Continence problems after stroke
|
|
|
- Zoe Rice
- 6 years ago
- Views:
Transcription
1 Stroke Helpline: Website: stroke.org.uk Continence problems after stroke It is common for people to have problems controlling their bladder and/or bowels after a stroke. Though initially very distressing, these problems are often resolved with time. This factsheet explains some of the continence problems that may happen after stroke, and outlines the treatment and services available to help in the short and longer term. About half of people admitted to hospital with a stroke will have lost control of their bladder, and a third will experience loss of bowel control. This is called incontinence. It is quite normal for incontinence to be a source of concern after a stroke. For many people loss of toilet control is a very sensitive and personal issue and some people may feel like they have lost their dignity. However, there is a lot that can be done to help, and just 15 per cent of stroke survivors will continue to have continence problems a year after their stroke. It is generally easier to regain bowel control than bladder control. Regaining control can improve both your morale and overall recovery. Why do continence problems develop? There are different reasons why you may develop continence problems after a stroke. For example, as with any serious illness or accident, if you are not fully conscious or aware of your surroundings, you may wet or soil yourself without realising it. Your stroke may have damaged the part of the brain that controls your bladder and/ or the bowel. As with other after-effects, it may take time to recover. If you have difficulty walking or moving around (or you need help getting to the toilet) you may not always be able to get there in time. The same may be true if you have communication difficulties and cannot make yourself understood in time. Any extra exertion involved in moving may itself make it more difficult to maintain control. Being less mobile than usual can make you more prone to constipation (difficulty emptying your bowels), which in turn may cause continence problems. You may not be able to eat or drink as much as usual because of the stroke and may be undernourished or dehydrated. This may also lead to constipation. Some medicines, including ones commonly prescribed after a stroke, may affect bladder or bowel control. For instance medicines called diuretics, which may be taken to help lower your blood pressure, may initially affect bladder control. Stroke Association April
2 You may already have had mild continence problems before your stroke, which are likely to be made worse by any lengthy period in bed. Urine retention (being unable to empty your bladder completely) may cause your bladder to swell painfully. It is also more likely that you will suffer bladder infections during any period of inactivity, and these can cause temporary incontinence. Which continence problems can occur after stroke? There are many different types of continence problems that can occur (sometimes in combination) as a result of stroke. These include: Frequency needing to pass urine more often Urgency feeling a sudden, urgent and uncontrollable need to pass urine. This is due to bladder spasm or contractions. Often there is no time to get to the toilet, so you may have an accident Nocturnal incontinence wetting the bed while asleep Functional incontinence caused when the physical effects of a stroke impede mobility or make it difficult to unfasten clothes in time to use the toilet Stress incontinence small amounts of urinary leakage on coughing, sneezing or laughing. This usually happens because the muscles in the pelvic floor or urethral sphincter are weak or damaged. Reflex incontinence passing urine without realising it. This happens when a stroke has affected the part of the 2 brain that senses and controls bladder movement Overflow incontinence where the bladder leaks due to being too full. This can be due to a loss of feeling in your bladder, or difficulty in emptying your bladder effectively (urine retention) Bowel problems Faecal incontinence or uncontrolled bowel movement. This can be caused by damage to the part of the brain controlling the bowel, not being able to get to the toilet in time, diarrhoea or constipation. Constipation with overflow large stools can get stuck and block the bowel. Liquid stools above the blockage can flow around it causing watery stools to leak. Faecal impaction dry and hardened stools collect in the rectum, they can press on your bladder and make any problems you have with emptying your bladder worse. Initial care after stroke Until you are well enough to start actively regaining control of your bladder or bowel, you may need to wear incontinence pads. These should be changed rapidly by the nursing staff if they become soiled. If you have good bladder and bowel function but are unable to indicate when you need the toilet, the nurses may offer you the toilet or commode every two hours or so. While you are in bed, you may be transferred to the commode using a hoist, or offered a bottle or sheath urinal (designed for men) or Stroke Association April 2012
