Type II odontoid fractures in the elderly: early failure of nonsurgical treatment
|
|
|
- Octavia Gray
- 6 years ago
- Views:
Transcription
1 Neurosurg Focus 8 (6):Article 7, 2000, Click here to return to Table of Contents Type II odontoid fractures in the elderly: early failure of nonsurgical treatment CHARLES KUNTZ, IV, M.D., SOHAIL K. MIRZA, M.D., ABEL D. JARELL, M.D., JENS R. CHAPMAN, M.D., CHRISTOPHER I. SHAFFREY, M.D., AND DAVID W. NEWELL, M.D. Departments of Neurological Surgery and Orthopaedic Surgery, University of Washington, Seattle, Washington The optimum treatment of Type II odontoid fractures in the geriatric population remains controversial. Coexisting medical conditions encountered in the elderly patient often increase operative risk and make cervical immobilization difficult to tolerate. Previous studies have shown increased morbidity and mortality and decreased fusion rates for Type II odontoid fractures treated with cervical orthoses in the geriatric population, whereas low morbidity and mortality rates with operative management have recently been documented. To investigate the role of surgical and nonsurgical treatment, a retrospective analysis was performed of patients with Type II odontoid fractures who were at least 65 years old and were consecutively admitted to a single medical center from 1994 to Twenty patients met inclusion criteria. In 12 patients nonsurgical management with a cervical orthosis was attempted. The nonsurgical management failed early in six patients, with one associated death. Eleven patients were treated surgically with either anterior odontoid screw fixation or posterior C1 2 transarticular screw fixation and modified Gallie fusion. Postoperatively one patient required revision of the C1 2 transarticular screws, and there was one death. In conclusion Type II odontoid fractures in this elderly population were associated with early 10% morbidity and 20% mortality rates. Nonsurgical management of Type II odontoid fractures failed early in six (50%) of 12 patients, whereas surgical treatment failed early in one of 11 (9%) patients. Both the nonsurgical and surgical treatments resulted in approximately 10% morbidity and 10% mortality rates. KEY WORDS odontoid fracture geriatric surgical management nonsurgical management The optimum treatment of Type II odontoid fractures in the elderly remains controversial. 7,10 12 The medical frailty of the geriatric patient often compromises treatment, increasing the risks of both nonsurgical management with a cervical orthosis and surgical treatment with internal fixation and fusion. Surgical and nonsurgical treatment of odontoid fractures in the elderly is associated with higher morbidity and mortality rates when compared with younger patients with similar injuries. 7,10,11 Authors of recent investigations have reported that prolonged cervical immobilization in a halo-thoracic vest is often not well tolerated by the geriatric patient, leading to increased morbidity and mortality rates and a high rate of nonunion, while authors of contemporary reports of surgically treated Type II odontoid fractures in the elderly have found acceptably low morbidity and mortality rates with a high rate of union. 4, 7,11 To further investigate the role of surgical and nonsurgical treatment of Type II odontoid fractures in the elderly, we retrospectively reviewed the records of all patients aged 65 years or older in whom a diagnosis of Type II odontoid fracture had been made and who were admitted to Harborview Medical Center between 1994 and Abbreviation used in this manuscript: SCI = spinal cord injury. CLINICAL MATERIAL AND METHODS A retrospective review was performed of the records of patients aged 65 years or older who were consecutively admitted to a single medical center (regional level 1 trauma center) with a diagnosis of C-2 fracture between 1994 and Thirty-six patients aged 65 years or older were consecutively admitted with a diagnosis of C-2 fracture during the years of the study. Odontoid fractures were classified according to the method of Anderson and D Alonzo. 1 Of the 36 patients, 20 had Type II odontoid fractures. There were 12 men and eight women, ranging in age from 66 to 92 years (mean 80 years). These 20 patients represent approximately 4% of all patients admitted to Harborview Medical Center for management of cervical spine fractures during the years of the study. After obtaining approval from the human subjects review committee, the radiological studies and medical records for each of the study patients were reviewed. Each case was categorized according to age, sex, mechanism of injury, type of spine fracture, odontoid displacement, neurological injury, associated nonspinal injuries, treatment given, complications, hospitalization days, follow-up period, and outcome. Follow-up assessment consisted of reviewing outpatient medical records and radiographic studies; when follow up was limited over time, the patient or patient s Neurosurg. Focus / Volume 8 / June,
2 C. Kuntz IV, et al. family was contacted regarding long-term outcome. Fusion was defined as evidence of bone healing at the odontoid fracture site or posterior C1 2 bone graft fusion site and, when available, absence of movement on flexion extension radiographs. Early failure of treatment was defined as inadequate immobilization of the fracture within the first 30 days of treatment, inability of the patient to tolerate the treatment resulting in a change of the treatment plan, or death of the patient within 30 days of the treatment. RESULTS Patient Population The mechanism of injury was a fall in 15 patients, a motor vehicle accident in three patients, bicycle accident in one patient, and one patient was struck by an automobile. Four patients had associated spine fractures at other segmental levels, and nine patients had associated nonspinal injuries. The number of days in the hospital ranged from 1 to 24 days, with a mean of 12.5 days. The surgical and nonsurgical groups were similar with respect to age, sex, mechanism of injury, type of spine fracture, SCI, associated nonspinal injuries, and follow-up period (Tables 1 and 2). Evaluation of initial radiological studies revealed that at the time of diagnosis the odontoid displacement ranged from 0 to 11 mm, with a mean displacement of 5.4 mm. In the nonsurgical group the mean odontoid displacement was 4.5 mm, whereas in the surgical group the mean odontoid displacement was 6.6 mm. The odontoid fragment was anteriorly displaced in three patients and posteriorly displaced in 16 patients. Spinal cord injury was present in three patients and was always associated with posterior displacement of the odontoid. Management Protocol All patients were evaluated at Harborview Medical Center. When an odontoid fracture was suspected or diagnosed, the neurological