Between January 1981 and January 1982 all infants
|
|
|
- Egbert Harmon
- 5 years ago
- Views:
Transcription
1 Archives of Disease in Childhood, , Parenteral nutrition compared with feeding E J GLASS, R HUME, M A LANG, AND J 0 FORFAR Departmentt of Child Life and Health, Uniiversity of Edinblurgh, Simtipsoni Memiorial Maternity Pavilion, Edinblurgh SUMMARY Fifty nine infants of birthweight less than 1500 g were allocated alternately to initial total parenteral nutrition or to feeding. Mortality was similar between the two groups. Ten of the 29 infants in the group failed to establish full enteral nutrition during the first week of life. No beneficial effects on growth were shown in infants receiving parenteral nutrition. Acquired bacterial infection was higher in the parenteral group and associated with morbidity and mortality. Conjugated hyperbilirubinaemia occurred only in the parenterally fed infants. The incidence of necrotising enterocolitis was higher in the group. Parenteral nutrition does not confer any appreciable benefit and because of greater complexity and higher risk of complications should be reserved for those infants in whom enteral feeding is impossible. Adequate nutrition of the very low birthweight infant is necessary both for immediate survival' and for optimal growth and development.2-4 It may be difficult to achieve these aims on feeding initially by the enteral route because of limitations imposed by an immature gastrointestinal tract and the respiratory effects associated with tube feeding. " Some of the problems of enteral feeding may be overcome by delivering the milk feed beyond the pylorus.7 Total parenteral nutrition allows a higher caloric intake per unit volume of feed' and avoids respiratory complications, but the technique is complicated and extensive biochemical and bacteriological monitoring is needed. Enteral feeds containing 85 kcal/l1)0 ml are in common use in Europe, but few parenteral regimens achieve this energy density. Although there are many reports of the feasibility of total parenteral nutrition in preterm neonates, there have been few controlled studies comparing total parenteral nutrition with the enteral nutrition." "' We compared two groups of infants of birthweight less than 1500 g. In one group initial parenteral nutrition was followed by the gradual introduction of nasoduodenal feeding until full enteral feeding was achieved. Infants in the other group were fed ally from birth, followed by nasogastric feeding (see below). 13 Patients and methods Between January 1981 and January 1982 all infants of birthweight 750 to 1500 g admitted to the special care unit, Simpson Memorial Maternity Pavilion, Edinburgh within 24 hours of birth were entered into the study. The infants were allocated alternately to the parenteral or groups on a rigidly observed basis uninfluenced by the initial clinical condition of the infant. More infants born elsewhere were included in the parenteral group (Table I): this occurred solely by chance and without bias. Transpyloric feeding was administered by a 5 FG silastic nasoduodenal tube (Vygon) and began when the tube was in position (confirmed radiologically). The optimum tube end site was the third part of the duodenum.7 Fresh expressed milk from the infant's own mother was used but if not available, SMA Gold Cap (Wyeth Laboraitories) was substituted. Milk was infused continuously, beginning at 1 ml/hr and increasing by 1 ml increments at 6 hourly intervals. Supplementary intravenous dextrose electrolyte solution completed the infants' planned fluid requirements. In parenteral group infants, intravenous feeding was by a central venous catheter inserted by a
2 132 Glass, Hume, Lang, and Forfar Table 1 Initialparamete, rs in infants in the parenteral and ments made on the basis of the infants' state of feeding group7s hydration. Both groups were fed by intermittent No of infants Boys/girls Birthweight (g) Mean (SD) Range Gestation (weeks) Mean (SD) Range Apgar score, mean (SD) 1 minute 5 minutes Outborn/inborn Crown to heel length at birth (cm). mean (SD) (No of infants) Occipitofrontal circumference on 3rd postnatal day (cm), mean (SD) (No of infants) hourly nasogastric feeding at 1600 g and subsequent Parenteral Original P value progression to breast or bottle feeding was detergroup mined on an individual basis. The growth parameters measured were weight, crown to heel length, and occipitofrontal circumfer- 18/12 17/12 ence. Infants were weighed naked on admission then daily until discharge, using an integrated 1237 (196) 1280 (176) NS electronic balance (Mettler PS 15). Crown to heel length was measured on admission and weekly thereafter using a Harpenden neonatometer. The 29 5 (2.1) 29 7 (1-8) NS initial measurement of occipitofrontal circumfer ence was taken on day three, repeated on day 8, and then weekly. 81 (1.7) 748 (2.0) NS Statistical analysis of acquired bacterial infection was by Wilcoxon rank sum tests, mortality rates and 10/20 3/26 <0-05 number of outborn v inborn infants by 2 x 4 contingency tables. All other statistical analysis was 383 (27) 394 (1.6) NS by Student's t test. (25) (25) 271 (14) 272 (13) (26) (25) percutaneous technique.)3 In systemic bacterial infection a peripheral line was used. During the first 12 hours infants received dextrose electrolyte solution alone; Vamin with glucose (KabiVitrum) was introduced at 12 hours and Intralipid 20% (KabiVitrum) at 24 hours. Thereafter these were infused in a 9:3:2 (dextrose electrolyte solution:vamin with glucose:intralipid 20%/) ratio. Intralipid was not infused if there was evidence of systemic bacterial infection. Addition to parenteral solutions and the priming of tubing were carried out using sterile techniques in a room set aside for the purpose. All fluids, extension sets etc were changed daily. A 0-22,u Micropore filter was incorporated into the circuit. Once the infant's clinical status was stable or respiratory distress settled, a nasoduodenal tube was passed and infusion of milk supplementary to parenteral feeding began at 1 ml/hr and remained at this level for two to three days. The volume was then increased by 1 ml