Christine Miemban. Clinical Case Report Competition. Utopia Academy. First Place Winner. Massage Therapists Association of British Columbia
|
|
|
- Neil Davis
- 6 years ago
- Views:
Transcription
1 Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy November 2013 First Place Winner Christine Miemban The effects of neuromuscular technique on surgically repaired Achilles tendom rupture P: F: massagetherapy.bc.ca MTABC 2013
2 Table of Contents Acknowledgements 2 Abstract.. 3 Introduction 4 Case Subject History.. 6 Methods..8 Results 10 Discussion.. 14 Conclusion..16 References Appendix A 20 Appendix B
3 Acknowledgements To my case advisor, Aaron Ashe, thank you for all your help with this case study. Your insight has been extremely invaluable to me. To Jim Bowie, thank you for continuously sharing your knowledge with me. It has been a pleasure working with you and learning from you. 2
4 Abstract Objective: To determine if neuromuscular technique (NMT) performed on the gastrocnemius and soleus complex will increase ankle dorsiflexion and decrease scar tissue adhesion in an individual with surgical reattachment of the Achilles tendon, following an Achilles tendon rupture. Background: The subject is a 37 year old, healthy and physically active male. He sustained a complete Achilles tendon rupture to his left ankle while participating in an ultimate Frisbee game in June of Surgical reattachment of the Achilles tendon was performed one day following the injury. Methods: A series of 10 treatments were performed on the subject over a 5 week period. Treatments consisted of Swedish massage, followed by treatment of the left leg utilizing NMT on the gastrocnemius/soleus complex and scar tissue on the Achilles tendon. Results: Significant increases in both passive and weight bearing dorsiflexion have been observed. An overall increase of 17 degrees in passive dorsiflexion was recorded from treatment #1 to treatment #10 with a mean increase of 2.5 degrees at the end of each treatment. Knee-to- Wall Test measurements revealed an overall increase of 4.5 cm in weight-bearing dorsiflexion, with a mean increase of 0.49 cm with each treatment. Scar tissue adhesions decreased and pliability increased over the treatment period and width measurements were found to decrease incrementally over time. Conclusion: NMT, in conjunction with remedial exercises, was determined to be an effective treatment modality in the treatment of a surgically repaired Achilles tendon following a complete Achilles tendon rupture. Key words: Neuromuscular Technique (NMT), Friction, Achilles Tendon Rupture, Achilles Tendinopathy 3
5 Introduction A tendon is a fibrous tissue that serves to attach muscle to bone 1. The Achilles tendon is located on the posterior leg and attaches to the posterior portion of the calcaneal bone 1. It serves as a common tendon for the gastrocnemius and soleus muscles, both of which function in plantar flexion of the ankle 1. This function is essential as it allows individuals to walk, run, jump and stand on one s toes. Achilles tendon rupture occurs when the tendon itself is torn off of its attachment on the calcaneal bone 2. This tearing may occur anywhere along the tendon, as well as the musculotendinous junction. The exact mechanism of this injury remains unclear as it tends to occur spontaneously, particularly during sporting events or vigorous types of activities 2. It is thought that because the Achilles tendon is subject to large amounts of load in the body, repetitive stress to this tendon causes it to be susceptible to injury 3. Individuals who have sustained this injury often describe the initial sensation as if he/she was hit or kicked in the back of the leg, and there is often an audible sound 2. The gastrocnemius and soleus muscles are greatly affected and the individual is unable to plantar flex at the ankle. In addition, dorsiflexion becomes limited, especially with reattachment of the tendon 2. An individual is unable to lengthen the gastrocnemius and soleus and this can ultimately affect one s gait and ability to do certain activities. The injury occurs in 18 out of 100,000 people 4 and often occurs in athletes between the ages of 30 and 40 years, with a 10:1 ratio of males to females 2. A recent study, conducted in Edmonton, Alberta, Canada, determined that an average of 8.3 persons per 100,000 sustained an Achilles tendon rupture 5. 4
6 Debate currently exists over the optimal treatment for Achilles tendon ruptures. Surgical repair has been the preferred method, as several studies have indicated the rate of re-rupture after surgery is low 6,7. Although surgery is often the chosen method of treatment, some practitioners argue that it is unnecessary as the risk of infection and other complications are increased. Alternative treatments that have also been used in Achilles tendon rupture include cast immobilization and functional bracing 8. Functional braces or orthoses allow the ankle to be locked into plantar flexion. Adjustments on the brace can be made by a physician or physiotherapist to gradually move the ankle into dorsiflexion 8. Several studies support this nonconservative method. One such study indicated that 80% of subjects reported good to excellent results with the use of a customized polypropylene orthosis 9. Surgical intervention is often the treatment of choice and this typically involves reattachment of the Achilles tendon. Following surgery, the patient is casted in a plaster and/or fibreglass cast in a neutral position. If the patient is not casted, he/she is placed in a removable boot with wedges under the heel to allow the ankle to rest in plantar flexion. The wedges are progressively taken down to allow the ankle to gradually move into dorsiflexion 8. Physicians often recommend physical therapy following removal of the cast or when the ankle is able to move into a neutral position 8. The purpose of this case study is to determine if massage therapy can increase range of motion at the ankle joint, as well as decrease scar tissue size and adhesions, following surgical reattachment of the Achilles tendon resulting from a complete Achilles tendon rupture. It is hypothesized that: 1) Neuromuscular technique (NMT) performed on the gastrocnemius and soleus complex increases dorsiflexion of the ankle and 2) NMT on scar tissue decreases adhesions and tissue size. 5
