Controlled randomised trial of visual biofeedback
|
|
|
- Silvester Johnathan Morrison
- 5 years ago
- Views:
Transcription
1 Gut 1995; 37: Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones, St Mark's Hospital, City Road, London EC1V 2PS. Accepted for publication 1 November 1994 TABLE I Controlled randomised trial of visual biofeedback versus muscle training without a visual display for intractable constipation D Koutsomanis, J E Lennard-Jones, A J Roy, M A Kamm Abstract Training to contract the abdominal muscles effectively and to relax the pelvic floor during defecation straining helps some patients with severe constipation. Hitherto all such training has used a visible or audible signal of sphincter muscle activity as a biofeedback method to assist in relaxation. A randomised controlled trial comparing the outcome of muscular training without any biofeedback device with the same training supplemented by an electromyographic (EMG) record visible to the patient is reported. Significant symptomatic improvement was noted and electromyographic measurements confirmed a decrease in pelvic floor muscle activity during defecation straining after treatment in both groups. The outcome was similar in the two treatment groups. Muscular coordination training using personal instruction and encouragement without a visual display is thus a potentially successful treatment suitable for outpatient use by paramedical personnel. (Gut 1995; 37: 95-99) Keywords: constipation, muscular coordination training, biofeedback, electromyography. Two types of muscular incoordination may affect the ability to defecate - some patients contract rather than relax the muscles around the anal canal, others are unable to generate propulsive force in the pelvis.' Biofeedback designed to help patients relax the pelvic floor benefits some of these patients. All techniques reported thus far have used some measuring Comparability of the initial treatment groups Characteristics BFgroup MCTgroup No 3 3 Age (y) (mean (range)) 4 (2-64) 41 (23-63) Sex 24f 29f Length of history (y) (mean (range)) 14 (1-4) 13 (3-4) Bowel frequency (/wk): < > Episodes of straining (/wk): < >7 7 5 No of patients who digitated No of patients who used laxatives No of patients with slow transit (>4 markers at 12 h) 7 1 No of patients who were unable to expel a water filled balloon No of patients who had an increase of EMG activity during defecation straining No of patients who withdrew 1 BF=biofeedback; MCT=muscular coordination training; EMG=electromyographic. device which enables the patient to know whether or not the pelvic floor muscles contract on defecation straining. Controlled study is now needed to simplify muscular training to its essential elements. This paper describes the first randomised controlled trial to show if the visual biofeedback component is necessary to help the patient learn pelvic floor muscular relaxation. If, as our results suggest, muscular training without any measuring equipment relieves the symptoms of many patients, then this safe, effective, and long lasting treatment is applicable as an outpatient technique which can be undertaken by paramedical personnel. Patients and methods SELECTION OF PATIENTS We studied a consecutive series of 6 adult patients, referred to the physiological laboratory for biofeedback treatment: all complained of a bowel frequency of less than three stools weekly or excessive straining on defecation, or both. None was responsive to standard treatments with a high fibre diet and laxatives, and the symptoms were severe enough for referral to a specialist hospital. There were no exclusion criteria on grounds of age or other personal factors. Patients with structural disease of the rectum or colon, as judged by barium enema, defecating proctography, or absence of the rectoanal distension reflex were not included. Most patients showed evidence of pelvic incoordination judged by an increase in pelvic floor muscular activity, determined by electromyographic (EMG) measurements or by the inability to expel a water filled balloon from the rectum on defecation straining (Table I), but those who complained of severe constipation were treated consecutively and these criteria were not required as essential for entry into the trial. CONDUCT OF THE TRIAL The basis of muscular coordination training was explained to each patient. If this treatment was accepted, it was further explained that the need for a visual display of muscular activity is uncertain and the patient was asked to accept initial randomisation into a group treated with or without the display. Each patient was assured that if the first treatment used was unsuccessful after at least two sessions, the alternative treatment would be offered. Before treatment, and after completion of one or both 95
2 96 treatments, the patient was asked to complete a diary card of bowel symptoms and to accept a number of physiological measurements as described elsewhere.'. If the patient gave signed consent to enter the trial, randomisation using a consecutive set of random numbers in sealed envelopes was performed. If the first treatment given was judged unsuccessful by both patient and doctor after two training sessions, the alternative treatment was given. The diary card and repeat physiological measurements were repeated immediately after the last treatment given. Symptomatic follow up by diary card was repeated twice during the two to three months after ending treatment. The patient was not seen between the end of treatment and the follow up assessments. ASSESSMENT OF SYMPTOMS BY DIARY CARD On each of seven consecutive days the patient recorded the number of bowel actions and stool consistency; the number of straining episodes and total time spent straining each day; the need for digitation; use of laxatives, suppositories, or enemas; episodes of abdominal pain and their duration; and an overall assessment of symptoms as better, the same, or worse than usual. PHYSIOLOGICAL ASSESSMENT Whole gut transit rate An abdominal radiograph was performed 12 hours after taking radio-opaque markers. For this study, retention of more than 2% of the markers at 12 hours was regarded as abnormal.2 Electromyography Two adhesive EMG electrodes were placed on the skin over the external anal sphincter at the anal margin. The mean amplitudes (pgv) of the resting trace, the increased activity on maximal voluntary contraction of the anal canal, and the amplitude during straining in an attempt to evacuate a 5 ml air filled balloon were recorded. An anismus index was calculated. This expresses the increment of electrical activity on defecation straining over