Repair of spondylolysis using compression with a modular link and screws
|
|
|
- Emory Nelson
- 5 years ago
- Views:
Transcription
1 Repair of spondylolysis using compression with a modular link and screws F. Altaf, N. A. Osei, E. Garrido, M. Al-Mukhtar, C. Natali, A. Sivaraman, H. H. Noordeen From the Royal National Orthopaedic Hospital, Stanmore, United Kingdom We describe the results of a prospective case series of patients with spondylolysis, evaluating a technique of direct stabilisation of the pars interarticularis with a construct that consists of a pair of pedicle screws connected by a U-shaped modular link passing beneath the spinous process. Tightening the link to the screws compresses bone graft in the defect in the pars, providing rigid intrasegmental fixation. We have carried out this procedure on 20 patients aged between nine and 21 years with a defect of the pars at L5, confirmed on CT. The mean age of the patients was 13.9 years (9 to 21). They had a grade I or less spondylolisthesis and no evidence of intervertebral degeneration on MRI. The mean followup was four years (2.3 to 7.3). The patients were assessed by the Oswestry Disability Index (ODI) and a visual analogue scale (VAS). At the latest follow-up, 18 patients had an excellent clinical outcome, with a significant (p < 0.001) improvement in their ODI and VAS scores. The mean ODI score at final follow-up was 8%. Assessment of the defect by CT showed a rate of union of 80%. There were no complications involving the internal fixation. The strength of the construct removes the need for post-operative immobilisation. F. Altaf, BSc(Hons), MRCS, Specialist Registrar in Trauma and Orthopaedics N. A. Osei, FRCS(Tr & Orth), Spinal Fellow E. Garrido, MRCS, EBOT, Spinal Fellow M. Al-Mukhtar, MRCS, Registrar in Orthopaedics H. H. Noordeen, MD, FRCS(Orth), Consultant Spinal Surgeon Royal National Orthopaedic Hospital, Brockley Hill, Stanmore, Middlesex HA7 4LP, UK. C. Natali, BSc, FRCS(Orth), Consultant Spinal Surgeon A. Sivaraman, FRCS(Orth), Consultant Spinal Surgeon Royal London Hospital, Whitechapel Road, Whitechapel, London E1 1BB, UK. Correspondence should be sent to Mr F. Altaf; farhaanaltaf@hotmail.com 2011 British Editorial Society of Bone and Joint Surgery doi: / x.93b $2.00 J Bone Joint Surg [Br] 2011;93-B:73-7. Received 23 February 2010; Accepted after revision 23 September 2010 A spondylolysis is a defect of the pars interarticularis. Usually there is a complete break in the pars on one or both sides of the neural arch. The condition is often asymptomatic, but may be the cause of pain in the back. Free nerve endings with nociceptive function have been identified in the area of the lysis by Schneiderman et al. 1 Neuropeptides which mediate in the sensation of pain have been described at the site of the defect by Eisenstein et al. 2 The surgical management of symptomatic spondylolysis or isthmic spondylolisthesis was first described by Albee, 3 Hibbs, 4 and Bosworth et al 5 using posterior fusion to stabilise the defect by eliminating the movement segment. Cleveland, Bosworth and Thompson 6 and Watkins 7 described the technique of posterolateral fusion. Kimura 8 was the first to describe the direct repair of the pars defect using an isolated bone graft without instrumentation. Patients who underwent this procedure had to remain recumbent for a number of weeks, followed by external immobilisation in a cast for up to six months. Buck 9 first described the technique of direct repair by filling the gap in the defect with iliac cancellous autograft and placing screws directly through the defect itself. A number of techniques have since been described for direct repair of the defect, but have been associated with complications such as loosening and breakage of the internal fixation, technical difficulty, extensive muscle and tissue dissection, and variable rates of consolidation of the defect. We describe a prospective case series evaluating a technique of direct repair of the pars stabilised with a construct consisting of a pair of pedicle screws connected by a U-shaped modular link passing beneath the spinous process. Tightening the link to the screws compresses the bone graft in the defect, providing rigid intrasegmental fixation. This technique was first described by the senior author (HHN). Patients and Methods Patients were selected who had chronic disabling pain located in the lower back without sciatica, which had been resistant to conservative treatment for at least 12 months, including modification of activity and a trial of bracing and physiotherapy. All had defects in the pars at L5 on CT scans. Other inclusion criteria were the absence of adjacent degenerative disc disease confirmed by normal T2-weighted MRI, and no more than a grade I spondylolisthesis. 10 Of the 20 patients in this series, 12 were male and eight were female, and nine had grade I spondylolisthesis. There was one VOL. 93-B, No. 1, JANUARY
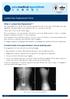
