Int J Clin Exp Med 2016;9(11): /ISSN: /IJCEM
|
|
|
- Lesley Harris
- 6 years ago
- Views:
Transcription
1 Int J Clin Exp Med 2016;9(11): /ISSN: /IJCEM Original Article Comparison of anterior cervical discectomy and fusion with the zero-profile implant and cage-plate implant in treating two-level degenerative cervical spondylosis Yi Yang 1, Litai Ma 1, Junfeng Zeng 1, Hao Liu 1, Ying Hong 2, Beiyu Wang 1, Chen Ding 1, Yuxiao Deng 1, Yueming Song 1 1 Department of Orthopedics, 2 Operation Room, West China Hospital, Sichuan University, Chengdu, P. R. China Received September 23, 2016; Accepted October 28, 2016; Epub November 15, 2016; Published November 30, 2016 Abstract: Previous studies based on small sample sizes have reported the application of the Zero-P implant (Zero-P, Synthes GmbH, Switzerland) in single anterior cervical discectomy and fusion (ACDF) surgery with excellent outcomes. However, the safety and effectiveness of two-level ACDF with Zero-P implant still remains controversial. A retrospective study was conducted to compare the clinical outcomes and complications between Zero-P implant and conventional cage-plate implant in two-level ACDF for the treatment of degenerative cervical spondylosis. The Japanese Orthopedic Association (JOA) scale score, neck and arm visual analog scale (VAS), bony fusion rates and main complications were recorded. Dysphagia was evaluated according to the Bazaz grading system. A total of 67 consecutive patients in Zero-P group and 72 consecutive patients in Plate group were enrolled in this retrospective study. The total incidence of dysphagia in Zero-P group and Plate group were 40.00% and 55.56% at one week, respectively. Similar improvements were observed in the JOA and VAS pain scores in both groups at the final follow-up (P>0.05). There were no significant difference between two groups concerning other complications such as postoperative hematoma, recurrent laryngeal nerve palsy, cerebrospinal fluid leakage and pseudarthrosis. The Zero-P implant and the traditional titanium plate with cage are both effective treatments for two-level degenerative cervical spondylosis, but the Zero-P implant has a lower dysphagia incidence. Future prospective, randomized and controlled studies with larger sample size are needed. Keywords: ACDF, Zero-P, degenerative cervical spondylosis, plate, anterior cervical discectomy and fusion Introduction Anterior cervical discectomy and fusion (ACDF) has been regarded as the gold-standard procedure in the treatment of degenerative cervical spondylosis for several decades [1, 2]. At first simple discectomy and fusion with iliac bone graft was performed and then intervertebral cages with or without an additional anterior cervical plate were widely applied in ACDF procedure. Anterior cervical plate can significantly increase interbody fusion rates compared AC- DF without additional anterior cervical plate [3, 4]. In addition, anterior cervical plate can also increase cervical stability and maintain or ameliorate cervical sagittal alignment [5, 6]. However, previous studies have also reported that anterior cervical plate may increase some other complications such as increased dysphagia rates, perforation of esophagus, plate malposition, tracheoesophageal lesions, and accelerated adjacent disc degeneration [7-9]. In order to reduce the complications associated with traditional cervical anterior plate and maintain the advantages of traditional cervical anterior plate, a new zero-profile, stand-alone device (Zero-P, Synthes GmbH, Switzerland) for ACDF has been introduced in recent years [10-13]. Previous studies based on small sample sizes have reported the application of the Zero-P in single ACDF surgery with excellent clinical and radiographic outcomes [11, 14-16]. However, two-level ACDF with Zero-P has been little reported. The biomechanical stability and fusion rates of two-level ACDF with the Zero-P remains unknown. Results from a biomechanical 3-dimensional spine test showed that segmental sta-
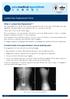
2 Figure 1. Intraoperative anteroposterior, lateral X-rays of two-level anterior cervical discectomy and fusion using the Zero-P implant. Table 1. The Bazaz grading system Severity Liquid Solid 0-None None None 1-Mild None Rare 2-Moderate None or rare Occasionally 3-Severe None or rare Frequent bility decreases with the number of instrumented segments regardless of the used implant, but the locking plate and cage construct was stiffer in all test modes than the Zero-P devices in multilevel constructs [17]. However, whether this difference will have an impact on the clinical outcomes and fusion rates still remain unclear. A retrospective study was conducted in our hospital aimed to compare the clinical outcomes with radiographic data and complications between Zero-P implant and conventional cage-plate implant in two-level ACDF for the treatment of degenerative cervical spondylosis. To the best of our knowledge, this is the largest sample size with the longest available follow-up duration study concerning Zero-P and cage-plate implants in two-level ACDF in the literature. Materials and methods Patient inclusion and exclusion criteria The current retrospective study was approved by Medical Ethical Committee of West China Hospital, Sichuan University. All of the patients provided informed consent for the analysis of erated on two-level ACDF during this period were included if they meet the following inclusion criteria: (1) signs and symptoms of degenerative cervical spondylosis which was unresponsive to conservative treatment more than six months; (2) two level degenerative cervical spondylosis confirmed by imaging such as computed tomography (CT) scan and magnetic resonance imaging (MRI); (3) age >18 years and (4) complete and continuous clinical and imaging data. Exclusion criteria consisted of severe osteoporosis of the cervical spine, presence of active infections, pathologic fractures of the vertebrae, patients with spinal deformity, ankylosing spondylitis or rheumatoid arthritis, continuous or combined ossification of the posterior