Lydia Cheung RN BSN MSN KCC Spinal Cord Rehabilitation Centre 2014/2/22 1
|
|
|
- Godfrey Morton
- 5 years ago
- Views:
Transcription
1 Lydia Cheung RN BSN MSN KCC Spinal Cord Rehabilitation Centre 2014/2/22 1
2 Reference with acknowledgment Guidelines for Management of Neurogenic Bowel Dysfunction after Spinal Cord Injury Produced by the Spinal Cord Injury Centres of the United Kingdom and Ireland Initiated by Multidisciplinary Association of Spinal Cord Injury Professionals Supported by an educational grant from Coloplast Ltd 2014/2/22 2
3 Neurogenic Bowel Dysfunction Upper motor neuron dysfunction causes constipation with slow colonic transit and stool retention due to spasticity. Reflexes allowing defecation may remain intact. Cauda equina causes lower motor neuron dysfunction causing constipation with slow colonic transport and incontinence due to a flaccid sphincter. 2014/2/22 3
4 Motor Function 2014/2/22 4
5 Sensory Function If sensation is present in the saddle area around the perineum, the individual is likely to have anorectal sensation. If sensation is present digital interventions may be uncomfortable; rectal stimulants (suppositories, enemas) may cause less discomfort. Local anaesthetic gel can be introduced into the rectum prior to bowel care to increase tolerance if needed. 2014/2/22 5
6 Outline bowel management programmes 2014/2/22 6
7 Aim of effective bowel management It is fundamental to the rehabilitation process, but more importantly, It is fundamental to the successful reintegration of the SCI individual back into the community. Faecal incontinence has a major impact on quality of life. This plan will be the result of a multidisciplinary assessment, and will be negotiated with the patient and relevant third parties. 2014/2/22 7
8 Objectives of bowel management To optimise comfort, safety, privacy and dignity To establish individualised bowel management routine To avoid incontinence, constipation, diarrhoea and autonomic dysreflexia To avoid / minimise the development of secondary ano-rectal complications associated with bowel management (rectal over-distension, haemorrhoids, anal fissure etc) To have identified the minimum necessary physical and pharmacological interventions required by the individual for satisfactory bowel management prior to discharge from initial rehabilitation To work with other members of the multidisciplinary team, identify appropriate transfer methods, equipment and adaptive devices to promote independence in bowel management for the individual To evaluate the outcomes of bowel management. The Bristol Scale (Heaton 1992) will be used to record stool form. Duration of bowel management episodes and any unplanned bowel evacuations should be recorded Through effective education, to provide the individual with a toolkit of knowledge with which they can manage and adapt their bowel care in the long-term 2014/2/22 8
9 Evaluating bowel care Outcome measures for evaluating bowel management are: Duration of management episodes Stool form recorded Frequency of episodes of incontinence Have pharmacological interventions been minimised as far as possible? Is the patient as independent as possible? Feedback from the patient regarding satisfaction and perceived autonomy 2014/2/22 9
10 Frequency of re-evaluation during initial rehabilitation On cessation of spinal shock On mobilisation When the patient is ready to begin bowel management on the toilet If a patient changes to oral intake from nasogastric/gastrostomy feeding At any time where it seems appropriate but at least fortnightly throughout admission 2014/2/22 10
11 The Bristol Stool Scale The Bristol Stool Scale was developed in the United Kingdom by a small team of gastroenterologists at the University of Bristol. It is designed to be a representative explanation for stools commonly seen in toilet water. In the different categories, the chart explains the correlation between the stool's physical attributes and the length of time the stool remained in the colon. This scale is useful to anyone who would like to determine the condition of their colon because it is a generic indicator; it is not an absolute diagnostic tool. It is, however, a good indicator of what action you may need to take. Below are the chart and the analysis for your use at home. Lewis SJ, Heaton KW (1997). "Stool form scale as a useful guide to intestinal transit time". Scand. J. Gastroenterol. 32 (9): /2/22 11
12 2014/2/22 12
13 2014/2/22 13
14 2014/2/22 14
15 The bowel management programme The bowel management programme will specify the following: Specific interventions to be used The frequency (twice daily, daily, alternate day) and timing (morning, evening) of the bowel programme The location for bowel management (bed, toilet etc) Who will perform bowel care (the patient, a specific relative, care staff, community nurse) Equipment and adaptations required (shower chair, padded toilet seat etc) A recognized generic or Trust-specific manual handling risk assessment 2014/2/22 15
16 The development of the bowel management programme will be informed by consideration of the following factors: Level and density of spinal cord injury Type of neurogenic bowel dysfunction Evaluation of bowel care during the acute stage Mobility of the individual Limiting factors such as spasticity and poor balance Self-care abilities of the patient Patient preferences where feasible Age of the patient Weight of the patient Cultural requirements Domestic circumstances 2014/2/22 16
17 The development of the bowel management programme will be informed by consideration of the following factors: Availability of carers Availability of bowel care aids and equipment Accessibility and suitability of facilities at discharge destination Any pre- or post-injury bowel related complications Pre-injury bowel habit Relevant medical history Prevention of dysreflexia in susceptible patients Supervision requirements (is it safe to leave the patient during bowel management episodes?) Planned future family commitments, employment or education Other lifestyle considerations (Ash 2005, Weeks 2000, Coggrave 2004, 2005 & Slater 2003) 2014/2/22 17
18 Reflex bowel management Bowel evacuation in reflex neurogenic bowel dysfunction can be produced by the use of chemical rectal stimulants and digital rectal stimulation (Shafik et al 2000), or a combination of both (Coggrave et al 2008), but often must be followed by digital removal of faeces (DRF) to ensure complete evacuation (Coggrave et al 2008, Haas et al 2006). The optimal combination should be developed on an individual basis. 2014/2/22 18
