Hip Arthroscopy. An information guide
|
|
|
- Caren Craig
- 6 years ago
- Views:
Transcription
1 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Hip Arthroscopy An information guide
2 Hip Arthroscopy This is a generalised information booklet to provide you and your relatives with some basic information about the procedure and what can be expected on the day of your operation and beyond. Specific questions regarding your underlying condition should be discussed directly with your surgeon. This procedure is a relatively recent way to investigate and treat a multitude of hip conditions. It is especially useful for younger patients with chronic hip symptoms or sporting injuries. It is a minimally invasive technique or keyhole surgery which uses a fibre optic telescope to view inside the joint. Arthroscopic surgery became popular in the late 1970s and 80s, but mainly for the treatment of sports injuries of the shoulder and knee. It allows surgeons to look inside a joint to confirm a diagnosis to treat certain diseases, which may be either of the bone or soft tissues. Hip arthroscopy is less commonly performed and is more invasive than a knee arthroscopy taking longer to recover from post operatively. This is due to the anatomy of the hip and the difficulty in gaining access. However, it is still performed as a day case procedure. 2
3 Anatomy of the hip (Figures 1 & 2) The hip is a ball and socket joint which is the largest weight bearing joint in the body. The round head of the femur (thigh bone) forms the ball that fits into the socket of the acetabulum (pelvis). Both the surface of the ball and socket are covered by cartilage which is a smooth, resistant material which cushions the bone and allows for gliding movement. To reduce frictional forces, a small amount of viscous fluid stays within the joint (synovial fluid). The rim of the bony socket is lined by another type of cartilage, the labrum (Figure 2), which makes the socket deeper and providing a suction seal for the femoral head. The joint is supported by ligaments which connects the ball to the socket and to keep the hip from dislocating. On x-ray imaging an elliptical head rather than spherical one suggests a Cam lesion (Figure 1). While too much coverage by the acetabulum over the femoral head creates a Pincer lesion. 3
4 Fig.1 - Normal Hip anatomy & Cam Lesion (FAI) Fig.2 - Hip anatomy soft tissues 4
5 Indications for hip arthroscopy The majority of conditions treated are listed below, but as this type of surgery is developing at a rapid pace this list is by no means exhaustive and therefore may not necessarily include your condition. 1) Torn labrum - at present this is the main reason to perform a hip arthroscopy, as it is the indication in around 60% of cases. This is a tear in the cartilage that lines the rim of the socket. It can be the result of injury or due to simple age-related degeneration. The main symptoms associated are a sharp groin pain, giving way, or the sensation of locking or catching. Confirmation of the condition is done with magnetic resonance imaging using a contrast injection. During arthroscopy a tear can be treated by either trimming or repairing the cartilage. However not all labral tears need surgery. 2) Femoroacetabular impingement (FAI) - this condition is caused by an abnormal shape to the head/neck junction of the thigh bone, it may also be called a bump or cam lesion (Figure 1). FAI may also be caused by an abnormal socket or pincer lesion. This creates a lack of room during hip movements leading to the cartilage or bone pinching each other resulting in early joint wear. The main symptoms are pain felt in the groin and/or hip area (worst when the hip is flexed and rotated inwards). It is more common in athletic men and aggravated by activity. It may also be aggravated by long periods of being seated upright. The main investigation is computerised tomography (CT) scanning with three-dimensional reconstruction of the images. The arthroscopic treatment is to recontour the surfaces, mainly by trimming the bony bumps. In the past this condition was treated by open surgery. 5
6 3) Loose bodies - similar to when these are noted in other joints, arthroscopy may be used to remove loose bodies. These are usually fragments of cartilage or bone which are a direct result of trauma. The main symptom is a sharp pain due to the loose bodies getting trapped but they may also limit the range of movement. These are usually identifiable on plain x-ray but sometimes a CT (Computerised Tomography) or MR (Magnetic Resonance) which are more detailed scans can be ordered. Unfortunately, despite a surgeon s best efforts, some loose bodies are never found during surgery. 4) Articular cartilage injuries (osteochondral defects) - the cartilage lining either the femoral head or the acetabular socket can be torn or damaged by an injury. It is usually caused by a high impact from either a sport which involves running or jumping or trauma such as motor vehicle collision. The torn fragment can intermittently protrude into the joint which causes pain and is most symptomatic when the hip is flexed as the underlying bone is left unprotected. Before proceeding to surgery this is normally investigated with a MRI scan with contrast medium. Arthroscopic surgery tries to either re-attach the cartilage or to stimulate new cartilage growth through a variety of techniques. 5) Ligamentum teres injury - the central ligament (Figure 2) that connects the pelvis with the femoral head can be torn and become a source for hip or groin pain. Symptoms are usually due to the mechanical block it causes in the joint. Through keyhole surgery the ligament can be either trimmed or repaired. 6) Release of snapping hips - coxa sultans or snapping hips is a painful condition where one of two tendons can flick across bony prominences around the hip joint, producing the characteristic 6
