The role of microsurgical varicocelectomy in treating male infertility
|
|
|
- Rosemary Jenkins
- 6 years ago
- Views:
Transcription
1 Review Article The role of microsurgical varicocelectomy in treating male infertility Alexander J. Tatem 1, Robert E. Brannigan 2 1 Department of Urology, Indiana University, Indiana University School of Medicine, Indianapolis, Indiana, USA; 2 Department of Urology, Northwestern University, Feinberg School of Medicine, Chicago, IL, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: All authors; (III) Provision of study material or patients: All authors; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Dr. Alexander J. Tatem, MD. Indiana University Department of Urology, 535 Barnhill Drive, Suite 150, Indianapolis, Indiana, 46205, USA. tatema@iupui.edu. Abstract: Varicoceles are the most common cause of male infertility. They afflict 15 20% of the general male population and 40% of males with primary infertility. Although multiple treatment modalities exist, including radiographic embolization and laparoscopy, open subinguinal microsurgical varicocelectomy is currently the gold standard of treatment for this condition. In this article, we discuss the role of varicocelectomy in the treatment of the modern infertile male and present a practical, safe, and reproducible technique for the microsurgical approach. Keywords: Infertility; microsurgery; pampiniform plexus; sperm; testicle; varicocele; varicocelectomy Submitted Jun 15, Accepted for publication Jul 07, doi: /tau View this article at: Introduction Varicocele is the most common diagnosis in men presenting with concerns regarding their fertility (1). While the incidence of varicocele has been estimated to be between 15 20% in the general population, this value increases to 35 40% amongst men who present with primary infertility (2,3). Although it is estimated that approximately 80% of men with varicoceles will be fertile and not experience any sequelae as a result of their diagnosis, there is a preponderance of data suggesting that, for some men, the presence of a varicocele can negatively impact both Sertoli and Leydig cell function in a progressive fashion (4-9). Consequently, the evaluation and treatment of varicoceles has become one of the backbones of modern male reproductive medicine. Pathophysiology and anatomy Defined as a dilatation or tortuosity of the venous plexus that drains the testicle, a thorough understanding of testicular physiology and relevant anatomy provides the foundation upon which varicocele treatment is based. While there are several hypotheses that attempt to explain the correlation between varicoceles and subfertility, the most commonly acknowledged mechanism is that of testicular hyperthermia. The male scrotum is maintained at a temperature approximately 1 2 cooler than core body temperature. This thermoregulation is essential to proper testicular function and is achieved by a number of mechanisms (10). Chief among these is thin scrotal skin, which lacks an insulating layer of subcutaneous fat and the presence of a counter-current heat exchange system based around the pampiniform plexus. First proposed in 1959, this system allows arterial blood to be cooled by testicular venous return prior to reaching the testis (11). Dilatation of this network of veins allows the pooling of blood, which can then act as a radiator and raise the temperature of the entire scrotum (12,13). Although it is unclear exactly why these lower temperatures are so essential for proper testicular function, the detrimental effects of elevated scrotal
2 Translational Andrology and Urology, Vol 6, No 4 August temperatures are well documented, both clinically and on a histopathologic level. Varicoceles have been shown to result in the testicular atrophy of both subfertile men and fertile controls while demonstrating an association with relatively thin germinal epithelium and late stage maturation arrest on testicular biopsy (4,14,15). From an anatomic standpoint, blood supply to the testis, epididymis, and vas deferens is achieved by the following vessels: the internal spermatic artery (also known as the gonadal artery), the deferential artery, and the cremasteric artery (also known as the external spermatic artery) (16). The internal spermatic artery and the deferential artery arise from the aorta and inferior vesical artery, respectively. As such, they both follow the spermatic cord within the internal spermatic fascia and are considered deep. The cremasteric artery arises from the inferior epigastric artery and supplies the surface of the cord at the level of the external inguinal ring before traveling within external spermatic fascia distally and ultimately anastomosing with the internal spermatic and deferential. It is also considered deep, but it is important to note that it travels in a distinct fascial compartment from its two cohorts and runs between the internal and external spermatic fascial layers. All three vessels are ultimately responsible for supplying blood to the testis and epididymis, although the majority of blood flow comes from the larger caliber internal spermatic artery. In regards to venous drainage, all urologists are familiar with the network of veins known as the pampiniform plexus. It is this structure that, when dilated, is responsible for the pathognomonic bag of worms first described by Dubin and Amelar in 1970 (17). However, we advocate that successful microsurgeons should strive for a deeper understanding of the spermatic cord s venous vasculature. Fortunately, this is relatively simple if one applies what is readily known about fascial compartments of the spermatic cord and its aforementioned arteries. It is a well-established anatomic maxim that veins typically follow arteries and this statement holds true for the spermatic cord. Consequently, there are three groupings of veins: the internal spermatic veins (also known as the gonadal veins), the deferential veins, and the cremasteric veins. The internal spermatic and deferential veins course within the internal spermatic fascia while the cremasteric veins travel between the external and internal fascial layers. The cremasteric veins are only accessible at the inguinal/subinguinal level and by virtue of this are missed when performing laparoscopic or retroperitoneal repairs. This is significant as studies have shown these vessels to be involved in up to 50% of varicoceles (18). The internal spermatic, deferential, and cremasteric veins intertwine and anastomose several times over as they approach the testis, creating the familiar pampiniform plexus. Collateral venous drainage of the testis is then provided by the gubernacular veins at the base of the testis that later coalesce with superficial scrotal veins. With a subinguinal microsurgical approach, the internal spermatic and cremasteric veins are ligated while venous drainage is maintained through the gubernacular and deferential vessels. If the surgeon elects to deliver the testis and ligate the gubernacular veins, drainage is maintained solely by the differentials. Other vital structures that are contained within the spermatic cord include the cremasteric muscle fibers, the genital branch of the genitofemoral nerve, and the vas deferens. The cremasteric muscle fibers and the genital branch of the genitofemoral nerve travel alongside the cremasteric vessels between the external and internal layers of spermatic fascia while the vas deferens travels within the internal spermatic fascia and is intimately associated with its own named vessels. As with all veins, the internal spermatic, deferential, and cremasteric veins possess valves that are designed to help prevent retrograde flow. It is the failure of these valves that is thought to precipitate varicocele formation. Clinically, varicoceles are most commonly found on the left side. This finding is thought to be due to the longer course that the spermatic vessels must take on this side prior to inserting on the renal vein. This longer course means that veins on this side are exposed to greater hydrostatic pressure, potentially leading to preferential valve failure. It is also worth noting is that the insertion of the left internal spermatic vein into the left renal vein is directly perpendicular, allowing for direct transmittance of elevated renal vein pressures down the entire length of the vein. On the contralateral side, the right internal spermatic vein inserts directly on the inferior vena cava after a much shorter course and at an oblique angle. This course is protective and shields the right gonadal vein from experiencing elevated pressures. As a result, isolated right-sided varicoceles are quite rare and the presence of one should always prompt imaging to rule out more sinister pathology. Treatment indications Below we will discuss indication for treating varicoceles for men with infertility, hypogonadism, and pain. (This manuscript does not specifically address varicoceles in the