and orthopedic surgical teams were consulted. Patients with suspected or diagnosed odontoid fractures underwent high-resolution computerized tomography scanning from the occiput to C-3. Magnetic resonance imaging was performed in all patients with suspected or diagnosed SCIs. After the diagnosis of odontoid fracture was made, the patient either underwent cervical traction for realignment of the odontoid or a cervical orthosis was directly applied. The treatment options were discussed with the patient and family, including a review of the advantages and risks of nonsurgical and surgical treatments. Treatment selection was based on the surgeon s recommendation and patient family preferences. The primary treatment was nonsurgical in 14 patients and surgical in six patients. The goal of nonsurgical and surgical treatment was to stabilize the Type II odontoid fracture and mobilize the patient early during the hospitalization. After treatment with either a cervical orthosis or surgical fixation/fusion, serial cervical radiographs were performed with the patient in the supine and upright positions to evaluate for evidence of instability. If the patient was unable to tolerate the cervical orthosis or if fracture alignment could not be maintained in the cervical orthosis, the patient underwent surgical fixation/fusion. Inadequate stabilization of the odontoid fracture in the cervical orthosis was determined on serial cervical radiographs by the senior treating surgeon over a period of time ranging from 6 to 28 days after the injury. RESULTS OF PATIENT FOLLOW-UP REVIEW Outcome analysis revealed that four patients died during the initial hospitalization. Two patients died after admission to the hospital, secondary to injuries unrelated to the odontoid fracture: a 91-year-old woman with severe dementia and a closed head injury died soon after admission when support was withdrawn and an 81-year-old man treated in a Minerva brace died of a significant closed head injury 6 days after the injury. The two remaining deaths occurred during treatment of the Type II odontoid fracture (one in the nonsurgical group and one in the surgical group): an 86-year-old man treated in a Minerva brace developed pneumonia and died after a respiratory arrest and an 84-year-old man died of cardiopulmonary failure postoperatively. Of the 16 patients discharged from the hospital, follow-up data were available for 15 patients with a mean follow-up time of 14 months. For one patient discharged from the hospital who was doing well, there was no information after the initial hospitalization. Nonsurgical Treatment Nonsurgical management was used in 14 of the 20 patients (Table 1). The mean age in the nonsurgical group was 81 years, of whom 57% were men. The mechanism of injury was a fall in nine patients and associated spinal fractures were present at other segmental levels in three patients. One patient had an SCI, and seven patients had associated nonspinal injuries. The mean hospitalization time was 13 days for patients who were initially managed nonsurgically. The average follow-up time in the nonsurgical group was 13 months. After admission to the hospital two patients died of injuries unrelated to the odontoid fracture or treatment of the odontoid fracture; these two patients have been excluded from the further analysis of nonsurgical management. Of the remaining 12 patients, eight were treated with a halo-thoracic vest, two were treated with a Minerva brace, and two were treated with a collar. The type of cervical orthosis was chosen based on the anatomy of the fracture combined with the medical frailty of the patient. Nondisplaced nondistracted Type II fractures in medically frail patients were more likely to be treated with a collar, whereas displaced distracted Type II fractures in medically healthy patients were more likely to be treated with a Minerva brace or halo-thoracic vest. The nonsurgical treatment failed early in six patients and was associated with a complication in one patient. The nonsurgical early failures included: an 86-year-old man treated with a Minerva brace who developed pneumonia and died after a respiratory arrest; a 92-year-old woman treated with a halo-thoracic vest who developed failure to thrive (unable to ambulate in the halo-thoracic vest, she became depressed and refused to eat) and subsequently underwent a posterior fixation and fusion with 2 Neurosurg. Focus / Volume 8 / June, 2000
3 Type II odontoid fractures in the elderly TABLE 1 Characteristics of patients who were managed nonsurgically* Mech- Odontoid Hospital- Follow Outcome Case Age (yrs), anism Type Displace- Associated ization Up No. Sex of Injury of Fx ment (mm) SCI Injuries Treatment (days) (mos) Radiological Clinical 1 83, F fall II 0 no minor CHI 3 5 stable fusion routine activity 2 89, F fall II 2 ant no CVA halo 12 4 stable fusion routine activity 3 81, M fall II 3 post no major CHI Minerva 7 NA NA death 7 days after CHI 4 87, F fall II 8 post no none 12 2 stable routine activity 5 81, M fall II 1 post no minor CHI, Minerva inadequate sta- NA radius & bilization, metacarpal failed Minerva fx 6 92, F fall II 5 post no none halo 24 6 adequate stabili- failure to thrive, zation failed halo 10 66, M fall II 2 post no scalp lacer- halo inadequate sta- NA ation bilization, failed halo 12 79, M bicycle II & 5 post no none halo 9 5 stable fusion routine activity accident C , M MVA II 10 post cent none halo inadequate sta- NA cord bilization, synd failed halo 14 76, F pedes- II 3 post no minor CHI, halo NA routine activity trian pelvic, tibia, (death from GI struck fibula & bleed 24 mos by car ankle fx after injury) 15 86, M MVA II & 2 ant no none Minerva 10 NA NA death from C-1 pneumonia/ respiratory arrest 10 days after injury 16 80, M fall II 2 post no none halo & 8 3 nonunion, stable routine activity 18 91, F fall II 10 post no major CHI 1 NA NA death 1 day support withdrawn 20 70, M MVA II, C-1, 10 post no none halo inadequate sta- NA C6 7 bilization, failed laminae, T-5 comp after injury * Ant = anterior; cent cord synd = central cord syndrome; CHI = closed head injury; comp = compound; CVA = cerebrovascular accident; fx = fracture; GI = gastrointestinal; MVA = motor vehicle accident; NA = not available; post = posterior. halo removal of the halo-thoracic vest postoperatively; and four patients (three treated with a halo-thoracic vest and one treated with a Minerva brace) who had inadequate stabilization of the fracture in the cervical orthosis and required surgical intervention (Fig. 1). The average odontoid movement/dynamic displacement in the halo-thoracic vest or Minerva brace for the four patients with inadequate stabilization of the fracture was 6.3 mm. The nonsurgical complication was a pin site infection with loosening of the halo ring requiring antibiotics and