longitudinal ligament (OPLL), developmental stenosis, patients who underwent ACDF not using an anterior plate or Zero-P device, and patients suffering from acute or chronic serious diseases which might increase the perioperative risk. Surgical technique their clinical data. All of the enrolled patients were treated and followed-up at the West China Hospital, Sichuan University in Chengdu city, China. A total of 67 consecutive patients who underwent two-level ACDF using Zero-P implant (Zero-P group) and 72 consecutive patients who underwent two-level ACDF using conventional cage-plate implant (Plate group) between December 2011 and November 2014 were enrolled in this retrospective study. All patients op- All surgeries were performed via a classic right Smith-Robinson approach after induction of general anesthesia in a supine position [18]. With the help of fluoroscopy and metal markers, a horizontal right side skin incision was determined. The intervertebral disc and herniated nucleus pulpous were extirpated and then the posterior longitudinal ligament and along with osteophytes were resected. The subchondral endplate of each vertebral body was prepared with a high speed drill and curette while Int J Clin Exp Med 2016;9(11):
3 Table 2. Patient demographic and baseline data for two groups Group Zero-P Group (N=60) the bony endplate was preserved as much as possible to prevent implant subsidence. After complete decompression and preparation of the endplate, the disc space was distracted and a trial implant of appropriate size was inserted under image control. Then appropriate Zero-P implant or cage filled with composite synthetic bone graft (β-tricalcium-phosphate) was implanted into intervertebral space. Lateral and anterior-posterior fluoroscopic images were performed and the correct position of the implant was adjusted. In Zero-P group, four locking screws were inserted using torque limitation after preparing the pilot hole oriented through the aiming device (Figure 1). In Plate group, the appropriate anterior plate was paced and adjusted with the help of fluoroscopic images. Similarly locking screws were inserted using torque limitation after preparing the pilot hole and the plate was implanted. Hemostasis is rechecked, and the skin was sutured subcutaneously. All the patients were obeyed to wear a cervical collar postoperatively for 12 weeks. Clinical and radiographic evaluations Plate Group (N=63) Age (y): Mean SD 47.90± ± Gender (Female/Male) 24/36 28/ JOA 9.6± ± VAS for neck 7.27± ± VAS for arm 7.18± ± Intraoperative time (min) ± ± Estimated blood loss (ml) ± ± Length of hospital stay (d) 12.44± ± Data were shown as mean ± SD. Charts and medical records of all patients were reviewed. The following data for each patient including age, gender, intraoperative time, estimated blood loss, length of hospital stay, operated levels, and kinds of instrumentation. Plain radiographs (including flexion/extension views) and MRI were performed before surgery. Neurological examination and functional assessment were recorded at 1, 3, 6, 12 and 24 months and at the latest follow-up assessment. The neurologic status was assessed using the Japanese Orthopedic Association (JOA) scale score. Neck and arm pain was evaluated using P for fusion evaluation [20]. Implant failure, including screw loosening or breakage was recorded. Screw loosening was defined as an initial halo sign, followed by a double halo sign on later plain radiographs or CT scans [21]. Statistical analysis The data were analyzed using the Chi-square test, Student t-test and Mann-Whitney U test, when appropriate. The statistical program SPSS version 19.0 (SPSS Inc. for windows) was used for all statistical analysis. P-values of less than 0.05 were accepted as significant. Results the 10-point visual analog scale (VAS). Dysphagia was evaluated according to the Bazaz grading system [19] which was widely used by many spinal surgeons (0-None; 1-Mild; 2-Moderate; 3-Severe; as listed in Table 1). The standard definition: evidence of continuous bridging bone between the adjacent endplates of the involved motion segment, radiolucent lines at 50% or less of the graft-vertebra interfaces in CT scan, and 2 or less of segmental rotation on lateral flexion/ extension radiographs, was used The Zero-P group included 67 consecutive patients with a mean age of years and a mean follow-up duration of 3 years. The Plate group included 72 consecutive patients with a mean age of years and a mean follow-up duration of 3 years. There were seven patients in the Zero-P group and nine patients in the Plate group did not complete the final follow-up and these patients were excluded from the final analyses. The results are based on 60 patients in the Zero-P group and 63 patients in the Plate group. The Zero-P group had a mean intraoperative blood loss of ±39.35 ml, a mean intraoperative time of ±19.81 minutes and a mean length of hospital stay of 12.44± 4.19 days. The Plate group had a mean intraoperative blood loss of ±34.23 ml, a mean intraoperative time of ±25.32 minutes and a mean length of hospital stay of 12.78± 3.56 days. There were no significant difference between two groups concerning age, gender, VAS for neck, VAS for arm and JOA scores before surgery (all, P>0.05) as shown in Table Int J Clin Exp Med 2016;9(11):
