BARTS ENDOCRINE E-PROTOCOLS REPRODUCTIVE ENDOCRINOLOGY
|
|
|
- Griffin Harper
- 5 years ago
- Views:
Transcription
1 FEMALE SCREENING FOR OVULATION INDICATION To confirm ovulation in a woman with menstrual periods who presents with infertility. [LH and FSH rise for approximately 48 hours ("surge") at the onset of the ovulatory phase. Progesterone production rises in the ovulatory phase to maximum during the luteal phase.] CONTRAINDICATIONS None specific PRECAUTIONS Test not feasible in a patient without a menstrual cycle PREPARATION Confirm menstruation. Exclude other causes of infertility (hyperprolactinaemia, chromosomal problems, thyroid dysfunction, PCOS, premature ovarian failure and structural /gynaecological causes). PROCEDURE Blood sample on day 21 of the cycle for progesterone. As cycle length sometimes variable, better to take blood on days 18, 21 and 24 (mark day of cycle on form). INTERPRETATION Progesterone >30 nmol/l between days = adequate luteal phase that cycle. SENSITIVITY AND SPECIFICITY Sensitivity 86% and specificity 83% REFERENCES Sverdloff R.S. et al., Endo. Metab. Clin. N. Amer. 17, (1988). Jordon J. Et al., Fertil Steril.62:54-62 (1994) The Practice Committee of the American Society of Reproductive Medicine. Fertil. Steril. 82, s1 (2004) PROGESTERONE CHALLENGE INDICATION To induce bleeding in amenorrhoea and to differentiate between causes of amenorrhoea.
2 CONTRAINDICATIONS Patients with previous reactions to progestogens PRECAUTIONS Exclude pregnancy as cause of amenorrhoea PREPARATION None specific PROCEDURE Medroxyprogesterone acetate 10 mg po daily for 5-10 days (depending on response) INTERPRETATION 1) If patient has bleeding within one week of stopping progesterone, then she has: sufficient oestrogen to stimulate endometrial growth and normal outflow tract These women are at risk for endometrial hyperplasia from unopposed estrogen. Treat with cyclic progesterone ( 4 times per year), or COCP if preferred. 2) If patient has no bleeding, then she has: Oestrogen deficiency (ovarian failure or hypogonadotrophic hypogonadism) or outflow tract obstruction. COCP can be used to induce menstruation if no outflow obstruction and no contraindication. Consider US/S pelvis if anovulatory state is longstanding to rule out significant hyperplasia. SENSITIVITY AND SPECIFICITY Progesterone challenge test in patients with endometrial pathology for detection of endometrial proliferation activity: sensitivity 76%, specificity 100% REFERENCES Macia M et al, Int.J.Gyn.Obs Feb:40(2):145-9 CLOMIPHENE TEST INDICATION Demonstration of the capacity for ovulation to be induced in a woman with anovulation. CONTRAINDICATIONS Pregnancy
3 Do not carry out test if body weight <50kg PRECAUTIONS Arrange by fertility clinic to enable follicle tracking by ultrasound Rarely causes abdominal bloating. Small risk of multiple pregnancy. Rarely, ovarian hyperstimulation with cardiovascular collapse, ascites and pleural effusions. PREPARATION Explain timing: first day of period = day 0). Women without cycles start test at arbitrary time. PROCEDURE Start clomiphene on day 0 of cycle and give 2-3mg/kg in divided doses (reasonable start dose is 50mg tds). Take bloods at D0, D4, D7 and D10 measuring LH, FSH, progesterone and oestradiol and follicle tracking. If the test is unsuccessful over 2 cycles, repeat using higher doses of clomiphene INTERPRETATION LH and FSH rise, probably as a consequence of an anti-oestrogen stimulating GnRH. This leads to follicular maturation, oestrogen production, LH release, and ovulation. Positive result: rise in LH (to >20 U/l). rise in FSH (to >10 U/l). rise in progesterone to >30 nmol/l. SENSITIVITY AND SPECIFICITY Poorly defined. Note: Within a general infertile population, abnormal CCT were found in 3% of women younger than 30, 7% in women aged 30-34, 10% in women aged and 26% aged 40 or older. An abnormal test predicts lower pregnancy rate with conception rate in 43% of women with normal results and 9% in those with abnormal results. REFERENCE Sverdloff R.S. et al., Endo. Metab. Clin N. Amer. 17, (1988). Scott Rt et al., Obstet Gynecol Oct;82(4Pt1):539-44
4 POLYCYSTIC OVARIAN SYNDROME DIAGNOSIS Variable criteria from different sources Need a pattern rather than a single diagnostic test NIH NICHD criteria: Both hyperandrogenism and chronic anovulation Rotterdam criteria: Two of the following conditions: hyperandrogenism; chronic anovulation; polycystic ovaries on ultrasound Androgen Excess Society criteria: Hyperandrogenism and ovarian dysfunction (including infrequent or irregular ovulation or anovulation) and/or polycystic ovaries. CLINICAL FEATURES TO RECORD Menarche Thelarche Adrenarche Current / previous menstrual cycles range of cycle length and duration of bleeding Current and previous menstrual cycle / range of duration of bleeding and range of interval from first day of bleed to first day of the next. Onset, progression and location of hirsutism Measures used to remove hair and frequency Greasy skin and acne Fertility history Temporal recession / clitoromegaly (virilisation signs) BIOCHEMICAL SUPPORTING EVIDENCE Raised LH:FSH ratio, elevated androgens, mildly elevated prolactin, low SHBG Exclude significant hyperprolactinemia, non-classical congenital adrenal hyperplasia (SST with 17-OHP), thyroid dysfunction, androgen-secreting tumours, Cushing's syndrome first (LDDST with androgens) and consider acromegaly TREATMENT There is no curative treatment Identify the most troublesome symptom(s) to manage
5 1) HYPERANDROGENAEMIA (HIRSUTISM, ALOPECIA, ACNE) Oral contraceptive pill Dianette anti-androgenic because: increases SHBG, competes for 5-alpha -reductase and decreases adrenal androgen production. (In contrast, OCP s with levonorgestrel are androgenic) Indications: Desire for regular bleeds Contraindications: Obesity, thromboembolic disease, history of breast cancer, smoker Antiandrogens Cyproterone acetate (50mg day 1-10 of cycle), spironolactone, flutamide, finasteride. Potentially teratogenic, use with reliable contraception. Vaniqa cream Apply to face. Slow to take effect (up to 4 months). May cause local irritation. Skin laser therapy Best for dark hair on fair skin. Rarely available via NHS (try Royal Free hospital) Regaine (minoxidil) Effective for androgenic alopecia but effects wear off if stopped. Available over the counter (2% solution), not NHS. 2) OLIGOMENORRHOEA Oral contraceptive pill See notes above Metformin Moderately effective at restoring cycles. Intermittent progestagens Medroxyprogesterone acetate 10 mg od for 5-10 days, 3-4 times per year. 3) SUBFERTILITY Full assessment of patient and partner to identify all contributing factor Metformin Moderately effective in restoring ovulatory cycles, but the live birth rate compared to clomiphene is poor. Not licensed for PCOS. Clomiphene citrate Via fertility unit for follicle tracking. Outcomes better than metformin in obtaining conception and live births in most, but not all, head-to-head trials.
