tendinopathy in tennis
|
|
|
- Alberta Hines
- 6 years ago
- Views:
Transcription
1 Musculoskeletal tendinopathy in tennis Written by Neeru Jayanthi, USA Tendinopathy in the tennis player is common and can either affect playing ability or even prevent a player from being on court. If the tissue pathology is addressed properly, traditional treatments of training load modifications and eccentric strength training that involve a functional component can be quite effective. However secondary management with more innovative techniques may be necessary in recalcitrant cases. Surgery is not necessary in the majority of cases of chronic tendinopathy. Tennis-specific return may need to involve stroke modifications, bracing and possible volume adjustment. Long-term success with chronic tendinopathy in tennis can still be encouraging if a structured approach is utilised. GENERAL CONCEPTS OF TENDINOPATHY Tendinopathy generally refers to an abnormal tendon. This term is much more reflective of the actual pathophysiology of this condition, rather than the more common term of tendinitis because there is rarely a pathological finding of -itis or inflammation. Nirschl described angiofibroblastic tendinosis with few inflammatory cells on histological evaluation of elbow tendinopathy 1. Tendinosis implies cumulative load to the tendon resulting in some degenerative changes. Australia s Professor Jill Cook further describes the process of tendinopathy to be in three stages (Figure 1) 2 : 1. Reactive 2. Dysrepair, 3. Degenerative, where there is often a combination of all of these stages. Ultimately, the stage of tendinopathy helps determine the treatment plan. Reactive tendinopathy is increased load from accumulation of eccentric loading or training without degenerative changes, resulting in a painful tendon. In this stage, it is most important to evaluate training load and modify or reduce the eccentric component of this load where possible. Other modifications such as patellar tendon straps or heel lifts for Achilles tendinopathy may help to unload the tendon. Dysrepair may include stages prior to development of tendinopathy. Evaluating the rehabilitation that would contribute to tendon healing rather than worsening tendon pathology is the main goal during these earlier stages. For example, it may be better to apply loads that reduce overall pain in the earlier phases (such as isometric load or resistance training in the mid-range that is done isometrically). Degenerative tendinopathy involves the terminal stages of tendon pathology. Degenerative tendinopathy responds best to eccentric strengthening as has been shown in multiple studies 2. The exception may be when there is reactive on top of degenerative tendinopathy and this type of irritable tendon would need load reduction and modifications prior to initiating eccentric strength training. EPIDEMIOLOGY As tendinopathy is degenerative and cumulative, it rarely occurs in players younger than 18 years old. Adult recreational players are most at risk for development of tendinopathy based on age, playing volume and in some cases, technique. A cross-sectional self-report survey of 529 USTA recreational adult league players of an average age of 46.9 years old found that there was an injury incidence of 3.0 injuries/1000 hours of play, while there was a prevalence of 53 injuries/100 players 3. The elbow was the most common site of injury (20% of all injuries), while the shoulder was 498
2 Stress shielded Optimised load Optimised load Normal or excessive load +/- individual factors Unloaded Normal tendon Adaption Excessive load + individual factors Appropriate modified load Strengthen injury to the pronator teres and flexor carpi radialis muscles at the origin on the medial epicondyle. Reactive tendinopathy Tendon dysrepair Degenerative tendinopathy Figure 1: The three stages of tendinopathy. the second most common with 15% of all injuries. Other studies have found a 50% lifetime incidence of elbow pain in adult tennis players over 30 years old 4. While true tennis elbow is a relatively common condition in the adult tennis player, another study which followed 700 elite players followed at the French Open over 3 years, including the seniors, had only one reported case of tennis elbow 5. This suggests that proper technique may be protective of this condition despite advancing age. Rates of shoulder injury have generally been reported between 4 and 17% of players (including rotator cuff tendinopathy as well as all other tennis-specific shoulder conditions). Reports of shoulder pain may be as high as 24% in high level competitive players aged 12 to 19, and 50% in middle aged players 6. Other common areas for tendinopathy include the Achilles and patellar tendons. The rate of other tendinopathies in tennis players has not been as well documented as in the elbow or shoulder. COMMON AREAS OF TENDINOPATHY IN TENNIS Elbow Anatomy of elbow tendinopathy Lateral epicondylosis (or lateral elbow tendinosis) typically involves injury to the extensor carpi radialis brevis muscle but may also involve the extensor digitorum communis muscle. Medial epicondylosis (or medial elbow tendinosis) involves Treatment The treatment of these conditions most frequently depends on the stage of the tendinopathy (Figure 2). Short-term solutions for pain control may include non-steroidal anti-inflammatory drugs, counterforce bracing, light eccentric strengthening and activity modifications which may all help to improve symptoms within the first 6 weeks. Counterforce bracing may actually limit forces to the extensor carpi radialis brevis, while addressing the true tendon pathology through isokinetic eccentric strengthening programmes has been shown to be most effective in reducing pain and even the appearance of the tendon at 1 month 7. A small study demonstrated that a single novel eccentric strengthening exercise using a rubber bar improved all outcome measures compared to standard physical therapy 8. Shoulder rotation strength is often weak in elbow tendinopathy patients, so a functional component to rehabilitation engaging the entire upper quarter and kinetic chain should be utilised as well. The addition of a steroid injection may be helpful up to 6 weeks, but isolated steroid injections were less effective than physiotherapy and wait and see approach at 52 weeks, with higher rates of recurrence with steroid injection 9. Injection with fenestrations with limited or no steroid may address the tendon pathology better and result in longer term improvements. In chronic cases where the symptoms become recalcitrant, other interventional or pro-inflammatory options may need sports medicine in tennis TARGETED TOPIC 499
3 Musculoskeletal Diagnosis of medial epicondylitis; signs include: Tender medial epicondyle Pain with passive wrist extension Pain with resisted wrist flexion OR Diagnosis of lateral epicondylitis; signs include: Tender lateral epicondyle Pain with passive wrist flexion Pain with resisted wrist extension Phase 1: Initial management (<6 weeks symptom duration) Activity modifications Counterforce brace Topical and oral NSAIDs Passive range of motion in terminal extension and flexion with light eccentric strengthening Improved function and pain: +/- brace painful activities Continue home exercises Injury prevention education Expectant management Continuing or worsening function/pain: Phase 2 treatment: 3-view elbow X-rays Formal rehabilitation with eccentric strengthening, +/- iontophoresis Activity modification or avoidance (work/sport) Counterforce brace, dynamic extension splint or volar splint Consider injection (+/- steroid) 6-week follow-up Improved function and pain: +/- brace painful activities Continue home exercises Injury prevention education Expectant management Continuing or worsening function: Dx: Chronic elbow tendinosis Reassess and adjust rehabilitation programme Consider different type of brace Refer to chronic epicondylitis algorithm Identify other pathology: Treat new diagnosis Referral to appropriate specialist Figure 2: Algorithm for acute epicondylitis (epicondylosis) (reprinted with permission from NSAIDS=non-steroidal antiinflammatory drugs. 500
