Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion
|
|
|
- Justina Cain
- 6 years ago
- Views:
Transcription
1 UROLOGICAL ONCOLOGY Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion Bin Sun, Jing-Min Yan, Jian-Ye Li, He-Qing Guo, Quan Hong, Zhi-Yong Yao, Gao-Biao Zhou, Guang-Xin Pan, Xian- Chu Li Department of Urology, the General Air Force Hospital of People's Liberation Army, Beijing , China. Purpose: The aim of this study was to investigate the long-term clinical effects of sigmoidrectal pouch for urinary diversion. Materials and Methods: A total of 45 patients, including 40 males and 5 females, underwent sigmoid-rectal pouch procedure. The patients aged from 38 to 70 years with a mean age of 59 years. The postoperative follow-up ranged from 6 months to 19 years with an average of 6 years. Postoperative continence and voiding were analyzed, urinary reservoir pressure was measured and the complications of upper urinary tract were determined. The index of quality of life (QoL) in the International Prostate Symptom Score (IPSS) was used to evaluate the degree of satisfaction to urinate. Corresponding Author: Heqing Guo, MD Department of Urology, the General Air Force Hospital of People's Liberation Army, No. 30 Fucheng Road Haidian District, Beijing , China. Tel: Fax: heqingguocn@126.com Results: Forty patients had slight incontinence in the early postoperative stage and could control urination well 30 days postoperatively. The volume of pouch was ml with an average of 375 ml. The basic pressure during filling period was 6-20 cmh 2 O with an average 15 cmh 2 O, the maximum filling pressure was cmh 2 O with an average 26 cmh 2 O. The compliance of sigmoid-rectal pouch was fine with an average of 30 (range 18-40) ml/ cmh 2 O. There were no severe complications such as hyperchloremic acidosis or retrograde pyelonephritis. Six patients had slight hydronephrosis. The index of QoL were 0-2 in 20 patients, 3 in five patients and 4 in two patients. Conclusion: The sigmoid-rectal pouch operation was simple and acceptable by surgeons and patients. It may be an ideal urinary diversion for patients with muscle-invasive bladder cancer, especially for patients on whom urethrectomy should be done. Received October 2013 Accepted April 2014 Keywords: reconstructive surgical procedures; urinary diversion; methods; urinary reservoirs; surgery; continent; carcinoma; transitional cell; urinary bladder neoplasms. Vol. 11 No. 03 May - June
2 INTRODUCTION The incidence of bladder cancer ranks 11th among all malignant tumors in the world and ranks 7th in men, out of place in the top 10 in women. (1) In Urinary tract malignant tumors, the incidence of bladder cancer ranks second, while transitional cell carcinoma accounts for 90%. (2) Although most bladder cancers are non-muscle invasive, about 30% still manifest or develop into invasive cancers, requiring radical cystectomy, pelvic lymphadenectomy and urinary diversion (UD), which can improve the survival rates and reduce the chance of local recurrence and distant metastasis in patients. There are many methods of UD and mainly be categorized into noncontinent diversion, continent diversion. Among those methods, orthotopic neobladder and Bricker operation are most widely performed on the patients. The former could make patients to urinate near to physiological. Moreover, the recurrence of cancer in residual urethra is also a concern. Bricker operation is simple and more endurable, but patients have to carry urine collection bag due to abdominal colostomy. Continence preserved with anus is another choice. In early operations, ureters were connected to sigmoid flexure or rectum directly and this kind of operations tends to lead to retrograde infection, hyperchloremic acidosis and hydronephrosis. In 1993, Fisch reported urinary diversion in which sigmoid colon and rectum were folded to form a pouch and ureterosigmoidostomy was performed to control defecation and urination by anus (Mainz pouch II). Relative to early operations, this improved operation reduces the complications and can get reasonable compliance of urinary reservoir. The continence and life quality of patients greatly improved. For summarizing the long-term clinical effects of sigmoid-rectal pouch for urinary diversion, we analyzed the clinical data of 45 patients who were performed sigmoid-rectal pouch for UD. MATERIALS AND METHODS Clinical Data Forty-five patients were included in our study treated by radical cystectomy for invasive bladder cancer with the urinary diversion of sigmoid-rectal pouch between June 1993 to June 2012 at the Air Force General Hospital. Data of the patients are summarized in Table 1. All the cases were muscle invasive bladder cancer, which were mainly multiple bladder tumors or/and invaded bladder trigon and posterior urethra. In preoperative preparation, the sense of perianal skin was checked; digital rectal examination was conducted; barium enema was carried out to diagnose problems with rectum and sigmoid colon; at the same time, 500 ml of saline was utilized for retention enema for 1 hour to confirm that anal sphincter functioned well. This study was conducted in accordance with the declaration of Helsinki and with approval from the Ethics Committee of the General Hospital of Air Force. Written informed consent was obtained from all