Human oocyte cryopreservation and the fate of cortical granules
|
|
|
- Allen Golden
- 6 years ago
- Views:
Transcription
1 Human oocyte cryopreservation and the fate of cortical granules Yehudith Ghetler, Ph.D., a,b,c Ehud Skutelsky, Ph.D., b Isaac Ben Nun, M.D., c Liah Ben Dor, M.Sc., a,b Dina Amihai, M.Sc., b and Ruth Shalgi, Ph.D. a a Department of Cell and Developmental Biology and b Department of Pathology, Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel; and c IVF Unit, Meir Hospital (affiliated with Tel Aviv University), Kfar Saba, Israel Objective: To examine the effect of the commonly used oocyte cryopreservation protocol on the cortical granules (CGs) of human immature germinal vesicle (GV) and mature metaphase II (MII) oocytes. Design: Laboratory study. Setting: IVF unit. Intervention(s): Unfertilized, intracytoplasmic sperm injected (ICSI) oocytes, and immature oocytes were cryopreserved using a slow freezing rapid thawing program with 1,2-propanediol (PROH) as a cryoprotectant. Main Outcome Measure(s): Cortical granule exocytosis (CGE) was assessed by either confocal microscopy or transmission electron microscopy (TEM). Result(s): The survival rates of frozen-thawed oocytes (mature and immature) were significantly lower compared with zygotes. Both mature and immature oocytes exhibited increased fluorescence after cryopreservation, indicating the occurrence of CGE. Mere exposure of oocytes to cryoprotectants induced CGE of 70% the value of control zygotes. The TEM revealed a drastic reduction in the amount of CGs at the cortex of frozen-thawed GV and MII oocytes, as well as appearance of vesicles in the ooplasm. Conclusion(s): The commonly used PROH freezing protocol for human oocytes resulted in extensive CGE. This finding explains why ICSI is needed to achieve fertilization of frozen-thawed human oocytes. (Fertil Steril 2006; 86: by American Society for Reproductive Medicine.) Key Words: Cryopreservation, cortical granules, exocytosis, mature human oocyte, immature human oocyte Cryopreservation of human embryos at different developmental stages is successfully applied in IVF treatment programs. However, the cryopreservation of human oocytes still generally yields unsatisfactory results and is therefore considered experimental. The ability to cryopreserve human oocytes is of great importance because it avoids serious ethical and legal issues arising from embryo freezing, such as disposal, donation, or dispute over ownership. Furthermore, cryopreservation of human oocytes could lay the ground for egg donation programs and for establishing oocyte banks, offering the opportunity to preserve the fertility potential of women who face chemotherapy or radiation therapy. Successful cryopreservation of mammalian oocytes had already been reported by several investigators (1, 2). The technologies for cryopreservation of human oocytes used in IVF clinics are derived from traditional protocols of embryo cryopreservation and, as such, render results that are inconsistent and suboptimal. Cryopreservation of oocytes results in low survival rate, hardening of the zona pellucida (ZP), and various types of injuries, including damage to the meiotic spindle and microfilaments (3 7). Attempts have been Received June 8, 2005; revised and accepted December 5, Reprint requests: Ruth Shalgi, Ph.D., Department of Cell and Developmental Biology, Sackler Faculty of Medicine, Tel Aviv University, Ramat Aviv, Tel Aviv 69978, Israel (FAX: ; shalgir@ post.tau.ac.il). made to freeze immature oocytes at the germinal vesicle (GV) stage, where the DNA is still enclosed within the nucleus and protected by a membrane and may be less sensitive to stressful environmental conditions (8). Immature oocytes, excised from unstimulated follicles or from ovarian tissue, could, in part, survive and mature, but their developmental capability is still very low (9, 10). The common protocol used for oocyte cryopreservation is slow freezing rapid thawing in 1,2-propanediol (PROH) (11 13). Other protocols such as slow freezing rapid thawing in dimethyl sulphoxyde (DMSO) (14, 15) and an ultrarapid method (16, 17) have also been introduced. Some research groups have used variations of vitrification (18, 19), including vitrification at specially enhanced cooling rates using open pooled straws (20), electron microscope grids (21), and minimum drop size in supercooled liquid nitrogen (22). Human oocytes that survived cryopreservation had, reportedly, a low fertilization rate (23), indicating that the normal process of the sperm penetration is impaired. Therefore, cryopreserved human oocytes are fertilized by intracytoplasmic sperm injection (ICSI) in an effort to improve their fertilization rate (5, 13). The cortical granules (CGs) are Golgi-derived membranebound spherical or slightly ovoid organelles formed during the early stages of oocyte growth and maturation and are 210 Fertility and Sterility Vol. 86, No. 1, July /06/$32.00 Copyright 2006 American Society for Reproductive Medicine, Published by Elsevier Inc. doi: /j.fertnstert
2 present in the cortex of mature unfertilized oocytes of most animal species (24). Both density and distribution of CGs change when they translocate to the cortical region of the oocyte during the process of oocyte maturation (25, 26). The CG s content is released into the perivitelline space (PVS) immediately after oocyte fertilization or activation and is believed to alter the ZP glycoproteins, establishing the block to polyspermy, and preventing the penetration of additional spermatozoa (27). Due to the major role of CGs in inducing the block to polyspermy, their fate in frozen-thawed oocytes is of great importance, but research results have been inconsistent, ranging from a reduction in the number of CGs following cryopreservation (3, 28) to an apparently normal density and distribution of CGs in frozen-thawed oocytes (29 31). In view of this inconsistency, we aimed to examine the affect of the commonly used oocyte PROH cryopreservation protocol on the CGs of human immature GV and mature metaphase II (MII) oocytes by using confocal microscopy as well as transmission electron microscopy (TEM). MATERIALS AND METHODS Oocytes included in this study were donated by consenting patients undergoing IVF-ICSI procedures and represent material that is otherwise discarded. The study was approved by the local review board. The ovulation induction (by a long protocol of GnRH analog and hmg) and the ICSI procedure used were as described previously (32, 33). Oocytes that failed to be fertilized by ICSI (unfertilized [UF]) and immature oocytes not suitable for ICSI were used. The UF oocytes were reassessed 24 h after ICSI to rule out late fertilization occurrence and only then were they frozen. The immature oocytes were handled according to their developmental state: GV oocytes were frozen on the retrieval day, whereas oocytes at the first metaphase (MI) stage were further cultured for 24 h in the routinely used culture media (Cook Culture System; Cook, Brisbane, Australia). Only oocytes that were able to mature in vitro to the MII stage were cryopreserved. The UF as well as in vitro matured MII oocytes served as a model of mature oocytes throughout this research. Abnormally fertilized (one pronucleus [1PN] or three pronuclei [3PN]) oocytes served as positive control for occurrence of cortical granule exocytosis (CGE). Study Groups Several experimental groups were included in the research. Group 1: Untreated mature oocytes do not undergo CGE (34) served as a negative control for assessing CG status (n 13). Group 2: Mature oocytes that were subjected to the freezing-thawing solutions, according to the protocol, but not to the actual freezing procedure, served as a control for the effect of the solutions on the CGs fate, (n 16). Group 3 consisted of mature oocytes that were frozen 1 week before thawing (n 23). Group 4 consisted of GV oocytes that were frozen 1 week before thawing (n 10). Group 5: Abnormally fertilized oocytes (1PN or 3PN) after ICSI served as a positive control for CGE occurrence (n 11); in a previous study we demonstrated that these abnormally fertilized ICSI oocytes exhibit an intense CGE (34). All oocytes were assessed for CGE by confocal microscopy or TEM. Cryopreservation Protocol The slow freezing rapid thawing method was used throughout the study. The freezing/thawing solutions (Cook) and protocols were the routine protocols used in our IVF program for zygote and early embryo cryopreservation. In brief, a three-step cryopreservation system was used with HEPESbuffered salt solution (HBSS) containing PROH and sucrose as cryoprotectants: step 1: incubation in prewarmed (37 C) HBSS for 10 minutes at room temperature (RT); step 2: incubation in HBSS containing 1.5 mol/l PROH for 10 minutes at RT; step 3: transfer into HBSS containing 1.5 mol/l PROH and 0.1 mol/l sucrose, loading the samples into straws at RT, and transfering them into an automated Kryo 10 biologic vertical freezer (Kryo 10 series III, Planer, Middlesex, UK). Cooling steps: starting at 20 C, cooling at 2 C/min down to 7 C, soaking for 10 minutes, manual seeding, holding 10 minutes, cooling at 0.3 C/min down to 30 C, cooling at 50 C/min down to 150 C and plunging into liquid nitrogen ( 196 C). Samples were stored in liquid nitrogen for 1 week. For thawing, straws were removed from liquid nitrogen and kept 30 seconds at RT before being immersed in a 30 C water bath until all the ice melted. The cryoprotectant was removed with four consecutive steps of 5 minutes each incubation at RT: step 1: HBSS containing 1.0 mol/l PROH and 0.2 mol/l sucrose; step 2: HBSS containing 0.5 mol/l PROH and 0.2 mol/l sucrose; step 3: HBSS containing 0.2 mol/l sucrose; step 4: only HBSS followed by additional 5 minutes at 37 C. Finally, the oocytes were incubated in culture medium (Cook) at 37 C with 5% CO 2 in humidified air for 1 hour and then assessed morphologically. Only oocytes that survived the whole process of freezing-thawing were further examined. Assessment of CGE The assessment of cortical reaction was performed by labeling the oocytes with the lectin Lens culinaris agglutinin (LCA), which binds specifically to CG content and exudate (35). The studied oocytes were briefly exposed to 0.25% pronase (Sigma, St. Louis, MO) for ZP removal, followed by three rinses in HTF-HEPES medium (Irvine, Santa Ana, CA) supplemented with 10% synthetic serum substitute (Irvine). The ZP-free oocytes were fixed with 3% paraformaldehyde in DPBS for 30 minutes at RT and washed three times in DPBS supplemented with 1% bovine serum albumin (Fraction V; Sigma). The fixated oocytes were stained for 30 minutes with Fertility and Sterility 211