7 snap sound. The noise is usually accompanied by pain of varying intensity. 7) Biopsy - arthroscopy can be used to take samples of tissue from the hip joint in a less invasive manner than if performed by open surgery. 8) Infection - when infection exists in the hip, whether it is a patient s own hip or an artificial one, an arthroscopic approach can help to drain it in a less invasive way than opening the joint in the traditional fashion. This causes less damage to the healthy tissues as well as reducing the possibility of introducing a new infective organism into the joint. 9) Abnormalities of the synovium - there are certain conditions of the joint lining such as pigmented villonodular synovitis (PVNS) or primary synovial chondromatosis, which cause thickening and can benefit from being trimmed. 10) Trochanteric Bursitis - the bursa is a pillow-like structure that protects the bony prominences (greater and lesser trochanters, Figure 1) of the proximal thigh bone. These can become inflamed and painful. Arthroscopic surgery can be used in certain cases that are resistant to more conventional and less invasive treatments. Options for treatment As with all conditions seen by orthopaedic surgeons, the first option is usually to avoid surgery, this is referred to as conservative treatment. When this approach fails or the damage identified to the hip joint during investigation is thought unlikely to improve with conservative treatment, your surgeon may suggest surgery. 7
8 Conservative treatment will usually include: (1) activity modification (which may include weight loss), (2) painkillers and/or anti-inflammatory drugs (NSAIDS), and (3) physiotherapy - your physiotherapist will determine an exercise program to treat muscle imbalances, stretch out the tendons and to strengthen the muscles and ligaments around the hip joint. In certain cases (4) a steroid injection mixed with local anaesthetic is indicated. Surgical treatment will usually be discussed after all conservative methods have been tried and symptoms have not settled or have progressed. In certain cases the aim is to restore the anatomy which will help to prevent or slow the progression of arthritis in the joint. In other cases the goal is to reduce pain and/or improve the range of movement. Outcomes from the procedure will very much depend on the type and extent of pre-existent damage in the joint. When do I need surgery Surgery is usually only discussed when symptoms are not controlled by activity modification and the other types of conservative management have been exhausted. Before the operation Once referred by your GP, an initial clinic visit will be organised. At this time your surgeon will ask you questions about your medical history, including any operations you may have had in the past. They will also want to know what medications you take and if you have any allergies. A physical examination will also be performed so it is strongly recommended that you wear light and loose clothing. An x-ray of the pelvis is likely to be performed. Changes on the x-ray may be subtle though and frequently initial x-rays can be interpreted as normal. 8
9 If further imaging is deemed necessary by your surgeon it is likely that either a CT or MR scan will be ordered on an outpatient basis at a later date. If physiotherapy has not been tried previously it may be arranged. When a decision is made for surgery and you are given a date, you will need to prepare an overnight bag to bring in with you. The night before surgery, take no food or drink from 3am (medicines and painkillers may be taken at regular times though with a small sip of water). Please remove all nail polish before coming into hospital, and if absolutely necessary light make-up only is recommended. Contact lenses, jewellery and dentures will be removed for surgery so try to avoid bringing them if possible. Please do bring your hearing aids and eyeglasses so that you are able to answer questions and read any documentation. What risks of surgery should I be aware of? As with any medical procedure, hip arthroscopy has its own risks. Complications occur globally in around 4 to 7% of patients. These effects may be temporary or, in a few cases, they may be permanent. Fortunately though, permanent complications are rare. The rate of major complications is between % (i.e. less than 1 in 172 cases) while minor complications occur more frequently. The most common temporary complication is nerve injury (2% or 1 in 50, but has been reported in one case series as being diagnosed in almost half of cases), and usually resolves over 3-6 weeks but may take up to 6 months or longer. Re-operations occur 6.3% of the time by 16 months from arthroscopy. The most common of these operations (just under half) are total hip replacements. In less than 2% of cases one of the cartilage surfaces may be damaged by the surgeon as they introduce their instruments into the hip joint. 9
10 Similar to other orthopaedic surgeries of the hip the same general risks are present which include bleeding, infection (<1:1000), damage to nerves, blood vessels or nearby structures, blood clots such as a deep vein thrombosis (DVT) or pulmonary embolism (PE) (<0.5%), and pain (often worst immediately postoperatively). More specific risks of hip arthroscopy include the chance of experiencing recurrent/ongoing pain or symptoms, stiffness, avascular necrosis of the femoral head (which will cause collapse of the hip joint due to interruption of the blood supply - fortunately rare) and long term it may increase the risk of needing a total hip replacement. Occasionally the postoperative recovery may be very slow (greater than 3 months). There is an additional risk from the traction used, as this may cause injuries to nerves or the skin. Most frequently this would manifest itself as bruising or numbness/altered sensation between the legs. Nerve damage can also present itself anywhere along the legs including the feet. The traction can also cause pressure sores, blistering, fracture, or impotence rarely. Sometimes it is impossible to get the instruments into the hip joint due to stiffness and the procedure has to be abandoned. On the day of surgery You will need to arrive in the early morning (i.e. 7:30 am) at the hospital to be admitted by nursing staff who will go through a preoperative checklist with you. Once there you will be asked to change into a gown, and vital signs (such as blood pressure, pulse and temperature) will be measured. 10