participants. Indications and Contraindications of Sigmoid-Rectal Pouch The indications are bladder malignancy, bladder exstrophy/ epispadias, trauma and sinus urogenitalis. The contraindications are colon cancer and polyps, and deteriorated anal sphincter function. In this study, all the patients had bladder cancers. Surgical Procedure After resection of bladder, prostate and urinary tract, anal canal was cannulated into anus, through which 200 ml diluted iodophor was installed into rectum and sustained for 10 min. The boundary spot between sigmoidal colon and rectum was taken as midpoint, where to fold and suture seromuscular layer adjacent to sigmoidal colon and rectum. Intestinal canal was split over cm along antimesenteric border in an inverted "V" shape. The wall of adjacent sigmoid colon and rectum was all sutured with catgut continuously till the nadir. The left and right ureters were dissociated and pulled out of the incision, and then derived to the paries medialis and posterior of sigma neobladder. Ureters were pulled out of two selected entrances on the neighboring intestinal wall. From these two entrances a 2-3 cm submucosal tunnel was built downwardly. A small circular incision was built on the mucosa of lower tunnel. The ureter could go through the tunnel and the mucosa of ureteral end was connected with the intestinal mucosa. An 8 French (F) supportive silicone catheter was implanted in the ureters till the pelvis, fixed and marked, and driven out of the anus. The ends from left or right ureter were marked correspondingly to observe the urine output from left and right kidney (Figure). The paries anterior of neobladder was sutured to construct the urinary reservoir, which was placed in the abdominal cavity and was fastened to the longitudinal ligaments of sacral promontory. (3) After 1630 Urological Oncology
3 Follow-Up of Sigmoid-Rectal Pouch for Urinary Diversion Sun et al Table 1. Clinical and demographic characteristics of participants. Figure. A: Reconfiguration of 20 to 24 cm of rectosigmoid into U shape to construct Mainz II pouch. B: Submucosal tunnel technique for bilateral normal caliber ureter, bilateral ureteral stents and anal tube are drawn out extracorporeally through the anus. Variables Values Sex, no. (%) Male 40 (88.9) Female 5 (11.1) Age (years), mean (range) 59 (38-70) Histopathology, no. (%) Transitional cell carcinoma 40 (88.9) Adenocarcinoma 3 (6.7) Squamous carcinoma 2 (4.4) Radical urethrectomy, no. (%) Male 32 (80) Female 0.0 (0.0) the surgery the patient should perform ambrosia and intravenous injection with high nutrient for 5-7 days, and sustaining gastro-intestinal decompression 3-5 days. The anal tube was removed 5-7 days postoperatively and the two ureter supportive catheters were removed or self-released days postoperatively. Follow-up Postoperatively, patients were evaluated at 3-month intervals for the first year, with 6-month intervals for the years 2 and 3, and annually thereafter. Urodynamic tests of urinary reservoir and ultrasound of upper urinary tract were performed at six month, one, five, ten and fifteen years, postoperatively. Intravenous urography (IVU) examination was conducted on the patients with hydronephrosis. Hydronephrosis, as well as vesicoureteral reflux and urinary tract infections were recorded. Interviews and frequency-volume charts were used to determine voiding behavior, daytime and nighttime continence. We defined daytime continence as completely dry without use of a pad and nighttime continence as completely dry with 2 or fewer voids per night. A satisfactory continence result was defined if no more than 1 pad was required during the day or night. All other cases were defined as incontinent. The European Organization for Research and Treatment of Cancer Quality of Life Questionnaire (EORTC QLQ-C30) survey was utilized to estimate the general health state of the patients. In this survey, two subjective answers from the patients were referred as the most characteristic of their health state and life quality RESULTS Follow-up All operations were performed successfully and there was no serious complication. The postoperative follow-up ranged from 6 months to 19 years with an average of 6 years. Fourteen patients died from tumor recurrence and metastasis, and 4 patients died from cardiovascular and cerebrovascular diseases. The patients survived more than 15 years in 2 cases, years in 4 cases, 5-10 years in 10 cases an 6 months to 5 years in 11 cases. Continence and Voiding After removal of anal tube, 45 patients had different degrees of daytime and nighttime incontinence in the early days. They passed urine and stools 6 to 10 times (mean 8 times) in the daytime, while 4 to 8 times (mean 5 times) at night. Three months after the surgery, all the patients well controlled defecation and urination; they passed urine and stools 4 to 6 times (mean 5 times) in the daytime and 1 to 4 times (mean 2 times) at night. From 6 months on, all the patients satisfied with urinary control. Good urinary control in the daytime was observed in 27 cases from six months to 15 years in follow-up. Three patients required urinal pad. Urinating and stools separately were achieved in 80% cases. Urinary incontinence occurred in six patients when they had diarrhea and cough. Table 2 demonstrates patient voiding patterns during follow-up. Urodynamic Testing Maximum storage capacity was ml with an average Vol. 11 No. 03 May - June