the resting value as a percentage of the increase on maximal voluntary contraction. The value is positive if the pressure on TABLE II Outcome of biofeedback (BF) and muscular coordination training (MCT) given as the first treatment and as an alternative treatment afterfailure of the first First treatments Cross overs BF MCT BF-*MCT MCT->BF No of patients Patient reported improvement Bowel frequency: Increased Decreased Unchanged Total time spent straining decreased Decrease of EMG activity during straining EMG=electromyographic. Koutsomanis, Lennard-j3ones, Roy, Kamm straining is greater than the resting pressure and negative if the straining pressure is less than the resting pressure. The normal value approximates to zero3 indicating that the anal pressure does not increase over the resting pressure on straining. Simulated defecation A lubricated balloon attached to a catheter was inserted into the rectum and inflated with 5 ml of water. The subject sat on a commode in privacy and was asked to expel the balloon. Success was recorded as passage of the balloon within five minutes. The ability to expel a similar balloon containing 5 ml of air was tested in the lateral position with the legs partially flexed. To maintain gentle constant initial traction and to detect descent of the pelvic floor, the catheter was attached to a spring balance and constant traction of 25 g was applied as the patient began to strain. MUSCULAR COORDINATION TRAINING All patients lay comfortably on their side with the hips and knees partly flexed. A lubricated balloon attached to a catheter was inserted into the lower rectum and inflated with 5 ml of air. All patients were asked to contract the anal canal vigorously and note the sensation. They were also taught to direct propulsive force into the pelvis by taking a deep breath, contracting the upper abdominal (and diaphragmatic) muscles, and at the same time relaxing and protruding the lower abdomen. Correct performance of the manoeuvre was judged by visible protrusion of the lower abdomen. They were then asked to try and expel the balloon without developing any sense of contraction in the anal region while contracting the abdominal muscles as already practiced. Relaxation of the pelvic floor and effective abdominal straining were gauged by downward movement and then passage of the balloon. The movement of the intrarectal balloon was detected by the instructor through gentle traction on the catheter. Repeated instruction and when appropriate, encouragement and praise, were given. The group using biofeedback were taught exactly as described above but, in addition, they watched the EMG trace on a monitor. A resting trace was first displayed and then 'frozen' on one channel of the screen. The wider amplitude of the trace on voluntary muscular contraction compared with the resting trace was next demonstrated using another channel. During balloon expulsion, the patient was taught to maintain a low amplitude of the trace recording muscular activity using the resting record constantly displayed as a model. ETHICAL APPROVAL The project was approved by the Ethical Committee of the City and Hackney Health Authority.
3 Controlled randomised trial of visual biofeedback versus muscle training without a visual display for intractable constipation 97 TABLE III Symptoms recorded on diary cards before, at the end of treatment, and on follow up in the two treatment groups. Numbers shown represent numbers ofpatients or median (range) to 1 CD c I,- z H- 15H Before treatment End of treatment Follow up BF MCT BF MCT BF MCT No No straining episodes/wk 3 (-42) 5-5 (-23) 3 (-7) 3 (-7) 3 (-7) 2-5 (-7) Time spent straining (min/wk) 12 (-12) 15-5 (-96) 4 (-12) 4-5 (-315)*** 4 (-36)** 2 (-23)*** Digitation Pain duration (minlwk) 14 (-9) 6 (-9) 5 (-74)* 15 (-48)** 2 (-18) 2 (-48)* Significance of differences from before treatment *p<o5, **p<-2, ***p<.1. BF=biofeedback, MCT=muscular coordination training. POWER OF THE TRIAL AND STATISTICAL ANALYSIS The total number of patients needed to show a difference in success rate of 3% from the previously established success rate1 of about 5% was regarded as a clinically significant difference. A series of 6 patients was judged to be necessary to show such a difference (p<5) in success rate in three out of four trials. Differences between before and after treatment in each group were assessed as median and range by the one sample Wilcoxon signed rank test, or by Fisher's exact test. Results Biofeedback group COMPARABILITY OF THE TREATMENT GROUPS Of 6 patients who entered the trial, one withdrew from the biofeedback (BF) group after one session and no follow up is available on that patient. Initial and follow up data are available for 29 patients treated first with BF and 3 treated with muscular coordination training (MCT) without a visual display; these 59 are regarded as the evaluable groups. A comparison of the major symptoms and physiological parameters in the two treatment groups is shown in Table I: no major differences are apparent. The increased bowel frequency reported by 23 patients is explained Muscle training group No of bowel M <=2 actions/wk M 37 M >7 Before After Follow Before After Follow treatment treatment up treatment treatment up Figure 1: Weekly bowelfrequency before and after treatment in the two treatment groups. Before treatment some patients experienced decreasedfrequency and others complained of increasedfrequency due to repeated straining efforts. After treatment the proportion of patients with a normal bowelfrequency of 3-7 stools weekly increased similarly in both groups. by frequent straining efforts with the passage of small stools. Two patients in the BF group and one in the MCT group has a rectocele with barium trapping on defecating proctography. Difficulty in defecation, rather than infrequent stools, was the commonest problem reported by both groups. OUTCOME OF FIRST TREATMENT After two sessions neither the patient nor the instructor considered that any benefit had resulted for three patients receiving biofeedback and five patients who received training without biofeedback, these eight patients were then treated in the alternative manner. The results of treatment among the patients who received BF or MCT as the only treatment, and also the results of cross over treatments are shown in Table II. No difference in outcome between the two initial treatments is apparent. The small numbers in the cross over group are not sufficient for any conclusion, though no trend is apparent. OUTCOME AT END OF TREATMENT Full assessment was undertaken at the end of treatment. For 51 patients this was the initial mode of training, for eight patients it was at the end of the second treatment given after crossover. Overall, 14 of 31 patients in the Bf group regarded themselves as improved on seven consecutive days compared with 12 of 28 in the MCT group; one of 31 patients regarded their symptoms as unchanged or worse on each of 7 days in the BF group and eight of 28 in the MCT group (p<. 