Management of spinal cord injury in general practice Part 1
|
|
|
- Catherine Lewis
- 5 years ago
- Views:
Transcription
1 clinical practice James W Middleton MBBS, PhD, FAFRM(RACP), is Director, Statewide Spinal Cord Injury Service, and Associate Professor, Rehabilitation Studies Unit, Faculty of Medicine, The University of Sydney, New South Wales. j.middleton@usyd.edu.au Grace Leong MBBS(Hons) BSc, FAFRM(RACP), is Spinal Rehabilitation Specialist, Statewide Spinal Outreach Service, and Spinal Research Specialist, Spinal Cord Injuries Unit, Royal North Shore Hospital, New South Wales. Linda Mann MBBS, FRACGP, BSc(Med), DRANZCOG, is Medical Educator, SIGPET, New South Wales. Management of spinal cord injury in general practice Part 1 Background Spinal cord injury (SCI) is a complex disability, often requiring specialised knowledge and expertise to manage multisystem impairments. This topic is often not included in undergraduate medical education and the general practitioner may understandably feel underprepared for managing a patient with SCI. Objective This two part article provides an overview of common complications associated with SCI. Discussion Common management issues in SCI include neurogenic bladder and bowel dysfunction, autonomic dysreflexia, sexuality, fertility, pressure areas, pain, spasticity, musculoskeletal disorders, neurological complications, general health and psychological wellbeing. Armed with key information, management of the patient with SCI can be systematically addressed in the general practice setting. The general practitioner plays a vital role in the primary care of people with spinal cord injury. In a previous article we illustrated how practice structures can accommodate people with disabilities, allowing health surveillance/promotion and disease prevention activities through a comprehensive, systematic approach. 1 Bladder function Spinal cord injury (SCI) disrupts bladder control, affecting reciprocal coordination between detrusor and bladder neck, proximal urethra and pelvic floor muscles. Bladder management methods include: clean intermittent self catheterisation (CISC) with an anticholinergic medication such as oxybutynin hydrochloride (preferred method where sufficient hand function exists) drainage by permanent indwelling urethral or suprapubic catheter, or reflex voiding with an external collecting device. 2 Urological complications are common after SCI, including urinary tract infection (UTI), nephrolithiasis, epididymo-orchitis, urethral stricture/false passage, and rarely, bladder cancer in those with a permanent catheter for more than years. 3 Conditions affecting the general population should not be forgotten (eg. benign prostatic hypertrophy). Sustained high bladder filling pressures from poorly controlled detrusor hyperactivity and/or reduced bladder compliance may cause upper tract deterioration, hydronephrosis and renal failure. Renal function should therefore be routinely monitored. Urea, electrolytes, creatinine, estimated glomerular filtration rate (egfr) are recommended annually, with renal tract imaging (ie. ultrasound or intravenous pyelogram) performed every 2 years. Symptoms listed in Table 1 should alert the GP of underlying pathology requiring expedient action. Urinary tract infection is very common but symptoms may be altered or absent in a person with SCI. Colonisation and asymptomatic bacteriuria occurs frequently in populations with permanent catheters in situ, particularly with low pathogenic organisms such as Pseudomonas aeruginosa or mixed growth. Treatment (when symptomatic) should be based on microurine examination, culture and Reprinted from Australian Family Physician Vol. 37, No. 4, April
2 clinical practice Management of spinal cord injury in general practice Part 1 Table 1. Urological symptoms that should alert the GP to action Increased frequency of UTIs Increased or new episodes of incontinence Obstructive symptoms hesitancy, poor stream, frequency (in patients who void spontaneously) Lower abdominal discomfort or bladder spasms Passing grit' or 'stones in urine Difficulty passing an intermittent self catheter Penile erosions Increased spasticity or episodes of autonomic dysreflexia triggered by bladder fullness or pathology Blood in urine, weight loss (especially if the patient is a smoker or has had an indwelling catheter for more than years) Gradually increasing blood pressure Worsening renal blood tests if results known Lost to follow up with no recent (within 5 years) urological imaging or testing sensitivity in a fresh urine specimen taken at new catheter change. Inappropriate, frequent or prolonged antibiotic therapy can predispose to development of antibiotic resistant strains over time. Criteria to assist clinical decision making are shown in Table 2. Recurrent UTIs call for review of patient hygiene and catheterisation techniques and consideration of further investigation to exclude bladder calculi, diverticulum or catheter cystitis. Antiseptic medications (eg. Hiprex or cranberry juice/tablets) are not effective. 4 Gastrointestinal system and bowel management Bowel dysfunction is common following SCI, secondary to impaired colonic transit time, altered compliance, immobility and medication side effects (eg. anticholinergics, antidepressants, narcotic analgesics). 