increments daily for two to three days and then 12 hourly until planned fluid requirements were reached. In both groups drugs, blood, and blood products were administered by a separate peripheral venous line. Planned fluid requirements in both and parenteral groups began at 50 ml/kg on day 1 and increased by 25 ml/kg/day to 200 ml/kg, based on the infants' daily weight. An additional 25 ml/kg was given during phototherapy and further adjust- Results Patients. Fifty nine infants were studied-29 in the group and 30 in the parenteral. There were no differences between the groups (Table 1). Three infants were small for gestational age, two in the group and one in the parenteral. Ten of the 29 infants in the group failed to establish full enteral nutrition during the first week of life and were given either partial or total parenteral nutrition (the failed group). Two of these 10 infants developed hypoxia during the passage of the tube; four failed to maintain the tube in position; one developed acute renal failure; two developed necrotising enterocolitis and a third was treated as such on the basis of abdominal distension and blood in the stools, although radiological features were absent. Idiopathic respiratory distress syndrome was present in 15 infants in the parenteral group and 14 infants in the group-among the latter five failed to establish enteral nutrition during the first week of life. The number of infants ventilated was similar in the two groups. Enteral feeding. Thirty six of the 59 infants studied established full enteral feeding. Infants in the group began feeding during the first day of life at 1 to 22 hours (mean 9-9 hours). Enteral (nasoduodenal) nutrition in the parenteral group was begun between 1 and 26 days (mean 6-7 days). Establishment of full enteral feeding in the parenteral group ranged from 10 to 44 days (mean 20-7 days) and from 2 to 8 days (mean 4-9 days) in the
3 group. The time to establish full enteral feeding in the failed group was similar to that in the parenteral group. The number of tubes passed in surviving infants was between one and 7 (mean 2.7). The most common reason for replacement of the nasoduodenal tube was spontaneous displacement or removal by the infant. Less frequently the tube was pulled up during oropharyngeal suction and on occasion snapped or became blocked. Loose stools in four infants settled with temporary reduction in the volume of milk infused. Blood stained gastric aspirates in 6 infants were treated with the administration of 1 ml/hr milk nasogastrically, and in all the bleeding ceased within 24 hours. Aspiration of volumes of bile greater than 5 ml was not uncommon during feeding, and one infant who had two episodes of bile aspiration needed ventilation on one occasion. No episode of milk aspiration was recorded. Fluid and calorie intake. There was no difference between the groups in fluid intake during the first postnatal week, but during the second and third weeks fluid intake in the group was greater than in the parenteral (Table 2). The mean caloric intake was greater in the parenteral than the failed and groups during the first week (Table 2), but during the second and third weeks the mean caloric intake in the group was greater than in the parenteral and failed groups. Table 2 Comparativefluid and caloric intakes during the first four postnatal weeks in infants in the (n=19), parenteral (n=30), and failed (n=1o) groups. Values are mean (SD) Daily fluid intake (mvkg/24 hours) Postnatal week (19-5) 1616 (24.3) (21-7) NS (25-3) (14.7) (33-8) T v P<0-001 T v FT< (29.5) (15-4) (25.7) T v P<O-l1 T v FT< (40.7) (20.8) (19-8) T v P<0-05 Daily calorie intake (kcavkg/24 hours) Postnatal week (10-9) 95-8 (17.6) 86-1 (12-1) P v FPT<0001 P v T<0* (243) (10.2) 1105 (187) T v P<0*01 T v FT< (246) 1399 (11.0) 1144 (16.0) T v P<001 T v FP1< (25-5) (12-4) (112) NS T= group; P=parenteral group1- FT= failed group. Parenteral nutrition compared with feeding 133 Growth patterns. The timing of maximal postnatal weight loss was earlier in infants in the parenteral group than in the and failed groups (Table 3). There was no difference in the maximal postnatal weight loss between the groups of infants nor was there any difference in postnatal age at which birthweight was regained. Growth was considered in infants who survived from birth until the expected date of delivery or time of discharge if earlier (infants transferred to other hospitals excluded). The average weekly gain in growth for each infant was calculated by dividing the difference between the measurements at birth and those at completion of the study by the number of weeks in the study. These comparisons are justified in that the gestational age at birth and the postconceptual age at last measurement (37-38 weeks) did not differ between the groups. There were no differences in the average gain in weight or crown to heel length but a marginally greater increase in occipitofrontal circumference was noted in the than in the parenteral group (Table 3). During the third week the weight gain of infants in the group was greater than the parenteral group (as the switch to enteral feeding in the parenteral group was in progress) and marginally greater than that of the failed group. Complications. During the study 20 infants died, 12 (40%) in the parenteral group and 8 (28%) in the original group-four of whom failed to establish feeding in the first week. Most deaths occurred during the first week and were usually caused by intraventricular haemorrhage. Table 3 Growth parameters. The number of infants measured in each group until 37 to 38 weeks were parenteral (15), (15), and failed (6). Values are mean (SD) No entering study () Postnatal weight loss (%) 11-1 (4-5) 12-5 (4-0) 16(0 (5-2) Day maximal postnatal weight loss 3-6 (1-1) 5-1 (1l1) 5-3 (1-4) P v T<l()X)l P v FP<0-01 Regain birthweight (days) 10(5 (4-5) 12-5 (2-1) 12 (1-8) Weight gain (g/week) (381) (32-6) 128X7 (27-2) Crown to heel length gain (cm/week) (186 (0-21) 0-85 (1125) 0 81 (0(109) Occipitofrontal circumference gain (cm/week) 0-66 (0-15) 0-77 (0-14) 0-76 (0-21) T v P<0-05 P=parenteral group; T= group; FP=failed group.
