CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT
|
|
|
- Rodney Holmes
- 5 years ago
- Views:
Transcription
1 GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large number of operative procedures which have been developed 1,2. Surgery outcomes are also unpredictable and decision-making is difficult when the physician only knows the patient has pain through a subjective report from the patient. Treatment of patella joint problems is still a black hole in orthopaedics. For athletes, a cartilage injury is a major problem as operative procedures in the patellofemoral joint are quite complex in comparison to other joints, which can be treated transarthroscopically 3-6. INCIDENCE Widuchowski et al 7 presented findings on 25,124 patients who underwent knee arthroscopy and found an incidence of 60% for chondral injuries, with patellar lesions accounting for 36% of those. Flanigan et al 8 found a 36% overall prevalence of full-thickness focal chondral defects in athletes. Patellofemoral defects (37%) were more common than femoral condyle (35%) and tibial plateau defects (25%). Patella defects were also more common than trochlea defects (64% vs 36%). It is important to note that 14% of athletes were asymptomatic at the time of diagnosis. Subsequently, we do see a lot of patellofemoral chondral damage when performing arthroscopies and we have to be careful when choosing the suitability of surgical intervention 8. TYPE AND ORIGIN OF LESIONS Patellofemoral lesions can be divided into six categories: 1. Pure chondromalaciae patellae. 2. Lesions due to direct trauma-contusion chondral damage. 3. Lesions due to traumatic dislocation of the patella. 4. Lesions due to direct/indirect trauma due to repeated instability. 5. Lesions due to defective extensor mechanisms after anterior/posterior cruciate ligament (ACL/PCL) injuries and repairs. 6. Primary osteoarthritis (OA) of the patellofemoral joint. INSTABILITY The majority of lesions could be caused by some degree of instability with or without dysplasia of the patellofemoral joint 5. Subsequently, different degrees of instability and dysplasia need to be 236 Journal TT Cartilage 10 Final.indd 236
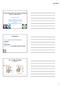
2 1 3 2 Figure 1: A patella defect prepared by a burr to create a subchondral space for a Maioregen implant. Figure 2: An exact size of the defect is cut out from a Maioregen collagen implant to be inserted into the patella defect in a press fit manner. Figure 3: The Maioregen collagen implant is put into place and covered with fibrin glue. identified if a surgical procedure is to be performed and all co-morbidities need to be addressed at the time of surgery. TREATMENT ALTERNATIVES In various studies, reliable and satisfying clinical results have been obtained in the treatment of cartilage lesions located on the medial and lateral femoral condyles, however patellar defects still present a challenge, with substantially poorer treatment outcomes3. The explanation for these inferior results lies in the specific biomechanical properties of the anterior compartment of the knee joint. There are many biological repair options available for treatment of patellofemoral cartilage defects, but there are very few studies showing long-term results for different methods. Many of the cartilage repair methods available today could be performed transarthroscopically for different location sites in the knee but most techniques require an arthrotomy when performed in the patellofemoral joint. Defect size and defect location within the patella have been found to be significantly associated with clinical outcome9,10. Larger cartilage lesions of the patella are associated with an inferior outcome. Cartilage defects located on the lateral patellar facet are correlated with a better clinical outcome than those located on the medial facet or those involving both facets9,10. Debridement/chondroplasty Trimming of cartilage flaps in International Cartilage Repair Society (ICRS) Grade I and/or II lesions might be an option even in large defects, when the patient suffers from locking phenomena but has no major pain component11,12. Pure bone marrow stimulation Microfracture and abrasion arthroplasty can be performed transarthroscopically. Drilling of the patella surface can be done retrograde or with the use of flexible drills. A few reports indicate that one may achieve acceptable long-term results at least in young patients13. Augmentation with a membrane such as the Autologous MatrixInduced Chondrogenesis (AMIC) technique is a possible alternative14. Shouldering cartilage is then needed. There are now instruments with curved guides combined with flexible drills that can be used to drill the patella surface transarthroscopiclly. A retrograde drilling into a patellar defect with a vector guide is another option. Bone marrow stimulation in conjunction with a cell ingrowth guiding matrix Chopin carbon pads15 and the biomimetic scaffold MaioRegen 16 (Figures 1 to 3) can both be implanted into the subchondral bone to induce strong cell ingrowth and repair tissue induction. Both of these techniques can be used as a salvage CARTILAGE SURGICAL OPTIONS TARGETED TOPIC Journal TT Cartilage 10 Final.indd
