Continence and using the toilet
|
|
|
- Arnold Gilbert
- 6 years ago
- Views:
Transcription
1 Continence and using the toilet Factsheet 502LP September 2016 People with dementia can experience difficulties with using the toilet. Accidents and incontinence can also cause problems, particularly as their condition progresses. This can be upsetting for the person and for those around them. However, incontinence is not an inevitable consequence of dementia and support is available. This can be a sensitive topic for many people, but talking about it can help to deal with the problem. This factsheet looks at what causes problems with using the toilet and incontinence, and how they might affect a person with dementia. It gives practical tips to help prevent or manage incontinence, and looks at the professional support available. Contents nn What is incontinence? nnwhy might a person become incontinent? nntips for carers: the importance of maintaining a healthy bladder and bowels nntips for carers: reducing accidents nntips for carers: dealing with an accident nnensuring good personal hygiene nnprofessional support nncontinence aids nnother useful organisations.
2 2 What is incontinence? Incontinence is the involuntary (not on purpose) leakage of urine or faeces, or both, known as double incontinence. Urinary incontinence Urinary incontinence may be a small occasional leak, a trickling after passing urine, or total loss of bladder control. There are several different types of urinary incontinence. Probably the most common form in people with dementia is an overactive bladder. This gives the feeling of a sudden and intense need to go, and frequent urination. Women are also at particular risk of a different type of urinary incontinence called stress incontinence. This is when a cough, sneeze or laugh causes a small leak of urine. Faecal incontinence Faecal incontinence may range from passing a small amount of faeces when breaking wind, to having no bowel control at all. Faecal incontinence is less common than urinary incontinence. It affects men and women about equally. Older people in general have a higher risk of incontinence. In some cases this is because of a medical condition, which may be treatable.
3 3 Why might a person become incontinent? Incontinence in older people Older people in general have a higher risk of incontinence. In some cases this is because of a medical condition, which may be treatable. Medical causes of incontinence, in older people with or without dementia, include: nurinary tract infection (UTI) this is where bacteria get into the urethra (the tube that allows the passage of urine from the bladder to outside the body) and infect the bladder or kidneys. Symptoms can include a sudden urge to urinate, pain or a burning feeling when passing urine, a fever and urinary incontinence. A urinary tract infection can usually be treated with a course of antibiotics nconstipation this is uncomfortable and makes both emptying the bladder and holding on more difficult. Constipation is also a very common cause of faecal incontinence, for example when liquid faeces flow around a hard, impacted stool nprostate gland trouble this condition affects men, and may be treatable nside effects of medication the GP may be able to address this by changing the person s prescription or altering the dose nother gut conditions such as irritable bowel syndrome. Many people feel embarrassed about these problems and this stops them seeking help from health professionals. However, it is important to talk about them with the GP or specialists, as medical causes can often be treated or managed. Incontinence and toilet problems in people with dementia A person with dementia is more likely to have accidents, problems with the toilet or incontinence than a person of the same age who doesn t have dementia.
4 4 The reasons for this can include: nnot being able to react quickly enough to the sensation of needing to use the toilet nfailing to get to the toilet in time for example, because of mobility problems nnot being able to tell someone that they need to go to the toilet because of problems communicating nnot being able to find, recognise, or use the toilet. If someone becomes confused about their surroundings, they may urinate in an inappropriate place (such as a wastepaper basket) because they have mistaken it for a toilet nnot understanding a prompt from someone to use the toilet nnot being able to, or forgetting how to, perform the activities of using the toilet, such as undoing clothing and personal hygiene nnot letting others help with going to the toilet, perhaps due to embarrassment or not understanding an offer of help nnot making any attempt to find the toilet this could be due to depression or lack of motivation, or because the person is distracted nembarrassment after an accident, which the person unsuccessfully tries to deal with. This may lead to wet or soiled clothes or faeces being put out of sight. For example, they may be wrapped up and put at the back of a drawer to be dealt with later, only to be forgotten about. For some people, incontinence develops because messages between the brain and the bladder or bowel don t work properly. This may mean people don t recognise that they have a full bladder or bowel, or have the control needed to empty them. However, this is not a common cause of toilet problems and incontinence in people with dementia. It usually only occurs when the person s dementia is more advanced.
