Recruitment challenges of a multicenter randomized controlled varicocelectomy trial
|
|
|
- Randolph Heath
- 6 years ago
- Views:
Transcription
1 Recruitment challenges of a multicenter randomized controlled varicocelectomy trial J. C. Trussell, M.D., a Gregory M. Christman, M.D., b Dana A. Ohl, M.D., c Richard S. Legro, M.D., d Stephen A. Krawetz, Ph.D., e,f Peter J. Snyder, M.D., g Pasquale Patrizio, M.D., M.B.E., h Alex J. Polotsky, M.D., i Michael P. Diamond, M.D., e,j Peter R. Casson, M.D., k Christos Coutifaris, M.D., Ph.D., l Kurt Barnhart, M.D., M.S.C.E., l Robert G. Brzyski, M.D., Ph.D., m William D. Schlaff, M.D., i Randall Meacham, M.D., n David Shin, M.D., o Tracey Thomas, M.P.H., p Meizhuo Zhang, Ph.D., p Nanette Santoro, M.D., i Esther Eisenberg, M.D., M.P.H., q,r and Heping Zhang, Ph.D., p for the Reproductive Medicine Network a Department of Urology, SUNY Upstate University Hospital, Syracuse, New York; b Department of Obstetrics and Gynecology and c Division of Sexual and Reproductive Medicine, Department of Urology, University of Michigan, Ann Arbor, Michigan; d Department of Obstetrics and Gynecology, Pennsylvania State University School of Medicine, Hershey, Pennsylvania; e Department of Obstetrics and Gynecology and f Center for Molecular Medicine and Genetics, Wayne State University, Detroit, Michigan; g School of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania; h Department of Obstetrics and Gynecology, School of Medicine, Yale University, New Haven, Connecticut; i Department of Obstetrics and Gynecology, j School of Medicine, University of Colorado, Aurora, Colorado; Clinical and Translational Research, Wayne State University, Detroit, Michigan; k Department of Obstetrics and Gynecology, University of Vermont, Burlington, Vermont; l Division of Reproductive Endocrinology and Infertility, School of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania; m Department of Obstetrics and Gynecology, University of Texas Health Science Center, San Antonio, Texas; n Division of Urology, School of Medicine, University of Colorado, Aurora, Colorado; o Department of Urology, Hackensack University Medical Center, Hackensack, New Jersey; p Collaborative Center for Statistics in Science, School of Epidemiology and Public Health, Yale University, New Haven, Connecticut; q Obstetrics and Gynecology, Vanderbilt University Medical Center, Vanderbilt University, Nashville, Tennessee; and r Eunice Kennedy Shriver National Institute of Child Health and Human Development, Bethesda, Maryland Objective: To review reasons for suboptimal recruitment for a randomized controlled trial (RCT) of varicocelectomy versus intrauterine insemination (IUI) for treatment of male infertility and to suggest means for improving future study recruitment. Design: Survey of Reproductive Medicine Network (RMN) participating sites. Setting: Reproductive Medicine Network. Patient(s): None. Intervention(s): None. Main Outcome Measure(s): Ascertain reasons for inadequate recruitment and suggest improvements for future varicocelectomy trails. Result(s): This study screened seven and enrolled three couples, with the first couple randomized on June 30, The study was subsequently stopped on March 30, The following themes were cited most frequently by sites and therefore determined to be most likely to have played a role in suboptimal recruitment: [1] men must be screened at the beginning of a couple s infertility evaluation, [2] inclusion of infertile women who had failed previous fertility interventions appeared to be associated with the couple s intolerance of a placebo arm, and [3] an apparent bias against the use of unstimulated IUI cycles indicated a prejudicial preference for surgical intervention in the male partner. Conclusion(s): Improved recruitment may be realized through screening infertile men as early as possible while minimizing study-related time commitments. Focused patient education may promote improved equipoise and acceptance of a placebo arm in male infertility studies. Creative approaches to implementing varicocelectomy trials must be considered in addition to having a network of motivated researchers who carry a high volume of possible study participants because very large numbers may need to be screened to complete the clinical trial enrollment. (Fertil Steril Ò 2011;96: Ó2011 by American Society for Reproductive Medicine.) Key Words: Accrual, consent, enrollment, prospective, randomization, recruitment, varicocele, varicocelectomy Received September 13, 2011; revised October 19, 2011; accepted October 20, J.C.T. has nothing to disclose. G.M.C. has nothing to disclose. D.A.O. has nothing to disclose. R.S.L. has nothing to disclose. S.A.K. has nothing to disclose. P.J.S. has nothing to disclose. P.P. has nothing to disclose. A.J.P. has nothing to disclose. M.P.D. has nothing to disclose. P.R.C. has nothing to disclose. C.C. has nothing to disclose. K.B. has nothing to disclose. R.G.B. has nothing to disclose. W.D.S. has nothing to disclose. R.M. has nothing to disclose. D.S. has nothing to disclose. T.T. has nothing to disclose. M.Z. has nothing to disclose. N.S. has nothing to disclose. E.E. has nothing to disclose. H.Z. has nothing to disclose. Supported by National Institutes of Health (NIH)/Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) grants U10 HD38992 (J.C.T., R.S.L.), U10 HD (G.M.C., D.A.O.). U10 HD39005 (S.A.K., M.P.D.), U10 HD (P.P., T.T., M.Z., H.Z.), U10 HD (P.R.C.), U10 HD27049 (C.C.), U10 HD (R.G.B.), U10 HD38998 (W.D.S.). Supported by Bayer (unrestricted research grant) (A.J.P.). Clinicaltrials.gov: NCT Reprint requests: J. C. Trussell, M.D., Department of Urology, Upstate University Hospital, 750 East Adams Street, Syracuse, New York ( trusselj@upstate.edu) /$36.00 Fertility and Sterility â Vol. 96, No. 6, December doi: /j.fertnstert Copyright ª2011 American Society for Reproductive Medicine, Published by Elsevier Inc.