3 a bedpan (for women). If your bladder is not emptying completely, then a catheter may be used to empty it. This involves gently inserting a fine tube to drain urine from the bladder into a bag. This may need to be done several times a day (intermittent catheterisation) to keep you comfortable and reduce the risk of developing a urinary tract infection (UTI). If you develop soreness through skin contact with your urine, or the catheterisation causes discomfort, an indwelling (or semi-permanent) catheter may be used. Faecal containment bags are used in intensive care, but you are more likely to wear pads if you are on a stroke unit. Good hygiene and skin care are therefore important to protect your skin from damage. Assessment If you stay in hospital after your stroke, in the second week or so, your medical team will carry out an assessment to establish the nature and cause of your difficulties and devise an effective treatment programme. The continence assessment may include: a medical history of any problems you had before the stroke and your current medication that could be affecting control a simple chart recording your fluid intake and output (by volume and frequency) over at least two days further tests ranging from a simple physical examination to bladder ultrasound scan, abdominal x-ray or specialist investigations to determine exactly how your bladder and bowel are working. What are the treatments for bladder incontinence? Once the underlying cause of incontinence has been determined, suitable treatment will be offered. This may include: Bladder training which reduces urgency and frequency by gradually retraining your bladder to be less active and to hold more urine. This is done by making regular visits to the toilet, and gradually extending the time between visits until your bladder learns how to hold on. Pelvic floor exercises help strengthen muscles so that they provide support. This will help improve bladder control and improve or stop leakage of urine. Bladder stimulation vibrating devices are sometimes effective where there is difficulty in emptying the bladder. Medication may help to reduce urine production, urgency and frequency. Weight loss (if you are overweight) will often improve bladder control in the longer term. a urine sample analysis to rule out infections a chart recording bowel movements and consistency Stroke Association April
4 What are the treatments for bowel incontinence? Treatment for bowel (faecal) incontinence may include: Bowel training through regular visits to the toilet (usually after meals, when the bowels are stimulated to move by a natural reflex). You also learn to delay bowel movements once on the toilet to improve your ability to hold on. Medication to help reduce movement in the bowel or make the sphincter muscle tighter to avoid leakage. Treatment for constipation using laxatives. A bowel regimen which uses medicine to make you constipated followed by an enema (putting liquid into your anus) to clear the bowel in a controlled way. Dietary changes such as eating more fibre if you have constipation and eating less fibre if you have diarrhoea. Which professionals can help me? Your medical team will investigate and treat your continence problems. They should also train you in managing your (or your loved one s) continence problems and arrange for a supply of any necessary continence products before you are discharged from hospital. Community health and social care services should arrange any ongoing support that you may need once you are back at home. If you are eligible to receive a regular supply 4 of continence products through the NHS Continence Service, you should also receive a regular review of your needs in this respect (at least once a year). Eligibility varies throughout the UK. In Scotland, most Health Boards allocate supplies free of charge, but will limit the type of products that can be provided within their area. Continence advisers are specialist nurses who are trained to help with incontinence. They can develop a plan that is tailored to your individual circumstances. Your local health centre, or the Bladder and Bowel Foundation (see Useful organisations) can provide details of your nearest continence clinic. Your GP can also advise you, though you do not need a GP referral for this service. If you need further help, you may need to see a specialist consultant, such as a urologist, gastroenterologist, gynaecologist or geriatrician. A doctor s referral will be needed for this. Physiotherapists provide training and exercises to improve mobility. They can show you how best to move from your bed or chair to a commode or toilet, and teach you exercises to strengthen your pelvic floor muscles and improve bladder or bowel function. These are effective, though you may have to persevere for several months before you see results. Occupational therapists help you regain your independence through activities to support your recovery. They can also help if your home needs to be adapted (for instance by having hand rails put up) or if any mobility equipment is needed to make it easier to use the toilet, such as walking aids or a wheelchair. Stroke Association April 2012
5 Speech and language therapists can assess the right texture of food for you if you are having difficulty swallowing safely. Dietitians can recommend a suitable well balanced diet and fluid intake, as well as any dietary changes that may help with continence problems. Social workers can help with financial issues, such as obtaining benefits, and securing any grant you may be entitled to if you need to adapt your bathroom or build one downstairs. In some circumstances social services may help with bedding but this varies depending on where you live. Living with ongoing incontinence While it does involve extra thought and effort, with good advice and preparation, incontinence can be managed discreetly as part of daily living. There are various continence products available. These include high-absorbency pads and pull ups, with a built-in hydrophobic layer for skin protection. Your GP or continence adviser will be able to tell you what is provided free of charge through your local NHS. Absorbent, washable seat pads can be used to protect your furniture and are made in a range of colours. Mattress