Prior Authorization Review Panel MCO Policy Submission
|
|
|
- Chastity O’Connor’
- 5 years ago
- Views:
Transcription
1 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review. Plan: Aetna Better Health Submission Date: 08/01/2018 Policy Number: 0413 Policy Name: Varicocele: Selected Treatments Effective Date: Revision Date: 04/26/2018 Type of Submission Check all that apply: New Policy Revised Policy* Annual Review No Revisions *All revisions to the policy must be highlighted using track changes throughout the document. Please provide any clarifying information for the policy below: CPB 413 Varicocele: Selected Treatments This CPB has been revised to state that the following are considered experimental and investigational: (i) addition of a sclerosant agent to coil embolization to improve outcomes, and (ii) endovenous laser ablation (EVLA) of the spermatic vein for the treatment of varicocele. Name of Authorized Individual (Please type or print): Signature of Authorized Individual: Dr. Bernard Lewin, M.D. Revised 04/26/2018
2 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 1 of 31 ( Varicocele: Selected Treatments Number: 0413 Policy Aetna considers percutaneous embolization (by means of balloon or metallic coil) or ligation medically necessary for the treatment of varicocele for any of the following conditions: 1. Adolescents with grade 2 or 3 varicoceles associated with ipsilateral testicular growth retardation; or 2. Males with infertility problems who have decreased sperm motility and lower sperm concentrations; or 3. Post-surgical (ligation) recurrence of varicoceles; or 4. Scrotal pain associated with varicoceles. Aetna considers surgical treatment (ligation, embolization) for subclinical varicocele experimental and investigational because of insufficient evidence to support its effectiveness. Policy History Last Review 04/26/2018 Effective: 05/04/2000 Next Review: 04/25/2019 Review History Definitions Additional Information Clinical Policy Bulletin Notes
3 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 2 of 31 Aetna considers percutaneous embolization or ligation of varicoceles for persons who do not meet these criteria experimental and investigational. Aetna considers microsurgical varicocelectomy an acceptable alternative method of treating a varicocele when any of the afore-mentioned criteria is met. Aetna considers the following interventions experimental and investigational because their effectiveness has not been established: Addition of a sclerosant agent to coil embolization to improve outcomes Endoluminal occlusion devices (e.g., the ArtVentive endoluminal occlusion system) Endovenous laser ablation (EVLA) of the spermatic vein for the treatment of varicocele Background Varicoceles (dilations of the pampiniform venous plexus) are found in 10 to 15 % of the male population and they occur predominantly on the left side. The etiology may be a longer left spermatic vein with its right-angle insertion into the left renal vein and/or absence of valves, which results in a higher hydrostatic pressure in the left spermatic vein causing dilatation. Also, the left renal vein may be compressed between the superior mesenteric artery and the aorta.
4 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 3 of 31 This nutcracker phenomenon may result in elevated pressure in the left testicular venous system. Moreover, the incidence of varicocele in men with impaired fertility is about 30 %; varicoceles are the most common surgically correctable cause of male infertility. A clinical grading system classifies varicoceles into 3 grades: (i) grade 1 (small) -- palpable only during a Valsalva maneuver, (ii) grade 2 (moderate) - palpable without the need of the Valsalva maneuver, and (iii) grade 3 (large) -- visible. Although varicoceles can be diagnosed by a thorough physical examination, ultrasonography is the most practical and accurate non-invasive method in diagnosing this condition. Surgical ligation (varicocelectomy) is the conventional approach in managing varicoceles. However, percutaneous embolization by means of balloon or metallic coil has been shown to be a safe and effective alternative to ligation in treating varicoceles. Embolization (of spermatic veins) of varicoceles in males with semen abnormalities has been demonstrated to improve sperm count and motility in up to 75 % of patients, and reported pregnancy rates after ablation of varicoceles vary from 30 to 60 %. Furthermore, embolization therapy has been reported to increase testicular size in adolescents with testicular hypotrophy. Polito and colleagues (2004) stated that the impact of varicocele on male infertility is still controversial since its role on the impairment of semen quality has never been fully demonstrated. These researchers studied a series of young adult males (n = 426) undergoing percutaneous treatment of varicocele and semen
5 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 4 of 31 parameters were evaluated at baseline and 12 months of follow-up. They concluded that the correction of varicocele in young adults is not a major indication when semen alteration is the only clinical problem. This is in agreement with the findings of Nabi et al (2004) who compared the semen quality in men with or without pregnancy after percutaneous embolization of varicoceles in the management of infertility (n = 102). They concluded that varicocele embolization is a technically feasible, minimally invasive, outpatient procedure that improves semen quality significantly in patients with a preembolization semen density of 10 to 30 million/ml. However, no correlation was found between the improvements in semen quality and the pregnancy rate. Bechara et al (2009) compared the treatment outcome of percutaneous embolization treatment versus laparoscopic varicocelectomy in patients with symptomatic varicoceles. Patients with varicoceles undergoing either laparoscopic varicocelectomy or percutaneous coil embolization of the testicular vein during a recent 5-year period were analyzed. Treatment outcome and hospital costs of these two minimally invasive treatment modalities were compared. A total of 41 patients underwent percutaneous coil embolization of the testicular vein, which were compared with a cohort of 43 patients who underwent laparoscopic varicocelectomy. Technical success in interventional and laparoscopic treatment was 95 % and 100 %, respectively. The mean operative time or procedural time was 63 +/- 13 mins and 52 +/- 25 mins for interventional and laparoscopic cohorts (not significant),
6 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 5 of 31 respectively. Embolization treatment resulted in 2 recurrent varicoceles (4.8 %) compared to 1 patient following laparoscopic repair (2.3 %, not significant). Embolization treatment was associated with a lower complication rate than laparoscopic repair (9.7 % versus 16.3 %, p = 0.03). Regarding cost analysis, no significant difference in hospital cost was noted between the interventional or laparoscopic treatment strategies. Both laparoscopic varicocelectomy and coil embolization are effective treatment modalities for varicoceles. With lower treatment complication rates in the interventional treatment group, coil embolization of the testicular vein offers treatment advantage compared with laparoscopic repair in patients with varicoceles. Ayechu-Diaz et al (2009) stated that there are still doubts as to the most suitable criteria when considering surgery as the indication and optimal treatment for adolescent varicocele. These investigators reviewed the hospital and primary health care histories of patients diagnosed by ultrasound for varicocele over the last 7 years. Data were taken from computerized clinical histories and hard copy back-up material stored and processed in computer format. They studied 135 cases (mean age of 12.8 years). A total of 125 were referred for scrotal swelling or as a result of chance detection, except for 10 patients who reported pain or scrotal asymmetry; 73 underwent surgery and 62 continued as controls over the study period. The surgical indication was significant progressive asymmetry in testicular volume (n = 28), high grade varicocele (n = 41) as well as other reasons (n = 4). These researchers undertook percutaneous
7 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 6 of 31 embolization in 44 patients (with a 66 % relapse rate) and laparoscopic section of the spermatic cord with no arterial preservation in 29 (no relapses but 7 post-surgery hydroceles). No testicles were lost. At the end of the study 10 children continued as controls, 34 were discharged after recovery, 56 were referred to urology due to their age group, and 35 were lost to the study. The authors concluded that in the controversy over the treatment of varicocele, their experience showed a high degree of relapses after embolization. Section of the spermatic vessels (including the artery) with no lymphatic preservation is highly effective but involves 27 % post-surgical hydroceles, usually self-limiting (only 1 patient had to undergo surgery later), with no testicular atrophy or other complications. These investigators prefer complete laparoscopic section of the spermatic pedicle to embolization; but it would be advisable to introduce modifications to avoid post-surgical hydrocele. Embolization must be reserved for patients with 1 testicle or with bilateral disease. Storm and colleagues (2010) noted that postoperative hydrocele development is a frustrating complication of varicocele surgical repair. To avoid this complication, these investigators began to offer percutaneous embolization as a treatment option. They presented their initial experience with this technique. There were 27 patients with a mean age of 16 years (range of 13 to 19 years). Indications included pain (48 %), varicocele size (30 %) and persistent testicular asymmetry (22 %). Four patients had experienced failure of a previous surgical repair. Follow-up data were available for 21 patients (mean of 9 months). The varicocele resolved in
8 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 7 of patients (91 %) with no evidence of hydrocele formation in any of the boys. There was resolution of pain in all patients for whom this was the indication for the procedure. In the 2 failures, access to the lower spermatic vein was not possible owing to the number and tortuosity of the vessels. The authors concluded that percutaneous embolization and sclerotherapy represent a truly minimally invasive treatment with low morbidity, minimal pain and rapid recovery. In the authors' experience, since lymphatic channels are completely avoided, there appears to be no risk of hydrocele formation. Microsurgical Varicocelectomy: Kondoh et al (2010) stated that surgical ligation for varicocele is primarily used in the management of male infertility patients. However, effectiveness of the ligation for painful varicocele is still controversial. These investigators reviewed records from 18 patients (average age of 17.8 years) who underwent varicocele ligation done for pain at the authors' institution from June 1999 to May The varicocele was on the left side and was grade III in 15 cases and grade II in 3 cases. The pain was classified into 3 types: (i) discomfort, (ii) dull pain, and (iii) sharp pain. Microsurgical varicocelectomy was done with inguinal or subinguinal approach. Evaluation of postoperative pain was available in 17 patients, and 15 patients (88 %) reported complete resolution of the pain with averaged follow-up duration of 11 months (3 to 53 months). The authors concluded that microsurgical varicocelectomy using the inguinal or subinguinal
