28 Nursing made Incredibly Easy! July/August
|
|
|
- Hope Knight
- 5 years ago
- Views:
Transcription
1 The ABCs of male 28 Nursing made Incredibly Easy! July/August
2 reproductive cancer Reproductive cancer represents a significant risk to the male population. Prostate cancer is the most common nonskin cancer in the United States, testicular cancer is the most common solid malignancy affecting men ages 15 to 35, and penile cancer comprises 20% of cancers in men in Africa, Asia, and South America. We ll take a look at all three. By Rhonda Lawes MS, RN, CNE Assistant Professor University of Oklahoma Tulsa College of Nursing Tulsa, Okla. The author has disclosed that she has no significant relationships with or financial interest in any commercial companies that pertain to this educational activity. Mr. B is a 67-year-old retired attorney in New York, Mr. T is a 21-year-old college student in Southern California, and Mr. K is a 63-year-old farmer in Kenya. What could all three of these men have in common? They represent groups of men most at risk for developing reproductive cancer, more specifically, prostate, testicular, and penile cancer. The male population is at significant risk for reproductive cancer. Prostate cancer is the most common nonskin cancer in America, affecting one in six men (see Picturing prostate cancer). Testicular cancer is the most common solid malignancy affecting men ages 15 to 35. The National Cancer Institute (NCI) estimates that one in 271 men will be diagnosed with cancer of the testis in their lifetime (see Picturing testicular cancer). Penile cancer is rare in developed countries, but comprises 20% of cancers in men in Africa, Asia, and South America. In this article, I ll give you an overview of all three types of male reproductive cancer. Prostate cancer At his annual checkup, Mr. B mentions to his physician that he has been having trouble urinating and is experiencing some pain in his pelvic area. His physician performs a digital rectal exam and feels some areas that are tender and hardened in the prostate. Because of this finding, in addition to Mr. B s age and symptoms, the physician orders a prostate-specific antigen (PSA) test, which comes back elevated with a level of 23 ng/ml. Mr. B is scheduled for a transrectal biopsy. Testing for prostate cancer PSA. This blood test measures PSA (a protein produced by prostate cells) levels in the bloodstream. It s normal for men to have a level under 4 ng/ml. According to the American Cancer Society, there s a 25% chance of prostate cancer with PSA levels of 4 to 10 ng/ml, and a 50% chance of prostate cancer with levels greater than 10 ng/ml. This test is meant to be a screening; there are some issues that can elevate the PSA that are noncancerous, such as ejaculation (no ejaculation for at least 2 days before the test), advancing age, inflammation of the prostate gland, and benign prostatic hyperplasia (an enlarged prostate). Digital rectal exam. During this test, the healthcare provider inserts a lubricated, gloved finger into the rectum to feel the back wall of the prostate gland to determine if it s enlarged, tender, or has any lumps or hard areas. Transrectal ultrasound. During this test, a small probe, which uses sound waves to create a picture of the prostate gland, is inserted into the rectum. Transrectal biopsy. A biopsy gun is inserted into the rectum to obtain biopsies of the prostate gland. The gun retrieves small sections of tissue through a thin needle, and 2.5 ANCC CONTACT HOURS July/August 2011 Nursing made Incredibly Easy! 29
3 the samples are analyzed in the lab to determine if cancer is present. Staging The Gleason grading system is a scoring system based on microscopic tumor patterns that are measured by the pathologist. The system is subjective by nature and requires considerable skill by the pathologist. Scores range from 2 to 10, and the prognosis becomes poorer as the score increases. Staging describes the severity of a person s cancer and whether it has spread to other parts of the body. It s useful in determining the most effective plan of care (see NCI prostate cancer staging). The results are in... Mr. B s biopsy comes back positive for cancer. The prostate samples are evaluated and graded at Stage II, with a Gleason score of 2. These results indicate that the cancer Male reproductive cancer Statistics Prostate Testicular Penile Most common nonskin cancer in America Affects 1 in 6 men More than 65% of all prostate cancers are diagnosed In men over age 65 Most common solid malignancy Affects men ages 15 to 35 Responsible for 1% of all cancer in men Rare in developed countries Responsible for 20% of cancers in men in parts of Africa, Asia, and South America cheat sheet Signs and symptoms Changes in urinary or sexual function Frequent pain or stiffness in the lower back, hips, or upper thighs Nodule or painless swelling of the testicle Dull ache or heavy sensation in the lower abdomen, perianal area, or scrotum 10% of patients experience acute pain; some show gynecomastia (male breast enlargement) Redness Irritation A sore or lesion A lump on the penis Risk factors Tall height Lack of exercise and a sedentary lifestyle High calcium intake African descent Family history Cryptorchidism (undescended testicle) Orchiopexy (surgery for an undescended testicle) Phimosis Chronic inflammatory conditions Smoking Human papillomavirus Diagnostics PSA test Digital rectal exam Transrectal ultrasound Transrectal biopsy Scrotal ultrasound Lab tests for tumor markers (alpha-fetoprotein, beta-human chorionic gonadotropin, and lactate dehydrogenase); up to 50% of early state nonseminomas won t show these markers Biopsy Biopsy Urethroscopy MRI 30 Nursing made Incredibly Easy! July/August
4 hasn t yet spread outside his prostate. His physician explains the results of the biopsy and together they discuss treatment options, including watchful waiting, radiation therapy, hormone therapy, chemotherapy, and surgical removal of the prostate. Treatment options If prostate cancer is in the very early stage, hasn t spread, and is slow growing, watchful waiting may be an appropriate treatment option in consultation with a physician. This is also sometimes called active surveillance. The patient has regular follow-up screenings and testing to monitor the progression of the cancer. According to the National Comprehen sive Cancer Network s Clinical Practice Guidelines in Oncology for prostate cancer, additional treatment may be indicated based on the following PSA test results: for men who ve been in the watchful waiting phase and whose PSA level has doubled in fewer than 3 years, or they have a PSA velocity (change in PSA level over time) of greater than 0.75 ng/ml per year, or they have a prostate biopsy showing evidence of worsening cancer for men who ve had a radical prostatectomy (removal of the prostate gland) whose PSA level doesn t fall below the limits of detection after surgery, or they have a detectable PSA level (greater than 0.3 ng/ml) that increases on two or more subsequent measurements after having no detectable PSA for men who ve had other initial therapy, such as radiation therapy with or without hormonal therapy, whose PSA level has risen by 2 ng/ml or more after having no detectable PSA or a very low PSA level. The goal of radiation therapy is to kill the cancer cells. Adverse reactions include painful urination and frequency, erectile dysfunction, and rectal symptoms such as loose Picturing prostate cancer Prostate gland Sphincter urethrae stools or pain. There are two types of radiation (grouped by method of delivery) that can be considered: external beam radiation therapy. Computed tomography (CT) scans and magnetic resonance imaging (MRI) are used to identify where the cancer cells are located. For therapy, the patient lies on a table and a machine delivers the radiation treatment to the area of the body where the cancer has been located. Treatment is usually 5 days a week for several weeks as an outpatient. brachytherapy. Radioactive iodine or palladium in metal pellets, about the size of a grain of rice, is placed in the prostate tissue using an ultrasound-guided needle. Over several months, these pellets deliver a lowdose, constant delivery of radiation. After a year or so, the pellets will stop giving off radiation and can remain in the prostate. This therapy allows the patient the freedom to not have to return to the hospital as frequently as external beam radiation therapy. Membranous urethra Prostate carcinoma Bladder Seminal vesicle Ejaculatory duct July/August 2011 Nursing made Incredibly Easy! 31
