european urology xxx (2006) xxx xxx
|
|
|
- Wesley Fletcher
- 5 years ago
- Views:
Transcription
1 available at journal homepage: Female Urology - Incontinence Supratrigonal VVF Repair by Modified O Connor s Technique- An Experience of 26 Cases 6 7 Divakar Dalela a, Priyadarshi Ranjan b, *, Pushpa Lata Sankhwar c, Satya N. Sankhwar a, Vineet Naja a, Apul Goel a 8 a Department of Urology, King George Medical University, Lucknow, UP, India 9 b Department of Surgery, King George Medical University, Lucknow, UP, India c Department of Obstetrics and Gynecology, King George Medical University, Lucknow, UP, India Article info Article history: Accepted December 13, 2005 Published online ahead of print on Keywords: Supratrigonal Vesico-vaginal fistula Cystotomy Abstract Objective: To report the technical modifications of O Connor s procedure and their outcome in 26 supratrigonal vesico vaginal fistulae. Materials and methods: Twenty-six cases of supratrigonal VVF (17 primary, 9 recurrent) were operated using the described modifications. It consisted of approaching the bladder transperitoneally, without dissecting the retropubic space, making a short sagittal or parasagittal cystotomy in between stay sutures, liberal use of bladder rotation flaps instead of midline closure, using single layer, continuous, closely placed, interlocking stitches for bladder as well as vaginal approximation and universal use of vascularised tissue interposition. Results: Mean fistula size was 2.8 cm (range 1.0 to 3.7). Mean operative time was 104 minutes, and blood loss was insignificant. Three patients required ureteroneocystostomy. All patients were dry after 2 3 weeks of suprapubic and per urethral catheter drainage. One patient persisted with stress urinary incontinence. No patient on follow up complained of features suggestive of prolonged ileus, peritonitis or adhesive intestinal obstruction. Conclusion: Modified O Connor s repair is safe and achieves excellent functional results. It requires a shorter cystotomy instead of bi-valving of the bladder, thus minimizes tissue trauma, intraoperative blood loss and operating time. It also gives option of tailoring the cystotomy in sagittal or parasagittal line, according to the site and size of the fistula, and thus permits closure of fistula by rotation of bladder flap into the defect without any lateral traction on the bladder edges. Retropubic dissection and drainage of the retropubic space is also not required. # 2005 Published by Elsevier B.V. * Corresponding author. Sector-20, house-no-25, Indira Nagar, Lucknow, UP , India. Tel address: priydarshiranjan@sify.com (P. Ranjan) /$ see front matter # 2005 Published by Elsevier B.V. doi: /j.eururo
2 Introduction 2. Materials and methods Vesicovaginal fistula (VVF) is a distressing disease with social, hygienic, urological, and psychosexual consequences. Supratrigonal VVF results from a variety of causes- in west more common is to see iatrogenic fistula, while in developing world obstetric etiology prevails. In the west, 90% cases are caused by inadvertent trauma to the bladder during surgery [1]. Hysterectomy accounts for 75% of such fistulae [2]. Recent meta-analysis by Gilmour suggests that iatrogenic bladder injury occurs in 10.4 per 1000 cases [3]. In developing countries, such fistulae often result following caesarean section for prolonged/complicated obstructed labour where a combination of surgical trauma and ischemia (caused by fetal head compression) jointly contribute to the occurrence of fistula. The variations in the degree of ischemic damage and resultant fibrosis have forced surgeons to modify their techniques to achieve the best results [4]. The O Connor operation has been the most accepted method of repairing such supratrigonal VVF till date. The traditional O Connor s technique utilizes suprapubic access for extra-peritoneal dissection of the retropubic space to dissect the urinary bladder, followed by long sagittal cystotomy (bivalving the bladder) carried till the fistula (Fig. 1). The fistulous tract is then excised followed by two-layered closure after tissue transposition in between the vagina and the bladder walls. Herein we describe our modifications of the O Connor technique for repairing a supratrigonal VVF using the trans peritoneal approach. Fig. 1 Traditional O Connor s procedure involves a long cystotomy coursing through the anterior wall and dome of the bladder (bi-valving). Twenty-six patients (17 primary, 9 recurrent) admitted between January 2000 to June 2004 with supratrigonal VVF were operated using these modifications. The interval between the onset of leakage and final surgical correction ranged from 6 weeks to 8 years (median 10 weeks). A detailed medical history was recorded focusing on the cause of fistula and previous attempts at repair. None of the patients had received