1), the remaining patients felt better on some days and unchanged or worse on others. Apart from this criterion, symptomatic results were similar (Table III). Bowel frequency tended to increase among those with fewer than three bowel actions per week during the pretreatment period, and decrease in patients with more than seven bowel actions weekly as a result of a decreased number of straining episodes (Fig 1). As a result most patients reported a bowel frequency between three and seven weekly after treatment. Changes in bowel frequency before and after treatment were similar in both groups. The number of straining episodes over seven days decreased to a similar extent in both groups as shown by a reduction in the number of patients with very frequent episodes as well as in the total time spent straining each week (Table III). Digitation was common in both
4 98 Koutsomanis, Lennard-Jones, Roy, Kamm TABLE IV Physiological measurements before and after treatment. Numbers shown represent numbers ofpatients or median (range) Io i.,j5..d,, -u Before treatment After treatment BF MCT BF MCT No EMG amplitude (puv) on straining 1 (36-152) 19 (44-24) 65 (32-124)**** 66 (24-112)**** Anismusindex 45 ( ) 39 (-57+74) 6 (- 47+1)** 8 ( )*** Balloon expulsion: Water Air Absent pelvic floor descent Distension sensation (ml) threshold 6 (1-23) 42 (5-18) 4 (2-15)** 4 (15-1) Urgency 14 (4-43) 125 (15-3) 1 (4-3)** 1 (4-18) MTV 24 (11-7) 19 (5-4) 17 (1o4)**** 155 (8-3)*** Significance between before and after treatment in each group *p<.5, **p<.2, ***p<-1, ****p<-1). BF=biofeedback; MCT=muscular coordination training; EMG=electromyographic; MTV=maximal tolerated volume. groups but its occurrence at least once weekly did not alter with treatment. The duration of abdominal pain decreased similarly and significantly in both groups. There was little change in laxative consumption. The anismus index improved similarly and significantly in both groups (Table IV and Fig 2). EMG activity of the external anal sphincter on defecation straining improved equally and significantly compared with pretreatment results in both groups (Table IV). The pelvic floor failed to descend on straining in nine patients in the BF group, and in seven patients in MCT group, before treatment but did descend in four and one of these patients respectively after treatment. There was also a trend towards increased ability to pass a water filled balloon in both groups (Table III). The volume of air in the rectal balloon necessary to elicit sensation decreased significantly at the end of treatment in the BF group (threshold median 6 v 42 ml, p< 2; urgency 14 v 1 ml, p< 2; maximal tolerated volume 24 v 17 ml, p<.1). Changes in sensation were similar in the MCT group but were significant only for maximal tolerated volume. There was no consistent effect on measured intestinal transit rate, even among patients with slow transit initially. NUMBER OF TRAINING SESSIONS Training was considered adequate by patient and doctor after a mean of 3 (range 1-7) sessions in the BF group and 2 (1-4) in the MCT group. FOLLOW UP The symptoms at the two follow up periods were so similar that only the results of the first diary card after completing treatment are shown in Table III. All patients returned one diary card during follow up but three patients in the BF group and two patients in the MCT group did not return their fourth and final card. There was little difference from the symptoms recorded at the end of treatment. Overall, 12 patients in each of the treatment groups described their symptoms as better on all seven days; seven patients in the BF group and five in the MCT group were unchanged or worse. i,.3.,vj/.ci,.t 'n... Discussion S ,:.' :+, :..s T+--n A- L n1-1- T.. sl_n-4> 4b1_ <_ 4 t is evicent rrom i abie 1 tnat tne commonest symptoms experienced by the patients in this study related to difficulty in defecation rather than infrequent bowel actions. Thus three- * quarters of the patients experienced three or more episodes of defecation straining a week, and about half used a finger to assist defecation. These symptoms are reflected in two physiological observations - 25 of 59 patients were unable to expel a water filled balloon from the rectum when seated on a commode, and in over two thirds there was EMG evidence of increased muscular activity (as compared with the normal decrease) in the anal sphincter on simulated defecation strain ;.-.",..i ". - k.;i A.+Q+' + 4 +m +ik-+:+;++-,:.o.+.'#+.:.+++ ` ,++.-i..r.,..~ IBMWO Figure 2: The anismus index before and after treatment in the two treatment Normal values approximate to zero or a negative figure. (Points with similar overlap.) Three reviews of the published reports,4-6 show that behavioural treatment directed mainly at relaxation of the striated pelvic floor muscles on defecation benefits many patients complaining of severe constipation. All previgroups. ous studies, including our own previous values study,' have used some form of biofeedback technique in which the patients sees or hears,
5 Controlled randomised trial of visual biofeedback versus muscle training without a visual display for intractable constipation 99 or both, a signal indicating external anal sphincter activity during defecation straining. Most of these studies have selected patients for treatment who contract, rather than relax, the pelvic floor muscles on straining. Physiological measurements by others37 have shown that, as in the results reported here, behavioural training succeeds in teaching such adults and children to relax the external anal sphincter during defecation straining. Isotopic proctography has shown that training increases the anorectal angle on straining and the defecation rate.3 We have confirmed the results of another study which showed that biofeedback reduces the volume needed to elicit a sense of distension in the rectum.3 In our previous study,' about half of a consecutive unselected series of patients benefited from the method of biofeedback used for the patients in this trial and the results were similar here: in both groups about 4% of patients regarded their symptoms as improved on every day during two weeks of assessment. Furthermore, we observed that two types of muscular incoordination seem