4 Table 1 to be considered (Figure 3). These proinflammatory options are emerging rapidly, while the scientific support is still relatively new. These options will be discussed in more detail at the end of this review with regards to all types of tendinopathy. Nirschl found about 97% improvement with his technique of arthroscopic drilling of the lateral epicondyle and debridement of the ECRB with return to tennis after surgery within 3 months, however this was not a controlled study 10. Surgical techniques may also include open repair or percutaneous releases. Most studies show minimal differences in outcomes between the techniques, although most studies evaluate treatment in mainly non-tennis playing populations 10. Adult recreational player Shoulder Rotator cuff impingement/tear internal impingement SLAP/labral tear Elbow Later epicondylosis Stroke affected Cocking/loading phase of serve Follow through/ deceleration phase One-handed backhand, forearm pronation (forehand, serve, follow through) Stroke modification Retract scapula in loading/ cocking phase, lower body force generation Decrease rapid internal rotation on follow through, lower force generation Limit wrist extension on onehanded backhand at contact and late follow through Tennis-specific recommendations Equipment: Nirschl criteria were developed to measure appropriate grip size based on the measurement equal to the number of inches from the proximal palmar crease to the tip of the ring finger. Following Nirschl criteria with up to 0.25 inches of difference did not influence forces to the lateral epicondyle, but our tennisrelated impression is that assessing grip size may still be a reasonable part of the tennis-specific evaluation 10. While limiting vibrations to the elbow is intuitive in limiting progression to injury, this has not been effective. Modifications of vibrations with vibration dampeners are negligible as the weight of strings is about 1/10th the weight of the racquet itself. Similarly, the weight of the racquet, either too heavy or too light, seems to have little effect on development of tendinopathy. A good general rule is to use the heaviest racquet that does not affect swing speed. Tennis stroke modifications The development of lateral or medial elbow tendinosis may occur through one of the following mechanisms 10,11 (Table 1): 1. Excess forearm pronation on serves or forehands (either lateral or medial tendinosis) (Figure 4). 2. Increased wrist extension, leading elbow or forearm pronation or lateral tendinosis excess wrist extension at the point of contact or on the follow through on one handed backhands (Figure 4). Medial epicondylosis Early eccentric phase of wrist extension or late eccentric follow through on one-handed backhand Forehand, extreme topspin 3. Extreme forehand western or semiwestern grips that result in extreme supination with ulnar deviation of the wrist with early rapid rotation and acceleration on topspin forehands (medial elbow tendinosis) and slice/ spin serves. This may often occur in the more advanced or competitive player. Ilfeld found that stroke modification combined with conservative therapy led to resolution in more than 90% of cases of tennis elbow 12. Interestingly, many cases were not just painful on backhands, but also with forearm pronation on forehand and serve follow-through. The twohanded backhand may help limit the end ranges of motion of the wrist, even though measured wrist extensor activity may be the same. Volume of tennis of >2 hours/ day has been associated with increased risk of tennis elbow, however there was no increase in risk of injury with up to 6 hours/weekly 11. The risk of injury in adult recreational players related to playing Reduce forearm pronation on forehand serve Avoid extreme western grip and heavy topspin forehand, limit slice serves Table 1: Stroke modifications for shoulder and elbow pathology in tennis (table adopted with permission from CSMR), SLAP=superior labrum anterior and posterior. tennis between 6 and 10 hours weekly has not been investigated. Rotator cuff tendon Tendinopathy in the tendon may be similar in appearance to partial thickness tears on the bursal or articular side. It has been postulated that bursal-sided tears and tendinopathy may be related to mechanical trauma such as a downsloping acromion, while articular-sided pathology are felt to be related to age-related degenerative factors 13. Rotator cuff tendinopathy is most commonly found in the supraspinatus tendon, while infraspinatus and subscapularis may also be involved. Scapular dyskinesis may contribute to the impingement process and play a role in functional deficits during tennis overhead strokes. The rotator cuff is commonly involved and also noted to have more MRI documented degenerative changes on the dominant side of overhead athletes than the non-dominant side, even when asymptomatic. sports medicine in tennis TARGETED TOPIC 501
5 Musculoskeletal Figure 3: Algorithm for chronic epicondylitis (epicondylosis) (reprinted with permission from com) MRI=magnetic resonance imaging, PRP=platelet rich plasma, US=ultrasound. Diagnosis of chronic medial epiconylitis (>12 weeks symptoms) Signs include: Tender medial epicondyle Pain with passive wrist extension Pain with resisted wrist flexion OR Diagnosis of chronic lateral epicondylitis (>12 weeks symptoms) Signs include: Tender lateral epicondyle Pain with passive wrist flexion Pain with resisted wrist extension Phase 2 treatment: 6-12 weeks Continue or initiate eccentric strengthening Continue activity avoidance or modification Consider or repeat injection (+/- steroid) Injection with multiple fenestrations Improved function and pain: +/- brace painful activities Continue home exercises Injury prevention education Expectant management Continued or worsened function/pain: Review negative predictors Review secondary gain issues Identify other pathology: Treat new diagnosis Referral to appropriate specialist Referral to appropriate specialist: Phase 3 treatment options Advanced imaging MRI Musculoskeletal US Surgical options (>6 months) Debridement with +/- arthroscopic drilling Open debridement Percutaneous tenotomy Alternate treatment options Nitroglycerin patches Buffered PRP injections Autologous blood injections Acupuncture Prolotherapy Botulinum toxin A injection Sclerosing polidocanol injections US-guided tenotomy Improved function and pain: Continue home exercises Injury prevention education Expectant management 502