protectors and absorbent bed pads with tuck-in flaps (known as draw sheets) will reduce how often you need to change your bedding. A commode is like a chair with a removable potty under the seat, and can be useful to have in the bedroom, especially at night. You may be able to obtain a commode through your local social services. Otherwise they are available from specialist suppliers or to order from retailers such as Boots. Practical measures like planning access to toilets, when you are out, and having a change of clothing and hygiene kit with you (which might include plastic bags for disposal or laundry, soap and flannel, antibacterial wet wipes and latex gloves) will help you manage in any situation. The National Key Scheme (NKS), or Royal Association for Disability Rights (RADAR) Scheme, provides keys to public disabled toilets designed for wheelchair access. The scheme is available to people with disabilities or health conditions seriously affecting their continence. If you are eligible your council may provide a key free of charge. See Useful organisations section. A daily routine of regular visits to the toilet, and reducing the amount you drink before bed time, will help to avoid accidents. An alarm can be used to schedule a visit to the toilet during the night, or you may prefer to try a moisture alarm on your bed, which will sound when wetness is detected. This is designed to wake you up so that you can finish emptying your bladder in the toilet. You may wish to wear a silent vibrating alarm watch, which can be set to give a discreet reminder at regular intervals. A silent alarm also has advantages at night time, if you wish to avoid disturbing others. Specialised products such as catheters, anal plugs, urine drainage bags and appliances for men can be obtained on prescription from your GP. In Scotland pads are also available on prescription. Normal prescription charges and exemptions apply. Stroke Association April
6 Washable or disposable waterproof bed and seat covers are generally not provided by the NHS. Products can also be purchased from some pharmacies and by mail order or online. If you buy products from a chemist or by mail order, they can give you a form to sign so you do not pay VAT. The moisture, friction and bacteria associated with incontinence can cause skin rashes and infection. Careful hygiene and skin care around the affected area are needed to avoid the risk of dermatitis (inflammation of the skin). If your skin is badly affected, an indwelling catheter, in which the bag is attached to the leg and worn under clothing, may be recommended, though this is generally used as a last resort. In some cases a supra-pubic catheter, where the catheter is inserted into the bladder through the abdomen wall, may prove a more convenient method of permanent drainage. Your continence adviser should be able to advise you in detail about these procedures. Helping yourself Adopt a routine (as outlined above) to help avoid accidents. Remember to follow all the tips and exercises your physiotherapist has given you it takes time for the effects to show (and to be maintained). Drink plenty of fluids during the day especially water. This will help to avoid infections of the bladder and also constipation. Try to have 6-8 glasses of fluid each day, and more if you have a catheter. 6 Cut down on drinks which contain caffeine such as tea, coffee and cola, and alcoholic drinks, as they can irritate the bladder. Follow a balanced diet with plenty of fruits and vegetables. They contain valuable fibre, which helps bowel movements. Keep as active as you can. This will help stimulate the bowel to move regularly. Try to use the toilet as soon as you need to, and empty your bladder fully. This can also help to avoid infections. Wear clothes that are easier to unfasten, for example with Velcro or elasticated waistbands instead of buttons or fiddly fasteners. Take care of your skin by using mild soap or specialised products and take care to cleanse and dry thoroughly. Dispose of incontinence materials safely. Ensure that disposal bags are secure and leak-proof and use a bin with a lid. If you are caring for someone You may feel out of your depth when faced with incontinence, even if you are emotionally and physically strong. You and your loved one may well find it difficult to preserve their comfort and dignity while following a toileting routine, giving and receiving intimate care or dealing with soiled clothes and bed linen. You may find it useful to speak to a specialist continence adviser or one of the organisations listed on page 7. They will be able to talk through your questions and concerns, help you to consider all of the Stroke Association April 2012
7 options, and make practical arrangements for the longer term. If you decide to take on caring for your loved one at home, then our factsheet F4, Stroke: a carer s guide will prove useful, and our Stroke Helpline can put you in contact with your local carer support services. Useful organisations All organisations listed are UK-wide unless otherwise stated. Stroke Association Stroke Helpline: Website: stroke.org.uk info@stroke.org.uk Contact us for information about stroke, emotional support and details of local services and support groups. Age UK Incontinence Tel: Website: This continence advice and product ordering service is run as a business in association with Age UK. Sample packs of a wide range of products are available to order. Bladder and Bowel Foundation Nurse Helpline: info@bladderandbowelfoundation.org Website: Offers information and support and a Just Can t Wait toilet card ( 5 or free to subscribers) for people with continence issues. Has a UK-wide Directory of NHS and private continence