Patient selection for assisted reproductive technology treatments
|
|
|
- Stewart Mitchell
- 6 years ago
- Views:
Transcription
1 Patient selection for assisted reproductive technology treatments LP Cheung Assisted reproductive technology refers to procedures in which the oocyte is handled or manipulated in vitro before replacement, either as an oocyte or an embryo. Because of rapid advances in this area, infertile couples may seek direct referral for assisted reproductive treatments, instead of trying simpler measures such as ovulation induction and intrauterine insemination. It is important to establish whether these conventional infertility treatments are appropriate, as such treatments are generally safer, less stressful, and more affordable. On the other hand, subjecting infertile couples to unnecessary delay by offering inappropriate treatments for example, ovulation induction for tubal infertility or intrauterine insemination for severe male-factor infertility would reduce the overall chance of success because of the age-related decline in female fecundity. The choice of infertility treatments thus depends on a balance of factors: the chance of pregnancy without treatment; the chance with simpler and safer, but less successful, infertility treatments; or the chance with the more complex and costly, but more effective, assisted reproductive treatments. The factors that should be taken into consideration include the age of the woman, the duration of infertility, the causes of infertility, the availability and cost of alternative treatments, and most importantly the acceptability. HKMJ 2000;6: Key words: Fertilization in vitro; Infertility/diagnosis; Infertility/therapy; Patient selection; Pregnancy rate; Reproduction techniques Introduction Infertility is defined as the failure by a couple of reproductive age to conceive after 12 months or more of regular coitus without using contraception. This definition is based on epidemiological studies, which have shown that 80% of couples in the general population normally conceive by that stage. 1 It is estimated that 15% of couples living in developed countries are infertile. 2 There has been no major change in prevalence, but there has been an increase in demand for treatment during the past decade because of the perception that effective assisted reproductive technology (ART) treatments are now available. Table 1 summarises the ART procedures that are most commonly practised throughout the world. Although ART was initially developed for patients with tubal infertility, it is currently used for almost all Department of Obstetrics and Gynaecology, The Chinese University of Hong Kong, Prince of Wales Hospital, Shatin, Hong Kong LP Cheung, MRCOG, FHKAM (Obstetrics and Gynaecology) Correspondence to: Dr LP Cheung kinds of infertility problem, because its success rates are expected to be higher than those of conventional treatments. However, ART treatment also has disadvantages. It involves greater expense, and potentially serious complications such as ovarian hyperstimulation syndrome and multiple pregnancies can occur. There are also fears that drugs that induce ovulation may increase the risk of ovarian cancer. Infertility treatment should therefore be individualised to avoid subjecting couples to unnecessary risks due to overtreatment, such as the unnecessary use of ART treatments, or to inappropriate delay because of undertreatment. Table 2 summarises common infertility treatments and their indications. It should be emphasised that the choice of treatment is also influenced by other factors such as the age of the woman and the duration of infertility. The age of the female partner is one of the most important factors determining spontaneous fertility. It is also a major factor in determining the success of any form of infertility treatment. Using the database established in 1991 by the Human Fertilisation and Embryology Authority, Templeton et al 3 analysed in vitro fertilisation (IVF) cycles that HKMJ Vol 6 No 2 June
2 Cheung Table 1. Common assisted reproductive technology procedures Type of assisted reproductive technology In vitro fertilisation Gamete intrafallopian transfer Intracytoplasmic sperm injection Microsurgical epididymal sperm aspiration Testicular sperm extraction Frozen embryos Procedure A four-stage procedure, which includes controlled ovarian hyperstimulation, oocyte retrieval under transvaginal ultrasound guidance, fertilisation with sperm in vitro, and embryo replacement into the uterus Similar to in vitro fertilisation, except that the oocytes and sperm are injected into the fallopian tube under laparoscopic guidance and fertilisation take places within the body A single sperm is injected directly into the oocyte to facilitate fertilisation; at least a few viable sperm must be present in the ejaculate, epididymis, or testis For treatment of obstructive azoospermia when no sperm are found in the ejaculate; sperm are directly recovered from the epididymis through needle aspiration For treatment of obstructive or non-obstructive azoospermia when no sperm are found in the ejaculate or the epididymis; sperm are directly recovered from the testis through open biopsy Excess embryos (more than the numbers required for transfer) can be frozen and stored in liquid nitrogen for future use Table 2. Common infertility treatments and their indications Infertility treatment Ovulation induction alone Intrauterine insemination alone Ovulation induction and intrauterine insemination Gamete intrafallopian transfer In vitro fertilisation Intracytoplasmic sperm injection Oocyte donation Indications Anovulation Coital problems, immunological factors, cervical factors, borderline male factors Unexplained infertility, minimal-to-mild endometriosis, borderline male factors Unexplained infertility, minimal-to-mild endometriosis Tubal infertility, moderate-to-severe endometriosis, male-factor infertility, failure of other treatments Severe male-factor infertility, previous fertilisation failure Primary or secondary ovarian failure, familial genetic disorders, repeated ART failure were performed in the United Kingdom. They found a marked decline in pregnancy rates in women older than 35 years, and no pregnancies were recorded for women older than 45 years except in the oocyte donation programme. It seems that although young patients in their 20s may have the option to use safer but only moderately effective treatments, by their late 30s, treatment should be more aggressive. On the other hand, aggressive infertility treatments should be discouraged in women in their 40s because of poor success rates. The duration of infertility is another major factor determining the likelihood of spontaneous pregnancy in untreated infertile couples. 4 As most infertility is not absolute but includes some degree of subfertility, many couples have a background chance of conceiving naturally. The longer the duration of infertility, however, the less likely is that probability. This predictive value is of particular importance to couples with unexplained infertility. Even in normal couples with proven fertility, the average monthly conception rate is only 20% to 25%. The peak rate is 33% in the first month of trying, falling rapidly to approximately 5% each month thereafter. 5 The expectation of any infertility treatment must be judged against this finding. Infertility treatment should be offered when the chance of conceiving naturally is unacceptably low (<1% to 2% per cycle or 20% to 30% after 2 years). 6 Simple treatments such as ovulation induction and intrauterine insemination (IUI) are suitable only in certain situations (Table 2) and will be expected to achieve a pregnancy rate of approximately 10% per cycle. Assisted reproductive techniques are suitable for almost all kinds of infertility problems, but treatment with even the most advanced ART is expected to achieve only a 25% to 30% success rate per cycle. Treatment may need to be repeated several times before success is achieved. As a constant rise in the cumulative pregnancy rates during the six initial 178 HKMJ Vol 6 No 2 June 2000