4 Figure 2. A 70-year-old male patient was operated on two-level anterior cervical discectomy and fusion using the Zero-P implant at segment of C3/4 and C4/5 because of herniation of intervertebral discs (A-C), one week postoperative X-rays and CT scan showed the good position of the implants (D, E), six months postoperative CT scan showed bony fusion at C3/4 but not at C4/5 (F), 12 months postoperative (G) and 18 months postoperative (H) CT scan showed bony fusion at C3/4 and C4/5. 2. The JOA and VAS pain scores in two groups were significantly improved after surgery (all, P<0.05). Similar improvements were observed in the JOA and VAS pain scores in both groups at the final follow-up (P>0.05). The zero-p group had a lower fusion rates at the 3, 6 months follow-up, but the fusion rates were found to be similar and satisfying in two groups at the 12 months follow-up and at the final follow-up (Figure 2). There were three patients in the Zero-P group and four patients in the Plate group did not reach bony fusion according to the standard definition listed above (Figure 3). Radiographic and clinical outcomes at the final follow-up between the two groups are listed in Table 3. The total incidence of dysphagia in Zero-P groups was 40.00% at one week, 23.33% at one month, 18.33% at three months, 10.00% at six months, 8.33% at 12 months and 5.00% at the latest follow-up. The total incidence of dysphagia in Plate group was 55.56% at one week, 46.03% at one month, 33.33% at three months, 25.40% at six months, 17.46% at 12 months and 15.87% at the latest follow-up. The incidences of dysphagia for two groups are listed in detail in Table 4. There were no wound infection, esophageal perforation, instrumentation failure, nerve root injury, pulmonary em- bolism, perioperative cardiac event or other serious complications in two study groups. For other post-operative complications such as postoperative hematoma, recurrent laryngeal nerve palsy, cerebrospinal fluid leakage and pseudarthrosis, there were no significant difference between two groups (Table 5; all, P>0.05). Discussion ACDF for the treatment of degenerative cervical spondylosis has been introduced as a classical spinal procedure more than 60 years. Aimed to increase the immediate postoperative stability after bone grafting, avoid long time plaster immobilization and increase the fusion rates, anterior plate was developed in recent decades. However, the necessity and selectivity for additional instrumentation after decompression still remain controversial. Anterior cervical plate have been reported to reduce the incidence of the cage subsidence and displacement and increase the fusion rates but have also been reported to be associated with some relative complications and disadvantages. In order to overcome the disadvantages and limitations but maintain the advantages of anterior cervical plate, a new zero-profile, stand-alone device (Zero-P, Synthes GmbH, Switzerland) for ACDF has been developed in recent years and it has Int J Clin Exp Med 2016;9(11):
5 Figure 3. A 53-year-old female patient was operated on two-level anterior cervical discectomy and fusion using the Zero-P implant at segment of C5/6 and C6/7, one week postoperative CT scan showed the good position of the implant (A), 3 months postoperative showed no evidence of bony fusion (B), 6 months postoperative CT scan showed bony fusion at C5/6 but not C6/7 (C), 12 months postoperative CT scan showed bony fusion at C5/6 and C6/7 (D). Table 3. Radiographic and clinical outcomes at the final follow-up Zero-P group (N=60) Plate group (N=63) JOA 14.5± ± VAS for neck 1.37± ± VAS for arm 1.18± ± Fusion rate 95.00% 93.65% Data were shown as mean ± SD. been also widely reported in previous studies in single level ACDF with excellent clinical outcomes. Results from a biomechanical 3-dimensional spine test showed that segmental stability decreases with the number of instrumented segments. So the safety and validity of twolevel ACDF using Zero-P implant remains uncl- P ear. Aimed to compare the clinical outcomes with radiographic data and complications between Zero-P implant and conventional cageplate implant in two-level ACDF for the treatment of degenerative cervical spondylosis, we conducted this retrospective study. In this study, we observed that the overall clinical and radiographic results were similar in two groups. Three months after surgery the neck pain and arm pain VAS score in both groups were significantly decreased compared with preoperative VAS score. Previous studies have reported the rate of postoperative transient dysphagia following ACDF ranges from 2% to 67% [19, 22, 23]. Similarly the results from our study also indicated that the patients in Plate group had a much higher incidence of dyspha Int J Clin Exp Med 2016;9(11):
6 Table 4. The incidences of dysphagia for two-level ACDF using Zero-P and cage-plate Time Zero-P group (N=60) None Mild Moderate Severe Total incidence Plate group (N=63) None Mild Moderate Severe Total incidence One week % % One month % % Three months % % Six months % % One year % % The final follow-up % % #Mann-Whitney U test. P # Table 5. Postoperative complications of two-level ACDF using Zero-P and cage-plate Zero-P group (N=60) gia compared to patients in Zero-P group at each follow-up. Most of the dysphagia in two groups was found to be mild and gradually decreased in the following three months. Moderate or severe dysphagia was not common in two groups. However, in this study there were still 5% patients in Zero-P group and 15.87% patients in Plate group suffering from dysphagia at the latest follow-up. Lee et al. has demonstrated that design and thickness of anterior plates has an impact on postoperative dysphagia incidence [24]. Anterior plating is associated with higher rates of postoperative dysphagia in ACDF surgery [25, 26]. The Zero-P implant may decrease the incidence of dysphagia as it avoid the direct impinging as the anterior cervical locking plate is placed directly posterior to the esophagus [10, 27]. However, the exact pathophysiologic mechanism of dysphagia remains unknown, and the dysphagia is often regarded as a multi-factor result. Plate thickness or a zero-profile device is just one of the multiple factors which influence the incidence of post-operative dysphagia. In our study, we also found an excellent fusion rate with good stability. The zero-p group had a Plate group (N=63) Postoperative hematoma Wound Infection 0 0 NA Recurrent Laryngeal Nerve Palsy Cerebrospinal fluid leakage Esophageal Perforation 0 0 NA Instrumentation Failure 0 0 NA Pseudarthrosis P lower fusion rates at 3, 6 months after surgery, but the fusion rates were also similar and satisfying in two groups at 12 months after surgery and at the final follow-up. The self-locking devices were reported to ensure excellent primary temporary stability of the implant and promote early bony fusion. In addition, the