Spontaneous or idiopathic osteonecrosis of the medial
|
|
|
- Sheryl Paul
- 5 years ago
- Views:
Transcription
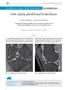
1 A Case Report & Literature Review Focal Spontaneous Osteonecrosis and Medial Meniscus Tear: Two Cases and a Literature Review Christopher Brown, BA, and Jeffery L. Stambough, MD, MBA Mr. Brown is Medical Student, College of Medicine, University of Cincinnati, Cincinnati, Ohio. Dr. Stambough is Consultant, Back and Treatment Center, Deaconess Hospital, and Adjunct Professor, Department of Medical and Industrial Engineering, University of Cincinnati, Cincinnati, Ohio. Address correspondence to: Jeffrey L. Stambough, MD, MBA, 4600 Smith Road, Suite B, Cincinnati, OH ( , drstambough@fuse.net). Am J Orthop. 2008;37(2): Copyright Quadrant HealthCom Inc Spontaneous or idiopathic osteonecrosis of the medial femoral condyle is a well-recognized cause of acute pain, tenderness over the joint line, effusion, and synovitis. Since the disease was first described by Ahlback and colleagues 1 in 1968, it has been the subject of several studies. Results from history, examination, and clinical studies suggest a complicated problem involving biomechanical and blood supply changes that tend to increase the susceptibility of the medial femoral condyle to avascular necrosis in the presence of meniscal pathology. 2-9 It remains unclear if the focal type of osteonecrosis arises from the insult of the arthroscopy or from an underappreciation of the disease in its early stages. There are 2 types of avascular necrosis in the skeleton. The first, which occurs more commonly in patients aged 50 years or older, is focal spontaneous osteonecrosis (SO); the second, which tends to occur in patients aged 30 to 50, is secondary osteonecrosis (2nd ON). The clinical presentations of these types of osteonecrosis must be distinguished when diagnosing and treating patients. SO is associated with tenderness over the joint line, unilateral knee involvement, and acute pain exacerbated by increased weight-bearing. 4,8,10,11 With SO, most patients can remember the exact moment of symptom onset, and they describe pain increasing at night or at rest. 1,4,8,10-12 In contrast, 2nd ON generally shows bilateral involvement of multiple joints with gradual onset of diffuse pain. 8 Secondary osteonecrosis is commonly associated with such predisposing factors as corticosteroid therapy, alcoholism, and systemic lupus erythematosus. 2,5,8,13-15 In patients with knee pain, early diagnosis requires a high index of suspicion for SO, as the diagnosis may not become apparent until months or years after symptom onset. Radiography, magnetic resonance imaging (MRI), and radionuclide bone scanning have proved capable of distinguishing SO from 2nd ON. 8 MR and bone scan images are commonly used to identify the disease in its early stages, and plain films are commonly used to rule out advanced disease when disease duration is not clear. Radionuclide techniques tend to confirm all 4 osteonecrosis stages. 8,10,11,16 Without early detection, SO treatment can become complicated by the treatment required for the apparent overlying pathologies (eg, degenerative medial meniscal tears). When patients aged 50 years or older present with acute onset of medially-based knee pain, the most common differential diagnosis includes SO, medial compartment osteoarthritis, and degenerative medial meniscus pathology. Here we describe 2 cases of SO diagnosed and treated initially as degenerative medial meniscus tears, and we illustrate the clinical diagnostic features of the disease. Case Reports Case 1 A woman in her early 50s presented to her local orthopedist with left knee pain and swelling that had progressively worsened over 3 weeks. The patient noted that the pain was exacerbated when walking and standing and partly relieved at rest. She also complained of sleeping problems, with an occasional increase in pain at night. The patient was 5 feet 6 inches tall, weighed 185 pounds, and was a nonsmoker of general good health, except for hypercholesterolemia. She had a completely benign medical history in regard to the knee, which to our knowledge included no prior injuries and no corticosteroid steroid treatments. Physical examination revealed tenderness about the medial joint line but not about the medial distal femoral condyle. Range of motion was slightly restricted in flexion. The patient had mild patellofemoral crepitus, a small effusion, and diffuse synovitis. The collateral and cruciate ligaments were intact, and the hip and neurovascular examinations were normal. She had a positive McMurray sign. At presentation, weight-bearing plain films showed mild narrowing of the medial joint line and early medial compartmental osteoarthritis, and T 2 -weighted MR images showed a displaced degenerative tear involving the posterior horn of the medial meniscus with a Baker cyst measuring 5.0 cm posteromedially (Figures 1A, 1B) and moderate chondromalacia of the medial compartment with moderate joint effusion, but no evidence of SO. These images were obtained approximately 3 weeks before index surgery. February
2 Focal Spontaneous Osteonecrosis and Medial Meniscus Tear A B A B Figure 1. Case 1 preoperative fat-suppressed T 2 -weighted coronal (A) and sagittal (B) magnetic resonance images show posterior horn medial meniscus pathology and no recognizable evidence of focal spontaneous osteonecrosis of the medial femoral condyle. All conservative measures, including physical therapy, use of nonsteroidal anti-inflammatory drugs, and intraarticular corticosteroid injections, failed to relieve the patient s symptoms. Arthroscopy of the knee was then scheduled for approximately 6 weeks after symptom onset. With the patient under general anesthesia and in the supine position, the surgery was performed with a 30 videoarthroscopy system. The principal pathology was located in the medial compartment, where there was an irreparable complex tear of the posterior horn of the medial meniscus consistent with the patient s symptoms. In addition, there was a radial and longitudinal component along with mild chondromalacia of the undersurface of the patella, without significant arthritis. The anterior cruciate ligament (ACL) and the lateral meniscus were both intact. The patient did not have a chondroplasty, nor were any electrothermal therapies applied. The procedure proceeded without complications. By 9 weeks after surgery, the patient s knee findings and pain