GYNAELASE SPECIALIST CLINICS OF AUSTRALIA. for successful applicants. No need to wait for treatment.
|
|
|
- April Butler
- 5 years ago
- Views:
Transcription
1 SPECIALIST CLINICS OF AUSTRALIA GYNAELASE Finance available through MacCredit for successful applicants. No need to wait for treatment.
2 GynaeLase Urodynamics for Stress Incontinence GynaeLase is a safe, non-invasive laser therapy for the treatment of a weak bladder. What does it do? In three sessions it will: Tighten the urethral and anterior vaginal wall so the bladder is better supported Stimulate collagen remodelling and development of new collagen fibres to help you regain your natural continence function. How does it work? After childbirth it is common for the bladder to lose its strength and start to sag as can be seen in diagram 1. Diagram 1 Diagram 2 GynaeLase works by targeting the lax skin that supports the bladder with photothermal energy to initially tighten and lift the bladder as can be seen in diagram 2. Eventually the goal is to restore the continence function that you had pre-childbirth and this is achieved through collagen neogenesis or the creation of new vaginal mucosa tissue and fibres. What happens during the treatment? The procedure takes place in our modern surgical suite and is similar to that of a pap smear. If you would like a pap smear conducted at the same time this can be arranged. During the treatment a laser is used to pass laser light technology into the vagina. The initial heat from the laser causes contraction of lax tissue. As a result the collagen contracts and new collagen formation begins strengthening, firming and tightening the urethral and anterior vaginal wall. How long does it take? Treatment takes 20 to 30 minutes. How many treatments do I need? Three treatments recommended one month apart. What does it feel like? Clients report feeling a warm sensation in the treatment area. It is not considered a painful treatment that requires any pain relief. Is there any downtime? No, GynaeLase is a fast, patient-friendly procedure that doesn t involve any anaesthesia allowing you to return to your normal routine right away. We do advise to wait one week after treatment before sexual intercourse. When will I start to notice results? Optimal results will take place a month after the third treatment where you will notice a definite change to the support of the bladder and return to a more natural continence function. How long will my results last? GynaeLase results last a year. This can vary depending on skin laxity and age. When we age, the density of our collagen fibres reduce, therefore overtime the strength and elasticity of our skin will start to sag. In this case the skin supporting the bladder may start to lose its laxity and a maintenance treatment may be required a year or so later. Studies have shown that most people seek a follow up treatment 2 years later.
3 GynaeLase for Stress Incontinence Repeated maintenance treatments long term will increase new collagen growth and maintain bladder support. Will it work for everyone? No, the severity of stress incontinence is due to the amount of laxity of the vaginal tissues in most cases. This treatment will always tighten and strengthen the vaginal tissue with time. The degree of improvement will somewhat depend of the severity of this laxity. Severe stress incontinence will still probably require surgical intervention. This is a treatment for early stages of stress incontinence. It will also help with the early stages of vaginal prolapse. There are other forms of incontinence that will not be improved with this vaginal tightening and strengthening. Other benefits There are many other side benefits of this treatment including the reduction of frequent vaginal infections including bacterial, fungal and yeast infections. It will also help external vulval infections. It will also help several conditions causing pain during intercourse (dyspareunia). Are there any side effects? There are no side effects with GynaeLase. It is a non-surgical and non-invasive treatment; gentle enough to be used on the most sensitive tissue. How much does it cost? $2900 for the series of three treatments. *Pricing was correct at time of printing and may change Is there any post care required? No aftercare is required but we do advise to wait a week before sexual intercourse.
