Pelvic exenteration. Information for patients and their families/carers
|
|
|
- Lily Simmons
- 5 years ago
- Views:
Transcription
1 Pelvic exenteration Information for patients and their families/carers
2 Your doctor has recommended that you have an operation to remove your rectum, bladder and (if you are male) possibly your prostate. This operation is known as pelvic exenteration. To allow you to still pass faeces and urine, we may also recommend that you have a special combined stoma constructed. This is explained later in the leaflet. We hope this leaflet will help you to understand what this operation involves and how it will affect you. It is natural to be anxious and nervous about the operation. It is important that you and your family talk to the Advanced Nurse Practitioner or surgeon about your concerns or any questions that you have. They will be able to explain all the information in this leaflet in more detail. You can contact the Colorectal Advanced Nurse Practitioner and Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner at the following hospitals: John Radcliffe Hospital Tel: or (9.00am to 5.00pm, Monday to Friday, excluding bank holidays) Churchill Hospital Tel: (9.00am to 5.00pm, Monday to Friday, excluding bank holidays) It is often helpful to have a partner, family member or friend with you when you have your appointments at the hospital. They can make notes and help with remembering what was discussed. page 2
3 Why do I need this operation? This operation is usually carried out for people who have cancer affecting their rectum, bladder and/or prostate (in men) or urethra (in women). If you are having this treatment for cancer, the surgeon will also remove some of the healthy tissue around the tumour, to make sure all the cancer is removed. page 3
4 What does the operation involve? The operation will involve open surgery, not keyhole surgery. This involves making a cut down the centre of your abdomen (tummy). When your rectum is removed, you will no longer have an anus through which to pass a bowel motion (stool/poo/ faeces). The removal of your bladder and prostate (if you are male) means you will also no longer be able to pass urine in the usual way. Your ureters (tubes from your kidneys to your bladder) will be attached to your bowel (sigmoid colon). The surgeon will then use some of the lower part of your large bowel to create a tube (colostomy or stoma ) to the outside of your abdomen. The stoma will be used to divert your urine and faeces, so it all flows out through this opening and into a secure bag. This is a type of combined stoma known as a wet colostomy. The operation will involve using a part of your abdominal muscles to cover the operated area and close the anus. kidney kidney ureter ureter bowel page 4
5 We will encourage you to get up and move around with help, within hours of your operation. However, you will also need to make sure you regularly rest in bed, to help you recover. You will have drips and drains attached to you, but the nurses will help you with these when you need to move. It is important that you start to walk around as soon as you can, as this will help increase your breathing and circulation. It will also help you to regain your strength, as well as reducing some of the risks associated with surgery, such as blood clots, chest infections and pneumonia. Womb Bladder Vagina Ovaries Cervix Rectum Illustration showing the female pelvic organs. We will show you the areas that will be removed during your operation. page 5
6 Bladder Prostate gland Rectum Penis Urethra Testicle Scrotum Illustration showing the male pelvic organs. We will show you the areas that will be removed during your operation. Creating a stoma Your surgeon will have told you that this operation will result in you needing a permanent colostomy or stoma. A stoma is a surgically created opening on the abdomen, which allows faeces or urine to exit the body and pass into a secure, disposable bag. The type of stoma you will have will collect both faeces and urine into one bag. The Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner will talk to you in more detail about this part of the operation, and will explain all you need to know about caring for your stoma once you leave hospital. The Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner will also be able to give you a lot of information about recovery from the operation and life with a stoma. This will include advice about things such as work, travel and diet, which will help you to return to your normal everyday activities. page 6
7 How long does the operation take? This operation itself usually takes between 8 to 10 hours, but you will be away from the ward for longer than this, as you will be taken to the recovery area after your operation. Due to the length of time in theatre and the complexity of your surgery, you will then go to the Intensive Care Unit for added support after the surgery. There will be three types of surgeon involved in your surgery: A colorectal surgeon, to remove your rectum and create the stoma. A urologist, to remove your bladder and/or prostate and attach your ureters (kidney tubes) to your large bowel. A plastic surgeon, to assist with the muscle flap to cover over your bottom area (by using a piece of your abdominal muscle to cover the area between your genitals and anus). How long will I be in hospital? The average length of stay in hospital is about days; however, this can vary considerably from person to person, depending on how well you recover and whether you have any other medical requirements. page 7