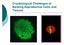
3 TABLE 1 Survival rate of frozen thawed oocytes and zygotes. Study group Number of oocytes/ zygotes Survival rate* (mean % SEM) Zygotes a Mature ocytes b GV oocytes b Note: Survival of thawed oocytes and zygotes was morphologically determined after 1 h of culture. a,b Different superscripts within column denote significant differences (P.001). Ghetler. Cortical granules in cryopreserved human oocytes. Fertil Steril g/ml LCA-biotin (Vector, Burlingame, CA), washed, and stained with 2 g/ml Texas red streptavidin (Vector) for 30 minutes, thus labeling the membrane of exocytosed granules and the exudate. For high-quality assessment of the CGE, a confocal laser scanning microscope (CLSM) (LSM 410; Ziess, Oberkochen, Germany) equipped with a 25 mw krypton-argon laser was used. The oocytes were scanned every 5 m and the composite image of micrographs taken at all focal planes of each oocyte was displayed. The fluorescence intensity of each individual oocyte was quantified, with the aid of the LSM software, and presented as the ratio between the fluorescent area and the total area of the oocyte, which was then related to the fluorescence intensity of the positive control (group 5) which was set arbitrarily as 1. Assessment of Meiotic Status Oocytes were incubated for 10 minutes in the presence of 2 g/ml DNA-specific fluorochrome (Hoechst 33342, Sigma) and then washed three times in DPBS. Analysis of each oocyte was performed at the time of CGE assessment, using the CLSM. Electron Microscopy (EM) The ultrastructure of CGs of oocytes from the various experimental groups was examined using TEM. At least three oocytes from each group were sectioned and analyzed. The oocytes were fixed for 1 hour in Karnovsky fixative (36), washed twice in 0.2 mol/l cacodylate buffer, ph 7.4, postfixed in 1% osmium tetroxide, washed, and gradually dehydrated through ascending grades of ethanol and propylene oxide. Each oocyte was individually embedded in Araldite (Polysciences, Warrington, PA) and sectioned ( nm) on an LKB III Ultratome. The ultrathin sections were mounted on grids and stained with uranyl acetate followed by lead citrate. The sections were examined using a JOEL-100CX TEM at 80 kv (37). Statistical Analysis The significance of differences between experimental groups was determined by one-way analysis of variance after arcsin square root of proportion transformation (for survival study) and ln transformation (for the fluorescence study) to achieve normal distribution, combined with Tukey s method for multiple comparisons. RESULTS Survival rate of the frozen-thawed oocytes was compared to the survival rate of zygotes (2 PN) cryopreserved in our IVF program (Table 1). The overall survival rate of oocytes was low and inconsistent (0% 92%). The survival rate of zygotes in our IVF unit during the same period of time was 74.7% 4.2% (mean SEM), similar to other reports (38) and significantly (P.001) higher than the survival rate of either immature (31.4% 7.1%) or mature oocytes (40.8% 4.9%). There was no significant difference between the survival rate of mature and immature oocytes. We used the CLSM for assessing the CGE occurrence as an indicator of the fate of CGs in frozen-thawed oocytes. The treated oocytes (groups 2, 3, 4) and the negative control FIGURE 1 Detection of cortical granule exocytosis (CGE) by labeling with biotinylated lectin Lens culinaris agglutinin and Texas red strepavidin. Composite confocal microscopy images (A D) and light microscopy images (a d) of untreated mature oocyte (A, a), untreated 3PN zygote (B, b), frozenthawed (slow freezing rapid thawing in 1,2 propanediol) mature oocyte (C, c), and frozenthawed (slow freezing rapid thawing in 1,2 propanediol) germinal vesicle stage oocyte (D, d), illustrating the degree of CGE at the various treatments. Bar 35 m. Ghetler. Cortical granules in cryopreserved human oocytes. Fertil Steril Ghetler et al. Cortical granules in cryopreserved human oocytes Vol. 86, No. 1, July 2006
4 TABLE 2 Fluorescence intensity of frozen-thawed oocytes. Study group Number of oocytes Fluorescence intensity (mean SEM) a b b,c c Note: Relative fluorescence intensity expressed as ratio of the abnormally ICSI-fertilized oocytes (group 5). Group 1: untreated mature oocytes. Group 2: mature oocytes following exposure to freezingthawing solutions. Group 3: frozen-thawed mature oocytes. Group 4: frozen-thawed germinal vesicle oocytes. Group 5: abnormally fertilized oocytes, fluorescence intensity arbitrarily defined as 1. a,b,c Different superscripts within column denote significant differences P.001). Ghetler. Cortical granules in cryopreserved human oocytes. Fertil Steril (group 1) did not show activation, as indicated by Hoechst staining. However, our results demonstrate that both mature and immature frozen-thawed oocytes underwent CGE (Figs. 1C and D, respectively) compared with untreated oocytes (Fig. 1A) or fertilized oocytes (Fig. 1B). The calculated CGE intensity is presented in Table 2. Untreated mature oocytes (group 1, negative control) exhibited very low fluorescence relative to the positive control group of abnormally fertilized oocytes (group 5). The mere exposure to cryopreservation solutions (group 2) resulted in a strong CGE: about 70% of the positive control value and significantly different from the untreated mature oocytes (P.001). The CGE of oocytes, both mature (group 3) and immature (group 4), passing through the complete freezingthawing procedure was significantly stronger than that of untreated oocytes. The GV frozen-thawed oocytes exhibited a higher (but not statistically different) degree of CGE relative to the frozen-thawed mature oocytes. We examined ultrathin sections of mature and immature untreated oocytes by TEM and compared them to sections of oocytes that survived the freezing-thawing procedure. Mature untreated oocytes exhibited an abundant number of CGs consisting of dark (electron-dense) and light subpopulations (Fig. 2, top). The dark granules were restricted only to the cortical region, whereas light granules were scattered all through the cytoplasm as well. The GV untreated oocytes contained few granules at the cortex (mostly dark) and many clusters of light granules throughout the cytoplasm (Fig. 3, top). A change in the CG distribution pattern was observed in both mature and immature oocytes after freezing-thawing procedure (Figs. 2, bottom, and 3, bottom). Only very few dark CGs were observed within frozen-thawed oocytes. Mature frozen-thawed oocytes had only a few scattered CGs deeper in the cytoplasm, whereas GV frozen-thawed oocytes had a few CGs at the cortex and aggregates of light granules throughout the cytoplasm. All the frozen-thawed oocytes formed membrane-coated electron-transparent vesicles, which in some cases were aggregated with CGs (Figs. 2, bottom, and 3, bottom). No such vesicles could be observed within the oocytes before cryopreservation. FIGURE 2 The effect of cryopreservation on mature oocytes. (Top) An untreated oocyte: Abundant dark electron-dense granules (white arrow) are present in the cortex, and light (black arrow) granules are present mainly deeper in the cytoplasm. (Bottom) A frozen-thawed oocyte: Very few granules are present at the cortex. Light (black arrow) and a few dark (white arrow) granules are in the inner region. A large number of membrane-coated transparent vesicles (V) are observed, scattered throughout the ooplasm. ZP zona pellucida. Bar 2 m. Ghetler. Cortical granules in cryopreserved human oocytes. Fertil Steril Fertility and Sterility 213
5 FIGURE 3 The effect of cryopreservation on immature (geminal vesicle stage) oocytes. (Top) An untreated oocyte: Dark electron-dense granules (white arrow) are present in the cortex. Numerous aggregated light (black arrow) granules appear throughout the cytoplasm. (Bottom) A frozenthawed oocyte: Very few dark (white arrow) granules are present at the cortex. Light (black arrow) aggregated granules are in the inner cytoplasm. A large number of membrane-coated transparent vesicles (V) were observed scattered throughout the ooplasm. ZP zona pellucida. Bar 2 m. Ghetler. Cortical granules in cryopreserved human oocytes. Fertil Steril DISCUSSION Oocyte cryopreservation is a feasible procedure yielding birth of healthy babies, although clinical efficiency is still low (39). In the present research we tried to elucidate one of the pitfalls of fertilizing frozen-thawed oocytes, i.e., the premature occurrence of CGE. We demonstrated that the most commonly used procedure of cryopreserving human oocytes, the PROH slow freezing-rapid thawing procedure, has a detrimental effect on the CGs. Our findings explain the low fertilization rate of human frozen-thawed oocytes and justify the need for ICSI for this population of oocytes. The initial step of the cryopreservation procedure, the dehydration step, which included exposure to cryoprotectants at RT, had already caused the release of content from a significant number of CGs. Similar effect on CGs of mouse and human oocytes was demonstrated following exposure to PROH or DMSO (28). Further exocytosis was demonstrated after the freezing-thawing process, as indicated by the fluorescence of CG exudate in mature as well as immature