4 GynaeLase for for Stress Vaginal Incontinence Laxity GynaeLase is a safe, non-invasive photo thermal laser treatment for tightening of the vaginal canal and restoring natural hydration. Laxity of the vagina and introitus can occur from vaginal delivery or can be part of the natural ageing process. It can be a bothersome condition to patients and impact on happiness and sexual function. What does it do? In three sessions it will: Tighten the vaginal canal; Stimulate the natural regeneration of vaginal tissue for longer term elasticity and natural flexibility; Treat vaginal atrophy by restoring mucosa hydration through improved mucosa retention capabilities; How does it work? Ageing and childbirth together can alter vaginal elasticity and laxity of the internal skin mucosa and structure. The vaginal tissues also change overtime affecting the volume of protective mucosa generated and natural lubrication. This can result in discomfort for many women. GynaeLase fixes both of these issues through laser-induced thermal technology in the vaginal canal. It stimulates collagen remodelling of the internal tissue and synthesis of new collagen fibres for vaginal contraction. These additional collagen fibres enable a greater holding ability of mucosa for a more lubricated internal environment and thus more comfort, especially during intercourse. What happens during the treatment? The procedure takes place in our modern surgical suite and is similar to that of a pap smear. During the treatment a special probe of the HiScan V2LR scanning system directs laser onto the mucosa of the walls. The initial heat from the laser causes contraction and then the new collagen formation begins tightening, reshaping, toning, stimulating tissue and regenerating collagen. How long does it take? Treatment takes 20 to 30 minutes. How many treatments do I need? Three treatments recommended, one a month. What does it feel like? Patients report feeling a warm sensation in the treatment area. It is not considered a painful treatment that requires any pain relief. Is there any downtime? No, this is a fast, patient-friendly procedure that doesn t involve any anaesthesia allowing you to return to your normal routine right away. We do advise to wait one week after treatment before sexual intercourse. When will I start to notice results? Results appear after a few days with the build up of collagen in the vaginal mucosa and continue progressively over 3-6 months, tightening the vaginal walls in the process and restoring the elasticity and moisture. How long will my results last? GynaeLase results last approximately a year. This can vary depending on skin laxity and age. When we age, the density of our collagen fibres reduce, therefore over time the strength and elasticity of our skin will start to sag. In this case the area we have tightened may start to lose its laxity so a maintenance treatment may be required a year or so later. Studies have shown that most people seek a follow up treatment 2 years later.
5 GynaeLase for Vaginal Laxity Repeated maintenance treatments long term will increase new collagen growth and maintain vaginal canal strength and hydration. After all this is an ageing concern. Are there any side effects? There are no side effects with GynaeLase. It is a non-surgical and non-invasive treatment, gentle enough to be used on the most sensitive tissue How much does it cost? $2900 for the series of three treatments. *Pricing was correct at time of printing and may change Is there any post care required? No aftercare is required but we do advise to wait a week before sexual intercourse.
6 GynaeLase Vaginal Relaxation for Vaginal Syndrome Laxity Causes of VRS The process of ageing is not the only factor, which takes its toll on a woman s body. Pregnancy and childbirth, menopause and variations in weight gain, are factors which impact on all of a woman s organs and systems. Childbirth requires the vagina to stretch prodigiously in the course of delivery, weight gain also stretches the body tissues as it does in pregnancy and with the onset of menopause, even the healthiest women will experience the natural process of vaginal stretching (VRS). VRS When does it start? This condition first manifests itself in women from the ages of 30-40, primarily due to childbirth or weight gain and continues to affect the mucosal lining of the vagina. The vagina gradually changes from being an organ with a strong, thick, moist mucosal lining, able to regenerate collagen continuously, to one with a thin, frail and dry mucosal lining which is increasingly unable to regenerate new collagen fibres. Collagen is the protein essential for strengthening connective tissue in all parts of the body including the vagina. Just as skin gradually loses moisture and elasticity, so does the vaginal wall and mucosa. Symptoms of VRS may also include: Vaginal Irritation with itching and burning Dryness Pain during intercourse (dyspareunia) Low vaginal ph, making the environment open to infection Degrees of urinary incontinence due to weakened vaginal mucosa Er-YAG and CO2 Treatment Two Non Invasive Laser solutions from: Various prescribed tightening creams and sprays to