7 Case Subject History The subject is a 37 year old male, who is a mechanical engineer. He currently maintains a physically active lifestyle, which includes weight training (3-4 days/week), kite boarding (1-2 days/week), ultimate Frisbee (1 day/week) and beach volleyball (1 day/week). No other conditions have been reported. In June of 2012, the subject participated in a 2 day ultimate Frisbee tournament. On day 1 of the tournament, the subject reported feeling good after having played two games. During the second game on day 2 of the tournament, the subject reported sprinting down the field and feeling a kick in the back of his left heel, causing him to fall to the ground. He did not experience any pain initially. He was taken to the hospital where radiographs confirmed the complete rupture. The Achilles tendon was surgically reattached to the calcaneus the following day. The subject was casted in dorsiflexion for one week in a plaster cast and 4 weeks thereafter in a fibreglass cast. Rehabilitation began after the cast was removed and entailed 3 days a week of physiotherapy, massage therapy and athletic training. Strengthening, increasing muscle mass and proprioceptive training were the main goals in physiotherapy and athletic training, while treating compensatory structures and decreasing scar tissue formation were the main goals in massage therapy. The subject continued with 3 days per week of treatments until the end of December of that year. Despite efforts to decrease scar tissue formation, a significant amount of scar tissue remains on the Achilles tendon. This, coupled with constant hypertonicity in the gastrocnemius and soleus muscles, has contributed to a decrease in range of motion at the ankle joint. Consequently, the subject has found a decrease in performance in the activities he partakes in. 6
8 The subject has not sought any therapy for his injury since the end of December of He currently presents with hypertoned gastrocnemius and soleus muscles, as well as limited dorsiflexion of his left ankle. A significant amount of scar tissue has formed around the surgical incision, as well as on the Achilles tendon and has resulted in restrictions in movement of the ankle. The subject continues to feel tightness in his left leg and in the area of the scar tissue and stretches both the gastrocnemius and soleus muscles when the tightness arises. 7
9 Methods Assessment Tools & Protocols Assessment took approximately 15 minutes before each treatment, and measurements were taken before and after each treatment. Range of motion of the ankle was taken using a goniometer with focus placed on active dorsiflexion and plantar flexion. In addition, dorsiflexion of the ankle with weight bearing was taken using the Knee-to-Wall Test 10 (Appendix A). Scar tissue widths were taken at 3 points along the scar using a skin-fold caliper at the end of each treatment session. The first point was measured at 14.2 cm from the floor; the second point was measured 12.2 cm from the floor; and the third point was measured 10.2 cm from the floor. These points were determined by the top, middle and bottom of the scar tissue in relation to the floor. Measurements for each point were taken three times and the average of these three measurements was then recorded. Assessment also included a Manual Muscle Test (MMT) of both the gastrocnemius and soleus muscles to gauge the muscles strength and functionality 11. The MMT was performed at treatments 1, 4, 7 and 10. Scar tissue adhesion and pliability was assessed with movement in 4 directions: superior, inferior, medial and lateral 12. Treatment Protocol The subject was treated for 60 minutes. Each treatment consisted of 20 minutes of Swedish massage and petrissage techniques on the right leg, as well as on the gluteal group, quadriceps, hamstrings and tibialis anterior muscles of the left leg. This was followed by 40 minutes of treatment to the posterior aspect of the lower left leg. NMT was performed on the gastrocnemius and soleus muscles to decrease hypertonicity 12. Longitudinal frictions and bowing were performed on the Achilles tendon to further lengthen the muscles. The scar tissue 8
10 was treated with bowing, picking up and peeling of the tissue off of the underlying structures. Cross-fibre frictions were incorporated in treatment of the scar tissue. Three 1.5 minute sets of frictions were performed on the tissue, with each set followed by passive stretching of the gastrocnemius and soleus muscles. The first set of frictions involved moderate pressure while the following two sets involved progressively deeper application of pressure. The three sets were then repeated along the scar tissue. The subject was advised to place ice on the left Achilles tendon over the scar after each treatment for 10 minutes. Passive stretches for the gastrocnemius and soleus were demonstrated and prescribed 2 times a day (once in the morning and once in the evening) and the subject was asked to hold each stretch for 30 seconds. Eccentric heel drops, both with the knee kept straight and with the knee bent, were prescribed to strengthen the gastrocnemius and soleus muscles 13 (Appendix A). This exercise was prescribed at 2 sets of 10 repetitions each and done once a day. 9