11 You will be seen by your surgeon to confirm your consent for surgery. They will also confirm the correct surgical site and mark it with a marker pen. You will also be seen by your anaesthetist and the type of anaesthetic discussed. In most cases you will be asleep under a general anaesthetic but sometimes this may also incorporate a nerve block as well. Once you arrive in the anaesthetic room, a further checklist will be performed and an intravenous line (cannula) will be inserted. Your hip and the surrounding region will be scrubbed and shaved if required. You will usually be anaesthetised for between 1 and 3 hours. The first step is to distract the hip with a traction apparatus attached to a special radioluscent (x-ray friendly) table. This allows access to the central part of the hip joint. Traction is applied through foam padded boots and perineal (groin) post to protect the skin (Figure 3 over the page). The joint is identified under x-ray guidance by inserting either air or a contrast medium. Small skin incisions, approximately 5-10mm, are made with the scalpel, and then the telescope is inserted (usually up to 3 incisions). Once inside, large volumes of fluid are pumped through the joint. The procedure itself will usually take between minutes, depending on the complexity of what needs to be done. 11
12 Figure 3 - Boot for traction During the procedure 3 things will be assessed/repaired: 1) the articular cartilage, 2) acetabular rim/labrum, and; 3) femoral head/neck. Further x-ray imaging may be required during the operation. 12
13 During an operation for hip impingement your surgeon will attempt to reshape the junction between head and neck of the femur using a small mechanical resection device called a burr. Any excessive portion of acetabulum will be trimmed as well. Before and after surgery your surgeon will check the range of hip movement. For labral tears, the torn edges will be smoothed using a shaver or radio-frequency (RF) emitting device that uses sound waves to remove damaged tissue. Sometimes the tear can be repaired with suture anchors in the bone. For articular cartilage injuries the damaged tissue may be removed or smoothed down with a shaver or RF device. Certain types of defects are amenable to trying to regrow the cartilage using a technique known as micro-fracture. This treatment consists of making multiple small holes in the bone which will stimulate bleeding, clotting and formation of a fibro-cartilage scar to fill the defect. A local anaesthetic or other medications may be introduced into the joint before closure to help control postoperative pain. Closure is usually performed with a few sutures and covered with simple sticky dressings. A larger bulky dressing is probably what you will see when you wake up however. Some thigh swelling will be noted postoperatively. You will wake up in the recovery room where your vital signs and pain levels will be checked regularly and stabilised, before transfer back to the ward. When back on the ward, physiotherapists will review you and try to mobilise you out of bed. When you are safe on your feet and recovered from anaesthetic you will probably be 13
14 safe for discharge, this will usually be on the same day as your surgery. Postoperative period and follow-up Depending on your operation, for the first 2-6 weeks it is likely that you will be advised to mobilise with 2 crutches. Then a single crutch can be used until your follow-up appointment in the outpatient clinic. The pain felt is variable but will usually be controlled with paracetamol +/- codeine and ibuprofen. The discomfort or pain will most commonly be felt in your groin but may also be felt in your lower back, buttock, knee or even ankle. Swelling may also be present in the groin, buttock or thigh although this usually resolves within a few days. A small area of numbness is common around the incisions and is generally not a concern to most patients. A formal wound check will be arranged at 2 weeks when the stitches will be removed and until that appointment it is recommended that you monitor your leg for any signs of early infection (i.e. redness, swelling, heat, and/or pain). It is normal for a small amount of fluid or blood to leak from the wound during the first few days. At the 6 week appointment you will meet up with your surgeon again, at this time they will go through the findings and treatments provided during your procedure. Any non-urgent questions you may have can be addressed at this time. Further appointments will vary in their timing and number. Outpatient physiotherapy will continue with a personalised rehabilitation program. They will monitor your progress and gradually advance the exercises. It is normal that low impact activities only will be advised during the first 2-3 months. The main goals for rehabilitation are to regain early range of movement and 14
15 joint stability, followed by strength and endurance. Most patients will be walking relatively pain free by the 8-12 week mark. Return to competitive sport can be attempted in 4-6 months (but may take up to a year). Activities to avoid or limit in the first 6 weeks include: prolonged standing or walking on hard surfaces, heavy lifting or squatting. Your sitting position in chairs should be altered to achieve an upright position and prevent deep flexion of the hip (i.e. more than 90 degree angle of your hip). Try sleeping on your back or on the non-operated side with a pillow between your legs. If the left hip was operated on, it is best to avoid driving a manual car during the first few weeks post procedure. Checklist of questions for your surgeon: What conditions will be treated? How long will I be in hospital? 15