5 Problems such as constipation, faecal incontinence or bowel accidents, abdominal distension and pain can significantly impact on social and emotional wellbeing, participation and quality of life. 6 Diseases such as reflux oesophagitis and gallstones causing repeated complaints of abdominal bloating or nausea are also more prevalent in SCI population, but may be misdiagnosed due to altered sensation. The prevalence of chronic gastrointestinal symptoms Table 2. Guidelines for antibiotic treatment of UTIs 4 Antibiotics are indicated if: microscopy showing WCC >100 associated with a pure growth of organisms, OR leucocyte esterase of +++ to ++++ on urine dip stick, AND at least one category 1 OR at least 2 category 2 symptoms, as defined below: Category 1 symptoms Elevated temperature (>38º core or 37.5º per axilla) New or worsening symptoms of autonomic dysreflexia Category 2 symptoms Increased frequency or strength of muscle spasms Onset of urinary incontinence (eg. leaking around catheter or in between self catheterisation) despite taking usual anticholinergic medications to control detrusor overactivity New abdominal discomfort, unexplained by other pathology Table 3. Key principles in management of neurogenic bowel Determine type of bowel impairment by doing a rectal examination. Patients often have loss of voluntary control over defecation and external anal sphincter (EAS). There are generally 2 types of bowel impairment: upper motor neuron (UMN) or reflexic bowel (usually with lesions above T12). There is intact defecation and anocutaneous reflexes and hypertonic EAS with anorectal dyssynergia lower motor neuron (LMN) or areflexic bowel. Patient often has loss of sacral reflexes including defecation and anocutaneous reflex and poor EAS tone Develop individualised regular bowel routine (daily or every second day for UMN, or twice per day or daily for LMN). Bowel care should be done at the same time every day with: bowel emptying timed minutes after a meal (to utilise gastrocolic reflex) rectal emptying achieved using an enema, suppositories, anal digital stimulation and/or manual evacuation (latter being particularly helpful in LMN type bowel dysfunction) positioning over toilet can assist with stool emptying 230 Reprinted Australian from Family Australian Physician Family Vol. 37, Physician No. 4, April 2008 Vol. 37, No. 4, April 2008
3 Management of spinal cord injury in general practice Part 1 clinical practice increases with time after injury, suggesting that these problems are acquired and potentially preventable. 7 Bowel regimens should be individualised, taking into consideration the level and extent of neurological impairment, functional status, skin integrity, diet and nutritional factors, the individual s problem solving skills, social situation and lifestyle goals. Principles for establishing or adjusting a bowel program appear in Table 3. Bowel function and program should be reviewed regularly as part of an annual cycle of care using a structured questionnaire. 1 Modifications to management are likely to be necessary over time. Constipation is common and can present with a range of symptoms such as abdominal distension, pain, early satiety, nausea, respiratory compromise from diaphragmatic splinting, worsening haemorrhoids with rectal bleeding, autonomic dysreflexia, diarrhoea (spurious), and bowel accidents. A systematic approach begins with consideration of the patient s premorbid GI function, concurrent conditions, current bowel regimen, medication use and defaecation procedure (time taken for evacuation, frequency, amount and stool consistency, eg. using Bristol Stool Chart). Fundamentals of treatment are adequate hydration, a high fibre diet, regular bowel care, minimisation of constipating medications and appropriate aperients when required (Table 4). Haemorrhoids with per rectal (PR) bleeding are also common, 8 often worsened by manual procedures, enemas and constipation. Minor symptomatic cases can often be managed with topical therapy or banding. In some, haemorrhoids can act as a trigger for autonomic dysreflexia and can cause recurrent major bleeding, Table 4. Advice for management of common bowel problems Problem Possible causes Recommended action/s Notes Hard, dry and pebbly stool or no result from bowel care Medication side effects Poor fluid intake (<1.5 L/day) Review and rationalise medications (eg. narcotic analgesics) Alternating diarrhoea (spurious) and hard, inspissated stools (indicates impaction) Soft, poorly formed stool (loose or diarrhoea) Bowel accidents Insufficient stool softeners and/or bulking agents Decrease in physical activity Change in bowel regimen or lifestyle factors Irregular bowel regimen (eg. taking stool softeners and/or bulking agents once per day or every second day) ± some or all of the above contributing factors High impaction with spurious diarrhoea Bowel pattern may be changing Excessive laxative use and/or medication side effects Recent antibiotic use Excess fluid intake Unbalanced diet (insufficient insoluble fibres) Too much alcohol and highly spicy food Gastrointestinal illness Insufficient time for bowel care or insufficient evacuation Stool too soft Certain irritant enemas or suppositories can cause incontinence or residue later in the day Change in diet Gastrointestinal illness Increase fluid intake ( 2 L/day) and review dietary fibre intake Increase softeners or decrease bulking agents; review timing If using physical interventions, review technique. If not, consider adding to assist bowel motion Patient may require disimpaction if hard