pelvic irradiation. Two cases had vesical calculus, which was removed by transurethral cystolitholapaxy 2 3 weeks prior to definitive closure. Both these patients had an obstetric fistula. Prior stone removal eliminates the potential source of infection and mucosal edema of the bladder and thus provides optimal bladder tissue for healing of the fistula [5]. We prefer transurethral cystolitholapaxy for such stones owing to its minimally invasive nature and the ability to break even large stones [5]. Vaginal assessment was done to inspect and palpate the vaginal opening of the fistula. Any local genital infection was treated before surgery. Cystoscopy was done to establish the supratrigonal location of the fistula and assess its proximity to the ureteric orifices. An excretory urogram was performed in selected patients where ureteric orifices were too close to VVF. One patient had bilateral and 2 patients had unilateral ureteric orifice involvement. For this procedure, the patient is placed in trendelenberg position. The abdomen is opened via an infraumbilical midline/pfannensteil incision. The peritoneum is opened to approach the posterior surface of bladder. The bowel is gently packed with sponges before the cystotomy and effective suction is used to minimize urinary spillage. To elevate the posterior bladder wall, full thickness stay sutures are placed, using chromic catgut, at the lower end of posterior wall of the bladder. An 18F Foley catheter is put in the bladder perurethrally, prior to placement of stay sutures, and the balloon is inflated upto cc. It facilitates the perception of thickness of posterior bladder wall while placing full thickness stay sutures and at the same time prevents entrapment of anterior bladder wall. A short cystotomy beginning about 2 3 cms away from cul-de-sac is made in between these stay sutures, limited to the posterior bladder wall (Fig. 2). Routinely we use three fine malleable daever retractors to enhance the intra vesical visibility by appropriate retraction within the cystotomy. The shorter cystotomy does not compromise vision. The proximity of the ureteric orifice to the VVF is assessed at this stage and only in those cases where orifice sits close to the fistula edge, a 5 6 Fr infant feeding tube is passed into the ureters before fistula dissection is commenced. As the dissection progresses towards and around the fistula, additional stay sutures are placed along the edges of the cystotomy at mirror image locations. These stay sutures later on act as guide for approximation of cystotomy edges. Apart from providing effective anchorage to lift up the posterior bladder wall, they also minimize oozing from the cystotomy edges, and are thus haemostatic. In a small fistula, the cystotomy is extended to encircle the fistula and excision of the fistula is done as the traditional
3 Fig. 2 The cystotomy is made only on the posterior bladder wall in between stay sutures. technique. If the fistula is large (>2.5 cm), the cystotomy is directed in parasagittal line towards one side of the fistula (Fig. 3). It leads to formation of a flap of bladder wall after the fistula is excised (Fig. 4). This flap is subsequently rotated to close the bladder wall defect (Fig. 5). Complete excision of the fistula is done and the plane between bladder and vaginal wall is dissected as in traditional O Connor s procedure. This method of bladder closure ensures a tensionless suture line (Fig. 6). The vaginal wall is closed in single layer with continuous interlocking, closely placed stitches using either 1 0 0/ polyglecaperone (monocryl) or polyglactin (vicryl) in a transverse line. Greater omentum is mobilized and is anchored to anterior vaginal wall to completely cover the vaginal suture line. In 2 patients, where omentum was considered insufficient, paravesical peritoneal flaps were used Fig. 3 The cystotomy is extended in parasagittal line to one side, in case of a large fistula. Fig. 4 The medial portion of the bladder edge after excision of fistula forms a flap. Fig. 5 The bladder flap is rotated and advanced into the defect. for interposition. The urinary bladder is also closed in single layer using polyglecaprone or polyglactin by continuous interlocking, closely placed stitches. Suprapubic cystostomy (SPC) and per urethral catheters are placed to drain the bladder and the cystotomy is closed. The SPC is extraperitonealized and the laparotomy wound is closed in layers. No drain is placed routinely. The suprapubic catheter is removed after 2 weeks and the per urethral catheter is removed after 3 weeks. The patients