elastic modulus of the anchored cage is similar to that of bone, which theoretically helps to decrease stress shielding and increase bony fusion [11]. Of course, surgi- cal techniques that include optimal preparation of the fusion bed and proper disc space distraction may also have an impact on fusion rate. There were no wound infection, esophageal perforation, instrumentation failure, nerve root injury, pulmonary embolism, perioperative cardiac event or other serious complications in two study groups. For other post-operative complications such as postoperative hematoma, recurrent laryngeal nerve palsy, cerebrospinal fluid leakage and pseudarthrosis, there were no significant difference between two groups. However, there are also some limitations in our study. First, the design of the study is a retrospective study. In addition, only 123 consecutive patients were included in this study. Thus, future prospective, randomized, controlled studies with larger sample size are needed. In conclusion, the results of this study do not show significant differences between Zero-P implant and the traditional titanium plate with cage for degenerative cervical spondylosis in terms of improvement in JOA scores, VAS pain scores, fusion rate, and main complications. The Zero-P implant and the traditional titanium plate with cage are both effective treatments Int J Clin Exp Med 2016;9(11):
7 for two-level degenerative cervical spondylosis, but the Zero-P implant was associated with a lower dysphagia incidence. Future prospective, randomized, controlled studies with larger sample size are needed. Acknowledgements This study was supported by the foundation of Science and Technology Department of Sichuan Province Government, PR China (No. 2014SZ- 0236). Disclosure of conflict of interest None. Address correspondence to: Hao Liu, Department of Orthopedics, West China Hospital, Sichuan University, 37 Guoxuexiang, Chengdu , Sichuan Province, P. R. China. liuhao6304@hotmail. com References [1] Simmons EH. Anterior cervical discectomy and fusion. Proc R Soc Med 1970; 63: [2] Simmons EH and Bhalla SK. Anterior cervical discectomy and fusion. A clinical and biomechanical study with eight-year follow-up. The Journal of bone and joint surgery. J Bone Joint Surg Br 1969; 51: [3] Kaiser MG, Haid RW, Subach BR, Barnes B and Rodts GE. Anterior cervical plating enhances arthrodesis after discectomy and fusion with cortical allograft. Neurosurgery 2002; 50: [4] Wang JC, McDonough PW, Endow KK and Delamarter RB. Increased fusion rates with cervical plating for two-level anterior cervical discectomy and fusion. Spine 2000; 25: [5] Kim SW, Limson MA, Kim SB, Arbatin JJ, Chang KY, Park MS, Shin JH and Ju YS. Comparison of radiographic changes after ACDF versus Bryan disc arthroplasty in single and bi-level cases. Eur Spine J 2009; 18: [6] Pitzen TR, Chrobok J, Stulik J, Ruffing S, Drumm J, Sova L, Kucera R, Vyskocil T and Steudel WI. Implant Complications, Fusion, Loss of Lordosis, and Outcome After Anterior Cervical Plating With Dynamic or Rigid Plates Two-Year Results of a Multi-Centric, Randomized, Controlled Study. Spine 2009; 34: [7] Bazaz R, Lee MJ and Yoo JU. Incidence of dysphagia after anterior cervical spine surgery-a prospective study. Spine 2002; 27: [8] Sahjpaul RL. Esophageal perforation from anterior cervical screw migration. Surg Neurol 2007; 68: [9] Yang Y, Ma L, Liu H and Xu M. A Meta-Analysis of the Incidence of Patient-Reported Dysphagia After Anterior Cervical Decompression and Fusion with the Zero-Profile Implant System. Dysphagia 2016; 31: [10] Scholz M, Schnake KJ, Pingel A, Hoffmann R and Kandziora F. A New Zero-profile Implant for Stand-alone Anterior Cervical Interbody Fusion. Clin Orthop Relat Res 2011; 469: [11] Wang Z, Jiang W, Li X, Wang H, Shi J, Chen J, Meng B and Yang H. The application of zeroprofile anchored spacer in anterior cervical discectomy and fusion. Eur Spine J 2015; 24: [12] Dong J, Lu M, Lu T, Liang B, Xu J, Zhou J, Lv H, Qin J, Cai X, Huang S, Li H, Wang D and He X. Meta-Analysis Comparing Zero-Profile Spacer and Anterior Plate in Anterior Cervical Fusion. PLoS One 2015; 10: e [13] Shao H, Chen J, Ru B, Yan F, Zhang J, Xu S and Huang Y. Zero-profile implant versus conventional cage-plate implant in anterior cervical discectomy and fusion for the treatment of degenerative cervical spondylosis: a meta-analysis. J Orthop Surg Res 2015; 10: 148. [14] Qi M, Chen H, Liu Y, Zhang Y, Liang L and Yuan W. The use of a zero-profile device compared with an anterior plate and cage in the treatment of patients with symptomatic cervical spondylosis A preliminary clinical investigation. Bone Joint J 2013; 95B: [15] Barbagallo GM, Romano D, Certo F, Milone P, Albanese V. Zero-P: a new zero-profile cageplate device for single and multilevel ACDF. A single Institution series with four years maximum follow-up and review of the literature on zero-profile devices. Eur Spine J 2013; 22: S868-S878. [16] Yan B and Nie L. Clinical comparison of Zeroprofile interbody fusion device and anterior cervical plate interbody fusion in treating cervical spondylosis. Int J Clin Exp Med 2015; 8: [17] Scholz M, Schleicher P, Pabst S and Kandziora F. A zero-profile anchored spacer in multilevel cervical anterior interbody fusion: biomechanical comparison to established fixation techniques. Spine (Phila Pa 1976) 2015; 40: E [18] Aronson N, Filtzer DL and Bagan M. Anterior cervical fusion by the smith-robinson approach. J Neurosurg 1968; 29: [19] Bazaz R, Lee MJ and Yoo JU. Incidence of dysphagia after anterior cervical spine surgery: a Int J Clin Exp Med 2016;9(11):