16 If English is not your frst language and you need help, please contact the Ethnic Health Team on Jeżeli angielski nie jest twoim pierwszym językiem i potrzebujesz pomocy proszę skontaktować się z załogą Ethnic Health pod numerem telefonu For general enquiries please contact the Patient Advice and Liaison Service (PALS) on For enquiries regarding clinic appointments, clinical care and treatment please contact and the Switchboard Operator will put you through to the correct department / service Date of publication: November 2014 Date of review: November 2017 Ref: PI_SU_864 The Pennine Acute Hospitals NHS Trust Wood pulp sourced from sustainable forests
HIP ARTHROSCOPY. A Patient s Guide. Guidance prepared on behalf of the International Society for Hip Arthroscopy (
 HIP ARTHROSCOPY A Patient s Guide Guidance prepared on behalf of the International Society for Hip Arthroscopy (www.isha.net) Authors: Singh PJ *, O Donnell JM **, Pritchard MG ** * Nuffield Orthopaedic
HIP ARTHROSCOPY A Patient s Guide Guidance prepared on behalf of the International Society for Hip Arthroscopy (www.isha.net) Authors: Singh PJ *, O Donnell JM **, Pritchard MG ** * Nuffield Orthopaedic
Anterior Cruciate Ligament (ACL) Reconstruction. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
Arthroscopy Day Case. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Arthroscopy Day Case An information guide Arthroscopy Day Case Arthroscopy Day case Post-operative regime The post-operative rehabilitation
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Arthroscopy Day Case An information guide Arthroscopy Day Case Arthroscopy Day case Post-operative regime The post-operative rehabilitation
Welcome to the Royal Orthopaedic Hospital (ROH). For further information please visit
 Produced: Feb2012 Ref: 011/02 Author: Directorate for Large Joints Review: Feb 2014 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Hip Arthroscopy Welcome to the Royal Orthopaedic
Produced: Feb2012 Ref: 011/02 Author: Directorate for Large Joints Review: Feb 2014 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Hip Arthroscopy Welcome to the Royal Orthopaedic
Inferior Vena Cava (IVC) filter insertion. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Inferior Vena Cava (IVC) filter insertion An information guide Inferior Vena Cava (IVC) Filter Insertion Introduction This leaflet tells
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Inferior Vena Cava (IVC) filter insertion An information guide Inferior Vena Cava (IVC) Filter Insertion Introduction This leaflet tells
FAQ s: Hip Arthroscopy with Dr. Boyle
 AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
Hip arthroscopy. Anatomy The hip is functionally a ball and socket joint.
 Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Hip Arthroscopy Booklet
 Hip Arthroscopy Booklet 2. Hip Anatomy The bones that make up the hip joint are the femur (the thighbone) and the pelvis. At the top end of the femur is a ball called the femoral head. The femoral head
Hip Arthroscopy Booklet 2. Hip Anatomy The bones that make up the hip joint are the femur (the thighbone) and the pelvis. At the top end of the femur is a ball called the femoral head. The femoral head
Flexible Cystoscopy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Flexible Cystoscopy An information guide Flexible Cystoscopy What is it? This is a procedure to examine your bladder. To perform this procedure,
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Flexible Cystoscopy An information guide Flexible Cystoscopy What is it? This is a procedure to examine your bladder. To perform this procedure,
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
KNEE ARTHROSCOPY PATIENT INFORMATION SHEET
 KNEE ARTHROSCOPY PATIENT INFORMATION SHEET Introduction It has been recommended that you undergo an arthroscopy of your knee. This information sheet is designed to explain what is involved in an arthroscopy,
KNEE ARTHROSCOPY PATIENT INFORMATION SHEET Introduction It has been recommended that you undergo an arthroscopy of your knee. This information sheet is designed to explain what is involved in an arthroscopy,
Knee arthroscopy surgery
 Golden Jubilee National Hospital NHS National Waiting Times Centre Knee arthroscopy surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Arthroplasty
Golden Jubilee National Hospital NHS National Waiting Times Centre Knee arthroscopy surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Arthroplasty
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Arthroscopy. Turnberg Building Orthopaedics
 Arthroscopy Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Introduction An arthroscopy is a type of keyhole surgery used both to diagnose and treat
Arthroscopy Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Introduction An arthroscopy is a type of keyhole surgery used both to diagnose and treat
Percutaneous transhepatic cholangiogram (PTC) and biliary drainage. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Percutaneous transhepatic cholangiogram (PTC) and biliary drainage An information guide Percutaneous transhepatic cholangiogram (PTC) and
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Percutaneous transhepatic cholangiogram (PTC) and biliary drainage An information guide Percutaneous transhepatic cholangiogram (PTC) and
Argon Laser (photo coagulation) An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Argon Laser (photo coagulation) An information guide Argon Laser (photo coagulation) What is argon laser (photo coagulation)? This is a
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Argon Laser (photo coagulation) An information guide Argon Laser (photo coagulation) What is argon laser (photo coagulation)? This is a
Physiotherapy Post Head & Neck Surgery. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Physiotherapy Post Head & Neck Surgery An information guide Physiotherapy Post Head & Neck Surgery Within this leaflet you will find Post-operative
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Physiotherapy Post Head & Neck Surgery An information guide Physiotherapy Post Head & Neck Surgery Within this leaflet you will find Post-operative
Laser Peripheral Iridotomy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Laser Peripheral Iridotomy An information guide Laser Peripheral Iridotomy What is laser peripheral iridotomy? Laser peripheral iridotomy
