Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review
|
|
|
- Sharyl Cooper
- 6 years ago
- Views:
Transcription
1 Techniques in Knee Surgery 5(1):47 52, 2006 T E C H N I Q U E Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review Shane J. Nho, MD, Christopher C. Dodson, MD, and Thomas L. Wickiewicz, MD Sports Medicine and Shoulder Service, The Hospital for Special Surgery Weil Medical College of Cornell University New York, New York, U.S.A. Nikhil N. Verma, MD Section of Sports Medicine, Department of Orthopedic Surgery Rush Medical College, Rush University Medical Center Chicago, Illinois, U.S.A. Ó 2006 Lippincott Williams & Wilkins, Philadelphia ABSTRACT Isolated patellofemoral osteoarthritis is poorly understood problem without a definitive treatment. The purpose of the study is to present a technique combining lateral patellectomy with concomitant tibial tubercle elevation. In a retrospective review, four patients with an average follow-up of 62 months were evaluated with postoperative clinical examination, International Knee Documentation Committee (IKDC) scoring scale, visual analog scale (VAS), and plain radiographs. The mean IKDC score was 59 (range, 35 to 72). The mean VAS score was 6.3 mm (range, 0 mm to 13 mm) out of a possible 100 mm. All four patients were able to return to a moderate level of activity without significant knee pain. Three of four patients expressed no difficulty or minimal difficulty with stair climbing and kneeling, but one patient reported moderate difficulty to the same questions. All patients demonstrated hardware in the same position as the intra-operative radiographs, hemipatella centrally located in the trochlea sulcus, and healing of the tibial osteotomy. Although both the lateral facetectomy and the Maquet tibial tubercle elevation have previously described, the two procedures have not been performed concurrently, and together the combined approach may address the existing patellofemoral osteoarthritis, prevent progression of joint degeneration, limit complications associated with tibial tubercle elevation, and avoid donor site morbidity with iliac crest bone graft. Keywords: patellofemoral osteoarthritis, lateral patellectomy, tibial tubercle osteotomy, extensor realignment Address correspondence and reprint requests to Thomas L. Wickiewicz, The Hospital for Special Surgery, 535 East 70th Street, New York, NY 10021, U.S.A. wickiewiczt@hss.edu. HISTORICAL PERSPECTIVE Patellofemoral osteoarthritis in isolation or in combination with tibiofemoral compartment degeneration is an important cause of knee pain and disability. In patients older than sixty years, the prevalence of patellofemoral joint space narrowing is 32.7% in men and 36.1% in women, and isolated patellofemoral compartment degeneration occurs in 15.4% of men and 13.6% of women. 1 For the treatment of isolated patellofemoral osteoarthritis, Maquet described a surgical technique involving a 2.0 to 2.5 cm anterior advancement of the tibial tubercle. 6,8 The rationale behind the procedure was to decrease the force and enlarge the contact area of the patellofemoral joint by anterior displacement of the tibial tubercle. Maquet and other investigators 4Y6,13 reported good initial clinical results for the treatment of patellofemoral osteoarthritis; however, there have also been a high rate of complications associated with the originally described technique including fractures of the osseous shingle, nonunion, wound infections, and osteomyelitis. 2 The amount of anterior elevation of the tibial tubercle has been the subject of much debate, and the technique has been modified by several investigators to attempt to limit the complications. Biomechanical studies have demonstrated that 1.25 cm of patella tendon elevation reduces the average stress on the patellofemoral joint by greater than 80%. 2 However, depending on the direction of tubercle advancement, the contact pressure of the proximal and medial aspects of the patella may actually increase with tubercle osteotomy. In 1986, Radin 8 conducted a study to evaluate the effect of elevation of the anterior tibial tubercle. In a prospective study of 53 patients and greater than 2 year follow-up, he compared three groups with differing Volume 5, Issue 1 47
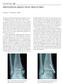