11 Results Increases in range of motion, particularly with dorsiflexion, were observed. The results for range of motion are located in Tables 1, 2 and Figures 1, 2. The results show linear increases in dorsiflexion over the course of 10 treatments. According to Figure 1 of the results, there are marked increases in passive dorsiflexion of the subject s left ankle following each treatment session. The mean increase in dorsiflexion before and after treatment was calculated to be 2.5 degrees with an overall increase of 17 degrees in the left ankle. Similar results are observed with dorsiflexion in weight bearing in the Knee-to-Wall Test, pre- and post-treatment (Figure 2). The average increase in dorsiflexion between pre- and post-treatment was calculated at 0.49 cm. Despite the small increases between the treatment sessions, the subject made an overall increase of 4.5 cm. The end measurement for the Knee-to- Wall Test was 11.7 cm. RANGE OF MOTION PRE- TREATMENT RANGE OF MOTION POST- TREATMENT Treatment # Dorsiflexion Plantar Flexion Treatment Dorsiflexion Plantar Flexion 1 R 16 o R 48 o 1 R 20 o R 48 o L 3 o L 48 o L 6 o L 49 o 2 R 20 o R 48 o 2 R 20 o R 48 o L 5 o L 48 o L 10 o L 50 o 3 R 20 o R 48 o 3 R 20 o R 48 o L 3 o L 48 o L 10 o L 50 o 4 R 20 o R 50 o 4 R 20 o R 50 o L 10 o L 50 o L 13 o L 50 o 5 R 20 o R 48 o 5 R 20 o R 50 o L 12 o L 50 o L 15 o L 50 o 6 R 18 o R 48 o 6 R 20 o R 49 o L 14 o L 47 o L 16 o L 50 o 7 R 18 o R 49 o 7 R 18 o R 49 o L 14 o L 48 o L 16 o L 50 o 8 R 18 o R 48 o 8 R 18 o R 50 o L 15 o L 50 o L 18 o L 50 o 9 R 18 o R 50 o 9 R 20 o R 50 o L 18 o L 50 o L 18 o L 50 o 10 R 20 o R 49 o 10 R 20 o R 50 o L 19 o L 50 o L 20 o L 50 o Table 1: Range of motion measured pre- and post- treatment 10
12 Dorsiflexion Measurements of LeP Ankle Range of MoCon (o) Treatment # Pre- Treatment Post- Treatment Figure 1: Progress in dorsiflexion of left ankle pre- and post- treatment KNEE TO WALL TEST Treatment # Pre- Treatment (cm) Post- Treatment (cm) 1 R L R L R L R L R L R L R L R L R L R L Table 2: Measurements of Knee to Wall Test pre- and post- treatment 11
13 Knee- to- Wall Measurement of LeP Ankle Measurement (cm) Treatment # Pre- Treatment Post- Treatment Figure 2: Trend of Knee to Wall Test measurements pre- and post- treatment Decreases in scar tissue size are seen in the following Table 3 and Figure 3. Images of the left Achilles tendon are seen in Appendix B. Each of the three measured points in relation to the scar tissue reported a total decrease of 8 mm, 4 mm and 5 mm, respectively. Furthermore, tissue pliability increased while adhesion decreased. Movement of the scar tissue in 4 directions (lateral, medial, superior and inferior) increased and the therapist was able to lift the scar tissue off the Achilles tendon. SCAR TISSUE WIDTH MEASUREMENTS Treatment # Post- Treatment (mm) Table 3: Measurement of scar tissue width pre- and post- treatment 12
14 Scar Tissue Measurements Post- Treatment Measurement (mm) Treatment # PosiCon 1 PosiCon 2 PosiCon 3 Figure 3: Scar Tissue Measurements post- treatment No changes were seen in the MMT of the gastrocnemius and soleus muscles. A grade of 5 for both muscles was recorded at treatments 1, 4, 7 and
15 Discussion Massage therapy, including Swedish and NMT, were effective in increasing range of motion and decreasing scar tissue adhesions after an Achilles tendon rupture and surgical repair. Limited literature exists in regards to Achilles tendon rupture and NMT. The results from this study are consistent with literature on the effects of neuromuscular technique on increasing range of motion and decreasing scar tissue adhesions 14,15. One such study s results indicated that the use of frictions increased the pliability of scar tissue due to the mechanical forces that induce change at the cellular level 15. In addition, massage therapy combined with remedial exercises, are consistent with literature on the use of eccentric exercises following repair of an Achilles tendon rupture 13,16,17. The subject reported a noticeable decrease in overall tightness of the gastrocnemius and soleus muscles and found an improvement in function while participating in physical activities. Furthermore, the restrictions around the scar tissue that the subject had experienced previously have diminished. The subject also found the remedial exercises to be of benefit, particularly on days between treatments. Physical therapy has often been chosen by physicians for rehabilitation of Achilles tendon rupture and repair. This study has given valuable information regarding massage therapy in the treatment of an Achilles tendon rupture. The results suggest that NMT effectively increased range of motion and decreased scar tissue adhesions. This information is beneficial for massage therapists as many therapists utilize NMT in the treatment of many pathologies. Since there is limited literature regarding massage therapy and Achilles tendon rupture and repair, the results of this study are encouraging for massage therapists and massage therapy provides an excellent adjunct to current therapies for this particular injury. 14