8 prospective study. Spine (Phila Pa 1976) 2002; 27: [20] Fraser JF and Haertl R. Anterior approaches to fusion of the cervical spine: a metaanalysis of fusion rates. J Neurosurg Spine 2007; 6: [21] Sanden B, Olerud C, Petren-Mallmin M, Johansson C and Larsson S. The significance of radiolucent zones surrounding pedicle screws- Definition of screw loosening in spinal instrumentation. J Bone Joint Surg Br 2004; 86: [22] Frempong-Boadu A, Houten JK, Osborn B, Opulencia T, Kells T, Guida TD and Le Roux PD. Swallowing and speech dysfunction in patients undergoing anterior cervical discectomy and fusion: A prospective, objective preoperative and postoperative assessment. J Spinal Disord Tech 2002; 15: [23] Smith-Hammond CA, New KC, Pietrobon R, Curtis DJ, Scharver CH and Turner DA. Prospective analysis of incidence and risk factors of dysphagia in spine surgery patients - Comparison of anterior cervical, posterior cervical, and lumbar procedures. Spine 2004; 29: [24] Lee MJ, Bazaz R, Furey CG and Yoo J. Influence of anterior cervical plate design on dysphagia - A 2-year prospective longitudinal follow-up study. J Spinal Disord Tech 2005; 18: [25] Hofstetter CP, Kesavabhotla K and Boockvar JA. Zero-profile Anchored Spacer Reduces Rate of Dysphagia Compared With ACDF With Anterior Plating. J Spinal Disord Tech 2015; 28: E [26] Yang Y, Ma L, Liu H, Liu Y, Hong Y, Wang B, Ding C, Deng Y, Song Y and Liu L. Comparison of the incidence of patient-reported post-operative dysphagia between ACDF with a traditional anterior plate and artificial cervical disc replacement. Clin Neurol Neurosurg 2016; 148: [27] Li Y, Hao D, He B, Wang X and Yan L. The Efficiency of Zero-profile Implant in Anterior Cervical Discectomy Fusion A Prospective Controlled Long-term Follow-up Study. J Spinal Disord Tech 2015; 28: Int J Clin Exp Med 2016;9(11):
Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report
 Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Case Report Two-year follow-up results of artificial disc replacement C7-T1
 Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Case Report Three-level anterior cervical decompression and fusion using the Zero-profile implant system
 Int J Clin Exp Med 2016;9(8):16847-16855 www.ijcem.com /ISSN:1940-5901/IJCEM0028686 Case Report Three-level anterior cervical decompression and fusion using the Zero-profile implant system Yi Yang 1, Aiping
Int J Clin Exp Med 2016;9(8):16847-16855 www.ijcem.com /ISSN:1940-5901/IJCEM0028686 Case Report Three-level anterior cervical decompression and fusion using the Zero-profile implant system Yi Yang 1, Aiping
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
The application of zero-profile anchored spacer in anterior cervical discectomy and fusion
 Eur Spine J (2015) 24:148 154 DOI 10.1007/s00586-014-3628-9 ORIGINAL ARTICLE The application of zero-profile anchored spacer in anterior cervical discectomy and fusion Zhiwen Wang Weimin Jiang Xuefeng
Eur Spine J (2015) 24:148 154 DOI 10.1007/s00586-014-3628-9 ORIGINAL ARTICLE The application of zero-profile anchored spacer in anterior cervical discectomy and fusion Zhiwen Wang Weimin Jiang Xuefeng
Zongyu Zhang 1, Yawei Li 2 and Weimin Jiang 1*
 Zhang et al. BMC Musculoskeletal Disorders (2018) 19:119 https://doi.org/10.1186/s12891-018-2033-7 RESEARCH ARTICLE Open Access A comparison of zero-profile anchored spacer (ROI-C) and plate fixation in
Zhang et al. BMC Musculoskeletal Disorders (2018) 19:119 https://doi.org/10.1186/s12891-018-2033-7 RESEARCH ARTICLE Open Access A comparison of zero-profile anchored spacer (ROI-C) and plate fixation in
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Original Article Incidence and risk factor analysis of dysphagia after anterior cervical corpectomy and fusion: evidence from 297 patients
 Int J Clin Exp Med 2017;10(4):6973-6979 www.ijcem.com /ISSN:1940-5901/IJCEM0048214 Original Article Incidence and risk factor analysis of dysphagia after anterior cervical corpectomy and fusion: evidence
Int J Clin Exp Med 2017;10(4):6973-6979 www.ijcem.com /ISSN:1940-5901/IJCEM0048214 Original Article Incidence and risk factor analysis of dysphagia after anterior cervical corpectomy and fusion: evidence
Quintex Cervical Plating System
 Quintex Cervical Plating System Product Brochure Aesculap Spine Driven by proven plating technology. Inspired by the future of ACDF. Quintex Cervical Plating System Today s most versatile plating system,
Quintex Cervical Plating System Product Brochure Aesculap Spine Driven by proven plating technology. Inspired by the future of ACDF. Quintex Cervical Plating System Today s most versatile plating system,
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Outcomes and revision rates following multilevel anterior cervical discectomy and fusion
 Original Study Outcomes and revision rates following multilevel anterior cervical discectomy and fusion Joseph L. Laratta 1, Hemant P. Reddy 2, Kelly R. Bratcher 1, Katlyn E. McGraw 1, Leah Y. Carreon
Original Study Outcomes and revision rates following multilevel anterior cervical discectomy and fusion Joseph L. Laratta 1, Hemant P. Reddy 2, Kelly R. Bratcher 1, Katlyn E. McGraw 1, Leah Y. Carreon
Dynamic anterior cervical plating for multi-level spondylosis: Does it help?
 Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
Original Article Application of Zero-P on anterior cervical decompression and bone fusion
 Int J Clin Exp Med 2017;10(4):7077-7083 www.ijcem.com /ISSN:1940-5901/IJCEM0049328 Original Article Application of Zero-P on anterior cervical decompression and bone fusion Yuxiang Xiao, Yongxiang Shi,
Int J Clin Exp Med 2017;10(4):7077-7083 www.ijcem.com /ISSN:1940-5901/IJCEM0049328 Original Article Application of Zero-P on anterior cervical decompression and bone fusion Yuxiang Xiao, Yongxiang Shi,
Instructions for use Prodisc -C Vivo Cervical disc prosthesis
 Instructions for use Prodisc -C Vivo Cervical disc prosthesis Instructions for use Prodisc-C Vivo Cervical disc prosthesis Safety precautions Please read these instructions for use, the Synthes brochure
Instructions for use Prodisc -C Vivo Cervical disc prosthesis Instructions for use Prodisc-C Vivo Cervical disc prosthesis Safety precautions Please read these instructions for use, the Synthes brochure
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review comparing multilevel versus single-level surgery
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Fixation of multiple level anterior cervical disc using cages versus cages and plating
 Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Anterior Cervical Fusion: What is the Effect on Swallow Function?
