Bilateral endoscopic totally extraperitoneal (TEP) inguinal hernia repair does not impair male fertility
|
|
|
- Milton Allan Clark
- 6 years ago
- Views:
Transcription
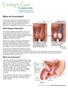
1 Hernia (2017) 21: ORIGINAL ARTICLE Bilateral endoscopic totally extraperitoneal (TEP) inguinal hernia repair does not impair male fertility M. M. Roos 1 G. J. Clevers 1 E. J. Verleisdonk 1 P. H. Davids 1 C. van de Water 2 R. J. Spermon 3 L. S. Mulder 4 J. P. J. Burgmans 1 Received: 27 March 2017 / Accepted: 20 August 2017 / Published online: 29 August 2017 Springer-Verlag France SAS 2017 Abstract Purpose Endoscopic totally extraperitoneal (TEP) hernia repair with polypropylene mesh has become a well-established technique. However, since the mesh is placed in close contact with the spermatic cord, mesh-induced inflammation may affect its structures, possibly resulting in impaired fertility. The aim of this observational prospective cohort study was to assess fertility after bilateral endoscopic TEP inguinal hernia repair in male patients. Methods Fifty-seven male patients (22 60 years old) with primary, reducible, bilateral inguinal hernias underwent elective bilateral endoscopic TEP hernia repair with use of polypropylene mesh. The primary outcome was testicular perfusion; secondary outcomes were testicular volume, endocrinological status, and semen quality. All patients were assessed preoperatively and 6 months postoperatively. Results Follow-up was completed in 44 patients. No statistically significant differences in measurements of testicular blood flow parameters or testicular volume were found. Postoperative LH levels were significantly higher [preoperative median 4.3 IU/L (IQR ) versus postoperative median 5.0 IU/L (IQR ), p = 0.03]. Levels of inhibin B were significantly lower postoperatively [preoperative * M. M. Roos mroos@diakhuis.nl 1 Department of Surgery/Hernia Clinic, Diakonessenhuis Utrecht/Zeist, Utrecht, The Netherlands 2 3 Department of Clinical Chemistry, Diakonessenhuis Utrecht/Zeist, Utrecht, The Netherlands Department of Urology, Diakonessenhuis Utrecht/Zeist, Utrecht, The Netherlands 4 Department of Radiology, Diakonessenhuis Utrecht/Zeist, Utrecht, The Netherlands median ng/l (IQR ) versus postoperative median 27.0 ng/l (IQR ), p = 0.01]. No significant changes in FSH or testosterone levels were observed. There were no differences in semen quality. Conclusions Our data suggest that bilateral endoscopic TEP hernia repair with polypropylene mesh does not impair fertility, as no differences in testicular blood flow, testicular volume, or semen quality were observed. Postoperative levels of LH and inhibin B differed significantly from preoperative measurements, yet no clinical relevance could be ascribed to these findings. Keywords Inguinal hernia Bilateral Endoscopic TEP Fertility Introduction Inguinal hernia repair is the most commonly performed general surgical procedure worldwide, with a lifetime risk of developing an inguinal hernia of 27% for men and 3% for women [1]. There has been a considerable reduction in recurrence rates since the introduction of tension-free mesh repair, which has now become standard practice [2]. Endoscopic totally extraperitoneal (TEP) hernia repair, based on the concept of strengthening the weak inguinal floor by reducing the sac and placing preperitoneal mesh, has become increasingly popular, since this approach provides faster recovery and a lower incidence of postoperative (chronic) pain compared to open techniques [3 5]. Hypothetically, mesh-induced fibrosis or direct iatrogenic damage may affect the structures of the spermatic cord and impair testicular function and fertility. Rare but potentially harmful complications that may occur after hernia surgery include ischemic orchitis, testicular atrophy, or obstructive Vol.:( )
2 888 Hernia (2017) 21: azoospermia [6]. Several experimental animal studies and case reports have described patients with these complications after open hernia repair with implantation of polypropylene mesh [7 10]. A systematic review on male infertility following inguinal hernia repair was recently conducted; however, the majority of procedures were open (99.5%) and unilateral (>80%) [11]. Men undergoing bilateral mesh hernia repair or unilateral hernia repair with pre-existing impairment of the contralateral testis are considered to be at greatest risk of fertility impairment, but relevant large and prospective clinical trials on endoscopic bilateral hernia repair are lacking. The objective of this study was to evaluate the effect of endoscopic bilateral TEP inguinal hernia repair on male fertility by analyzing testicular perfusion and volume, semen analysis, and endocrinological status. Patients and methods Patients This observational, prospective study was conducted on male patients (22 60 years old) with primary bilateral inguinal hernias at the Department of Surgery in a high-volume hospital in the Netherlands specialized in the TEP technique for inguinal hernia repair (Diakonessenhuis Utrecht/Zeist). The aim of this study was to evaluate male fertility preoperatively and 6 months after bilateral TEP inguinal hernia surgery. The study was approved by the regional Medical Ethics Committee (VCMO, Nieuwegein, The Netherlands) and the hospital s Ethics Board, and it was registered in the Netherlands National Trial Registry (NTR2208). Written informed consent was obtained from all participants. Patients eligible for inclusion were men of fertile age (18 60 years old) with primary, bilateral inguinal hernias who were scheduled for elective endoscopic totally extraperitoneal (TEP) hernia repair. Patients with an ASA classification >III, recurrent and/or femoral/scrotal hernias, a medical history of testicular pathology, pelvic surgery or radiotherapy, known fertility problems, co-morbidity associated with possible fertility problems, and use of medication that might impair fertility were excluded from participation (Table 1). Participants were recruited at their first visit to the outpatient clinic and enrolled after signing informed consent. Preoperative patient data [age, medical history, smoking habit, and body mass index (BMI)] were obtained through measurements and a general questionnaire. Surgical procedure Patients underwent simultaneous bilateral endoscopic TEP inguinal hernia repair with use of a double-mesh implantation technique. The procedure was performed under general anesthesia. Two identical polypropylene meshes (Prolene, cm) were positioned in a tension-free manner in the preperitoneal space. The mesh graft was not fixed to avoid possible entrapment neuralgia. Nyhus classification, operative time, and intraoperative complications were recorded during surgery. Surgeons with extensive expertise in this procedure (>500 procedures per surgeon) performed all Table 1 Inclusion and exclusion criteria Inclusion criteria Male gender Age 18 and 60 years Primary, reducible inguinal hernias Bilateral hernias Eligible for TEP (and therefore for general anesthesia) Exclusion criteria Female gender Age 60 years Period of high fever prior to semen analysis Recurrent inguinal hernias Unilateral hernias Hydrocele and/or varicocele Femoral or scrotal hernia Incarcerated hernia ASA classification III Previous medical history of: Testicular infarction Testicular torsion Cryptorchidism Inguinal, scrotal, testicular or prostate surgery Vasectomy Radiotherapy of pelvic region Diabetes mellitus Cystic fibrosis Fertility problems and/or treatment, erection disorders or (other) problems in sexual function Use of gonadotropins Use of anabolic steroids TEP totally extraperitoneal, ASA american society of anesthesiologists