2 Nho et al degrees of elevation: 2.0Y2.5 cm, classic Maquet; 1.5Y2.0 cm, modified Maquet; and 1.25 cm, Ferguson modification. Eleven of 12 patients in the classic Maquet group had satisfactory results, but five of 12 had complications including three with slow wound healing, fracture of the tibial shingle, and thrombophlebitis. Of the 32 patients in the modified Maquet group, 30 had satisfactory results, and only five of the 32 patients had complications including 2 with thrombophlebitis, delayed wound healing, osteomyelitis, and lateral compartment syndrome. Six of 9 patients in the Ferguson modification group had satisfactory results, and two patients developed postoperative hemorrhage that developed thrombophlebitis. The author concluded that the modified Maquet procedure is an effective procedure with relatively low incidence of complications. Radin and Pan 9 reviewed 42 knees that underwent the modified Maquet procedure with an average follow-up of 6.1 years and determined that 79% had good to excellent results. The patients were divided into groups according to etiology of osteoarthritis: the post-traumatic osteoarthritis group had 86% excellent and good results, osteoarthritis secondary to recurrent subluxation group had 75% excellent and good results, and osteoarthritis after patellectomy group had 50% with good results. The failures were attributed to patients with psychosocial reasons and unrecognized tibiofemoral osteoarthritis. The complications observed included two nonunions, osteomyelitis, and distal tibial shingle fractures. With an average follow-up of 16 years, Schmid 11 reported 80% very good and good results of 35 knees after the Maquet procedure. There appeared to be a correlation with amount of tibial tubercle elevation and clinical outcome; that is, the greater the elevation, the better the result. The patients with unsatisfactory results were attributed to undetected tibiofemoral degeneration and inadequate advancement of the tibial tubercle. In 1990, Martens and De Rycke 7 described a procedure involving a 1 cm excision of the lateral border of the patella with a simultaneous lateral release. Out of a total of twenty patients with an average age of 60 years and a mean follow-up of two years, there were 13 good, 5 moderate, and 2 poor results. The 5 patients with moderate scores had some improvement in pain but functional disability with long distance and stair climbing. The 2 patients with poor results had marked degeneration in tibiofemoral compartment and demonstrated no symptomatic improvement and no further deterioration. Eight of seventeen patients also demonstrated progression of osteoarthritis in the patellofemoral compartment. In the present study, the authors present a surgical technique that combines the anterior tibial tubercle elevation with lateral facetectomy for the treatment of isolated lateral facet patellofemoral osteoarthritis. Using the described technique, the surgeon is able to treat the existing patellofemoral osteoarthritis through the lateral facetectomy and to decrease contact pressure in the remaining patellofemoral joint through elevation of the tibial tubercle. The purpose of this study is to present the surgical technique for lateral facet hemipatellectomy with anterior tibial tubercle transfer, and to present the clinical results of a series of cases treated with this technique. INDICATIONS AND CONTRAINDICATIONS Patellofemoral osteoarthritis may involve the articular surface of patella and/or the trochlea. 10 The lateral facet of the patella is the most common area of cartilage degeneration seen both clinically and in autopsy studies 3 and implies that the lateral facet experiences varying degrees of tilt, maldistribution of force, or malalignment. 10 Soft tissue realignment procedure may be indicated for patellofemoral arthritis with radiographic evidence of tilt without subluxation or instability. 10 A young patient presenting with anterior knee pain, extensor malalignment, and isolated patellofemoral joint degeneration may be appropriate for lateral patellectomy with tibial tubercle elevation. The extent of patellofemoral osteoarthritis must be confined to the lateral facet but the severity of disease may vary. The lateral patellectomy will directly address the patella, and the tibial tubercle elevation will unload and prevent further progression of the entire patellofemoral joint. In this setting, the trochlea chondral lesion may be amenable to a cartilage repair procedure such as debridement, microfracture, osteochondral autograft, osteochondral allograft, or autologous chondrocyte implantation. 