4 134 Glass, Hume, Lang, and Forfar There were four deaths during the fourth postnatal week in the parenteral group, three from septicaemia and one from chronic lung disease (Table 4). The incidence of acquired bacterial infection was greater in the parenteral than the group (Table 4). The principal organisms were Escherichia coli and Staphylococcus albus. There were 20 episodes of septicaemia among 30 infants in the parenteral group (67%), two among 19 infants in the group (11%), and four among 10 infants in the failed group (40%). Nineteen of the 20 episodes of septicaemia in the parenteral group and two of the four in the failed group occurred during parenteral nutrition, and in 12 of these a central venous line was in situ. The incidence of septicaemia was one episode/ 21 days with a central line and 1/37 days with a peripheral line. Three infants in the group developed necrotising enterocolitis during the first week of life and a further infant was treated for suspected necrotising enterocolitis (Table 4). Another two infants in this group developed symptoms suggestive of necrotising enterocolitis at one month of age. One infant in the parenteral group developed necrotising enterocolitis on day 13, when 25% of fluids were being given nasoduodenally, and required surgical treatment, but all the other infants with necrotising enterocolitis were treated medically. There was one death in an infant who developed necrotising enterocolitis and acute renal failure. Eight infants developed conjugated hyperbilirubinaemia after the first week of life-6 in the parenteral group and two in the failed enteral group (Table 4). A raised alanine aminotransferase activ- Table 4 Complications No entering Deaths (40%) (21%) (40%) No with infection P v T<0-05 Pneumonia Septicaemia P v T<0-01 Necrotising enterocolitis P v T<0 01 Conjugated hyperbilirubinaemia 6-2 P v T<0-05 Infants with septicaemia may have had a coincidental meningitis or pneumonia. Three of the cases of necrotising enterocolitis in the group were suspected clinically but had either equivocal radiological features or none. ity was also noted in four of these infants. In all cases liver function reverted to normal. Discussion One third of infants allocated to the feeding group failed to establish adequate enteral feeding during the first week of life. This was usually for technical reasons that might have been obviated, but other important causes were exacerbation of pre-existing respiratory distress and the development of necrotising enterocolitis. In general, no problem was experienced in the feeding of infants who were already being ventilated.7 While there was no difference in the maximal postnatal weight loss between the two groups the time of maximal weight loss was earlier in the parenteral group. In contrast, however, to the findings of Yu et alit that parenterally fed infants regained their birthweight sooner, no difference was noted between the groups in our study. This may be related to the timing of introduction of enteral feeding.9 10 The use of total parenteral nutrition may prevent the maturation of the gut hormonal system.1 It had been hoped that the more adequate initial caloric intake in the parenteral group could be combined with stimulation of the gut by gradual introduction of milk feeding, thus preventing the deterioration in growth pattern associated with the switch from parenteral to enteral nutrition. There is, however, no evidence from our study that this aim was achieved, although increased catabolism associated with acquired bacterial infection may have adversely affected growth in the parenteral group. Because infants who failed to establish feeding initially (failed group) were among the sicker members allocated to this group, the group had a selective advantage over the parenteral group, and this should be considered when longer term growth is compared. No differences in average weekly weight gain or crown to heel length were noted in comparing the three groups over the whole period. There was a greater increase in occipitofrontal circumference in the enteral group than in the parenteral over the study period. The timing of peak velocity of head growth may have influenced this finding since this is related to gestational age, with less mature infants having a later peak velocity. Impaired caloric intake and illness are, however, also known to affect head growth.'2 13 Sepsis, to which the preterm infant is particularly prone, is recognised to be the most serious complication of parenteral nutrition in paediatric
5 patients.'4 Acquired bacterial infection occurred in two thirds of the infants in the parenteral group. An incidence of (-50% has been recorded in various series. 6 Sondheimer et alit considered sepsis to be almost inevitable in the very low birthweight infant receiving parenteral nutrition. Septicaemia has been reported less commonly in infants receiving peripheral parenteral nutrition'6 and strict attention to asepsis decreases the risk of acquired bacterial infection during parenteral nutrition. Hepatic dysfunction, which is known to occur during parenteral nutrition,'5 developed in 8 of our infants and a striking temporal relation with infection was noted. Necrotising enterocolitis was diagnosed in five ally fed infants and suggestive symptoms and signs were present in one other. The infants studied were a high risk group for the development of necrotising enterocolitis, which can be related to the onset of milk feeding.'7 A high fluid intake is associated with an increased risk'8 and three infants developed symptoms during the first weeks of life, at which time the fluid intake was relatively high. The role of different types of enteral feeding in the aetiology of necrotising enterocolitis is unclear, as the disorder occurs not only in infants fed ally but also in those fed nasogastrically. "' Parenteral feeding does not confer any significant benefit and because of the greater complexity of parenteral feeding and the serious risk of complications, we consider that it should be reserved for those infants in whom enteral nutrition is impossible. We do not agree with those authors who advocate that enteral nutrition be witheld from infants of less than 1500 g birthweight for 2 to 3 weeks in order to prevent necrotising enterocolitis'9 without consideration of other risks involved. References Heird WC, Driscoll JM, Schullinger JN, Grebin B, Winters RW. Intravenous alimentation in paediatric patients. J Pediatr 1972;80: Drillien CM. The growth and development of the prematurely born infant. Edinburgh: Livingstone, 1964: Shaw JCL. Parentcral nutrition in the management of the sick low birth weight infant. Pediatr Clin North Am 1973;20: Parenteral nutrition compared with feeding Dobbing J. The later development of the brain and its vulnerability. In: Davis JA, Dobbing J, eds. Scientific foundations of paediatrics. 2nd ed. London: Heinemann, 1981: Wharton BA, Bower BD. Immediate or later feeding for premature babies? Lancet 1965;ii: YU VYH, Rolfe P. Effect of feeding on ventilation and respiratory mechanics in newborn infants. Arch Dis Child 1976;51: Dryburgh E. Transpyloric feeding in 49 infants undergoing intensive care. Arch Dis Child 1980;55: x Hume R, Giles MM, Cockburn F. Amino acid analysis in parenteral nutrition of the newborn. In: Rattenbury JM, ed. Amino Acid Analysis. Chichester: Ellis Horwood, 1981: Gunn T, Reaman G, Outerbridge EW, Colle E. Peripheral total parenteral nutrition for premature infants with the respiratory distress syndrome: a controlled study. J Pediatr 1978;92: '0 Yu VYH, James B, Hendry P, MacMahon RA. Total parenteral nutrition in very low birth weight infants: a controlled trial. Arch Dis Child 1979;54: Becker DJ. Reaction: gastrointestinal hormones in the neonate. Sunshine P, ed. Stanford University. 79th Ross Conference, Glass L, Lala RV, Jaiswal V, Nigam SK. Effect of thermal environment and caloric intake on head growth of low birth weight infants during the late neonatal period. Arch Dis Child 1975;50: Fujimura M. Factors which influence the timing of maximum growth rate of the head in low birth weight infants. Arch Dis Child 1977;52: Reimer SL, Michener WM, Steiger E. Nutritional support of the critically ill child. Pediatr Clin Nortih Ain 198t):27: Sondheimer JM, Bryan H, Andrews W. Forstner GG. Cholestatic tendencies in premature infants on and off parenteral nutrition. Pediatrics 1978;62: Brans YW. Parenteral nutrition of the very low birth weight neonate: a critical view. Clin Perinatol 1977;4: Sweet AY. Necrotising enterocolitis. Sunshine P, ed. Stanford University. 79th Ross Conference, Bell EG, Warburton D, Stonestreet BS, Oh W. High volume fluid intake predisposes premature infants to necrotising enterocolitis. Lancet 1980;ii:90. 9 Eyal F, Sagi E, Arad 1, Avital AA. Necrotising enterocolitis in the very low birth weight infant: expressed breast milk feeding compared with parenteral feeding. Arch Dis Child 1982;57: Correspondence to Dr R Hume, Department of Child Life and Health, Simpson Memorial Maternity Pavilion, Lauriston Place, Edinburgh EH3 9EF. Received 7 November 1983
Minimal Enteral Nutrition
 Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
NUTRITIONAL REQUIREMENTS
 NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
INTRAVENOUS FLUIDS PRINCIPLES
 INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
ENTERAL NUTRITION Identifying risk of patients for enteral feeding problems: Low risk: Moderate risk: High risk:
 ENTERAL NUTRITION Statement of best practice Feeding with mother s own breastmilk is protective against sepsis, NEC and death All mothers should be informed about this and strongly encouraged to express
ENTERAL NUTRITION Statement of best practice Feeding with mother s own breastmilk is protective against sepsis, NEC and death All mothers should be informed about this and strongly encouraged to express
Neonatal Hypoglycaemia Guidelines
 N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
Guideline scope Neonatal parenteral nutrition
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial. A. Salhotra and S.