6 Prednisolone in reversed circadian rhythm 2.5mg on rising and 5mg on retiring will effectively suppress ACTH and hence ACTH-dependent androgens. This prednisolone should not be enteric-coated as it is poorly and variably absorbed and may not cause adequate suppression. May work when all else fails but note that patients becomes steroid-dependent and will need the usual counselling regarding steroid card, sick day rules etc (see adrenal protocols). The treatment is usually associated with a return of menstrual cyclicity. Acne often improves but prenisolone alone improves hirsutism in only 25%. 4) METABOLIC DYSFUNCTION Document BMI and advise accordingly Screen for type 2 Diabetes and check lipid profile Estimate insulin resistance using HOMA-IR model: Fasting glucose (mmol/l) x Fasting Insulin (µu/ml) 22.5 = IR IR > 2.5 suggestive of insulin resistance Difficult to use this model for estimation in several circumstances including puberty REFERENCES Dunaif et al. Nature Clinical Practice Endocrinology & Metabolism (2008) vol. 4 (5) pp Koulouri et al. Clin Endocrinol (Oxf)(2008) vol. 68 (5) pp Legro et al. N. Engl. J. Med. (2007) vol. 356 (6) pp Qublan HS et al, J Obstet Gynaecol Oct;29(7): Azziz R et al, Fertil Steril Feb;91(2): Epub 2008 Oct 23. Review FEMALE HRT INDICATIONS Absence of ovarian function (eg Turner s syndrome etc) Premature ovarian failure (autoimmune, iatrogenic,idiopathic etc) Secondary ovarian failure (hypogonadotrophic hypogonadism, pituitary disease) Relief of severe menopausal symptoms
7 CONTRAINDICATIONS BARTS ENDOCRINE E-PROTOCOLS Oestrogen-driven malignancy Genetic cancer prone syndrome with History of thromboembolic disease PRECAUTIONS Oestrogen treatment can lead to nausea, headaches, breast tenderness, weight gain and hypertension these may be avoided by changing the preparation type There is an increased risk of thromboembolic disease and breast cancer depending on dose, preparation and circumstances under which the replacement is prescribed Aim to stop after 7-10 years post natural time of menopause PRINCIPLES AND PREPARATIONS The ovary makes oestrogen, progesterone and some testosterone. HRT describes oestrogen replacement in women whose own oestrogen levels are low Progesterone must be given to all women receivign oestrogen who have a uterus oestrogen alone can cause endometrial cancer and this is prevented by progesterone administration The principle of administration of HRT is for oestrogen to be administered continuously; progesterone can be given through part of the cycle, the removal of progesterone leading to a withdrawal bleed. Alternatively progesterone can be given (in older women) continuously for period-free HRT ( Continuous combined HRT. ) The combination of oestrogen and progesterone may be pre-ordained within the preparation or bespoke by prescribing the two hormones separately. Familiarise yourself with the available combinations but be aware of the types and doses of the component hormones which they contain and the cyclical dose variation Oestrogens vary by source, by route of administration and by potency Progestogens vary by source and chemical structure (first / second / third generation), by route of administration, thrombogenic potential and androgenic quality Tibolone (Livial) is a synthetic steroid with oestrogenic, progestational and androgenic properties, first marketed in 1991 for post-menopausal vasomotor symptoms. Tibolone is now also licensed for the prevention of osteoporosis - however, at present, there are no data on whether tibolone prevents fractures. You may wish to use this first line for HRT in postmenopausal women as it is free of withdrawal bleeds and particularly as the risk of thromboembolism may be lower than traditional HRT. There may be an increased stroke risk
8 especially if there are other prior risk factors in which case avoid. RCT by Cummings SR et eal also suggestive of reduction in breast cancer (although there may be a small increase in endometrial cancer) REFERENCES Cummings SR et al.the effects of tibolone in older postmenopausal women. N Engl J Med Aug 14;359(7): Oestrogen subtypes Type Route Dose equivalence Conjugated equine oestrogen oral 0.625mg standard (1.25mg available) Oestradiol valerate oral 2mg standard (1mg and 4mg also available) Oestrogen patch transdermal 50mcg is equivalent (doses of mcg per 24h available) Synthetic oestrogens eg Ethinyl oestradiol (in COCP) Greater effect on liver function Oestrogen implants oral 20mcg is equivalent to above Most COCP contain 30mcg Some COCP contain more Subcut implant Dose as BNF Local oestrogen vaginal Dose not absorbed systemically Application in gel / on pessary for local symptom relief only Progesterone subtypes Type Examples Dose equivalence / Notes First generation Norethindrone acetate Ethynodiol diacetate MPA Less androgenic than 1 st gen; more than 3 rd gen Oral or im. Oral doses mg for days 1-10 Second generation Levonorgestrel Norgestrel Norethisterone Dose 1-2.5mg pper day for part of cycle Third generation (thrombogenic) Desogestrel Norgestimate Gestodene Less androgenic, less metabolic impact Less androgenic
9 MALE SEMEN ANALYSIS Parameter Normal Value Volume >2.0ml Viscosity Normal Morphology Normal (no strict criteria for this) ph Sperm concentration (million/ml) >20 Motility Total >50%, >25% rapid progressive Vitality (% live/% dead) >50% MAR IgG (direct sperm antibody) Negative Nucleated / round cells (million/ml) <1 Leucocytes per μl <25-75 HUMAN CHORIONIC GONADOTROPHIN TEST (hcg stimulation) INDICATIONS Differential diagnosis of male hypogonadism, looking at Leydig cell function. CONTRAINDICATIONS / PRECAUTIONS None PROCEDURE hcg 2000 units IM on days 0 and 2 / Paediatric dose < 2 years, 1000 units daily for 3 days. Samples for testosterone on days 0, 2 and 4. INTERPRETATION Normal response is for testosterone to rise to outside the normal range. This shows that a testis is present, which may be intraabdominal if none palpable. In gonadotrophin deficiency, without primary testicular abnormality, the low basal testosterone value should triple after hcg. SENSITIVITY AND SPECIFICITY Most studies done in children so the values would not apply to our patients REFERENCES Tzvetkova P et al., Systems Biol Reprod Med. Jan 1997;39:163-71
10 TESTOSTERONE REPLACEMENT Testosterone therapy is used for male patients with hypogonadism. Therapy is usually started when the serum testosterone level is less than 9 nmol/l (normal range: 9-35 nmol/l). However, metaanalyses have shown positvie results in some patients with a serum testosterone <12 nmol/l (the grey zone ) There are a number of preparations that are available for use. These include testosterone injection, implant, oral tablets and transdermal patches. General side effects include prostatic disorders, gynaecomastia, mood disorders, hypertension, dizziness and changes to laboratory tests (polycythaemia and lipid changes). Careful and regular monitoring of the prostate gland and breast must be performed at least once yearly and twice yearly in elderly patients and at-risk (with clinical and familial factors). Prior to testosterone initiation, all patients must undergo a detailed examination in order to exclude a risk of pre-existing prostate cancer (do not prescribe if total serum PSA > 4 ng/ml). Contraindications include: Cancer patients at risk of hypercalcaemia due to bone metastases. Hypertension (relative contraindication only) Epilepsy Migraine Testosterone injection (Sustanon and testosterone enanthate) Injection intramuscularly 2-4 weekly. Variable testosterone levels which may be clinically apparent. Aim to keep peak (7 days after injection) and trough (prior to next injection) within the reference range. NB Arachis oil excipient relevant for patients with peanut allergy Long-acting testosterone formulation for injection (nebido) By deep intramuscular injection Initial injection 1g then second injection after 6 weeks for more rapid achievement of steady state. Injections thereafter every weeks dictated by serum testosterone and clinical status Testosterone implants (pellets implanted every 6 months) Insertion by trained individual. Pellets may be extruded after insertion.