19 Reflex bowel management The aim is to produce effective evacuation (i.e. avoiding faecal incontinence or constipation) within a reasonable duration, suggested to be one hour (Consortium for Spinal Cord Medicine 1998). Manipulating stool consistency through diet, fluids and if necessary, medication to achieve Bristol Scale 4 produces the optimal stool for effective reflex bowel function. 2014/2/22 19
20 Reflex bowel management Establishing a regular pattern for bowel care helps to ensure that stool is present in the rectum and sigmoid colon ready for evacuation at the chosen time. This can be assisted if required by the use of stimulant laxatives as part of a discrete bowel management episode. 2014/2/22 20
21 2014/2/22 21
22 Areflexic bowel management As there are no preserved anorectal reflexes, pharmacological or digital stimulation of the anorectum are not effective. Digital removal of faeces is the basic physical intervention in areflexic neurogenic bowel dysfunction. Use of straining/valsalva manoeuvre without digital removal of faeces is the cultural norm in some countries, but is associated with a high degree of incontinence, constipation and other difficulties with evacuation and development of haemorrhoids and prolapse (Yim, 2001) and should be discouraged. 2014/2/22 22
23 Areflexic bowel management To facilitate digital removal of faeces, and to reduce the risk of stress incontinence due to the areflexic, relaxed anal sphincters, individuals are recommended to aim for a firm stool (Bristol Stool type 2-3) (Ash et al 2006, Consortium for Spinal Cord Medicine 1998). 2014/2/22 23
24 2014/2/22 24
25 2014/2/22 25
26 Establishing a routine Establishing a regular routine is fundamental to gaining control over continence and avoiding the build up of stool in the colon. The frequency with which the programme is conducted will vary depending on the needs of the individual; those with flaccid bowel function may manage their bowel daily or twice daily (sometimes more) while individuals with reflex bowel function may evacuate their bowel on a daily or alternate day routine (Coggrave et al 2008). Less frequent or irregular bowel management may contribute to constipation (Coggrave et al 2008). However, overly strict adherence to a rigid bowel routine is associated with increased impact on quality of life (Coggrave et al 2008) and the capacity for flexibility should be maintained where possible. 2014/2/22 26
27 Manipulating diet to alter stool consistency 2014/2/22 27
28 Diet More than 50% of SCI individuals report they manipulate their diet (Coggrave et al 2008) to assist their bowel management even though there is no robust evidence to support any dietary intervention. Hence in this population it is generally advised that a diet containing five portions of fruit and vegetables and significant levels of whole grain foods, such as wholemeal bread or unrefined cereals, each day should be encouraged, in accordance with the government 5 a day strategy (Department of Health 2003). Stool consistency can then be assessed and the diet adjusted accordingly to achieve an appropriate stool consistency. Individuals with reflex bowel function are encouraged to aim for a soft-formed stool consistency (Bristol Scale 4 see Glossary (Heaton et al 1992)), while those with flaccid bowel function are more likely to avoid faecal incontinence if they aim for firmer stools (Bristol Scale 2-3 see Glossary (Heaton et al 1992)). Digital removal of faeces is also facilitated by a firmer consistency. 2014/2/22 28
29 Dietary factors that may affect stool consistency Dietary fibre is the main food component that is likely to need altering when adjustment to stool consistency is required. Current guidelines are for an average daily dietary fibre intake of 18g. This should be aimed for but when there are problems with stool consistency there may need to be adjustments to the amount consumed. 2014/2/22 29
30 2014/2/22 30
31 Enteral tube feeding As with patients who are on normal diets, those on enteral tube feeds will be able to tolerate differing levels of fibre contained in enteral feeds. Anecdotal experience among dieticians working in the spinal injuries centres has suggested that it is preferable to start with a feed that does not contain fibre, especially in a newly injured patient. The quantity of fibre can then be increased as tolerated along similar lines to those who are taking oral diet. 2014/2/22 31
32 Fluids With regard to fluid intake, it has been suggested that 500 mls per day for the SCI individual should be added to the recommended fluid intake for healthy able-bodied individuals (Consortium for Spinal Cord Medicine 1998). However, there is no research evidence to support this with regard to bowel management, and fluid intake may be determined by specific bladder management approaches. The British Dietetic Association recommends between 1.5L and 2.5L of fluid daily for the general adult population, depending on level of activity and prevailing weather conditions (BDA 2006). Urine colour is correlated with the concentration of urine; urine of a pale straw colour indicates adequate hydration (BDA 2006), and is a simple rule of thumb which is useful to patients. 2014/2/22 32
33 Digital rectal stimulation Explain the procedure to the patient (if necessary) and obtain consent. Even if the patient consents to the procedure, if they request you to stop at any time, you must do so. The patient should be invited to have an escort present if they wish Ensure a private environment Observe the patient throughout the procedure for signs of autonomic dysreflexia or other adverse events (Addison and Smith 2000) If the patient s spinal injury is stable, position the patient in a lateral position (usually left side) with knees flexed. Flexing the knees promotes the stability of the patient and helps to expose the anus (Campbell 1993). If the spinal injury is unstable bowel management will be conducted during a team log roll, maintaining spinal alignment at all times. 2014/2/22 33
34 Digital rectal stimulation This procedure may also be conducted over the toilet/commode by the patient or the carer Place protective pad under the patient if appropriate Wash hands, put on two pairs of disposable gloves and an apron local anaesthetic gel may be instilled into the rectum prior to the procedure (Furasawa 2008, Cosman 2005). This requires 5-10 minutes to take effect and lasts up to 90 minutes. Note that long term use should be avoided due to systemic effects (BNF 2008) Lubricate gloved finger with water soluble gel Inform patient you are about to begin Insert single gloved, lubricated finger (Addison and Smith 2000) slowly and gently into rectum 2014/2/22 34