3 GENERAL OVERVIEW treatment for early OA of the patellofemoral joint and bipolar lesions and when shouldering cartilage is lacking. Bone marrow aspirate concentrate (BMAC)-derived multipotent stem cells17 implantation is another one-stage procedure which can be used for patellar lesions, but needs to be done via open surgery. Bone marrow is harvested from the ipsilateral iliac crest using a special aspiration kit and centrifuged using a commercially available system to obtain a concentration of bone marrow cells four to six times the baseline value. With the use of an enzyme, the bone marrow concentrate is activated to produce a sticky clot material. The clot is put into the defect and covered by periosteum, collagen membrane or a hyaluronan membrane and anchored by sutures17. An augmentated bone marrow stimulated lesion with a strong induced artificial blood clot formation is another interesting alternative18. New scaffolds also ensure the contours of the facets, which should be compared with the difficulties of using mosaicplasty plugs, to avoid incongruity. Shouldering cartilage is not needed for chondrocyte implantation. Since the introduction of ACI in 1987 it has been confirmed that this technique can produce mechanically and functionally stable cartilage in patients with full-thickness cartilage defects and is cost-effective, even though cell expansion in-vitro is expensive28. As an example of a fourth generation chondrocyte implantation, one may consider the use of particulated auto- or allografts22,29. Cartilage is harvested as a onestage procedure and the biopsy is crushed into small fragments, put onto a resorbable membrane covered with fibrin glue and implanted into the cartilage lesions with the fragments facing the defect. The most active cells migrate out of the crushed cartilage into the defect area to start a repair process. Mini metal implants Small metal implants that can be implanted into the subchondral bone are now seen more and more frequently and can be used as a salvage treatment for failed biological grafts and as an initial treatment option in osteonecrotic lesions30,31. Patellofemoral joint arthroplasties When the patellofemoral joint becomes osteoarthritic, with the remaining compartments more or less healthy, a patellofemoral joint prosthesis might be a good alternative32. 4 Osteochondral autografts It is difficult to find the right matching plugs due to mismatches between cartilage height in the patella and the donor sites. Short-term results are good, but as yet not enough long-term results have been published. Shouldering cartilage is also needed for this procedure19,20. Osteochondral allografts Aside from the difficulties in the right donor and the risk of transmission, the allograft is of when treating large defects patellofemoral joint21,22. finding disease interest in the Chondrocyte implantation There are several studies showing that it is possible to use autologous chondrocyte implantation (ACI) for patellofemoral joint cartilage repair, with optimal results occurring when co-morbidities have been addressed The clinical results of ACI have been found to differ significantly with the site of the cartilage damage in most published studies. Usually, patellofemoral ACI procedures require open surgery. However, today s third generation ACI facilitates the use of patellofemoral ACI treatments transarthrocopically in the patellofemoral joint. Figure 4: A large trochlear defect. 5 Figure 5: The large trochlear defect has been covered by a chondrocyte seeded hyaluronic acid membrane. A second layer of the cell seeded membrane is prepared and will be placed over the first layer to cover the defect completely. 238 Journal TT Cartilage 10 Final.indd 238
4 We do see a lot of patellofemoral chondral damage when performing arthroscopies and we have to be careful when choosing the suitability of surgical intervention 8 SURGUCAL OUTCOMES IN THE PATELLOFEMORAL JOINT In various studies, reliable and satisfying clinical results have been obtained in the treatment of cartilage lesions located on the medial and lateral femoral condyles, however patellar defects still present a challenge with substantially poorer outcomes reported 23. Although the lower proportion of satisfactory clinical results following treatment of retropatellar defects is not restricted to the ACI technique and has also been observed with other cartilage repair procedures such as microfracture and mosaicplasty, the clinical results of ACI have been found to differ significantly