adjustment of the pins. Of the 12 patients in whom nonsurgical treatment with a cervical orthosis was attempted, six patients were discharged from the hospital in the cervical orthosis and completed the course of treatment in the cervical orthosis. Of those six patients, all returned to routine activity with no late neurological deterioration. Radiological evaluation revealed that three of the six patients developed a stable bone fusion, one patient developed a stable nonunion, and one patient with dementia treated with a collar was stable at 2-month follow up (in one patient there was Neurosurg. Focus / Volume 8 / June, 2000 insufficient follow-up radiographic data). The mean initial odontoid displacement in patients who completed a course of treatment in a cervical orthosis was 3.3 mm, whereas the mean initial odontoid displacement in patients in whom the cervical orthosis failed early was 5 mm. Age, mechanism of injury, type of spine fracture, and associated nonspinal injuries were similar among those patients in whom nonsurgical treatment failed and those patients who completed a course of nonsurgical treatment in a cervical orthosis. Operative Treatment Operative stabilization was performed in 11 of the 20 patients (Table 2). The mean age in the surgical group was 76 years, with 73% being men. The mechanism of injury was a fall in nine patients, and associated spinal fractures were present at other segmental levels in two patients. Three patients had SCIs, and four patients had associated nonspinal injuries. The mean hospitalization time was 14 3
4 C. Kuntz IV, et al. TABLE 2 Characteristics of patients who underwent surgery as a primary or secondary treatment* Outcome Mech- Odontoid Hospital- Follow Case Age (yrs), anism Type Displace- Associated ization Up Radio- No. Sex of Injury of Fx ment (mm) SCI Injuries Treatment (days) (mos) logical Clinical Primary operative management 7 84, M fall II 5 post no none trans screws w/ 5 NA NA died 3 days after modified surgery/cardio- Gallie/Phil- pulmonary adelphia failure 8 74, M fall II 9 post no scalp lac- trans screws w/ stable routine activity eration fusion (died of pros- tate cancer 3 yrs postinjury) 9 66, M fall II, C-1 7 post Frankel none trans screws w/ 19 0 NA NA D halo 11 71, M fall II 2 post Frankel none trans screws w/ 18 3 stable Frankel A, venti- A fusion lator-dependent Philadelphia quadriplegic 17 86, F fall II 11 post no none trans screws w/ 18 6 stable routine activity fusion 19 79, F fall II 11 post no ankle fx trans screws w/ stable routine activity fusion Secondary operative management 5 81, M fall II 1 post no minor CHI, odontoid screw/ stable routine activity radius and halo fusion metacarpal fx 6 92, F fall II 5 ant no none trans screws w/ 24 6 stable routine activity fusion 10 66, M fall II 2 post no scalp lac- odontoid screw/ stable routine activity eration halo fusion 13 71, M MVA II 10 post cent no trans screws w/ NA routine activity cord synd 20 70, M MVA II, C-1, 10 post no none trans screws w/ stable routine activity C6 7 Gallie BG fusion lami- (no wiring)/ nae, Minerva T-5 comp * trans = transarticular. days for patients who were initially treated surgically. The average follow-up period in the surgical group was 17 months. Surgical treatment consisted of posterior C1 2 transarticular screw fixation with a modified Gallie fusion in nine patients and anterior odontoid screw fixation in two patients. The patients treated primarily with surgery and those treated surgically after failure of nonsurgical treatment were similar with respect to age, sex, mechanism of injury, type of spine fracture, SCI, associated nonspinal injuries, and follow-up period. The mean initial odontoid displacement in patients primarily treated with surgery was 7.5 mm, whereas the mean initial odontoid displacement in patients in whom nonsurgical treatment failed and who required surgical intervention was 5.6 mm. Surgical treatment failed early in one patient and was associated with a complication in one patient. The surgical early failure occurred in an 84-year-old man who died of cardiopulmonary failure in the early postoperative period. The complication occurred in a 66-year-old man with an associated C-1 fracture and SCI who required revision of the posterior C1 2 transarticular screw fixation and placement in a halo-thoracic brace postoperatively. Of the nine patients treated with posterior C1 2 transarticular screw fixation with a modified Gallie fusion, eight were managed postoperatively with either a Philadelphia collar or a collar for an average of 4 to 6 weeks. Halo-thoracic vest immobilization had failed in both patients treated with anterior odontoid screw fixation because of excessive movement at the fracture site; postoperatively both patients were maintained in the halo-thoracic vest because of poor odontoid screw fixation in osteoporotic bone. The anterior odontoid screw succeeded in providing internal fixation and prevented further odon- 4 Neurosurg. Focus / Volume 8 / June, 2000
5 Type II odontoid fractures in the elderly Fig. 1. Radiographs of the cervical spine obtained in a 71-year-old man involved in a motor vehicle accident who sustained a Type II odontoid fracture and an incomplete SCI. A: A supine lateral radiograph revealing near anatomical alignment of the odontoid fracture in a halo-thoracic vest. B: An upright lateral radiograph revealing posterior displacement of the odontoid in the halo-thoracic vest. C: Despite attempted nonsurgical management, the odontoid fracture was not adequately immobilized in the halo-thoracic vest, and the patient required posterior C1 2 transarticular screw fixation with modified Gallie fusion. toid movement at the fracture site but did not obviate the need for postoperative halo-thoracic vest immobilization. Of the 10 patients discharged from the hospital after surgical treatment, eight returned to routine activity with no late neurological deterioration; one patient was doing well at the time of discharge but there was no long-term follow-up data available; and one patient remained a Frankel Grade A ventilator-dependent quadriplegic at 3- month follow-up examination. A stable bone fusion was achieved in all eight patients with available radiological follow-up data. DISCUSSION Treatment of odontoid fractures in the elderly can be difficult and is often associated with significant morbidity and mortality rates. 