35 Digital rectal stimulation Turn the finger so that the padded inferior surface is in contact with the bowel wall Rotate the finger in a clockwise direction for at least 10 seconds, maintaining contact with the bowel wall throughout Withdraw the finger and await reflex evacuation Repeat every 5-10 minutes until rectum is empty or reflex activity ceases Remove soiled glove and replace, re-lubricating as necessary between insertions If no reflex activity occurs during the procedure, do not repeat it more than 3 times. Use digital removal of faeces (DRF) if stool is present in the rectum During the procedure the person delivering care may carry out abdominal massage 2014/2/22 35
36 Digital rectal stimulation Once the rectum is empty on examination, conduct a final digital check of the rectum after 5 minutes to ensure that evacuation is complete Place faecal matter in an appropriate receptacle as it is removed, and dispose of it and any other waste in a suitable clinical waste bag When the procedure is completed, wash and dry the patient s buttocks and anal area and position comfortably before leaving Remove gloves and apron and wash hands Record outcomes, record and report abnormalities 2014/2/22 36
37 Digital removal of faeces Explain the procedure to the patient (if necessary) and obtain consent. Even if the patient consents to the procedure, if they request you to stop at any time, you must do so. The patient should be invited to have an escort present if they wish Observe the patient throughout the procedure for signs of Autonomic Dysreflexia or other adverse events (RCN 2000) Ensure a private environment If the patient s spinal injury is stable, position the patient in a lateral position (usually left side) with knees flexed. Flexing the knees promotes the stability of the patient and helps to expose the anus (Campbell 1993). If the spinal injury is unstable bowel management will be conducted during a team roll, maintaining spinal alignment at all times Place protective pad under the patient Wash hands, put on disposable gloves and apron 2014/2/22 37
38 Digital removal of faeces If the patient suffers local discomfort or Autonomic Dysreflexia during this procedure local anaesthetic gel may be applied prior to the procedure (Furusawa 2008, Cosman 2005). This requires 5-10 minutes to take effect and lasts up to 90 minutes. Note that long term use should be avoided due to systemic effects (BNF 2008) Lubricate gloved finger with water soluble gel Inform patient you are about to begin Insert single gloved, lubricated finger (Addison and Smith 2000) slowly and gently into rectum If stool is a solid mass, push finger into centre, split it and remove small sections until none remain. If stool is in small separate hard lumps remove a lump at a time. Great care should be taken to remove stool in such a way as to avoid damage to the rectal mucosa and anal sphincters i.e. do not over-stretch the sphincters by using a hooked finger to remove large pieces of hard stool which may also graze the mucosa 2014/2/22 38
39 Digital removal of faeces Using a hooked finger can lead to scratching or scoring of the mucosa and should be avoided. Where stool is hard, impacted and difficult to remove other approaches should be employed in combination with digital removal of faeces. If the rectum is full of soft stool continuous gentle circling of the finger may be used to remove stool: this is still digital removal of faeces During the procedure the person delivering care may carry out abdominal massage Once the rectum is empty on examination, conduct a final digital check of the rectum after 5 minutes to ensure that evacuation is complete Place faecal matter in an appropriate receptacle as it is removed, and dispose of it in a suitableclinical waste bag When the procedure is completed, wash and dry the patient s buttocks and anal area and position comfortably before leaving Remove gloves and apron and wash hands Record outcome, record and report abnormalities 2014/2/22 39
40 Autonomic dysreflexia and digital interventions for bowel management Both digital stimulation of the rectum and digital removal of faeces may be associated with autonomic dysreflexic symptoms in individuals with spinal cord injury at or above the sixth thoracic vertebra. Autonomic dysreflexia is an abnormal sympathetic nervous system response to a noxious stimulus below the level of injury; acute episodes may result in rapidly rising blood pressure with accompanying risk of brain haemorrhage and death (Kavchak-Keyes 2000). Among susceptible individuals, 36% report dysreflexic symptoms occasionally and 9% always when they conduct bowel management (Coggrave et al 2008). Raised blood pressure during bowel management without symptoms has been recorded (Furusawa 2007, Kirshblum 2003). However, it is not clear that any treatment is required in the absence of symptoms (Kirshblum 2003), hence recording blood pressure when undertaking this intervention has little benefit. 2014/2/22 40
41 Autonomic dysreflexia and digital interventions for bowel management The patient should be observed for symptoms of autonomic dysreflexia which include flushing, sweating and blotchiness ( large,irregular marks ) above the lesion, chills, nasal congestion and headache. Some individuals experience these symptoms mildly whenever they evacuate their bowel. Less often, where the bowel is loaded with constipated stool or severe haemorrhoids or anal fissure are present, acute autonomic dysreflexia may occur in response to bowel care, including digital interventions. The cardinal sign of acute autonomic dysreflexia is a rapidly developing severe headache. In this instance bowel management should be stopped and a medical assessment undertaken. 2014/2/22 41
42 Autonomic dysreflexia and digital interventions for bowel management If acute autonomic dysreflexia persists after stopping the procedure this should be treated promptly, according to local policy, but usually using sublingual nifedipine or a glycerine trinitrate patch. Ano-rectal problems should be treated appropriately and steps should be taken to ensure that the bowel care programme is effective and any faecal loading or constipation is eradicated. Bowel management must still be continued on a regular basis; local anaesthetic gel, applied prior to digital interventions may reduce or eradicate the autonomic dysreflexic response during bowel care (Cosman 2005), though this is not suitable for prolonged use (BNF 2008). Autonomic dysreflexia is most likely to occur in response to ineffective bowel care due to withholding of essential interventions. 2014/2/22 42
43 Stool consistency Medications to adjust stool consistency (e.g. colace, Lactulose, dulcolax suppository) should be taken if needed 2014/2/22 43