12 Contraindications to lateral patellectomy with tibial tubercle elevation include patellofemoral arthritis involving the central ridge and medial facet, the presence of tibiofemoral joint degeneration, and ligamentous instability. PREOPERATIVE PLANNING All patients had plain radiographs as part of the preoperative evaluation including, anteroposterior, 45 degree flexion lateral, and Merchant views. Patients typically demonstrate patellofemoral joint space narrowing, lateral tilt, lateral displacement, and osteosclerosis with osteophyte formation seen on Merchant and lateral views (Fig. 1). The orientation of the patella within the trochlea groove will dictate the appropriate tibial tubercle osteotomy. Tilting of the patella may benefit from lateral release, whereas lateral patella subluxation may require medialization in addition to the anterior elevation of the tibial tubercle to centralize the patella. The tibiofemoral 48 Techniques in Knee Surgery
3 Lateral Patellectomy With Anterior Tibial Tubercle Elevation trochlea lesion must also be addressed with cartilage repair techniques depending on the patient, location, and chondromalacia grade. 12 Although outside of scope of the present article, the possibility of debridement, microfracture, osteochondral autograft, osteochondral allograft, or autologous chondrocyte implantation must be planned prior to surgery and may influence the postoperative rehabilitation. FIGURE 1. Preoperative radiographs of isolated patellofemoral osteoarthritis. A, Anteroposterior view. B, Sunrise view demonstrating joint space narrowing and tilt of the lateral facet with osteophytes. Gray lines demonstrate the resection of the sclerotic bone from the lateral facet at roughly 60 degrees from the patella ridge. joint must also be assessed to determine the presence of osteoarthritis and overall alignment of the knee. A preoperative magnetic resonance image may be obtained prior to the procedure to assess the articular surface of the patella and trochlea. Although the patella chondral lesion will be resected, the corresponding TECHNIQUE After administration of epidural anesthesia, the patient is placed in a supine position with a tourniquet wrapped in the proximal thigh of the operative leg. Physical examination under anesthesia is performed to assess range of motion, patella tracking, and ligament stability. All patients undergo a complete diagnostic arthroscopy to evaluate the extent of patellofemoral disease as well as a global assessment of intra-articular pathology. In our series, all patients had severe degenerative change in the patellofemoral joint with Grade IV full thickness chondral lesions and eburnated subchondral bone involving greater than 50% of the lateral facet. One patient also demonstrated Grade II chondral lesions of the medial facet. The two patients with a history of recurrent patella dislocations also had evidence of chondromalacia of the lateral trochlea directly inferior to the lateral facet. Following diagnostic arthroscopy, a standard midline incision is created from 3 cm proximal to the superior patellar pole extending distally to the tibial tubercle. Soft tissue dissection is continued through the subcutaneous tissue to the level of the prepatellar bursa, and a flap is elevated laterally to the lateral edge of the patella extending distally to the tibial tubercle. If there is evidence of patella tilt, a lateral release is performed beginning at the superolateral border of the patella staying just distal to the vastus lateralis, through the lateral retinaculum, and continuing distally along the lateral aspect of the patellar tendon to its insertion into the tibial tubercle. The electrocautery is used to incise through the infrapatellar fat pad with careful attention to avoid injury to the lateral meniscus. Once the arthrotomy is complete, the patella is inverted and the articular surface is meticulously examined to characterize the location, size, and Outerbridge grade of the chondral and subchondral pathology. A scalpel is used to separate the superficial fascia overlying the patella from the anterior surface of the patella, exposing the entire lateral facet. Typically with lateral facet osteoarthritis, there is a demarcation from exposed sclerotic bone of the lateral facet and the remaining articular cartilage of the remaining patella. This is the point of resection on the articular side. The pre-patella cortex lateral is preserved for the purpose of cosmetic contour and bone stock in the event that a future total knee Volume 5, Issue 1 49