complaints had not improved but worsened. The patient presented with gradually increasing recurrent medially based knee pain exacerbated by use and relieved at rest. Despite prior aspiration and an intra-articular steroid injection (triamcinolone acetonide), symptoms persisted. Additional physical therapy had not been effective. There was no interval trauma. Physical examination revealed thickening and swelling around the medial joint space (1+ effusion). There was no pes anserinus tenderness or neurovascular change. The patient did not have any restricted hip motion or gait abnormalities that would suggest the knee pain was referred from the hip. Range of motion was -5 to Plain films obtained approximately 9 weeks after surgery showed mild to moderate osteoarthritis of the patellofemoral joint and mild arthritis of the medial joint space with mild joint space narrowing in the knee. There was no significant osteophyte formation. Compared with the right knee joint space, the left showed a 50% reduction. Figure 2. Case 1 postoperative fat-suppressed T 2 -weighted coronal (A) and sagittal (B) magnetic resonance images show osteonecrosis and collapse of the medial femoral condyle, stage IV. Technetium bone scans, also obtained approximately 9 weeks after surgery, revealed increased uptake at the medial joint space. Cultures were negative at this time. Plain films obtained 6 to 8 months after surgery showed a large osteochondral defect (1.5x1.0 cm) in the medial femoral condyle involving the weight-bearing portion, consistent with SO. There were secondary degenerative changes, medially of the distal femur and proximal tibia, with progressive varus deformity. MR images obtained around the same time showed osteonecrosis and collapse of the medial femoral condyle, which fit the clinical pattern of a stage IV lesion (Figures 2A, 2B). In addition, the patient still had a Baker cyst (4.0x1.0 cm) in the medial aspect of the knee and severe complete secondary chondromalacia of both the medial femoral condyle and the medial proximal tibial plateau. No new medial meniscal tear was seen. The patient was offered an elective left medial total knee arthroplasty. The patient declined the procedure and progressed to advanced medial compartment osteoarthritis with varus deformity and no resolution of pain. Case 2 A man in his mid 50s presented with acute and severe medially-based right knee pain that had progressively worsened over a week. The patient was 5 feet 5 inches tall, weighed approximately 250 pounds, and was a nonsmoker with hypertension, generalized osteoarthritis, and severe degenerative disc disease. The disabling pain made weight-bearing impossible. There was no recent history of trauma, and the patient denied popping, snapping, effusion, bleeding, and ecchymosis. To our knowledge, he had not undergone any previous knee injury or any form of corticosteroid treatment other than the single intra-articular cortisone injection (triamcinolone acetonide) given at presentation, and to which he had not responded. Physical examination revealed that the right knee pain was localized along the medial collateral ligament (MCL). Tenderness was evident medially along the collat- 82 The American Journal of Orthopedics
3 C. Brown and J. L. Stambough Figure 3. Case 2 12 days before surgery, fat-suppressed T 2 - weighted coronal (A) and sagittal (B) magnetic resonance images show posterior horn medial meniscus pathology. There is no definitive evidence of focal spontaneous osteonecrosis of the medial femoral condyle, but there may be, in retrospect, some subtle changes at the articular surface medially. A surgeon who notices these changes should follow the patient and consider bone scanning. eral ligament and pes anserinus but mostly the joint line. The MCL was intact, as were the ACL and the posterior cruciate ligament (PCL). The patellofemoral joint was asymptomatic, and the patient was neurovascularly intact. Initial plain films obtained at 1 week were negative and showed no loose bodies. MR images obtained 1.5 and 3 weeks before the index surgery showed a degenerative complex tear of the posterior horn and midbody of the medial meniscus with moderate to marked adjacent medial compartment chondromalacia (Figures 3A, 3B). There was also a small effusion with slight extension of fluid into the semimembranosus and gastrocnemius bursa. Diagnostic and surgical videoarthroscopy of the right knee was scheduled. At videoarthroscopy, with the patient under general anesthesia, partial medial meniscectomy and chondroplasty of the medial femoral chondral were performed. The partial meniscectomy involved basket resection of the majority of the posterior horn of the medial meniscus, which was unstable because of radial and horizontal components of the degenerative medial meniscus tear. The chondroplasty involved the articular weight-bearing surface of the medial femoral condyle. A mechanical shaver was used in this procedure, but drilling and electrothermal therapy were not required. The unstable osteochondral flap and the fraying of the articular cartilage, consistent with Outerbridge grade III changes, were addressed over an area of approximately 3 to 4 cm, but electrothermal therapies were not applied. The patient s condition worsened rapidly after surgery. The patient did not want to bear weight because of the severe pain. He continued having severe recurrent medially based pain and effusions (1+/2+), and a mild varus deformity was rapidly developing. Additional physical therapy, an additional intra-articular injection of steroids Figure 4. Case 2 22 days after surgery, fat-suppressed T 2 - weighted coronal (A) and sagittal (B) magnetic resonance images show a frank osteochondral fracture of the medial femoral condyle and associated avascular necrosis of a large, detached, nondisplaced osteochondral fragment. (triamcinolone acetonide), and rest all failed to relieve symptoms 3 weeks after surgery. Physical examination revealed normal motion and no cruciate or collateral ligament instability. There was medial tenderness, particularly over the femoral condyle. Plain films obtained approximately 3 weeks after surgery now clearly showed an osteochondral defect to the medial femoral condyle and a 75% collapse in the medial compartment. Standard sagittal, axial, and coronal MR images obtained around the same time showed intermediate grade II to III patellofemoral chondromalacia with minimal joint effusion. A frank osteochondral fracture had