important. Firstly, some patients contract rather than relax the pelvic floor. Secondly, other patients seem unable to generate propulsive force in the pelvis, an observation confirmed by a study which showed that some patients fail to increase their intrarectal pressure normally on straining.8 This trial was designed solely to test whether or not the visual/auditory signal is an important component of the training technique. Our results show that training in abdominal muscle contraction with pelvic floor relaxation is equally effective with or without a measuring device to help the patient know whether or not the pelvic floor muscles relax. We cannot exclude the possibility that a few patients may benefit from such a device but training in muscular coordination alone can be the first treatment. This training requires assessment of the patient's muscular relaxation of the pelvic floor and contraction of the abdominal muscles by the instructor. The patient is constantly encouraged and praised for successful muscular control. These findings are unlikely to be the result of a placebo effect. All the patients had been unsuccessfully treated with increased dietary fibre and drugs before entry to the study. We are not aware of any report of a significant placebo reduction in the need to strain at stool, increased bowel frequency in those in whom it was reduced, or altered physiological responses demonstrated by EMG of the pelvic floor muscles. Yoga, a non-specific form of relaxation did not improve the symptoms of five patients with severe defecation difficulties attributed to puborectalis dysfunction verified by EMG; only one of the five patients regained a normal EMG pattern of response." The sustained symptomatic benefit on follow up in this and other studies also argues against a placebo response. Nonetheless, a placebo controlled study of biofeedback in adult constipation is awaited. This study did not involve a placebo arm, the encouragement provided by the therapist served as a positive reinforcement to the patient learning abdomino-pelvic muscular coordination. This treatment is harmless and long lasting.' 67 9 Since our results suggest that it does not require the facilities of a physiological laboratory it could be used by clinical paramedical personnel. The treatment does require a good rapport between patient and instructor. Its mode of action may be more subtle than muscular retraining alone.' The reason for an inability to strain effectively or relax the pelvic floor needs further assessment since psychological factors may be important in some patients. DK was supported by the Alimentary Pharmacology and Therapeutics Trust and the British Digestive Foundation, MAK was supported by the St Mark's Research Foundation. 1 Koutsomanis D, Lennard-Jones JE, Kamm MA. Prospective study of biofeedback treatment for patients with slow and normal transit constipation. Europ Jf Gastroenterol Hepatol 1994; 6: Evans RC, Kamm MA, Hinton JM, Lennard-Jones JE. The normal range and a simple diagram for recording whole gut transit time. IntJ Colorect Dis 1992; 7: Papachrysostomou M, Smith AN. Effect of biofeedback on obstructive defecation - reconditioning of the defecation reflex? Gut 1994; 35: Enck P. Biofeedback training in disordered defecation: a critical review. Dig Dis Sci 1993; 38: Bassotti G, Whitehead WE. Biofeedback as a treatment approach to gastrointestinal tract disorders. Am J Gastroenterol 1994; 89: Kamm MA. Motility and functional diseases of the large intestine. Current opinion in Gastroenterology 1993; 9: Loening-Baucke V. Modulation of abnormal defecation dynamics by biofeedback treatment in chronically constipated children with encopresis. Jf Pediatr 199; 116: Roberts JP, Thorpe AC, Williams NS. Assessment of defective rectal evacuation by dynamic integrated proctography. BrJSurg 1991; 78: Kawimbe BM, Papachrysostomou M, Binnie NR, Clare N, Smith AN. Outlet obstruction constipation (anismus) managed by biofeedback. Gut 1991; 32: Denis P. Biofeedback for constipation. In: Kamm MA, Lennard-Jones JE. Constipation. Petersfield: Wrightson Biomedical, 1994: Dolk A, Holmstrom B, Johansson C, Frostell C, Nilsson BY. The effect of yoga on puborectalis paradox. Int J Colorect Dis 1991; 6:
Biofeedback provides long term benefit for patients with intractable, slow and normal transit constipation
 Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Response to a behavioural treatment, biofeedback, in constipated patients is associated with improved gut transit and autonomic innervation
 214 St Mark s Hospital, Northwick Park, Watford Road, Harrow, Middlesex HA1 3UJ, UK A V Emmanuel M A Kamm Correspondence to: Professor M Kamm. Kamm@ic.ac.uk Accepted for publication 12 February 2001 Response
214 St Mark s Hospital, Northwick Park, Watford Road, Harrow, Middlesex HA1 3UJ, UK A V Emmanuel M A Kamm Correspondence to: Professor M Kamm. Kamm@ic.ac.uk Accepted for publication 12 February 2001 Response
Langley Catheter Protocols
 Langley Catheter Protocols Stericom Ltd Units 1&2 Higham Mead Chesham HP5 2AH England Tel: +44 (0)1494 794315 Fax: +44 (0)1494 772759 info@stericom.com www.stericom.com Instructions for use The 2-balloon
Langley Catheter Protocols Stericom Ltd Units 1&2 Higham Mead Chesham HP5 2AH England Tel: +44 (0)1494 794315 Fax: +44 (0)1494 772759 info@stericom.com www.stericom.com Instructions for use The 2-balloon
Effect of biofeedback therapy on anorectal physiological parameters among patients with fecal evacuation disorder
 DOI 10.1007/s12664-017-0731-y ORIGINAL ARTICLE Effect of biofeedback therapy on anorectal physiological parameters among patients with fecal evacuation disorder Abhai Verma 1 & Asha Misra 1 & Uday C Ghoshal
DOI 10.1007/s12664-017-0731-y ORIGINAL ARTICLE Effect of biofeedback therapy on anorectal physiological parameters among patients with fecal evacuation disorder Abhai Verma 1 & Asha Misra 1 & Uday C Ghoshal
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
NIH Public Access Author Manuscript Best Pract Res Clin Gastroenterol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: Best Pract Res Clin Gastroenterol. 2011 February ; 25(1): 159 166. doi:10.1016/j.bpg.2011.01.004. BIOFEEDBACK THERAPY FOR CONSTIPATION
NIH Public Access Author Manuscript Published in final edited form as: Best Pract Res Clin Gastroenterol. 2011 February ; 25(1): 159 166. doi:10.1016/j.bpg.2011.01.004. BIOFEEDBACK THERAPY FOR CONSTIPATION
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
PREPARING FOR ANORECTOAL MANOMETRY. ManoScan Anorectal Manometry System
 PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
Outlet syndrome: is there a surgical option?'
