The proximal colonic motor response to rectal mechanical and chemical stimulation
|
|
|
- Osborn Pierce
- 5 years ago
- Views:
Transcription
1 Am J Physiol Gastrointest Liver Physiol 282: G443 G449, First published October 24, 2001; /ajpgi The proximal colonic motor response to rectal mechanical and chemical stimulation P. A. BAMPTON, 1 P. G. DINNING, 1 M. L. KENNEDY, 2 D. Z. LUBOWSKI, 2 AND I. J. COOK 1 Departments of 1 Gastroenterology and 2 Colorectal Surgery, The St. George Hospital, University of New South Wales, Sydney, Australia 2217 Received 7 July 2001; accepted in final form 5 November 2001 Bampton, P. A., P. G. Dinning, M. L. Kennedy, D. Z. Lubowski, and I. J. Cook. The proximal colonic motor response to rectal mechanical and chemical stimulation. Am J Physiol Gastrointest Liver Physiol 282: G443 G449, First published October 24, 2001; /ajpgi We aimed to determine whether rectal distension and/or infusion of bile acids stimulates propagating or nonpropagating activity in the unprepared proximal colon in 10 healthy volunteers using a nasocolonic manometric catheter (16 recording sites at 7.5-cm spacing). Sensory thresholds and proximal colonic motor responses were assessed following rectal distension by balloon inflation and rectal instillation of chenodeoxycholic acid. Maximum tolerated balloon volume and the volume that stimulated a desire to defecate were both significantly (P 0.01) reduced after rectal chenodeoxycholic acid. The frequency of colonic propagating pressure wave sequences decreased significantly in response to initial balloon inflations (P 0.05), but the frequency doubled after subsequent chenodeoxycholic acid infusion (P 0.002). Nonpropagating activity decreased after balloon inflation, was not influenced by acid infusion, and demonstrated a further decrease in response to repeat balloon inflation. We concluded that rectal chenodeoxycholic acid in physiological concentrations is a potent stimulus for propagating pressure waves arising in the proximal colon and reduces rectal sensory thresholds. Rectal distension inhibits all colonic motor activity. chenodeoxycholic acid; colon; manometry; peristalsis; afferent PROPAGATING PRESSURE WAVES contribute to the episodic flow of colonic content and to defecation (2, 9, 17, 24, 26). The factors that initiate and modulate these propagating sequences (PSs) are partially understood. Extrinsic neural pathways probably exert a modulatory effect and may be capable of activating these pressure wave patterns, because propagating sequences virtually disappear during stable sleep, whereas arousal from sleep is a potent and immediate stimulus of PSs (14, 22, 26, 31). Local colocolonic reflex pathways exist within the colon that are likely to be involved in the modulation of propagating activity, because chemical and physical stimuli may stimulate colonic propagating motor patterns and defecation (7, 20). For example, rectal glycerol stimulates myoelectrical activity in the Address for reprint requests and other correspondence: I. J. Cook, Director of Gastroenterology, The St. George Hospital, Kogarah 2217, New South Wales, Australia ( I.cook@unsw.edu.au). left colon (10), and rectal bisacodyl initiates propagating pressure waves in the proximal colon that culminate in defecation (20). Rectal distension delays colonic transit time in the pig, suggesting that mechanical and chemical stimuli may have opposing effects (25). Mechanical distension and chemoreceptor activation, perhaps acting synergistically, are two candidate mechanisms whereby colonic motor patterns might be stimulated. Intraluminal distension elicits peristaltic contractions in the esophagus and small bowel. However, a similar response to colonic distension has not been consistently demonstrated (4, 16, 25). Rectal and ascending colon distension with 500 and 750 ml of isotonic saline, respectively, have not been demonstrated to provoke a motor response (12, 30). Chenodeoxycholic acid, when administered in supraphysiological concentrations, is a recognized stimulus of colonic propagating activity (33). However, chenodeoxycholic acid infused rectally in physiological concentrations ( mm) (5) does not influence rectal motor activity despite the observation that these subjects reported a strong defecation urge (5, 12). The presence of this defecatory urge and subsequent defecation in a number of subjects suggested to us that chenodeoxycholic acid might be an important chemical stimulant of colonic motility. It appears that physiological concentrations of bile acids are sufficient to stimulate rectal afferents and the defecation urge, but supraphysiological concentrations might be necessary to stimulate the accompanying defecatory motor responses. Unfortunately that study did not measure motility proximal to the rectum. Hence, it remains unknown whether physiological concentrations of rectal bile acids might stimulate proximal colonic motor patterns that might facilitate defecation. A dissociation between sensory perception of defecation urge and the usual accompanying colonic motor patterns is also a possible explanation. This concept has important clinical implications. Heightened rectal sensitivity with diminished colonic contractile activity might be relevant to the pathophysiology of the syndrome of constipation with outlet delay or obstructed defecation. For example, these patients have a frequent The costs of publication of this article were defrayed in part by the payment of page charges. The article must therefore be hereby marked advertisement in accordance with 18 U.S.C. Section 1734 solely to indicate this fact /02 $5.00 Copyright 2002 the American Physiological Society G443
2 G444 defecation urge, frequent ineffective attempts at defecation, and may have normal or diminished colonic transit and colonic propagating sequences (8, 11, 23). We hypothesized that chemical and mechanical stimulation of the rectum interact to enhance proximal colonic propagating pressure waves and to retard nonpropagating colonic activity. These responses would be predicted to enhance the transport of luminal content distally and might culminate in defecation. Our aim, therefore, was to determine the effects of rectal infusion of physiological doses of chenodeoxycholic acid and rectal distension on proximal colonic propagating activity and whether the two stimuli act synergistically. METHODS Subjects Ten consecutive healthy volunteers (9 males, 1 female; mean age yr, range 23 52) with no history of gastrointestinal complaints and who reported between two bowel movements per day and one bowel movement every 2 days, were recruited by advertisement. None had taken laxatives or other medications. None had had previous abdominal surgery other than appendicectomy. Written informed consent was obtained from the participants, and the study was approved by the Human Ethics Committees of the South Eastern Area Health Service, Sydney, and the University of New South Wales. Manometric Technique The technique of pancolonic manometry has been described in detail previously (2). Briefly, we used a 17-channel (16 recording sideholes), 4.5-m-long extruded Silastic perfused manometric assembly (Dentsleeve, Wayville, South Australia) with an overall diameter of 3.5 mm. Each recording lumina had an internal diameter of 0.5 mm with an intersidehole distance of 7.5 cm. A latex balloon at the tip of the catheter could be inflated and deflated with air through the core channel (internal diameter 0.8 mm). The catheter was rendered radiopaque by curing strips of barium pasted to its exterior. The recording lumina were perfused with degassed, distilled water preceded by a CO 2 flush to ensure removal of all air bubbles from the catheter, thus minimizing compliance (27). A low-compliance pneumohydraulic perfusion pump drove the perfusate at 0.15 ml/min (Dentsleeve, Wayville, South Australia). Pressures were measured from each sidehole with 16 external pressure transducers (Abbott Critical Care Systems, North Chicago, IL). Signals were amplified and digitized at 10 Hz by preamplifiers (AqcKnowledge III Software, BIOPAC Systems, Santa Barbara, CA). We have previously demonstrated that the rise rate characteristics afforded by a catheter of this nature are adequate for recording colonic pressure waves (2). Experimental Protocol Catheter placement. After an overnight fast, catheter placement commenced at The catheter tip was passed via the nose and through the pylorus under fluoroscopic control. The balloon was then inflated to a diameter of 2 cm with a volume of air according to a previously determined volume-diameter calibration curve. The catheter was manually fed through the nose in increments of 40 cm each hour or as needed. To prevent the catheter from looping in the stomach, the position and conformation of the catheter were checked fluoroscopically every 2 h. As the tip of the catheter approached the ileocolonic junction, the balloon was progressively deflated to a diameter of 0.5 cm to avoid impaction in the distal ileum. When the catheter tip had passed through the ileocolonic junction, the balloon was reinflated to a diameter of 2 cm. Total fluoroscopy time was s, and the maximum whole body effective radiation dose equivalent was msv. At 1400 on the third day of the study, subjects were placed in the left lateral position, a polyvinylchloride rectal catheter was inserted, which incorporated two perfused recording channels 3 and 4 cm from the tip and a central core for balloon inflation. The catheter was positioned 4 cm from the internal anal verge, with the distal recording sidehole within the anal sphincter and the proximal sidehole in the rectum. A latex balloon at the tip of the catheter could be manually inflated with air. After the rectal catheter was placed, baseline manometric recordings were made for 20 min from the pernasally placed and rectal catheters, with the subject lying in the left lateral position. Rectal distension sensory threshold testing. The rectal balloon was then inflated with air by a hand-held syringe in a slow ramp fashion at a rate of 50 ml/min (32) on three occasions with a 5-min interval between inflations. Subjects reported 1) rectal sensory volume, defined as the volume corresponding to the onset of perception of the balloon; 