4 Fig. 6 The bladder flap achieves tensionless suture line in the bladder wall. are advised for sexual abstinence for 3 months. All patients were advised to void at frequent intervals to prevent over distension of the bladder. Patients desiring future pregnancy were advised strict antenatal monitoring, regular follow up in the antenatal clinic and elective caesarean section. 3. Results Mean age of our patients was 21.4 (range-18 to 41) years. Four patients had fistula after hysterectomy (2-transvaginal hysterectomy and 2 transabdominal), while 22 patients had a VVF following manipulations for obstructed labour. Twenty out of 22 patients who had obstructed labor were short statured (height less than 5 feet). Nine patients had recurrent VVF, following previous attempts at repair. Four out of them had undergone transvaginal repair and 5 were treated transabdominally at peripheral centers (no records were available). One case had developed VVF 8 years earlier and had undergone three previous failed attempts at repair, twice vaginally and once transabdominally. Mean fistula size was 2.8 cm (range 1.0 to 3.7). Three fistulae were encroaching the ureteric orifice and they required additional ureteroneocystostomy. Eighteen patients had a larger fistula (>2.5 cm) and were managed using parasagittal cystotomy. All of them achieved tensionless closure using the above technique. It was possible to interpose greater omentum in 24 cases whereas in 2 patients the omentum was small and atrophic hence vascularised paravesical peritoneal flap was used. Transurethral cystolitholapaxy was done in 2 patients having vesical calculi 2 3 weeks prior to VVF closure. Thus the bladder wall edema associated with stone was negligible at the time of repair and local tissue vitality was good. Mean operative time was 104 minutes, intra operative blood loss was insignificant and none of the patients required postoperative blood transfusion. All patients were dry after 2 weeks of suprapubic and per urethral catheter drainage. The patients were followed up regularly in our out patients department, and were largely asymptomatic except some irritative lower urinary tract symptoms in 6 cases which settled spontaneously in 4 6 weeks. Postoperative micturating cystogram was done only in selected patients to document dryness. Since majority of our patients were young (mean age-21.4 years) and were desirous of future pregnancy all patients were advised caesarean section. Four patients became pregnant and had a successful outcome of pregnancy by elective caesarean section, with no resultant urological infirmity. Only 1 had stress urinary incontinence associated with urethral incompetence. She later on underwent colposuspension and was relieved. Laparotomy wound was infected in 1 patient, which healed by secondary intention. No patient on follow up complained of features suggestive of adhesive intestinal obstruction, prolonged ileus or peritonitis. Only 21 patients reported for follow up after 1 5 years and they were urologically asymptomatic and continent. Three patients had dysparaunia prior to surgery, possibly due to previous surgery, which was not relieved. 4. Discussion O Connor s technique is advocated as the gold standard technique for managing supratrigonal VVF [10]. Traditional technique described by O Connor involves extraperitoneal approach to the urinary bladder [11]. It involves dissection of the urinary bladder extraperitoneally in the retropubic space. A longitudinal cystotomy is made on the anterior wall of bladder, which is advanced, coursing through the dome of the bladder, backwards towards the fistula. It results in a long cystotomy which almost bivalves the bladder. The vaginal wall is closed in 2 layers and a vascularised tissue is often interposed in between before the closure of bladder. It can be local pelvic tissue, retro pubic fat or the greater omentum after opening up the peritoneal cavity. Recently use of free grafts has also been described [12]. Ureteric catheters are placed and the bladder is closed over
5 5 Table 1 Advantages and disadvantages of our modifications of the O Connor s technique Advantages 1-Shorter cystotomy, avoids bivalving 2-Decreased blood loss 3-Decreased operating time 4-Decreased risk of anesthesia 5-Decreased postoperative voiding dysfunction 6-Preservation of retro pubic space for future SUI surgery 7-Drainage of retro pubic space not required 8-Suture economy 9-Option to tailor the cystotomy in sagittal/parasagittal plane to achieve tensionless closure of large fistula. 