3 Hernia (2017) 21: operations. The operation and perioperative care did not differ from those of patients not participating in the study. Postoperative management and follow up Patients were discharged on the day of surgery, unless complications prohibited early discharge. Duration of hospital stay and postoperative complications were recorded. Patients were advised to take pain medication as needed (paracetamol, and if necessary, diclofenac) and to avoid strenuous physical activity (such as lifting and sports) during the first postoperative week. The routine follow-up schedule after TEP hernia repair in our center was followed: patients were followed-up by telephone 6 weeks after surgery and were scheduled for an additional visit to the outpatient clinic in case of complaints. Six months postoperatively, all participants visited the outpatient clinic for assessment of fertility parameters. Outcome measures Male fertility parameters were assessed preoperatively on the day of surgery and 6 months postoperatively by means of bilateral scrotal ultrasonography, semen analysis, and biochemical analysis. The primary outcome of this study was testicular perfusion, and secondary outcome measures were testicular volume, semen quality, and serum endocrinological status. Testicular perfusion and volume Bilateral testicular perfusion and volume were determined by measuring the blood flow velocity (cm/s) by color Doppler ultrasonography (CDUS) and gray-scale ultrasonography, respectively. Measurements were performed by experienced ultrasound technicians, who received specific instructions for the purpose of this study. The patient was placed in the supine position and the penis was held suprapubically. For testicular perfusion, blood flow was measured at four different points: the inguinal and extratesticular intrascrotal level of the testicular artery, the capsular arteries, and the intratesticular arteries. The parameters assessed were peak systolic velocity (PSV), end diastolic velocity (EDV), resistive index (RI), pulsatility index (PI), and acceleration time (ATA). To improve intraobserver reliability, each parameter was measured three different times and the mean value was calculated. Possible signs of distension of the epididymis and/or vas deferens, as well as formation of a thrombus in the pampiniform plexus, were also assessed. To determine testicular volume, length, width, and height were measured separately, and the ultrasonography device performed a volume calculation with these dimensions. Semen analysis 889 For semen analysis, seminal volume (ml), sperm concentration (10 6 cells/ml), motility (% progression), VCM (volume concentration progressive motility), and ph were analyzed. Semen was obtained in our hospital by means of masturbation after which the sample was analyzed within an hour. Patients were instructed to remain abstinent for 48 h so that reliable semen samples could be obtained. Biochemical analysis Endocrinological status was assessed by determining serum levels of luteinizing hormone (LH), follicle-stimulating hormone (FSH), and testosterone. Inhibin B serum level was also collected. Blood samples were obtained and analyzed in our hospital. Statistical analysis Statistical analyses were performed using SPSS version 23.0 (IBM Corp., Armonk, NY, USA). Differences in preoperative and postoperative fertility parameters were analyzed by means of the paired sample t-test (parametric data) or the Wilcoxon signed-rank test (non-parametric data). Comparison of preoperative and postoperative measurements of testicular perfusion and volume was done separately for the left and right testes. In case of a statistically significant difference in blood hormone levels, an additional calculation with the reference change value (RCV) formula was performed. The RCV formula incorporates analytical variation and intraindividual biological variation, and the difference in hormone level must exceed the RCV to be clinically significant [12]. A p value <0.05 was considered statistically significant. Results Fifty-seven consecutive patients were recruited and operated on between March 2010 and March 2016 (Table 2). The median age of the study population was 51 years (range years). One patient with a history of appendicitis complicated by abscess formation had multiple adhesions, leading to bladder perforation intraoperatively, which was managed conservatively with an indwelling catheter. Two patients were clinically diagnosed with a recurrent hernia and underwent an additional operation: one patient developed an early recurrence 5 days after surgery, the other recurrence was diagnosed 4 months after surgery. Two patients required an additional visit to the outpatient clinic due to pain. Ultrasonography showed postoperative hematomas in both patients, and the pain subsided with conservative
4 890 Hernia (2017) 21: Table 2 Patient and treatment characteristics (n = 57) Age (years) 51.0 ( ) BMI (kg/m 2 ) 24.7 ( ) ASA classification (%) I 77 II 23 Smoking (%) No 82 Yes 18 Type of hernia (%) Left, medial 54 Left, lateral 46 Right, medial 49 Right, lateral 51 Operation time (min) 28.0 ( ) Intraoperative complications (%) Bladder injury 2 Conversion rate (%) 0 Postoperative complications (%) Hematoma 4 Recurrence 4 Continuous data are presented as median (IQR) BMI body mass index, ASA american society of anesthesiologists treatment. No readmissions after discharge from the hospital were reported. In total, 44 patients (78.6%) completed the follow-up period of 6 months. One patient was excluded since he was not able to obtain semen preoperatively. One patient who was only experiencing symptoms in the right inguinal region requested a change to unilateral intervention hours before surgery. Eight of the patients withdrew their consent, and 3 of the patients could not be reached for follow-up, despite multiple attempts by telephone and . Testicular perfusion and volume There were no significant changes in PSV, EDV, RI, PI, and AT between pre- and postoperative measurements of testicular perfusion at all levels of both sides (Table 3). There was an increase in the PSV and EDV of the left intratesticular arteries from preoperative to postoperative assessment that trended towards significance. A thrombus in the right-sided pampiniform plexus was observed in 1 patient preoperatively and 3 patients postoperatively. None of the patients had a thrombus in the left pampiniform plexus on preoperative assessment; postoperatively, this finding was present in 3 patients. Analysis of bilateral testicular volume showed no significant differences between pre- and postoperative measurements. Endocrinological status Comparison of blood hormone values revealed higher LH levels postoperatively with a median value of 5.0 IU/L (IQR ) compared to 4.3 IU/L (IQR ) (Table 4). Both measurements were within the LH reference range of IU/L. There were no significant differences in FSH or testosterone levels. Levels of inhibin B were significantly lower postoperatively with a preoperative median of ng/l (IQR ) versus a postoperative median of ng/l (IQR ); both measurements were within the inhibin B reference range (<400 ng/l). Semen quality No statistically significant differences in semen volume, concentration, motility, VCM, or ph after bilateral TEP inguinal hernia repair were found (Table 4). Discussion The present study shows no impairment of fertility 6 months after bilateral endoscopic TEP inguinal hernia repair. Polypropylene, the biomaterial most commonly used in mesh hernia repair, has good mechanical stability and induces an acute inflammatory reaction followed by a chronic foreign body fibroblastic reaction, which is essential for optimal fixation and incorporation of the biomaterial in the abdominal wall [13]. During the TEP procedure, the mesh is placed in close contact with the vas deferens, testicular vessels, autonomic nerves, and fascia. Injuries to the vas deferens and/or spermatic vessels may be a result of direct iatrogenic injury by dissection of the preperitoneal space, or delayed obstruction caused by scar tissue from the mesh-induced inflammatory tissue response, which is part of the normal healing process [9, 14]. No significant differences in testicular perfusion or volume 6 months after bilateral mesh hernia repair were observed. Blood supply through the spermatic vessels was assessed in this study using CDUS, a well-documented procedure for investigating testicular vascularization and perfusion [15]. Due to interdependence of flow within an arterial network, the blood flow was measured on testicular, intracapsular, and intratesticular levels to avoid false normal results from partial measurements. On CDUS measurements, the RI and PI are used for interpretation of vascular resistance and tissue perfusion. When testicular perfusion is disrupted, a decrease in end diastolic pressure and an increase in RI and PI can be seen, with an elevated RI suggestive of ischemia [16]. While we did not find significant changes in blood flow parameters for left and right testicular perfusion, we did observe a trend