5 Proton therapy allows for extreme precision in targeting prostate cancer cells. The machines to deliver this therapy cost between $25 and $150 million, and are consequently not widely available. As technology advances, this may become a more accessible option. Hormone therapy is another treatment option. Most prostate cancer cells need the male hormone testosterone to grow. Adverse reactions include erectile dysfunction, decreased libido, loss of muscle and bone mass, and weight gain. There s also some concern regarding the long-term use of hormone therapy and increased risk of cardiovascular problems. Some prostate cancer cells aren t dependent on testosterone and don t respond to hormone therapy. However, for those cells that do respond to testosterone, the goal of hormone therapy is to significantly decrease the amount of hormone available in the body. This can be accomplished in one of three ways: medication to decrease testosterone production. Gonadotropin-releasing hormone agonists inhibit the pituitary gland from stimulating the testicles to make testosterone. Examples of these medications include leuprolide and histrelin. medications to block testosterone. Antiandrogen medications are antagonists that block testosterone from reaching the cancer cells. Examples of these types of drugs are bicalutamide and flutamide. NCI prostate cancer staging Stage Stage 0 Definition Carcinoma in situ Stage I, II, and III Higher numbers indicate more extensive disease: larger tumor size or spread of the cancer beyond the organ in which it first developed to nearby lymph nodes or organs adjacent to the location of the primary tumor Stage IV The cancer has spread to another organ(s) Source: National Cancer Institute. Detection/staging. removal of the testicles (orchiectomy). Although it seems odd to remove the testicles to treat prostate cancer, the testicles are responsible for producing 90% of the body s testosterone. Removing the testicles will significantly lower the testosterone level. This procedure is done on an outpatient basis, and is permanent and irreversible. Chemotherapy drugs are aimed at rapidly growing cancer cells. Adverse reactions include hair loss, gastrointestinal upset, fatigue, leucopenia, thrombocytopenia, and some neuropathy. Chemotherapy may be considered in conjunction with other therapies, especially for treating cancers that aren t responsive to testosterone-limiting therapies. Docetaxel has been shown to prolong the survival of men with advanced prostate cancer that no longer responds to hormonal therapy. Cabazitaxel was approved in 2010 for patients who no longer respond to docetaxel. Surgical options include: radical prostatectomy. This procedure is the removal of the entire prostate gland and some of the surrounding tissue through an open incision in the abdomen or scrotum. The abdominal approach has a lower risk of nerve damage that can cause erectile dysfunction and bladder control problems. The perianal approach has a quicker recovery time, but has an increased risk of nerve damage and lymph nodes aren t as easily accessible. laparoscopic radical prostatectomy. This procedure is similar to the radical prostatectomy, but there s no open incision. The prostate is removed via a laparoscope. A surgical robot may also be used to assist the surgeon. Incisions are made that are only large enough to insert the tools and scope. Recovery time is usually quicker than an open incision surgery. Keeping up with our patient Mr. B opts for undergoing a prostatectomy. As his post-op nurse, you re aware that pain control, wound management, preventing 32 Nursing made Incredibly Easy! July/August
6 immobility complications, and facilitating urination are the most important priorities following his surgery. You ll need to work closely with the physician and Mr. B to manage his pain at an appropriate level. Mr. B may have abdominal drains in place for 3 to 5 days, depending on the amount of output. His dressings should be changed according to the surgeon s orders. Encourage Mr. B to sit up and ambulate as soon as possible following surgery to decrease the chance of deep vein thrombosis and pulmonary complications. The prostate gland is very close to the rectum; following surgery, the rectum is vulnerable for injury. Stool softeners and laxatives will be given to reduce the amount of straining. Enemas and rectal thermometers should be avoided. If the surgeon determines that the nerve bundles on the sides of the prostate that are responsible for erections are cancer-free, these may not have to be removed during the procedure. This is called a nerve-sparing radical prostatectomy (NSRP). NSRP has significantly decreased the incidence of erectile dysfunction. After a radical prostatectomy, male patients will no longer experience fluid ejaculation, but can still experience sexual desire and arousal and achieve orgasm. Because the urethra runs through the middle of the prostate, the urethra has to be cut above and below the prostate and then reattached to the bladder. In an effort to decrease incontinence and prevent urethral strictures from scar tissue, the patient will require a urinary catheter until the reconnection has had time to heal, sometimes up to 2 to 3 weeks. After prostatectomy, 25% of patients report leakage or lack of control requiring pads for 6 months. Routine in-hospital urinary catheter protocols should be followed, and you should teach Mr. B in-home care, as he ll be discharged with the urinary catheter in place. Mr. B is discharged home with his drains removed and a urinary catheter in place. He has decided after consulting with his physician to begin an active surveillance plan of treatment. He ll be returning for post-op follow-up in addition to regular screenings to monitor any potential advance of the disease. Testicular cancer Mr. T notices a swelling and a lump in his left testicle over the past several weeks, and a dull ache in his lower abdomen has recently developed. Because Mr. T is a college student, he makes an appointment with the university s nurse practitioner, who refers him to his primary care physician. After ruling out other possible causes, such as inguinal hernia, orchitis (inflammation of the testicles), epididy mitis (inflammation of the epididymis), and torsion, and based on his symptoms and physical exam, the physician orders a testicular ultrasound. Testing for testicular cancer Scrotal ultrasound. During this test, the patient lies on his back with his legs spread and a handheld ultrasound probe is placed on the scrotum to obtain the ultrasound images. The ultrasound helps the physician evaluate the lump in the testicle to determine if it s solid or filled with fluid and if it s inside the testicle. Lab tests. These tests include a complete blood cell count and tumor markers used for testicular cancer (alpha-fetoprotein, betahuman chorionic gonadotropin, and lactate dehydrogenase). These tests may detect a tumor that isn t large enough to be felt on exam or X-ray, but negative markers don t guarantee that there isn t a tumor. Tumor markers are also used in the follow-up of the disease after treatment. Radiographic imaging. A high-resolution CT scan of the abdomen and pelvis and a chest X-ray are used to look for evidence of regional lymph node metastasis. Your prostatectomy patient will be discharged home with a urinary catheter. July/August 2011 Nursing made Incredibly Easy! 33