8 What are the risks? This is a major operation and, as with any operation, it will carry risks. The chance of any of these risks happening varies from person to person, depending on lots of factors, such as age, weight and general health. Your surgeon and Advanced Nurse Practitioner will explain what the chance is of these risks affecting you, as well as any specific risks which might also apply to you. General risks of surgery include: risks related to general anaesthetic (these will be discussed with you in more detail by the anaesthetist before your surgery) blood clots in the leg or lung (thrombosis) chest infection urinary infection myocardial infarction (heart attack) stroke death. Specific risks of this operation include: bleeding wound infection deterioration of the muscle flap formation of internal scar tissue (adhesions) leakage from the point where the ureters join the large bowel damage to the nerves supplying the sexual organs (this could affect your sexual function). This can vary if your prostate is removed and may even be permanent. a very small risk of injury to the spleen (a small organ in the abdomen that plays a part in the body s immune system) and ureter (tube that drains the kidney) during surgery. If there is anything you are unsure about, or if you have any questions, please speak to your surgeon or Colorectal Advanced page 8
9 Nurse Practitioner before signing the consent form for the operation to go ahead (either at your pre-operative assessment or on the day of your admission). What pain relief will I be given? This is a major operation, so you will feel sore and uncomfortable afterwards; most people describe feeling very bruised. As the swelling from the operation goes down, this discomfort will also lessen. We will do our best to make sure that you have all the pain relief that you need. Before your operation the anaesthetist will talk to you about the options for pain relief after the operation. You may have an epidural (spinal pain relief), or possibly a self controlled pain relief pump (PCA) for the first few days after your operation. You will receive a leaflet explaining this in more detail, during your preoperative assessment appointment. The nurses on the ward will regularly ask you about your pain to make sure that it is under control and will give you further pain relief if you need it. page 9
10 After the operation You will have a bag over your stoma that will be emptied regularly by the nurse, until you are able to do this yourself. Urine will pass into the bag immediately after the operation and faeces will usually start to pass after hours. At first, your faeces will be liquid; this is normal and as your appetite increases they will become firmer and well-formed. The exit site where your stoma opens from your abdomen will be swollen to begin with. There will be a plastic rod (7.5cms in length) supporting your stoma for the first 5-7 days and you will also have dissolvable stitches surrounding the edge of the stoma. The removal of this rod is straightforward and your Advanced Nurse Practitioner or ward nurse will be able to carry this out. This should not be painful. You will also have two stents (thin, long plastic tubes) which go through your stoma and into your bowel, to support the join between the ureter (kidney tubes) and the bowel. These will stay in place for approximately days. As they are held in place with dissolvable stitches, they will either fall out when they are ready or can be removed by your Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner. page 10
11 What is enhanced recovery? Enhanced recovery is a new way of improving the experience and wellbeing of people who have had surgery. It can help you to recover sooner, so that life can return to normal as quickly as possible. The programme focuses on making sure that you are actively involved in your recovery. This will be discussed with you at your pre-operative assessment appointment. Sitting after surgery After surgery on your bottom, you will be advised by your surgeon not to sit on this area for long periods of time. You may need to lie down regularly to avoid pressure on the wound while it is healing. Immediately after the surgery, the nurses will help to keep you comfortable and will help you into positions to avoid putting pressure on your healing wound. Your surgeon will tell you how long you will need to avoid sitting on your wound after surgery, as this varies from person to person, depending on how quickly you heal and feel comfortable. page 11
12 Getting back to normal How soon can I drive after surgery? Your nurse specialist will discuss this with you. Most insurance policies state that you are not covered until 6 weeks after abdominal surgery. This is because it is likely that your reaction time will be slower than normal if you have to complete an emergency stop. If you feel that you are safe and ready to return to driving before 6 weeks, please discuss this with your GP. They may be able to give you the go ahead to drive and you can then check this with your insurance company. When can I make love? When you feel you want to! The anxiety and stress of surgery can often reduce your sex drive. This is quite common and will return to normal in time. It is important that you and your partner take the time to talk about your feelings. This will help you both to relax more and enjoy your lovemaking when you feel ready to. You may find that the surgery affects your sexual function. This affects men and women differently. In men, after the operation the nerves controlling erection can sometimes be bruised, as they are located close to the rectum. If you are experiencing difficulties gaining or maintaining an erection, give yourself time to recover from the surgery. If this problem continues, please seek advice from your GP or Advanced Nurse Practitioner, as there may be some further treatment that can help. If you are male and your prostate is removed during this surgery, there is a chance that problems with sexual function and/or impotence could be permanent. If you are a woman, feeling nervous or anxious can make you tense. This can cause lovemaking to be uncomfortable and possibly page 12