4 Table 2. Daytime and nighttime voiding patterns of 45 patients with sigmoid-rectal pouch. Voiding < 3-month (mean) 3-6 month (mean) 6 month (mean) Daytime Times 6-10 (8) 4-6 (5) 4-6 (5) Pad use (piece) Continence (%) Nighttime Times 4-8 (5) 1-4 (2) 1-4 (2) Pad use (piece) Continence (%) of 375 ml (more than 500 ml was considered as reverse flow in sigmoid colon); the average filling pressure in neobladder was 26 cmh 2 O. The compliance of sigmoid-rectal pouch was fine with an average of 30 (range 18-40) ml/cmh 2 O. The maximum pressure in neobladder at urination [15-30 cmh 2 O (average, 26 cmh 2 O)] was equal to abdominal pressure at micturition. Upper Urinary Tract There was one case of high fever complicated with unilateral hydronephrosis in the early days, which was cured by pyelostomy. In long-term follow-up, five patients had waist pain with fever and were relieved by anti-inflammatory therapy. Unilateral hydronephrosis was indicated by ultrasound and IVU in six cases. Early metabolic acidosis was observed in two patients who were recovered three months later. In the long-term follow-up, there was no metabolic acidosis, retrograde infection of the kidney or renal failure. QoL Evaluation The index of QoL and general health state of the patients were evaluated by EORTC QLQ C-30 survey at 1 year postoperatively (Table 3). Secondary Tumors There was no colorectal cancer in the 45 sigmoid-rectal pouch patients during follow up but one 64-year old patient was diagnosed as benign polyps of colon at the 2nd year postoperatively. The polyps were resected via a wire loop using colonoscopy. DISCUSSION The options of surgical procedures for UD are according to specific conditions of patients, such as age, complications, life expectancy and the history of pelvic operation, as well as the requirements of patients and the experience of surgeons. The ultimate goal of treatment is protecting renal function and improving QoL in patients. (4) Moreover, UD has not only achieved simple urine shunt and the protection of upper urinary tract, but also has reconstructed the lower urinary tract, which provides a safe, controllable method to storage and discharge urine, improves the patient's QoL. Currently, the most common procedure is orthotopic neobladder. However, only non-continent UD, such as Bricker operation, can be applied to most patients who simultaneously underwent total urethrectomy. The patients have to carry urine collection bag lifelong due to abdominal colostomy in Bricker operation, and the incidence of stoma complication is up to 24%. (5) Neobladder, allowing micturition through urethra, is most mimicking physiological state, but not suitable for the patients who have urethrostenosis or undergo urethrectomy. In addition, the surgery is complex, and the incidence of early and late operation complications is up to 12-37%. (6) Mainz pouch II is confluence of urine and feces improved by Fisch, which allows patients to control urination by anus. This operation could approve urinary continence, improve the quality of patients life and the incidence of complications is acceptable. Because of the resection of all posterior urethra, the recurrence of cancer is the same as Bricker operation theoretically. From 1993, we performed this operation on 45 selective bladder cancer patients and the inclusion criteria mainly included cancers in trigone of bladder, bladder-neck and men s posterior urethra and patients expected without good compliance. For investigating the long-term effect of Mainz pouch II, we follow-up visited all patients. Mainz pouch II controls urination by anus. Therefore, the function of anal sphincter was assessed in the patients before 1632 Urological Oncology
5 Follow-Up of Sigmoid-Rectal Pouch for Urinary Diversion Sun et al Table 3. QLQ C-30 survey: life quality, health status and number of patients. QLQ C-30 scale Very bad Excellent No. of patients Health status Life quality Key: EORTC QLQ-C30, European Organization for Research and Treatment of Cancer Quality of Life Questionnaire. surgery. (2,6) All the patients in our study underwent digital rectal examination and urodynamic examination to exclude patients with dysfunction of anal sphincter. After ordinary enema and defecation, 500 ml saline with diodone was used for retention enema and imaging. We observed the shape and pathological changes of rectum and sigmoid colon, estimated rectal bladder capacity and calculated urination time controlled by anus. The pressure of anal sphincter was measured with urodynamic device after enema. Although all the patients had different degrees of urinary incontinence in early time, especially at night, they could well control urination 6 months after the surgery. The longer the postoperative time lasted, the better the effect of urinary control was achieved, which was speculated to correlated with that long retention of anal tube damaged the function of anal sphincter, (6) and colonic mucosal did not adapt to the stimulation of urine, as well as anastomotic edema in the early days after surgery. The stimulation from urine reduced over time, and the function of anal sphincter gradually increased. Six patients lived more than ten years and had no incontinence in