 Original Article Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial A. Salhotra and S. Ramji From the Neonatal Division, Department of Pediatrics,
Original Article Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial A. Salhotra and S. Ramji From the Neonatal Division, Department of Pediatrics,
Nutrition in the premie World
 SURVIVAL AND GROWTH NUTRITION ESSENTIALS Nutrition in the premie World DR VISH SUBRAMANIAN MD MRCP (UK) FAAP NEONATAL CRITICAL CARE MERCY CHILDRENS HOSPITAL., SPRINGFIELD MO Prematurity Nutritional Requirements
SURVIVAL AND GROWTH NUTRITION ESSENTIALS Nutrition in the premie World DR VISH SUBRAMANIAN MD MRCP (UK) FAAP NEONATAL CRITICAL CARE MERCY CHILDRENS HOSPITAL., SPRINGFIELD MO Prematurity Nutritional Requirements
Indian Pediatrics - Editorial
 Page 1 of 7 Home Past Issue About IP About IAP Feedback Links Author Info. Subscription Original Articles Indian Pediatrics 2004; 41:435-441 Slow versus Fast Enteral Feed Advancements in Very Low Birth
Page 1 of 7 Home Past Issue About IP About IAP Feedback Links Author Info. Subscription Original Articles Indian Pediatrics 2004; 41:435-441 Slow versus Fast Enteral Feed Advancements in Very Low Birth
4/15/2014. Nurses Take the Lead to Improve Overall Infant Growth. Improving early nutrition. Problem Identification
 Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Aggressive Nutrition in Preterm Infants
 Aggressive Nutrition in Preterm Infants Jatinder Bhatia, MD, FAAP Declaration of potential conflicts of interest Regarding this presentation the following relationships could be perceived as potential
Aggressive Nutrition in Preterm Infants Jatinder Bhatia, MD, FAAP Declaration of potential conflicts of interest Regarding this presentation the following relationships could be perceived as potential
Guidelines for the Prevention and Management of Hypoglycaemia
 ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
ASHFORD & ST PETER S HOSPITALS NHS TRUST CHILDREN S SERVICES Guidelines for the Prevention and Management of Hypoglycaemia 1. The Care Plan for Prevention of Hypoglycaemia on Labour Ward and the Postnatal
The Case Begins. The case continued. Necrotizing Enterocolitis
 Bugs, Drugs and Things that go Bump in the Night From ghoulies to ghosties and long leggety beasties & things that go bump in the night, good lord deliver us Old Cornish Prayer Caring for premature infant
Bugs, Drugs and Things that go Bump in the Night From ghoulies to ghosties and long leggety beasties & things that go bump in the night, good lord deliver us Old Cornish Prayer Caring for premature infant
Efficacy of Breast Milk Gastric Lavage in Preterm Neonates. Archana B. Patel and Samiuddin Shaikh
 Research Papers Efficacy of Breast Milk Gastric Lavage in Preterm Neonates Archana B. Patel and Samiuddin Shaikh From the Department of Pediatrics and Clinical Epidemiology Unit, Indira Gandhi Medical
Research Papers Efficacy of Breast Milk Gastric Lavage in Preterm Neonates Archana B. Patel and Samiuddin Shaikh From the Department of Pediatrics and Clinical Epidemiology Unit, Indira Gandhi Medical
PROTOCOL FOR PARENTERAL NUTRITION
 PROTOCOL FOR PARENTERAL NUTRITION Based on; Roberton s textbook of neonatology. 4 th edition. 2005. Sudha Chaudari and Sandeep Kumar.TPN in neonates. Indian Paediatrics. November 2006 Deepak Chawla, Anu
PROTOCOL FOR PARENTERAL NUTRITION Based on; Roberton s textbook of neonatology. 4 th edition. 2005. Sudha Chaudari and Sandeep Kumar.TPN in neonates. Indian Paediatrics. November 2006 Deepak Chawla, Anu
Routine endotracheal cultures for the prediction of sepsis in ventilated babies
 Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Randomised controlled trial of trophic feeding and gut motility
 F54 Regional Neonatal Intensive Care Unit, St James s University Hospital, Leeds LS9 7TF R J McClure S J Newell Correspondence to: Dr SJ Newell. Accepted 13 August 1998 Randomised controlled trial of trophic
F54 Regional Neonatal Intensive Care Unit, St James s University Hospital, Leeds LS9 7TF R J McClure S J Newell Correspondence to: Dr SJ Newell. Accepted 13 August 1998 Randomised controlled trial of trophic
Under-five and infant mortality constitutes. Validation of IMNCI Algorithm for Young Infants (0-2 months) in India
 R E S E A R C H P A P E R Validation of IMNCI Algorithm for Young Infants (0-2 months) in India SATNAM KAUR, V SINGH, AK DUTTA AND J CHANDRA From the Department of Pediatrics, Kalawati Saran Children s
R E S E A R C H P A P E R Validation of IMNCI Algorithm for Young Infants (0-2 months) in India SATNAM KAUR, V SINGH, AK DUTTA AND J CHANDRA From the Department of Pediatrics, Kalawati Saran Children s
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
Recommendations for Hospital Quality Measures in 2011:
 Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Satellite Symposium. Sponsored by
 Satellite Symposium Sponsored by Management of fluids and electrolytes in the preterm infant in the first week of life Pam Cairns St Michaels Hospital Bristol Healthy, term, breast fed babies Limited intake
Satellite Symposium Sponsored by Management of fluids and electrolytes in the preterm infant in the first week of life Pam Cairns St Michaels Hospital Bristol Healthy, term, breast fed babies Limited intake
Resuscitating neonatal and infant organs and preserving function. GI Tract and Kidneys
 Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
PRACTICE GUIDELINES WOMEN S HEALTH PROGRAM
 C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
Advances in intestinal Rehabilitation Susan Hill Gastroenterology Consultant
 Advances in intestinal Rehabilitation Susan Hill Gastroenterology Consultant 2 Indication for intravenous nutrition/pn: Intestinal Failure Inability to maintain weight and growth despite adequate enteral
Advances in intestinal Rehabilitation Susan Hill Gastroenterology Consultant 2 Indication for intravenous nutrition/pn: Intestinal Failure Inability to maintain weight and growth despite adequate enteral
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359
 Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Randomised controlled study of clinical outcome following trophic feeding
 Arch Dis Child Fetal Neonatal Ed 2000;82:F29 F33 Regional Neonatal Intensive Care Unit, St James s University Hospital, Leeds R J McClure S J Newell Correspondence to: Dr R J McClure, Neonatal Services,
Arch Dis Child Fetal Neonatal Ed 2000;82:F29 F33 Regional Neonatal Intensive Care Unit, St James s University Hospital, Leeds R J McClure S J Newell Correspondence to: Dr R J McClure, Neonatal Services,
SOUTHERN WEST MIDLANDS NEWBORN NETWORK
 SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title : Person Responsible for Review : Management of Gastro-Intestinal Stomata In Neonates R. Wragg & G.Jawaheer
SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title : Person Responsible for Review : Management of Gastro-Intestinal Stomata In Neonates R. Wragg & G.Jawaheer
Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation
 Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation Version: 1.3 Issued: Review date: Author: Melanie Drewett The procedural aspects of this guideline can be
Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation Version: 1.3 Issued: Review date: Author: Melanie Drewett The procedural aspects of this guideline can be
Evaluation of a taurine containing amino acid
 Archives ofdisease in Childhood 1991; 66: 21-25 21 Coombe Lying-In Hospital, Dublin 8, Republic of Ireland L Thornton E Griffim Correspondence to: Dr Griffm. Accepted 26 July 199 Evaluation of a taurine
Archives ofdisease in Childhood 1991; 66: 21-25 21 Coombe Lying-In Hospital, Dublin 8, Republic of Ireland L Thornton E Griffim Correspondence to: Dr Griffm. Accepted 26 July 199 Evaluation of a taurine
Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number:
 This is an official Northern Trust policy and should not be edited in any way Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number: NHSCT/10/293 Target audience: Midwifery,
This is an official Northern Trust policy and should not be edited in any way Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number: NHSCT/10/293 Target audience: Midwifery,
Early Life Nutrition: Feeding Preterm Babies for Lifelong Health
 Early Life Nutrition: Feeding Preterm Babies for Lifelong Health Jane Alsweiler Frank Bloomfield Anna Tottman Barbara Cormack Tanith Alexander Jane Harding Feeding Preterm Babies for Lifelong Health Why
Early Life Nutrition: Feeding Preterm Babies for Lifelong Health Jane Alsweiler Frank Bloomfield Anna Tottman Barbara Cormack Tanith Alexander Jane Harding Feeding Preterm Babies for Lifelong Health Why
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN
 PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
Wali R Johnson et. al. / International Journal of New Technologies in Science and Engineering Vol. 2, Issue 4, October 2015, ISSN
 Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
SWISS SOCIETY OF NEONATOLOGY. Neonatal gastric perforation
 SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
Factors affecting survival in neonatal surgery unit in a tertiary care university hospital during 26 years
 The Turkish Journal of Pediatrics 2016; 58: 457-463 Original Factors affecting survival in neonatal surgery unit in a tertiary care university hospital during 26 years Önder Özden, İbrahim Karnak, Arbay
The Turkish Journal of Pediatrics 2016; 58: 457-463 Original Factors affecting survival in neonatal surgery unit in a tertiary care university hospital during 26 years Önder Özden, İbrahim Karnak, Arbay
Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi
 Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi Outline O Background O Challenges in preterm nutrition O Parenteral Nutrition
Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi Outline O Background O Challenges in preterm nutrition O Parenteral Nutrition
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc
 Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Dr Shipa Shah, Lorraine Bell Dietician
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Enteral feeding and use of fortification and supplements in the preterm infant Dr Shipa Shah, Lorraine Bell Dietician Neonatalogy
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Enteral feeding and use of fortification and supplements in the preterm infant Dr Shipa Shah, Lorraine Bell Dietician Neonatalogy
Fluid & Electrolyte Balances in Term & Preterm Infants. Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital
 Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
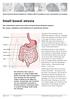 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Introduce the basics of the newborn resuscitation period Practice calculations for TPN orders Learn how to manage basic ventilator settings
 Introduce the basics of the newborn resuscitation period Practice calculations for TPN orders Learn how to manage basic ventilator settings Complex concepts you may be expected to know Not taught this
Introduce the basics of the newborn resuscitation period Practice calculations for TPN orders Learn how to manage basic ventilator settings Complex concepts you may be expected to know Not taught this
Fortification of Maternal Expressed Breast Milk
 Fortification of Maternal Expressed Breast Milk Title: Version: 2 Ratification Date: April 2016 Review Date: April 2019 Approval: Nottingham Neonatal Service Clinical Guideline Group 20 th April 2016 Author:
Fortification of Maternal Expressed Breast Milk Title: Version: 2 Ratification Date: April 2016 Review Date: April 2019 Approval: Nottingham Neonatal Service Clinical Guideline Group 20 th April 2016 Author:
Clinical evaluation Jaundice skin and mucous membranes
 JAUNDICE Framework The definition of Neonatal Jaundice Billirubin Metabolism Special characteristic in neonates Dangerous of the Hyperbillirubinemia The diseases in relation with Neonatal Jaundice Objectives:
JAUNDICE Framework The definition of Neonatal Jaundice Billirubin Metabolism Special characteristic in neonates Dangerous of the Hyperbillirubinemia The diseases in relation with Neonatal Jaundice Objectives:
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
[No conflicts of interest]
![[No conflicts of interest] [No conflicts of interest]](/thumbs/86/94144068.jpg) [No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
[No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
CYANOTIC ATTACKS IN NEWBORN INFANTS
 BY R. S. ILLINGWORTH From the Jessop Hospital for Women and the Children's Hospital, the United Sheffield Hospitals (RECEIVED FOR PUBLICATION MARCH 10, 1957) By the term 'cyanotic attacks in newborn infants'
BY R. S. ILLINGWORTH From the Jessop Hospital for Women and the Children's Hospital, the United Sheffield Hospitals (RECEIVED FOR PUBLICATION MARCH 10, 1957) By the term 'cyanotic attacks in newborn infants'
Exchange Transfusion
 Approved by: Exchange Transfusion Gail Cameron Director, Maternal, Neonatal & Child Health Programs Neonatal Nursery Policy & Procedures Manual : Next Review March 2016 Dr. Ensenat Medical Director, Neonatology
Approved by: Exchange Transfusion Gail Cameron Director, Maternal, Neonatal & Child Health Programs Neonatal Nursery Policy & Procedures Manual : Next Review March 2016 Dr. Ensenat Medical Director, Neonatology
Perforated Necrotizing Enterocolitis: What Is The Rational Approach? Peritoneal Drainage or Laparotomy?