11 Oral testosterone undecanoate Short half life therefore tds administration Erratic testosterone levels (monitor DHT rather than testosterone) Disproportionately high DHT levels (theoretically greater risk of polycythaemia and raised PSA) Transdermal patches (andropatch) Stable levels but high incidence of skin irritation and may be fiddly to use Testogel and Testim (and tostran) Transdermal testosterone gel applied to skin. Well tolerated although sachets fiddly and instructions to wait before showering. 50mg of testosterone applied once daily. Maximum of 100mg per day can be used. Only 9-14% of the dose is bioavailable and therefore 50mg/day gel will deliver 5mg/day testosterone. The patient himself should administer the application, onto clean, dry, healthy skin over both shoulders or both arms or abdomen. These gels can be transferred to other persons by close skin to skin contact, resulting in increased testosterone serum levels and possible adverse effects. The doctor must inform the patient carefully about the risk of testosterone transfer and about safety instructions as set out in the Summary of Product Characteristics (SPC). Testim comes in a more convenient tube packaging but has a distinctive odour. Tostran available in metred-dose delivery bottle and higher concentration (therefore smaller volume of application) FERTILITY INDUCTION IN HYPOGONADOTROPHIC HYPOGONADISM INDICATION Induction of spermatogenesis in patients with hypogonadotrophic hypogonadism, by replacing LH and FSH CONTRAINDICATIONS Untreated cause of infertility in partner
12 PRECAUTIONS BARTS ENDOCRINE E-PROTOCOLS Discontinue testosterone replacement Couples must be warned that medical therapy can take months to years to reach maximal effect and so must be counselled about other options [assisted reproduction /adoption.] PROCEDURE (Variants of regime in use: discuss with individual consultant) Document testosterone level and sperm count at outset Prescribe hcg (Pregnyl) 1500iu subcutaneously twice per week for 6 months. hcg has the action of pituitary LH. LH stimulates the Leydig cells to make testosterone. If levels exceed the upper limit of normal (30nmol/l), the dose can be halved.. Different sperm induction regimes are in current use: discuss with individual consultant. One option is to prescribe 6 months of LH action (via Pregnyl) alone, adding in FSH only if sperm count still < 10 million / ml after 6 months. After 6 months prescribe Menopur 150 units subcutaneously three times a week. Menopur contains 75u LH and 75u FSH. The aim of this is for the FSH component to hopefully induce spermatogenesis. The LH component of Menopur is not an issue in sperm induction and therefore, no adjustment of the Pregnyl dose is necessary Some consultants prefer to prescribe FSH concurrently with LH from the outset of therapy. If FSH action inactive at a dose of 150 units subcutaneously 3 times a week, increase to 300 units three times a week (some consultants prescribe 300 units three times a week as the starting dose) For FSH action, an alternative to menopur is follitropin-alfa or Gonal-F. This may be more readily available although is more expensive. The dose is equivalent. Check testosterone levels and semen analysis at 3 months and 6 months after starting therapy. The dose of both Pregnyl and Menopur can be halved if testosterone levels exceed 30nmol/l. Note that patients (especially with acquired diseases like NFPA) get pregnant very early on in this regimen (ie with very poor sperm counts). If successful induction of spermatogenesis occurs consider sperm freezing at 6 months. The maximal duration of treatment is debated although on average conception occurs 2-3 years of gonadotrophin therapy and therapy should probably not be further continued. Preparations of high-purity synthetic FSH are available, but these are needed for stimulation of follicles in females, where LH will of course cause problems. These high-purity preparations are more expensive, and are not required in males, where LH is given anyway, provided that menopur is available REFERENCES Liu PY et al., JCEM 2009 Mar;94(3): Epub 2008 Dec 9 Mahukar et al., J Androl. 2009;30:95-112
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Definition: the diagnostic criteria Evidence of hyperandrogenism, biochemical &/or clinical (hirsutism, acne & male pattern baldness). Ovulatory dysfunction; amenorrhoea; oligomenorrhoea
Polycystic Ovary Syndrome Definition: the diagnostic criteria Evidence of hyperandrogenism, biochemical &/or clinical (hirsutism, acne & male pattern baldness). Ovulatory dysfunction; amenorrhoea; oligomenorrhoea
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018
 Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Amenorrhoea: polycystic ovary syndrome
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
12/13/2017. Important references for PCOS. Polycystic Ovarian Syndrome (PCOS) for the Family Physician. 35 year old obese woman
 Polycystic Ovarian Syndrome (PCOS) for the Family Physician Barbara S. Apgar MD, MS Professor or Family Medicine University of Michigan Ann Arbor, Michigan Important references for PCOS Endocrine Society
Polycystic Ovarian Syndrome (PCOS) for the Family Physician Barbara S. Apgar MD, MS Professor or Family Medicine University of Michigan Ann Arbor, Michigan Important references for PCOS Endocrine Society
PCOS and Obesity DUB is better treated by OCPs
 PCOS and Obesity DUB is better treated by OCPs Dr. Ritu Joshi Senior consultant Fortis escorts Hospital, Jaipur Chairperson Family welfare com. FOGSI (20092012) Vice President FOGSI 2014 Introduction One
PCOS and Obesity DUB is better treated by OCPs Dr. Ritu Joshi Senior consultant Fortis escorts Hospital, Jaipur Chairperson Family welfare com. FOGSI (20092012) Vice President FOGSI 2014 Introduction One
Case Questions. Polycystic Ovarian Syndrome: Treatment Goals and Options. Differential Diagnosis of Hyperandrogenic Anovulation
 Polycystic Ovarian Syndrome: Treatment Goals and Options Marc Cornier, MD Division of Endocrinology, Metabolism and Diabetes Colorado Center for Health and Wellness University of Colorado School of Medicine
Polycystic Ovarian Syndrome: Treatment Goals and Options Marc Cornier, MD Division of Endocrinology, Metabolism and Diabetes Colorado Center for Health and Wellness University of Colorado School of Medicine
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guideline for the Investigation and Management of Polycystic Ovary Syndrome Author: Contact Name and Job Title
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guideline for the Investigation and Management of Polycystic Ovary Syndrome Author: Contact Name and Job Title
UPDATE: Women s Health Issues
 UPDATE: Women s Health Issues Renee B. Alexis, MD, MBA, MPH, FACOG Associate Professor Department of OBGYN Kiran C. Patel College of Osteopathic Medicine Disclosure of Conflicts of Interest I have no financial
UPDATE: Women s Health Issues Renee B. Alexis, MD, MBA, MPH, FACOG Associate Professor Department of OBGYN Kiran C. Patel College of Osteopathic Medicine Disclosure of Conflicts of Interest I have no financial
Overview of Reproductive Endocrinology
 Overview of Reproductive Endocrinology I have no conflicts of interest to report. Maria Yialamas, MD Female Hypothalamic--Gonadal Axis 15 4 Hormone Secretion in the Normal Menstrual Cycle LH FSH E2, Progesterone,
Overview of Reproductive Endocrinology I have no conflicts of interest to report. Maria Yialamas, MD Female Hypothalamic--Gonadal Axis 15 4 Hormone Secretion in the Normal Menstrual Cycle LH FSH E2, Progesterone,
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Polycystic Ovary Syndrome (PCOS):
 Polycystic Ovary Syndrome (PCOS): Current diagnosis and treatment Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the end of this presentation,
Polycystic Ovary Syndrome (PCOS): Current diagnosis and treatment Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the end of this presentation,
Dr Mary Birdsall. Fertility Associates Auckland
 Dr Mary Birdsall Fertility Associates Auckland Period Problems Mary Birdsall Medical Director Fertility Associates Auckland Period Problems Basic Physiology No Periods Irregular Periods Heavy Periods
Dr Mary Birdsall Fertility Associates Auckland Period Problems Mary Birdsall Medical Director Fertility Associates Auckland Period Problems Basic Physiology No Periods Irregular Periods Heavy Periods
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is common. It can cause period problems, reduced fertility, excess hair growth, and acne. Many women with PCOS are also overweight. Treatment
Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is common. It can cause period problems, reduced fertility, excess hair growth, and acne. Many women with PCOS are also overweight. Treatment
Estrogens and progestogens
 Estrogens and progestogens Estradiol and Progesterone hormones produced by the gonads are necessary for: conception embryonic maturation development of primary and secondary sexual characteristics at puberty.
