Abstract. Original Article
|
|
|
- Augustine Cox
- 5 years ago
- Views:
Transcription
1 Original Article Middle East Journal of Cancer; July 2015; 6(3): A Comparison of Early Results and Patient Satisfaction Rate between Modified Radical Cystectomy with Mainz II Urinary Diversion and Standard Radical Cystectomy with Continent Ileocecal Urinary Diversion Saeed Shakeri*, Hossein Zeighami**, Mehdi Salehipour*, Hossein Beik Mohammadloo*, Aria Shakeri***, Arash Shakeri****, Shahryar Zeighami* *Department of Urology, Shiraz University of Medical Sciences, Shiraz, Iran **Student Research Committee, Fasa University of Medical Sciences, Fasa, Iran ***University of Toronto, Toronto, Canada ****University of Waterloo, Waterloo, Canada Corresponding Author: Shahryar Zeighami, MD Department of Urology, Shiraz University of Medical Sciences, Shiraz, Iran zeyghamishahryar@yahoo.com Abstract Background: This study compared the early success, complication and patient satisfaction rates of modified extraperitoneal radical cystectomy (Mainz II urinary diversion) with standard intraperitoneal radical cystectomy (continent ileocecal urinary diversion) in a group of patients with muscle invasive urothelial carcinoma of the urinary bladder. Methods: From September 2009 until November 2013, this randomized study enrolled 60 patients with muscle invasive transitional cell carcinoma of the urinary bladder who underwent radical cystectomy and urinary diversion. The patients were randomly allocated to two groups via block randomization. Group A included 30 patients (28 men and 2 women) who underwent modified small incision extraperitoneal radical cystectomy with a Mainz II urinary diversion. Group B included 30 patients (27 men and 3 women) who had classic intraperitoneal radical cystectomy and ileocecal continent diversion. The data were extracted and analyzed. The patients were followed for one year after surgery. Results: Group A patients had a mean age of 61.47±8.63 years. Group B patients had a mean age of 60.77±6.82 years. There were no statistically significant differences in blood loss, electrolyte and acid-base abnormalities, and early post- operative complication rates between the two groups. However, surgical and hospitalization times were significantly shorter in group A (P<0.001). In addition, patients were mobilized earlier and had shorter nothing by moth time. Patient satisfaction rate was significantly more in group A. Conclusion: Small incision extraperitoneal radical cystectomy and Mainz II urinary diversion is a safe, less complicated, effective and more rapid technique with excellent short term outcome. It seems this technique is a reliable alternative for continent urinary diversion in selected bladder cancer patients, mainly in those with urethral involvement. Keywords: Mainz II, Radical cystectomy, Bladder tumor Received: December 16, 2014; Accepted: April 6, 2015
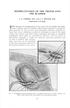
2 Saeed Shakeri et al. Introduction Bladder cancer is the second most common genitourinary cancer after prostate cancer. This cancer is the fourth most common solid cancer in men and seventh to ninth most common cancer in women. 1 It is four times more prevalent in men. More than 90% of bladder cancers originate from the urothelium and are urothelial tumors. 2 These urothelial tumors are broadly classified into two major histological groups. Non-muscle invasive urothelial tumors (NMI-UT) are confined to the submucosa. Despite a high risk of recurrence, progression to the muscular layer is rarely seen and the cancer specific mortality rate is low. The standard of care for NMI-UBT is a transurethral resection of the tumor (TUR). The second group, muscle invasive urothelial tumors (MI-UT) invades the detrusor muscle and adventitia. In patients with extravesical involvement, approximately one third have recurrence, even after invasive surgery and negative pelvic lymph nodes. 3 The standard approach in patients with MI- UBT is radical cystectomy and urinary diversion. There are many factors that influence selection of the type of urinary diversion, including comorbidities, patient body figure, expected survival, age, sex and patient choice. Fisch and Hohenfellner 4 have introduced a variation of ureterosigmoidostomy urinary diversion later termed the "Sigma rectum or Mainz II pouch". According to these researchers, this procedure is less technically demanding, easier, more rapid, and does not need a catheter, collection bags or appliances, which also makes the technique more cost effective. In an effort to decrease procedural complexity without violating the principles of oncologic surgery, we have combined small incision extraperitoneal radical cystectomy with Mainz II urinary diversion and compared the early results with classic radical cystectomy and continent urinary diversion. Patients and Methods From September 2009 to November 2013, 60 patients with muscle invasive urothelial bladder cancer (T2-T3) enrolled in this study. After description of treatment methods, informed consent was taken. Patients with decreased renal function and hydronephrotic changes of the kidneys were excluded. All patients were randomly allocated into two groups (Table 1). Group A consisted of 30 patients (28 males and 2 females) with a mean age of 61.47±8.63 years (range: years) who underwent modified (small incision extraperitoneal approach) radical cystectomy and Mainz II pouch (Figure 1). In this modification we used a low midline infraumbilical incision. Without opening the peritoneum, a classic bilateral pelvic lymph node dissection and radical cystoprostatectomy were performed extraperitoneally. After completion of a cystectomy, a small window was made in the peritoneum to expose the rectosigmoid. The Mainz II urinary diversion was performed as described by Hohenfellner. 