13 painful. The more relaxed you can be the better. Take your time and don t let yourself feel rushed if you are not ready. You may find that using lubricants or changing your position may help. When can I return to work? You can return to work when you feel ready to. Deciding when to return to work is an individual decision. If your job involves lifting, pulling, pushing or stretching, then it is better not to go back to work for 2-3 months. Returning to work with light duties to begin with may also help. If your job is very active, we recommend that you wear a hernia support garment, to reduce the chance of developing an abdominal hernia. Your Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner can give you advice on these, if you require it. Developing a hernia is a common complication following the formation of a stoma. A hernia is described as a bulge or swelling, which forms as a result of a weakness in the abdominal wall. Not everyone with a stoma will develop a hernia, but if they do, how severe it is and how it impacts on stoma care will vary from person to person. We will give you further information on hernia prevention if we feel you will be at risk. Tiredness It is normal to feel tired when you go home from hospital. When you first get home from hospital after your operation, try to plan your time so that you have regular rests throughout the day. It may take some time to return to your full strength. Please think about any support you might need during this initial recovery period at home, and talk to your Advanced Nurse Practitioner and the ward staff if you have any concerns. It may be a good idea to have a friend or family member stay with you when you return home, to help with shopping, cooking and cleaning. This will be a great help whilst you are feeling tired. If you have children or grandchildren you should also be cautious of picking them up, as this may cause an abdominal hernia. page 13
14 Exercise You should try to build up your strength slowly once you are home. Start by going for a short walk every day and increase this distance each time. The physiotherapist will show you some exercises while you are in hospital, which you can continue to do at home, to help to build up your muscle strength. You will be able to return your normal activities when you feel well enough. If you normally take part in any regular sporting activities or exercise, these can be re-introduced into your routine slowly. Please speak with your surgeon or Advanced Nurse Practitioner before returning to contact sports, such as rugby. Please take care when lifting, bending or stretching, particularly in the first few weeks after your surgery. Pelvic floor exercises can be beneficial before your operation, to strengthen your muscle tone around your bladder and bowels. We can give you more information about these exercises before your surgery. Wound care It is likely that your tummy and bottom wounds will not be completely healed before you go home. They may need to be dressed by the practice nurse at your GP s surgery or, if you are unable to get there, your local district nurse will come out to you. This will be arranged by the ward nurse, before you are discharged from hospital. page 14
15 Urinary infections Due to the nature of this surgery (because your ureters are joined to your bowel) you will always be at potential risk of developing a urine infection. The symptoms of this are a fever (high temperature) and lower back pain, but the infection usually responds quickly to antibiotics. Urinary infections can occasionally be caused by a narrowing or blockage in the ureters. This may need further investigation if it becomes a persistent problem. Follow-up care Your Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner will telephone you once you are home, to check everything is going well. They will arrange a home visit about 7-10 days after your discharge from hospital, to check the stoma and that you are coping well. Please contact your Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner if you have any concerns before this visit. It is sometimes good to write down your questions or worries, so you can ask them when they contact you. If you live in a county outside of Oxfordshire we will refer you to your local team, to give you on-going support. An outpatient appointment will be made for you approximately 2-4 weeks after your discharge from hospital. If you have any non-urgent questions, this is a good time to ask them. At this stage we may discuss whether you need further oncological treatment, such as chemotherapy. As well as a routine follow-up with your colorectal surgeon (lead consultant), you will also have a follow-up appointment with the plastic surgeon, to make sure your wound is healing well, and the urologist, to check you do not have any urine infection symptoms. page 15
16 Further information Colostomy Association Tel: Website: Macmillan Cancer Support Tel: Website: Other patients or colostomates are also available to be buddied up, for you to talk to before or after your operation. Please ask your Colorectal Advanced Nurse Practitioner, Stoma Specialist Nurse Practitioner or Advanced Nurse Practitioner for contact information. If you have a specific requirement, need an interpreter, a document in Easy Read, another language, large print, Braille or audio version, please call or PALS@ouh.nhs.uk Author Contributors Catherine Brooks, Stoma Care Specialist Nurse Practitioner Richard Guy, Consultant Surgeon Jay Bradbury, Senior Nurse/Advanced Nurse Practitioner July 2016 Review: July 2019 Oxford University Hospitals NHS Foundation Trust Oxford OX3 9DU OMI 13177P
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
ABDOMINAL PERINEAL RESECTION. Patient information Leaflet
 ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
To help you understand your operation, it is helpful to have a basic knowledge of how the body works (see Figure 1).