3 Couple presents with infertility General advice: stop smoking and drinking History and examination of both partners Exclude coital difficulties Female partner Rubella antibody status Measure levels of follicle-stimulating hormone, luteinizing hormone, and oestradiol on day 3 of cycle Measure prolactin level and thyroid function test if cycles are irregular Confirm ovulation with basal body temperature chart or the level of mid-luteal phase progesterone Laparoscopy with chromotubation or hysterosalpingography Male partner Semen analysis Repeat semen analysis if the first result is abnormal Severe semen abnormality Borderline semen abnormality Genetic counselling Anovulatory problems Endometriosis* Tubal infertility* Minimal-to-mild Moderate-to-severe Ovulation induction Ovulation induction + intrauterine insemination Gamete intrafallopian transfer In vitro fertilisation In vitro fertilisation + intracytoplasmic sperm injection Intrauterine insemination Unexplained infertility of >3 years * Surgical treatment of endometriosis and tubal infertility is not shown Fig. The investigation and management of the infertile couple cycles has been demonstrated, 7 in general it is worth pursuing treatment for up to six cycles. Before an infertile couple is recruited into an IVF programme, they should be warned that both the cumulative pregnancy and live-birth rates decline with the age of the woman. Tan et al 8 have reported that the cumulative pregnancy and live-birth rates after five IVF cycles were 54% and 45%, respectively, at age <35 years, 38.7% and 28.9% at 35 to 39 years, and 20.2% and 14.4% at age 40 years. 8 The stress, time away from work, cost, and complications of the treatment should also be emphasised. Alternatives such as adoption or childlessness should be discussed. Patient acceptability is very important, but it is often neglected during the infertility evaluation. Infertility evaluation The Figure summarises the investigation and management of an infertile couple. The cornerstone of any infertility evaluation relies on the assessment of coital difficulties, cervical or immunological factors, ovulation, tuboperitoneal pathology, and semen quality. Assessment of coital, cervical, or immunological problems Coital difficulties should be recognised if a detailed sexual history is obtained. Cervical or immunological factors need to be considered when results from postcoital tests are repeatedly negative. Further investigations to detect antibodies against components of sperm are then necessary. The use of systemic corticosteriods to treat men who have anti-sperm antibodies is not recommended, as the evidence of benefit is conflicting and there are potentially serious side effects such as aseptic hip necrosis. 9 Treatment using IUI with or without ovarian stimulation can bypass the problem of sperm progression through cervical mucus. However, ART should be considered after repeated failure of IUI treatments. Assessment of ovulation A detailed menstrual, medical, and drug history should be obtained. Women with normal regular menstrual cycles of 28 to 30 days are usually ovulating. Simple assessments such as a biphasic pattern of the basal body temperature chart or an appropriate rise of the HKMJ Vol 6 No 2 June
4 Cheung midluteal serum progesterone concentration provide presumptive evidence of ovulation. In patients with suspected anovulation, the following tests should be performed: measurement of the levels of follicle-stimulating hormone (FSH), luteinizing hormone (LH), oestradiol, and testosterone (all samples having been taken at early follicular phase before day 5 of the cycle), as well as the prolactin level and the thyroid function test. After excluding any secondary medical or endocrine causes, anovulatory problems are usually categorised under four conditions. 10 Hyperprolactinaemic anovulation Patients with hypergonadotrophic anovulation may present with galactorrhoea. If a serum prolactin concentration confirms hyperprolactinaemia, investigations to exclude a pituitary adenoma and hypothyroidism are performed. These tests comprise computerised tomography or magnetic resonance imaging of the pituitary gland and the thyroid function test. Taking a detailed drug history is also important, because the use of some commonly prescribed drugs such as phenothiazine, haloperidol, metoclopramide, cimetidine, and methyldopa is associated with hyperprolactinaemia. The first-line treatment is the use of dopamine agonists such as bromocriptine. These drugs can be combined with anti-oestrogens, if ovulation does not occur despite normalised prolactin concentrations. 11 Hypogonadotrophic anovulation The causes of hypogonadotrophic hypogonadism are often functional and transient. Anovulation may be stress-induced or related to weight loss or excessive exercise. An organic cause should be excluded, however, particularly if there are neurological symptoms. The evidence for hypogonadotrophic hypogonadism is a low level of FSH, LH, and oestrogen, and the absence of withdrawal bleeding after a progesterone challenge test. The primary aim of treatment should be to correct the underlying cause. It has been shown that spontaneous ovulation will return in underweight women after correction of their nutritional deficiency. 12 Anti-oestrogens are not effective in this condition, owing to the non-functioning hypothalamic-pituitaryovarian axis. Ovulation induction should be achieved by using either a pulsatile gonadotrophin-releasing hormone (GnRH) or gonadotrophins in a specialist infertility centre, in which the woman is intensively monitoring during ovulation induction. Hypergonadotrophic anovulation Hypergonadotrophic anovulation implies ovarian resistance or failure and is diagnosed when plasma concentrations of FSH are higher than 20 IU/L from repeated measurements. If the patient is younger than 40 years, this condition should be further investigated and treated as a premature menopause. The only effective practical treatment for hypergonadotrophic anovulation is oocyte donation. Normogonadotrophic anovulation Patients with normogonadotrophic anovulation have normal FSH concentrations, but LH concentrations may be elevated. They are not hypo-oestrogenic and will bleed in response to a progesterone withdrawal test. The majority of these women have polycystic ovaries. 13 This condition should be suspected if the woman is obese and hirsute, or if there is hyperandrogenaemia or an elevated LH to FSH ratio. 