2 The Reproductive Medicine Network (RMN) is a multicenter clinical trial network funded by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) to formulate and conduct clinical trials focused on improving reproductive outcomes in subfertile populations. The current iteration of the RMN is unique in that it included coinvestigators from each RMN unit (RMNU) with expertise in male-factor infertility, giving them a mandate to design and implement a clinical trial specifically focused on male infertility. Two male-factor projects were developed. The first project was not implemented due to concern that an adequate numbers of patients could not be enrolled. The second project, a varicocele trial titled A Prospective, Randomized Study of Microsurgical Varicocelectomy versus No Surgery in the Treatment of Male Partners with a Palpable Varicocele and an Abnormal Semen Analysis was prioritized to begin. Unexpected poor recruitment led to closure by the Data Safety Monitoring Board (DSMB). In this article we critically review the investigators collective experience from all five participating sites in an effort to identify reasons for poor recruitment and develop methods to overcome them. MATERIALS AND METHODS We critically reviewed the experiences of each RMN site to assess patient recruitment. This feedback was obtained through teleconferences, face-to-face meetings, questionnaires ed to each participating site, and review of data submitted to the Data Coordinating Center (DCC). Upon cancellation, further feedback and pertinent information was collected from the coinvestigators, gathered into themes, and summarized. Study Overview The primary goal of the study was to determine whether varicocelectomy increased the rate of pregnancy and live birth compared with intrauterine insemination (IUI) or timed intercourse. Inclusion criteria for the varicocelectomy trial were at least 6 months of infertility as a couple and the ability to have regular intercourse. Men between 18 and 50 years of age with bilateral grade I or unilateral grades II III varicoceles on physical examination and with an abnormal semen analysis were eligible to participate. An abnormal semen analysis was defined as isolated oligospermia (a sperm concentration of between 5 and 20 million/cc) or a sperm concentration of at least 5 million/cc with sperm motility less than 50% (using World Health Organization II criteria) or a strict morphology score of less than 15% (as defined by Kruger criteria). Their female partners were between 18 and 40 years of age with evidence of at least one patent fallopian tube, a history of regular ovulatory cycles (lasting 25 to 35 days), and the ability to detect a midcycle urinary luteinizing hormone (LH) surge using an ovulation predictor kit. Exclusion criteria included previous sterilization procedures such as vasectomy or tubal ligation. Men were excluded for recurrent varicocele, the presence of retrograde ejaculation, or uncorrectable ejaculatory dysfunction. Female partners were excluded for decreased ovarian reserve as evidenced by a day-3 follicle-stimulating hormone (FSH) level of R12 miu/ml, current pregnancy, or medical contraindications to pregnancy as determined by each site investigator s local clinical practice. Figure 1 summarizes the study design. The project involved two separate randomizations: [1] eligible men were randomized to microsurgical varicocelectomy or no surgery; [2] eligible couples were randomized to start conception attempts with either timed intercourse or unstimulated intrauterine insemination (IUI). Future cycles for each couple would then alternate between timed intercourse and IUI until either a total of eight cycles had transpired or conception occurred. The unique aspect of this study design is that the placebo arm for surgical therapy included medical treatment with IUI alternating with timed intercourse. The rationale for performing unstimulated IUI was to show, as a secondary outcome, the added value of IUI over intercourse in women with normal cycles. Most of the published literature showing the potential benefit of varicocelectomy versus no surgery has focused on the incidence of pregnancy over time in couples where the female partner is not receiving ovulation induction treatment. Although it is often common clinical practice to offer controlled ovarian stimulation with IUI as a therapy for couples with varicocele-associated infertility, incorporating this methodology into the study posed a difficulty with statistical modeling to achieve sufficient power without the framework of published reference studies. We followed the methodology of prior studies (with the exception of adding unstimulated IUI) because the effectiveness of ovulation induction with IUI has never been evaluated in comparison with simple observation in this population. After 8 months of alternating timed intercourse (four) with IUI (four) cycles, the couples were to continue monthly contact with their research coordinators to track pregnancy rates and secondary outcome measures for a total of 12 months. Noting the difficulties in recruitment with our study design suggests a need for additional clinical research on the relative effectiveness of treatment options for varicocele other than surgery. Power Calculations for the Original RMN Varicocele Trial The proposed study was powered (using nquery Advisor 6.01; Statistical Solutions) to test if there would be a difference in pregnancy rates between the two main arms of the study (varicocelectomy vs. no varicocelectomy) as well as the effects of timed intercourse versus IUI. Reviews from several other studies found a pregnancy rate (over 1 year) of 33% to 36.4% in couples after varicocelectomy as compared with 16% to 20% in untreated couples (1, 2). Similar pregnancy rates (32.9% and 13.9% at 1 year) were reported (subsequent to this power analysis) by Abdel-Meguid et al. (3). A study with a similar design to the RMN trial had investigated whether varicocele treatment before IUI significantly affected IUI success rates (4). In that study, a total of 58 infertile couples were included, and the pregnancy rate was statistically significantly higher in the treated group (32.4%) when compared with the untreated group (16.7%), well within the range previously observed (1, 2). The requisite sample size was set to maintain 80% power with the significance level at.05 for a two-sided test. We examined a variety of detectable effects sizes when we fixed 50 patients in each of the four treatment groups. For convenience, we calculated the detectable differences by considering two of the treatment groups at a time (e.g., varicocelectomy followed by IUI first vs. varicocelectomy followed by timed intercourse first). With this design, we could detect an absolute difference of approximately 25% (41% vs. 16%), which was somewhat higher than but within a reasonable range of what had been previously reported. Our study power is greater than 80% if we merge four arms into two major arms each with 100 patients. The total required sample size is 200. To account for the possibility of up to 20% study dropout in both groups, the goal was to enroll 232 couples from all RMN clinical sites. This would require recruitment of about 33 couples from each of the seven (original) clinical sites of the RMN. Study-Related Feedback The RMN investigators who provided patient recruitment-related feedback included a spectrum of male reproductive specialists, 1300 Trussell et al. Varicocele trial: recruitment challenges Vol. 96, No. 6, December 2011