4 The ureters were anastomosed to the sigmoid colon at suitable sites after creating submucosal tunnels. We used the principles of detubularization and spherical reshaping of the sigmoid and rectum to make a low pressure reservoir. A drain was put in the Retzius space, while the patients had two rectal tubes for free drainage of urine through the rectum. Group B consisted of 30 patients (27 males and 3 females) with a mean age of 60.77±6.82 years (range: years) who underwent standard intraperitoneal radical cystectomy and an ileocecal pouch. In brief, an extensive midline incision from 2 cm below the xyphoid to the symphysis pubis was made. The peritoneal cavity was entered and explored. A classic pelvic lymph node Figure1. Small incision extraperitoneal lymph node dissection and radical cystectomy. 166 Middle East J Cancer 2015; 6(3):
3 Comparison of Modified Versus Standard Radical Cystectomy Table 1. Comparison of demographic criteria of patients in groups A and B. Group (n) Sex Age (years) (m ± sd) Co-morbidity(n) Habits(n) Male Female DM =2 A (30) ± 8.63 IHD =2 Smoker=5 COPD =1 Opium=4 DM =3 B (30) ± 6.82 IHD =4 Smoker=6 COPD =0 Opium=5 DM =Diabetes mellitus; IHD =Ischemic heart disease; COPD =Chronic obstructive pulmonary disease dissection and radical cystoprostatectomy were performed. A pouch was made from the terminal ileum and cecum using the appendix as the catheterizable Stoma. After discharge from the hospital, patients returned for follow up one week later and then each month to have renal ultrasound and laboratory exams for a period of one year after surgery. Data were gathered by a questionnaire and analyzed using the t- and chi-square tests. Results There was no significant difference in risk factors and co-morbidities between the two groups (Table 1). Two patients in each study group died during the early post-op period secondary to medical complications (myocardial infarction) and urosepsis. There were no significant differences in blood loss, ICU care and metabolic abnormalities between the groups. A total of 10 patients from each group needed ICU care, however the mean ICU time in group B (26 h) was longer than group A (16 h). The surgical time, hospital stay, NPO time and narcotic injections were significantly less in group A (Tables 2 and 3). Patients in group A had a shorter bed rest time and were mobilized sooner. These patients also showed a more rapid return to normal bowel movements. In group A, one patient had mild pre-op renal insufficiency (Cr=1.9) and developed increased BUN, creatinine and hypocalcemia during the first 60 days after surgery which was alleviated by regular rectal emptying and oral alkalinizing drugs. Bilateral hydronephrosis and pyelonephritis developed in one patient, which was managed with bilateral nephrostomy tubes and antibiotic therapy. One patient in Mainz II group developed acute abdominal pain 25 days after surgery which was attributed to ischemia of the colon. The patient was treated by colostomy and ileal conduit diversion. Wound dehiscence was seen in two cases from group A and three from group B, however this difference was not statistically significant. All patients in both groups were continent during the day and night over long-term follow-up. However, one patient in group A had enuresis. There were similar rates of wound infection, pyelonepritis and sepsis in both groups, which was not statistically significant (Table 3). Although the rate of wound infection and dehiscence was small, there was a remarkable association between history of opium addiction to wound infection (P=0.007) and dehiscence (P< 0.000). Evaluation of satisfaction was based on two critical questions. 1. Did urinary diversion disturb your daily life? 2. Did urinary diversion meet your expectations? In group A, 90% of patients answered "No" to the first question and "Yes" to the second question, whereas 60% of group B patients responded in the same manner. Patient response of No to the first question and Yes to the second question was defined as a satisfactory response; any other response was defined as an unsatisfactory response. Discussion Simon, in 1852, was the first surgeon who used the bowels for urinary diversion and Coffey in 1905 was the first who described anastomosis of the ureters to sigmoid for urinary diversion. 8 Due to the lack of antibiotics, poor surgical Middle East J Cancer 2015; 6(2):
4 Saeed Shakeri et al. Table 2. Comparison of surgical, hospitalization and NPO times between groups. Variable Group P-value A B Surgical time (mean, min) <0.001 NPO time (mean, days) <0.001 Hospital stay (mean, days) <0.001 techniques and low standard of care at that time, this type of urinary diversion had unacceptable complications in terms of morbidity and mortality, and was replaced by other procedures such as the ileal conduit. 6 Fisch and Hohenfellner in 1991 described a type of ureterosigmoidostomy that later was modified and named the "Sigma rectum" or Mainz pouch II urinary diversion. Feasibility and reproducibility were mentioned as two important advantages of the Mainz pouch II. Detubalization of the sigmoid colon makes a capacious low pressure reservoir which decreases the possibility of reflux and pyelonephritis, thus assisting the patient with continence. 4,7 Improvement of surgical techniques, particularly anti-reflux reimplantation of the ureters to the sigmoid accompanied with long-term antibiotic therapy and alkalinizing agents have decreased infectious complications and mortality rate in the Mainz Pouch II, which makes this technique safe and reliable for urinary diversion in advanced bladder cancer. The early complication rate of the Mainz pouch II is reported to be 6.8%. 