7 Picturing testicular cancer Vas deferens Staging The overall prognosis for each patient is significantly impacted by the stage of the disease and the type of tumor. The testicles produce both testosterone and sperm. The germ cells in the testicles produce immature sperm cells that travel through the tubules and are stored in the epididymis as they mature. Most (95%) testicular cancers are germ cell tumors and are divided into two main types: seminomas and nonseminomas. Seminoma tumors are more sensitive to radiation. Nonseminoma tumors are more aggressive and likely to spread to other parts of the body. The earlier the disease is identified, the more positive the prognosis (see The International Germ Cell Consensus Classification). The results are in... The ultrasound shows that the lump in Mr. T s left testicle is a solid mass. Fortunately for Mr. T, his cancer is identified as Stage I seminoma, which has a cure rate of greater than 95%. The initial tumor markers are elevated, and after discussion with his physician, Mr. T decides to pursue surgery with a radical inguinal orchiectomy. Although removal of a testicle seems like an extreme approach, biopsy of the testicle through the scrotum is generally not performed due to the risk of the biopsy puncture spreading cancer to other tissues. In some cases, when the tumor markers are normal but the ultrasound identifies a nonpalpable mass, a biopsy may be done to determine the need for the orchiectomy. The testicle is surgically removed and the tissue samples are analyzed by the lab to determine if the cells are cancerous. Before the surgery, Mr. T elects to cryopreserve semen as a precautionary measure. Many testicular cancer patients have sperm abnormalities before treatment and will be oligospermic during chemotherapy. However, a study has shown that 70% of patients were able to father children following treatment. Post-op care is relatively routine following orchiectomy. You ll facilitate pain control and wound management. Provide ice packs to the groin for 15 to 20 minutes every hour to help with the swelling. An athletic supporter may also help with comfort. Testicular cancer Epididymis Testis Treatment options In addition to orchiectomy, a plan consisting of frequent monitoring, chemotherapy, or radiation therapies will be considered. The physician and patient will discuss the best options based on the stage of the cancer cells, whether the tumor is seminoma or nonseminoma, and the tumor marker levels. Treatment options for Stage I testicular cancers include: 34 Nursing made Incredibly Easy! July/August
8 The International Germ Cell Consensus Classification Good prognosis Nonseminoma Seminoma Percentage Assessment/involvement Survival rate 56% to 61% of nonseminomas 90% of seminomas Intermediate prognosis Nonseminoma 13% to 28% of nonseminomas Seminoma Poor prognosis Nonseminoma 10% of seminomas 16% to 26% of nonseminomas Testis/retroperitoneal primary, and No nonpulmonary visceral metastases, and Good markers: Alpha-fetoprotein (AFP) less than 1,000 ng/ml Human chorionic gonadotropin (hcg) less than 1,000 ng/ml Lactate dehydrogenase (LDH) less than 1.5 times the upper limit of normal Any primary site, and no nonpulmonary visceral metastases, and normal AFP, any hcg, any LDH Testis/retroperitoneal primary, and No nonpulmonary visceral metastases, and Intermediate markers: AFP 1,000 ng/dl or more hcg 1,000 ng/dl or more LDH 1.5 times the upper limit of normal or more Any primary site, and Nonpulmonary visceral metastases, and Normal AFP, any hcg, any LDH Mediastinal primary, or Nonpulmonary visceral metastases, or Poor markers: AFP more than 10,000 ng/ml hcg more than 10,000 ng/ml LDH more than 10 times the upper limit of normal This is a sample speech pillow that will say clever things. 5-year progressionfree survival (PFS) is 89% 5-year survival is 92% to 94% 5-year PFS is 82% 5-year survival is 86% 5-year PFS is 75% 5-year survival is 80% to 83% 5-year PFS is 67% 5-year survival is 72% 5-year PFS is 41% 5-year survival is 71% Seminoma No patients are classified as poor prognosis Source: International Germ Cell Consensus Classification: a prognostic factor-based staging system for metastatic germ cell cancers. International Germ Cell Cancer Collaborative Group. J Clin Oncol. 1997;15(2): Stage I seminoma radical inguinal orchiectomy, no radiation, and frequent monitoring radical inguinal orchiectomy, followed by single-dose carboplatin adjuvant therapy radical inguinal orchiectomy followed by radiation therapy Stage 1 nonseminoma radical inguinal orchiectomy with retroperitoneal lymph node dissection (RPLND) radical inguinal orchiectomy with no RPLND, followed by exams every 1 to 2 months, serum marker tests, and periodic CT scan evaluations. Keeping up with our patient After considering the treatment options, Mr. T and his physician decide to follow a treatment plan that involves only frequent monitoring versus additional chemotherapy or radiation. Mr. T agrees to follow the July/August 2011 Nursing made Incredibly Easy! 35
9 After testicular cancer treatment, your patient requires lifelong monitoring. recommended plan and is discharged home with instructions. Recommended follow-up after testicular cancer treatment includes: year one monthly serum marker tests, chest X-rays, and physical exam year two bimonthly serum marker tests, chest X-rays, and physical exam lifelong serum markers, chest X-rays, and monthly physical exams. Periodic CT scans are also recommended. Penile cancer Mr. K notes a sore that hasn t healed near the tip of his penis. Finally, after many months and the development of a lump, he agrees to see a physician. Mr. K s history reveals that he has chronic phimosis (the foreskin can t be pulled back over the glans), has had several sexual partners, has smoked since he was age 14, and appears to have poor personal hygiene. All of these are risk factors for developing penile cancer. Because this type of cancer has a wide variety of ways it can present, the physician who examines Mr. K is concerned about the possibility of the lesion being cancerous. Testing for penile cancer Mr. K agrees to a biopsy of the area. After receiving a local anesthetic, a small tissue sample from the area and some of the fluid and cells from the growth are taken. These will be sent to a pathologist for evaluation. In addition, a urethroscopy and MRI are performed to evaluate the lesion and possible metastasis. Staging The Tumor Node Metastasis, or TNM, staging system is used to stage penile cancer (see Staging penile cancer). The results are in... Most penile malignancies are squamous cell carcinomas, and Mr. K s is no exception. Unfortunately, Mr. K s cancer has progressed beyond carcinoma in situ (premetastatic stage), but hasn t invaded the lymph nodes and isn t poorly differentiated (T1a, N0, M0). Treatment options One of the challenges of determining the best treatment option for penile cancer is identifying the best option to remove the risk of cancer reoccurring and preserving as much normal function of the organ as possible. Similar to other cancers, the treatment options that are considered for penile cancer include surgery, radiation therapy, and chemotherapy. Surgical options include: Mohs micrographic surgery. In Mohs microsurgery, very thin layers of skin are removed. After each layer is removed, it s viewed under a microscope to check for cancerous cells. This procedure allows the surgeon to take just enough tissue to remove the cancerous cells while leaving as much healthy tissue as possible to retain normal function. partial or total penectomy. Depending on the involvement of the surrounding tissues, surgical treatment may involve a partial penectomy (removal of any part of the penis) or a total penectomy (removal of the entire penis). The goal is to preserve as much urinary and sexual function as possible; however, if the surgery compromises the patient s ability to urinate, the surgeon will create a perineal urethrostomy. The urethra is diverted to the perineal area between the scrotum and the anus. The patient would then need to sit when urinating. Radiation therapy can be used to treat early-stage penile cancer instead of surgery, in addition to surgery to reduce the risk of reoccurrence, or in advanced cancer to try to slow cancer growth or relieve symptoms. Men who ll be receiving radiation who aren t already circumcised are circumcised to prevent swelling and constriction of the foreskin during treatment. The types of radiation therapy that are considered for penile cancer include: 36 Nursing made Incredibly Easy! July/August