4 Nho et al arthroplasty is required. The lateral patellectomy is performed with an oscillating saw at the demarcation between the sclerotic bone and articular cartilage with an oblique angle at 60 degrees toward the patella ridge (Fig. 1B). The resection is continued proximally to the superior pole and distally to the inferior pole of the patella. The lateral facet is passed off the table and saved for bone graft. A curette is used to remove adjacent areas of full thickness cartilage loss and to create a smooth contour of the cut edge of the patella. A Kirschner wire is used to create multiple holes through the subchondral bone to stimulate the fibrocartilaginous repair. After the resection, care must be taken to ensure there is no contact between the lateral patella and the trochlea whereas the knee is taken through a range of motion. The tibial tubercle is identified and the overlying soft tissue and anterior compartment muscle is removed with a periosteal elevator to provide exposure of the medial and lateral cortices. The medial cut is 5 mm posterior to the cortex and angled 45 degrees, and the lateral cut is 7 mm posterior to the cortex along the coronal plane. Both cuts are extended distally and converged at 5 cm from the surface of the tibial plateau to create a triangular osteotomy with a broad proximal base. With a 4.5 drill bit, a proximal hole is created through the anterior cortex just distal to the patellar tendon insertion. A second hole is drilled at the distal end of the bone block. Two one inch osteotomes are placed at the most distal aspect of the osteotomies and used to carefully elevate the bone block 15 mm without creating a fracture through the intact distal cortex. If the patella is laterally subluxed in the trochlear groove, tibial tubercle medialization as well as elevation may be performed to centralize the resected patella. The lateral facet is prepared by removing cartilage from the articular surface and soft tissue from the anterior surface. The lateral facet is used as autologous bone graft and impacted under the elevated tubercle at the most proximal end. A 3.2 drill is continued through the previously drilled proximal and distal holes through the posterior cortex. A 6.5 fully threaded bi-cortical cancellous screw is placed through the proximal hole. A second 6.5 mm screw is placed in the distal hole to achieve secure fixation of the osteotomy. The knee is then manipulated through a complete range of motion with close attention to patella tracking. The patella is confirmed to be in the well seated in the central ridge without excessive tilt or translation. The tourniquet is taken down and adequate hemostasis is achieved. The wound is copiously irrigated with normal saline. The lateral release is maintained and a Constavaci CBCII (Stryker, Kalamazoo, MI) drain was placed. The superficial subcutaneous tissue is closed with interrupted inverted 0 Vicryl (Ethicon, Inc., Somerville, NJ) sutures, and the skin is closed with a running 2-0 Prolene (Ethicon, Inc., Somerville, NJ) suture. A sterile dressing is applied with a Robert Jones dressing. The leg is placed in a Bledsoe brace (Bledsoe brace systems, Grand Prairie, TX) locked in extension. RESULTS Six patients from October 1998 to February 2000 with isolated lateral facet patellofemoral osteoarthritis were treated with lateral hemipatellectomy, lateral release, and anterior tibial tubercle osteotomy. Two patients were lost to follow-up, and the remaining four patients had an mean age of 36 years (range, 25 to 51 years) with an average follow-up period of 62 months (range, 58 to 67 months). All patients included in the study completed questionnaires with International Knee Documentation Committee (IKDC) Score, Visual Analog Scale (VAS), and radiographs were included in the analysis. All patients underwent informed consent process, and the study was approved by the Institutional Review Board at the Hospital for Special Surgery. All four patients were females involving three right knees and one left knee. Two patients had a history of recurrent