 Page 1 of 11 Anterior resection Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what the procedure involves and also some of the common complications
Page 1 of 11 Anterior resection Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what the procedure involves and also some of the common complications
The Children s Hospital, Tom s Ward. Hirschsprung Disease. Information for parents
 The Children s Hospital, Tom s Ward Hirschsprung Disease Information for parents What is Hirschsprung disease? Hirschsprung disease is a rare disorder of the bowels, most commonly the large bowel (colon).
The Children s Hospital, Tom s Ward Hirschsprung Disease Information for parents What is Hirschsprung disease? Hirschsprung disease is a rare disorder of the bowels, most commonly the large bowel (colon).
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
Hydrocele repair. Information for parents and carers
 Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
ABDOMINAL PERINEAL RESECTION
 ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
Laparoscopic (keyhole) colorectal (bowel) resection
 Laparoscopic (keyhole) colorectal (bowel) resection Your operation explained Information for patients Colorectal Surgery Introduction This leaflet should be read together with a booklet which explains
Laparoscopic (keyhole) colorectal (bowel) resection Your operation explained Information for patients Colorectal Surgery Introduction This leaflet should be read together with a booklet which explains
Retroperineal Lymph Node Dissection (RPLND)
 Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Advice for patients after laparoscopic hernia repair
 Advice for patients after laparoscopic hernia repair Day Surgery Unit Patient Information Leaflet Introduction This leaflet is for patients who have had a laparoscopic hernia repair. It gives advice on
Advice for patients after laparoscopic hernia repair Day Surgery Unit Patient Information Leaflet Introduction This leaflet is for patients who have had a laparoscopic hernia repair. It gives advice on
Your Bowel Operation Hartmanns Procedure
 Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Urology Department Percutaneous Nephrolithotomy (PCNL)
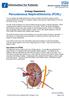 Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Femoral endarterectomy
 Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Trans urethral resection of prostate (TURP)
 Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients
 Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Maternity Information Leaflet
 Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Repair of Hydrocele. Patient Information. Day Surgery. Ward 3, Leigh Infirmary
 Repair of Hydrocele Patient Information Day Surgery Ward 3, Leigh Infirmary Author ID: LS Leaflet Number: SW3.002 Version: 5 Name of Leaflet: Repair of Hydrocele Date Produced: August 2017 Review Date:
Repair of Hydrocele Patient Information Day Surgery Ward 3, Leigh Infirmary Author ID: LS Leaflet Number: SW3.002 Version: 5 Name of Leaflet: Repair of Hydrocele Date Produced: August 2017 Review Date:
Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP)
 Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP) This leaflet will answer any questions you may have about having holmium laser treatment for your enlarged
Treating your enlarged prostate gland using holmium laser enucleation of the prostate (HoLEP) This leaflet will answer any questions you may have about having holmium laser treatment for your enlarged
Laser Trans Urethral Resection of Prostate (TURP)
 Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Colposuspension operation
 Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Surgery. In this fact sheet. Surgery: English
 Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Advice for patients after hernia repair
 Advice for patients after hernia repair Day Surgery Unit Patient Information Leaflet Introduction This leaflet is for patients who have had a hernia repair. It gives advice on what you should do when you
Advice for patients after hernia repair Day Surgery Unit Patient Information Leaflet Introduction This leaflet is for patients who have had a hernia repair. It gives advice on what you should do when you
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Undescended testes. Information for parents and carers
 Undescended testes Information for parents and carers The testes (or testicles) start developing high inside the tummy near the kidneys. At about 2 months before a boy is born they move down or descend
Undescended testes Information for parents and carers The testes (or testicles) start developing high inside the tummy near the kidneys. At about 2 months before a boy is born they move down or descend
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Abdomino Perineal Excision of Rectum (APER)
 PATIENT INFORMATION Abdomino Perineal Excision of Rectum (APER) Introduction/Procedure This leaflet tells you about the procedure known as abdomino perineal excision/resection (APER) of the rectum. What
PATIENT INFORMATION Abdomino Perineal Excision of Rectum (APER) Introduction/Procedure This leaflet tells you about the procedure known as abdomino perineal excision/resection (APER) of the rectum. What
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients
 Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Hernia Operations. What is a hernia? What does the operation involve? What are the benefits of an operation?