10 external beam radiation. This type is given 5 days a week over a period of approximately 6 weeks. brachytherapy. This type of interstitial radiation allows for the radioactive material to be placed right next to the tumor. The radiation only impacts a relatively small area so the other tissues are relatively safe. Hollow needles are placed in the penis and tiny radioactive pellets are then inserted through the needles. These pellets remain in place for several days and then the needles are removed. plesiobrachytherapy. This type of brachytherapy utilizes plastic cylinders around the penis or a mold of the penis to hold the radioactive material in place for several days. More research is needed regarding cytotoxic drugs to treat penile cancer. The available studies have been limited and the results have been somewhat inconclusive. However, cisplatin, bleomycin, and methotrexate are three examples of drugs that have been used with some success. Keeping up with our patient The surgeon is able to perform a partial penectomy with the hope of preserving Mr. K s sexual and urinary functions. If his residual penile length hadn t been able to be preserved, a perineal urethrostomy would ve been performed. Due to difficulty with healthcare access for Mr. K, the decision is made for brachytherapy following the penectomy. If there had been evidence that the disease had progressed farther, chemotherapy agents, such as cisplatin, bleomycin, methotrexate, or vincristine, would ve been considered. Following surgery and 5 days of interstitial radiation and hospitalization, Mr. K is discharged home with instructions for wound care, pain, and a follow-up visit within a week. The effects of the brachytherapy may be worse in 1 to 2 weeks, so Mr. K is taught to be aware of changes in the penis and the surrounding tissues and to notify the physician of any problems. A prescription to Staging penile cancer Stage 0 (carcinoma in situ) In stage 0, abnormal cells are found on the surface of the skin of the penis. These abnormal cells may become cancer and spread into nearby normal tissue. Stage 0 is also called carcinoma in situ. Stage I In stage I, cancer has formed and spread to connective tissue just under the skin of the penis. Stage II In stage II, cancer has spread to: connective tissue just under the skin of the penis and to one lymph node in the groin or erectile tissue (spongy tissue that fills with blood to make an erection), and may have spread to one lymph node in the groin. Stage III In stage III, cancer has spread to: connective tissue or erectile tissue of the penis and to more than one lymph node on one or both sides of the groin or the urethra or prostate, and may have spread to one or more lymph nodes on one or both sides of the groin. Stage IV In stage IV, cancer has spread to: tissues near the penis and may have spread to lymph nodes in the groin or pelvis or anywhere in or near the penis and to one or more lymph nodes deep in the pelvis or groin or distant parts of the body. Source: Cleveland Clinic. Stages of penile cancer. disorders/penile_cancer/hic_penile_cancer.aspx. address potential nausea and GI upset is also given to Mr. K. At the post-op visit, it s assessed that his urinary functions have continued to remain intact. Sexual function won t be assessed for several more weeks. Get equipped! No matter in which geographical location you work, reproductive cancer has the chance of impacting your patients. Being aware of the risk factors, signs and symptoms, assessment findings, and treatment options can help you become more comfortable with this sometimes uncomfortable men s health topic and better equipped to be a strong patient advocate. July/August 2011 Nursing made Incredibly Easy! 37
11 The more CE, the merrier! Learn more about it Brydøy M, Fosså SD, Klepp O, et al. Paternity following treatment for testicular cancer. J Natl Cancer Inst. 2005;97(21): Delacroix SE Jr, Pettaway CA. Therapeutic strategies for advanced penile carcinoma. Curr Opin Support Palliat Care. 2010;4(4): Gleason Score: Prostate and Male Health Resource. Gleason Score. Hegarty PK, Rees RW, Borley NC, Ralph DJ, Minhas S. Contemporary management of penile cancer. BJU Int. 2008;102(8): International Germ Cell Consensus Classification: a prognostic factor-based staging system for metastatic germ cell cancers. International Germ Cell Cancer Collaborative Group. J Clin Oncol. 1997;15(2): Lynch DF. Carcinoma of the penis: Diagnosis, treatment, and prognosis. carcinoma-of-the-penis-diagnosis-treatment-andprognosis. National Cancer Institute. Prostate-specific antigen (PSA) test. detection/psa#r4. National Cancer Institute. SEER stat fact sheets: Testis. Pathophysiology Made Incredibly Visual! Philadelphia, PA: Lippincott Williams & Wilkins; 2008:238,240. Pizzocaro G, Algaba F, Horenblas S, et al. European Association of Urology guidelines on penile cancer. Prostate Cancer Foundation. Understanding prostate cancer. b /k.d271/prostate_cancer_risk_factors.htm. Rossari JR, Vora T, Gil T. Advances in penile cancer management. Curr Opin Oncol. 2010;23(3): Steele GS, Richie JP, Oh WK, Michaelson MD. Clinical manifestations, diagnosis, and staging of testicular germ cell tumors. DOI /01.NME dc For more than 57 additional continuing education articles related to cancer topics, go to Nursingcenter.com/CE. TEST INSTRUCTIONS To take the test online, go to our secure Web site at CE/nmie. On the print form, record your answers in the test answer section of the CE enrollment form on page 54. Each question has only one correct answer. You may make copies of these forms. Complete the registration information and course evaluation. Mail the completed form and registration fee of $24.95 to: Lippincott Williams & Wilkins, CE Group, 2710 Yorktowne Blvd., Brick, NJ We will mail your certificate in 4 to 6 weeks. For faster service, include a fax number and we will fax your certificate within 2 business days of receiving your enrollment form. You will receive your CE certificate of earned contact hours and an answer key to review your results.there is no minimum passing grade. Registration deadline is August 31, INSTRUCTIONS The ABCs of male reproductive cancer Earn CE credit online: Go to and receive a certificate within minutes. DISCOUNTS and CUSTOMER SERVICE Send two or more tests in any nursing journal published by Lippincott Williams & Wilkins together by mail and deduct $0.95 from the price of each test. We also offer CE accounts for hospitals and other health care facilities on nursingcenter. com. Call for details. PROVIDER ACCREDITATION Lippincott Williams & Wilkins, publisher of Nursing made Incredibly Easy!, will award 2.5 contact hours for this continuing nursing education activity. Lippincott Williams & Wilkins is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. This activity is also provider approved by the California Board of Registered Nursing, Provider Number CEP for 2.5 contact hours. Lippincott Williams & Wilkins is also an approved provider of continuing nursing education by the District of Columbia and Florida #FBN2454. Your certificate is valid in all states. The ANCC s accreditation status of Lippincott Williams & Wilkins Department of Continuing Education refers only to its continuing nursing educational activities and does not imply Commission on Accreditation approval or endorsement of any commercial product. 38 Nursing made Incredibly Easy! July/August
Testicular Cancer: Questions and Answers. Testicular cancer is a disease in which cells become malignant (cancerous) in one or both testicles.
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Testicular Cancer: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Testicular Cancer: Questions
What is Testicular cancer?
 Testicular Cancer What is Testicular cancer? Testicular cancer is a disease in which cancer cells form in the tissues of one or both testicles. The testicles are 2 egg-shaped glands located inside the
Testicular Cancer What is Testicular cancer? Testicular cancer is a disease in which cancer cells form in the tissues of one or both testicles. The testicles are 2 egg-shaped glands located inside the
General information about prostate cancer
 Prostate Cancer General information about prostate cancer Key points Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the prostate. Signs of prostate cancer include
Prostate Cancer General information about prostate cancer Key points Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the prostate. Signs of prostate cancer include
PROSTATE CANCER CONTENT CREATED BY. Learn more at
 PROSTATE CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Ask your doctor about screening and treatment options. WHAT IS PROSTATE CANCER? 4 WATCHFUL
PROSTATE CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Ask your doctor about screening and treatment options. WHAT IS PROSTATE CANCER? 4 WATCHFUL
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
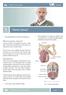 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
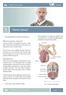 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen).