other pharmacological approaches and hormonal pessaries, all of which provided limited results and the need for repeated application. Behavioural options such as Kegel exercises which have a short term effectiveness. Surgical procedures in which vaginal and associated tissues are incised and reshaped (vaginoplasty) offer a longer lasting result, but come with increased risk of scar formation, infection or nerve damage. Now GynaeLase offers three painless, nonsurgical treatment options, both of which induce collagen regeneration in the vaginal mucosa, strengthening the vaginal walls and narrowing (tightening) the diameter of the vaginal cavity. Treatment takes only a few minutes and produces immediate tightening and contraction. Both partners will experience significant sexual gratification due to the improved strength and thickness of the vaginal wall. This improved structural strength also assists in supporting the bladder as previously. VRS no longer need be a condition that women have to endure, along with its unpleasant accompanying symptoms and causing impact on quality of life. Prior to GynaeLase procedures to alleviate symptoms of VRS, the treatment options ranged
7 Stress Incontinence What is Stress Incontinence? Incontinence is the leakage of urine from the bladder. This can occur for several reasons but the most common cause is a weakness of the stretched vaginal wall underneath that supports it. There are several types of incontinence but the most common is Stress Incontinence, where bladder leakage occurs with many things that cause an increase in pressure across the pelvis. Commonly things such as a cough, a sneeze, a laugh, exercise or straining. How can Stress Incontinence be treated? One of the most novel treatments, is the use of some of the new modern lasers in the treatment of stress incontinence of urine. Many women suffer a minor nuisance or a more significant interfering range of symptoms of bladder leakage or stress incontinence. This is a common condition after childbirth, where the vaginal wall becomes lax and weakened, and no longer supports the overlying bladder wall. This alters the dynamics of the bladder sphincter and many women suffer such mild bladder leakage with such occurrences as coughing, sneezing, exercise, either mild or moderate, laughing or anything else that will affect the pressure on the bladder. A surprisingly simple answer and treatment for this is both the use of the CO2 and Erbium vaginal lasers, to strengthen, tighten, firm and lift the vaginal wall, thus increasing the support of the bladder and significantly improving the symptoms of this bladder leakage of stress incontinence. Are the Lasers used in Gynaecology safe? These vaginal laser treatments have been successfully used throughout the world in the last three years or so and are gradually becoming much more common treatments in gynaecological centres. Surprisingly these lasers do not produce any pain or discomfort, or down time, or in any way long term risks. The procedure takes approximately twenty minutes, and normal vaginal intercourse can recommence within three to five days, following treatments. The treatment course generally consists of three treatments a month apart and maintenance treatments are usually required. These treatments can be performed for people of any age, but of course better results are achieved if attended to early, before the bladder leakage becomes more severe and chronic. Most people do not seek help for these symptoms as they consider it to be part of normal ageing and the result of childbirth. Where they do seek standard gynaecological care, the alternatives are much more complex, expensive and with varying levels of success. These include pelvic floor exercises, bladder training with physios, thereby various forms of gynaecological surgery, which are significantly invasive. How do I find out if the Vaginal Laser treatment is suitable for me? Gynaecological consultation appointments can be made with any of our gynaecologists, at Specialist Clinics of Australia. Consultations are initially performed and investigations included in our Gynaecology Centre include full history and examination and urodynamic studies and ultrasounds. This is a very scientific way of assessing the bladder condition and helping to diagnose the type of Incontinence and predict the outcome of treatments. The laser procedure can be performed in the same consultation treatment