9 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 8 of 31 approach was an effective treatment modality for varicocele-associated pain. Seo et al (2010) evaluated the improvement of seminal characteristics and pregnancy rates after microsurgical varicocelectomy in men with subclinical varicocele. A total of 143 patients with a subclinical left-sided varicocele were included in this study. Patients who agreed to microsurgical varicocelectomy (n = 25, surgery group), medical treatment with L-carnitine (n = 93 drug group), and those who did not agree to any treatment (n = 25, observation group) were enrolled. Semen characteristics were re-evaluated twice 6 months after treatment. The natural pregnancy rates were estimated by telephone interview between 1 and 2 years after treatment. In the surgery group, sperm counts improved significantly after microsurgical varicocelectomy. In the drug group, however, sperm parameters did not significantly improve after treatment. Natural pregnancy rates were 60.0 % in the surgery group, 34.5 % in the drug group, and 18.7 % in the observation group. The natural pregnancy rate of the surgery group was higher than the other groups, and there were statistically significant differences among the 3 groups. The authors concluded that surgical treatment is the best option for management of subclinical varicocele. In a prospective, non-masked, parallel-group randomized, controlled trial, Abdel-Meguid and colleagues (2011) examined if varicocele treatment is superior or inferior to no treatment in male infertility from an evidence-based perspective. Married men 20 to 39 years of age who had experienced infertility greater than or
10 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 9 of 31 equal to 1 year, had palpable varicoceles, and with at least 1 impaired semen parameter (e.g., sperm concentration less than 20 million/ml, progressive motility less than 50 %, or normal morphology less than 30 %) were eligible. Exclusions included subclinical or recurrent varicoceles, normal semen parameters, and azoospermia. Sample size analysis suggested 68 participants per arm. Participants were randomly allocated to observation (the control arm [CA]) or subinguinal microsurgical varicocelectomy (the treatment arm [TA]). Semen analyses were obtained at baseline (3 analyses) and at follow-up months 3, 6, 9, and 12. The mean of each sperm parameter at baseline and follow-ups was determined. These researchers measured the spontaneous pregnancy rate (the primary outcome), changes from baseline in mean semen parameters, and the occurrence of adverse events (AE-the secondary outcomes) during 12-month follow-up; p < 0.05 was considered significant. Analysis included 145 participants (CA: n = 72; TA: n = 73), with a mean age plus or minus standard deviation of /- 5.7 in the CA and /- 5.7 in the TA (p = 0.34). Baseline characteristics in both arms were comparable. Spontaneous pregnancy was achieved in 13.9 % (CA) versus 32.9 % (TA), with an odds ratio of 3.04 (95 % confidence interval [CI]: 1.33 to 6.95) and a number needed to treat of 5.27 patients (95 % CI: 1.55 to 8.99). In CA within-arm analysis, none of semen parameters revealed significant changes from baseline (sperm concentration [p = 0.18], progressive motility [p = 0.29], and normal morphology [p = 0.05]). Conversely, in TA withinarm analysis, the mean of all semen parameters improved significantly in follow-up versus
11 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 10 of 31 baseline (p < ). In between-arm analysis, all semen parameters improved significantly in the TA versus CA (p < ). No AEs were reported. The authors concluded that these findings provided level 1b evidence of the superiority of varicocelectomy over observation in infertile men with palpable varicoceles and impaired semen quality, with increased odds of spontaneous pregnancy and improvements in semen characteristics within 1-year of follow-up. Diegidio and colleagues (2010) reviewed all the various techniques and their results and efficiencies to provide practicing urologists with some guidance for choice of technique. These investigators discussed improvements of varicocelectomy techniques in the last 15 years and their impact on results of surgery. Pregnancy rates were highest with microsurgical subinguinal technique. Varicocele recurrence rates were lowest with microsurgical subinguinal technique. Hydrocele formation rates were lowest with microsurgical inguinal technique. Surgical complications were highest in the laparoscopic technique. Varicocelectomy by itself or in conjunction with in-vitro fertilization is costeffective. The authors concluded that microsurgical subinguinal or microsurgical inguinal techniques offer best outcomes; and varicocelectomy is a cost- effective treatment modality for infertility. The European Association of Urology (EAU)'s guidelines on pediatric urology (Tekgul et al, 2009) stated that for the treatment of varicocele in children and adolescents, surgical intervention is based on ligation or occlusion of the internal spermatic veins. Ligation is
12 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 11 of 31 performed at different levels: (i) inguinal (or subinguinal) microsurgical ligation, and (ii) suprainguinal ligation, using open or laparoscopic techniques. The advantage of the former is the lower invasiveness of the procedure, while the advantage of the latter is a considerably lower number of veins to be ligated and safety of the incidental division of the internal spermatic artery at the suprainguinal level. Moreover, lymphatic-sparing varicocelectomy is preferred to prevent hydrocele formation and testicular hypertrophy development and to achieve a better testicular function according to the luteinizing hormonereleasing hormone stimulation test. The methods of choice are subinguinal or inguinal microsurgical (microscopic) repairs, or suprainguinal open or laparoscopic lymphaticsparing repairs. Furthermore, the EAU's guidelines on male infertility (Dohle et al, 2010) stated that several treatments are available for varicocele, and that the type of intervention chosen depends mainly on the therapist s experience. Morevoer, an accompanying table in the EAU guideline reported a lower recurrence rate (0.8 % to 4.0 %) with microsurgical varicocelectomy than with alternative approaches (3.0 % to 29.0 %). In a randomized study, Pourmand et al (2014) examined if addition of L-carnitine therapy to standard varicocelectomy adds any extra benefit in terms of improvement in semen parameters or deoxyribonucleic acid (DNA) damage. A total of 100 patients enrolled in this study and were randomly divided into 2 groups (50 patients in each group). In group 1, standard inguinal
13 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 12 of 31 varicocelectomy and, in group 2, standard inguinal varicocelectomy plus oral anti-oxidant therapy (oral L-carnitine, 250 mg 3 times a day) were performed for 6 months. For all patients, routine semen analysis and DNA damage test of spermatozoa (by 2 methods of terminal deoxynucleotidyl transferase dutp nick end labeling and protamine damage assay) were performed at baseline and at 3 and 6 months post-operatively. In both groups, the improvement in semen analysis parameters and DNA damage was observed, but there was not any statistically significant difference between the 2 groups in these parameters, although the slope of improvement in DNA damage was slightly better in group 2 (that was not statistically significant). The authors concluded that addition of 750 mg of L-carnitine orally daily to standard inguinal varicocelectomy does not add any extra benefit in terms of improvement in semen analysis parameters or DNA damage. In a Cochrane review, Showell and colleagues (2014) evaluated the safety and effectiveness of oral supplementation with anti-oxidants for subfertile male partners in couples seeking fertility assistance. These investigators searched the Cochrane Menstrual Disorders and Subfertility Group Specialised Register, CENTRAL, MEDLINE, EMBASE, CINAHL, PsycINFO and AMED databases (from inception until January 2014); trial registers; sources of unpublished literature and reference lists. An updated search was run in August 2014 when potentially eligible studies were placed in 'studies awaiting assessment'. These researchers included randomized controlled trials (RCTs) comparing any type or dose of anti-oxidant supplement (single or
14 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 13 of 31 combined) taken by the subfertile male partner of a couple seeking fertility assistance with a placebo, no treatment or another antioxidant. Two review-authors independently selected eligible studies, extracted the data and assessed the risk of bias of the included studies. The primary review outcome was live birth; secondary outcomes included clinical pregnancy rates, adverse events, sperm DNA fragmentation, sperm motility and concentration. Data were combined, where appropriate, to calculate pooled odds ratios (ORs) or mean differences (MD) and 95 % CIs. Statistical heterogeneity was assessed using the I(2) statistic. The authors assessed the overall quality of the evidence for the main outcomes using GRADE methods. This updated review included 48 RCTs that compared single and combined antioxidants with placebo, no treatment or another anti-oxidant in a population of 4,179 subfertile men. The duration of the trials ranged from 3 to 26 weeks with follow-up ranging from 3 weeks to 2 years. The men were aged from 20 to 52 years. Most of the men enrolled in these trials had low total sperm motility and sperm concentration. One study enrolled men after varicocelectomy, 1 enrolled men with a varicocoele, and 1 recruited men with chronic prostatitis. Three trials enrolled men who, as a couple, were undergoing in-vitro fertilization (IVF) or intra-cytoplasmic sperm injection (ICSI) and 1 trial enrolled men who were part of a couple undergoing intra-uterine insemination (IUI). Funding sources were stated by 15 trials; 4 of these trials stated that funding was from a commercial source and the remaining 11 obtained funding through non-commercial avenues or university grants; 33 trials did not report any funding sources. A limitation of this
15 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 14 of 31 review was that in a sense these researchers had included 2 different groups of trials, those that reported on the use of anti-oxidants and the effect on live birth and clinical pregnancy, and a second group that reported on sperm parameters as their primary outcome and had no intention of reporting the primary outcomes of this review. These investigators included 25 trials reporting on sperm parameters and only 3 of these reported on live birth or clinical pregnancy. Other limitations included poor reporting of study methods, imprecision, the small number of trials providing usable data, the small sample size of many of the included studies and the lack of adverse events reporting. The evidence was graded as 'very low' to 'low'. The data were current to January 31, Live birth: antioxidants may have increased live birth rates (OR 4.21, 95 % CI: 2.08 to 8.51, p < , 4 RCTs, 277 men, I(2) = 0 %, low quality evidence). This suggested that if the chance of a live birth following placebo or no treatment is assumed to be 5 %, the chance following the use of antioxidants is estimated to be between 10 % and 31 %. However, this result was based on only 44 live births from a total of 277 couples in 4 small studies. Clinical pregnancy rate: anti-oxidants may have increased clinical pregnancy rates (OR 3.43, 95 % CI: 1.92 to 6.11, p < , 7 RCTs, 522 men, I(2) = 0 %, low quality evidence). This suggested that if the chance of clinical pregnancy following placebo or no treatment is assumed to be 6 %, the chance following the use of antioxidants is estimated at between 11 % and 28 %. However, there were only 7 small studies in this analysis and the quality of the evidence was rated as low. Miscarriage: only 3 trials reported on this outcome and the event rate was very low.