3 724 Tatem and Brannigan. Techniques and complications from the masters in andrologic surgery pediatric population, and this condition has its own set of criteria governing the decision to pursue therapeutic correction.) Male infertility As per the American Society for Reproductive Medicine and Society for Male Reproduction and Urology s Practice Committee report Report on varicocele and infertility: a committee opinion varicoceles should be treated when each of the following criteria are met: (I) The varicocele is palpable on physical examination of the scrotum; (II) The couple has known infertility; (III) The female partner has normal fertility or a potentially treatable cause of infertility; (IV) The male partner has abnormal semen parameters (19). In regards to infertility, scrotal ultrasound has a very limited role in the evaluation of varicoceles. Repair of subclinical varicoceles that are visible on ultrasound but not apparent on physical exam has not been shown to improve fertility and as such is not considered standard of care. However, US may be utilized to evaluate for the presence of varicoceles in men in whom an adequate scrotal exam is not possible. Although official, data-driven criteria are lacking, most experts agree that multiple spermatic veins > mm in diameter at rest and with Valsalva tend to indicate the presence of a clinically significant varicocele (20). While intrauterine insemination (IUI) and in vitro fertilization/intracytoplasmic sperm injection (IVF- ICSI) are options for couples experiencing varicocelerelated infertility, patients should be educated that these approaches circumvent, rather than treat, their underlying pathology. Varicocele repair offers a durable solution for pure varicocele-related infertility with 80% of patients demonstrating improvement in semen analysis parameters and 40% ultimately achieving spontaneous pregnancy (21). Comparatively, IUI and IVF-ICSI are required for each attempt at pregnancy and as a result are much less cost effective (22-24). Even if IUI or IVF-ICSI are ultimately required due to female factors, a recent meta-analysis examining a total of 870 IVF cycles showed that couples in which the male partner underwent varicocelectomy prior to IVF were over twice as likely to achieve a live birth when compared to those who elected observation (25). Varicocelectomy may also improve the male partner s semen analysis parameters to a point where the couple, who may have previously only qualified IVF-ICSI, can become candidates for IUI. Conversely, for couples in which time is a factor, varicocele repair can be deferred until after a pregnancy has been achieved through the use of assisted reproductive technologies (ART). This approach allows the male partner s semen parameters to recover while the female partner is pregnant and optimizes his semen parameters for any future pregnancy attempts. For men with non-obstructive azoospermic (NOA), varicocele repair has been shown to return sperm to the ejaculate for approximately ~40% of patients with a live birth rate of 6% (26). This is encouraging as return of sperm to the ejaculate may obviate the need for testicular extraction. However, the overwhelming majority of these patients will still require some form of ART and as such some authors have found that directly proceeding to microsurgical testicular sperm extraction (M-TESE) may be a more cost-effective option (27). Adult men with clinically significant varicoceles and normal semen analysis parameters should be offered observation with annual or biennial semen analyses given the risk for progressive testicular dysfunction (5-8). Hypogonadism The idea of varicocelectomy as a treatment for hypogonadism is an emerging and controversial concept. Although early studies did not demonstrate any increase in serum testosterone, these were small in scale and did not specifically screen for hypogonadal men. Rather, the men were primarily infertile with varying hormonal profiles (28,29). Since that time, several studies have demonstrated an increase in serum testosterone for subpopulations of infertile men with both low serum testosterone and hypogonadal symptomology (30,31). In their recent meta-analysis, Li et al. found that, on average, men undergoing varicocelectomy experienced an increase in their serum testosterone of ng/dl (32). This has led some authors to advocate for adding hypogonadism to the list of indications for varicocelectomy and propose early intervention as a way to avoid future androgen deficiency (8,33). Although these findings are promising, it is important to note that the idea of varicocelectomy as treatment for hypogonadism is still nascent. It not yet considered to be standard of care and has yet to be recommended by any governing body.
4 Translational Andrology and Urology, Vol 6, No 4 August Symptomatic varicoceles The final indication for varicocelectomy is that of pain or discomfort. Typically described as an aching or dull pain localizing to the ipsilateral testicle or inguinal region, there is a tremendous amount of variability in the characterization, intensity, and frequency of this discomfort. Patients may often have other chronic pain syndromes or have sought care from several other providers prior to presentation. We believe that a methodical and conservative approach beginning with lifestyle modifications, judicious non-steroidal anti-inflammatory use, and pelvic floor physical therapy frequently benefit this population prior to proceeding with surgical repair. When conservative measures fail, patients should be counseled that surgery may not relieve their discomfort. There is significant variability regarding the outcomes of varicocelectomy when performed for pain with series success rates ranging from 53 94% (8). Options for repair The foundation upon which varicocele repair is based is that, by interrupting the venous return from the engorged veins of the pampiniform plexus, collateral flow can be forced to egress through the gubernacular and deferential veins and the pooling of blood will be prevented. This must be accomplished while preserving all vital structures of the testicular cord, to include the internal spermatic artery, vas deferens, and spermatic cord lymphatics. A variety of surgical approaches ranging from the classic Ivanissevich and Palomo repairs to laparoscopy have been developed to achieve these goals (34,35). However, due to its high success rate and minimal complication rates, microsurgical varicocelectomy has been well established as the gold standard for varicocele repair in the modern era (36-39). With proper technique and experience, recurrence rates and incidence of hydrocele approach 1 2% and 0 1%, respectively (37). Embolization remains a nonsurgical option, but is typically reserved as a second-line treatment for patients who fail surgery as its own failure rate is approximately 4%, significantly higher than that of the microsurgical approach (40). There is also the notinsignificant concern about gonadal radiation exposure in an already vulnerable population. Technique In regards to incision site selection, there are essentially two options for microsurgical varicocelectomy: that of the more traditional inguinal approach or a sub-inguinal incision. The inguinal approach, originally described by Ivanissevich, is centered at the external inguinal ring and requires the incision of the external oblique aponeurosis (34). This has the advantage of avoiding distal arborization, leading to the discovery of fewer veins that require ligation and a decreased chance of encountering multiple arteries (41). This can facilitate safe and expeditious dissection, but the incision of the external oblique aponeurosis and subsequent repair is typically associated with greater post-operative discomfort. As such, we prefer the subinguinal approach at our institution. For the subinguinal approach, the location of the external inguinal ring is identified by invaginating the scrotal skin with an index finger parallel to the spermatic cord as it passes over the pubic tubercle. An oblique 2.5 to 3-cm incision is made along Langer s lines just below this level. Camper s and Scarpa s fasciae are then divided with electrocautery. The wound is deepened with blunt dissection utilizing Army/Navy retractors until the level of the spermatic cord is reached. The cord is most easily identified as it passes over the pubic tubercle. Gentle traction on the ipsilateral testicle and palpation at this level can help identify the cord in challenging circumstances. Once identified, the cord is encircled with the use of the index finger and the thumb, although some surgeons may prefer to use a Babcock instrument. A 1-inch Penrose drain is then looped underneath the cord and used to gently deliver the cord from the wound. If there is any difficulty in elevating the cord, we advocate encircling the cord more distally as posterior cremasteric attachments are frequently encountered as the cord immediately exits the external ring. It is at this point that the floor of the incision is inspected to ensure the entirety of the cord has been isolated and elevated. With the cord isolated and elevated, the operating microscope is brought into the field and the cord is examined under 20 magnification. The cord is then draped over the operating surgeon s index finger at the distal interphalangeal joint and its contents are evenly spread. Gerald forceps without teeth are used to bluntly perforate the external oblique fascia and access the inside of the spermatic cord, and Bovie electrocautery is used to incise the external and internal spermatic fasciae. Some authors use Jacobsen hemostats to secure the spermatic cord fascial edges for traction, and but we simply let the fascial edges splay laterally with back pressure on the spermatic cord