2) defecation urge, defined as the onset of the desire to defecate; and 3) maximum tolerated volume, defined as the volume at which they noted the onset of discomfort. Chenodeoxycholic acid infusion. A second single lumen polyvinylchloride rectal catheter was then inserted, and 150 ml of 1 mmol chenodeoxycholic acid (Sigma, St Louis, MO) were infused over 3 min and manometric recording continued for a further 20 min. This dose of bile acid was chosen because it approximates the measured concentration of unbound bile acid in stool water of normal subjects ( mm) (5). The slow ramp balloon inflations were then repeated again three times with a 5-min interval between inflations, after which recording was continued for 20 min. Manometric Definitions We used the same method of analysis of the manometric trace as described in our previous papers (2). To recap briefly, once pressure waves had been identified, a propagating sequence was defined as an array of three or more pressure waves recorded from adjacent recording sites in which the conduction velocity between wave onset within that sequence lay between 0.2 and 12 cm/s. Propagating sequences were further qualified by the terms antegrade or retrograde, depending on the direction of propagation Propagating sequences were subclassified as high-amplitude propagating sequences if the amplitude of at least one component propagating pressure waves was 116 mmhg (representing the mean amplitude plus 2 standard deviations of colonic propagating sequences). The area under the pressure curve (AUC) was used as an overall measure of colonic motor activity and as an appropriate index of nonpropagating activity, because this was by far the most prevalent pressure pattern seen. Cough- or straininduced artefacts occurring during an epoch in which the AUC was to be calculated were removed from the trace. A value equivalent to the average for the remainder of the epoch was then assigned to the removed segment.
3 G445 Data Analysis The colon, for the purposes of analysis, was divided into 16 regions, with region 1 being the cecum, region 4 the hepatic flexure, region 8 the splenic flexure, and region 16 the rectum. Propagating sequence site of origin and extent of propagation was referenced to these regions. The colon was divided into three segments for the purpose of analysis of regional responses in nonpropagating activity: segment cecoascending colon (regions 1 4), transverse colon (regions 5 8), and descending colon (regions 9 12). The manometric trace was examined for propagating sequences in 4 15-min epochs. These epochs were the 15 min before the first set of balloon inflations, the 15 min during and immediately following the first set of inflations, the 15 min after the chenodeoxycholic acid infusion, and the 15 min during the final set of balloon inflations. The AUC was measured in 5-min epochs during these times. Volume within the rectal balloon corresponding to each of the three rectal sensory thresholds was compared before and after chenodeoxycholic acid infusion using a paired t-test. Inferences among propagating sequence frequency, amplitude, and velocity at baseline, after balloon inflation, and after chenodeoxycholic acid infusion were made again based on a paired t-test with Bonferroni correction factor for repeated measures. Inferences regarding regional variability of motor activity were made using a repeated-measures ANOVA. All data are expressed as means SE unless stated otherwise. RESULTS Catheter Placement In all 10 subjects, the tip of the catheter lay distal to the splenic flexure at the time of stimulation studies. It was located at the distal descending colon in five, proximal sigmoid colon in two, and distal sigmoid colon in three. We did not analyze data from the sigmoid colon, because the number of sideholes in the sigmoid colon was too small to give meaningful results. Rectal Sensory Thresholds No time-dependent effect of distension volume was noted. Hence data for the three inflations were averaged. Chenodeoxycholic acid did not significantly influence the rectal sensory threshold, but it did reduce significantly the defecatory urge threshold from 81 9 to 56 7 mls (P 0.01) and the maximum tolerated rectal volume from to ml (P 0.01; Fig. 1). Fig. 1. Effect of chenodeoxycholic acid on rectal sensory thresholds to balloon inflation. Rectal infusion of chenodeoxycholic acid significantly reduced the threshold for defecatory urge and the maximum tolerated volume (P 0.01) but did not influence the first perception of distension. Colonic Motor Responses Propagating pressure wave sequences. When compared with the baseline frequency of propagating sequences in all regions of the proximal colon ( /15 min), PS frequency was significantly reduced to during the initial set of balloon inflations (P 0.045). In response to the second set of balloon inflations, PS frequency was reduced to per 15 mins, which was also significantly lower than baseline frequency (P 0.05; Fig. 2). Indeed, repeat balloon stimulation following chenodeoxycholic acid instillation appeared to switch off the increased propagating activity stimulated by the chenodeoxycholic acid. Chenodeoxycholic acid had a relatively prompt stimulatory effect on proximal colonic propagating pressure waves (Fig. 3). When compared with baseline, propagating sequence frequency more than doubled to per 15 min after chenodeoxycholic acid infusion (P 0.002; Fig. 2). The preferential site of origin of PSs changed in response to chemical rectal stimulation. During the baseline period, 67% of PSs originated in the cecoascending colon. This proportion increased to 72% following chenodeoxycholic acid infusion. Only 50% of the few propagating sequences occurring after balloon inflation arose from the cecoascending colon, suggesting that propagating sequences arising from this site may have been inhibited by rectal distension. There were no significant differences in the extent of propagation by the propagating sequences among the experimental conditions. The mean amplitude of propagating pressure waves was lower in propagating sequences that occurred following chenodeoxycholic acid infusion (34 5 mmhg) than in those during baseline recording (55 8 mmhg, P 0.03). The propagating sequences occurring after balloon inflation were of a similar amplitude (36 6 mmhg) to those occurring after chenodeoxycholic acid infusion. Responses to either stimulus were not immediate. Propagating sequences occurred a mean of min (range 1 14 min) after commencement of chenodeoxycholic acid infusion, compared with min after commencement of balloon inflation (not significant). AUC When compared with a baseline value of 2, mmhg/s, the AUC in the cecoascending colon de-
4 G446 and this urge was associated with a proximal colonic propagating sequence in three subjects. One subject experienced successive urges associated with propagating sequences and defecated 8 min after infusion. A further four patients defecated within the hour after the completion of the study. Hence, in all, five patients defecated 8 60 min after the rectal chenodeoxycholic acid infusion. DISCUSSION Fig. 2. Effect of rectal balloon inflation and chenodeoxycholic acid on the frequency of colonic propagating sequences. Initial (P 0.05) and subsequent (P 0.02) rectal balloon inflations significantly inhibited the frequency of propagating sequences in the proximal colon. Chenodeoxycholic acid significantly augmented propagating sequence frequency (P 0.002). creased significantly in response to rectal balloon inflation to 2, mmhg/s (P 0.001). No significant alterations in AUC were observed in the transverse or descending colon after the first set of inflations; however, in response to the second set of inflations, the AUC in the cecoascending colon decreased further to 1, mmhg/s (P ), and on this occasion, there was a significant decrease in the transverse colon compared with the baseline 1, (P 0.002). In contrast, there were no statistically significant alterations in the AUC in response to balloon inflations in the descending colon, and the infusion of chenodeoxycholic acid appeared to have no effect on the AUC in any part of the colon. (Fig. 4). Symptoms No patients experienced an urge to defecate after the initial set of balloon inflations. Five of the ten subjects experienced an urge to defecate within 10 min of commencement of the chenodeoxycholic acid instillation, We have demonstrated that chenodeoxycholic acid in physiological concentrations reduces sensory thresholds to rectal balloon distension. This study demonstrates that the stimulation of rectal afferents can elicit both inhibitory and excitatory responses from the unprepared proximal human colon. In contrast to this synergism in effects on rectal sensation between chemical and mechanical stimuli, these stimuli had opposing effects in terms of colonic motor responses. Rectal instillation of a physiological concentration of chenodeoxycholic acid initiates propagating sequences in the proximal unprepared colon. Balloon distension of the rectum inhibits all types of proximal colonic activity. These responses are presumed to be mediated by long colocolonic pathways. These observations are consistent with the hypothesis that a combination of chemical and mechanical rectal stimulation enhances proximal colonic propagating activity while retarding nonpropagating activity and that such a combination of responses is likely to facilitate colonic transit and defecation. The colon is responsive to stretch in vivo and in vitro (4, 28). We found that rectal balloon distension suppressed both propagating and nonpropagating activity and that this response was most pronounced in the cecoascending colon. The reported observations to date are conflicting with some (16) showing colonic distension to have little or no effect on the elicitation of colonic propagating events in the human colon, whereas others (4) found balloon distension to elicit Fig. 3. Propagating sequence initiated by rectal infusion of chenodeoxycholic acid. In this example, sideholes extend from the terminal ileum through to the sigmoid colon. A propagating sequence is seen to originate in the cecum and propagates to the descending colon following the infusion of chenodeoxycholic acid into the rectum.