16 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 15 of 31 There was insufficient evidence to show whether there was a difference in miscarriage rates between the anti-oxidant and placebo or no treatment groups (OR 1.74, 95 % CI: 0.40 to 7.60, p = 0.46, 3 RCTs, 247 men, I(2) = 0 %, very low quality evidence). The findings suggested that in a population of subfertile men with an expected miscarriage rate of 2 %, use of an anti-oxidant would result in the risk of a miscarriage lying between 1 % and 13 %. Gastro-intestinal upsets: there was insufficient evidence to show whether there was a difference in gastro-intestinal upsets when anti-oxidants were compared to placebo or no treatment as the event rate was very low (OR 1.60, 95 % CI: 0.47 to 5.50, p = 0.46, 6 RCTs, 429 men, I(2) = 0 %). These researchers were unable to draw any conclusions from the anti-oxidant versus anti-oxidant comparison as not enough trials compared the same interventions. The authors concluded that there is low quality evidence from only 4 small RCTs suggesting that anti-oxidant supplementation in subfertile males may improve live birth rates for couples attending fertility clinics. Low quality evidence suggested that clinical pregnancy rates may increase. There is no evidence of increased risk of miscarriage but this is uncertain as the evidence is of very low quality. Data were lacking on other adverse effects. They stated that further large well-designed RCTs are needed to clarify these results. Endoluminal Occlusion Device: Venbrux et al (2014) determined the safety and effectiveness of a new endoluminal occlusion device, ArtVentive endoluminal occlusion system (EOS), to occlude the spermatic vein in
17 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 16 of 31 symptomatic males with varicoceles. The ArtVentive EOS device has been developed for percutaneous, peripheral occlusion of the peripheral arterial and venous vasculature. The system is comprised of an implantable occlusion device and a delivery catheter. At present, there are 2 device sizes: (i) size 1 for target vessels ranging between 3.5 and 5.5 mm in diameter, and (ii) size 2 for target vessels 5.5 to 8.5 mm in diameter. The treatment group included 6 adult males, aged 22 to 34 years; 9 target vessels were occluded and a total of 20 devices were implanted in 6 subjects. The acute occlusion rate at the end of the procedure was 100 % occurring in 9 of 9 vessels. The spermatic veins of all patients remained occluded on venography at 30 days follow-up. Pain scores related to varicoceles decreased in 5 of 6 patients. The authors concluded that although they recognized this study was limited, initial experience indicated that the ArtVentive EOS is a safe and effective new device for occlusion of vessels (varicoceles). They stated that the device has potential applications in other clinical conditions requiring occlusion of veins or arteries. Surgical Treatment for Subclinical Varicocele: In a systematic review and meta-analysis, Kim and colleagues (2015) noted that recent metaanalysis by the Cochrane collaboration concluded that treatment of varicocele may improve an infertile couple's chance of pregnancy. However, there has been no consensus on the management of subclinical varicocele. These researchers determined the impact of varicocele treatment on semen parameters and pregnancy rate in men with subclinical varicocele. The RCTs
18 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 17 of 31 that evaluated the presence and/or treatment of subclinical varicocele were included for systematic review and meta-analysis. Random effect model was used to calculate the weighted MD of semen parameters and ORs of pregnancy rates. A total of 7 trials with 548 participants, 276 in subclinical varicocelectomy and 272 in notreatment or clomiphene citrate subjects, were included. Although there was also no statistically significant difference in pregnancy rate (OR 1.29, 95 % CI: 0.99 to 1.67), surgical treatment resulted in statistically significant improvements on forward progressive sperm motility (MD 3.94, 95 % CI: 1.24 to 6.65). The authors concluded that there is insufficient evidence to allow final conclusions because the quality of included studies was very low and further research is needed. Furthermore, an UpToDate review on Evaluation of nonacute scrotal pathology in adult men (Eyre, 2016) states that Subclinical varicoceles are often discovered as part of an infertility evaluation by demonstrating retrograde flow to the scrotum by Color Doppler ultrasonography. The role of surgical ligation for subclinical varicoceles associated with subfertility is not clear. Addition of Sclerosants to Coil Embolization: In a retrospective study, Favard and associates (2015) evaluated pain, radiation and recurrence rates in patients undergoing varicocele embolization with 3 different embolic materials. This trial included a total of 182 consecutive patients who underwent transcatheter retrograde varicocele embolization from July
19 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 18 of to May 2015 with glue (Glubran2) (group 1, n = 63), mechanical agents (coils and/or plugs) (group 2, n = 53) or a sclerosing agent (polidocanol) (group 3, n = 66). Patients were asked by telephone interview to evaluate pain during embolization and at 1, 7 and 30 days using a quantitative pain scale ranging from 0 to 10. Duration of scopy, kinetic energy released per unit mass (kerma) and dose area product (DAP) were assessed as radiation parameters during embolization procedures. Recurrence rates after treatment were also evaluated. Statistical analyses were performed using parametric and non-parametric tests. Patients in the 3 study groups were comparable for age, clinical indication and embolization side. No difference was noted for significant pain (pain score greater than or equal to 3) during embolization and at 1, 7 and 30 days after treatment. Discomfort (pain score less than 3) was more frequent in group 1 than in groups 2 and 3 at 7 days after the procedure (p = 0.049). No difference in discomfort was noted during embolization or at 1 and 30 days. Duration of scopy was shorter (p < ) and kerma was lower (p = ) in group 1 than in groups 2 and 3. DAP was lower in group 1 than in group 2 (p = 0.04) but no difference was noted between groups 1 and 3, and groups 2 and 3. The recurrence rate at a mean follow-up of 24.4 months (range of 2 to 53 months) was significantly lower in group 1 than in the 2 other groups (p = 0.032). The authors concluded that the use of Glubran2 acrylic glue as an embolic agent for percutaneous embolization of varicocele was a therapeutic alternative that is effective, safe, inexpensive, and easily feasible in an out-patient setting, and had a high technical success rate. Glubran2 triggered a
20 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 19 of 31 local inflammatory reaction that promoted sclerosis and thrombosis, but without causing more significant pain than was the case with other embolic agents. The liquid nature of the embolization product allowed diffusion through the gonadal vein and its collaterals, which appeared to reduce recurrence rates and improve results. Lastly, the use of glue allowed fast procedures, leading to less radiation than treatment with mechanical or sclerosing agents. The authors stated that this study had several limitations. First, this was a retrospective review of a cohort from a single center, with some patients lost to follow-up. Second, one goal of the study was to evaluate tolerance to embolization of the spermatic vein with different embolic materials during the procedure and at 1, 7 and 30 days. Almost 50 % of the patients in each group had symptomatic varicocele. After embolization, it usually took a few weeks for the pain to disappear completely. Consequently, it was difficult to know whether pain reported at 30 days in some patients was related to the procedure or just due to normal recovery in symptomatic patients treated with embolization. Third, the results of this study must be interpreted with caution. Indeed, although these researchers attempted to compare gluing, mechanical and sclerosing agents with each other for varicocele embolization, polidocanol was not used alone in the sclerotherapy group but in combination with coils. This could have led to longer procedure times and higher radiation during the procedure in comparison with sclerotherapy alone. Fourth, the fact that recurrence rate of varicocele, which required a new treatment, was significantly lower in group 1
21 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 20 of 31 than in the 2 other groups may have been due to 2 factors. The mean follow-up in this group was significantly shorter than in groups 2 and 3. Indeed, in the authors daily practice, glue has come into use more recently in this setting and is now the only embolic agent used for varicocele treatment. Furthermore, no systematic ultrasound imaging follow-up was performed beyond 2 months following the procedure, which could have led to potential lower detection rate of long-term varicocele recurrence. Lastly, infertility was the clinical indication for treatment in a large proportion of these patients. In this setting, varicocele was often asymptomatic and recurrence after embolization could not be determined without ultrasound imaging. The authors stated that the results of this study must be validated in future prospective RCTs with longer follow-up times to determine whether the embolic material can affect outcome. In a systematic review, Makris and colleagues (2018) evaluated the current evidence regarding the safety and effectiveness of the various embolic materials used in varicoceles embolization. A systematic review was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines. Databases were searched for clinical studies that investigated the clinical outcomes of embolization treatment for the management of testicular varicoceles. Study methodological quality was analyzed. A total of 23 retrospective and 7 prospective clinical studies were identified with a total of 3,505 patients. Technical success rates appeared to be above 90 % for all embolic materials without any significant differences. In terms of recurrence rates, glue (n = 251)