1,3,4,7, 9 12 Pepin, et al., 11 reported on 41 patients with odontoid fractures, 19 of whom were aged 60 years or older. Halo-thoracic vest immobilization was attempted in four patients older than 60 years; in three the halo-thoracic vest failed, leading to death in one patient and requiring removal of the orthosis in the other two. The authors concluded that a more conservative approach would be beneficial in the elderly. Hanigan, et al., 7 reported on 19 patients aged 80 years or older with odontoid fractures. Five (26%) of the 19 patients died during hospitalization. All five deaths were associated with bed rest and nonsurgical management in a cervical collar. Of two patients treated in a halo-thoracic vest one required removal of the halo secondary to respiratory compromise. None of the five patients surgically treated died, and there was no evidence of late neurological deterioration in patients who developed a stable nonunion. The authors concluded that prolonged bed rest and rigid immobilization Neurosurg. Focus / Volume 8 / June, 2000 were associated with significant morbidity and mortality rates, whereas treatment in a Philadelphia collar with formation of a stable fibrous union may be sufficient in the elderly. Ryan, et al., 12 reported on 30 patients aged 60 years or older with Type II odontoid fractures. Only one patient underwent primary spinal fusion with the remaining treatments ranging from nothing to a halocast. In this geriatric population there was a 77% nonunion rate but no evidence of late neurological deterioration on follow-up evaluation. Bednar, et al., 4 reported a 46% in-hospital mortality rate in 33 consecutive elderly patients with Type II odontoid fractures who were managed nonsurgically and no in-hospital deaths in 11 consecutive patients who were treated surgically. The authors concluded that an aggressive primary surgical management protocol can significantly decrease in-hospital mortality. The authors of three recent series on surgically treated elderly patients with odontoid fractures have reported surgical mortality rates from 0 to 57%. 5,6,10 The current study represents a retrospective review of patients aged 65 years or older with Type II odontoid fractures who were consecutively admitted to a single medical center over a 5-year period. Consistent with previous investigations, low-energy falls accounted for the majority of the fractures, posterior displacement of the odontoid predominated, SCI was associated with posterior displacement of the odontoid, and associated in-hospital deaths were high at 20%. 4,7,9,11,12 Initial treatment was chosen based on the anatomy of the fracture and the medical frailty of the patient, combined with the wishes of the patient and family. The mean initial odontoid displacement was greatest (7.5 mm) in those patients treated primarily with surgery and least in those patients who completed a course of treatment in a cervical orthosis (3.3 mm). 5
6 C. Kuntz IV, et al. In 14 (70%) of 20 patients the primary treatment was nonsurgical. The nonsurgical treatment consisted of an external cervical orthosis, which was a halo-thoracic vest, Minerva brace, or collar. The goal of treatment with the cervical orthosis was stabilization of the odontoid fracture and early mobilization of the patient. Of the 12 patients treated in a cervical orthosis six were treatment failures. All of the treatment failures and complications were in patients treated in either a halo-thoracic vest or Minerva brace. Treatment failed in six of 10 patients treated with either a halo-thoracic vest or Minerva brace. The failure of these cervical orthoses in which a a thoracic vest was used was secondary to either restricted mobility producing respiratory compromise and failure to thrive or inadequate stabilization of the fracture. Lind, et al., 8 published data suggesting that there might be decreased ventilatory capacity in patients wearing halo-thoracic orthoses, and Anderson, et al., 2 documented movement of the cervical spine in the halo-thoracic vest after cervical spine injury. A possible explanation for the high failure rate of cervical orthoses in which a thoracic vest is used in the elderly is that the decreased respiratory reserve in the geriatric population is significantly further compromised by the thoracic vest, leading to morbidity and death. The decreased respiratory reserve in the elderly may also limit a tight fit between the vest and the thorax, resulting in inadequate external immobilization. A true evaluation of the less restrictive collar is not possible in this study because of the small number of patients treated with this cervical orthosis. The goal of surgical treatment of Type II odontoid fractures is internal fixation and ultimately fusion of the fracture or bone graft. Although both anterior odontoid screw fixation and posterior C1 2 transarticular screw fixation with modified Gallie fusion achieved these goals in this population, the two patients treated with anterior odontoid screws were maintained in a halo-thoracic vest postoperatively because of poor odontoid screw fixation in osteoporotic bone. Because halo-thoracic vest immobilization has been associated with increased morbidity and death in the geriatric population in multiple studies (including this study), the posterior C1 2 transarticular screw fixation with modified Gallie fusion was a superior procedure, providing better internal fixation and allowing for earlier mobilization in a less restrictive brace. The morbidity and mortality rates for the nonsurgical and surgical groups were similar; however, there was a higher rate of failure in the nonsurgical group. For those patients completing nonsurgical and surgical management, the clinical outcomes were similar, but the surgical group had a higher rate of stable fusion based on followup radiographic evaluation. The long-term outcome of a stable nonunion in the geriatric population may be adequate and needs to be further studied. CONCLUSIONS Type II odontoid fractures in this elderly population were associated with an in-hospital rates of 10% morbidity and 20% mortality. Nonsurgical treatment with a halothoracic vest or Minerva brace resulted in a 60% early failure rate (six of 10 patients) with 10% morbidity and 10% mortality rates, whereas surgical treatment was well tolerated, resulting in a 9% early failure rate (one of 11 patients) with 9% morbidity and 9% mortality rates. Posterior C1 2 transarticular screw fixation with modified Gallie fusion provided superior internal fixation and avoided the need for postoperative halo-thoracic vest or Minerva brace immobilization when the Type II odontoid fracture was not associated with other spinal fractures. Further study needs to be undertaken to investigate the role of less restrictive cervical orthoses and surgical intervention in the long-term outcome of Type II odontoid fractures in the geriatric population. References 1. Anderson LD, D Alonzo RT: Fractures of the odontoid process of the axis. J Bone Joint Surg (Am) 56: , Anderson PA, Budorick TE, Easton KB, et al: Failure of halo vest to prevent in vivo motion in patients with injured cervical spines. Spine 16 (Suppl 10):S501 S505, Apuzzo MLJ, Heiden JS, Weiss MH, et al: Acute fractures