services. British Red Cross Tel: Website: Local branches offer short-term loan of equipment such as commodes. DLF (Disabled Living Foundation) Helpline: advice@dlf.org.uk Website: Provides free, impartial and authoritative advice about equipment and resources to help with all aspects of daily living. ERIC (Education and Resources for Improving Childhood Continence) Helpline: Website: A national charity supporting children and young people, families and health professionals on childhood continence bedwetting, daytime wetting, soiling and constipation, and potty training. PromoCon Disabled Living Centre, Redbank House, 4 St Chad s Street, Manchester M8 8QA Helpline: info@disabledliving.co.uk Website: promocon Offers a national display of continence products, a helpline and individual continence assessments. Disability Rights UK Tel: enquiries@disabilityrightsuk.org Website: Co-ordinates the National Key Scheme for wheelchair accessible toilets, supplying keys and a directory of over 8,000 toilets fitted with a RADAR lock at nominal cost. Stroke Association April
8 Disclaimer: The Stroke Association provides the details of other organisations for information only. Inclusion in this factsheet does not constitute a recommendation or endorsement. Produced by the Stroke Association s Information Service. For sources used, visit stroke.org.uk Stroke Association Factsheet 12, version 01 (published April 2012, next review due September 2013). Item code: A01F12 The Stroke Association is a charity. We rely on your support. Text STROKE 5 to to donate % of your donation goes to the Stroke Association. Find out how your support helps at stroke.org.uk/savelives Stroke Association is registered as a charity in England and Wales (No ) and in Scotland (SC037789). Also registered in Northern Ireland (XT33805), Isle of Man (No 945) and Jersey (NPO 369). Stroke Association April
Continence problems after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Continence problems after stroke This guide explains some of the bladder and bowel problems that may happen after stroke. It also looks
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Continence problems after stroke This guide explains some of the bladder and bowel problems that may happen after stroke. It also looks
For details on how to order other Age UK Factsheets and information materials go to section 8.
 Factsheet 23 January 2011 Help with continence About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or
Factsheet 23 January 2011 Help with continence About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries
 Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
WHAT TYPES OF CONTINENCE PRODUCTS ARE THERE?
 15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
Coping with incontinence
 Coping with incontinence Incontinence can be upsetting and humiliating for the person with dementia and stressful for the carer. But approaching the problem with understanding, matter-of-factness and humour
Coping with incontinence Incontinence can be upsetting and humiliating for the person with dementia and stressful for the carer. But approaching the problem with understanding, matter-of-factness and humour
A word about incontinence
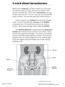 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
Help with continence. Factsheet 23 March About this factsheet
 Factsheet 23 March 2014 About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or manage incontinence and
Factsheet 23 March 2014 About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or manage incontinence and
Discussions about having a Supra pubic catheter
 Discussions about having a Supra pubic catheter What is a supra pubic catheter? A supra pubic catheter is used to drain urine from the bladder by inserting a catheter (narrow hollow drainage tube) directly
Discussions about having a Supra pubic catheter What is a supra pubic catheter? A supra pubic catheter is used to drain urine from the bladder by inserting a catheter (narrow hollow drainage tube) directly
Information and instruction for Home Helps caring for clients with indwelling urinary catheters
 Information and instruction for Home Helps caring for clients with indwelling urinary catheters This leaflet provides you with information and instructions on caring for clients who have an indwelling
Information and instruction for Home Helps caring for clients with indwelling urinary catheters This leaflet provides you with information and instructions on caring for clients who have an indwelling
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
Indwelling Urinary Catheters And Drainage systems
 If you require this leaflet in any other format, e.g., large print, please telephone 01935 384256 Indwelling Urinary Catheters And Drainage systems Useful organisations Ms Society Helpline Tel: 0808 800
If you require this leaflet in any other format, e.g., large print, please telephone 01935 384256 Indwelling Urinary Catheters And Drainage systems Useful organisations Ms Society Helpline Tel: 0808 800
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Urinary Catheter Passport
 Urinary Catheter Passport Catheter Change Record and Looking After Your Urinary Catheter Please take this booklet with you if you are admitted to hospital or have an appointment Patient details Name Address
Urinary Catheter Passport Catheter Change Record and Looking After Your Urinary Catheter Please take this booklet with you if you are admitted to hospital or have an appointment Patient details Name Address
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS
 Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
It is possible to manage the bladder problems of MSA even if they cannot be cured.