 What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
LIVING WITH. Understanding Your Treatment Options 1510
 Get the Support You Need Having prostate cancer can be hard to cope with. But you don t have to keep your feelings to yourself. Talk with family and friends. Try a prostate cancer support group. Sharing
Get the Support You Need Having prostate cancer can be hard to cope with. But you don t have to keep your feelings to yourself. Talk with family and friends. Try a prostate cancer support group. Sharing
Introduction. Growths in the prostate can be benign (not cancer) or malignant (cancer).
 This information was taken from urologyhealth.org. Feel free to explore their website to learn more. Another trusted website with good information is the national comprehensive cancer network (nccn.org).
This information was taken from urologyhealth.org. Feel free to explore their website to learn more. Another trusted website with good information is the national comprehensive cancer network (nccn.org).
BLADDER PROSTATE PENIS TESTICLES BE YO ND YO UR CA NC ER
 BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
Chapter 18: Glossary
 Chapter 18: Glossary Sutter Health Cancer Service Line: Prostate Committee Advanced cancer: When the cancer has spread to other parts of the body (including lymph nodes, bones, or other organs) and is
Chapter 18: Glossary Sutter Health Cancer Service Line: Prostate Committee Advanced cancer: When the cancer has spread to other parts of the body (including lymph nodes, bones, or other organs) and is
Patient Information. Prostate Tissue Ablation. High Intensity Focused Ultrasound for
 High Intensity Focused Ultrasound for Prostate Tissue Ablation Patient Information CAUTION: Federal law restricts this device to sell by or on the order of a physician CONTENT Introduction... 3 The prostate...
High Intensity Focused Ultrasound for Prostate Tissue Ablation Patient Information CAUTION: Federal law restricts this device to sell by or on the order of a physician CONTENT Introduction... 3 The prostate...
Prostate Cancer. What is prostate cancer?
 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Prostate Cancer. What is prostate cancer?
 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum, below the bladder and above the base of the penis. Your doctor may perform
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum, below the bladder and above the base of the penis. Your doctor may perform
We are gong to focus on: Unit 9. Before we begin: Chronic Renal Failure/Uremia ESRD/Dialysis Prostate Cancer Testicular Cancer Renal Cancer
 Unit 9 Problems with excretion Before we begin: You are to understand on your own: A & P of Renal System Common terms of renal system How to perform a focused health history How to perform a Physical Exam
Unit 9 Problems with excretion Before we begin: You are to understand on your own: A & P of Renal System Common terms of renal system How to perform a focused health history How to perform a Physical Exam
Testicular Cancer. What is testicular cancer? What are the symptoms? Patient Information. Risk factors for testicular cancer.
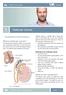 Patient Information English 31 Testicular Cancer The underlined terms are listed in the glossary. What is testicular cancer? The testicles (also called the testes ) are part of the male reproductive system
Patient Information English 31 Testicular Cancer The underlined terms are listed in the glossary. What is testicular cancer? The testicles (also called the testes ) are part of the male reproductive system
Your Guide to Prostate Cancer
 Your Guide to Prostate Cancer If you face a diagnosis of prostate cancer, what s next? We can help. A prostate cancer diagnosis can be overwhelming. The good news is that while prostate cancer can be serious,
Your Guide to Prostate Cancer If you face a diagnosis of prostate cancer, what s next? We can help. A prostate cancer diagnosis can be overwhelming. The good news is that while prostate cancer can be serious,
Information for Patients. Testicular Cancer. English
 Information for Patients Testicular Cancer English Table of contents What is testicular cancer?... 3 What are the symptoms?... 3 How is testicular cancer diagnosed?... 3 What is staging?... 4 Stages of
Information for Patients Testicular Cancer English Table of contents What is testicular cancer?... 3 What are the symptoms?... 3 How is testicular cancer diagnosed?... 3 What is staging?... 4 Stages of
1: : Lifetime risk for prostate cancer 1:27. Lifetime risk for. testicular cancer. Lifetime risk for. penile cancer
 *Based on the National Cancer Registry of 2010 Lifetime risk for prostate cancer 1:27 Lifetime risk for testicular cancer Lifetime risk for penile cancer 1:2 040 1:1 114 Prostate cancer 1 in 27 South African
*Based on the National Cancer Registry of 2010 Lifetime risk for prostate cancer 1:27 Lifetime risk for testicular cancer Lifetime risk for penile cancer 1:2 040 1:1 114 Prostate cancer 1 in 27 South African
PROSTATE CANCER. What is Prostate Cancer?
 1 Medical Topics - Prostate Cancer PROSTATE CANCER What is Prostate Cancer? Prostate cancer is cancer that occurs in a man's prostate a small walnut-shaped gland that produces the seminal fluid that nourishes
1 Medical Topics - Prostate Cancer PROSTATE CANCER What is Prostate Cancer? Prostate cancer is cancer that occurs in a man's prostate a small walnut-shaped gland that produces the seminal fluid that nourishes
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Prostate Cancer Case Study 1. Medical Student Case-Based Learning
 Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer. David Wilkinson MD Gulfshore Urology
 Prostate Cancer David Wilkinson MD Gulfshore Urology What is the Prostate? Male Sexual Gland Adds nutrients and fluids for sperm This fluid is added to sperm during ejaculation Urethra (urine channel)
Prostate Cancer David Wilkinson MD Gulfshore Urology What is the Prostate? Male Sexual Gland Adds nutrients and fluids for sperm This fluid is added to sperm during ejaculation Urethra (urine channel)
Chapter 2. Understanding My Diagnosis
 Chapter 2. Understanding My Diagnosis With contributions from Nancy L. Brown, Ph.D.,Palo Alto Medical Foundation Research Institute; and Patrick Swift, M.D., Alta Bates Comprehensive Cancer Program o Facts
Chapter 2. Understanding My Diagnosis With contributions from Nancy L. Brown, Ph.D.,Palo Alto Medical Foundation Research Institute; and Patrick Swift, M.D., Alta Bates Comprehensive Cancer Program o Facts
Prostate Cancer Awareness - Prevention, Symptoms and. Treatment
 Quality Assurance Lunch and Learn Sessions: Prostate Cancer Awareness - Prevention, Symptoms and What s wrong with my prostate? Treatment??? Sponsored by the Chief Engineer s Team and Quality Assurance
Quality Assurance Lunch and Learn Sessions: Prostate Cancer Awareness - Prevention, Symptoms and What s wrong with my prostate? Treatment??? Sponsored by the Chief Engineer s Team and Quality Assurance
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 34 Caring for Male Clients with Reproductive System Disorders Benign Prostatic Hyperplasia (BPH) Testosterone
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 34 Caring for Male Clients with Reproductive System Disorders Benign Prostatic Hyperplasia (BPH) Testosterone
Prostate Cancer. Diagnosis and Treatment. September 2016 Saskatchewan Prostate Assessment Pathway
 Prostate Cancer Diagnosis and Treatment September 016 Saskatchewan Prostate Assessment Pathway Table of Contents Introduction... Patient and Coach Information... Nurse Navigators... About Your Prostate...