patella dislocations, one patient sustained direct trauma to the patella in a motor vehicle accident with sympathetic dystrophy, and the last patient had an insidious onset of patellofemoral joint degeneration. Prior to the index procedure, one patient had previously had a lateral release, debridement, and microfracture of the lateral facet of the patella, another patient underwent arthroscopic debridement of the patella chondral surface, and a third patient had failed medial imbrication. On physical examination, all patients demonstrated varying degrees of pain, effusions, and crepitus with range of motion. The two patients with recurrent patella dislocations demonstrated valgus alignment and had apprehension with lateral patella subluxation. One patient had undergone previous partial medial meniscectomy and continued to have mild medial joint line tenderness, but demonstrated no mechanical symptoms. All knees had normal stability to Lachman, posterior drawer, varus and valgus stress testing. All patients demonstrated patellofemoral joint space obliteration, lateral tilt, lateral displacement, and osteosclerosis with osteophyte formation seen on Merchant and lateral views (Fig. 1). Three patients did not show any evidence of joint degeneration in the medial and lateral compartments. One patient had minimal joint space narrowing in the other two compartments consistent with mild osteoarthritis. Four patients with an average age of 36 years (range, 24 to 51 years) at the time of surgery and an average follow-up of 62 months (range, 58 to 67 months) were 50 Techniques in Knee Surgery
5 Lateral Patellectomy With Anterior Tibial Tubercle Elevation available for review. All patients included in the study underwent lateral hemipatellectomy with anterior tibial tubercle elevation. Two patients had adjacent lateral trochlea cartilage lesions. One patient with a Grade IV trochlear defect underwent a microfracture of the defect, and one patient with a Grade III trochlear defect underwent debridement of the defect. All patients completed questionnaires with the clinical outcome measures to determine overall assessment of the knee including IKDC and subjective visual analog pain scales (VAS). The mean IKDC score was 59 (range, 35 to 72). The mean VAS score was 6.3 mm (range, 0 mm to 13 mm) out of a possible 100 mm. All four patients were able to return to a moderate level of activity without significant knee pain. Three of four patients expressed no difficulty or minimal difficulty with stair climbing and kneeling, but one patient reported moderate difficulty to the same questions. Postoperative radiographs were obtained at six weeks after surgery and twelve weeks after surgery to assess position of the hardware and evidence of osseous consolidation of the tibial tubercle osteotomy. At most recent follow-up, all patients demonstrated hardware in the same position as the intra-operative radiographs, hemipatella centrally located in the trochlea sulcus, and healing of the tibial osteotomy (Fig. 2). COMPLICATIONS The most common complication associated with the procedure is pain over the tibial tubercle screws. The procedure involves anterior elevation of the tibial tubercle which makes an existing bony prominence more proud, and the screws further exacerbate the problem on a sensitive extensor surface. Of the four patients, two required a second procedure to remove the screws after adequate osseous healing was evident on plain radiographs. One patient sustained postoperative weakness of the extensor hallicus longus muscle presumably thought to be due to subclinical anterior compartment syndrome. Prior to this incident, an anterior fasciotomy was performed when clinically indicated at the time of surgery; after the incident, however, all patients underwent prophylactic anterior compartment fasciotomy. Of the patients in the series, two patients also had concomitant anterior compartment fasciotomy. POSTOPERATIVE MANAGEMENT After surgery, patients begin continuous passive motion beginning from 0Y60 degrees to a goal of 90 degrees and patients are able to weight bear as tolerated with a Bledsoe brace locked in extension. At the six week postoperative visit, the patient is advanced to full weight bearing out of the brace if plain radiographs demonstrate evidence of healing of the osteotomy. Patients should continue physical therapy with an emphasis