2 74 F. ALTAF, N. A. OSEI, E. GARRIDO, M. AL-MUKHTAR, C. NATALI, A. SIVARAMAN, H. H. NOORDEEN Fig. 1 Photograph showing the construct in a model spine. The shaded lines illustrate the location of the pars defects. Fig. 3 Anteroposterior radiograph showing the construct at L5. Fig. 2 Photograph showing the construct in situ from above. The rod is firmly fixed against the spinous process and the laminae, which promotes compression of the graft in the defect and stabilises the posterior arch. smoker, who was male. The mean age of the patients was 13.9 years (9 to 21). None had a motor or sensory deficit. Bony union of the pars was assessed by plain lateral radiographs and CT scans in all patients. The clinical outcome was evaluated using the Oswestry Disability Index (ODI),11 and a visual analogue scale (VAS) 12 with 0 representing no pain and 10 maximum pain), both preoperatively and at follow-up. Complications were also recorded. Statistical analysis used the paired t-test and the Wilcoxon s signed-ranks test. Significance was set at p < Surgical technique. The patient is positioned prone. A midline incision is made and the paraspinal musculature elevated laterally to expose the lamina, the pars and the base of the transverse process. Care is taken not to injure the capsule of the facet joint. The defect in the pars is exposed and the fibrocartilaginous element curetted. A burr is used to decorticate the defect and the corresponding lamina and transverse process. Anatomical landmarks and fluoroscopy are then used to determine the starting point for the pedicle screw. A starting hole is burred and a pedicle finder used to enter the pedicle. The walls and floor are assessed with a ball-tipped probe, and the hole is tapped and prepared for a 5 mm pedicle screw. Bone graft is harvested from the iliac crest, placed in the defect and impacted before insertion of the screw. After placement of the screw, a rod is contoured in a U-shape, placed just caudal to the spinous process, deep to the interspinous ligament of the affected level, and attached to each pedicle screw (Figs 1 and 2). When tightened to the screws, the rod compresses the defects. It is firmly fixed against the spinous process and the laminae, which promotes compression of the graft in the defect and stabilises the posterior arch. Finally, fluoroscopic imaging (Fig. 3) confirms correct placement of the screw and link. Post-operative instructions include the administration of intravenous antibiotics until the wound is dry. The patient is mobilised without a brace. Results The mean follow-up was four years (2.3 to 7.3). None of the patients was lost to follow-up. The mean in-patient stay was three days (2 to 5). Post-operative complications THE JOURNAL OF BONE AND JOINT SURGERY
3 REPAIR OF SPONDYLOLYSIS USING COMPRESSION WITH A MODULAR LINK AND SCREWS 75 Fig. 4a Fig. 4b Lateral radiographs showing a) the pars defect at L5 pre-operatively and b) union of the pars defect at six months post-operatively. Fig. 5a Fig. 5b Lateral CT scans showing a) the pars defect at L5 pre-operatively and b) union of the pars defect at six months post-operatively. included one superficial wound haematoma which did not require evacuation, and two superficial wound infections which responded to antibiotic treatment. Bony union of the defect (Figs 4 and 5) occurred in 16 of the 20 patients. Three of the four patients with nonunion had a grade I spondylolisthesis. At the latest follow-up, 18 of the 20 patients had a significant (p < 0.001) improvement in their ODI (Table I) and in their VAS scores compared with the pre-operative levels. The mean ODI improved from 54% (42 to 78) pre-operatively, denoting severe disability, to 8% (0 to 42), indicating minimal disability. The mean VAS improved from 8.1 (6.5 to 10) preoperatively to 1.6 (0 to 8.2) after operation. The mean ODI and VAS of the 16 patients with union of the defect was 3% and 0.4 respectively, at final follow-up. The two patients who did not have a significant improvement in outcome had no evidence of union of the pars defect on the CT scan. The other two patients with nonunion were asymptomatic. Of the two patients who developed a symptomatic nonunion, one was classified as having severe disability at follow-up. He was a smoker, and was offered a further grafting procedure. The second patient was classified as having moderate disability, was a non-smoker, and had grade I spondylolisthesis. This patient had some subjective improvement and wanted no further intervention. No breakage or loosening of the internal fixation was encountered, and none was removed. Discussion The aetiology of spondylolysis remains unknown, but current opinion is that there is an element of weakness which is genetically determined, or a degree of dysplasia at the pars interarticularis which renders it susceptible to the stresses of normal activity, resulting in a stress fracture. VOL. 93-B, No. 1, JANUARY 2011
4 76 F. ALTAF, N. A. OSEI, E. GARRIDO, M. AL-MUKHTAR, C. NATALI, A. SIVARAMAN, H. H. NOORDEEN Table I. Post-operative clinical assessment using the Oswestry Disability Index11 Score (%) Excellent (minimal disability) 0 to Good (moderate disability) 21 to 40 1 Fair (severe disability) 41 to 60 1 Poor (complete disability) 61 to 80 0 Very poor (bedbound) 81 to Number of patients A minority of those affected need treatment and only a few require surgery. Most patients considered for surgical treatment have had the time for adjacent disc disease to develop, or have a spondylolisthesis. Lumbosacral fusion is the most common operation performed in these cases. For a grade I or less spondylolisthesis, a direct repair of the pars defect may be considered. This has the advantage of preserving adjacent movement segments and dealing directly with the anatomical defect responsible for any listhesis. Buck 9 initially carried out his technique of direct repair in 16 patients. None developed nonunion, which was assessed radiologically, but three patients had a poor outcome. He suggested that this technique should only be used in cases where the gap in the neural arch was < 3 mm to 4 mm. In he described a larger series of 75 patients, 88% of whom had a satisfactory result. The accurate placement of the screw in this technique was found to be difficult, with a lengthy learning curve, and complications of this procedure most commonly arose secondary to screw loosening or misplacement. 