16 Despite the overall effectiveness of the case study, there are a number of limitations that need to be addressed. As this study focused on the results of one individual, it is important to note that the results seen in this study may not be representative of a larger population and therefore, a future study should include a larger sample size. The efficacy of the massage treatments versus the efficacy of the remedial exercises are yet to be determined, as it is difficult to say whether one or the other, or a combination of both, contributed to the success of the study. As such, it may be of benefit to consider utilizing massage therapy or remedial exercises rather than a combination of the two when conducting a study. This may aid in determining what the results are attributable to. Furthermore, this study only takes into account treatment of the Achilles tendon rupture and repair in a chronic state. Perhaps the results would differ if treatment was provided closer to the date of injury and repair, rather than a year following the injury. 15
17 Conclusion The effectiveness of neuromuscular technique on increasing range of motion in the ankle, as well as decreasing scar tissue size and adhesions, is strongly evident in this study. The results show a significant increase in dorsiflexion and slight decreases in scar tissue. 16
18 References 1. Tortora, G., Derrickson, B. Principles of Anatomy & Physiology. 13 th ed. Hoboken, New Jersey: John Wiley & Sons, Inc.; Brukner, P. and Khan, K. Clinical Sports Medicine. 3 rd ed. Australia: McGraw-Hill; Nandra, R., Matharu, G. and Porter, K. Acute Achilles tendon rupture. Trauma. 2011; 14(1): Aktas, S., Kocaoglu, B., Nalbantoglu, U., et al. End-to-End Versus Augmented Repair in the Treatment of Acute Achilles Tendon Ruptures. The Journal of Foot & Ankle Surgery. 2007, September; 46(5): Suchak, A., Bostick, G., Reid, D., Blitz, S., Jomha, N. The Incidence of Achilles Tendon Ruptures in Edmonton, Canada. Foot & Ankle International. 2005, November 1; 26: Nyyssonen, T., Saarikoski, H., Kaukonen, J., et al. Simple end-to-end suture versus augmented repair in acute Achilles tendon ruptures: a retrospective comparison in 98 patients. Acta Orthop Scand. 2003, April; 74(2): Bhandari, M., Guyatt, G., Siddiqui, F., et al. Treatment of acute Achilles tendon ruptures: a systematic review and meta-analysis. Clin Orthop. 2002, July; 431: Khan, R., Fick, D., Keogh, A., Crawford, J., Brammar, T., Parker, M. Treatment of Acute Achilles Tendon Ruptures: A Meta-Analysis of Randomized, Controlled Trials. Journal of Bone and Joint Surgery. 2005, October; 87(10): McComis, G., Nawoczenski, D., De Haven, K. Functional bracing for rupture of the Achilles tendon: Clinical results and analysis of ground-reaction forces and temporal data. Journal of Bone and Joint Surgery. 1997, December 1; 79(12):
19 10. Konor, M., Morton, S., Eckerson, J., Grindstaff, T. Reliability of Three Measurements of Ankle Dorsiflexion Range of Motion. The International Journal of Sports Physical Therapy. 2012, June; 7(3): Kendall, F., McCreary, E., Provance, P., Rodgers, M., Romani, W. Muscles: Testing and Function with Posture and Pain. 5 th ed. Baltimore: Lippincott Williams & Wilkins, Rattray, F., Ludwig, L. Clinical Massage Therapy: Understanding, Assessing and Treating over 70 Conditions. Elora, Ontario: Talus Inc.; Grigg, N., Smeathers, J., Wearing, S., Urry, S. Tendon rehabilitation: Isolated eccentric loading invokes a greater reduction in Achilles tendon thickness than concentric loading. Journal of Medicine and Science in Sport. 2008, January; 12: S Sorosky, B., Press, J., Plastaras, C., Rittenberg, J. The practical management of Achilles Tendonopathy. Clinical Journal of Sport Medicine. 2004; 14: Thuzar, S., Bordeaux, J. The Role of Massage in Scar Management: A Literature Review. Dermatologic Surgery. 2012, March; 48: Henriksen, M., Aaboe, J., Bliddal, H., Langberg, H. Journal of Biomechanics. 2009, December 11; 42(16): Fahlstrom, M., Jonsson, P., Lorentzon, R., Alfredson, H. Chronic Achilles Tendon pain treated with eccentric calf-muscle training. Knee Surgery Sports Traumatology, Arthroscopy. 2003, September; 11(5): Vicenzino, B., Branjerdporn, M., Teys, P., Jordan, K. Initial Changes in Posterior Talar Glide and Dorsiflexion of the Ankle After Mobilization With Movement in Individuals With Recurrent Ankle Sprain. Journal of Orthopaedic & Sports Physical Therapy. 2006, July; 36(7):
20 19. Griffiths, I. Ian Griffiths Sports Podiatry. 2010, February 28. Retrieved 2013, November Hoch, M., Staton, G., McKeon, P. Dorsiflexion range of motion significantly influences dynamic balance. Journal of Science and Medicine in Sport. 2010, January 21; 14(2011): Davis, J. Running Writings. 2011, August 22. Retrieved 2013, November
21 Appendix A Knee-to-Wall Test This test is also known as the Weight Bearing Lunge Test (WBLT). A tape measure is placed on the floor with the wall measured at 0 cm. The subject is then asked to place the tested foot next to or on top of the tape measure. A lunge is then performed with the second toe, centre of heel and knee perpendicular to the wall and the heel firmly on the ground 18. The subject lunges forward so that the knee touches the wall and the heel is still in contact with the ground. If the knee cannot touch the wall, the subject moves the foot closer to the wall and perform the lunge until contact with the wall occurs. Measurement is taken from the wall to the first toe. Figure A: Final position of test 19 Figure B: Patient positioning during the test 20 Eccentric Heel Drop Exercises A - The patient stands on the edge of a platform and stands on tips of toes. B - The patient then lowers one heel with the knee straight. Figure C: Positioning for heel drop exercises 21 C - Steps A & B are repeated with the knee bent after completing 10 repetitions with the knee straight. 20