5 Hernia (2017) 21: Table 3 Testicular perfusion and volume (n = 44) Preoperative Postoperative p value Left Right Left Right Left Right Perfusion testicular artery (inguinal) PSV (cm/s) 15.5 ( ) 15.9 ( ) 15.5 ( ) 14.4 ( ) EDV (cm/s) 2.3 ( ) 2.4 ( ) 2.0 ( ) 2.5 ( ) RI 0.8 ( ) 0.8 ( ) 0.8 ( ) 0.8 ( ) PI 2.2 ( ) 2.6 ( ) 2.4 ( ) 2.5 ( ) AT (ms) ( ) ( ) ( ) ( ) Perfusion testicular artery (scrotal) PSV (cm/s) 12.2 ( ) 10.6 ( ) 11.1 ( ) 11.8 ( ) EDV (cm/s) 2.5 ( ) 2.3 ( ) 2.4 ( ) 2.6 ( ) RI 0.8 ( ) 0.8 ( ) 0.8 ( ) 0.8 ( ) PI 1.9 ( ) 1.8 ( ) 1.8 ( ) 1.9( ) AT (ms) 79.0 ( ) 80.0 ( ) 86.0 ( ) 76.3 ( ) Perfusion intracapsular arteries PSV (cm/s) 9.4 ( ) 9.2 ( ) 9.1 ( ) 10.0 ( ) EDV (cm/s) 3.1 ( ) 3.0 ( ) 2.9 ( ) 3.0 ( ) RI 0.7 ( ) 0.7 ( ) 0.7 ( ) 0.7 ( ) PI 1.4 ( ) 1.4 ( ) 1.4 ( ) 1.3 ( ) AT (ms) 53.0 ( ) 47.3 ( ) 49.1 ( ) 52.3 ( ) Perfusion intratesticular arteries PSV (cm/s) 6.7 ( ) 5.6 ( ) 7.7 ( ) 6.1 ( ) EDV (cm/s) 2.5 ( ) 2.4 ( ) 3.1 ( ) 2.4 ( ) RI 0.6 ( ) 0.6 ( ) 0.6 ( ) 0.6 ( ) PI 1.0 ( ) 1.1 ( ) 1.1 ( ) 1.1 ( ) AT (ms) 31.1 ( ) 24.0 ( ) 34.5( ) 25.9 ( ) Testicular volume (ml) 15.5 ( ) 16.5 ( ) 15.4 ( ) 17.4 ( ) Data are presented as median (IQR) PSV peak systolic velocity, EDV end diastolic velocity, RI resistive index, PI pulsatility index, AT acceleration time Table 4 Endocrinological status and semen analysis (n = 44) Preoperative Postoperative p value Endocrinological status LH (IU/L) 4.3 ( ) 5.0 ( ) 0.03 FSH (IU/L) 5.0 ( ) 5.0 ( ) 0.99 Testosterone (nmol/l) 15.1 ( ) 14.7 ( ) 0.14 Inhibin B (pg/ml) ( ) ( ) 0.01 Semen quality Volume (ml) 3.0 ( ) 3.0 ( ) 0.74 Concentration (10 6 cells/ml) 49.0 ( ) 39.0 ( ) 0.21 Motility (% progression) 41.5 ( ) 42.0 ( ) 0.86 VCM (10 6 ) 51.5 ( ) 28.5 ( ) 0.29 ph (mol/l) 7.7 ( ) 7.7 ( ) 0.87 Data are presented as median (IQR) LH luteinizing hormone, FSH follicle-stimulating hormone, VCM volume concentration progressive motility
6 892 Hernia (2017) 21: towards significance in higher PSV and EDV values of the left intratesticular arteries. However, RI and PI ratios calculated from the PSV and EDV were not significantly different, so we did not regard these differences as clinically relevant. Since the start of this study, several other studies have investigated the effect of endoscopic mesh hernia repair on testicular perfusion and volume [17 23]. Results of these studies may be divided into early postoperative (1 7 days after surgery) and late postoperative (3 months 3 years after surgery) categories. With respect to early postoperative results of testicular perfusion, Stula et al. demonstrated an increase in PSV at the testicular, capsular, and intratesticular level, and higher RI and PI ratios of the intratesticular artery 2 days after laparoscopic TAPP hernia repair, which normalized in the late postoperative period after 5 months [17]. While not statistically significant, Lal et al. demonstrated a trend of increased RI of testicular, capsular, and intratesticular arteries 1 day after laparoscopic TEP repair, which then decreased to preoperative values 7 days after surgery [18]. Ersin et al. noticed a significant decrease in RI of capsular and intratesticular arteries and an increase in PSV and EDV of the capsular artery on the first day postoperative that normalized 1 week after the operation [19]. In summary, the findings of these studies suggest only a transient change in testicular perfusion in the early postoperative period. The results might be influenced by hypervascularity and edema of the testes and epididymes, as these are known to occur in the early postoperative period. Thus, the short-term effects on perfusion appear to be a result of the operation itself rather than the fibroblastic tissue response, which would be expected to have more long-term effects. In concordance with our study, the studies that assessed testicular perfusion between 3 months and 3 years after mesh hernia repair did not find clinically relevant changes in the testicular blood supply [20 23]. Since interruption of the testicular blood supply may result in testicular atrophy, testicular volume was also taken into account. No significant differences in testicular volume were found in our study population. Akbulut et al. found a significant decrease in testicular volume after TEP hernia repair; however, postoperative testicular volume remained within normal limits, and this finding was not considered as testicular atrophy [24]. This study did not assess testicular perfusion. Thrombosis of the pampiniform plexus may result from overzealous dissection of the cord or excessive use of cauterization intraoperatively, or from pressure exerted by a large hematoma in the groin postoperatively [25]. Pampiniform plexus thrombosis may cause venous outflow obstruction and testicular infarction. Although a few patients had plexus pampiniformis thrombi on scrotal ultrasound, no testicular infarction was observed in our study population. In our opinion, it is more likely that these thrombi are the result of postoperative hematoma or are not even related to the surgical intervention. Six months postoperatively, significantly higher blood levels of LH and lower blood levels of Inhibin B were found. LH, also called interstitial cell-stimulating hormone in males, stimulates secretion of the steroid hormone testosterone by Leydig cells [24]. High levels of LH could indicate testicular dysfunction due to decreased testosterone production. In the case of low testosterone, hypothalamic secretion of GnRH and hypophysic secretion of LH and FSH would be stimulated to increase spermatogenesis. However, FSH was not increased in our study. Furthermore, when applying the reference change value (RCV) for LH, which takes biological and analytic variations between separate measurements into account, LH levels did not increase significantly. Inhibin B, secreted by the Sertoli cells, inhibits production of FSH, thereby leading to decreased spermatogenesis. However, levels of FSH did not differ significantly, and the RCV formula showed that the decrease in inhibin B was not significant. Taking these factors into consideration, we did not regard the isolated higher levels of LH and decreased levels of inhibin B as clinically relevant. Our findings on LH, FSH, and testosterone levels are in line with other studies that analyzed blood hormone levels after endoscopic inguinal hernia repair and did not find significant changes in endocrinological parameters in the early postoperative to 6 months postoperative period [18, 22, 24]. Inhibin B has, to our knowledge, not been investigated in this context before. Semen analysis can be used as a parameter for seminal tract patency or obstruction. No significant differences in semen volume, concentration, motility, or ph were found after TEP hernia repair. Several other studies performed semen analysis after endoscopic inguinal hernia repair [17, 21, 22, 26]. Only the study conducted by Peeters et al. found a significant decrease in one of the parameters assessed in semen [21]. In this trial, where quality of life and fertility analysis after laparoscopic inguinal hernia repair were compared between patients who received a lightweight (Vypro II, TiMesh) versus a heavyweight (Marlex) mesh, sperm motility was decreased at 1-year follow-up in the lightweight group. This decrease in sperm motility could not be confirmed in a long-term follow-up of 3 years [23]. The clinical relevance of this isolated decreased sperm motility is not entirely clear, as fertility depends on several factors and all other sperm parameters remained within normal limits. To our knowledge, this study represents the first clinical prospective trial assessing testicular perfusion and volume, semen quality, and endocrinological status after endoscopic TEP inguinal hernia repair in a human patient population comprised solely of bilateral hernia repairs. This study design ensured that a healthy contralateral side did not positively influence our results. More than 80% of