5 5 Tips for carers: the importance of maintaining a healthy bladder and bowels Keeping the urinary tract and bowels healthy is a good first step to preventing toilet problems and incontinence. You can help to make sure the person with dementia is following these tips: ndrink six to eight glasses of fluids each day more if the person has hard stools. Not drinking enough fluids, or not drinking them for long periods of time (for example, to avoid the need to go to the toilet during the night), can cause constipation. neat a balanced diet with at least five daily portions of fruit and vegetables, and enough fibre to ensure regular bowel movement. Fibre can be found in cereals, brown rice and potatoes, for example. nkeep active. Walking every day (if the person is able to) helps with regular bowel movements. ntry to build going to the toilet into the person s daily routine, and allow enough time for the person to empty their bowels. Trying to go a few minutes after a meal often works many people favour going after breakfast. If a health professional has suggested the person with dementia might have an overactive bladder, they will also advise avoiding drinks which may irritate the bladder. This could include replacing tea, coffee, cola or alcohol with water, herbal teas, squash and diluted fruit juices. Women with mild dementia and urinary stress incontinence sometimes learn pelvic floor exercises, with the support of a specialist continence nurse or physiotherapist. These exercises can cure stress incontinence caused by weakness of the pelvic floor muscles due to childbirth or ageing. Constipation If the person with dementia has constipation, laxatives might be able to help. Laxatives are a type of medication designed to relieve constipation and are widely available over the counter. However, they should not be used for more than a week without seeking advice from a GP or pharmacist, as the symptoms may be masking another condition.
6 6 If constipation is the cause of faecal incontinence, it is possible to massage the person s abdomen to relieve the blockage. Specialist continence nurses can train you to use this technique, although being successful will depend on how the person with dementia reacts. It requires the person with dementia to co-operate, and they may not like this sensation. Tips for carers: reducing accidents Help with using the toilet at home The following ideas may help someone to find, recognise and use the toilet more easily. nhelp the person to identify where the toilet is. A sign on the door, including both words and a picture, may help. It needs to be clearly visible, so place it within the person s line of vision and make sure the sign is bright so it s easy to see. You can also help the person to know when the toilet is vacant by leaving the toilet door open when it s not in use. Check the location of mirrors in the bathroom. The person with dementia may confuse their reflection for someone else already in the room, and not go because they think the toilet is occupied. nmake it easier for the person to find their way to the toilet. Move any awkwardly placed furniture and open any doors the person may find hard to open themselves. The room and the route to the toilet should be well lit, especially at night. Movement sensor lights in the bedroom and bathroom can also help at night time. These are available from shops selling independent living aids and equipment, or through an occupational therapist ask the GP or social services. nmake it easier for people with mobility problems to use the toilet. Handrails and a raised toilet seat may help. An occupational therapist can give free advice on these, or you can ask someone at a local independent living shop. n Help the person to identify and use the toilet. A contrasting colour (for example, a black seat on a white base) can make it easier to see. Some men who have poor mobility or balance, or who can no longer direct their penis when urinating, may find it easier to sit rather than stand.
7 7 nchoose clothing with fastenings that will be easier for the person to undo when using the toilet. Trousers with an elasticated waist are often easier than zips. Some people find adaptive clothing with Velcro fastenings easier to use than zips or buttons. nif getting to the toilet becomes too difficult because of mobility problems, an aid such as a commode may be useful. This will require the person to recognise the commode, know how to use it and be willing to use it. PromoCon (see Other useful organisations ) and independent living shops provide information on commodes and other aids. Alternatively, you can ask the occupational therapist, community nurse or social services. nensure the person has privacy in the toilet, but check that they don t have difficulty managing locks. Some people with dementia struggle with this. To avoid the person locking themselves in, disable the locks or check that you can open them quickly from the outside (for example with the edge of a coin). Some of these products are available from Alzheimer s Society s online shop. Go to shop.alzheimers.org.uk Help when out and about Toilet problems and incontinence can make it harder to be out and about. Being more confident and able to cope with accidents is important, because toilet problems can lead to giving up activities or becoming socially isolated. There are several ways to make travelling or being out and about easier for the person with dementia. nplan in advance for example, find out where accessible toilets are. nbe prepared for example, fit a light pad (the kind that attaches to underwear) and carry spare clothing and pads, as well as a bag for soiled items. n Buy a RADAR key. This gives disabled people including people with dementia independent access to thousands of locked public toilets around the country (see Other useful organisations ).