 Journal of the Royal Society of Medicine Volume 77 July 1984 559 Outlet syndrome: is there a surgical option?' M R B Keighley MS FRCS P Shouler FRCS Department of Surgery, General Hospital, Birmingham
Journal of the Royal Society of Medicine Volume 77 July 1984 559 Outlet syndrome: is there a surgical option?' M R B Keighley MS FRCS P Shouler FRCS Department of Surgery, General Hospital, Birmingham
reconditioning of the defecation reflex?
 252 Departments of Surgery and Gastroenterology, University of Edinburgh, Western General Hospital, Edinburgh M Papachrysostomou A N Smith Correspondence to: Professor A N Smith, Department of Surgery,
252 Departments of Surgery and Gastroenterology, University of Edinburgh, Western General Hospital, Edinburgh M Papachrysostomou A N Smith Correspondence to: Professor A N Smith, Department of Surgery,
Neurogenic Bowel: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Peer reviewed article systematic review: The management of constipation using physical therapies including biofeedback
 Peer reviewed article systematic review: The management of constipation using physical therapies including biofeedback Abstract Constipation can be a symptom of many diseases and disorders. Functional
Peer reviewed article systematic review: The management of constipation using physical therapies including biofeedback Abstract Constipation can be a symptom of many diseases and disorders. Functional
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients
 A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients Feran Agachan, M.D., Teng Chen, M.D., Johann Pfeifer, M.D., Petachia Reissman, M.D., Steven D. Wexner, M.D.,
A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients Feran Agachan, M.D., Teng Chen, M.D., Johann Pfeifer, M.D., Petachia Reissman, M.D., Steven D. Wexner, M.D.,
Dyssynergic defecation, also termed anismus, 1 or pelvic floor. Digital Rectal Examination Is a Useful Tool for Identifying Patients With Dyssynergia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:955 960 Digital Rectal Examination Is a Useful Tool for Identifying Patients With Dyssynergia KASAYA TANTIPHLACHIVA, PRIYANKA RAO, ASHOK ATTALURI, and SATISH
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:955 960 Digital Rectal Examination Is a Useful Tool for Identifying Patients With Dyssynergia KASAYA TANTIPHLACHIVA, PRIYANKA RAO, ASHOK ATTALURI, and SATISH
The efficacy of a multidisciplinary approach to the management of constipation: a case series
 Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 36 44 CLINICAL PAPER The efficacy of a multidisciplinary approach to the management of constipation: a case
Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 36 44 CLINICAL PAPER The efficacy of a multidisciplinary approach to the management of constipation: a case
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Authors and Disclosures
 Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Biofeedback Program. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Constipation. H. David Vargas, MD. Overview
 Constipation H. David Vargas, MD Overview Constipation is a very common complaint affecting upwards of 15% of all Americans. Fortunately, constipation usually is simple to avoid and easy to treat when
Constipation H. David Vargas, MD Overview Constipation is a very common complaint affecting upwards of 15% of all Americans. Fortunately, constipation usually is simple to avoid and easy to treat when
Randomised controlled trial of biofeedback training in persistent encopresis with anismus
 Arch Dis Child 1998;79:131 135 131 Clinical Epidemiology and Biostatistics Unit, Melbourne University Department of Paediatrics, Royal Children s Hospital, Parkville Victoria, Australia 3052 T Nolan Department
Arch Dis Child 1998;79:131 135 131 Clinical Epidemiology and Biostatistics Unit, Melbourne University Department of Paediatrics, Royal Children s Hospital, Parkville Victoria, Australia 3052 T Nolan Department
Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P.
 UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 4 October, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.4.532 How to Interpret
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 4 October, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.4.532 How to Interpret
MEDICAL POLICY SUBJECT: BIOFEEDBACK
 MEDICAL POLICY PAGE: 1 OF: 6 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 6 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Populations Interventions Comparators Outcomes Individuals: With fecal incontinence
 Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Biofeedback pelvic floor exercise therapy for pelvic floor dyssynergia: an observational study
 International Surgery Journal Porwal A et al. Int Surg J. 2017 Oct;4(10):3461-3465 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174516
International Surgery Journal Porwal A et al. Int Surg J. 2017 Oct;4(10):3461-3465 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174516
Function of the anal sphincters in patients with
 Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Physical Therapy. Pelvic Floor Physical Therapy for Gastrointestinal Conditions. Objectives: Upon completion, participants will be able to:
 Pelvic Floor Physical Therapy for Gastrointestinal Conditions By Meghan Z. Markowski, PT, DPT, WCS, BCB-PMD Brigham and Women s s Hospital Department of Rehabilitation Services 850 Boylston Street, Suite
Pelvic Floor Physical Therapy for Gastrointestinal Conditions By Meghan Z. Markowski, PT, DPT, WCS, BCB-PMD Brigham and Women s s Hospital Department of Rehabilitation Services 850 Boylston Street, Suite
mcompass Interpretation Quick Reference Guide
 mcompass Interpretation Quick Reference Guide This document is designed to give you a starting point for reviewing of the mcompass anorectal manometry results. By no means are these the only questions
mcompass Interpretation Quick Reference Guide This document is designed to give you a starting point for reviewing of the mcompass anorectal manometry results. By no means are these the only questions
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing
 Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Application of Anorectal Dynamics in the Treatment of Colon Disease Packing Zongyue Gao 1, 2, a, Yuyan Liu 1, 2, b, Chunxia Wan 1, 2, c 3, d* and Xiaoli Zhou 1 Henan Province Hospital of TCM, 450000, Henan,
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2014 Origination: 7/2008 Next Review: 7/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2014 Origination: 7/2008 Next Review: 7/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Constipation An Overview. Definition Physiology of GI tract Etiology Assessment Treatment
 CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
Constipation. (Medical Aspects)
 Constipation (Medical Aspects) By Dr. Ehab Abdel Khalik MD. Anatomy of the anorectum The rectum is 12-15 15 cm. long. It connects with the sigmoid colon by the rectosigmoid junction which is believed to
Constipation (Medical Aspects) By Dr. Ehab Abdel Khalik MD. Anatomy of the anorectum The rectum is 12-15 15 cm. long. It connects with the sigmoid colon by the rectosigmoid junction which is believed to
Predictive Capability of Anorectal Physiologic Tests for Unfavorable Outcomes Following Biofeedback Therapy in Dyssynergic Defecation
 ORIGINAL ARTICLE Gastroenterology & Hepatology DOI: 10.3346/jkms.2010.25.7.1060 J Korean Med Sci 2010; 25: 1060-1065 Predictive Capability of Anorectal Physiologic Tests for Unfavorable Outcomes Following
ORIGINAL ARTICLE Gastroenterology & Hepatology DOI: 10.3346/jkms.2010.25.7.1060 J Korean Med Sci 2010; 25: 1060-1065 Predictive Capability of Anorectal Physiologic Tests for Unfavorable Outcomes Following
ANMS-ESNM position paper and consensus guidelines on biofeedback therapy for anorectal disorders
 Neurogastroenterology & Motility Neurogastroenterol Motil (2015) 27, 594 609 doi: 10.1111/nmo.12520 POSITION PAPER ANMS-ESNM position paper and consensus guidelines on therapy for anorectal disorders S.
Neurogastroenterology & Motility Neurogastroenterol Motil (2015) 27, 594 609 doi: 10.1111/nmo.12520 POSITION PAPER ANMS-ESNM position paper and consensus guidelines on therapy for anorectal disorders S.
Efficacy and Safety of Lubiprostone. Laura Wozniak February 23, 2010 K30 Monthly Journal Club
 Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Constipation is a common disorder in children,
 The Effect of Anorectal Manometry on the Outcome of Treatment in Severe Childhood Constipation: A Randomized, Controlled Trial Rijk van Ginkel, MD*; Hans A. Büller, PhD ; Guy E. Boeckxstaens, PhD ; Roos
The Effect of Anorectal Manometry on the Outcome of Treatment in Severe Childhood Constipation: A Randomized, Controlled Trial Rijk van Ginkel, MD*; Hans A. Büller, PhD ; Guy E. Boeckxstaens, PhD ; Roos
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Constipation. Disease Review
 bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 2.01.64 Biofeedback as a Treatment of Fecal Incontinence or Constipation Section 2.0 Medicine Subsection Effective Date February 15, 2015 Original Policy Date December 15, 2014 Next Review Date December
2.01.64 Biofeedback as a Treatment of Fecal Incontinence or Constipation Section 2.0 Medicine Subsection Effective Date February 15, 2015 Original Policy Date December 15, 2014 Next Review Date December
Human Anatomy rectum
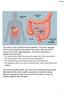 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
Patient satisfaction after biofeedback for constipation and pelvic floor dyssynergia
 Original article Peer reviewed article SWISS MED WKLY 2001;131:152 156 www.smw.ch 152 Patient satisfaction after biofeedback for constipation and pelvic floor dyssynergia Paul H Wiesel, Gian Dorta, Patrick
Original article Peer reviewed article SWISS MED WKLY 2001;131:152 156 www.smw.ch 152 Patient satisfaction after biofeedback for constipation and pelvic floor dyssynergia Paul H Wiesel, Gian Dorta, Patrick
Anal sphincter exercises. Information for patients Sheffield Teaching Hospitals
 Anal sphincter exercises Information for patients Sheffield Teaching Hospitals Anal sphincter exercises to help lessen leakage from the bowel Sphincter exercises, when practiced correctly, can build up
Anal sphincter exercises Information for patients Sheffield Teaching Hospitals Anal sphincter exercises to help lessen leakage from the bowel Sphincter exercises, when practiced correctly, can build up
Medical Policy. MP Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Medical Policy MP 2.01.64 BCBSA Ref. Policy: 2.01.64 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.27 Biofeedback as a Treatment of Urinary Incontinence in
Medical Policy MP 2.01.64 BCBSA Ref. Policy: 2.01.64 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.27 Biofeedback as a Treatment of Urinary Incontinence in
Chapter 2 Overview of Testing of Motility and of the Anorectum
 Chapter 2 Overview of Testing of Motility and of the Anorectum Vanessa C. Costilla and Amy E. Foxx-Orenstein Chapter Objectives At the conclusion of reading this chapter, the reader will be able to: 1.