Prostate Cancer Diagnosis and Treatment September 016 Saskatchewan Prostate Assessment Pathway Table of Contents Introduction... Patient and Coach Information... Nurse Navigators... About Your Prostate...
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer overview Prostate cancer is the most common form of cancer in American men, most prevalent in men over age 65 and fairly common in men 50-64
Scan for mobile link. Prostate Cancer Treatment Prostate cancer overview Prostate cancer is the most common form of cancer in American men, most prevalent in men over age 65 and fairly common in men 50-64
Esophageal Cancer. Source: National Cancer Institute
 Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Prostate Cancer: Low Dose Rate (Seed) Brachytherapy. Information for patients, families and friends
 Prostate Cancer: Low Dose Rate (Seed) Brachytherapy Information for patients, families and friends About this booklet This booklet is designed to give you information about low dose-rate (seed) brachytherapy
Prostate Cancer: Low Dose Rate (Seed) Brachytherapy Information for patients, families and friends About this booklet This booklet is designed to give you information about low dose-rate (seed) brachytherapy
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
General Information Key Points
 The content of this booklet was adapted from content originally published by the National Cancer Institute. Male Breast Cancer Treatment (PDQ ) Patient Version. Updated September 29,2017. https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq
The content of this booklet was adapted from content originally published by the National Cancer Institute. Male Breast Cancer Treatment (PDQ ) Patient Version. Updated September 29,2017. https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Date of preparation- January 2018 Janssen Biotech, Inc /18 em Reporter s guide to. prostate cancer
 Date of preparation- January 2018 Janssen Biotech, Inc. 2018 02/18 em-01856 Reporter s guide to prostate cancer What is the prostate? The prostate is a gland located below the bladder, wrapped around the
Date of preparation- January 2018 Janssen Biotech, Inc. 2018 02/18 em-01856 Reporter s guide to prostate cancer What is the prostate? The prostate is a gland located below the bladder, wrapped around the
Appendix D Answers to the KAP Survey
 From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
From Trainer s Resource Book to accompany Management of Men s Reproductive Health Problems 2003 EngenderHealth Appendix D Answers to the KAP Survey In the answer key that follows: The answers appear in
A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW
 A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW 1. Why men need to know more Good health is vital for a happy and full life. But, with work and family responsibilities, men often overlook their own health
A USER S GUIDE WHAT EVERY MAN NEEDS TO KNOW 1. Why men need to know more Good health is vital for a happy and full life. But, with work and family responsibilities, men often overlook their own health
Testicular Malignancies /8/15
 Collecting Cancer Data: Testis 2014-2015 NAACCR Webinar Series January 8, 2015 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data: Testis 2014-2015 NAACCR Webinar Series January 8, 2015 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Definition Prostate cancer
 Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
ADVICE TO PATIENTS REQUESTING PSA MEASUREMENT
 Frequently-Asked Questions What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication of prostate cancer, is available to you if you want
Frequently-Asked Questions What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication of prostate cancer, is available to you if you want
ADVICE TO PATIENTS REQUESTING PSA MEASUREMENT FREQUENTLY-ASKED QUESTIONS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk ADVICE TO
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk ADVICE TO
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Information for Patients. Primary urethral cancer. English
 Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Wilms' tumor most often occurs in just one kidney, though it can sometimes be found in both kidneys at the same time.
 Wilms' Tumor Wilms' tumor is a rare kidney cancer that primarily affects children. Also known as nephroblastoma, Wilms' tumor is the most common cancer of the kidneys in children. Wilms' tumor most often
Wilms' Tumor Wilms' tumor is a rare kidney cancer that primarily affects children. Also known as nephroblastoma, Wilms' tumor is the most common cancer of the kidneys in children. Wilms' tumor most often
Prostate cancer. A guide for men who ve just been diagnosed
 Prostate cancer A guide for men who ve just been diagnosed 2 Prostate cancer A guide for men who ve just been diagnosed About this booklet This booklet is for men who ve recently been diagnosed with prostate
Prostate cancer A guide for men who ve just been diagnosed 2 Prostate cancer A guide for men who ve just been diagnosed About this booklet This booklet is for men who ve recently been diagnosed with prostate
When should I ask my doctor about my fertility?
 Preserving Fertility for Men with Cancer Some cancers and their treatments can affect a man s ability to father a child (his fertility). These changes can last for a short time, or may be permanent. This
Preserving Fertility for Men with Cancer Some cancers and their treatments can affect a man s ability to father a child (his fertility). These changes can last for a short time, or may be permanent. This
When to worry, when to test?
 Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
AllinaHealthSystems 1
 2018 Dimensions in Oncology Genitourinary Cancer Disclosures I have no financial or commercial relationships relevant to this presentation. Matthew O Shaughnessy, MD, PhD Director of Urologic Oncology
2018 Dimensions in Oncology Genitourinary Cancer Disclosures I have no financial or commercial relationships relevant to this presentation. Matthew O Shaughnessy, MD, PhD Director of Urologic Oncology
Cardiff MRCS OSCE Courses Testicular Cancer
 Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Ultrasound - Prostate
 Scan for mobile link. Ultrasound - Prostate Ultrasound of the prostate uses sound waves to produce pictures of a man s prostate gland and to help diagnose symptoms such as difficulty urinating or an elevated
Scan for mobile link. Ultrasound - Prostate Ultrasound of the prostate uses sound waves to produce pictures of a man s prostate gland and to help diagnose symptoms such as difficulty urinating or an elevated
Information for Patients. Prostate cancer. English
 Information for Patients Prostate cancer English Table of contents What is prostate cancer?... 3 The role of hormones in prostate cancer cell growth... 3 Stages of the disease... 3 Risk factors for prostate
Information for Patients Prostate cancer English Table of contents What is prostate cancer?... 3 The role of hormones in prostate cancer cell growth... 3 Stages of the disease... 3 Risk factors for prostate
Localized Prostate Cancer Have we finally got it right? Shingai Mutambirwa Professor & Chair-Division Urology DGMAH & SMU Pretoria SOUTH AFRICA
 Localized Prostate Cancer Have we finally got it right? Shingai Mutambirwa Professor & Chair-Division Urology DGMAH & SMU Pretoria SOUTH AFRICA ESMO Cape Town 14 Feb 2018 Disclosures Advisory boards/lecturer/consultant-
Localized Prostate Cancer Have we finally got it right? Shingai Mutambirwa Professor & Chair-Division Urology DGMAH & SMU Pretoria SOUTH AFRICA ESMO Cape Town 14 Feb 2018 Disclosures Advisory boards/lecturer/consultant-
What are Varicoceles?