13 Polycystic ovaries can be diagnosed using ultrasonography. Apart from weight loss in obese normogonadotrophic anovulation patients, 14 the first-line treatment is the use of anti-oestrogens such as colmifene (clomiphene) citrate. The starting dose of clomifene is 50 mg/d for 5 days, from day 2 to day 6 of each cycle. The dosage can be increased in monthly increments up to 200 mg/d. Early referral to specialist infertility centres should be considered if patients are still anovulatory at the maximum dosage (clomifene resistance) or if there is failure to conceive after 12 cycles of successful treatment with confirmation of ovulation (clomifene failure). The alternatives for patients with clomifene resistance polycystic ovarian disease are either medical induction of ovulation with pulsatile GnRH or gonadotrophins, or surgical treatment with ovarian wedge resection or laparoscopic ovarian drilling. Medical treatments provide a good cumulative pregnancy rate, but they increase the risk of multiple pregnancies and ovarian hyperstimulation. 10 The spontaneous ovulation rate after surgical treatment is reported to be 60% to 80%, 15,16 but the efficacy in terms of pregnancy and the ovarian damage associated with the procedure has yet to be evaluated. 17 Assessment and treatment of tuboperitoneal disease Tubal damage and pelvic adhesions may result from pelvic inflammatory disease, or may be secondary to endometriosis or previous lower abdominal or pelvic surgery. There is still debate regarding the appropriate time for testing tubal patency. Early investigation for tuboperitoneal pathology should be undertaken when there is a suspicious history or the presence of symptoms such as dysmenorrhoea or dyspareunia. However, in low-risk patients, the common practice is to delay a test of tubal patency until there have 180 HKMJ Vol 6 No 2 June 2000
5 been up to six to12 ovulatory cycles. This approach has been challenged, however, as pelvic infection or endometriosis can be completely silent. Serological tests for Chlamydia trachomatis infection have been suggested as a simple screening method for unsuspected previous infection, which would indicate likely tubal damage. 18 Early laparoscopy is then indicated in seropositive women. 19 Methods used to assess tubal patency include laparoscopy with chromotubation, or hysterosalpingography. The latter technique may be used as a screening test for tubal patency in low-risk patients. However, laparoscopy with chromotubation should be the preferred method of investigation, particularly when there is a strong suspicion of peritoneal disease. Laparoscopy may also be necessary when there is a hysterosalpingogram showing suspected falsepositive results due to tubal spasm or during planning for infertility surgery. The two choices for the treatment of tubal infertility are tubal surgery or IVF. In general, pregnancy rates after tubal surgery are not as good as those achieved by IVF. The overall 2-year cumulative pregnancy rate after tubal surgery is only 20%, 20 which can now be expected in a single cycle of IVF treatment. Tubal surgery may still be appropriate in carefully selected cases, because different types of tubal surgery have different prognoses. Surgery may be offered in cases of mild pelvic adhesions, proximal tubal obstruction, or mild distal tubal disease, although the eventual chance of pregnancy after 2 years is not much more than 50%. 20 Hence, if a pregnancy has not occurred within 12 months (at most 24 months) of tubal surgery, IVF should be offered. Owing to the poor prognosis of tubal surgery, IVF should be the first-line treatment for significant pelvic adhesions or moderate-to-severe distal tubal disease. 20 Early referral for IVF is also necessary for women of advanced age or when coexisting problems such as male-factor infertility are present. Endometriosis-associated infertility Endometriosis, even of a minor degree, is associated with marked subfertility. 6 Medical treatment of endometriosis has no proven benefit in infertility. 21,22 On the contrary, the chance of pregnancy is delayed by the duration of medical treatment. Surgical ablation of minimal-to-mild endometriosis has been shown to improve fertility in subfertile women, 23 so this should be considered at the time of a diagnostic laparoscopy. Ovulation induction by using IUI should be offered to patients with minimal-to-mild endometriosis if the duration of infertility is more than 3 years, as studies have shown that ovulation induction with IUI is more effective than either no treatment or IUI alone. 24 There is no evidence that medical treatment of moderate-to-severe endometriosis either alone or as an adjunct to surgery improves fertility. 21,22 Surgical treatment of moderate-to-severe endometriosis has been shown to improve fertility, but a full explanation of the high surgical risk should be given. 22,25 In vitro fertilisation should also be offered as an alternative to or following unsuccessful surgery. 9 Semen quality and the treatment of male-factor infertility Table 3 lists the criteria of the World Health Organization (WHO) for normal semen characteristics. 26 It has been estimated that less than 10% of male-factor infertility is amenable to conventional medical or surgical treatments. Referral for IUI or ART procedures should be considered if there are two abnormal semen samples that have been taken at least 3 months apart. 26 In patients with borderline semen abnormality, sperm preparation for IUI may correct the abnormality, but a minimum of 10 million motile sperm per whole sample is still required. For a severe semenfactor (sperm concentration <10 million spermatozoa per millilitre; or <20% motility; or <20% normal forms) or when there is history of fertilisation failure, IVF and intracytoplasmic sperm injection (ICSI) should be the primary treatment option. 27 With the Table 3. World Health Organization criteria for normal semen characteristics 26 Characteristic Value Volume 2.0 ml ph Sperm concentration 20 x 10 6 spermatozoa per ml Motility 50% with forward progression, or 25% with rapid progression Morphology 30% with normal forms Vitality 75% live, ie excluding dye White blood cells <1 x 10 6 /ml Immunobead test <20% spermatozoa with adherent particles Mixed antiglobulin reaction test <10% spermatozoa with adherent particles HKMJ Vol 6 No 2 June
6 Cheung introduction of ICSI, which requires only a single sperm to be injected per oocyte, it is now possible to use epididymal or testicular sperm even when there are no sperm in the ejaculate. Epididymal sperm can be obtained by performing microsurgical epididymal sperm aspiration in men with obstructive azoospermia. Alternatively, testicular sperm can be obtained by using testicular sperm extraction in men with nonobstructive azoospermia. It is thus worthwhile referring affected couples to specialist infertility centres for urological assessment and, if necessary, to perform sperm recovery and ICSI. However, prior to offering any treatment to these couples, particular consideration should be given to the relevant genetic issues. Increasing evidence has suggested a genetic linkage to reproductive failure in 10% to 30% of men with severe oligoasthenoteratospermia. 28 Accordingly, these patients should be counselled about the possibility of transmitting sex chromosomal aberrations or fertility problems to their offspring before they are recruited into the ICSI programmes. 22,29 Unexplained infertility In 20% of couples presenting with infertility, a detailed history and examination followed by complete investigation will fail to elicit any clear explanation for the couple s problem. The main factors determining the chance of conceiving naturally are the duration of infertility, the woman s age and the previous pregnancy history. 