8 Stress Incontinence session on some occasions or can be rebooked for a later date. Female Urinary Incontinence is an Untreated Condition for 50% of Sufferers As many as one in four of all sexually active women suffer some form of urinary incontinence, a debilitating, restrictive condition, particularly in women who have experienced vaginal childbirth. Contrary to common perception, urinary incontinence is not just an issue for older women who have lost muscle tone through ageing, but for a large and often silent majority of younger women (statistically up to 50% remain undiagnosed) who often silently accept the condition as a consequence of childbirth. Stretching and loss of elasticity, together with damage to the connective tissue of the pelvic floor, causes degrees of incontinence. Types of Female Incontinence Stress Incontinence (SI) is leakage caused by coughing, laughing or during physical exertion; urinary urge incontinence (UUI) or overactive bladder can be caused by damage to muscles or the nervous system and Mixed Urinary Incontinence (MUI) is a combination of both. Existing Alternative Treatments of Female Urinary Incontinence Conservative, first lines of treatment for UI are Kegel exercises to strengthen the pelvic floor muscles or electro or magnetic stimulation of pelvic floor muscles. Two types of surgical procedures, the TOT (trans-obturator tape) sling and the TVT (tension free vaginal tape) sling are commonly performed. A study comparing the two procedures found that 6 months after the procedure, the TOT had worked for 21 in 100 women compared with 45 in 100 for the TVT (ref 78) Er-YAG Laser treatment is delivered through the vagina, emitting microsecond long laser impulses which create a controlled temperature increase in the connective tissue of the vagina. The increased heating shrinks the collagen and mucosal tissue and the vaginal wall tightens. This process stimulates the body to naturally continue the tissue regeneration, reducing sagging of the vaginal walls as well as thickening and strengthening the vaginal mucosa, which in turn provides a stronger support for the bladder. Benefits of Er-YAG Laser treatment for SUI & MUI Average treatment time is 20 to30 minutes Painless procedure (almost no discomfort) with no hospitalisation or anaesthetic required Patients report improved sexual gratification due to tightening of vaginal walls The body s natural repair process continues for up to 6 months Patients can return to daily activities immediately (although advised to avoid sex and tampon use for a few days to a week) *Clinical Trials Testing Effectiveness of Er-YAG Laser Treatment procedure over a 12 month period involved 107 participants diagnosed with SUI or MUI. Participants had an average age of 50 years and 67 were diagnosed with SUI and 40 with MUI. Results after 6 months Of 51 patients with moderate to severe SUI, 45 remained dry, only 6 patients still had moderate SUI, 10 reported mild remaining SUI but none had severe SUI. Of the 40 patients with moderate to very
9 severe MUI only 7 reported remaining moderate or severe gravity MUI. 33 reported none or mild MUI.84 of 107 patients assessed the improvement of their UI after 6 months as excellent, 15 reported significant change and 8 reported mild to moderate UI improvement. No participants reported discomfort during the procedure or any adverse after effects. Stress Incontinence
10 Stress Vaginal Incontinence Atrophy Vaginal atrophy symptoms generally appear four to five years after the onset of menopause and affect up to 50% of post-menopausal women. A variety of VA symptoms manifest themselves, directly due to the cessation of the ovaries production of estrogen after menopause. Lack of estrogen in the vaginal mucosal lining and the subsequent frailty of the vaginal mucosa can cause symptoms of itchiness, decreased lubrication, pain (dyspareunia) and/ or vaginal bleeding during sexual intercourse, polyuria (excessive urination) and leukhorrea (vaginal discharge). In contrast to menopausal symptoms (hot flushes, night sweats, insomnia and mood swings) which are usually temporary, vaginal atrophy (VA) can negatively impact long term on quality of life, but despite this, only 25% of patients seek medical help. Although vaginal atrophy is considered a public health issue because it involves up to half the female population experiencing menopause, perception of the condition has been often underestimated, as a large percentage of women believed they must accept the condition as a natural consequence of bodily ageing. In 2014, with the exception of women in third world countries where women s health is a low priority, most women live more than a third of their lives after menopause, contrary to earlier times when life expectancy was considerably shorter for women. Today however, the demand for functional genital organ treatment post-menopause is increasing. The primary goal of VA treatment is to reduce symptoms and restore the normal physiological conditions of the vagina. As this condition has existed in women of post menopausal age over the centuries, various treatments ranging from direct application of traditional herbal and fruit treatments to electroshock and radiotherapy have been used in the past to try and improve the condition of the vagina and sexual functionality. Today s current therapies are wide ranging and include: Topical, non-hormonal lubricants and moisturisers which are usually the first line of treatment for patients experiencing symptoms of VA. Lubricants relieve vaginal dryness during sexual activity and don t provide a long term solution. Vaginal moisturisers may relieve VA symptoms by exerting some eutrophic (nutritional) effects on the vaginal mucosa. Local (vaginal) estrogen therapies that alleviate symptoms and are safe at very low doses for women who have only VA as a sole menopausal complaint. Hormone replacement therapy (HRT) which