of the odontoid process. An analysis of 45 cases. J Neurosurg 48: 85 91, Bednar DA, Parikh J, Hummel J: Management of type II odontoid process fractures in geriatric patients; a prospective study of sequential cohorts with attention to survivorship. J Spinal Disord 8: , Berlemann U, Schwarzenbach O: Dens fractures in the elderly. Results of anterior screw fixation in 19 elderly patients. Acta Orthop Scand 68: , Campanelli M, Kattner KA, Stroink A, et al: Posterior C1-C2 transarticular screw fixation in the treatment of displaced type II odontoid fractures in the geriatric population review of seven cases. Surg Neurol 51: , Hanigan WC, Powell FC, Elwood PW, et al: Odontoid fractures in elderly patients. J Neurosurg 78:32 35, Lind B, Bake B, Lundqvist C, et al: Influence of halo vest treatment on vital capacity. Spine 12: , Marchesi DG: Management of odontoid fractures. Orthopedics 20: , Muller EJ, Wick M, Russe O, et al: Management of odontoid fractures in the elderly. Eur Spine J 8: , Pepin JW, Bourne RB, Hawkins RJ: Odontoid fractures, with special reference to the elderly patient. Clin Orthop (193): , Ryan MD, Taylor TKF: Odontoid fractures in the elderly. J Spinal Disord 6: , 1993 Manuscript received April 24, Accepted in final form May 25, Address reprint requests to: Charles Kuntz, IV, M.D., Department of Neurological Surgery, University of Cincinnati, Mayfield Clinic and Spine Institute, 231 Bethesda Avenue, Cincinnati, Ohio Neurosurg. Focus / Volume 8 / June, 2000
CERVICAL SPINE INJURIES IN THE ELDERLY
 CERVICAL SPINE INJURIES IN THE ELDERLY ISADOR H. LIEBERMAN, JOHN K. WEBB From University Hospital, Queen s Medical Centre, Nottingham, England We reviewed 41 patients over the age of 65 years (mean 76.5)
CERVICAL SPINE INJURIES IN THE ELDERLY ISADOR H. LIEBERMAN, JOHN K. WEBB From University Hospital, Queen s Medical Centre, Nottingham, England We reviewed 41 patients over the age of 65 years (mean 76.5)
Geriatric Odontoid Fractures
 Geriatric Odontoid Fractures M A R K E S K E N A Z I, M. D. S P I N E I N S T I T U T E O F S O U T H F L O R I D A A F F I L I A T E A S S I S T A N T P R O F E S S O R O F C L I N I C A L B I O M E D
Geriatric Odontoid Fractures M A R K E S K E N A Z I, M. D. S P I N E I N S T I T U T E O F S O U T H F L O R I D A A F F I L I A T E A S S I S T A N T P R O F E S S O R O F C L I N I C A L B I O M E D
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Kanji Mori, Kazuya Nishizawa, Akira Nakamura, and Shinji Imai. 1. Introduction. 2. Case Presentation
 Case Reports in Orthopedics Volume 2015, Article ID 301858, 4 pages http://dx.doi.org/10.1155/2015/301858 Case Report Atraumatic Occult Odontoid Fracture in Patients with Osteoporosis-Associated Thoracic
Case Reports in Orthopedics Volume 2015, Article ID 301858, 4 pages http://dx.doi.org/10.1155/2015/301858 Case Report Atraumatic Occult Odontoid Fracture in Patients with Osteoporosis-Associated Thoracic
Prognosis of Odontoid Fractures
 Acta Orthopaedica Scandinavica ISSN: 0001-6470 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iort19 Prognosis of Odontoid Fractures Alan Roberts & Jack Wickstrom To cite this article:
Acta Orthopaedica Scandinavica ISSN: 0001-6470 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iort19 Prognosis of Odontoid Fractures Alan Roberts & Jack Wickstrom To cite this article:
Odontoid Fractures and Other Cervical Trauma: Geriatric Considerations
 Odontoid Fractures and Other Cervical Trauma: Geriatric Considerations Vishal Khatri, MD Division of Spine Surgery Department of Orthopaedic Surgery Cooper Bone and Joint Institute Cooper University Health
Odontoid Fractures and Other Cervical Trauma: Geriatric Considerations Vishal Khatri, MD Division of Spine Surgery Department of Orthopaedic Surgery Cooper Bone and Joint Institute Cooper University Health
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
 Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
Case Report Traumatic Death due to Simultaneous Double Spine Fractures in Patient with Ankylosing Spondylitis
 Case Reports in Orthopedics Volume 2015, Article ID 590935, 4 pages http://dx.doi.org/10.1155/2015/590935 Case Report Traumatic Death due to Simultaneous Double Spine Fractures in Patient with Ankylosing
Case Reports in Orthopedics Volume 2015, Article ID 590935, 4 pages http://dx.doi.org/10.1155/2015/590935 Case Report Traumatic Death due to Simultaneous Double Spine Fractures in Patient with Ankylosing
Pediatric cervical spine injuries with neurological deficits, treatment options, and potential for recovery
 SICOT J 2017, 3, 53 Ó The Authors, published by EDP Sciences, 2017 DOI: 10.1051/sicotj/2017035 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Pediatric cervical spine injuries with neurological
SICOT J 2017, 3, 53 Ó The Authors, published by EDP Sciences, 2017 DOI: 10.1051/sicotj/2017035 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Pediatric cervical spine injuries with neurological
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
ISPUB.COM. Fracture Through the Body of the Axis. B Johnson, N Jayasekera CASE REPORT
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 B Johnson, N Jayasekera Citation B Johnson, N Jayasekera.. The Internet Journal of Orthopedic Surgery. 2007 Volume 8 Number 1. Abstract
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 B Johnson, N Jayasekera Citation B Johnson, N Jayasekera.. The Internet Journal of Orthopedic Surgery. 2007 Volume 8 Number 1. Abstract
Posterior cervical fusion in children
 Posterior cervical fusion in children JOE M. MCWHORTER, M.D., EBEN ALEXANDER, JR., M.D., COURTLAND H. DAVIS, JR., M.D., AND DAVID L. KELLY, JR., M.D. Section on Neurosurgery, Department of Surgery, Bowman
Posterior cervical fusion in children JOE M. MCWHORTER, M.D., EBEN ALEXANDER, JR., M.D., COURTLAND H. DAVIS, JR., M.D., AND DAVID L. KELLY, JR., M.D. Section on Neurosurgery, Department of Surgery, Bowman
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Odontoid process fracture in 2 year old child: a rare case report
 Romanian Neurosurgery Volume XXXI Number 4 2017 October-December Article Odontoid process fracture in 2 year old child: a rare case report Prajapati Hanuman Prasad, Singh Deepak Kumar, Singh Rakesh Kumar,
Romanian Neurosurgery Volume XXXI Number 4 2017 October-December Article Odontoid process fracture in 2 year old child: a rare case report Prajapati Hanuman Prasad, Singh Deepak Kumar, Singh Rakesh Kumar,
Spinal Cord Injury. North American Spine Society Public Education Series
 Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Pediatric multilevel spine injuries: an institutional experience
 Childs Nerv Syst (2011) 27:1095 1100 DOI 10.1007/s00381-010-1348-y ORIGINAL PAPER Pediatric multilevel spine injuries: an institutional experience Martin M. Mortazavi & Seref Dogan & Erdinc Civelek & R.