on quadriceps strengthening and open chain knee extension exercises. POSSIBLE CONCERNS, FUTURE OF TECHNIQUE Of the patients in our clinical series, there appeared to be two distinct subsets of patients. Two of the patients were recurrent dislocators with valgus alignment and kissing chondral lesions on the lateral patella facet and lateral trochlea. The other two patients were non-dislocators FIGURE 2. Postoperative radiographs after tibial tubercle anterior elevation and lateral patellectomy. A, Anteroposterior view. B, Sunrise view demonstrating resection of the lateral hemipatella and congruent patellofemoral joint. C, Lateral view demonstrating excellent healing of the anterior tibial tubercle. Volume 5, Issue 1 51
6 Nho et al TABLE 1. Characteristics of patients with patellofemoral osteoarthritis Patient Age/ gender Follow-up (months) Mechanism of injury Additional procedure(s) IKDC VAS Comments 1 24/F 60 Direct impact Lateral release, anterior Painful hardware fasciotomy 2 51/F 58 Insidious 72 0 EHL paralysis 3 25/F 62 Recurrent dislocations Lateral release, microfracture 61 3 Painful hardware lateral trochlea 4 43/F 67 Recurrent dislocations Lateral release, anterior fasciotomy, lateral trochlea debridement 35 9 with normal alignment and a lack of degeneration of the lateral trochlea. Those patients with recurrent dislocations had IKDC scores of 61 and 35 compared with the non-dislocators with IKDC scores of 72 and 69 (Table 1). Interestingly, there appeared to be no difference in VAS scores between recurrent dislocators and non-dislocators. Given the small sample size, it is difficult to determine the rationale behind the performance of the two groups but likely to be a combination of alignment, stability, and degree of chondromalacia of the underlying lateral trochlea. Lateral patellectomy and anterior tibial tubercle elevation is an excellent treatment of patients with isolated patellofemoral osteoarthritis. There are a number of theoretical and practical advantages in the combined technique. The described approach is based on the treatment of patellofemoral osteoarthritis by resection of the lateral facet and the reduction of the compressive loads across the patellofemoral joint by anterior elevation of the tibial tubercle. Performing both procedures concomitantly allow the use of the lateral facet as autogenous bone graft for the anterior tibial tubercle elevation, thereby avoiding an additional procedure to obtain iliac crest bone graft. A lateral release or tibial tubercle anteromedialization may also be performed if there is evidence of patella tilt or maltracking, respectively. The degree of chondromalacia of the lateral trochlea must also be addressed and may be treated with debridement, microfracture, osteochondral autograft, osteochondral allograft, or autologous chondrocyte implantation. Isolated patellofemoral joint degeneration is a poorly understood problem without a reliable treatment. A number of different treatments have been described, but no single technique is considered to be the definitive treatment of isolated patellofemoral osteoarthritis. Although both the lateral facetectomy and the Maquet tibial tubercle elevation have previously described, the two procedures have not been performed concurrently, and together the combined approach may address the existing patellofemoral osteoarthritis, prevent progression of joint degeneration, limit complications associated with tibial tubercle elevation, and avoid donor site morbidity with iliac crest bone graft. ACKNOWLEDGEMENT No authors received financial support for the research or preparation of the manuscript. REFERENCES 1. Davies AP, Vince AS, Shepsonte L, et al. The radiographic prevalence of patellofemoral osteoarthritis. Clin Orthop. 2002;402:206Y Ferguson AB Jr, Brown TD, Fu FH, et al. Relief of patellofemoral contact stress by anterior displacement of the tibial tubercle. J Bone Joint Surg Am. 1979;61:159Y Fulkerson JP, Hungerford DS. Patellar tilt/compression and the excessive lateral pressure syndrome (ELPS). In: Fulkerson JP, Hungerford DS eds. Disorders of the patellofemoral joint. Baltimore, MD: Williams and Wilkins, 1990:102Y Kaufer H. Mechanical function of the patella. J Bone Joint Surg Am. 1971;53:1551Y Maquet PGJ. Biomechanics of the knee. With applications to the pathogenesis and the surgical treatment of osteoarthritis. Berlin-Heidelberg: Springer-Verlag, Maquet PGJ. Consideration biomechanique sur L arthrose du genou. Un traitment biomechanique de l arthrose femoropatellaire. L Advancement du tendon rotulien. Rev Rheum Mal Osteoartic. 