44 Pharmacological rectal stimulation: suppositories, micro-enemas Glycerin suppositories act as a mild local stimulus and lubricant (British National Formulary 2008) and usually produce a response in around 20 minutes, while bisacodyl suppositories deliver a stimulant laxative resulting in increased gut motility (British National Formulary 2005). Bisacodyl suppositories with a polyethylene glycol base are reported to act more rapidly than those with a hydrogenated vegetable oil base (Frisbie 1997;House & Stiens 1997;Stiens 1995) (Frisbie 1997;House & Stiens 1997;Stiens 1995); bisacodyl in a vegetable oil base produces a response in approximately 30 minutes. Rectal stimulants alone are seldom sufficient to prompt complete evacuation; most individuals also require digital stimulation or digital evacuation of stool (Coggrave et al 2008). 2014/2/22 44
45 Oral laxatives The use of oral laxatives is reported in 60% of SCI individuals (Coggrave et al 2008); however, little research has been conducted to evaluate the efficacy of laxatives in neurogenic bowel management. Commonly used oral laxatives include stimulants (e.g. senna, bisacodyl), softeners (e.g. dioctyl), bulkers (e.g. metamucil) and osmotics (e.g. polyethylene glycol, lactulose). Laxatives aimed at modulating stool form (softeners, bulkers and osmotics) should be taken regularly to maintain a predictable consistency while stimulants (senna, bisacodyl) which prompt increased bowel activity resulting in the movement of stool into the sigmoid colon and rectum should be taken only prior to planned evacuation of stool. Use of oral laxatives is associated with faecal incontinence; they are not essential for all individuals with neurogenic bowel dysfunction and should be used only when individualised assessment indicates that they may be beneficial. 2014/2/22 45
46 Adjunctive interventions for neurogenic bowel management 2014/2/22 46
47 Gastrocolic reflex The gastrocolic reflex is a reflexic response to the introduction of food or drink into the stomach, resulting in an increase in muscular activity throughout the gut (Harari 2004) which can result in movement of stool into the rectum ready for evacuation. While the response may be reduced in SCI individuals (Aaronson et al 1985;Glick et al 1984;Menardo et al 1987) it is still regarded as worthy of trial in assisting with management (Walter et al 2003, Harari et al 1997). The individual is advised to take some food or drink minutes prior to commencing other bowel management activities; this reflex response is strongest after the first meal of the day. 2014/2/22 47
48 Abdominal massage The use of abdominal massage has been reported by 22-30% of individuals with neurogenic bowel dysfunction (Coggrave et al 2008, Han 1998). Several small studies have suggested that it is beneficial in some patient groups (Albers et al 2006, Richards 1998, Emley 1993) while a study of massage in constipated elderly individuals found no effect (Klauser et al 1992). Recent physiological studies have demonstrated that massage produces a measurable response in the rectum and anus (Coggrave et al 2007a). Massage is applied to the abdomen following the supposed lie of the colon in a clockwise direction; using the back or heel of the hand or a tennis ball or similar, pressure is applied and released firmly but gently in a continuous progression around the abdomen. Lighter stroking movements may also be used, which may trigger somatovisceral reflexes. Massage may be used before and after digital rectal stimulation, insertion of stimulants or digital removal of faeces to aid evacuation (Coggrave 2005). 2014/2/22 48
49 Valsalva manoeuvre/straining This technique results in a rise in intra abdominal pressures and therefore intra rectal pressure. A very short episode of straining at the beginning of bowel evacuation can be considered as part of the normal physiology of defaecation (Pocock and Richards 2006). Patients with cervical and thoracic spinal cord injuries lack control of the abdominal muscles and so are unable to perform this intervention. Patients with lower lesions can strain to assist with evacuation; however straining as the main method of evacuation is associated with a high degree of incontinence, constipation and other difficulties with evacuation (Yim 2001) and should be discouraged. In addition excessive straining can cause severe renal and cardiovascular complications, and may interfere with proper functioning of implanted medical devices such as baclofen pumps. Therefore patients with lower lesions need to be taught to use straining with caution, if at all (Coggrave 2005). 2014/2/22 49
50 2014/2/22 50
51 References 2014/2/22 51
52 References 2014/2/22 52
53 Thank You 2014/2/22 53
Guidelines for the Manual Evacuation of Faeces
 Rationale Guidelines for the Manual Evacuation of Faeces These guidelines are to provide the required information for designated registered nurses, health care assistants and bank support workers to perform
Rationale Guidelines for the Manual Evacuation of Faeces These guidelines are to provide the required information for designated registered nurses, health care assistants and bank support workers to perform
Neurogenic Bowel: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Neurogenic Bowel: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about bowel movements After SCI, you may need more
Bowel Management. Part One
 Bowel Management Part One Introduction Bowel Management in Adults With Spinal Cord Injury If you have a spinal cord injury (SCI) then a regular bowel management routine is vitally important, both physically
Bowel Management Part One Introduction Bowel Management in Adults With Spinal Cord Injury If you have a spinal cord injury (SCI) then a regular bowel management routine is vitally important, both physically
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Bernie Foran, Suzanne Hodson, Jane Mason, Rebecca Mills, Jan Siddall, Rebecca Walsh, Clare
SPINAL CORD MEDICINE EDUCATIONAL MATERIALS FOR PATIENT AND FAMILY BOWEL MANAGEMENT FOLLOWING SPINAL CORD INJURY/IMPAIRMENT FRAZIER REHAB INSTITUTE
 SPINAL CORD MEDICINE EDUCATIONAL MATERIALS FOR PATIENT AND FAMILY BOWEL MANAGEMENT FOLLOWING SPINAL CORD INJURY/IMPAIRMENT FRAZIER REHAB INSTITUTE DISCLAIMER The information contained herein is intended
SPINAL CORD MEDICINE EDUCATIONAL MATERIALS FOR PATIENT AND FAMILY BOWEL MANAGEMENT FOLLOWING SPINAL CORD INJURY/IMPAIRMENT FRAZIER REHAB INSTITUTE DISCLAIMER The information contained herein is intended
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Stool softeners are medicines like (ducolox - pericolace - senokot). You want the stool to remain soft so it is easier to empty the bowel.