22 Appendix B Treatment #1 Treatment #4 Treatment #7 Treatment #10 21
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
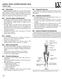 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Achilles Tendon Rupture
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
Dave Tam. Clinical Case Report Competition. WCCMT New Westminster. Third Place Winner. Registered Massage Therapists Association of British Columbia
 Registered Massage Therapists Association of British Columbia Clinical Case Report Competition WCCMT New Westminster December 2014 Third Place Winner Dave Tam Postoperative Achilles tendon rupture: Effects
Registered Massage Therapists Association of British Columbia Clinical Case Report Competition WCCMT New Westminster December 2014 Third Place Winner Dave Tam Postoperative Achilles tendon rupture: Effects
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Foot and Ankle Conditioning Program
 Foot and Ankle Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Foot and Ankle Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Foot and Ankle Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Achilles tendinopathy rehabilitation Non-insertional
 Achilles tendinopathy rehabilitation Non-insertional The Achilles tendon inserts into the back of your heel, and has its origins in the gastrocnemius and soleus muscles in your lower leg. Achilles tendinopathy
Achilles tendinopathy rehabilitation Non-insertional The Achilles tendon inserts into the back of your heel, and has its origins in the gastrocnemius and soleus muscles in your lower leg. Achilles tendinopathy
Foot and Ankle Conditioning Program
 Foot and Ankle Conditioning Program Studies show, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. A program of this nature, focused
Foot and Ankle Conditioning Program Studies show, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. A program of this nature, focused
Sky Ridge Medical Center, Aspen Building Ridgegate Pkwy., Suite 309 Lone Tree, Colorado Office: Fax:
 ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
ANKLE SPRAINS. Explanation. Causes. Symptoms
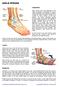 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE JOINT ANATOMY 3. TALRSALS = (FOOT BONES) Fibula. Frances Daly MSc 1 CALCANEUS 2. TALUS 3. NAVICULAR 4. CUBOID 5.
 ANKLE JOINT ANATOMY The ankle joint is a synovial joint of the hinge type. The joint is formed by the distal end of the tibia and medial malleolus, the fibula and lateral malleolus and talus bone. It is
ANKLE JOINT ANATOMY The ankle joint is a synovial joint of the hinge type. The joint is formed by the distal end of the tibia and medial malleolus, the fibula and lateral malleolus and talus bone. It is
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
NHS Buckinghamshire Musculoskeletal Integrated Care Service (MusIC) Achilles tendinopathy
 NHS Buckinghamshire Musculoskeletal Integrated Care Service (MusIC) Achilles tendinopathy What is the Achilles tendon? The Achilles tendon is the biggest and strongest tendon in the body. It is found at
NHS Buckinghamshire Musculoskeletal Integrated Care Service (MusIC) Achilles tendinopathy What is the Achilles tendon? The Achilles tendon is the biggest and strongest tendon in the body. It is found at
ANTERIOR ANKLE IMPINGEMENT
 ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
Dr Schock Achilles Tendon Repair Protocol
 Dr Schock Achilles Tendon Repair Protocol Phase 1- Maximum Protective Phase (2-4 post-op) Goals for Phase 1 Protect integrity of repair Minimize effusion ROM per guidelines listed Immobilization/Weight
Dr Schock Achilles Tendon Repair Protocol Phase 1- Maximum Protective Phase (2-4 post-op) Goals for Phase 1 Protect integrity of repair Minimize effusion ROM per guidelines listed Immobilization/Weight
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Servers Disease (Calcaneal Apophysitis ) 101
 Servers Disease (Calcaneal Apophysitis ) 101 Servers Disease Causes a disturbance to the growing area at the back of the heel bone (calcaneus) where the strong Achilles tendon attaches to it. It is most
Servers Disease (Calcaneal Apophysitis ) 101 Servers Disease Causes a disturbance to the growing area at the back of the heel bone (calcaneus) where the strong Achilles tendon attaches to it. It is most
Ankle Rehabilitation with Wakefield Sports Clinic
 Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Caring For Your Lateral Ankle Middlebury College
 Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Physiotherapy information for Achilles Tendinopathy
 Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Preventative Exercises for the Achilles
 Preventative Exercises for the Achilles Outline 1. Toe walk x 15 each foot 2. Feet out walk x 15 each foot 3. Feet in walk x 15 each foot 4. Ankle in walk x 10 each foot 5. Ankle out walk x 10 each foot
Preventative Exercises for the Achilles Outline 1. Toe walk x 15 each foot 2. Feet out walk x 15 each foot 3. Feet in walk x 15 each foot 4. Ankle in walk x 10 each foot 5. Ankle out walk x 10 each foot
ACHILLES TENDON DISORDERS
 MUSCULOSKELETAL YOUR GUIDE TO ACHILLES TENDON DISORDERS An IPRS Guide to provide you with exercises and advice to ease your condition Contents What is the Achilles Tendon?.....................................