5 G447 Fig. 4. Effect of balloon inflation and chenodeoxycholic acid on the area under the pressure curve (AUC). The 3 graphs represent averaged data from all regions within cecoascending (A), transverse (B), and descending colon (C). All effects were more pronounced in the proximal colonic regions than they were in the distal colon. Initial balloon inflation of the rectum induced a significant reduction in AUC that was confined to the cecoascending colon (P 0.001), whereas subsequent inflation induced further significant reductions in cecoascending (P ) and transverse colon (P 0.002). Infusion of chenodeoxycholic acid did not affect the AUC. propulsive activity in 53% of subjects. Rectal balloon distension in the dog does not elicit giant migrating contractions that are the manometric correlate of defecation (21). On the other hand, rectal distension in pigs prolongs colonic transit time (25) and decreases colonic myoelectrical activity in humans (13). Our findings, in the context of these previous studies, suggest that rectal distension activates inhibitory pathways, thereby reducing proximal colonic motor activity, with the net effect of delaying colonic transit. It is likely that such a response to rectal distension prevents further passage of stool to a loaded rectum, which might further challenge continence mechanisms. This hypothetical extrinsic pathway is supported by studies on isolated canine colonic loops in which extrinsic adrenergic neural pathways appear to mediate the colocolonic inhibitory reflex (18) Bile acids are well known to cause diarrhea by stimulating motility and, at higher doses, by promoting secretion (6, 12, 15, 29, 33). The rectal infusion of chenodeoxycholic acid, both in supraphysiological and physiological concentrations, decreases rectal sensory thresholds to balloon inflation (12, 19, 30). In supraphysiological but not physiological concentrations, rectal chenodeoxycholic acid has been associated with initiation of a colonic motor response despite the observation that physiological concentrations did induce a defecatory urge in the majority (6, 12, 15, 19, 22, 29, 30, 33). However, those studies may have overlooked proximal colonic motor responses to lower doses of chenodeoxycholic acid, because only distal colonic activity was measured. Indeed many of the propagating motor patterns that culminate in a defecatory urge originate in the proximal colon (2). From our data, it is not possible to determine whether the affects on rectal afferents are direct, via chemoreceptor activation, or indirect, via chemical-induced alterations in colonic wall tone or compliance. In the present study, we demonstrate a twofold increase in proximal colonic propagating sequence frequency after rectal instillation of 1 mmol chenodeoxycholic acid. The propagating sequences initiated by chenodeoxycholic acid in our study travelled a relatively short distance ( 18% of the length of the colon) and were of a relatively low amplitude. These motor patterns do not fit within the definition of high amplitude propagating contractions, previously described as occurring before spontaneous defecation and defecation stimulated by bisacodyl (2, 17, 20). Nevertheless, we and others (17) have shown some propagating sequences that do not extend all the way to the rectum do occur before spontaneous defecation. Furthermore, propagating pressure waves of comparable amplitude to those induced in response to chenodeoxycholic acid in the present study have been shown previously to have the capacity to move colonic content (9, 24) and do occur with increasing frequency in the hour before defecation (2). Randomization of the stimuli administration would have been desirable. However, due to the persistence of the bile acid within the rectum after infusion and the indeterminate nature of the duration of its effect, it was not possible to randomize the stimuli as well as examine the hypothesis that bile acids sensitize the rectum to subsequent distension. However, it is unlikely that the lack of such randomization biased the results. Existing colonic motility studies have not observed a sudden fall followed abruptly by a fourfold increase in propagated sequence frequency (1, 3, 14, 22, 26). Furthermore, is difficult to comprehend poten-
6 G448 tial bias, which might account for both a decrease then an increase in propagating activity as seen in the present study. Alternatively, the effect attributed to chenodeoxycholic acid infusion in the present study could represent a late response to the balloon inflation rather than a response to the chenodeoxycholic acid infusion per se. However, the response to distension is unlikely to account for the massive stimulatory effect of chenodeoxycholic acid, because the response to distension has been shown, convincingly, to be inhibitory in nature. Any effect of the distension would have served only to attenuate the response to chenodeoxycholic acid. Although measurement of colonic tone was beyond the scope of this study, one might speculate that increased colonic tone following chenodeoxycholic acid infusion or decreased tone in response to rectal distension might enhance and attenuate, respectively, the ability of the catheters to detect phasic colonic wall motion and thereby account, in part, for our observations. On the basis of an earlier study by Von der Ohe et al. (34), we think this is unlikely. In that study, they compared the detection of phasic events by a colonic barostat with perfusion manometry and found that phasic events were recorded with similar fidelity, although once the colonic barostat balloon was inflated beyond 5.6 cm in that study, the frequency of phasic events detected by perfusion manometry was less than that detected by the barostat. However, a colonic diameter as great as 5.6 cm is quite nonphysiological and would not be expected in normal volunteers. Furthermore, if changes in tone alone were responsible for our observation, then we would expect the detection of both propagating and nonpropagating waves to be increased after chenodeoxycholic acid infusion. In contrast, we observed only an increase in propagating pressure waves after this stimulus. Hence, we feel that the regional activation and the actual frequency of phasic events, and certainly the prevalence of propagating sequences, were unlikely to have been affected substantially by any changes in wall tone. The possibility remains, however, that the actual amplitude of phasic pressure waves and AUC may have been influenced by changes in tone. We conclude that rectal chemoreceptor stimulation may play an important physiological role in the initiation of proximal colonic propagating sequences. Rectal mechanoreceptor stimulation is inhibitory to the unprepared proximal human colon. These findings support the hypothesis that long colocolonic