 "Bowel Management" How the Body Works The food you eat and drink provides your body with many nutrients. These nutrients give you energy and help you stay healthy. As food moves through your body it breaks
"Bowel Management" How the Body Works The food you eat and drink provides your body with many nutrients. These nutrients give you energy and help you stay healthy. As food moves through your body it breaks
Transanal irrigation. Toolbox for neurogenic bowel management. Information for patients Spinal Injuries
 Transanal irrigation Toolbox for neurogenic bowel management Information for patients Spinal Injuries Neurogenic bowel dysfunction A number of people with a spinal injury experience faecal incontinence
Transanal irrigation Toolbox for neurogenic bowel management Information for patients Spinal Injuries Neurogenic bowel dysfunction A number of people with a spinal injury experience faecal incontinence
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Managing your Bowels. Below is a diagram of the different parts of the digestive system and what they do. The Digestive System:
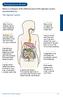 Managing your Bowels Below is a diagram of the different parts of the digestive system and what they do. The Digestive System: 1. Mouth When food is chewed, saliva starts digesting carbohydrates. 2. Oesophagus
Managing your Bowels Below is a diagram of the different parts of the digestive system and what they do. The Digestive System: 1. Mouth When food is chewed, saliva starts digesting carbohydrates. 2. Oesophagus
11/04/2011 OVERVIEW. Neurogenic Bowel Management. in adults with Spinal Cord Injury (S.C.I.) Sequence of events in normal Defecation
 Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Patient Information Leaflet
 Patient Information Leaflet Background Faecal incontinence is a common health problem, affecting over 1% of community-dwelling adults (1;2). Chronic constipation may affect 3-5% of the population depending
Patient Information Leaflet Background Faecal incontinence is a common health problem, affecting over 1% of community-dwelling adults (1;2). Chronic constipation may affect 3-5% of the population depending
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
Bowel Function After Spinal Cord Injury
 Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
AUTONOMIC DYSREFLEXIA
 NATIONAL SPINAL INJURIES CENTRE STOKE MANDEVILLE HOSPITAL HANDOUT PREPARED BY SPINAL OUTPATIENT SERVICES AUTONOMIC DYSREFLEXIA Spinal Outpatient Services Reviewed July 2013, for review July 2016 AUTONOMIC
NATIONAL SPINAL INJURIES CENTRE STOKE MANDEVILLE HOSPITAL HANDOUT PREPARED BY SPINAL OUTPATIENT SERVICES AUTONOMIC DYSREFLEXIA Spinal Outpatient Services Reviewed July 2013, for review July 2016 AUTONOMIC
B l a d d e r & B o w e l C a r e. For Patients with Spinal Cord Injuries
 B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
How to perform a digital removal of faeces
 How to perform a digital removal of faeces For some patients, such as those with spinal cord injury, cauda equina, spina bifida and multiple sclerosis, the digital removal of faeces is an integral part
How to perform a digital removal of faeces For some patients, such as those with spinal cord injury, cauda equina, spina bifida and multiple sclerosis, the digital removal of faeces is an integral part
Patient Information Leaflet Guidelines for the use of Rectal Irrigation
 Patient Information Leaflet Guidelines for the use of Rectal Irrigation Page 1 of 8 Introduction You have been referred by your consultant for rectal irrigation in the Nurse Specialist Clinic, as a means
Patient Information Leaflet Guidelines for the use of Rectal Irrigation Page 1 of 8 Introduction You have been referred by your consultant for rectal irrigation in the Nurse Specialist Clinic, as a means
CONTINENCE MODULE 3 MIMIMUM STANDARDS FOR SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF CONSTIPATION AND FAECAL INCONTINENCE
 CONTINENCE MODULE 3 MIMIMUM STANDARDS FOR SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF CONSTIPATION AND FAECAL INCONTINENCE The minimum standards required to initiate specialised conservative treatment
CONTINENCE MODULE 3 MIMIMUM STANDARDS FOR SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF CONSTIPATION AND FAECAL INCONTINENCE The minimum standards required to initiate specialised conservative treatment
Guidelines for Management of Neurogenic Bowel Dysfunction in Individuals with Central Neurological Conditions
 Guidelines for Management of Neurogenic Bowel Dysfunction in Individuals with Central Neurological Conditions Initiated by the Multidisciplinary Association of Spinal Cord Injured Professionals Supported
Guidelines for Management of Neurogenic Bowel Dysfunction in Individuals with Central Neurological Conditions Initiated by the Multidisciplinary Association of Spinal Cord Injured Professionals Supported
Biofeedback Program. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Foreword. Bowel Management
 2 Bowel Management Foreword The section on is very similar to that of Bladder Care and Management section, as there are many issues to be addressed. You should always remember that what works for one individual
2 Bowel Management Foreword The section on is very similar to that of Bladder Care and Management section, as there are many issues to be addressed. You should always remember that what works for one individual
Bowel Management. Part Two
 Bowel Management Part Two Bowel Management in Adults with Spinal Cord Injury Part 2 What is the goal of medications in my bowel management programme? The goal of medications as part of your bowel management
Bowel Management Part Two Bowel Management in Adults with Spinal Cord Injury Part 2 What is the goal of medications in my bowel management programme? The goal of medications as part of your bowel management
Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 416 Effective Date: August 31, 2006 SUBJECT: ENEMAS 1. PURPOSE: A. To relieve distention and gas by absorption,
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 416 Effective Date: August 31, 2006 SUBJECT: ENEMAS 1. PURPOSE: A. To relieve distention and gas by absorption,
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
Bright-red bleeding: If you have piles, you might see bright-red bleeding on the toilet paper, in the toilet bowl or on the surface of the faeces.