14 The Scott technique 15 involved stabilisation of the loose posterior arch by cerclage wiring of the transverse process to the spinous process of the involved vertebra with fusion of the defect. This technique requires greater surgical exposure, with extensive stripping of the muscle in order to expose the transverse process completely. Placement of the wires under the transverse processes is difficult and can lead to substantial bleeding. There is also a risk of injuries to the nerve root. Several cases of wire breakage have been reported. 16 Salib and Pettine 17 described a modification of this technique that consisted of a tension band wire around the posterior spinous process, with a screw in the pedicle. The proposed advantages were that there was no need to pass the wire around the transverse process, with its associated risk of injury to the nerve root, and the better anchorage of the wire using the pedicle screw. The strength and linkage of wires and the diversion of the compression force away from the graft mass are disadvantages. Songer and Rovin 18 described a small series in which the cerclage wire was replaced by a cable passing underneath the lamina, fixed on a pair of pedicle screws, in a technique that requires specific instrumentation. In 1984, Morscher, Gerber and Fasel 19 described a new repair technique that used a laminar hook positioned in the defect and a compressive force placed upon it with a spring held against a screw within the articular process. The proposed advantages of this technique were that the fixation did not depend on the shape of the defect; it allowed for maximal grafting of the defect; and it would exert a compressive force across the lamina. Numerous problems have been encountered with this technique, including difficulty in screw placement, screw loosening 20 and breakage, 21 and a high rate of failure. Tokuhashi and Matsuzaki 22 described a modified technique that stabilised bone grafted to the pars defect with a pedicular screw, a hook and a rod used in combination. They described significant relief of symptoms in six patients over a limited period of follow-up. Kakiuchi 23 used a variable-angle pedicle screw, a rod and a laminar hook with bone graft placed across the defect. The proposed advantage was fixation which was more rigid. He reported resolution of symptoms in 13 of 16 patients and bony union in all at a mean follow-up of 25 months. Gillet and Petit 24 described direct repair by placing screws on the pedicles of the involved vertebra and fixing the loose posterior arch with a solid rod bent into a V-shape, taking purchase on the spinous process and laminae. They achieved excellent results in six of ten patients, with no complications. In our series of 20 patients we achieved an excellent clinical outcome in 18, with a mean follow-up of four years. Union of the pars defect was achieved in 16 patients (80%). Contradictory opinions have been reported as to the effect of nonunion on outcome. According to Nicol and Scott, 25 Debnath et al, 26 Wu, Lee and Chen 27 and Dai et al, 28 patients with a pseudarthrosis have a poor or fair outcome. However, Hefti, Seelig and Morscher, 29 Johnson and Thompson 30 and Pellisé et al 31 could not prove this relationship. In our series, of the four patients with a nonunion,32 two had a poor and two an excellent outcome. The treatment of defects of the pars that appear cold on a bone scan is associated with a higher rate of nonunion. 32 Although the patients in our study did not have a preoperative bone scan, this may be a useful investigation to identify the rate of nonunion in those patients who have a cold lesion. Biomechanical studies may also be useful to further evaluate the distribution of compressive forces across the pars defect in our construct. Most studies 9,16,18,19,23 on spondylolysis have used plain radiographs for the assessment of union, with its associated limited sensitivity. 33 In our study we used CT imaging, which is more sensitive and specific when used to assess union. 33 This may give an impression of a higher rate of pseudarthrosis in our study as compared with other studies which have used radiographs to assess union. Some authors 30,34,35 consider that a slight degree of spondylolisthesis does not affect the outcome of patients undergoing direct repair of the pars. Others 36,37 carry out direct repair of the pars in patients with a spondylolisthesis of up to 25%. Jeanneret 38 found no difference in outcome THE JOURNAL OF BONE AND JOINT SURGERY
5 REPAIR OF SPONDYLOLYSIS USING COMPRESSION WITH A MODULAR LINK AND SCREWS 77 between patients with a spondylolisthesis of between 0% and 25%. In our series, nine of the 20 patients had grade I spondylolisthesis, three of whom developed a nonunion of the defect. Our patients were aged between nine and 21 years, with no evidence of adjacent level disc disease on MRI, and spondylolisthesis not greater than grade I. Numerous authors have found that patients in the age range 20 to 30 years have worse results than younger patients The primary reason for this failure is thought to be associated with the appearance of degenerative disc disease. Our technique uses readily available instrumentation to provide a strong construct. The bone graft in the pars defect is not hindered by screws, allowing for high rates of union. Postoperative recovery is made easier as the strength of the construct removes the need for post-operative immobilisation. Listen live Listen to the abstract of this article at No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article. References 1. Schneiderman GA, McLain RF, Hambly MF, Nielsen