with the site of the cartilage damage in most published studies 33. The explanation for these inferior results lies in the specific biomechanical properties of the anterior compartment of the knee joint. There are greater shear forces than in the medial and lateral compartments, which hinder the differentiation of transplanted cartilage cells compared to the hydrostatic forces that are dominant in the femoral condyle and during stair climbing. The forces arising in the femoropatellar compartment reach 8 to 10 times body weight Bone marrow stimulation There is very little written about microfracture and the patellofemoral joint. Steinwachs et al write that AMIC seems to be particularly suited to treating damaged retropatellar cartilage, which is advantagous because these defects can be hard to treat with standard microfracture alone, however they have no clinical longterm results to present 34. Dhollander et al 14 presented a prospective 2-year clinical and magnetic resonance imaging (MRI) outcome of AMIC for the treatment of patellofemoral cartilage defects in the knee. Ten patients were clinically prospectively evaluated over 2-years. A clinical improvement became apparent during the 24-months of followup but the magnetic resonance observation of cartilage repair tissue (MOCART) scoring system revealed a slight, but statistically significant tendency to deterioration on MRI, between 1 and 2 years of follow-up. The formation of intralesional osteophytes was observed in 3 of the 10 patients (30%). The authors concluded that AMIC is safe and feasible for the treatment of symptomatic patellofemoral cartilage defects and resulted in a clinical improvement. However, the favourable clinical outcome of the AMIC technique was not confirmed by MRI findings. Their AMIC procedure was performed with a collagen membrane, but there are now different modified AMIC procedures available. Gobbi et al studied a BMAC with ACI variant matrix-induced autologous chondrocyte implantation (MACI). MACI patients with trochlear lesions showed better results than those with patellar lesions, while location was not a prognostic factor in the BMAC group. MRI showed complete filling of the defects in 76% of patients with MACI and 81% of patients with BMAC and histological analysis revealed hyaline-like features. Both techniques were viable and effective for large patellofemoral chondral lesions at minimum 3-year follow-up 17. AMIC procedures with the use of a hyaluronan membrane might, however, give different results. Osteochondral autografts Hangody et al presented good-toexcellent results in 79% of those treated with patellar and/or trochlear mosaicplasties at mean 10 years post-surgery 19. They recently showed a significantly better result with lesions on the condyles in a group of elite soccer players, compared with lesions on the patella or on the trochlea region 35. Osteochondral allograft (OCA) Gracitelli et al 36 showed that patellar allograft survivorship was 78.1% at 5 and 10 years and 55.8% at 15 years. Pain and function improved from the preoperative visit to latest follow-up and 89% of patients were very satisfied with the results of the OCA transplantation. OCA transplantation was successful as a salvage treatment procedure for cartilage injuries of the patella 36. Autologous chondrocyte implantation Peterson et al reviewed the long-term clinical durability of treatment with ACI in CARTILAGE SURGICAL OPTIONS TARGETED TOPIC 239 Journal TT Cartilage 10 Final.indd 239
5 GENERAL OVERVIEW 61 consecutive patients. Good-to-excellent results were seen in 85% of patients (29 of 32) who had defects on the femoral condyles, including osteochondritis dissecans lesions. Overall, there were 10 treatment failures among the 61 patients (16%), with failure rates lowest among patients with isolated femoral condylar lesions (11%) and osteochondritis dissecans lesions (14%) and somewhat higher in those who had ACI combined with ACL repair (18%) and highest among the patients treated for patellar lesions (24%)24. In another study26, clinical results obtained in 70 patients treated with ACI for full-thickness patellar defects, with special reference to defect location and size, age, body mass index and sports activity were presented. Defect size and defect location within the patella were found to be significantly associated with clinical outcome. Larger cartilage lesions of the patella were associated with an inferior outcome (p=0.007) and cartilage defects located on the lateral patellar facet were correlated with a better clinical outcome than those located on the medial facet or those involving both facets (p=0.017). Reported results for patellar ACI include a mixed population of patients with/without a concomitant correction of the extensor mechanism26. Forty-four patients were included in a study designed to compare the outcome of patellar