developed on the weight-bearing aspect of the medial femoral condyle, with associated osteonecrosis of a large, detached, but nondisplaced osteochondral fragment (3x1.5 cm x 4 mm in depth) (Figures 4A, 4B). As unrelenting severe pain and varus deformity continued over several months, a cemented total knee arthroplasty (using a PCL-sacrificing technique) was performed on the right knee. The avascular medial femoral condyle was resected and grafted from resected bone as needed. A cystic lesion (1.5x1.0 cm x 8 mm) was aggressively curettaged and locally grafted. No complications occurred during the procedure, and surgical bone pathology was consistent with avascular necrosis. The patient had good pain relief, but range of motion was slightly decreased in flexion (0-100 ). At 2-year follow-up, there were no clinical or radiographic signs of implant loosening and no residual pain. Discussion Since Ahlback and colleagues 1 first described the symptoms commonly associated with SO, several cases have been documented, illustrating a high incidence rate of SO of the medial femoral condyle. 2,4-9 The exact etiology of SO after meniscectomy is unclear, but a literature search turned up 3 theories for development of osteonecrosis of the knee (Figure 5). February
4 Focal Spontaneous Osteonecrosis and Medial Meniscus Tear FOCAL KNEE P PAIN AI (Medial N (Media or Lateral) l or L a tera l) B MENISCUS M U S TEAR T E A R MENISCUS M U S TEART E A R A ARTHROSCOPY A SPONTANEOUS OSTEONECROSISSI S Figure 5. Theories for the development of focal spontaneous osteonecrosis (SO) of the knee. Natural-history-of-SO theory (A): Knee pain results from idiopathic SO, which is subclinical (patient in early stage of disease, diagnosis not apparent). Altered-stressbiomechanics theory (B): Knee pain results from meniscus tearing, which secondarily causes abnormal loading leading to SO. Iatrogenic theory (C): Knee pain results from medial meniscus tear, and subsequent arthroscopy may contribute to SO. Three Theories for the Development of Knee Osteonecrosis The first may be referred to as the natural-history-of-so theory, according to which the patient is in the early stage of the disease process and is symptomatic, but the diagnosis is not yet apparent. The disease itself has been described as following a 4-stage course: I, generally no observational findings; II, small flattening of the medial femoral condyle; III, increased flattening with an apparent lesion indicated by a sclerotic halo; IV, articular cartilage collapse and additional degenerative changes that cause varus or valgus deformities. 8,11,17 Soucacos and colleagues 11 reported that the interval for stage I after symptom onset was 6 to 8 weeks; stage II, 2 to 4 months; stage III, 3 to 6 months; stage IV, 9 months to 1 year. With an evolving disease like osteonecrosis, it is difficult to establish whether positive meniscal pathology is a predisposing factor or simply an overlying pathology that may be present during the course of the disease. Reports have emphasized that preexisting meniscal pathology correlates well with the later overlying diagnosis of SO and indicates a high rate of SO of the medial femoral condyle after arthroscopy. 2,4-7,9 The Table illustrates a series of patients who had concurrent meniscus pathology and were later diagnosed with SO after surgery. The second theory may be referred to as the alteredstress-biomechanics theory, according to which meniscus tearing causes altered knee loading leading to SO. Knee overloading has been suggested as possibly causing microfractures and later ischemic conditions. 7-10,18 In a study of 33 patients (mean age, 60 years), Norman and Baker 4 speculated that meniscal pathology may play a crucial role in the disease evolution by adding weight-bearing stress to the surrounding articular surface. Muscolo and colleagues 7 similarly suggested that abnormal loading may be involved, and they indicated that 50% of the force was transferred through the meniscus in extension and 85% when the knee is flexed at 90. C Altered Blood Supply: A Common Thread? n all 3 theories, development of SO in the medial femoral Icondyle appears to be a compound problem involving an altered blood supply. 2-5 In particular, vascular compromise of the subchondral bone has been described as contributing to the advance of the disease. The resulting insufficient blood flow produces edema and increased pressure within the problem area, and these changes further impede the vascular supply. 5,10 Examining histopathologic studies of 7 patients with SO in the medial femoral condyle, Yamamoto and Bullough 18 indicated that the primary event leading to later stages of the disease may have been a subchondral fracture resulting from underlying osteoporosis. Thrombosis, atherosclerosis, occlusion of venous flow, and marrow changes have been suggested as possible factors leading to ischemic conditions. 8 With regard to blood supply, Reddy and Fredrick3 provided a plausible explanation for a high incidence of avascular necrosis of the medial condyle relative to the lateral femoral condyle. The vasculature of 12 adult cadaver legs showed a differential pattern of blood flow between the medial and lateral femoral condyles. The medial femoral condyle received vascular flow predominantly from the superior medial geniculate artery, with small contributions from branches of the popliteal artery. More important, the vascular supply was primarily to the middle third of the condyle and in effect created an anterior watershed zone. The medial condyle collateral system was lacking compared with the lateral femoral condyle system, which was supplied by both the superior lateral geniculate and anastomotic branches of the inferior lateral geniculate. The finding of an anterior watershed zone and diminished collateral system may also help explain the high incidence rate of SO of the medial femoral condyle. The last theory may be referred to as the iatrogenic theory, according to which arthroscopy after a medial meniscus tear may contribute to SO. Muscolo and colleagues 7 claimed that removal of more than 15% to 34% of the medial meniscus can increase the contact pressure such that the contact area may be reduced by as much as 50% after meniscectomy. Kobayashi and colleagues 2 reported that bone marrow changes in 32 patients after meniscectomy were evident only on the surgical side for both lateral and medial meniscal procedures. They concluded that the degree of meniscectomy affected prevalence of postmeniscectomy bone changes. Progression of SO on Scans Plain films, MR images, and bone scans are all used to verify changes in the structure of the skeleton. With the progression of SO through 4 stages, it appears that there is an interval after symptom onset in which the disease in its earlier stages may not be readily distinguished with MRI and radiography. In a study of 6 patients with 84 The American Journal of Orthopedics