6 a b c Treatment Treatment and successful return to play after rotator cuff tendinopathy may be challenging. Full thickness rotator cuff tears (not associated with an acute injury atraumatic) can be treated conservatively with a dedicated rehabilitation programme in approximately 75% of cases with 2-year follow up 14. This may involve a d Figure 4: (a) Forearm pronation at end of aggressive forehand topspin stroke, (b) reducing forearm pronation on forehand at end of stroke, (c) increased early wrist extension with leading elbow on backhand, (d) proper one-handed backhand with linear shoulder/elbow/arm movements and reduced wrist extension. supervised physical therapy programme, or independent home exercises addressing rotator cuff strength deficits and range of motion. They were not targeted or sportsspecific rehabilitation programmes as the subjects included a variety of types of patients who were not necessarily athletes. Partial thickness rotator cuff tendinopathy may be treated non-operatively in the majority of cases. Eccentric strengthening of the rotator cuff tendon may be helpful in improving rotator cuff tendinopathy. This must be incorporated at the appropriate time, such as after addressing scapular deficits and reducing some of the pain, so the rehabilitation is effective without causing more pain. Kibler has extensively described functional strengthening with addressing of scapular dyskinesis for rotator cuff impingement 15. More detailed rotator cuff rehabilitation programmes in the tennis player are beyond the scope of this review, but are well covered in other manuscripts. Pro-inflammatory options for chronic and recalcitrant rotator cuff tendinopathy are still being investigated. These are also presented at the end of this review. Surgical decompression of the acromion with possible rotator cuff repair is an option if the athlete has failed a high quality rehabilitation programme. This may require a mean of 9.8 months away from tennis 16. Tennis-specific recommendations Return to tennis following rotator cuff tendinopathy may involve some important volume and stroke recommendations. Kibler describes incorporating the kinetic chain to utilise optimum (>50%) lower body force generation 17, while >10 knee bend may limit forces to the shoulder and elbow. These numbers tend to be reversed in the recreational player where upper body forces predominate. Utilising the kinetic chain on a serve may involve a deeper knee bend and more powerful hip rotation, Incorporating scapular retraction into the serve may help reduce rotator cuff impingement symptoms related to tendinopathy. Kovacs describes an eight-stage model (which include preparation, acceleration and followthrough phases) to limit upper extremity problems in the serve which also involves optimum shoulder elevation without excess sports medicine in tennis TARGETED TOPIC 503
7 Musculoskeletal Patient presents with non-insertional or insertional Achilles tendinopathy (<6 weeks) Exclude rupture, other causes evaluate peritendinous structures Phase 1: Evaluate and treat biomechanical faults (heel lift or orthotics) Reduce total load in acute (reactive) Achilles tendinopathy Phase 2: Begin eccentric heel-drop protocol 6-12 weeks (with some pain) No response Response, progress to decline, higher load, higher rate, and then functional return to tennis Secondary options (chronic, degenerative >12 weeks): Continue eccentric strengthening Consider GTN patch, US-guided PRP or autologous blood, sclerosants, Botulinum A Consider US-guided tenotomy versus MRI Surgical evaluation (more likely if insertional) Figure 5: Achilles tendinopathy algorithm. GTN=glycerol trinitrate, PRP=platelet rich plasma, MRI=magnetic resonance imaging, US=ultrasound. hyperangulation and external rotation, in addition to proper lower body force generation 18. Achilles tendinopathy Anatomy of Achilles tendinopathy Tennis players are required to repetitively perform sudden eccentric contractions of the Achilles tendon with forefoot loading during most strokes, particularly when on the forefoot for volleys, split steps and directional changes on groundstrokes. The Achilles tendon may develop tendinopathy in the non-insertional and the insertional region. Non-insertional tendinopathy of the Achilles tendon may typically occur approximately 2 to 6 cm proximal to the calcaneal insertion and develop thickening, nodularity and disorganised tendon architecture. This is considered a relatively avascular region. Insertional Achilles tendinopathy may be the result of mechanical irritation such as squaring of the posterior superior calcaneus (Haglund s 504
8 Volume of tennis of >2 hours/day has been associated with increased risk of tennis elbow, however there was no increase in risk with up to 6 hours/weekly deformity) or be mistaken for retrocalcaneal bursitis, retroachilles bursitis or even posterior ankle impingement from such structures as an os trigonum. Treatment A natural history study of 5-year outcomes of Achilles tendinopathy suggests that the majority of cases have good outcomes with Alfredson s exercisebased heel-drop eccentric strengthening programme alone 19. Eccentric strength training has been shown to be effective in the majority of cases on non-insertional Achilles tendinopathy, even through pain (Figure 5). The important component is the heel-drop eccentric portion of the strengthening. This should be progressive, starting with body weight loading then loading with extra weight, such as a backpack and even the speed at which it is done to deliver even higher loads. Outcomes for insertional Achilles tendinopathy are less reliable as there may be other mechanical components involved such as a Haglund s deformity. The heel drop eccentric strengthening programme should be used, but modified to the heel drop only to neutral in cases of insertional Achilles tendinopathy. Pro-inflammatory options have been described and will be outlined at the end of this review. Surgery should only be considered as a last resort in nontraumatic cases of Achilles tendinopathy. Tennis-specific modifications Heel lifts may unload the Achilles tendon during tennis. Reduction of offcourt eccentric training and limiting forefoot loading and repetitive plantar flexion in training and competition is also recommended. Also, consider playing on surfaces with low friction that allow sliding (e.g. clay vs hard court) and to make sure the outsole of the shoe matches the court surface. Patellar tendinopathy Anatomy of patellar tendinopathy Repetitive knee eccentric loading occurs where a flexed knee is extended in most strokes of competitive tennis players, particularly when utilising lower body force generation. Most pathology of patellar tendinopathy develops in the proximal patellar tendon, while mid-substance and distal tendinopathy may still occur. Treatment Eccentric strength training of the patellar tendon has been effective in treating chronic patellar tendinopathy (Figure 6). This treatment has been shown to be equivalent to patellar tenotomy in one randomised study 20. This effect is not seen when done in season, presumably due to excess load to the tendon. To augment results, a decline squat eccentric strengthening programme should be done at 25 and may have weights added as well to increase rehabilitative load 20. While numerous anecdotal cases exist of chronic patellar tendinopathy in elite tennis players, there is little tennis-specific data of this condition. Quadriceps tendinopathy may occur much less commonly and can be treated with similar eccentric strengthening as for patellar tendinopathy. Tennis-specific recommendations Reduce load with training (i.e. plyometrics, post-exercise eccentric training, inseason eccentrics, including uphill or downhill training). Patellar tendon straps may reduce forces to the tendon during play. Reduction of high load and rapid directional changes during training or competition such as limiting serve and volley is recommended. A player may consider slicing balls (under-spin) more often to reduce lower body load for lower balls rather than needing lower body force generation for heavy spin. Knee pain ratings have also been found to be better on clay courts than hard courts. OTHER TENDINOPATHIES Less common tendinopathies may occur in tennis players in other areas of the body around the lateral hip, ankle and the knee. Gluteus medius tendinopathy may often be labelled as other conditions such as greater trochanter syndrome or trochanteric bursitis. Many coaches may not be aware of this improved understanding sports medicine in tennis TARGETED TOPIC 505