SL. The pars defect as a pain source: a histologic study. Spine 1995;20: Eisenstein SM, Ashton IK, Roberts S, et al. Innervation of the spondylolysis ligament. Spine 1994;19: Albee FH. Spondylolisthesis. J Bone Joint Surg 1927;9: Hibbs RA. An operation for progressive spinal deformities: a preliminary report of three cases from the service of the orthopaedic hospital, Clin Orthop 2007;460: Bosworth DM, Fielding JW, Demarest L, Bonaquist M. Spondylolisthesis: a critical review of the consecutive series of cases treated by arthrodesis. J Bone Joint Surg [Am] 1955;37-A: Cleveland M, Bosworth DM, Thompson FR. Pseudoarthrosis in the lumbosacral spine. J Bone Joint Surg [Am] 1948;30-A: Watkins MB. Posterolateral fusion of the lumbar and lumbosacral spine. J Bone Joint Surg [Am] 1953;35-A: Kimura M. My method of filing the lesion with spongy bone in spondylolysis and spondylolisthesis. Seikei Geka 1968;19: (in Japanese). 9. Buck JE. Direct repair of the defect in spondylolisthesis: preliminary report. J Bone Joint Surg [Br] 1970;52-B: Meyerding HW. Spondylolisthesis: surgical treatment and results. J Bone Joint Surg 1943;25: Fairbank JC, Couper J, Davies JB, O Brien JP. The Oswestry low back pain disability questionnaire. Physiotherapy 1980;66; Huskisson EC. Measurement of pain. Lancet 1974;2: Buck JE. Further thoughts on direct repair of the defect in spondylolysis [abstract]. J Bone Joint Surg [Br] 1979;61-B: Beckers L. Buck s operation for treatment of spondylolysis and spondylolisthesis. Acta Orthop Belg 1986;52: Scott JHS. The Edinburgh repair of isthmic (Group II) spondylolysis [abstract]. J Bone Joint Surg [Br] 1987;69-B: Bradford DS, Iza J. Repair of the defect in spondylolysis or minimal degrees of spondylolisthesis by segmental wire fixation and bone grafting. Spine 1985;10: Salib RM, Pettine KA. Modified repair of a defect in spondylolysis or minimal spondylolisthesis by pedicle screw, segmental wire fixation, and bone grafting. Spine 1993;18: Songer MN, Rovin R. Repair of the pars interarticularis defect with a cable-screw construct: a preliminary report. Spine 1998;23: Morscher E, Gerber B, Fasel J. Surgical treatment of spondylolisthesis by bone grafting and direct stabilization of spondylolysis by means of a hook screw. Arch Orthop Trauma Surg 1984;103: Dreyzin V, Esses SI. A comparative analysis of spondylolysis repair. Spine 1994;19: Sales de Gauzy J, Vadier F, Cahuzac JP. Repair of lumbar spondylolysis using Morscher material: 14 children followed for 1-5 years. Acta Orthop Scand 2000;71: Tokuhashi Y, Matsuzaki H. Repair of defects in spondylolysis by segmental pedicular screw hook fixation: a preliminary report. Spine 1996;21: Kakiuchi M. Repair of the defect in spondylolysis: durable fixation with pedicle screws and laminar hooks. J Bone Joint Surg [Am] 1997;79-A: Gillet P, Petit M. Direct repair of spondylolysis without spondylolisthesis, using a rod-screw construct and bone grafting of the pars defect. Spine 1999;24: Nicol RO, Scott JH. Lytic spondylolysis: repair by wiring. Spine 1986;11: Debnath UK, Freeman BJ, Gregory P, et al. Clinical outcome and return to sport after surgical treatment of spondylolysis in young athletes. J Bone Joint Surg [Br] 2003;85-B: Wu SS, Lee CH, Chen PQ. Operative repair of symptomatic spondylolysis following a positive response to diagnostic pars injection. J Spinal Disord 1999;12: Dai LY, Jia LS, Yuan W, Ni B, Zhu HB. Direct repair of defect in lumbar spondylolysis and mild isthmic spondylolisthesis by bone grafting, with or without facet joint fusion. Eur Spine J 2001;10: Hefti F, Seelig W, Morscher E. Repair of lumbar spondylolysis with a hookscrew. Int Orthop 1992;16: Johnson GV, Thompson AG. The Scott wiring technique for direct repair of lumbar spondylolysis. J Bone Joint Surg [Br] 1992;74-B: Pellisé F, Toribio J, Rivas A, et al. Clinical and CT scan evaluation after direct defect repair in spondylolysis using segmental pedicular screw fixation. J Spinal Disord 1999;12: van der Oever M, Merrick MV, Scott JH. Bone scintigraphy in symptomatic spondylolysis. J Bone Joint Surg [Br] 1987;69-B: Congeni J, McCulloch J, Swanson K. Lumbar spondylolysis: a study of natural progression in athletes. Am J Sports Med 1997;25: Buring K, Fredensborg N. Osteosynthesis of spondylolysis. Acta Orthop Scand 1973;44: van der Werf GJ, Tonino AJ, Zeegers WS. Direct repair of lumbar spondylolysis. Acta Orthop Scand 1985;56: Pedersen AK, Hagen R. Spondylolysis and spondylolisthesis: treatment by internal fixation and bone-grafting of the defect. J Bone Joint Surg [Am] 1988;70-A: Albassir A, Samson I, Hendrickx L. Treatment of painful spondylolysis using Morscher s hook. Acta Orthop Belg 1990;56: (in French). 38. Jeanneret B. Direct repair of spondylolysis. Acta Orthop Scand Suppl 1993;251: Suh PB, Esses SI, Kostuik JP. Repair of pars interarticularis defect: the prognostic value of pars infiltration. Spine 1991;16(Suppl): Pavlovcic V. Surgical treatment of spondylolysis and spondylolisthesis with a hook screw. Int Orthop 1994;18:6-9. VOL. 93-B, No. 1, JANUARY 2011
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
Repair of spondylolytic defect with a cable screw reconstruction
 International Orthopaedics (SICOT) (2008) 32:121 125 DOI 10.1007/s00264-006-0277-6 ORIGINAL PAPER Repair of spondylolytic defect with a cable screw reconstruction Vasudeva S. Pai & Bruce Hodgson & Vishal
International Orthopaedics (SICOT) (2008) 32:121 125 DOI 10.1007/s00264-006-0277-6 ORIGINAL PAPER Repair of spondylolytic defect with a cable screw reconstruction Vasudeva S. Pai & Bruce Hodgson & Vishal
Spondylolysis. Lysis (Greek λύσις, lýsis from lýein "to separate") refers to the breaking down.