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 17, Issue 5 Ver. 12(May. 218), PP 19-23 www.iosrjournals.org Perforated Necrotizing Enterocolitis: What
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 17, Issue 5 Ver. 12(May. 218), PP 19-23 www.iosrjournals.org Perforated Necrotizing Enterocolitis: What
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel Approach
 653738JHLXXX10.1177/0890334416653738Journal of Human LactationSimpson et al research-article2016 Original Research: Brief Report Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel
653738JHLXXX10.1177/0890334416653738Journal of Human LactationSimpson et al research-article2016 Original Research: Brief Report Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel
RD s In Practice: Advancing Pediatric Nutrition
 RD s In Practice: Advancing Pediatric Nutrition A Strong Beginning Mindy Morris, DNP, NNP-BC, CNS Extremely Low Birth Weight Program Coordinator Objectives Understand the challenges associated with the
RD s In Practice: Advancing Pediatric Nutrition A Strong Beginning Mindy Morris, DNP, NNP-BC, CNS Extremely Low Birth Weight Program Coordinator Objectives Understand the challenges associated with the
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
HYPOGLYCEMIA IN SICK PRETERM INFANTS AND THE THERAPEUTIC EFFECT OF 12.5% DEXTROSE IN WATER COMPARED WITH 10% DEXTROSE IN WATER
 HYPOGLYCEMIA IN SICK PRETERM INFANTS AND THE THERAPEUTIC EFFECT OF 12.5% DEXTROSE IN WATER COMPARED WITH 10% DEXTROSE IN WATER F. Nili * and M. Ghafuri Department of Pediatrics, Division of Neonatology,
HYPOGLYCEMIA IN SICK PRETERM INFANTS AND THE THERAPEUTIC EFFECT OF 12.5% DEXTROSE IN WATER COMPARED WITH 10% DEXTROSE IN WATER F. Nili * and M. Ghafuri Department of Pediatrics, Division of Neonatology,
Challenges in Pediatric Nutritional Support. Donald E. George, MD
 Challenges in Pediatric Nutritional Support Donald E. George, MD What is so special about Kids They Grow They Change They Explore They Frequently get better What is so special about Kids They require more
Challenges in Pediatric Nutritional Support Donald E. George, MD What is so special about Kids They Grow They Change They Explore They Frequently get better What is so special about Kids They require more
SWISS SOCIETY OF NEONATOLOGY. Hypertrophic pyloric stenosis in a preterm infant
 SWISS SOCIETY OF NEONATOLOGY Hypertrophic pyloric stenosis in a preterm infant February 2014 2 Georgi R, Berger M, Schnyder I, Berger S, McDougall J, Division of Neonatology (GR, BM, McDJ), Department
SWISS SOCIETY OF NEONATOLOGY Hypertrophic pyloric stenosis in a preterm infant February 2014 2 Georgi R, Berger M, Schnyder I, Berger S, McDougall J, Division of Neonatology (GR, BM, McDJ), Department
Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN *
 For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
BACTERIAL TRANSLOCATION AND INTESTINAL PERMEABILITY IN PRETERM INFANTS
 BACTERIAL TRANSLOCATION AND INTESTINAL PERMEABILITY IN PRETERM INFANTS Dr Paul Fleming Consultant Neonatal Medicine Homerton University Hospital Honorary Research Fellow Barts and the London School of
BACTERIAL TRANSLOCATION AND INTESTINAL PERMEABILITY IN PRETERM INFANTS Dr Paul Fleming Consultant Neonatal Medicine Homerton University Hospital Honorary Research Fellow Barts and the London School of
Neonatal Perforated Gut: Etiology and Risk Factors
 Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Mostafa Kotb 1 * and Marwa Beyaly 2 1 Pediatric Surgery Department, Alexandria Faculty of Medicine, Egypt. 2 Human Genetics Department, Medical Research
Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Mostafa Kotb 1 * and Marwa Beyaly 2 1 Pediatric Surgery Department, Alexandria Faculty of Medicine, Egypt. 2 Human Genetics Department, Medical Research
Prolonged Neonatal Jaundice
 Prolonged Neonatal Jaundice Ahmed Laving KPA Annual Scientific Conference 2018 Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Case Presentation
Prolonged Neonatal Jaundice Ahmed Laving KPA Annual Scientific Conference 2018 Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Prolonged Jaundice? >6 months >3 months >2 weeks >4 weeks Case Presentation
Summary of Changes: References/content updated to reflect most current standards of practice.