9 Musculoskeletal Patient presents with patellar tendinopathy (acute <6 weeks) Painful decline squat Phase 1: Evaluate and treat biomechanical faults (patellar tendon strap) Reduce total load in acute (reactive) patellar tendinopathy Phase 2: Begin eccentric decline squat protocol 6-12 weeks (with some pain) No response Response, progress to decline, higher load, higher rate, and then functional return to tennis Secondary options (chronic, degenerative >12 weeks): Continue eccentric strengthening Consider GTN patch, US-guided PRP or autologous blood, sclerosants, Botulinum A Consider US-guided tenotomy versus MRI Surgical evaluation for patellar tenotomy Figure 6: Patellar tendinopathy algorithm. GTN=glycerol trinitrate, PRP=platelet rich plasma, MRI=magnetic resonance imaging, US=ultrasound. so health professionals may need to provide education via available channels. Traditionally, hip abduction strengthening combined with manual treatments to restore normal gluteus medius tendon pathology and symmetric pelvic stability are typical first line treatments. Procedures may also include injection of glucocorticoid, but probably done with fenestrations and may even include other pro-inflammatory or regenerative injections. Tennis players may get asymmetric pain patterns in the pelvis related to training and style of play. Ankle tendinopathy may occur in the posterior tibialis tendon or peroneal tendons, in addition to Achilles tendinopathy. Nonachilles ankle tendons function to stabilise the ankle and the posterior tibialis tendon may play a role in forming the arch of the foot. Addressing foot alignment with orthotics, ankle bracing and combining this with proper eccentric strength training may help with treatment of these conditions. Occasionally, longitudinal tears and/or progression of the posterior tibialis tendon may require surgical debridement or larger reconstructive procedures. SECONDARY OPTIONS FOR TENDINOPATHY When traditional methods for treating tendinopathy fail, particularly appropriate mechanical loading with eccentric 506
10 strengthening and volume reduction over extended periods, then it may be worthwhile to consider other non-surgical approaches. To induce or stimulate the healing process of the tendon, pro-inflammatory (or regenerative) measures may be considered. There has been a large growth in the use of these agents, while there are still limited data to support their widespread use. Data are emerging in specific locations with specific types of procedures. The more common methods have included topical glycerin nitrate patches, platelet rich plasma (PRP)/autologous blood injections, ultrasound-guided percutaneous tenotomy, extracorporal shock-wave therapy, acupuncture and other types of injections. Aggressive, augmented soft tissue mobilisation using tools during rehabilitation has also been utilised with widespread anecdotal successes, but without controlled studies demonstrating its efficacy. These types of options should be considered secondary management when traditional therapies fail and the patient also would not like to consider surgical options. Surgical treatment typically may be considered in chronic tendinopathy in severe cases where appropriate primary and secondary management has failed for >6 months and the patient is not willing to continue to try non-operative treatments. Topical glyceryl trinitrate The use of daily topical nitroglycerin patches as a non-invasive means to improve collagen synthesis to a relatively avascular tendinopathy has been shown to be effective in chronic lateral elbow tendinopathy over a 6-month period 21. This can be applied in other settings of tendinopathy in patients who have no hypotension, use of other nitrates or other contraindications. One of the frequent side-effects that may limit usefulness is migraine-like headaches but this can be limited with a start low, go slow dosing schedule. Ultrasound-guided percutaneous tenotomy Non-surgical tenotomies to address chronic tendinopathies have been studied in the elbow, Achilles and patellar tendon, but have been applied in other regions. McShane et al demonstrated that fenestrations of the tendon, breaking up of calcifications and potentially abrading the bone showed improvement in severe cases of chronic lateral elbow pain/ tendinopathy in series of patients who were considering surgery in this nonrandomised trial 22. These improvements continued even with long-term follow-up of up to 28 months with avoidance of surgery. Mafulli et al found long-term improvement with multiple longitudinal percutaneous tenotomy in mid-portion chronic Achilles tendinopathy when there was no involved paratendinopathy 23. Similar findings of improvement with percutaneous tenotomy in chronic patellar tendinopathy have also been reported. None of these studies had control groups, i.e. the quality of evidence is low. PRP injections PRP injections have been used in a variety of settings to introduce high volumes of growth factors (platelets) to promote healing when using centrifuged blood of the patient. PRP injections have more recently come into favour as secondary management for chronic tendinopathy. A small study on chronic epicondylosis suggests that 80% of patients with buffered PRP injections showed improvement, however the number of patients in the control group was small 24. Additionally, PRP injections have been evaluated in patellar tendinopathy and actually found to accelerate healing compared to eccentric strength training alone, however the treatment effect dissipated with time 25. PRP has not been shown to be effective in rotator cuff tendinopathy. Autologous blood injections These injections involve simply taking autologous blood without isolating the platelet component and injecting into chronic tendinopathy. Some feel that it is more likely that multiple treatments may be necessary compared to PRP. However, it appears that there may be a similar treatment effect with this in refractory tendinopathy, but the effect dissipates by 6 months 10. It is unclear if the effect is from the autologous blood or the dry needling (or tendon fenestrations). Extracorporal shock wave therapy This is an aggressive way to treat chronic tendinopathy. There are studies in chronic elbow tendinosis and other tendinopathies, but this isolated treatment can be quite painful and data is not convincing for its regular use. Other injections Other experimental treatments such as prolotherapy (injection of irritant), sclerosing polidocanol injections and Botulinum A injections have evidence in small supportive studies in chronic tendinopathy (typically of the elbow). There does appear to be a potential risk of transient