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Laser Peripheral Iridotomy An information guide Laser Peripheral Iridotomy What is laser peripheral iridotomy? Laser peripheral iridotomy
Minor oral surgery under local anaesthetic. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Minor oral surgery under local anaesthetic An information guide Minor oral surgery under local anaesthetic Pre-operative advice Please ensure
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Minor oral surgery under local anaesthetic An information guide Minor oral surgery under local anaesthetic Pre-operative advice Please ensure
Caudal Epidural Injection. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Caudal Epidural Injection An information guide Caudal Epidural Injection If you are on blood thinning medications such as Warfarin, Nicoumalone
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Caudal Epidural Injection An information guide Caudal Epidural Injection If you are on blood thinning medications such as Warfarin, Nicoumalone
Northumbria Healthcare NHS Foundation Trust. Knee Arthroscopy. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Antenatal Exercises and Advice. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Antenatal Exercises and Advice An information guide Antenatal Exercises and Advice Key Points Pelvic floor exercises are important in pregnancy
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Antenatal Exercises and Advice An information guide Antenatal Exercises and Advice Key Points Pelvic floor exercises are important in pregnancy
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, "arthro" (joint)
Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, "arthro" (joint)
Physiotherapy after your hip arthroscopy
 Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Blood tests - what you need to know
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Blood Tests - what you need to know An information guide Blood tests - what you need to know Blood Tests Your General Practitioner (GP)
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Blood Tests - what you need to know An information guide Blood tests - what you need to know Blood Tests Your General Practitioner (GP)
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
Lumbar Sympathetic Block with Local Anaesthetic. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Lumbar Sympathetic Block with Local Anaesthetic An information guide Lumbar Sympathetic Block with Local Anaesthetic If you are on blood
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Lumbar Sympathetic Block with Local Anaesthetic An information guide Lumbar Sympathetic Block with Local Anaesthetic If you are on blood
Having a radiologically inserted gastrostomy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
WHAT IS HIP ARTHROSCOPY?
 HIP ARTHROSCOPY Information for patients WHAT IS HIP ARTHROSCOPY? Hip arthroscopy is a minimally invasive procedure. An arthroscopic camera provides a magnified image of all parts of the joint. With the
HIP ARTHROSCOPY Information for patients WHAT IS HIP ARTHROSCOPY? Hip arthroscopy is a minimally invasive procedure. An arthroscopic camera provides a magnified image of all parts of the joint. With the
Lidocaine Intravenous Infusion. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Lidocaine Intravenous Infusion An information guide Lidocaine Intravenous Infusion What is a Lidocaine Intravenous Infusion? A Lidocaine
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Lidocaine Intravenous Infusion An information guide Lidocaine Intravenous Infusion What is a Lidocaine Intravenous Infusion? A Lidocaine
( 1 ) Ball and socket. Shoulder capsule. Rotator cuff.
 Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet
 Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet Page 1 Arthroscopy of the knee joint Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. This booklet
Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet Page 1 Arthroscopy of the knee joint Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. This booklet
Radio Frequency Facet Nerve Ablation or Denervation. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Radio Frequency Facet Nerve Ablation or Denervation An information guide Radio Frequency Facet Nerve Ablation or Denervation If you are
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Radio Frequency Facet Nerve Ablation or Denervation An information guide Radio Frequency Facet Nerve Ablation or Denervation If you are
Radiological insertion of a nephrostomy and ureteric stent. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Radiological insertion of a nephrostomy and ureteric stent An information guide Radiological Insertion of Nephrostomy and Ureteric Stent
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Radiological insertion of a nephrostomy and ureteric stent An information guide Radiological Insertion of Nephrostomy and Ureteric Stent
A patient s guide to: Arthroscopy of the Hip
 A patient s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
A patient s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
Sleep Deprived EEG (SEEG) An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Sleep Deprived EEG (SEEG) An information guide Sleep Deprived EEG (SEEG) What is a sleep-deprived EEG (SEEG)? EEG stands for Electroencephalography.
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Sleep Deprived EEG (SEEG) An information guide Sleep Deprived EEG (SEEG) What is a sleep-deprived EEG (SEEG)? EEG stands for Electroencephalography.
Subacromial Impingement of Shoulder Orthopaedic Department Patient Information Leaflet
 Subacromial Impingement of Shoulder Orthopaedic Department Patient Information Leaflet Page 1 Subacromial Impingement of Shoulder About your shoulder The shoulder is a ball and socket joint formed by a
Subacromial Impingement of Shoulder Orthopaedic Department Patient Information Leaflet Page 1 Subacromial Impingement of Shoulder About your shoulder The shoulder is a ball and socket joint formed by a
What is Clexane and what is it used for?