cryopreserved oocytes. Although not statistically significant, GV oocytes appear more susceptible than MII oocytes to the harch procedure of freezing-thawing regarding their survival rate and degree of CGE. The difference might be attributed to possible differences in the composition of membranes of GV and MII oocytes. Cortical granule exocytosis might occur because of changes in the properties and permeability of the oocyte s membrane after chilling injury (40), toxicity of the cryoprotectant solutions (41), or osmotic shock induced by osmotic pressure changes that involve an Na /H exchange mediated signal transduction pathway (42). Mattioli et al. (43) demonstrated a clear biphasic Ca 2 rise in immature pig oocytes during cooling from 30 to 14 C which was related to DNA fragmentation. Ben-Yosef et al. (44) demonstrated cooling-induced rat egg activation, as manifested by intracellular calcium concentration (Ca 2 i) transients and second polar body extrusion. Such a rise in Ca 2 i may trigger CGE as well. The overall fluorescence of frozen-thawed oocytes (mature and immature) was higher than that of ICSI-fertilized (1PN and 3PN) positive control oocytes. It is possible that owing to changes in membrane properties and/or permeability that occur during cryopreservation the content of granules located deeper within the oocyte is also released into the PVS, whereas only cortically located granules are released during fertilization, or that there is leakage of lectin (LCA) binding molecules, which contributes to the massive fluorescent labeling. We demonstrated, by TEM analysis, changes in the distribution pattern of the CGs as well as cytoplasmic structural changes following cryopreservation. The cryopreservation procedure resulted in the loss of CGs from the cortical area and in the appearance of vesicles within the cytoplasm of both immature and mature cryopreserved oocytes, which might indicate structural damage occurring from the freezing-thawing process. Similar findings were reported after exposure of bovine oocytes to vitrification solutions (45). Further research is needed for determining the origin and meaning of the newly formed vesicles. Standard embryo cryopreservation technologies appear to have limitations when applied to oocytes. Cryosurvival is low and inconsistent, and oocytes that manage to survive this procedure exhibit structural and functional damage. An improved survival rate for human oocytes was obtained by raising the seeding temperature to 4.5 C, as close as possible to the melting point of the solution (46), indicat- 214 Ghetler et al. Cortical granules in cryopreserved human oocytes Vol. 86, No. 1, July 2006
6 ing that the commonly practiced seeding temperature of 7 C is not optimal. Because the initial step of cryopreservation (i.e., dehydration by exposure to cryoprotectants) had already caused an extensive release of CGs, effort should be directed toward modifying that step to minimize the damage and optimize the results. A new freezing protocol should be tailored for the cryopreservation of human oocytes to avoid oocyte damage and improve oocyte post-thaw survival rate. Acknowledgements: The authors thank Ruth Kaplan-Kraicer, M.Sc., Sackler Faculty of Medicine, Tel Aviv University, and Tal Rom, M.Sc., and Ayelet Itzkovitz, M.Sc., IVF Unit, Sapir Medical Center, Kfar Saba, for their technical assistance and Leonid Mittelman, M.D., Sackler Faculty of Medicine, for his assistance in confocal microscopy. This work is in partial fulfillment of the requirements for the Ph.D. degree of Y. Ghetler, Sackler Faculty of Medicine, Tel Aviv University. REFERENCES 1. Parkering TA, Tsunoda Y, Chang MC. Effects of various low temperatures, cryoprotective agents and cooling rates on the survival, fertilizability and development of frozen-thawed mouse eggs. J Exp Zool 1976;197: Al-Hasani S, Diedrich K, van der Ven H, Reinecke A, Hartje M, Krebs D. Cryopreservation of human oocytes. Hum Reprod 1987;2: Vincent C, Pickering SJ, Johnson MH. The hardening effect of dimethylsulphoxyde on the mouse zona pellucida requires the presence of an oocyte and is associated with a reduction in the number of cortical granules present. J Reprod Fertil 1990;89: Baka SG, Toth TH, Veek LL, Jones HW, Muasher SJ, Lanzendorf SE. Evaluation of the spindle apparatus of in vitro matured human oocytes following cryopreservation. Hum Reprod 1995;10: Borini A, Bonu MA, Coticchio G, Bianchi V, Cattoli M, Flamigni C. Pregnancies and births after oocyte cryopreservation. Fertil Steril 2004; 82: Rienzi L, Martinez F, Ubaldi F, Minasi MG, Iacobelli M, Tesarik J, Greco E. Polscope analysis of meiotic spindle changes in living metaphase II human oocytes during the freezing and thawing procedures. Hum Reprod 2004;19: Bianchi V, Coticchio G, Fava L, Flamigni C, Borini A. Meiotic spindle imaging in human oocytes frozen with a slow freezing procedure involving high sucrose concentration. Hum Reprod 2005;20: Tucker MJ, Morton PC, Wright G, Massey JB. Birth after cryopreservation of immature oocytes with subsequent in vitro maturation. Fertil Steril 1998;70: Kim SS, Soules MR, Bataglia DE. Follicular development, ovulation, and corpus luteum formation in cryopreserved ovarian tissue after xenotransplantation. Fertil Steril 2002;78: Oktay K, Economos K, Kan M, Rucinski J, Veek L, Rosenwaks Z. Endocrine function and oocyte retrieval after autologous transplantation of ovarian cortical strip to the forearm. JAMA 2001;286: Porcu E, Fabrri R, Seracchioli R, Chiotti P, Magrini O, Flamigni C. Birth of a healthy female after intracytoplasmic sperm injection of cryopreserved human oocytes. Fertil Steril 1997;68: Tucker MJ, Morton PC, Wright G, Sweitzer CL, Massey JB. Clinical application of human egg cryopreservation. Hum Reprod 1998;13: Fabbri R, Porcu E, Marsella T, Rocchetta G, Venturoli S, Flamigni C. Human oocyte cryopreservation: new perspectives regarding oocyte survival. Hum Reprod 2001;16: Hunter JE, Bernard A, Fuller B, Amso N, Shaw RW. Fertilization and development of the human oocyte following exposure to cryoprotectants, low temperatures and cryopreservation: a comparison of two techniques. Hum Reprod 1991;6: Paynter SJ, Cooper A, Gregory L, Fuller BJ, Shaw RW. Permeability characteristics of human oocytes in the presence of dimethylsulphoxide. Hum Reprod 1999;14: Trounson A, Sjoblom P. Cleavage and development of human embryos in vitro after ultrarapid freezing and thawing. Fertil Steril 1988;50: Hsieh YY, Tsai HD, Chang CC, Chang CC, LO HU, Lai ACH. Ultrarapid cryopreservation of human embryos: experience with 1582 embryos. Fertil Steril 1999;72: Hunter JE, Fuller BJ, Bernard A, Jackson A, Shaw RW. Vitrification of human oocytes following minimal exposure to cryoprotectants; initial studies on fertilization and embryonic development. Hum Reprod 1995; 10: Jelinkova L, Selman HA, Arav A, Strehler E, Reeka N, Sterzik K. Twin pregnancy after vitrification of 2-pronuclei human embryos. Fertil Steril 2002;77: Vajta G. Vitrification of the oocytes and embryos of domestic animals. Anim Reprod Sci 2000;60 61: Martino A, Songsagen N, Leibo SP. Development into blastocysts of bovine oocytes cryopreserved by ultra-rapid cooling. Biol Reprod 1996; 54: Arav A, Yavin S, Zeron J, Natan D, Dekel I, Gacitua H. New trends in gamete s cryopreservation. Mol Cell Endocrinol 2002;187: Kazem R, Thompson LA, Srikantharajah A, Laing MA, Hamilton MPR, Templeton A. Cryopreservation of human oocytes and fertilization by two techniques: in vitro fertilization and intracytoplasmic sperm injection. Hum Reprod 1995;10: Cran DG, Esper CR. Cortical granules and the cortical reaction in mammals. J Reprod Fertil Suppl 1990;42: Ducibella T, Duffy P, Buetow J. Quantification and localization of cortical granules during oogenesis in the mouse. Biol Reprod 1994;50: Connors SA, Kanatsu-Shinohara M, Schultz RM, Kopf G. Involvement of the cytoskeleton in the movement of cortical granules during oocyte maturation, and cortical granules anchoring in mouse eggs. Dev Biol 1998;200: Wessel GM, Brooks JM, Green E, Haley S, Voronina E, Wong J, et al. The biology of cortical granules. Int Rev Cytol 2001;209: Schalkoff ME, Oskowitz SP, Powers RD. Ultrastructural observations of human and mouse oocytes treated with cryopreservatives. Biol Reprod 1989;40: Van Blerkom J, Davis PW. Cytogenetic, cellular and developmental consequences of cryopreservation of immature and mature mouse and human oocytes. Microsc Res Techn 1994;27: Jones A, Van Blerkom J, Davis P, Toledo AA. Cryopreservation of metaphase II human oocytes effects mitochondrial membrane potential: implications for developmental competence. Hum Reprod 2004;19: Wood MJ, Whittingham DG, Lee SH. Fertilization failure of frozen mouse oocytes is not due to premature cortical granule release. Biol Reprod 1992;46: Shulman A, Ghetler Y, Beyth Y, Ben Nun I. The significance of early (premature) rise of plasma progesterone in in-vitro fertilization cycles induced by a long protocol of gonadotropin releasing hormone analogue and human menopausal gonadotropins. J Assist Reprod Genet 1996;13: Van Steirteghem A, Nagy ZP, Joris H, Liu J, Staessen C, Smitz J, Wisato A, Devroy P. High fertilization and implantation rate after intracytoplasmic sperm injection. Hum Reprod 1993;8: Ghetler Y, Raz T, Ben Nun I, Shalgi R. Cortical granules reaction after intracytoplasmic sperm injection. Mol Hum Reprod 1998;4: Cherr GN, Drobnis EZ, Katz DF. Localization of cortical granule constituents before and after exocytosis in the hamster egg. J Exp Zool 1988;246: Karnovsky MJ. A formaldehyde-glutaraldehyde fixative of high osmolarity for use in electron microscopy. J Cell Biol 1965;27:137a. Fertility and Sterility 215