weakness after injection with Botulinum A injections. CONCLUSIONS Tendinopathy in tennis players is generally limited to adult players where age and excess playing volume, combined with sub-optimal technique may contribute to degenerative tendinopathy. The majority of tendinopathies in tennis players are to the elbow, rotator cuff, Achilles tendon, and patellar tendon where appropriate primary management, volume reduction to reduce load, and alterations in technique where appropriate may improve symptoms. Depending on the stage of tendinopathy, a properly supervised program of eccentric strengthening rehabilitation is generally effective. Secondary management techniques and procedures have limited early and anecdotal data and should be reserved for recalcitrant cases where the player is not interested in surgery. Long term successful comprehensive programs are possible, and the need for surgical procedures is uncommon. Returning the tennis player successfully to the court may need medical and tennis specific recommendations. References Available at Neeru Jayanthi M.D., U.S.P.T.A. (United States Professional Tennis Association) Associate Professor Loyola University Chicago, Stritch School of Medicine Maywood, USA Contact: njayant@lumc.edu sports medicine in tennis TARGETED TOPIC 507
10/1/2009. October 15, 2009 Christina Kuo MD. Anatomy and pathophysiology of Epicondylitis Diagnosis
 October 15, 2009 Christina Kuo MD Anatomy and pathophysiology of Epicondylitis Diagnosis Treatment options Lawn tennis elbow Morris 1882 - described as an injury occurring from the backhand stroke Age
October 15, 2009 Christina Kuo MD Anatomy and pathophysiology of Epicondylitis Diagnosis Treatment options Lawn tennis elbow Morris 1882 - described as an injury occurring from the backhand stroke Age
Golf Injuries in the Upper Extremity
 Golf Injuries in the Upper Extremity David S. Zelouf, MD Philadelphia Hand to Shoulder Center March Meeting 2019 I have nothing to disclose Except that I m an avid, competitive golfer and I ve had golfer
Golf Injuries in the Upper Extremity David S. Zelouf, MD Philadelphia Hand to Shoulder Center March Meeting 2019 I have nothing to disclose Except that I m an avid, competitive golfer and I ve had golfer
Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions
 APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
Common Tendon Disorders of the Upper Extremity. Mark Tait MD
 Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
mechanical stresses on the tendon with repetitive loading
 Tendinopathy.. How does it happen? mechanical stresses on the tendon with repetitive loading Impingement of the tendon between adjacent structures (bones, ligaments) and impaired blood supply Presentation
Tendinopathy.. How does it happen? mechanical stresses on the tendon with repetitive loading Impingement of the tendon between adjacent structures (bones, ligaments) and impaired blood supply Presentation
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy
 Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
SPORTS MEDICINE OVERUSE MANAGEMENT PRINCIPLES FOR
 SPORTS MEDICINE OVERUSE INJURIES: DIAGNOSIS AND MANAGEMENT PRINCIPLES FOR THE FAMILY PHYSICIAN DR NG CHUNG SIEN MBBS (SPORE) MSPMED (AUSTRALIA) DFD CAW SENIOR REGISTRAR CHANGI SPORTS MEDICINE CENTRE CHANGI
SPORTS MEDICINE OVERUSE INJURIES: DIAGNOSIS AND MANAGEMENT PRINCIPLES FOR THE FAMILY PHYSICIAN DR NG CHUNG SIEN MBBS (SPORE) MSPMED (AUSTRALIA) DFD CAW SENIOR REGISTRAR CHANGI SPORTS MEDICINE CENTRE CHANGI
Elbow Muscle Power Deficits
 1 Elbow Muscle Power Deficits ICD-9-CM code: 726.32 Lateral epicondylitis ICF codes: Activities and Participation code: d4300 Lifting, d4452 Reaching, d4401 Grasping Body Structure code: s73012 Muscles
1 Elbow Muscle Power Deficits ICD-9-CM code: 726.32 Lateral epicondylitis ICF codes: Activities and Participation code: d4300 Lifting, d4452 Reaching, d4401 Grasping Body Structure code: s73012 Muscles
EPICONDYLITIS, LATERAL (Tennis Elbow)
 EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
What Are Bursitis and Tendinitis?
 Shoulder Tendinitis, Bursitis, and Impingement Syndrome What Are Bursitis and Tendinitis? Two types of tendinitis can affect the shoulder. Biceps tendinitis causes pain in the front or side of the shoulder.
Shoulder Tendinitis, Bursitis, and Impingement Syndrome What Are Bursitis and Tendinitis? Two types of tendinitis can affect the shoulder. Biceps tendinitis causes pain in the front or side of the shoulder.
Principles of Treatment. Case Studies. Principles of Treatment. Clinical Perspectives for the GP
 Principles of Treatment Clinical Perspectives for the GP Case Studies 1. Jumping athlete with an acute exacerbation of chronic patellar tendinopathy major competition in 9 days time 2 week tournament 2.
Principles of Treatment Clinical Perspectives for the GP Case Studies 1. Jumping athlete with an acute exacerbation of chronic patellar tendinopathy major competition in 9 days time 2 week tournament 2.
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
OCCUPATIONAL INJURIES OF THE ELBOW
 PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
Burwood Road, Concord 160 Belmore Road, Randwick
 www.orthosports.com.au 47 49 Burwood Road, Concord 160 Belmore Road, Randwick Conservative management of subacromial pathology Mel Cusi MBBS, Cert Sp Med, FACSP, FFSEM (UK) Presenting symptoms Shoulder
www.orthosports.com.au 47 49 Burwood Road, Concord 160 Belmore Road, Randwick Conservative management of subacromial pathology Mel Cusi MBBS, Cert Sp Med, FACSP, FFSEM (UK) Presenting symptoms Shoulder
Pilates for Brachialis Tendonitis (Tennis Elbow)
 Pilates for Brachialis Tendonitis (Tennis Elbow) Sally Dunford September 2017 Wimbledon, UK Abstract Tennis Elbow is a term used to describe a painful condition in which the tendons of the elbow are overloaded
Pilates for Brachialis Tendonitis (Tennis Elbow) Sally Dunford September 2017 Wimbledon, UK Abstract Tennis Elbow is a term used to describe a painful condition in which the tendons of the elbow are overloaded
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Lateral elbow tendinopathy
 Lateral elbow tendinopathy Lateral elbow tendinopathy is a common condition with an incidence of 1 2%. The pathology arises from the origin of extensor carpi radialis brevis where changes, consistent with
Lateral elbow tendinopathy Lateral elbow tendinopathy is a common condition with an incidence of 1 2%. The pathology arises from the origin of extensor carpi radialis brevis where changes, consistent with
Tendinopathy from Overuse: Overview and a New(er) Treatment Option
 Tendinopathy from Overuse: Overview and a New(er) Treatment Option Robert Flannery MD Assistant Professor, Division of Sports Medicine Department of Orthopedic Surgery, Case Western Reserve University
Tendinopathy from Overuse: Overview and a New(er) Treatment Option Robert Flannery MD Assistant Professor, Division of Sports Medicine Department of Orthopedic Surgery, Case Western Reserve University
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Rehabilitation Guidelines for Large Rotator Cuff Repair
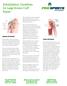 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
0RTHOPEDIC MASSAGE. Orthopedic Massage Benefits. Orthopedic Massage Applications
 0RTHOPEDIC MASSAGE Orthopedic Massage involves therapeutic assessment, manipulation, and movement of locomotor soft tissues to eliminate pain and dysfunction throughout the body. It is more than a technique.