the day time; mild urinary incontinence occurred only when they had diarrhea and cough. Moreover, most patients passed clear urine and stools separately, which was consistent with previous reports. (7-9) The common complications of various neobladder are urinary incontinence induced by inadequate urinary control and dysuria resulted from excessive urinary control, which turns better 6 to 12 months after surgery when the capacity and compliance of neobladder apparently improve. Bedwetting rate is especially high at night, which shows a huge difference in reports (0-67%). However, bedwetting rate of most orthotopic bladder at night is 20-30%. (10) Possible influencing factors are, detrusor-sphincter dyssynergia; the lack of feedback between neobladder and brain arousal system when the new bladder is filling at night; the deficiency of urethra sensory controlling branch, belonging to the basin plexus of pudendal nerve, could lead to the protective reflection deficiency of external sphincter when the near-end urethra is stimulated by urine; reduced muscle tension of pelvic floor at night; nocturia (due to osmotic diuresis of neobladder at night); the neobladder filling increases the occurrence of peristaltic wave. (11,12) Mainz pouch II allows patients to control urination by anus; uriesthesis is from awareness of defecation; urinary control depends on the function of anal sphincter. All the patients in our study controlled urination well, which was probably associated with evaluation of the function of anal sphincter before surgery and the training of contraction of anal sphincter after operation. There was no dysuria or residual urine in all cases. Dysuria is one of the common complications of neobladder. It is reported that 4-25% of patients need intermittent clean self-catheterization to void, which results from several reasons, including urethral angle; the opening of new bladder is not in the lowest position; allantoic wall blocks urethra opening; the patients are unable to urinate by using abdominal pressure or relaxing pelvic floor and etc. (13) The incidence of intermittent clean self-catheterization in female patients is 21-61% (14,15) due to chronic urine retention and urethral angle. Moreover, constipation is avoided because urine flushes rectum. Female patients do not change their habit of crouch a micturition. Secondary colorectal cancer is always a concern in sigmoidrectal pouch patients. The total ileo colon tumor risk in ureterosigmoidostomy (2.58%) was significantly higher than in other continent forms of UD. (16) Because the sample is small in the present study, we could not draw any conclusion on colorectal cancer rate in the 45 sigmoid-rectal pouch patients. The ideal urinary reservoir should have large capacity, low pressure and good compliance. The capacity of sigmoid-rec- Vol. 11 No. 03 May - June
6 tal pouch is equal to capacity of folded urinary reservoir plus rectum, and colon that has reverse flow can also be used as urinary reservoir with full bladder. However, the patients are not recommended to hold urine because it might increase the chance of retrograde acute pyelonephritis, and subsequent increase the risk of renal function deterioration. (17) Micturition depends on abdominal strain instead of strong contraction of urinary reservoir. In addition, the awareness of defecation from rectal can replace bladder sensation, which is missing for orthotopic neobladder. Some patients pass clear urine at most time. Urinary reservoir is established by folding sigmoid-colon rectum, which is separated from the cavity of sigmoid colon and rectum after fixation upwards and backwards, and mimic colonic diverticula. The urine continuously flushes downwards, stools form in sigmoid colon and are passed after arriving rectum, which rarely retrogrades to urinary reservoir. In addition, low pressure and good compliance of neobladder comply with resistance to reverse flow of sigmoid colon, which reduces the chance of retrograde infection. In long-term follow-up, five patients had flank pain with fever caused by retrograde infection and were treated by antibiotics. Due to the confluence of urine and excrement, urine and stool routine tests are not available. Therefore, the diagnosis of retrograde infection stands on the symptoms, such as fever with flank pain, and sometimes nephrostomy drainage is performed as early as possible if the efficacy is not satisfying. Hydronephrosis is one of the complications of UD. Various anti-reflux techniques always might result in anastomotic stenosis between ureter and urinary reservoir. It is controversial with respect to ureterocystic anti reflux replantation, which includes submucosal tunneling, ureteral papilla implantation and etc. Some people believe neobladder without high pressure and urinary catheterization rarely has reflex and infection, and anti-reflux techniques are not necessary to be performed. All the patients had submucosal tunneling, in which the tunnel was wide enough at anastomosis. Emphasis on anti-reflux increases the chance of obstruction. There were six cases of mild unilateral hydronephrosis during the follow up interval of 3 to 6 months. The temporary hydronephrosis might be correlated to the edema of anastomotic stoma mucosa. No special therapy was applied and the hydronephrosis disappeared