3 FIGURE 1 Varicocelectomy flow chart. comprising three urologists, four reproductive endocrinologists, a reproductive geneticist, and a male reproductive endocrinologist. The following factors were suggested by the investigators as possible impediments to recruitment and thus to the ability to complete the study. Limited number of sites Initially, all seven of the RMN sites were expected to participate in the trial. From this group, five sites obtained institutional review board approvals and were available to recruit for this study. During this period, three sites had a RMN coinvestigator (microsurgeon) on staff, and two sites lost their urology support (moved to a different academic center or clinical practice location). There was an effort to expand the pool of surgeon investigators to high-volume centers, which yielded two additional surgeons. One site noted limited interest of microsurgeons in this study and thus did not recruit. Bias Some investigators or referring providers may have unwittingly communicated their personal belief that IUI or varicocelectomy is clearly the better option. To these investigators, a randomized trial would not have been viewed as important or even necessary, so they would not have chosen to refer the patients who would otherwise qualify. In addition, reproductive endocrinologists may view stimulated IUI cycles as the standard of care and an unstimulated IUI cycle as an unwise option. Moreover, the potential patients tended to be older and were not typically treatment naive; thus, they were perceived as having a low tolerance for being randomized to the no varicocelectomy arm that would involve up to 4 months of no specific treatment. Many couples visit their gynecologist with fertility concerns, and the female partners are started on clomiphene citrate as an initial intervention. Many reproductive endocrinologists stated that they tend to see couples after the female partner has failed medical management; thus, the reproductive endocrinologists may not constitute the best referral source for the trial. In the era of IUI and in vitro fertilization (IVF), many couples prefer the option of aggressive treatment. Therefore, the lack of ovulation stimulation in the IUI arm would appear less attractive to those considering participation, especially if they were to wind up randomized to the nonsurgical arm. Moreover, many potentially eligible couples had already tried stimulated IUI without success. Many female partners had other reproductive issues (in addition to their male partner having a varicocele). For these patients, an unstimulated IUI cycle may not be an adequate inducement, no matter what other factors are involved. The man is an equal partner in reproduction and should undergo as timely and complete a screening as the woman, yet evaluation of the male partner beyond semen analysis is often not a part of the couple s initial infertility analysis. Couples whose only identifiable issue is a male varicocele tend to be a small subset of infertile couples, limiting the pool of eligible couples. At the point of Fertility and Sterility â 1301
4 FIGURE 2 Reproductive Medicine Network recruitment flowchart. considering enrolling in a fertility study, the men tended to push for intervention; specifically, they desired surgical intervention sooner rather than later. Moreover, they tended to see the existing interval of infertility as their placebo arm and wanted to proceed with an active intervention. DISCUSSION Increasing evidence suggests that varicocele ligation improves semen quality and pregnancy rates in couples with infertility. Unfortunately, the majority of these data come from retrospective, poorly controlled studies. The Male Infertility Best Practice Policy Committee of the American Urological Association and the Practice Committee of the American Society for Reproductive Medicine have recommended, based on the available literature, that varicocele surgery should be offered to the male partner of a couple attempting to conceive when all of the following are present: [1] a varicocele is palpable, [2] the couple has documented infertility, [3] the female partner has normal fertility or potentially correctable infertility, and [4] the male partner has one or more abnormal semen parameters or sperm function test results (5). A RCT provides level I evidence as well as the most unbiased (6) and reliable evidence for evaluating the effect of a health-care TABLE 1 Recent prospective randomized varicocelectomy trials. Prospective study Screened Chose assisted reproduction Randomized (% enrolled) Dropout Intervention/ control Nilson et al (27) 165 NA 96 (58%) NA NA Breznik et al (28) 96 NA 79 (82%) NA 38/41 Madgar et al (29) 57 NA 45 (79%) NA 25/20 Nieschlag et al (30) (10%) 203 (90%) 78 (38%) 62/63 Yamamoto et al (31) 92 NA 92 (100%) 7 (8%) 45/40 Abdel-Meguid et al (3) 251 NA 150 (60%) 5 (0.03%) 73/72 Current trial 7 1 (14%) 3 (43%) 1 (33%) 0/3 Note: NA ¼ not available Trussell et al. Varicocele trial: recruitment challenges Vol. 96, No. 6, December 2011
5 TABLE 2 Reproductive Medicine Network response to critiques of other varicocelectomy trials. Critique With IVF/ICSI, men are reluctant to risk a no treatment arm. Postoperative improved sperm parameters and pregnancy rates may take up to 5 and 7 months respectively. Sperm density improvements are better with initial sperm concentrations greater than 10 million/cc. Some studies included men with normal sperm parameters. Confounding variables included differing varicocelectomy techniques (embolization, sclerosis, or various surgical approaches). Studies included subclinical varicoceles. No assessment of semen analysis was tied to a specific time after surgery. No record was provided of the randomization technique. Studies lacked the couples baseline characteristics, including the woman s reproductive capacity. The results reported improved semen parameters and fertility rates but not live-birth rates. No information was provided on rates of dropout or loss to follow-up. RMN varicocelectomy trial Unstimulated IUI cycles provide an intervention/treatment. Study captured pregnancies and live births for up to 12 months. Participants must have: isolated oligospermia (5 20 M/cc) or concentration over 5 M/cc and motility <50% or strict Kruger morphology <15%. The only surgical option was a microsurgical inguinal/ subinguinal repair. Study only included bilateral grade I or unilateral grade II III on physical examination. We compared a screening semen analysis to a sample from 12 months after surgery. A unique identifier yielded two computer-generated randomizations: [1] surgery or not, and [2] start alternating fertility attempts with IUI or timed intercourse. We recorded a history and physical, baseline characteristics, evidence of regular periods, a patent fallopian tube, and ovarian reserve (day-3 FSH <12 miu/ml). The primary outcome was an improvement in live-birth rates. We minimized dropout rates by offering alternating IUI cycles for the first 8 (of 12) months. Note: FSH ¼ follicle-stimulating hormone; ICSI ¼ intracytoplasmic sperm injection; IUI ¼ intrauterine insemination; IVF ¼ in vitro fertilization. intervention (7, 8). However, recruiting clinicians and patients to randomized trials can be extremely difficult (9), which can result in a study being underpowered, over budget, and/or incomplete (10, 11). An underpowered study may inadvertently report that a clinically relevant effect does not have statistical significance. A finding that is not statistically significant could delay or eliminate consideration of the use of an effective intervention (9). The absence of evidence that a difference exists does not mean that a difference would not be realized if the sample size were larger (12). With increasing reliance on RCT findings for clinical and regulatory decisions (13), the importance of a successful, accurate, and properly powered trial with prompt and adequate recruitment cannot be understated. Historically, recruitment for RCTs would use trial and error (14), whereby a study would start by using multiple recruitment techniques, and then the more successful recruitment method(s) would be targeted for future efforts. It is estimated that less than 50% of the studies were able to meet their targeted enrollment, and a minority were able to meet enrollment numbers without extending the trial s time line (15 18). In addition, McDonald et al. (18) reported that the overall start to recruitment was delayed in 41% (n ¼ 47) of trials, and early recruitment problems were identified in 63% (n ¼ 77) of trials. Specific to varicoceles, a number of systematic reviews have concluded that properly conducted RCTs on the topic are scarce and often contradictory (2, 3, 19 22). The RMN s varicocelectomy study was posted on Clinicaltrails. gov on October 02, 2008, and was subsequently stopped on March 30, The interval required for institutional review board review and approval ranged from 2.0 to 3.5 months, which was similar to the time required for other studies in this same (RMN) network. The majority of the time was spent resolving unique challenges for this trial before the protocol was submitted for institutional review board review. A visual timeline for the study is provided on Figure 2. There