1963;30: Martens M, De Rycke J. Facetectomy of the patella inpatellofemoral osteoarthritis. Acta Orthop Belg. 1990;56:563Y Radin EL. The Maquet procedure - anterior displacement of the tibial tubercle. Clin Orthop. 1986;213:241Y Radin EL, Pan HQ. Long-term follow-up study on the Maquet procedure with special reference to the causes of failure. Clin Orthop. 1993;290:253Y Saleh KJ, Arendt EA, Eldridge J, et al. Symposium: Operative treatment of patellofemoral arthritis. J Bone Joint Surg Am. 2005;87:659Y Schmid F. The Maquet procedure in the treatment of patellofemoral osteoarthrosis. Long-term results. Clin Orthop. 1993;294:254Y Sellards RA, Nho SJ, Cole BJ. Chondral injuries. Curr Opin Rheumatol. 2002;14:134Y Waisbrod H, Treiman N. Intra-osseous venography in patellofemoral disorders. A preliminary report. J Bone Joint Surg Br. 1980;62-B:454Y Techniques in Knee Surgery
Which treatment? How I do a Maquet Osteotomy? Maquet: Maquet: Biomechanics. Maquet: /21/10. Philippe Landreau, MD
 Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
IKDC DEMOGRAPHIC FORM
 IKDC DEMOGRAPHIC FORM Your Full Name Your Date of Birth / / Your Social Security Number - - Your Gender: Male Female Occupation Today s Date / / The following is a list of common health problems. Please
IKDC DEMOGRAPHIC FORM Your Full Name Your Date of Birth / / Your Social Security Number - - Your Gender: Male Female Occupation Today s Date / / The following is a list of common health problems. Please
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
3/13/2018. Cartilage Cases. Case. Physical exam
 Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
PRONATION-ABDUCTION FRACTURES
 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
Technique Guide. 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Extensor Mechanism Rupture
 Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity
 ORTHOPEDICS May 2009;32(5):360. Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity by John P. Meehan, MD; Mohammad A. Khadder, MD; Amir A. Jamali,
ORTHOPEDICS May 2009;32(5):360. Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity by John P. Meehan, MD; Mohammad A. Khadder, MD; Amir A. Jamali,
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14 BEFORE: A. T. Patterson: Vice-Chair HEARING: November 3, 2014 at Toronto Oral DATE OF DECISION: April 17, 2015 NEUTRAL CITATION: 2015
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14 BEFORE: A. T. Patterson: Vice-Chair HEARING: November 3, 2014 at Toronto Oral DATE OF DECISION: April 17, 2015 NEUTRAL CITATION: 2015
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with:
 Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Maquet III procedure: what remains after initial complications - long-term results
 Fonseca et al. Journal of Orthopaedic Surgery and Research 2013, 8:11 RESEARCH ARTICLE Open Access Maquet III procedure: what remains after initial complications - long-term results Fernando Fonseca 1,2*,
Fonseca et al. Journal of Orthopaedic Surgery and Research 2013, 8:11 RESEARCH ARTICLE Open Access Maquet III procedure: what remains after initial complications - long-term results Fernando Fonseca 1,2*,
Custom Patellofemoral Arthroplasty of the Knee. Surgical Technique
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Custom Patellofemoral Arthroplasty of the Knee. Surgical Technique Domenick
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Custom Patellofemoral Arthroplasty of the Knee. Surgical Technique Domenick
Disclosures. Why Osteotomy? Osteotomies of the Knee Indications, Techniques and Outcomes
 Osteotomies of the Knee Indications, Techniques and Outcomes Tom Minas MD MS Director, Cartilage Repair Center BWH Associate Professor HMS, Boston Ma www.cartilagerepaircenter.org Disclosures Vericel (
Osteotomies of the Knee Indications, Techniques and Outcomes Tom Minas MD MS Director, Cartilage Repair Center BWH Associate Professor HMS, Boston Ma www.cartilagerepaircenter.org Disclosures Vericel (
Osteochondritis Dissecans of the Knee. M Lucas Murnaghan MD, MEd, FRCSC
 Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Nearly all of these fractures are displaced, given the paucity of soft tissue attachments.