4,30 As the spontaneous conception rate only starts to significantly decrease after 3 years of trying, 30 conservative management until then could be considered, taking into account the woman s age. 9 There is no evidence of any benefit from clomifene treatment, 31 and assisted conception should wait, except when the female partner is in her late 30s. After more than 3 years of infertility, the chances of natural conception are negligible. 30 Ovulation induction with IUI is a simple and moderately effective treatment, 32 and in general it is worth pursuing for up to six cycles of treatment, before considering ART. The advantage of this approach is that the risks associated with ART are avoided, particularly those relating to oocyte retrieval. Both gamete intrafallopian transfer and IVF are effective ART treatments in couples with unexplained infertility; both methods have similar efficacies. 33 In centres where IVF laboratories are available, however, IVF is the preferred method, because of the additional information it provides on fertilisation, which may be defective for couples with unexplained infertility. Furthermore, performing IVF avoids the anaesthetic and operative risks of laparoscopy. 9 Conclusion The main indications for assisted reproductive procedures include tubal disease, endometriosis, male infertility, and prolonged unexplained infertility. Assisted reproductive technology treatments are offered when the chance of conceiving by other means is unacceptably low or the women s age leaves insufficient time for other treatments. The major factor adversely affecting the success of ART is advanced female age, so early referral to specialist infertility centres should be considered, especially for women older than 35 years. On the other hand, aggressive ART treatment should be discouraged in women in their 40s, as the chance of success is often unrealistic except in oocyte donation programmes. References 1. Shaw R, Soutter P, Stanton S. Gynaecology. In: Thompson R, Heasley RN, editors. Investigation of the infertile couple. New York: Churchill Livingstone;1992: Jewelewicz R, Wallack EE. Evaluation of the infertile couple. In: Wallach EE, Zacur HA, editors. Reproductive medicine and surgery. St Louis (MO): Mosby Yearbook;1995: Templeton A, Morris JK, Parslow W. Factors that affect outcome of in vitro fertilisation treatment. Lancet 1996;348: Collins JA, Burrows EA, Willan AR. The prognosis for live birth among untreated infertile couples. Fertil Steril 1995; 64: Spira A. Epidemiology of human reproduction. Hum Reprod 1986;1: Hull MG. Infertility treatment: relative effectiveness of conventional and assisted conception methods. Hum Reprod 1992;7: Dor J, Seidman DS, Ben-Shlomo I, Levran D, Ben-Rafael Z, Mashiach S. Cumulative pregnancy rate following in-vitro fertilization: the significance of age and infertility aetiology. Hum Reprod 1996;11: Tan SL, Royston P, Campbell S, et al. Cumulative conception and livebirth rates after in-vitro fertilisation. Lancet 1992;339: The Guideline Development Group, Royal College of Obstetricians and Gynaecologists, UK. The management of infertility in secondary care. London: RCOG Press; The ESHRE Capri Workshop Group. Anovulatory infertility. Hum Reprod 1995;10: Diamant YZ, Yarkoni S, Evron S. Combined clomiphenebromocriptine treatment in anovulatory, oligomenorrhoeic and hyperprolactinaemic women resistant to separate clomiphene or bromocriptine regimens. Infertility 1980;3: The ESHRE Capri Workshop. Female infertility: treatment options for complicated cases. Hum Reprod 1997;12: Adams J, Franks S, Polson DW, et al. Multifollicular ovaries: clinical and endocrine features and response to pulsatile gonadotropin-releasing hormone. Lancet 1985;2: Clark AM, Ledger W, Galletly C, et al. Weight loss results in significant improvement in pregnancy and ovulation rates in anovulatory obese women. Hum Reprod 1995;10: HKMJ Vol 6 No 2 June 2000
7 15. Adashi EY, Rock JA, Guzick D, Wentz AC, Jones GS, Jones HW. Fertility following bilateral ovarian wedge resection: a critical analysis of 90 consecutive cases of the polycystic ovary syndrome. Fertil Steril 1981;36: Armar A, Lachelin G. Laparoscopic ovarian diathermy: an effective treatment for anti oestrogen resistant anovulatory infertility in women with PCOS. Br J Obstet Gynaecol 1993; 100: Dabirashrafi H, Mohamad K, Behjatnia Y, Moghadami-Tabrizi N. Adhesion formation after ovarian electrocoagulation on patients with PCO syndrome. Fertil Steril 1991;55: Mol BW, Dijkman B, Wertheim P, et al. The accuracy of serum chlamydial antibodies in the diagnosis of tubal pathology: a meta-analysis. Fertil Steril 1997;67: Conway D, Glazener CM, Caul EO, et al. Chlamydial serology in fertile and infertile women. Lancet 1984; 1(8370): Hull MG, Fleming CF. Tubal surgery versus assisted reproduction: assessing their role in infertility therapy. Curr Opin Obstet Gynecol 1995;7: Farquhar C, Sutton C. The evidence for the management of endometriosis. Curr Opin Obstet Gynecol 1998;10: Hughes EG, Fedorkow DM, Collins A. A quantitative overview of controlled trials in endometriosis-associated infertility. Fertil Steril 1993;59: Marcoux S, Maheux R, Berube S, Canadian Collaborative Group on Endometriosis. Laparoscopic surgery in infertile women with minimal or mild endometriosis. N Engl J Med 1997;337: Chaffkin LM, Nulsen JC, Luciano AA, Metzger DA. A comparative analysis of the cycle fecundity rates associated with combined human menopausal gonadotropin (hmg) and intrauterine insemination (IUI) versus either hmg or IUI alone. Fertil Steril 1991;55: Adamson GD, Pasta DJ. Surgical treatment of endometriosisassociated fertility: meta-analysis compared with survival analysis. Am J Obstet Gynecol 1994;171: World Health Organization. WHO laboratory manual for the examination of human semen and sperm cervical mucus interaction. 4th ed. Cambridge: Cambridge University Press; Hull MG. Effectiveness of infertility treatment: choice and comparative analysis. International J Gyneocol Obstet 1994; 47: Johnson MD. Genetic risks of intracytoplasmic sperm injection in the treatment of male infertility: recommendations for genetic counseling and screening. Fertil Steril 1998;70: Chandley AC, Hargreave TB. Genetic anomalies and ICSI. Hum Reprod 1996;11: Collins JA, Rowe TC. Age of the female partner is a prognostic factor in prolonged unexplained infertility: A multicenter study. Fertil Steril 1989;52: Fujii S, Fukui A, Fukushi Y, Kagiya A, Sato S, Saito Y. The effects of clomiphene citrate on normally ovulatory women. Fertil Steril 1997;68: Hughes EG. The effectiveness of ovulation induction and intrauterine insemination in the treatment of persistent fertility: a meta-analysis. Hum Reprod 1997;12: Leeton J, Healy D, Rogers P. A controlled study between the use of gamete intrafallopian transfer (GIFT) and in vitro fertilisation and embryo transfer in the management of idiopathic and male infertility. Fertil Steril 1987;48: HKMJ Vol 6 No 2 June
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Infertility. Thomas Lloyd and Samera Dean
 Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
Infertility. Review and Update Clifford C. Hayslip MD Intrauterine Inseminations
 Infertility Review and Update Clifford C. Hayslip MD Intrauterine Inseminations Beneficial effects of IUI not consistently documented in studies No deleterious effects on fertility 3-4 cycles of IUI should
Infertility Review and Update Clifford C. Hayslip MD Intrauterine Inseminations Beneficial effects of IUI not consistently documented in studies No deleterious effects on fertility 3-4 cycles of IUI should
Fertility. Assessment and treatment for people with fertility problems. Issued: February NICE clinical guideline 156. guidance.nice.org.