Estrogens and progestogens Estradiol and Progesterone hormones produced by the gonads are necessary for: conception embryonic maturation development of primary and secondary sexual characteristics at puberty.
Female Reproductive Endocrinology
 Female Reproductive Endocrinology Dr. Channa Jayasena PhD MRCP FRCPath Clinical Senior Lecturer & Consultant Endocrinologist Department of Gynaecology, Hammersmith Hospital Anovulation is a common cause
Female Reproductive Endocrinology Dr. Channa Jayasena PhD MRCP FRCPath Clinical Senior Lecturer & Consultant Endocrinologist Department of Gynaecology, Hammersmith Hospital Anovulation is a common cause
Topics. Periods Menopause & HRT Contraception Vulva problems
 Girls stuff Topics Periods Menopause & HRT Contraception Vulva problems Menorrhagia Excessive menstrual loss occurring with regular or irregular cycles Ovulatory Anovulatory Usual blood loss 30-40ml per
Girls stuff Topics Periods Menopause & HRT Contraception Vulva problems Menorrhagia Excessive menstrual loss occurring with regular or irregular cycles Ovulatory Anovulatory Usual blood loss 30-40ml per
12/27/2013. Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND
 Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND 7% of all women 18-45 Obesity 1/3 of all US women Incidence of PCOS is increasing with increase obesity Obesity Irregular
Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND 7% of all women 18-45 Obesity 1/3 of all US women Incidence of PCOS is increasing with increase obesity Obesity Irregular
Infertility for the Primary Care Provider
 Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU)
 ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
Hormonal Control of Human Reproduction
 Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Polycystic Ovarian Syndrome (PCOS) LOGO
 Polycystic Ovarian Syndrome (PCOS) Ma qianhong Ob/Gyn Department LOGO Contents Epidemiology and Definition Pathophysiology, Endocrinological Features Diagnostic Criteria Treatment Prognosis Introduction
Polycystic Ovarian Syndrome (PCOS) Ma qianhong Ob/Gyn Department LOGO Contents Epidemiology and Definition Pathophysiology, Endocrinological Features Diagnostic Criteria Treatment Prognosis Introduction
13 th Annual Women s Health Day PCOS. Saturday 02/09/2017 Dr Mathias Epee-Bekima O&G Consultant KEMH
 13 th Annual Women s Health Day PCOS Saturday 02/09/2017 Dr Mathias Epee-Bekima O&G Consultant KEMH Learning objectives Perform the appropriate investigations in women where there is a clinical suspicion
13 th Annual Women s Health Day PCOS Saturday 02/09/2017 Dr Mathias Epee-Bekima O&G Consultant KEMH Learning objectives Perform the appropriate investigations in women where there is a clinical suspicion
Abnormal Uterine Bleeding Case Studies
 Case Study 1 Abnormal Uterine Bleeding Case Studies Abigail, a 24 year old female, presents to your office complaining that her menstrual cycles have become a problem. They are now lasting 6 7 days instead
Case Study 1 Abnormal Uterine Bleeding Case Studies Abigail, a 24 year old female, presents to your office complaining that her menstrual cycles have become a problem. They are now lasting 6 7 days instead
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Kathleen Colleran, MD Professor of Medicine University of New Mexico HSC Presented for COMM-TC May 4, 2012 Objectives Understand the pathophysiology of PCOS Understand how to
Polycystic Ovary Syndrome Kathleen Colleran, MD Professor of Medicine University of New Mexico HSC Presented for COMM-TC May 4, 2012 Objectives Understand the pathophysiology of PCOS Understand how to
Polycystic Ovary Syndrome
 What is the polycystic ovary syndrome? Polycystic Ovary Syndrome The polycystic ovary syndrome (PCOS) is a clinical diagnosis characterized by the presence of two or more of the following features: irregular
What is the polycystic ovary syndrome? Polycystic Ovary Syndrome The polycystic ovary syndrome (PCOS) is a clinical diagnosis characterized by the presence of two or more of the following features: irregular
 www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc Conflict of interest none Outline Causes of ovulatory dysfunction Assessment of women with ovulatory dysfunction Management First line Second
www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc Conflict of interest none Outline Causes of ovulatory dysfunction Assessment of women with ovulatory dysfunction Management First line Second
New PCOS guidelines: What s relevant to general practice
 New PCOS guidelines: What s relevant to general practice Dr Michael Costello Fertility Specialist IVF Australia UNSW Royal Hospital for Women Sydney How do we know if something is new? Louvre Museum, Paris
New PCOS guidelines: What s relevant to general practice Dr Michael Costello Fertility Specialist IVF Australia UNSW Royal Hospital for Women Sydney How do we know if something is new? Louvre Museum, Paris
Hypogonadism 4/27/2018. Male Hypogonadism -- Definition. Epidemiology. Objectives HYPOGONADISM. Men with Hypogonadism. 95% untreated.
 Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
Clinical Problems in the Diagnosis and Treatment of PCOS During Adolescence
 Clinical Problems in the Diagnosis and Treatment of PCOS During Adolescence R a c h a n a S h a h, M D M S T A s s i s t a n t P r o f e s s o r o f P e d i a t r i c s D i v i s i o n o f E n d o c r
Clinical Problems in the Diagnosis and Treatment of PCOS During Adolescence R a c h a n a S h a h, M D M S T A s s i s t a n t P r o f e s s o r o f P e d i a t r i c s D i v i s i o n o f E n d o c r
Polycystic Ovarian Syndrome. Heidi Hallonquist, MD Concord Hospital Concord Obstetrics and Gynecology
 Polycystic Ovarian Syndrome Heidi Hallonquist, MD Concord Hospital Concord Obstetrics and Gynecology Outline Definition Symptoms Causal factors Diagnosis Complications Treatment Why are we talking about
Polycystic Ovarian Syndrome Heidi Hallonquist, MD Concord Hospital Concord Obstetrics and Gynecology Outline Definition Symptoms Causal factors Diagnosis Complications Treatment Why are we talking about
National Gender Identity Clinical Network for Scotland (NGICNS)
 National Gender Identity Clinical Network for Scotland (NGICNS) Endocrine Management of Adult Transgender Patients Revised 7 th July 2016 (First published 11 August 2015) This guidance is based on the
National Gender Identity Clinical Network for Scotland (NGICNS) Endocrine Management of Adult Transgender Patients Revised 7 th July 2016 (First published 11 August 2015) This guidance is based on the
Principles of Ovarian Stimulation
 Principles of Ovarian Stimulation Dr Genia Rozen Gynaecologist and Fertility Specialist Royal Women s Hospital and Melbourne IVF Learning objectives Why ovarian stimulation Recap physiology Ovarian cycle
Principles of Ovarian Stimulation Dr Genia Rozen Gynaecologist and Fertility Specialist Royal Women s Hospital and Melbourne IVF Learning objectives Why ovarian stimulation Recap physiology Ovarian cycle
REPRODUCTIVE ENDOCRINOLOGY
 Overview REPRODUCTIVE ENDOCRINOLOGY Specialist Portfolio Seminar 23 rd June 2014 Katie Jones Sandwell and West Birmingham Hospitals NHS Trust Hypothalamic pituitary gonadal axis Females Males Overview
Overview REPRODUCTIVE ENDOCRINOLOGY Specialist Portfolio Seminar 23 rd June 2014 Katie Jones Sandwell and West Birmingham Hospitals NHS Trust Hypothalamic pituitary gonadal axis Females Males Overview
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal myomectomy in leiomyoma management, 77 Abnormal uterine bleeding (AUB) described, 103 105 normal menstrual bleeding vs., 104
Index Note: Page numbers of article titles are in boldface type. A Abdominal myomectomy in leiomyoma management, 77 Abnormal uterine bleeding (AUB) described, 103 105 normal menstrual bleeding vs., 104
Menopause & HRT. Rosie & Alex. Image:
 Menopause & HRT Rosie & Alex Image: http://www.keepcalm-o-matic.co.uk/ Menopause The permanent cessation of menstruation for 12 months When does it happen? Average age 51 Image: Nature Medicine - 12, 612-613
Menopause & HRT Rosie & Alex Image: http://www.keepcalm-o-matic.co.uk/ Menopause The permanent cessation of menstruation for 12 months When does it happen? Average age 51 Image: Nature Medicine - 12, 612-613
2-Hypertrichosis:- Hypertrichosis is the
 Hirsutism And Virilization Hirsutism:- Is the development of androgen-dependent dependent terminal body hair in a woman in places in which terminal hair is normally not found, terminal body hairs are the
Hirsutism And Virilization Hirsutism:- Is the development of androgen-dependent dependent terminal body hair in a woman in places in which terminal hair is normally not found, terminal body hairs are the
Ovaries: In Sickness and Health. Mr N Pisal Consultant Gynaecologist The Portland Hospital
 Ovaries: In Sickness and Health Mr N Pisal Consultant Gynaecologist The Portland Hospital Topics for discussion How to assess ovarian function? AMH PCOS Ovarian pain Ovarian cysts Ovarian screening Menopause
Ovaries: In Sickness and Health Mr N Pisal Consultant Gynaecologist The Portland Hospital Topics for discussion How to assess ovarian function? AMH PCOS Ovarian pain Ovarian cysts Ovarian screening Menopause
Polycystic Ovary Syndrome (PCOS)
 Mr Nabil Haddad M. OBSTET, GYNAEC, FRCOG Consultant Gynaecologist Patient Information Polycystic Ovary Syndrome (PCOS) Mr Nabil Haddad Consultant Gynaecologist What is Polycystic Ovary Syndrome (PCOS)?
Mr Nabil Haddad M. OBSTET, GYNAEC, FRCOG Consultant Gynaecologist Patient Information Polycystic Ovary Syndrome (PCOS) Mr Nabil Haddad Consultant Gynaecologist What is Polycystic Ovary Syndrome (PCOS)?
Hyperandrogenism. Dr Jack Biko. MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany)
 Hyperandrogenism Dr Jack Biko MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany) 2012 Hyperandrogenism Excessive production of androgens Adrenal glands main source
Hyperandrogenism Dr Jack Biko MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany) 2012 Hyperandrogenism Excessive production of androgens Adrenal glands main source
Reproductive FSH. Analyte Information
 Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Management of polycystic ovarian syndrome
 14 Disorders of male and female sex hormones Management of polycystic ovarian syndrome LI-WEI CHO AND STEPHEN L. ATKIN Patients with polycystic ovarian syndrome can be challenging as they usually present
14 Disorders of male and female sex hormones Management of polycystic ovarian syndrome LI-WEI CHO AND STEPHEN L. ATKIN Patients with polycystic ovarian syndrome can be challenging as they usually present
What is PCOS? PCOS THE CONQUER PCOS E-BOOK. You'll be amazed when you read this...
 PCOS What is PCOS? You'll be amazed when you read this... What is PCOS?. Who is at risk? How to get tested? What are the complications. Is there a cure? What are the right ways to eat? What lifestyle changes
PCOS What is PCOS? You'll be amazed when you read this... What is PCOS?. Who is at risk? How to get tested? What are the complications. Is there a cure? What are the right ways to eat? What lifestyle changes
North of Tyne and Gateshead Area Prescribing Committee GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA
 North of Tyne and Gateshead Area Prescribing Committee GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care July 2014 (Minor update November 2014) (Review
North of Tyne and Gateshead Area Prescribing Committee GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care July 2014 (Minor update November 2014) (Review
Dr Stella Milsom. Endocrinologist Fertility Associates Auckland. 12:30-12:40 When Puberty is PCO
 Dr Stella Milsom Endocrinologist Fertility Associates Auckland 12:30-12:40 When Puberty is PCO Puberty or Polycystic Ovary Syndrome? Stella Milsom Endocrinologist Auckland DHB, University of Auckland,
Dr Stella Milsom Endocrinologist Fertility Associates Auckland 12:30-12:40 When Puberty is PCO Puberty or Polycystic Ovary Syndrome? Stella Milsom Endocrinologist Auckland DHB, University of Auckland,
Picking the Perfect Pill How to Effectively Choose an Oral Contraceptive
 Focus on CME at Queen s University Picking the Perfect Pill How to Effectively Choose an Oral Contraceptive By Susan Chamberlain, MD, FRCSC There are over 20 oral contraceptive (OC) preparations on the
Focus on CME at Queen s University Picking the Perfect Pill How to Effectively Choose an Oral Contraceptive By Susan Chamberlain, MD, FRCSC There are over 20 oral contraceptive (OC) preparations on the
Polycystic Ovary Syndrome
 Page 1 of 5 Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is common. It can cause period problems, reduced fertility, excess hair growth, and acne. Many women with PCOS are also overweight.