7 Hyperchloremic metabolic acidosis is a major complication that may be seen after any technique for urinary diversion that uses bowel segments, particularly in continent diversions and ureterosigmoidostomy. Impaired renal function is a predisposing factor for metabolic acidosis. For prevention of metabolic acidosis and potential bone demineralization over the long-term, patients should take alkalinizing drugs, monitor serum electrolytes and acid-base balances. 8,9 The use of alkalinizing agents is advised to prevent this complication. In various reports, 30%-70% of Mainz II patients must use oral alkalinizing drugs during the first year after surgery; after one year this rate decreases to approximately 8%. 4, 8, 10 Frequent loose bowel movements and urge incontinence are among most bothersome complications of classical ureterosigmoidostomy that impact quality of life of patients. However, with the Mainz II procedure, the risk of bowel incontinence can be decreased by detubularization of the rectosigmoid segment. 8, 11 In the current study, none of the patients have reported fecal incontinence with the exception of one who has occasional enuresis. All patients can hold for at least two hours during the day, however all need to evacuate at least once at night. Stenosis at the site of ureteric implantation is reported to be approximately 4% and mostly seen during the first two years after surgery. These patients are managed by retrograde balloon dilatation which is successful in 86% of cases. 10 We have not seen this complication in our patients. The most serious long-term complication of classic ureterosigmoidostomy is the risk of secondary colon malignancy, which is attributed to formation of a mixture of urine and feces, and exposure of the gastrointestinal epithelium to toxic material. For early diagnosis of these tumors, annual colonoscopy 5-10 years after surgery is recommended. 8, 11 The Mainz II procedure is a relatively new technique. There is a lack of data regarding longterm complications which should be addressed in future studies. However none of our patients have developed colon cancer during follow up. Detubularization and spherical reconfiguration of the rectosigmoid segment creates a low pressure and high capacity reservoir which prevents incontinence from one side and reflux of bowel contents into the ureter and pyelonephritis on the other side. 4 In patients with urethral involvement by the tumor and locally advanced neoplasms where 168 Middle East J Cancer 2015; 6(3):
5 Comparison of Modified Versus Standard Radical Cystectomy Table 3: Comparison of surgical & post-surgical factors in the two groups. Variable Group A Group B (Mainz II) (ileocecal) Surgical factors -Mean duration of surgery -292 minutes -452 minutes -Mean blood loss (ML) -1225cc -1163cc -Acid-base abnormality Mild. Acidosis; 5 pt Mild.acidosis :8 pt Mod. Acidosis: 3 pt Mod. Acidosis: 3 pt Electrolytes abnormality -No - No Post-surgical factors -Need to ICU care 10 patients 10 patients -Mean Hb droop the first 3.38 gr/dl 2.80 gr/dl days after operation -Mean analgesic injection mg mg during admission (pethedin) -Time of to get "out of Bed" 1.5 day 2.46 day -Meantime of beginning diet 5.24 days 7.29 day -Meantime of hospitalization 8.8 day 13.2 day -Electrolytes abnormally Normal K+ :50% Normal K+ :55% Mild hypokalemia:40% Mild hypokalemia: 40% Mod hypokalemia:10% Mod hypokalemia: 5% -Increasing, BUN,Cr 2 patients 3 patients -Wound infection 5 patients 6 patients -Wound dehiscence 2 patients 3 patients -Sepsis 2 patients 3 patients -Pyelonephritis 3 patients 2 patients - Ureteric implantation site None None stenosis - Day and night incontinence None None -Nocutria None None -Satisfaction rate 27 patients (=90%) 18 patients (=60%) orthotopic diversion is not indicated, the Mainz pouch II may be a valuable alternative for diversion. 11 Although orthotopic diversion has the advantage of near normal anatomy, however both the day and night continence rates in orthotopic diversion are reported to be 78%-89% versus 91%-100% in the Mainz pouch II. 11 Most patients need to perform the Valsalva maneuver for evacuation of urine. Approximately 30% of patients need Clean Intermittent Catheterization (CIC) to empty the neobladder. 11 Patients who undergo the Mainz II procedure do not need to perform intermittent catheterization or use any appliances which makes this technique convenient and acceptable by the patient. Other disadvantages of orthotopic urinary diversion include the risk of urethral recurrence, more technically complex and time consuming surgery, and higher risk of surgical complications. However, the risk of deterioration of the upper urinary tract over the long-term is the same as any other type of urinary diversion. 11,12 Additionally, there are special religious and cultural issues for Muslims patients. Thus, the issue of urinary diversion with no stoma, CIC, or appliance that will give a better body image, particularly in young females, makes the Mainz II an ideal urinary diversion for this group of patients. For most Muslim patients, urinary leakage from diversion and catheterization Stoma is a major problem because of religious concerns. According to the results of this procedure, decreased surgical and anesthesia times, less manipulation of intraperitoneal organs, shorter ICU care and hospitalization time, and faster Middle East J Cancer 2015; 6(2):