5 726 Tatem and Brannigan. Techniques and complications from the masters in andrologic surgery using the surgeon s index finger. As this approach requires a skilled assistant, some surgeons may prefer to rest the cord on knife handle or a tongue depressor sheathed within a Penrose drain. A key technical aspect of this procedure is to achieve exposure that transforms the spermatic cord from a cylindrical 3-dimensional structure to a more 2-dimensional configuration, facilitating identification of individual vessels and structures. This dissection is carried proximally to the level of the external inguinal ring. Some authors have described placing the testicle on mild traction to further expose the section of the cord that traditionally rests within the inguinal canal (42). A 3-mm micro-doppler is introduced before the fine dissection begins. We request that the anesthesiologist keep the patient s systolic blood pressure >100 mmhg to facilitate identification and differentiation of arterial signals. The field is copiously irrigated with 1% lidocaine solution to combat vasospasm, although a 1:5 dilution of papaverine (30 mg/ml) may also be used. Both of these maneuvers are worth emphasizing as they are frequently overlooked and early identification of the testicular artery is absolutely essential for safe dissection. It is with this exposure that we begin to search for the artery with our micro-doppler probe. Once this has been identified, great care is taken to protect it and re-confirm its identity throughout the dissection. If difficulty is encountered in identifying the artery, the surgeon should confirm that the systolic blood pressure is still > 100 mmhg. If the artery is still not identified, additional trouble shooting should include confirming that the irrigant being used is lidocaine alone and not lidocaine with epinephrine, as this latter solution will cause arterial vasospasm and suppress the Doppler signal. The vas deferens and its vascular packet are then identified and, when possible, brought to the lateral or medial edge of the cord and excluded from the operative field. It is at this point that we begin to identify and ligate the internal spermatic and cremasteric veins. Fine tipped Bishop forceps are used to grasp the adventitial tissues while a micro-tipped Jacobson clamp facilitates dissection. 3-0 or 4-0 silk ties are passed behind the veins, the micro Doppler is used once more to confirm their identity, and they are then ligated and divided. In order to improve efficiency, we advocate passing the midpoint of the silk tie underneath the vessel before cutting the tie in two, essentially turning what was a single silk tie into two. This minimizes any potential trauma from multiple passes under the same vessel. Some surgeons may prefer to use clips to ligate the vessels, although we have found the use of ties to be more precise in our experience. Any hemorrhage is immediately controlled with judicious use of fine-tipped bipolar electrocautery and saline irrigation. Any lymphatics are identified and preserved in order to minimize the risk of a post-operative hydrocele. Unfortunately, it is not uncommon to encounter periarterial veins that are intimately associated with the testicular artery or are scarred in as a result of some previous inflammatory response. In these scenarios, we recommend changing the angle of dissection. This can be achieved by approaching the structure in question from the opposite side of the table or even flipping the cord over for a posterior approach. When these maneuvers are unsuccessful, we endorse carrying the dissection superiorly, even if this requires opening the external ring. Due to distal venous arborization, an exceptionally challenging distal venous dissection may be exponentially more feasible at a more proximal location. Once all visible veins have been ligated and divided, the internal spermatic artery, or arteries, is inspected visually and with the Doppler once more to ensure patency. The vas is inspected as well. The cord and the wound are then irrigated copiously and the cord is returned to its orthotopic position. It is at this point that the cord is inspected in-situ for any collateral venous supply which is subsequently ligated when present. The wound is inspected for bleeding and infiltrated with a generous amount of 0.25% bupivacaine. A cord block is also performed. Scarpa s and Camper s fasciae are then closing with a running 3-0 absorbable-braided suture and the skin is closed with a 4-0 subcuticular monofilament. The wound is then reinforced with Steri-strips and a dry sterile dressing. Finally, a scrotal support with fluffy dressings is applied. Post-operatively, the patient is instructed to avoid any significant exertion or lifting for approximately 1 2 weeks. He is then seen at a standard 2-week post-op check to evaluate for proper healing. Semen analyses are obtained at 3-month intervals following surgery and patients are advised that they may not see optimization of their semen analysis parameters until 6 to 9 months following surgery. Complications Complications unique to microsurgical varicocelectomy include recurrence, hydrocele, testicular artery injury and vasal injury. Fortunately, these are all quite rare and their rates compare favorably to those of other surgical
6 Translational Andrology and Urology, Vol 6, No 4 August approaches and radiographic embolization (37,40,43). Testicular artery and vasal injury are considered by far to be the most catastrophic complications and should be considered never ever events as they can result in loss of the testicle and obstruction of the ipsilateral delivery of sperm, respectively. While vasal injury can be addressed with immediate repair using standard vasectomy reversal technique, arterial injury is almost never salvageable. Pediatric patients can arguably tolerate proximal ligation of the testicular artery reasonably well due the plasticity afforded by their age and collateral flow from the deferential and cremasteric arteries, but adults are almost completely dependent on their testicular artery for adequate gonadal perfusion (44). Fortunately, the incidence of testicular artery injury during varicocelectomy is less than 1% and careful use of the micro-doppler and adherence to basic surgical principles should drive the incidence of this complication to almost zero (45,46). Hydrocele following varicocelectomy is the result of inadvertent ligation of efferent lymphatics and is managed identically to idiopathic adult hydrocele. In the past, nonmicrosurgical approaches resulted in hydrocele formation in approximately 7% of patients while the introduction of the operating microscope has reduced this incidence to 0 1% (37,43,47). In our experience, patients with a history of prior inguinal or groin surgery are at a slightly higher risk for this and are counseled accordingly. The vast majority of hydroceles occurring after varicocelectomy in our experience are reactive and resolve on their own over several weeks to months after surgery. For the rare patient who develops a persistent hydrocele post-varicocelectomy, hydrocelectomy remains the gold standard to resolve the condition. Varicocele recurrence rates are similarly low and range from 1 2%. These are often thought to result from the collateralization of cremasteric veins that can be missed before they enter at the level of the external inguinal ring (16). Also, smaller veins that may have been missed during a patient s initial surgery can become engorged due to physiologic shifts and similarly incite recurrence. In these scenarios, both repeat surgery and radiographic embolization may be considered viable options as they both display success rates in excess of 90% (10,40,48). Conclusions Varicoceles remain the most common cause of malefactor infertility. Fortunately, they are also the most treatable. Microscopic varicocelectomy is a safe and reliable outpatient procedure that allows the majority of affected patients to optimize their fertility in a durable fashion. We believe that the detailed technique presented above offers a safe and effective approach that skilled microsurgeons can refer to while performing this staple of men s microsurgery. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Nagler HM, Grotas AB. Varicocele. In: Lipshultz LI, Howards S, Niederberger CS. editors. Infertility in the Male. New York: Cambridge University Press,2009: Clarke BG. Incidence of varicocele in normal men and among men of different ages. Jama 1966;198: Fretz PC, Sandlow JI. Varicocele: current concepts in pathophysiology, diagnosis, and treatment. Urol Clin North Am 2002;29: Lipshultz LI, Corriere JN Jr. Progressive testicular atrophy in the varicocele patient. J Urol 1977;117: Witt MA, Lipshultz LI. Varicocele: a progressive or static lesion? Urology 1993;42: Gorelick JI, Goldstein M. Loss of fertility in men with varicocele. Fertil Steril 1993;59: Chehval MJ, Purcell MH. Deterioration of semen parameters over time in men with untreated varicocele: evidence of progressive testicular damage. Fertil Steril 1992;57: Schlegel PN, Goldstein M. Alternate indications for varicocele repair: non-obstructive azoospermia, pain, androgen deficiency and progressive testicular dysfunction. Fertil Steril 2011;96: Tulloch WS. Varicocele in subfertility; results of treatment. Br Med J 1955;2: Masson P, Brannigan RE. The varicocele. Urol Clin North Am 2014;41: Dahl EV, Herrick JF. A vascular mechanism for maintaining testicular temperature by counter-current exchange. Surg Gynecol Obstet 1959;108:
7 728 Tatem and Brannigan. Techniques and complications from the masters in andrologic surgery 12. Goldstein M, Eid JF. Elevation of intratesticular and scrotal skin surface temperature in men with varicocele. J Urol 1989;142: Lewis RW, Harrison RM. Contact scrotal thermography: application to problems of infertility. J Urol 1979;122: Scott LS. Varicocele: a treatable cause of subfertility. Br Med J 1961;1: Elzanaty S. Varicocele repair in non-obstructive azoospermic men: diagnostic value of testicular biopsy - a meta-analysis. Scand J Urol 2014;48: Mirilas P, Mentessidou A. Microsurgical subinguinal varicocelectomy in children, adolescents, and adults: surgical anatomy and anatomically justified technique. J Androl 2012;33: Dubin L, Amelar RD. Varicocele size and results of varicocelectomy in selected subfertile men with varicocele. Fertil Steril 1970;21: Chehval MJ, Purcell MH. Varicocelectomy: incidence of external spermatic vein involvement in the clinical varicocele. Urology 1992;39: Report on varicocele and infertility: a committee opinion. Fertil Steril 2014;102: Stahl P, Schlegel PN. Standardization and documentation of varicocele evaluation. Curr Opin Urol 2011;21: Marmar JL, Agarwal A, Prabakaran S, et al. Reassessing the value of varicocelectomy as a treatment for male subfertility with a new meta-analysis. Fertil Steril 2007;88: Schlegel PN. Is assisted reproduction the optimal treatment for varicocele-associated male infertility? A costeffectiveness analysis. Urology 1997;49: Chiles KA, Schlegel PN. Cost-effectiveness of varicocele surgery in the era of assisted reproductive technology. Asian J Androl 2016;18: Penson DF, Paltiel AD, Krumholz HM, et al. The costeffectiveness of treatment for varicocele related infertility. J Urol 2002;168: Esteves SC, Roque M, Agarwal A. Outcome of assisted reproductive technology in men with treated and untreated varicocele: systematic review and meta-analysis. Asian J Androl 2016;18: Weedin JW, Khera M, Lipshultz LI. Varicocele repair in patients with nonobstructive azoospermia: a meta-analysis. J Urol 2010;183: Lee R, Li PS, Goldstein M, et al. A decision analysis of treatments for nonobstructive azoospermia associated with varicocele. Fertil Steril 2009;92: Segenreich E, Shmuely H, Singer R, et al. Andrological parameters in patients with varicocele and fertility disorders treated by high ligation of the left spermatic vein. Int J Fertil 1986;31: Hudson RW, Perez-Marrero RA, Crawford VA, et al. Hormonal parameters in incidental varicoceles and those causing infertility. Fertil Steril 1986;45: Abdel-Meguid TA, Farsi HM, Al-Sayyad A, et al. Effects of varicocele on serum testosterone and changes of testosterone after varicocelectomy: a prospective controlled study. Urology 2014;84: Whelan P, Levine L. Effects of varicocelectomy on serum testosterone. Transl Androl Urol 2016;5: Li F, Yue H, Yamaguchi K, et al. Effect of surgical repair on testosterone production in infertile men with varicocele: a meta-analysis. Int J Urol 2012;19: Bach PV, Najari BB, Goldstein M. Varicocele - a case for early intervention. F1000Res 2016;5. pii: F1000 Faculty Rev Ivanissevich O. Left varicocele due to reflux; experience with 4,470 operative cases in forty-two years. J Int Coll Surg 1960;34: Palomo A. Radical cure of varicocele by a new technique; preliminary report. J Urol 1949;61: Al-Kandari AM, Shabaan H, Ibrahim HM, et al. Comparison of outcomes of different varicocelectomy techniques: open inguinal, laparoscopic, and subinguinal microscopic varicocelectomy: a randomized clinical trial. Urology 2007;69: Cayan S, Shavakhabov S, Kadioglu A. Treatment of palpable varicocele in infertile men: a meta-analysis to define the best technique. J Androl 2009;30: Ding H, Tian J, Du W, et al. Open non-microsurgical, laparoscopic or open microsurgical varicocelectomy for male infertility: a meta-analysis of randomized controlled trials. BJU Int 2012;110: Wang J, Xia SJ, Liu ZH, et al. Inguinal and subinguinal micro-varicocelectomy, the optimal surgical management of varicocele: a meta-analysis. Asian J Androl 2015;17: Cassidy D, Jarvi K, Grober E, et al. Varicocele surgery or embolization: Which is better? Can Urol Assoc J 2012;6: Hopps CV, Lemer ML, Schlegel PN, et al. Intraoperative varicocele anatomy: a microscopic study of the inguinal versus subinguinal approach. J Urol 2003;170: Wu K, Yan G, Yin W, et al. A Novel Approach of
8 Translational Andrology and Urology, Vol 6, No 4 August Microscopic Subinguinal Varicocelectomy with a Pulling Strategy. Urology 2017;104: Al-Said S, Al-Naimi A, Al-Ansari A, et al. Varicocelectomy for male infertility: a comparative study of open, laparoscopic and microsurgical approaches. J Urol 2008;180: Raman JD, Goldstein M. Intraoperative characterization of arterial vasculature in spermatic cord. Urology 2004;64: Leung L, Ho KL, Tam PC, et al. Subinguinal microsurgical varicocelectomy for male factor subfertility: ten-year experience. Hong Kong Med J 2013;19: Wosnitzer M, Roth JA. Optical magnification and Doppler ultrasound probe for varicocelectomy. Urology 1983;22: Szabo R, Kessler R. Hydrocele following internal spermatic vein ligation: a retrospective study and review of the literature. J Urol 1984;132: Rotker K, Sigman M. Recurrent varicocele. Asian J Androl 2016;18: Cite this article as: Tatem AJ, Brannigan RE. The role of microsurgical varicocelectomy in treating male infertility. Transl Androl Urol 2017;6(4): doi: /tau
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele
 Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
THE PATIENT S GUIDE TO VARICOCELE
 The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY
 MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
Comparing three different surgical techniques used in adult bilateral varicocele
 Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
What are Varicoceles?
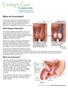 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy
 Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients
 Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Urol Sci 2010;21(1):30 37 ORIGINAL ARTICLE Microsurgical Subinguinal Varicocelectomy An Experience of 327 Operations in 224 Patients Chia-Feng Lee 1, Pei-Yu Lin 1,2, I-Hung Chen 1,2, Yu-Sheng Cheng 1,2,
Early experience of laparoscopic varicocelectomy in College
 Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
Varicocele anatomy during subinguinal microsurgical varicocelectomy in Chinese men
 ORIGINAL ARTICLE Varicocele anatomy during subinguinal microsurgical varicocelectomy in Chinese men K.-L. Lv*, J.-T. Zhuang*, L. Zhao, Z. Wan, Y.-D. Zhang, Y. Gao, X.-Z. Sun, S.-P. Qiu, C.-H. Deng & X.-A.
ORIGINAL ARTICLE Varicocele anatomy during subinguinal microsurgical varicocelectomy in Chinese men K.-L. Lv*, J.-T. Zhuang*, L. Zhao, Z. Wan, Y.-D. Zhang, Y. Gao, X.-Z. Sun, S.-P. Qiu, C.-H. Deng & X.-A.
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Laparoscopic versus open inguinal spermatic vessel ligation in infertile men with varicocele.