gradually. Recently, Jin and colleagues (18) has demonstrated that ureteral obstruction is the first and independent risk factor of renal function damage in the patients who survive more than 10 years after ileal conduit UD and ileal orthotopic bladder. In ileal, colonic neobladder and all kinds of intestinal bladder substitution, the incidences of pure metabolic acidosis are 5.5%, 13.3% and 11.1%, and the incidence with concomitant hyperchloremia are 5.5%, 8.9% and 7.9%, respectively. Oral sodium bicarbonate is usually administered for acidosis. (19) Mainz pouch II involves less and lower intestinal canal, thus the complications occur less, which is one of the advantages. There were two cases of metabolic acidosis and hypokalemia who discontinued the 1.5 g postoperative bicarbonate daily protocol, and were corrected with oral intake of bicarbonate and potassium tablets. The incidence of metabolic acidosis and hypokalemia was lower than previous report which described high incidence of acidosis and even lethal acidosis. (7,20) This was considered to correlate with long segment of intestine and inadequate compensatory renal function. The surgery is simple and easy for surgeons to perform and for patients to accept. The procedure involves folding and suture of seromuscular layer adjacent to sigmoid colon and rectum, as well as simple submucosal tunneling for anastomosis. There is no need to intercept large segment of intestine canal and perform complex anti reflex techniques. The index of QoL were high in patients. (21-23) Except some male patients were not used to crouch a micturition, most patients satisfied QoL in our research. The ideal UD should meet the following conditions: neobladder can independently control urination, enough capacity, low pressure, resistant to retrograde infection, without metabolic disorders, simple procedures, easy to learn and low incidence of surgical complications. (24) Most pristine urochesia diversions were abandoned because of lack of aforementioned characteristics, but some improved operations can also reach satisfied effect and improve the patients QoL. According to our follow-up, Mainz pouch II basically meets the above requirements. It may be an ideal UD technique for patients who need total urethrectomy due to tumor in urinary tract, have normal function of anal sphincter, and are unable to pass urine through urethra because of urethrostenosis. One of the most important objective of UD is to improve patients QoL. Orthotopic neobladder is the main method 1634 Urological Oncology
7 Follow-Up of Sigmoid-Rectal Pouch for Urinary Diversion Sun et al selected by many medical centers because it could make patients to recover physiological urination as possible. It s long-term complications includes, urinary incontinence (20-30%), ureter-intestines anastomotic stenosis (3-18%), retention of urine (4-12%), metabolic disease and etc. (25,26) Some urologists think the reasonable urinary reservoir and QoL improving of Mainz pouch II may be superior to orthotopic neobladder, so patients should be told the advantages and disadvantages of both operations and return the options to patients themselves if the pathogenic conditions permit. CONFLICT OF INTEREST None declared. REFERENCES 1. Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics CA Cancer J Clin. 2011;61: Fleshner NE, Herr HW, Stewart AK, Murphy GP, Mettlin C, Menck HR. The National Cancer Data Base report on bladder carcinoma. Cancer. 1996;78: Lampel A, Fisch M, Stein R, et al. Continent diversion with the Mainz pouch. World J Urol. 1996;14: Elmar WG, Alexander R, Wiking M. Complications and quality of life following urinary diversion after cystectomy. EAU Update Series. 2005;: Madersbacher S, Schmidt J, Ebele JM, et al. Long-term outcome of ileal conduit diversion. J Urol. 2003;169: Szűcs M, Keszthelyi A, Szendrői A, et al. Investigation of anal sphincter function following Mainz pouch type II urinary diversion after radical cystectomy. Int Urol Nephrol. 2012;44: Zhvania G, Mshvildadze Sh, Managadze G, Khvadagiani G. Results of radical cystectomy with Mainz pouch II diversion (single institution experience). Georgian Med News. 2012;211: Alemu MH: Mainz II pouch: continent urinary diversion, for bladder extrophy epispadia complex and irreparable VVF: a 5 year comprehensive retrospective analysis. Ethiop Med J. 2010;48: Sherwani Afak Y, Wazir BS, Hamid A, Wani MS, Aziz R. Comparative study of various forms of urinary diversion after radical cystectomy in muscle invasive carcinoma urinary bladder. Int J Health Sci. 2009;3: Hautmann RE, Abol-EneinH, Hafez K, et al. Urinary diversion. Urology. 2007;69 (1 Suppl): Ghoneim MA, Shaaban AA, Mahran MR, Kock NG. Further experience with the urethral Kock pouch. J Urol. 1992;147: Steers WD. Voiding dysfunction in the orthotopic neobladder. World J Urol. 2000;18: Anderson CB, Cookson MS, Chang SS, Clark PE, Smith JA Jr, Kaufman MR. Voiding function in women with orthotopic neobladder urinary diversion. J Urol. 2012;188: Finley DS, Lee U, McDonough D, Raz S, dekernion J. Urinary retention after orthotopic neobladder substitution in females. J Urol. 2011;186: Hautmann RE, Abol-Enein H, Davidsson T, et al. ICUD-EAU International Consultation on Bladder Cancer 2012: Urinary diversion. Eur Urol. 2013; 63: Osawa T, Shinohara N, Maruyama S, et al. Long-term renal function outcomes in bladder cancer after radical cystectomy. Urol J. 2013;10: Jin XD, Roethlisberger S, Burkhard FC, Birkhaeuser F, Thoeny HC, Studer UE. Long-term renal function after urinary diversion by ileal conduit or orthotopic ileal bladder substitution. Eur Urol. 2012;61: Varol C, Studer UE. Managing patients after an ileal orthotopic bladder substitution. J Br Urol. 2004;93: Ignjatovic I, Basic D. Modified Mainz pouch II (Sigma Rectum pouch) urinary diversion: 12 years experience. Acta Chir Iugosl. 