 Hernia Operations Hernia Operations What is a hernia? The abdomen (the medical word for the tummy) contains many organs such as the liver spleen and intestines (the medical word for insides ) and these
Hernia Operations Hernia Operations What is a hernia? The abdomen (the medical word for the tummy) contains many organs such as the liver spleen and intestines (the medical word for insides ) and these
Leg artery bypass (fem-pop bypass)
 Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
Cystectomy. A Guide for Patients and Family. Department of Urology, Forth Valley NHS
 Cystectomy A Guide for Patients and Family Department of Urology, Forth Valley NHS 1 This leaflet has been produced to give you general information about the cystectomy procedure. The leaflet should answer
Cystectomy A Guide for Patients and Family Department of Urology, Forth Valley NHS 1 This leaflet has been produced to give you general information about the cystectomy procedure. The leaflet should answer
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
There are many types of pelvic floor repair that may have been called:
 Pelvic floor repair This information explains: Overview... 1 Your admission Date... 2 The Anaesthetic... 2 The Repair Operation... 2 After the Operation... 2 Going home... 3 Getting back to Normal... 3
Pelvic floor repair This information explains: Overview... 1 Your admission Date... 2 The Anaesthetic... 2 The Repair Operation... 2 After the Operation... 2 Going home... 3 Getting back to Normal... 3
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
Hernia surgery in adults
 Page 1 of 9 Hernia surgery in adults Introduction This leaflet will give you information about having hernia surgery. It also answers some of the commonly asked questions and outlines some of the risks
Page 1 of 9 Hernia surgery in adults Introduction This leaflet will give you information about having hernia surgery. It also answers some of the commonly asked questions and outlines some of the risks
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information
 PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
Physiotherapy Following Your Spinal Discectomy
 Physiotherapy Following Your Spinal Discectomy Patient information How to contact us Physiotherapy Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire,
Physiotherapy Following Your Spinal Discectomy Patient information How to contact us Physiotherapy Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire,
Reproduced with the kind permission of Health Press Ltd, Oxford
 Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
The Children s Hospital Intussusception and its treatment Information for parents
 The Children s Hospital Intussusception and its treatment Information for parents What is intussusception? Intussusception occurs when one part of the bowel slides into another part of bowel, like a telescope,
The Children s Hospital Intussusception and its treatment Information for parents What is intussusception? Intussusception occurs when one part of the bowel slides into another part of bowel, like a telescope,
Department of surgery. Cystectomy for men
 Department of surgery Cystectomy for men Introduction Your doctor has recommended a cystectomy as treatment for your condition. This information describes: what a cystectomy involves what happens during
Department of surgery Cystectomy for men Introduction Your doctor has recommended a cystectomy as treatment for your condition. This information describes: what a cystectomy involves what happens during
This operation is necessary to remove the area of bowel that is diseased.