 Biomedical Research 2018; 29 (7): 1389-1393 ISSN 0970-938X www.biomedres.info Laparoscopic versus open inguinal spermatic vessel ligation in infertile men with varicocele. Shuang Liu, Chuanyi Hu *, Ning
Biomedical Research 2018; 29 (7): 1389-1393 ISSN 0970-938X www.biomedres.info Laparoscopic versus open inguinal spermatic vessel ligation in infertile men with varicocele. Shuang Liu, Chuanyi Hu *, Ning
Chapter 5 Treatment Modalities
 Chapter 5 Treatment Modalities In this chapter, we discuss the therapeutic modalities that have been applied to the treatment of varicocele, including medical therapy, surgical repair and embolization
Chapter 5 Treatment Modalities In this chapter, we discuss the therapeutic modalities that have been applied to the treatment of varicocele, including medical therapy, surgical repair and embolization
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Varicocele: surgical techniques in 2005
 Daniel H. Williams, MD, Edward Karpman, MD, Larry I. Lipshultz, MD Department of Urology, Baylor College of Medicine, Houston, Texas, USA WILLIAMS DH, KARPMAN E, LIPSHULTZ LI. Varicocele: surgical techniques
Daniel H. Williams, MD, Edward Karpman, MD, Larry I. Lipshultz, MD Department of Urology, Baylor College of Medicine, Houston, Texas, USA WILLIAMS DH, KARPMAN E, LIPSHULTZ LI. Varicocele: surgical techniques
M. Al-Mohtaseb. Tala Saleh. Faisal Nimri
 4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
Original Research Article
 Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
The Varicocele as Related to Fertility
 The Varicocele as Related to Fertility JORDAN S. BROWN, M.D., LAWRENCE DUBIN, M.D., and ROBERT S. HOTCHKISS, M.D. VARICOCELECTOMY in the subfertile male, where indication for this procedure exists, has
The Varicocele as Related to Fertility JORDAN S. BROWN, M.D., LAWRENCE DUBIN, M.D., and ROBERT S. HOTCHKISS, M.D. VARICOCELECTOMY in the subfertile male, where indication for this procedure exists, has
حسام أبو عوض. -Dr. Mohammad Muhtasib. 1 P a g e
 5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Chapter 4 Varicocele Classification
 Chapter 4 Varicocele Classification In this chapter, we examine the several classification modes have been used to diagnose and grade varicocele, including physical exam, venographic examination, color
Chapter 4 Varicocele Classification In this chapter, we examine the several classification modes have been used to diagnose and grade varicocele, including physical exam, venographic examination, color
OPEN APPROACH VERSUS MINIMALLY APPROACH FOR THE TREATMENT OF VARICOCELE IN CHILDREN - AN EPIDEMIOLOGICAL STUDY
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 1 PREVENTIVE MEDICINE - LABORATORY ORIGINAL PAPERS OPEN APPROACH VERSUS MINIMALLY APPROACH FOR THE TREATMENT OF VARICOCELE IN CHILDREN - AN EPIDEMIOLOGICAL
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 1 PREVENTIVE MEDICINE - LABORATORY ORIGINAL PAPERS OPEN APPROACH VERSUS MINIMALLY APPROACH FOR THE TREATMENT OF VARICOCELE IN CHILDREN - AN EPIDEMIOLOGICAL
Advantages of microsurgical varicocelectomy over conventional techniques
 European Review for Medical and Pharmacological Sciences Advantages of microsurgical varicocelectomy over conventional techniques B. PAJOVIC, N. RADOJEVIC, A. DIMITROVSKI 1, M. RADOVIC 2, R. ROLOVIC, M.
European Review for Medical and Pharmacological Sciences Advantages of microsurgical varicocelectomy over conventional techniques B. PAJOVIC, N. RADOJEVIC, A. DIMITROVSKI 1, M. RADOVIC 2, R. ROLOVIC, M.
Does the duration of infertility affect semen parameters and pregnancy rate after varicocelectomy? A retrospective study
 Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Evaluation of the role of varicocelectomy including external spermatic vein ligation in patients with scrotal pain
 Blackwell Science, LtdOxford, UKIJUInternational Journal of Urology0919-81722005 Blackwell Publishing Asia Pty LtdApril 2005124484488Original ArticleRole of varicocelectomy for paink Karademir et al. International
Blackwell Science, LtdOxford, UKIJUInternational Journal of Urology0919-81722005 Blackwell Publishing Asia Pty LtdApril 2005124484488Original ArticleRole of varicocelectomy for paink Karademir et al. International
Surgery Illustrated Surgical Atlas Inguinal orchidectomy for testicular cancer
 Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
The management of varicoceles by microdissection of the spermatic cord at the external inguinal ring
 FERTILITY AND STERILITY Copyright 1985 The American Fertility Society Printed in U.8A. The management of varicoceles by microdissection of the spermatic cord at the external inguinal ring Joel L. Marmar,
FERTILITY AND STERILITY Copyright 1985 The American Fertility Society Printed in U.8A. The management of varicoceles by microdissection of the spermatic cord at the external inguinal ring Joel L. Marmar,
Inguinal Canal. It is an oblique passage through the lower part of the anterior abdominal wall. Present in both sexes
 Inguinal canal Inguinal Canal It is an oblique passage through the lower part of the anterior abdominal wall Present in both sexes It allows structures to pass to and from the testis to the abdomen in
Inguinal canal Inguinal Canal It is an oblique passage through the lower part of the anterior abdominal wall Present in both sexes It allows structures to pass to and from the testis to the abdomen in
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
The role of animal models in the study of varicocele
 Review Article The role of animal models in the study of varicocele Matthew J. Katz, Bobby B. Najari, Philip S. Li, Marc Goldstein Department of Urology, Weill Cornell Medical College, New York, NY, USA
Review Article The role of animal models in the study of varicocele Matthew J. Katz, Bobby B. Najari, Philip S. Li, Marc Goldstein Department of Urology, Weill Cornell Medical College, New York, NY, USA
COMPARATIVE STUDY OF LAPAROSCOPIC VARICOCELE LIGATION VERSUS INGUINAL VARICOCELECTOMY
 International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article COMPARATIVE STUDY OF LAPAROSCOPIC VARICOCELE
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article COMPARATIVE STUDY OF LAPAROSCOPIC VARICOCELE
Shunt-type and stop-type varicocele in adolescents: prognostic value of these two different hemodynamic patterns
 Shunt-type and stop-type varicocele in adolescents: prognostic value of these two different hemodynamic patterns Mohammad Javad Mohseni, M.D., Hamid Nazari, M.D., Erfan Amini, M.D., Niloufar Javan-Farazmand,
Shunt-type and stop-type varicocele in adolescents: prognostic value of these two different hemodynamic patterns Mohammad Javad Mohseni, M.D., Hamid Nazari, M.D., Erfan Amini, M.D., Niloufar Javan-Farazmand,
DEFINITION HX & PH/EX
 DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
أحمد رواجبة- محمود الحربي- أحمد السالمان-
 -6 أحمد رواجبة- محمود الحربي- أحمد السالمان- 1 P a g e The Male Reproductive System The male genital system structures are divided into: Internal structures: 1- Prostate 3-Ejaculatory ducts External structures:
-6 أحمد رواجبة- محمود الحربي- أحمد السالمان- 1 P a g e The Male Reproductive System The male genital system structures are divided into: Internal structures: 1- Prostate 3-Ejaculatory ducts External structures:
MALE FACTOR. Gerald J. Matthews, M.D.,* Ellen Dakin Matthews, R.N., and Marc Goldstein, M.D.*
 FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
FERTILITY AND STERILITY VOL. 70, NO. 1, JULY 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. MALE FACTOR Induction
How-To Booklet: Pediatric Spay-Neuter. Surgical Techniques Pictorial
 How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
Male Infertility Caused by Varicoceles