5 C. Brown and J. L. Stambough meniscus pathology (4 medial and 2 lateral meniscal tears), Johnson and colleagues 6 found that the SO diagnosis was unidentifiable 6 weeks before surgery, after symptom onset, but was made after partial meniscectomy at a mean of 4 months. Kobayashi and colleagues 2 reported that bone marrow changes were most often visible on MR images within 8 months after surgery. In an animal study, Nakamura and colleagues 19 observed that it may take up to 4 weeks after symptom onset to confirm SO by MRI. Muscolo and colleagues 7 reported on 8 patients who had medial meniscus tears within a mean of 18 weeks before MRI diagnosis and showed evidence of SO after arthroscopy. Examining plain films, Norman and Baker 4 reported the earliest evidence of flattening of the medial condyle (3 months after symptom onset). Also using plain films, al-rowaih and colleagues 20 reported that the typical SO lesion in 14 knees was observed at a mean of 28 weeks. These cases also seem to emphasize the evolution of the disease process. Treatment and Prognosis The prognosis and treatment options for patients with SO seem to vary with the extent of the lesion. Ecker and Lotke 10 noted that lesions that make up more than 50% of the condyle have a poor prognosis. Lotke and colleagues 21 found a poor prognosis for lesions when the ratio of its transverse width to the affected condyle was larger than 0.4. Muheim and Bohne 22 found that a ratio of lesion width to lesion length indicated a poor prognosis with lesions larger than 5 cm 2. Finding small lesions early on tends to result in good prognoses with conservative treatments of therapy and limited weight-bearing activity. 5,10,11 Larger lesions tend to require surgical interventions ranging from débridement, core decompression, and osteotomy to prosthetic replacement. 8,10,11 Many factors (eg, extent and location of bone necrosis) ultimately determine the prognosis and can be difficult to quantify in a patient. When patients...present with medially based knee pain and have normal plain films and MR images, scintigraphy should be performed... The majority of cases show early signs of SO with MRI during the initial diagnosis. 2,7-10 However, discrepancies have been reported in the specificity of MRI when used to detect early changes in an evolving disease, such as avascular necrosis, and bone scans have shown increased uptake in patients who develop SO when MR images and plain films do not show initial abnormalities in the subchondral bone. 7,8,11 For example, in 1997, after reviewing 101 patients with SO not related to a degenerative meniscus, Soucacos and colleagues 11 found normal plain films at 6 to 8 weeks and generally no T 2 -weighted abnormalities, but positive scintigraphy. At 2 to 4 months, some abnormalities appeared on plain films and MR images, but diagnoses were mainly on the basis of technetium 99 bone scans. After 3 to 6 months, significant abnormalities were apparent on plain films, MR images, and bone scans. Pollack and colleagues 16 reported on 10 knees with SO symptoms and positive scintigraphy; 2 of the 10 knees appeared normal on MRI. Similarly, Bjorkengren and colleagues, 17 in a study of 16 patients with SO and positive radionuclide bone scans, found 2 patients with normal T 1 -weighted MR images and 4 patients with normal T 2 -weighted MR images. MRI and radiography are better tools for diagnosing SO in its later stages, while radionuclide bone scans may provide evidence of early changes suggestive of an underlying pathology of SO. 6,8-11 With there being variation in the reported appearance of SO both before and after surgery, we should not underestimate the importance of ruling out SO in its early stages, especially when a meniscal pathology could parallel these stages. Conclusions We presented 2 cases of SO of the medial femoral condyle after arthroscopy in 2 patients with no history of trauma or identifiable predisposing SO factors other than age. Similarly, no predisposing 2nd ON factors were identified. Initial preoperative MR images and plain films showed medial meniscal tears and no definitive evidence of SO. Radionuclide bone scans were not used in preoperative diagnosis because both patients had evident medial pathology consistent with symptoms. Failure to improve with rest and continued pain at night and/or at rest should suggest the diagnosis of SO. SO of the medial femoral condyle is a significant finding in conjunction with a degenerative medial meniscus tear. When patients, particularly older patients, present with medially based knee pain and have normal plain films and MR images, scintigraphy should be performed so that misdiagnosis and unneeded arthroscopy can be avoided. Early recognition of SO may help prevent collapse, deformity, and secondary osteoarthritis of the involved joint space. SO is relatively uncommon compared with medial meniscus tears, and this should be kept in mind when the patient s knee pain is nonmechanical, worsens with inactivity or at night, fails to improve after arthroscopy, or is out of proportion to what might be expected from meniscal pathology alone. Whether the development of SO after arthroscopy is due to the procedure, the unrecognizable early-stage degenerative joint disease, or the meniscal tear itself has not yet been established, but meniscal tears have been reported as existing before the disease develops (Figure 5). Most likely, SO is a separate entity, and factors such as medial meniscus tears and arthroscopy do not cause SO but may February