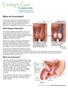 What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
What are Varicoceles? A varicocele is when veins become enlarged inside your scrotum (the pouch of skin that holds your testicles). These veins are called the pampiniform plexus. Ten to 15 of every 100
Localized Prostate Cancer and Its Treatment- A Patient Guide
 Your Health Matters Localized Prostate Cancer and Its Treatment- A Patient Guide Department of Urology UCSF Helen Diller Family Comprehensive Cancer Center University of California. San Francisco 550 16th
Your Health Matters Localized Prostate Cancer and Its Treatment- A Patient Guide Department of Urology UCSF Helen Diller Family Comprehensive Cancer Center University of California. San Francisco 550 16th
Clinical Diagnosis. your PR.i.VATES.
 your PR.i.VATES Clinical Diagnosis What is an orchidectomy? What to expect after orchidectomy Results and Confirmed Diagnosis What is the lymphatic system? www.yourprivates.org.uk CONTENTS CLINICAL DIAGNOSIS
your PR.i.VATES Clinical Diagnosis What is an orchidectomy? What to expect after orchidectomy Results and Confirmed Diagnosis What is the lymphatic system? www.yourprivates.org.uk CONTENTS CLINICAL DIAGNOSIS
Testicular Biopsy and Sperm Extraction for Fertility Preservation
 Testicular Biopsy and Sperm Extraction for Fertility Preservation This fact sheet aims to provide information about why and when a testicular biopsy or aspiration might be offered, what it involves and
Testicular Biopsy and Sperm Extraction for Fertility Preservation This fact sheet aims to provide information about why and when a testicular biopsy or aspiration might be offered, what it involves and
Esophageal cancer. What is esophageal cancer? Esophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the esophagus.
 Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
Esophageal Cancer Esophageal cancer What is esophageal cancer? What are risk factors? Signs and symptoms Tests for esophageal cancer Stages of esophageal cancer Treatment options What is esophageal cancer?
UNDERSTANDING. Permanent Birth Control for Men
 UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
QUESTIONS TO ASK A UROLOGIST
 QUESTIONS TO ASK A UROLOGIST For the patient: You should review these questions and determine if the answers would satisfy a better understanding of what to expect and ease your concerns. If there are
QUESTIONS TO ASK A UROLOGIST For the patient: You should review these questions and determine if the answers would satisfy a better understanding of what to expect and ease your concerns. If there are
In some cases, a medical evaluation may be needed, to be performed by your primary care physician about 2-4 weeks prior to surgery.
 Robotic Assisted Laparoscopic Prostatectomy Information Sheet Preoperative Events: You will have a consultation appointment with one of the robotic surgeons. We will try to schedule this within a month
Robotic Assisted Laparoscopic Prostatectomy Information Sheet Preoperative Events: You will have a consultation appointment with one of the robotic surgeons. We will try to schedule this within a month
PROSTATE HEALTH. Non-metastatic CastrationResistant Prostate Cancer. (nmcrpc) Patient Guide
 PROSTATE HEALTH Non-metastatic CastrationResistant Prostate Cancer (nmcrpc) Patient Guide Table of Contents Prostate Health Committee Introduction Introduction.... 3 GET THE FACTS How Does the Prostate
PROSTATE HEALTH Non-metastatic CastrationResistant Prostate Cancer (nmcrpc) Patient Guide Table of Contents Prostate Health Committee Introduction Introduction.... 3 GET THE FACTS How Does the Prostate
Cancer , The Patient Education Institute, Inc. ocf80101 Last reviewed: 06/08/2016 1
 Cancer Introduction Cancer begins in your cells, which are the building blocks of your body. Extra cells can form a mass called a tumor. Some tumors aren t cancerous, while other ones are. Cells from cancerous
Cancer Introduction Cancer begins in your cells, which are the building blocks of your body. Extra cells can form a mass called a tumor. Some tumors aren t cancerous, while other ones are. Cells from cancerous
Cervical cancer is a disease in which malignant (cancer) cells form in the tissues of the cervix.
 Cervical Cancer Cervical cancer is a disease in which malignant (cancer) cells form in the tissues of the cervix. The cervix is the lower, narrow end of the uterus (the hollow, pear-shaped organ where
Cervical Cancer Cervical cancer is a disease in which malignant (cancer) cells form in the tissues of the cervix. The cervix is the lower, narrow end of the uterus (the hollow, pear-shaped organ where
GUIDELINES ON TESTICULAR CANCER
 38 (Text updated March 2005) P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro Introduction Compared with other types of cancer
38 (Text updated March 2005) P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro Introduction Compared with other types of cancer
A schematic of the rectal probe in contact with the prostate is show in this diagram.
 Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
About the authors Dr S. Larry Goldenberg Dr Tom Pickles Dr Kim N. Chi
 Authors S. Larry Goldenberg, CM, OBC, MD, FRCSC, FCAHS Professor and Head, University of British Columbia Department of Urologic Sciences, Stephen A. Jarislowski Chair in Urologic Sciences at Vancouver
Authors S. Larry Goldenberg, CM, OBC, MD, FRCSC, FCAHS Professor and Head, University of British Columbia Department of Urologic Sciences, Stephen A. Jarislowski Chair in Urologic Sciences at Vancouver
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Case Scenario 1 Discharge Summary Pathology Report Final Diagnosis: Oncology Consult
 Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Testicular Cancer. What is cancer?
 What is cancer? Testicular Cancer The body is made up of trillions of living cells. Normal body cells grow, divide, and die in an orderly fashion. During the early years of a person's life, normal cells
What is cancer? Testicular Cancer The body is made up of trillions of living cells. Normal body cells grow, divide, and die in an orderly fashion. During the early years of a person's life, normal cells
Vaginal cancer: Know what to expect
 Vaginal cancer: Know what to expect For women with vaginal cancer What is the vagina? The vagina is a hollow canal that connects the cervix and the uterus to the outside. of the body. When a woman gives
Vaginal cancer: Know what to expect For women with vaginal cancer What is the vagina? The vagina is a hollow canal that connects the cervix and the uterus to the outside. of the body. When a woman gives
The prostate can be affected by three conditions that may cause problems for men as they get older.
 The Prostate Gland The Prostate gland specific to males only, located in the pelvis between the bladder and rectum. It is about the shape and size of a walnut or satsuma and gets bigger as you get older.
The Prostate Gland The Prostate gland specific to males only, located in the pelvis between the bladder and rectum. It is about the shape and size of a walnut or satsuma and gets bigger as you get older.
Every year in the UK over 50,000 men will be diagnosed with a male-specific cancer: prostate, testicular or penile.