Childs Nerv Syst (2011) 27:1095 1100 DOI 10.1007/s00381-010-1348-y ORIGINAL PAPER Pediatric multilevel spine injuries: an institutional experience Martin M. Mortazavi & Seref Dogan & Erdinc Civelek & R.
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Case Report A Case of Delayed Myelopathy Caused by Atlantoaxial Subluxation without Fracture
 Case Reports in Orthopedics Volume 2013, Article ID 421087, 4 pages http://dx.doi.org/10.1155/2013/421087 Case Report A Case of Delayed Myelopathy Caused by Atlantoaxial Subluxation without Fracture Ryo
Case Reports in Orthopedics Volume 2013, Article ID 421087, 4 pages http://dx.doi.org/10.1155/2013/421087 Case Report A Case of Delayed Myelopathy Caused by Atlantoaxial Subluxation without Fracture Ryo
Subaxial Cervical Spine Trauma
 Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Original Article Management of combination fractures of the atlas and axis: a report of four cases and literature review
 Int J Clin Exp Med 2014;7(8):2074-2080 www.ijcem.com /ISSN:1940-5901/IJCEM0001212 Original Article Management of combination fractures of the atlas and axis: a report of four cases and literature review
Int J Clin Exp Med 2014;7(8):2074-2080 www.ijcem.com /ISSN:1940-5901/IJCEM0001212 Original Article Management of combination fractures of the atlas and axis: a report of four cases and literature review
A New Orthosis for Fixation of the Cervical Spine Fronto- Occipito-Zygomatic Orthosis
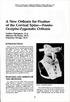 A New Orthosis for Fixation of the Cervical Spine Fronto- Occipito-Zygomatic Orthosis Toshiro Nakamura, O.A. Mitsuru Oh-Hama, M.D. Hikosuke Shingu, M.D. INTRODUCTION Most of the cervical orthoses for longterm
A New Orthosis for Fixation of the Cervical Spine Fronto- Occipito-Zygomatic Orthosis Toshiro Nakamura, O.A. Mitsuru Oh-Hama, M.D. Hikosuke Shingu, M.D. INTRODUCTION Most of the cervical orthoses for longterm
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Surgical management of combined fracture of atlas associated with fracture of axis vertebrae (CAAF): Case Series
 Romanian Neurosurgery (2015) XXIX 3: 335-341 335 Surgical management of combined fracture of atlas associated with fracture of axis vertebrae (CAAF): Case Series Guru Dutta Satyarthee, Gaurang Vaghani,
Romanian Neurosurgery (2015) XXIX 3: 335-341 335 Surgical management of combined fracture of atlas associated with fracture of axis vertebrae (CAAF): Case Series Guru Dutta Satyarthee, Gaurang Vaghani,
C2 Body Fracture: Report of Cases Managed Conservatively by Philadelphia Collar
 C2 Body Fracture: Report of Cases Managed Conservatively by Philadelphia Collar The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
C2 Body Fracture: Report of Cases Managed Conservatively by Philadelphia Collar The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
Atlas and axis injuries role of Halovest
 International Journal of Health Sciences, Qassim University, Vol. 8, No. 4 (Oct-Dec 2014) Dr. Younis Kamal, MS Ortho 1, 2 Senior Resident, Postgraduate Department of Orthopaedics GMC SRINAGAR Email kdryounis@gmail.com
International Journal of Health Sciences, Qassim University, Vol. 8, No. 4 (Oct-Dec 2014) Dr. Younis Kamal, MS Ortho 1, 2 Senior Resident, Postgraduate Department of Orthopaedics GMC SRINAGAR Email kdryounis@gmail.com
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
2 nd Annual Spine Trauma Summit May 20-21, 2016 at the Seattle Science Foundation AGENDA. Friday, May 20, 2016
 2 nd Annual Spine Trauma Summit May 20-21, 2016 at the Seattle Science Foundation AGENDA Friday, May 20, 2016 6:00pm 6:30pm 9:00pm Buffet Dinner Served (not accredited) Case Reviews and Discussions All
2 nd Annual Spine Trauma Summit May 20-21, 2016 at the Seattle Science Foundation AGENDA Friday, May 20, 2016 6:00pm 6:30pm 9:00pm Buffet Dinner Served (not accredited) Case Reviews and Discussions All
Introduction. Objectives C-Spine: Where Are We Now? NAEMSP Medical Director Course 1/9/2013
 NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of direct C1 lateral mass screw procedure for cervical spine stabilisation Introduction
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of direct C1 lateral mass screw procedure for cervical spine stabilisation Introduction
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/08/2012 Radiology Quiz of the Week # 102 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation *
 Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Competence of the Deltoid Ligament in Bimalleolar Ankle Fractures After Medial Malleolar Fixation * BY PAUL TORNETTA, III, M.D. Investigation performed at Kings County Hospital, New York, N.Y. Abstract
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Treatment of odontoid fractures: A clinical challenge and reality
 National Journal of Clinical Orthopaedics 2017; 1(2): 10-15 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(2): 10-15 Received: 03-05-2017 Accepted: 04-06-2017
National Journal of Clinical Orthopaedics 2017; 1(2): 10-15 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(2): 10-15 Received: 03-05-2017 Accepted: 04-06-2017
FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE?
 FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE? Original Article Orthopaedics R S Bajoria 1, Mahendra Panwar 2, Anand Rao 3, Sameer Gupta 4 1 - Associate
FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE? Original Article Orthopaedics R S Bajoria 1, Mahendra Panwar 2, Anand Rao 3, Sameer Gupta 4 1 - Associate
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Posterior Cervical Fusion procedures. Patient Guide to Neck Surgery Posterior Cervical Fusion NexPosure NexPosure MIS Access provides
The following is a sampling of products offered by Zimmer Spine for use in Posterior Cervical Fusion procedures. Patient Guide to Neck Surgery Posterior Cervical Fusion NexPosure NexPosure MIS Access provides
Deterioration following spinal cord injury
 J Neurosurg 66:400-404,1987 Deterioration following spinal cord injury A multicenter study LAWRENCE F. MARSHALL, M.D., SHAREN KNOWLTON, R.N., STEVEN R. GARFIN, M.D., MELVILLE R. KLAUBER, PH.D., HOWARD
J Neurosurg 66:400-404,1987 Deterioration following spinal cord injury A multicenter study LAWRENCE F. MARSHALL, M.D., SHAREN KNOWLTON, R.N., STEVEN R. GARFIN, M.D., MELVILLE R. KLAUBER, PH.D., HOWARD
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3
 OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
PARAPLEGIA. B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture.
 16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series
 Article ID: WMC005027 ISSN 2046-1690 Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series Peer review status: No Corresponding Author: Dr. Mohit K Jindal, Senior Resident,
