Thermo-expandable metallic urethral stents for managing recurrent bulbar urethral strictures: To use or not?
|
|
|
- Brittney Howard
- 5 years ago
- Views:
Transcription
1 Arab Journal of Urology (2013) 11, Arab Journal of Urology (Official Journal of the Arab Association of Urology) STONES/ENDOUROLOGY ORIGINAL ARTICLE Thermo-expandable metallic urethral stents for managing recurrent bulbar urethral strictures: To use or not? Mohamed M. Abdallah *, Mohamed Selim, Tarek Abdelbakey Urology Department, Menoufiya University Hospital, Menoufiya, Egypt Received 18 November 2012, Received in revised form 17 December 2012, Accepted 18 December 2012 Available online 24 January 2013 KEYWORDS Bulbar urethral stricture; Stents; Recurrent stricture ABBREVIATIONS DSD, detrusor sphincter dyssynergia; DVIU, direct visual internal urethrotomy; PVR, postvoid residual (urine) Abstract Objectives: To assess the role of temporary thermally expandable urethral stents in maintaining urethral patency in patients with a recurrent bulbar urethral stricture. Patients and methods: Twenty-three men with a recurrent bulbar urethral stricture after several attempts at direct visual internal urethrotomy (DVIU) and/ or failed urethroplasty were managed with a thermally expandable, biocompatible nickel titanium alloy urethral stent (MemokathÒ MK044, Pnn Medical, Kvistgaard, Denmark). The stents were applied by a special mounting device via a rigid urethroscope after DVIU. All patients were followed using plain radiography, uroflowmetry and urine analysis every 3 months for 1 year, and then every 6 months. Results: The mean (SD) age of the patients was 55.4 (7.3) years and the mean (SD) stricture length was 3.6 (1.2) cm. All patients tolerated the stent, with minimal discomfort in some patients. Four patients (17%) had urinary tract infections, three (13%) had haematuria, three (13%) had obstructed stents due to encrustation, in five (22%) the stent migrated, and two patients had no delayed complications. The mean (SD) follow-up was 17.4 (6.1) months. * Corresponding author. Address: Department of Urology, Faculty of Medicine, Shibin Elkom, Minofia, Egypt. Tel.: address: mmarzouk@yahoo.com (M.M. Abdallah). Peer review under responsibility of Arab Association of Urology. Production and hosting by Elsevier X ª 2013 Arab Association of Urology. Production and hosting by Elsevier B.V. All rights reserved.
2 86 Abdallah et al. Conclusion: Urethral stenting with nickel titanium alloy thermally expandable stents can be an acceptable temporary procedure for patients with recurrent bulbar urethral strictures who are unfit for or who refuse urethroplasty. However, they have limitations; the search for an ideal urethral stent continues. ª 2013 Arab Association of Urology. Production and hosting by Elsevier B.V. All rights reserved. Introduction A urethral stricture results from a scarring process that affects the anterior urethra, with subsequent spongiofibrosis that is gradually progressive and results in a decrease in the diameter of the urethral lumen. Patients usually start to complain of obstructive symptoms, according to the severity of the obliteration [1,2]. A definitive diagnosis can be made with an ascending urethrogram coupled with diagnostic cystoscopy [3]. The use of ultrasonography has been advocated as a reliable method to define the extent of spongiofibrosis and the absolute length of the urethral stricture [4]. The treatment plan for a urethral stricture includes variable options, e.g. dilatation, urethrotomy, stenting and reconstructive surgical techniques, and no one technique is appropriate for all stricture diseases [5]. Urethral dilatation alone or coupled with direct visual internal urethrotomy (DVIU) is not curative in all cases, but can be in selected patients [6]. DVIU is especially suitable for a short stricture in the bulbar urethra with no spongiofibrosis, has high failure rates when the stricture is long, and should not be used in the penile urethra. Also, several failed DVIU procedures compromise the chances of success in a future urethroplasty [5]. Urethroplasty remains the best option, with higher success rates and a satisfactory outcome, when indicated [6]. Urethral stents are another method used to oppose the forces of wound contraction after internal urethrotomy or dilatation. Removable urethral stents are designed to prevent the process of epithelialisation from incorporating the stent into the urethral wall, and are often left in place for up to 6 12 months before they are removed. Table 1 [7 18] shows the indications, complications and success rates of different types of stents, as given in previous reports. A thermo-expandable stent with an inherited shape memory, made of Nitinol, has been assessed in many studies in the USA, assessing its efficacy as a temporary treatment for urethral strictures [7]. In the present study we assessed the role of temporary thermo-expandable urethral stents in maintaining urethral patency in patients with a recurrent bulbar urethral stricture. Patients and methods This study was conducted in the Urology department of Menoufiya University Hospital, Menoufiya University, Egypt, from August 2008 to November The study was reviewed and approved by the hospital ethics committee. The study included a heterogeneous group of 23 men who presented with symptoms of BOO due to a recurrent urethral stricture. Most of the patients had undergone dilatation or DVIU and urethroplasty. The study included patients who had a recurrent stricture of the bulbar urethra, referred to treatment, that was 50 mm long on urethrography and with 10 mm of healthy urethral tissue distal to the external sphincter. Patients were excluded if there was <10 mm of visibly healthy bulbar urethral tissue distal to the external sphincter, or any urological condition that would require additional urethral instrumentation, e.g. BPH requiring treatment, active prostate cancer, bladder malignancy, or recurrent urinary stone formation. Patients were counselled about their condition and the possible management options. Patients who chose stent insertion were informed about possible complications and disadvantages. Written informed consent was obtained from all patients. Preoperative preparation All patients had a history taken, a general and local examination, preoperative laboratory tests and retrograde urethrography, uroflowmetry, an estimate of their postvoid residual (PVR) urine volume, and urethroscopy at the time of the stent insertion. Instrumentation The thermo-expandable stent (MemokathÒ MK044, Pnn Medical, Kvistgaard, Denmark) for bulbar urethral strictures was used; this is a temporary stent, made of a nickel titanium alloy that has a shape memory feature [8]. This alloy is present in two crystalline forms, the more rigid form holding the memorised shape of the Memokath at body temperature and higher. The other form is softer and pliable; transition to this form takes place when the alloy is cooled to 10 C [19]. The stent is available in lengths from 30 to 70 mm in intervals of 10 mm. It expands from 24 to 44 F at its proximal end, forming a cone that fixes it to the urethra and prevents migration. Operative procedure The operating table for insertion should have available urethral dilators (up to 26 F), a guidewire (0.09 mm,