 Alaska Native Medical Center: Mother Baby Unit Guideline: Neonatal Hypoglycemia Subject: Neonatal Hypoglycemia REVISION DATE: Jan 2015,12/2011, 02/2009, 11, 2007, 07/2007,04/2001, 04/1999 REPLACES: NSY:
Alaska Native Medical Center: Mother Baby Unit Guideline: Neonatal Hypoglycemia Subject: Neonatal Hypoglycemia REVISION DATE: Jan 2015,12/2011, 02/2009, 11, 2007, 07/2007,04/2001, 04/1999 REPLACES: NSY:
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Gastric Residuals in Preterm Infants
 Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
LOW BIRTH- WEIGHT INFANTS
 Med. J. Malaysia Vo!. 39 No. 3 September 1984 THE ROLE OF INTRAVENOUS NUTRITION IN LOW BIRTH- WEIGHT INFANTS ZAINAL ABIDIN N.KUHAN SUMMARY Seven infants with birth weights less than ls00g received total
Med. J. Malaysia Vo!. 39 No. 3 September 1984 THE ROLE OF INTRAVENOUS NUTRITION IN LOW BIRTH- WEIGHT INFANTS ZAINAL ABIDIN N.KUHAN SUMMARY Seven infants with birth weights less than ls00g received total
7/11/2018. Oral Dextrose Gel Treatment for Newborns with Hypoglycemia Reduces NICU Admissions DISCLOSURE. Objectives
 Gaps in Knowledge, Competence, Performance, or Patient Outcomes DISCLOSURE The content of this presentation does not relate to any product of a commercial entity; therefore, I have no relationships to
Gaps in Knowledge, Competence, Performance, or Patient Outcomes DISCLOSURE The content of this presentation does not relate to any product of a commercial entity; therefore, I have no relationships to
ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME
 INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
Total Parenteral Nutrition and Enteral Nutrition in the Home. Original Policy Date 12:2013
 MP 1.02.01 Total Parenteral Nutrition and Enteral Nutrition in the Home Medical Policy Section Durable Medical Equipment Issue Original Policy Date Last Review Status/Date Return to Medical Policy Index
MP 1.02.01 Total Parenteral Nutrition and Enteral Nutrition in the Home Medical Policy Section Durable Medical Equipment Issue Original Policy Date Last Review Status/Date Return to Medical Policy Index
Department of Pediatrics, Coimbatore Medical College Hospital, Coimbatore, Tamilnadu, India Correspondence to: Senthilkumar P,
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. VIII (Aug. 2017), PP 40-45 www.iosrjournals.org A Randomized Trial of Intravenous Fluid
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. VIII (Aug. 2017), PP 40-45 www.iosrjournals.org A Randomized Trial of Intravenous Fluid
Original Article Effect of Intravenous Fluid Supplementation on Serum Bilirubin Level in Jaundiced Healthy Neonates during Conventional Phototherapy
 Original Article Effect of Intravenous Fluid Supplementation on Serum Bilirubin Level in Jaundiced Healthy Neonates during Conventional Phototherapy Abstract R. Iranpour MD*, R. Nohekhan MD**, I. Haghshenas
Original Article Effect of Intravenous Fluid Supplementation on Serum Bilirubin Level in Jaundiced Healthy Neonates during Conventional Phototherapy Abstract R. Iranpour MD*, R. Nohekhan MD**, I. Haghshenas
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
NEONATOLOGY Healthy newborn. Neonatal sequelaes
 NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Melinda Elliott, MD Senior Director, Clinical Education and Professional Development, Prolacta Bioscience Neonatologist, Pediatrix Medical Group of
 Melinda Elliott, MD Senior Director, Clinical Education and Professional Development, Prolacta Bioscience Neonatologist, Pediatrix Medical Group of Maryland Breast Milk is for Babies, Cows Milk is for
Melinda Elliott, MD Senior Director, Clinical Education and Professional Development, Prolacta Bioscience Neonatologist, Pediatrix Medical Group of Maryland Breast Milk is for Babies, Cows Milk is for
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086)
 Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
HYPOGLYCAEMIA OF THE NEWBORN ON BIRTHING SUITE AND POSTNATAL WARD
 HYPOGLYCAEMIA OF THE NEWBORN ON BIRTHING SUITE AND POSTNATAL WARD INTRODUCTION Healthy term infants are able to mobilise energy stores through a process known as counter regulation and are unlikely to
HYPOGLYCAEMIA OF THE NEWBORN ON BIRTHING SUITE AND POSTNATAL WARD INTRODUCTION Healthy term infants are able to mobilise energy stores through a process known as counter regulation and are unlikely to
A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH
 A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH 1* Paul Leeson, PhD, FRCP and 1 Adam J. Lewandowski, DPhil 1 Oxford Cardiovascular Clinical Research Facility, Division of Cardiovascular Medicine,
A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH 1* Paul Leeson, PhD, FRCP and 1 Adam J. Lewandowski, DPhil 1 Oxford Cardiovascular Clinical Research Facility, Division of Cardiovascular Medicine,
Follow up studies at home were randomly performed
 Archives of Disease in Childhood, 1985, 60, 856-860 Oral versus intravenous rehydration therapy in severe gastroenteritis J SHARIFI, F GHAVAMI, Z NOWROUZI, B FOULADVAND, M MALEK, M REZAEIAN, AND M EMAMI
Archives of Disease in Childhood, 1985, 60, 856-860 Oral versus intravenous rehydration therapy in severe gastroenteritis J SHARIFI, F GHAVAMI, Z NOWROUZI, B FOULADVAND, M MALEK, M REZAEIAN, AND M EMAMI
Infection Screening for Newborn Babies
 Infection Screening for Newborn Babies Patient Information Leaflet If you require a translation or an alternative format of this leaflet please speak to the nurse in charge or call the Patient Advice Liaison
Infection Screening for Newborn Babies Patient Information Leaflet If you require a translation or an alternative format of this leaflet please speak to the nurse in charge or call the Patient Advice Liaison
Pathogenesis of Metabolic Acidosis in Preterm Infants
 Original Article Pathogenesis of Metabolic Acidosis in Preterm Infants DOI: IJNMR/2013/5233.1976 Acid Base Balance Section Christopher Geoffrey Alexander Aiken ABSTRACT Objective: To determine how the