reflexes exist and may well be important in modulating colonic flow and defecation. This work was supported by a National Health and Medical Research (Australia) project grant. Dr. P. Bampton is a recipient of a National Health and Medical Research Council (Australia) Medical Postgraduate Research Scholarship. REFERENCES 1. Bampton PA, Dinning PG, Kennedy ML, Lubowski DZ, and Cook IJ. Prolonged multipoint recording of colonic manometry in the unprepared human colon providing insight into potentially relevant pressure wave parameters. Am J Gastroenterol 96: , Bampton PA, Dinning PG, Kennedy ML, Lubowski DZ, decarle DJ, and Cook IJ. Spatial and temporal organization of pressure patterns throughout the unprepared colon during spontaneous defecation. Am J Gastroenterol 95: , Bassotti G and Gaburri M. Manometric investigation of highamplitude propagated contractile activity of the human colon. Am J Physiol Gastrointest Liver Physiol 255: G660 G664, Bassotti G, Gaburri M, Imbimbo BP, Morelli A, and Whitehead WE. Distension-stimulated propagated contractions in human colon. Dig Dis Sci 39: , Bjork J, Soergel K, and Wood C. The composition of free stool water. Gastroenterology 70: A-6/864, Chadwick V, Gaginella T, Carlson G, Debongnie J, Phillips S, and Hoffman A. Effect of molecular structure on bileacid induced alterations in absorptive function, permeability, and morphology in the perfused rabbit colon. J Lab Clin Med 94: , Christensen J. The motility of the colon. In: Physiology of the Gastrointestinal Tract (3rd ed.), edited by Johnson L. New York: Raven, 1994, p Cook IJ. Colon and anorectum: constipation, urgency, pain syndromes. Clinical physiology. In: Functional disorders of the gut, edited by Phillips SF and Wingate DL. London: Saunders, 1998, p Cook IJ, Furukawa Y, Panagopoulos V, Collins PJ, and Dent J. Relationships between spatial patterns of colonic pressure and individual movements of content. Am J Physiol Gastrointest Liver Physiol 278: G329 G341, Delvaux M, Camman F, Staumont G, Fioramonti J, Beuno J, and Fexinos J. Glycerol induces a recto-colonic reflex associating a stimulation of colonic myoelectrical activity and a decrease in colonic tone in man. Gastrointestinal Motility 5: 186, Dinning PG, Bampton PA, Andre J, Kennedy ML, Lubowski DZ, and Cook IJ. Constipation due to obstructed defecation is likely to be a colonic, rather than an ano-rectal disorder (Abstract). Gastroenterology 120: A751, Edwards CA, Brown S, Baxter AJ, Bannister JJ, and Read NW. Effects of bile acid on anorectal function in man. Gut 30: , Empinet O, Bommelaer G, and Dapoigny M. Does rectal distension effect colonic response to the meal in patients with anorectal dysfunction? Neurogastroenterol Motil 5: 189, Furukawa Y, Cook IJ, Panagopoulos V, McEvoy RD, Sharp DJ, and Simula M. Relationship between sleep patterns and human colonic motor patterns. Gastroenterology 107: , Gordon S, Kinsey M, Magen J, Joseph R, and Kowlessar O. Structure of bile acids associated with secretion in the rat caecum. Gastroenterology 77: 38 44, Hardcastle JD and Mann CV. Physical factors in the stimulation of colonic peristalsis. Gut 11: 41 46, Herbst F, Kamm MA, Morris GP, Britton K, Woloszko J, and Nicholls RJ. Gastrointestinal transit and prolonged ambulatory motility in health and fecal incontinence. Gut 41: , Hughes SF, Scott SM, Pilot MA, and Williams NS. Adrenoceptors and colocolonic inhibitory reflex. Dig Dis Sci 44: , Kamath PS, Hoepfner MT, and Phillips SF. Short-chain fatty acids stimulate motility of the canine ileum. Am J Physiol Gastrointest Liver Physiol 253: G423 G427, Kamm MA, van der Sup JR, and Lennard-Jones JE. Colorectal and anal motility during defecation. Lancet 339: 820, Karaus M and Sarna SK. Giant migrating contractions during defecation in the dog colon. Gastroenterology 92: , Lemann M, Flourie B, Picon L, Coffin B, Jian R, and Rambaud JC. Motor activity recorded in the unprepared colon of healthy humans. Gut 37: , 1995.
7 G Mertz H, Naliboff B, and Mayer E. Physiology of refractory chronic constipation. Am J Gastroenterol 94: , Moreno-Osset E, Bazzocchi G, Lo S, Trombley E, Ristow E, Reddy SN, Villanueva-Meyer J, Fain J, Jing J, Mena I, and Snape WJ. Association between postprandial changes in colonic intraluminal pressure and transit. Gastroenterology 96: , Musial F, Crowell MD, French AW, and Guiv N. Effect of prolonged, continuous rectal distension on mouth-to-cecum and colonic transit time in pigs. Physiol Behav 52: , Narducci F, Bassotti G, Gaburri M, and Morelli A. Twenty four hour manometric recording of colonic motor activity in healthy man. Gut 28: 17 25, Omari T, Bakewell M, Fraser R, Davidson G, and Dent J. Intraluminal micromanometry: an evaluation of the dynamic performance of micro-extrusions and sleeve sensors. Neurogastroenterol Motil 8: , Schang JC and Devroede G. Fasting and postprandial myoelectrical spiking activity in the human sigmoid colon. Gastroenterology 85: , Snape WJ, Sullivan MA, and Cohen S. Abnormal gastro-colic response in patients with intestinal pseudo-obstruction. Arch Intern Med 140: , Spiller RC, Brown ML, and Phillips SF. Decreased fluid tolerance, accelerated transit, and abnormal motility of the human colon induced by oleic acid. Gastroenterology 91: , Sun EA, Snape WJ, Cohen S, and Renny A. The role of opiate receptors and cholinergic neurons in the gastrocolonic response. Gastroenterology 82: , Sun WM, Read NW, Prior A, Daly J, Cheah SK, and Grundy D. Sensory and motor responses to rectal distension vary according to rate and pattern of balloon inflation. Gastroenterology 99: , Taylor I, Basu P, Hammond P, and Flynn M. Effect of bile acid perfusion on colonic motor function in patients with the irritable colon syndrome. Gut 21: , Von der Ohe MR, Hanson RB, and Camilleri M. Comparison of simultaneous recordings of human colonic contractions by manometry and a barostat. Neurogastroenterol Motil 6: , 1994.
Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D.
 Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D. OBJECTIVES: 1. Contrast the types of motility in the small intestine. 2. Describe the neural circuits that mediate peristalsis.
Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D. OBJECTIVES: 1. Contrast the types of motility in the small intestine. 2. Describe the neural circuits that mediate peristalsis.
Small-Bowel and colon Transit. Mahsa Sh.Nezami October 2016
 Small-Bowel and colon Transit Mahsa Sh.Nezami October 2016 Dyspeptic symptoms related to dysmotility originating from the small bowel or colon usually include : Abdominal pain Diarrhea Constipation However,
Small-Bowel and colon Transit Mahsa Sh.Nezami October 2016 Dyspeptic symptoms related to dysmotility originating from the small bowel or colon usually include : Abdominal pain Diarrhea Constipation However,
... SELECTED ABSTRACTS...
 ... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
RECTO-COLONIC REFLEX IS IMPAIRED IN PATIENTS WITH IRRITABLE BOWEL SYNDROME
 5 RECTO-COLONIC REFLEX IS IMPAIRED IN PATIENTS WITH IRRITABLE BOWEL SYNDROME Patrick P.J. van der Veek, Marjan Steenvoorden, Jeroen Steens, Peter J. van der Schaar, Jessica Brussee, and Ad A. M. Masclee
5 RECTO-COLONIC REFLEX IS IMPAIRED IN PATIENTS WITH IRRITABLE BOWEL SYNDROME Patrick P.J. van der Veek, Marjan Steenvoorden, Jeroen Steens, Peter J. van der Schaar, Jessica Brussee, and Ad A. M. Masclee
Chapter 3 EFFECT OF ALOSETRON ON LEFT COLONIC MOTILITY IN NON-CONSTIPATED IBS PATIENTS AND HEALTHY VOLUNTEERS
 EFFECT OF ALOSETRON ON LEFT COLONIC MOTILITY IN NON-CONSTIPATED IBS PATIENTS AND HEALTHY VOLUNTEERS C.H.M. Clemens, M. Samsom, G.P van Berge Henegouwen, M. Fabri, A.J.P.M. Smout Aliment Pharmacol Ther
EFFECT OF ALOSETRON ON LEFT COLONIC MOTILITY IN NON-CONSTIPATED IBS PATIENTS AND HEALTHY VOLUNTEERS C.H.M. Clemens, M. Samsom, G.P van Berge Henegouwen, M. Fabri, A.J.P.M. Smout Aliment Pharmacol Ther
ELECTROSIGMOIDOGRAM, ELECTRORECTOGRAM AND THEIR RELATION
 [Frontiers in Bioscience 2, b12-16, September 15, 1997] ELECTROSIGMOIDOGRAM, ELECTRORECTOGRAM AND THEIR RELATION Ahmed Shafik, MD, PhD Professor and Chairman, Department of Surgery and Experimental Research,
[Frontiers in Bioscience 2, b12-16, September 15, 1997] ELECTROSIGMOIDOGRAM, ELECTRORECTOGRAM AND THEIR RELATION Ahmed Shafik, MD, PhD Professor and Chairman, Department of Surgery and Experimental Research,
Distension-Stimulated Propagated Contractions in Human Colon
 Digestive Diseases and Sciences, VoL 39, No. 9 (September 1994), pp. 1955-1960 Distension-Stimulated Propagated Contractions in Human Colon GABRIO BASSOTI'I, MD, PhD, MANUELA GABURRI, MD, BRUNO PIETRO
Digestive Diseases and Sciences, VoL 39, No. 9 (September 1994), pp. 1955-1960 Distension-Stimulated Propagated Contractions in Human Colon GABRIO BASSOTI'I, MD, PhD, MANUELA GABURRI, MD, BRUNO PIETRO
of healthy humans Motor activity recorded in the unprepared colon 15, 25, 35, 45, 50, 55, 60, 65, 70, and 75 cm
 Gut 1995; 37: 649-653 Motor activity recorded in the unprepared colon of healthy humans 649 Service de GastroentCrologie et Unite de Recherche sur les Fonctions Intestinales et la Nutrition, INSERM U290,
Gut 1995; 37: 649-653 Motor activity recorded in the unprepared colon of healthy humans 649 Service de GastroentCrologie et Unite de Recherche sur les Fonctions Intestinales et la Nutrition, INSERM U290,
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation. Introduction. Predisposing factor. Introduction.
 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P.
 UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
Measurement of colonic transit time with the Transit-Pellets TM method
 Measurement of colonic transit time with the Transit-Pellets TM method Measurement of colonic transit time is an important investigation in clinical gastroenterology. The measurement is indicated particularly
Measurement of colonic transit time with the Transit-Pellets TM method Measurement of colonic transit time is an important investigation in clinical gastroenterology. The measurement is indicated particularly
Langley Catheter Protocols
 Langley Catheter Protocols Stericom Ltd Units 1&2 Higham Mead Chesham HP5 2AH England Tel: +44 (0)1494 794315 Fax: +44 (0)1494 772759 info@stericom.com www.stericom.com Instructions for use The 2-balloon
Langley Catheter Protocols Stericom Ltd Units 1&2 Higham Mead Chesham HP5 2AH England Tel: +44 (0)1494 794315 Fax: +44 (0)1494 772759 info@stericom.com www.stericom.com Instructions for use The 2-balloon
Human Anatomy rectum
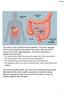 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Measurement of anal pressure and motility
 Measurement of anal pressure and motility B. D. HANCOCK' From the University Hospital of South Manchester Gut, 1976, 17, 645-651 SUMMARY A fine open perfused system and a closed balloon system for the
Measurement of anal pressure and motility B. D. HANCOCK' From the University Hospital of South Manchester Gut, 1976, 17, 645-651 SUMMARY A fine open perfused system and a closed balloon system for the
Evidence that nitric oxide mechanisms regulate small intestinal motility in humans
 72 Department of Medicine, Royal Adelaide Hospital, North Terrace, Adelaide, South Australia 5 A Russo R Fraser K Adachi M Horowitz G Boeckxstaens Correspondence to: Dr R Fraser. Accepted for publication
72 Department of Medicine, Royal Adelaide Hospital, North Terrace, Adelaide, South Australia 5 A Russo R Fraser K Adachi M Horowitz G Boeckxstaens Correspondence to: Dr R Fraser. Accepted for publication
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing
 Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Color Atlas of High Resolution Manometry
 Color Atlas of High Resolution Manometry Color Atlas of High Resolution Manometry Edited by Jeffrey Conklin, MD GI Motility Program Mark Pimentel, MD, FRCP(C) Cedars-Sinai Medical Center Edy Soffer, MD
Color Atlas of High Resolution Manometry Color Atlas of High Resolution Manometry Edited by Jeffrey Conklin, MD GI Motility Program Mark Pimentel, MD, FRCP(C) Cedars-Sinai Medical Center Edy Soffer, MD
Motility Disorders In Diverticular Disease. M. Kreis. Ludwig-Maximilians Universität München Klinikum Großhadern, Chirurgische Klinik
 Motility Disorders In Diverticular Disease. M. Kreis Ludwig-Maximilians Universität München Klinikum Großhadern, Chirurgische Klinik Pathophysiology Diet? Age? Diverticula Disposition? Constipation? Toxines?
Motility Disorders In Diverticular Disease. M. Kreis Ludwig-Maximilians Universität München Klinikum Großhadern, Chirurgische Klinik Pathophysiology Diet? Age? Diverticula Disposition? Constipation? Toxines?
INTRODUCTION TO GASTROINTESTINAL FUNCTIONS
 1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Chapter 5 TONE AND PHASIC MOTILITY OF THE LEFT COLON IN DIVERTICULAR DISEASE
 TONE AND PHASIC MOTILITY OF THE LEFT COLON IN DIVERTICULAR DISEASE C.H.M. Clemens, M. Samsom, J.M.M. Roelofs, G.P. van Berge Henegouwen, A.J.P.M. Smout. Submitted ABSTRACT Background & Aims: Asymptomatic
TONE AND PHASIC MOTILITY OF THE LEFT COLON IN DIVERTICULAR DISEASE C.H.M. Clemens, M. Samsom, J.M.M. Roelofs, G.P. van Berge Henegouwen, A.J.P.M. Smout. Submitted ABSTRACT Background & Aims: Asymptomatic
mcompass Interpretation Quick Reference Guide
 mcompass Interpretation Quick Reference Guide This document is designed to give you a starting point for reviewing of the mcompass anorectal manometry results. By no means are these the only questions
mcompass Interpretation Quick Reference Guide This document is designed to give you a starting point for reviewing of the mcompass anorectal manometry results. By no means are these the only questions
CHAPTER 3. J.M. Conchillo 1, N.Q. Nguyen 2, M. Samsom 1, R.H. Holloway 2, A.J.P.M. Smout 1
 CHAPTER 3 Multichannel ntraluminal impedance monitoring in the evaluation of patients with non-obstructive dysphagia J.M. Conchillo 1, N.Q. Nguyen 2, M. Samsom 1, R.H. Holloway 2, A.J.P.M. Smout 1 1 Department
CHAPTER 3 Multichannel ntraluminal impedance monitoring in the evaluation of patients with non-obstructive dysphagia J.M. Conchillo 1, N.Q. Nguyen 2, M. Samsom 1, R.H. Holloway 2, A.J.P.M. Smout 1 1 Department
Positive correlation between symptoms and circulating
 Gut, 1985, 26, 1059-1064 Positive correlation between symptoms and circulating motilin, pancreatic polypeptide and gastrin concentrations in functional bowel disorders D M PRESTON, T E ADRIAN, N D CHRISTOFIDES,
Gut, 1985, 26, 1059-1064 Positive correlation between symptoms and circulating motilin, pancreatic polypeptide and gastrin concentrations in functional bowel disorders D M PRESTON, T E ADRIAN, N D CHRISTOFIDES,
Gut-focused hypnotherapy normalizes disordered rectal sensitivity in patients with irritable bowel syndrome
 Aliment Pharmacol Ther 2003; 17: 635 642. doi: 10.1046/j.0269-2813.2003.01486.x Gut-focused hypnotherapy normalizes disordered rectal sensitivity in patients with irritable bowel syndrome R. LEA*, L. A.