7 Hernia (2017) 21: studies that have been performed on male fertility after inguinal hernia repair consisted of unilateral repairs [11]. Studies involving bilateral inguinal hernia repairs often had mixed populations of uni- and bilateral hernias, did not involve TEP hernia repair, had relatively small numbers of patients, or measured different outcome parameters. Since we are an expertise TEP hernia center, our patient population involved only bilateral TEP hernia repairs, making our results not applicable to other frequently performed preperitoneal techniques. However, since clinical outcomes of laparoendoscopic techniques are similar, we do not expect differences in fertility outcomes between TEP and TAPP. In open preperitoneal operations such as TIPP and TREPP mesh placement and possible damage to the vas are theoretically comparable with laparoendoscopic techniques. However, long-term outcomes of these techniques have not been studied thoroughly and there is insufficient evidence to recommend these techniques for primary (bilateral) inguinal hernia repair. With regard to frequently performed open techniques with anterior mesh placement (Lichtenstein), we would like to recommend performing a study similar to ours. Even though studies evaluating fertility after Lichtenstein repair demonstrated good results with low rates of infertility-related complications, no prospective study had a patient population consisting of bilateral inguinal hernia repairs only [11]. A limitation of this study is the relatively small sample size and the high percentage of loss to follow-up. Participant enrollment was slow due to the fact that many patients had been previously sterilized or were not willing to participate due to the study needs (two times scrotal ultrasonography and collection of semen, additional visit to the hospital after surgery), therefore we closed the study prematurely after 6 years. However, the sample size that we initially calculated (76 patients) was based on 2 studies with very small patient numbers [27]. Also, the size of our patient population is comparable to the previously mentioned studies that assessed fertility. In this study, we did not assess early postoperative effects on fertility, therefore we may have missed significant changes in early testicular perfusion, semen quality, or endocrinological status that have been shown in other studies. However, we regard the long-term outcomes as clinically relevant, since the early postoperative effects can be attributed to the impact of the surgical intervention itself and its natural postoperative course. Since it is assumed that the mesh-related inflammatory reaction subsides after 6 months, we deliberately chose our follow-up period at this time point [28]. After this time interval it is not likely to expect any decrease of perfusion or other late-delayed complications impairing fertility. This is in accordance with the long-term follow-up study of Peeters et al., where no significant changes in testicular volume 893 or flow and no other fertility-related complications were reported until 3 years after TEP inguinal hernia repair [23]. In conclusion, the available data suggest that there are no clinically relevant long-term effects of endoscopic bilateral TEP hernia repair on fertility. Based on our current results, we think bilateral TEP inguinal hernia repair can be safely performed in men of fertile age. Author contributions MR: data collection, analysis and interpretation of data, drafting of manuscript. GJC: study conception and design, critical revision, EJV: study conception and design, critical revision. PD: study conception and design, critical revision. CW: study conception and design (clinical chemistry), interpretation of data (clinical chemistry), critical revision. RS: study conception and design (urology), interpretation of data (urology), critical revision. LSM: study conception and design (radiology), interpretation of data (radiology), critical revision. IB: study conception and design, drafting of manuscript, critical revision. Compliance with ethical standards Conflicts of interest The authors declare that they have no conflict of interests. Ethical approval Ethical approval was obtained by the Regional Medical Ethics Committee and the hospitals EthicsBoard. Human and animal rights This article does not contain any studies with human participants or animals performed by any of the authors. Informed consent References All subjects signed informed consent. 1. Simons MP, Aufenacker T, Bay-Nielsen M et al (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13(4): Bay-Nielsen M, Kehlet H, Strand L et al (2001) Quality assessment of herniorrhaphies in Denmark: a prospective nationwide study. Lancet 358(9288): Kehlet H (2008) Chronic pain after groin hernia repair. Br J Surg 95(2): Kuhry E, Van Veen RN, Langeveld HR et al (2007) Open or endoscopic total extraperitoneal inguinal hernia repair? A systematic review. Surg Endosc 21(2): O Reilly EA, Burke JP, O Connell PR (2012) A meta-analysis of surgical morbidity and recurrence after laparoscopic and open repair of primary unilateral hernia. Ann Surg 255(5): Fitzgibbons RJ (2005) Can we be sure polypropylene mesh causes infertility? Ann Surg 241(4): Maciel LC, Glina S, Palma PCR et al (2007) Histopathological alterations of the vas deferens in rats exposed to polypropylene mesh. BJU Int 100(1): Peiper C, Junge K, Klinge U et al (2006) Is there a risk of infertility after inguinal mesh repair? Experimental studies in the pig and the rabbit. Hernia 10(1): Shin D, Lipshultz LI, Goldstein M et al (2005) Herniorrhaphy with polypropylene mesh causing inguinal vasal obstruction. Ann Surg 241(4):
8 894 Hernia (2017) 21: Yamaguchi K, Ishikawa T, Nakano Y et al (2008) Rapidly progressing, late-onset obstructive azoospermia linked to herniorrhaphy with mesh. Fertil Steril 90(5): Kordzadeh A, Liu MO, Jayanthi NV (2016) Male infertility following inguinal hernia repair: a systematic review and pooled analysis. Hernia. doi: /s Goruroglu Ozturk O (2012) Using biological variation data for reference change values in clinical laboratories. Biochem Anal Biochem 1(4): Bellón JM, Contreras LA, Buján J et al (1998) Tissue response to polypropylene meshes used in the repair of abdominal wall defects. Biomaterials 19(7 9): Ridgway PF, Shah J, Darzi A (2002) Male genital tract injuries after contemporary inguinal hernia repair. BJU Int 90(3): Dilek ON (2014) Hernioplasty and testicular perfusion. SpringerPlus 21(3): Middleton W, Thorne D, Melson G (1989) Color Doppler ultrasound of the testis. AJR Am J Roentgenol 152(2): Stula I, Druzijanic N, Srsen D et al (2015) Influence of inguinal hernia mesh repair on testicular flow and sperm autoimmunity. Hernia 16(4): Lal P, Bansal B, Sharma R et al (2016) Laparoscopic TEP repair of inguinal hernia does not alter testicular perfusion. Hernia 20(3): Ersin S, Aydin U, Makay O (2006) Is testicular perfusion influenced during laparoscopic inguinal hernia surgery? Surg Endosc 20: Gurbulak EK, Gurbulak B, Akgun IE et al (2015) Effects of totally extraperitoneal (TEP) and Lichtenstein hernia repair on testicular blood flow and volume. Surgery 158(5): Peeters E, Spiessens C, Oyen R et al (2010) Laparoscopic inguinal hernia repair in men with lightweight meshes may significantly impair sperm motility: a randomized controlled trial. Ann Surg 252(2): Skawran S, Weyhe D, Schmitz B et al (2011) Bilateral endoscopic total extraperitoneal (TEP) inguinal hernia repair does not induce obstructive azoospermia: data of a retrospective and prospective trial. World J Surg 35(7): Peeters E, Spiessens C, Oyen R et al (2014) Sperm motility after laparoscopic inguinal hernia repair with lightweight meshes: 3-year follow-up of a randomised clinical trial. Hernia 18: Akbulut G, Serteser M, Yucel A et al (2003) Can laparoscopic hernia repair alter function and volume of testis? Randomized clinical trial. Surg Laparosc Ednosc Percutan Tech 13(6): Wantz GE (1982) Testicular atrophy as a risk inguinal hernioplasty. Surg Gynecol Obstet 154(4): Sucullu I, Filiz AI, Sen B et al (2010) The effects of inguinal hernia repair on testicular function in young adults: a prospective randomized study. Hernia 14(2): Schouten N, Van Dalen T, Smakman N et al (2012) Male infertility after endoscopic totally extraperitoneal (TEP) hernia repair (Main): rationale and design of a prospective observational cohort study. BMS Surg 21(12):7 28. Kehlet H, Roumen RM, Reinpold W et al (2013) Invited commentary: persistent pain after inguinal hernia repair: what do we know and what do we need to know? Hernia 17:
Male infertility after endoscopic Totally Extraperitoneal (Tep) hernia repair (Main): rationale and design of a prospective observational cohort study