 What You Need to Know About Male Infertility Caused by Varicoceles INTERVENTIONAL RADIOLOGY Find us on www.sirweb.org Q&A Questions and Answers About Male Infertility Caused by Varicoceles Q. What is a
What You Need to Know About Male Infertility Caused by Varicoceles INTERVENTIONAL RADIOLOGY Find us on www.sirweb.org Q&A Questions and Answers About Male Infertility Caused by Varicoceles Q. What is a
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 5 CBULP 2011 021 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 5 CBULP 2011 021 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Applied Anatomic Study of Testicular Veins in Adult Cadavers and in Human Fetuses
 Clinical Urology Anatomy of Testicular Veins in Adults and Human Fetuses International Braz J Urol Vol. 33 (2): 176-180, March - April, 2007 Applied Anatomic Study of Testicular Veins in Adult Cadavers
Clinical Urology Anatomy of Testicular Veins in Adults and Human Fetuses International Braz J Urol Vol. 33 (2): 176-180, March - April, 2007 Applied Anatomic Study of Testicular Veins in Adult Cadavers
Undescended Testicle
 What is the normal descending testis? The testicle begins to form just before the second fetal month and starts to look like a testicle around the fourth fetal month. By then it has migrated down from
What is the normal descending testis? The testicle begins to form just before the second fetal month and starts to look like a testicle around the fourth fetal month. By then it has migrated down from
Inguinal and Femoral Hernias. August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center
 Inguinal and Femoral Hernias August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center Background Approximately 20 million groin hernias are repaired each
Inguinal and Femoral Hernias August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center Background Approximately 20 million groin hernias are repaired each
Iliac vein compression cause of varicocele. syndrome: An unusual
 Iliac vein compression cause of varicocele syndrome: An unusual M. David Bomalaski, MD, Joseph L. Mills, MD, Luis R. Argueso, MD, Roy M. Fujitani, MD, Alvin L. Sago, MD, and Allen E. Joseph, MD, Lackland
Iliac vein compression cause of varicocele syndrome: An unusual M. David Bomalaski, MD, Joseph L. Mills, MD, Luis R. Argueso, MD, Roy M. Fujitani, MD, Alvin L. Sago, MD, and Allen E. Joseph, MD, Lackland
The Acute Scrotum: Sonographic Findings
 The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes
 Advances in Urology Volume 2013, Article ID 370969, 4 pages http://dx.doi.org/10.1155/2013/370969 Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes Mustafa
Advances in Urology Volume 2013, Article ID 370969, 4 pages http://dx.doi.org/10.1155/2013/370969 Clinical Study Influence of Preoperative Pain Duration on Microsurgical Varicocelectomy Outcomes Mustafa
Effect of female partner age on pregnancy rates after vasectomy reversal
 MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
MALE FACTOR Effect of female partner age on pregnancy rates after vasectomy reversal Edward R. Gerrard, Jr., M.D., a Jay I. Sandlow, b Robert A. Oster, Ph.D., c John R. Burns, M.D., a Lyndon C. Box, M.D.,
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Phil V. Bach, Bobby B. Najari, Marc Goldstein
 REVIEW Varicocele a case for early intervention [version 1; referees: 3 approved] Phil V. Bach, Bobby B. Najari, Marc Goldstein Weill Cornell Medical College, New York, NY, 10065, USA v1 First published:
REVIEW Varicocele a case for early intervention [version 1; referees: 3 approved] Phil V. Bach, Bobby B. Najari, Marc Goldstein Weill Cornell Medical College, New York, NY, 10065, USA v1 First published:
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
BENIGN & MALIGNANT TESTIS DISEASES. Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES
 BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Microsurgical Management of the Infertile Male
 Microsurgical Management of the Infertile Male a report by Jonathan D Schiff, MD and Natan Bar-Chama, MD Assistant Clinical Professor of Urology and Associate Professor of Urology, Obstetrics/Gynecology
Microsurgical Management of the Infertile Male a report by Jonathan D Schiff, MD and Natan Bar-Chama, MD Assistant Clinical Professor of Urology and Associate Professor of Urology, Obstetrics/Gynecology
Original Article Clinical effect of microscopic subinguinal varicocelectomy or bypass surgery on nutcracker phenomenon-associated varicocele
 Int J Clin Exp Med 2018;11(12):13750-13756 www.ijcem.com /ISSN:1940-5901/IJCEM0080040 Original Article Clinical effect of microscopic subinguinal varicocelectomy or bypass surgery on nutcracker phenomenon-associated
Int J Clin Exp Med 2018;11(12):13750-13756 www.ijcem.com /ISSN:1940-5901/IJCEM0080040 Original Article Clinical effect of microscopic subinguinal varicocelectomy or bypass surgery on nutcracker phenomenon-associated
THE PATIENT S GUIDE TO VASECTOMY REVERSAL
 The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
Infertility is a common problem in the urologic practice. Surgical Management of Male Infertility. Chapter Contents
 6 Surgical Management of Male Infertility Sandro C Esteves, Alaa Hamada, Ashok Agarwal Chapter Contents Surgical Treatment to Improve Sperm Production Reconstructive Surgeries of Ductal System Ejaculatory
6 Surgical Management of Male Infertility Sandro C Esteves, Alaa Hamada, Ashok Agarwal Chapter Contents Surgical Treatment to Improve Sperm Production Reconstructive Surgeries of Ductal System Ejaculatory
Surgical Approach and Occlusion of the Vasa
 From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth 5 Surgical Approach and Occlusion of the Vasa A lthough the no-scalpel technique is almost bloodless, an
From No-Scalpel Vasectomy: An Illustrated Guide for Surgeons, Third Edition 2003 EngenderHealth 5 Surgical Approach and Occlusion of the Vasa A lthough the no-scalpel technique is almost bloodless, an
Varicocele repair for infertility: what is the evidence?
 REVIEW C URRENT OPINION Varicocele repair for infertility: what is the evidence? Vincenzo Ficarra a, Alessandro Crestani a, Giacomo Novara a, and Vincenzo Mirone b Purpose of review Considering the persistent
REVIEW C URRENT OPINION Varicocele repair for infertility: what is the evidence? Vincenzo Ficarra a, Alessandro Crestani a, Giacomo Novara a, and Vincenzo Mirone b Purpose of review Considering the persistent
The Role of Testicular Volume in Adolescents With Varicocele: The Better Way and Time of Surgical Treatment
 The Role of Testicular Volume in Adolescents With Varicocele: The Better Way and Time of Surgical Treatment Claudio Spinelli, Martina Di Giacomo, Roberto Lo Piccolo, Alessandra Martin and Antonio Messineo
The Role of Testicular Volume in Adolescents With Varicocele: The Better Way and Time of Surgical Treatment Claudio Spinelli, Martina Di Giacomo, Roberto Lo Piccolo, Alessandra Martin and Antonio Messineo
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
I would be happy to discuss all of these options for fertility after vasectomy with you at the time of our consultation or over the phone.
 F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
Lymphatic and testicular artery-sparing laparoscopic varicocelectomy in children and adolescents Abdelaziz Yehya
 Original article 1 Lymphatic and testicular artery-sparing laparoscopic varicocelectomy in children and adolescents Abdelaziz Yehya Al-Azhar University Hospitals, Cairo, Egypt Correspondence to Abdelaziz
Original article 1 Lymphatic and testicular artery-sparing laparoscopic varicocelectomy in children and adolescents Abdelaziz Yehya Al-Azhar University Hospitals, Cairo, Egypt Correspondence to Abdelaziz
Transurethral Resection of Ejaculatory Duct Obstruction: Monopolar, Bipolar or Holmium Laser?