gives proven long term results in reducing VA but which can produce adverse side effects with extended use and may be a contributing factor in breast cancer. Surgical treatment of vaginal laxity and traditional plastic surgery for the correction of vulvo-vaginal alterations caused by pregnancy, hereditary factors or natural ageing. These procedures are invasive and have variable healing times and outcomes. Both laser procedures require no prior preparation by the patient as they are outpatient treatments needing no anaesthesia, with each session lasting up to 20 minutes. The special thermic effect caused by laser encourages renewed functional activity in the treated sections of tissue. This natural regeneration process continues after the 3 treatments have finished, with the vaginal mucosa naturally regenerating collagen and thus rolling back the years in the condition of the vagina. The greater majority of patients who have
11 undergone the procedure have reported considerable satisfaction with the ease of the procedure; the lessening of VA symptoms and the resulting improved sexual activity. Vaginal Atrophy
12 SPECIALIST CLINICS OF AUSTRALIA CONTACT US telephone website address 263 George Street, Sydney NSW 2000 clinic hours Monday - Friday 8.30am to 6pm
VAGINAL REJUVENATION
 VAGINAL REJUVENATION FOR ULTIMATE COMFORT AND CONFIDENCE LOTUS GYNOLASER ADVANCED AND RELIABLE Ageing, childbirth, illness and medication can affect you in many ways, but hidden problems can often be the
VAGINAL REJUVENATION FOR ULTIMATE COMFORT AND CONFIDENCE LOTUS GYNOLASER ADVANCED AND RELIABLE Ageing, childbirth, illness and medication can affect you in many ways, but hidden problems can often be the
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Guide to strengthening the pelvic floor muscles
 Exercise Cones Pelvic Exercise Made Easy Exercise Cones Pelvic Exercise Made Easy This system is clinically proven to strengthen the pelvic floor muscle to help with the control and prevention of stress
Exercise Cones Pelvic Exercise Made Easy Exercise Cones Pelvic Exercise Made Easy This system is clinically proven to strengthen the pelvic floor muscle to help with the control and prevention of stress
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Gynaecology Department Patient Information Leaflet
 Vaginal pessaries Gynaecology Department Patient Information Leaflet Introduction We have developed this information leaflet to answer some commonly-asked questions about what a vaginal pessary is, how
Vaginal pessaries Gynaecology Department Patient Information Leaflet Introduction We have developed this information leaflet to answer some commonly-asked questions about what a vaginal pessary is, how
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Treating your prolapse
 Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Year: Issue 1 Obs/Gyne The silent epidemic: Postmenopausal vaginal atrophy
 Year: 2013 - Issue 1 Obs/Gyne The silent epidemic: Postmenopausal vaginal atrophy By: Dr David W Sturdee, Immediate past President International Menopause Society and Hon Consultant Gynaecologist, Solihull
Year: 2013 - Issue 1 Obs/Gyne The silent epidemic: Postmenopausal vaginal atrophy By: Dr David W Sturdee, Immediate past President International Menopause Society and Hon Consultant Gynaecologist, Solihull
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Vaginal Tapes to Treat Stress Incontinence. Patient Information
 Vaginal Tapes to Treat Stress Incontinence Patient Information Author ID: JD Leaflet Number: Gyn 044 Version: 6 Name of Leaflet: Vaginal Tapes to Treat Stress Incontinence Date Produced: May 2017 Review
Vaginal Tapes to Treat Stress Incontinence Patient Information Author ID: JD Leaflet Number: Gyn 044 Version: 6 Name of Leaflet: Vaginal Tapes to Treat Stress Incontinence Date Produced: May 2017 Review
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Pessaries for vaginal prolapse. Information for patients Gynaecology
 Pessaries for vaginal prolapse Information for patients Gynaecology We have written this information to help explain the use of vaginal pessaries in the treatment of women with a vaginal prolapse. If you
Pessaries for vaginal prolapse Information for patients Gynaecology We have written this information to help explain the use of vaginal pessaries in the treatment of women with a vaginal prolapse. If you
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Bulkamid. Patient Information. Obstetrics & Gynaecology Department
 Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Inclusion Criteria Exclusion Criteria No of Patients included
 Table 1 Description of the studies included Inclusion and exclusion criteria and sample description Year First Author Country Type of UI Inclusion Criteria Exclusion Criteria No of Patients included Age
Table 1 Description of the studies included Inclusion and exclusion criteria and sample description Year First Author Country Type of UI Inclusion Criteria Exclusion Criteria No of Patients included Age
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
Stress. incontinence FACTS, ADVICE, AND EXERCISES.
 Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS.
 IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Patient Information. Tension Free Vaginal/ Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust
 Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
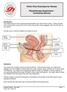 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy - Woman s Health Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. 2 Introduction Physiotherapists, doctors and nurses know that exercising
Pelvic Floor Exercises Physiotherapy - Woman s Health Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. 2 Introduction Physiotherapists, doctors and nurses know that exercising
MENOPAUSE - WHAT TO EXPECT CONCLUSION WEB LINKS
 NOTES CONCLUSION The average Canadian woman can expect to live to 80 years of age or older. This means you may live more than one-third of your life after menopause. Knowing what to expect and how to care
NOTES CONCLUSION The average Canadian woman can expect to live to 80 years of age or older. This means you may live more than one-third of your life after menopause. Knowing what to expect and how to care
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Vagina Dialogue. Laser Vaginal Rejuvenation
 Vagina Dialogue Sat, 2013 03 16 23:58 csb Esther Loh chats to two Singaporean plastic surgeons about making vaginas prettier and how to rectify vaginal laxity. After giving birth to several babies naturally,
Vagina Dialogue Sat, 2013 03 16 23:58 csb Esther Loh chats to two Singaporean plastic surgeons about making vaginas prettier and how to rectify vaginal laxity. After giving birth to several babies naturally,
Stress Urinary Incontinence in Women. What YOU can do about it...
 Stress Urinary Incontinence in Women What YOU can do about it... www.gynecare.com Stress Urinary Incontinence in Women: It's Common. It's Treatable. Would it surprise you... To learn that more than 13
Stress Urinary Incontinence in Women What YOU can do about it... www.gynecare.com Stress Urinary Incontinence in Women: It's Common. It's Treatable. Would it surprise you... To learn that more than 13
Your pelvic floor muscles
 Continence office Ballochmyle Suite, University Hospital Ayr Telephone 019 177 Your pelvic floor muscles Advice and exercise for women Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa
Continence office Ballochmyle Suite, University Hospital Ayr Telephone 019 177 Your pelvic floor muscles Advice and exercise for women Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Stress Incontinence. Susannah Elvy Urogynaecology CNS
 Stress Incontinence Susannah Elvy Urogynaecology CNS Definitions Prevalence Assessment Investigation Treatment Surgery Men International Continence Society define as the complaint of any involuntary leakage
Stress Incontinence Susannah Elvy Urogynaecology CNS Definitions Prevalence Assessment Investigation Treatment Surgery Men International Continence Society define as the complaint of any involuntary leakage
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
A Simple Solution. to a Common Problem. Find relief from sudden, unplanned urine leakage.
 A Simple Solution to a Common Problem Find relief from sudden, unplanned urine leakage. A Common Problem Millions of women suffer from stress urinary incontinence (SUI). This condition results in accidental
A Simple Solution to a Common Problem Find relief from sudden, unplanned urine leakage. A Common Problem Millions of women suffer from stress urinary incontinence (SUI). This condition results in accidental
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
The Leeds Teaching Hospitals NHS Trust Feminine care after pelvic radiotherapy
 n The Leeds Teaching Hospitals NHS Trust Feminine care after pelvic radiotherapy Information for patients This leaflet is designed to give you information about the late side-effects following radiotherapy
n The Leeds Teaching Hospitals NHS Trust Feminine care after pelvic radiotherapy Information for patients This leaflet is designed to give you information about the late side-effects following radiotherapy
Vaginal hysterectomy. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Vaginal hysterectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Vaginal hysterectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Laparoscopic Sacrohysteropexy
 Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
FemTouch Treatment for Improving Vulvovaginal Health
 FemTouch Treatment for Improving Vulvovaginal Health Dr. M. Marziali MD PhD in Gynecology and Obstetric Introduction Vulvovaginal atrophy (VVA) accompanies the natural aging of the vagina and affects up
FemTouch Treatment for Improving Vulvovaginal Health Dr. M. Marziali MD PhD in Gynecology and Obstetric Introduction Vulvovaginal atrophy (VVA) accompanies the natural aging of the vagina and affects up
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Gemcitabine and carboplatin (Breast)
 Gemcitabine and carboplatin (Breast) Gemcitabine and carboplatin (Breast) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy
Gemcitabine and carboplatin (Breast) Gemcitabine and carboplatin (Breast) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy
 Page 1 of 5 Menopause and the decision to replace hormones August FREE health seminars How MonaLisa Touch can help Microneedling Menopause and the decision to replace hormones Menopause is a much misunderstood
Page 1 of 5 Menopause and the decision to replace hormones August FREE health seminars How MonaLisa Touch can help Microneedling Menopause and the decision to replace hormones Menopause is a much misunderstood
Burch Colposuspension
 Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Laparoscopic Hysteropexy
 Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place.