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Clexane and what is it used for? An information guide What is Clexane and what is it used for? CLEXANE (also known as Enoxaparin)
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Clexane and what is it used for? An information guide What is Clexane and what is it used for? CLEXANE (also known as Enoxaparin)
Exercise Tolerance Test. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Exercise Tolerance Test An information guide Exercise Tolerance Test Your doctor or specialist nurse would like you to have a test called
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Exercise Tolerance Test An information guide Exercise Tolerance Test Your doctor or specialist nurse would like you to have a test called
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Small Fibre Neuropathy Tests. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Small Fibre Neuropathy Tests An information guide Small Fibre Neuropathy Tests What is Small Fibre Neuropathy? Within the nerves there are
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Small Fibre Neuropathy Tests An information guide Small Fibre Neuropathy Tests What is Small Fibre Neuropathy? Within the nerves there are
Osteoarthritis of the Hip
 Osteoarthritis of the Hip Sometimes called "wear-and-tear" arthritis, osteoarthritis is a common condition that many people develop during middle age or older. Osteoarthritis of the hip causes pain and
Osteoarthritis of the Hip Sometimes called "wear-and-tear" arthritis, osteoarthritis is a common condition that many people develop during middle age or older. Osteoarthritis of the hip causes pain and
Home Exercises for the Cardiac Rehabilitation programme. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Exercises for the Cardiac Rehabilitation programme An information guide Cardiac Rehabilitation Patient Exercises To gain a beneficial
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Exercises for the Cardiac Rehabilitation programme An information guide Cardiac Rehabilitation Patient Exercises To gain a beneficial
Home Intravenous Therapy Team - IV Cannula. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Intravenous Therapy Team - IV Cannula An information guide Home Intravenous Therapy Team - IV Cannula Home Intravenous Therapy Team
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Home Intravenous Therapy Team - IV Cannula An information guide Home Intravenous Therapy Team - IV Cannula Home Intravenous Therapy Team
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Fundus Fluorescein Angiogram (FFA) An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Fundus Fluorescein Angiogram (FFA) An information guide Fundus Fluorescein Angiogram (FFA) What is a Fundus Fluorescein Angiogram? It is
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Fundus Fluorescein Angiogram (FFA) An information guide Fundus Fluorescein Angiogram (FFA) What is a Fundus Fluorescein Angiogram? It is
Ankle Arthroscopy PATIENT INFORMATION. What is an ankle arthroscopy? Common disorders in which ankle arthroscopy is useful.
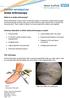 PATIENT INFORMATION Ankle Arthroscopy What is an ankle arthroscopy? Ankle arthroscopy is also known as keyhole surgery or minimally invasive ankle surgery. Ankle arthroscopy involves using very small incisions
PATIENT INFORMATION Ankle Arthroscopy What is an ankle arthroscopy? Ankle arthroscopy is also known as keyhole surgery or minimally invasive ankle surgery. Ankle arthroscopy involves using very small incisions
Having an MR Proctogram. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having an MR Proctogram An information guide Having an MR Proctogram Introduction This leaflet contains information for patients, parents
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having an MR Proctogram An information guide Having an MR Proctogram Introduction This leaflet contains information for patients, parents
The Manchester Leg Circulation Service. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION The Manchester Leg Circulation Service An information guide The Manchester Leg Circulation Service Peripheral arterial disease Peripheral
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION The Manchester Leg Circulation Service An information guide The Manchester Leg Circulation Service Peripheral arterial disease Peripheral
 The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
Gastroscopy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Gastroscopy An information guide Gastroscopy Your stay on the endoscopy unit could be up to 2 hours or more depending on individual recovery
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Gastroscopy An information guide Gastroscopy Your stay on the endoscopy unit could be up to 2 hours or more depending on individual recovery
Disorders of the Rotator Cuff and Acromio-clavicular Joint
 Disorders of the Rotator Cuff and Acromio-clavicular Joint The rotator cuff is a sheath of muscles which surrounds the shoulder joint, it helps to stabilise the shoulder and powers the wide range of movements
Disorders of the Rotator Cuff and Acromio-clavicular Joint The rotator cuff is a sheath of muscles which surrounds the shoulder joint, it helps to stabilise the shoulder and powers the wide range of movements
A Guide to Common Ankle Injuries
 A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
Pelvic Girdle Pain (PGP) An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic Girdle Pain (PGP) An information guide Pelvic Girdle Pain (PGP) This is the term used for all pelvic pain. This includes pain anywhere
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic Girdle Pain (PGP) An information guide Pelvic Girdle Pain (PGP) This is the term used for all pelvic pain. This includes pain anywhere
Pelvic floor exercises for anal incontinence
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for anal incontinence An information guide Pelvic floor exercises for anal incontinence Introduction The muscles
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for anal incontinence An information guide Pelvic floor exercises for anal incontinence Introduction The muscles
Urodynamic Studies. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Urodynamic Studies An information guide Urodynamic Test After reading this leaflet we hope that you will have a greater understanding about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Urodynamic Studies An information guide Urodynamic Test After reading this leaflet we hope that you will have a greater understanding about
Surgery for Haglund s deformity
 Patient information Surgery for Haglund s deformity Introduction This leaflet outlines the surgical treatments available for the heel condition known as Haglund s deformity. What is Haglund s deformity?
Patient information Surgery for Haglund s deformity Introduction This leaflet outlines the surgical treatments available for the heel condition known as Haglund s deformity. What is Haglund s deformity?
