, leading stroke experts Does it Matter? Definitely! Patient Dignity / QOL
Stress. incontinence FACTS, ADVICE, AND EXERCISES.
 Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