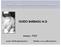
3 Thermo-expandable metallic urethral stents for managing recurrent bulbar urethral strictures 87 Table 1 Study Indications, complications and success rates of different types of stents in previous studies. No. of patients Stent type Indication Complications, n or n (%) Mean follow-up Success, n or (months) n (%) UTI Encrustation Migration Hyperplasia [9] 175 Urolume BUS 15 (11) NS 7 (4) All had ES (93) [11] 29 Memokath DSD 10 (35) 14 (48) 7 (24) NS 21 NS [12] 8 Medinvent wallstent BUS NS NS NS All had ES 8 NS [7] 18 Metallic coil self-expanding BUS 7 (39) No NS No 8 17 (94) [13] 20 Expandable titanium BPH & BUS No No No No (75) [14] 7 Medinvent wallstent BUS NS NS NS [15] 49 Memotherm 25 BPH 21 BUS-otomy NS NS NS 2 (4) (91) [16] 12 Medinvent wallstent DSD No No No No 60 5 [10] 60 Urolume BUS NS NS NS NS (87) [8] 211 Memokath BPH (6) No (13) NS 96 (63) [18] 13 Urolume Posterior US 5 NS 2 NS 18 7 [17] 10 Memokath BUS (B)US, (bulbar) urethral stricture; NS, not specified; ES, encrustation of the stent inch) with a straight tip, a 50 ml plastic syringe, a thermometer, two markers and a ruler. An antibiotic was administered intravenously before the procedure. Most patients received spinal anaesthesia and some received local anaesthesia with intra-urethral 2% lidocaine gel 5 10 min before the procedure, and a mild sedative (midazolam) at a dose of 0.03 mg/kg given slowly over at least 2 min [20]. The patients were placed in the lithotomy position, prepared and draped appropriately; cysto-urethroscopy was used to assess the site of the urethral stricture and exclude the presence of stones or neoplasia. The urethral strictures were treated by internal urethrotomy to a minimum diameter of 26 F, then the length of the stricture assessed to define the appropriate length of the Memokath stent, based on the estimated stricture length plus 2.0 cm to allow for a 10-mm overlap at either end of the stricture. The three retaining straps from the Memokath transport shell were removed using a scalpel, the transport shells removed from the stent delivery system, and the mandrel was pushed out of the delivery system, by inserting the cystoscope lens into the hub of the delivery system. The locking collar at the base of the insertion sheath was then rotated clockwise. A soft rubber ring inside the collar is compressed to create a watertight junction between the sheath and the cystoscope lens. Sterile water or saline is connected at 635 C to the stopcock and the light source is mounted. The stent, on its introducing sheath, is mounted onto the cystoscope so that the tip of the cystoscope is clear of the stent by 2 3 mm, the cystoscope is advanced until the tip passes 1 cm proximal to the proximal end of the stricture, then 50 ml of hot water (50 C) is flushed through the cystoscope. This expands the proximal 4 6 mm into a cone shape (44 F) which locks the stent into position. The stent is released from the sheath when the cystoscope lens is withdrawn from the black connector at the tip of the stent. Under direct vision, while the outer sheath is steady, the joined inner sheath and the cystoscope lens are gently retracted from the outer sheath until the black connector at the tip of the introducer is outside the stent. The stent was then released [8]. The procedure was done as one-day surgery. Follow-up An antibiotic was administered intravenously for 3 days after the procedure, and then oral antibiotics for 7 days; analgesics were given on demand [21]. Patients were discharged after taking a control plain film, uroflowmetry and an estimate of the PVR, to ensure the appropriate position and function of the stent. The patients were asked to take vitamin C to acidify their urine and thus decrease the incidence of encrustation. Patients were followed up by uroflowmetry, urine analysis and plain radiography at 2 weeks after the procedure and then every 3 months for the first year, and then every 6 months. For stent removal the patients had local intra-urethral anaesthesia as noted above. Cold saline (5 10 C) was used as the irrigant, and diagnostic cysto-urethroscopy was used to check the distal end of the Memokath stent. The tip of the stent was grasped by forceps and pulled distally, then released turn-by-turn linearly (Figs. 1 and 2) [19]. Results The mean (SD) age of the 23 patients with a recurrent bulbar urethral stricture was 55.4 (7.3) years. All patients had a history of DVIU, dilatations and urethroplasties. The mean (SD, range) preoperative flow rate was 4.6 (1.2, 3 7) ml/s and the preoperative PVR volume was 165 (19, ) ml. The mean (SD) stricture
4 88 Abdallah et al. Figure 1 Impact of the stent rings on the urethra. managed conservatively, with no stent removal required. Urethral hyperplasia was noted in two patients (8%) who presented with lower urinary tract obstructive symptoms, and the diagnosis was confirmed by cystoscopy; they required removal of the stents. Three patients (13%) had obstructed stents due to encrustation during the first 6 months, and needed lithotripsy to clear the encrustation, which failed in one and the stent was exchanged (Fig. 2). In five patients (22%) the stent migrated, requiring exchange and correctly positioned new stents (Fig. 3). Two patients felt uncomfortable with the stent and had their stent removed at their request. Two patients were free of delayed complications. The mean (SD) follow-up was 17.4 (6.1) months. Thus overall, 10 patients (43%) developed complications (migration, urethral hyperplasia and encrustation) that required intervention. Discussion Figure 2 Stent removal. length was 3.6 (1.2) cm. The procedure was done under spinal anaesthesia in 18 patients (78%) and with intraurethral xylocaine gel and a mild sedative in five (22%). The mean (SD) operative duration was 34 (9) min. All patients tolerated the stent, with minimal discomfort in some patients. Perineal pain occurred in six patients (26%) that was transient and disappeared within a few weeks of follow-up. The urinary flow rate improved after stent insertion, to a mean (SD, range) of 21 (2.5, 17 25) ml/s. The PVR volume decreased after stent insertion to 50 (14, 30 70) ml. Four patients (17%) had UTIs twice or three times during the first 3 months of follow-up, and these were controlled by appropriate antibiotics, according to urine culture and antibiotic-sensitivity tests. Three patients (13%) had intermittent gross haematuria during the first 2 weeks after insertion. The haematuria was initially painful; one patient complained of the presence of a few drops of blood at the urethral meatus, and was Urethral stents were first introduced in 1980 by Fabian [22] for treating infravesical obstruction due to BPH. Subsequently, the indications were expanded to include the treatment of detrusor sphincter dyssynergia (DSD) due to spinal cord injury and, in 1988, the treatment of urethral strictures [23]. Thermo-expandable urethral stents were first introduced by Soni et al. [24] to treat patients with DSD. In the present series, 23 patients with recurrent bulbar urethral strictures were treated with the Memokath thermo-expandable urethral stent. The insertion of these stents was simple and minimally invasive, comparable with dilatation and DVIU. Unfortunately the stents failed to give good results during the long-term followup. This situation might differ in the near future, as there are further reports of urethroplasty and its acceptable results [25,26]. The main indications for their use are recurrent bulbar urethral strictures after failure of several previous urethroplasties and DVIUs, or in patients with medical comorbidities who are unfit for major surgery, or for those who refuse urethroplasty [27]. In the present study the original cause of the stricture had no effect on the decision to insert a stent or on the incidence of complications. This was similar to the results reported by Palminteri et al. [28] in their study of the management of patients with failed urethral stents. There was an appropriate stent position and function in all the present patients immediately after stent insertion, with an improvement in the flow rate and PVR. Also, Perry et al. [8] reported that most patients treated with the Memokath stent for BOO of the prostatic urethra voided immediately after the procedure, so that the outcome of stent placement was immediately apparent. Recurrent UTI was noted in 17% of the present 23 patients, which was lower than the rate observed by Badlani et al. [9],
5 Thermo-expandable metallic urethral stents for managing recurrent bulbar urethral strictures 89 Figure 3 (A) A urethral stent normally placed; (B) Urethral stent migrated upwards into the prostatic urethra. who reported UTI in 27% of the 60 patients in whom a Urolume stent was inserted and who were followed for 2 years. This difference might be due to the small sample size and the short follow-up in our study (the mean follow-up was 17.4 months). The incidence of UTI might be attributed to a previous history of UTI, together with a prolonged obstructed urinary flow and the presence of the stent as a foreign body. All these factors predispose to a high incidence of UTI that also might be resistant to treatment. Haematuria was present in 13% of the present patients, a higher rate than reported by Perry et al. [8] of 3% in their cases. This was explained by the previous DVIU done during stent insertion, and added vigorous perineal trauma (as during riding a bicycle). Although the Memokath stent has a funnel shape at one end to resist migration, the stent migrated in 22% of the present patients (five of 23). Migration was related to accidental perineal trauma, a faulty trial of catheterisation, and the presence of the stricture close to the sphincter. This was a higher rate than reported by Perry et al. [8], who had stent migration in 13% of their cases (29 patients of 211), and because the Urolume stents do not migrate due to their incorporation into the wall of the urethra [10]. Obstructive symptoms and a decreased flow rate were reported in eight of the present patients (35%). The symptoms became gradually more severe over 6 9 months. Encrustation was noted in five of these patients, that necessitated urethroscopy and lithotripsy to remove the encrusted material. Perry et al. [8] found encrustation in 2% of their cases (five of 211) and mentioned that the reason for the lack of encrustation on these stents was not known, but was attributed to the exceptional smoothness of the surface of the stent and the inert property of the alloy. Encrustation in the present patients was attributed to the higher incidence of UTI and the prolonged obstruction of urinary flow. Also, noncompliance of some patients with the prescribed medications for urine acidification predisposed them to encrustation. Urethral hyperplasia was noted at the ends of the stent in two patients (8%) who gradually developed obstructive symptoms after 9 11 months. This was managed by transurethral resection after stent removal. This rate was slightly lower than that reported by Badlani et al. [9] in their study of the Urolume stent (41.3%). The narrowing was the result of urethral epithelium overgrowth through the interstices of the stent. The low incidence of urethral hyperplasia with the Memokath stent was attributed to the tight coiling of the stent, the inert property of the nickel titanium alloy from which it is made, and the short duration of indwelling. Yachia [29] reported that with the current urethral stents, other than the Memokath, occasional tissue ingrowth between the loops of the coils, and reactive tissue proliferation at the sphincter end, can cause partial or complete obliteration of the stent. The reason for such reactive tissue proliferation is that the radial stiffness of the sphincter end of the stent causes repeated friction to the urethral wall during opening and closing of the sphincter. Also, Eisenberg et al. [18] found that the most common surgical interventions required for failed urethral stent were transurethral resection of the hyperplasia (32%) and endoscopic litholapaxy for stent encrustation or stones (17%). In the present study the occurrence of complications increased with time. The mean (SD) period for encrustation was 9.8 (2) months, while that of hyperplasia was 10 (1.4) months, and that for migration was 10 (3) months. With an increasing follow-up the stents tended to have a high failure rate that ultimately required removal of the stents in 35% of the patients after a mean (SD) period of 9 (3) months. This period was shorter than that reported by Chapple and Bhargava [27] in their study on managing the failure of a permanently implanted urethral stent, as the mean (range) duration for the stents to remain in situ before their removal due to failure was 26 (3 85) months. This suggested to us that the Memokath stent was best reserved for use as a temporary stent and not for permanent use. The failure rate in our study was 52% (12 patients) and of these, eight stents were removed due to complications, for migration in five, in one for encrustation, in