10-Early assessment of omentum Disadvantages 1-Limited vision 2-Needs expertise suprapubic and per urethral catheters. A drain is put in the reteropubic space. The modifications, we used in our patients consisted of approaching the bladder transperitoneally (without doing any dissection in retropubic space), which provides quick access to the posterior wall of the bladder. Stay sutures provide effective anchorage to lift up the posterior wall and minimize the oozing from the cystotomy edges. The cystotomy is very small and avoids classical bivalving of the bladder, which accounts for increased blood loss and prolonged operative time. Some people have even speculated its role in enhancing postoperative voiding dysfunction and reflux [12]. It is also possible to direct the cystotomy in parasagittal line if the fistula is large and medial side of the bladder may be rotated as a flap into the bladder defect. Thus, it minimizes the traction on the lateral edges of the bladder defect, which is inevitable when such a large fistula is closed using sagittal cystotomy. The fistulous edges are excised and the closure of both vaginal as well as bladder defect is done in single layer using closely placed interlocking stitches. We prefer to use polyglecaprone (monocryl) for this purpose as it glides through the tissues without any abrasive effect. Approaching the urinary bladder directly through the peritoneum has not added to peritonitis, adhesive intestinal obstruction or prolonged ileus, instead it allows an early inspection of omentum and offers a wider field of vision for the surgeon. The urinary spillage is negligible and of no consequence. A table enumerating the advantages and disadvantages of our modifications is enlisted (Table 1). We prefer to use omental interposition in all patients. In case it is short or atrophic we have used paravesical fat/peritoneal flap. Our approach has given us 100% success in terms of achieving continence. Ever since transabdominal approach to VVF has been described, [13] continuous refinements in the technique have given better results. Several surgical techniques have been used in these cases with failure rates ranging from 4 to 35% [14,15]. Nesrallah LJ evaluated the success rate of transperitoneal O Connor s procedure to be 100% [10] and consider it to be the gold standard for supratrigonal fistulae. In a series of 23 VVFs, Cetin concluded that the fistulas located above the interureteric ridge and fistulas encroaching the ureteric orifices, were good candidates for suprapubic approach [16]. In a series of 68 VVFs, Motiwala and colleagues attributed the success of transvesical technique to simple access, construction of a vascularised flap and utilization of vicryl suture [17]. A recent review by Huang has emphasized the importance of individually tailoring the technique and approach for each fistula [18]. Regardless of whether a transabdominal or transvaginal approach is selected, the concepts of using healthy tissue, tension free closures and reinforcing the closures in high risk situations will ensure success nearly in all times. Transabdominal-transvesical approach is the preferred method of managing large supratrigonal VVFs [6,7]. Mondet evaluated the anatomic and functional results of transperitoneal- transvesical fistula repair and concluded that it to be the reference treatment for complex supratrigonal VVFs [8]. Leng and coworkers also reported that limited transvesical repair of uncomplicated supratrigonal VVFs offers reliable success with minimal morbidity and hospital stay comparable to the transvaginal approach [9]. Recently laparoscopic VVF repairs are gaining importance [19]. Consensus is emerging that laparoscopic repair of VVF is feasible and efficacious. The modified O Connor s approach as described by us may be adopted in laparoscopic surgery as well. 5. Conclusion Vesicovaginal fistulas represent a distressing urological condition for the patient and demand meticulous skilled surgical attention [20,21]. We
6 have suggested some modifications to the original technique of O Connor s repair by approaching the fistula transperitoneally, making a smaller cystotomy limited to the posterior wall, liberal use of stay sutures to enhance exposure and reduce bleeding, using parasagittal cystotomy in large VVFs and totally avoiding reropubic dissection and drain. These modifications have minimized intraoperative blood loss and operating time without compromising the exposure and ultimate outcome. Since the retropubic space is not disturbed, it leaves the option for subsequent SUI surgery. The modifications are simple to understand and easily practicable. References [1] Tancer ML. Observations on prevention and management of vesico-vaginal fistula after total hysterectomy. Surg Gynecol Obstet 1992;175: [2] Lee AL, Symmonds RE, Williams TJ. Current status of genitourinary fistula. Obstet Gynecol 1988;72: [3] Gilmour DI, Dwyer PL, Carey MP. Lower urinary tract injury during gynecologic surgery and its detection by intraoperative cystoscopy. Obstet Gynecol 1999;94: [4] Bhandari M, Dalela D. Complexities of a vesicovaginal fistula. Arch Esp Urol 1994;47(3): [5] Dalela D, Goel A, Sankhwar SN, Singh KM. Vesical calculi with unrepaired vesicovaginal fistula: A clinical appraisal of an uncommon association. J Urol 2003;170: [6] Diaz CE, Calatrava GS, Caldentey GM, Moreno PF, Lapuerta TE, Garcia