8 8 Remembering to go to the toilet Giving the person with dementia regular reminders about using the toilet is a common way to help reduce accidents. For someone with urinary incontinence, the carer should ask regularly (every two to four hours) whether the person needs the toilet. The person should also be given encouragement and assistance if they ask for help. It is important to check that they have used the toilet, and not forgotten or become distracted. There is evidence that, over time, this can help some people reduce the number of accidents they have. You should be sensitive when prompting the person to use the toilet, to avoid patronising, annoying or upsetting them. Watch discreetly for signs that the person wants to go to the toilet, especially if they cannot communicate this clearly. These signs may include fidgeting, pacing, getting up and down, or pulling at their clothes. Developing a routine For someone who regularly wets themselves, it may be helpful to develop a timetable that offers a reminder for going to the toilet. For example, the timetable could list when the person wakes up, before each meal, at coffee or tea times, and before bed. An automatic reminder for example, on a smart phone can also be useful in prompting a person to use the toilet or to check if their pad needs changing. For faecal incontinence, it is often possible to make the person continent again by going to the toilet at a set time each day, and helping them to stay long enough to have a bowel movement. At night-time Many older people wake during the night to urinate. A person with dementia may wake disorientated and be unable to act quickly enough to find (or get to) the toilet. Ideas that might help include: nmotion sensors for lights or night lights in the bedroom, hallways and bathroom n a urinal bottle (designed for men and women) or commode next to the bed at night
9 9 nnot drinking anything for two hours before going to bed but ensuring that the person drinks enough during the day to avoid becoming dehydrated. Tips for carers: dealing with an accident Hygiene and going to the toilet are very personal and private issues, and having difficulties or being incontinent can make someone feel like they are losing control. This can affect their dignity as well as their self-esteem. Many people find it very hard to accept that they need help from someone else in such an intimate area of their life. It can be particularly difficult if the help is from someone very close to them. Every individual will react differently to the experience of incontinence. Some people find it very upsetting, while others find it easier to accept. Approaching the problem with understanding, a matter-of-fact attitude and humour, if it feels appropriate, can help to improve the situation for everyone concerned. If someone has an accident, it is important for carers and friends to: nremember that it s not the person s fault ntry to overcome any embarrassment or upset they may feel navoid appearing angry or upset. This may not always be easy. If you find feelings about incontinence difficult to handle, it is a good idea to talk things through with a health professional. This could be the GP, a community nurse or a continence adviser (a nurse with specialist training in management of incontinence). It is important to try not to let dealing with incontinence get in the way of your relationship with the person you are caring for.
10 10 Ensuring good personal hygiene Incontinence can lead to skin irritation and a general feeling of discomfort. After an accident, it is important to act quickly to make sure the person feels comfortable again, and to ensure they maintain a good level of hygiene. nif someone has become wet or soiled, they should wash afterwards with mild soap and warm water, and dry carefully before putting on clean clothes and fresh pads, with assistance if necessary. nsoiled clothes, reusable pads or bedding should be washed immediately, or soaked in an airtight container until they are washed. nused pads should be stored in an appropriate container and disposed of as soon as possible. nmoist toilet tissues may be suitable for minor accidents, but be aware that some can irritate the skin. Professional support It can be hard to seek professional help for incontinence. Many people do so only at a point of crisis, as it may feel to the person with dementia like they are losing their dignity. Some may see incontinence as inevitable, but for many people with dementia, given the right advice and patience, accidents and incontinence can be managed or sometimes even cured. The GP should be the first point of contact. They should review the symptoms and any underlying medical conditions (eg urinary tract infection or constipation), diet or medications that might be causing the problems. The doctor may do an internal examination of the bowel. If this assessment is unable to resolve the problem, ask for the person to be referred to a continence adviser. NHS continence services across the country are quite variable and you may have to be persistent to see someone who understands incontinence in people with dementia. You may have to wait for these services. The continence adviser will assess the person s problems and how they are affecting their quality of life, as well as yours. It is common to be asked to keep a chart of toilet habits.
11 11 After a thorough assessment the continence adviser will write up a continence care plan tailored to the individual. This should include things that the person with dementia and any carer can do to help. It should also describe the support that professionals should provide, as well as followup and next steps. The aim should be to cure toilet problems or incontinence wherever possible. This should be agreed with the person with dementia and their carer. In many cases, identifying and addressing practical issues, changing medications or making simple changes to lifestyle (such as diet, drinks and exercise) can help to achieve this. In a few cases, the person may need to be referred to a further specialist (eg geriatrician, urologist or gynaecologist). For some people, advice will focus not on curing but rather on containing the incontinence as comfortably as possible using aids (see Incontinence aids below). Other health professionals can visit the person at home and offer support. na community nurse can help with access to NHS-funded continence products and give advice on management of the problems, hygiene and how to protect the skin. nan occupational therapist can give advice on adaptations and equipment. na physiotherapist can give advice if the person has problems with coordination or movement. na community psychiatric nurse, Admiral Nurse or the community mental health team can help if behavioural changes are affecting how someone uses the toilet. Speak to the GP about getting a referral to any of these professionals.