 Every year in the UK over 50,000 men will be diagnosed with a male-specific cancer: prostate, testicular or penile. This leaflet offers information on the three cancers from signs and symptoms, risk factors
Every year in the UK over 50,000 men will be diagnosed with a male-specific cancer: prostate, testicular or penile. This leaflet offers information on the three cancers from signs and symptoms, risk factors
Male Cancer. Awareness, diagnosis and treatment. Revised 4th Edition
 Male Cancer Awareness, diagnosis and treatment Revised 4th Edition 2 Every year in the UK over 50,000 men will be diagnosed with a male-specific cancer: prostate, testicular or penile. This leaflet offers
Male Cancer Awareness, diagnosis and treatment Revised 4th Edition 2 Every year in the UK over 50,000 men will be diagnosed with a male-specific cancer: prostate, testicular or penile. This leaflet offers
Taking Care of Your Sexual Health
 Sexual health is an important part of overall health. Taking responsibility for caring for their sexual health will help men and women stay healthy for a lifetime. Things for Everyone to Know Staying Clean
Sexual health is an important part of overall health. Taking responsibility for caring for their sexual health will help men and women stay healthy for a lifetime. Things for Everyone to Know Staying Clean
Case Scenario 1 Discharge Summary Pathology Report Final Diagnosis: Oncology Consult
 Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
CANCER. Mrs. Davis Health Education
 CANCER Mrs. Davis Health Education Cancer Terms: Tumors: Masses of useless tissue Benign: Non-cancerous Malignant: Cancerous Metastasis: Spread of cancer from the point where it originated to other parts
CANCER Mrs. Davis Health Education Cancer Terms: Tumors: Masses of useless tissue Benign: Non-cancerous Malignant: Cancerous Metastasis: Spread of cancer from the point where it originated to other parts
PCSANM 2015 Seminar. Basic Knowledge: Test for Prostate Cancer. Jerry Cross. 15 item quiz, no grades given
 Basic Knowledge: Test for Prostate Cancer Jerry Cross 15 item quiz, no grades given Basic Knowledge: Test for Prostate Cancer From http://prostatesnatchers.blogspot.com/ January 27, 2015 BY MARK SCHOLZ,
Basic Knowledge: Test for Prostate Cancer Jerry Cross 15 item quiz, no grades given Basic Knowledge: Test for Prostate Cancer From http://prostatesnatchers.blogspot.com/ January 27, 2015 BY MARK SCHOLZ,
Doppler ultrasound of the abdomen and pelvis, and color Doppler
 - - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
- - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
Chapter 7. Male Reproductive System. Copyright 2018 Elsevier Inc. All rights reserved.
 Chapter 7 Male Reproductive System Chapter 7 Objective 1: Pronounce organs and anatomic structures of the male reproductive system. Organs (1 of 2) The organs of the male reproductive system include the
Chapter 7 Male Reproductive System Chapter 7 Objective 1: Pronounce organs and anatomic structures of the male reproductive system. Organs (1 of 2) The organs of the male reproductive system include the
Questions and Answers About the Prostate-Specific Antigen (PSA) Test
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Questions and Answers
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Questions and Answers
Bladder Cancer Early Detection, Diagnosis, and Staging
 Bladder Cancer Early Detection, Diagnosis, and Staging Detection and Diagnosis Catching cancer early often allows for more treatment options. Some early cancers may have signs and symptoms that can be
Bladder Cancer Early Detection, Diagnosis, and Staging Detection and Diagnosis Catching cancer early often allows for more treatment options. Some early cancers may have signs and symptoms that can be
BOWEL CANCER. Causes of bowel cancer
 A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
Santa Clara. Prostate Cancer Care Multidisciplinary Clinic. Discharge planning begins upon admission. kp.org
 Santa Clara Prostate Cancer Care Multidisciplinary Clinic Discharge planning begins upon admission. kp.org Table of Contents Introduction...ii The Prostate Gland...1 Anatomy of the Prostate Gland...2 Prostate
Santa Clara Prostate Cancer Care Multidisciplinary Clinic Discharge planning begins upon admission. kp.org Table of Contents Introduction...ii The Prostate Gland...1 Anatomy of the Prostate Gland...2 Prostate
Breast Imaging & You
 Breast Imaging & You What s Inside: Breast Imaging... 2 Digital Breast Tomosynthesis (DBT) mammograms... 4 Breast cancer screening... 6 Dense breast tissue... 8 Automated Breast Ultrasound (ABUS)... 9
Breast Imaging & You What s Inside: Breast Imaging... 2 Digital Breast Tomosynthesis (DBT) mammograms... 4 Breast cancer screening... 6 Dense breast tissue... 8 Automated Breast Ultrasound (ABUS)... 9
Prostate Gland Disorders
 Prostate Gland Disorders THE PROSTATE GLAND A male s prostate gland is located in the floor of the pelvis surrounding the urethra between the bladder and the penis. The prostate is positioned immediately
Prostate Gland Disorders THE PROSTATE GLAND A male s prostate gland is located in the floor of the pelvis surrounding the urethra between the bladder and the penis. The prostate is positioned immediately
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER?
 PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
Controversy Surrounds Question of Who Needs to be Treated for Prostate Cancer No One Size Fits All Diagnosis or Treatment
 For Immediate Release Media Contact: Nancy Sergeant, Sergeant Marketing, 973-334-6666, nsergeant@sergeantmarketing.com Mary Appelmann, Sergeant Marketing, 973-263-6392, mappelmann@sergeantmarketing.com
For Immediate Release Media Contact: Nancy Sergeant, Sergeant Marketing, 973-334-6666, nsergeant@sergeantmarketing.com Mary Appelmann, Sergeant Marketing, 973-263-6392, mappelmann@sergeantmarketing.com
Oncology 101. Cancer Basics
 Oncology 101 Cancer Basics What Will You Learn? What is Cancer and How Does It Develop? Cancer Diagnosis and Staging Cancer Treatment What is Cancer? Cancer is a group of more than 100 different diseases
Oncology 101 Cancer Basics What Will You Learn? What is Cancer and How Does It Develop? Cancer Diagnosis and Staging Cancer Treatment What is Cancer? Cancer is a group of more than 100 different diseases
Testicular Germ Cell Cancer Explained
 The Beatson West of Scotland Cancer Centre Pan Glasgow Urology / Oncology Patient Information Testicular Germ Cell Cancer Explained The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow
The Beatson West of Scotland Cancer Centre Pan Glasgow Urology / Oncology Patient Information Testicular Germ Cell Cancer Explained The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
What is Prostate Cancer?
 What is Prostate Cancer? Prostate cancer is a malignant tumor that begins in the prostate gland of men. Over 95% of prostate cancers are adenocarcinomas, cancers that develop in glandular tissue. Another
What is Prostate Cancer? Prostate cancer is a malignant tumor that begins in the prostate gland of men. Over 95% of prostate cancers are adenocarcinomas, cancers that develop in glandular tissue. Another
Prostate Cancer. What Are the Risk Factors? Prostate cancer is the second leading cancer that causes death to men in the U.S.
 Prostate cancer is the second leading cancer that causes death to men in the U.S. What Are the Risk Factors? Prostate cancer is unusual because it does not behave the same way in all men. Sometimes the
Prostate cancer is the second leading cancer that causes death to men in the U.S. What Are the Risk Factors? Prostate cancer is unusual because it does not behave the same way in all men. Sometimes the
Talking about Prostate Cancer
 Talking about Prostate Cancer Talking about Prostate Cancer If I can avoid going to a doctor, I will but not when we re talking about prostate cancer. Why take chances with a condition that might be serious?
Talking about Prostate Cancer Talking about Prostate Cancer If I can avoid going to a doctor, I will but not when we re talking about prostate cancer. Why take chances with a condition that might be serious?
Prostate cancer that is detected early when it's still confined to the prostate gland has a better chance of successful treatment.
 Diseases and Conditions Prostate cancer By Mayo Clinic Staff Prostate cancer is cancer that occurs in a man's prostate a small walnut shaped gland that produces the seminal fluid that nourishes and transports
Diseases and Conditions Prostate cancer By Mayo Clinic Staff Prostate cancer is cancer that occurs in a man's prostate a small walnut shaped gland that produces the seminal fluid that nourishes and transports