Aliment Pharmacol Ther 2003; 17: 635 642. doi: 10.1046/j.0269-2813.2003.01486.x Gut-focused hypnotherapy normalizes disordered rectal sensitivity in patients with irritable bowel syndrome R. LEA*, L. A.
Introduction of Rapid barostat bag (RBB) protocol for the assessment of rectal function
 New technology for assessment and treatment of colorectal dysfunction Ascona 23rd of April 2015 Introduction of Rapid barostat bag (RBB) protocol for the assessment of rectal function Matthias Sauter Division
New technology for assessment and treatment of colorectal dysfunction Ascona 23rd of April 2015 Introduction of Rapid barostat bag (RBB) protocol for the assessment of rectal function Matthias Sauter Division
Metoclopramide in gastrooesophageal reflux
 Metoclopramide in gastrooesophageal reflux C. STANCIU AND JOHN R. BENNETT From the Gastrointestinal Unit, Hull Royal Infirmary Gut, 1973, 14, 275-279 SUMMARY In 3 patients with gastrooesophageal reflux,
Metoclopramide in gastrooesophageal reflux C. STANCIU AND JOHN R. BENNETT From the Gastrointestinal Unit, Hull Royal Infirmary Gut, 1973, 14, 275-279 SUMMARY In 3 patients with gastrooesophageal reflux,
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
UvA-DARE (Digital Academic Repository) Functional defecation disorders in children Kuizenga-Wessel, S. Link to publication
 UvA-DARE (Digital Academic Repository) Functional defecation disorders in children Kuizenga-Wessel, S. Link to publication Citation for published version (APA): Kuizenga-Wessel, S. (2017). Functional defecation
UvA-DARE (Digital Academic Repository) Functional defecation disorders in children Kuizenga-Wessel, S. Link to publication Citation for published version (APA): Kuizenga-Wessel, S. (2017). Functional defecation
Measurement of upper esophageal sphincter tone and relaxation during swallowing in premature infants
 Measurement of upper esophageal sphincter tone and relaxation during swallowing in premature infants T. OMARI, 1 A. SNEL, 2 C. BARNETT, 2 G. DAVIDSON, 1 R. HASLAM, 2 AND J. DENT 3 1 Gastroenterology Unit
Measurement of upper esophageal sphincter tone and relaxation during swallowing in premature infants T. OMARI, 1 A. SNEL, 2 C. BARNETT, 2 G. DAVIDSON, 1 R. HASLAM, 2 AND J. DENT 3 1 Gastroenterology Unit
doi: /nmo Please cite this article as:
 Archived at the Flinders Academic Commons: http://dspace.flinders.edu.au/dspace/ This is the accepted version of the following article: Arkwright, J. W., Dickson, A., Maunder, S. A., Blenman, N. G., Lim,
Archived at the Flinders Academic Commons: http://dspace.flinders.edu.au/dspace/ This is the accepted version of the following article: Arkwright, J. W., Dickson, A., Maunder, S. A., Blenman, N. G., Lim,
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 20 No. 1 January, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2014.20.1.74 Original Article Utilizing
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 20 No. 1 January, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2014.20.1.74 Original Article Utilizing
Nizatidine Enhances the Gastrocolonic Response and the Colonic Peristaltic Reflex in Humans
 0022-3565/01/2991-159 163$3.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 299, No. 1 Copyright 2001 by The American Society for Pharmacology and Experimental Therapeutics 3855/933929
0022-3565/01/2991-159 163$3.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 299, No. 1 Copyright 2001 by The American Society for Pharmacology and Experimental Therapeutics 3855/933929
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Patients with irritable bowel syndrome (IBS) frequently report
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:201 208 Lipid-Induced Colonic Hypersensitivity in the Irritable Bowel Syndrome: The Role of Bowel Habit, Sex, and Psychologic Factors MAGNUS SIMRÉN, HASSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:201 208 Lipid-Induced Colonic Hypersensitivity in the Irritable Bowel Syndrome: The Role of Bowel Habit, Sex, and Psychologic Factors MAGNUS SIMRÉN, HASSE
Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring
 14 Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring A.J. Bredenoord B.L.A.M. Weusten D. Sifrim R. Timmer A.J.P.M. Smout Dept. of Gastroenterology,
14 Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring A.J. Bredenoord B.L.A.M. Weusten D. Sifrim R. Timmer A.J.P.M. Smout Dept. of Gastroenterology,
Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease
 Brazilian Journal of Medical and Biological Research (6) 39: 27-31 ISSN -879X 27 Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease C.G. Aben-Athar and R.O.
Brazilian Journal of Medical and Biological Research (6) 39: 27-31 ISSN -879X 27 Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease C.G. Aben-Athar and R.O.
Preview from Notesale.co.uk Page 1 of 34
 Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
A Guide to Gastrointestinal Motility Disorders
 A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord André Smout Jan Tack A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord Gastroenterology and Hepatology Academic Medical
A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord André Smout Jan Tack A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord Gastroenterology and Hepatology Academic Medical
Irritable bowel syndrome (IBS) is a ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome
 ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
What part of the gastrointestinal (GI) tract is composed of striated muscle and smooth muscle?
 CASE 29 A 34-year-old man presents to his primary care physician with the complaint of increased difficulty swallowing both solid and liquid foods. He notices that he sometimes has more difficulty when
CASE 29 A 34-year-old man presents to his primary care physician with the complaint of increased difficulty swallowing both solid and liquid foods. He notices that he sometimes has more difficulty when
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 21 No. 1 January, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm14025 Original Article Comparison
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 21 No. 1 January, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm14025 Original Article Comparison
Function of the anal sphincters in patients with
 Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Rectosigmoid Motility and Myoelectric Activity in Progressive Systemic Sclerosis
 GASTROENTEROLOGY 1989;96:428-32 Rectosigmoid Motility and Myoelectric Activity in Progressive Systemic Sclerosis WILLIAM E. WHITEHEAD, GRETA TAITELBAUM, FREDERICK M. WIGLEY, and MARVIN M. SCHUSTER Departments
GASTROENTEROLOGY 1989;96:428-32 Rectosigmoid Motility and Myoelectric Activity in Progressive Systemic Sclerosis WILLIAM E. WHITEHEAD, GRETA TAITELBAUM, FREDERICK M. WIGLEY, and MARVIN M. SCHUSTER Departments
Colonic manometry in children with chronic intestinal pseudo-obstruction
 Gut 1993; 34:803-807 Colonic manometry in children with chronic intestinal pseudo-obstruction 803 Departments of Pediatrics and Medicine, Harbor-UCLA Medical Center, Martin Luther KingJr General Hospital,
Gut 1993; 34:803-807 Colonic manometry in children with chronic intestinal pseudo-obstruction 803 Departments of Pediatrics and Medicine, Harbor-UCLA Medical Center, Martin Luther KingJr General Hospital,
Minimum standards of anorectal manometry
 Neurogastroenterol. Mot. (22) 14, 553 559 Minimum standards of anorectal manometry S. S. C. RAO, F. AZPIROZ,* N. DIAMANT, P. ENCK,à G. TOUGAS & A. WALD University of Iowa, Iowa City, USA; *Hospital General
Neurogastroenterol. Mot. (22) 14, 553 559 Minimum standards of anorectal manometry S. S. C. RAO, F. AZPIROZ,* N. DIAMANT, P. ENCK,à G. TOUGAS & A. WALD University of Iowa, Iowa City, USA; *Hospital General
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands
 Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514
 Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily
Biofeedback provides long term benefit for patients with intractable, slow and normal transit constipation
 Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
Esophageal Manometry. John M. Wo, M.D. October 1, 2009
 Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury
 The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
ORIGINAL CONTRIBUTION Anorectal Stimulation Causes Increased Colonic Motor Activity in Subjects With Spinal Cord Injury
 #6 ORIGINAL CONTRIBUTION Anorectal Stimulation Causes Increased Colonic Motor Activity in Subjects With Spinal Cord Injury Mark A. Korsten, MD; Ashwani K. Singal, MD; Amit Monga, MD; Geeta Chaparala, MD;
#6 ORIGINAL CONTRIBUTION Anorectal Stimulation Causes Increased Colonic Motor Activity in Subjects With Spinal Cord Injury Mark A. Korsten, MD; Ashwani K. Singal, MD; Amit Monga, MD; Geeta Chaparala, MD;
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
A collection of High Resolution Esophageal Manometry Patterns
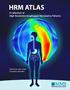 A collection of High Resolution Esophageal Manometry Patterns Distinctive color maps of motility disorders Table of contents Introduction... 3 Normal HRM [B.1]... 4 Achalasia... 5 Classic Achalasia with
A collection of High Resolution Esophageal Manometry Patterns Distinctive color maps of motility disorders Table of contents Introduction... 3 Normal HRM [B.1]... 4 Achalasia... 5 Classic Achalasia with
CHAPTER 2. N.Q. Nguyen 1, R. Rigda 1, M. Tippett 1, J.M. Conchillo 2, A.J.P.M. Smout 2, R.H. Holloway 1
 CHAPTER 2 Assessment of esophageal motor function using combined perfusion manometry and multichannel intraluminal impedance measurement in normal subjects N.Q. Nguyen 1, R. Rigda 1, M. Tippett 1, J.M.