 Fertility Assessment and treatment for people with fertility problems Issued: February 2013 NICE clinical guideline 156 guidance.nice.org.uk/cg156 NICE has accredited the process used by the Centre for
Fertility Assessment and treatment for people with fertility problems Issued: February 2013 NICE clinical guideline 156 guidance.nice.org.uk/cg156 NICE has accredited the process used by the Centre for
Intrauterine (IUI) and Donor Insemination (DI) Policy (excluding In vitro fertilisation (IVF) & Intracytoplasmic sperm injection (ICSI) treatment)
 Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Subfertility B Y A L I S O N, B E N A N D J O H N
 Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
Clinical guideline Published: 20 February 2013 nice.org.uk/guidance/cg156
 Fertility problems: assessment and treatment Clinical guideline Published: 20 February 2013 nice.org.uk/guidance/cg156 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Fertility problems: assessment and treatment Clinical guideline Published: 20 February 2013 nice.org.uk/guidance/cg156 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Neil Goodman, MD, FACE
 Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Infertility DR. RAHUL BEVARA
 Infertility DR. RAHUL BEVARA Definitions Infertility is defined as the inability to conceive after one year of unprotected coitus. Affects 10-15% of couples Primary Infertility, that is inability to conceive
Infertility DR. RAHUL BEVARA Definitions Infertility is defined as the inability to conceive after one year of unprotected coitus. Affects 10-15% of couples Primary Infertility, that is inability to conceive
Understanding Infertility, Evaluations, and Treatment Options
 Understanding Infertility, Evaluations, and Treatment Options Arlene J. Morales, M.D., F.A.C.O.G. Fertility Specialists Medical Group, Inc. What We Will Cover Introduction What is infertility? Briefly
Understanding Infertility, Evaluations, and Treatment Options Arlene J. Morales, M.D., F.A.C.O.G. Fertility Specialists Medical Group, Inc. What We Will Cover Introduction What is infertility? Briefly
Fertility Assessment and Treatment Pathway
 Rejected referrals sent back to GP Fertility Assessment and Treatment Pathway Patients with fertility problems go to the GP GP Advice and Assessment GP to inform patient of access criteria for NHS-funded
Rejected referrals sent back to GP Fertility Assessment and Treatment Pathway Patients with fertility problems go to the GP GP Advice and Assessment GP to inform patient of access criteria for NHS-funded
Assisted Reproduction. By Dr. Afraa Mahjoob Al-Naddawi
 Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Treating Infertility
 Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Interim Clinical Commissioning Policy: Assisted Conception. Agreed: September 2013 Reference: N-SC/037. England
 Interim Clinical Commissioning Policy: Assisted Conception Agreed: September 2013 Reference: N-SC/037 England 1 Interim Clinical Commissioning Policy Assisted Conception First published: November 2013
Interim Clinical Commissioning Policy: Assisted Conception Agreed: September 2013 Reference: N-SC/037 England 1 Interim Clinical Commissioning Policy Assisted Conception First published: November 2013
Fertility in the 21 st Century Dr Leigh Searle
 Fertility in the 21 st Century Dr Leigh Searle Fertility Specialist, Obstetrician, Gynaecologist FRANZCOG, PGDipOMG, MBChB Dr Kate Van Harselaar Fertility Specialist, Obstetrician and Gynaecologist Overview
Fertility in the 21 st Century Dr Leigh Searle Fertility Specialist, Obstetrician, Gynaecologist FRANZCOG, PGDipOMG, MBChB Dr Kate Van Harselaar Fertility Specialist, Obstetrician and Gynaecologist Overview
Evaluation of the Infertile Couple
 Overview and Definition Infertility is defined as the inability of a couple to fall pregnant after one year of unprotected intercourse. Infertility is a very common condition as in any given year about
Overview and Definition Infertility is defined as the inability of a couple to fall pregnant after one year of unprotected intercourse. Infertility is a very common condition as in any given year about
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
INFERTILITY CAUSES. Basic evaluation of the female
 INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
Fertility assessment and assisted conception
 Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Unexplained Infertility
 Unexplained Infertility Kaylen M. Silverberg, M.D. Thomas C. Vaughn, M.D. Texas Fertility Center Austin, Texas Introduction Infertility is generally defined as the inability to conceive following one year
Unexplained Infertility Kaylen M. Silverberg, M.D. Thomas C. Vaughn, M.D. Texas Fertility Center Austin, Texas Introduction Infertility is generally defined as the inability to conceive following one year
5/5/2010. Infertility FINANCIAL DISCLOSURE. Infertility Definition. Objectives. Normal Human Fertility. Normal Menstrual Cycle
 Infertility FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology I AM RECEIVING COMPENSATION
Infertility FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology I AM RECEIVING COMPENSATION
Infertility. F r e q u e n t l y A s k e d Q u e s t i o n s. Q: What causes infertility in men? A: Infertility in men is most often caused by:
 Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Infertility. Dafydd Ywain & Kayleigh Hansen
 Infertility Dafydd Ywain & Kayleigh Hansen Terminology Epidemiology Aetiology Male infertility Female infertility Conclusion Content Terminology Fecundability The probability of conceiving during a single
Infertility Dafydd Ywain & Kayleigh Hansen Terminology Epidemiology Aetiology Male infertility Female infertility Conclusion Content Terminology Fecundability The probability of conceiving during a single
Recent Developments in Infertility Treatment
 Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Fertility Assessment and Treatment Pathway
 Fertility Assessment and Treatment Pathway Rejected referrals sent back to GP Patients with fertility problems go to the GP GP Advice and Assessment GP to inform patient of access criteria for NHS-funded
Fertility Assessment and Treatment Pathway Rejected referrals sent back to GP Patients with fertility problems go to the GP GP Advice and Assessment GP to inform patient of access criteria for NHS-funded
Fertility 101. About SCRC. A Primary Care Approach to Diagnosing and Treating Infertility. Definition of Infertility. Dr.
 Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
EVALUATING THE INFERTILE PATIENT-COUPLES. Stephen Thorn, MD
 EVALUATING THE INFERTILE PATIENT-COUPLES Stephen Thorn, MD Overview The field of reproductive medicine continues to evolve rapidly by offering newer diagnostic testing and therapeutic options to improve
EVALUATING THE INFERTILE PATIENT-COUPLES Stephen Thorn, MD Overview The field of reproductive medicine continues to evolve rapidly by offering newer diagnostic testing and therapeutic options to improve
Complete failure of fertilization in couples with unexplained infertility: implications for subsequent in vitro fertilization cycles
 r FERTILITY AND STERILITY Copyright ~ 1993 The American Fertility Society Printed on acid-free paper in U.S.A. Complete failure of fertilization in couples with unexplained infertility: implications for
r FERTILITY AND STERILITY Copyright ~ 1993 The American Fertility Society Printed on acid-free paper in U.S.A. Complete failure of fertilization in couples with unexplained infertility: implications for
COMMISSIONING POLICY. Tertiary treatment for assisted conception services
 Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Current Evidence On Infertility Treatment
 Current Evidence On Infertility Treatment Mahmoud A.M. Abdel-Aleem Regina Kulier WHO/GFMER 2003 Problem of Infertility It is a state in which a couple, desirous of a child, cannot conceive after 12 months
Current Evidence On Infertility Treatment Mahmoud A.M. Abdel-Aleem Regina Kulier WHO/GFMER 2003 Problem of Infertility It is a state in which a couple, desirous of a child, cannot conceive after 12 months
Director of Commissioning, Telford and Wrekin CCG and Shropshire CCG. Version No. Approval Date August 2015 Review Date August 2017
 Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services, in Shropshire and Telford and Wrekin Owner(s) Version No. Director of
Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services, in Shropshire and Telford and Wrekin Owner(s) Version No. Director of
Infertility: A Generalist s Perspective
 Infertility: A Generalist s Perspective Learning Objectives Fertility and Lifestyle: Patient education Describe the basic infertility workup Basic treatment strategies unexplained Heather Huddleston, MD
Infertility: A Generalist s Perspective Learning Objectives Fertility and Lifestyle: Patient education Describe the basic infertility workup Basic treatment strategies unexplained Heather Huddleston, MD
Infertility. Rhian Allen & David Rogers.