mass is found on PR Review bowel regimen and change lifestyle factors Abdominal X-ray may help to confirm diagnosis In addition to the above, ensure aperients are taken on a regular basis (ie. twice per day) Start a stool chart and review if bowel routine is adequate Review medications and aperients (consider adding or increasing bulking agents or decease softeners) Consider stool culture and Clostridium difficile toxin if recently on antibiotics Review fluid and dietary fibre intake May need increase of digital stimulation Allow sufficient time for bowel care Review carer s technique Review aperients and enemas or suppositories used Consider stool culture An increase in fibre needs to be matched with an increase in fluid intake or the constipation can worsen If the patient has good results one day and minimal on alternate days, bowel pattern may be changing and may be more suited to an alternate bowel program Avoid irritant stimulants if possible If abdominal X-ray reveals proximal GI faecal loading, Movicol 8 sachets over a day may be effective Avoid irritant stimulants if possible Poorly formed stool can be difficult to evacuate completely during bowel care, predisposing to bowel accidents Reprinted from Australian Family Physician Vol. 37, No. 4, April
4 clinical practice Management of spinal cord injury in general practice Part 1 which should prompt consideration of haemorrhoidectomy. The presence of haemorrhoids and rectal trauma in SCI can give a high false positive rate on faecal occult blood testing and this test should not be relied on for screening of colorectal cancer (CRC). There is no definitive evidence to date to suggest that there is an increased risk of CRC in SCI and screening should follow that recommended for the general population. Autonomic dysreflexia Autonomic dysreflexia (AD) is a potentially life threatening condition affecting persons with a SCI lesion at or above T6 level. 9 In these individuals, a nociceptive stimulus (Table 5) below SCI level triggers excessive reflex activity of sympathetic nervous system (major splanchnic outflow) causing severe vasoconstriction with rapidly rising, uncontrolled blood pressure (BP). Secondary parasympathetic activity (elevated BP sensed by aortic/carotid baroreceptors) produces vagal activation with bradycardia and blood vessel dilatation above the injury level, insufficient to lower BP. Table 6 lists common signs and symptoms of AD. Individuals may experience combinations of symptoms peculiar to them, without all of the typical symptoms of the condition. If the condition is unrecognised or not treated promptly, intracranial haemorrhage, encephalopathy and seizures or a cardiac arrhythmia may occur, which can result in death. Remember that BP for people with high paraplegia or tetraplegia is typically low (~90 100/60 mmhg lying down and possibly lower while sitting). Autonomic dysreflexia symptoms may occur within the normal BP range for the general population (ie mmhg above resting systolic level). 10 Autonomic dysreflexia is most commonly related to bladder/ urinary tract problems such as distended or severely spastic bladder, urinary tract infection, bladder or renal stones, and epididymoorchitis; followed by bowel problems such as constipation, rectal distension, enlarged haemorrhoids, and irritation by enema. Other causes may relate to skin (eg. pressure sores, burns, ingrown toenails) or other systems (eg. fracture, distended stomach, labour, severe menstrual cramping, sexual stimulation). Case study Bob, 42 years of age, with C5 incomplete tetraplegia from a motor vehicle accident 5 years ago, presents to his GP complaining of an intermittent pounding headache with flushing over his face, sweating and feeling anxious. He also mentions having experienced abdominal cramps. Using the SOS Health questionnaire, 1 the GP elicits the following history. Bob s bladder is managed by suprapubic catheter on free drainage. He reports taking oxybutynin (Ditropan) 2.5 mg twice per day, which he had reduced from 5 mg three times per day due to a dry mouth. He drinks about 2 L/day and a carer changes his catheter every month. He has had three UTIs in the past 6 months (with Klebsiella grown on several previous cultures). Over the past 3 weeks Bob has noticed large amounts of urinary debris and occasional blood clots with frequent catheter blockages and some leaking of urine around his SPC site and per urethra. He has abdominal distension and a feeling of fullness and discomfort in his abdomen and is spending up to 2 hours on the toilet for bowel care, with his stool dribbling out. He has a second daily bowel regimen, taking Coloxyl two 120 mg tablets per day as well as 60 ml of pear juice twice per day. He uses Bisalax enemas to initiate evacuation, describing sweating during emptying and prolonged rectal discharge. Bob denies any changes in his medications or dietary intake. He reports that his skin is intact. On examination, Bob s BP is 139/86 mmhg sitting in wheelchair, HR 90 bpm and temperature 37.6 C. He has mild abdominal distension with no tenderness or rigidity on palpation. A PR reveals an empty rectum and prolapsed haemorrhoids which bleed on contact. The SPC site looks moist but there is no skin breakdown or purulent discharge. Urine in the catheter appears cloudy and urine analysis reveals positive leucocytes and nitrites. The GP s provisional diagnosis is AD precipitated by bladder distension caused by