MUSCULOSKELETAL YOUR GUIDE TO ACHILLES TENDON DISORDERS An IPRS Guide to provide you with exercises and advice to ease your condition Contents What is the Achilles Tendon?.....................................
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
Contents The Ankle Joint What is a sprained ankle? What treatment can I receive? Exercises Introduction Please take note of the following
 Contents The Ankle Joint................................ 3 What is a sprained ankle?.................... 4 MUSCULOSKELETAL YOUR GUIDE TO ANKLE SPRAINS An IPRS Guide to provide you with exercises and advice
Contents The Ankle Joint................................ 3 What is a sprained ankle?.................... 4 MUSCULOSKELETAL YOUR GUIDE TO ANKLE SPRAINS An IPRS Guide to provide you with exercises and advice
Achilles Tendinopathy (Mid-portion)
 Achilles Tendinopathy (Mid-portion) What is Achilles tendinopathy? Achilles tendinopathy or tendinitis is a term that has been used for many years to describe pain, swelling and thickening around the Achilles
Achilles Tendinopathy (Mid-portion) What is Achilles tendinopathy? Achilles tendinopathy or tendinitis is a term that has been used for many years to describe pain, swelling and thickening around the Achilles
Badminton. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Badminton Badminton's origin may be traced as far back as fifth century China when players would volley a
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Badminton Badminton's origin may be traced as far back as fifth century China when players would volley a
ACHILLES RUPTURE YOUR GUIDE TO. An IPRS Guide to provide you with exercises and advice to ease your condition
 YOUR GUIDE TO ACHILLES RUPTURE Contents What is an Achilles Rupture?..................................... 3 What treatment can I receive?................................... 4 What exercises should I do?......................................
YOUR GUIDE TO ACHILLES RUPTURE Contents What is an Achilles Rupture?..................................... 3 What treatment can I receive?................................... 4 What exercises should I do?......................................
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Stress Fracture Rehabilitation Guideline
 Stress Fracture Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation following
Stress Fracture Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation following
Everything. You Should Know. About Your Ankles
 Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ANKLE SPRAIN, ACUTE. Description
 Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
(Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage)
 Lateral Meniscus Tear (Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage) What is a lateral meniscus tear? The knee joint comprises of the union of two
Lateral Meniscus Tear (Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage) What is a lateral meniscus tear? The knee joint comprises of the union of two
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
Proximal Medial Gastrocnemius Release (PMGR)
 Proximal Medial Gastrocnemius Release (PMGR) Physiotherapy and Orthopaedic Department Patient information leaflet Date: Name of Patient: Name of Physiotherapist: Telephone: 01483 464153 This leaflet has
Proximal Medial Gastrocnemius Release (PMGR) Physiotherapy and Orthopaedic Department Patient information leaflet Date: Name of Patient: Name of Physiotherapist: Telephone: 01483 464153 This leaflet has
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Common Athletic Injuries of the Ankle
 Common Athletic Injuries of the Ankle Common Injuries of the Ankle in Athletes Ankle Sprains Chronic Lateral Ankle Instability Peroneal Tendon Injuries Achilles Tendon Tears Ankle Sprains What s an Ankle
Common Athletic Injuries of the Ankle Common Injuries of the Ankle in Athletes Ankle Sprains Chronic Lateral Ankle Instability Peroneal Tendon Injuries Achilles Tendon Tears Ankle Sprains What s an Ankle
Plantar Fasciitis. Equipment: Anti-inflammatory drugs: Night splints keep the plantar fascia from getting will relieve pain and reduce swelling.