0RTHOPEDIC MASSAGE Orthopedic Massage involves therapeutic assessment, manipulation, and movement of locomotor soft tissues to eliminate pain and dysfunction throughout the body. It is more than a technique.
Elbow Pain. Lateral Elbow Pain. Lateral Elbow Pain. tennis elbow lateral epicondylitis extensor tendinopathy
 Elbow Pain Peter Brukner OAM, FACSP Associate Professor in Sports Medicine Centre for Health, Exercise and Sports Medicine University of Melbourne Lateral Elbow Pain tennis elbow lateral epicondylitis
Elbow Pain Peter Brukner OAM, FACSP Associate Professor in Sports Medicine Centre for Health, Exercise and Sports Medicine University of Melbourne Lateral Elbow Pain tennis elbow lateral epicondylitis
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
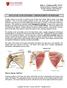 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
Elite tennis players make it look so easy and effortless. By comparison, your
 The Tennis Player in Motion C h a p t 1 e r Elite tennis players make it look so easy and effortless. By comparison, your movement skills, strokes, and fitness may leave something to be desired. Good coaches
The Tennis Player in Motion C h a p t 1 e r Elite tennis players make it look so easy and effortless. By comparison, your movement skills, strokes, and fitness may leave something to be desired. Good coaches
SHOULDER Highly mobile, so less stable. Abnormalities cloaked within extensive musculature, dx can be difficult Bony abnormalities less common than li
 SPORTS MEDICINE CASES A quick tour of some local joints Featuring gco common o and unusual problems SHOULDER Highly mobile, so less stable. Abnormalities cloaked within extensive musculature, dx can be
SPORTS MEDICINE CASES A quick tour of some local joints Featuring gco common o and unusual problems SHOULDER Highly mobile, so less stable. Abnormalities cloaked within extensive musculature, dx can be
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ELBOW INJURIES IN THE TENNIS PLAYER
 ELBOW INJURIES IN THE TENNIS PLAYER A CONCISE REVIEW Written by Brian Grawe, David Dines and Josh Dines, USA INTRODUCTION The worldwide popularity of tennis has grown in recent years and it is estimated
ELBOW INJURIES IN THE TENNIS PLAYER A CONCISE REVIEW Written by Brian Grawe, David Dines and Josh Dines, USA INTRODUCTION The worldwide popularity of tennis has grown in recent years and it is estimated
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
A Patient s Guide to Tendonitis. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Tendonitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Tendonitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Exploring the Rotator Cuff
 Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Shoulder Labral Tear and Shoulder Dislocation
 Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
UPPER EXTREMITY INJURIES. Recognizing common injuries to the upper extremity
 UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
THE OLDER TENNIS AND GOLF ATHLETE: INJURY MANAGEMENT AND PREVENTION
 THE OLDER TENNIS AND GOLF ATHLETE: INJURY MANAGEMENT AND PREVENTION William Micheo, MD Professor and Chairman Physical Medicine, Rehabilitation, and Sports Medicine Department University of Puerto Rico
THE OLDER TENNIS AND GOLF ATHLETE: INJURY MANAGEMENT AND PREVENTION William Micheo, MD Professor and Chairman Physical Medicine, Rehabilitation, and Sports Medicine Department University of Puerto Rico
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) William T. Grant, MD
 A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
Theodore B. Shybut, M.D.
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Non-operative Shoulder Rehabilitation Protocol Basic shoulder program for: o Scapular Dyskinesis (proximally
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Non-operative Shoulder Rehabilitation Protocol Basic shoulder program for: o Scapular Dyskinesis (proximally
Grundkurs SGSM-SSMS Sion Sports Elbow. Dr Stéphane Kämpfen
 Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
Dr abedi yekta. Assistant Professor of Sports and Exercise Medicine Faculty of Medicine shahid beheshti University of Medical Sciences
 Dr abedi yekta Assistant Professor of Sports and Exercise Medicine Faculty of Medicine shahid beheshti University of Medical Sciences Pain in midportion of Achilles tendon. Morning stiffness Tendinitis
Dr abedi yekta Assistant Professor of Sports and Exercise Medicine Faculty of Medicine shahid beheshti University of Medical Sciences Pain in midportion of Achilles tendon. Morning stiffness Tendinitis
Soft Tissue Rheumatism. Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group
 Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Practical Reporting of Musculoskeletal Imaging Studies: MRI Elbow
 Practical Reporting of Musculoskeletal Imaging Studies: MRI Elbow James F Griffith History Where is pain located? For how long? Trauma if so, what and when Radiographers can get this info Grade. Don t
Practical Reporting of Musculoskeletal Imaging Studies: MRI Elbow James F Griffith History Where is pain located? For how long? Trauma if so, what and when Radiographers can get this info Grade. Don t
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Achilles tendon injury
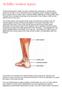 Achilles tendon injury Achilles tendinopathy is highly prevalent in athletes who participate in running-based sports but can also occur in racket sports and in sedentary people. Research suggests there
Achilles tendon injury Achilles tendinopathy is highly prevalent in athletes who participate in running-based sports but can also occur in racket sports and in sedentary people. Research suggests there
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Large/Massive Rotator Cuff Repair
 Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Extracorporeal Shockwave Therapy. Outcomes in Shoulder Tendinopathy and Plantar Fasciitis. American University of Beirut Medical Center
 Extracorporeal Shockwave Therapy. Outcomes in Shoulder Tendinopathy and Plantar Fasciitis Nagham HADDAD, PT Nagham HADDAD, PT American University of Beirut Medical Center Introduction: Tendinosis is the
Extracorporeal Shockwave Therapy. Outcomes in Shoulder Tendinopathy and Plantar Fasciitis Nagham HADDAD, PT Nagham HADDAD, PT American University of Beirut Medical Center Introduction: Tendinosis is the
Latest technology in the treatment of chronic recalcitrant tendinopathy
 Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
A Patient s Guide to Posterior Tibial Tendon Problems
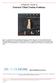 A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Arthroscopic Anterior Stabilization Rehab
 Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Tendon & Ligament Application of PRP