6 90 Abdallah et al. two for urethral hyperplasia and in four as the patients were unwilling to continue with the stent. This rate was similar to that reported by Mehta and Tophill [11]. We had no difficulty in removing the Memokath stents, which might be attributed to the synthetic nature of the stents and the short period of insertion. This contrasts with the report by Elkassaby et al. [30], that failure of a permanently implanted urethral stent represents a significant therapeutic challenge, which often leads to a difficult substitution procedure, with consequent limitation of the success of the procedure. As permanent urethral stents tend to be incorporated into the wall of the urethra, this hinders their removal. In conclusion, we recommend only the temporary use of thermo-expandable (Memokath) stents for patients with previously failed urethroplasties who refuse further surgical management, or those who are medically unfit for urethroplasty. The long-term results of the Memokath stent were not encouraging and the patients had complications related to the stent; they are also expensive. The use of these stents was associated with complications that sometimes required exchange or removal of the stent. The overall experience with Memokath stents was disappointing, and thus we use this stent only with highly selected patients, as noted, and do not use them when urethral reconstruction is feasible. Conflict of interest No conflict of interest. Source of Funding None. References [1] Bhargava S, Chapple CR. Buccal mucosal urethroplasty: is it the new gold standard? BJU Int 2004;93: [2] Bhargava S, Chapple CR, Bullock AJ, Layton C, MacNeil S. Tissue-engineered buccal mucosa for substitution urethroplasty. BJU Int 2004;93: [3] Chapple CR. The importance of endoscopic surveillance in the follow up of patients with urethral stricture disease. J Urol 2009;167(Suppl.). [4] McAninch JW, Laing Jr FC. Sonourethrography in the evaluation of urethral stricture. J Urol 1988;139: [5] Peterson AC, Webster GD. Management of urethral stricture disease: developing options for surgical intervention. BJU Int 2004;94: [6] Andrich DE, Mundy AR. Urethral strictures and their surgical treatment. BJU Int 2000;86: [7] Yachia D, Beyar M. Temporarily implanted urethral coil stent for the treatment of recurrent urethral strictures: a preliminary report. J Urol 1991;146: [8] Perry MJ, Roodhouse AJ, Gidlow AB, Spicer TG, Ellis BW. Thermo-expandable intraprostatic stents in bladder outlet obstruction: an 8-year study. BJU Int 2002;90: [9] Badlani GH, Press SM, Defalco A, Oesterling JE, Smith AD. Urolume endourethral prosthesis for the treatment of urethral stricture disease: long-term results of the North American Multicenter UroLume Trial. Urology 1995;45: [10] Sertcelik N, Sagnak L, Imamoglu A, Temel M, Tuygun C. The use of self-expanding metallic urethral stents in the treatment of recurrent bulbar urethral strictures: long-term results. BJU Int 2000;86: [11] Mehta SS, Tophill PR. Memokath stents for the treatment of detrusor sphincter dyssynergia (DSD) in men with spinal cord injury: the Princess Royal Spinal Injuries Unit 10-year experience. Spinal cord 2006;44:1 6. [12] Milroy E. Stents in therapy of urethral strictures. Urologe A 1998;37:51 5. [13] Boullier JA, Parra RO. Prostatic titanium urethral stents. A new treatment option for obstructive uropathy: early clinical results and indications. ASAIO Trans 1991;37:M [14] Baert L, Verhamme L, Van Poppel H, Vandeursen H, Baert J. Long-term consequences of urethral stents. J Urol 1993;150: [15] Ricciotti G, Bozzo W, Perachino M, Pezzica C, Puppo P. Heatexpansible permanent intraurethral stents for benign prostatic hyperplasia and urethral strictures. J Endourol 1995;9: [16] McFarlane IP, Foley SJ, Shah PJ. Long-term outcome of permanent urethral stents in the treatment of detrusor-sphincter dyssynergia. Br J Urol 1996;78: [17] Abdallah M, Bissada NM. Experience with urethral stents for recurrent urethral stricture. Urology 2009;74:S87 8. [18] Eisenberg ML, Elliott SP, McAninch JW. Preservation of lower urinary tract function in posterior urethral stenosis: selection of appropriate patients for urethral stents. J Urol 2007;178: [19] Barber NJ, Roodhouse AJ, Rathenborg P, Nordling J, Ellis BW. Ease of removal of thermo-expandable prostate stents. BJU Int 2005;96: [20] Song YS, Song ES, Kim KJ, Park YH, Ku JH. Midazolam anesthesia during rigid and flexible cystoscopy. Urol Res 2007;35: [21] Turan H, Balci U, Erdinc FS, Tulek N, Germiyanoglu C. Bacteriuria, pyuria and bacteremia frequency following outpatient cystoscopy. Int J Urol 2006;13:25 8. [22] Fabian KM. The intra-prostatic partial catheter (urological spiral) (author s transl). Urologe A 1980;19: [23] Milroy EJ, Chapple CR, Cooper JE, Eldin A, Wallsten H, Seddon AM, et al. A new treatment for urethral strictures. Lancet 1988;1: [24] Soni BM, Vaidyanatham S, Krishnan KR. Use of Memokath, a second generation urethral stent for relief of urinary retention in male spinal cord injured patients. Paraplegia 1994;32: [25] Palminteri E. Stents and urethral strictures: a lesson learned? Eur Urol 2008;54: [26] Palminteri E, Berdondini E, Fusco F, Nunzio CD, Giannitsas K, Shokeir AA. Versatility of the ventral approach in bulbar urethroplasty using dorsal, ventral or dorsal plus ventral oral grafts. Arab J Urol 2011;10: [27] Chapple CR, Bhargava S. Management of the failure of a permanently implanted urethral stent a therapeutic challenge. Eur Urol 2008;54: [28] Palminteri E, Gacci M, Berdondini E, Poluzzi M, Franco G, Gentile V. Management of urethral stent failure for recurrent anterior urethral strictures. Eur Urol 2010;57: [29] Yachia D. Recent advances in ureteral stents. Curr Opin Urol 2008;18: [30] Elkassaby AA, Al-Kandari AM, Shokeir AA. The surgical management of obstructive stents used for urethral strictures. J Urol 2007;178:204 7.
Long-term results of permanent memotherm urethral stent in the treatment of recurrent bulbar urethral strictures
 ORIGINAL Article Vol. 40 (1): 80-86, January - February, 2014 doi: 10.1590/S1677-5538.IBJU.2014.01.12 Long-term results of permanent memotherm urethral stent in the treatment of recurrent bulbar urethral
ORIGINAL Article Vol. 40 (1): 80-86, January - February, 2014 doi: 10.1590/S1677-5538.IBJU.2014.01.12 Long-term results of permanent memotherm urethral stent in the treatment of recurrent bulbar urethral
Early Experience With a Thermo-Expandable Stent (Memokath) for the Management of Recurrent Urethral Stricture
 www.kjurology.org http://dx.doi.org/.4/kju..54..85 Endourology/Urolithiasis Early Experience With a Thermo-Expandable Stent (Memokath) for the Management of Recurrent Urethral Stricture Hyun Su Jung, Joon
www.kjurology.org http://dx.doi.org/.4/kju..54..85 Endourology/Urolithiasis Early Experience With a Thermo-Expandable Stent (Memokath) for the Management of Recurrent Urethral Stricture Hyun Su Jung, Joon
Recanalisation of urethral strictures with new-generation temporary covered biocompatible metal endoprostheses
 Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Policy #: 213 Latest Review Date: September 2012
 Name of Policy: Temporary Prostatic Stent Policy #: 213 Latest Review Date: September 2012 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
Name of Policy: Temporary Prostatic Stent Policy #: 213 Latest Review Date: September 2012 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Japanese Neurogenic Bladder Society Meeting. Kofu - Japan. September 29th - October 1st, 2010
 Japanese Neurogenic Bladder Society Meeting Kofu - Japan September 29th - October 1st, 2010 Reconstruction of penile and bulbar urethra Evaluation of anterior urethral stricture Urethrography Retrograde
Japanese Neurogenic Bladder Society Meeting Kofu - Japan September 29th - October 1st, 2010 Reconstruction of penile and bulbar urethra Evaluation of anterior urethral stricture Urethrography Retrograde
Balancing clinical outcomes and quality of life aspects in the treatment of LUTS/BPH van Dijk, M.M.