 How the bladder works What goes wrong? What investigations need to be done? Who can help? Advice Medication Equipment Other help Useful contacts Continence in MSA It is possible to manage the bladder problems
How the bladder works What goes wrong? What investigations need to be done? Who can help? Advice Medication Equipment Other help Useful contacts Continence in MSA It is possible to manage the bladder problems
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Continence in MSA. How the bladder works
 How the bladder works What goes wrong? What investigations need to be done? Who can help? Advice Medication Equipment Other help Useful contacts Continence in MSA Bladder problems are very common in people
How the bladder works What goes wrong? What investigations need to be done? Who can help? Advice Medication Equipment Other help Useful contacts Continence in MSA Bladder problems are very common in people
Managing your bladder with a Supra-pubic catheter at home
 Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Caring for your indwelling urinary catheter
 Caring for your indwelling urinary catheter Information for patients This information is produced by the Continence, Urology and Colorectal Service Leeds Community Healthcare NHS Trust Having a urinary
Caring for your indwelling urinary catheter Information for patients This information is produced by the Continence, Urology and Colorectal Service Leeds Community Healthcare NHS Trust Having a urinary
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Patient Urinary Catheter Passport
 Useful contact details: Continence Service (Community) 01724 298325 Continence Service (Goole) 01482 336951 Continence Service (SGH) 01724 282282 Ext 2823 Continence Service (DPOW) 01472 874111 Infection
Useful contact details: Continence Service (Community) 01724 298325 Continence Service (Goole) 01482 336951 Continence Service (SGH) 01724 282282 Ext 2823 Continence Service (DPOW) 01472 874111 Infection
Chapter 18. Assisting With Urinary Elimination. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 18 Assisting With Urinary Elimination The urinary system: The Urinary System Removes waste products from the blood Maintains the body s water balance 2 Normal Urination The healthy adult produces
Chapter 18 Assisting With Urinary Elimination The urinary system: The Urinary System Removes waste products from the blood Maintains the body s water balance 2 Normal Urination The healthy adult produces
Patient Urinary Catheter Passport
 Useful contact details Name Contact Number Produced by Adapted from Worth by Michelle Pickering, Continence Specialist Practitioner Hambleton and Richmondshire Locality Continence Advisory Service and
Useful contact details Name Contact Number Produced by Adapted from Worth by Michelle Pickering, Continence Specialist Practitioner Hambleton and Richmondshire Locality Continence Advisory Service and
NHS Urinary Catheter Passport
 South Sefton Care Home Innovation Programme (CHIP) PROTOCOL 07:Urinary Catheter Passport NHS Urinary Catheter Passport Information for patients and carers The passport is a hand held patient document for
South Sefton Care Home Innovation Programme (CHIP) PROTOCOL 07:Urinary Catheter Passport NHS Urinary Catheter Passport Information for patients and carers The passport is a hand held patient document for
A Stress Urinary Incontinence fact sheet for
 A Stress Urinary Incontinence fact sheet for women and teenagers What is Stress Urinary Incontinence? Get to know your gusset - the science bit Stress urinary incontinence (SUI) is defined as a sudden
A Stress Urinary Incontinence fact sheet for women and teenagers What is Stress Urinary Incontinence? Get to know your gusset - the science bit Stress urinary incontinence (SUI) is defined as a sudden
Your catheter. Information for patients and carers. NHS Grampian Continence Service
 Your catheter Information for patients and carers NHS Grampian Continence Service Healthcare professional details Name: Contact number:. GP: Telephone number: Reason for catheterisation:... Date of initial
Your catheter Information for patients and carers NHS Grampian Continence Service Healthcare professional details Name: Contact number:. GP: Telephone number: Reason for catheterisation:... Date of initial
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
Indwelling urinary catheter
 Indwelling urinary catheter Information for patients and carers RDaSH leading the way with care What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder. Following
Indwelling urinary catheter Information for patients and carers RDaSH leading the way with care What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder. Following
University College Hospital at Westmoreland Street. Urinary sheaths. Urology Directorate
 University College Hospital at Westmoreland Street Urinary sheaths Urology Directorate If you would like this document in another language or format, or require the services of an interpreter, contact