 Schouten et al. BMC Surgery 2012, 12:7 STUDY PROTOCOL Male infertility after endoscopic Totally Extraperitoneal (Tep) hernia repair (Main): rationale and design of a prospective observational cohort study
Schouten et al. BMC Surgery 2012, 12:7 STUDY PROTOCOL Male infertility after endoscopic Totally Extraperitoneal (Tep) hernia repair (Main): rationale and design of a prospective observational cohort study
 BMC Surgery This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Male infertility after endoscopic
BMC Surgery This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Male infertility after endoscopic
Does the use of hernia mesh in surgical inguinal hernia repairs cause male infertility? A systematic review and descriptive analysis
 Dong et al. Reproductive Health (2018) 15:69 https://doi.org/10.1186/s12978-018-0510-y REVIEW Open Access Does the use of hernia in surgical inguinal hernia repairs cause male infertility? A systematic
Dong et al. Reproductive Health (2018) 15:69 https://doi.org/10.1186/s12978-018-0510-y REVIEW Open Access Does the use of hernia in surgical inguinal hernia repairs cause male infertility? A systematic
JMSCR Vol 04 Issue 09 Page September 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i9.21 Effect of Prosthetic Mesh in Laparoscopic
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i9.21 Effect of Prosthetic Mesh in Laparoscopic
COMPLICATIONS OF HERNIA REPAIR
 COMPLICATIONS OF HERNIA REPAIR Stanley Rogers, MD Associate Clinical Professor of Surgery University of Califronia, San Francisco Paré was respected as a hernia specialist, and was known to have elevated
COMPLICATIONS OF HERNIA REPAIR Stanley Rogers, MD Associate Clinical Professor of Surgery University of Califronia, San Francisco Paré was respected as a hernia specialist, and was known to have elevated
COMPARISON OF OUTCOMES (EARLY AND LATE) FOLLOWING OPEN AND LAPAROSCOPIC REPAIR OF INGUINAL HERNIAS: AN EXPERIENCE OF A SINGLE SURGICAL UNIT
 IMPACT: International Journal of Research in Applied, Natural and Social Sciences (IMPACT: IJRANSS) ISSN(E): 2321-8851; ISSN(P): 2347-4580 Vol. 2, Issue 2, Feb 2014, 163-168 Impact Journals COMPARISON
IMPACT: International Journal of Research in Applied, Natural and Social Sciences (IMPACT: IJRANSS) ISSN(E): 2321-8851; ISSN(P): 2347-4580 Vol. 2, Issue 2, Feb 2014, 163-168 Impact Journals COMPARISON
Hallén, Magnus; Sandblom, Gabriel; Nordin, Pär; Gunnarsson, Ulf; Kvist, Ulrik; Westerdahl, Johan
 Male infertility after mesh hernia repair: A prospective study. Hallén, Magnus; Sandblom, Gabriel; Nordin, Pär; Gunnarsson, Ulf; Kvist, Ulrik; Westerdahl, Johan Published in: Surgery DOI: 10.1016/j.surg.2010.04.027
Male infertility after mesh hernia repair: A prospective study. Hallén, Magnus; Sandblom, Gabriel; Nordin, Pär; Gunnarsson, Ulf; Kvist, Ulrik; Westerdahl, Johan Published in: Surgery DOI: 10.1016/j.surg.2010.04.027
Postgraduate Training in Reproductive Health
 SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
SURGICAL TREATMENT OF MALE INFERTILITY Georges A. de Boccard, M.D. Consultant Urologist F.M.H., F.E.B.U. Postgraduate Training in Reproductive Health Geneva Foundation for Medical Education and Research
Keywords TEP repair Lightweight mesh Heavyweight mesh Chronic groin pain Mesh awareness Quality of life
 Surg Endosc (2015) 29:3171 3178 DOI 10.1007/s00464-014-4049-x and Other Interventional Techniques Three-month results of the effect of Ultrapro or Prolene mesh on post-operative pain and well-being following
Surg Endosc (2015) 29:3171 3178 DOI 10.1007/s00464-014-4049-x and Other Interventional Techniques Three-month results of the effect of Ultrapro or Prolene mesh on post-operative pain and well-being following
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
JMSCR Vol 04 Issue 09 Page September 2016
 JMSCR Vol 4 Issue 9 Page 4-47 September 6 www.jmscr.igmpublication.org Impact Factor 5.44 Index Copernicus Value: 8.7 ISSN (e)-47-76x ISSN (p) 455-45 DOI: http://dx.doi.org/.855/jmscr/v4i9.7 Comparative
JMSCR Vol 4 Issue 9 Page 4-47 September 6 www.jmscr.igmpublication.org Impact Factor 5.44 Index Copernicus Value: 8.7 ISSN (e)-47-76x ISSN (p) 455-45 DOI: http://dx.doi.org/.855/jmscr/v4i9.7 Comparative
TRIALS. Abstract. Schouten et al. Trials 2012, 13:76
 Schouten et al. Trials 2012, 13:76 TRIALS STUDY PROTOCOL Open Access The effect of ultrapro or prolene mesh on postoperative pain and well-being following endoscopic Totally Extraperitoneal (TEP) hernia
Schouten et al. Trials 2012, 13:76 TRIALS STUDY PROTOCOL Open Access The effect of ultrapro or prolene mesh on postoperative pain and well-being following endoscopic Totally Extraperitoneal (TEP) hernia
Role of Colour Doppler Ultrasonography in evaluation of scrotal pain and swelling
 Original Research Article Role of Colour Doppler Ultrasonography in evaluation of scrotal pain and swelling Assistant Professor, Department of Radiodiagnosis, Government Medical College, Rajnandgaon Chattisghar,
Original Research Article Role of Colour Doppler Ultrasonography in evaluation of scrotal pain and swelling Assistant Professor, Department of Radiodiagnosis, Government Medical College, Rajnandgaon Chattisghar,
Left Side Approach in Laparoscopic Transabdominal Preperitoneal Inguinal Herniorrhaphy is Feasible for Any Type of Inguinal Hernia
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(3):118-123 Journal of Minimally Invasive Surgery Left Side Approach in Laparoscopic Transabdominal Preperitoneal Inguinal
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(3):118-123 Journal of Minimally Invasive Surgery Left Side Approach in Laparoscopic Transabdominal Preperitoneal Inguinal
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele
 Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
Chapter 11 Guidelines and Best Practice Statements for the Evaluation and Management of Infertile Adult and Adolescent Males with Varicocele With the continuous growth of medical knowledge and the need
What are Varicoceles?
 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Perhaps the most controversial of new laparoscopic operations is the repair of the inguinal hernia. The
 JOURNAL OF LAPAROENDOSCOPIC SURGERY Volume 2, Number 6, 1992 Mary Ann Liebert, Inc., Publishers Extraperitoneal Endoscopie Inguinal Hernia Repair GEORGE S. FERZLI, M.D., F.A.C.S., AZIZ MASSAD, M.D., and
JOURNAL OF LAPAROENDOSCOPIC SURGERY Volume 2, Number 6, 1992 Mary Ann Liebert, Inc., Publishers Extraperitoneal Endoscopie Inguinal Hernia Repair GEORGE S. FERZLI, M.D., F.A.C.S., AZIZ MASSAD, M.D., and
Inguinal and Femoral Hernias. August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center
 Inguinal and Femoral Hernias August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center Background Approximately 20 million groin hernias are repaired each
Inguinal and Femoral Hernias August 10, 2016 Basic Science Lecture Department of Surgery University of Tennessee Health Science Center Background Approximately 20 million groin hernias are repaired each
Open Tension-Free Mesh Repair for Adult Inguinal Hernia: Eight Years of Experience in a Community Hospital
 Original Articles Asian Journal of Surgery Excerpta Medica Asia Ltd Open Tension-Free Mesh Repair for Adult Inguinal Hernia: Eight Years of Experience in a Community Hospital Shunji Yamamoto, Toshiki Maeda,
Original Articles Asian Journal of Surgery Excerpta Medica Asia Ltd Open Tension-Free Mesh Repair for Adult Inguinal Hernia: Eight Years of Experience in a Community Hospital Shunji Yamamoto, Toshiki Maeda,
Male History, Clinical Examination and Testing
 Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
DEFINITION HX & PH/EX
 DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
Assessment of the intratesticular resistive index by colour Doppler ultrasonography measurements as a predictor of spermatogenesis
 Sexual Medicine PINGGERA et al. Assessment of the intratesticular resistive index by colour Doppler ultrasonography measurements as a predictor of spermatogenesis Germar-Michael Pinggera, Michael Mitterberger,
Sexual Medicine PINGGERA et al. Assessment of the intratesticular resistive index by colour Doppler ultrasonography measurements as a predictor of spermatogenesis Germar-Michael Pinggera, Michael Mitterberger,
Setting The setting was a hospital. The economic study was carried out in Parma, Italy.