CHAPTER 2 Assessment of esophageal motor function using combined perfusion manometry and multichannel intraluminal impedance measurement in normal subjects N.Q. Nguyen 1, R. Rigda 1, M. Tippett 1, J.M.
traction forces during fasting and after feeding
 Gutl1994; 35:625-63 Human small intestinal and aboral traction forces during fasting and after feeding 625 Department of Medicine, Section of Gastroenterology, University of Manchester Medical School,
Gutl1994; 35:625-63 Human small intestinal and aboral traction forces during fasting and after feeding 625 Department of Medicine, Section of Gastroenterology, University of Manchester Medical School,
pissn: eissn: Journal of Neurogastroenterology and Motility
 JNM J Neurogastroenterol Motil, Vol. 20 No. 3 July, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm14022 Original Article Effects of Chili Treatment on Gastrointestinal and Rectal
JNM J Neurogastroenterol Motil, Vol. 20 No. 3 July, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm14022 Original Article Effects of Chili Treatment on Gastrointestinal and Rectal
Chapter 2 Overview of Testing of Motility and of the Anorectum
 Chapter 2 Overview of Testing of Motility and of the Anorectum Vanessa C. Costilla and Amy E. Foxx-Orenstein Chapter Objectives At the conclusion of reading this chapter, the reader will be able to: 1.
Chapter 2 Overview of Testing of Motility and of the Anorectum Vanessa C. Costilla and Amy E. Foxx-Orenstein Chapter Objectives At the conclusion of reading this chapter, the reader will be able to: 1.
Sigmoid motility in diverticular disease and the
 Gut, 1988, 29, 218-222 Sigmoid motility in diverticular disease and the irritable bowel syndrome I F TROTMAN AND J J MISIEWICZ From the Department of Gastroenterology and Nutrition, Central Middlesex Hospital,
Gut, 1988, 29, 218-222 Sigmoid motility in diverticular disease and the irritable bowel syndrome I F TROTMAN AND J J MISIEWICZ From the Department of Gastroenterology and Nutrition, Central Middlesex Hospital,
Bowel dysfunctions following hysterectomy
 Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
UNDERSTANDING IBS AND CC Implications for diagnosis and management
 UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
Constipation An Overview. Definition Physiology of GI tract Etiology Assessment Treatment
 CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
Principles of Anatomy and Physiology 14 th Edition CHAPTER 24 The Digestive System Introduction The purpose of this chapter is to Identify the anatomical components of the digestive system as well as their
SACRAL NERVE STIMULATION FOR EXPERIENCE IN CHILDREN
 SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
Relationship between ultrasonically detected phasic antral contractions and antral pressure
 Am J Physiol Gastrointest Liver Physiol 281: G95 G101, 2001. Relationship between ultrasonically detected phasic antral contractions and antral pressure K. HVEEM, 1 W. M. SUN, 2 G. HEBBARD, 3 M. HOROWITZ,
Am J Physiol Gastrointest Liver Physiol 281: G95 G101, 2001. Relationship between ultrasonically detected phasic antral contractions and antral pressure K. HVEEM, 1 W. M. SUN, 2 G. HEBBARD, 3 M. HOROWITZ,
For more information about how to cite these materials visit
 Author: John Williams, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author: John Williams, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
MOTOR MECHANISMS UNDERLYING TRANSPYLORIC FLOW OF A HIGH- AND LOW-CALORIC LIQUID NUTRIENT
 MOTOR MECHANISMS UNDERLYING TRANSPYLORIC FLOW OF A HIGH- AND LOW-CALORIC LIQUID NUTRIENT Marco W. Mundt Trygve Hausken Melvin Samsom Submitted 125 ABSTRACT The patterning of antral motor and pressure events
MOTOR MECHANISMS UNDERLYING TRANSPYLORIC FLOW OF A HIGH- AND LOW-CALORIC LIQUID NUTRIENT Marco W. Mundt Trygve Hausken Melvin Samsom Submitted 125 ABSTRACT The patterning of antral motor and pressure events
Abstract. Abnormal peristaltic waves like aperistalsis of the esophageal body, high amplitude and broader waves,
 Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
ANAL SPHINCTER PRESSURE CHARACTERISTICS
 GASTROENTEROLOGY Copyright 1967 by The Williams & Wilkins Co. Vol. 52, No.3 Printed in U.S.A. ANAL SPHINCTER PRESSURE CHARACTERISTICS LEONARD A. KATZ, M.D., HERBERT J. KAUFMANN, M.D., AND HOWARD M. SPIRO,
GASTROENTEROLOGY Copyright 1967 by The Williams & Wilkins Co. Vol. 52, No.3 Printed in U.S.A. ANAL SPHINCTER PRESSURE CHARACTERISTICS LEONARD A. KATZ, M.D., HERBERT J. KAUFMANN, M.D., AND HOWARD M. SPIRO,
Endorectal Balloon during Image Guided Radiation Therapy for Prostate Carcinoma Reduces Radiation Proctitis at 2 Years
 Endorectal Balloon during Image Guided Radiation Therapy for Prostate Carcinoma Reduces Radiation Proctitis at 2 Years Poster No.: R-0041 Congress: Type: 2015 ASM Scientific Exhibit Authors: R. Botten,
Endorectal Balloon during Image Guided Radiation Therapy for Prostate Carcinoma Reduces Radiation Proctitis at 2 Years Poster No.: R-0041 Congress: Type: 2015 ASM Scientific Exhibit Authors: R. Botten,
Physiologic study of the terminal digestive tract in
 Gut, 1986, 27, 1018-1024 Physiologic study of the terminal digestive tract in chronic painful constipation PATRICK MEUNIER From the Manometric Investigation Laboratory, INSERM U 45, Faculte de Medecine
Gut, 1986, 27, 1018-1024 Physiologic study of the terminal digestive tract in chronic painful constipation PATRICK MEUNIER From the Manometric Investigation Laboratory, INSERM U 45, Faculte de Medecine
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
Weekly Prevalence of Symptoms USA vs. Colombia
 THE OVERLAP BETWEEN INFLAMMATORY BOWEL DISEASE AND FUNCTIONAL GASTROINTESTINAL DISORDERS: CHALLENGES AND TREATMENT IMPLICATIONS Miguel Saps, MD Professor of Pediatrics, Ohio State University Director of
THE OVERLAP BETWEEN INFLAMMATORY BOWEL DISEASE AND FUNCTIONAL GASTROINTESTINAL DISORDERS: CHALLENGES AND TREATMENT IMPLICATIONS Miguel Saps, MD Professor of Pediatrics, Ohio State University Director of
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Effect of ileal infusion of glycochenodeoxycholic acid on segmental transit, motility, and flow in the human