Arthroscopy. This booklet can also be provided in large print on request. Please call Delivering Excellence. Nuffield Orthopaedic Centre
 This booklet can also be provided in large print on request. Please call 01865 738126 Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Arthroscopy Marketing & Communications Nuffield Orthopaedic
This booklet can also be provided in large print on request. Please call 01865 738126 Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Arthroscopy Marketing & Communications Nuffield Orthopaedic
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
A Patient information guide to. Ankle Arthroscopy. Foot and Ankle Unit. Mr Amit Amin Mr Ali Abbasian ANKLE ARTHROSCOPY JAN
 A Patient information guide to Ankle Arthroscopy Foot and Ankle Unit Mr Amit Amin Mr Ali Abbasian 1 What does surgery involve? An ankle arthroscopy is a keyhole operation to gain access to the inside of
A Patient information guide to Ankle Arthroscopy Foot and Ankle Unit Mr Amit Amin Mr Ali Abbasian 1 What does surgery involve? An ankle arthroscopy is a keyhole operation to gain access to the inside of
BCG Bladder Instillation. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION BCG Bladder Instillation An information guide BCG Bladder Instillation After reading this leaflet we hope you and your family will have
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION BCG Bladder Instillation An information guide BCG Bladder Instillation After reading this leaflet we hope you and your family will have
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Arthroscopic shoulder stabilisation surgery
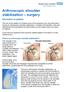 Arthroscopic shoulder stabilisation surgery Information for patients The aim of this leaflet is to answer some of the questions you may have about having an arthroscopic shoulder stabilisation. It explains
Arthroscopic shoulder stabilisation surgery Information for patients The aim of this leaflet is to answer some of the questions you may have about having an arthroscopic shoulder stabilisation. It explains
Angioplasty and Stenting. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Angioplasty and Stenting An information guide Angioplasty and Stenting This leaflet tells you about having an angioplasty and stent insertion.
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Angioplasty and Stenting An information guide Angioplasty and Stenting This leaflet tells you about having an angioplasty and stent insertion.
Coeliac Plexus Block with Alcohol. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Coeliac Plexus Block with Alcohol An information guide Coeliac Plexus Block with Alcohol If you are on blood thinning medications such as
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Coeliac Plexus Block with Alcohol An information guide Coeliac Plexus Block with Alcohol If you are on blood thinning medications such as
Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA. Dr Allen Turnbull Hip and Knee Surgery
 Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA Hip Anatomy Labrum Fovea Femoral Head Articular Cartilage Ligamentum Teres Labral Tears Function of Labrum Deepens acetabulum by 20%
Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA Hip Anatomy Labrum Fovea Femoral Head Articular Cartilage Ligamentum Teres Labral Tears Function of Labrum Deepens acetabulum by 20%
A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip
 A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet
A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet
Arthroscopic capsular release. Information for patients Orthopaedics - Upper Limb
 Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Cirrhosis. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Cirrhosis An information guide Cirrhosis What is cirrhosis? Cirrhosis is the result of long term, continuous damage to the liver and may
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Cirrhosis An information guide Cirrhosis What is cirrhosis? Cirrhosis is the result of long term, continuous damage to the liver and may
A Patient s Guide to Labral Tears of the Hip
 A Patient s Guide to Labral Tears of the Hip 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Labral Tears of the Hip 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
Induced Sputum. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Induced Sputum An information guide Induced Sputum Introduction Your doctor has referred you for an Induced Sputum. This leaflet will explain
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Induced Sputum An information guide Induced Sputum Introduction Your doctor has referred you for an Induced Sputum. This leaflet will explain
UNDERSTANDING ARTHROSCOPY
 UNDERSTANDING ARTHROSCOPY Diagnosing and Treating Your Joint Problem Looking into a Problem Joint Whether you re taking a step or raising your hand, your joints help you move freely. A worn, torn, or injured
UNDERSTANDING ARTHROSCOPY Diagnosing and Treating Your Joint Problem Looking into a Problem Joint Whether you re taking a step or raising your hand, your joints help you move freely. A worn, torn, or injured
Methotrexate in Inflammatory Bowel Disease. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Methotrexate in Inflammatory Bowel Disease An information guide Methotrexate in Inflammatory Bowel Disease Your doctor is planning to start
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Methotrexate in Inflammatory Bowel Disease An information guide Methotrexate in Inflammatory Bowel Disease Your doctor is planning to start
Arthroscopy for Hip Osteoarthritis
 Appendix: Script #1: Health scenarios Arthroscopy for Hip Osteoarthritis Introduction Hip arthroscopy is a surgical procedure that gives doctors a clear view of the inside of the hip joint. This helps
Appendix: Script #1: Health scenarios Arthroscopy for Hip Osteoarthritis Introduction Hip arthroscopy is a surgical procedure that gives doctors a clear view of the inside of the hip joint. This helps
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Clopidogrel 600mg tablets. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Clopidogrel 600mg tablets An information guide Clopidogrel 600mg tablets Your doctor has recommended that you have percutaneous coronary
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Clopidogrel 600mg tablets An information guide Clopidogrel 600mg tablets Your doctor has recommended that you have percutaneous coronary
Knee joint arthroscopy
 Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Floaters & Flashes. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Floaters & Flashes An information guide Floaters & Flashes What are floaters? Floaters are small specks or clouds in your field of vision.