6 Saeed Shakeri et al. return to normal activities and lifestyle without external application make Mainz pouch II an acceptable diversion. Preservation of body image has a positive psychosocial effect on patients with the Mainz pouch II. These patients have a nearly normal voiding pattern. In the current study, most patients met their pre-surgical expectations from this surgery and were satisfied regarding personal ability and daily life. Overall, we believe the Mainz pouch II has a good early outcome, however long-term results remain to be evaluated. Conclusion The Mainz pouch II is an effective, safe, less complicated, and cost-effective urinary diversion in selected patients with muscle invasive urothelial bladder tumor. Patients should have competent anal sphincter, normal renal function and no history of pelvic radiotherapy in order to be considered for this procedure. International edition: Saunders Elsevier; 2011.p McKiernan, JM; DeCastro, GJ; Benson, MC. Cutaneous Continent Urinary Diversion. In: McDougal, Wein, Kavoussi, Novick, Partin, Peters, Ramchandani, editors. Campbell-Walsh Urology. 10 th ed. International edition: Saunders Elsevier; 2011.p Pannek J, Senge T. History of urinary diversion. Urol Int. 1998;60(1): Nitkunan T, Leaver R, Patel HR, Woodhouse CR. Modified ureterosigmoidostomy (Mainz II): a longterm follow-up. BJU Int. 2004;93(7): Hadzi-Djokic JB, Basic DT. A modified sigma-rectum pouch (Mainz pouch II) technique: analysis of outcomes and complications on 220 patients. BJU Int. 2006;97(3): D'elia G, Pahernik S, Fisch M, Hohenfellner R, Thüroff JW. Mainz Pouch II technique: 10 years' experience. BJU Int. 2004;93(7): Nesrallah LJ, Srougi M, Dall'Oglio MF. Orthotopic ileal neobladder: the influence of reservoir volume and configuration on urinary continence and emptying properties. BJU Int. 2004;93(3): Conflict of Interest No conflict of interest is declared. References 1. Siegel R, Naishadham D, Jemal A. Cancer statistics, CA Cancer J Clin. 2013;63(1): David, P; Wood, Jr. Urothelial Tumors of the Bladder. In: McDougal, Wein, Kavoussi, Novick, Partin, Peters, Ramchandani, editors. Campbell-Walsh Urology 10th ed. International edition: Saunders Elsevier p Dozić J, Bogdanović J. Current diagnostic and therapeutic approaches to invasive bladder cancer [Article in Serbian]. Med Pregl. 2005;58(9-10): Pahernik S, Wiesner C, Gillitzer R, Stein R, Thüroff JW. Conversion from colonic conduit into rectosigmoid pouch (Mainz pouch II). BJU Int. 2006;97(1): Bastian PJ, Albers P, Haferkamp A, Schumacher S, Müller SC. Modified ureterosigmoidostomy (Mainz Pouch II) in different age groups and with different techniques of ureteric implantation. BJU Int. 2004;94(3): Skinner, EC; Skinner, DG; Stein, JP. Orthotopic Urinary Diversion. In: McDougal WS, Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA, Ramchandani P, editors. Campbell-Walsh Urology. 10 th edition. 170 Middle East J Cancer 2015; 6(3):
Bladder replacement in men and women: when and when not? Outline. Continent Diversion History
 1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
URINARY DIVERSIONS. Winter 2016 Dr P. O Malley
 URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
URINARY DIVERSIONS. Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania
 URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report
 198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
Cystectomies and bladder preservation: What you need to know
 Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Comparison of Three Types of Continent Urinary Diversions in a Single Center
 Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Muscle-invasive bladder cancer
 Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent Pouch with Abdominal Stoma
 Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Recovery of sexual function after radical cystectomy with orthotopic neobladder
 Recovery of sexual function after radical cystectomy with orthotopic neobladder C. Gingu, V. Olaru, A. Dick, C. Baston, M. Crăsneanu, C. Surcel, S. Voinea, Liliana Domnişor, I. Sinescu Center of Urological
Recovery of sexual function after radical cystectomy with orthotopic neobladder C. Gingu, V. Olaru, A. Dick, C. Baston, M. Crăsneanu, C. Surcel, S. Voinea, Liliana Domnişor, I. Sinescu Center of Urological
Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate
 European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
Long-Term Complications of Conduit Urinary Diversion
 Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
Modified ureterosigmoidostomy for management of malignant and non-malignant
 334 E a s t A f r i c a n M e d i c a l J o u r n a l July 2008 East African Medical Journal Vol. 85 No. 7 July 2008 Modified ureterosigmoidostomy for management of malignant and non-malignant conditions
334 E a s t A f r i c a n M e d i c a l J o u r n a l July 2008 East African Medical Journal Vol. 85 No. 7 July 2008 Modified ureterosigmoidostomy for management of malignant and non-malignant conditions
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016
 BLADDER CANCER Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016 BLADDER CANCER = UROTHELIAL CANCER Antiquated term is Transitional Cell Carcinoma
BLADDER CANCER Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016 BLADDER CANCER = UROTHELIAL CANCER Antiquated term is Transitional Cell Carcinoma
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution
 European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
Department of Urology, Theodor Bilharz research Institute, Cairo, Egypt
 Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
A patient with recurrent bladder cancer presents with the following history:
 MP/H Quiz A patient with recurrent bladder cancer presents with the following history: 9/23/06 TURB 1/12/07 TURB 4/1/07 TURB 7/12/07 TURB 11/14/07 Non-invasive papillary transitional cell carcinoma from