 Plantar fasciitis is the most common cause of heel pain for which professional care is sought. This is caused by irritation of the plantar fascia a thickened fibrous band that runs from the heel to the
Plantar fasciitis is the most common cause of heel pain for which professional care is sought. This is caused by irritation of the plantar fascia a thickened fibrous band that runs from the heel to the
A Patient s Guide to Ankle Sprain and Instability. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Ankle Sprain and Instability Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written
A Patient s Guide to Ankle Sprain and Instability Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written
TREATMENT GUIDELINES FOR GRADE 3 PCL TEAR
 GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
POSTERIOR TIBIAL TENDON RUPTURE
 POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
Symptoms usually come on gradually. Depending on the severity of the injury, they can include:
 What is the Achilles tendon? The Achilles tendon is situated above the heel and forms the lower part of the calf muscles. It is a continuation of the two calf muscles, the gastrocnemius and soleus muscles,
What is the Achilles tendon? The Achilles tendon is situated above the heel and forms the lower part of the calf muscles. It is a continuation of the two calf muscles, the gastrocnemius and soleus muscles,
FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]
![FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test] FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]](/thumbs/83/88335212.jpg) FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
Achilles Tendon Repair and Rehabilitation
 1 Achilles Tendon Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The poorest blood supply to the Achilles tendon is in the central part of the tendon approximately
1 Achilles Tendon Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The poorest blood supply to the Achilles tendon is in the central part of the tendon approximately
Managing Tibialis Posterior Tendon Injuries
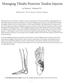 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
SEMIMEMBRANOSUS TENDINITIS
 SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
Rebound Achilles Wedge Kit
 Rebound Achilles Wedge Kit Clinical Indications Indications for Use The Achilles Wedge Kit is intended for use in treating full or partial ruptures of the Achilles Tendon. The Achilles Wedge Kit can be
Rebound Achilles Wedge Kit Clinical Indications Indications for Use The Achilles Wedge Kit is intended for use in treating full or partial ruptures of the Achilles Tendon. The Achilles Wedge Kit can be
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Dr. Abigail R. Hamilton, MD
 ACHILLES TENDINITIS Dr. Abigail R. Hamilton, MD ANATOMY The Achilles tendon is a strong tendon that connects the calf muscles to the heel. When the calf muscles contract, they pull on the Achilles tendon
ACHILLES TENDINITIS Dr. Abigail R. Hamilton, MD ANATOMY The Achilles tendon is a strong tendon that connects the calf muscles to the heel. When the calf muscles contract, they pull on the Achilles tendon
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Principles of Treatment. Case Studies. Principles of Treatment. Clinical Perspectives for the GP
 Principles of Treatment Clinical Perspectives for the GP Case Studies 1. Jumping athlete with an acute exacerbation of chronic patellar tendinopathy major competition in 9 days time 2 week tournament 2.
Principles of Treatment Clinical Perspectives for the GP Case Studies 1. Jumping athlete with an acute exacerbation of chronic patellar tendinopathy major competition in 9 days time 2 week tournament 2.
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN Tel: Fax:
 Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Hamstring Strain. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com.
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Hamstring Strain The hamstring muscles are very susceptible to tears, strains and other common sporting
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Hamstring Strain The hamstring muscles are very susceptible to tears, strains and other common sporting
A Patient s Guide to Achilles Tendon Problems
 A Patient s Guide to Achilles Tendon Problems 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Achilles Tendon Problems 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this booklet is compiled
Acute Achilles Tendon Repair Protocol
 Acute Achilles Tendon Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that you
Acute Achilles Tendon Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that you
Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture
 19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
LATERAL LIGAMENT SPRAIN OF THE ANKLE
 MUSCULOSKELETAL YOUR GUIDE TO LATERAL LIGAMENT SPRAIN OF THE ANKLE An IPRS Guide to provide you with exercises and advice to ease your condition Contents The ankle joint..................................................
MUSCULOSKELETAL YOUR GUIDE TO LATERAL LIGAMENT SPRAIN OF THE ANKLE An IPRS Guide to provide you with exercises and advice to ease your condition Contents The ankle joint..................................................
Week 1 Orthotics- 1. Knee brace locked in full extension at all times except for rehab exercises 2. Elastic bandage as needed to control swelling
 General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
Copyright 2012 by The McGraw-Hill Companies, Inc. All rights reserved. McGraw-Hill/Irwin
 CHAPTER 8: THE LOWER EXTREMITY: KNEE, ANKLE, AND FOOT KINESIOLOGY Scientific Basis of Human Motion, 12 th edition Hamilton, Weimar & Luttgens Presentation Created by TK Koesterer, Ph.D., ATC Humboldt State
CHAPTER 8: THE LOWER EXTREMITY: KNEE, ANKLE, AND FOOT KINESIOLOGY Scientific Basis of Human Motion, 12 th edition Hamilton, Weimar & Luttgens Presentation Created by TK Koesterer, Ph.D., ATC Humboldt State
WHAT IS PLANTAR FASCIITIS?
 WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
Protocols for Posterior Tibial Tendon Dysfunction & Achilles Tendinosis. Tara Bries, PT
 Protocols for Posterior Tibial Tendon Dysfunction & Achilles Tendinosis Tara Bries, PT Non-Operative Protocol for Posterior Tibialis Tendon Dysfunction Based on research by Alvarez et al. (2006) entitled
Protocols for Posterior Tibial Tendon Dysfunction & Achilles Tendinosis Tara Bries, PT Non-Operative Protocol for Posterior Tibialis Tendon Dysfunction Based on research by Alvarez et al. (2006) entitled
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Plantar Fasciitis, Myofascial Connections and Yoga
 Friday, September 20, 2013 Plantar Fasciitis, Myofascial Connections and Yoga The therapeutic benefits of Hatha yoga arise from whole body energetic balancing combined with distinct biomechanical adjustments.