VF. Surgical repair of vesico-vaginal fistula with abdominal transvesical approach. Comments on this technique and long-term results. Arch Esp Urol 1997;50: [7] Sanchez JM, Gullian MC, Parra ML, Gomez SC, Laguna MP, Garcia AJ. Transvesical repair of non-complicated vesicovaginal fistula. Actas Urol Esp 2000;24: [8] Mondet F, Chartier EJ, Conrot P, Bitker MO, Chatelain C, Richard F. Anatomic and functional results of transperitoneal- transvesical vesico-vaginal fistula repair. Urology 2001;58: [9] Leng WW, Amundsen CL, McGuire EJ. Management of female genitourinary fistulas: transvesical or transvaginal approach. J Urol 1998;160: [10] Nesrallah LJ, Srougi M, Gittes RF. The O Connor technique: the gold standard for supratrigonal vesicovaginal fistula repair. Urology 1999;161(2): [11] O Connor VJ. Review of experience with vesicovaginal fistula repair. J Urol 1980;123: [12] El-Lateef Moharram AA, El-Raouf MA. Retropubic repair of genitourinary fistula using a free supporting graft. BJU Int 2004 Mar;93(4): [13] Legueu F. La voie trans-peritoneo-vesicale pour la cure de certaines fistules vesico-vaginales operatoires. Arch Urol Clin Necker 1914;I:1. [14] Goodwin WE, Scardino PT. Vesicovaginal and ureterovaginal fistulas: a summary of 25 years of experience. J Urol 1980;123:370. [15] Kristensen JK, Lose G. Vesicovaginal fistulas: the transperitoneal repair revisited. Scand J Urol Nephrol 1994;157:101. [16] Cetin S, Yazicioglu A, Ozgur S, Ilker Y, Dalva I. Vesicovaginal fistula repair: a simple suprapubic transvesical approach. Int Urol Nephrol 1988;20: [17] Motiwala HG, Amlani JC, Desai KD, Shah KN, Patel PC. Transvesical vesicovaginal fistula repair: a revival. Eur Urol 1991;19:24 8. [18] Huang WC, Zinman LN, Bihrle III W. Surgical repair of vesico-vaginal fistulas. Urol Clin North Am 2002;29: [19] Sotelo R, Mariano MB, Garcia-Segui A, Dubois R, Spaliviero M. Laparoscopic repair of vesicovaginal fistula. J Urol 2005;173(5): [20] Blaivas JG, Heritz DM, Rominzi LI. Early versus late repair of vesicovaginal fistulas: vaginal and abdominal approaches. J Urol 1995;153: [21] Zimmern PE, Ganabathi K, Leach GE. Vesicovaginal fistula repair. Urol Clin North Am 1994;2:
Research Article Transvesicoscopic Repair of Vesicovaginal Fistula
 Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital
 Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
SciFed Journal of Public Health. Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature
 SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
THE operation of reimplantation of the ureter into the bladder has undergone
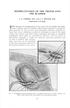 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Pan African Urological Surgeons Association. African Journal of Urology.
 African Journal of Urology (2012) 18, 175 179 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Martius flap and anterior vaginal wall
African Journal of Urology (2012) 18, 175 179 Pan African Urological Surgeons Association African Journal of Urology www.ees.elsevier.com/afju www.sciencedirect.com Martius flap and anterior vaginal wall
Laparoscopic extravesical vesicovaginal fistula repair: our technique and 15-year experience
 DOI 10.1007/s00192-014-2458-y ORIGINAL ARTICLE Laparoscopic extravesical vesicovaginal fistula repair: our technique and 15-year experience John R. Miklos & Robert D. Moore Received: 26 March 2014 /Accepted:
DOI 10.1007/s00192-014-2458-y ORIGINAL ARTICLE Laparoscopic extravesical vesicovaginal fistula repair: our technique and 15-year experience John R. Miklos & Robert D. Moore Received: 26 March 2014 /Accepted:
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Recent advances have improved the
 SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
Interposition of Omentum, Perivesical Fat, Martious Fat in Management of Lower Urinary Tract Fistula - A Comparative Study
 ORIGINAL ARTICLE Interposition of Omentum, Perivesical Fat, Martious Fat in Management of Lower Urinary Tract Fistula - A Comparative Study KHIZAR HAYAT 1, SHAH JAHAN UR REHMAN 2, MUJAHID ALAM 3, SAJJAD
ORIGINAL ARTICLE Interposition of Omentum, Perivesical Fat, Martious Fat in Management of Lower Urinary Tract Fistula - A Comparative Study KHIZAR HAYAT 1, SHAH JAHAN UR REHMAN 2, MUJAHID ALAM 3, SAJJAD
11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri)
 February 2019 11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri) Prescription for a woman whose urine is in an irksome
February 2019 11 th Dynasty- Egyptian mummies : Queen Henhenit circa 2050 BC wife of King Mentuhotep II VVF 550 BC- Ancient Egyptian documents (papyri) Prescription for a woman whose urine is in an irksome
Management of Urethrovaginal Fistulas
 european urology 50 (2006) 1000 1005 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Urethrovaginal Fistulas Dmitri Y. Pushkar *, Vladimir V.