6 Focal Spontaneous Osteonecrosis and Medial Meniscus Tear Table. Summary of Reported Cases of Focal Spontaneous Osteonecrosis (SO) With Meniscus Pathology* Mean Steroid Chondro- Arthroscopic Area SO or Study Sex Age (y) Use MMT LMT malacia Arthroscopy Meniscectomy Time SO Change Muscolo et al 7 M 54 No Flap FC Yes Partial 16 wk Focal SO MFC F 57 No Flap Yes Total 20 wk Focal SO MFC F 62 No Flap FC Yes Partial 6 wk Focal SO MFC F 65 No BH Yes Total 36 wk Focal SO MFC F 65 No LT FC Yes Total 8 wk Focal SO MFC M 69 No HT Yes Total 7 wk Focal SO MFC M 70 No HT FC Yes Partial 32 wk Focal SO MFC M 75 No LT Yes Total 17 wk Focal SO MFC Brahme et al 9 4M/3F HT 6FC Yes 7 partial with 2-14 mo 6 focal 5 SO MFC 2 BH debridge 1 SO MFC/TP 1 AT 1 both Yes 1 focal 1 SO LFC/TP Johnson et al 6 F 79 No MMT FC Yes Partial, CP 3 mo Focal SO MFC M 58 No MMT Both Yes Partial, CP 5 mo Focal SO MFC F 75 No LMT Yes Partial 4 mo Focal SO LFC M 41 No MMT Both Yes Partial 6 mo Focal SO MFC M 54 No MMT FC Yes Partial, CP 3 mo Focal SO TP F 53 No MMT FC Yes Partial, CP 3 mo Focal SO MFC F 62 No LMT FC Yes Partial, CP 4 mo Focal SO TP Santori et al 5 21 Radial/ Yes Partial <1 mo Focal SO MFC posterior horn F 47 BH Yes Partial 1 mo Focal SO MFC Norman & Baker 4 14M/19F 60 45% 21 MMT No 31 SO MFC intra- 6 no tear 1 SO LFC articular 6 N/A 1 SO MFC/LFC Kobayashi et al 2 51M/42F MMT 49 LMT 17 medial/ Yes 57 partial 8 mo Marrow changes in 10 lateral 36 total 16 FC/TP 6 FC 10 TP Narvaez et al 8 5M/8F 49 2 gluco- 3 MMT No 105 d 4 polytopic 4 bilateral with corticoid ± 9 focal FC/TP 2nd ON 2 alcoholism 120 d 4 MFC/TP 2 renal transplant 2 unilateral 1 thalassemia FC/TP 1 leukemia 2 LFC 3 systemic steroid 1 MFC 7M/17F 66 No 22 MMT No 24 focal 19 SO MFC *MMT indicates medial meniscus tear; LMT, lateral meniscus tear; BH, bucket handle; LT, longitudinal tear; HT, horizontal tear; AT, anterior tear; CP, chondroplasty; Time, postoperative time until SO diagnosis; MFC, medial femoral condyle; TP, tibial plateau; LFC, lateral femoral condyle; FC, femoral condyle; 2nd ON, secondary osteonecrosis. Outerbridge 23 classification grade II/III. 3 SO TP 2 SO MFC/LFC 86 The American Journal of Orthopedics
7 C. Brown and J. L. Stambough hasten SO symptom onset because of secondary collapse or osteoarthritis. This scenario seems consistent with the cases presented here and the literature reviewed. Authors Disclosure Statement The authors report no actual or potential conflict of interest in relation to this article. References 1. Ahlback S, Bauer GC, Bohne WH. Spontaneous osteonecrosis of the knee. Arthritis Rheum. 1968;11: Kobayashi Y, Kimura M, Higuchi H, Terauchi M, Shirakura, Takagishi K. Juxta-articular bone marrow signal changes on magnetic resonance imaging following arthroscopic meniscectomy. Arthroscopy. 2002;18: Reddy AS, Fredrick RW. Evaluation of the intraosseous and extraosseous blood supply to the distal femoral condyles. Am J Sports Med. 1998;26: Norman A, Baker ND. Spontaneous osteonecrosis of the knee and medial meniscal tears. Radiology. 1978;129: Santori N, Condello V, Adriana E, Mariani PP. Osteonecrosis after arthroscopic medial meniscectomy. Arthroscopy. 1995;11: Johnson TC, Evans JA, Gilley JA, DeLee JC. Osteonecrosis of the knee after arthroscopic surgery for meniscal tears and chondral lesions. Arthroscopy. 2000;16; Muscolo DL, Costa-Paz M, Makino A, Ayerza MA. Osteonecrosis of the knee following arthroscopic meniscectomy in patients over 50-years old. Arthroscopy. 1996;12: Narvaez J, Narvaez JA, Rodriguez-Moreno J, Roig-Escofet D. Osteonecrosis of the knee: differences among idiopathic and secondary types. Rheumatology (Oxford). 2000;39: Brahme SK, Fox JM, Ferkel RD, Friedman MJ, Flannagan BD, Resnick DL. Osteonecrosis of the knee after arthroscopic surgery. Diagnosis with MR imaging. Radiology. 1991;178: Ecker ML, Lotke PA. Spontaneous osteonecrosis of the knee. J Am Acad Orthop Surg. 1994;2: Soucacos NP, Xenakis T, Beris A, Soucacos KP, Georgoulis A. Idiopathic osteonecrosis of the medial femoral condyle. Clin Orthop. 1997;341: Lotke PA, Ecker ML, Alavi A. Painful knees in older patients. Radionuclide diagnosis of possible osteonecrosis with spontaneous resolution. J Bone Joint Surg Am. 1997;59; Havel PE, Ebraheim NA, Jackson WT. Steroid induced bilateral avascular necrosis of the lateral femoral condyles. Clin Orthop. 1989;243: Kelman GJ, William GW, Colwell CW Jr. Steroid-related osteonecrosis of the knee: two case reports and a literature review. Clin Orthop. 1990;257: Siemsen JK, Brook J, Meister L. Lupus erythematosus and avascular bone necrosis: a clinical study of 3 cases and review of the literature. Arthritis Rheum. 1962;5: Pollack MS, Dalinka MA, Kressel HY, Lotke PA, Spritzer CE. Magnetic resonance imaging in the evaluation of suspect osteonecrosis of the knee. Skeletal Radiol. 1987;19: Bjorkengren AG, al-rowaih A, Lindstrand A, Wingstrand H, Thorngren KG, Pettersson H. Spontaneous osteonecrosis of the knee: value of MR imaging in determining prognosis. AJR Am J. Roentgenol. 1990;154: Yamamoto T, Bullough PG. Spontaneous osteonecrosis of the knee: the result of subchondral insufficiency fracture. J Bone Joint Surg Am. 2000;82: Nakamura T, Matsumoto T, Nishino M, Tomita K, Kadoya M. Early magnetic resonance imaging and histological findings in a model of femoral head necrosis. Clin Orthop. 1997;334: al-rowaih A, Lindstrand A, Bjorkengren A, Wingstrand H, Thorngren KG. Osteonecrosis of the knee. Diagnosis and outcome in 40 patients. Acta Orthop Scand. 1991;62: Lotke PA, Abend JA, Ecker ML. The treatment of osteonecrosis of the medial femoral condyle. Clin Orthop. 1982;171: Muheim G, Bohne WH. Prognosis in spontaneous osteonecrosis of the knee. Investigation by radionuclide scintimetry and radiography. J Bone Joint Surg Br. 1970;52: Outerbridge RE. The etiology of chondromalacia patellae. J Bone Joint Surg Br. 1961;43: This paper will be judged for the Resident Writer s Award Resident Writer s he 2008 Resident Writer s Award competition is sponsored through an unrestricted grant provided by T DePuy, a Johnson & Johnson company. Orthopedic residents are invited to submit original studies, reviews, or case studies for publication. Papers published in 2008 will be judged by The American Journal of Orthopedics Editorial Board. Honoraria will be presented to the winners at the 2009 AAOS annual meeting. $1,500 for the First-Place Award $1,000 for the Second-Place Award $500 for the Third-Place Award To qualify for consideration, papers must have the resident as the first-listed author and must be accepted through the journal s standard blinded-review process. Papers submitted in 2008 but not published until 2009 will automatically qualify for the 2009 competition. Manuscripts should be prepared according to our Information for Authors and submitted via our online submission system, Editorial Manager, at Through an unrestricted grant provided by February
Spontaneous osteonecrosis of the knee. Treatment and evolution.