MP/H Quiz A patient with recurrent bladder cancer presents with the following history: 9/23/06 TURB 1/12/07 TURB 4/1/07 TURB 7/12/07 TURB 11/14/07 Non-invasive papillary transitional cell carcinoma from
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Original Paper. Urol Int 2002;69:
 Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Wednesday 21st September - Leeds
 Diane Leach Wednesday 21st September - Leeds Outline of presentation Treatment options Types of urinary diversion Radical cystectomy and ileal conduit Patient counselling Care of the stoma Types of appliances
Diane Leach Wednesday 21st September - Leeds Outline of presentation Treatment options Types of urinary diversion Radical cystectomy and ileal conduit Patient counselling Care of the stoma Types of appliances
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
THE operation of reimplantation of the ureter into the bladder has undergone
 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Interventional management of postoperative ureteric complications after pelvic surgery
 Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Section H Bladder and Bowel
 Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT
 Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled urinary, sexual and reproductive conditions. The chapter
Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled urinary, sexual and reproductive conditions. The chapter
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Laparoscopic Resection Of Colon & Rectal Cancers. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan
 ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org Conservative Treatment of Invasive Bladder Cancer Luis Souhami, MD Professor Department of Radiation Oncology
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org Conservative Treatment of Invasive Bladder Cancer Luis Souhami, MD Professor Department of Radiation Oncology
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Surgical Atlas Politano-Leadbetter ureteric reimplantation
 Surg Ill SURGERY ILLUSTRATED STEFFENS et al. Surgical Atlas Politano-Leadbetter ureteric reimplantation JOACHIM STEFFENS, EBERHARD STARK, BJÖRN HABEN and ADRIAN TREIYER Department of Urology and Paediatric
Surg Ill SURGERY ILLUSTRATED STEFFENS et al. Surgical Atlas Politano-Leadbetter ureteric reimplantation JOACHIM STEFFENS, EBERHARD STARK, BJÖRN HABEN and ADRIAN TREIYER Department of Urology and Paediatric
Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $
 European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Rectal Cancer. About the Colon and Rectum. Symptoms. Colorectal Cancer Screening
 Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Open Radical Cystectomy Tips and Tricks in Males and Females
 Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Radical cystectomy and urinary diversion: Normal anatomy and complications
 Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
Mainz Pouch II technique: 10 years experience
 Original Article 10 YEARS EXPERIENCE OF MAINZ POUCH II G. D ELIA et al. In this section, the use of the Mainz Pouch II is examined in some detail, from Mainz (where it originated), and from London. Both
Original Article 10 YEARS EXPERIENCE OF MAINZ POUCH II G. D ELIA et al. In this section, the use of the Mainz Pouch II is examined in some detail, from Mainz (where it originated), and from London. Both
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion
 UROLOGICAL ONCOLOGY Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion Bin Sun, Jing-Min Yan, Jian-Ye Li, He-Qing Guo, Quan Hong, Zhi-Yong Yao, Gao-Biao Zhou, Guang-Xin Pan,
UROLOGICAL ONCOLOGY Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion Bin Sun, Jing-Min Yan, Jian-Ye Li, He-Qing Guo, Quan Hong, Zhi-Yong Yao, Gao-Biao Zhou, Guang-Xin Pan,
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Indications and effectiveness of the open surgery in vesicoureteral reflux
 Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Urologic Surgical Complications In Renal Transplantation
 Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Part II: Treatment. A Woman-to-Woman Talk with Dr. Armine Smith. Wednesday, March 8, Presented by
 Women & Bladder Cancer A Woman-to-Woman Talk with Dr. Armine Smith Wednesday, March 8, 2017 Part II: Treatment Presented by Dr. Smith is an Assistant Professor of Urology at Johns Hopkins University and
Women & Bladder Cancer A Woman-to-Woman Talk with Dr. Armine Smith Wednesday, March 8, 2017 Part II: Treatment Presented by Dr. Smith is an Assistant Professor of Urology at Johns Hopkins University and
CHILDREN who require urinary diversion rarely have malignant disease, therefore,
 THE ILEAL CONDUIT IN THIRTY-FIVE CHILDREN RALPH A. STRAFFON, M.D., Department of Urology RUPERT B. TURNBULL, JR., M.D., Department of General Surgery and ROBERT D. MERCER, M.D. Department of Pediatrics
THE ILEAL CONDUIT IN THIRTY-FIVE CHILDREN RALPH A. STRAFFON, M.D., Department of Urology RUPERT B. TURNBULL, JR., M.D., Department of General Surgery and ROBERT D. MERCER, M.D. Department of Pediatrics
BCAN Fall Series: Survivorship
 BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
Hollow Visceral Myopathy in a 5-year old Boy: a Case Report
 Hollow Visceral Myopathy in a 5-year old Boy: a Case Report S.H.T. Zaidi,Z. Zaidi ( The Kidney Centre Postgraduate Training Institute. Karachi. ) M. Arif ( Department of Paediatric Urology and Histopathology,
Hollow Visceral Myopathy in a 5-year old Boy: a Case Report S.H.T. Zaidi,Z. Zaidi ( The Kidney Centre Postgraduate Training Institute. Karachi. ) M. Arif ( Department of Paediatric Urology and Histopathology,
90% of bladder tumours are transitional cell carcinoma (TCC), the remaining 10% of cases are squamous cell carcinoma, adenocarcinoma and sarcoma.