22 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 21 of 31 appeared to have the lowest and sclerosants alone (n = 728) the highest recurrence rates, which were 4.2 % (3.08 to 11 %, SD: 5.9) and % (5.15 to 18.8 %, SD: 6.06) within an average follow-up (f/u) of and months, respectively. Coils alone (n = 898) had an average recurrence rate of 9.1 % (1.4 to 17.8 %; SD: 5.79) and a mean f/u of 39.3 months. After an average of 12 months of f/u, the addition of sclerosants (n = 1,628) as an adjunct to coils did not improve recurrence rates (8.44 %, 5.1 to 16.5 %; SD: 3.4). No differences were reported regarding the safety profile of the various embolic materials. The authors concluded that despite the heterogeneity of the included studies, preliminary evidence supported the safe and effective use of the various embolic materials currently used for the management of varicoceles. At 1 year, glue appeared to be the most effective in preventing recurrence with coils being the second most effective. The addition of sclerosants to the coil embolization did not appear to have an impact on recurrence rates. They stated that further research is needed to elucidate the cost-effectiveness of these approaches. Endovenous Laser Ablation of Spermatic Vein for the Treatment of Varicocele: Basile and colleagues (2017) examined the feasibility and the reliability of endovenous laser ablation (EVLA) of the spermatic vein for the treatment of varicocele. These researchers consecutively and prospectively treated 11 patients (age range of 24 to 45 years, mean of 31) with left varicocele, phlebografically classified as Bahren type I and with indication for
23 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 22 of 31 percutaneous treatment. Clinical success was evaluated by color Doppler ultrasound (CDUS) 1 week, 1 months and 3 months after the procedures. These investigators also evaluated the pain feeling for 48 hours after the procedure on the basis of the visual analogue score (VAS) obtained through telephonic interview. Technical success was achieved in all cases. In all cases varicocele disappeared at CDUS at 1 and 3 months with reflux abolition; 2 cases of small vein laceration were noted without sequelae, no other complication has been described. All patients reported improvements either regarding symptoms and/or spermiographicparameters. The authors concluded that EVLA of spermatic vein was a feasible and safe treatment in patients with Bahren type I varicocele. The key advantage of this technique was the adoption of a standardized protocol, which remained one of the main problems in gaining scientific evidence in case of coil or sclerosant embolization (type and number of coils, amount of sclerosant agent, etc.). The main drawback of this study was the narrow population investigated, limited to Bahren type 1 for this first trial; these researchers awaited laser s manufacturer to develop a dedicated radio-opaque marker for fiber stip. Furthermore, an UpToDate review on Treatments for male infertility (Anawalt and Page, 2018) does not mention endovenous laser ablation as a therapeutic option. CPT Codes / HCPCS Codes / ICD-10 Codes Information in the [brackets] below has been added for clarification purposes. Codes requiring a 7th character are represented by "+":
24 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 23 of 31 Code Code Description CPT codes covered if selection criteria are met: Vascular embolization or occlusion, inclusive of all radiological supervision and interpretation, intraprocedural roadmapping, and imaging guidance necessary to complete the intervention; venous, other than hemorrhage (eg, congenital or acquired venous malformations, venous and capillary hemangiomas, varices, varicoceles) Other CPT codes related to the CPB: Transluminal balloon angioplasty, percutaneous; venous Unlisted procedure, vascular surgery Excision of varicocele or ligation of spermatic veins for varicocele [not covered for subclinical varicocele] Laparoscopy, surgical, with ligation of spermatic veins for varicocele [not covered for subclinical varicocele] HCPCS codes not covered for indications listed in the CPB: ArtVentive endoluminal occlusion system - no specific cde: ICD-10 codes covered if selection criteria are met: E29.1 Testicular hypofunction I86.1 Scrotal varices N N N N Azoospermia Oligospermia
25 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 24 of 31 The above policy is based on the following references: 1. Cornud F, Belin X, Amar E, et al. Varicocele: Strategies in diagnosis and treatment. Eur Radiol. 1999;9(3): Lukkarinen O, Hellstrom P, Leinonen S, Juntunen K. Is varicocele treatment useful? Ann Chir Gynaecol. 1997;86(1): Shlansky-Goldberg RD, VanArsdalen KN, Rutter CM, et al. Percutaneous varicocele embolization versus surgical ligation for the treatment of infertility: Changes in seminal parameters and pregnancy outcomes. J Vasc Interv Radiol. 1997;8(5): Rivilla F, Casillas JG. Testicular size following embolization therapy for paediatric left varicocele. Scand J Urol Nephrol. 1997;31 (1): Punekar SV, Prem AR, Ridhorkar VR, et al. Post-surgical recurrent varicocele: Efficacy of internal spermatic venography and steel-coil embolization. Br J Urol. 1996;77(1): Rivilla F, Casillas JG, Gallego J, Lezana AH. Percutaneous venography and embolization of the internal spermatic vein by spring coil for treatment of the left varicocele in children. J Pediatr Surg. 1995;30(4): Zuckerman AM, Mitchell SE, Venbrux AC, et al. Percutaneous varicocele occlusion: Longterm follow-up. J Vasc Interv Radiol. 1994;5 (2): Demas BE, Hricak H, McClure RD. Varicoceles: Radiologic diagnosis and treatment. Radiol Clin North Am. 1991;29 (3): Kuroiwa T, Hasuo K, Yasumori K, et al. Transcatheter embolization of testicular vein
26 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 25 of 31 for varicocele testis. Acta Radiol. 1991;32 (4): Wheatley JK, Bergman WA, Green B, Walther MM. Transvenous occlusion of clinical and subclinical varicoceles. Urology. 1991;37 (4): Sigman M, Howards SS. Male infertility. In: Campbell's Urology. 7 th Ed. Vol. II. PC Walsh, et al., eds. Philadelphia, PA: W.B. Saunders Co.; 1998; Ch. 43: Alqahtani A, Yazbeck S, Dubois J, et al. Percutaneous embolization of varicocele in children: A Canadian experience. J Pediatr Surg. 2002;37(5): Tay KH, Martin ML, Mayer AL, et al. Selective spermatic venography and varicocele embolization in men with circumaortic left renal veins. J Vasc Interv Radiol. 2002;13 (7): Evers JL, Collins JA, Clarke J. Surgery or embolisation for varicocele in subfertile men. Cochrane Database Syst Rev. 2009; (1):CD Sivanathan C, Abernethy LJ. Retrograde embolisation of varicocele in the paediatric age group: A review of 10 years' practice. Ann R Coll Surg Engl. 2003;85(1): Polito M Jr, Muzzonigro G, Centini R, et al. Percutaneous therapy of varicocele: Effects on semen parameters in young adults. Urol Int. 2004;72(2): Nabi G, Asterlings S, Greene DR, Marsh RL. Percutaneous embolization of varicoceles: Outcomes and correlation of semen improvement with pregnancy. Urology. 2004;63(2): Gat Y, Bachar GN, Everaert K, et al. Induction of spermatogenesis in azoospermic men
27 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 26 of 31 after internal spermatic vein embolization for the treatment of varicocele. Hum Reprod. 2005;20(4): Wagner L, Tostain J; Comite Andrologie de l'association Française d'urologie. Varicocele and male infertility: AFU 2006 guidelines. Prog Urol. 2007;17(1): French DB, Desai NR, Agarwal A. Varicocele repair: Does it still have a role in infertility treatment? Curr Opin Obstet Gynecol. 2008;20(3): Bechara CF, Weakley SM, Kougias P, et al. Percutaneous treatment of varicocele with microcoil embolization: Comparison of treatment outcome with laparoscopic varicocelectomy. Vascular. 2009;17 Suppl 3:S129-S Ayechu-Díaz A, Oscoz-Lizarbe M, Pérez- Martínez A, et al. Treatment of adolescent varicocele: Is percutaneous embolization better? Cir Pediatr. 2009;22(3): Storm DW, Hogan MJ, Jayanthi VR. Initial experience with percutaneous selective embolization: A truly minimally invasive treatment of the adolescent varicocele with no risk of hydrocele development. J Pediatr Urol. 2010;6(6): Tekgül S, Riedmiller H, Gerharz E, et al. Guidelines on paediatric urology. Arnheim, The Netherlands: European Association of Urology; Available at: Accessed April 16, Dohle GR, Diemer T, Giwercman A, et al. Guidelines on male infertility. Arnheim, The Netherlands: European Association of Urology; Avilable at:
28 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 27 of 31 20Infertility% pdf. Accessed April 16, Kondoh N, Nagai J, Yamamoto S. Clinical outcome of microsurgical varicocelectomy done for pain. Hinyokika Kiyo. 2010;56 (12): Seo JT, Kim KT, Moon MH, Kim WT. The significance of microsurgical varicocelectomy in the treatment of subclinical varicocele. Fertil Steril. 2010;93(6): Abdel-Meguid TA, Al-Sayyad A, Tayib A, Farsi HM. Does varicocele repair improve male infertility? An evidence-based perspective from a randomized, controlled trial. Eur Urol. 2011;59(3): Diegidio P, Jhaveri JK, Ghannam S, et al. Review of current varicocelectomy techniques and their outcomes. BJU Int. 2011;108(7): Ficarra V, Crestani A, Novara G, Mirone V. Varicocele repair for infertility: What is the evidence? Curr Opin Urol. 2012;22(6): Li F, Yamaguchi K, Okada K, et al. Significant improvement of sperm DNA quality after microsurgical repair of varicocele. Syst Biol Reprod Med. 2012;58(5): Ding H, Tian J, Du W, et al. Open nonmicrosurgical, laparoscopic or open microsurgical varicocelectomy for male infertility: A meta-analysis of randomized controlled trials. BJU Int. 2012;110(10): Shi Q, Zhu H, Wang XS, et al. Comparison of 3 microsurgical approaches to the treatment of varicocele: Report of 120 cases. Zhonghua Nan Ke Xue. 2013;19(10):