european urology 50 (2006) 1000 1005 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Management of Urethrovaginal Fistulas Dmitri Y. Pushkar *, Vladimir V.
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Surgery of urogenital trauma in condition of war or precarity
 Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon
 Provisional PDF Published 27 April 2010 Case report, Volume 5, issue 6, 2010 Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon Pierre Marie
Provisional PDF Published 27 April 2010 Case report, Volume 5, issue 6, 2010 Quality care in vesico-vaginal obstetric fistula: case series report from the regional hospital of Maroua-Cameroon Pierre Marie
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Original Article. Abstract. Introduction
 Original Article Surgical Management of Genitourinary Fistula Muhammad Shahbaz Hanif, Khalid Saeed, Masood Ahmed Sheikh Department of Urology, Jinnah Postgraduate Medical Centre, Karachi. Abstract Objective:
Original Article Surgical Management of Genitourinary Fistula Muhammad Shahbaz Hanif, Khalid Saeed, Masood Ahmed Sheikh Department of Urology, Jinnah Postgraduate Medical Centre, Karachi. Abstract Objective:
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
The circumferential obstetric fistula: characteristics, management and outcomes
 DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Urethral Diverticula, Urethro-Vaginal Fistulae, Vesico-Vaginal Fistulae
 EAU Update Series 1 (2003) 178 185 Urethral Diverticula, Urethro-Vaginal Fistulae, Vesico-Vaginal Fistulae C.R. Chapple * Royal Hallamshire Hospital, Sheffield Teaching Hospitals NHS Trust, Glossop Road,
EAU Update Series 1 (2003) 178 185 Urethral Diverticula, Urethro-Vaginal Fistulae, Vesico-Vaginal Fistulae C.R. Chapple * Royal Hallamshire Hospital, Sheffield Teaching Hospitals NHS Trust, Glossop Road,
Primary Realignment of Posterior Urethral Rupture
 Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Retrospective study of 213 cases of female urogenital fistulae at the Department of Urology & Transplantation Civil Hospital Quetta, Pakistan
 Original Article Retrospective study of 213 cases of female urogenital fistulae at the Department of Urology & Transplantation Civil Hospital Quetta, Pakistan Haq Nawaz, Masha Khan, Faiz Muhammed Tareen,
Original Article Retrospective study of 213 cases of female urogenital fistulae at the Department of Urology & Transplantation Civil Hospital Quetta, Pakistan Haq Nawaz, Masha Khan, Faiz Muhammed Tareen,
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Changing trends in the etiology and management of vesicovaginal fistula
 International Journal of Urology (08) 5, 5--9 doi: 0./iju.49 Review Article Changing trends in the etiology and management of vesicovaginal fistula Muhammad A Malik, Muhammad Sohail, Muhammad TB Malik,
International Journal of Urology (08) 5, 5--9 doi: 0./iju.49 Review Article Changing trends in the etiology and management of vesicovaginal fistula Muhammad A Malik, Muhammad Sohail, Muhammad TB Malik,
For personal use only. Injury-free vaginal surgery: Case-based protective tactics
 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
6 THE OPERATIONS BASIC PRINCIPLES
 6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA
 ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA Il. Saltirov, Ts. Petkov, G. Georgiev, K.Petkova Department of Urology and Nephrology, Military Medical
ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA Il. Saltirov, Ts. Petkov, G. Georgiev, K.Petkova Department of Urology and Nephrology, Military Medical
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Surgical Atlas Politano-Leadbetter ureteric reimplantation
 Surg Ill SURGERY ILLUSTRATED STEFFENS et al. Surgical Atlas Politano-Leadbetter ureteric reimplantation JOACHIM STEFFENS, EBERHARD STARK, BJÖRN HABEN and ADRIAN TREIYER Department of Urology and Paediatric
Surg Ill SURGERY ILLUSTRATED STEFFENS et al. Surgical Atlas Politano-Leadbetter ureteric reimplantation JOACHIM STEFFENS, EBERHARD STARK, BJÖRN HABEN and ADRIAN TREIYER Department of Urology and Paediatric