 Infertility Rhian Allen & David Rogers http://www.worldofsurrogacy.com Objectives Definition & Epidemiology Female Gonadal Axis Normal Menstrual Cycle Causes Patient History Patient Examination Investigations
Infertility Rhian Allen & David Rogers http://www.worldofsurrogacy.com Objectives Definition & Epidemiology Female Gonadal Axis Normal Menstrual Cycle Causes Patient History Patient Examination Investigations
Policy statement. Fertility treatments. This policy is unchanged from the version approved by the CCG in July 2014.
 Policy statement Fertility treatments This policy is unchanged from the version approved by the CCG in July 2014. Title Policy statement: Fertility treatments v2.0 Author Jacky Walters Approved by Kingston
Policy statement Fertility treatments This policy is unchanged from the version approved by the CCG in July 2014. Title Policy statement: Fertility treatments v2.0 Author Jacky Walters Approved by Kingston
NaProTechnology. An Integrated Approach to Infertility. Tracy Parnell. Geneva 2005
 NaProTechnology An Integrated Approach to Infertility Tracy Parnell Geneva 2005 Outline Scientific foundations Illustrative case history Research Discussion and questions NPT Natural Procreative Technology(NPT)
NaProTechnology An Integrated Approach to Infertility Tracy Parnell Geneva 2005 Outline Scientific foundations Illustrative case history Research Discussion and questions NPT Natural Procreative Technology(NPT)
This information explains the advice about assessment and treatment for people with fertility problems that is set out in NICE guideline CG156.
 Assessment and treatment for people with fertility problems Information for the public Published: 1 February 2013 nice.org.uk About this information NICE guidelines provide advice on the care and support
Assessment and treatment for people with fertility problems Information for the public Published: 1 February 2013 nice.org.uk About this information NICE guidelines provide advice on the care and support
International Federation of Fertility Societies. Global Standards of Infertility Care
 International Federation of Fertility Societies Global Standards of Infertility Care Standard 8 Reducing the incidence of multiple pregnancy following treatment for infertility Name Version number Author
International Federation of Fertility Societies Global Standards of Infertility Care Standard 8 Reducing the incidence of multiple pregnancy following treatment for infertility Name Version number Author
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Chapter 1. Chapter 2. Chapter 3
 Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
The assessment and investigation of the infertile couple
 The assessment and investigation of the infertile couple BIRUTE ZILAITIENE, MD, PHD, PROF., FECSM DEPARTMENT OF ENDOCRINOLOGY AND INSTITUTE OF ENDOCRINOLOGY, LITHUANIAN UNIVERSITY OF HEALTH SCIENCES, KAUNAS,
The assessment and investigation of the infertile couple BIRUTE ZILAITIENE, MD, PHD, PROF., FECSM DEPARTMENT OF ENDOCRINOLOGY AND INSTITUTE OF ENDOCRINOLOGY, LITHUANIAN UNIVERSITY OF HEALTH SCIENCES, KAUNAS,
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
East and North Hertfordshire CCG. Fertility treatment and referral criteria for tertiary level assisted conception
 East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
Reproductive Endocrinology and Infertility Rotation Objectives. Reproductive Endocrinology and Infertility Specialists
 Reproductive Endocrinology and Infertility Rotation Objectives Reproductive Endocrinology and Infertility Specialists Terry O Grady M.D., FRCSC Sarah Healey M.D., FRCSC Deanna Murphy M.D., FRCSC Sean Murphy
Reproductive Endocrinology and Infertility Rotation Objectives Reproductive Endocrinology and Infertility Specialists Terry O Grady M.D., FRCSC Sarah Healey M.D., FRCSC Deanna Murphy M.D., FRCSC Sean Murphy
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Management of Female infertility Tim Chang
 Management of Female infertility Tim Chang www.drtchang.com.au Assess and manage as a couple because: 30% infertility male factor related emotional support Role of the physician 1) diagnose and treat the
Management of Female infertility Tim Chang www.drtchang.com.au Assess and manage as a couple because: 30% infertility male factor related emotional support Role of the physician 1) diagnose and treat the
Causes of Infertility and Treatment Options
 Causes of Infertility and Treatment Options Dr Mrs.Kiran D. Sekhar Former vice President-FOGSI Former Chairperson- Genetics and Foetal medicine-fogsi Founder and Medical Director-Kiran Infertility centre
Causes of Infertility and Treatment Options Dr Mrs.Kiran D. Sekhar Former vice President-FOGSI Former Chairperson- Genetics and Foetal medicine-fogsi Founder and Medical Director-Kiran Infertility centre
Reproductive Endocrinology & Infertility Glossary
 Reproductive Endocrinology & Infertility Glossary The following is a glossary of terms you may hear during your association with the University of Mississippi Health Care's reproductive endocrinology and
Reproductive Endocrinology & Infertility Glossary The following is a glossary of terms you may hear during your association with the University of Mississippi Health Care's reproductive endocrinology and
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE. Anatomy : Male and Female genital tract
 POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Obstetrics and Gynecology. Infertility. Dr. Layla Zaghal. Definition
 Obstetrics and Gynecology Infertility Dr. Layla Zaghal Definition The term infertility is no more used and has been replaced by the term subfertility ; when you tell a couple that they are infertile, it
Obstetrics and Gynecology Infertility Dr. Layla Zaghal Definition The term infertility is no more used and has been replaced by the term subfertility ; when you tell a couple that they are infertile, it
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
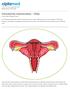 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