Chapter 2 Overview of Testing of Motility and of the Anorectum Vanessa C. Costilla and Amy E. Foxx-Orenstein Chapter Objectives At the conclusion of reading this chapter, the reader will be able to: 1.
Measurement of colonic transit time with the Transit-Pellets TM method
 Measurement of colonic transit time with the Transit-Pellets TM method Measurement of colonic transit time is an important investigation in clinical gastroenterology. The measurement is indicated particularly
Measurement of colonic transit time with the Transit-Pellets TM method Measurement of colonic transit time is an important investigation in clinical gastroenterology. The measurement is indicated particularly
Research Article Efficacy of Adaptive Biofeedback Training in Treating Constipation-Related Symptoms
 Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 959734, 5 pages http://dx.doi.org/10.1155/2015/959734 Research Article Efficacy of Adaptive Biofeedback Training in Treating
Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 959734, 5 pages http://dx.doi.org/10.1155/2015/959734 Research Article Efficacy of Adaptive Biofeedback Training in Treating
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 21 No. 1 January, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm14025 Original Article Comparison
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 21 No. 1 January, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm14025 Original Article Comparison
Constipation in childhood is characterized by a low defecation frequency in combination with either involuntary loss of
 USE OF ROME II CRITERIA IN CHILDHOOD DEFECATION DISORDERS: APPLICABILITY IN CLINICAL AND RESEARCH PRACTICE WIEGER P. VOSKUIJL, MD, JAROM HEIJMANS, HUGO S. A. HEIJMANS, MD, PHD, JAN A. J. M. TAMINIAU,MD,PHD,
USE OF ROME II CRITERIA IN CHILDHOOD DEFECATION DISORDERS: APPLICABILITY IN CLINICAL AND RESEARCH PRACTICE WIEGER P. VOSKUIJL, MD, JAROM HEIJMANS, HUGO S. A. HEIJMANS, MD, PHD, JAN A. J. M. TAMINIAU,MD,PHD,
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Constipation in children
 Search date August 2003 Gregory Rubin QUESTIONS Effects of treatments...397 395 INTERVENTIONS CONSTIPATION Trade off between benefits and harms Cisapride with or without magnesium oxide*...397 Unknown
Search date August 2003 Gregory Rubin QUESTIONS Effects of treatments...397 395 INTERVENTIONS CONSTIPATION Trade off between benefits and harms Cisapride with or without magnesium oxide*...397 Unknown
Constipation is one of the most common digestive
 ORIGINAL CONTRIBUTION Successful Physical Therapy for Constipation Related to Puborectalis Dyssynergia Improves Symptom Severity and Quality of Life Christina Lewicky-Gaupp, M.D. 1 Daniel M. Morgan, M.D.
ORIGINAL CONTRIBUTION Successful Physical Therapy for Constipation Related to Puborectalis Dyssynergia Improves Symptom Severity and Quality of Life Christina Lewicky-Gaupp, M.D. 1 Daniel M. Morgan, M.D.
Patient Information Leaflet. Sphincter Exercises for people with Bowel Control Problems
 Patient Information Leaflet Sphincter Exercises for people with Bowel Control Problems Sphincter Exercises for people with Bowel Control Problems Introduction Sphincter exercises can help you to improve
Patient Information Leaflet Sphincter Exercises for people with Bowel Control Problems Sphincter Exercises for people with Bowel Control Problems Introduction Sphincter exercises can help you to improve
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands
 Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
The American Society of Colon and Rectal Surgeons
 CLINICAL PRACTICE GUIDELINES Downloaded from https://journals.lww.com/dcrjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3IJrtBKuSsQVRz8fA4yAY0a8W1YLRn6mHykFpaZ5LFvI= on 03/16/2018
CLINICAL PRACTICE GUIDELINES Downloaded from https://journals.lww.com/dcrjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3IJrtBKuSsQVRz8fA4yAY0a8W1YLRn6mHykFpaZ5LFvI= on 03/16/2018
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
Common Gastrointestinal Problems in the Elderly
 Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
MCOMPASS ANAL MANOMETRY AN OVERVIEW
 MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
MCOMPASS ANAL MANOMETRY AN OVERVIEW ANAL MANOMETRY MEASURES PRESSURE ALLOWS INTERPRITATION SENSATION RAIR RECTAL COMPLIANCE MOTIVATION OF THE PATIENT FUNCTION OF THE PUDENDAL NERVE WHEN TO USE ANAL MANOMETRY
Proctogram examination
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Proctogram examination Radiology Department You have been referred by your doctor for a Proctogram examination as you may have
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Proctogram examination Radiology Department You have been referred by your doctor for a Proctogram examination as you may have
Sacral Nerve Stimulation for Faecal Incontinence
 Sacral Nerve Stimulation for Faecal Incontinence Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital
Sacral Nerve Stimulation for Faecal Incontinence Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital
UNDERSTANDING IBS AND CC Implications for diagnosis and management
 UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
Sphincter exercises for people with bowel control problems. Information for patients. Physiotherapy Department
 Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Constipation. Self-study course
 Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Improving Your Bowel Function