University College Hospital at Westmoreland Street Urinary sheaths Urology Directorate If you would like this document in another language or format, or require the services of an interpreter, contact
Discussions about Mitrofanoff
 Discussions about Mitrofanoff This booklet provides general supporting information, alongside clinical information, which will be provided by your Doctor or Specialist Nurse. What is a Mitrofanoff? A Mitrofanoff,
Discussions about Mitrofanoff This booklet provides general supporting information, alongside clinical information, which will be provided by your Doctor or Specialist Nurse. What is a Mitrofanoff? A Mitrofanoff,
Continence and using the toilet
 Continence and using the toilet Factsheet 502LP September 2016 People with dementia can experience difficulties with using the toilet. Accidents and incontinence can also cause problems, particularly as
Continence and using the toilet Factsheet 502LP September 2016 People with dementia can experience difficulties with using the toilet. Accidents and incontinence can also cause problems, particularly as
Keeping control What you should expect from your NHS bladder and bowel service
 Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
My Urinary Catheter Passport Looking after my urinary catheter
 Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
University College Hospital. Discharge information for patients after HIFU (High Intensity Focused Ultrasound) Urology Directorate
 University College Hospital Discharge information for patients after HIFU (High Intensity Focused Ultrasound) Urology Directorate 2 If you would like this document in another language or format, or require
University College Hospital Discharge information for patients after HIFU (High Intensity Focused Ultrasound) Urology Directorate 2 If you would like this document in another language or format, or require
CATHETER PASSPORT. Looking after your Urinary Catheter. The Catheter Passport should be given to all patients with a urinary catheter.
 CATHETER PASSPORT Looking after your Urinary Catheter The Catheter Passport should be given to all patients with a urinary catheter. Health care staff should ensure that page 10 is completed. This document
CATHETER PASSPORT Looking after your Urinary Catheter The Catheter Passport should be given to all patients with a urinary catheter. Health care staff should ensure that page 10 is completed. This document
Pelvic floor muscle exercises
 Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
HELPING SCHOOLS MANAGE CONTINENCE PROBLEMS. The Right to
 HELPING SCHOOLS MANAGE CONTINENCE PROBLEMS The Right to Go Continence problems in childhood are common and as a result it is not unusual for schools to have at least one child with a wetting or soiling
HELPING SCHOOLS MANAGE CONTINENCE PROBLEMS The Right to Go Continence problems in childhood are common and as a result it is not unusual for schools to have at least one child with a wetting or soiling
Urinary catheter passport
 Urinary catheter passport The aim of this passport is to provide you with the all the necessary information to enable you to care for your urinary catheter. It will also provide a useful form of communication
Urinary catheter passport The aim of this passport is to provide you with the all the necessary information to enable you to care for your urinary catheter. It will also provide a useful form of communication
B l a d d e r & B o w e l C a r e. For Patients with Spinal Cord Injuries
 B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Intermittent self catheterisation (ISC) Information for patients Gynaecology
 Intermittent self catheterisation (ISC) Information for patients Gynaecology page 2 of 8 What is ISC? Intermittent self catheterisation (ISC) is a simple technique where a narrow tube (catheter) is inserted
Intermittent self catheterisation (ISC) Information for patients Gynaecology page 2 of 8 What is ISC? Intermittent self catheterisation (ISC) is a simple technique where a narrow tube (catheter) is inserted
Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises
 MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
opyright 2017 SAMPLE COPY Property of Hayward Bell Ltd Copyright 2017 Bladder and bowel conditions can affect anyone
 Bladder and bowel conditions can affect anyone This booklet could be your first positive step to a full and active life Contents 1. Introduction 2. A bladder 3. The most common problems 5. A bowel 6. Functional
Bladder and bowel conditions can affect anyone This booklet could be your first positive step to a full and active life Contents 1. Introduction 2. A bladder 3. The most common problems 5. A bowel 6. Functional
Managing your suprapubic catheter
 Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Please read the following information and have the child follow the bladder retraining protocol included.