were five sites available; two sites screened seven couples of which three were randomized. The first patient was randomized on June 3, The second site enrolled their sole patient on December 1, The study was stopped on March 3, 2011, because of the likelihood that the required number of participants could not be recruited over the projected remaining time period. Unlike three other prospective studies underway with the current iteration of the RMN for which recruitment (over 1,200 patients so far) has proceeded according to expectations, the RMN s RCT on microscopic varicocelectomy experienced not only a delayed startup but substantial difficulties with recruitment, which resulted in discontinuation. Upon review, it became apparent that the several factors played a role in this outcome, some of which are common to many RCTs but others are more specific to this trial. [1] Delayed startup for such an RCT is particularly harmful, as it reduces available recruitment time. [2] When the screening for male-factor infertility occurs late in the couples evaluation, it becomes more likely that other infertility factors will be found, rendering the couple ineligible or intolerant of male-only interventions. [3] Infertile women screened for this trial had often failed previous interventions, and when given the option, their male partners disliked entering an inactive placebo arm; instead, many men wanted to proceed directly with surgery. Fertility and Sterility â 1303
6 Review of the Literature Regarding Recruitment There have been several studies and reviews examining specific ways to improve recruitment into a RCT (9, 13, 23). Based on varicocelectomy literature, review articles, meta-analyses, and a Cochrane review, recurring critiques stand out as to why this body of literature is so difficult to assimilate. Enrollment for the most recent varicocelectomy RCTs are listed in Table 1. There is lack of consensus among reviewers, with some reviews espousing varicocelectomy benefits while others refute this conclusion (24, 25). There is thus no consensus on what constitutes the best practice, and we continue to believe that a randomized, clinical trial is necessary to answer this question in a definitive fashion. The RMN varicocelectomy trial attempted to proactively address as many controversial points as possible in its design. Table 2 lists the specific RMN protocol decisions next to critiques of prior studies. Lastly, Krause et al. (26), a single varicocelectomy RCT, reported poor recruitment, a high dropout rate of greater than 50%, and, more importantly, specific reasons for these challenges. They compared pregnancy rates 1 year after antegrade/retrograde varicocele sclerosis versus a wait and see approach. This was a collaborative, multi-institutional study involving 15 German andrology centers whose initial goal was to recruit 300 patients. These investigators provided seven reasons to account for their challenges with recruitment and follow-up evaluations: 1. Private physicians had already diagnosed males with a varicocele and referred the males to the andrology center for treatment; the men anticipated a surgical intervention. 2. Many patients and doctors prefer the immediate intervention of assisted reproductive techniques (IUI or intracytoplasmic sperm injection) as compared with waiting for slow improvement in sperm parameters (after varicocelectomy). 3. The patients themselves desired immediate, active treatment targeted to the male partner. 4. Patients and doctors found it hard to accept treatment based on computer randomization. 5. The andrology centers overestimated the number of patients presenting with varicoceles. 6. The medical staff was not sufficiently motivated to recruit patients. 7. Medical staff turnover hampered the study s record completeness. For success, complex RCTs such as this varicocelectomy study will require a flexible platform. To accomplish this, a pilot study may be considered that would allow for both an interim end-point analysis and opportunities to review recruitment challenges and adjust the protocol accordingly. Feedback provided by postenrollment patient questionnaires or even patient-based focus groups could be used to discern reasons for study declinations or suggest study improvements. Moreover, dropout rates tended to be high in this younger, mobile population and must be accounted for, either by more careful screening or larger sample sizes. Recruitment may be enhanced by offering a crossover period whereby those in the control arm can subsequently choose varicocelectomy. Finally, an opportunity for future collaboration and data pooling may be possible. For example, there is a prospective varicocelectomy study from Canada, currently awaiting accrual, looking for postvaricocelectomy improvements in fertility and testicular function (Clinical Trails.gov Identifier NCT ). To optimize any RCT recruitment, patients need to be educated in an unbiased fashion about their particular health problem. The consent process should be easy to understand and culturally sensitive. To optimize varicocelectomy RCT recruitment, male partners of infertile couples should be evaluated as early as possible. Enabling participation of clinical urologists who are interested in taking part in studies that answer important clinical questions regarding surgical treatments would increase the pool of men with varicoceles who could be recruited. Funding for such trials may need to be expanded to insurers and other funding sources interested in identifying cost-effective treatments, which could extend the life span of a slow-recruiting trial beyond the period of an NIH-funded clinical trials network (such as the RMN). REFERENCES 1. Sharlip ID, Jarow J, Belker AM, Damewood M, Howards SS, Lipshultz LI, et al. Report on varicocele and infertility. Linthicum, MD: American Urological Association; 2001: Ficarra V, Cerruto MA, Ligouri G, Mazzoni G, Minnuci S, Tracia A, et al. Treatment of varicocele in subfertile men: the Cochrane review a contrary opinion. Eur Urol 2006;49: Abdel-Meguid TA, Al-Sayyad A, Tayib A, Farsi HM. Does varicocele repair improve male infertility? An evidence-based perspective from a randomized, controlled trial. Eur Urol 2011;59: Daitch JA, Bedaiwy MA, Pasqualotto EB, Hendin BN, Hallak J, Falcone T, et al. Varicocelectomy improves intrauterine insemination success rates in men with varicocele. J Urol 2001;165: Male Infertility Best Practice Policy Committee of the American Urological Association; Practice Committee of the American Society for Reproductive Medicine. Report on varicocele and infertility. Fertil Steril 2004;82(Suppl 1):S Kunz R, Vist G, Oxman AD. Randomisation to protect against selection bias in healthcare trials. Cochrane Database Syst Rev 2007;2:MR Barton S. Which clinical studies provide the best evidence? The best RCT still trumps the best observational study. BMJ 2000;321: Sackett DL, Rosenberg WM, Gray JA, Haynes RB, Richardson WS. Evidence based medicine: what it is and what it isn t. BMJ 1996;312: Treweek S, Pitkethly M, Cook J, Kjeldstrom M, Taskila T, Johansen M, et al. Strategies to improve recruitment to randomised controlled trials. Cochrane Database Syst Rev 2010;4: Walson PD. Patient recruitment: US perspective. Pediatrics 1999;104: Easterbrook PJ, Matthews DR. Fate of research studies. J R Soc Med 1992;85: Altman DG, Bland JM. Absence of evidence is not evidence of absence. BMJ 1995;311: Caldwell PHY, Hamilton S, Tan A, Craig JC. Strategies for increasing recruitment to randomised controlled trails: Systematic review. PLoS Med 2010;7: Zifferblatt SM. Recruitment in large-scale clinical trials. In: Weiss SM, editor. Proceedings of the National Heart and Lung Institute Working Conference on health behavior. Bethesda, MD: National Institutes of Health; 1975: Charlson ME, Horwitz RI. Applying results of randomised trials to clinical practice: impact of losses before randomisation. BMJ 1984;289: Haidich AB, Ioannidis JPA. Patterns of patient enrollment in randomized controlled trials. J Clin Epidemiol 2001;54: Foy R, Parry J, Duggan A, Delaney B, Wilson S, Lewin-van den Broek NT, et al. How evidencebased are recruitment strategies for randomized controlled trials in primary care? Experience from seven studies. Fam Pract 2003;20: McDonald AM, Knight RC, Campbell MK, Entwistle VA, Grant AM, Cook JA, et al. What influences recruitment to randomised controlled trials? A review of trials funded by two UK funding agencies. Trials 2006;7: Agarwal A, Deepinder F, Cocuzza M, Agarwal A, Deepinder F, Cocuzza M, et al. Efficacy of varicocelectomy in improving semen parameters: new metaanalytical approach. Urology 2007;70: Marmar JL, Agarwal A, Prabakaran S, Agarwal R, Short RA, Benoff S, et al. Reassessing the value of varicocelectomy as a treatment for male subfertility with a new meta-analysis. Fertil Steril 2007;88: Evers JL, Collins JA. Surgery or embolization for varicocele in subfertile men. Cochrane Database Syst Rev 2004;3:CD Evers JL, Collins JA. Assessment of efficacy of varicocele repair for male subfertility: a systematic review. Lancet 2003;361: Watson JM, Torgerson DJ. Increasing recruitment to randomised trails: a review of randomised controlled trails. BMC Med Res Methodol 2006;6: Trussell et al. Varicocele trial: recruitment challenges Vol. 96, No. 6, December 2011