Article ID: WMC005027 ISSN 2046-1690 Crossed Steinmann Pin Fixation In Supracondylar Femur Fractures In Adults A Case Series Peer review status: No Corresponding Author: Dr. Mohit K Jindal, Senior Resident,
Traumatic spondylolisthesis of the axis has been
 Bulletin Hospital for Joint Diseases Volume 60, Number 2 2001-2002 61 Traumatic Spondylolisthesis of the Axis 42 Cases Myung-Sang Moon MD Jeong-Lim Moon MD Young-Wan Moon MD Doo-Hoon Sun MD PhD and Won-Tai
Bulletin Hospital for Joint Diseases Volume 60, Number 2 2001-2002 61 Traumatic Spondylolisthesis of the Axis 42 Cases Myung-Sang Moon MD Jeong-Lim Moon MD Young-Wan Moon MD Doo-Hoon Sun MD PhD and Won-Tai
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Fractures and dislocations around elbow in adult
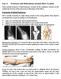 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CASE REPORT. Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report
 Nagoya J. Med. Sci. 79. 551 ~ 557, 2017 doi:10.18999/nagjms.79.4.551 CASE REPORT Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report Takaaki Shinohara 1
Nagoya J. Med. Sci. 79. 551 ~ 557, 2017 doi:10.18999/nagjms.79.4.551 CASE REPORT Distal radius nonunion after volar locking plate fixation of a distal radius fracture: a case report Takaaki Shinohara 1
COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF EXTERNAL AND INTERNAL FIXATION IN TREATMENT OF COMMINUTED DISTAL RADIUS FRACTURES
 COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF EXTERNAL AND INTERNAL FIXATION IN TREATMENT OF COMMINUTED DISTAL RADIUS FRACTURES R. Sahaya Jose 1 1Assistant Professor, Department of Orthopaedics, Sree Mookambika
COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF EXTERNAL AND INTERNAL FIXATION IN TREATMENT OF COMMINUTED DISTAL RADIUS FRACTURES R. Sahaya Jose 1 1Assistant Professor, Department of Orthopaedics, Sree Mookambika
Management of cervical spinal cord injury in ankylosing spondylitis: the intervertebral disc as a cause of cord compression
 J Neurosurg 77:241-246, 1992 Management of cervical spinal cord injury in ankylosing spondylitis: the intervertebral disc as a cause of cord compression DAVID W. ROWED, M.D., F.R.C.S.(C) Division of Neurosurgery,
J Neurosurg 77:241-246, 1992 Management of cervical spinal cord injury in ankylosing spondylitis: the intervertebral disc as a cause of cord compression DAVID W. ROWED, M.D., F.R.C.S.(C) Division of Neurosurgery,
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director
 Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Original Article Efficacy and safety of different treatments for Grauer type II odontoid fractures: a preliminary study
 Int J Clin Exp Med 2016;9(5):8145-8152 www.ijcem.com /ISSN:1940-5901/IJCEM0020836 Original Article Efficacy and safety of different treatments for Grauer type II odontoid fractures: a preliminary study
Int J Clin Exp Med 2016;9(5):8145-8152 www.ijcem.com /ISSN:1940-5901/IJCEM0020836 Original Article Efficacy and safety of different treatments for Grauer type II odontoid fractures: a preliminary study
Traumatic thoracic spinal fracture dislocation with minimal or no cord injury
 J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
J Neurosurg (Spine 3) 96:333 337, 2002 Traumatic thoracic spinal fracture dislocation with minimal or no cord injury Report of four cases and review of the literature SCOTT SHAPIRO M.D., TODD ABEL, M.D.,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit
 Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
Long Posterior Fixation with Short Fusion for the Treatment of TB Spondylitis of the Thoracic and Lumbar Spine with or without Neurologic Deficit Shih-Tien Wang MD, Chien-Lin Liu MD 王世典劉建麟 School of Medicine,
subluxation: a radiographic comparison
 Annals of the Rheumatic Diseases, 1980, 39, 485-489 Cervical collars in rheumatoid atlanto-axial subluxation: a radiographic comparison BO ALTHOFF AND IAN F. GOLDIE From the Department of Orthopaedic Surgery
Annals of the Rheumatic Diseases, 1980, 39, 485-489 Cervical collars in rheumatoid atlanto-axial subluxation: a radiographic comparison BO ALTHOFF AND IAN F. GOLDIE From the Department of Orthopaedic Surgery
Journal of Rehabilitation Sciences and Research. Evaluation of the Efficiency of Minerva Collar on Cervical Spine Motions
 JRSR 2 (2017) 47-52 Journal of Rehabilitation Sciences and Research Journal Home Page: jrsr.sums.ac.ir Original Article Evaluation of the Efficiency of Minerva Collar on Cervical Spine Motions Mohammad
JRSR 2 (2017) 47-52 Journal of Rehabilitation Sciences and Research Journal Home Page: jrsr.sums.ac.ir Original Article Evaluation of the Efficiency of Minerva Collar on Cervical Spine Motions Mohammad
E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus
 Shoulder & Elbow. ISSN 1758-5732 E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus Alexander A. Weening, Kim M. Brouwer, Margaritha Adams & David Ring Orthopaedic Hand
Shoulder & Elbow. ISSN 1758-5732 E ORIGINAL ARTICLE Low extra-articular (transcondylar) fractures of the distal humerus Alexander A. Weening, Kim M. Brouwer, Margaritha Adams & David Ring Orthopaedic Hand
5/31/2018. Ipsilateral Femoral Neck And Shaft Fractures. Ipsilateral Neck-Shaft Fractures Introduction. Ipsilateral Neck-Shaft Fractures Introduction
 Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Management of severe cervical kyphosis in a patient with Larsen syndrome
 J Neurosurg Pediatrics 1:320 324, 2008 Management of severe cervical kyphosis in a patient with Larsen syndrome Case report MARCI MADERA, M.D., 1 ALVIN CRAWFORD, M.D., 2 AND FRANCESCO T. MANGANO, D.O.
J Neurosurg Pediatrics 1:320 324, 2008 Management of severe cervical kyphosis in a patient with Larsen syndrome Case report MARCI MADERA, M.D., 1 ALVIN CRAWFORD, M.D., 2 AND FRANCESCO T. MANGANO, D.O.
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Correspondence to: Bharat Sutariya DOI: /ijmsph Received Date: Accepted Date:
 RESEARCH ARTICLE COMPARISON OF FUNCTIONAL AND NEUROLOGICAL OUTCOME OF CONSERVATIVE AND OPERATIVE MANAGEMENT IN PATIENTS WITH CERVICAL SPINE INJURY WITH COMPLETE QUADRIPLEGIA Amit Patel, Bharat Sutariya
RESEARCH ARTICLE COMPARISON OF FUNCTIONAL AND NEUROLOGICAL OUTCOME OF CONSERVATIVE AND OPERATIVE MANAGEMENT IN PATIENTS WITH CERVICAL SPINE INJURY WITH COMPLETE QUADRIPLEGIA Amit Patel, Bharat Sutariya
Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture
 779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis
 Acta Orthop Scand 1988;59(4):425-429 Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis 03 17878 1 luli lrl Herman H. de Boer', Abraham J. Verbout', Hans K. L. Nielsen2 and
Acta Orthop Scand 1988;59(4):425-429 Free vascularized fibular graft for tibial pseudarthrosis in neurofibromatosis 03 17878 1 luli lrl Herman H. de Boer', Abraham J. Verbout', Hans K. L. Nielsen2 and
Imaging of Orthopedic Spinal Devices: What Every Radiologist Should Know.