2007;54: Dzamic Z, Hadzi Djokic J, Acimovic M, et al. Modified Mainz pouch II urinary diversion and quality of life. Acta Chir Iugosl. 2007;54: Romics I, Riesz P, Keszthelyi A, Pánovics J. Experiences with radical cystectomy combined with urinary diversion by ureteral sigma pouch (Mainz-pouch II) in bladder cancer patients. Orv Hetil. 2006;147: Patrick JB, Peter A, Herbert H, et al. Health-related quality-of-life following modified ureterosigmoidostomy (Mainz pouch II) as continent urinary diversion. Eur Urol. 2004;46: Ardelt PU, Woodhouse CR, Riedmiller H, Gerharz EW. The efferent segment in continent cutaneous urinary diversion: a comprehensive review of the literature. BJU Int. 2012;109: Stein JP, Dunn MD, Quek ML, Miranda G, Skinner DG. The orthotopic T pouch ileal neobladder: experience with 209 patients. J Urol. 2004;172: Abol-Enein H, Ghoneim MA. Functional results of orthotopic ileal neobladder with serous-lined extramural ureteral reimplantation: experience with 450 patients. J Urol. 2001;165: El Bahnasawy MS, Osman Y, Gomha MA, Shaaban AA, Ashamallah A, Ghoneim MA. Nocturnal enuresis in men with an orthotopic ileal reservoir: urodynamic evaluation. J Urol. 2000;164:10-3. Vol. 11 No. 03 May - June
Bladder replacement in men and women: when and when not? Outline. Continent Diversion History
 1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $
 European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution
 European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
URINARY DIVERSIONS. Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania
 URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent Pouch with Abdominal Stoma
 Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Abstract. Original Article
 Original Article Middle East Journal of Cancer; July 2015; 6(3): 165-170 A Comparison of Early Results and Patient Satisfaction Rate between Modified Radical Cystectomy with Mainz II Urinary Diversion
Original Article Middle East Journal of Cancer; July 2015; 6(3): 165-170 A Comparison of Early Results and Patient Satisfaction Rate between Modified Radical Cystectomy with Mainz II Urinary Diversion
URINARY DIVERSIONS. Winter 2016 Dr P. O Malley
 URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
Surgical Atlas Orthotopic ileal neobladder
 Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Comparison of Three Types of Continent Urinary Diversions in a Single Center
 Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate
 European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report
 198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
Cystectomies and bladder preservation: What you need to know
 Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Radical cystectomy and urinary diversion: Normal anatomy and complications
 Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
Modified ureterosigmoidostomy for management of malignant and non-malignant
 334 E a s t A f r i c a n M e d i c a l J o u r n a l July 2008 East African Medical Journal Vol. 85 No. 7 July 2008 Modified ureterosigmoidostomy for management of malignant and non-malignant conditions
334 E a s t A f r i c a n M e d i c a l J o u r n a l July 2008 East African Medical Journal Vol. 85 No. 7 July 2008 Modified ureterosigmoidostomy for management of malignant and non-malignant conditions
Department and Clinic of Urology, Medical University of Silesia, Katowice, Poland
 BioMed Research International Volume 2015, Article ID 306191, 4 pages http://dx.doi.org/10.1155/2015/306191 Clinical Study Sacrocolpopexy with Polypropylene Tape as Valuable Surgical Modification during
BioMed Research International Volume 2015, Article ID 306191, 4 pages http://dx.doi.org/10.1155/2015/306191 Clinical Study Sacrocolpopexy with Polypropylene Tape as Valuable Surgical Modification during
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Department of Urology, Theodor Bilharz research Institute, Cairo, Egypt
 Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Mainz Pouch II technique: 10 years experience
 Original Article 10 YEARS EXPERIENCE OF MAINZ POUCH II G. D ELIA et al. In this section, the use of the Mainz Pouch II is examined in some detail, from Mainz (where it originated), and from London. Both
Original Article 10 YEARS EXPERIENCE OF MAINZ POUCH II G. D ELIA et al. In this section, the use of the Mainz Pouch II is examined in some detail, from Mainz (where it originated), and from London. Both
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Original Paper. Urol Int 2002;69:
 Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Long-Term Complications of Conduit Urinary Diversion
 Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Muscle-invasive bladder cancer
 Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Hydronephrosis. What is hydronephrosis?