7 37. Raz T, Skutelsky E, Amihai D, Hammel I, Shalgi R. Mechanisms leading to cortical reaction in the mammalian egg. Mol Reprod Dev 1998;51: Al-Hasani S, Ludwig M, Gagsteiger F, Kupfer W, Sturm R, Yilmaz A, et al. Comparison of cryopreservation of supernumerary pronuclear human oocytes obtained after intracytoplasmic sperm injection and after conventional in-vitro fertilization. Hum Reprod 1998;11: Van der Elst J. Oocyte freezing: here to stay? Hum Reprod Update 2003;5: Zeron Y, Pearl M, Borochov A, Arav A. Kinetic and temporal factors influence chilling injury to germinal vesicle and mature bovine oocytes. Cryobiology 1999;38: Wusteman MC, Pegg DE, Robinson MP, Wang LH, Fitch P. Vitrification media: toxicity, permeability, and dielectric properties. Cryobiology 2002;44: Inagaki N, Suzuki S, Kuji N, Kitai H, Nagatogawa N, Nozawa S. Egg activation induced by osmotic pressure change and the effect of amiloride on the cryopreservation of mouse oocytes. Mol. Hum Reprod 1996;2: Mattioli M, Barboni B, Luisa G, Loi P. Cold-induced calcium elevation triggers DNA fragmentation in immature pig oocytes. Mol Reprod Dev 2003;65: Ben-Yosef D, Oron Y, Shalgi R. Low temperature and fertilizationinduced Ca 2 changes in rat eggs. Mol Reprod Dev 1995;42: Hyttel P, Vajta G, Callesen H. Vitrification of bovine oocytes with the open pulled straw method: ultrastructural consequences. Mol Reprod Dev 2000;56: Trad FS, Toner M, Biggers JD. Effects of cryoprotectants and iceseeding temperature on intracellular freezing and survival of human oocytes. Hum Reprod 1999;14: Ghetler et al. Cortical granules in cryopreserved human oocytes Vol. 86, No. 1, July 2006
Cryopreservation of human oocytes with slow freezing techniques
 ESHRE Campus Symposium Cryobiology and cryopreservation of human gametes and embryos Athens, Greece 25-26 September 2009 Cryopreservation of human oocytes with slow freezing techniques Giovanni Coticchio
ESHRE Campus Symposium Cryobiology and cryopreservation of human gametes and embryos Athens, Greece 25-26 September 2009 Cryopreservation of human oocytes with slow freezing techniques Giovanni Coticchio
Improved human oocyte development after vitrification: a comparison of thawing methods
 FERTILITY AND STERILITY VOL. 72, NO. 1, JULY 1999 Copyright 1999 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Improved human oocyte
FERTILITY AND STERILITY VOL. 72, NO. 1, JULY 1999 Copyright 1999 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Improved human oocyte
Report of four donor-recipient oocyte cryopreservation cycles resulting in high pregnancy and implantation rates
 Report of four donor-recipient oocyte cryopreservation cycles resulting in high pregnancy and implantation rates Jason Barritt, Ph.D., Martha Luna, M.D., Marlena Duke, M.Sc., Lawrence Grunfeld, M.D., Tanmoy
Report of four donor-recipient oocyte cryopreservation cycles resulting in high pregnancy and implantation rates Jason Barritt, Ph.D., Martha Luna, M.D., Marlena Duke, M.Sc., Lawrence Grunfeld, M.D., Tanmoy
FERTILITY PRESERVATION. Juergen Eisermann, M.D., F.A.C.O.G South Florida Institute for Reproductive Medicine South Miami Florida
 FERTILITY PRESERVATION Juergen Eisermann, M.D., F.A.C.O.G South Florida Institute for Reproductive Medicine South Miami Florida 1 2 3 4 Oocyte Cryopreservation Experimental option Offer to single cancer
FERTILITY PRESERVATION Juergen Eisermann, M.D., F.A.C.O.G South Florida Institute for Reproductive Medicine South Miami Florida 1 2 3 4 Oocyte Cryopreservation Experimental option Offer to single cancer
The 5th World congress of the INTERNATIONAL SOCIETY FOR FERTILITY PRESERVATION Vienna, Austria November 16-18, 2017
 Vitrification: "Robots" versus Human Comparing automated vitrification outcomes The 5th World congress of the INTERNATIONAL SOCIETY FOR FERTILITY PRESERVATION Vienna, Austria November 16-18, 2017 Zsolt
Vitrification: "Robots" versus Human Comparing automated vitrification outcomes The 5th World congress of the INTERNATIONAL SOCIETY FOR FERTILITY PRESERVATION Vienna, Austria November 16-18, 2017 Zsolt
University Hospital of Ghent, Ghent, Belgium
 FERTILITY AND STERILITY VOL. 74, NO. 3, SEPTEMBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Cryopreservation
FERTILITY AND STERILITY VOL. 74, NO. 3, SEPTEMBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Cryopreservation
Interspecies Challenges
 Cryobiological Challenges of Banking Reproductive Cells, and Tissues Interspecies Challenges Mammals Domestic species Lab animal species Endangered Species Humans (Reproductive Med) Birds Domestic species
Cryobiological Challenges of Banking Reproductive Cells, and Tissues Interspecies Challenges Mammals Domestic species Lab animal species Endangered Species Humans (Reproductive Med) Birds Domestic species
Effects of sucrose concentration on the developmental potential of human frozen thawed oocytes at different stages of maturity
 Human Reproduction Vol.19, No.10 pp. 2345 2349, 2004 Advance Access publication August 6, 2004 DOI: 10.1093/humrep/deh442 Effects of sucrose concentration on the developmental potential of human frozen
Human Reproduction Vol.19, No.10 pp. 2345 2349, 2004 Advance Access publication August 6, 2004 DOI: 10.1093/humrep/deh442 Effects of sucrose concentration on the developmental potential of human frozen
RBMOnline - Vol 14. No Reproductive BioMedicine Online; on web 14 November 2006
 RBMOnline - Vol 14. No 1. 2007 64-71 Reproductive BioMedicine Online; www.rbmonline.com/article/2455 on web 14 November 2006 Novel protocols have increased survival and fertilization rates of cryopreserved
RBMOnline - Vol 14. No 1. 2007 64-71 Reproductive BioMedicine Online; www.rbmonline.com/article/2455 on web 14 November 2006 Novel protocols have increased survival and fertilization rates of cryopreserved
Outcome of 518 salvage oocyte-cryopreservation cycles performed as a routine procedure in an in vitro fertilization program
 OOCYTE CRYOPRESERVATION Outcome of 518 salvage oocyte-cryopreservation cycles performed as a routine procedure in an in vitro fertilization program Giovanni B. La Sala, M.D., a Alessia Nicoli, B.Sc., a
OOCYTE CRYOPRESERVATION Outcome of 518 salvage oocyte-cryopreservation cycles performed as a routine procedure in an in vitro fertilization program Giovanni B. La Sala, M.D., a Alessia Nicoli, B.Sc., a
Cryopreservation of human prophase I oocytes collected from unstimulated follicles
 FERTILITY AND STERILITY Copyright c 1994 The American Fertility Society Vol. 61, No.6, June 1994 Printed on acid-free paper in U. S. A. Cryopreservation of human prophase I oocytes collected from unstimulated
FERTILITY AND STERILITY Copyright c 1994 The American Fertility Society Vol. 61, No.6, June 1994 Printed on acid-free paper in U. S. A. Cryopreservation of human prophase I oocytes collected from unstimulated
RapiDVIT & rapidwarm oocyte. Specialised media for oocyte vitrification.
 RapiDVIT & rapidwarm oocyte Specialised media for oocyte vitrification. Special media for A unique cell Cryopreservation of oocytes requires care. Some preservation techniques cause premature oocyte activation
RapiDVIT & rapidwarm oocyte Specialised media for oocyte vitrification. Special media for A unique cell Cryopreservation of oocytes requires care. Some preservation techniques cause premature oocyte activation
Vitrification: "Robots" versus Human Comparing automated vitrification outcomes
 Vitrification: "Robots" versus Human Comparing automated vitrification outcomes The 5th World congress of the INTERNATIONAL SOCIETY FOR FERTILITY PRESERVATION Vienna, Austria November 16-18, 2017 Zsolt
Vitrification: "Robots" versus Human Comparing automated vitrification outcomes The 5th World congress of the INTERNATIONAL SOCIETY FOR FERTILITY PRESERVATION Vienna, Austria November 16-18, 2017 Zsolt
 Slow freezing of mouse embryos Slow freezing of domestic animal embryos Slow freezing of human embryos 1972 1973/74 1983 Slow freezing of human embryos Slow freezing of human oocytes 1985 1989 1993 1996
Slow freezing of mouse embryos Slow freezing of domestic animal embryos Slow freezing of human embryos 1972 1973/74 1983 Slow freezing of human embryos Slow freezing of human oocytes 1985 1989 1993 1996
Pregnancies and births after oocyte cryopreservation
 FERTILITY AND STERILITY VOL. 82, NO. 3, SEPTEMBER 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Pregnancies and births after
FERTILITY AND STERILITY VOL. 82, NO. 3, SEPTEMBER 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Pregnancies and births after
Optimal ICSI timing after the first polar body extrusion in in vitro matured human oocytes
 Human Reproduction Vol.22, No.7 pp. 1991 1995, 2007 Advance Access publication on May 18, 2007 doi:10.1093/humrep/dem124 Optimal ICSI timing after the first polar body extrusion in in vitro matured human
Human Reproduction Vol.22, No.7 pp. 1991 1995, 2007 Advance Access publication on May 18, 2007 doi:10.1093/humrep/dem124 Optimal ICSI timing after the first polar body extrusion in in vitro matured human
Vitrification of Oocytes: Biological Lessons Learned From Mice, Applied to Women
 ESHRE Cryobiology Mtg Athens, Greece 9/26/09 Vitrification of Oocytes: Biological Lessons Learned From Mice, Applied to Women Gary D. Smith Ph.D., HCLD Associate Professor Director of Reproductive Sciences
ESHRE Cryobiology Mtg Athens, Greece 9/26/09 Vitrification of Oocytes: Biological Lessons Learned From Mice, Applied to Women Gary D. Smith Ph.D., HCLD Associate Professor Director of Reproductive Sciences
Ovary Transplantation, VS Oocyte Freezing
 Ovary Transplantation, VS Oocyte Freezing Outline of Talk Ovarian Tissue Cryopreservation Oocyte Cryopreservation Ovary Tissue vs Oocyte Freezing It All Begins Here The Epiblast Primordial Germ Cells Primordial
Ovary Transplantation, VS Oocyte Freezing Outline of Talk Ovarian Tissue Cryopreservation Oocyte Cryopreservation Ovary Tissue vs Oocyte Freezing It All Begins Here The Epiblast Primordial Germ Cells Primordial
Oocyte morphology does not affect post-warming survival rate in an egg-cryobanking donation program
 J Assist Reprod Genet (2011) 28:1177 1181 DOI 10.1007/s10815-011-9677-7 GAMETE BIOLOGY Oocyte morphology does not affect post-warming survival rate in an egg-cryobanking donation program Amanda Souza Setti