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Floaters & Flashes An information guide Floaters & Flashes What are floaters? Floaters are small specks or clouds in your field of vision.
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Shoulder Instability
 Shoulder Instability The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The
Shoulder Instability The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The
A patient guide to Hip Impingement Non-Surgical Management. Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy
 A patient guide to Hip Impingement Non-Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Contents Page: 1 Cover 2 Contents 3 Hip impingement information 4 Conservative rehabilitation
A patient guide to Hip Impingement Non-Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Contents Page: 1 Cover 2 Contents 3 Hip impingement information 4 Conservative rehabilitation
What is Dysphagia? An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
Adolescent Hip Dysplasia
 Adolescent Hip Dysplasia The hip is a "ball-and-socket" joint. In a normal hip, the ball at the upper end of the femur (thighbone) fits firmly into the socket, which is a curved portion of the pelvis called
Adolescent Hip Dysplasia The hip is a "ball-and-socket" joint. In a normal hip, the ball at the upper end of the femur (thighbone) fits firmly into the socket, which is a curved portion of the pelvis called
Thousand Oaks High School AP Research STEM
 Investigating open surgical and arthroscopic surgical treatments and non-surgical alternatives for femoral acetabular impingement and torn acetabular labrum Thousand Oaks High School AP Research STEM 2
Investigating open surgical and arthroscopic surgical treatments and non-surgical alternatives for femoral acetabular impingement and torn acetabular labrum Thousand Oaks High School AP Research STEM 2
Osteoarthritis of the Hip
 Osteoarthritis of the Hip Information on hip osteoarthritis is also available in Spanish: Osteoartritis de cadera (topic.cfm?topic=a00608). Sometimes called "wear and tear" arthritis, osteoarthritis is
Osteoarthritis of the Hip Information on hip osteoarthritis is also available in Spanish: Osteoartritis de cadera (topic.cfm?topic=a00608). Sometimes called "wear and tear" arthritis, osteoarthritis is
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patien
 The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
Arthroscopy of the Knee
 Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Heartburn and Hiatus Hernia. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Heartburn and Hiatus Hernia An information guide Heartburn and Hiatus Hernia What is Heartburn? Heartburn is a pain behind the breastbone,
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Heartburn and Hiatus Hernia An information guide Heartburn and Hiatus Hernia What is Heartburn? Heartburn is a pain behind the breastbone,
St. George s Shoulder Unit Patient Information
 St. George s Shoulder Unit Patient Information SHOULDER ARTHROSCOPY & ROTATOR CUFF REPAIR Mr. T.D.Tennent FRCS(Orth), Mr Y.O.Pearse FRCS(Orth) This information booklet has been produced to help you obtain
St. George s Shoulder Unit Patient Information SHOULDER ARTHROSCOPY & ROTATOR CUFF REPAIR Mr. T.D.Tennent FRCS(Orth), Mr Y.O.Pearse FRCS(Orth) This information booklet has been produced to help you obtain
Your Arthroscopic Shoulder Procedure
 Your Arthroscopic Shoulder Procedure Education from Contents Regain Your Active Lifestyle 3 What is Arthroscopic Shoulder Surgery? 4 Who is a Candidate for Arthroscopic Shoulder Surgery? 6 Anatomy and
Your Arthroscopic Shoulder Procedure Education from Contents Regain Your Active Lifestyle 3 What is Arthroscopic Shoulder Surgery? 4 Who is a Candidate for Arthroscopic Shoulder Surgery? 6 Anatomy and
Subacromial Decompression
 PATIENT INFORMATION Subacromial Decompression You will be admitted for surgery to your shoulder as a result of a subacromial impingement syndrome. The subacromial impingement syndrome is a condition where
PATIENT INFORMATION Subacromial Decompression You will be admitted for surgery to your shoulder as a result of a subacromial impingement syndrome. The subacromial impingement syndrome is a condition where
Jaundice. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Jaundice An information guide What is Jaundice? Jaundice is characterised by the yellow discolouration of the skin, sclera (whites of the
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Jaundice An information guide What is Jaundice? Jaundice is characterised by the yellow discolouration of the skin, sclera (whites of the
Anterior Cruciate Ligament Reconstruction Patient Information
 Anterior Cruciate Ligament Reconstruction Patient Information This information sheet is designed to help you to understand what an Anterior Cruciate Ligament (ACL) Reconstruction involves. I perform ACL
Anterior Cruciate Ligament Reconstruction Patient Information This information sheet is designed to help you to understand what an Anterior Cruciate Ligament (ACL) Reconstruction involves. I perform ACL
Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction)
 Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery
Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery
Welcome to Audiology. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Welcome to Audiology An information guide Welcome to Audiology The Audiology Department at North Manchester General Hospital is a specialist
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Welcome to Audiology An information guide Welcome to Audiology The Audiology Department at North Manchester General Hospital is a specialist