 Hernioplasty and simultaneous laparoscopic cholecystectomy: a prospective randomized study of open tension-free versus laparoscopic inguinal hernia repair Sarli L, Villa F, Marchesi F Record Status This
Hernioplasty and simultaneous laparoscopic cholecystectomy: a prospective randomized study of open tension-free versus laparoscopic inguinal hernia repair Sarli L, Villa F, Marchesi F Record Status This
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
CAT FOR TREATMENT. Clinical Scenario:
 CAT FOR TREATMENT Clinical Scenario: A 30-year old male footballer presented at surgical OPD with clinical of painful, reducible groin hernia. I advice him for surgical management and gave him the possible
CAT FOR TREATMENT Clinical Scenario: A 30-year old male footballer presented at surgical OPD with clinical of painful, reducible groin hernia. I advice him for surgical management and gave him the possible
Hybrid Laparoscopic and Anterior Approach for Postsurgical Inguinal Hernia After Iliofemoral Arterial Bypass
 Int Surg 2015;100:431 435 DOI: 10.9738/INTSURG-D-14-00226.1 Case Report Hybrid Laparoscopic and Anterior Approach for Postsurgical Inguinal Hernia After Iliofemoral Arterial Bypass Tomoya Tsukada 1,2,
Int Surg 2015;100:431 435 DOI: 10.9738/INTSURG-D-14-00226.1 Case Report Hybrid Laparoscopic and Anterior Approach for Postsurgical Inguinal Hernia After Iliofemoral Arterial Bypass Tomoya Tsukada 1,2,
Technical points of the laparoscopic transabdominal preperitoneal (TAPP) approach in inguinal hernia repair
 Surgical Technique Page 1 of 5 Technical points of the laparoscopic transabdominal preperitoneal (TAPP) approach in inguinal hernia repair Qiwei Shen, Qiyuan Yao Department of General Surgery, Huashan
Surgical Technique Page 1 of 5 Technical points of the laparoscopic transabdominal preperitoneal (TAPP) approach in inguinal hernia repair Qiwei Shen, Qiyuan Yao Department of General Surgery, Huashan
JMSCR Vol. 03 Issue 08 Page August 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.18535/jmscr/v3i8.40 Comparison of Outcome between Lightweight Mesh & Heavy Weight Mesh in Lichtenstein Groin
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.18535/jmscr/v3i8.40 Comparison of Outcome between Lightweight Mesh & Heavy Weight Mesh in Lichtenstein Groin
Comparing three different surgical techniques used in adult bilateral varicocele
 Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Asian J Endosc Surg ISSN 1758-5902 ORIGINAL ARTICLE Comparing three different surgical techniques used in adult bilateral varicocele HB Sun, Y Liu, MB Yan, ZD Li & XG Gui Department of Urology, Fifth Affiliated
Original Research Article
 Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Original Research Article Evaluation of Effects of Varicocele Repair on Seminal Parameters in Cases of Clinical and Subclinical Varicocele A Two Year Study Suresh Kumar 1, Kishore Kumar Markapuram 2, B
Vikram Dogra, M.D. Professor of Radiology, Urology & BME Department of Imaging Sciences University Of Rochester Medical Center
 Ultrasound of the Scrotum Vikram Dogra, M.D. Professor of Radiology, Urology & BME Department of Imaging Sciences University Of Rochester Medical Center Etiologies of Acute Scrotal Pain Epididymitis/Orchitis
Ultrasound of the Scrotum Vikram Dogra, M.D. Professor of Radiology, Urology & BME Department of Imaging Sciences University Of Rochester Medical Center Etiologies of Acute Scrotal Pain Epididymitis/Orchitis
Early experience of laparoscopic varicocelectomy in College
 Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-2, 32-36 Original Article Early experience of laparoscopic varicocelectomy in College of Medical Sciences, Teaching Hospital, Bhartpur,, Nepal
1. Introduction. 2. Material and methods Methodology
 Clinical evaluation on 96 patients of the SWING-CONTACT meshes in the treatment of groin hernia: a new three-dimensional device with atraumatic grips on both sides 1. Introduction This data collection
Clinical evaluation on 96 patients of the SWING-CONTACT meshes in the treatment of groin hernia: a new three-dimensional device with atraumatic grips on both sides 1. Introduction This data collection
EFFECT OF BILATERAL LICHTENSTEIN HERNIA REPAIR ON MALE GONADAL FUNCTION: A PROSPECTIVE STUDY
 EFFECT OF BILATERAL LICHTENSTEIN HERNIA REPAIR ON MALE GONADAL FUNCTION: A PROSPECTIVE STUDY * Shailesh Kumar, Meheraj S. K. and Priyadasrhi Dikshit Department of General Surgery, PGIMER & Dr. RML Hospital,
EFFECT OF BILATERAL LICHTENSTEIN HERNIA REPAIR ON MALE GONADAL FUNCTION: A PROSPECTIVE STUDY * Shailesh Kumar, Meheraj S. K. and Priyadasrhi Dikshit Department of General Surgery, PGIMER & Dr. RML Hospital,
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Sexual function after Stoppa hernia repair in patients with bilateral inguinal hernia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Sexual function after Stoppa hernia repair in patients with bilateral inguinal hernia Downloaded
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Sexual function after Stoppa hernia repair in patients with bilateral inguinal hernia Downloaded
LAPAROSCOPIC TOTAL EXTRAPERITONEAL INGUINAL HERNIA REPAIR: A STUDY AT RAWALPINDI MEDICAL COLLEGE AND ALLIED TEACHING HOSPITALS ABSTRACT
 ORIGINAL ARTICLE LAPAROSCOPIC TOTAL EXTRAPERITONEAL INGUINAL HERNIA REPAIR: A STUDY AT RAWALPINDI MEDICAL COLLEGE AND ALLIED TEACHING HOSPITALS Muhammad Hanif 1, Anis Ahmed 2, Muhammad Mussadiq Khan 3
ORIGINAL ARTICLE LAPAROSCOPIC TOTAL EXTRAPERITONEAL INGUINAL HERNIA REPAIR: A STUDY AT RAWALPINDI MEDICAL COLLEGE AND ALLIED TEACHING HOSPITALS Muhammad Hanif 1, Anis Ahmed 2, Muhammad Mussadiq Khan 3
Assessment and comparison of laparoscopic hernia repair versus open hernia: a non-randomized study
 International Surgery Journal Murthy PK et al. Int Surg J. 2018 Mar;5(3):1021-1025 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20180823
International Surgery Journal Murthy PK et al. Int Surg J. 2018 Mar;5(3):1021-1025 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20180823
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS
 Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
ABSITE Review: Hernias
 ABSITE Review: Inguinal and Femoral Hernias Sybile Val M.D. SUNY Downstate Medical Center Department of Surgery June 27, 2008 Objectives www.downstatesurgery.org Correctly identify anatomical landmarks
ABSITE Review: Inguinal and Femoral Hernias Sybile Val M.D. SUNY Downstate Medical Center Department of Surgery June 27, 2008 Objectives www.downstatesurgery.org Correctly identify anatomical landmarks
Appendix D Answers to the KAP Survey
 From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
حسام أبو عوض. -Dr. Mohammad Muhtasib. 1 P a g e
 5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Varicoceles : co-relation of clinical examination with Color Doppler Sonograpghy at a tertiary care hospital
 Original article: Varicoceles : co-relation of clinical examination with Color Doppler Sonograpghy at a tertiary care hospital 1Dr. Neeraj Prajapati, 2 Dr. S.K.Ratogi, 3 Dr. Vijay Kulshrestha, 4 Dr. Abhinav
Original article: Varicoceles : co-relation of clinical examination with Color Doppler Sonograpghy at a tertiary care hospital 1Dr. Neeraj Prajapati, 2 Dr. S.K.Ratogi, 3 Dr. Vijay Kulshrestha, 4 Dr. Abhinav
Highlights from the International Guidelines for Groin Hernia Management
 Editorial Page 1 of 5 Highlights from the International Guidelines for Groin Hernia Management Sathien Tumtavitikul Department of Surgery, Vichaiyut Hospital, Bangkok, Thailand Correspondence to: Sathien
Editorial Page 1 of 5 Highlights from the International Guidelines for Groin Hernia Management Sathien Tumtavitikul Department of Surgery, Vichaiyut Hospital, Bangkok, Thailand Correspondence to: Sathien
First Transumbilical Transabdominal Preperitoneal Inguinal Hernia Repair in the Middle East
 ISPUB.COM The Internet Journal of Surgery Volume 25 Number 1 First Transumbilical Transabdominal Preperitoneal Inguinal Hernia Repair in the Middle East A Al-Dowais Citation A Al-Dowais. First Transumbilical
ISPUB.COM The Internet Journal of Surgery Volume 25 Number 1 First Transumbilical Transabdominal Preperitoneal Inguinal Hernia Repair in the Middle East A Al-Dowais Citation A Al-Dowais. First Transumbilical
THE PATIENT S GUIDE TO VARICOCELE
 The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
The Varicocele Decision Varicoceles are a relatively common problem that can hurt a man's fertility. The good news is that this is a fairly simple problem to fix. Dr. Fisch has treated hundreds of men
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