intermittent catheter blockages related to recurrent UTIs, as well as possible bowel impaction. The GP also considers reduced bladder compliance and/or detrusor hyper-reflexia following reduction of anticholinergic medication. The GP discusses a management plan with Bob. He changes the suprapubic catheter and sends a fresh urine specimen for culture before starting appropriate antibiotic treatment (considering Klebsiella pneumoniae to be the most likely organism). He advises Bob to increase his fluid intake to 3 L/day, drinking consistently throughout the day. The GP gives him a prescription for Nitrolingual Spray and an Autonomic Dysreflexia Emergency Treatment Card. He also arranges for the community or practice nurse to educate Bob and his carers further on what to do in case another episode occurs. The GP suggests that Bob reduce current softeners and increase the fibre in his diet or add a bulking agent such as Metamucil or Normafibre to firm the consistency of his stools (checking abdominal X-ray first to exclude faecal impaction with overflow). The GP recommends a bowel chart to monitor stool consistency changes making further necessary adjustments after 3 5 bowel cycles. Bisalax can cause local irritation to the rectum and may be the cause of the discharge. Microlax enemas or glycerine suppositories are a gentler alternative in combination with digital stimulation and abdominal massage techniques to assist with facilitating the defecation reflex. Results of investigations (catheter specimen of urine [CSU], blood tests, renal tract ultrasound and abdominal X-ray) reveal Klebsiella pneumoniae and a 1 cm bladder calculus. The GP refers Bob to an urologist for a cystoscopy and opinion about performing a videourodynamic study. The urologist performs a cystoscopy, removing the stone, and finds areas of reactive catheter cystitis requiring diathermy. Videourodynamics on oxybutynin 2.5 mg twice per day reveals high detrusor pressures with detrusor hyper-reflexia. The GP suggests oxybutynin be increased to 5 mg three times per day, but reminds Bob that this may cause constipation and increased aperients may be needed. 232 Reprinted Australian from Family Australian Physician Family Vol. 37, Physician No. 4, April 2008 Vol. 37, No. 4, April 2008
5 Management of spinal cord injury in general practice Part 1 clinical practice Table 5. Common precipiants of autonomic dysreflexia Bladder urinary tract infection, epididymo-orchitis, bladder distension, renal tract calculus, urological procedures Bowel constipation, rectal irritation, haemorrhoids Skin pressure area, burn, ingrown toenail, tight clothing or stockings Gastrointestinal biliary colic, appendicitis, other causes of acute abdomen Obstetric and gynaecological onset of labour, severe menstrual cramping Musculoskeletal fracture Table 6. Common symptoms and signs of autonomic dysreflexia Sudden hypertension Pounding headache Bradycardia Flushing/blotching of skin above spinal injury level Profuse sweating above spinal injury level Skin pallor and piloerection below spinal injury level Chills without fever Nasal congestion Blurred vision (dilatation of pupils) Shortness of breath, sense of apprehension or anxiety If AD is suspected, get help and do not leave the patient alone. Sit the person upright (to buffer rise in BP), loosen tight clothing, compression stockings and abdominal binders. Ask if they suspect a cause (usually due to bladder or bowel problems). Identify the cause (eg. check bladder drainage equipment for kinks, obstruction to flow of urine into bag). Monitor BP every 2 5 minutes. Gentle irrigation (with ~30 ml saline) can be tried to unblock a nondraining catheter. 2 If unsuccessful or bladder is managed by CISC or reflex voiding, catheterise the patient using a generous amount of lubricant containing local anaesthetic gel (eg. 2% lignocaine jelly). Similarly, if constipation is suspected, check the rectum for faecal material and evacuate the contents after anaesthetic gel is inserted for several minutes. 7 If BP is >150 mmhg, drug treatment should be commenced. Glyceryl trinitrate (GTN) can be given sublingually as a spray (Nitrolingual) or half to one tablet (Anginine) or transdermally (5 mg patch), repeated every 5 10 minutes up to three times. If GTN is unavailable or contraindicated, give nifedipine (10 mg tablet crushed, mixed with water and swallowed). 11 In severe cases with a persisting noxious stimulus, parenteral treatment or epidural anaesthesia may be necessary. Close monitoring after the episode is recommended. A MedicAlert bracelet may be considered along with carrying GTN and an Autonomic Dysreflexia Medical Emergency Card to alert medical personnel of this condition. Warning: do not use GTN spray/tablets if phophodiesterase (PDE5) inhibitors such as sildenafil (Viagra), vardenafil (Levitra) have been taken in the previous 24 hours or tadalafil (Cialis) within last 48 hours. Conclusion Secondary prevention and management of conditions arising from SCI require specialised knowledge. Common diseases also occur, but may not present typically because of altered sensation, therefore calling for a high degree of suspicion. The GP is ideally placed to deliver first line care and support for people with SCI. Resources Clinical information booklets, listed below, are available at nsw.gov.au by following the specialties link: Middleton J. Management of the neurogenic bladder for adults with spinal cord injuries