 Spontaneous osteonecrosis of the knee. Treatment and evolution. J. R. Valentí Nín; M. Leyes; D. Schweitzer ABSTRACT We performed a retrospective study on 21 patients affected by unilateral spontaneous
Spontaneous osteonecrosis of the knee. Treatment and evolution. J. R. Valentí Nín; M. Leyes; D. Schweitzer ABSTRACT We performed a retrospective study on 21 patients affected by unilateral spontaneous
Idiopathic osteonecrosis of the medial tibial plateau
 Idiopathic osteonecrosis of the medial tibial plateau J. R. Valenti J. A. Illescas A. Barriga R. Dölz ABSTRACT Osteonecrosis of the medial tibial plateau is characterized by acute pain on the medial aspect
Idiopathic osteonecrosis of the medial tibial plateau J. R. Valenti J. A. Illescas A. Barriga R. Dölz ABSTRACT Osteonecrosis of the medial tibial plateau is characterized by acute pain on the medial aspect
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
American College of Physicians 2013 Ohio Chapter Scientific Meeting Columbus, OH October 11, 2013
 American College of Physicians 2013 Ohio Chapter Scientific Meeting Columbus, OH October 11, 2013 Paul J. Gubanich, MD, MPH Assistant Professor of Internal Medicine/Sports Medicine Team Physician, Ohio
American College of Physicians 2013 Ohio Chapter Scientific Meeting Columbus, OH October 11, 2013 Paul J. Gubanich, MD, MPH Assistant Professor of Internal Medicine/Sports Medicine Team Physician, Ohio
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Spontaneous Osteonecrosis of Knee After Arthroscopy Is Not Necessarily Related to the Procedure
 An Original Study Spontaneous Osteonecrosis of Knee After Arthroscopy Is Not Necessarily Related to the Procedure Caitlin Chambers, MD, ATC, Joseph G. Craig, MD, Raimonds Zvirbulis, MD, and Fred Nelson,
An Original Study Spontaneous Osteonecrosis of Knee After Arthroscopy Is Not Necessarily Related to the Procedure Caitlin Chambers, MD, ATC, Joseph G. Craig, MD, Raimonds Zvirbulis, MD, and Fred Nelson,
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Oh My Aching Knee. Oh My Aching Knee WHO AM I? 10/15/2012. Jan Pieter Hommen, MD Orthopedic Surgeon Sports Medicine Arthroscopy Joint Replacements
 Oh My Aching Knee Jan Pieter Hommen, MD Orthopedic Surgeon Sports Medicine Arthroscopy Joint Replacements Oh My Aching Knee Jan Pieter Hommen, MD Orthopedic Surgeon Sports Medicine Arthroscopy Joint Replacements
Oh My Aching Knee Jan Pieter Hommen, MD Orthopedic Surgeon Sports Medicine Arthroscopy Joint Replacements Oh My Aching Knee Jan Pieter Hommen, MD Orthopedic Surgeon Sports Medicine Arthroscopy Joint Replacements
Original Date: December 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries
 Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14 BEFORE: A. T. Patterson: Vice-Chair HEARING: November 3, 2014 at Toronto Oral DATE OF DECISION: April 17, 2015 NEUTRAL CITATION: 2015
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14 BEFORE: A. T. Patterson: Vice-Chair HEARING: November 3, 2014 at Toronto Oral DATE OF DECISION: April 17, 2015 NEUTRAL CITATION: 2015
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Osteonecrosis of the knee: differences among idiopathic and secondary types
 Rheumatology 000;39:98 989 Osteonecrosis of the knee: differences among idiopathic and secondary types J. Narváez, J. A. Narváez, J. Rodriguez-Moreno and D. Roig-Escofet Department of Rheumatology, Hospital
Rheumatology 000;39:98 989 Osteonecrosis of the knee: differences among idiopathic and secondary types J. Narváez, J. A. Narváez, J. Rodriguez-Moreno and D. Roig-Escofet Department of Rheumatology, Hospital
Imaging the Knee 17/10/2017. Friction syndrome Common in runners or cyclists Fluid between ITB and Lateral femoral condyle
 17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
FILED: KINGS COUNTY CLERK 04/23/ :08 PM INDEX NO /2016 NYSCEF DOC. NO. 29 RECEIVED NYSCEF: 04/23/2018
 SUPREME COURT OF THE STATE OF NEW YORK COUNTY OF KINGS ----------------------------------------------------------------X BETHZAIDA CARO, Plaintiff(s), -against- PHYSICIAN' PHYSICIAN'S AFFIRMATION Index
SUPREME COURT OF THE STATE OF NEW YORK COUNTY OF KINGS ----------------------------------------------------------------X BETHZAIDA CARO, Plaintiff(s), -against- PHYSICIAN' PHYSICIAN'S AFFIRMATION Index
What is Medial Plica Syndrome?
 What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
I have nothing to disclose
 Management of Common Knee Disorders: What You Knee d to Know UCSF Essentials of Women s Health July 8, 2015 Carlin Senter, M.D. I have nothing to disclose Learning objectives: in 1 hour you will be able
Management of Common Knee Disorders: What You Knee d to Know UCSF Essentials of Women s Health July 8, 2015 Carlin Senter, M.D. I have nothing to disclose Learning objectives: in 1 hour you will be able
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
In comparison to anterior and lateral knee pain, chronic. Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain.