 The Role of the Interventional Radiologist in Management of Post-Radical Cystectomy Ureteral Obstruction : A Case Review of Retrograde Transileal Conduit Ureteric Stents. Poster No.: C-2288 Congress: ECR
The Role of the Interventional Radiologist in Management of Post-Radical Cystectomy Ureteral Obstruction : A Case Review of Retrograde Transileal Conduit Ureteric Stents. Poster No.: C-2288 Congress: ECR
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al.
 Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Urological Tumours 1 Kidney tumours 2 Bladder tumours
 Urological Tumours 1 Kidney tumours 2 Bladder tumours Tim Bracey SpR Histopathology Derriford Hospital Kidney tumours What are we going to talk about?! Anatomy of urinary tract! Types of kidney tumours!
Urological Tumours 1 Kidney tumours 2 Bladder tumours Tim Bracey SpR Histopathology Derriford Hospital Kidney tumours What are we going to talk about?! Anatomy of urinary tract! Types of kidney tumours!
SEROUS LINED EXTRAMURAL ILEAL VALVE: A NEW CONTINENT URINARY OUTLET
 0022-5347/99/1613-0786$03.00/0 THE JOURNAL OF UROLOGY Vol. 161, 786 791, March 1999 Copyright 1999 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. SEROUS LINED EXTRAMURAL ILEAL VALVE: A NEW
0022-5347/99/1613-0786$03.00/0 THE JOURNAL OF UROLOGY Vol. 161, 786 791, March 1999 Copyright 1999 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. SEROUS LINED EXTRAMURAL ILEAL VALVE: A NEW
Robotic Appendicovesicostomy
 Robotic Appendicovesicostomy Cheryl Baxter, MSN,RN,CPNP Daniel DaJusta, MD Kristina Booth, MSN,RN,FNP Roadmap for Presentation Part 1 Pre-surgical/historical neurogenic bladder- Baxter Part 2 Robotic appendicovesicostomy/
Robotic Appendicovesicostomy Cheryl Baxter, MSN,RN,CPNP Daniel DaJusta, MD Kristina Booth, MSN,RN,FNP Roadmap for Presentation Part 1 Pre-surgical/historical neurogenic bladder- Baxter Part 2 Robotic appendicovesicostomy/
SECTION H: BLADDER AND BOWEL. H0100: Appliances. Item Rationale Health-related Quality of Life. Planning for Care
 SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
Primary Realignment of Posterior Urethral Rupture
 Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
UTI and UrinaryTract Reconstruction
 EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder
 Jpn J Clin Oncol 2002;32(1)14 18 Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder Isao Hara, Hideaki Miyake, Shoji Hara, Akinobu Gotoh, Hiroshi
Jpn J Clin Oncol 2002;32(1)14 18 Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder Isao Hara, Hideaki Miyake, Shoji Hara, Akinobu Gotoh, Hiroshi
Clinical Significance of Bacteriuria in Patients with Orthotopic Sigmoid Neobladder after Radical Cystectomy
 African Journal of Urology 1110-5704 Vol. 15, No. 4, 2009 233-237 Original Article Clinical Significance of Bacteriuria in Patients with Orthotopic Sigmoid Neobladder after Radical Cystectomy INTRODUCTION
African Journal of Urology 1110-5704 Vol. 15, No. 4, 2009 233-237 Original Article Clinical Significance of Bacteriuria in Patients with Orthotopic Sigmoid Neobladder after Radical Cystectomy INTRODUCTION
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Management of Perforated Colon Cancers
 Management of Perforated Colon Cancers Introduction Colon and rectal cancers are the most common gastrointestinal cancers. They are 3 rd most common and 2 nd most common causes of cancer deaths among men
Management of Perforated Colon Cancers Introduction Colon and rectal cancers are the most common gastrointestinal cancers. They are 3 rd most common and 2 nd most common causes of cancer deaths among men
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
ROBOTIC VS OPEN RADICAL CYSTECTOMY
 ROBOTIC VS OPEN RADICAL CYSTECTOMY A REVIEW Colin Lundeen December 14, 2016 Objectives Review the history of radical cystectomy Critically analyze recent RCTs comparing open radical cystectomy (ORC) to
ROBOTIC VS OPEN RADICAL CYSTECTOMY A REVIEW Colin Lundeen December 14, 2016 Objectives Review the history of radical cystectomy Critically analyze recent RCTs comparing open radical cystectomy (ORC) to
Surgical Atlas Orthotopic ileal neobladder
 Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
UCSF UROLOGY TRANSITIONAL UROLOGY CLINIC
 UCSF UROLOGY TRANSITIONAL UROLOGY CLINIC Thank you for choosing the UCSF Transitional Urology Clinic. This clinic was created to serve patients with urologic conditions diagnosed in childhood as they become
UCSF UROLOGY TRANSITIONAL UROLOGY CLINIC Thank you for choosing the UCSF Transitional Urology Clinic. This clinic was created to serve patients with urologic conditions diagnosed in childhood as they become
Bladder Cancer Guidelines
 Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
LARGE BOWEL OBSTRUCTION MARCUS BURNSTEIN