Stolzenhein G. Management of the neuropathic bowel for adults with spinal cord injuries Middleton J. Treatment of autonomic dysreflexia for adults with spinal cord injuries: a medical emergency Jannings W, Temblett J, Cairns G, Pryor J. Solving common bowel problems. A resource tool for persons with spinal cord injury. Rehabilitation Nursing Research & Development Unit Available from the Continence Foundation telephone Autonomic Dysreflexia Medical Emergency Card. Telephone SSCIS Conflict of interest: none declared. References 1. Mann L, Middleton JW, Leong G. Fitting disability into practice: focus on spinal cord injury. Aust Fam Physician 2007;36: Consortium for Spinal Cord Medicine Clinical Practice Guidelines. Bladder management in adults with spinal cord injury: a clinical practice guideline for heathccare providers. Paralyzed Veterans of America, Groah SL, Weitzenkamp D, Lammertse DP, et al. Excess risk of bladder cancer in spinal cord injury: Evidence for an association between indwelling catheter use and bladder cancer. Arch Phys Med Rehabil 2002;83: Lee BB, Haran MJ, Hunt LM, et al. Spinal-injured neuropathic bladder antisepsis (SINBA) trial. Spinal Cord 2007;45: Lynch AC, Antony A, Dobbs BR, Frizelle FA. Bowel dysfunction following spinal cord injury. Spinal Cord 2001;39: Rajendran SK, Reiser JR, Bauman W, Zhang RL, Gordon SK, Korsten MA. Gastrointestinal transit after spinal cord injury: effect of cisapride. Am J Gastroenterol 1992;87: Consortium for Spinal Cord Medicine Clinical Practice Guidelines. Neurogenic bowel management in adults with spinal cord injury. Paralyzed Veterans of America, Stone JM, Nino-Murcia M, Wolfe VA, et al. Chronic gastrointestinal problems in spinal cord injury patients: a prospective analysis. Am J Gastroenterol 1990;85: Cole TM, Kottke FJ, Olson M, et al. Alterations of cardiovascular control in high spinal myelomalacia. Arch Phys Med Rehabil 1967;48: Consortium for Spinal Cord Medicine Clinical Practice Guidelines. Acute management of autonomic dysreflexia: individuals with spinal cord injury presenting to healthcare facilities. 2nd edn. Paralyzed Veterans of America, Braddom RL, Rocco JF. Autonomic dysreflexia: a survey of current treatment. Am J Phys Med Rehabil 1991;70: correspondence afp@racgp.org.au Reprinted from Australian Family Physician Vol. 37, No. 4, April
A medical emergency. Treatment of Autonomic Dysreflexia. for adults with spinal cord injuries. Targeting Health Professionals
 JUNE 2002 Revised 2005 Rural Spinal Cord Injury Project A collaborative project between: Prince Henry & Prince of Wales Hospital Royal North Shore Hospital Royal Rehabilitation Centre Sydney Spinal Cord
JUNE 2002 Revised 2005 Rural Spinal Cord Injury Project A collaborative project between: Prince Henry & Prince of Wales Hospital Royal North Shore Hospital Royal Rehabilitation Centre Sydney Spinal Cord
Autonomic Dysreflexia
 Autonomic Dysreflexia A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review date October 2016 This document has been developed to provide health service providers
Autonomic Dysreflexia A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review date October 2016 This document has been developed to provide health service providers
B l a d d e r & B o w e l C a r e. For Patients with Spinal Cord Injuries
 B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
AUTONOMIC DYSREFLEXIA
 NATIONAL SPINAL INJURIES CENTRE STOKE MANDEVILLE HOSPITAL HANDOUT PREPARED BY SPINAL OUTPATIENT SERVICES AUTONOMIC DYSREFLEXIA Spinal Outpatient Services Reviewed July 2013, for review July 2016 AUTONOMIC
NATIONAL SPINAL INJURIES CENTRE STOKE MANDEVILLE HOSPITAL HANDOUT PREPARED BY SPINAL OUTPATIENT SERVICES AUTONOMIC DYSREFLEXIA Spinal Outpatient Services Reviewed July 2013, for review July 2016 AUTONOMIC
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
autonomic dysreflexia
 ! autonomic dysreflexia AUTONOMIC DYSREFLEXIA & YOU Recognize and act WHAT IS AUTONOMIC DYSREFLEXIA (AD)? It is a dangerous rise in your blood pressure that is triggered by a painful or non-painful stimulation
! autonomic dysreflexia AUTONOMIC DYSREFLEXIA & YOU Recognize and act WHAT IS AUTONOMIC DYSREFLEXIA (AD)? It is a dangerous rise in your blood pressure that is triggered by a painful or non-painful stimulation
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries
 Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
SPINAL CORD MEDICINE EDUCATIONAL MATERIALS FOR PATIENT AND FAMILY BOWEL MANAGEMENT FOLLOWING SPINAL CORD INJURY/IMPAIRMENT FRAZIER REHAB INSTITUTE
 SPINAL CORD MEDICINE EDUCATIONAL MATERIALS FOR PATIENT AND FAMILY BOWEL MANAGEMENT FOLLOWING SPINAL CORD INJURY/IMPAIRMENT FRAZIER REHAB INSTITUTE DISCLAIMER The information contained herein is intended
SPINAL CORD MEDICINE EDUCATIONAL MATERIALS FOR PATIENT AND FAMILY BOWEL MANAGEMENT FOLLOWING SPINAL CORD INJURY/IMPAIRMENT FRAZIER REHAB INSTITUTE DISCLAIMER The information contained herein is intended
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
LIVING WITH PARALYSIS. Bladder Management
 LIVING WITH PARALYSIS Bladder Management CAN WE TALK ABOUT YOUR BLADDER? For most people, when, where and how they re going to go isn t something that s given a lot of thought or planned for in advance.
LIVING WITH PARALYSIS Bladder Management CAN WE TALK ABOUT YOUR BLADDER? For most people, when, where and how they re going to go isn t something that s given a lot of thought or planned for in advance.