 Spondylolysis Lysis (Greek λύσις, lýsis from lýein "to separate") refers to the breaking down. Thomas J Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Spondylolysis Defect in the
Spondylolysis Lysis (Greek λύσις, lýsis from lýein "to separate") refers to the breaking down. Thomas J Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Spondylolysis Defect in the
Spondylolysis, a defect in the pars interarticularis of. Multi-level Spondylolysis. A Case Report and Review of the Literature
 ulletin of the NYU Hospital for Joint Diseases 2011;69(4):339-43 339 Multi-level Spondylolysis Case Report and Review of the Literature David S. Hersh, M.D., Yong H. Kim, M.D., and fshin Razi, M.D. bstract
ulletin of the NYU Hospital for Joint Diseases 2011;69(4):339-43 339 Multi-level Spondylolysis Case Report and Review of the Literature David S. Hersh, M.D., Yong H. Kim, M.D., and fshin Razi, M.D. bstract
Travis Clegg, MD, Leah Carreon, MD, Ian Mutchnick, MD, and Rolando Puno, MD AJO
 An Original Study Clinical Outcomes Following Repair of the Pars Interarticularis Travis Clegg, MD, Leah Carreon, MD, Ian Mutchnick, MD, and Rolando Puno, MD Abstract Spondylolysis is a source of back
An Original Study Clinical Outcomes Following Repair of the Pars Interarticularis Travis Clegg, MD, Leah Carreon, MD, Ian Mutchnick, MD, and Rolando Puno, MD Abstract Spondylolysis is a source of back
Spondylolysis is a unilateral or bilateral defect in the. Spondylolysis outcomes in adolescents after direct screw repair of the pars interarticularis
 J Neurosurg Spine 21:329 333, 2014 AANS, 2014 Spondylolysis outcomes in adolescents after direct screw repair of the pars interarticularis Clinical article Laura A. Snyder, M.D., 1 Harry Shufflebarger,
J Neurosurg Spine 21:329 333, 2014 AANS, 2014 Spondylolysis outcomes in adolescents after direct screw repair of the pars interarticularis Clinical article Laura A. Snyder, M.D., 1 Harry Shufflebarger,
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
PARADIGM SPINE. Brochure. coflex-f Minimally Invasive Lumbar Fusion
 PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
Management of fractures of the pedicle after instrumentation with transpedicular screws
 Management of fractures of the pedicle after instrumentation with transpedicular screws A REPORT OF THREE PATIENTS F. Lattig, T. F. Fekete, D. Jeszenszky From the Schulthess Clinic, Zürich, Switzerland
Management of fractures of the pedicle after instrumentation with transpedicular screws A REPORT OF THREE PATIENTS F. Lattig, T. F. Fekete, D. Jeszenszky From the Schulthess Clinic, Zürich, Switzerland
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Spondylolytic spondylolisthesis:
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Spring 2011 Vol 10 No 3 / Page 85 C L I N I C A L A RT I C L E Spondylolytic spondylolisthesis: Surgical management of adult presentation AJ Vlok MBChB, MMed(Neurosurg),
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Spring 2011 Vol 10 No 3 / Page 85 C L I N I C A L A RT I C L E Spondylolytic spondylolisthesis: Surgical management of adult presentation AJ Vlok MBChB, MMed(Neurosurg),
Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis
 Journal of Orthopaedic Surgery 2006;14(1):21-6 Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis DN Inamdar, M Alagappan, L Shyam, S Devadoss,
Journal of Orthopaedic Surgery 2006;14(1):21-6 Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis DN Inamdar, M Alagappan, L Shyam, S Devadoss,
A biomechanical comparison of three spondylolysis repair techniques in a calf spine model
 Orthopaedics & Traumatology: Surgery & Research (2013) 99, 66 71 Available online at www.sciencedirect.com ORIGINAL ARTICLE A biomechanical comparison of three spondylolysis repair techniques in a calf
Orthopaedics & Traumatology: Surgery & Research (2013) 99, 66 71 Available online at www.sciencedirect.com ORIGINAL ARTICLE A biomechanical comparison of three spondylolysis repair techniques in a calf
Dingjun Hao, Baorong He, Liang Yan. Hong Hui Hospital, Xi an Jiaotong University College. of Medicine, Xi an, Shaanxi , China
 Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis
 Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis Issue 6: March 2016 Review date: February 2019 Following your recent investigations and consultation with your spinal surgeon, it
Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis Issue 6: March 2016 Review date: February 2019 Following your recent investigations and consultation with your spinal surgeon, it
In Situ Fusion L5 to S1
 Chapter 2 In Situ Fusion L5 to S1 Stuart L. Weinstein, M.D. DIAGNOSIS Spondylolisthesis COMMON INDICATIONS n In symptomatic low grade Spondylolysis and listhesis of less than 30 % n Pain unresponsive to