12 12 Continence aids Sometimes, you might try everything you can but the toilet problems or incontinence don t go away. In this case, using continence aids can help to keep the person comfortable and protect clothing, furniture and bedding. The main aids are listed below. nincontinence pads and pull-up pants. These can be worn day and night, or during the night only, to draw fluids away from the skin. It is important to find the right type and absorbency for the individual. They should be comfortable without chafing the skin or leaking. They should be changed as often as necessary. nmale continence sheath. This is a silicone condom which drains into a bag attached to the leg. It may be especially helpful when worn at night. nabsorbent bed pad. This is an under-sheet which provides a dry surface on a bed or a chair. These are available as washable or disposable products. nwaterproof mattress protector. This is often used in combination with an absorbent bed pad. The protector should not come into contact with the skin, as it may cause chafing and soreness. You can also buy special protective duvet covers and pillowcases. You should talk to the continence adviser or community nurse for advice, or to find out how to get NHS-funded supplies. The NHS should supply enough continence products to meet a person s needs. However, this varies across the country, and many people top up supplies or buy different versions of products independently with their own money. You can get advice and buy products from independent living shops or large branches of highstreet chemists. For national organisations that can help, see Other useful organisations below.
13 13 Other useful organisations Continence Product Advisor Website that gives impartial advice on continence products, written by healthcare professionals. Disability Rights UK Ground Floor CAN Mezzanine East Road London N1 6AH (not an advice line) Disability Rights UK sells the RADAR National Key Scheme, which offers disabled people independent access to locked public toilets around the country. Toilets fitted with National Key Scheme locks can now be found in shopping centres, pubs, cafés, department stores, bus and train stations and many other locations in most parts of the country. PromoCon Disabled Living Burrows House 10 Priestley Road Wardley Industrial Estate Worsley Manchester M28 2LY (Helpline, 9am 4pm, Tuesday Friday) Provides a national service to improve life for all people with bladder or bowel problems by offering product information, advice and practical solutions to professionals and the general public.
14 Factsheet 502LP Last reviewed June 2013 by Professor Vari Drennan, Faculty of Health and Social Care Sciences, Kingston University and St George s University of London and Dr Ann Capewell, Consultant Physician, St Helens and Knowsley Teaching Hospitals NHS Trust, Merseyside Last reviewed September 2016 by Alzheimer s Society Next review due: September 2019 This factsheet has also been reviewed by people affected by dementia. Alzheimer s Society National Dementia Helpline England, Wales and Northern Ireland: am 8pm Monday Wednesday 9am 5pm Thursday Friday 10am 4pm Saturday Sunday This publication contains information and general advice. It should not be used as a substitute for personalised advice from a qualified professional. Alzheimer s Society does not accept any liability arising from its use We strive to ensure that the content is accurate and up to date, but information can change over time. Please refer to our website for the latest version and for full terms and conditions. Alzheimer s Society, All rights reserved. Except for personal use, no part of this work may be distributed, reproduced, downloaded, transmitted or stored in any form without the written permission of Alzheimer s Society. alzheimers.org.uk Alzheimer s Society is the UK s leading dementia charity. We provide information and support, improve care, fund research, and create lasting change for people affected by dementia. Alzheimer s Society operates in England, Wales and Northern Ireland. Registered charity number
Coping with incontinence
 Coping with incontinence Incontinence can be upsetting and humiliating for the person with dementia and stressful for the carer. But approaching the problem with understanding, matter-of-factness and humour
Coping with incontinence Incontinence can be upsetting and humiliating for the person with dementia and stressful for the carer. But approaching the problem with understanding, matter-of-factness and humour
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
A word about incontinence
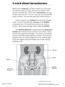 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
WHAT TYPES OF CONTINENCE PRODUCTS ARE THERE?
 15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment
 Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Please read the following information and have the child follow the bladder retraining protocol included.