29 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 28 of 31 qawww.aetna.com/cpb/medical/data/400_499/0413_draft.html 07/15/ Masson P, Brannigan RE. The varicocele. Urol Clin North Am. 2014;41(1): Wang C, Swerdloff RS. Treatment of male infertility. UpToDate [online serial]. Waltham, MA: UpToDate; reviewed February Venbrux AC, Rudakov L, Plass A, et al. A new occlusion device: Application of the ArtVentive endoluminal occlusion system (EOS) -- first in human clinical trial. Cardiovasc Intervent Radiol. 2014;37(1): Pourmand G, Movahedin M, Dehghani S, et al. Does L-carnitine therapy add any extra benefit to standard inguinal varicocelectomy in terms of deoxyribonucleic acid damage or sperm quality factor indices: A randomized study. Urology. 2014;84(4): Showell MG, Mackenzie-Proctor R, Brown J, et al. Antioxidants for male subfertility. Cochrane Database Syst Rev. 2014;12:CD Practice Committee of the American Society for Reproductive Medicine; Society for Male Reproduction and Urology. Report on varicocele and infertility: A committee opinion. Fertil Steril. 2014;102(6): Wang J, Xia SJ, Liu ZH, et al. Inguinal and subinguinal micro-varicocelectomy, the optimal surgical management of varicocele: A meta-analysis. Asian J Androl. 2015;17 (1): Pajovic B, Radojevic N, Dimitrovski A, et al. Advantages of microsurgical varicocelectomy over conventional techniques. Eur Rev Med Pharmacol Sci. 2015;19(4): Kim HJ, Seo JT, Kim KJ, et al. Clinical significance of subclinical varicocelectomy in
30 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 29 of 31 male infertility: Systematic review and metaanalysis. Andrologia. 2016;48(6): Eyre RC. Evaluation of nonacute scrotal pathology in adult men. UpToDate [online serial]. Waltham, MA: UpToDate; reviewed February Esteves SC, Miyaoka R, Roque M, Agarwal A. Outcome of varicocele repair in men with nonobstructive azoospermia: Systematic review and meta-analysis. Asian J Androl. 2016;18(2): Li M, Wang Z, Li H. Laparoendoscopic singlesite surgery varicocelectomy versus conventional laparoscopic varicocele ligation: A meta-analysis. J Int Med Res. 2016;44 (5): Zhang Z, Zheng SJ, Yu W, et al. Comparison of surgical effect and postoperative patient experience between laparoendoscopic single-site and conventional laparoscopic varicocelectomy: a systematic review and meta-analysis. Asian J Androl. 2017;19(2): Favard N, Moulin M, Fauque P, et al. Comparison of three different embolic materials for varicocele embolization: Retrospective study of tolerance, radiation and recurrence rate. Quant Imaging Med Surg. 2015;5(6): Locke JA, Noparast M, Afshar K. Treatment of varicocele in children and adolescents: A systematic review and meta-analysis of randomized controlled trials. J Pediatr Urol. 2017;13(5): Wu X, Liu Q, Zhang R, et al. Therapeutic efficacy and safety of laparoscopic surgery versus microsurgery for varicocele of adult males: A meta-analysis. Medicine (Baltimore).
31 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 30 of ;96(34):e Basile A, Motta A, Failla G, et al. Endovenous laser ablation of spermatic vein for the treatment of varicocele. Eur J Radiol Open. 2017;4: Anawalt BD, Page ST. Treatments for male infertility. UpToDate Inc., Waltham, MA. Last reviewed February Makris GC, Efthymiou E, Little M, et al. Safety and effectiveness of the different types of embolic materials for the treatment of testicular varicoceles: A systematic review. Br J Radiol Mar 12: [Epub ahead of print].
32 Varicocele: Selected Treatments - Medical Clinical Policy Bulletins Aetna Page 31 of 31 Copyright Aetna Inc. All rights reserved. Clinical Policy Bulletins are developed by Aetna to assist in administering plan benefits and constitute neither offers of coverage nor medical advice. This Clinical Policy Bulletin contains only a partial, general description of plan or program benefits and does not constitute a contract. Aetna does not provide health care services and, therefore, cannot guarantee any results or outcomes. Participating providers are independent contractors in private practice and are neither employees nor agents of Aetna or its affiliates. Treating providers are solely responsible for medical advice and treatment of members. This Clinical Policy Bulletin may be updated and therefore is subject to change. Copyright Aetna Inc.
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele
 Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Varicocele repair for infertility: what is the evidence?
 REVIEW C URRENT OPINION Varicocele repair for infertility: what is the evidence? Vincenzo Ficarra a, Alessandro Crestani a, Giacomo Novara a, and Vincenzo Mirone b Purpose of review Considering the persistent
REVIEW C URRENT OPINION Varicocele repair for infertility: what is the evidence? Vincenzo Ficarra a, Alessandro Crestani a, Giacomo Novara a, and Vincenzo Mirone b Purpose of review Considering the persistent
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Corporate Medical Policy
 Corporate Medical Policy Ovarian, Internal Iliac and Gonadal Vein Embolization, Ablation and File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ovarian_and_internal_iliac_vein_embolization
Corporate Medical Policy Ovarian, Internal Iliac and Gonadal Vein Embolization, Ablation and File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ovarian_and_internal_iliac_vein_embolization
Comparing three different surgical techniques used in adult bilateral varicocele
 Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY
 ADULT UROLOGY PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY G. NABI, S. ASTERLINGS, D. R. GREENE, AND R. L. MARSH ABSTRACT Objectives. To assess
ADULT UROLOGY PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY G. NABI, S. ASTERLINGS, D. R. GREENE, AND R. L. MARSH ABSTRACT Objectives. To assess
Chapter 8 Effect of Varicocele Treatment
 Chapter 8 Effect of Varicocele Treatment Although multiple pathophysiological derangements have been documented in varicocele, the central issue is whether or not repair of this condition improves fertility.
Chapter 8 Effect of Varicocele Treatment Although multiple pathophysiological derangements have been documented in varicocele, the central issue is whether or not repair of this condition improves fertility.
Endovenous laser ablation of spermatic vein for the treatment of varicocele
 Endovenous laser ablation of spermatic vein for the treatment of varicocele Poster No.: C-22 Congress: ECR 207 Type: Scientific Exhibit Authors: A. Motta, G. Caltabiano, M. Pizzarelli, G. Failla, S. Palmucci,
Endovenous laser ablation of spermatic vein for the treatment of varicocele Poster No.: C-22 Congress: ECR 207 Type: Scientific Exhibit Authors: A. Motta, G. Caltabiano, M. Pizzarelli, G. Failla, S. Palmucci,
Early experience of laparoscopic varicocelectomy in College
 Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
COMPARATIVE STUDY OF LAPAROSCOPIC VARICOCELE LIGATION VERSUS INGUINAL VARICOCELECTOMY
 International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article COMPARATIVE STUDY OF LAPAROSCOPIC VARICOCELE
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article COMPARATIVE STUDY OF LAPAROSCOPIC VARICOCELE
Comparison of Two Percutaneous Approaches in Varicocele Embolization: Study of Complications, Radiations and Recurrence Rate
 Med. J. Cairo Univ., Vol. 86, No. 3, June: 1479-1484, 2018 www.medicaljournalofcairouniversity.net Comparison of Two Percutaneous Approaches in Varicocele Embolization: Study of Complications, Radiations
Med. J. Cairo Univ., Vol. 86, No. 3, June: 1479-1484, 2018 www.medicaljournalofcairouniversity.net Comparison of Two Percutaneous Approaches in Varicocele Embolization: Study of Complications, Radiations
OPEN APPROACH VERSUS MINIMALLY APPROACH FOR THE TREATMENT OF VARICOCELE IN CHILDREN - AN EPIDEMIOLOGICAL STUDY
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 1 PREVENTIVE MEDICINE - LABORATORY ORIGINAL PAPERS OPEN APPROACH VERSUS MINIMALLY APPROACH FOR THE TREATMENT OF VARICOCELE IN CHILDREN - AN EPIDEMIOLOGICAL
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 1 PREVENTIVE MEDICINE - LABORATORY ORIGINAL PAPERS OPEN APPROACH VERSUS MINIMALLY APPROACH FOR THE TREATMENT OF VARICOCELE IN CHILDREN - AN EPIDEMIOLOGICAL
THE PATIENT S GUIDE TO VARICOCELE
 The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
Original Research Article
 Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes
 Advances in Urology Volume 2013, Article ID 370969, 4 pages http://dx.doi.org/10.1155/2013/370969 Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes Mustafa
Advances in Urology Volume 2013, Article ID 370969, 4 pages http://dx.doi.org/10.1155/2013/370969 Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes Mustafa
Chapter 4 Varicocele Classification
 Chapter 4 Varicocele Classification In this chapter, we examine the several classification modes have been used to diagnose and grade varicocele, including physical exam, venographic examination, color
Chapter 4 Varicocele Classification In this chapter, we examine the several classification modes have been used to diagnose and grade varicocele, including physical exam, venographic examination, color
Sexual Dysfunction/Male Infertility. Kyu Hyun Kim, Joo Yong Lee, Dong Hyuk Kang 1, Hyungmin Lee 2, Ju Tae Seo 3, Kang Su Cho
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.703 Sexual Dysfunction/Male Infertility Impact of Surgical Varicocele Repair on Pregnancy Rate in Subfertile Men With Clinical Varicocele and
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.703 Sexual Dysfunction/Male Infertility Impact of Surgical Varicocele Repair on Pregnancy Rate in Subfertile Men With Clinical Varicocele and
Lindsay Machan, MD University of British Columbia Vancouver, British Columbia
 Varicocele Embolization and Serum Testosterone: What is the Evidence? Lindsay Machan, MD University of British Columbia Vancouver, British Columbia Lindsay Machan, MD, FSIR Stock: A4L, Calgary Scientific,
Varicocele Embolization and Serum Testosterone: What is the Evidence? Lindsay Machan, MD University of British Columbia Vancouver, British Columbia Lindsay Machan, MD, FSIR Stock: A4L, Calgary Scientific,
Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome. Original Policy Date
 MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY
 MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Advantages of microsurgical varicocelectomy over conventional techniques
 European Review for Medical and Pharmacological Sciences Advantages of microsurgical varicocelectomy over conventional techniques B. PAJOVIC, N. RADOJEVIC, A. DIMITROVSKI 1, M. RADOVIC 2, R. ROLOVIC, M.