 What are haemorrhoids/piles? In the inner lining of the anus there are three haemorrhoidal cushions of tissue, which help to seal the anus and contribute to the control of the bowels (continence). Often,
What are haemorrhoids/piles? In the inner lining of the anus there are three haemorrhoidal cushions of tissue, which help to seal the anus and contribute to the control of the bowels (continence). Often,
Bowel and Bladder Management following TM
 Presenter: Janet Dean, CRNP Johns Hopkins University School of Medicine Transcription from presentation available at https://youtu.be/nksrjv2oeko [00:30] So I am going to be talking about bowel and bladder
Presenter: Janet Dean, CRNP Johns Hopkins University School of Medicine Transcription from presentation available at https://youtu.be/nksrjv2oeko [00:30] So I am going to be talking about bowel and bladder
Primary Care Constipation Guidelines. Version 1 November 2016
 Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Constipation. Self-study course
 Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Constipation An Overview. Definition Physiology of GI tract Etiology Assessment Treatment
 CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS
 Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Constipation: Treatment of Chronic Constipation and Soiling
 Patient and Family Education Constipation: Treatment of Chronic Constipation and Soiling While it is normal for a child to be constipated now and then, ongoing problems are not. This handout gives a treatment
Patient and Family Education Constipation: Treatment of Chronic Constipation and Soiling While it is normal for a child to be constipated now and then, ongoing problems are not. This handout gives a treatment
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Prescribing Guidance for the Treatment of Constipation in Children
 Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Q3. If the Trust does not, how is bowel care managed in the above patient groups who present with this care need?
 Response sent by email 10 February 2017 St Helier Hospital Wrythe Lane Carshalton Surrey SM5 1AA Tel: 020 8296 2000 Direct dial tel: 020 8296 4992 Re: Freedom of Information request - Ref: FOI 3799 Thank
Response sent by email 10 February 2017 St Helier Hospital Wrythe Lane Carshalton Surrey SM5 1AA Tel: 020 8296 2000 Direct dial tel: 020 8296 4992 Re: Freedom of Information request - Ref: FOI 3799 Thank
Slide 1. Slide 2. Slide 3. A New Standard of Care for Persons with Disability: Bowel Management
 Slide 1 A New Standard of Care for Persons with Disability: Bowel Management CYNTHIA HERNANDEZ, MSN/ED.,RN,CRRN Slide 2 Objectives Describe standards for bowel management based on disability Discuss the
Slide 1 A New Standard of Care for Persons with Disability: Bowel Management CYNTHIA HERNANDEZ, MSN/ED.,RN,CRRN Slide 2 Objectives Describe standards for bowel management based on disability Discuss the
Continence/Constipation Workshop for RNs in Long-Term Care
 Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
Bowel management workbook
 Premium Health First Aid and Specialised Health Solutions PO Box 7072, Brighton Vic 3185 Phone: 1300 72 12 92 Fax: 03 9596 1766 Email: info@premiumhealth.com.au www.premiumhealth.com.au RTO No. 104032
Premium Health First Aid and Specialised Health Solutions PO Box 7072, Brighton Vic 3185 Phone: 1300 72 12 92 Fax: 03 9596 1766 Email: info@premiumhealth.com.au www.premiumhealth.com.au RTO No. 104032
A patient s guide to the. management of constipation following surgery
 A patient s guide to the management of constipation following surgery This leaflet has been designed to give you more information about using laxatives after your surgery. What is constipation? After your
A patient s guide to the management of constipation following surgery This leaflet has been designed to give you more information about using laxatives after your surgery. What is constipation? After your
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Bladder and Bowel Symptoms Troubleshooting Tips
 Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Bladder and Bowel Symptoms Troubleshooting Tips Unwilling to accept assistance with using the toilet There may be an underlying condition that causes this resistance, or the individual may not understand
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN
 Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN Dr. Alberto Peña, Chief of Surgery at Schneider Children's Hospital created the posterior sagittal anorectoplasty
Bowel Management for Children with Anorectal Malformations by Kathleen Guardino, RN, MSN Dr. Alberto Peña, Chief of Surgery at Schneider Children's Hospital created the posterior sagittal anorectoplasty
Bowel and Bladder Management Following Transverse Myeli5s
 Bowel and Bladder Management Following Transverse Myeli5s Janet Dean, MS, RN, CRRN, CRNP Pediatric Nurse Prac55oner Interna5onal Center for Spinal Cord Injury Department of Physical Medicine and Rehabilita5on
Bowel and Bladder Management Following Transverse Myeli5s Janet Dean, MS, RN, CRRN, CRNP Pediatric Nurse Prac55oner Interna5onal Center for Spinal Cord Injury Department of Physical Medicine and Rehabilita5on
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Anorectal physiology test
 Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
PROCEDURE FOR THE USE OF PERISTEEN ANAL IRRIGATION SYSTEM FOR ADULTS (FOR THE PURPOSE OF RECTAL IRRIGATION)
 PROCEDURE FOR THE USE OF PERISTEEN ANAL IRRIGATION SYSTEM FOR ADULTS (FOR THE PURPOSE OF RECTAL IRRIGATION) Issue History Issue Version Purpose of Issue/Description of Change Planned Review Date One To
PROCEDURE FOR THE USE OF PERISTEEN ANAL IRRIGATION SYSTEM FOR ADULTS (FOR THE PURPOSE OF RECTAL IRRIGATION) Issue History Issue Version Purpose of Issue/Description of Change Planned Review Date One To
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
MANAGING CONSTIPATION
 MANAGING CONSTIPATION INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Constipation is. The Symptoms of Constipation. How to Help Manage Constipation. WHAT IS CONSTIPATION?
MANAGING CONSTIPATION INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Constipation is. The Symptoms of Constipation. How to Help Manage Constipation. WHAT IS CONSTIPATION?
Protocol to support reducing the use of and the effective use of laxatives. HaRD CCG employed Pharmacists and Medicines Optimisation Technicians.