2017 United HealthCare Services, Inc.
 UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number 2.0 Ratified by HVCCG Exec Team Date Ratified 9 th November 2017 Name of Originator/Author Dr Raj Nagaraj
Fertility treatment and referral criteria for tertiary level assisted conception Version Number 2.0 Ratified by HVCCG Exec Team Date Ratified 9 th November 2017 Name of Originator/Author Dr Raj Nagaraj
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Brighton & Hove CCG PLS CONFERENCE Dr Carole Gilling-Smith Medical Director
 Brighton & Hove CCG PLS CONFERENCE 2016 Dr Carole Gilling-Smith Medical Director FERTILITY CHALLENGES IN THE NHS A TERTIARY CARE PERSPECTIVE LEARNING OBJECTIVES Understand the pathways through assisted
Brighton & Hove CCG PLS CONFERENCE 2016 Dr Carole Gilling-Smith Medical Director FERTILITY CHALLENGES IN THE NHS A TERTIARY CARE PERSPECTIVE LEARNING OBJECTIVES Understand the pathways through assisted
Independent Review of Assisted Reproductive Technologies
 Assisted Reproductive Technologies Review Committee Report of the Independent Review of Assisted Reproductive Technologies APPENDICES Assisted Reproductive Technologies Review Committee APPENDIX A February
Assisted Reproductive Technologies Review Committee Report of the Independent Review of Assisted Reproductive Technologies APPENDICES Assisted Reproductive Technologies Review Committee APPENDIX A February
Bleeding and spontaneous abortion after therapy for infertility
 FERTILITY AND STERILITY VOL. 74, NO. 3, SEPTEMBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Bleeding and spontaneous
FERTILITY AND STERILITY VOL. 74, NO. 3, SEPTEMBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Bleeding and spontaneous
Infertility for the Primary Care Provider
 Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Appendix 1: Specialist Fertility Services Commissioning Policy
 Appendix 1: Specialist Fertility Services Commissioning Policy Author: EoE CCG Fertility Consortium Version No: 4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces
Appendix 1: Specialist Fertility Services Commissioning Policy Author: EoE CCG Fertility Consortium Version No: 4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces
The cost of infertility diagnosis and treatment in Canada in 1995
 Human Reproduction vol.12 no.5 pp.951 958, 1997 The cost of infertility diagnosis and treatment in Canada in 1995 J.A.Collins 1,2,4, D.Feeny 3,2 and J.Gunby 1 treatment. This information is needed to provide
Human Reproduction vol.12 no.5 pp.951 958, 1997 The cost of infertility diagnosis and treatment in Canada in 1995 J.A.Collins 1,2,4, D.Feeny 3,2 and J.Gunby 1 treatment. This information is needed to provide
Can diagnostic laparoscopy be avoided in routine investigation for infertility?
 BJOG 000,10(), pp. 118 Can diagnostic laparoscopy be avoided in routine investigation for infertility? N. P. Johnson Senior Registrar, K. Taylor Medical Student, A. A. Nadgir Specialist Registrar, D. J.
BJOG 000,10(), pp. 118 Can diagnostic laparoscopy be avoided in routine investigation for infertility? N. P. Johnson Senior Registrar, K. Taylor Medical Student, A. A. Nadgir Specialist Registrar, D. J.
FACTSHEET FERTILITY INVESTIGATIONS
 FACTSHEET FERTILITY INVESTIGATIONS Most people nowadays know enough about contraception to expect a pregnancy to occur reasonably soon after contraceptive precautions are stopped. If your own fertility
FACTSHEET FERTILITY INVESTIGATIONS Most people nowadays know enough about contraception to expect a pregnancy to occur reasonably soon after contraceptive precautions are stopped. If your own fertility
Fertility Treatment: Do not be Distracted
 Fertility Treatment: Do not be Distracted Fertility Treatment: do not be distracted by worthless recommendation Fertility Treatment: Do not be Distracted When contemplating options for fertility treatment
Fertility Treatment: Do not be Distracted Fertility Treatment: do not be distracted by worthless recommendation Fertility Treatment: Do not be Distracted When contemplating options for fertility treatment
ACT TRYING TO HAVE A BABY? YOUR STEP-BY-STEP GUIDE TO ASSISTED CONCEPTION THE ACT PATHWAY
 ACT TRYING TO HAVE A BABY? YOUR STEP-BY-STEP GUIDE TO CONCEPTION THE ACT PATHWAY ACT HOW TO USE THE ACT PATHWAY BOOKLET Firstly: You are not alone. Up to 1 in 6 couples around the world will experience
ACT TRYING TO HAVE A BABY? YOUR STEP-BY-STEP GUIDE TO CONCEPTION THE ACT PATHWAY ACT HOW TO USE THE ACT PATHWAY BOOKLET Firstly: You are not alone. Up to 1 in 6 couples around the world will experience
Wiltshire CCG Fertility Policy
 Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: PA.018.MH Last Review Date: 08/04/2016 Effective Date: 01/01/2017
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
Assisted Conception Policy
 Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
Hum. Reprod. Advance Access published April 7, 2004
 Human Reproduction Page 1 of 6 Hum. Reprod. Advance Access published April 7, 2004 DOI: 10.1093/humrep/deh219 An economic evaluation of laparoscopic ovarian diathermy versus gonadotrophin therapy for women
Human Reproduction Page 1 of 6 Hum. Reprod. Advance Access published April 7, 2004 DOI: 10.1093/humrep/deh219 An economic evaluation of laparoscopic ovarian diathermy versus gonadotrophin therapy for women
PROCEDURES LAPAROSCOPY
 PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
NORCOM COMMISSIONING POLICY
 NORCOM COMMISSIONING POLICY North Derbyshire, South Yorkshire and Bassetlaw Commissioning Consortium NHS Eligibility Criteria for In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) and
NORCOM COMMISSIONING POLICY North Derbyshire, South Yorkshire and Bassetlaw Commissioning Consortium NHS Eligibility Criteria for In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) and
Dr Manuela Toledo - Procedures in ART -
 Dr Manuela Toledo - Procedures in ART - Fertility Specialist MBBS FRANZCOG MMed CREI Specialities: IVF & infertility Fertility preservation Consulting Locations East Melbourne Planning a pregnancy - Folic
Dr Manuela Toledo - Procedures in ART - Fertility Specialist MBBS FRANZCOG MMed CREI Specialities: IVF & infertility Fertility preservation Consulting Locations East Melbourne Planning a pregnancy - Folic
Blackpool CCG. Policies for the Commissioning of Healthcare. Assisted Conception
 1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
FERTILITY & TCM. On line course provided by. Taught by Clara Cohen
 FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
FERTILITY & TCM On line course provided by Taught by Clara Cohen FERTILITY & TCM FERTILITY AND TCM THE PRACTITIONER S ROLE CAUSES OF INFERTILITY RISK FACTORS OBJECTIVES UNDERSTANDING TESTS Conception in
Unexplained infertility Evidence based management
 Unexplained infertility Evidence based management Dr Mark Hamilton Consultant Gynaecologist NHS Grampian/University of Aberdeen m.hamilton@abdn.ac.uk www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc
Unexplained infertility Evidence based management Dr Mark Hamilton Consultant Gynaecologist NHS Grampian/University of Aberdeen m.hamilton@abdn.ac.uk www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc
A prospective study comparing unilateral and bilateral laparoscopic ovarian diathermy in women with the polycystic ovary syndrome
 FERTILITY AND STERILITY Copyright " 1994 The American Fertility Society Vol. 62, No.5, November 1994 Printed on acid-free paper in U. S. A. A prospective study comparing unilateral and bilateral laparoscopic
FERTILITY AND STERILITY Copyright " 1994 The American Fertility Society Vol. 62, No.5, November 1994 Printed on acid-free paper in U. S. A. A prospective study comparing unilateral and bilateral laparoscopic
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 25 June 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 25 June 2008 PERGOVERIS 150 IU/75 IU, powder and solvent for solution for injection B/1 glass vial - one 1 ml vial
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 25 June 2008 PERGOVERIS 150 IU/75 IU, powder and solvent for solution for injection B/1 glass vial - one 1 ml vial
Fertility Assisted Conception Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives
 NHS Dorset Clinical Commissioning Group Fertility Assisted Conception Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives POLICY TRAIL AND VERSION CONTROL SHEET: Policy Reference:
NHS Dorset Clinical Commissioning Group Fertility Assisted Conception Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives POLICY TRAIL AND VERSION CONTROL SHEET: Policy Reference:
GPVTS TEACHING APRIL 2016 FERTILITY
 GPVTS TEACHING APRIL 2016 FERTILITY Djavid Alleemudder - Consultant Obstetrics & Gynaecology DEFINITIONS What is the definition of infertility? Failure to conceive after 12 months despite regular, unprotected
GPVTS TEACHING APRIL 2016 FERTILITY Djavid Alleemudder - Consultant Obstetrics & Gynaecology DEFINITIONS What is the definition of infertility? Failure to conceive after 12 months despite regular, unprotected
LCCG Fertility Services Commissioning Policy
 LCCG Fertility Services Commissioning Policy Author: Emma Dwyer & Dr Fiona Sim Version No: V.4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces all previous versions.