 Tendon & Ligament Application of PRP Sang Chul Lee, M.D, PhD. Department of Physical Medicine & Rehabilitation, Myongji hospital, Kwandong University College of Medicine Tendon and Ligament Low metabolic
Tendon & Ligament Application of PRP Sang Chul Lee, M.D, PhD. Department of Physical Medicine & Rehabilitation, Myongji hospital, Kwandong University College of Medicine Tendon and Ligament Low metabolic
Introduction. Anatomy
 the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
Adjunctive Treatments for Tendinopathy. Brendan O Neill Sports Physician Anglesea Sports Medicine Unisports Sports Medicine
 Adjunctive Treatments for Tendinopathy Brendan O Neill Sports Physician Anglesea Sports Medicine Unisports Sports Medicine About Me Sports Physician Unisports Sports Medicine Anglesea Sports Medicine BikeNZ
Adjunctive Treatments for Tendinopathy Brendan O Neill Sports Physician Anglesea Sports Medicine Unisports Sports Medicine About Me Sports Physician Unisports Sports Medicine Anglesea Sports Medicine BikeNZ
Clinical pearls for the shoulder/arm exam and the treatment. What is seeing youare you seeing it
 Clinical pearls for the shoulder/arm exam and the treatment What is seeing youare you seeing it W. Ben Kibler, MD Medical director Case 1 18 y/o R hand dominant high school pitcher, with 6 week hx gradual
Clinical pearls for the shoulder/arm exam and the treatment What is seeing youare you seeing it W. Ben Kibler, MD Medical director Case 1 18 y/o R hand dominant high school pitcher, with 6 week hx gradual
The use of Ultrasound for the Diagnosis and Treatment of the Musculoskeletal System
 The use of Ultrasound for the Diagnosis and Treatment of the Musculoskeletal System St. Joseph s Refresher Course March 2019 Kenneth Iles, DC John Finkenstadt, MD THIS WORKSHOP WILL FOCUS ON 2 MAIN TOPICS:
The use of Ultrasound for the Diagnosis and Treatment of the Musculoskeletal System St. Joseph s Refresher Course March 2019 Kenneth Iles, DC John Finkenstadt, MD THIS WORKSHOP WILL FOCUS ON 2 MAIN TOPICS:
Tendon Fenestration. Disclosures. Outline: questions. Introduction: Peritendon Steroid Injections. Jon A. Jacobson, MD. Patellar Tendon: tendinosis
 Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendinopathies Enthesopathies, Overuse Injuries and Alphabet Soup
 Tendinopathies Enthesopathies, Overuse Injuries and Alphabet Soup AMMA Brisbane 2012 COL Tony Delaney RFD MB BS FACSP Sports Physician-Musculoskeletal and Exercise Medicine, Narrabeen Sports Medicine Centre
Tendinopathies Enthesopathies, Overuse Injuries and Alphabet Soup AMMA Brisbane 2012 COL Tony Delaney RFD MB BS FACSP Sports Physician-Musculoskeletal and Exercise Medicine, Narrabeen Sports Medicine Centre
Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery
 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery These rehabilitation protocols are based on current studies detailing healing time
2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Dr. Denard s Rehabilitation Protocols Arthroscopic Shoulder Surgery These rehabilitation protocols are based on current studies detailing healing time
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
Guide to Prevention of Sports Injuries
 Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefits for your physical and mental health. While exercise and sports-related activities often have a positive
Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefits for your physical and mental health. While exercise and sports-related activities often have a positive
Small Rotator Cuff Repair
 Small Rotator Cuff Repair 1. Defined a. Surgical repair of the rotator cuff (most commonly supraspinatus muscle) utilizing sutures b. May be done arthroscopically or open. c. May be done in conjunction
Small Rotator Cuff Repair 1. Defined a. Surgical repair of the rotator cuff (most commonly supraspinatus muscle) utilizing sutures b. May be done arthroscopically or open. c. May be done in conjunction
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects
 Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
Physical Examination of the Shoulder in the Primary Care Setting 783 John M. McShane, Michael J. Graveley, and Bruce D. Hopper
 SPORTS MEDICINE, PART I Preface Vincent Morelli xiii Physical Examination of the Shoulder in the Primary Care Setting 783 John M. McShane, Michael J. Graveley, and Bruce D. Hopper Shoulder problems are
SPORTS MEDICINE, PART I Preface Vincent Morelli xiii Physical Examination of the Shoulder in the Primary Care Setting 783 John M. McShane, Michael J. Graveley, and Bruce D. Hopper Shoulder problems are
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Subacromial Bursa Injection
 Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Proximal wrist extensor tendinopathy
 Curr Rev Musculoskelet Med (2008) 1:48 52 DOI 10.1007/s12178-007-9005-0 Proximal wrist extensor tendinopathy Joseph Ihm Published online: 2 November 2007 Ó Humana Press 2007 Abstract Proximal wrist extensor
Curr Rev Musculoskelet Med (2008) 1:48 52 DOI 10.1007/s12178-007-9005-0 Proximal wrist extensor tendinopathy Joseph Ihm Published online: 2 November 2007 Ó Humana Press 2007 Abstract Proximal wrist extensor
4/12/2016. Goals. Anatomy. Basic Anatomy. Biomechanics. Function. Traumatic Rupture of Proximal Biceps: In-season Rehabilitation and Management
 Goals Traumatic Rupture of Proximal Biceps: In-season Rehabilitation and Management Thomas F. LaPorta, MD To understand the anatomy of the biceps at the shoulder To present the mechanism, signs and symptoms,
Goals Traumatic Rupture of Proximal Biceps: In-season Rehabilitation and Management Thomas F. LaPorta, MD To understand the anatomy of the biceps at the shoulder To present the mechanism, signs and symptoms,
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
Dr Hamish Osborne. Sport & Exercise Medicine Physician Dunedin
 Dr Hamish Osborne Sport & Exercise Medicine Physician Dunedin New Approaches to Handling Tendinopathies By Hamish Osborne Definition Tendinopathy Absence of tightly packed collagen bundles Large amount
Dr Hamish Osborne Sport & Exercise Medicine Physician Dunedin New Approaches to Handling Tendinopathies By Hamish Osborne Definition Tendinopathy Absence of tightly packed collagen bundles Large amount
WEEKEND 2 Elbow. Elbow Range of Motion Assessment
 Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Elbow Elbow Range of Motion Assessment - Patient Positioning: Sitting or supine towards the edge of the bed - Indications:
Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Elbow Elbow Range of Motion Assessment - Patient Positioning: Sitting or supine towards the edge of the bed - Indications:
Rotator Cuff Tears. Dr. Anthony Levenda September, 2017
 Rotator Cuff Tears Dr. Anthony Levenda September, 2017 Rotator cuff tears come in a variety of shapes and sizes. No two are exactly the same, and as such, they are not all treated the same. It is important