Friday, September 20, 2013 Plantar Fasciitis, Myofascial Connections and Yoga The therapeutic benefits of Hatha yoga arise from whole body energetic balancing combined with distinct biomechanical adjustments.
PLANTAR FASCIITIS - Advice & Rehabilitation Leaflet
 Dr Patrick Wheeler Consultant in Sport and Exercise Medicine Leicester General Hospital Gwendolen Road, Leicester, LE5 4PW Telephone: 0116 258 4365 Patient information and rehabilitation leaflet Plantar
Dr Patrick Wheeler Consultant in Sport and Exercise Medicine Leicester General Hospital Gwendolen Road, Leicester, LE5 4PW Telephone: 0116 258 4365 Patient information and rehabilitation leaflet Plantar
Leo Kormanik DC, MS, CCSP Ohio Sports Chiropractic
 Leo Kormanik DC, MS, CCSP Ohio Sports Chiropractic ! Been running at a high level for 15 years.! 2012 Olympics Trials qualifier in the marathon and 6-time All-American in college! Owner of Ohio Sports
Leo Kormanik DC, MS, CCSP Ohio Sports Chiropractic ! Been running at a high level for 15 years.! 2012 Olympics Trials qualifier in the marathon and 6-time All-American in college! Owner of Ohio Sports
Dr. Gene Desepoli Anterolateral Shin Splints Summary Treatment Sheet
 Dr. Gene Desepoli Anterolateral Shin Splints Summary Treatment Sheet Pathology: Anterolateral shin splints results from strain to the tibialis anterior muscle from eccentric overuse, running on hard ground
Dr. Gene Desepoli Anterolateral Shin Splints Summary Treatment Sheet Pathology: Anterolateral shin splints results from strain to the tibialis anterior muscle from eccentric overuse, running on hard ground
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
A calf strain often occurs when the calf muscles are working eccentrically ( working while under a stretch), such as coming down from a jump, and
 A calf strain often occurs when the calf muscles are working eccentrically ( working while under a stretch), such as coming down from a jump, and also during the time when you are about to push off to
A calf strain often occurs when the calf muscles are working eccentrically ( working while under a stretch), such as coming down from a jump, and also during the time when you are about to push off to
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
chapter1 integrated crosstraining
 chapter1 integrated crosstraining Adventure isn t hanging on a rope off the side of a mountain. Adventure is an attitude that we must apply to the day-to-day obstacles of life facing new challenges, seizing
chapter1 integrated crosstraining Adventure isn t hanging on a rope off the side of a mountain. Adventure is an attitude that we must apply to the day-to-day obstacles of life facing new challenges, seizing
FUNCTIONAL INJURY PREVENTION EXERCISES Part 3. The Ankle Complex
 FUNCTIONAL INJURY PREVENTION EXERCISES Part 3 The Ankle Complex Talk to any athlete and ask them if they have ever sprained their ankle. I would say, about 90% will tell you they have at least rolled their
FUNCTIONAL INJURY PREVENTION EXERCISES Part 3 The Ankle Complex Talk to any athlete and ask them if they have ever sprained their ankle. I would say, about 90% will tell you they have at least rolled their
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Southern Sports & Orthopaedics
 Knee conditioning program This knee conditioning program is designed to help you rehabilitate from your knee injury. In some cases, the program is being used as pre-habilitation, that is strengthening
Knee conditioning program This knee conditioning program is designed to help you rehabilitate from your knee injury. In some cases, the program is being used as pre-habilitation, that is strengthening
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
What are the symptoms of plantar fasciitis? The main symptoms of plantar fasciitis include: What causes plantar fasciitis?
 Plantar Fasciitis Plantar fasciitis is a condition which can cause heel pain. It happens when the strong band of tissue on the sole of your foot (fascia) becomes irritated, after repetitive use or due
Plantar Fasciitis Plantar fasciitis is a condition which can cause heel pain. It happens when the strong band of tissue on the sole of your foot (fascia) becomes irritated, after repetitive use or due
Human anatomy reference:
 Human anatomy reference: Weak Glut Activation Weak gluteal activation comes from poor biomechanics, poor awareness when training or prolonged exposure in deactivated positions such as sitting. Weak Glut
Human anatomy reference: Weak Glut Activation Weak gluteal activation comes from poor biomechanics, poor awareness when training or prolonged exposure in deactivated positions such as sitting. Weak Glut
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
It is also important to make note of your function, as this may be your first indication of improvement.
 Back Pain 1 Management of Back Pain The resolution of pain involves gradually increasing the number of repetitions or resistance of the exercises performed. However, it is important to stay within a range
Back Pain 1 Management of Back Pain The resolution of pain involves gradually increasing the number of repetitions or resistance of the exercises performed. However, it is important to stay within a range
Tendo Achilles rupture
 Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
ILIOTIBIAL BAND SYNDROME
 Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Stay Strong REST AND RECOVERY
 Start Running! Running improves your physical, emotional and mental health perhaps that s why its the most popular fitness activity around the world. The Ohio State University Wexner Medical Center Sports
Start Running! Running improves your physical, emotional and mental health perhaps that s why its the most popular fitness activity around the world. The Ohio State University Wexner Medical Center Sports