Original Article Pathogenesis of Metabolic Acidosis in Preterm Infants DOI: IJNMR/2013/5233.1976 Acid Base Balance Section Christopher Geoffrey Alexander Aiken ABSTRACT Objective: To determine how the
Role of human milk fortifier on weight gain in very low birth weight babies
 International Journal of Contemporary Pediatrics Verma GK et al. Int J Contemp Pediatr. 2018 Mar;5(2):353-358 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Verma GK et al. Int J Contemp Pediatr. 2018 Mar;5(2):353-358 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
Ashley Robson Canyon Creek Dr. Mckinney, TX 75070
 1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
HOW TO DO EARLY NUTRITION in VLBW INFANTS. David H Adamkin M.D. University of Louisville USA
 HOW TO DO EARLY NUTRITION in VLBW INFANTS David H Adamkin M.D. University of Louisville USA NUTRITIONAL CHALLENGES in EARLY NUTRITION Strategies to Prevent Postnatal Growth Failure Early Total Parenteral
HOW TO DO EARLY NUTRITION in VLBW INFANTS David H Adamkin M.D. University of Louisville USA NUTRITIONAL CHALLENGES in EARLY NUTRITION Strategies to Prevent Postnatal Growth Failure Early Total Parenteral
ARTIFICIAL INTELLIGENCE FOR PREDICTION OF SEPSIS IN VERY LOW BIRTH WEIGHT INFANTS
 ARTIFICIAL INTELLIGENCE FOR PREDICTION OF SEPSIS IN VERY LOW BIRTH WEIGHT INFANTS Markus Leskinen MD PhD, Neonatologist Children s Hospital, University of Helsinki and Helsinki University Hospital The
ARTIFICIAL INTELLIGENCE FOR PREDICTION OF SEPSIS IN VERY LOW BIRTH WEIGHT INFANTS Markus Leskinen MD PhD, Neonatologist Children s Hospital, University of Helsinki and Helsinki University Hospital The
Intensive Care Nutrition. Dr Alan Race BSc(Hons) PhD FRCA
 Intensive Care Nutrition Dr Alan Race BSc(Hons) PhD FRCA Objectives 1. What examiners say 2. Definition 3. Assessment 4. Requirements 5. Types of delivery 6. CALORIES Trial 7. Timing 8. Immunomodulation
Intensive Care Nutrition Dr Alan Race BSc(Hons) PhD FRCA Objectives 1. What examiners say 2. Definition 3. Assessment 4. Requirements 5. Types of delivery 6. CALORIES Trial 7. Timing 8. Immunomodulation
A STUDY OF REBOUND HYPERBILIRUBINEMIA IN POST PHOTOTHERAPY NEONATES
 wjpmr, 2017,3(8), 226-235 SJIF Impact Factor:.103 Arakhita et al. WORLD JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.wjpmr.com Research Article ISSN 255-3301 WJPMR A STUDY OF REBOUND HYPERBILIRUBINEMIA
wjpmr, 2017,3(8), 226-235 SJIF Impact Factor:.103 Arakhita et al. WORLD JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.wjpmr.com Research Article ISSN 255-3301 WJPMR A STUDY OF REBOUND HYPERBILIRUBINEMIA
(1 280 ± 286) g; (1 436 ± 201) g
 259 ( 100730) : 34 1 800 g 24 (, 11 ) (, 13 ) 50%, 100 ml / (kg d) FM85, ; (30.6 ± 2.9), (1 280 ± 286) g; (31.6 ± 1.9), (1 436 ± 201) g, 81.6%, 34.1 24.6 d [18.9 vs 17.1 g / (kg d), P = 0.364] (1.16 vs
259 ( 100730) : 34 1 800 g 24 (, 11 ) (, 13 ) 50%, 100 ml / (kg d) FM85, ; (30.6 ± 2.9), (1 280 ± 286) g; (31.6 ± 1.9), (1 436 ± 201) g, 81.6%, 34.1 24.6 d [18.9 vs 17.1 g / (kg d), P = 0.364] (1.16 vs
A retrospective review of tracheal suction at birth in neonates with meconium aspiration syndrome
 A retrospective review of tracheal suction at birth in neonates with meconium aspiration syndrome D. Manickam MBBS, DCH, MRCP, MIAC, Paediatric Department, Penang General Hospital, 10450 Pulau Pinang Summary
A retrospective review of tracheal suction at birth in neonates with meconium aspiration syndrome D. Manickam MBBS, DCH, MRCP, MIAC, Paediatric Department, Penang General Hospital, 10450 Pulau Pinang Summary
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant
 SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
ENTERAL NUTRITION IN THE CRITICALLY ILL
 ENTERAL NUTRITION IN THE CRITICALLY ILL 1 Ebb phase Flow phase acute response (catabolic) adoptive response (anabolic) 2 3 Metabolic Response to Stress (catabolic phase) Glucose and Protein Metabolism
ENTERAL NUTRITION IN THE CRITICALLY ILL 1 Ebb phase Flow phase acute response (catabolic) adoptive response (anabolic) 2 3 Metabolic Response to Stress (catabolic phase) Glucose and Protein Metabolism
Massive pulmonary haemorrhage in the newborn infant
 Archives of Disease in Childhood, 1975, 50, 123. Massive pulmonary haemorrhage in the newborn infant R. TROMPETER, V. Y. H. YU, A. AYNSLEY-GREEN, and N. R. C. ROBERTON From the Department of Paediatrics,
Archives of Disease in Childhood, 1975, 50, 123. Massive pulmonary haemorrhage in the newborn infant R. TROMPETER, V. Y. H. YU, A. AYNSLEY-GREEN, and N. R. C. ROBERTON From the Department of Paediatrics,
NEONATAL INTENSIVE CARE SKILLS CHECKLIST
 NEONATAL INTENSIVE CARE SKILLS CHECKLIST NAME: DATE: Please check the appropriate letter of proficiency for the following types of clinical situations and equipment. GENERAL Gestational assessment Physical
NEONATAL INTENSIVE CARE SKILLS CHECKLIST NAME: DATE: Please check the appropriate letter of proficiency for the following types of clinical situations and equipment. GENERAL Gestational assessment Physical
Plasma alkaline phosphatase activity and its relation to rickets in pre-term infants
 Ann Clin Biochem 1986; 23: 652--656 Plasma alkaline phosphatase activity and its relation to rickets in pre-term infants E G WALTERS, J F MURPHY', P HENRYt, a P GRAY' and G HELDER From the Departmentsof
Ann Clin Biochem 1986; 23: 652--656 Plasma alkaline phosphatase activity and its relation to rickets in pre-term infants E G WALTERS, J F MURPHY', P HENRYt, a P GRAY' and G HELDER From the Departmentsof
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
2015 Prolacta Bioscience
 Housekeeping Items 1 Presentation will be available on-demand http://www.prolacta.com/webinars/feeding-protocols 2 Turn up your speaker volume 3 Use the Ask a Question feature 4 Use the full screen feature
Housekeeping Items 1 Presentation will be available on-demand http://www.prolacta.com/webinars/feeding-protocols 2 Turn up your speaker volume 3 Use the Ask a Question feature 4 Use the full screen feature