 UvA-DARE (Digital Academic Repository) Balancing clinical outcomes and quality of life aspects in the treatment of LUTS/BPH van Dijk, M.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Balancing clinical outcomes and quality of life aspects in the treatment of LUTS/BPH van Dijk, M.M. Link to publication Citation for published version (APA): van
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use
 Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Title risk patients with urinary retentio. Citation 泌尿器科紀要 (2005), 51(4):
 Title Urethral stent (Angiomed-Memotherm) risk patients with urinary retentio Uchikoba, Takushi; Horiuchi, Kazuta Author(s) Oka, Fumiatsu; Saitoh, Yuka; Tsuboi Taiji Citation 泌尿器科紀要 (2005), 51(4): 235-239
Title Urethral stent (Angiomed-Memotherm) risk patients with urinary retentio Uchikoba, Takushi; Horiuchi, Kazuta Author(s) Oka, Fumiatsu; Saitoh, Yuka; Tsuboi Taiji Citation 泌尿器科紀要 (2005), 51(4): 235-239
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Urethral Stricture Management. AUA Guidelines. Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas
 Urethral Stricture Management AUA Guidelines Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas Urethral Stricture Guidelines Systematic peer-reviewed literature review
Urethral Stricture Management AUA Guidelines Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas Urethral Stricture Guidelines Systematic peer-reviewed literature review
BULKAMID STANDARD OPERATING PROCEDURE
 BULKAMID STANDARD OPERATING PROCEDURE Contents 1 1 2 3-4 5-6 5-6 7 9-12 9 10 11 12 13 13 13 15 16 Products Bulkamid multiple use instruments Bulkamid single use instruments The Bulkamid system Pre-procedure
BULKAMID STANDARD OPERATING PROCEDURE Contents 1 1 2 3-4 5-6 5-6 7 9-12 9 10 11 12 13 13 13 15 16 Products Bulkamid multiple use instruments Bulkamid single use instruments The Bulkamid system Pre-procedure
European Urology 43 (2003)
 European Urology European Urology 43 (2003) 539 543 The Use of the Memokath TM Stent in thetreatment of Detrusor Sphincter Dyssynergia in Spinal Cord Injury Patients: A Single-Centre Seven-Year Experience
European Urology European Urology 43 (2003) 539 543 The Use of the Memokath TM Stent in thetreatment of Detrusor Sphincter Dyssynergia in Spinal Cord Injury Patients: A Single-Centre Seven-Year Experience
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Thermo-expandable intraprostatic stents in bladder outlet obstruction: an 8-year study
 BJU International (22), 9, 216 223 Thermo-expandable intraprostatic stents in bladder outlet obstruction: an 8-year study M.J.A. PERRY, A.J. ROODHOUSE, A.B. GIDLOW, T.G. SPICER and B.W. ELLIS Department
BJU International (22), 9, 216 223 Thermo-expandable intraprostatic stents in bladder outlet obstruction: an 8-year study M.J.A. PERRY, A.J. ROODHOUSE, A.B. GIDLOW, T.G. SPICER and B.W. ELLIS Department
urethral stricture recurrence after internal urethrotomy.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 9-, p-issn: 9-.Volume, Issue Ver. II (Nov. ), PP - www.iosrjournals.org Effects of Intralesional Triamcinalone injection following Internal
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 9-, p-issn: 9-.Volume, Issue Ver. II (Nov. ), PP - www.iosrjournals.org Effects of Intralesional Triamcinalone injection following Internal
Colonic Metal Stents MAKING A DIFFERENCE TO HEALTH
 Colonic Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Colonic Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents MAKING A DIFFERENCE TO HEALTH
 Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Introduction. Etiology. Incidence 2/18/17
 Introduction Urethral stricture refers to narrowing of the urethral lumen from scar tissue. Usually used for anterior urethral disease Posterior Urethral strictures usually is a stenotic process after
Introduction Urethral stricture refers to narrowing of the urethral lumen from scar tissue. Usually used for anterior urethral disease Posterior Urethral strictures usually is a stenotic process after
THE BULKING AGENT WITH LONG-LASTING EFFECT!
 THE BULKING AGENT WITH LONG-LASTING EFFECT! Urogyn BV Transistorweg 5a 6534 AT Nijmegen The Netherlands t +31(0) 24 711 41 30 info@urogynbv.com www.urogynbv.com THE FIRST INJECTABLE IMPLANT THAT CAN COMPETE
THE BULKING AGENT WITH LONG-LASTING EFFECT! Urogyn BV Transistorweg 5a 6534 AT Nijmegen The Netherlands t +31(0) 24 711 41 30 info@urogynbv.com www.urogynbv.com THE FIRST INJECTABLE IMPLANT THAT CAN COMPETE
Intraurethral Catheter: Alternative Management for Urinary
 Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 113-117 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 113-117 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Complications and outcomes of JJ stenting of the ureter in urological practice: A single-centre experience I
 Arab Journal of Urology (2012) 10, 372 377 Arab Journal of Urology (Official Journal of the Arab Association of Urology) www.sciencedirect.com STONES/ENDOUROLOGY ORIGINAL ARTICLE Complications and outcomes
Arab Journal of Urology (2012) 10, 372 377 Arab Journal of Urology (Official Journal of the Arab Association of Urology) www.sciencedirect.com STONES/ENDOUROLOGY ORIGINAL ARTICLE Complications and outcomes
Medical technologies guidance Published: 1 February 2018 nice.org.uk/guidance/mtg35
 Memokath-051 stent for ureteric obstruction Medical technologies guidance Published: 1 February 2018 nice.org.uk/guidance/mtg35 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Memokath-051 stent for ureteric obstruction Medical technologies guidance Published: 1 February 2018 nice.org.uk/guidance/mtg35 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size
 Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Combined Antegrade And Retrograde Endoscopic Realignment Of Traumatic Urethral Disruption
 ISPUB.COM The Internet Journal of Urology Volume 7 Number 1 Combined Antegrade And Retrograde Endoscopic Realignment Of Traumatic Urethral Disruption I SO, O OA, E JO, B BO, A RA Citation I SO, O OA, E
ISPUB.COM The Internet Journal of Urology Volume 7 Number 1 Combined Antegrade And Retrograde Endoscopic Realignment Of Traumatic Urethral Disruption I SO, O OA, E JO, B BO, A RA Citation I SO, O OA, E
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Clinical Commissioning Policy Proposition: Urethroplasty for benign urethral strictures in adult men
 Clinical Commissioning Policy Proposition: Urethroplasty for benign urethral strictures in adult men Reference: NHS England B14X06/01 Information Reader Box (IRB) to be inserted on inside front cover for
Clinical Commissioning Policy Proposition: Urethroplasty for benign urethral strictures in adult men Reference: NHS England B14X06/01 Information Reader Box (IRB) to be inserted on inside front cover for
Despite developments in the surgical techniques,
 Reconstructive Urology Long-term Results of Small Intestinal Submucosa Graft in Bulbar Urethral Reconstruction Enzo Palminteri, Elisa Berdondini, Ferdinando Fusco, Cosimo De Nunzio, and Andrea Salonia
Reconstructive Urology Long-term Results of Small Intestinal Submucosa Graft in Bulbar Urethral Reconstruction Enzo Palminteri, Elisa Berdondini, Ferdinando Fusco, Cosimo De Nunzio, and Andrea Salonia
The use of Amplatz renal dilators in the minimally invasive management of complex urethral strictures
 301 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY The use of Amplatz renal dilators in the minimally invasive management of complex urethral strictures Michael Nomikos 1, Sarantis Papanikolaou
301 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY The use of Amplatz renal dilators in the minimally invasive management of complex urethral strictures Michael Nomikos 1, Sarantis Papanikolaou
Subject: Temporary Prostatic Stent and Prostatic Urethral Lift
 02-54000-21 Original Effective Date: 03/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Temporary Prostatic Stent and Prostatic Urethral Lift THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-54000-21 Original Effective Date: 03/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Temporary Prostatic Stent and Prostatic Urethral Lift THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
TRANSURETHRAL RESECTION
 TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
Gastric / EUS Metal Stents
 Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Reconstructive Surgery
 Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Urethroplasty for Long Anterior Urethral Strictures Report of Long-term Results
 Reconstructive Surgery Urethroplasty for Long Anterior Urethral Strictures Report of Long-term Results Mahmoudreza Moradi, As ad Moradi Introduction: We reviewed the long-term outcome of substitution urethroplasty
Reconstructive Surgery Urethroplasty for Long Anterior Urethral Strictures Report of Long-term Results Mahmoudreza Moradi, As ad Moradi Introduction: We reviewed the long-term outcome of substitution urethroplasty
THE PLACE OF ENDOSCOPIC URETHROTOMY IN THE MANAGEMENT OF URETHRAL STRICTURE
 THE PLACE OF ENDOSCOPIC URETHROTOMY IN THE MANAGEMENT OF URETHRAL STRICTURE Pages with reference to book, From 99 To 102 J.P. Mitchell ( Dept. of Surgery, Bristol Royal Infirmary, Bristol BS2 8HW, U.K.