No Mesh Technique of Inguinal Hernia Repair Desarda s Repair
 Quest Journals Journal of Medical and Dental Science Research Volume 3~ Issue 6 (2016) pp: 35-39 ISSN(Online) : 2394-076X ISSN (Print):2394-0751 www.questjournals.org Research Paper No Mesh Technique of
Quest Journals Journal of Medical and Dental Science Research Volume 3~ Issue 6 (2016) pp: 35-39 ISSN(Online) : 2394-076X ISSN (Print):2394-0751 www.questjournals.org Research Paper No Mesh Technique of
Comparative Evaluation Of Preservation Versus Elective Division Of The Ilioinguinal Nerve In Open Mesh Repair Of Inguinal Hernias
 ISPUB.COM The Internet Journal of Surgery Volume 30 Number 1 Comparative Evaluation Of Preservation Versus Elective Division Of The Ilioinguinal Nerve In Open Mesh Repair Of Inguinal Hernias A Bansal.,
ISPUB.COM The Internet Journal of Surgery Volume 30 Number 1 Comparative Evaluation Of Preservation Versus Elective Division Of The Ilioinguinal Nerve In Open Mesh Repair Of Inguinal Hernias A Bansal.,
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Comparison of Transabdominal Preperitoneal and Total Extra Peritoneal: A Prospective Study
 Original Article DOI:.1734/ijss/21/23 Comparison of Transabdominal Preperitoneal and Total Extra Peritoneal: A Prospective Study T Shivakumar 1, B M Pavan 1, C S Gurukiran 2, N Chandrashekar 2, N Satish
Original Article DOI:.1734/ijss/21/23 Comparison of Transabdominal Preperitoneal and Total Extra Peritoneal: A Prospective Study T Shivakumar 1, B M Pavan 1, C S Gurukiran 2, N Chandrashekar 2, N Satish
DISORDERS OF MALE GENITALS
 Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 9. Testicular disorders/disorders of male genitals. Horm Res 2007;68(suppl 2):63 66 ESPE Code Diagnosis OMIM ICD10
A comparative study of inguinal hernia repair: Shouldice versus Lichtenstein repair
 International Surgery Journal Shah RS et al. Int Surg J. 2018 Jun;5(6):2238-2243 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182229
International Surgery Journal Shah RS et al. Int Surg J. 2018 Jun;5(6):2238-2243 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182229
Journal of Innovations in Pharmaceuticals and Biological Sciences
 Journal of Innovations in Pharmaceuticals and Biological Sciences www.jipbs.com JIPBS ISSN: 2349-2759 Research article A Study on retrospective analysis of inguinal hernia repair by various methods in
Journal of Innovations in Pharmaceuticals and Biological Sciences www.jipbs.com JIPBS ISSN: 2349-2759 Research article A Study on retrospective analysis of inguinal hernia repair by various methods in
MALE GENITAL SURGICAL PROCEDURES
 Male Genital Surgical ProceduresDecember 22, 2015 (effective March 1, 201) PENIS Slit of prepuce (complete care) S5 - newborn... 14.35 S58 - infant... 21.50 S59 - adult or child... 30.25 EXCISION Circumcision
Male Genital Surgical ProceduresDecember 22, 2015 (effective March 1, 201) PENIS Slit of prepuce (complete care) S5 - newborn... 14.35 S58 - infant... 21.50 S59 - adult or child... 30.25 EXCISION Circumcision
Laparoscopic Inguinal Hernia Repair in Children
 SCIENTIFIC PAPER Laparoscopic Inguinal Hernia Repair in Children Palanivelu Chinnaswamy, MCh (GE), Vijaykumar Malladi, MS, Kalpesh V. Jani, DNB, MS, R. Parthasarthi, MBBS, Roshan A. Shetty, MS, Alfie Jose
SCIENTIFIC PAPER Laparoscopic Inguinal Hernia Repair in Children Palanivelu Chinnaswamy, MCh (GE), Vijaykumar Malladi, MS, Kalpesh V. Jani, DNB, MS, R. Parthasarthi, MBBS, Roshan A. Shetty, MS, Alfie Jose
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Information for Patients. Male infertility. English
 Information for Patients Male infertility English Table of contents What is male infertility?... 3 Diagnosis... 3 Medical history... 3 Physical examination... 3 Hormone blood tests... 3 Semen analysis...
Information for Patients Male infertility English Table of contents What is male infertility?... 3 Diagnosis... 3 Medical history... 3 Physical examination... 3 Hormone blood tests... 3 Semen analysis...
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Measure ID Domain Measure Title Measure Description/Definition Numerator Denominator Denominator Exclusions Denominator Exceptions
 n-qpp s ID Domain Title Description/Definition Numerator Denominator Denominator Exclusions Denominator Exceptions Riskadjustment AQUA3 (inverse) Cryptorchidism: Inappropriate use of scrotal/groin ultrasound
n-qpp s ID Domain Title Description/Definition Numerator Denominator Denominator Exclusions Denominator Exceptions Riskadjustment AQUA3 (inverse) Cryptorchidism: Inappropriate use of scrotal/groin ultrasound
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY
 MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
MICROSCOPIC AND CONVENTIONAL SUB INGUINAL VARICOCELECTOMY COMPARITIVE STUDY Mahmoud Abou Amraa Surgery Department, Al-Azhar University, Assiut ---------------------------------------------------------------------------------------------------
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Case Report Testicular Arteriovenous Malformation: Gray-Scale and Color Doppler Ultrasonography Features
 Volume 2011, Article ID 876206, 4 pages doi:10.11/2011/876206 Case Report Testicular Arteriovenous Malformation: Gray-Scale and Color Doppler Ultrasonography Features Fatih Gulsen, 1 Ismail Mihmanli, 1
Volume 2011, Article ID 876206, 4 pages doi:10.11/2011/876206 Case Report Testicular Arteriovenous Malformation: Gray-Scale and Color Doppler Ultrasonography Features Fatih Gulsen, 1 Ismail Mihmanli, 1
Chapter 9. Summary & conclusion
 Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Laparoscopic Orchiopexy for a Nonpalpable Testis
 www.kjurology.org DOI:1.4111/kju.21.51.2.16 Laparoscopy/Robotics Laparoscopic Orchiopexy for a Nonpalpable Testis Jongwon Kim, Gyeong Eun Min 1, Kun Suk Kim Department of Urology, University of Ulsan College
www.kjurology.org DOI:1.4111/kju.21.51.2.16 Laparoscopy/Robotics Laparoscopic Orchiopexy for a Nonpalpable Testis Jongwon Kim, Gyeong Eun Min 1, Kun Suk Kim Department of Urology, University of Ulsan College
VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD
 Nagoya J. Med. Sci. 49. 53-59, 1987 VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD KOJI MIYAKE, MASANORI YAMAMOTO and HIDEO MITSUYA Department of Urology, Nagoya University
Nagoya J. Med. Sci. 49. 53-59, 1987 VASOVASOSTOMY FOR OBSTRUCTIVE AZOOSPERMIA DUE TO HERNIORRHAPHY IN CHILDHOOD KOJI MIYAKE, MASANORI YAMAMOTO and HIDEO MITSUYA Department of Urology, Nagoya University
Combined Transurethral Prostatectomy And Inguinal Hernioplasty
 ISPUB.COM The Internet Journal of Surgery Volume 20 Number 1 Combined Transurethral Prostatectomy And Inguinal Hernioplasty I Othman, A Abdel-Maguid Citation I Othman, A Abdel-Maguid. Combined Transurethral
ISPUB.COM The Internet Journal of Surgery Volume 20 Number 1 Combined Transurethral Prostatectomy And Inguinal Hernioplasty I Othman, A Abdel-Maguid Citation I Othman, A Abdel-Maguid. Combined Transurethral
Acute scrotum. Acute Epididymo-orchitis. Phyllis Yan, APDR (QEH)
 Acute scrotum Acute Epididymo-orchitis Phyllis Yan, APDR (QEH) Conditions leading to acute pain Torsion Acute Epididymitis / Epididymoorchitis Scrotal trauma Inguinal hernias Testicular tumors Epididymitis/epididymo
Acute scrotum Acute Epididymo-orchitis Phyllis Yan, APDR (QEH) Conditions leading to acute pain Torsion Acute Epididymitis / Epididymoorchitis Scrotal trauma Inguinal hernias Testicular tumors Epididymitis/epididymo
A Randomised Control Study on Neurosensory Outcomes of lioingunal Neurectomy in Lichtenstein s Hernia Repair
 A Randomised Control Study on Neurosensory Outcomes of lioingunal Neurectomy in Lichtenstein s Hernia Repair Dr Kudva A; Dr Lakshminarayana B; Dr Addala PK; Dr Prasad S October 2015 Volume 10 Issue 1 Doctors
A Randomised Control Study on Neurosensory Outcomes of lioingunal Neurectomy in Lichtenstein s Hernia Repair Dr Kudva A; Dr Lakshminarayana B; Dr Addala PK; Dr Prasad S October 2015 Volume 10 Issue 1 Doctors
The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
 pissn: 2287-4208 / eissn: 2287-490 World J Mens Health 2014 April 32(1): 5-0 http://dx.doi.org/10.5534/wjmh.2014.32.1.5 Original Article The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
pissn: 2287-4208 / eissn: 2287-490 World J Mens Health 2014 April 32(1): 5-0 http://dx.doi.org/10.5534/wjmh.2014.32.1.5 Original Article The Incidence of Fever after Subinguinal Microsurgical Varicocelectomy
The Acute Scrotum: Sonographic Findings
 The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
International Journal of Science and Research (IJSR) ISSN (Online): Index Copernicus Value (2013): 6.14 Impact Factor (2013): 4.