European Review for Medical and Pharmacological Sciences Advantages of microsurgical varicocelectomy over conventional techniques B. PAJOVIC, N. RADOJEVIC, A. DIMITROVSKI 1, M. RADOVIC 2, R. ROLOVIC, M.
Male Infertility Caused by Varicoceles
 What You Need to Know About Male Infertility Caused by Varicoceles INTERVENTIONAL RADIOLOGY Find us on www.sirweb.org Q&A Questions and Answers About Male Infertility Caused by Varicoceles Q. What is a
What You Need to Know About Male Infertility Caused by Varicoceles INTERVENTIONAL RADIOLOGY Find us on www.sirweb.org Q&A Questions and Answers About Male Infertility Caused by Varicoceles Q. What is a
What are Varicoceles?
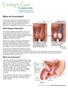 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
MP Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome
 Medical Policy MP 4.01.18 BCBSA Ref. Policy: 4.01.18 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: OB/GYN Reproduction Related Policies 4.01.11 Occlusion of Uterine Arteries Using Transcatheter
Medical Policy MP 4.01.18 BCBSA Ref. Policy: 4.01.18 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: OB/GYN Reproduction Related Policies 4.01.11 Occlusion of Uterine Arteries Using Transcatheter
Is Semen Analysis Necessary for Varicocele Patients in Their Early 20s?
 pissn: 22874208 / eissn: 22874690 World J Mens Health 2014 April 32(1): 5055 http://dx.doi.org/10.5534/wjmh.2014.32.1.50 Original Article Is Semen Analysis Necessary for Varicocele Patients in Their Early
pissn: 22874208 / eissn: 22874690 World J Mens Health 2014 April 32(1): 5055 http://dx.doi.org/10.5534/wjmh.2014.32.1.50 Original Article Is Semen Analysis Necessary for Varicocele Patients in Their Early
Real-time scrotal sonography of varicocele: new observations and laboratory findings correlation
 Real-time scrotal sonography of varicocele: new observations and laboratory findings correlation Poster No.: C-0137 Congress: ECR 2014 Type: Scientific Exhibit Authors: A. Babaei Jandaghi 1, H. Moradi
Real-time scrotal sonography of varicocele: new observations and laboratory findings correlation Poster No.: C-0137 Congress: ECR 2014 Type: Scientific Exhibit Authors: A. Babaei Jandaghi 1, H. Moradi
Varıcocele among healthy young men in Turkey; prevalence and relationship wıth body mass index
 ORIGINal ARTICLE Vol. 38 (1): 116-121, January - February, 2012 Varıcocele among healthy young men in Turkey; prevalence and relationship wıth body mass index Haluk Soylemez, Murat Atar, Ahmet Ali Sancaktutar,
ORIGINal ARTICLE Vol. 38 (1): 116-121, January - February, 2012 Varıcocele among healthy young men in Turkey; prevalence and relationship wıth body mass index Haluk Soylemez, Murat Atar, Ahmet Ali Sancaktutar,
Number: Policy *Please see amendment for Pennsylvania Medicaid at the end. Last Review 06/09/2016 Effective: 08/14/2001 Next Review: 06/08/2017
 1 of 6 Number: 0552 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. Aetna considers laser peripheral nerve block (laser neurolysis) experimental and investigational for any
1 of 6 Number: 0552 Policy *Please see amendment for Pennsylvania Medicaid at the end of this CPB. Aetna considers laser peripheral nerve block (laser neurolysis) experimental and investigational for any
Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients
 Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Evaluation of the role of varicocelectomy including external spermatic vein ligation in patients with scrotal pain
 Blackwell Science, LtdOxford, UKIJUInternational Journal of Urology0919-81722005 Blackwell Publishing Asia Pty LtdApril 2005124484488Original ArticleRole of varicocelectomy for paink Karademir et al. International
Blackwell Science, LtdOxford, UKIJUInternational Journal of Urology0919-81722005 Blackwell Publishing Asia Pty LtdApril 2005124484488Original ArticleRole of varicocelectomy for paink Karademir et al. International
Evaluation of Varicocele Frequency in Adolescents in the City of Isfahan
 Original Article Evaluation of Varicocele Frequency in Adolescents in the City of Isfahan Homayoun Abbasi, M.D. 1, 2, Amir Ghanbarian, M.D. 3, Saeid Salimi Khoozani, M.D. 1, Mohammad Hossein Nasr Esfahani,
Original Article Evaluation of Varicocele Frequency in Adolescents in the City of Isfahan Homayoun Abbasi, M.D. 1, 2, Amir Ghanbarian, M.D. 3, Saeid Salimi Khoozani, M.D. 1, Mohammad Hossein Nasr Esfahani,
Laparoscopic versus open inguinal spermatic vessel ligation in infertile men with varicocele.
 Biomedical Research 2018; 29 (7): 1389-1393 ISSN 0970-938X www.biomedres.info Laparoscopic versus open inguinal spermatic vessel ligation in infertile men with varicocele. Shuang Liu, Chuanyi Hu *, Ning
Biomedical Research 2018; 29 (7): 1389-1393 ISSN 0970-938X www.biomedres.info Laparoscopic versus open inguinal spermatic vessel ligation in infertile men with varicocele. Shuang Liu, Chuanyi Hu *, Ning
Evaluation of the Association of the Presence of Subclinical Varicocele with Subfertility in Men
 Evaluation of the Association of the Presence of Subclinical Varicocele with Subfertility in Men Original Article Ahmed M Hassanin, Hamed Abdalla Hamed, Maha Abdallah Arafat Department of Andrology and
Evaluation of the Association of the Presence of Subclinical Varicocele with Subfertility in Men Original Article Ahmed M Hassanin, Hamed Abdalla Hamed, Maha Abdallah Arafat Department of Andrology and
Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen Analysis
 African Journal of Urology 1110-5704 Vol. 17, No. 4, 2011 115-121 Original article Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen
African Journal of Urology 1110-5704 Vol. 17, No. 4, 2011 115-121 Original article Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen
Microscopic varicocelectomy as a treatment option for patients with severe oligospermia
 Original Article - Sexual Dysfunction/Infertility pissn 2466-0493 eissn 2466-054X Microscopic varicocelectomy as a treatment option for patients with severe oligospermia Chirag Gupta 1, Arun Chinchole
Original Article - Sexual Dysfunction/Infertility pissn 2466-0493 eissn 2466-054X Microscopic varicocelectomy as a treatment option for patients with severe oligospermia Chirag Gupta 1, Arun Chinchole
The Role of Testicular Volume in Adolescents With Varicocele: The Better Way and Time of Surgical Treatment
 The Role of Testicular Volume in Adolescents With Varicocele: The Better Way and Time of Surgical Treatment Claudio Spinelli, Martina Di Giacomo, Roberto Lo Piccolo, Alessandra Martin and Antonio Messineo
The Role of Testicular Volume in Adolescents With Varicocele: The Better Way and Time of Surgical Treatment Claudio Spinelli, Martina Di Giacomo, Roberto Lo Piccolo, Alessandra Martin and Antonio Messineo
Ultrasonographic diagnosis of varicoceles
 FERTILITY AND STERILITY Copyright 1993 The American Fertility Society Vol. 60, No, 4, October 1993 Printed on acid-free paper in U. S. A. Ultrasonographic diagnosis of varicoceles L. Andrew Eskew, M,D,*
FERTILITY AND STERILITY Copyright 1993 The American Fertility Society Vol. 60, No, 4, October 1993 Printed on acid-free paper in U. S. A. Ultrasonographic diagnosis of varicoceles L. Andrew Eskew, M,D,*
The significance of clinical practice guidelines on adult varicocele detection and management
 (2016) 18, 269 275 2016 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access INVITED REVIEW The significance of clinical practice guidelines
(2016) 18, 269 275 2016 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access INVITED REVIEW The significance of clinical practice guidelines
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
Original Article Clinical effect of microscopic subinguinal varicocelectomy or bypass surgery on nutcracker phenomenon-associated varicocele
 Int J Clin Exp Med 2018;11(12):13750-13756 www.ijcem.com /ISSN:1940-5901/IJCEM0080040 Original Article Clinical effect of microscopic subinguinal varicocelectomy or bypass surgery on nutcracker phenomenon-associated
Int J Clin Exp Med 2018;11(12):13750-13756 www.ijcem.com /ISSN:1940-5901/IJCEM0080040 Original Article Clinical effect of microscopic subinguinal varicocelectomy or bypass surgery on nutcracker phenomenon-associated
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea. Original Policy Date
 MP 4.01.10 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.10 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Chapter 1. Chapter 2. Chapter 3
 Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Does the duration of infertility affect semen parameters and pregnancy rate after varicocelectomy? A retrospective study
 Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Evaluation of the Effect of Varicocelectomy on Semen Parameters and Fertility
 Evaluation of the Effect of Varicocelectomy on Semen Parameters and (MBCh) 1 Abstract Background: Varicocele is the major reversible cause of male infertility. It is observed in 35% 40% of all men with
Evaluation of the Effect of Varicocelectomy on Semen Parameters and (MBCh) 1 Abstract Background: Varicocele is the major reversible cause of male infertility. It is observed in 35% 40% of all men with
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update
 Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME
 Oxford UnitedHealthcare Oxford Clinical Policy EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME Policy Number: SURGERY 105.8 T2 Effective Date: November 1, 2018 Instructions for
Oxford UnitedHealthcare Oxford Clinical Policy EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME Policy Number: SURGERY 105.8 T2 Effective Date: November 1, 2018 Instructions for
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Percutaneous Venography and Occlusion in the Management of Spermatic Varicoceles
 635 Percutaneous Venography and Occlusion in the Management of Spermatic Varicoceles z. j. B. Morag Rubinstein1 B. Goldwasser A. Yerushalmi3 B. Lunnenfeld3 Spermatic venography was performed in 140 patients;
635 Percutaneous Venography and Occlusion in the Management of Spermatic Varicoceles z. j. B. Morag Rubinstein1 B. Goldwasser A. Yerushalmi3 B. Lunnenfeld3 Spermatic venography was performed in 140 patients;
Setting The setting was secondary care. The economic study was carried out in Denver (CO), USA.