 Urology Clinic Hospital for Sick Children Please read the following information and have the child follow the bladder retraining protocol included. Information on bladder retraining, urinary tract infections
Urology Clinic Hospital for Sick Children Please read the following information and have the child follow the bladder retraining protocol included. Information on bladder retraining, urinary tract infections
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment
 Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Trans urethral resection of prostate (TURP)
 Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
A Healthy Bladder. What to do if things go wrong.
 A Healthy Bladder What to do if things go wrong www.bladderandbowel.org Contents Introduction How the bladder works What can go wrong with the bladder? Keeping a healthy bladder What can be done to treat
A Healthy Bladder What to do if things go wrong www.bladderandbowel.org Contents Introduction How the bladder works What can go wrong with the bladder? Keeping a healthy bladder What can be done to treat
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Fatigue after stroke. What is post-stroke fatigue? Who is affected by post-stroke fatigue?
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Fatigue after stroke Fatigue affects half of all stroke survivors, but the signs of fatigue are not always obvious to other people and
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Fatigue after stroke Fatigue affects half of all stroke survivors, but the signs of fatigue are not always obvious to other people and
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
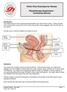 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
How will a colostomy affect me?
 How will a colostomy affect me? Freephone helpline: 0800 328 4257 www.colostomyassociation.org.uk Contents... Introduction 4 What is a colostomy? 6 What will it look and feel like? 6 Will I always have
How will a colostomy affect me? Freephone helpline: 0800 328 4257 www.colostomyassociation.org.uk Contents... Introduction 4 What is a colostomy? 6 What will it look and feel like? 6 Will I always have
University Hospitals Bristol NHS Foundation Trust NHS. Catheterisation using a Mitrofanoff
 University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
Self Catheterisation for Men
 Intermittent Self Catheterisation for Men www.fittleworth.com Opening Hours: 8 am to 8 pm Monday to Friday 9 am to 1 pm Saturday National: 0800 378 846 Scotland: 0800 783 7148 Intermittent Self Catheterisation
Intermittent Self Catheterisation for Men www.fittleworth.com Opening Hours: 8 am to 8 pm Monday to Friday 9 am to 1 pm Saturday National: 0800 378 846 Scotland: 0800 783 7148 Intermittent Self Catheterisation
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Module 5 Management Of Urinary Incontinence
 Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
Management Of Urinary Incontinence V3: Last Reviewed September 2017 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence
UROLOGY SYDNEY Level 1, St George Medical Centre 1 South Street Kogarah NSW 2217 Ph: Fax:
 Pre Operative care: Preop investigations: Radical Prostatectomy Pre and Post Operative Care Once your surgery date has been decided you will be sent for routine blood and urine tests, an ECG will also
Pre Operative care: Preop investigations: Radical Prostatectomy Pre and Post Operative Care Once your surgery date has been decided you will be sent for routine blood and urine tests, an ECG will also
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire
 Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries
 Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries page 2 of 8 This leaflet has been produced in support of the explanation and counselling provided by your urologist and nurse specialist.
Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries page 2 of 8 This leaflet has been produced in support of the explanation and counselling provided by your urologist and nurse specialist.