 NY&AWC Medicines Management Team Protocol to support reducing the use of and the effective use of laxatives Applies to HaRD CCG employed Pharmacists and Medicines Optimisation Technicians. These protocols
NY&AWC Medicines Management Team Protocol to support reducing the use of and the effective use of laxatives Applies to HaRD CCG employed Pharmacists and Medicines Optimisation Technicians. These protocols
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS OVERVIEW
 Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate.
 NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
Delormes Operation for Rectal Prolapse
 Delormes Operation for Rectal Prolapse Your Questions Answered What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the rectum become weakened, allowing the muscle of the rectum
Delormes Operation for Rectal Prolapse Your Questions Answered What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the rectum become weakened, allowing the muscle of the rectum
Patient Information Leaflet
 Patient Information Leaflet Your Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal
Patient Information Leaflet Your Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal
Indwelling Urinary Catheter Template for Care Plan Development Problem No: be a last resort when all suprapubic catheter in CAUTI
 Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Sacral Nerve Stimulation for Faecal Incontinence
 Sacral Nerve Stimulation for Faecal Incontinence Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital
Sacral Nerve Stimulation for Faecal Incontinence Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Management of the Neurogenic Bowel. June st National SBAA Conference Bloomington, Minnesota
 Management of the Neurogenic Bowel June 2016 41st National SBAA Conference Bloomington, Minnesota DEPARTMENT OF NURSING Rhonda Bolin, BSN, RN, CPN Spina Bifida Nurse Texas Children s Hospital Spina Bifida
Management of the Neurogenic Bowel June 2016 41st National SBAA Conference Bloomington, Minnesota DEPARTMENT OF NURSING Rhonda Bolin, BSN, RN, CPN Spina Bifida Nurse Texas Children s Hospital Spina Bifida
Patient Information Leaflet
 Patient Information Leaflet Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal act like
Patient Information Leaflet Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal act like
Chapter 22. Bowel Needs. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 22 Bowel Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 22.1 Define the key terms and key abbreviations in this chapter. Describe normal defecation and the observations to report.
Chapter 22 Bowel Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 22.1 Define the key terms and key abbreviations in this chapter. Describe normal defecation and the observations to report.
Chapter 19. Assisting With Bowel Elimination. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Assisting With Bowel Elimination Normal Bowel Elimination Time and frequency of bowel movements (BMs) vary. To assist with bowel elimination, you need to know these terms: Defecation is the
Chapter 19 Assisting With Bowel Elimination Normal Bowel Elimination Time and frequency of bowel movements (BMs) vary. To assist with bowel elimination, you need to know these terms: Defecation is the
Irritable bowel syndrome in adults
 Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Constipation. Disease Review
 bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
DIETARY ADVICE FOR CONSTIPATION
 Leicestershire Nutrition and Dietetic Services DIETARY ADVICE FOR CONSTIPATION What is constipation? Constipation is one of the most common digestive complaints and it can affect people of all ages. Bowel
Leicestershire Nutrition and Dietetic Services DIETARY ADVICE FOR CONSTIPATION What is constipation? Constipation is one of the most common digestive complaints and it can affect people of all ages. Bowel
Peristeen Anal Irrigation
 Peristeen Anal Irrigation Advice & Instructions Anal Irrigation Advice and Instructions for patients.indd 1 04/05/2011 11:29:28 Contents Introduction 3 History 3 The bowel system 4 Constipation 6 Faecal
Peristeen Anal Irrigation Advice & Instructions Anal Irrigation Advice and Instructions for patients.indd 1 04/05/2011 11:29:28 Contents Introduction 3 History 3 The bowel system 4 Constipation 6 Faecal
Information and instruction for Home Helps caring for clients with indwelling urinary catheters
 Information and instruction for Home Helps caring for clients with indwelling urinary catheters This leaflet provides you with information and instructions on caring for clients who have an indwelling
Information and instruction for Home Helps caring for clients with indwelling urinary catheters This leaflet provides you with information and instructions on caring for clients who have an indwelling
NORTHWICK PARK DEPENDENCY SCORE
 NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Bowel Dysfunction in Neurological Disease Best Practice in an Evolving Disorder
 Bowel Dysfunction in Neurological Disease Best Practice in an Evolving Disorder Anton Emmanuel October 2016 National Hospital for Neurology & Neurosurgery Regulation of colonic function Brain gut axis
Bowel Dysfunction in Neurological Disease Best Practice in an Evolving Disorder Anton Emmanuel October 2016 National Hospital for Neurology & Neurosurgery Regulation of colonic function Brain gut axis
PREPARING FOR ANORECTOAL MANOMETRY. ManoScan Anorectal Manometry System
 PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
Peristeen and the Neurogenic Bowel Dysfunction Score (NBD) for pediatric patients with spina bifida
 Peristeen and the Neurogenic Bowel Dysfunction Score (NBD) for pediatric patients with spina bifida Coloplast develops products and services that make life easier for people with very personal and private
Peristeen and the Neurogenic Bowel Dysfunction Score (NBD) for pediatric patients with spina bifida Coloplast develops products and services that make life easier for people with very personal and private
Advice for Parents and Carers
 Advice for Parents and Carers 1 2 CONTENTS 4. What is constipation? 4. What is faecal impaction? 5. How common is constipation in children? 5. How to tell if your child may be constipated 6. How constipation
Advice for Parents and Carers 1 2 CONTENTS 4. What is constipation? 4. What is faecal impaction? 5. How common is constipation in children? 5. How to tell if your child may be constipated 6. How constipation
Anal sphincter exercises. Information for patients Sheffield Teaching Hospitals
 Anal sphincter exercises Information for patients Sheffield Teaching Hospitals Anal sphincter exercises to help lessen leakage from the bowel Sphincter exercises, when practiced correctly, can build up
Anal sphincter exercises Information for patients Sheffield Teaching Hospitals Anal sphincter exercises to help lessen leakage from the bowel Sphincter exercises, when practiced correctly, can build up
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bowel Health in Adults
 Bowel Health in Adults Patient Information Contact Details: Bladder and Bowel Specialist Nurse Service First Floor New Alderley House Macclesfield District General Hospital Victoria Road Macclesfield SK10
Bowel Health in Adults Patient Information Contact Details: Bladder and Bowel Specialist Nurse Service First Floor New Alderley House Macclesfield District General Hospital Victoria Road Macclesfield SK10
Bowel-Spinal Cord Injury Manual
 Thomas Jefferson University Jefferson Digital Commons Spinal Cord Injury Manual (English) Regional Spinal Cord Injury Center of the Delaware Valley Spinal Cord Injury Manual 2009 Bowel-Spinal Cord Injury
Thomas Jefferson University Jefferson Digital Commons Spinal Cord Injury Manual (English) Regional Spinal Cord Injury Center of the Delaware Valley Spinal Cord Injury Manual 2009 Bowel-Spinal Cord Injury
BOWEL PROBLEMS. Multiple Sclerosis Basic Facts Series. The bowel: what it is, what it does
 Multiple Sclerosis Basic Facts Series BOWEL PROBLEMS The bowel: what it is, what it does The bowel, also known as the colon or large intestine, is the lower portion of the digestive system. This is the
Multiple Sclerosis Basic Facts Series BOWEL PROBLEMS The bowel: what it is, what it does The bowel, also known as the colon or large intestine, is the lower portion of the digestive system. This is the
Adult Bowel Care Guidelines
 SH CP 205 Version: 1 Summary: Keywords: Target Audience: This guideline defines statements documenting the standards and expectations for the clinical assessment and management of adult bowel dysfunction.