Chapter 2 In Situ Fusion L5 to S1 Stuart L. Weinstein, M.D. DIAGNOSIS Spondylolisthesis COMMON INDICATIONS n In symptomatic low grade Spondylolysis and listhesis of less than 30 % n Pain unresponsive to
Dymaxeon Spine System. Simple, Streamlined, Smart. Surgical Procedure
 Simple, Streamlined, Smart Surgical Procedure Introduction The Dymaxeon pedicle screw system offers the spinal surgeon an outstanding system for stabilization of spinal deformity, reduction of spondylolisthesis,
Simple, Streamlined, Smart Surgical Procedure Introduction The Dymaxeon pedicle screw system offers the spinal surgeon an outstanding system for stabilization of spinal deformity, reduction of spondylolisthesis,
The reduction and direct repair of isthmic spondylolisthesis using the smiley face rod method in adolescent athlete : Technical note
 168 CASE REPORT The reduction and direct repair of isthmic spondylolisthesis using the smiley face rod method in adolescent athlete : Technical note Kazuta Yamashita, MD, Kosaku Higashino, MD, PhD, Toshinori
168 CASE REPORT The reduction and direct repair of isthmic spondylolisthesis using the smiley face rod method in adolescent athlete : Technical note Kazuta Yamashita, MD, Kosaku Higashino, MD, PhD, Toshinori
Coflex TM for Lumbar Stenosis with
 Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
Coflex TM for Lumbar Stenosis with Segmental Instability : 1 yr outcomes Eun-Sang Kim, M.D., Ph.D. Clinical Professor Dept of Neurosurgery Samsung Medical Center Seoul, Korea Surgery for Spinal Stenosis
L8 Spine System SURGICAL TECHNIQUE. Add: No.1-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China
 Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
T.L.I.F. Transforaminal Lumbar Interbody Fusion
 T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS. Surgical Technique
 UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS Surgical Technique Joint Spine Sports Med MySpine Surgical Technique Joint Spine Sports Med 2 INTRODUCTION MySpine is a patient matched, pedicle targeted technology
UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS Surgical Technique Joint Spine Sports Med MySpine Surgical Technique Joint Spine Sports Med 2 INTRODUCTION MySpine is a patient matched, pedicle targeted technology
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Zimmer Facet Screw System Surgical Technique
 Zimmer Facet Screw System Surgical Technique 2 Zimmer Facet Screw System Surgical Technique Zimmer Facet Screw System Surgical Technique Description, Indications & Contraindications...3 Surgical Technique...4
Zimmer Facet Screw System Surgical Technique 2 Zimmer Facet Screw System Surgical Technique Zimmer Facet Screw System Surgical Technique Description, Indications & Contraindications...3 Surgical Technique...4
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity: Technical Note Involving 13 Cases
 Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
Lumbar Disc Replacement FAQs
 ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Treatment of thoracolumbar burst fractures by vertebral shortening
 Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis
 Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
A Patient s Guide to Lumbar Spondylolysis. William T. Grant, MD
 A Patient s Guide to Lumbar Spondylolysis Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
A Patient s Guide to Lumbar Spondylolysis Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
Minimally invasive direct repair of lumbar spondylolysis with a pedicle screw and hook construct
 Neurosurg Focus 25 (2):E15, 2008 Minimally invasive direct repair of lumbar spondylolysis with a pedicle screw and hook construct JOSEPH C. NOGGLE, B.S., 1 DANIEL M. SCIUBBA, M.D., 1 AMER F. SAMDANI, M.D.,
Neurosurg Focus 25 (2):E15, 2008 Minimally invasive direct repair of lumbar spondylolysis with a pedicle screw and hook construct JOSEPH C. NOGGLE, B.S., 1 DANIEL M. SCIUBBA, M.D., 1 AMER F. SAMDANI, M.D.,
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
 Visit our website on www.biotech-medical.com The DLP - Dorso-Lumbar Polyaxial Screw System has been designed to address the pathologies of the thoracolumbar spine. The DLP System contains a wide range
Visit our website on www.biotech-medical.com The DLP - Dorso-Lumbar Polyaxial Screw System has been designed to address the pathologies of the thoracolumbar spine. The DLP System contains a wide range
Technique Guide. C1/C2 Access System. Percutaneous transarticular screw fixation.
 Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
FUNCTIONAL OUTCOME OF SPONDYLOLISTHESIS TREATED BY TRANSFORAMINAL LUMBAR INTERBODY FUSION WITH CAGE AND PEDICULAR SCREW FIXATION A PROSPECTIVE STUDY
 FUNCTIONAL OUTCOME OF SPONDYLOLISTHESIS TREATED BY TRANSFORAMINAL LUMBAR INTERBODY FUSION WITH CAGE AND PEDICULAR SCREW FIXATION A PROSPECTIVE STUDY Original Article Orthopaedics Latchoumibady. K 1, Pragash.