 Gut, 1989, 30, 609-617 Effect of ileal infusion of glycochenodeoxycholic acid on segmental transit, motility, and flow in the human jejunum and ileum R PENAGINI, R C SPILLER, J J MISIEWICZ, AND P G FROST
Gut, 1989, 30, 609-617 Effect of ileal infusion of glycochenodeoxycholic acid on segmental transit, motility, and flow in the human jejunum and ileum R PENAGINI, R C SPILLER, J J MISIEWICZ, AND P G FROST
A.J. Bredenoord B.L.A.M. Weusten S. Carmagnola A.J.P.M. Smout
 5 Double-peaked high-pressure zone at the esophagogastric junction in controls and in patients with a hiatal hernia: A study using high-resolution manometry A.J. Bredenoord B.L.A.M. Weusten S. Carmagnola
5 Double-peaked high-pressure zone at the esophagogastric junction in controls and in patients with a hiatal hernia: A study using high-resolution manometry A.J. Bredenoord B.L.A.M. Weusten S. Carmagnola
A ir swallowing during eating and drinking is a normal
 1561 OESOPHAGUS Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring A J Bredenoord, B L A M Weusten, D Sifrim, R Timmer, A J P M Smout... See end
1561 OESOPHAGUS Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring A J Bredenoord, B L A M Weusten, D Sifrim, R Timmer, A J P M Smout... See end
Cholinergic stimulation enhances colonic motor activity, transit, and sensation in humans
 Am J Physiol Gastrointest Liver Physiol 281: G1228 G1237, 2001. Cholinergic stimulation enhances colonic motor activity, transit, and sensation in humans NGAI-MOH LAW, 1 ADIL E. BHARUCHA, 1 ANITA S. UNDALE,
Am J Physiol Gastrointest Liver Physiol 281: G1228 G1237, 2001. Cholinergic stimulation enhances colonic motor activity, transit, and sensation in humans NGAI-MOH LAW, 1 ADIL E. BHARUCHA, 1 ANITA S. UNDALE,
Cholinergic stimulation enhances colonic motor activity, transit, and sensation in humans
 Am J Physiol Gastrointest Liver Physiol 281: G1228 G1237, 2001. Cholinergic stimulation enhances colonic motor activity, transit, and sensation in humans NGAI-MOH LAW, 1 ADIL E. BHARUCHA, 1 ANITA S. UNDALE,
Am J Physiol Gastrointest Liver Physiol 281: G1228 G1237, 2001. Cholinergic stimulation enhances colonic motor activity, transit, and sensation in humans NGAI-MOH LAW, 1 ADIL E. BHARUCHA, 1 ANITA S. UNDALE,
Effect of Biofeedback Therapy in Constipation According to Rectal Sensation
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 157-162 ORiginal Article Effect of Biofeedback Therapy in Constipation According to Rectal Sensation Ji Yong Ahn, Seung-Jae Myung, Kee Wook Jung, Dong-Hoon
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 157-162 ORiginal Article Effect of Biofeedback Therapy in Constipation According to Rectal Sensation Ji Yong Ahn, Seung-Jae Myung, Kee Wook Jung, Dong-Hoon
SPHINCTER OF ODDI DYSFUNCTION (SOD)
 SPHINCTER OF ODDI DYSFUNCTION (SOD) Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice
SPHINCTER OF ODDI DYSFUNCTION (SOD) Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice
Use of Anorectal Manometry During Rectal Infusion of Saline to Investigate Sphincter Function in Incontinent Patients
 GASTROENTEROLOGY 1983;85:105-13 Use of Anorectal Manometry During Rectal Infusion of Saline to Investigate Sphincter Function in Incontinent Patients N. W. READ, W. G. HAYNES, D. C. C. BARTOLO, J. HALL,
GASTROENTEROLOGY 1983;85:105-13 Use of Anorectal Manometry During Rectal Infusion of Saline to Investigate Sphincter Function in Incontinent Patients N. W. READ, W. G. HAYNES, D. C. C. BARTOLO, J. HALL,
Lab 5 Digestion and Hormones of Digestion. 7/16/2015 MDufilho 1
 Lab 5 Digestion and Hormones of Digestion 1 Figure 23.1 Alimentary canal and related accessory digestive organs. Mouth (oral cavity) Tongue* Parotid gland Sublingual gland Submandibular gland Salivary
Lab 5 Digestion and Hormones of Digestion 1 Figure 23.1 Alimentary canal and related accessory digestive organs. Mouth (oral cavity) Tongue* Parotid gland Sublingual gland Submandibular gland Salivary
STUDIES IN HIRSCHSPRUNG'S DISEASE
 STUDIES IN HIRSCHSPRUNG'S DISEASE BY J. R. TROUNCE and A. NIGHTINGALE From the Department of Experimental Medicine and Department ofphysics, Guy's Hospital, London (RECEIVED FOR PUBLICATION NOVEMBER 12,
STUDIES IN HIRSCHSPRUNG'S DISEASE BY J. R. TROUNCE and A. NIGHTINGALE From the Department of Experimental Medicine and Department ofphysics, Guy's Hospital, London (RECEIVED FOR PUBLICATION NOVEMBER 12,
Controlled randomised trial of visual biofeedback
 Gut 1995; 37: 95-99 Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones,
Gut 1995; 37: 95-99 Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones,
Official Publication of the American Gastroe1lterological Association
 GASTROENTEROLOGY@ Official Publication of the American Gastroe1lterological Association COPYRIGHT 1977 THE WILLIAMS & WILKINS Co. Vol. 72 March 1977 Number 3 ALIMENTARY TRACT EVIDENCE THAT ABNORMAL MYOELECTRICAL
GASTROENTEROLOGY@ Official Publication of the American Gastroe1lterological Association COPYRIGHT 1977 THE WILLIAMS & WILKINS Co. Vol. 72 March 1977 Number 3 ALIMENTARY TRACT EVIDENCE THAT ABNORMAL MYOELECTRICAL
Small Bowel Motility Affects Glucose Absorption in a Healthy Man
 Pathophysiology/Complications O R I G I N A L A R T I C L E Small Bowel Motility Affects Glucose Absorption in a Healthy Man MATTHIJS P. SCHWARTZ, MD, PHD MELVIN SAMSOM, MD, PHD WILLEM RENOOIJ, PHD LEO
Pathophysiology/Complications O R I G I N A L A R T I C L E Small Bowel Motility Affects Glucose Absorption in a Healthy Man MATTHIJS P. SCHWARTZ, MD, PHD MELVIN SAMSOM, MD, PHD WILLEM RENOOIJ, PHD LEO
Propulsion and mixing of food in the alimentary tract Chapter 63
 Propulsion and mixing of food in the alimentary tract Chapter 63 Types of GI movements: Propulsive movement-peristalsis Propulsion: controlled movement of ingested foods, liquids, GI secretions, and sloughed
Propulsion and mixing of food in the alimentary tract Chapter 63 Types of GI movements: Propulsive movement-peristalsis Propulsion: controlled movement of ingested foods, liquids, GI secretions, and sloughed
127 Chapter 1 Chapter 2 Chapter 3
 CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