J Assist Reprod Genet (2011) 28:1177 1181 DOI 10.1007/s10815-011-9677-7 GAMETE BIOLOGY Oocyte morphology does not affect post-warming survival rate in an egg-cryobanking donation program Amanda Souza Setti
Outlook Truths and myths of oocyte sensitivity to controlled rate freezing
 RBMOnline - Vol 15. No 1. 2007 24-30 Reproductive BioMedicine Online; www.rbmonline.com/article/2797 on web 22 May 2007 Outlook Truths and myths of oocyte sensitivity to controlled rate freezing Giovanni
RBMOnline - Vol 15. No 1. 2007 24-30 Reproductive BioMedicine Online; www.rbmonline.com/article/2797 on web 22 May 2007 Outlook Truths and myths of oocyte sensitivity to controlled rate freezing Giovanni
Comparison of survival and embryonic development in human oocytes cryopreserved by slow-freezing and vitrification
 Comparison of survival and embryonic development in human oocytes cryopreserved by slow-freezing and vitrification Yun-Xia Cao, M.D., Ph.D., Qiong Xing, M.D., Li Li, M.D., Lin Cong, M.D., Zhi-Guo Zhang,
Comparison of survival and embryonic development in human oocytes cryopreserved by slow-freezing and vitrification Yun-Xia Cao, M.D., Ph.D., Qiong Xing, M.D., Li Li, M.D., Lin Cong, M.D., Zhi-Guo Zhang,
Original Article Vitrification of mouse oocyte versus slow freezing: evaluation of ultrastructure and developmental potential
 Int J Clin Exp Med 2018;11(12):13092-13099 www.ijcem.com /ISSN:1940-5901/IJCEM0080119 Original Article Vitrification of mouse oocyte versus slow freezing: evaluation of ultrastructure and developmental
Int J Clin Exp Med 2018;11(12):13092-13099 www.ijcem.com /ISSN:1940-5901/IJCEM0080119 Original Article Vitrification of mouse oocyte versus slow freezing: evaluation of ultrastructure and developmental
Effect of Bovine Follicular Fluid Added to the Maturation Medium on Sperm Penetration in Pig Oocytes Matured In Vitro
 Article Effect of Bovine Follicular Fluid Added to the Maturation Medium on Sperm Penetration in Pig Oocytes Matured In Vitro Abstract Naoki ISOBE Research Associate Graduate School for International Development
Article Effect of Bovine Follicular Fluid Added to the Maturation Medium on Sperm Penetration in Pig Oocytes Matured In Vitro Abstract Naoki ISOBE Research Associate Graduate School for International Development
Abstract. Introduction. RBMOnline - Vol 19. No Reproductive BioMedicine Online; on web 21 August 2009
 RBMOnline - Vol 19. No 4. 2009 521 525 Reproductive BioMedicine Online; www.rbmonline.com/article/4153 on web 21 August 2009 Article Increasing dehydration of human cleavagestage embryos prior to slow
RBMOnline - Vol 19. No 4. 2009 521 525 Reproductive BioMedicine Online; www.rbmonline.com/article/4153 on web 21 August 2009 Article Increasing dehydration of human cleavagestage embryos prior to slow
Oocyte Cryopreservation
 J. Mamm. Ova Res. Vol. 24, 2 7, 2007 2 Mini Review Oocyte Cryopreservation Masashige Kuwayama 1 * 1 Kato Ladies Clinic, Advanced Medical Research Institute of Fertility, 7-20-3, Nishishinjuku, Shinjuku,
J. Mamm. Ova Res. Vol. 24, 2 7, 2007 2 Mini Review Oocyte Cryopreservation Masashige Kuwayama 1 * 1 Kato Ladies Clinic, Advanced Medical Research Institute of Fertility, 7-20-3, Nishishinjuku, Shinjuku,
Cryotop Vitrification Affects Oocyte Quality and Embryo Developmental Potential
 Cronicon OPEN ACCESS Ling Jia*, Bo Xu*, Yu-sheng Liu and Xian-hong Tong Center for Reproductive Medicine, Anhui Provincial Hospital Affiliated to Anhui Medical University, China *These authors contributed
Cronicon OPEN ACCESS Ling Jia*, Bo Xu*, Yu-sheng Liu and Xian-hong Tong Center for Reproductive Medicine, Anhui Provincial Hospital Affiliated to Anhui Medical University, China *These authors contributed
Article Cryopreservation of immature and in-vitro matured human oocytes by vitrification
 RBMOnline - Vol 19 No 3. 2009 369-373 Reproductive BioMedicine Online; www.rbmonline.com/article//3704 on web 8 July 2009 Article Cryopreservation of immature and in-vitro matured human oocytes by vitrification
RBMOnline - Vol 19 No 3. 2009 369-373 Reproductive BioMedicine Online; www.rbmonline.com/article//3704 on web 8 July 2009 Article Cryopreservation of immature and in-vitro matured human oocytes by vitrification
Limited recovery of meiotic spindles in living human oocytes after cooling rewarming observed using polarized light microscopy
 Human Reproduction Vol.16, No.11 pp. 2374 2378, 2001 Limited recovery of meiotic spindles in living human oocytes after cooling rewarming observed using polarized light microscopy Wei-Hua Wang 1,2,4, Li
Human Reproduction Vol.16, No.11 pp. 2374 2378, 2001 Limited recovery of meiotic spindles in living human oocytes after cooling rewarming observed using polarized light microscopy Wei-Hua Wang 1,2,4, Li
Assessment of a ne w cryoloop vitrif ication protocol in the cryopreservation of mouse mature oocytes
 38 2008 2 17 1, 3,, (,,, 100730) ED15 (15 %ethylene glycol, EG + 15 % dimethylsulphoxide, DMSO),,, ( EG) (DMSO) 0 1 2 h, ;, 98. 2 %, 0 1 2 h (87. 0 % 90. 9 % 90. 3 % vs 95 %, P > 0. 05 ;91. 3 % 95. 4 %
38 2008 2 17 1, 3,, (,,, 100730) ED15 (15 %ethylene glycol, EG + 15 % dimethylsulphoxide, DMSO),,, ( EG) (DMSO) 0 1 2 h, ;, 98. 2 %, 0 1 2 h (87. 0 % 90. 9 % 90. 3 % vs 95 %, P > 0. 05 ;91. 3 % 95. 4 %
The births of ve Spanish babies from cryopreserved donated oocytes
 Human Reproduction Vol.18, No.7 pp. 1417±1421, 2003 DOI: 10.1093/humrep/deg297 The births of ve Spanish babies from cryopreserved donated oocytes N.Fosas, F.Marina, P.J.Torres, I.JoveÂ, P.MartõÂn, N.PeÂrez,
Human Reproduction Vol.18, No.7 pp. 1417±1421, 2003 DOI: 10.1093/humrep/deg297 The births of ve Spanish babies from cryopreserved donated oocytes N.Fosas, F.Marina, P.J.Torres, I.JoveÂ, P.MartõÂn, N.PeÂrez,
MORPHOLOGICAL MARKERS of OOCYTE QUALITY
 MORPHOLOGICAL MARKERS of OOCYTE QUALITY Thomas Ebner Landes- Frauen- und Kinderklinik, IVF-Unit Linz, Austria ESHRE Campus Tours April 2008 William HARVEY: Exercitationes de Generatione Animalium (1651)
MORPHOLOGICAL MARKERS of OOCYTE QUALITY Thomas Ebner Landes- Frauen- und Kinderklinik, IVF-Unit Linz, Austria ESHRE Campus Tours April 2008 William HARVEY: Exercitationes de Generatione Animalium (1651)
Article A rational approach to oocyte cryopreservation
 RBMOnline - Vol 10. No 5. 2005 578 586 Reproductive BioMedicine Online; www.rbmonline.com/article/1657 on web 28 February 2005 Article A rational approach to oocyte cryopreservation Dr Paynter was awarded
RBMOnline - Vol 10. No 5. 2005 578 586 Reproductive BioMedicine Online; www.rbmonline.com/article/1657 on web 28 February 2005 Article A rational approach to oocyte cryopreservation Dr Paynter was awarded
The Cytotoxic Effect of Cryoprotective Agents on in vitro Fertilization Rates of Mammalian Oocytes
 Cean A. et al./scientific Papers: Animal Science and Biotechnologies, 2013, 46 (2) The Cytotoxic Effect of Cryoprotective Agents on in vitro Fertilization Rates of Mammalian Oocytes Ada Cean 1,2,*, Ivan
Cean A. et al./scientific Papers: Animal Science and Biotechnologies, 2013, 46 (2) The Cytotoxic Effect of Cryoprotective Agents on in vitro Fertilization Rates of Mammalian Oocytes Ada Cean 1,2,*, Ivan
Abstract. Introduction. Materials and methods. Patients and methods
 RBMOnline - Vol 8. No 3. 344-348 Reproductive BioMedicine Online; www.rbmonline.com/article/1178 on web 20 January 2004 Article Cumulative live birth rates after transfer of cryopreserved ICSI embryos
RBMOnline - Vol 8. No 3. 344-348 Reproductive BioMedicine Online; www.rbmonline.com/article/1178 on web 20 January 2004 Article Cumulative live birth rates after transfer of cryopreserved ICSI embryos
Oocyte freezing: basics, current status and potential applications in reproductive biology
 International Journal of Animal Biotechnology, Vol.1, No.1 (Dec. 2011) ISSN 2277-4122 General article Oocyte freezing: basics, current status and potential applications in reproductive biology S. K. Gautam
International Journal of Animal Biotechnology, Vol.1, No.1 (Dec. 2011) ISSN 2277-4122 General article Oocyte freezing: basics, current status and potential applications in reproductive biology S. K. Gautam
Effect of Warming on the Survivability and Fertilizability of Vitrified Matured Bovine Oocytes
 International Journal of Agricultural Technology 2014 Vol. 10(1):49-58 Available online http://www.ijat-aatsea.com ISSN 2630-0192 (Online) Fungal Diversity Effect of Warming on the Survivability and Fertilizability
International Journal of Agricultural Technology 2014 Vol. 10(1):49-58 Available online http://www.ijat-aatsea.com ISSN 2630-0192 (Online) Fungal Diversity Effect of Warming on the Survivability and Fertilizability
Tammie Roy Genea Biomedx Sydney, Australia. Declared to be stakeholder in Genea Biomedx
 Tammie Roy Genea Biomedx Sydney, Australia Declared to be stakeholder in Genea Biomedx 1 24-25 September 2015 Madrid and Alicante, Spain Importance of cryopreservation in Assisted Reproductive Technology
Tammie Roy Genea Biomedx Sydney, Australia Declared to be stakeholder in Genea Biomedx 1 24-25 September 2015 Madrid and Alicante, Spain Importance of cryopreservation in Assisted Reproductive Technology
Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm
 Journal of Reproduction & Contraception (2005) 16 (4):195-200 ORIGINAL PAPER Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm Xin-qiang LAI 1, Wei-jie ZHU 2, Jing LI 3, Fu-xing
Journal of Reproduction & Contraception (2005) 16 (4):195-200 ORIGINAL PAPER Effects of Cryopreservation on the Ultrastructure of Human Testicular Sperm Xin-qiang LAI 1, Wei-jie ZHU 2, Jing LI 3, Fu-xing
STUDIES OF THE HUMAN UNFERTILIZED TUBAL OVUM*t
 FERTILITY AND STERILITY Copyright @ 1973 by The Williams & Wilkins Co. Vol. 24, No.8, August 1973 Printed in U.S.A. STUDIES OF THE HUMAN UNFERTILIZED TUBAL OVUM*t C. NORIEGA, M.D., AND C. OBERTI, M.D.
FERTILITY AND STERILITY Copyright @ 1973 by The Williams & Wilkins Co. Vol. 24, No.8, August 1973 Printed in U.S.A. STUDIES OF THE HUMAN UNFERTILIZED TUBAL OVUM*t C. NORIEGA, M.D., AND C. OBERTI, M.D.