 What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
BCAN Fall Series: Survivorship
 BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan
 ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Body Image Following Radical Cystectomy and Ileal Neobladder or Conduit in Korean Patients
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.3.161 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.3.161&domain=pdf&date_stamp=2014-03-17
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.3.161 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.3.161&domain=pdf&date_stamp=2014-03-17
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Radical Cystectomy Often Too Late? Yes, But...
 european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT
 Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled urinary, sexual and reproductive conditions. The chapter
Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled urinary, sexual and reproductive conditions. The chapter
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al.
 Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Physiologic Anatomy and Nervous Connections of the Bladder
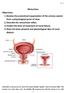 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Find Medical Solutions to Your Problems HYDRONEPHROSIS. (Distension of Renal Calyces & Pelvis)
 HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
Urinary diversion: A seven year experience in Maiduguri North Eastern Nigeria
 Sky Journal of Medicine and Medical Sciences Vol. 3(6), pp. 071-076, September, 2015 Available online http://www.skyjournals.org/sjmms ISSN 2315-8808 2015 Sky Journals Full Length Research Paper Urinary
Sky Journal of Medicine and Medical Sciences Vol. 3(6), pp. 071-076, September, 2015 Available online http://www.skyjournals.org/sjmms ISSN 2315-8808 2015 Sky Journals Full Length Research Paper Urinary
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal neobladder after radical cystectomy
 Talat et al. BMC Urology (2018) 18:94 https://doi.org/10.1186/s12894-018-0406-8 TECHNICAL ADVANCE Open Access The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal
Talat et al. BMC Urology (2018) 18:94 https://doi.org/10.1186/s12894-018-0406-8 TECHNICAL ADVANCE Open Access The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
CHILDREN who require urinary diversion rarely have malignant disease, therefore,
 THE ILEAL CONDUIT IN THIRTY-FIVE CHILDREN RALPH A. STRAFFON, M.D., Department of Urology RUPERT B. TURNBULL, JR., M.D., Department of General Surgery and ROBERT D. MERCER, M.D. Department of Pediatrics
THE ILEAL CONDUIT IN THIRTY-FIVE CHILDREN RALPH A. STRAFFON, M.D., Department of Urology RUPERT B. TURNBULL, JR., M.D., Department of General Surgery and ROBERT D. MERCER, M.D. Department of Pediatrics
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
MP A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction. Gaines W. Hammond Jr.
 MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
MP73-06 - A Prospective Evaluation of the Catheter Science M3 Mini Catheter for Patients with Prostatic Obstruction Gaines W. Hammond Jr. MD FACS M3 Mini Catheter M3 Segmented M3 Plus Dynamic Wings M3
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
THE operation of reimplantation of the ureter into the bladder has undergone
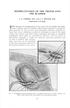 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY. THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel
 PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional Outcomes, Urodynamic Features, and Complications
 Original Article http://dx.doi.org/10.3349/ymj.2013.54.3.690 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(3):690-695, 2013 The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional
Original Article http://dx.doi.org/10.3349/ymj.2013.54.3.690 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(3):690-695, 2013 The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Information for Patients. Primary urethral cancer. English
 Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Rectal Cancer. About the Colon and Rectum. Symptoms. Colorectal Cancer Screening
 Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Section H Bladder and Bowel
 Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
Continence Promotion. CATHETER CARE CONTINENCE CARE CONVEENS STOMAS
 Continence Promotion. 1 CATHETER CARE CONTINENCE CARE CONVEENS STOMAS CHARACTERISTICS OF URINE 2 A liquid excrement consisting of water, salts, and urea, which is made in the kidneys then released through
Continence Promotion. 1 CATHETER CARE CONTINENCE CARE CONVEENS STOMAS CHARACTERISTICS OF URINE 2 A liquid excrement consisting of water, salts, and urea, which is made in the kidneys then released through
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER WITH SEROUS-LINED EXTRAMURAL URETERAL REIMPLANTATION: EXPERIENCE WITH 450 PATIENTS
 0022-5347/01/1655-1427/0 THE JOURNAL OF UROLOGY Vol. 165, 1427 1432, May 2001 Copyright 2001 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER
0022-5347/01/1655-1427/0 THE JOURNAL OF UROLOGY Vol. 165, 1427 1432, May 2001 Copyright 2001 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing
 Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Open Radical Cystectomy Tips and Tricks in Males and Females
 Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
The Malone Antegrade Continence Enema (MACE) Principle In Children: Is It Important If the Conduit Is Implanted In the Left or the Right Colon?