 The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place. Think of it as the hammock of muscle that holds up your uterus, vagina, bladder, small intestine,
The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place. Think of it as the hammock of muscle that holds up your uterus, vagina, bladder, small intestine,
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Top 10 Tips Bladder Control
 Top 10 Tips Bladder Control for Your Personal Guide to a Sensitive Bladder Dr. Mache Seibel Leading authority on women s wellness and menopause Message from Dr. Mache Seibel Thank you for downloading this
Top 10 Tips Bladder Control for Your Personal Guide to a Sensitive Bladder Dr. Mache Seibel Leading authority on women s wellness and menopause Message from Dr. Mache Seibel Thank you for downloading this
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Tension Free vaginal tape. Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD
 Tension Free vaginal tape Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD What is a TVT procedure? A TVT (Tension Free Vaginal Tape) procedure is an operation
Tension Free vaginal tape Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD What is a TVT procedure? A TVT (Tension Free Vaginal Tape) procedure is an operation
Renewing Intimacy & Sexuality after Gynecologic Cancer
 Renewing Intimacy & Sexuality after Gynecologic Cancer foundationforwomenscancer.org Over 90,000 women are diagnosed with a gynecologic cancer each year. The challenge for a woman with cancer and her healthcare
Renewing Intimacy & Sexuality after Gynecologic Cancer foundationforwomenscancer.org Over 90,000 women are diagnosed with a gynecologic cancer each year. The challenge for a woman with cancer and her healthcare
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
International Journal of Women s Health Care
 Research Article International Journal of Women s Health Care Impact of Action II Petite Lady Laser Machine in the Treatment of Urinary Incontinence and Sexual Dysfunction in Female Najwa Alfarra 1 * and
Research Article International Journal of Women s Health Care Impact of Action II Petite Lady Laser Machine in the Treatment of Urinary Incontinence and Sexual Dysfunction in Female Najwa Alfarra 1 * and
Patient Information Incontinence & Prolapse Self-help
 Patient Information Incontinence & Prolapse Self-help Urogynaecology Introduction This leaflet is produced as a self-help guide for women of East and North Herts that are experiencing issues with continence.
Patient Information Incontinence & Prolapse Self-help Urogynaecology Introduction This leaflet is produced as a self-help guide for women of East and North Herts that are experiencing issues with continence.
New Treatments for Vaginal Health. Sarah Azad, MD El Camino Women s Medical Group
 New Treatments for Vaginal Health There s Hope Sarah Azad, MD El Camino Women s Medical Group The Genitrourinary Syndrome of Menopause (GSM) Problems with genital health secondary to the changes that occur
New Treatments for Vaginal Health There s Hope Sarah Azad, MD El Camino Women s Medical Group The Genitrourinary Syndrome of Menopause (GSM) Problems with genital health secondary to the changes that occur
Periurethral bulking injections for stress urinary incontinence
 n The Leeds Teaching Hospitals NHS Trust Periurethral bulking injections for stress urinary incontinence Information for patients Leeds Centre for Women s Health Urinary incontinence is the involuntary
n The Leeds Teaching Hospitals NHS Trust Periurethral bulking injections for stress urinary incontinence Information for patients Leeds Centre for Women s Health Urinary incontinence is the involuntary
Tips & Tricks for Usage
 Life. Not leaks. BLADDER SUPPORT FOR WOMEN Tips & Tricks for Usage Based on feedback from users and clinicians, here are some questions and answers that might help with using your uresta bladder support
Life. Not leaks. BLADDER SUPPORT FOR WOMEN Tips & Tricks for Usage Based on feedback from users and clinicians, here are some questions and answers that might help with using your uresta bladder support
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
What you should know about your diagnosis of incontinence
 What you should know about your diagnosis of incontinence What is Stress Urinary Incontinence? WHAT IS NORMAL URINARY FUNCTION? Urine is a normal waste product of the body that is manufactured by the kidneys
What you should know about your diagnosis of incontinence What is Stress Urinary Incontinence? WHAT IS NORMAL URINARY FUNCTION? Urine is a normal waste product of the body that is manufactured by the kidneys