 [ Primary Care ] Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain William E. Bylund, BS,* and Kevin de Weber, MD Context: Semimembranosus tendinopathy (SMT) is an uncommon cause
[ Primary Care ] Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain William E. Bylund, BS,* and Kevin de Weber, MD Context: Semimembranosus tendinopathy (SMT) is an uncommon cause
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
Non-Surgical vs. Surgical Treatment of Meniscus Tears of the Knee
 Non-Surgical vs. Surgical Treatment of Meniscus Tears of the Knee Greg I. Nakamoto, MD FACP Section of Orthopedics and Sports Medicine Virginia Mason Medical Center CASE 1 45 y/o construction worker sent
Non-Surgical vs. Surgical Treatment of Meniscus Tears of the Knee Greg I. Nakamoto, MD FACP Section of Orthopedics and Sports Medicine Virginia Mason Medical Center CASE 1 45 y/o construction worker sent
Introduction Knee Anatomy and Function Making the Diagnosis
 Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
MRI of the Knee: Part 2 - menisci. Mark Anderson, M.D. University of Virginia Health System
 MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
Chondral Disease of the Knee
 Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
Diagnosis and Management of Knee Conditions. Jenny Love / Lynn Robertson AFLAR Oct 2009
 Diagnosis and Management of Knee Conditions Jenny Love / Lynn Robertson AFLAR Oct 2009 AIMS Review 4 common Knee Conditions: Anterior knee pain Meniscal Injuries Ligament injuries ACL Osteoarthritis Discuss
Diagnosis and Management of Knee Conditions Jenny Love / Lynn Robertson AFLAR Oct 2009 AIMS Review 4 common Knee Conditions: Anterior knee pain Meniscal Injuries Ligament injuries ACL Osteoarthritis Discuss
MENISCAL INJURY. Meniscus. Anterior Roots. Medial Meniscus. Lateral Meniscus. Posterior Roots. MRI and Arthroscopic Findings
 Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Osteochondritis Dissecans of the Knee. M Lucas Murnaghan MD, MEd, FRCSC
 Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
DECISION NO. 2870/16
 Counsel: H.K., for Worker No one for Employer 2016 ONWSIAT 3235 Ontario Workplace Safety and Insurance Appeals Tribunal Decision No. 2870/16 2016 CarswellOnt 19003, 2016 ONWSIAT 3235 DECISION NO. 2870/16
Counsel: H.K., for Worker No one for Employer 2016 ONWSIAT 3235 Ontario Workplace Safety and Insurance Appeals Tribunal Decision No. 2870/16 2016 CarswellOnt 19003, 2016 ONWSIAT 3235 DECISION NO. 2870/16
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques
 Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Priorities Forum Statement GUIDANCE
 Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
CASE REPORT GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT
 Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
SOFT TISSUE KNEE INJURIES
 SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
An older systematic review looked at the evidence behind the best approach to evaluate acute knee pain in primary care (Ann Int Med.2003;139:575).
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
Case Report Detached Anterior Horn of the Medial Meniscus Mimicking a Parameniscal Cyst
 Case Reports in Orthopedics Volume 2015, Article ID 706241, 4 pages http://dx.doi.org/10.1155/2015/706241 Case Report Detached Anterior Horn of the Medial Meniscus Mimicking a Parameniscal Cyst Shoji Fukuta,
Case Reports in Orthopedics Volume 2015, Article ID 706241, 4 pages http://dx.doi.org/10.1155/2015/706241 Case Report Detached Anterior Horn of the Medial Meniscus Mimicking a Parameniscal Cyst Shoji Fukuta,
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA
 Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Differential Diagnosis
 Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Case 31yo M who sustained an injury to L knee while playing Basketball approximately 2 weeks ago. He describes pivoting and hyperextending his knee, which swelled over the next few days. He now presents
Lateral knee injuries
 Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
DISEASES AND DISORDERS
 DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
Evaluation and Management of Knee Pain. Michael Cassat, MD University of Arkansas for Medical Sciences
 Evaluation and Management of Knee Pain Michael Cassat, MD University of Arkansas for Medical Sciences Disclosure I have no actual or potential conflict of interest in relation to this program/presentation.
Evaluation and Management of Knee Pain Michael Cassat, MD University of Arkansas for Medical Sciences Disclosure I have no actual or potential conflict of interest in relation to this program/presentation.
Evaluation and Treatment of Knee Arthritis Classification of Knee Arthritis Osteoarthritis Osteoarthritis Osteoarthritis of Knee
 1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
A comparative study of MRI versus arthroscopic findings in ACL and meniscal injuries of the knee
 International Journal of Research in Orthopaedics Kulkarni OP et al. Int J Res Orthop. 2018 Mar;4(2):198-202 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180123
International Journal of Research in Orthopaedics Kulkarni OP et al. Int J Res Orthop. 2018 Mar;4(2):198-202 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180123
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
MENISCAL INJURIES. (copyright s h palmer 2009) MENISCAL FUNCTION
 (copyright s h palmer 2009) MENISCAL FUNCTION MENISCAL INJURIES Menisci are important for weight bearing, load distribution, joint stability and proprioception. Figure 1: A normal medial meniscus Any load
(copyright s h palmer 2009) MENISCAL FUNCTION MENISCAL INJURIES Menisci are important for weight bearing, load distribution, joint stability and proprioception. Figure 1: A normal medial meniscus Any load
Knee Injury Assessment
 Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Evidence Process for Knee Pain Guideline Research 3/27/3018
 Evidence Process for Knee Pain Guideline Research 3/27/3018 Guideline Review using ADAPTE method and AGREE II instrument 41 Potentially relevant guidelines identified in various resources* Searches done
Evidence Process for Knee Pain Guideline Research 3/27/3018 Guideline Review using ADAPTE method and AGREE II instrument 41 Potentially relevant guidelines identified in various resources* Searches done
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB.
 ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB www.fisiokinesiterapia.biz Overview History Examination X-rays Fractures and Dislocations. Soft Tissue Injuries Other Knee/Lower limb Problems Anatomy
ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB www.fisiokinesiterapia.biz Overview History Examination X-rays Fractures and Dislocations. Soft Tissue Injuries Other Knee/Lower limb Problems Anatomy
BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F ASPLUNDH TREE EXPERT COMPANY
 BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F610272 DAWN POHL ASPLUNDH TREE EXPERT COMPANY CLAIMANT RESPONDENT LIBERTY MUTUAL INSURANCE COMPANY, RESPONDENT INSURANCE CARRIER OPINION
BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F610272 DAWN POHL ASPLUNDH TREE EXPERT COMPANY CLAIMANT RESPONDENT LIBERTY MUTUAL INSURANCE COMPANY, RESPONDENT INSURANCE CARRIER OPINION
Case Report Double-Layered Lateral Meniscus in an 8-Year-Old Child: Report of a Rare Case
 Case Reports in Orthopedics Volume 2016, Article ID 5263248, 4 pages http://dx.doi.org/10.1155/2016/5263248 Case Report Double-Layered Lateral Meniscus in an 8-Year-Old Child: Report of a Rare Case Susumu
Case Reports in Orthopedics Volume 2016, Article ID 5263248, 4 pages http://dx.doi.org/10.1155/2016/5263248 Case Report Double-Layered Lateral Meniscus in an 8-Year-Old Child: Report of a Rare Case Susumu
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 43 rd Annual Symposium on Sports Medicine UT Health Science Center San Antonio School of Medicine January 22-23, 2016 Intra-articular / Extra-synovial 38 mm length / 13 mm width Fan-shaped structure narrowest-midportion
43 rd Annual Symposium on Sports Medicine UT Health Science Center San Antonio School of Medicine January 22-23, 2016 Intra-articular / Extra-synovial 38 mm length / 13 mm width Fan-shaped structure narrowest-midportion
Epidemiology. Meniscal Injury & Repair. Meniscus Anatomy. Meniscus Anatomy
 Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
Osteonecrosis - Spectrum of imaging findings
 Osteonecrosis - Spectrum of imaging findings Poster No.: C-1861 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Ninitas, A. L. Amado Costa, A. Duarte, I. Távora ; Lisbon/ 1 1 2 1 1 2 PT, Costa
Osteonecrosis - Spectrum of imaging findings Poster No.: C-1861 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Ninitas, A. L. Amado Costa, A. Duarte, I. Távora ; Lisbon/ 1 1 2 1 1 2 PT, Costa
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Case Report Double-Layered Lateral Meniscus Accompanied by Meniscocapsular Separation
 Case Reports in Orthopedics Volume 2015, Article ID 357463, 5 pages http://dx.doi.org/10.1155/2015/357463 Case Report Double-Layered Lateral Meniscus Accompanied by Meniscocapsular Separation Aki Fukuda,
Case Reports in Orthopedics Volume 2015, Article ID 357463, 5 pages http://dx.doi.org/10.1155/2015/357463 Case Report Double-Layered Lateral Meniscus Accompanied by Meniscocapsular Separation Aki Fukuda,
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
KNEE EXAMINATION. Tips & Tricks from an Emergency Physician Perspective. EM Physicians Less Exposed to MSK Medicine
 KNEE EXAMINATION Tips & Tricks from an Emergency Physician Perspective Dr P O CONNOR Emergency Medicine Physician EUSEM 10/09/2018 EM Physicians Less Exposed to MSK Medicine Musculoskeletal Medicine becoming
KNEE EXAMINATION Tips & Tricks from an Emergency Physician Perspective Dr P O CONNOR Emergency Medicine Physician EUSEM 10/09/2018 EM Physicians Less Exposed to MSK Medicine Musculoskeletal Medicine becoming
11/4/2018 SUBTLETIES OF LOWER EXTREMITY TRAUMA IMAGING SPEAKER DISCLOSURES
 SUBTLETIES OF LOWER EXTREMITY TRAUMA IMAGING Charles S. Resnik, M.D. Professor of Radiology University of Maryland School of Medicine Upon completion of this presentation, participants will be better able
SUBTLETIES OF LOWER EXTREMITY TRAUMA IMAGING Charles S. Resnik, M.D. Professor of Radiology University of Maryland School of Medicine Upon completion of this presentation, participants will be better able
BATES VISUAL GUIDE TO PHYSICAL EXAMINATION. OSCE 4: Knee Pain
 BATES VISUAL GUIDE TO PHYSICAL EXAMINATION OSCE 4: Knee Pain This video format is designed to help you prepare for objective structured clinical examinations, or OSCEs. You are going to observe and participate
BATES VISUAL GUIDE TO PHYSICAL EXAMINATION OSCE 4: Knee Pain This video format is designed to help you prepare for objective structured clinical examinations, or OSCEs. You are going to observe and participate
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Post-injury painful and locked knee
 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 24 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Lower Extremity Impairment Guides Part 4 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 24 Madison, WI 53719 Phone: (608) 663-6355
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Chronic knee pain in adults - a multimodality approach or which modality to choose and when?
 Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
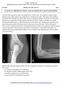 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 10/6/2012 Radiology Quiz of the Week # 93 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 10/6/2012 Radiology Quiz of the Week # 93 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
The Meniscus. History. Anatomy. Anatomy. Blood Supply. Attachments
 History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
Discoid Medial Meniscus Tear, with a Literature Review of Treatments
 Case Report Knee Surg Relat Res 2017;29(3):237-242 https://doi.org/10.5792/ksrr.15.054 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Discoid Medial Meniscus Tear, with a Literature Review
Case Report Knee Surg Relat Res 2017;29(3):237-242 https://doi.org/10.5792/ksrr.15.054 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Discoid Medial Meniscus Tear, with a Literature Review