 Imaging of Orthopedic Spinal Devices: What Every Radiologist Should Know. Poster No.: C-1656 Congress: ECR 2016 Type: Educational Exhibit Authors: E. Federici, C. Dell'atti, M. Bartocci, D. Beomonte Zobel,
Imaging of Orthopedic Spinal Devices: What Every Radiologist Should Know. Poster No.: C-1656 Congress: ECR 2016 Type: Educational Exhibit Authors: E. Federici, C. Dell'atti, M. Bartocci, D. Beomonte Zobel,
Treatment of thoracolumbar burst fractures by vertebral shortening
 Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
Eur Spine J (2002) 11 :8 12 DOI 10.1007/s005860000214 TECHNICAL INNOVATION Alejandro Reyes-Sanchez Luis M. Rosales Victor P. Miramontes Dario E. Garin Treatment of thoracolumbar burst fractures by vertebral
The craniocervical junction
 Anver Jameel, MD The craniocervical junction A biomechanical and anatomical unit that extends from the skull base to C2 Includes the clivus, foramen magnum and contiguous occipital bone, the occipital
Anver Jameel, MD The craniocervical junction A biomechanical and anatomical unit that extends from the skull base to C2 Includes the clivus, foramen magnum and contiguous occipital bone, the occipital
Imaging of Cervical Spine Trauma
 Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
MAY 2006 The Surgical Technologist
 Overview of cervical spine injuries Cervical spine injuries comprise approximately 10,000 new spinal cord injuries annually. Approximately 80% of the injured individuals are male and less than 40 years
Overview of cervical spine injuries Cervical spine injuries comprise approximately 10,000 new spinal cord injuries annually. Approximately 80% of the injured individuals are male and less than 40 years
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Direct anterior screw fixation for recent and remote odontoid fractures
 Neurosurg Focus 8 (6):Article 2, [JNS:Spine Preview, October 2000], Click here to return to Table of Contents Direct anterior screw fixation for recent and remote odontoid fractures RONALD I. APFELBAUM,
Neurosurg Focus 8 (6):Article 2, [JNS:Spine Preview, October 2000], Click here to return to Table of Contents Direct anterior screw fixation for recent and remote odontoid fractures RONALD I. APFELBAUM,
Case Report Pediatric Transepiphyseal Seperation and Dislocation of the Femoral Head
 Case Reports in Orthopedics Volume 2013, Article ID 703850, 4 pages http://dx.doi.org/10.1155/2013/703850 Case Report Pediatric Transepiphyseal Seperation and Dislocation of the Femoral Head Mehmet Elmadag,
Case Reports in Orthopedics Volume 2013, Article ID 703850, 4 pages http://dx.doi.org/10.1155/2013/703850 Case Report Pediatric Transepiphyseal Seperation and Dislocation of the Femoral Head Mehmet Elmadag,
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
The treatment of combination atlas-axis fractures
 CHAPTER 13 TOPIC CHAPTER 13 Timothy C. Ryken, MD, MS* Mark N. Hadley, MD Bizhan Aarabi, MD, FRCSC Sanjay S. Dhall, MD Daniel E. Gelb, MDk R. John Hurlbert, MD, PhD, FRCSC# Curtis J. Rozzelle, MD** Nicholas
CHAPTER 13 TOPIC CHAPTER 13 Timothy C. Ryken, MD, MS* Mark N. Hadley, MD Bizhan Aarabi, MD, FRCSC Sanjay S. Dhall, MD Daniel E. Gelb, MDk R. John Hurlbert, MD, PhD, FRCSC# Curtis J. Rozzelle, MD** Nicholas
No greater tragedy can befall on a young adult in this most
 SUPPLEMENT TO JAPI may 2012 VOL. 60 19 Operative Management of Spinal Injuries Sajan Hegde * Introduction No greater tragedy can befall on a young adult in this most active period of life than a spinal
SUPPLEMENT TO JAPI may 2012 VOL. 60 19 Operative Management of Spinal Injuries Sajan Hegde * Introduction No greater tragedy can befall on a young adult in this most active period of life than a spinal
Shoulder Trauma (Fractures and Dislocations)
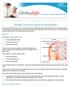 Shoulder Trauma (Fractures and Dislocations) Trauma to the shoulder is common. Injuries range from a separated shoulder resulting from a fall onto the shoulder to a high-speed car accident that fractures
Shoulder Trauma (Fractures and Dislocations) Trauma to the shoulder is common. Injuries range from a separated shoulder resulting from a fall onto the shoulder to a high-speed car accident that fractures
A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of The Tibia
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
PRONATION-ABDUCTION FRACTURES
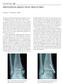 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
Spinal Trauma at the Pediatric Age
 Spinal Trauma at the Pediatric Age Burçak B LG NER Nejat AKALAN ABSTRACT Spinal trauma is relatively rare in pediatric patients. The anatomy and biomechanics of the growing spine produce failure patterns
Spinal Trauma at the Pediatric Age Burçak B LG NER Nejat AKALAN ABSTRACT Spinal trauma is relatively rare in pediatric patients. The anatomy and biomechanics of the growing spine produce failure patterns
Development of a Novel Biofedelic Skull-Neck- Thorax Model Capable of Quantifying Motions of aged Cervical Spine
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 11-23-2009 Development of a Novel Biofedelic Skull-Neck- Thorax Model
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 11-23-2009 Development of a Novel Biofedelic Skull-Neck- Thorax Model
Adult Spinal Deformity Robert Hart. Dept. Orthopaedics and Rehab OHSU
 Adult Spinal Deformity 2010 Robert Hart Dept. Orthopaedics and Rehab OHSU What is Adult Spinal Deformity? Untreated Idiopathic Scoliosis Flat Back Syndrome Adjacent Segment Stenosis Non-Union Degenerative
Adult Spinal Deformity 2010 Robert Hart Dept. Orthopaedics and Rehab OHSU What is Adult Spinal Deformity? Untreated Idiopathic Scoliosis Flat Back Syndrome Adjacent Segment Stenosis Non-Union Degenerative
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
CORE STANDARDS STANDARDS USED IN TARN REPORTS
 CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma
 Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma a* a a a b a a b ʼ 2 ʼ August 2012 Spinal Deformity with
Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma a* a a a b a a b ʼ 2 ʼ August 2012 Spinal Deformity with
Conservative management of craniovertebral junction injuries: Still a good option
 SNI: Spine OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop University Hospital, Mineola, NY, USA Original Article Conservative management
SNI: Spine OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop University Hospital, Mineola, NY, USA Original Article Conservative management
Diabetics. Referred for management of complex pilon fracture? 5/10/2017. Pilon Fractures: Exfix as definitive treatment (DM?)
 Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Primary total hip arthroplasty after acetabular fracture using intra-acetabular bended plates
 Acta Orthop. Belg., 2017, 83, 93-97 ORIGINAL STUDY Primary total hip arthroplasty after acetabular fracture using intra-acetabular bended plates Valentinas Uvarovas, Igoris Šatkauskas, Giedrius Petryla,
Acta Orthop. Belg., 2017, 83, 93-97 ORIGINAL STUDY Primary total hip arthroplasty after acetabular fracture using intra-acetabular bended plates Valentinas Uvarovas, Igoris Šatkauskas, Giedrius Petryla,
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do?
 HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do? TRAUMA 101 2018 FRACTURE CARE FOR THE COMMUNITY ORTHOPEDIST William W. Cross III, MD Assistant Professor Division of Orthopaedic Trauma Chair, Division
HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do? TRAUMA 101 2018 FRACTURE CARE FOR THE COMMUNITY ORTHOPEDIST William W. Cross III, MD Assistant Professor Division of Orthopaedic Trauma Chair, Division
Management of Hip Fractures
 Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Pilon Fractures - OrthoInfo - AAOS. Copyright 2010 American Academy of Orthopaedic Surgeons. Pilon Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Prophylactic surgical correction of Crawford s type II anterolateral bowing of the tibia using Ilizarov s method
 Acta Orthop. Belg., 2005, 71, 577-581 ORIGINAL STUDY Prophylactic surgical correction of Crawford s type II anterolateral bowing of the tibia using Ilizarov s method Hani EL-MOWAFI, Mazen ABULSAAD, Wael
Acta Orthop. Belg., 2005, 71, 577-581 ORIGINAL STUDY Prophylactic surgical correction of Crawford s type II anterolateral bowing of the tibia using Ilizarov s method Hani EL-MOWAFI, Mazen ABULSAAD, Wael
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