Lower Urinary Tract Infection (UTI) in Males
 Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Indwelling urinary catheter
 Indwelling urinary catheter Information for patients and carers RDaSH leading the way with care What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder. Following
Indwelling urinary catheter Information for patients and carers RDaSH leading the way with care What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder. Following
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Incontinence in neurological disease
 nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
Autonomic Dysreflexia
 Autonomic Dysreflexia Autonomic dysreflexia (AD) is a potentially life threatening condition that can be considered a medical emergency. It mainly affects people with injuries at T-6 or higher. Although
Autonomic Dysreflexia Autonomic dysreflexia (AD) is a potentially life threatening condition that can be considered a medical emergency. It mainly affects people with injuries at T-6 or higher. Although
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Bowel and Bladder Management following TM
 Presenter: Janet Dean, CRNP Johns Hopkins University School of Medicine Transcription from presentation available at https://youtu.be/nksrjv2oeko [00:30] So I am going to be talking about bowel and bladder
Presenter: Janet Dean, CRNP Johns Hopkins University School of Medicine Transcription from presentation available at https://youtu.be/nksrjv2oeko [00:30] So I am going to be talking about bowel and bladder
Bowel and Bladder Management Following Transverse Myeli5s
 Bowel and Bladder Management Following Transverse Myeli5s Janet Dean, MS, RN, CRRN, CRNP Pediatric Nurse Prac55oner Interna5onal Center for Spinal Cord Injury Department of Physical Medicine and Rehabilita5on
Bowel and Bladder Management Following Transverse Myeli5s Janet Dean, MS, RN, CRRN, CRNP Pediatric Nurse Prac55oner Interna5onal Center for Spinal Cord Injury Department of Physical Medicine and Rehabilita5on
Continence Promotion in
 Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Bowel Function After Spinal Cord Injury
 Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Urinary tract disorders
 Urinary tract disorders Medicines Formulary Contents: 1. Urinary retention 1 2. Urinary incontinence 2 3. Urethral pain prevention during catheterisation 3 4. Indwelling catheters maintenance of patency
Urinary tract disorders Medicines Formulary Contents: 1. Urinary retention 1 2. Urinary incontinence 2 3. Urethral pain prevention during catheterisation 3 4. Indwelling catheters maintenance of patency
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Video urodynamics in spinal injuries. Information for patients Spinal Injuries
 Video urodynamics in spinal injuries Information for patients Spinal Injuries page 2 of 8 Video Urodynamics (VUD) This is a specialised x-ray examination to visualise the function, capacity and emptying
Video urodynamics in spinal injuries Information for patients Spinal Injuries page 2 of 8 Video Urodynamics (VUD) This is a specialised x-ray examination to visualise the function, capacity and emptying
Elimination Patterns: Bladder
 Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Common Complaints in Spinal Cord Injury Population in Primary Care setting and Emergency Room
 Common Complaints in Spinal Cord Injury Population in Primary Care setting and Emergency Room Min Jee Kim, DO Spinal Cord Injury/Disorder Center, VA Palo Alto, Palo Alto, CA mkimpmr@gmail.com Disclosure
Common Complaints in Spinal Cord Injury Population in Primary Care setting and Emergency Room Min Jee Kim, DO Spinal Cord Injury/Disorder Center, VA Palo Alto, Palo Alto, CA mkimpmr@gmail.com Disclosure
Ageing with Spinal Cord Injury
 Ageing with Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review Date October 2016 This document has been developed to provide health service
Ageing with Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review Date October 2016 This document has been developed to provide health service
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Autonomic Dysreflexia
 2 Autonomic Dysreflexia Autonomic Dysreflexia What is it? Autonomic Dysreflexia is the name given to a condition where there is a sudden and potentially lethal rise in blood pressure (BP). It is your body
2 Autonomic Dysreflexia Autonomic Dysreflexia What is it? Autonomic Dysreflexia is the name given to a condition where there is a sudden and potentially lethal rise in blood pressure (BP). It is your body
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
11/04/2011 OVERVIEW. Neurogenic Bowel Management. in adults with Spinal Cord Injury (S.C.I.) Sequence of events in normal Defecation
 Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Continence/Constipation Workshop for RNs in Long-Term Care
 Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
What is a spinal cord injury?
 Spinal Cord Injury What is a spinal cord injury? A spinal cord injury (SCI) is when the spinal cord is damaged Such damage causes 2 things: - loss or change of movement (paralysis) - loss or change of
Spinal Cord Injury What is a spinal cord injury? A spinal cord injury (SCI) is when the spinal cord is damaged Such damage causes 2 things: - loss or change of movement (paralysis) - loss or change of
Case studies: LUTS. Case 1 history. Case 1 - questions. Case 1 - outcome. Case 2 - history. Case 1 learning point 14/07/2015 DR JON REES
 Case 1 history Case studies: LUTS DR JON REES A 49 year old male comes to see you he has had gradual deterioration of his flow over the last few years- he saw a colleague of yours 6 weeks ago who recorded
Case 1 history Case studies: LUTS DR JON REES A 49 year old male comes to see you he has had gradual deterioration of his flow over the last few years- he saw a colleague of yours 6 weeks ago who recorded
Bowel Management. Part One
 Bowel Management Part One Introduction Bowel Management in Adults With Spinal Cord Injury If you have a spinal cord injury (SCI) then a regular bowel management routine is vitally important, both physically
Bowel Management Part One Introduction Bowel Management in Adults With Spinal Cord Injury If you have a spinal cord injury (SCI) then a regular bowel management routine is vitally important, both physically
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS
 Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Managing your Bowels. Below is a diagram of the different parts of the digestive system and what they do. The Digestive System:
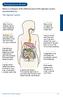 Managing your Bowels Below is a diagram of the different parts of the digestive system and what they do. The Digestive System: 1. Mouth When food is chewed, saliva starts digesting carbohydrates. 2. Oesophagus
Managing your Bowels Below is a diagram of the different parts of the digestive system and what they do. The Digestive System: 1. Mouth When food is chewed, saliva starts digesting carbohydrates. 2. Oesophagus
SUPRA PUBIC CATHETER(SPC)
 Suprapubic versus urethral catheter? When a long-term catheter to drain the bladder is advised, it can be placed in the urethra (water pipe) or suprapubically (directly into the bladder through the skin
Suprapubic versus urethral catheter? When a long-term catheter to drain the bladder is advised, it can be placed in the urethra (water pipe) or suprapubically (directly into the bladder through the skin
URINARY TRACT INFECTIONS
 URINARY TRACT INFECTIONS Learning Objectives Identify signs and symptoms that may indicate presence of UTI (both complicated and uncomplicated) List common causative organisms and risk factors for UTIs
URINARY TRACT INFECTIONS Learning Objectives Identify signs and symptoms that may indicate presence of UTI (both complicated and uncomplicated) List common causative organisms and risk factors for UTIs
Nursing Rehab Competency: Elimination
 Nursing Rehab Competency: Elimination Presented by: Nicholas Joachimides RN, BSc.N(c) Bloorview Kids Rehab Learning Objectives Basic review of anatomy and physiology of the bladder and bowel. To recognize
Nursing Rehab Competency: Elimination Presented by: Nicholas Joachimides RN, BSc.N(c) Bloorview Kids Rehab Learning Objectives Basic review of anatomy and physiology of the bladder and bowel. To recognize
Bladder Management. Why is a Bladder Program so Important?