Effects of Centrifugation and Lipid Removal on the Cryopreservation of in Vitro Produced Bovine Embryos at the Eight-Cell Stage
 CRYOBIOLOGY 36, 206 212 (1998) ARTICLE NO. CY982077 Effects of Centrifugation and Lipid Removal on the Cryopreservation of in Vitro Produced Bovine Embryos at the Eight-Cell Stage M. Murakami,* T. Otoi,
CRYOBIOLOGY 36, 206 212 (1998) ARTICLE NO. CY982077 Effects of Centrifugation and Lipid Removal on the Cryopreservation of in Vitro Produced Bovine Embryos at the Eight-Cell Stage M. Murakami,* T. Otoi,
Dr. Andrea Borini Clinical and Scientific Director Tecnobios Procreazione Bologna, Italy
 Oocyte Cryopreservation: Beating the Clock Dr. Andrea Borini Clinical and Scientific Director Tecnobios Procreazione Bologna, Italy Question Why do we need to cryopreserve oocytes? Answers For women suffering
Oocyte Cryopreservation: Beating the Clock Dr. Andrea Borini Clinical and Scientific Director Tecnobios Procreazione Bologna, Italy Question Why do we need to cryopreserve oocytes? Answers For women suffering
ASSISTED REPRODUCTIVE TECHNOLOGIES (ART)
 ASSISTED REPRODUCTIVE TECHNOLOGIES (ART) Dr. Herve Lucas, MD, PhD, Biologist, Andrologist Dr. Taher Elbarbary, MD Gynecologist-Obstetrician Geneva Foundation for Medical Education and research Definitions
ASSISTED REPRODUCTIVE TECHNOLOGIES (ART) Dr. Herve Lucas, MD, PhD, Biologist, Andrologist Dr. Taher Elbarbary, MD Gynecologist-Obstetrician Geneva Foundation for Medical Education and research Definitions
E.S.C. Siqueira-Pyles 1, F.C. Landim-Alvarenga 1,2
 Anim. Reprod., v.2. n.1, p.63-69, Jan./March 2005 Effect of meiotic stage on viability and developmental competence of bovine oocytes vitrified in TCM-199 and bovine follicular fluid E.S.C. Siqueira-Pyles
Anim. Reprod., v.2. n.1, p.63-69, Jan./March 2005 Effect of meiotic stage on viability and developmental competence of bovine oocytes vitrified in TCM-199 and bovine follicular fluid E.S.C. Siqueira-Pyles
Iranian Journal of Reproductive Medicine Vol.5. No.4. pp: , Autumn 2007
 Iranian Journal of Reproductive Medicine Vol.5. No.4. pp: 165-170, Autumn 2007 Comparing the viability and in vitro maturation of cumulus germinal vesicle break down (GVBD) oocyte complexes using two vitrification
Iranian Journal of Reproductive Medicine Vol.5. No.4. pp: 165-170, Autumn 2007 Comparing the viability and in vitro maturation of cumulus germinal vesicle break down (GVBD) oocyte complexes using two vitrification
Ultrarapid freezing of early cleavage stage human embryos and eight-cell mouse embryos*
 FERTILITY AND STERILITY Copyright 1988 The American Fertility Society Printed in U.S.A. Ultrarapid freezing of early cleavage stage human embryos and eight-cell mouse embryos* Alan Trounson, Ph.D.t:!:
FERTILITY AND STERILITY Copyright 1988 The American Fertility Society Printed in U.S.A. Ultrarapid freezing of early cleavage stage human embryos and eight-cell mouse embryos* Alan Trounson, Ph.D.t:!:
Abstract. Introduction. RBMOnline - Vol 8. No Reproductive BioMedicine Online; on web 15 December 2003
 RBMOnline - Vol 8. No 2. 207-211 Reproductive BioMedicine Online; www.rbmonline.com/article/1023 on web 15 December 2003 Article Determining the most optimal stage for embryo cryopreservation Anthony Anderson
RBMOnline - Vol 8. No 2. 207-211 Reproductive BioMedicine Online; www.rbmonline.com/article/1023 on web 15 December 2003 Article Determining the most optimal stage for embryo cryopreservation Anthony Anderson
Article Comparison of open and closed methods for vitrification of human embryos and the elimination of potential contamination
 RBMOnline - Vol 11. No 5. 2005 608 614 Reproductive BioMedicine Online; www.rbmonline.com/article/1925 on web 26 September 2005 Article Comparison of open and closed methods for vitrification of human
RBMOnline - Vol 11. No 5. 2005 608 614 Reproductive BioMedicine Online; www.rbmonline.com/article/1925 on web 26 September 2005 Article Comparison of open and closed methods for vitrification of human
The Outcome of Cryopreserved Human Embryos After Intracytoplasmic Sperm Injection and Traditional IVF
 CLINICAL ASSISTED REPRODUCTION The Outcome of Cryopreserved Human Embryos After Intracytoplasmic Sperm Injection and Traditional SERENA EMILIANI, 1,2,3 MARC VAN DEN BERGH, 1,2 ANNE-SOPHIE VANNIN, 1 JAMILA
CLINICAL ASSISTED REPRODUCTION The Outcome of Cryopreserved Human Embryos After Intracytoplasmic Sperm Injection and Traditional SERENA EMILIANI, 1,2,3 MARC VAN DEN BERGH, 1,2 ANNE-SOPHIE VANNIN, 1 JAMILA
Oocyte cryopreservation: slow freezing and vitrification. Laura Rienzi, Rome, Italy Senior Clinical Embryologist
 Consensus meeting on fertility preservation Barcelona, June 6 th -7 th 2011 Oocyte cryopreservation: slow freezing and vitrification Laura Rienzi, Rome, Italy Senior Clinical Embryologist Cryopreservation
Consensus meeting on fertility preservation Barcelona, June 6 th -7 th 2011 Oocyte cryopreservation: slow freezing and vitrification Laura Rienzi, Rome, Italy Senior Clinical Embryologist Cryopreservation
Center, University of Bologna, Bologna, Italy. Keywords: human oocyte cryopreservation; slow freezing; high sucrose concentration; embryo quality
 Human Reproduction Vol.23, No.8 pp. 1771 1777, 2008 Advance Access publication on May 12, 2008 doi:10.1093/humrep/den119 Freezing within 2 h from oocyte retrieval increases the efficiency of human oocyte
Human Reproduction Vol.23, No.8 pp. 1771 1777, 2008 Advance Access publication on May 12, 2008 doi:10.1093/humrep/den119 Freezing within 2 h from oocyte retrieval increases the efficiency of human oocyte
Article Human oocyte vitrification: in-vivo and in-vitro maturation outcomes
 RBMOnline - Vol 17. No 5. 2008 684-688 Reproductive BioMedicine Online; www.rbmonline.com/article/3484 on web 30 September 2008 Article Human oocyte vitrification: in-vivo and in-vitro maturation outcomes
RBMOnline - Vol 17. No 5. 2008 684-688 Reproductive BioMedicine Online; www.rbmonline.com/article/3484 on web 30 September 2008 Article Human oocyte vitrification: in-vivo and in-vitro maturation outcomes
Theoretical and experimental basis of slow freezing
 Reproductive BioMedicine Online (2011) 22, 125 132 www.sciencedirect.com www.rbmonline.com REVIEW Theoretical and experimental basis of slow freezing Lucia De Santis a, Giovanni Coticchio b, * a IVF Unit,
Reproductive BioMedicine Online (2011) 22, 125 132 www.sciencedirect.com www.rbmonline.com REVIEW Theoretical and experimental basis of slow freezing Lucia De Santis a, Giovanni Coticchio b, * a IVF Unit,
Oocyte slow freezing using a M sucrose concentration protocol: is it really the time to trash the cryopreservation machine?
 Oocyte slow freezing using a 0.2 0.3 M sucrose concentration protocol: is it really the time to trash the cryopreservation machine? Veronica Bianchi, Ph.D., Michela Lappi, B.Sc., Maria Antonietta Bonu,
Oocyte slow freezing using a 0.2 0.3 M sucrose concentration protocol: is it really the time to trash the cryopreservation machine? Veronica Bianchi, Ph.D., Michela Lappi, B.Sc., Maria Antonietta Bonu,
Optimizing human oocyte cryopreservation for fertility preservation patients: should we mature then freeze or freeze then mature?
 ORIGINAL ARTICLES: FERTILITY PRESERVATION Optimizing human oocyte cryopreservation for fertility preservation patients: should we mature then freeze or freeze then mature? Joseph A. Lee, B.S., a Jason
ORIGINAL ARTICLES: FERTILITY PRESERVATION Optimizing human oocyte cryopreservation for fertility preservation patients: should we mature then freeze or freeze then mature? Joseph A. Lee, B.S., a Jason
Name: Xueming Zhao. Professional Title: Professor. Animal embryo biotechnology, mainly including in vitro maturation (IVM), in vitro fertilization
 Name: Xueming Zhao Professional Title: Professor Telephone:86-010-62815892 Fax:86-010-62895971 E-mail: zhaoxueming@caas.cn Website: http://www.iascaas.net.cn/yjspy/dsjj/sssds/dwyzyzypz1/62040.htm Research
Name: Xueming Zhao Professional Title: Professor Telephone:86-010-62815892 Fax:86-010-62895971 E-mail: zhaoxueming@caas.cn Website: http://www.iascaas.net.cn/yjspy/dsjj/sssds/dwyzyzypz1/62040.htm Research
The first human birth from a frozen oocyte
 FERTILITY Egg freezing is no longer deemed experimental. Here are current protocols, fertility expectations, and safety outcomes as well as ethical considerations for oocyte cryopreservation. Mary E. Abusief,
FERTILITY Egg freezing is no longer deemed experimental. Here are current protocols, fertility expectations, and safety outcomes as well as ethical considerations for oocyte cryopreservation. Mary E. Abusief,
RBMOnline - Vol 15. No Reproductive BioMedicine Online; on web 19 July 2007
 RBMOnline - Vol 15. No 3. 2007 338-345 Reproductive BioMedicine Online; www.rbmonline.com/article/2889 on web 19 July 2007 Recent studies of fundamental cryobiology, empirical observations and more systematic
RBMOnline - Vol 15. No 3. 2007 338-345 Reproductive BioMedicine Online; www.rbmonline.com/article/2889 on web 19 July 2007 Recent studies of fundamental cryobiology, empirical observations and more systematic
Vitrification by Cryotop and the Maturation, Fertilization, and Developmental Rates of Mouse Oocytes
 Iran Red Crescent Med J. 215 October; 17(1): e18172. Published online 215 October 6. DOI: 1.5812/ircmj.18172 Research Article Vitrification by Cryotop and the Maturation, Fertilization, and Developmental
Iran Red Crescent Med J. 215 October; 17(1): e18172. Published online 215 October 6. DOI: 1.5812/ircmj.18172 Research Article Vitrification by Cryotop and the Maturation, Fertilization, and Developmental
Comparison and Avoidance of Toxicity of Penetrating Cryoprotectants
 Comparison and Avoidance of Toxicity of Penetrating Cryoprotectants Edyta A. Szurek 1, Ali Eroglu 1,2,3,4 * 1 Institute of Molecular Medicine and Genetics, Georgia Health Sciences University, Augusta,
Comparison and Avoidance of Toxicity of Penetrating Cryoprotectants Edyta A. Szurek 1, Ali Eroglu 1,2,3,4 * 1 Institute of Molecular Medicine and Genetics, Georgia Health Sciences University, Augusta,
Synchronization between embryo development and endometrium is a contributing factor for rescue ICSI outcome
 Reproductive BioMedicine Online (2012) 24, 527 531 www.sciencedirect.com www.rbmonline.com ARTICLE Synchronization between embryo development and endometrium is a contributing factor for rescue ICSI outcome
Reproductive BioMedicine Online (2012) 24, 527 531 www.sciencedirect.com www.rbmonline.com ARTICLE Synchronization between embryo development and endometrium is a contributing factor for rescue ICSI outcome
Maturation and Freezing of Bovine Oocytes
 Maturation and Freezing of Bovine Oocytes D. Mapes and M. E. Wells Story in Brief Immature bovine oocytes were aspirated from small to medium size follicles of bovine ovaries by needle and syringe. The
Maturation and Freezing of Bovine Oocytes D. Mapes and M. E. Wells Story in Brief Immature bovine oocytes were aspirated from small to medium size follicles of bovine ovaries by needle and syringe. The
Ultrastructure of human mature oocytes after slow cooling cryopreservation using different sucrose concentrations
 Human Reproduction Vol.22, No.4 pp. 1123 1133, 2007 Advance Access publication December 11, 2006 doi:10.1093/humrep/del463 Ultrastructure of human mature oocytes after slow cooling cryopreservation using
Human Reproduction Vol.22, No.4 pp. 1123 1133, 2007 Advance Access publication December 11, 2006 doi:10.1093/humrep/del463 Ultrastructure of human mature oocytes after slow cooling cryopreservation using
Problems in the cryopreservation of unfertilized eggs by slow cooling in dimethyl sulfoxide*
 FERTILITY AND STERILITY Vol. 52, No.5, November 1989 Copyright" 1989 The American Fertility Society Printed on acid-free paper in U.S.A. Problems in the cryopreservation of unfertilized eggs by slow cooling
FERTILITY AND STERILITY Vol. 52, No.5, November 1989 Copyright" 1989 The American Fertility Society Printed on acid-free paper in U.S.A. Problems in the cryopreservation of unfertilized eggs by slow cooling
Effect of sucrose and propylene glycol on the vitrification of sheep oocytes
 Journal of Cell and Animal Biology Vol. 7 (3), pp. 25-30, March 2013 Available online at http://www.academicjournals.org/jcab DOI: 10.5897/JCAB12.033 ISSN 1996-0867 2013 Academic Journals Full Length Research
Journal of Cell and Animal Biology Vol. 7 (3), pp. 25-30, March 2013 Available online at http://www.academicjournals.org/jcab DOI: 10.5897/JCAB12.033 ISSN 1996-0867 2013 Academic Journals Full Length Research
Sucrose concentration influences the rate of human oocytes with normal spindle and chromosome configurations after slow-cooling cryopreservation*
 Human Reproduction Vol.21, No.7 pp. 1771 1776, 2006 Advance Access publication March 20, 2006. doi:10.1093/humrep/del073 Sucrose concentration influences the rate of human oocytes with normal spindle and
Human Reproduction Vol.21, No.7 pp. 1771 1776, 2006 Advance Access publication March 20, 2006. doi:10.1093/humrep/del073 Sucrose concentration influences the rate of human oocytes with normal spindle and
Robert W. McGaughey, Ph.D.