 Laparoscopic varicocele ligation: are there advantages compared with the microscopic subinguinal approach McManus M C, Barqawi A, Meacham R B, Furness P D, Koyle M A Record Status This is a critical abstract
Laparoscopic varicocele ligation: are there advantages compared with the microscopic subinguinal approach McManus M C, Barqawi A, Meacham R B, Furness P D, Koyle M A Record Status This is a critical abstract
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy
 Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Chapter 5 Treatment Modalities
 Chapter 5 Treatment Modalities In this chapter, we discuss the therapeutic modalities that have been applied to the treatment of varicocele, including medical therapy, surgical repair and embolization
Chapter 5 Treatment Modalities In this chapter, we discuss the therapeutic modalities that have been applied to the treatment of varicocele, including medical therapy, surgical repair and embolization
Iliac vein compression cause of varicocele. syndrome: An unusual
 Iliac vein compression cause of varicocele syndrome: An unusual M. David Bomalaski, MD, Joseph L. Mills, MD, Luis R. Argueso, MD, Roy M. Fujitani, MD, Alvin L. Sago, MD, and Allen E. Joseph, MD, Lackland
Iliac vein compression cause of varicocele syndrome: An unusual M. David Bomalaski, MD, Joseph L. Mills, MD, Luis R. Argueso, MD, Roy M. Fujitani, MD, Alvin L. Sago, MD, and Allen E. Joseph, MD, Lackland
Michael Meuse, MD Vascular and Interventional Radiology
 Michael Meuse, MD Vascular and Interventional Radiology OBJECTIVES BACKGROUND PATHOPHYSIOLOGY SYMPTOM COMPLEX EVALUATION AND RX OPTIONS INDICATION FOR EMBOLOTHERAPY RESULTS 1857 Richet: Chronic pelvic
Michael Meuse, MD Vascular and Interventional Radiology OBJECTIVES BACKGROUND PATHOPHYSIOLOGY SYMPTOM COMPLEX EVALUATION AND RX OPTIONS INDICATION FOR EMBOLOTHERAPY RESULTS 1857 Richet: Chronic pelvic
2019 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule
 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
Varicocele: surgical techniques in 2005
 Daniel H. Williams, MD, Edward Karpman, MD, Larry I. Lipshultz, MD Department of Urology, Baylor College of Medicine, Houston, Texas, USA WILLIAMS DH, KARPMAN E, LIPSHULTZ LI. Varicocele: surgical techniques
Daniel H. Williams, MD, Edward Karpman, MD, Larry I. Lipshultz, MD Department of Urology, Baylor College of Medicine, Houston, Texas, USA WILLIAMS DH, KARPMAN E, LIPSHULTZ LI. Varicocele: surgical techniques
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007
 ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
Laparoscopic Management of Varicocele A Hospital based study
 ISPUB.COM The Internet Journal of Surgery Volume 23 Number 2 Laparoscopic Management of Varicocele A Hospital based study A Tarun, J Veenu, K Dhanesh, P Sanjay Citation A Tarun, J Veenu, K Dhanesh, P Sanjay.
ISPUB.COM The Internet Journal of Surgery Volume 23 Number 2 Laparoscopic Management of Varicocele A Hospital based study A Tarun, J Veenu, K Dhanesh, P Sanjay Citation A Tarun, J Veenu, K Dhanesh, P Sanjay.
LEFT RENAL VEIN COMPRESSION
 MANAGEMENT of LEFT RENAL VEIN COMPRESSION in PATIENTS PRESENTING LEFT GONADAL VEIN REFLUX J. LEAL MONEDERO, MD S. ZUBICOA EZPELETA, MD angiovascularlyz@gmail.com Hospital Ruber Internacional. Madrid Á.
MANAGEMENT of LEFT RENAL VEIN COMPRESSION in PATIENTS PRESENTING LEFT GONADAL VEIN REFLUX J. LEAL MONEDERO, MD S. ZUBICOA EZPELETA, MD angiovascularlyz@gmail.com Hospital Ruber Internacional. Madrid Á.
Concomitant Varicocelectomy and Jaboulay's Operation
 Concomitant Varicocelectomy and Jaboulay's Operation Ali Hamdan Alkinany Haider Mahdy Alaaridhy* College of Medicine, University of Al-Qadisiah, Iraq. *College of Medicine, University of Al-Kufa, Iraq.
Concomitant Varicocelectomy and Jaboulay's Operation Ali Hamdan Alkinany Haider Mahdy Alaaridhy* College of Medicine, University of Al-Qadisiah, Iraq. *College of Medicine, University of Al-Kufa, Iraq.
Name of Policy: Ovarian and Internal Iliac Vein Embolization as Treatment of Pelvic Congestion Syndrome
 Name of Policy: Ovarian and Internal Iliac Vein Embolization as Treatment of Pelvic Congestion Syndrome Policy #: 172 Latest Review Date: June 2014 Category: Surgery Policy Grade: C Background/Definitions:
Name of Policy: Ovarian and Internal Iliac Vein Embolization as Treatment of Pelvic Congestion Syndrome Policy #: 172 Latest Review Date: June 2014 Category: Surgery Policy Grade: C Background/Definitions:
Male infertility too often ignored & forgotten
 Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Male infertility too often ignored & forgotten The journey 1. of the men A review of the guidelines Joo Teoh FRANZCOG MRCP(Ire) MRCOG MBBCh MSc(Lon) MD(Glasgow) SubspecialtyRepromed(UK) Consultant Obstetrician
Transurethral Resection of Ejaculatory Duct Obstruction: Monopolar, Bipolar or Holmium Laser?