 Bladder Management A clear understanding of the principles and skills involved in bladder management will help you prevent complications such as a urinary tract infection. Before your injury, waste products
Bladder Management A clear understanding of the principles and skills involved in bladder management will help you prevent complications such as a urinary tract infection. Before your injury, waste products
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Bladder neck incision
 Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Indwelling Urinary Catheters And Drainage systems
 If you require this leaflet in any other format, e.g., large print, please telephone 01935 384256 Indwelling Urinary Catheters And Drainage systems Useful organisations Ms Society Helpline Tel: 0808 800
If you require this leaflet in any other format, e.g., large print, please telephone 01935 384256 Indwelling Urinary Catheters And Drainage systems Useful organisations Ms Society Helpline Tel: 0808 800
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Neurogenic Bowel: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
UTI IN ELDERLY. Zeinab Naderpour
 UTI IN ELDERLY Zeinab Naderpour Urinary tract infection (UTI) is the most frequent bacterial infection in elderly populations. While urinary infection in the elderly person is usually asymptomatic, symptomatic
UTI IN ELDERLY Zeinab Naderpour Urinary tract infection (UTI) is the most frequent bacterial infection in elderly populations. While urinary infection in the elderly person is usually asymptomatic, symptomatic
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Suprapubic Catheter Insertion Clinic
 Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter Why may I need a suprapubic catheter? A suprapubic catheter enters the bladder through an incision
Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter Why may I need a suprapubic catheter? A suprapubic catheter enters the bladder through an incision
Burch Colposuspension
 Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Stool softeners are medicines like (ducolox - pericolace - senokot). You want the stool to remain soft so it is easier to empty the bowel.
 "Bowel Management" How the Body Works The food you eat and drink provides your body with many nutrients. These nutrients give you energy and help you stay healthy. As food moves through your body it breaks
"Bowel Management" How the Body Works The food you eat and drink provides your body with many nutrients. These nutrients give you energy and help you stay healthy. As food moves through your body it breaks
Urodynamic Tests. Department of Gynaecology. Patient Information
 Urodynamic Tests Department of Gynaecology Patient Information What are urodynamic tests? Urodynamic tests assess the dynamic function of the lower urinary tract. The tests assess 3 functions; The ability
Urodynamic Tests Department of Gynaecology Patient Information What are urodynamic tests? Urodynamic tests assess the dynamic function of the lower urinary tract. The tests assess 3 functions; The ability
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Hydronephrosis. What is hydronephrosis?
 What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
Suprapubic Catheter Insertion Clinic
 Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter A urinary catheter is a tube used to drain urine from the bladder. The commonest catheters are ones
Suprapubic Catheter Insertion Clinic Exceptional healthcare, personally delivered Suprapubic Catheter A urinary catheter is a tube used to drain urine from the bladder. The commonest catheters are ones
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Bladder and Bowel Symptoms Troubleshooting Tips
 Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Indwelling Urinary Catheter Template for Care Plan Development Problem No: be a last resort when all suprapubic catheter in CAUTI
 Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Guidelines for the Manual Evacuation of Faeces
 Rationale Guidelines for the Manual Evacuation of Faeces These guidelines are to provide the required information for designated registered nurses, health care assistants and bank support workers to perform
Rationale Guidelines for the Manual Evacuation of Faeces These guidelines are to provide the required information for designated registered nurses, health care assistants and bank support workers to perform
Appendix E: Continence Care and Bowel Management Program Training Presentation. Audience: For Registered Staff Release Date: December 22, 2010
 Appendix E: Continence Care and Bowel Management Program Training Presentation Audience: For Registered Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix E: Continence Care and Bowel Management Program Training Presentation Audience: For Registered Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Looking after your suprapubic catheter. Information for patients
 Looking after your suprapubic catheter Information for patients What is a suprapubic catheter? A catheter is a soft hollow tube, which is used to drain urine from the bladder. The catheter is inserted
Looking after your suprapubic catheter Information for patients What is a suprapubic catheter? A catheter is a soft hollow tube, which is used to drain urine from the bladder. The catheter is inserted
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS OVERVIEW
 Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Slide 1. Slide 2. Slide 3. A New Standard of Care for Persons with Disability: Bowel Management
 Slide 1 A New Standard of Care for Persons with Disability: Bowel Management CYNTHIA HERNANDEZ, MSN/ED.,RN,CRRN Slide 2 Objectives Describe standards for bowel management based on disability Discuss the
Slide 1 A New Standard of Care for Persons with Disability: Bowel Management CYNTHIA HERNANDEZ, MSN/ED.,RN,CRRN Slide 2 Objectives Describe standards for bowel management based on disability Discuss the