Rotator Cuff Tears Dr. Anthony Levenda September, 2017 Rotator cuff tears come in a variety of shapes and sizes. No two are exactly the same, and as such, they are not all treated the same. It is important
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendinopathy in dancers, 831 832 treatment of PRP in, 871 872 Achilles tendinopathy/tendonitis in ultramarathon athletes, 847
Index Note: Page numbers of article titles are in boldface type. A Achilles tendinopathy in dancers, 831 832 treatment of PRP in, 871 872 Achilles tendinopathy/tendonitis in ultramarathon athletes, 847
Upper Limb Biomechanics SCHOOL OF HUMAN MOVEMENT STUDIES
 Upper Limb Biomechanics Phases of throwing motion 1. Wind up Starts: initiate first movement Ends: lead leg is lifted & throwing hand removed from glove COG raised 2. Early Cocking Start: lead leg is lifted
Upper Limb Biomechanics Phases of throwing motion 1. Wind up Starts: initiate first movement Ends: lead leg is lifted & throwing hand removed from glove COG raised 2. Early Cocking Start: lead leg is lifted
*Agonists are the main muscles responsible for the action. *Antagonists oppose the agonists and can help neutralize actions. Since many muscles have
 1 *Agonists are the main muscles responsible for the action. *Antagonists oppose the agonists and can help neutralize actions. Since many muscles have more than 1 action sometimes a muscle has to neutralize
1 *Agonists are the main muscles responsible for the action. *Antagonists oppose the agonists and can help neutralize actions. Since many muscles have more than 1 action sometimes a muscle has to neutralize
Servers Disease (Calcaneal Apophysitis ) 101
 Servers Disease (Calcaneal Apophysitis ) 101 Servers Disease Causes a disturbance to the growing area at the back of the heel bone (calcaneus) where the strong Achilles tendon attaches to it. It is most
Servers Disease (Calcaneal Apophysitis ) 101 Servers Disease Causes a disturbance to the growing area at the back of the heel bone (calcaneus) where the strong Achilles tendon attaches to it. It is most
SHOULDER PAIN. A Real Pain in the Neck. Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017
 SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
Secrets and Staples of Training the Athletic Shoulder
 Secrets and Staples of Training the Athletic Shoulder Eric Beard Corrective Exercise Specialist Athletic Performance Enhancement Specialist EricBeard.com AthleticShoulder.com Presentation Overview Rationale
Secrets and Staples of Training the Athletic Shoulder Eric Beard Corrective Exercise Specialist Athletic Performance Enhancement Specialist EricBeard.com AthleticShoulder.com Presentation Overview Rationale
Impingement syndrome. Clinical features. Management. Rotator cuff tear diagnosed. Go to rotator cuff tear
 Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
Impingement syndrome Clinical features Management Poor response Good response Refer to orthopaedic surgery R Review as appropriate Investigations Rotator cuff tear diagnosed Go to rotator cuff tear Consider
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Monster Walk Stand with your feet slightly closer than shoulder-width apart in an athletic stance. Loop an elastic band around your ankles.
 Off-season Lower-Body Tennis Exercises Research conducted on elite tennis players shows that lower-body strength is the same on both the left and right sides. Therefore, lower-body training for tennis
Off-season Lower-Body Tennis Exercises Research conducted on elite tennis players shows that lower-body strength is the same on both the left and right sides. Therefore, lower-body training for tennis
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop. W. Scott Black, MD Physician Assistant Studies Program University of Kentucky
 KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
Disclosures Head to Toe: Common Sports Injuries in Kids
 Disclosures Head to Toe: Common Sports Injuries in Kids None R. Jay Lee MD Director Pediatric Orthopaedic Fellowship Assistant Professor Pediatric Orthopaedics Johns Hopkins / Bloomberg Children s Objectives
Disclosures Head to Toe: Common Sports Injuries in Kids None R. Jay Lee MD Director Pediatric Orthopaedic Fellowship Assistant Professor Pediatric Orthopaedics Johns Hopkins / Bloomberg Children s Objectives
Shoulder Instability and Tendon Injuries
 Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a
A Patient s Guide to Posterior Tibial Tendon Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a
Elbow injuries in athletes
 Elbow injuries in athletes Babette Pluim IOC Advanced Team Physician s Course, Oslo Case # 1 13 yr old junior elite tennis player Medial and lateral elbow pain 24-month history with episodes of elbow pain,
Elbow injuries in athletes Babette Pluim IOC Advanced Team Physician s Course, Oslo Case # 1 13 yr old junior elite tennis player Medial and lateral elbow pain 24-month history with episodes of elbow pain,
Overuse Injuries. Dr. John Greco 927 Franklin Street, Huntsville, AL /
 Overuse Injuries There are basically two types of injuries: acute injuries and overuse injuries. Acute injuries are usually the result of a single, traumatic event. Common examples include wrist fractures,
Overuse Injuries There are basically two types of injuries: acute injuries and overuse injuries. Acute injuries are usually the result of a single, traumatic event. Common examples include wrist fractures,
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity
 Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Anterior knee pain.
 Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
Core deconditioning Smoking Outpatient Phase 1 ROM Other
 whereby the ball does not stay properly centered in the shoulder socket during shoulder movement. This condition may be associated with impingement of the rotator cuff on the acromion bone and coracoacromial
whereby the ball does not stay properly centered in the shoulder socket during shoulder movement. This condition may be associated with impingement of the rotator cuff on the acromion bone and coracoacromial
ORTHOPAEDIC SUMMIT 2016
 Injuries to the Extensor Mechanism Quadriceps & Patellar tendon Pearls and Pitfalls M.Mike Malek, M.D. Washington Orthopaedic and Knee Clinic ORTHOPAEDIC SUMMIT 2016 Las Vegas, Nevada December 8, 2016
Injuries to the Extensor Mechanism Quadriceps & Patellar tendon Pearls and Pitfalls M.Mike Malek, M.D. Washington Orthopaedic and Knee Clinic ORTHOPAEDIC SUMMIT 2016 Las Vegas, Nevada December 8, 2016
REMINDER. Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns
 Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems 2659 Professional Circle Suite 1110 Naples, FL 34119 Phone: 239-596-0100 Fax: 239-596-6737 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Posterior Tibial Tendon Problems 2659 Professional Circle Suite 1110 Naples, FL 34119 Phone: 239-596-0100 Fax: 239-596-6737 DISCLAIMER: The information in this booklet is compiled