 Comparative Study on the Application of Surgipro Partiene Mesh and Light Partiene Mesh, in Patients with Inguinal Hernia Surgery with the Lichtenstein Method Dr. Gordana Bozhinovska - Beaka MOB "th September"
Comparative Study on the Application of Surgipro Partiene Mesh and Light Partiene Mesh, in Patients with Inguinal Hernia Surgery with the Lichtenstein Method Dr. Gordana Bozhinovska - Beaka MOB "th September"
Surgical Sperm Retrieval
 Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Saint Mary s Hospital Department of Reproductive Medicine Information for Patients Surgical Sperm Retrieval About one man in a hundred produces no sperm (10-15% of all sub fertile men) - a condition known
Groin hernia repair after radical prostatectomy and adenomectomy: versus patient without prostatectomie Club hernie database results.
 APHS Tokyo 27-28 October 2016 EHS Vienna 25-27 MAY 2017 MESH Paris 15-17 Juin 2017 Groin hernia repair after radical prostatectomy and adenomectomy: versus patient without prostatectomie Club hernie database
APHS Tokyo 27-28 October 2016 EHS Vienna 25-27 MAY 2017 MESH Paris 15-17 Juin 2017 Groin hernia repair after radical prostatectomy and adenomectomy: versus patient without prostatectomie Club hernie database
Does the duration of infertility affect semen parameters and pregnancy rate after varicocelectomy? A retrospective study
 Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Clinical Urology Varicocele and duration of infertility International Braz J Urol Vol. 37 (6): 745-750, November - December, 2011 Does the duration of infertility affect semen parameters and pregnancy
Associations of Ultrasonographic Features with Scrotal Pain after Vasectomy
 www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.11.782 Infection/Inflammation Associations of Ultrasonographic Features with Scrotal Pain after Vasectomy Seung Hoon Cho, Seung Ki Min, Seung Tae
www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.11.782 Infection/Inflammation Associations of Ultrasonographic Features with Scrotal Pain after Vasectomy Seung Hoon Cho, Seung Ki Min, Seung Tae
Repair of inguinal hernia utilizing external oblique muscle sheath as posterior wall strengthening and placing spermatic cord subcutaneously
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Original Research Article Volume 3, Issue 11-2017 DOI: http://dx.doi.org/10.22192/ijcrms.2017.03.11.009
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Original Research Article Volume 3, Issue 11-2017 DOI: http://dx.doi.org/10.22192/ijcrms.2017.03.11.009
Laparoscopic Repair of Inguinal Hernia with Biomimetic Matrix
 SCIENTIFIC PAPER Laparoscopic Repair of Inguinal Hernia with Biomimetic Matrix Arthur Fine, MD ABSTRACT Background and Objectives: Materials utilized for the repair of hernias fall into 2 broad categories,
SCIENTIFIC PAPER Laparoscopic Repair of Inguinal Hernia with Biomimetic Matrix Arthur Fine, MD ABSTRACT Background and Objectives: Materials utilized for the repair of hernias fall into 2 broad categories,
Male genital tract injuries after contemporary inguinal hernia repair
 BJU International (2002), 90, 272 276 REVIEW Male genital tract injuries after contemporary inguinal hernia repair P.F. RIDGWAY, J. SHAH and A.W. DARZI Department of Surgical Oncology and Technology, Imperial
BJU International (2002), 90, 272 276 REVIEW Male genital tract injuries after contemporary inguinal hernia repair P.F. RIDGWAY, J. SHAH and A.W. DARZI Department of Surgical Oncology and Technology, Imperial
Objectives. Hesselbach s Triangle 11/30/2009. Myopectineal Orifice of Fruchaud. Hernias: Who, What, When, Where, Why?
 Objectives Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Identify patients at risk for
Objectives Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Identify patients at risk for
M. Al-Mohtaseb. Tala Saleh. Faisal Nimri
 4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA
 PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA Dr. Abdulrahman A. Al-Bassam, FRCS(Ed) Assistant Professor & Consultant Paediatric Surgeon King Khalid University Hospital
PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA Dr. Abdulrahman A. Al-Bassam, FRCS(Ed) Assistant Professor & Consultant Paediatric Surgeon King Khalid University Hospital
SDRP JOURNAL OF ANESTHESIA & SURGERY
 SDRP JOURNAL OF ANESTHESIA & SURGERY 2017 RESEARCH Hernia defect closure with corresponding mesh site fixation only in laparoscopic inguinal hernia repair. DOI: 10.15436/JAS.2.1.3 ISSN:2473-2184 Ahmed
SDRP JOURNAL OF ANESTHESIA & SURGERY 2017 RESEARCH Hernia defect closure with corresponding mesh site fixation only in laparoscopic inguinal hernia repair. DOI: 10.15436/JAS.2.1.3 ISSN:2473-2184 Ahmed
Tension-Free Inguinal Hernia Repair: TEP Versus Mesh-Plug Versus Lichtenstein
 ANNALS OF SURGERY Vol. 237, No. 1, 142 147 2003 Lippincott Williams & Wilkins, Inc. Tension-Free Inguinal Hernia Repair: TEP Versus Mesh-Plug Versus Lichtenstein A Prospective Randomized Controlled Trial
ANNALS OF SURGERY Vol. 237, No. 1, 142 147 2003 Lippincott Williams & Wilkins, Inc. Tension-Free Inguinal Hernia Repair: TEP Versus Mesh-Plug Versus Lichtenstein A Prospective Randomized Controlled Trial
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
I would be happy to discuss all of these options for fertility after vasectomy with you at the time of our consultation or over the phone.
 F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
Male Reproductive System Dr. Gary Mumaugh
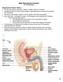 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Department of Medical Imaging, The Ottawa Hospital. Satheesh Krishna Sabarish Narayanasamy Wael Shabana Adnan Sheikh
 Department of Medical Imaging, The Ottawa Hospital. Satheesh Krishna Sabarish Narayanasamy Wael Shabana Adnan Sheikh Nothing to disclose Common and unusual presentations and manifestations of testicular
Department of Medical Imaging, The Ottawa Hospital. Satheesh Krishna Sabarish Narayanasamy Wael Shabana Adnan Sheikh Nothing to disclose Common and unusual presentations and manifestations of testicular
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Acute Groin Pain Following Trauma
 Lehigh Valley Health Network LVHN Scholarly Works Department of Family Medicine Acute Groin Pain Following Trauma Victoria Chen MD Lehigh Valley Health Network, victoria.chen@lvhn.org Follow this and additional
Lehigh Valley Health Network LVHN Scholarly Works Department of Family Medicine Acute Groin Pain Following Trauma Victoria Chen MD Lehigh Valley Health Network, victoria.chen@lvhn.org Follow this and additional
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
THE PATIENT S GUIDE TO VASECTOMY REVERSAL
 The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
The Basics of Vasectomy Reversal What is a Vasectomy? A vasectomy is a safe, simple, quick and effective method of contraception. As shown in Figure 1a, the testicles are continually producing sperm even
Follow this and additional works at: Part of the Other Medical Specialties Commons, and the Surgery Commons
 Lehigh Valley Health Network LVHN Scholarly Works Department of Surgery Hernias Lauren Dudas MD Lehigh Valley Health Network, Lauren.Dudas@lvhn.org Follow this and additional works at: http://scholarlyworks.lvhn.org/surgery
Lehigh Valley Health Network LVHN Scholarly Works Department of Surgery Hernias Lauren Dudas MD Lehigh Valley Health Network, Lauren.Dudas@lvhn.org Follow this and additional works at: http://scholarlyworks.lvhn.org/surgery