THE PLACE OF ENDOSCOPIC URETHROTOMY IN THE MANAGEMENT OF URETHRAL STRICTURE Pages with reference to book, From 99 To 102 J.P. Mitchell ( Dept. of Surgery, Bristol Royal Infirmary, Bristol BS2 8HW, U.K.
Single-stage repair of obliterated anterior urethral strictures using buccal mucosa graft and dorsal penile skin flap
 International Journal of Urology (2019) 26, 90--95 doi: 10.1111/iju.13816 Original Article: Clinical Investigation Single-stage repair of obliterated anterior urethral strictures using buccal mucosa graft
International Journal of Urology (2019) 26, 90--95 doi: 10.1111/iju.13816 Original Article: Clinical Investigation Single-stage repair of obliterated anterior urethral strictures using buccal mucosa graft
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 10 th Mediterranean Congress of Urology 10 and 8 th Congress of Pan African
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 10 th Mediterranean Congress of Urology 10 and 8 th Congress of Pan African
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
MP A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction. Gaines W. Hammond Jr.
 MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
You have been booked for a. Flexible Cystoscopy. Under Local Anaesthetic
 You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
Transurethral Resection of Prostate (TURP)
 Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Transurethral Resection of Prostate (TURP) Department of Urology Patient Information What What and and where where is the is prostate? the prostate? The prostate is a small gland, about the size of a walnut,
Center for Reconstructive Urethral Surgery Guido Barbagli Center for Reconstructive Urethral Surgery Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: info@urethralcenter.it Website: www.urethralcenter.it SHANGHAI February 6 8, 2009 Prof. Qiang FU Professor FU day Professor FU and night Anterior urethroplasty using
Guido Barbagli Arezzo - Italy E-mail: info@urethralcenter.it Website: www.urethralcenter.it SHANGHAI February 6 8, 2009 Prof. Qiang FU Professor FU day Professor FU and night Anterior urethroplasty using
Experience the Innovative Therapy for Benign Prostate Enlargement
 Experience the Innovative Therapy for Benign Prostate Enlargement A Guide to Treatment of Benign Prostatic Hyperplasia 1. 2. The Prostate The prostate gland is a part of the male reproductive system. A
Experience the Innovative Therapy for Benign Prostate Enlargement A Guide to Treatment of Benign Prostatic Hyperplasia 1. 2. The Prostate The prostate gland is a part of the male reproductive system. A
Introduction. Key Words: temporary prostatic stent, prostatic stent, urethral stent, benign prostatic hyperplasia, colonization
 Infectious complications associated with the use of temporary prostatic urethral stents in patients with benign prostatic hyperplasia Haidar M. Abdul-Muhsin, MBChB, 1 Nicholas J. Jakob, 1 Ryan M. McLemore,
Infectious complications associated with the use of temporary prostatic urethral stents in patients with benign prostatic hyperplasia Haidar M. Abdul-Muhsin, MBChB, 1 Nicholas J. Jakob, 1 Ryan M. McLemore,
Cleveland Clinic Quarterly
 Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Portuguese Andrological Association National Meeting June 21-23, 2008 Oporto
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Portuguese Andrological Association National Meeting June 21-23, 2008 Oporto
Challenging Non-Traumatic Posterior Urethral Strictures Treated with Urethroplasty: A Preliminary Report
 Clinical Urology Urethroplasty for Challenging Posterior Urethral Strictures International Braz J Urol Vol. 35 (4): 442-449, July - August, 2009 Challenging Non-Traumatic Posterior Urethral Strictures
Clinical Urology Urethroplasty for Challenging Posterior Urethral Strictures International Braz J Urol Vol. 35 (4): 442-449, July - August, 2009 Challenging Non-Traumatic Posterior Urethral Strictures
Reconstruction of Urethral Strictures in Patients with a Long History of Blind Urethral Dilatation
 Reconstruction of Urethral Strictures in Patients with a Long History of Blind Urethral Dilatation Ivan Ignjatovic, Ivica Stojkovic, Dragoslav Basic, Jablan Stankovic, Milan Potic, Ljubomir Dinic RECONSTRUCTIVE
Reconstruction of Urethral Strictures in Patients with a Long History of Blind Urethral Dilatation Ivan Ignjatovic, Ivica Stojkovic, Dragoslav Basic, Jablan Stankovic, Milan Potic, Ljubomir Dinic RECONSTRUCTIVE
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
A report on the clinical efficacy of a new Bougie-internal urethrectomy
 Original research Original research A report on the clinical efficacy of a new Bougie-internal urethrectomy Choe Sung Hyn, MD; * Kim Han Jong, MD; Choe Un Chol, MD * Director of Urology Research Center,
Original research Original research A report on the clinical efficacy of a new Bougie-internal urethrectomy Choe Sung Hyn, MD; * Kim Han Jong, MD; Choe Un Chol, MD * Director of Urology Research Center,
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
PERINEAL PROSTATECTOMY
 Abstract PERINEAL PROSTATECTOMY Pages with reference to book, From 204 To 206 Altaf Hussain Rathore ( Dept. of Surgery, Punjab Medical College, Faisalabad. ) A series of twenty-five medically high risk
Abstract PERINEAL PROSTATECTOMY Pages with reference to book, From 204 To 206 Altaf Hussain Rathore ( Dept. of Surgery, Punjab Medical College, Faisalabad. ) A series of twenty-five medically high risk
Describing the learning curve for bulbar urethroplasty
 Original Article Describing the learning curve for bulbar urethroplasty Marco Spilotros, Sachin Malde, Tamsin J. Greenwell Department of Urology, University College London Hospital, London, UK Contributions:
Original Article Describing the learning curve for bulbar urethroplasty Marco Spilotros, Sachin Malde, Tamsin J. Greenwell Department of Urology, University College London Hospital, London, UK Contributions:
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