7 24. Evers JLH, Collins J, Clarke J. Surgery or embolization for varicoceles in subfertile men. Cochrane Database Syst Rev 2010;11: Will MA, Swain J, Fode M, Sonksen J, Christman GM, Ohl D. The great debate: varicocele treatment and impact on fertility. Fertil Steril 2011;95: Krause W, Muller HH, Schafer H, Weidner W. Does treatment of varicocele improve male fertility? Results of the Deutsche Varikozelenstudie, a multicentre study of 14 collaborating centres. Andrologia 2002;34: Nilson S, Edvinsson A, Nilson B. Improvement of semen and pregnancy rate after ligation and division of the internal spermatic vein: fact or fiction? Br J Urol 1979;51: Breznik R, Vlausavlievic V, Borko E. Treatment of varicocele and male fertility. Arch Androl 1993;30: Madgar I, Weissenberg R, Lunenfeld B, Karasik A, Goldwasser B. Controlled trail of high spermatic vein ligation for varicocele in infertile men. Fertil Steril 1995;63: Nieschlag E, Hertle L, Fischedick A, Abshagen K, Behre HM. Update on treatment of varicocele: counseling as effective as occlusion of the vena spermatica. Hum Reprod 1998;113: Yamamoto M, Hibi H, Hirata Y, Miyake K, Ishigaki T. Effect of varicocelectomy on sperm parameters and pregnancy rate in patients with subclinical varicocele: a randomized prospective controlled study. J Urol 1996;155: Fertility and Sterility â 1305
Varicocele repair for infertility: what is the evidence?
 REVIEW C URRENT OPINION Varicocele repair for infertility: what is the evidence? Vincenzo Ficarra a, Alessandro Crestani a, Giacomo Novara a, and Vincenzo Mirone b Purpose of review Considering the persistent
REVIEW C URRENT OPINION Varicocele repair for infertility: what is the evidence? Vincenzo Ficarra a, Alessandro Crestani a, Giacomo Novara a, and Vincenzo Mirone b Purpose of review Considering the persistent
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Sexual Dysfunction/Male Infertility. Kyu Hyun Kim, Joo Yong Lee, Dong Hyuk Kang 1, Hyungmin Lee 2, Ju Tae Seo 3, Kang Su Cho
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.703 Sexual Dysfunction/Male Infertility Impact of Surgical Varicocele Repair on Pregnancy Rate in Subfertile Men With Clinical Varicocele and
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.703 Sexual Dysfunction/Male Infertility Impact of Surgical Varicocele Repair on Pregnancy Rate in Subfertile Men With Clinical Varicocele and
Effect of female partner age on pregnancy rates after vasectomy reversal
 MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
Controlled trial of high spermatic vein ligation for varicocele infertile men* Avraham Karasik, M.D.:j: Benad Goldwasser, M.D.t
 Urology-andrology FERTILITY AND STERILITY Copyright 1995 American Society for Reproductive Medicine Vol. 63, No. I, January 1995 Printed on acid-free paper in U. S. A. Controlled trial of high spermatic
Urology-andrology FERTILITY AND STERILITY Copyright 1995 American Society for Reproductive Medicine Vol. 63, No. I, January 1995 Printed on acid-free paper in U. S. A. Controlled trial of high spermatic
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele
 Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
CLINICAL ASSISTED REPRODUCTION
 Journal of Assisted Reproduction and Genetics, Vol. 17, No. 4. 2000 CLINICAL ASSISTED REPRODUCTION CLINICAL ASSISTED REPRODUCTION Effect of Clinical and Semen Characteristics on Efficacy of Ovulatory Stimulation
Journal of Assisted Reproduction and Genetics, Vol. 17, No. 4. 2000 CLINICAL ASSISTED REPRODUCTION CLINICAL ASSISTED REPRODUCTION Effect of Clinical and Semen Characteristics on Efficacy of Ovulatory Stimulation
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007
 ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Intrauterine (IUI) and Donor Insemination (DI) Policy (excluding In vitro fertilisation (IVF) & Intracytoplasmic sperm injection (ICSI) treatment)
 Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Infertility services reported by men in the United States: national survey data
 MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy
 Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Subfertility B Y A L I S O N, B E N A N D J O H N
 Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
COMMISSIONING POLICY. Tertiary treatment for assisted conception services
 Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Current Evidence On Infertility Treatment
 Current Evidence On Infertility Treatment Mahmoud A.M. Abdel-Aleem Regina Kulier WHO/GFMER 2003 Problem of Infertility It is a state in which a couple, desirous of a child, cannot conceive after 12 months
Current Evidence On Infertility Treatment Mahmoud A.M. Abdel-Aleem Regina Kulier WHO/GFMER 2003 Problem of Infertility It is a state in which a couple, desirous of a child, cannot conceive after 12 months
Varicocele treatment in the light of evidence-based andrology
 Human Reproduction Update, Vol.7, No.1 pp. 65±69, 2001 Varicocele treatment in the light of evidence-based andrology A.Kamischke and E.Nieschlag 1 Institute of Reproductive Medicine of the University,
Human Reproduction Update, Vol.7, No.1 pp. 65±69, 2001 Varicocele treatment in the light of evidence-based andrology A.Kamischke and E.Nieschlag 1 Institute of Reproductive Medicine of the University,
Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen Analysis
 African Journal of Urology 1110-5704 Vol. 17, No. 4, 2011 115-121 Original article Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen
African Journal of Urology 1110-5704 Vol. 17, No. 4, 2011 115-121 Original article Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen
Understanding Infertility, Evaluations, and Treatment Options
 Understanding Infertility, Evaluations, and Treatment Options Arlene J. Morales, M.D., F.A.C.O.G. Fertility Specialists Medical Group, Inc. What We Will Cover Introduction What is infertility? Briefly
Understanding Infertility, Evaluations, and Treatment Options Arlene J. Morales, M.D., F.A.C.O.G. Fertility Specialists Medical Group, Inc. What We Will Cover Introduction What is infertility? Briefly
The use of assisted reproductive technology before male factor infertility evaluation
 Original Article The use of assisted reproductive technology before male factor infertility evaluation Madhur Nayan 1, Nahid Punjani 2, Ethan Grober 1, Kirk Lo 1,3,4, Keith Jarvi 1,3,4 1 Division of Urology,
Original Article The use of assisted reproductive technology before male factor infertility evaluation Madhur Nayan 1, Nahid Punjani 2, Ethan Grober 1, Kirk Lo 1,3,4, Keith Jarvi 1,3,4 1 Division of Urology,
MALE FACTOR. Gerald J. Matthews, M.D.,* Ellen Dakin Matthews, R.N., and Marc Goldstein, M.D.*
 FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
The evidence for insemination versus intercourse or IVF
 To inseminate or not: that s the question! The evidence for insemination versus intercourse or IVF B.Cohlen, Genk 2009 There are believers and non-believers Ovarian stimulation protocols (anti-oestrogens,
To inseminate or not: that s the question! The evidence for insemination versus intercourse or IVF B.Cohlen, Genk 2009 There are believers and non-believers Ovarian stimulation protocols (anti-oestrogens,
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Varicocele anatomy during subinguinal microsurgical varicocelectomy in Chinese men
 ORIGINAL ARTICLE Varicocele anatomy during subinguinal microsurgical varicocelectomy in Chinese men K.-L. Lv*, J.-T. Zhuang*, L. Zhao, Z. Wan, Y.-D. Zhang, Y. Gao, X.-Z. Sun, S.-P. Qiu, C.-H. Deng & X.-A.