 Transurethral Resection of Ejaculatory Duct Obstruction: Monopolar, Bipolar or Holmium Laser? Selahittin Çayan, MD, FECSM Professor of Urology University of Mersin School of Medicine, Department of Urology,
Transurethral Resection of Ejaculatory Duct Obstruction: Monopolar, Bipolar or Holmium Laser? Selahittin Çayan, MD, FECSM Professor of Urology University of Mersin School of Medicine, Department of Urology,
Concomitant Varicocelectomy and Jaboulay's Operation
 Concomitant Varicocelectomy and Jaboulay's Operation Ali Hamdan Alkinany Haider Mahdy Alaaridhy* College of Medicine, University of Al-Qadisiah, Iraq. *College of Medicine, University of Al-Kufa, Iraq.
Concomitant Varicocelectomy and Jaboulay's Operation Ali Hamdan Alkinany Haider Mahdy Alaaridhy* College of Medicine, University of Al-Qadisiah, Iraq. *College of Medicine, University of Al-Kufa, Iraq.
PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY
 ADULT UROLOGY PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY G. NABI, S. ASTERLINGS, D. R. GREENE, AND R. L. MARSH ABSTRACT Objectives. To assess
ADULT UROLOGY PERCUTANEOUS EMBOLIZATION OF VARICOCELES: OUTCOMES AND CORRELATION OF SEMEN IMPROVEMENT WITH PREGNANCY G. NABI, S. ASTERLINGS, D. R. GREENE, AND R. L. MARSH ABSTRACT Objectives. To assess
Lindsay Machan, MD University of British Columbia Vancouver, British Columbia
 Varicocele Embolization and Serum Testosterone: What is the Evidence? Lindsay Machan, MD University of British Columbia Vancouver, British Columbia Lindsay Machan, MD, FSIR Stock: A4L, Calgary Scientific,
Varicocele Embolization and Serum Testosterone: What is the Evidence? Lindsay Machan, MD University of British Columbia Vancouver, British Columbia Lindsay Machan, MD, FSIR Stock: A4L, Calgary Scientific,
Surgical Sperm Retrieval
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Downloaded from journal.gums.ac.ir at 3:01 IRST on Sunday February 17th 2019
 (Ph.D) (M.D) (M.D) - : * gh.mokhtari@yahoo.com : /// : (M.D) * //: % " : ". : : (n=)... (%/) : (/%). (p
(Ph.D) (M.D) (M.D) - : * gh.mokhtari@yahoo.com : /// : (M.D) * //: % " : ". : : (n=)... (%/) : (/%). (p
Review Article The Onstep Method for Inguinal Hernia Repair: Operative Technique and Technical Tips
 Surgery Research and Practice Volume 2016, Article ID 6935167, 7 pages http://dx.doi.org/10.1155/2016/6935167 Review Article The Onstep Method for Inguinal Hernia Repair: Operative Technique and Technical
Surgery Research and Practice Volume 2016, Article ID 6935167, 7 pages http://dx.doi.org/10.1155/2016/6935167 Review Article The Onstep Method for Inguinal Hernia Repair: Operative Technique and Technical
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
Alternate indications for varicocele repair: non-obstructive azoospermia, pain, androgen deficiency and progressive testicular dysfunction
 Alternate indications for varicocele repair: non-obstructive azoospermia, pain, androgen deficiency and progressive testicular dysfunction Peter N. Schlegel, M.D., and Marc Goldstein, M.D. Department of
Alternate indications for varicocele repair: non-obstructive azoospermia, pain, androgen deficiency and progressive testicular dysfunction Peter N. Schlegel, M.D., and Marc Goldstein, M.D. Department of
Microscopic varicocelectomy as a treatment option for patients with severe oligospermia
 Original Article - Sexual Dysfunction/Infertility pissn 2466-0493 eissn 2466-054X Microscopic varicocelectomy as a treatment option for patients with severe oligospermia Chirag Gupta 1, Arun Chinchole
Original Article - Sexual Dysfunction/Infertility pissn 2466-0493 eissn 2466-054X Microscopic varicocelectomy as a treatment option for patients with severe oligospermia Chirag Gupta 1, Arun Chinchole
EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY
 Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Comparison of Open and Laparoscopic Varicocelectomies in Terms of Operative Time, Sperm Parameters, and Complications
 Laparoscopic Urology Comparison of Open and Laparoscopic Varicocelectomies in Terms of Operative Time, Sperm Parameters, and Complications Ali Shamsa, Leila Mohammadi, Mehran Abolbashari, Mohammad-Taghi
Laparoscopic Urology Comparison of Open and Laparoscopic Varicocelectomies in Terms of Operative Time, Sperm Parameters, and Complications Ali Shamsa, Leila Mohammadi, Mehran Abolbashari, Mohammad-Taghi
Preoperative Consultation
 Easy Vasectomy Reversal A vasectomy reversal is a microsurgical procedure that reconnects the vas deferens where it was interrupted by a vasectomy. Although vasectomy has historically been considered a
Easy Vasectomy Reversal A vasectomy reversal is a microsurgical procedure that reconnects the vas deferens where it was interrupted by a vasectomy. Although vasectomy has historically been considered a
Clinical Characteristics and Surgical Outcomes in Adolescents and Adults with Varicocele
 www.kjurology.org DOI:10.4111/kju.2011.52.7.489 Pediatric Urology Clinical Characteristics and Surgical Outcomes in and with Varicocele Hun Joo Lee, Sang Hyeon Cheon, Young Hwan Ji, Kyung Hyun Moon, Kun
www.kjurology.org DOI:10.4111/kju.2011.52.7.489 Pediatric Urology Clinical Characteristics and Surgical Outcomes in and with Varicocele Hun Joo Lee, Sang Hyeon Cheon, Young Hwan Ji, Kyung Hyun Moon, Kun
2. List the 8 pelvic spaces: list one procedure or dissection which involves entering that space.
 Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
Name: Anatomy Quiz: Pre / Post 1. In making a pfannensteil incision you would traverse through the following layers: a) Skin, Camper s fascia, Scarpa s fascia, external oblique aponeurosis, internal oblique
Evaluation of Varicocele Frequency in Adolescents in the City of Isfahan
 Original Article Evaluation of Varicocele Frequency in Adolescents in the City of Isfahan Homayoun Abbasi, M.D. 1, 2, Amir Ghanbarian, M.D. 3, Saeid Salimi Khoozani, M.D. 1, Mohammad Hossein Nasr Esfahani,
Original Article Evaluation of Varicocele Frequency in Adolescents in the City of Isfahan Homayoun Abbasi, M.D. 1, 2, Amir Ghanbarian, M.D. 3, Saeid Salimi Khoozani, M.D. 1, Mohammad Hossein Nasr Esfahani,
This review is based on the complete
 V O L U M E 6 6. N. 4. D I C E M B R E 2 0 1 4 REVIEWS MINERVA UROL NEFROL 2014;66:257-82 Pathophysiology, diagnosis and treatment of varicoceles: a review P. VANLANGENHOVE 1, E. DHONDT 1, K. EVERAERT
V O L U M E 6 6. N. 4. D I C E M B R E 2 0 1 4 REVIEWS MINERVA UROL NEFROL 2014;66:257-82 Pathophysiology, diagnosis and treatment of varicoceles: a review P. VANLANGENHOVE 1, E. DHONDT 1, K. EVERAERT
VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD
 Nagoya J. Med. Sci. 49. 53-59, 1987 VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD KOJI MIYAKE, MASANORI YAMAMOTO and HIDEO MITSUYA Department of Urology, Nagoya University
Nagoya J. Med. Sci. 49. 53-59, 1987 VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD KOJI MIYAKE, MASANORI YAMAMOTO and HIDEO MITSUYA Department of Urology, Nagoya University
Vikram Dogra, M.D. Professor of Radiology, Urology & BME Department of Imaging Sciences University Of Rochester Medical Center
 Ultrasound of the Scrotum Vikram Dogra, M.D. Professor of Radiology, Urology & BME Department of Imaging Sciences University Of Rochester Medical Center Etiologies of Acute Scrotal Pain Epididymitis/Orchitis
Ultrasound of the Scrotum Vikram Dogra, M.D. Professor of Radiology, Urology & BME Department of Imaging Sciences University Of Rochester Medical Center Etiologies of Acute Scrotal Pain Epididymitis/Orchitis
The significance of clinical practice guidelines on adult varicocele detection and management
 (2016) 18, 269 275 2016 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access INVITED REVIEW The significance of clinical practice guidelines
(2016) 18, 269 275 2016 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access INVITED REVIEW The significance of clinical practice guidelines
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
Chapter 8 Effect of Varicocele Treatment
 Chapter 8 Effect of Varicocele Treatment Although multiple pathophysiological derangements have been documented in varicocele, the central issue is whether or not repair of this condition improves fertility.