 Transurethral Resection of Ejaculatory Duct Obstruction: Monopolar, Bipolar or Holmium Laser? Selahittin Çayan, MD, FECSM Professor of Urology University of Mersin School of Medicine, Department of Urology,
Transurethral Resection of Ejaculatory Duct Obstruction: Monopolar, Bipolar or Holmium Laser? Selahittin Çayan, MD, FECSM Professor of Urology University of Mersin School of Medicine, Department of Urology,
MALE FACTOR. Gerald J. Matthews, M.D.,* Ellen Dakin Matthews, R.N., and Marc Goldstein, M.D.*
 FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
The Varicocele as Related to Fertility
 The Varicocele as Related to Fertility JORDAN S. BROWN, M.D., LAWRENCE DUBIN, M.D., and ROBERT S. HOTCHKISS, M.D. VARICOCELECTOMY in the subfertile male, where indication for this procedure exists, has
The Varicocele as Related to Fertility JORDAN S. BROWN, M.D., LAWRENCE DUBIN, M.D., and ROBERT S. HOTCHKISS, M.D. VARICOCELECTOMY in the subfertile male, where indication for this procedure exists, has
Differences in Biochemical Markers and Body Mass Index Between Patients With and Without Varicocele
 ORIGINAL ARTICLE Differences in Biochemical Markers and Body Mass Index Between Patients With and Without Varicocele Shiou-Sheng Chen 1,2, William J. Huang 2,3 * 1 Division of Urology, Taipei City Hospital
ORIGINAL ARTICLE Differences in Biochemical Markers and Body Mass Index Between Patients With and Without Varicocele Shiou-Sheng Chen 1,2, William J. Huang 2,3 * 1 Division of Urology, Taipei City Hospital
The role of animal models in the study of varicocele
 Review Article The role of animal models in the study of varicocele Matthew J. Katz, Bobby B. Najari, Philip S. Li, Marc Goldstein Department of Urology, Weill Cornell Medical College, New York, NY, USA
Review Article The role of animal models in the study of varicocele Matthew J. Katz, Bobby B. Najari, Philip S. Li, Marc Goldstein Department of Urology, Weill Cornell Medical College, New York, NY, USA
Controlled trial of high spermatic vein ligation for varicocele infertile men* Avraham Karasik, M.D.:j: Benad Goldwasser, M.D.t
 Urology-andrology FERTILITY AND STERILITY Copyright 1995 American Society for Reproductive Medicine Vol. 63, No. I, January 1995 Printed on acid-free paper in U. S. A. Controlled trial of high spermatic
Urology-andrology FERTILITY AND STERILITY Copyright 1995 American Society for Reproductive Medicine Vol. 63, No. I, January 1995 Printed on acid-free paper in U. S. A. Controlled trial of high spermatic
Use of donor semen in the treatment of
 Use of donor semen in the treatment of male infertility Where is the evidence? Max H.J.M. Curfs Isala clinics Zwolle, The Netherlands Strength of evidence Systematic review Meta-analysis RCT 1A 1A 1B
Use of donor semen in the treatment of male infertility Where is the evidence? Max H.J.M. Curfs Isala clinics Zwolle, The Netherlands Strength of evidence Systematic review Meta-analysis RCT 1A 1A 1B
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Applied Anatomic Study of Testicular Veins in Adult Cadavers and in Human Fetuses
 Clinical Urology Anatomy of Testicular Veins in Adults and Human Fetuses International Braz J Urol Vol. 33 (2): 176-180, March - April, 2007 Applied Anatomic Study of Testicular Veins in Adult Cadavers
Clinical Urology Anatomy of Testicular Veins in Adults and Human Fetuses International Braz J Urol Vol. 33 (2): 176-180, March - April, 2007 Applied Anatomic Study of Testicular Veins in Adult Cadavers
CY2015 Hospital Outpatient: Endovascular Procedure APCs and Complexity Adjustments
 CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
The role of microsurgical varicocelectomy in treating male infertility
 Review Article The role of microsurgical varicocelectomy in treating male infertility Alexander J. Tatem 1, Robert E. Brannigan 2 1 Department of Urology, Indiana University, Indiana University School
Review Article The role of microsurgical varicocelectomy in treating male infertility Alexander J. Tatem 1, Robert E. Brannigan 2 1 Department of Urology, Indiana University, Indiana University School
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Management of Male Infertility: Roles of Contact
 97 Rubem Pochaczevsky1 Won J. Lee1 Errol Mallett2 Received September 12, 1985; accepted after revision January 30, 1986. 1 Department of Radiology, Department of Surgery, Long Island Jewish Medical Center,
97 Rubem Pochaczevsky1 Won J. Lee1 Errol Mallett2 Received September 12, 1985; accepted after revision January 30, 1986. 1 Department of Radiology, Department of Surgery, Long Island Jewish Medical Center,
Clinical Policy Bulletin: Nusinersen (Spinraza)
 Clinical Policy Bulletin: Nusinersen (Spinraza) Number: 0915 Policy *Pleasesee amendment forpennsylvaniamedicaidattheendofthiscpb. Note: REQUIRES PRECERTIFICATION.Footnotes for Precertification of nusinersen
Clinical Policy Bulletin: Nusinersen (Spinraza) Number: 0915 Policy *Pleasesee amendment forpennsylvaniamedicaidattheendofthiscpb. Note: REQUIRES PRECERTIFICATION.Footnotes for Precertification of nusinersen
EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY
 Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Clinical Policy: Essure Removal Reference Number: CP.MP.131
 Clinical Policy: Reference Number: CP.MP.131 Effective Date: 11/16 Last Review Date: 11/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.131 Effective Date: 11/16 Last Review Date: 11/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
The management of varicoceles by microdissection of the spermatic cord at the external inguinal ring
 FERTILITY AND STERILITY Copyright 1985 The American Fertility Society Printed in U.8A. The management of varicoceles by microdissection of the spermatic cord at the external inguinal ring Joel L. Marmar,
FERTILITY AND STERILITY Copyright 1985 The American Fertility Society Printed in U.8A. The management of varicoceles by microdissection of the spermatic cord at the external inguinal ring Joel L. Marmar,
EMBOLIZATION OF THE OVARIAN AND ILIAC VEINS FOR PELVIC CONGESTION SYNDROME
 UnitedHealthcare of California (HMO) UnitedHealthcare Benefits Plan of California (IEX EPO, IEX PPO) UnitedHealthcare of Oklahoma, Inc. UnitedHealthcare of Oregon, Inc. UnitedHealthcare Benefits of Texas,
UnitedHealthcare of California (HMO) UnitedHealthcare Benefits Plan of California (IEX EPO, IEX PPO) UnitedHealthcare of Oklahoma, Inc. UnitedHealthcare of Oregon, Inc. UnitedHealthcare Benefits of Texas,
MALE FACTOR. Preoperative semen analysis as a predictor of seminal improvement following varicocelectomy
 FERTILITY AND STERILITY VOL. 75, NO. 1, JANUARY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Preoperative
FERTILITY AND STERILITY VOL. 75, NO. 1, JANUARY 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Preoperative
FERTILITY SERVICE POLICY
 FERTILITY SERVICE POLICY Page 1 of 8 FERTILITY SERVICE POLICY Please note that all Clinical Commissioning policies are currently under review and elements within the individual policies may have been replaced
FERTILITY SERVICE POLICY Page 1 of 8 FERTILITY SERVICE POLICY Please note that all Clinical Commissioning policies are currently under review and elements within the individual policies may have been replaced
The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
 pissn: 2287-4208 / eissn: 2287-490 World J Mens Health 2014 April 32(1): 5-0 http://dx.doi.org/10.5534/wjmh.2014.32.1.5 Original Article The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
pissn: 2287-4208 / eissn: 2287-490 World J Mens Health 2014 April 32(1): 5-0 http://dx.doi.org/10.5534/wjmh.2014.32.1.5 Original Article The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
Clinical Policy: Digital Breast Tomosynthesis Reference Number: CP.MP.90
 Clinical Policy: Reference Number: CP.MP.90 Effective Date: 01/18 Last Review Date: 12/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.90 Effective Date: 01/18 Last Review Date: 12/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H
 Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Lymphatic and testicular artery-sparing laparoscopic varicocelectomy in children and adolescents Abdelaziz Yehya
 Original article 1 Lymphatic and testicular artery-sparing laparoscopic varicocelectomy in children and adolescents Abdelaziz Yehya Al-Azhar University Hospitals, Cairo, Egypt Correspondence to Abdelaziz
Original article 1 Lymphatic and testicular artery-sparing laparoscopic varicocelectomy in children and adolescents Abdelaziz Yehya Al-Azhar University Hospitals, Cairo, Egypt Correspondence to Abdelaziz
Final MPFS 2014 Summary SIR
 Final MPFS 2014 Summary SIR The CY 2014 PFS CF is $27.2006 (p531) Impact Tables (p1285) Refinement Panel Recommendations (p183) Table 23 presents information on the work RVUs for the codes considered by
Final MPFS 2014 Summary SIR The CY 2014 PFS CF is $27.2006 (p531) Impact Tables (p1285) Refinement Panel Recommendations (p183) Table 23 presents information on the work RVUs for the codes considered by
Pelvic Congestion Syndrome
 Pelvic Congestion Syndrome 1 Pelvic Congestion Syndrome (PCS) Condition and Symptom Background Condition Overview Urogynecological Symptoms 2 Non-cyclic pelvic pain affecting 39.1% of women at some point
Pelvic Congestion Syndrome 1 Pelvic Congestion Syndrome (PCS) Condition and Symptom Background Condition Overview Urogynecological Symptoms 2 Non-cyclic pelvic pain affecting 39.1% of women at some point
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Shunt-type and stop-type varicocele in adolescents: prognostic value of these two different hemodynamic patterns
 Shunt-type and stop-type varicocele in adolescents: prognostic value of these two different hemodynamic patterns Mohammad Javad Mohseni, M.D., Hamid Nazari, M.D., Erfan Amini, M.D., Niloufar Javan-Farazmand,
Shunt-type and stop-type varicocele in adolescents: prognostic value of these two different hemodynamic patterns Mohammad Javad Mohseni, M.D., Hamid Nazari, M.D., Erfan Amini, M.D., Niloufar Javan-Farazmand,
Significant decrease in sperm deoxyribonucleic acid fragmentation after varicocelectomy
 Significant decrease in sperm deoxyribonucleic acid fragmentation after varicocelectomy Philip Werthman, M.D., FACS, a Regina Wixon, Ph.D., b Kay Kasperson, B.S., b and Donald P. Evenson, Ph.D. c a Center
Significant decrease in sperm deoxyribonucleic acid fragmentation after varicocelectomy Philip Werthman, M.D., FACS, a Regina Wixon, Ph.D., b Kay Kasperson, B.S., b and Donald P. Evenson, Ph.D. c a Center
Recommended Interim Policy Statement 150: Assisted Conception Services
 Southampton City Clinical Commissioning Group (CCG) took on commissioning responsibility for Assisted Conception Services from 1 April 2013 for its population and agreed to adopt the interim policy recommendations
Southampton City Clinical Commissioning Group (CCG) took on commissioning responsibility for Assisted Conception Services from 1 April 2013 for its population and agreed to adopt the interim policy recommendations
Pelvic Congestion Syndrome and Its Relationship to Varices of the Lower Extremities
 250 JDMS 25:250-254 September/October 2009 Pelvic Congestion Syndrome and Its Relationship to Varices of the Lower Extremities A Literature Review KATHLEEN WHEELOCK, RVT Pelvic congestion syndrome occurs
250 JDMS 25:250-254 September/October 2009 Pelvic Congestion Syndrome and Its Relationship to Varices of the Lower Extremities A Literature Review KATHLEEN WHEELOCK, RVT Pelvic congestion syndrome occurs
Infertility Pregnancy After Varicocelectomy: Impact of Postoperative Motility and DFI
 Infertility Pregnancy After Varicocelectomy: Impact of Postoperative Motility and DFI Karen Baker, John McGill, Rakesh Sharma, Ashok Agarwal, and Edmund Sabanegh, Jr. OBJECTIVE METHODS RESULTS CONCLUSION
Infertility Pregnancy After Varicocelectomy: Impact of Postoperative Motility and DFI Karen Baker, John McGill, Rakesh Sharma, Ashok Agarwal, and Edmund Sabanegh, Jr. OBJECTIVE METHODS RESULTS CONCLUSION