Radiation Oncology Patient information. Radiation Therapy for gynaecological cancers
 Radiation Oncology Patient information Radiation Therapy for gynaecological cancers Radiation Therapy for gynaecological cancers 1 Radiation therapy for gynaecological cancers Gynaecological cancers include
Radiation Oncology Patient information Radiation Therapy for gynaecological cancers Radiation Therapy for gynaecological cancers 1 Radiation therapy for gynaecological cancers Gynaecological cancers include
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT
 URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
The Radiotherapy Department Radiotherapy for endometrium cancer Information for women
 The Radiotherapy Department Radiotherapy for endometrium cancer Information for women page 2 There are a number of treatments the doctor may use to treat your endometrial cancer. These include surgery,
The Radiotherapy Department Radiotherapy for endometrium cancer Information for women page 2 There are a number of treatments the doctor may use to treat your endometrial cancer. These include surgery,
POSTNATAL EXERCISES & ADVICE. Physiotherapy Department
 POSTNATAL EXERCISES & ADVICE Physiotherapy Department This booklet provides advice and exercises to help you to get back to normal after the birth or your baby. Rest: After having your baby it is important
POSTNATAL EXERCISES & ADVICE Physiotherapy Department This booklet provides advice and exercises to help you to get back to normal after the birth or your baby. Rest: After having your baby it is important
Radiotherapy to the pelvis for gynaecological cancers
 Radiotherapy to the pelvis for gynaecological cancers What happens next? In the clinic today, you and your doctor have agreed that you are going to have radiotherapy treatment for your cancer. This booklet
Radiotherapy to the pelvis for gynaecological cancers What happens next? In the clinic today, you and your doctor have agreed that you are going to have radiotherapy treatment for your cancer. This booklet
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Colposuspension for Stress Incontinence
 INFORMATION FOR PATIENTS Colposuspension for Stress Incontinence We advise you to take your time to read this leaflet, any questions you have please write them down on the sheet provided (towards the back)
INFORMATION FOR PATIENTS Colposuspension for Stress Incontinence We advise you to take your time to read this leaflet, any questions you have please write them down on the sheet provided (towards the back)
Outpatient Rehabilitation Services
 Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
GUIDE TO WOMEN S HEALTH
 GUIDE TO WOMEN S HEALTH Women s health According to the World Health Organisation (WHO) women outlive men by approximately 6 to 8 years on average and represent the majority of the population aged 85 or
GUIDE TO WOMEN S HEALTH Women s health According to the World Health Organisation (WHO) women outlive men by approximately 6 to 8 years on average and represent the majority of the population aged 85 or
Laser Treatment For Vaginal Health
 Laser Treatment For Vaginal Health Laser Treatment For Vaginal Health Indications Who is a candidate How it works Pre-treatment consult Preparing for your treatment What to expect after treatment Treatment
Laser Treatment For Vaginal Health Laser Treatment For Vaginal Health Indications Who is a candidate How it works Pre-treatment consult Preparing for your treatment What to expect after treatment Treatment
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Pelvic floor exercises for women
 Pelvic floor exercises for women The Continence Service Patient Information Leaflet Introduction Do any of these sound like you? I always leak urine when I do exercises. I cross my legs when I sneeze.
Pelvic floor exercises for women The Continence Service Patient Information Leaflet Introduction Do any of these sound like you? I always leak urine when I do exercises. I cross my legs when I sneeze.
Pelvic Floor Wand. Body-friendly Easy to use Designed for comfort
 Pelvic Floor Wand Body-friendly Easy to use Designed for comfort Kegel8 #GetAGrip Contents Welcome to Kegel8 What are Kegels? About Your Kegel8 Pelvic Floor Wand Getting Started Kegel8 Beginner s Exercise
Pelvic Floor Wand Body-friendly Easy to use Designed for comfort Kegel8 #GetAGrip Contents Welcome to Kegel8 What are Kegels? About Your Kegel8 Pelvic Floor Wand Getting Started Kegel8 Beginner s Exercise