FUNCTIONAL OUTCOME OF SPONDYLOLISTHESIS TREATED BY TRANSFORAMINAL LUMBAR INTERBODY FUSION WITH CAGE AND PEDICULAR SCREW FIXATION A PROSPECTIVE STUDY Original Article Orthopaedics Latchoumibady. K 1, Pragash.
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
VTI INTERLINK PEDICLE SCREW SYSTEM
 VTI INTERLINK PEDICLE SCREW SYSTEM SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. DEVICE DESCRIPTION The VTI InterLink Pedicle Screw System is comprised of polyaxial pedicle screws in various diameters
VTI INTERLINK PEDICLE SCREW SYSTEM SURGICAL TECHNIQUE FORWARD THINKING FOR THE BACK. DEVICE DESCRIPTION The VTI InterLink Pedicle Screw System is comprised of polyaxial pedicle screws in various diameters
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Axial Lumbosacral Interbody Fusion. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Patient Selection and Lumbar Operative Interventions
 Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
ifuse implant system for treating chronic sacroiliac joint pain
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE ifuse implant system for treating chronic sacroiliac joint pain 1 Technology 1.1 Description of the technology The ifuse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE ifuse implant system for treating chronic sacroiliac joint pain 1 Technology 1.1 Description of the technology The ifuse
KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients
 Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Table of contents. Introduction. Features and Benefits 2. AO Principles 4. Indications and Contraindiactions 5. Implants 6. Productinformation
 Technique Guide CerviFix. Modular tension band system for posterior fixation of the occipito - cervical spine, upper and lower cervical spine, and upper thoracic spine. Table of contents Introduction
Technique Guide CerviFix. Modular tension band system for posterior fixation of the occipito - cervical spine, upper and lower cervical spine, and upper thoracic spine. Table of contents Introduction
The imaging features of spondylolisthesis : what the clinician needs to know
 The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
Spina bifida occulta in high grade spondylolisthesis
 European Review for Medical and Pharmacological Sciences 2014; 18(Suppl 1): 8-14 Spina bifida occulta in high grade spondylolisthesis L. BABBI, S. TERZI, S. BANDIERA, G. BARBANTI BRODANO Department of
European Review for Medical and Pharmacological Sciences 2014; 18(Suppl 1): 8-14 Spina bifida occulta in high grade spondylolisthesis L. BABBI, S. TERZI, S. BANDIERA, G. BARBANTI BRODANO Department of
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
X-spine Surgical Technique
 X-spine Surgical Technique The X90 Pedicle Screw System Revolutionary Design and Function This document is intended exclusively for experts in the field, particularly physicians, and is not intended for
X-spine Surgical Technique The X90 Pedicle Screw System Revolutionary Design and Function This document is intended exclusively for experts in the field, particularly physicians, and is not intended for
Corporate Medical Policy
 Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
CERVIFIX Modular tension band system for posterior fixation of the occipito cervical spine, upper and lower cervical spine, and upper thoracic spine
 CERVIFIX Modular tension band system for posterior fixation of the occipito cervical spine, upper and lower cervical spine, and upper thoracic spine PRODUCT OBSOLETED 30th June 2017 DSEM/SPN/1215/0387(1)
CERVIFIX Modular tension band system for posterior fixation of the occipito cervical spine, upper and lower cervical spine, and upper thoracic spine PRODUCT OBSOLETED 30th June 2017 DSEM/SPN/1215/0387(1)
ILIF Interlaminar Lumbar Instrumented Fusion. Anton Thompkins, M.D.
 ILIF Interlaminar Lumbar Instrumented Fusion Anton Thompkins, M.D. Anton Thompkins, M.D. EDUCATION: BS, Biology, DePauw University, Greencastle, IN MD, University of Cincinnati College of Medicine RESIDENCY:
ILIF Interlaminar Lumbar Instrumented Fusion Anton Thompkins, M.D. Anton Thompkins, M.D. EDUCATION: BS, Biology, DePauw University, Greencastle, IN MD, University of Cincinnati College of Medicine RESIDENCY:
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
4.5 System. Surgical Technique. This publication is not intended for distribution in the USA.
 4.5 System Surgical Technique This publication is not intended for distribution in the USA. Contents EXPEDIUM 4.5 Spine System 2 Features and Benefits 3 Surgical Technique Extended Tandem Connector 4 Placement
4.5 System Surgical Technique This publication is not intended for distribution in the USA. Contents EXPEDIUM 4.5 Spine System 2 Features and Benefits 3 Surgical Technique Extended Tandem Connector 4 Placement
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Surgical Technique. Apache Anterior Lumbar Interbody Fusion
 Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
The Most Reliable Spinal Solution
 MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
Dorsal Fixation of the Thoracic and Lumbar Spine Techniques
 Pedicle, Facet, Cortical, and Translaminar Screw Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Dorsal Fixation of the Thoracic and Lumbar
Pedicle, Facet, Cortical, and Translaminar Screw Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Dorsal Fixation of the Thoracic and Lumbar
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Lumbar Facet Joint Replacement
 Rome Spine 2011 THE SPINE TODAY International Congress Rome 6-7th December 2011 Lumbar Facet Joint Replacement Prof. Dr. Karin Büttner-Janz Past President International Society for the Advancement of Spine
Rome Spine 2011 THE SPINE TODAY International Congress Rome 6-7th December 2011 Lumbar Facet Joint Replacement Prof. Dr. Karin Büttner-Janz Past President International Society for the Advancement of Spine
TM TM Surgical Technique
 TM TM Surgical Technique TABLE OF CONTENTS Reli SP Spinous Plating System Overview Device Description Implant Features Indications Instruments Access Instruments Preparation Instruments Insertion Instruments
TM TM Surgical Technique TABLE OF CONTENTS Reli SP Spinous Plating System Overview Device Description Implant Features Indications Instruments Access Instruments Preparation Instruments Insertion Instruments
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Surgical Technique Manual
 InterFuse S Interbody Fusion System Surgical Technique Manual VERTEBRAL TECHNOLOGIES MS 4043-02 Rev. O Product Overview Introduction The VTI InterFuse S implant is an interbody fusion device that combines
InterFuse S Interbody Fusion System Surgical Technique Manual VERTEBRAL TECHNOLOGIES MS 4043-02 Rev. O Product Overview Introduction The VTI InterFuse S implant is an interbody fusion device that combines
TRANSLAMINAR FACET SCREW FIXATION
 1. Introduction: Although the new era in spine surgery is highly focused on preserving mobility, fusion is still an accepted way of treatment for a variety of spinal disorders. To stabilize the spine until
1. Introduction: Although the new era in spine surgery is highly focused on preserving mobility, fusion is still an accepted way of treatment for a variety of spinal disorders. To stabilize the spine until
OPERATIVE TECHNIQUE. anterior cervical plating system
 OPERATIVE TECHNIQUE 3º anterior cervical plating system Introduction 1 Pre-Operative Technique 2 Oerative Technique 3 Instructions for Use 12 Part Numbers 16 The surgical technique shown is for illustrative
OPERATIVE TECHNIQUE 3º anterior cervical plating system Introduction 1 Pre-Operative Technique 2 Oerative Technique 3 Instructions for Use 12 Part Numbers 16 The surgical technique shown is for illustrative
Ref: Q400-09T1 EBI Spine. September 05/VS02. c/o BIOMET Spain Orthopaedics, S.L.
 Ref: Q400-09T1 EBI Spine. September 05/VS02 c/o BIOMET Spain Orthopaedics, S.L. www.ebimedical.com EBI Omega 21 TM LP Since its introduction in 1996, and with thousands of patients treated so far, the
Ref: Q400-09T1 EBI Spine. September 05/VS02 c/o BIOMET Spain Orthopaedics, S.L. www.ebimedical.com EBI Omega 21 TM LP Since its introduction in 1996, and with thousands of patients treated so far, the
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
ACP. Anterior Cervical Plate System SURGICAL TECHNIQUE
 ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
Spondylolysis To Brace or Not To Brace AMSSM 2014
 Spondylolysis To Brace or Not To Brace AMSSM 2014 Nothing to Disclose Disclosures To Brace? Goals of Treatment History/ Literature of Bracing Mechanics of Bracing Benefits to Brace. Earlier to return to
Spondylolysis To Brace or Not To Brace AMSSM 2014 Nothing to Disclose Disclosures To Brace? Goals of Treatment History/ Literature of Bracing Mechanics of Bracing Benefits to Brace. Earlier to return to
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion
 Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Translaminar facetal screw (Magerl s) fixation
 Review Article Translaminar facetal screw (Magerl s) fixation S. Rajasekaran, J. Naresh-Babu Department of Orthopaedics and Spine Surgery, Ganga Hospital, Coimbatore, India Translaminar facet screw fixation
Review Article Translaminar facetal screw (Magerl s) fixation S. Rajasekaran, J. Naresh-Babu Department of Orthopaedics and Spine Surgery, Ganga Hospital, Coimbatore, India Translaminar facet screw fixation
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis
 Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
Segmental stability following minimally invasive decompressive surgery with tubular retractor for lumbar spinal stenosis Department of Spinal surgery, Research Institute for Brain and Blood Vessels-Akita
NOT DESIGNATED FOR PUBLICATION BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. G DIANE THOMPSON, EMPLOYEE
 NOT DESIGNATED FOR PUBLICATION BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. G000709 DIANE THOMPSON, EMPLOYEE PERENNIAL BUSINESS, EMPLOYER GALLAGHER BASSETT SERVICES, INC., CARRIER/TPA
NOT DESIGNATED FOR PUBLICATION BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. G000709 DIANE THOMPSON, EMPLOYEE PERENNIAL BUSINESS, EMPLOYER GALLAGHER BASSETT SERVICES, INC., CARRIER/TPA
Transforaminal Lumbar Interbody Fusion
 Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Spinal fusion for paediatric lumbosacral spondylolisthesis
 South African Orthopaedic Journal http://journal.saoa.org.za Horn A et al. SA Orthop J 2018;17(4) DOI 10.17159/2309-8309/2018/v17n4a5 SPINE TRAUMA Spinal fusion for paediatric lumbosacral spondylolisthesis
South African Orthopaedic Journal http://journal.saoa.org.za Horn A et al. SA Orthop J 2018;17(4) DOI 10.17159/2309-8309/2018/v17n4a5 SPINE TRAUMA Spinal fusion for paediatric lumbosacral spondylolisthesis
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