 Robert W. McGaughey, Ph.D. Robert W. McGaughey, Ph.D. ART Laboratory Director Arizona Center for Fertility Studies EDUCATION: Augustana College B.A. 1963 University of Colorado M.A. 1965 Boston University
Robert W. McGaughey, Ph.D. Robert W. McGaughey, Ph.D. ART Laboratory Director Arizona Center for Fertility Studies EDUCATION: Augustana College B.A. 1963 University of Colorado M.A. 1965 Boston University
Retrospective analysis of outcomes following transfer of previously cryopreserved oocytes, pronuclear zygotes and supernumerary blastocysts
 Reproductive BioMedicine Online (2011) 23, 118 123 www.sciencedirect.com www.rbmonline.com ARTICLE Retrospective analysis of outcomes following transfer of previously cryopreserved oocytes, pronuclear
Reproductive BioMedicine Online (2011) 23, 118 123 www.sciencedirect.com www.rbmonline.com ARTICLE Retrospective analysis of outcomes following transfer of previously cryopreserved oocytes, pronuclear
Preimplantation genetic diagnosis: polar body and embryo biopsy
 Human Reproduction, Vol. 15, (Suppl. 4), pp. 69-75, 2000 Preimplantation genetic diagnosis: polar body and embryo biopsy Luca Gianaroli SISMER, Via Mazzini 12, 40138 Bologna, Italy Scientific Director
Human Reproduction, Vol. 15, (Suppl. 4), pp. 69-75, 2000 Preimplantation genetic diagnosis: polar body and embryo biopsy Luca Gianaroli SISMER, Via Mazzini 12, 40138 Bologna, Italy Scientific Director
Page 1 of 5 Egg Freezing Informed Consent Form version 2018 Main Line Fertility Center. Egg Freezing. Informed Consent Form
 Page 1 of 5 Egg Freezing Informed Consent Form version 2018 Egg Freezing Informed Consent Form Embryos and sperm have been frozen and thawed with good results for many years. Egg (oocyte) freezing is a
Page 1 of 5 Egg Freezing Informed Consent Form version 2018 Egg Freezing Informed Consent Form Embryos and sperm have been frozen and thawed with good results for many years. Egg (oocyte) freezing is a
How does a sperm fertilise a human egg in vitro?
 How does a sperm fertilise a human egg in vitro? A. Henry Sathananthan & Christopher Chen Monash University, Melbourne & Flinders Medical Centre, S. Australia & Singapore Sperm-oocyte fusion is the key
How does a sperm fertilise a human egg in vitro? A. Henry Sathananthan & Christopher Chen Monash University, Melbourne & Flinders Medical Centre, S. Australia & Singapore Sperm-oocyte fusion is the key
A critical appraisal of cryopreservation (slow cooling versus vitrification) of human oocytes and embryos
 Human Reproduction Update Advance Access published April 25, 2012 Human Reproduction Update, Vol.0, No.0 pp. 1 19, 2012 doi:10.1093/humupd/dms016 A critical appraisal of cryopreservation (slow cooling
Human Reproduction Update Advance Access published April 25, 2012 Human Reproduction Update, Vol.0, No.0 pp. 1 19, 2012 doi:10.1093/humupd/dms016 A critical appraisal of cryopreservation (slow cooling
Rejuvenation of Gamete Cells; Past, Present and Future
 Rejuvenation of Gamete Cells; Past, Present and Future Denny Sakkas PhD Scientific Director, Boston IVF Waltham, MA, USA Conflict of Interest I have no conflict of interest related to this presentation.
Rejuvenation of Gamete Cells; Past, Present and Future Denny Sakkas PhD Scientific Director, Boston IVF Waltham, MA, USA Conflict of Interest I have no conflict of interest related to this presentation.
Induction of the human sperm acrosome reaction by human oocytes*
 FERTILITY AND STERILITY Copyright C> 1988 The American Fertility Society Vol. 50, No.6, December 1988 Printed in U.S.A. Induction of the human sperm acrosome reaction by human oocytes* Christopher J. De
FERTILITY AND STERILITY Copyright C> 1988 The American Fertility Society Vol. 50, No.6, December 1988 Printed in U.S.A. Induction of the human sperm acrosome reaction by human oocytes* Christopher J. De
Impact of oocyte cryopreservation on embryo development
 Impact of oocyte cryopreservation on embryo development M. Cristina Magli, M.Sc., Michela Lappi, B.Sc., Anna P. Ferraretti, M.D., Alessandra Capoti, B.Sc., Alessandra Ruberti, B.Sc., and Luca Gianaroli,
Impact of oocyte cryopreservation on embryo development M. Cristina Magli, M.Sc., Michela Lappi, B.Sc., Anna P. Ferraretti, M.D., Alessandra Capoti, B.Sc., Alessandra Ruberti, B.Sc., and Luca Gianaroli,
(FITC) or rhodamine blue isothiocyanate (RBITC) for use in mixed egg-transfer experiments. Both FITC and RBITC bind to the zona pellucida
 THE LABELLING OF LIVING RABBIT OVA WITH FLUORESCENT DYES J. W. OVERSTREET Department of Anatomy and International Institute for the Study of Human Reproduction, Columbia University, College of Physicians
THE LABELLING OF LIVING RABBIT OVA WITH FLUORESCENT DYES J. W. OVERSTREET Department of Anatomy and International Institute for the Study of Human Reproduction, Columbia University, College of Physicians
A preclinical evaluation of pronuclear formation by microinjection of human spermatozoa into human oocytes
 FERTILITY AND STERILITY Copyright c 1988 The American Fertility Society Vol. 49, No.5, May 1988 Printed in U.S.A. A preclinical evaluation of pronuclear formation by microinjection of human spermatozoa
FERTILITY AND STERILITY Copyright c 1988 The American Fertility Society Vol. 49, No.5, May 1988 Printed in U.S.A. A preclinical evaluation of pronuclear formation by microinjection of human spermatozoa
Fertilization failures and abnormal fertilization after intracytoplasmic sperm injection
 Fertilization failures and abnormal fertilization after intracytoplasmic sperm injection Sean P.Flaherty 1, Dianna Payne and Colin D.Matthews Reproductive Medicine Unit, Department of Obstetrics and Gynaecology,
Fertilization failures and abnormal fertilization after intracytoplasmic sperm injection Sean P.Flaherty 1, Dianna Payne and Colin D.Matthews Reproductive Medicine Unit, Department of Obstetrics and Gynaecology,
Alterations of the cytoskeleton and polyploidy induced by cryopreservation of metaphase II mouse oocytes
 FERTILITY AND STERILITY VOL. 69, NO. 5, MAY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Alterations of the cytoskeleton
FERTILITY AND STERILITY VOL. 69, NO. 5, MAY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Alterations of the cytoskeleton
VERGE 3 Lundeberg 1. Dependence of fertilization in sea urchins, Strongylocentrotus purpuratus, on microfilament
 VERGE 3 Lundeberg 1 Dependence of fertilization in sea urchins, Strongylocentrotus purpuratus, on microfilament formation and internal calcium concentration Megan Lundeberg Amy Ruggerio and Amy Isaacson
VERGE 3 Lundeberg 1 Dependence of fertilization in sea urchins, Strongylocentrotus purpuratus, on microfilament formation and internal calcium concentration Megan Lundeberg Amy Ruggerio and Amy Isaacson
Failed fertilization after clinical intracytoplasmic sperm injection
 Failed fertilization after clinical intracytoplasmic sperm injection Reproductive BioMedicine Online 2009 Vol. 19 No.2. 216 220 Present by R4 郭恬妮 Introduction intracytoplasmic sperm injection (ICSI) choice
Failed fertilization after clinical intracytoplasmic sperm injection Reproductive BioMedicine Online 2009 Vol. 19 No.2. 216 220 Present by R4 郭恬妮 Introduction intracytoplasmic sperm injection (ICSI) choice
H.Van de Velde 1, Z.P.Nagy, H.Joris, A.De Vos and A.C.Van Steirteghem
 Human Reproduction vol.12 no.10 pp.2246 2250, 1997 Effects of different hyaluronidase concentrations and mechanical procedures for cumulus cell removal on the outcome of intracytoplasmic sperm injection
Human Reproduction vol.12 no.10 pp.2246 2250, 1997 Effects of different hyaluronidase concentrations and mechanical procedures for cumulus cell removal on the outcome of intracytoplasmic sperm injection
Cryopreservation in human assisted reproduction is now routine for embryos but remains a research procedure for oocytes
 Cryopreservation in human assisted reproduction is now routine for embryos but remains a research procedure for oocytes Jacqueline Mandelbaum 1 ' 2 ' 5, Joelle Belai'sch-Allart 3, Anne- Marie Junca 4,
Cryopreservation in human assisted reproduction is now routine for embryos but remains a research procedure for oocytes Jacqueline Mandelbaum 1 ' 2 ' 5, Joelle Belai'sch-Allart 3, Anne- Marie Junca 4,
A Vitrification Method by Means of a Straw to Prevent Infections in Mouse Pronuclear Embryos
 J. Mamm. Ova Res. Vol. 20, 124 128, 2003 124 Original A Vitrification Method by Means of a Straw to Prevent Infections in Mouse Pronuclear Embryos Mami Kumon 1 *, Yoko Kumasako 1, Takafumi Utsunomiya 1