Page 1 of 5 Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is common. It can cause period problems, reduced fertility, excess hair growth, and acne. Many women with PCOS are also overweight.
Cigna Drug and Biologic Coverage Policy
 Cigna Drug and Biologic Coverage Policy Subject Infertility Injectables Table of Contents Coverage Policy... 1 General Background...16 Coding/Billing Information...20 References...20 Effective Date...
Cigna Drug and Biologic Coverage Policy Subject Infertility Injectables Table of Contents Coverage Policy... 1 General Background...16 Coding/Billing Information...20 References...20 Effective Date...
Estrogens & Antiestrogens
 Estrogens & Antiestrogens Menstrual cycle... Changes and hormonal events Natural estrogens: Estadiol >> Estrone > Estriol Ineffective orally Synthesis: From cholesterol ; role of aromatase enzyme in converting
Estrogens & Antiestrogens Menstrual cycle... Changes and hormonal events Natural estrogens: Estadiol >> Estrone > Estriol Ineffective orally Synthesis: From cholesterol ; role of aromatase enzyme in converting
GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA. Information for Primary Care December 2015 (Review Date June 2016)
 GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care December 2015 (Review Date June 2016) Further information on this guideline can be obtained from: Claire
GUIDELINES FOR THE USE OF FEMINISING HORMONE THERAPY IN GENDER DYSPHORIA Information for Primary Care December 2015 (Review Date June 2016) Further information on this guideline can be obtained from: Claire
 Objectives 1. Be able to describe the classic presentation and diagnostic criteria 2. Be able to explain long-term health concerns associated with the diagnosis 3. Understand what basic treatment options
Objectives 1. Be able to describe the classic presentation and diagnostic criteria 2. Be able to explain long-term health concerns associated with the diagnosis 3. Understand what basic treatment options
Women s Issues in Epilepsy. Esther Bui, Epilepsy Fellow MD, FRCPC
 Women s Issues in Epilepsy Esther Bui, Epilepsy Fellow MD, FRCPC How are women different? Different habitus Different metabolism Different co-morbidities Different psychosocial stigma Different hormonal
Women s Issues in Epilepsy Esther Bui, Epilepsy Fellow MD, FRCPC How are women different? Different habitus Different metabolism Different co-morbidities Different psychosocial stigma Different hormonal
Hirsutism - Management
 Hirsutism - Management Scenario: Diagnosis of hirsutism How do I know my patient has it? Look for excessive terminal hair in androgen-dependent areas including the face, chest, linea alba, lower back,
Hirsutism - Management Scenario: Diagnosis of hirsutism How do I know my patient has it? Look for excessive terminal hair in androgen-dependent areas including the face, chest, linea alba, lower back,
Prof.Dr. Nabil Lymon Head of Internal Medicine Department
 By Prof.Dr. Nabil Lymon Head of Internal Medicine Department Definitions: Hirsutism: Is the presence of terminal hair in androgendependent sites where hair does not normally grow in women. This hair growth
By Prof.Dr. Nabil Lymon Head of Internal Medicine Department Definitions: Hirsutism: Is the presence of terminal hair in androgendependent sites where hair does not normally grow in women. This hair growth
PCOS. Kirtly Parker Jones MD
 PCOS Kirtly Parker Jones MD OBJECTIVES The participant will be able to use knowledge about ovarian physiology to council perimenarchal women about irregular periods The participant will be able to evaluate
PCOS Kirtly Parker Jones MD OBJECTIVES The participant will be able to use knowledge about ovarian physiology to council perimenarchal women about irregular periods The participant will be able to evaluate
Western Locality Shared care information ~ Gonadorelin Analogues (Gnrh)
 Western Locality Shared care information ~ Gonadorelin Analogues (Gnrh) Specialist: Please complete the Shared Care letter sending a request to GP (see bottom of the page) April 2013 GP: Please indicate
Western Locality Shared care information ~ Gonadorelin Analogues (Gnrh) Specialist: Please complete the Shared Care letter sending a request to GP (see bottom of the page) April 2013 GP: Please indicate
Polycystic Ovary Syndrome (PCOS)
 Polycystic Ovary Syndrome (PCOS) What are Polycystic Ovaries? Polycystic ovaries are slightly larger than normal ovaries and have twice the number of follicles (small cysts). Polycystic ovaries are very
Polycystic Ovary Syndrome (PCOS) What are Polycystic Ovaries? Polycystic ovaries are slightly larger than normal ovaries and have twice the number of follicles (small cysts). Polycystic ovaries are very
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
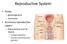 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Premature Menopause : Diagnosis and Management
 Guideline Number 3 : August 2010 Premature Menopause : Diagnosis and Management Introduction : Premature menopause is a serious condition that affects young women and remains an enigma. The challenges
Guideline Number 3 : August 2010 Premature Menopause : Diagnosis and Management Introduction : Premature menopause is a serious condition that affects young women and remains an enigma. The challenges
CREATING A PCOS TREATMENT PLAN. Ricardo Azziz, M.D., M.P.H., M.B.A. Georgia Regents University
 CREATING A PCOS TREATMENT PLAN Ricardo Azziz, M.D., M.P.H., M.B.A. Georgia Regents University PCOS: CREATING A TREATMENT PLAN Good treatment plans are based on sound and complete evaluations History of