ORIGINAL ARTICLE Varicocele anatomy during subinguinal microsurgical varicocelectomy in Chinese men K.-L. Lv*, J.-T. Zhuang*, L. Zhao, Z. Wan, Y.-D. Zhang, Y. Gao, X.-Z. Sun, S.-P. Qiu, C.-H. Deng & X.-A.
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
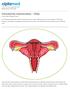 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Chapter 1. Chapter 2. Chapter 3
 Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Subfertility & prognostic factors & intrauterine insemination
 Subfertility & prognostic factors & intrauterine insemination N.Cem FIÇICIOĞLU, M.D., Ph.D. Professor and Director Department of Gynecology & Obstetrics and IVF Center Yeditepe University, School of Medicine
Subfertility & prognostic factors & intrauterine insemination N.Cem FIÇICIOĞLU, M.D., Ph.D. Professor and Director Department of Gynecology & Obstetrics and IVF Center Yeditepe University, School of Medicine
MALE FACTOR. Preoperative semen analysis as a predictor of seminal improvement following varicocelectomy
 FERTILITY AND STERILITY VOL. 75, NO. 1, JANUARY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Preoperative
FERTILITY AND STERILITY VOL. 75, NO. 1, JANUARY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Preoperative
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Bleeding and spontaneous abortion after therapy for infertility
 FERTILITY AND STERILITY VOL. 74, NO. 3, SEPTEMBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Bleeding and spontaneous
FERTILITY AND STERILITY VOL. 74, NO. 3, SEPTEMBER 2000 Copyright 2000 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Bleeding and spontaneous
Infertility: A Generalist s Perspective
 Infertility: A Generalist s Perspective Learning Objectives Fertility and Lifestyle: Patient education Describe the basic infertility workup Basic treatment strategies unexplained Heather Huddleston, MD
Infertility: A Generalist s Perspective Learning Objectives Fertility and Lifestyle: Patient education Describe the basic infertility workup Basic treatment strategies unexplained Heather Huddleston, MD
Blackpool CCG. Policies for the Commissioning of Healthcare. Assisted Conception
 1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
Fertility Policy. December Introduction
 Fertility Policy December 2015 Introduction Camden Clinical Commissioning Group (CCG) is responsible for commissioning a range of health services including hospital, mental health and community services
Fertility Policy December 2015 Introduction Camden Clinical Commissioning Group (CCG) is responsible for commissioning a range of health services including hospital, mental health and community services
Does the duration of infertility affect semen parameters and pregnancy rate after varicocelectomy? A retrospective study
 Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
DESTINATION :FAMILY. Reproductive Services TABLE OF CONTENTS
 DESTINATION :FAMILY Reproductive Services TABLE OF CONTENTS Which doctor should I choose? What resources are available to help me? What is covered? How will I afford treatment? What can I do to help prepare
DESTINATION :FAMILY Reproductive Services TABLE OF CONTENTS Which doctor should I choose? What resources are available to help me? What is covered? How will I afford treatment? What can I do to help prepare
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
5/5/2010. Infertility FINANCIAL DISCLOSURE. Infertility Definition. Objectives. Normal Human Fertility. Normal Menstrual Cycle
 Infertility FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology I AM RECEIVING COMPENSATION
Infertility FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology I AM RECEIVING COMPENSATION
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
Original Research Article
 Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Chapter 8 Effect of Varicocele Treatment
 Chapter 8 Effect of Varicocele Treatment Although multiple pathophysiological derangements have been documented in varicocele, the central issue is whether or not repair of this condition improves fertility.
Chapter 8 Effect of Varicocele Treatment Although multiple pathophysiological derangements have been documented in varicocele, the central issue is whether or not repair of this condition improves fertility.