ACI with extensor realignment to patellar ACI with normal patellofemoral tracking27. Patellar ACI with concomitant extensor realignment had a superior outcome to patellar ACI with normal patellofemoral tracking27. Gomoll et al33 presented multi-centre data on patella ACI grafts and found that when performed with attention to patellofemoral biomechanics, self-rated subjective good and excellent outcomes were achieved in more than 80% of patients treated with ACI, even in a patient population with large and frequently bipolar defects33. Filardo and colleagues37 found that patient characteristics differ between patellar and trochlear cartilage defects. The results obtained were significantly different, with a markedly good outcome in cases with trochlear lesions and less satisfactory results for patients affected by cartilage lesions of the patella37. Subsequently, the authors suggest that patellar and trochlear defects should be considered separately when evaluating the outcome of cartilage treatments in this anatomic region. The study included a total of 49 consecutive patients with full-thickness patellofemoral chondral lesions of the knee that were treated with MACI and followed prospectively for a minimum followup of 5 years. A statistically significant improvement in all scores was observed after treatment. Patellar lesions were more likey to require a realignment procedure and were more common in women. There were better results for trochlear lesions compared with patellar lesions at all follow-ups. Buckwalter et al22 studied the effect of using particulated allografted cartilage for patellar defects and had satisfactory results at short-term (mean 8.2 months) followup22. However, six of the 13 patients had concomitant anteromedialisation of the tibial tubercle performed at the same time as cartilage repair22. Similar results were also presented by Tompkins et al in CARTILAGE REPAIR CONCOMITANT PROCEDURES As mentioned in the introduction of this article, most patellofemoral cartilage lesions could be caused by some degree of instability with or without dysplasia of the patellofemoral joint. Those biomechanical issues need to be identified if a surgical procedure is to be undertaken and all comorbidities must be addressed at time of surgery. Tibial tubercle osteotomies and patellofemoral ligament reconstructions should be considered to stabilise and unload the joint and the lesions. Sometimes an unloading osteotomy is needed even in patients with normal patellofemoral biomechanics to improve the outcome. However, it is important to remember that as noted by Fulkerson9 elevation of the tubercle of 1.25 cm decreases patellofemoral contact forces by 60 to 80%, but further elevation provides less benefit and that most often no more than 1 cm of medialisation is needed. Medialisation may cause too much medial loading. Be extra careful when treating medial lesions! An overly medialised tibial tubercle with a painful and poorly-repaired patellar cartilage lesion may need to be returned to a lateral position via anterolateral tibial tubercle transfer. Proximal patellar lesions: the patella will articulate on more proximal cartilage with the knee flexed. This lesion responds poorly to tibial tubercle anteriorisation procedures as such an operation causes load shift onto the proximal patella. Lateral release will relieve abnormal tilt of the patella, but if there is lateral facet degeneration, osteotomy is also needed. Distal lateral patellar cartilage damage does well with anteromedialisation alone. Total patellar, bipolar and trochlear chondral lesions do poorly with anteromedialisation alone; good results could be achieved when ACI is added. Bipolar uncontained patellofemoral chondral lesions with bone erosion: consider patellofemoral arthroplasty 240 Journal TT Cartilage 10 Final.indd 240
6 Michael Regan - The FA/Getty Images with large biological implants such as MaioRegen, endoprosthetic surgery or osteochondral allografts. Outcomes of unloading Of interest to note is that Pidoriano et al10 correlated the region of the patellar articular cartilage lesion with patient outcomes in a series of patients who had Fulkerson s anteromedial tibial tuberosity transfer without cartilage restoration. They reported good and excellent results in 56% of patients with medial facet patellar lesions (Type III) and in 20% of patients with proximal pole or panpatellar lesions (Type IV)10. In addition, patients with central trochlear lesions had largely poor results with anteromedial tibial tubercle transfer. Trinh et al39 conducted a review that showed statistically significant improvements in patients undergoing both isolated ACI and ACI combined with osteotomy for patellofemoral chondral defects in all studies. Furthermore, significantly greater improvements in multiple clinical outcomes were observed in subjects undergoing