 Improving Your Bowel Function EDUCATES, SUPPORTS AND PROMOTES SPECIALIST PHYSIOTHERAPISTS Glossary symptoms - a feeling of a physical change / bothersome change rectum/back passage - where stool / faeces
Improving Your Bowel Function EDUCATES, SUPPORTS AND PROMOTES SPECIALIST PHYSIOTHERAPISTS Glossary symptoms - a feeling of a physical change / bothersome change rectum/back passage - where stool / faeces
Medicine. Rectal Hyposensitivity Is Associated With a Defecatory Disorder But Not Delayed Colon Transit Time in a Functional Constipation Population
 Medicine OBSERVATIONAL STUDY Rectal Hyposensitivity Is Associated With a Defecatory Disorder But Not Delayed Colon Transit Time in a Functional Constipation Population Ting Yu, PhD, Dong Qian, MSc, Yongping
Medicine OBSERVATIONAL STUDY Rectal Hyposensitivity Is Associated With a Defecatory Disorder But Not Delayed Colon Transit Time in a Functional Constipation Population Ting Yu, PhD, Dong Qian, MSc, Yongping
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES
 OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 9 May 2007
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 9 May 2007 RECTOGESIC 4 mg/g, rectal ointment B/1 (CIP 376 537-0) Applicant : PROSTRAKAN PHARMA SAS Glyceryl trinitrate
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 9 May 2007 RECTOGESIC 4 mg/g, rectal ointment B/1 (CIP 376 537-0) Applicant : PROSTRAKAN PHARMA SAS Glyceryl trinitrate
Transanal irrigation. Toolbox for neurogenic bowel management. Information for patients Spinal Injuries
 Transanal irrigation Toolbox for neurogenic bowel management Information for patients Spinal Injuries Neurogenic bowel dysfunction A number of people with a spinal injury experience faecal incontinence
Transanal irrigation Toolbox for neurogenic bowel management Information for patients Spinal Injuries Neurogenic bowel dysfunction A number of people with a spinal injury experience faecal incontinence
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
High Resolution Anorectal Manometry (HRARM) in Healthy Egyptian Population
 Med. J. Cairo Univ., Vol. 79, No. 2, December: 245-251, 2011 www.medicaljournalofcairouniversity.com High Resolution Anorectal Manometry (HRARM) in Healthy Egyptian Population HALA M.K. IMAM, M.D. and
Med. J. Cairo Univ., Vol. 79, No. 2, December: 245-251, 2011 www.medicaljournalofcairouniversity.com High Resolution Anorectal Manometry (HRARM) in Healthy Egyptian Population HALA M.K. IMAM, M.D. and
A 27-Year-Old Woman With Constipation: Diagnosis and Treatment
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:838 842 EDUCATION PRACTICE A 27-Year-Old Woman With Constipation: Diagnosis and Treatment ARNOLD WALD Section of Gastroenterology and Hepatology, University
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:838 842 EDUCATION PRACTICE A 27-Year-Old Woman With Constipation: Diagnosis and Treatment ARNOLD WALD Section of Gastroenterology and Hepatology, University
idiopathic megacolon Clinical features of idiopathic megarectum and normal, indicating sphincter damage or
 Gut 1997; 41: 93-99 93 Clinical features of idiopathic megarectum and idiopathic megacolon St Mark's Hospital, London J M Gattuso MA Kamm Correspondence to: Dr M A Kamm, St Mark's Hospital, Northwick Park,
Gut 1997; 41: 93-99 93 Clinical features of idiopathic megarectum and idiopathic megacolon St Mark's Hospital, London J M Gattuso MA Kamm Correspondence to: Dr M A Kamm, St Mark's Hospital, Northwick Park,
Summary and conclusion. Summary And Conclusion
 Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Minimum standards of anorectal manometry
 Neurogastroenterol. Mot. (22) 14, 553 559 Minimum standards of anorectal manometry S. S. C. RAO, F. AZPIROZ,* N. DIAMANT, P. ENCK,à G. TOUGAS & A. WALD University of Iowa, Iowa City, USA; *Hospital General
Neurogastroenterol. Mot. (22) 14, 553 559 Minimum standards of anorectal manometry S. S. C. RAO, F. AZPIROZ,* N. DIAMANT, P. ENCK,à G. TOUGAS & A. WALD University of Iowa, Iowa City, USA; *Hospital General
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Chronic constipation in the elderly
 Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
C onstipation is a common problem in children, accounting
 723 ORIGINAL ARTICLE Prognosis of constipation: clinical factors and colonic transit time F de Lorijn, M P van Wijk, J B Reitsma, R van Ginkel, J A J M Taminiau, M A Benninga... See end of article for
723 ORIGINAL ARTICLE Prognosis of constipation: clinical factors and colonic transit time F de Lorijn, M P van Wijk, J B Reitsma, R van Ginkel, J A J M Taminiau, M A Benninga... See end of article for
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Predictors of Response to Biofeedback Treatment in Anal Incontinence
 Predictors of Response to Biofeedback Treatment in Anal Incontinence Xose Fernández-Fraga, M.D., Fernando Azpiroz, M.D., Anna Aparici, R.N., Maite Casaus, R.N., Juan-R Malagelada, M.D. From the Digestive
Predictors of Response to Biofeedback Treatment in Anal Incontinence Xose Fernández-Fraga, M.D., Fernando Azpiroz, M.D., Anna Aparici, R.N., Maite Casaus, R.N., Juan-R Malagelada, M.D. From the Digestive
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
with irritable bowel syndrome?
 Gut, 1984, 25, 168-173 What is the benefit of coarse wheat bran in patients with irritable bowel syndrome? P A CANN, N W READ, AND C D HOLDSWORTH From the Clinical Research Unit, Royal Hallamshire Hospital,
Gut, 1984, 25, 168-173 What is the benefit of coarse wheat bran in patients with irritable bowel syndrome? P A CANN, N W READ, AND C D HOLDSWORTH From the Clinical Research Unit, Royal Hallamshire Hospital,