 LARGE BOWEL OBSTRUCTION MARCUS BURNSTEIN MCQ A 78 yr. old man (HT, DM, 2 coronary stents) has 3 mos. of irregular bowel habits and 72 hrs. of LBO. Distended, non-tender. Normal blood work. Plain xray,
LARGE BOWEL OBSTRUCTION MARCUS BURNSTEIN MCQ A 78 yr. old man (HT, DM, 2 coronary stents) has 3 mos. of irregular bowel habits and 72 hrs. of LBO. Distended, non-tender. Normal blood work. Plain xray,
Colon Cancer Surgery
 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Hong Kong College of Surgical Nursing
 Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Living Well With an Ostomy. Maggie Bork, RN, BSN, CWOCN
 Living Well With an Ostomy Maggie Bork, RN, BSN, CWOCN Objectives 1. Describe the 3 most common types of ostomies. 2. Discuss the results of recent research studies related to peristomal and stoma challenges.
Living Well With an Ostomy Maggie Bork, RN, BSN, CWOCN Objectives 1. Describe the 3 most common types of ostomies. 2. Discuss the results of recent research studies related to peristomal and stoma challenges.
Postoperative Appearance and Complications of the Urinary Tract Following Surgery: A Comprehensive Review
 Postoperative Appearance and Complications of the Urinary Tract Following Surgery: A Comprehensive Review Poster No.: C-2137 Congress: ECR 2018 Type: Authors: Keywords: DOI: Educational Exhibit N. Kinger
Postoperative Appearance and Complications of the Urinary Tract Following Surgery: A Comprehensive Review Poster No.: C-2137 Congress: ECR 2018 Type: Authors: Keywords: DOI: Educational Exhibit N. Kinger
Pelvioureteric junction obstruction of the lower collecting system associated with incomplete ureteral duplication: A case report
 Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Inflammatory Bowel Disease and Surgery: What You Should Know
 Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries
 Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries page 2 of 8 This leaflet has been produced in support of the explanation and counselling provided by your urologist and nurse specialist.
Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries page 2 of 8 This leaflet has been produced in support of the explanation and counselling provided by your urologist and nurse specialist.
Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions
 Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions J.A. Nieuwenhuijzen* R.R. de Vries* A. Bex H.G. van
Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions J.A. Nieuwenhuijzen* R.R. de Vries* A. Bex H.G. van
Bladder Sparing Treatment of Muscle Invasive Bladder Cancer
 Bladder Sparing Treatment of Muscle Invasive Bladder Cancer Pr Alexandre de la Taille CHU Mondor, Créteil INSERMU955Eq07 adelataille@hotmail.com High-Risk Invasive and Muscle-Invasive BCa Radical cystectomy
Bladder Sparing Treatment of Muscle Invasive Bladder Cancer Pr Alexandre de la Taille CHU Mondor, Créteil INSERMU955Eq07 adelataille@hotmail.com High-Risk Invasive and Muscle-Invasive BCa Radical cystectomy
Eiji Kikuchi, Yutaka Horiguchi, Jun Nakashima, Takashi Ohigashi, Mototsugu Oya, Ken Nakagawa, Akira Miyajima and Masaru Murai
 Assessment of Long-Term Quality of Life Using the FACT-BL Questionnaire in Patients with an Ileal Conduit, Continent Reservoir, or Orthotopic Neobladder Eiji Kikuchi, Yutaka Horiguchi, Jun Nakashima, Takashi
Assessment of Long-Term Quality of Life Using the FACT-BL Questionnaire in Patients with an Ileal Conduit, Continent Reservoir, or Orthotopic Neobladder Eiji Kikuchi, Yutaka Horiguchi, Jun Nakashima, Takashi
FISTULA CARE. FISTULA TREATMENT COMPLICATIONS: Reporting Guidelines. Updated 12/12/12
 FISTULA CARE FISTULA TREATMENT COMPLICATIONS: Reporting Guidelines Updated 12/12/12 EngenderHealth, 440 Ninth Avenue, New York, NY 10001, USA Telephone: 212-561-8000; Fax: 212-561-8067; E-mail: fistulacare@engenderhealth.org
FISTULA CARE FISTULA TREATMENT COMPLICATIONS: Reporting Guidelines Updated 12/12/12 EngenderHealth, 440 Ninth Avenue, New York, NY 10001, USA Telephone: 212-561-8000; Fax: 212-561-8067; E-mail: fistulacare@engenderhealth.org
Ureteral Reconstruction With Bowel Segments: Experience With Eight Patients in a Single Institute
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.742 Original Article - Reconstructive Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.742&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.742 Original Article - Reconstructive Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.742&domain=pdf&date_stamp=2014-11-16
Urinary stoma. This is the simplest and most straightforward form of
 This is the simplest and most straightforward form of urinary drainage following surgery to remove the bladder (cystectomy). You may see it referred to as a urostomy, an ileal conduit or urinary diversion.