The Team. Giuseppe Romano. Sl Salvatore Sansalone. Sofia Balò
 Ahmedabad India 25 26 June 2011 The Team Sl Salvatore Sansalone Giuseppe Romano Sofia Balò Bulbar urethroplasty: t past present future History of bulbar ba urethroplasty (1874-2011) 1874 1992 1993 2011
Ahmedabad India 25 26 June 2011 The Team Sl Salvatore Sansalone Giuseppe Romano Sofia Balò Bulbar urethroplasty: t past present future History of bulbar ba urethroplasty (1874-2011) 1874 1992 1993 2011
Introduction/Learning Objectives. Incontinence: Natural History. Course Outline 10/14/2016. Urinary Incontinence: Conservative Measures
 Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
One-Stage Repair of Long Bulbar Urethral Strictures Using Augmented Russell Dorsal Strip Anastomosis: Outcome of 234 Cases
 european urology 53 (2008) 420 424 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology One-Stage Repair of Long Bulbar Urethral Strictures Using Augmented
european urology 53 (2008) 420 424 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology One-Stage Repair of Long Bulbar Urethral Strictures Using Augmented
Guidelines of guidelines: a review of urethral stricture evaluation, management, and follow-up
 Review Article Guidelines of guidelines: a review of urethral stricture evaluation, management, and follow-up David B. Bayne 1, Thomas W. Gaither 1, Mohannad A. Awad 1, Gregory P. Murphy 1, E. Charles
Review Article Guidelines of guidelines: a review of urethral stricture evaluation, management, and follow-up David B. Bayne 1, Thomas W. Gaither 1, Mohannad A. Awad 1, Gregory P. Murphy 1, E. Charles
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
LESSON ASSIGNMENT. Urinary System Diseases/Disorders. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
Center for Reconstructive Urethral Surgery. Guido Barbagli. Center for Reconstructive Urethral Surgery. Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: info@urethralcenter.it Website: www.urethralcenter.it 22 nd Annual EAU Congress March 21-24, 2007 Berlin Germany Which type of urethroplasty - a critical overview
Guido Barbagli Arezzo - Italy E-mail: info@urethralcenter.it Website: www.urethralcenter.it 22 nd Annual EAU Congress March 21-24, 2007 Berlin Germany Which type of urethroplasty - a critical overview
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Symptomatic Male Urethral Diverticula- Presentation, Diagnosis and Management
 Original article Symptomatic Male Urethral Diverticula- Presentation, Diagnosis and Management Ratkal JM 1, Elias Sharma 2 1Associate Professor, Department of Urology, KIMS, Hubli 2Asst Professor, Department
Original article Symptomatic Male Urethral Diverticula- Presentation, Diagnosis and Management Ratkal JM 1, Elias Sharma 2 1Associate Professor, Department of Urology, KIMS, Hubli 2Asst Professor, Department
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE The UroLift system for the treatment of lower urinary tract symptoms secondary to benign prostatic hyperplasia 1
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it National Congress of the Morocco Association i of Urology April 27, 2007
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it National Congress of the Morocco Association i of Urology April 27, 2007
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Deferred endoscopic urethral realignment: Role in management of traumatic posterior urethral disruption
 African Journal of Urology (2014) 20, 82 87 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Original article Deferred endoscopic urethral
African Journal of Urology (2014) 20, 82 87 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Original article Deferred endoscopic urethral
Cystoscopy. Information for patients Spinal Injuries
 Cystoscopy Information for patients Spinal Injuries page 2 of 8 What is a cystoscopy? A cystoscopy is a procedure to look inside the bladder using a thin camera called a cystoscope. A cystoscope is inserted
Cystoscopy Information for patients Spinal Injuries page 2 of 8 What is a cystoscopy? A cystoscopy is a procedure to look inside the bladder using a thin camera called a cystoscope. A cystoscope is inserted
Can Bipolar Vaporization be Considered an Alternative Energy Source in the Endoscopic Treatment of Urethral Strictures and Bladder Neck Contracture?
 Clinical Urology Bipolar Energy for Treating Urethral Strictures International Braz J Urol Vol. 34 (5): 577-586, September - October, 2008 Can Bipolar Vaporization be Considered an Alternative Energy Source
Clinical Urology Bipolar Energy for Treating Urethral Strictures International Braz J Urol Vol. 34 (5): 577-586, September - October, 2008 Can Bipolar Vaporization be Considered an Alternative Energy Source
Mrs Maya Harris Consultant Urologist INDWELLING CATHETERS: COMPLICATIONS AND SOLUTIONS
 Mrs Maya Harris Consultant Urologist INDWELLING CATHETERS: COMPLICATIONS AND SOLUTIONS AIMS OF PRESENTATION Discuss what can go wrong Discuss reducing risks Discuss managing troublesome problems and when
Mrs Maya Harris Consultant Urologist INDWELLING CATHETERS: COMPLICATIONS AND SOLUTIONS AIMS OF PRESENTATION Discuss what can go wrong Discuss reducing risks Discuss managing troublesome problems and when
Clinical features and long-term outcomes of idiopathic urethrorrhagia
 The Turkish Journal of Pediatrics 2015; 57: 380-384 Original Clinical features and long-term outcomes of idiopathic urethrorrhagia Serdar Moralıoğlu, Ayşenur Cerrah-Celayir, Oktav Bosnalı Department of
The Turkish Journal of Pediatrics 2015; 57: 380-384 Original Clinical features and long-term outcomes of idiopathic urethrorrhagia Serdar Moralıoğlu, Ayşenur Cerrah-Celayir, Oktav Bosnalı Department of
Find Medical Solutions to Your Problems HYDRONEPHROSIS. (Distension of Renal Calyces & Pelvis)
 HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
Urethral Injuries: Realignment vs. Delayed Reconstruction
 Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
BIOPSY GUN. Delivered in sterile peel-open package. Device is made of Stainless Steel and PP material.
 BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
Role of Clean Intermittent Self Catheterization (CISC) in management of recurrent urethral strictures
 Original Article Role of Clean Intermittent Self Catheterization (CISC) in management of recurrent urethral strictures Mohammad Ali Sajid, Shahzad Ahmad, Mobasher Ahmed Saeed, Nasir Malik Departments of
Original Article Role of Clean Intermittent Self Catheterization (CISC) in management of recurrent urethral strictures Mohammad Ali Sajid, Shahzad Ahmad, Mobasher Ahmed Saeed, Nasir Malik Departments of
KIDNEY STONES. When to call for help Call these rooms if any of the following occur:
 KIDNEY STONES Background Kidney stones that move into the ureter (the narrow tube that drains each kidney) often cause a lot of pain. If the stones measure 5mm or less in diameter then most will eventually
KIDNEY STONES Background Kidney stones that move into the ureter (the narrow tube that drains each kidney) often cause a lot of pain. If the stones measure 5mm or less in diameter then most will eventually
Primary Realignment of Posterior Urethral Rupture
 Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Dorsolateral onlay urethroplasty for long segment anterior urethral stricture: outcome of a new technique
 Bangladesh Med Res Counc Bull 2011; 37: 78-82 Dorsolateral onlay urethroplasty for long segment anterior urethral stricture: outcome of a new technique Habib AKMK, Alam AKMK, Amanullah ATM, Rahman H, Hossain
Bangladesh Med Res Counc Bull 2011; 37: 78-82 Dorsolateral onlay urethroplasty for long segment anterior urethral stricture: outcome of a new technique Habib AKMK, Alam AKMK, Amanullah ATM, Rahman H, Hossain
Shock Wave Lithotripsy for Bladder Stones
 Human Journals Research Article February 2018 Vol.:11, Issue:3 All rights are reserved by Haider A. AbuAlmaali et al. Shock Wave Lithotripsy for Bladder Stones Keywords: Shock Wave Lithotripsy, Bladder
Human Journals Research Article February 2018 Vol.:11, Issue:3 All rights are reserved by Haider A. AbuAlmaali et al. Shock Wave Lithotripsy for Bladder Stones Keywords: Shock Wave Lithotripsy, Bladder
Manual Replacement of Double J Stent Without Fluoroscopy. Osman Kose, Sacit Nuri Gorgel, Sait Ozbir, Sekan Yenigurbuz, Cengiz Kara
 Int Surg 2015;100:381 385 DOI: 10.9738/INTSURG-D-13-00248.1 Manual Replacement of Double J Stent Without Fluoroscopy (Double j stent replacement) Osman Kose, Sacit Nuri Gorgel, Sait Ozbir, Sekan Yenigurbuz,
Int Surg 2015;100:381 385 DOI: 10.9738/INTSURG-D-13-00248.1 Manual Replacement of Double J Stent Without Fluoroscopy (Double j stent replacement) Osman Kose, Sacit Nuri Gorgel, Sait Ozbir, Sekan Yenigurbuz,
Combined Dorsal plus Ventral Double Buccal Mucosa Graft in Bulbar Urethral Reconstruction
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Combined Dorsal plus Ventral Double Buccal Mucosa Graft in Bulbar Urethral Reconstruction Enzo Palminteri
available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Combined Dorsal plus Ventral Double Buccal Mucosa Graft in Bulbar Urethral Reconstruction Enzo Palminteri
Iatrogenic Urethral Strictures Following Endoscopic Urethral Procedures: A Disheartening TUPR Outcome (And Pune, India)
 Iatrogenic Urethral Strictures Following Endoscopic Urethral Procedures: A Disheartening TUPR Outcome (And Pune, India) Dr Alex Kavanagh MD FRCSC UBC Urologic Sciences Grand Rounds Oct 4 / 2017 Objectives
Iatrogenic Urethral Strictures Following Endoscopic Urethral Procedures: A Disheartening TUPR Outcome (And Pune, India) Dr Alex Kavanagh MD FRCSC UBC Urologic Sciences Grand Rounds Oct 4 / 2017 Objectives
Renal Trauma: Management Options
 Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
DOWNLOAD OR READ : TREATMENT OF BENIGN PROSTATIC HYPERPLASIA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT OF BENIGN PROSTATIC HYPERPLASIA PDF EBOOK EPUB MOBI Page 1 Page 2 treatment of benign prostatic hyperplasia treatment of benign prostatic pdf treatment of benign prostatic
DOWNLOAD OR READ : TREATMENT OF BENIGN PROSTATIC HYPERPLASIA PDF EBOOK EPUB MOBI Page 1 Page 2 treatment of benign prostatic hyperplasia treatment of benign prostatic pdf treatment of benign prostatic
Surgical Outcome of Urethroplasty Using Penile Circular Fasciocutaneous Flap for Anterior Urethral Stricture
 pissn: 22874208 / eissn: 22874690 World J Mens Health 2014 August 32(2): 8792 http://dx.doi.org/10.5534/wjmh.2014.32.2.87 Original Article Surgical Outcome of Urethroplasty Using Penile Circular Fasciocutaneous
pissn: 22874208 / eissn: 22874690 World J Mens Health 2014 August 32(2): 8792 http://dx.doi.org/10.5534/wjmh.2014.32.2.87 Original Article Surgical Outcome of Urethroplasty Using Penile Circular Fasciocutaneous
OUTCOMES OF EARLY ENDOSCOPIC REALIGNMENT OF POST-TRAUMATIC COMPLETE POSTERIOR URETHRAL RUPTURE
 OUTCOMES OF EARLY ENDOSCOPIC REALIGNMENT OF POST-TRAUMATIC COMPLETE POSTERIOR URETHRAL RUPTURE RAHMAN MM 1, CHOWDHURY SA 2, RAHMAN MM 3, MIAH JI 4, GHOSH KC 5, RAHMAN NM 6, RAHMAN MM 7, AHMED TA 8, KARMAKER
OUTCOMES OF EARLY ENDOSCOPIC REALIGNMENT OF POST-TRAUMATIC COMPLETE POSTERIOR URETHRAL RUPTURE RAHMAN MM 1, CHOWDHURY SA 2, RAHMAN MM 3, MIAH JI 4, GHOSH KC 5, RAHMAN NM 6, RAHMAN MM 7, AHMED TA 8, KARMAKER
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
THE LONG-TERM SOLUTION FOR MALE INCONTINENCE
 THE LONG-TERM SOLUTION FOR MALE INCONTINENCE Urogyn BV Transistorweg 5a 6534 AT Nijmegen The Netherlands t +31(0) 24 711 41 30 info@urogynbv.com www.urogynbv.com THE FIRST INJECTABLE IMPLANT THAT CAN COMPETE
THE LONG-TERM SOLUTION FOR MALE INCONTINENCE Urogyn BV Transistorweg 5a 6534 AT Nijmegen The Netherlands t +31(0) 24 711 41 30 info@urogynbv.com www.urogynbv.com THE FIRST INJECTABLE IMPLANT THAT CAN COMPETE
20 Prostate Cancer Dan Ash
 20 Prostate Cancer Dan Ash 1 Introduction Prostate cancer is a disease of ageing men for which the aetiology remains unknown. The incidence rises up to 30 to 40% in men over 80. The symptoms of localised
20 Prostate Cancer Dan Ash 1 Introduction Prostate cancer is a disease of ageing men for which the aetiology remains unknown. The incidence rises up to 30 to 40% in men over 80. The symptoms of localised
University Journal of Surgery and Surgical Specialities
 University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 OUTCOME OF OPTICAL INTERNAL URETHROTOMY FOR SHORT SEGMENT BULBAR STRICTURES Pitchaibalashanmugam Karrupiah, Rajaraman Thiagarajan,
University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 OUTCOME OF OPTICAL INTERNAL URETHROTOMY FOR SHORT SEGMENT BULBAR STRICTURES Pitchaibalashanmugam Karrupiah, Rajaraman Thiagarajan,
Prophylactic urethral stenting with Memokath 028SW in prostate cancer patients undergoing prostate 125 I seed implants: phase I/II study
 Original article Clinical Investigations Prophylactic urethral stenting with Memokath 028SW in prostate cancer patients undergoing prostate 125 I seed implants: phase I/II study Samuel T. Chao, MD 1, Kenneth
Original article Clinical Investigations Prophylactic urethral stenting with Memokath 028SW in prostate cancer patients undergoing prostate 125 I seed implants: phase I/II study Samuel T. Chao, MD 1, Kenneth
Hong Kong College of Surgical Nursing
 Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