 Urology Clinic Hospital for Sick Children Please read the following information and have the child follow the bladder retraining protocol included. Information on bladder retraining, urinary tract infections
Urology Clinic Hospital for Sick Children Please read the following information and have the child follow the bladder retraining protocol included. Information on bladder retraining, urinary tract infections
University College Hospital at Westmoreland Street. Urinary sheaths. Urology Directorate
 University College Hospital at Westmoreland Street Urinary sheaths Urology Directorate If you would like this document in another language or format, or require the services of an interpreter, contact
University College Hospital at Westmoreland Street Urinary sheaths Urology Directorate If you would like this document in another language or format, or require the services of an interpreter, contact
Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises
 MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
My Urinary Catheter Passport Looking after my urinary catheter
 Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
Coping with memory loss
 alzheimers.org.uk Coping with memory loss Memory loss is a distressing part of dementia, both for the person with dementia and for those around them. However, there is plenty that can be done to help manage
alzheimers.org.uk Coping with memory loss Memory loss is a distressing part of dementia, both for the person with dementia and for those around them. However, there is plenty that can be done to help manage
Urinary tract infections (UTIs) and dementia
 Urinary tract infections (UTIs) and dementia Factsheet 528LP April 2015 Urinary tract infections (UTIs) are a type of infection that are common among older people. Women are more commonly affected by them
Urinary tract infections (UTIs) and dementia Factsheet 528LP April 2015 Urinary tract infections (UTIs) are a type of infection that are common among older people. Women are more commonly affected by them
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS
 Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
For details on how to order other Age UK Factsheets and information materials go to section 8.
 Factsheet 23 January 2011 Help with continence About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or
Factsheet 23 January 2011 Help with continence About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Pelvic floor exercises for men
 Information for men This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. Your GP or healthcare professional has advised
Information for men This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. Your GP or healthcare professional has advised
Discussions about having a Supra pubic catheter
 Discussions about having a Supra pubic catheter What is a supra pubic catheter? A supra pubic catheter is used to drain urine from the bladder by inserting a catheter (narrow hollow drainage tube) directly
Discussions about having a Supra pubic catheter What is a supra pubic catheter? A supra pubic catheter is used to drain urine from the bladder by inserting a catheter (narrow hollow drainage tube) directly
Your catheter. Information for patients and carers. NHS Grampian Continence Service
 Your catheter Information for patients and carers NHS Grampian Continence Service Healthcare professional details Name: Contact number:. GP: Telephone number: Reason for catheterisation:... Date of initial
Your catheter Information for patients and carers NHS Grampian Continence Service Healthcare professional details Name: Contact number:. GP: Telephone number: Reason for catheterisation:... Date of initial
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
CATHETER PASSPORT. Looking after your Urinary Catheter. The Catheter Passport should be given to all patients with a urinary catheter.
 CATHETER PASSPORT Looking after your Urinary Catheter The Catheter Passport should be given to all patients with a urinary catheter. Health care staff should ensure that page 10 is completed. This document
CATHETER PASSPORT Looking after your Urinary Catheter The Catheter Passport should be given to all patients with a urinary catheter. Health care staff should ensure that page 10 is completed. This document
Pelvic Floor Exercises
 Pelvic Floor Exercises Information for service users and carers RDaSH leading the way with care Pelvic Floor Muscles The pelvic floor muscles are a sling of muscles across the floor of the pelvis. The
Pelvic Floor Exercises Information for service users and carers RDaSH leading the way with care Pelvic Floor Muscles The pelvic floor muscles are a sling of muscles across the floor of the pelvis. The
Continence problems after stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Continence problems after stroke It is common for people to have problems controlling their bladder and/or bowels after a stroke. Though initially
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Continence problems after stroke It is common for people to have problems controlling their bladder and/or bowels after a stroke. Though initially
Worried about your memory?