This is the simplest and most straightforward form of urinary drainage following surgery to remove the bladder (cystectomy). You may see it referred to as a urostomy, an ileal conduit or urinary diversion.
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
The Need for Augmentation after Bladder Exstrophy Closure
 Annals of Pediatric Surgery Vol 5, No 2, April 2009, PP 109-114 Original Article The Need for Augmentation after Bladder Exstrophy Closure Mohammed Abdel-Latif Ayad, Ehab El-Shafei, Hatem Abdel-Kader,
Annals of Pediatric Surgery Vol 5, No 2, April 2009, PP 109-114 Original Article The Need for Augmentation after Bladder Exstrophy Closure Mohammed Abdel-Latif Ayad, Ehab El-Shafei, Hatem Abdel-Kader,
Urethral catheter removal 3 days after radical retropubic prostatectomy is feasible and desirable
 Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
BLADDER CANCER: PATIENT INFORMATION
 BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
Robotic assisted laparoscopic radical cystectomy for bladder carcinoma: early experience and oncologic outcomes
 Formosan Journal of Surgery (2012) 45, 178e182 Available online at www.sciencedirect.com journal homepage: www.e-fjs.com ORIGINAL ARTICLE Robotic assisted laparoscopic radical cystectomy for bladder carcinoma:
Formosan Journal of Surgery (2012) 45, 178e182 Available online at www.sciencedirect.com journal homepage: www.e-fjs.com ORIGINAL ARTICLE Robotic assisted laparoscopic radical cystectomy for bladder carcinoma:
Q&A. Fabulous Prizes. Collecting Cancer Data: Bladder, Renal Pelvis, and Ureter 5/2/13. NAACCR Webinar Series
 Collecting Cancer Data Bladder & Renal Pelvis NAACCR 2012 2013 Webinar Series Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data Bladder & Renal Pelvis NAACCR 2012 2013 Webinar Series Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Urological Care of the Paralyzed Patient*
 Urological Care of the Paralyzed Patient* ROBERT H. HACKLER, M.D. Urologist, McGuire Veterans Administration Hospital, Richmond, Virginia, and Assistant Pr?fessor o_f. [!rology, pep~rtment of Surgery,
Urological Care of the Paralyzed Patient* ROBERT H. HACKLER, M.D. Urologist, McGuire Veterans Administration Hospital, Richmond, Virginia, and Assistant Pr?fessor o_f. [!rology, pep~rtment of Surgery,
Prostate Cancer Case Study 1. Medical Student Case-Based Learning
 Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
URINARY DIVERSION SURGERY: WHAT THE RADIOLOGIST NEEDS TO KNOW
 URINARY DIVERSION SURGERY: WHAT THE RADIOLOGIST NEEDS TO KNOW Poster No.: C-2327 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Salvador; Santander/ES Keywords: Urinary Tract / Bladder, CT, Complications,
URINARY DIVERSION SURGERY: WHAT THE RADIOLOGIST NEEDS TO KNOW Poster No.: C-2327 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Salvador; Santander/ES Keywords: Urinary Tract / Bladder, CT, Complications,
1. Introduction. 2. Methods. high-risk NMIBC in men with and without a prior history of RT for PC.
 ISRN Urology Volume 2013, Article ID 405064, 5 pages http://dx.doi.org/10.1155/2013/405064 Research Article Radical Cystectomy after BCG Immunotherapy for High-Risk Nonmuscle-Invasive Bladder Cancer in
ISRN Urology Volume 2013, Article ID 405064, 5 pages http://dx.doi.org/10.1155/2013/405064 Research Article Radical Cystectomy after BCG Immunotherapy for High-Risk Nonmuscle-Invasive Bladder Cancer in
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
Health-Related Quality-of-Life Following Modified Ureterosigmoidostomy (Mainz Pouch II) as Continent Urinary Diversion
 European Urology European Urology 46 (2004) 591 597 Health-Related Quality-of-Life Following Modified Ureterosigmoidostomy (Mainz Pouch II) as Continent Urinary Diversion Patrick J. Bastian a,*, Peter
European Urology European Urology 46 (2004) 591 597 Health-Related Quality-of-Life Following Modified Ureterosigmoidostomy (Mainz Pouch II) as Continent Urinary Diversion Patrick J. Bastian a,*, Peter