 Pediatric Urology Malone Antegrade Continence Enema (MACE) International Braz J Urol Vol. 34 (2): 206-213, March - April, 2008 The Malone Antegrade Continence Enema (MACE) Principle In Children: Is It
Pediatric Urology Malone Antegrade Continence Enema (MACE) International Braz J Urol Vol. 34 (2): 206-213, March - April, 2008 The Malone Antegrade Continence Enema (MACE) Principle In Children: Is It
UTI and UrinaryTract Reconstruction
 EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique
 Bladder Cancer 1 (2015) 73 79 DOI 10.3233/BLC-140002 IOS Press Research Report 73 Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique Chandra K. Flack, M. Francesca
Bladder Cancer 1 (2015) 73 79 DOI 10.3233/BLC-140002 IOS Press Research Report 73 Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique Chandra K. Flack, M. Francesca
Koji Ichihara Hiroshi Kitamura Naoya Masumori Fumimasa Fukuta Taiji Tsukamoto
 Int J Clin Oncol (2013) 18:75 80 DOI 10.1007/s10147-011-0346-8 ORIGINAL ARTICLE Transurethral prostate biopsy before radical cystectomy remains clinically relevant for decision-making on urethrectomy in
Int J Clin Oncol (2013) 18:75 80 DOI 10.1007/s10147-011-0346-8 ORIGINAL ARTICLE Transurethral prostate biopsy before radical cystectomy remains clinically relevant for decision-making on urethrectomy in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity
 Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 1, March: 29-39, 2010 Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity OMAYA A.H. NASSAR, M.D., F.R.C.S.
Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 1, March: 29-39, 2010 Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity OMAYA A.H. NASSAR, M.D., F.R.C.S.
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Bowel Function After Spinal Cord Injury
 Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Robotic Appendicovesicostomy
 Robotic Appendicovesicostomy Cheryl Baxter, MSN,RN,CPNP Daniel DaJusta, MD Kristina Booth, MSN,RN,FNP Roadmap for Presentation Part 1 Pre-surgical/historical neurogenic bladder- Baxter Part 2 Robotic appendicovesicostomy/
Robotic Appendicovesicostomy Cheryl Baxter, MSN,RN,CPNP Daniel DaJusta, MD Kristina Booth, MSN,RN,FNP Roadmap for Presentation Part 1 Pre-surgical/historical neurogenic bladder- Baxter Part 2 Robotic appendicovesicostomy/
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Indications and effectiveness of the open surgery in vesicoureteral reflux
 Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
Radical cystectomy for bladder cancer: oncologic outcome in 271 Chinese patients
 Original Article : oncologic outcome in 271 Chinese patients Zhi-Ling Zhang, Pei Dong, Yong-Hong Li, Zhuo-Wei Liu, Kai Yao, Hui Han, Zi-Ke Qin and Fang-Jian Zhou Abstract Few large scale studies have reported
Original Article : oncologic outcome in 271 Chinese patients Zhi-Ling Zhang, Pei Dong, Yong-Hong Li, Zhuo-Wei Liu, Kai Yao, Hui Han, Zi-Ke Qin and Fang-Jian Zhou Abstract Few large scale studies have reported
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
90% of bladder tumours are transitional cell carcinoma (TCC), the remaining 10% of cases are squamous cell carcinoma, adenocarcinoma and sarcoma.
 The Role of the Interventional Radiologist in Management of Post-Radical Cystectomy Ureteral Obstruction : A Case Review of Retrograde Transileal Conduit Ureteric Stents. Poster No.: C-2288 Congress: ECR
The Role of the Interventional Radiologist in Management of Post-Radical Cystectomy Ureteral Obstruction : A Case Review of Retrograde Transileal Conduit Ureteric Stents. Poster No.: C-2288 Congress: ECR