 Worried about your memory? Find out more about memory problems and what you can do next alzheimers.org.uk Worried about memory problems? Everybody forgets things from time to time. But if you or other
Worried about your memory? Find out more about memory problems and what you can do next alzheimers.org.uk Worried about memory problems? Everybody forgets things from time to time. But if you or other
Continence problems after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Continence problems after stroke This guide explains some of the bladder and bowel problems that may happen after stroke. It also looks
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Continence problems after stroke This guide explains some of the bladder and bowel problems that may happen after stroke. It also looks
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Patient Urinary Catheter Passport
 Useful contact details Name Contact Number Produced by Adapted from Worth by Michelle Pickering, Continence Specialist Practitioner Hambleton and Richmondshire Locality Continence Advisory Service and
Useful contact details Name Contact Number Produced by Adapted from Worth by Michelle Pickering, Continence Specialist Practitioner Hambleton and Richmondshire Locality Continence Advisory Service and
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries
 Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy - Woman s Health Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. 2 Introduction Physiotherapists, doctors and nurses know that exercising
Pelvic Floor Exercises Physiotherapy - Woman s Health Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. 2 Introduction Physiotherapists, doctors and nurses know that exercising
Keep high, stay dry. Pelvic floor exercises for men
 Keep high, stay dry Pelvic floor exercises for men What is the pelvic floor? Layers of muscle stretch like a hammock from your pubic bone in the front to the bottom of your backbone (see diagram). These
Keep high, stay dry Pelvic floor exercises for men What is the pelvic floor? Layers of muscle stretch like a hammock from your pubic bone in the front to the bottom of your backbone (see diagram). These
Pelvic floor muscle exercises
 Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Advice for Parents and Carers
 Advice for Parents and Carers 1 2 CONTENTS 4. What is constipation? 4. What is faecal impaction? 5. How common is constipation in children? 5. How to tell if your child may be constipated 6. How constipation
Advice for Parents and Carers 1 2 CONTENTS 4. What is constipation? 4. What is faecal impaction? 5. How common is constipation in children? 5. How to tell if your child may be constipated 6. How constipation
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Drinking fluids and how they affect your bladder
 www.olarts.com Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS.
www.olarts.com Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS.
Urinary Catheter Passport
 Urinary Catheter Passport Catheter Change Record and Looking After Your Urinary Catheter Please take this booklet with you if you are admitted to hospital or have an appointment Patient details Name Address
Urinary Catheter Passport Catheter Change Record and Looking After Your Urinary Catheter Please take this booklet with you if you are admitted to hospital or have an appointment Patient details Name Address
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Indwelling urinary catheter
 Indwelling urinary catheter Information for patients and carers RDaSH leading the way with care What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder. Following
Indwelling urinary catheter Information for patients and carers RDaSH leading the way with care What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder. Following
Driving. Living with dementia series
 Driving Living with dementia series B For more information visit alzheimers.org.uk Driving If you drive, you may need to make some changes after getting a diagnosis of dementia. You may still be able to
Driving Living with dementia series B For more information visit alzheimers.org.uk Driving If you drive, you may need to make some changes after getting a diagnosis of dementia. You may still be able to
opyright 2017 SAMPLE COPY Property of Hayward Bell Ltd Copyright 2017 Bladder and bowel conditions can affect anyone
 Bladder and bowel conditions can affect anyone This booklet could be your first positive step to a full and active life Contents 1. Introduction 2. A bladder 3. The most common problems 5. A bowel 6. Functional
Bladder and bowel conditions can affect anyone This booklet could be your first positive step to a full and active life Contents 1. Introduction 2. A bladder 3. The most common problems 5. A bowel 6. Functional
Working together to prevent falls
 Quality Care - for you, with you Working together to prevent falls Introduction Falling is a common problem throughout our lifetime but as we get older the risk of injury from falls unfortunately gets
Quality Care - for you, with you Working together to prevent falls Introduction Falling is a common problem throughout our lifetime but as we get older the risk of injury from falls unfortunately gets
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Patient Urinary Catheter Passport
 Useful contact details: Continence Service (Community) 01724 298325 Continence Service (Goole) 01482 336951 Continence Service (SGH) 01724 282282 Ext 2823 Continence Service (DPOW) 01472 874111 Infection
Useful contact details: Continence Service (Community) 01724 298325 Continence Service (Goole) 01482 336951 Continence Service (SGH) 01724 282282 Ext 2823 Continence Service (DPOW) 01472 874111 Infection
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
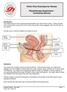 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
Help with continence. Factsheet 23 March About this factsheet
 Factsheet 23 March 2014 About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or manage incontinence and
Factsheet 23 March 2014 About this factsheet This factsheet briefly outlines the different types of incontinence. It also explains how to access NHS services that can help cure or manage incontinence and
Non-gonococcal urethritis. Looking after your sexual health
 Non-gonococcal urethritis Looking after your sexual health 2 3 Non-gonococcal urethritis Urethritis is inflammation (pain, redness or soreness) of the urethra (the tube that carries urine out of the body).
Non-gonococcal urethritis Looking after your sexual health 2 3 Non-gonococcal urethritis Urethritis is inflammation (pain, redness or soreness) of the urethra (the tube that carries urine out of the body).