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
Recommended Interim Policy Statement 150: Assisted Conception Services
 Southampton City Clinical Commissioning Group (CCG) took on commissioning responsibility for Assisted Conception Services from 1 April 2013 for its population and agreed to adopt the interim policy recommendations
Southampton City Clinical Commissioning Group (CCG) took on commissioning responsibility for Assisted Conception Services from 1 April 2013 for its population and agreed to adopt the interim policy recommendations
International Federation of Fertility Societies. Global Standards of Infertility Care
 International Federation of Fertility Societies Global Standards of Infertility Care Standard 8 Reducing the incidence of multiple pregnancy following treatment for infertility Name Version number Author
International Federation of Fertility Societies Global Standards of Infertility Care Standard 8 Reducing the incidence of multiple pregnancy following treatment for infertility Name Version number Author
Fertility Treatment: Do not be Distracted
 Fertility Treatment: Do not be Distracted Fertility Treatment: do not be distracted by worthless recommendation Fertility Treatment: Do not be Distracted When contemplating options for fertility treatment
Fertility Treatment: Do not be Distracted Fertility Treatment: do not be distracted by worthless recommendation Fertility Treatment: Do not be Distracted When contemplating options for fertility treatment
Policy updated: November 2018 (approved by Haringey and Islington s Executive Management Team on 5 December 2018)
 Islington CCG Fertility Policy First approved: 29 January 2015 Policy updated: November 2018 (approved by Haringey and Islington s Executive Management Team on 5 December 2018) Introduction Islington CCG
Islington CCG Fertility Policy First approved: 29 January 2015 Policy updated: November 2018 (approved by Haringey and Islington s Executive Management Team on 5 December 2018) Introduction Islington CCG
Optimizing Fertility and Wellness After Cancer. Kat Lin, MD, MSCE
 Optimizing Fertility and Wellness After Cancer Kat Lin, MD, MSCE University Reproductive Care University of Washington Nov. 6, 2010 Optimism in Numbers 5-year survival rate 78% for all childhood cancers
Optimizing Fertility and Wellness After Cancer Kat Lin, MD, MSCE University Reproductive Care University of Washington Nov. 6, 2010 Optimism in Numbers 5-year survival rate 78% for all childhood cancers
One Thousand Cases of Infertility
 One Thousand Cases of Infertility Clinical Review of a Five-Year Series Robert B. Wilson, M.D. THE RECORDS of 1032 women who complained of infertility have been reviewed. These patients were seen by various
One Thousand Cases of Infertility Clinical Review of a Five-Year Series Robert B. Wilson, M.D. THE RECORDS of 1032 women who complained of infertility have been reviewed. These patients were seen by various
16 East 40 th St, 2 nd Fl, New York, NY Ph fax
 Page 1 of 9 16 East 40 th St, 2 nd Fl, New York, NY 10016 Ph 212-679-2289 fax 212-679-2288 Please complete the following: Fertility Evaluation Name: Date of birth: Age: Partner s Name: Date of birth: Age:
Page 1 of 9 16 East 40 th St, 2 nd Fl, New York, NY 10016 Ph 212-679-2289 fax 212-679-2288 Please complete the following: Fertility Evaluation Name: Date of birth: Age: Partner s Name: Date of birth: Age:
Infertility. Thomas Lloyd and Samera Dean
 Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Recent Developments in Infertility Treatment
 Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Prepare your first visit to Sakthi Fertility
 Prepare your first visit to Sakthi Fertility Infertility History Form CONTACT INFORMATION FEMALE: First Name Middle Initial Last Name Date of birth (MM/DD/YY) / / Occupation Health card number Version
Prepare your first visit to Sakthi Fertility Infertility History Form CONTACT INFORMATION FEMALE: First Name Middle Initial Last Name Date of birth (MM/DD/YY) / / Occupation Health card number Version
East and North Hertfordshire CCG. Fertility treatment and referral criteria for tertiary level assisted conception
 East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
EVALUATING THE INFERTILE PATIENT-COUPLES. Stephen Thorn, MD
 EVALUATING THE INFERTILE PATIENT-COUPLES Stephen Thorn, MD Overview The field of reproductive medicine continues to evolve rapidly by offering newer diagnostic testing and therapeutic options to improve
EVALUATING THE INFERTILE PATIENT-COUPLES Stephen Thorn, MD Overview The field of reproductive medicine continues to evolve rapidly by offering newer diagnostic testing and therapeutic options to improve
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE
 ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY
 MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
ACT TRYING TO HAVE A BABY? YOUR STEP-BY-STEP GUIDE TO ASSISTED CONCEPTION THE ACT PATHWAY
 ACT TRYING TO HAVE A BABY? YOUR STEP-BY-STEP GUIDE TO CONCEPTION THE ACT PATHWAY ACT HOW TO USE THE ACT PATHWAY BOOKLET Firstly: You are not alone. Up to 1 in 6 couples around the world will experience
ACT TRYING TO HAVE A BABY? YOUR STEP-BY-STEP GUIDE TO CONCEPTION THE ACT PATHWAY ACT HOW TO USE THE ACT PATHWAY BOOKLET Firstly: You are not alone. Up to 1 in 6 couples around the world will experience
Relation between the Number and Size of Follicles in Ovulation Induction and the Rate of Pregnancy
 Relation between the Number and Size of Follicles in Ovulation Induction and the Rate of Pregnancy Aseel Mosa Jabber M.SC.G.O. The department of Obstetrics and Gynecology, Faculty of Medicine Thi-qar university
Relation between the Number and Size of Follicles in Ovulation Induction and the Rate of Pregnancy Aseel Mosa Jabber M.SC.G.O. The department of Obstetrics and Gynecology, Faculty of Medicine Thi-qar university
Varicocele repair: does it still have a role in infertility treatment? Dan B. French, Nisarg R. Desai and Ashok Agarwal
 Varicocele repair: does it still have a role in infertility treatment? Dan B. French, Nisarg R. Desai and Ashok Agarwal Reproductive Research Center, Glickman Urological and Kidney Institute, Cleveland
Varicocele repair: does it still have a role in infertility treatment? Dan B. French, Nisarg R. Desai and Ashok Agarwal Reproductive Research Center, Glickman Urological and Kidney Institute, Cleveland
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update
 Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
Neil Goodman, MD, FACE
 Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients
 Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Varicocele: surgical techniques in 2005
 Daniel H. Williams, MD, Edward Karpman, MD, Larry I. Lipshultz, MD Department of Urology, Baylor College of Medicine, Houston, Texas, USA WILLIAMS DH, KARPMAN E, LIPSHULTZ LI. Varicocele: surgical techniques
Daniel H. Williams, MD, Edward Karpman, MD, Larry I. Lipshultz, MD Department of Urology, Baylor College of Medicine, Houston, Texas, USA WILLIAMS DH, KARPMAN E, LIPSHULTZ LI. Varicocele: surgical techniques
Approved January Waltham Forest CCG Fertility policy
 Approved January 2015 Waltham Forest CCG Fertility policy Contents 1 Introduction 1 2 Individual Funding Requests 1 2.1 Eligibility criteria 1 2.2 Number of cycles funded 2 2.3 Treatment Pathway 3 Page
Approved January 2015 Waltham Forest CCG Fertility policy Contents 1 Introduction 1 2 Individual Funding Requests 1 2.1 Eligibility criteria 1 2.2 Number of cycles funded 2 2.3 Treatment Pathway 3 Page
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Assisted Conception Policy
 Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Planning for Parenthood After a Cancer Diagnosis
 Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Cancer and Fertility Planning for Parenthood After a Cancer Diagnosis If you or someone you love is facing cancer, preserving fertility may be the last thing on your mind. But if you re a woman of childbearing
Fertility assessment and assisted conception
 Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Medical Benefit Effective: 8/15/18 Pharmacy- Formulary 1 x Next Review: 6/18 Pharmacy- Formulary 2 x Date of Origin: 7/00 Injectable Fertility Medications: Bravelle,
Drug Therapy Guidelines Applicable Medical Benefit Effective: 8/15/18 Pharmacy- Formulary 1 x Next Review: 6/18 Pharmacy- Formulary 2 x Date of Origin: 7/00 Injectable Fertility Medications: Bravelle,
2017 United HealthCare Services, Inc.
 UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Comparison of single versus double intra uterine insemination
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pathak B. Int J Reprod Contracept Obstet Gynecol. 2017 Dec;6(12):5277-5281 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20175091
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pathak B. Int J Reprod Contracept Obstet Gynecol. 2017 Dec;6(12):5277-5281 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20175091
Information Booklet. Exploring the causes of infertility and treatment options.
 Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Infertility for the Primary Care Provider
 Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Evaluation of the Effect of Varicocelectomy on Semen Parameters and Fertility
 Evaluation of the Effect of Varicocelectomy on Semen Parameters and (MBCh) 1 Abstract Background: Varicocele is the major reversible cause of male infertility. It is observed in 35% 40% of all men with
Evaluation of the Effect of Varicocelectomy on Semen Parameters and (MBCh) 1 Abstract Background: Varicocele is the major reversible cause of male infertility. It is observed in 35% 40% of all men with
Policy statement. Commissioning of Fertility treatments
 Policy statement Commissioning of Fertility treatments NB: The policy relating to commissioning of fertility treatments is unchanged from the version approved by the CCG in March 2017. The clinical thresholds
Policy statement Commissioning of Fertility treatments NB: The policy relating to commissioning of fertility treatments is unchanged from the version approved by the CCG in March 2017. The clinical thresholds
Assisted Reproduction. Rajeevi Madankumar, 1,2 James Tsang, 1 Martin L. Lesser, 1 Daniel Kenigsberg, 1 and Steven Brenner 1 INTRODUCTION
 ( C 2005) DOI: 10.1007/s10815-005-4912-8 Assisted Reproduction Clomiphene citrate induced ovulation and intrauterine insemination: effect of timing of human chorionic gonadotropin injection in relation
( C 2005) DOI: 10.1007/s10815-005-4912-8 Assisted Reproduction Clomiphene citrate induced ovulation and intrauterine insemination: effect of timing of human chorionic gonadotropin injection in relation
PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY
 ADULT UROLOGY PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY G. NABI, S. ASTERLINGS, D. R. GREENE, AND R. L. MARSH ABSTRACT Objectives. To assess
ADULT UROLOGY PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY G. NABI, S. ASTERLINGS, D. R. GREENE, AND R. L. MARSH ABSTRACT Objectives. To assess
St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16
 St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16 1 Standard Operating Procedure St Helens CCG NHS Funded Treatment for Sub Fertility Policy Version 1 Implementation Date May 2015 Review
St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16 1 Standard Operating Procedure St Helens CCG NHS Funded Treatment for Sub Fertility Policy Version 1 Implementation Date May 2015 Review
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
WHY INVESTIGATE FOR INFERTILITY
 WHY INVESTIGATE FOR INFERTILITY Intrauterine Insemination 1 About this booklet This series of booklets has been developed and written with the support of leading fertility clinics across Australia, and
WHY INVESTIGATE FOR INFERTILITY Intrauterine Insemination 1 About this booklet This series of booklets has been developed and written with the support of leading fertility clinics across Australia, and
Unexplained infertility Evidence based management
 Unexplained infertility Evidence based management Dr Mark Hamilton Consultant Gynaecologist NHS Grampian/University of Aberdeen m.hamilton@abdn.ac.uk www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc
Unexplained infertility Evidence based management Dr Mark Hamilton Consultant Gynaecologist NHS Grampian/University of Aberdeen m.hamilton@abdn.ac.uk www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc
Policy statement. Fertility treatments. This policy is unchanged from the version approved by the CCG in July 2014.
 Policy statement Fertility treatments This policy is unchanged from the version approved by the CCG in July 2014. Title Policy statement: Fertility treatments v2.0 Author Jacky Walters Approved by Kingston
Policy statement Fertility treatments This policy is unchanged from the version approved by the CCG in July 2014. Title Policy statement: Fertility treatments v2.0 Author Jacky Walters Approved by Kingston
Male infertility. The role of varicocelectomy in management of male subfertility
 Male infertility Ashok Agarwal, Fnu Deepinder and Edmund S. Sabanegh Jr Center for Reproductive Medicine, Glickman Urological and Kidney Institute, The Cleveland Clinic, Cleveland, OH, USA The role of
Male infertility Ashok Agarwal, Fnu Deepinder and Edmund S. Sabanegh Jr Center for Reproductive Medicine, Glickman Urological and Kidney Institute, The Cleveland Clinic, Cleveland, OH, USA The role of
Treating Infertility
 Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Wiltshire CCG Fertility Policy
 Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
T39: Fertility Policy Checklist
 Patient Name: Address: Date of Birth: NHS Number: Consultant/Service to whom referral will be made: Institution Lifestyle Information Latest BMI: Latest BP: Smoking Status: Has the patient been referred
Patient Name: Address: Date of Birth: NHS Number: Consultant/Service to whom referral will be made: Institution Lifestyle Information Latest BMI: Latest BP: Smoking Status: Has the patient been referred
FACT SHEET. Failure of Ovulation Blocked or Damaged Fallopian TubesHostile Cervical Mucus Endometriosis Fibroids
 FACT SHEET Overview of infertility If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the Lithuania are infertile. Infertility is defined
FACT SHEET Overview of infertility If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the Lithuania are infertile. Infertility is defined
NHS FUNDED TREATMENT FOR SUBFERTILITY. ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs
 NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
Correlation between Sperm Motility and Morphology in the Success Rate of in Vitro Fertilization Procedure
 520 AMJ December 2016 Correlation between Sperm Motility and Morphology in the Success Rate of in Vitro Fertilization Procedure Praditya Virza Ramadhan, 1 Andri Rezano, 2 Wiryawan Permadi 3 1 Faculty of
520 AMJ December 2016 Correlation between Sperm Motility and Morphology in the Success Rate of in Vitro Fertilization Procedure Praditya Virza Ramadhan, 1 Andri Rezano, 2 Wiryawan Permadi 3 1 Faculty of
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
THE PATIENT S GUIDE TO VASECTOMY REVERSAL
 The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
Induction of spermatogenesis in azoospermic men after varicocele repair
 Human Reproduction Vol.18, No.1 pp. 108±112, 2003 DOI: 10.1093/humrep/deg032 Induction of spermatogenesis in azoospermic men after varicocele repair FaÂbio F.Pasqualotto 1, AntoÃnio M.Lucon, Jorge Hallak,
Human Reproduction Vol.18, No.1 pp. 108±112, 2003 DOI: 10.1093/humrep/deg032 Induction of spermatogenesis in azoospermic men after varicocele repair FaÂbio F.Pasqualotto 1, AntoÃnio M.Lucon, Jorge Hallak,
Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes
 Advances in Urology Volume 2013, Article ID 370969, 4 pages http://dx.doi.org/10.1155/2013/370969 Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes Mustafa
Advances in Urology Volume 2013, Article ID 370969, 4 pages http://dx.doi.org/10.1155/2013/370969 Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes Mustafa