CREATING A PCOS TREATMENT PLAN Ricardo Azziz, M.D., M.P.H., M.B.A. Georgia Regents University PCOS: CREATING A TREATMENT PLAN Good treatment plans are based on sound and complete evaluations History of
POTION OR POISON? MEDICAL TREATMENT ALTERNATIVES TO THE PILL. Lester Ruppersberger, D.O., FACOOG,CNFPI NFP only Gynecologist
 POTION OR POISON? MEDICAL TREATMENT ALTERNATIVES TO THE PILL Lester Ruppersberger, D.O., FACOOG,CNFPI NFP only Gynecologist THE PILL Released to US market in 1960 10-15 x dose of hormones in HRT Over 10-14
POTION OR POISON? MEDICAL TREATMENT ALTERNATIVES TO THE PILL Lester Ruppersberger, D.O., FACOOG,CNFPI NFP only Gynecologist THE PILL Released to US market in 1960 10-15 x dose of hormones in HRT Over 10-14
Polycystic Ovary Syndrome Therapy Dr. Pilar Vigil MD, PhD, FACOG
 Polycystic Ovary Syndrome Therapy Dr. Pilar Vigil MD, PhD, FACOG What is an ovulatory dysfunction? Mrs. Susana Godoy, Nurse-Midwife San José, Costa Rica Abril 2018 PONTIFICIA UNIVERSIDAD CATÓLICA DE CHILE
Polycystic Ovary Syndrome Therapy Dr. Pilar Vigil MD, PhD, FACOG What is an ovulatory dysfunction? Mrs. Susana Godoy, Nurse-Midwife San José, Costa Rica Abril 2018 PONTIFICIA UNIVERSIDAD CATÓLICA DE CHILE
Primary and secondary amenorrhoea
 BRITISH MEDICAL JOURNAL VOLUME 294 28 MARCH 1987 815 Clinical Aalgorithms Primary and secondary amenorrhoea S FRANKS Amenorrhoea, which is usually defined as no periods for six months or more, occurs in
BRITISH MEDICAL JOURNAL VOLUME 294 28 MARCH 1987 815 Clinical Aalgorithms Primary and secondary amenorrhoea S FRANKS Amenorrhoea, which is usually defined as no periods for six months or more, occurs in
06-Mar-17. Premature menopause. Menopause. Premature menopause. Menstrual cycle oestradiol. Premature menopause. Prevalence ~1% Higher incidence:
 Menopause Dr Sonia Davison MBBS FRACP PhD Endocrinologist and Clinical Fellow, Jean Hailes for Women s Health Women s Health Research Program, Monash University = the last natural menstrual period depletion
Menopause Dr Sonia Davison MBBS FRACP PhD Endocrinologist and Clinical Fellow, Jean Hailes for Women s Health Women s Health Research Program, Monash University = the last natural menstrual period depletion
By Dr Rukhsana Hussain 5 th April 2016
 By Dr Rukhsana Hussain 5 th April 2016 1. Is it indicated? Vasomotor symptoms (flushes/sweats) Vaginal atrophy Cycle control (In perimenopause consider low dose COCP (age
By Dr Rukhsana Hussain 5 th April 2016 1. Is it indicated? Vasomotor symptoms (flushes/sweats) Vaginal atrophy Cycle control (In perimenopause consider low dose COCP (age
F REQUENTLY A SKED Q UESTIONS
 Polycystic heart, blood vessels, and appearance. Women with PCOS have these characteristics: Ovarian high levels of male hormones, also called androgens an irregular or no menstrual cycle Syndrome may
Polycystic heart, blood vessels, and appearance. Women with PCOS have these characteristics: Ovarian high levels of male hormones, also called androgens an irregular or no menstrual cycle Syndrome may
Menopause management NICE Implementation
 Menopause management NICE Implementation Dr Paula Briggs Consultant in Sexual & Reproductive Health Southport and Ormskirk NHS Hospital Trust Why a NICE guideline (NG 23) Media reports about HRT have not
Menopause management NICE Implementation Dr Paula Briggs Consultant in Sexual & Reproductive Health Southport and Ormskirk NHS Hospital Trust Why a NICE guideline (NG 23) Media reports about HRT have not
POLYCYSTIC OVARIAN SYNDROME Laura Tatpati, MD Reproductive Endocrinology and Infertility. Based on: ACOG No. 108 Oct 2009; reaffirmed 2015
 POLYCYSTIC OVARIAN SYNDROME Laura Tatpati, MD Reproductive Endocrinology and Infertility Based on: ACOG No. 108 Oct 2009; reaffirmed 2015 NO DISCLOSURES PATIENT 26 years old presents with complaint of
POLYCYSTIC OVARIAN SYNDROME Laura Tatpati, MD Reproductive Endocrinology and Infertility Based on: ACOG No. 108 Oct 2009; reaffirmed 2015 NO DISCLOSURES PATIENT 26 years old presents with complaint of
GONADAL FUNCTION: An Overview
 GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE
 Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Menopause & HRT. Matt McKenna Elliot Davis
 Menopause & HRT Matt McKenna Elliot Davis Menopause Before age 40: Premature Menopause After 12 months clinical diagnosis made Depletion of Ovarian Follicles Oestrogen Progesterone LH FSH Spontaneous Amemorrhoea
Menopause & HRT Matt McKenna Elliot Davis Menopause Before age 40: Premature Menopause After 12 months clinical diagnosis made Depletion of Ovarian Follicles Oestrogen Progesterone LH FSH Spontaneous Amemorrhoea
Reproductive Health and Pituitary Disease
 Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
Prescribing advice for the management of menopause in primary care
 Prescribing advice for the management of menopause in primary care This guidance contains suggested advice for the management and treatment of women experiencing symptoms of menopause. It applies to Camden
Prescribing advice for the management of menopause in primary care This guidance contains suggested advice for the management and treatment of women experiencing symptoms of menopause. It applies to Camden
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
S. AMH in PCOS Research Insights beyond a Diagnostic Marker
 S. AMH in PCOS Research Insights beyond a Diagnostic Marker Dr. Anushree D. Patil, MD. DGO Scientist - D National Institute for Research in Reproductive Health (Indian Council of Medical Research) (Dr.
S. AMH in PCOS Research Insights beyond a Diagnostic Marker Dr. Anushree D. Patil, MD. DGO Scientist - D National Institute for Research in Reproductive Health (Indian Council of Medical Research) (Dr.
Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia
 Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome An Individualized Approach Alice Y. Chang, MD, MSc Assistant Professor Mayo Clinic Division of Endocrinology, Diabetes, Nutrition and Metabolism Learning Objectives: To Individualize
Polycystic Ovary Syndrome An Individualized Approach Alice Y. Chang, MD, MSc Assistant Professor Mayo Clinic Division of Endocrinology, Diabetes, Nutrition and Metabolism Learning Objectives: To Individualize
GUIDELINES ON. Introduction. G.R. Dohle, S. Arver, C. Bettocchi, S. Kliesch, M. Punab, W. de Ronde
 GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
Prescribing Framework for Testosterone in Adults
 Prescribing Framework for Testosterone in Adults Patient s Name:.. NHS Number: Patient s Address:... (Use addressograph sticker) GP s Name:... Communication We agree to treat this patient within this Prescribing
Prescribing Framework for Testosterone in Adults Patient s Name:.. NHS Number: Patient s Address:... (Use addressograph sticker) GP s Name:... Communication We agree to treat this patient within this Prescribing
PCOS guidelines: What s relevant to general practice
 PCOS guidelines: What s relevant to general Dr David Molloy Medical Director, Queensland Fertility Group International evidence based PCOS guidelines 1st ever internationally endorsed & evidence based
PCOS guidelines: What s relevant to general Dr David Molloy Medical Director, Queensland Fertility Group International evidence based PCOS guidelines 1st ever internationally endorsed & evidence based
Sexual dysfunction of chronic kidney disease. Razieh salehian.md psychiatrist
 Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Primary Care Gynaecology Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
 Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
HCG (human chorionic gonadotropin); Novarel Pregnyl (chorionic gonadotropin); Ovidrel (choriogonadotropin alfa)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.09 Subject: HCG Page: 1 of 5 Last Review Date: June 19, 2015 HCG Powder, Novarel, Pregnyl, Ovidrel
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.09 Subject: HCG Page: 1 of 5 Last Review Date: June 19, 2015 HCG Powder, Novarel, Pregnyl, Ovidrel
Orals,Transdermals, and Other Estrogens in the Perimenopause
 Orals,Transdermals, and Other Estrogens in the Perimenopause Cases Denise Black, MD, FRCSC Assistant Professor, Obstetrics, Gynecology and Reproductive Sciences University of Manitoba 6/4/18 197 Faculty/Presenter
Orals,Transdermals, and Other Estrogens in the Perimenopause Cases Denise Black, MD, FRCSC Assistant Professor, Obstetrics, Gynecology and Reproductive Sciences University of Manitoba 6/4/18 197 Faculty/Presenter
GUIDELINES ON MALE HYPOGONADISM
 GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
IVF Patient Information
 What is IVF? IVF (In Vitro Fertilisation) is a treatment by which fertilisation of eggs by sperm takes place outside the body in a dish in an IVF laboratory. An ovary has a pool of immature eggs. In a
What is IVF? IVF (In Vitro Fertilisation) is a treatment by which fertilisation of eggs by sperm takes place outside the body in a dish in an IVF laboratory. An ovary has a pool of immature eggs. In a
Approach to ovulation induction and superovulation in women with a history of infertility. Anatte E. Karmon, MD
 Approach to ovulation induction and superovulation in women with a history of infertility Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the
Approach to ovulation induction and superovulation in women with a history of infertility Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the
Nitasha Garg 1 Harkiran Kaur Khaira. About the Author
 https://doi.org/10.1007/s13224-017-1082-4 ORIGINAL ARTICLE A Comparative Study on Quantitative Assessment of Blood Flow and Vascularization in Polycystic Ovary Syndrome Patients and Normal Women Using
https://doi.org/10.1007/s13224-017-1082-4 ORIGINAL ARTICLE A Comparative Study on Quantitative Assessment of Blood Flow and Vascularization in Polycystic Ovary Syndrome Patients and Normal Women Using
Infertility DR. RAHUL BEVARA
 Infertility DR. RAHUL BEVARA Definitions Infertility is defined as the inability to conceive after one year of unprotected coitus. Affects 10-15% of couples Primary Infertility, that is inability to conceive
Infertility DR. RAHUL BEVARA Definitions Infertility is defined as the inability to conceive after one year of unprotected coitus. Affects 10-15% of couples Primary Infertility, that is inability to conceive
Infertility Investigations. Patient Information
 Infertility Investigations Patient Information Author ID: PH Leaflet Number: Gyn 048 Version: 4 Name of Leaflet: Infertility Investigations Date Produced: March 2017 Review Date: March 2019 Please be aware
Infertility Investigations Patient Information Author ID: PH Leaflet Number: Gyn 048 Version: 4 Name of Leaflet: Infertility Investigations Date Produced: March 2017 Review Date: March 2019 Please be aware
Polycystic Ovary Syndrome diagnosis & management
 Polycystic Ovary Syndrome diagnosis & management Dr Roisin Worsley, FRACP Endocrinologist, Jean Hailes at Epworth https://jeanhailes.org.au/contents/docume nts/resources/tools PCOS is a chronic condition
Polycystic Ovary Syndrome diagnosis & management Dr Roisin Worsley, FRACP Endocrinologist, Jean Hailes at Epworth https://jeanhailes.org.au/contents/docume nts/resources/tools PCOS is a chronic condition
Laboratoires Genevirer Menotrophin IU 1.8.2
 Important missing information VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Infertility is when a woman cannot get pregnant (conceive) despite having regular unprotected sexual
Important missing information VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Infertility is when a woman cannot get pregnant (conceive) despite having regular unprotected sexual
INFERTILITY CAUSES. Basic evaluation of the female
 INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
Gonadotrophin treatment in patients with Polycystic Ovary Syndrome
 Int. J. Adv. Res. Biol. Sci. (218). 5(4): 95-99 International Journal of Advanced Research in Biological Sciences ISSN: 2348-869 www.ijarbs.com DOI: 1.22192/ijarbs Coden: IJARQG(USA) Volume 5, Issue 4-218
Int. J. Adv. Res. Biol. Sci. (218). 5(4): 95-99 International Journal of Advanced Research in Biological Sciences ISSN: 2348-869 www.ijarbs.com DOI: 1.22192/ijarbs Coden: IJARQG(USA) Volume 5, Issue 4-218
Hirsutism: Diagnosis and Treatment. Roger A. Lobo M.D. Columbia University
 Hirsutism: Diagnosis and Treatment Roger A. Lobo M.D. Columbia University Signs of hyperandrogenism Acne, Hirsutism, Alopecia All explained by increased androgen production and/or increased sensitivity
Hirsutism: Diagnosis and Treatment Roger A. Lobo M.D. Columbia University Signs of hyperandrogenism Acne, Hirsutism, Alopecia All explained by increased androgen production and/or increased sensitivity
Metformin and Pioglitazone in Polycystic Ovarian Syndrome: A Comparative Study
 The Journal of Obstetrics and Gynecology of India (September-October 2012) 62(5):551 556 DOI 10.1007/s13224-012-0183-3 ORIGINAL ARTICLE Metformin and Pioglitazone in Polycystic Ovarian Syndrome: A Comparative
The Journal of Obstetrics and Gynecology of India (September-October 2012) 62(5):551 556 DOI 10.1007/s13224-012-0183-3 ORIGINAL ARTICLE Metformin and Pioglitazone in Polycystic Ovarian Syndrome: A Comparative
Infertility: A Generalist s Perspective
 Infertility: A Generalist s Perspective Learning Objectives Fertility and Lifestyle: Patient education Describe the basic infertility workup Basic treatment strategies unexplained Heather Huddleston, MD
Infertility: A Generalist s Perspective Learning Objectives Fertility and Lifestyle: Patient education Describe the basic infertility workup Basic treatment strategies unexplained Heather Huddleston, MD
The 6 th Scientific Meeting of the Asia Pacific Menopause Federation
 Predicting the menopause The menopause marks the end of ovarian follicular activity and is said to have occurred after 12 months amenorrhoea. The average age of the menopause is between 45 and 60 years
Predicting the menopause The menopause marks the end of ovarian follicular activity and is said to have occurred after 12 months amenorrhoea. The average age of the menopause is between 45 and 60 years
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
SAMPLE REPORT. Order Number: PATIENT. Age: 40 Sex: F MRN:
 Patient: Age: 40 Sex: F MRN: SAMPLE PATIENT Order Number: Completed: Received: Collected: SAMPLE REPORT Progesterone ng/ml 0.34 0.95 21.00 DHEA-S mcg/dl Testosterone ng/ml 48 35 0.10 0.54 0.80 430 Sex
Patient: Age: 40 Sex: F MRN: SAMPLE PATIENT Order Number: Completed: Received: Collected: SAMPLE REPORT Progesterone ng/ml 0.34 0.95 21.00 DHEA-S mcg/dl Testosterone ng/ml 48 35 0.10 0.54 0.80 430 Sex
Learning Objectives. Peri menopause. Menopause Overview. Recommendation grading categories
 Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