Chapter 8 Effect of Varicocele Treatment Although multiple pathophysiological derangements have been documented in varicocele, the central issue is whether or not repair of this condition improves fertility.
Varıcocele among healthy young men in Turkey; prevalence and relationship wıth body mass index
 ORIGINal ARTICLE Vol. 38 (1): 116-121, January - February, 2012 Varıcocele among healthy young men in Turkey; prevalence and relationship wıth body mass index Haluk Soylemez, Murat Atar, Ahmet Ali Sancaktutar,
ORIGINal ARTICLE Vol. 38 (1): 116-121, January - February, 2012 Varıcocele among healthy young men in Turkey; prevalence and relationship wıth body mass index Haluk Soylemez, Murat Atar, Ahmet Ali Sancaktutar,
Ultrasonographic diagnosis of varicoceles
 FERTILITY AND STERILITY Copyright 1993 The American Fertility Society Vol. 60, No, 4, October 1993 Printed on acid-free paper in U. S. A. Ultrasonographic diagnosis of varicoceles L. Andrew Eskew, M,D,*
FERTILITY AND STERILITY Copyright 1993 The American Fertility Society Vol. 60, No, 4, October 1993 Printed on acid-free paper in U. S. A. Ultrasonographic diagnosis of varicoceles L. Andrew Eskew, M,D,*
The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
 pissn: 2287-4208 / eissn: 2287-490 World J Mens Health 2014 April 32(1): 5-0 http://dx.doi.org/10.5534/wjmh.2014.32.1.5 Original Article The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
pissn: 2287-4208 / eissn: 2287-490 World J Mens Health 2014 April 32(1): 5-0 http://dx.doi.org/10.5534/wjmh.2014.32.1.5 Original Article The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
Does the number of veins ligated during microsurgical subinguinal varicocelectomy impact improvement in pain post-surgery?
 Original Article Does the number of veins ligated during microsurgical subinguinal varicocelectomy impact improvement in pain post-surgery? Haitham Elbardisi 1, Ashok Agarwal 2, Ahmad Majzoub 1, Sami Al
Original Article Does the number of veins ligated during microsurgical subinguinal varicocelectomy impact improvement in pain post-surgery? Haitham Elbardisi 1, Ashok Agarwal 2, Ahmad Majzoub 1, Sami Al
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
COMPARATIVE STUDY BETWEEN THE OUTCOME OF LAPAROSCOPIC PALOMO AND OPEN INGUINAL VARICOCELECTOMY
 COMPARATIVE STUDY BETWEEN THE OUTCOME OF LAPAROSCOPIC PALOMO AND OPEN INGUINAL VARICOCELECTOMY KARMAKER U 1, ALAM SMM 2, CHOWDHURY MSA 3, RAHMAN MM 4, ISLAM MN 5, RAHMAN MM 6, SAHA PK 7 Abstract: Background:
COMPARATIVE STUDY BETWEEN THE OUTCOME OF LAPAROSCOPIC PALOMO AND OPEN INGUINAL VARICOCELECTOMY KARMAKER U 1, ALAM SMM 2, CHOWDHURY MSA 3, RAHMAN MM 4, ISLAM MN 5, RAHMAN MM 6, SAHA PK 7 Abstract: Background:
CHILD HYDROCELE OPERATION. COPYRIGHT M.H.EDWARDS 2005 FILE NAME SW-CHHY OPERATION NO 037 SURGEON... Last updated
 CHILD HYDROCELE OPERATION COPYRIGHT M.H.EDWARDS 2005 FILE NAME SW-CHHY OPERATION NO 037 SURGEON... Last updated 30 12 05 CHILD HYDROCELE OPERATION GRADE 4 (SEVERE) THESE S COVER MALE PATIENT LESS THAN
CHILD HYDROCELE OPERATION COPYRIGHT M.H.EDWARDS 2005 FILE NAME SW-CHHY OPERATION NO 037 SURGEON... Last updated 30 12 05 CHILD HYDROCELE OPERATION GRADE 4 (SEVERE) THESE S COVER MALE PATIENT LESS THAN
Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen Analysis
 African Journal of Urology 1110-5704 Vol. 17, No. 4, 2011 115-121 Original article Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen
African Journal of Urology 1110-5704 Vol. 17, No. 4, 2011 115-121 Original article Spontaneous Pregnancy Outcome after Surgical Repair of Clinically Palpable Varicocele in Young Men with Abnormal Semen
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update
 Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
Induction of spermatogenesis in azoospermic men after varicocelectomy repair: an update Fábio Firmbach Pasqualotto, M.D., Ph.D., Bernardo Passos Sobreiro, M.D., Jorge Hallak, M.D., Ph.D., Eleonora Bedin
THE INS AND OUTS OF HERNIAS WHERE TO START? WHAT IS A HERNIA? CLINICAL INDICATIONS THE INGUINAL CANAL THE CLINICAL QUESTION 18/09/2018
 THE INS AND OUTS OF HERNIAS Cassandra Harrison BA/BSc, MMRU, AMS WHERE TO START? The Clinical Question Essential anatomy Inguinal hernia Scanning technique Variations WHAT IS A HERNIA? CLINICAL INDICATIONS
THE INS AND OUTS OF HERNIAS Cassandra Harrison BA/BSc, MMRU, AMS WHERE TO START? The Clinical Question Essential anatomy Inguinal hernia Scanning technique Variations WHAT IS A HERNIA? CLINICAL INDICATIONS
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Chapter 9. Summary & conclusion
 Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Ultrapro Hernia System Bi Layer Dr Cosmas Gora T SpB-KBD. dffdfdfxxgfxgfxgffxgxgxg
 Bi Layer Dr Cosmas Gora T SpB-KBD dffdfdfxxgfxgfxgffxgxgxg Why UHS? Lightweight Mesh Covering entire myopectineal orifices with underlay mesh in preperitoneal space (posterior repair) Covering the inguinal
Bi Layer Dr Cosmas Gora T SpB-KBD dffdfdfxxgfxgfxgffxgxgxg Why UHS? Lightweight Mesh Covering entire myopectineal orifices with underlay mesh in preperitoneal space (posterior repair) Covering the inguinal