Managing your suprapubic catheter
 Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
University College Hospital. Discharge information for patients after HIFU (High Intensity Focused Ultrasound) Urology Directorate
 University College Hospital Discharge information for patients after HIFU (High Intensity Focused Ultrasound) Urology Directorate 2 If you would like this document in another language or format, or require
University College Hospital Discharge information for patients after HIFU (High Intensity Focused Ultrasound) Urology Directorate 2 If you would like this document in another language or format, or require
TRIUMPH SPINAL CORD INJURY GUIDELINES 2018
 TELE-REHABILITATION GUIDELINE Management of Acute Autonomic Dysreflexia (AD) Drafted and Finalized: February 2014 Revised: February 2018 I. Definition, assessment, and diagnostic considerations A. Definition
TELE-REHABILITATION GUIDELINE Management of Acute Autonomic Dysreflexia (AD) Drafted and Finalized: February 2014 Revised: February 2018 I. Definition, assessment, and diagnostic considerations A. Definition
Cystoscopy and urethroscopy
 Page 1 of 5 Cystoscopy and urethroscopy Introduction This leaflet is provided to give you information about undergoing cystoscopy and/or urethroscopy. What is a cystoscopy? A cystoscopy is a procedure
Page 1 of 5 Cystoscopy and urethroscopy Introduction This leaflet is provided to give you information about undergoing cystoscopy and/or urethroscopy. What is a cystoscopy? A cystoscopy is a procedure
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Bladder Dysfunction in Multiple Sclerosis. by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN
 Clinical Bulletin Information for Health Professionals Bladder Dysfunction in Multiple Sclerosis by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN Effective bladder management strategies make it
Clinical Bulletin Information for Health Professionals Bladder Dysfunction in Multiple Sclerosis by Nancy J. Holland, EdD, RN and Nancy C. Reitman, MA, RN Effective bladder management strategies make it
Sacrocolpopexy. Department of Gynaecology. Patient Information
 Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Mr B M Soni Consultant in Spinal Injuries
 Mr B M Soni Consultant in Spinal Injuries Autonomic Dysreflexia in Spinal Cord Injury Patients 1 What is autonomic dysreflexia? Autonomic dysreflexia is a condition that develops after spinal cord injury
Mr B M Soni Consultant in Spinal Injuries Autonomic Dysreflexia in Spinal Cord Injury Patients 1 What is autonomic dysreflexia? Autonomic dysreflexia is a condition that develops after spinal cord injury
Bowel Management. Part Two
 Bowel Management Part Two Bowel Management in Adults with Spinal Cord Injury Part 2 What is the goal of medications in my bowel management programme? The goal of medications as part of your bowel management
Bowel Management Part Two Bowel Management in Adults with Spinal Cord Injury Part 2 What is the goal of medications in my bowel management programme? The goal of medications as part of your bowel management
Patient Information Leaflet
 Patient Information Leaflet Background Faecal incontinence is a common health problem, affecting over 1% of community-dwelling adults (1;2). Chronic constipation may affect 3-5% of the population depending
Patient Information Leaflet Background Faecal incontinence is a common health problem, affecting over 1% of community-dwelling adults (1;2). Chronic constipation may affect 3-5% of the population depending
Having a supra pubic urinary catheter
 Having a supra pubic urinary catheter Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a supra pubic urinary catheter Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Gastrointestinal Involvement in Adult Mitochondrial Disease
 Newcastle Mitochondrial Disease Guidelines At a glance guidelines: Gastrointestinal Involvement in Adult Mitochondrial Disease For full guideline visit: http://www.newcastle-mitochondria.com/service/patient-care-guidelines/
Newcastle Mitochondrial Disease Guidelines At a glance guidelines: Gastrointestinal Involvement in Adult Mitochondrial Disease For full guideline visit: http://www.newcastle-mitochondria.com/service/patient-care-guidelines/
NHS Urinary Catheter Passport
 South Sefton Care Home Innovation Programme (CHIP) PROTOCOL 07:Urinary Catheter Passport NHS Urinary Catheter Passport Information for patients and carers The passport is a hand held patient document for
South Sefton Care Home Innovation Programme (CHIP) PROTOCOL 07:Urinary Catheter Passport NHS Urinary Catheter Passport Information for patients and carers The passport is a hand held patient document for
Male Symptom Monitor
 Male Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Please fill out each section that is relevant to your problem Have you had any of the following
Male Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Please fill out each section that is relevant to your problem Have you had any of the following
Clinical guideline Published: 8 August 2012 nice.org.uk/guidance/cg148
 Urinary incontinence in neurological disease: assessment and management Clinical guideline Published: 8 August 2012 nice.org.uk/guidance/cg148 NICE 2018. All rights reserved. Subject to Notice of rights
Urinary incontinence in neurological disease: assessment and management Clinical guideline Published: 8 August 2012 nice.org.uk/guidance/cg148 NICE 2018. All rights reserved. Subject to Notice of rights
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW. Date: 17/10/2016
 EXPERT MEDICAL REPORT FOR THE COURT ON BREACH OF DUTY Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW Date: 17/10/2016 -------------------------------------------------------------------
EXPERT MEDICAL REPORT FOR THE COURT ON BREACH OF DUTY Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW Date: 17/10/2016 -------------------------------------------------------------------