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
Prospective study of use of drains in abdominal surgery in rural area
 Original article: Prospective study of use of drains in abdominal surgery in rural area Dr RN Patil, Dr Mudit Garg*, Dr Shaikh MH, Dr Aashay Shah, Dr Janvi Tomar, Dr Amit Karad Department of Surgery, PIMS
Original article: Prospective study of use of drains in abdominal surgery in rural area Dr RN Patil, Dr Mudit Garg*, Dr Shaikh MH, Dr Aashay Shah, Dr Janvi Tomar, Dr Amit Karad Department of Surgery, PIMS
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Appendix 1. Canadian Classification of Health Intervention Codes Used to Identify
 1 2 3 Appendix 1. Canadian Classification of Health Intervention Codes Used to Identify any Vaginal Mesh (Synthetic) Implantation Procedure(s) for Pelvic Organ Prolapse 4 Canadian Classification of health
1 2 3 Appendix 1. Canadian Classification of Health Intervention Codes Used to Identify any Vaginal Mesh (Synthetic) Implantation Procedure(s) for Pelvic Organ Prolapse 4 Canadian Classification of health
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum
 LUTS (2013) 5, 154 158 ORIGINAL ARTICLE Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum JaeHeonKIM, 1 Kwang Woo
LUTS (2013) 5, 154 158 ORIGINAL ARTICLE Risk Factors for De Novo Mixed Urinary Incontinence and Stress Urinary Incontinence Following Surgical Removal of a Urethral Diverticulum JaeHeonKIM, 1 Kwang Woo
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Reconstructive Surgery
 Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Laparoscopic Diverticulocystoplasty for Low Compliance Bladder in a Child
 CASE REPORT Laparoscopic Diverticulocystoplasty for Low Compliance Bladder in a Child Manickam Ramalingam, MCh, Kallappan Senthil, MCh, Anandan Murugesan, MCh, Mizar Ganapathy Pai, MCh ABSTRACT Low compliance
CASE REPORT Laparoscopic Diverticulocystoplasty for Low Compliance Bladder in a Child Manickam Ramalingam, MCh, Kallappan Senthil, MCh, Anandan Murugesan, MCh, Mizar Ganapathy Pai, MCh ABSTRACT Low compliance
Case: Spontaneous bladder rupture presenting as sudden-onset abdominal pain in a child after many years in remission from bladder rhabdomyosarcoma
 Case: Spontaneous bladder rupture presenting as sudden-onset abdominal pain in a child after many years in remission from bladder rhabdomyosarcoma Cyrus Chehroudi; Kourosh Afshar, MD University of British
Case: Spontaneous bladder rupture presenting as sudden-onset abdominal pain in a child after many years in remission from bladder rhabdomyosarcoma Cyrus Chehroudi; Kourosh Afshar, MD University of British
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY RETENTION WITH A PUBOVAGINAL SLING
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
PERINEAL PROSTATECTOMY
 Abstract PERINEAL PROSTATECTOMY Pages with reference to book, From 204 To 206 Altaf Hussain Rathore ( Dept. of Surgery, Punjab Medical College, Faisalabad. ) A series of twenty-five medically high risk
Abstract PERINEAL PROSTATECTOMY Pages with reference to book, From 204 To 206 Altaf Hussain Rathore ( Dept. of Surgery, Punjab Medical College, Faisalabad. ) A series of twenty-five medically high risk
Female Epispadias Repair
 hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
hoofdstuk 07 08-03-2001 15:25 Pagina 89 Female Epispadias Repair Female epispadias repair: a new 1-stage technique CHAPTER 7 Tom P.V.M de Jong, Pieter Dik and Aart J. Klijn Journal of Urology 2000, 164,
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Renal Trauma: Management Options
 Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Cleveland Clinic Quarterly
 Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Cleveland Clinic Quarterly Volume 31 JULY 1964 No. 3 A MEDICAL SILASTIC PROSTHESIS FOR THE CONTROL OF URINARY INCONTINENCE IN THE MALE A Preliminary Report J A M E S K. W A T K I N S, M. D., * R A L P
Colposuspension operation
 Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Daniel K Roberts MD, PhD 2014 Annual Clinical Update
 Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Complication of long indwelling urinary catheter and stent COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT
 151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
Posterior Deep Endometriosis. What is the best approach? Dept Gyn Obst CHU Clermont Ferrand France
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix - Rectum - Vagina Should we
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix - Rectum - Vagina Should we
Alimited degree of vaginal discharge is expected
 ADULT UROLOGY POSTHYSTERECTOMY VAGINAL CUFF FISTULA: DIAGNOSIS AND MANAGEMENT OF AN UNUSUAL CAUSE OF INCONTINENCE DAVID A. GINSBERG, ERIC S. ROVNER, AND SHLOMO RAZ ABSTRACT Objectives. Connection between
ADULT UROLOGY POSTHYSTERECTOMY VAGINAL CUFF FISTULA: DIAGNOSIS AND MANAGEMENT OF AN UNUSUAL CAUSE OF INCONTINENCE DAVID A. GINSBERG, ERIC S. ROVNER, AND SHLOMO RAZ ABSTRACT Objectives. Connection between
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Outcomes of Surgery of Female Urethral Diverticula Classified Using Magnetic Resonance Imaging
 european urology 51 (2007) 1664 1670 available at www.sciencedirect.com journal homepage: www.europeanurology.com Female Urology Incontinence Outcomes of Surgery of Female Urethral Diverticula Classified
european urology 51 (2007) 1664 1670 available at www.sciencedirect.com journal homepage: www.europeanurology.com Female Urology Incontinence Outcomes of Surgery of Female Urethral Diverticula Classified
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
Urethral catheter removal 3 days after radical retropubic prostatectomy is feasible and desirable
 Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
University of Alberta Reconstructive Urology Fellowship
 University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
University of Alberta Reconstructive Urology Fellowship 1. Overview 2. Eligibility Requirements 3. Funding 4. Clinical Expectations 5. Academic Expectations 6. Objectives of Training 7. Teaching Methods
Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy
 BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy John M. Fitzpatrick Mater Misericordiae University Hospital Dublin & University College Dublin, Ireland Accepted
BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Millin Retropubic Prostatectomy John M. Fitzpatrick Mater Misericordiae University Hospital Dublin & University College Dublin, Ireland Accepted
AUGS Global Health SIG: Evaluation and treatment of vesicovaginal and rectovaginal fistulas in lower resource settings
 AUGS Global Health SIG: Evaluation and treatment of vesicovaginal and rectovaginal fistulas in lower resource settings Learning Objectives Identify how to diagnosis and evaluate VVF and RVF in lower resource
AUGS Global Health SIG: Evaluation and treatment of vesicovaginal and rectovaginal fistulas in lower resource settings Learning Objectives Identify how to diagnosis and evaluate VVF and RVF in lower resource
Introduction/Learning Objectives. Incontinence: Natural History. Course Outline 10/14/2016. Urinary Incontinence: Conservative Measures
 Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma. Last reviewed June 2014
 Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Case Report Management of Recurrent Rectourethral Fistula by York Mason Posterior Transrectal Transsphincteric Approach
 Case Reports in Urology Volume 2015, Article ID 854365, 6 pages http://dx.doi.org/10.1155/2015/854365 Case Report Management of Recurrent Rectourethral Fistula by York Mason Posterior Transrectal Transsphincteric
Case Reports in Urology Volume 2015, Article ID 854365, 6 pages http://dx.doi.org/10.1155/2015/854365 Case Report Management of Recurrent Rectourethral Fistula by York Mason Posterior Transrectal Transsphincteric
TRANSURETHRAL RESECTION
 TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
TRANSURETHRAL RESECTION OF THE PROSTATE GLAND 21 Prostatic sonographic studies of patients who have undergone a transurethral resection of the prostate gland reveal large volumes of residual prostate tissue
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