 PATIENT INFORMATION Sigmoid Colectomy Introduction / Procedure This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of the common complications
PATIENT INFORMATION Sigmoid Colectomy Introduction / Procedure This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of the common complications
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~
 Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Endovascular aneurysm repair (EVAR)
 Endovascular aneurysm repair (EVAR) Arteries carry blood away from your heart to the rest of your body. An aneurysm occurs when the artery walls weaken and the vessel swells and balloons out. These usually
Endovascular aneurysm repair (EVAR) Arteries carry blood away from your heart to the rest of your body. An aneurysm occurs when the artery walls weaken and the vessel swells and balloons out. These usually
OG24 Posterior Repair
 www.rcseng.ac.uk www.rcsed.ac.uk www.pre-op.org OG24 Posterior Repair Expires end of February 2018 Issued May 2017 What is a posterior prolapse? A posterior prolapse is a bulge in the back wall of your
www.rcseng.ac.uk www.rcsed.ac.uk www.pre-op.org OG24 Posterior Repair Expires end of February 2018 Issued May 2017 What is a posterior prolapse? A posterior prolapse is a bulge in the back wall of your
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Laparoscopic Ventral Mesh Rectopexy
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Roboticassisted. laparoscopic nephrectomy
 Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Kent Oncology Centre
 Kent Oncology Centre High Dose Rate Intracavitary Gynaecological Brachytherapy Information for patients We hope this leaflet will help you to understand about brachytherapy (internal radiotherapy) to the
Kent Oncology Centre High Dose Rate Intracavitary Gynaecological Brachytherapy Information for patients We hope this leaflet will help you to understand about brachytherapy (internal radiotherapy) to the
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet
 Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Discharge Information following Bowel Surgery
 Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Cystectomy for women
 Department of surgery Cystectomy for women Introduction Your doctor has recommended a cystectomy as treatment for your condition. This information describes: what a cystectomy involves what happens during
Department of surgery Cystectomy for women Introduction Your doctor has recommended a cystectomy as treatment for your condition. This information describes: what a cystectomy involves what happens during
Vaginal Repair and Vaginal Hysterectomy
 Vaginal Repair and Vaginal Hysterectomy Patient Information Obstetrics & Gynaecology Department Author ID: JD/MC Leaflet Number: Gyn 027 Version: 5.1 Name of Leaflet: Vaginal Repairs Date Produced: February
Vaginal Repair and Vaginal Hysterectomy Patient Information Obstetrics & Gynaecology Department Author ID: JD/MC Leaflet Number: Gyn 027 Version: 5.1 Name of Leaflet: Vaginal Repairs Date Produced: February
Hernia Surgery in Adults
 Page 1 of 7 Hernia Surgery in Adults Introduction This leaflet provides information on hernias in the adult patient and the treatment options available. This leaflet is intended as a guide and is not a
Page 1 of 7 Hernia Surgery in Adults Introduction This leaflet provides information on hernias in the adult patient and the treatment options available. This leaflet is intended as a guide and is not a
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries
 Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
LAPAROSCOPIC RADICAL REMOVAL OF THE KIDNEY INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE )
 HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE ) What does the procedure involve? Removal of obstructing prostate tissue using a telescope and a laser. What are the alternatives to this procedure? Alternatives
HOLEP (HOLMIUM LASER ENUCLEATION OF PROSTATE ) What does the procedure involve? Removal of obstructing prostate tissue using a telescope and a laser. What are the alternatives to this procedure? Alternatives
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts
 Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
The organs and tissues of the body are made up of tiny building blocks called cells. Cancer is a disease of these cells.
 Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Urinary stoma. This is the simplest and most straightforward form of
 This is the simplest and most straightforward form of urinary drainage following surgery to remove the bladder (cystectomy). You may see it referred to as a urostomy, an ileal conduit or urinary diversion.
This is the simplest and most straightforward form of urinary drainage following surgery to remove the bladder (cystectomy). You may see it referred to as a urostomy, an ileal conduit or urinary diversion.
Surgery for an enlarged prostate transurethral resection of the prostate
 Surgery for an enlarged prostate transurethral resection of the prostate Urology Department Patient Information Leaflet Introduction This leaflet is about surgery for an enlarged prostate, known medically
Surgery for an enlarged prostate transurethral resection of the prostate Urology Department Patient Information Leaflet Introduction This leaflet is about surgery for an enlarged prostate, known medically
Hysterectomy. Will my ovaries be removed at the same time?