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
HELPING SCHOOLS MANAGE CONTINENCE PROBLEMS. The Right to
 HELPING SCHOOLS MANAGE CONTINENCE PROBLEMS The Right to Go Continence problems in childhood are common and as a result it is not unusual for schools to have at least one child with a wetting or soiling
HELPING SCHOOLS MANAGE CONTINENCE PROBLEMS The Right to Go Continence problems in childhood are common and as a result it is not unusual for schools to have at least one child with a wetting or soiling
Indwelling Urinary Catheters And Drainage systems
 If you require this leaflet in any other format, e.g., large print, please telephone 01935 384256 Indwelling Urinary Catheters And Drainage systems Useful organisations Ms Society Helpline Tel: 0808 800
If you require this leaflet in any other format, e.g., large print, please telephone 01935 384256 Indwelling Urinary Catheters And Drainage systems Useful organisations Ms Society Helpline Tel: 0808 800
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
Keeping control What you should expect from your NHS bladder and bowel service
 Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Preventing Pressure Ulcers
 Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Drugs used to relieve behavioural and psychological symptoms in dementia
 alzheimers.org.uk Drugs used to relieve behavioural and psychological symptoms in dementia People with dementia may develop behavioural and psychological symptoms including restlessness, aggression, delusions,
alzheimers.org.uk Drugs used to relieve behavioural and psychological symptoms in dementia People with dementia may develop behavioural and psychological symptoms including restlessness, aggression, delusions,
ONE IN THREE WOMEN WHO EVER HAD A BABY WET THEMSELVES EVERY WOMAN WHO HAS HAD A BABY SHOULD DO PELVIC FLOOR MUSCLE TRAINING.
 08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
AgePage. Urinary Incontinence
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
Urinary Catheter Passport for patients
 Urinary Catheter Passport for patients Nursing A guide for patients and visitors Contents Why people need a urinary catheter...1 How your bladder and kidneys work...1 What is a catheter?...3 Drainage bags...3
Urinary Catheter Passport for patients Nursing A guide for patients and visitors Contents Why people need a urinary catheter...1 How your bladder and kidneys work...1 What is a catheter?...3 Drainage bags...3
Delaware Valley Geriatric Education Center 1
 Welcome to the second of our two modules, Continence: A Matter of Dignity, Care of Chronic and Complex UI. We are here today to discuss a topic which, every day, affects our jobs and lives of those we
Welcome to the second of our two modules, Continence: A Matter of Dignity, Care of Chronic and Complex UI. We are here today to discuss a topic which, every day, affects our jobs and lives of those we
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Continence and prostate
 Continence and prostate A guide for men undergoing prostate surgery p r o m o t i n g b l a d d e r a n d b o w e l h e a lt h Continence Foundation of Australia, 2012 This book is copyright. Apart from
Continence and prostate A guide for men undergoing prostate surgery p r o m o t i n g b l a d d e r a n d b o w e l h e a lt h Continence Foundation of Australia, 2012 This book is copyright. Apart from
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
AgePage. Urinary Incontinence
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
Information about your Urodynamics Test
 Gynaecology Department Patient Information Information about your Urodynamics Test This information booklet has been given to you to help answer some of the questions you may have about having an urodynamic
Gynaecology Department Patient Information Information about your Urodynamics Test This information booklet has been given to you to help answer some of the questions you may have about having an urodynamic
Mouth care for people with dementia. Good habits for bedtime. Caring for someone with dementia
 Mouth care for people with dementia Good habits for bedtime Caring for someone with dementia 2 Dementia UK Looking after someone with dementia Caring for someone with dementia can be really difficult at
Mouth care for people with dementia Good habits for bedtime Caring for someone with dementia 2 Dementia UK Looking after someone with dementia Caring for someone with dementia can be really difficult at
Drug treatments for Alzheimer s disease
 Drug treatments for Alzheimer s disease Factsheet 407LP April 2018 There are no drug treatments that can cure Alzheimer s disease or any other common type of dementia. However, there are medicines for
Drug treatments for Alzheimer s disease Factsheet 407LP April 2018 There are no drug treatments that can cure Alzheimer s disease or any other common type of dementia. However, there are medicines for
Urine problems in men
 Fact sheet No.14 Easy Read Urine problems in men This fact sheet helps you to know what s normal and what you can expect to happen if a man gets a problem with their wee. Urine is another word for wee
Fact sheet No.14 Easy Read Urine problems in men This fact sheet helps you to know what s normal and what you can expect to happen if a man gets a problem with their wee. Urine is another word for wee
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Coping with urges and leaks?
 OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
Mouth care for people with dementia. Delirium (Confusion) Understanding changes in behaviour in dementia
 Mouth care for people with dementia Delirium (Confusion) Understanding changes in behaviour in dementia 2 Dementia UK Delirium (confusion) A sudden change in a person s mental state is known as delirium.
Mouth care for people with dementia Delirium (Confusion) Understanding changes in behaviour in dementia 2 Dementia UK Delirium (confusion) A sudden change in a person s mental state is known as delirium.
Urinary Incontinence. a problem for many
 Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Caring for a person with a stoma and dementia
 Caring for a person with a stoma and dementia www.colostomyuk.org Freephone helpline: 0800 328 4257 Caring for a person with a stoma and dementia Colostomy UK We are Colostomy UK. Here if you have questions,
Caring for a person with a stoma and dementia www.colostomyuk.org Freephone helpline: 0800 328 4257 Caring for a person with a stoma and dementia Colostomy UK We are Colostomy UK. Here if you have questions,
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire
 Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
PELVIC FLOOR MUSCLE TRAINING FOR WOMEN STRONG PELVIC FLOOR MUSCLES MEAN GOOD BLADDER AND BOWEL CONTROL WHAT ARE THE PELVIC FLOOR MUSCLES?
 06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
Mouth care for people with dementia. Mouth care for people with dementia. Staying well with dementia
 Mouth care for people with dementia Mouth care for people with dementia Staying well with dementia 2 Dementia UK Mouth care for people with dementia Maintaining good oral health is essential to your overall
Mouth care for people with dementia Mouth care for people with dementia Staying well with dementia 2 Dementia UK Mouth care for people with dementia Maintaining good oral health is essential to your overall
EXERCISE and ADVICE. after pregnancy
 EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
DEMENTIA INFORMATION FOR YOU AND YOUR FAMILY
 DEMENTIA INFORMATION FOR YOU AND YOUR FAMILY When you or a member of your family is diagnosed with dementia it is natural to feel anxious and to worry about what the future may hold. This booklet will
DEMENTIA INFORMATION FOR YOU AND YOUR FAMILY When you or a member of your family is diagnosed with dementia it is natural to feel anxious and to worry about what the future may hold. This booklet will
Bowel health and screening: carers guide. A booklet for carers of people who use easy read materials
 Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Continence in MSA. How the bladder works
 How the bladder works What goes wrong? What investigations need to be done? Who can help? Advice Medication Equipment Other help Useful contacts Continence in MSA Bladder problems are very common in people
How the bladder works What goes wrong? What investigations need to be done? Who can help? Advice Medication Equipment Other help Useful contacts Continence in MSA Bladder problems are very common in people
Bladder and Bowel Symptoms Troubleshooting Tips
 Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Trans Urethral Resection of Prostate (TURP)
 Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Trans Urethral Resection of Prostate (TURP) Patient Information Author ID: SF Leaflet Number: Urol 010 Version: 6 Name of Leaflet: Trans Urethral Resection of Prostate (TURP) Date Produced: March 2018
Women and Men s Health Physiotherapy Pelvic floor exercises for men
 James Paget University Hospitals NHS Foundation Trust Women and Men s Health Physiotherapy Pelvic floor exercises for men Patient Information Pelvic floor exercises for men Your pelvic floor muscles help
James Paget University Hospitals NHS Foundation Trust Women and Men s Health Physiotherapy Pelvic floor exercises for men Patient Information Pelvic floor exercises for men Your pelvic floor muscles help
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Urinary Incontinence? - gør dig ikke skakmat...
 Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Spasticity triggers What to do if you have a worsening of your muscle stiffness and/or spasms
 Spasticity triggers What to do if you have a worsening of your muscle stiffness and/or spasms Jane Lough Paula Cowan We hope you find the information in this book helpful. If you would like to speak with
Spasticity triggers What to do if you have a worsening of your muscle stiffness and/or spasms Jane Lough Paula Cowan We hope you find the information in this book helpful. If you would like to speak with
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Bulkamid. Patient Information. Obstetrics & Gynaecology Department
 Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
risk factors for falling
 Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Pelvic Floor Exercises
 Pelvic Floor Exercises Information for patients, relatives and carers For more information, please contact: Women s Health Physiotherapy Department The York Hospital Wigginton Road, York, YO31 8HE Tel:
Pelvic Floor Exercises Information for patients, relatives and carers For more information, please contact: Women s Health Physiotherapy Department The York Hospital Wigginton Road, York, YO31 8HE Tel:
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