J. Mamm. Ova Res. Vol. 20, 124 128, 2003 124 Original A Vitrification Method by Means of a Straw to Prevent Infections in Mouse Pronuclear Embryos Mami Kumon 1 *, Yoko Kumasako 1, Takafumi Utsunomiya 1
Toxic Effect of Cryoprotectants on Embryo Development in a Murine Model
 : 31 1 2004 Kor J Fertil Steril, Vol 31, No 1, 2004, 3 1 2,, 1 2 3 3 3 3 3 3 3* Toxic Effect of Cryoprotectants on Embryo Development in a Murine Model Kwan Cheal Yang 1, Hee-Gyoo Kang 2,Hoi-ChangLee 3,
: 31 1 2004 Kor J Fertil Steril, Vol 31, No 1, 2004, 3 1 2,, 1 2 3 3 3 3 3 3 3* Toxic Effect of Cryoprotectants on Embryo Development in a Murine Model Kwan Cheal Yang 1, Hee-Gyoo Kang 2,Hoi-ChangLee 3,
P.M.M.Kastrop 1, S.M.Weima, R.J.Van Kooij and E.R.Te Velde
 Human Reproduction vol.14 no.1 pp.65 69, 1999 Comparison between intracytoplasmic sperm injection and in-vitro fertilization (IVF) with high insemination concentration after total fertilization failure
Human Reproduction vol.14 no.1 pp.65 69, 1999 Comparison between intracytoplasmic sperm injection and in-vitro fertilization (IVF) with high insemination concentration after total fertilization failure
Distributions of Mitochondria and the Cytoskeleton in Hamster Embryos Developed In Vivo and In Vitro
 J. Mamm. Ova Res. Vol. 23, 128 134, 2006 128 Original Distributions of Mitochondria and the Cytoskeleton in Hamster Embryos Developed In Vivo and In Vitro Hiroyuki Suzuki 1 *, Manabu Satoh 1 ** and Katsuya
J. Mamm. Ova Res. Vol. 23, 128 134, 2006 128 Original Distributions of Mitochondria and the Cytoskeleton in Hamster Embryos Developed In Vivo and In Vitro Hiroyuki Suzuki 1 *, Manabu Satoh 1 ** and Katsuya
Cryopreservation of bovine oocytes: is cryoloop vitrification the future to preserving the female gamete?
 Cryopreservation of bovine oocytes: is cryoloop vitrification the future to preserving the female gamete? Andreas Mavrides, David Morroll To cite this version: Andreas Mavrides, David Morroll. Cryopreservation
Cryopreservation of bovine oocytes: is cryoloop vitrification the future to preserving the female gamete? Andreas Mavrides, David Morroll To cite this version: Andreas Mavrides, David Morroll. Cryopreservation
CIC Edizioni Internazionali
 Original article Oocyte vitrification/storage/handling/transportation/warming, effect on survival and clinical results in donation programmes Lodovico Parmegiani Antonio Manuel Maccarini Azzurra Rastellini
Original article Oocyte vitrification/storage/handling/transportation/warming, effect on survival and clinical results in donation programmes Lodovico Parmegiani Antonio Manuel Maccarini Azzurra Rastellini
Understanding eggs, sperm and embryos. Marta Jansa Perez Wolfson Fertility Centre
 Understanding eggs, sperm and embryos Marta Jansa Perez Wolfson Fertility Centre What does embryology involve? Aims of the embryology laboratory Creation of a large number of embryos and supporting their
Understanding eggs, sperm and embryos Marta Jansa Perez Wolfson Fertility Centre What does embryology involve? Aims of the embryology laboratory Creation of a large number of embryos and supporting their
Extended embryo culture in human assisted reproduction treatments
 Human Reproduction Vol.16, No.5 pp. 902 908, 2001 Extended embryo culture in human assisted reproduction treatments M.T.Langley 1,3, D.M.Marek 1, D.K.Gardner 2, K.M.Doody 1 and K.J.Doody 1 1 Center for
Human Reproduction Vol.16, No.5 pp. 902 908, 2001 Extended embryo culture in human assisted reproduction treatments M.T.Langley 1,3, D.M.Marek 1, D.K.Gardner 2, K.M.Doody 1 and K.J.Doody 1 1 Center for
Scanning Electron Microscopic Observations on the Sperm Penetration through the Zona Pellucida of Mouse Oocytes Fertilized in vitro
 Scanning Electron Microscopic Observations on the Sperm Penetration through the Zona Pellucida of Mouse Oocytes Fertilized in vitro Masatsugu MOTOMURA and Yutaka TOYODA School of Veterinary Medicine and
Scanning Electron Microscopic Observations on the Sperm Penetration through the Zona Pellucida of Mouse Oocytes Fertilized in vitro Masatsugu MOTOMURA and Yutaka TOYODA School of Veterinary Medicine and
A comparison of the effects of estrus cow. nuclear maturation of bovine oocytes
 A comparison of the effects of estrus cow serum and fetal calf serum on in vitro nuclear maturation of bovine oocytes J Spiropoulos, SE Long University of Bristol, School of Veterinary Science, Department
A comparison of the effects of estrus cow serum and fetal calf serum on in vitro nuclear maturation of bovine oocytes J Spiropoulos, SE Long University of Bristol, School of Veterinary Science, Department
SHORT COMMUNICATION SEOUL, SOUTH KOREA
 ( C 2006) DOI: 10.1007/s10815-005-9006-0 SHORT COMMUNICATION SEOUL, SOUTH KOREA Optimization of a Dilution Method for Human Expanded Blastocysts Vitrified Using EM Grids After Artificial Shrinkage Submitted
( C 2006) DOI: 10.1007/s10815-005-9006-0 SHORT COMMUNICATION SEOUL, SOUTH KOREA Optimization of a Dilution Method for Human Expanded Blastocysts Vitrified Using EM Grids After Artificial Shrinkage Submitted
AAB/CRB 2017 Houston, Texas
 AAB/CRB 2017 Houston, Texas Advanced Current & Future Cryogenic Technologies for ART James J. Stachecki Ph.D. Innovative Cryo Enterprises LLC Disclosures Founder of Innovative Cryo Enterprises LLC We focus
AAB/CRB 2017 Houston, Texas Advanced Current & Future Cryogenic Technologies for ART James J. Stachecki Ph.D. Innovative Cryo Enterprises LLC Disclosures Founder of Innovative Cryo Enterprises LLC We focus
Cleavage Stage Embryo Cryopreservation Slow Freezing Versus Vitrification
 Cleavage Stage Embryo Cryopreservation Slow Freezing Versus Vitrification Basak Balaban VKF American Hospital of Istanbul Assisted Reproduction Unit Head of IVF Laboratory Turkish Society of Clinical Embryologists
Cleavage Stage Embryo Cryopreservation Slow Freezing Versus Vitrification Basak Balaban VKF American Hospital of Istanbul Assisted Reproduction Unit Head of IVF Laboratory Turkish Society of Clinical Embryologists
Automation in the IVF laboratory: Results with a new device able to do both Vitrification/Rewarming of mice and bovine Oocytes and Embryos
 Automation in the IVF laboratory: Results with a new device able to do both Vitrification/Rewarming of mice and bovine Oocytes and Embryos P. Patrizio 1, Y. Natan 2, P. Levi Setti 3, M. Leong 4, A. Arav
Automation in the IVF laboratory: Results with a new device able to do both Vitrification/Rewarming of mice and bovine Oocytes and Embryos P. Patrizio 1, Y. Natan 2, P. Levi Setti 3, M. Leong 4, A. Arav
SUPPLEMENTARY MATERIAL. Sample preparation for light microscopy
 SUPPLEMENTARY MATERIAL Sample preparation for light microscopy To characterize the granulocytes and melanomacrophage centers, cross sections were prepared for light microscopy, as described in Material
SUPPLEMENTARY MATERIAL Sample preparation for light microscopy To characterize the granulocytes and melanomacrophage centers, cross sections were prepared for light microscopy, as described in Material
Assisted reproductive technology
 Assisted reproductive technology FERTILITY AND STERILITY Copyright 1994 The American Fertility Society Vol. 62, No.4, October 1994 Printed on acid-free paper in U. S. A. Cryopreservation of supernumerary
Assisted reproductive technology FERTILITY AND STERILITY Copyright 1994 The American Fertility Society Vol. 62, No.4, October 1994 Printed on acid-free paper in U. S. A. Cryopreservation of supernumerary
Slow cooling of human oocytes: ultrastructural injuries and apoptotic status
 Slow cooling of human oocytes: ultrastructural injuries and apoptotic status Roberto Gualtieri, Ph.D., a Mirella Iaccarino, B.S., b Valentina Mollo, B.S., a Marina Prisco, Ph.D., c Stefania Iaccarino,
Slow cooling of human oocytes: ultrastructural injuries and apoptotic status Roberto Gualtieri, Ph.D., a Mirella Iaccarino, B.S., b Valentina Mollo, B.S., a Marina Prisco, Ph.D., c Stefania Iaccarino,
Screening of conditions for rapid freezing of human oocytes: preliminary study toward their cryopreservation
 FERTILITY AND STERILITY Copyright~ 1989 The American Fertility Society Vol. 52, No.5, November 1989 Printed on acid-free paper in U.S.A. Screening of conditions for rapid freezing of human oocytes: preliminary
FERTILITY AND STERILITY Copyright~ 1989 The American Fertility Society Vol. 52, No.5, November 1989 Printed on acid-free paper in U.S.A. Screening of conditions for rapid freezing of human oocytes: preliminary