 Hysterectomy What is a hysterectomy? This is a major operation which removes the uterus (womb) and cervix (neck of the womb) from your body. Why is hysterectomy performed? Some hysterectomies are performed
Hysterectomy What is a hysterectomy? This is a major operation which removes the uterus (womb) and cervix (neck of the womb) from your body. Why is hysterectomy performed? Some hysterectomies are performed
A Guide to your Bowel Surgery
 A Guide to your Bowel Surgery Colorectal Department Patient information leaflet Contents page Introduction 3 What is colorectal cancer? 3 What is the function of the large bowel? 3 How is the diagnosis
A Guide to your Bowel Surgery Colorectal Department Patient information leaflet Contents page Introduction 3 What is colorectal cancer? 3 What is the function of the large bowel? 3 How is the diagnosis
University Hospitals Bristol NHS Foundation Trust NHS. Catheterisation using a Mitrofanoff
 University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
Body changes, washing, clothing and returning to normal activities after your stoma surgery
 Colorectal Nursing Department Body changes, washing, clothing and returning to normal activities after your stoma surgery Information for patients Body image It is completely normal not to immediately
Colorectal Nursing Department Body changes, washing, clothing and returning to normal activities after your stoma surgery Information for patients Body image It is completely normal not to immediately
Transurethral Resection of Prostate
 Transurethral Resection of Prostate Information for Patients This leaflet explains: What does the procedure involve?...2 What are the alternatives to this procedure?...2 What should I expect before the
Transurethral Resection of Prostate Information for Patients This leaflet explains: What does the procedure involve?...2 What are the alternatives to this procedure?...2 What should I expect before the
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Understanding your bowel surgery
 Understanding your bowel surgery Abdomino Perineal Excision of Rectum (APER) Hartmann s Procedure Pan Proctocolectomy Total Colectomy Subtotal Colectomy Information for patients, relatives and carers This
Understanding your bowel surgery Abdomino Perineal Excision of Rectum (APER) Hartmann s Procedure Pan Proctocolectomy Total Colectomy Subtotal Colectomy Information for patients, relatives and carers This
Abdominal surgery for Crohn's disease. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Abdominal surgery for Crohn's disease Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Abdominal surgery for Crohn's disease Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
Having a pancreas transplant alone (PTA)
 Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Laparoscopy. Department of Gynaecology. Patient information
 Laparoscopy Department of Gynaecology Patient information What is is a a laparoscopy? A laparoscopy is an operation performed under general anaesthetic to help your gynaecologist make a diagnosis by looking
Laparoscopy Department of Gynaecology Patient information What is is a a laparoscopy? A laparoscopy is an operation performed under general anaesthetic to help your gynaecologist make a diagnosis by looking
Obstructive Defaecation
 Oxford Pelvic Floor Service Obstructive Defaecation Information for patients page 2 What is obstructive defaecation? Obstructive defaecation is the inability to pass stools (open your bowels). This is
Oxford Pelvic Floor Service Obstructive Defaecation Information for patients page 2 What is obstructive defaecation? Obstructive defaecation is the inability to pass stools (open your bowels). This is
What is. Benefits. the operation? who. You will be asked. operation. identify. You will be visited. Radical prostatectomy
 Radical prostatectomy Radical prostatectomy This leaflet gives you information on the operation you aree due to have. It should cover most of your questions, but if you need further information please
Radical prostatectomy Radical prostatectomy This leaflet gives you information on the operation you aree due to have. It should cover most of your questions, but if you need further information please
Laparoscopic colon resection for colon cancer
 Laparoscopic colon resection for colon cancer Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Laparoscopic colon resection for colon cancer Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Recovery at home following open abdominal aortic aneurysm repair Vascular Surgery Patient Information Leaflet
 Recovery at home following open abdominal aortic aneurysm repair Vascular Surgery Patient Information Leaflet Surgeons, anaesthetists, radiologists and nurses from Russells Hall Hospital in Dudley, New
Recovery at home following open abdominal aortic aneurysm repair Vascular Surgery Patient Information Leaflet Surgeons, anaesthetists, radiologists and nurses from Russells Hall Hospital in Dudley, New