SH CP 205 Version: 1 Summary: Keywords: Target Audience: This guideline defines statements documenting the standards and expectations for the clinical assessment and management of adult bowel dysfunction.
CONSTIPATION. Patient Information Leaflet. Your Health. Our Priority. Microbiology Department Pathology Laboratory
 CONSTIPATION Patient Information Leaflet Your Health. Our Priority. Page 2 of 5 What is constipation? Constipation is infrequent or difficult passing of hard, dry faeces. In most cases, it is harmless,
CONSTIPATION Patient Information Leaflet Your Health. Our Priority. Page 2 of 5 What is constipation? Constipation is infrequent or difficult passing of hard, dry faeces. In most cases, it is harmless,
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Bowel Management following Spinal Cord Injury
 Bowel Management following Spinal Cord Injury Spinal Cord Injury InfoSheet 9 Level - All THE DIGESTIVE SYSTEM The digestive system has both upper and lower digestive tracts. The upper digestive tract breaks
Bowel Management following Spinal Cord Injury Spinal Cord Injury InfoSheet 9 Level - All THE DIGESTIVE SYSTEM The digestive system has both upper and lower digestive tracts. The upper digestive tract breaks
Episode 3.2 Show Notes Constipation
 Episode 3.2 Show Notes Constipation Presented by: Dr Jo Preston, Dr Iain Wilkinson & Mairéad O Malley Faculty: Clare Watson, Wendy Grosvenor Guest faculty: Dr Gaggandeep Singh Alg Broadcast Date: 28th
Episode 3.2 Show Notes Constipation Presented by: Dr Jo Preston, Dr Iain Wilkinson & Mairéad O Malley Faculty: Clare Watson, Wendy Grosvenor Guest faculty: Dr Gaggandeep Singh Alg Broadcast Date: 28th
Suppositories and Enemas
 Suppositories and Enemas Training Components Indication for use of suppository and enemas Prior to administering medication (8 Rs) Precautions Proper insertion technique Suppository Enema Storage Indication
Suppositories and Enemas Training Components Indication for use of suppository and enemas Prior to administering medication (8 Rs) Precautions Proper insertion technique Suppository Enema Storage Indication
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Patient Information Leaflet. Treating Rectal Prolapse Delormes Operation
 Patient Information Leaflet Treating Rectal Prolapse Delormes Operation Treating Rectal Prolapse - Delormes operation What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the
Patient Information Leaflet Treating Rectal Prolapse Delormes Operation Treating Rectal Prolapse - Delormes operation What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the
Procedure for removal and reinsertion of a supra pubic catheter
 Procedure for removal and reinsertion of a supra pubic catheter Equipment required collect prior to procedure Perform this procedure as an aseptic technique to minimise the risk of introducing Clean the
Procedure for removal and reinsertion of a supra pubic catheter Equipment required collect prior to procedure Perform this procedure as an aseptic technique to minimise the risk of introducing Clean the
Administering Rescue Medication into Children for Prolonged Seizures
 Standard Operating Procedure 10 (SOP 10) Administering Rescue Medication into Children for Prolonged Seizures Why we have a procedure? Black Country Partnership NHS Trust (hereafter referred to as the
Standard Operating Procedure 10 (SOP 10) Administering Rescue Medication into Children for Prolonged Seizures Why we have a procedure? Black Country Partnership NHS Trust (hereafter referred to as the
Bowel Management. Graphic: cfotosearch.com
 Bowel Management Graphic: cfotosearch.com The digestive tract as a whole is a hollow tube extending from the mouth to the anus. The bowel, the final portion of the tract, is where waste products of digested
Bowel Management Graphic: cfotosearch.com The digestive tract as a whole is a hollow tube extending from the mouth to the anus. The bowel, the final portion of the tract, is where waste products of digested
BRIEF INTERVENTIONS: ENCOPRESIS
 BRIEF INTERVENTIONS: ENCOPRESIS BI-PED PROJECT (BRIEF INTERVENTIONS: PEDIATRICS) Emotional Health Committee Maryland Chapter American Academy of Pediatrics David Bromberg M.D. Overview: Encopresis is diagnosed
BRIEF INTERVENTIONS: ENCOPRESIS BI-PED PROJECT (BRIEF INTERVENTIONS: PEDIATRICS) Emotional Health Committee Maryland Chapter American Academy of Pediatrics David Bromberg M.D. Overview: Encopresis is diagnosed
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