 Anterior Cervical Fusion: What is the Effect on Swallow Function? Rebecca L. Gould, MSC, CCC-SLP, BRS-S rebec26050@aol.com (561) 833-2090 www.med-speech.com STATE OF THE ART EVALUATION Anterior Cervical
Anterior Cervical Fusion: What is the Effect on Swallow Function? Rebecca L. Gould, MSC, CCC-SLP, BRS-S rebec26050@aol.com (561) 833-2090 www.med-speech.com STATE OF THE ART EVALUATION Anterior Cervical
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Comparison among perfect-c, zero-p, and plates with a cage in single-level cervical degenerative disc disease
 Noh and Zhang BMC Musculoskeletal Disorders (2018) 19:33 DOI 10.1186/s12891-018-1950-9 RESEARCH ARTICLE Open Access Comparison among perfect-c, zero-p, and plates with a cage in single-level cervical degenerative
Noh and Zhang BMC Musculoskeletal Disorders (2018) 19:33 DOI 10.1186/s12891-018-1950-9 RESEARCH ARTICLE Open Access Comparison among perfect-c, zero-p, and plates with a cage in single-level cervical degenerative
Surgical Technique INTERSOMATIC CERVICAL CAGE
 R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
R INTERSOMATIC CERVICAL CAGE NEOCIF IMPLANTS NEOCIF is an implant designed to make anterior cervical interbody fusion (ACIF) easier and to remove the need for structural autologous graft. The cage is made
Zero-profile Anchored Spacer Reduces Rate of Dysphagia Compared With ACDF With Anterior Plating
 e PRIMARY RESEARCH Zero-profile Anchored Spacer Reduces Rate of Dysphagia Compared With ACDF With Anterior Plating Christoph P. Hofstetter, MD, PhD, Kartik Kesavabhotla, BS, and John A. Boockvar, MD Study
e PRIMARY RESEARCH Zero-profile Anchored Spacer Reduces Rate of Dysphagia Compared With ACDF With Anterior Plating Christoph P. Hofstetter, MD, PhD, Kartik Kesavabhotla, BS, and John A. Boockvar, MD Study
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Matthew Colman, MD Assistant Professor, Spine Surgery and Musculoskeletal Oncology Rush University Medical Center ACDF
 is the most reliable option for twolevel anterior cervical surgery Matthew Colman, MD Assistant Professor, Spine Surgery and Musculoskeletal Oncology Rush University Medical Center Disclosures Medicrea:
is the most reliable option for twolevel anterior cervical surgery Matthew Colman, MD Assistant Professor, Spine Surgery and Musculoskeletal Oncology Rush University Medical Center Disclosures Medicrea:
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion
 Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Patient Information ACDF. Anterior Cervical Discectomy and Fusion
 Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
A cervical zero-profile cage with integrated angle-stable fixation : 24-months results
 Acta Orthop. Belg., 2014, 80, 558-566 ORIGINAL STUDY A cervical zero-profile cage with integrated angle-stable fixation : 24-months results Matti Scholz, Sebastiaan Schelfaut, Andreas Pingel, Philipp Schleicher,
Acta Orthop. Belg., 2014, 80, 558-566 ORIGINAL STUDY A cervical zero-profile cage with integrated angle-stable fixation : 24-months results Matti Scholz, Sebastiaan Schelfaut, Andreas Pingel, Philipp Schleicher,
5/19/2017. Disclosures. Introduction. How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations
 How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations Richard D. Guyer, M.D. Disclosures Guyer (a) Alphatec; (b) Spinal Kinetics, Spinal Ventures, Mimedix; (c) DePuy
How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations Richard D. Guyer, M.D. Disclosures Guyer (a) Alphatec; (b) Spinal Kinetics, Spinal Ventures, Mimedix; (c) DePuy
KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients
 Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Royal Oak Cervical Plate System
 Royal Oak Cervical Plate System Manufactured by Nexxt Spine, Inc. Royal Oak Cervical Plate System INTRODUCTION FEATURES AND BENEFITS Table of Contents SURGICAL TECHNIQUE Step 1. Patient Positioning Step
Royal Oak Cervical Plate System Manufactured by Nexxt Spine, Inc. Royal Oak Cervical Plate System INTRODUCTION FEATURES AND BENEFITS Table of Contents SURGICAL TECHNIQUE Step 1. Patient Positioning Step
Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft
 Asian Biomedicine Vol. 4 No. 1 February 2010; 147-152 Brief communication (Original) Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft Prakit Tienboon a, Surapon
Asian Biomedicine Vol. 4 No. 1 February 2010; 147-152 Brief communication (Original) Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft Prakit Tienboon a, Surapon
OPERATIVE TECHNIQUE. CONSTRUX Mini PTC. Mini PTC Spacer System
 OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
Axial Lumbosacral Interbody Fusion. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Cervical Motion Preservation
 Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Apache Cervical Interbody Fusion Device. Surgical Technique. Page of 13. LC-005 Rev F
 LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
PARADIGM SPINE. Anterior Cervical Fusion Cage. Cervical Interbody Fusion
 PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
ProDisc-L Total Disc Replacement. IDE Clinical Study
 Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Safety and Efficacy of Bioabsorbable Cervical Spacers and Low-Dose rhbmp-2 for Multilevel ACDF. Kaveh Khajavi, MD, FACS Alessandria Struebing, MSPH
 Safety and Efficacy of Bioabsorbable Cervical Spacers and Low-Dose rhbmp-2 for Multilevel ACDF Kaveh Khajavi, MD, FACS Alessandria Struebing, MSPH Disclosures FDA off-label usage rhbmp-2 (INFUSE, Medtronic
Safety and Efficacy of Bioabsorbable Cervical Spacers and Low-Dose rhbmp-2 for Multilevel ACDF Kaveh Khajavi, MD, FACS Alessandria Struebing, MSPH Disclosures FDA off-label usage rhbmp-2 (INFUSE, Medtronic
Anterior cervical discectomy and fusion with ROI-C peek cage: cervical alignment and patient outcomes
 DOI 10.1007/s00586-014-3553-y ORIGINAL ARTICLE Anterior cervical discectomy and fusion with ROI-C peek cage: cervical alignment and patient outcomes Giovanni Grasso Filippo Giambartino Giovanni Tomasello
DOI 10.1007/s00586-014-3553-y ORIGINAL ARTICLE Anterior cervical discectomy and fusion with ROI-C peek cage: cervical alignment and patient outcomes Giovanni Grasso Filippo Giambartino Giovanni Tomasello
Swallowing Function Following Anterior Cervical Discectomy and Fusion With and Without Anterior Plating: A SWAL-QOL and Radiographic Assessment
 Swallowing Function Following Anterior Cervical Discectomy and Fusion With and Without Anterior Plating: A SWAL-QOL and Radiographic Assessment Brittany E. Haws, MD1 ; Benjamin Khechen, BA1; Dil V. Patel,
Swallowing Function Following Anterior Cervical Discectomy and Fusion With and Without Anterior Plating: A SWAL-QOL and Radiographic Assessment Brittany E. Haws, MD1 ; Benjamin Khechen, BA1; Dil V. Patel,
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Adjacent segment disease after anterior cervical discectomy and fusion
 Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
Adjacent segment disease after anterior cervical discectomy and fusion, Besar, Akar and Abdelkader MD. 43 Adjacent segment disease after anterior cervical discectomy and fusion *Mohamed Abdulrahman Besar.MD;
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Artificial Intervertebral Disc: Cervical Spine
 Protocol Artificial Intervertebral Disc: Cervical Spine (701108) Medical Benefit Effective Date: 01/01/08 Next Review Date: 03/13 Preauthorization* No Review Dates: 06/07, 07/08, 05/09, 05/10, 03/11, 03/12
Protocol Artificial Intervertebral Disc: Cervical Spine (701108) Medical Benefit Effective Date: 01/01/08 Next Review Date: 03/13 Preauthorization* No Review Dates: 06/07, 07/08, 05/09, 05/10, 03/11, 03/12
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Stylianos Kapetanakis, Tryfon Thomaidis, George Charitoudis, Pavlos Pavlidis, Panagiotis Theodosiadis, Grigorios Gkasdaris
 Original Study Single anterior cervical discectomy and fusion (ACDF) using self- locking stand-alone polyetheretherketone (PEEK) cage: evaluation of pain and health-related quality of life Stylianos Kapetanakis,
Original Study Single anterior cervical discectomy and fusion (ACDF) using self- locking stand-alone polyetheretherketone (PEEK) cage: evaluation of pain and health-related quality of life Stylianos Kapetanakis,
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Heterotopic ossification in cervical disc arthroplasty: Is it clinically relevant?
 Original research Heterotopic ossification in cervical disc arthroplasty: Is it clinically relevant? 15 15 2 Heterotopic ossification in cervical disc arthroplasty: Is it clinically relevant? Authors Giuseppe
Original research Heterotopic ossification in cervical disc arthroplasty: Is it clinically relevant? 15 15 2 Heterotopic ossification in cervical disc arthroplasty: Is it clinically relevant? Authors Giuseppe
Intermediate Clinical Outcome of Bryan Cervical Disc Replacement for Degenerative Disk Disease and Its Effect on Adjacent Segment Disks
 Intermediate Clinical Outcome of Bryan Cervical Disc Replacement for Degenerative Disk Disease and Its Effect on Adjacent Segment Disks Chen Ding, MD; Ying Hong, BS; Hao Liu, MD; Rui Shi, MD; Tao Hu, MD;
Intermediate Clinical Outcome of Bryan Cervical Disc Replacement for Degenerative Disk Disease and Its Effect on Adjacent Segment Disks Chen Ding, MD; Ying Hong, BS; Hao Liu, MD; Rui Shi, MD; Tao Hu, MD;
Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty for degenerative cervical disc disease: a minimal five-year follow-up
 Wang et al. BMC Musculoskeletal Disorders (2018) 19:101 https://doi.org/10.1186/s12891-018-2017-7 RESEARCH ARTICLE Open Access Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty
Wang et al. BMC Musculoskeletal Disorders (2018) 19:101 https://doi.org/10.1186/s12891-018-2017-7 RESEARCH ARTICLE Open Access Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty
Zimmer Anterior Buttress Plate System. Surgical Technique
 Zimmer Anterior Buttress Plate System Surgical Technique 2 Zimmer Anterior Buttress Plate System Surgical Technique Zimmer Anterior Buttress Plate System Surgical Technique Description, Indications & Contraindications...
Zimmer Anterior Buttress Plate System Surgical Technique 2 Zimmer Anterior Buttress Plate System Surgical Technique Zimmer Anterior Buttress Plate System Surgical Technique Description, Indications & Contraindications...