Bladder and Bowel Symptoms Troubleshooting Tips
 Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
1st stage neuromodulation test
 1st stage neuromodulation test Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 12 This leaflet is to give you some background information
1st stage neuromodulation test Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 12 This leaflet is to give you some background information
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Incontinence Patient Information Form
 Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Suprapubic and Mitrofanoff Catheter Care
 Urinary catheters are tubes that drain urine from your child s bladder. There are many different types of urinary catheters. Your nurse will teach you how to care for these catheters. Here is information
Urinary catheters are tubes that drain urine from your child s bladder. There are many different types of urinary catheters. Your nurse will teach you how to care for these catheters. Here is information
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Urinary Catheter Passport for patients
 Urinary Catheter Passport for patients Nursing A guide for patients and visitors Contents Why people need a urinary catheter...1 How your bladder and kidneys work...1 What is a catheter?...3 Drainage bags...3
Urinary Catheter Passport for patients Nursing A guide for patients and visitors Contents Why people need a urinary catheter...1 How your bladder and kidneys work...1 What is a catheter?...3 Drainage bags...3
Staying steady. Health & wellbeing. Improving your strength and balance. AgeUKIG14
 Staying steady Improving your strength and balance Health & wellbeing AgeUKIG14 Age UK is the new force combining Age Concern and Help the Aged. With almost 120 years of combined history to draw on, we
Staying steady Improving your strength and balance Health & wellbeing AgeUKIG14 Age UK is the new force combining Age Concern and Help the Aged. With almost 120 years of combined history to draw on, we
Urodynamic Tests. Department of Gynaecology. Patient Information
 Urodynamic Tests Department of Gynaecology Patient Information What are urodynamic tests? Urodynamic tests assess the dynamic function of the lower urinary tract. The tests assess 3 functions; The ability
Urodynamic Tests Department of Gynaecology Patient Information What are urodynamic tests? Urodynamic tests assess the dynamic function of the lower urinary tract. The tests assess 3 functions; The ability
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
How to care for your urethral catheter
 How to care for your urethral catheter Department of Urology 2 Patient Information Contents What is a urethral catheter? 2 How should I care for my catheter? 2 Living with your catheter 3 Care of your
How to care for your urethral catheter Department of Urology 2 Patient Information Contents What is a urethral catheter? 2 How should I care for my catheter? 2 Living with your catheter 3 Care of your
TransUrethral Resection for a Bladder Tumour ~ TURBT Women ~
 TransUrethral Resection for a Bladder Tumour ~ TURBT Women ~ To learn about TransUrethral Resection of a Bladder Tumour, you will need to know what these words mean: The bladder stores urine that is made
TransUrethral Resection for a Bladder Tumour ~ TURBT Women ~ To learn about TransUrethral Resection of a Bladder Tumour, you will need to know what these words mean: The bladder stores urine that is made
Stricture guide. Urology department. yeovilhospital.nhs.uk
 Stricture guide Urology department 01935 384 394 yeovilhospital.nhs.uk What is a urethral stricture? A urethral stricture is a narrowing or restriction of the urethra (the tube from your bladder through
Stricture guide Urology department 01935 384 394 yeovilhospital.nhs.uk What is a urethral stricture? A urethral stricture is a narrowing or restriction of the urethra (the tube from your bladder through
Returning Home After Prostatectomy
 Returning Home After Prostatectomy Catholic Medical Center in conjunction with Manchester Urology Associates is proud to be one of the few hospitals in the United States to offer Robotic Assisted radical
Returning Home After Prostatectomy Catholic Medical Center in conjunction with Manchester Urology Associates is proud to be one of the few hospitals in the United States to offer Robotic Assisted radical
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Stoma Care Policy and Procedures
 Stoma Care Policy and Procedures Policy number 19.09 Approved by :CEO Version 1 Scheduled review date 28/3/2018 Created on 28/3/2017 POLICY STATEMENT Clients requiring management with the stoma will be
Stoma Care Policy and Procedures Policy number 19.09 Approved by :CEO Version 1 Scheduled review date 28/3/2018 Created on 28/3/2017 POLICY STATEMENT Clients requiring management with the stoma will be
Drinking fluids and how they affect your bladder
 www.olarts.com Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS.
www.olarts.com Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS.
Looking after your suprapubic catheter. Information for patients
 Looking after your suprapubic catheter Information for patients What is a suprapubic catheter? A catheter is a soft hollow tube, which is used to drain urine from the bladder. The catheter is inserted
Looking after your suprapubic catheter Information for patients What is a suprapubic catheter? A catheter is a soft hollow tube, which is used to drain urine from the bladder. The catheter is inserted
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
After care following insertion of suprapubic catheter
 After care following insertion of suprapubic catheter Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
After care following insertion of suprapubic catheter Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Discharge information for patients Fistula plug for anal fistula
 Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