LCCG Fertility Services Commissioning Policy Author: Emma Dwyer & Dr Fiona Sim Version No: V.4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces all previous versions.
Infertility in Women over 35. Alison Jacoby, MD Dept. of Ob/Gyn UCSF
 Infertility in Women over 35 Alison Jacoby, MD Dept. of Ob/Gyn UCSF Learning Objectives Review the effect of age on fertility Fertility counseling for the patient >35 - timing - lifestyle - workup Fertility
Infertility in Women over 35 Alison Jacoby, MD Dept. of Ob/Gyn UCSF Learning Objectives Review the effect of age on fertility Fertility counseling for the patient >35 - timing - lifestyle - workup Fertility
IVF. NHS North West London CCGs
 IVF NHS North West London CCGs Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services Adopted by NWL CCGs to be effective from
IVF NHS North West London CCGs Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services Adopted by NWL CCGs to be effective from
Aims of this talk. Evaluation & investigation. Basic treatments/options including ovulation induction & Intra uterine Insemination
 Basic treatments/options including ovulation induction & Intra uterine Insemination Karen Woodcock Clinical Nurse Specialist/ Nurse Manager Fertility & Assisted Conception Unit Countess of Chester NHS
Basic treatments/options including ovulation induction & Intra uterine Insemination Karen Woodcock Clinical Nurse Specialist/ Nurse Manager Fertility & Assisted Conception Unit Countess of Chester NHS
The outcome of in-vitro fertilization treatment in women with sonographic evidence of polycystic ovarian morphology
 Human Reproduction vol.14 no.1 pp.167 171, 1999 The outcome of in-vitro fertilization treatment in women with sonographic evidence of polycystic ovarian morphology Lawrence Engmann 1,2,5, Noreen Maconochie
Human Reproduction vol.14 no.1 pp.167 171, 1999 The outcome of in-vitro fertilization treatment in women with sonographic evidence of polycystic ovarian morphology Lawrence Engmann 1,2,5, Noreen Maconochie
The role of laparoscopy in intrauterine insemination: a prospective randomized reallocation study
 Human Reproduction Vol.20, No.11 pp. 3225 3230, 2005 Advance Access publication July 8, 2005. doi:10.1093/humrep/dei201 The role of laparoscopy in intrauterine insemination: a prospective randomized reallocation
Human Reproduction Vol.20, No.11 pp. 3225 3230, 2005 Advance Access publication July 8, 2005. doi:10.1093/humrep/dei201 The role of laparoscopy in intrauterine insemination: a prospective randomized reallocation
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 Cryopreservation to preserve e fertility in people diagnosed with cancer bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They
Cryopreservation to preserve e fertility in people diagnosed with cancer bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They
Introduction to Intrauterine Insemination (IUI) Service
 Introduction to Intrauterine Insemination (IUI) Service Assisted Reproductive Technology Unit The Chinese University of Hong Kong Prince of Wales Hospital 2017 Treatment Procedures IUI involves six main
Introduction to Intrauterine Insemination (IUI) Service Assisted Reproductive Technology Unit The Chinese University of Hong Kong Prince of Wales Hospital 2017 Treatment Procedures IUI involves six main
Diagnostic L/S: Is it ever indicated? Prof. Dr. Nilgün Turhan Fatih University Medical School
 Diagnostic L/S: Is it ever indicated? Prof. Dr. Nilgün Turhan Fatih University Medical School Diagnostic Laparoscopy (DLS) DLS is the gold standard in diagnosing tubal pathology and other intraabdominal
Diagnostic L/S: Is it ever indicated? Prof. Dr. Nilgün Turhan Fatih University Medical School Diagnostic Laparoscopy (DLS) DLS is the gold standard in diagnosing tubal pathology and other intraabdominal
Clinical review. Management of infertility. Summary points. Methods. What can a couple expect when trying to conceive? Causes of subfertility
 Management of infertility D J Cahill, P G Wardle University of Bristol Division of Obstetrics and Gynaecology, St Michael s Hospital, Bristol BS2 8EG D J Cahill consultant senior lecturer in reproductive
Management of infertility D J Cahill, P G Wardle University of Bristol Division of Obstetrics and Gynaecology, St Michael s Hospital, Bristol BS2 8EG D J Cahill consultant senior lecturer in reproductive
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE
 ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
Approach to ovulation induction and superovulation in women with a history of infertility. Anatte E. Karmon, MD
 Approach to ovulation induction and superovulation in women with a history of infertility Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the
Approach to ovulation induction and superovulation in women with a history of infertility Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the
Abstract. Introduction. RBMOnline - Vol 19. No Reproductive BioMedicine Online; on web 12 October 2009
 RBMOnline - Vol 19. No 6. 2009 847 851 Reproductive BioMedicine Online; www.rbmonline.com/article/4130 on web 12 October 2009 Article Significance of positive Chlamydia serology in women with normal-looking
RBMOnline - Vol 19. No 6. 2009 847 851 Reproductive BioMedicine Online; www.rbmonline.com/article/4130 on web 12 October 2009 Article Significance of positive Chlamydia serology in women with normal-looking
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