Surgical technique. SynCage-C short
 Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2014 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2014 Section: Surgery Place(s) of Service:
Department of Orthopaedic, Spine Center, West China Hospital, Sichuan University, Chengdu , China; 2
 Int J Clin Exp Med 2016;9(2):2237-2244 www.ijcem.com /ISSN:1940-5901/IJCEM0013676 Original Article Clinical outcome of a New Zero-profile Implant used in patients with cervical spondylosis: a retrospective
Int J Clin Exp Med 2016;9(2):2237-2244 www.ijcem.com /ISSN:1940-5901/IJCEM0013676 Original Article Clinical outcome of a New Zero-profile Implant used in patients with cervical spondylosis: a retrospective
Anterior Cervical Discectomy with Stand Alone PEEK Cage for Management of 3 and 4 Level Degenerative Cervical Disc Disease *
 WScJ 3: 201-209, 2016 Anterior Cervical Discectomy with Stand Alone PEEK Cage for Management of 3 and 4 Level Degenerative Cervical Disc Disease * Khaled MF Saoud, Hazem A Mashaly, Hatem Sabry Department
WScJ 3: 201-209, 2016 Anterior Cervical Discectomy with Stand Alone PEEK Cage for Management of 3 and 4 Level Degenerative Cervical Disc Disease * Khaled MF Saoud, Hazem A Mashaly, Hatem Sabry Department
Adjacent Segment Degeneration Following Anterior Cervical Discectomy and Fusion Versus the Bryan Cervical Disc Arthroplasty
 e-issn 1643-3750 DOI: 10.12659/MSM.905178 Received: 2017.05.05 Accepted: 2017.05.22 Published: 2017.06.02 Adjacent Segment Degeneration Following Anterior Cervical Discectomy and Fusion Versus the Bryan
e-issn 1643-3750 DOI: 10.12659/MSM.905178 Received: 2017.05.05 Accepted: 2017.05.22 Published: 2017.06.02 Adjacent Segment Degeneration Following Anterior Cervical Discectomy and Fusion Versus the Bryan
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Lumbar Disc Replacement FAQs
 ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
ISO 9001:2015 FS 550968 What is Lumbar Disc Replacement? The intervertebral discs are the shock absorbers between the bones of the spine. Unfortunately, they often degenerate tearing, bursting, or just
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF)
 Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
L-VARLOCK. Posterior Lumbar Cage with adjustable lordosis. S urgical T echnique
 L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
Stand-Alone Technology. Reginald Davis, M.D., FAANS, FACS Director of Clinical Research
 Stand-Alone Technology Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Stand-Alone Devices Optio-C Stalif C Coalition Prevail ROI-C Technology Descriptions Optio-C A no profile,
Stand-Alone Technology Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Stand-Alone Devices Optio-C Stalif C Coalition Prevail ROI-C Technology Descriptions Optio-C A no profile,
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis
 CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
SynCage-C short. Surgical Technique. This publication is not intended for distribution in the USA.
 SynCage-C short Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Implants 2 Indications/contra-indications
SynCage-C short Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Implants 2 Indications/contra-indications
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Surgical Technique. Apache Anterior Lumbar Interbody Fusion
 Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
CASE SERIES: PEEK-OPTIMA HA Enhanced Polymer Shows Early Clinical Success in Interbody Spinal Fusions
 CASE SERIES: PEEK-OPTIMA HA Enhanced Polymer Shows Early Clinical Success in Interbody Spinal Fusions North American Spine Society (NASS) Annual Meeting Presentation of Findings, October 2016 authors:
CASE SERIES: PEEK-OPTIMA HA Enhanced Polymer Shows Early Clinical Success in Interbody Spinal Fusions North American Spine Society (NASS) Annual Meeting Presentation of Findings, October 2016 authors:
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
EIT TLIF Cage. For Natural Bone Ingrowth with EIT Cellular Titanium
 EIT TLIF Cage For Natural Bone Ingrowth with EIT Cellular Titanium EIT TLIF Cage Surgical Technique EIT Cellular Titanium provides active fusion area» ~ 80% porosity» ~ 650 µm diamond pore size» open interconnected
EIT TLIF Cage For Natural Bone Ingrowth with EIT Cellular Titanium EIT TLIF Cage Surgical Technique EIT Cellular Titanium provides active fusion area» ~ 80% porosity» ~ 650 µm diamond pore size» open interconnected
Zero-P Instruments and Implants. Zero-profile anterior cervical interbody fusion (ACIF) device.
 Zero-P Instruments and Implants. Zero-profile anterior cervical interbody fusion (ACIF) device. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Zero-P
Zero-P Instruments and Implants. Zero-profile anterior cervical interbody fusion (ACIF) device. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Zero-P
ACP1 CERVICAL PLATE SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE II.
 I. ACP1 CERVICAL PLATE II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE I. Introduction The Gold Standard Orthopaedics, LLC ACP1 Spinal System was designed with surgeons to incorporate strength, functionality,
I. ACP1 CERVICAL PLATE II. SPINAL SYSTEM SURGICAL TECHNIQUE GUIDE I. Introduction The Gold Standard Orthopaedics, LLC ACP1 Spinal System was designed with surgeons to incorporate strength, functionality,
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Discecctomy and anterior fusion with cages: advantages and disavantages. A. Zagra
 Spinal Surgery Division 1 I. R. S. S. C. Galeazzi Orthpedic Institute Milan Chief : Prof. A. Zagra Discecctomy and anterior fusion with cages: advantages and disavantages A. Zagra CONSERVATIVE TREATMENT
Spinal Surgery Division 1 I. R. S. S. C. Galeazzi Orthpedic Institute Milan Chief : Prof. A. Zagra Discecctomy and anterior fusion with cages: advantages and disavantages A. Zagra CONSERVATIVE TREATMENT
SynCage. Surgical Technique. This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
 SynCage Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning This description alone
SynCage Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning This description alone
Biomechanical comparison between anterior cervical discectomy with fusion and without fusion.
 Biomedical Research 2017; 28 (4): 1706-1713 ISSN 0970-938X www.biomedres.info Biomechanical comparison between anterior cervical discectomy with fusion and without fusion. Andrei Stefan Iencean 1,2 Stefan
Biomedical Research 2017; 28 (4): 1706-1713 ISSN 0970-938X www.biomedres.info Biomechanical comparison between anterior cervical discectomy with fusion and without fusion. Andrei Stefan Iencean 1,2 Stefan
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Anterior cervical discectomy and fusion surgery versus total disc replacement: A comparative study with minimum of 10-year follow-up
 www.nature.com/scientificreports Received: 5 July 2017 Accepted: 16 November 2017 Published: xx xx xxxx OPEN Anterior cervical discectomy and fusion surgery versus total disc replacement: A comparative
www.nature.com/scientificreports Received: 5 July 2017 Accepted: 16 November 2017 Published: xx xx xxxx OPEN Anterior cervical discectomy and fusion surgery versus total disc replacement: A comparative