 CAPITELLAR FRACTURE Vasu Pai Nearly all of these fractures are displaced, given the paucity of soft tissue attachments. Nonsurgical management is fraught with complications including chronic pain, mechanical
CAPITELLAR FRACTURE Vasu Pai Nearly all of these fractures are displaced, given the paucity of soft tissue attachments. Nonsurgical management is fraught with complications including chronic pain, mechanical
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Evaluation and Treatment of Knee Arthritis Classification of Knee Arthritis Osteoarthritis Osteoarthritis Osteoarthritis of Knee
 1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT
 GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large
GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large
Joint-Preserving Osteotomies for Isolated Patellofemoral Osteoarthritis: Alternatives to Arthroplasty
 Joint-Preserving Osteotomies for Isolated Patellofemoral Osteoarthritis: Alternatives to Arthroplasty Am J Orthop. 2017 May;46(3):139-145 Authors: Vicente Sanchis-Alfonso, MD, PhD Jason L. Koh, MD, MBA
Joint-Preserving Osteotomies for Isolated Patellofemoral Osteoarthritis: Alternatives to Arthroplasty Am J Orthop. 2017 May;46(3):139-145 Authors: Vicente Sanchis-Alfonso, MD, PhD Jason L. Koh, MD, MBA
Original Date: December 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Patellofemoral Osteoarthritis
 Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
I have nothing to disclose
 Management of Common Knee Disorders: What You Knee d to Know UCSF Essentials of Women s Health July 8, 2015 Carlin Senter, M.D. I have nothing to disclose Learning objectives: in 1 hour you will be able
Management of Common Knee Disorders: What You Knee d to Know UCSF Essentials of Women s Health July 8, 2015 Carlin Senter, M.D. I have nothing to disclose Learning objectives: in 1 hour you will be able
Tibial Tubercle Osteotomy
 Techniques in Knee Surgery 2(1):28 42, 2003 T E C H N I Q U E 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Tibial Tubercle Osteotomy JACK FARR, M.D. Clinical Associate Professor of Orthopaedic
Techniques in Knee Surgery 2(1):28 42, 2003 T E C H N I Q U E 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Tibial Tubercle Osteotomy JACK FARR, M.D. Clinical Associate Professor of Orthopaedic
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Chondral Disease of the Knee
 Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Malalignment can affect any of the three
 ch05_anbari:layout 1 8/20/2009 2:12 PM Page 47 C H A P T E R 5 Osteotomies: High Tibial, Distal Femoral, and Tibial Tubercle Ammar Anbari, MD Malalignment can affect any of the three compartments of the
ch05_anbari:layout 1 8/20/2009 2:12 PM Page 47 C H A P T E R 5 Osteotomies: High Tibial, Distal Femoral, and Tibial Tubercle Ammar Anbari, MD Malalignment can affect any of the three compartments of the
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Novel Techniques in Articular Cartilage Restoration
 21 Novel Techniques in Articular Cartilage Restoration Adam B. Yanke, MD and Brian J. Cole, MD, MBA PART ONE: DENOVO NT Introduction DeNovo NT (Zimmer) is minced (1-mm cubes) juvenile allograft cartilage
21 Novel Techniques in Articular Cartilage Restoration Adam B. Yanke, MD and Brian J. Cole, MD, MBA PART ONE: DENOVO NT Introduction DeNovo NT (Zimmer) is minced (1-mm cubes) juvenile allograft cartilage
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Patella Fracture and Extensor Mechanism Injuries
 Patella Fracture and Extensor Mechanism Injuries Kyle T. Judd MS, MD, FACS David J. Hak MD, MBA, FACS Updated February 2016 1 Anatomy Patella Largest sesamoid bone Triangular shape (apex distal) Distal
Patella Fracture and Extensor Mechanism Injuries Kyle T. Judd MS, MD, FACS David J. Hak MD, MBA, FACS Updated February 2016 1 Anatomy Patella Largest sesamoid bone Triangular shape (apex distal) Distal
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions
 Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Hip, Knee and Shoulder Surgery
 Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
CASE REPORT. Antegrade tibia lengthening with the PRECICE Limb Lengthening technology
 CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
MSK Covered Services. Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components
 CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Davies and colleagues1 reported in a radiological
 30 Patellofemoral Arthritis Reuven B. Minkowitz M.D., and Joseph A. Bosco III, M.D. Abstract Patellofemoral joint arthritis is a common condition which can be extremely debilitating. Although it is a common
30 Patellofemoral Arthritis Reuven B. Minkowitz M.D., and Joseph A. Bosco III, M.D. Abstract Patellofemoral joint arthritis is a common condition which can be extremely debilitating. Although it is a common
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Tibial & Femoral Opening Wedge Osteotomy System. Surgical Technique
 Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