ACI combined with osteotomy39. In 2014, Gillogly and Arnold40 presented a study with a mean follow up of 7-years where patients with failed primary treatment of isolated patellar full-thickness articular cartilage defects and patellofemoral malalignment treated with ACI and anteromedialisation of the tibial tubercle at least 5 years prior were contacted for final postoperative outcome scores. A combined ACI and anteromedialisation resulted in significant improvements in symptoms and function, with a low incidence of adverse events in those patients with isolated symptomatic patellar chondral defects40. DISCUSSION Treatment of cartilage lesions in the patellofemoral joint is a true challenge. From studies published in the literature it seems clear that correcting the coexisting background factors with realignment, stabilising or unloading procedures, along with the treatment of cartilage lesions, will improve the clinical outcomes33. Noyes and Barber-Westlin41 tried to determine if there is an ideal operation for large advanced articular cartilage lesions on the undersurface of the patella in young patients. A systematic search of PubMed was conducted to determine the outcome of operations performed for large patellar lesions in young patients. The authors concluded that a long-term beneficial effect might not occur in a third of ACI and patellofemoral arthroplasties and in two-thirds of osteochondral allograft procedures. Furthermore, they were unable to determine an ideal surgical procedure to treat large symptomatic patellar lesions in patients under 50 years old41. However, in the author s experience of treating cartilage lesions in the patellofemoral joint for more than 25 years, bone marrow stimulation alone is not enough to achieve a satisfactory result CARTILAGE SURGICAL OPTIONS TARGETED TOPIC Journal TT Cartilage 10 Final.indd
7 GENERAL OVERVIEW In an active athlete a debridement of flaps and synovectomy as well as harvest of cartilage for the tissue bank might be the first option when conservative treatment has failed. in most instances. Small defects can be treated with augmentated bone marrow stimulation with a membrane (variants of AMIC), mini-fragment (particulated) auto- or allografts, a gel reinforcement of the blood clot or BMAC. Larger defects are better treated with ACI, a biomimetic duallayer implant or osteochondral allograft. Defects in the patellofemoral joint could also be treated by mini metal implants for both small and larger defects when primary solutions have failed. Pure isolated patellofemoral joint OA responds very well to arthroplasty. All these treatment options must be considered in conjunction with realignment procedures when needed. Failure to address such adjunct abnormalities will endanger the success of the repair, whatever the technique used. In athletes, however, a more conservative approach than in the general population may be required. In a recent study Kaplan et al 42 looked at 20 top asymptomatic basketball player s knees with MRI. The overall prevalence of articular cartilage lesions on MRI was 47.5% in their study group. There were trochlear groove articular lesions in 25%. The patella had articular cartilage lesions in 35% 42. It is subsequently important to remember that asymptomatic lesions are present in a high percentage of top athletes. In an active athlete a debridement of flaps and synovectomy as well as harvest of cartilage for the tissue bank might be the first option when conservative treatment has failed. In a trochlear lesion, filling the debrided defect with an augmented gel (BST- CarGel) or with an AMIC technique using a membrane of collagen or hyaluronan may be a less invasive option. Fragment ACIs especially with allograft fragments may also be suitable. For larger defects, ACI and osteochondral grafts are to be used but ideally after finishing the season or after retirement, as those techniques most often need open surgery and have longer rehabilitation times. However, a recent paper by Campbell et al 43 showed the rate of return to sports was greatest after : osteochondral autograft transplantation (89%) followed by: osteochondral allograft (88%) ACI (84%) microfracture (75%) Furthermore, osteochondral autograft transplantation and ACI had statistically significantly greater rates of return to sports than microfracture (P< 0.001) 43. They also found that athletes who had a better prognosis after surgery were the ones that 43 : were younger had a shorter preoperative duration of symptoms had undergone no previous surgical interventions took part in a more extensive rehabilitation protocol had smaller cartilage defects. Scillia et al 44 studied American Football players (NFL) and found that the majority (67%) were able to return to play after arthroscopic knee surgery including only debridement of flaps of injured articular cartilage lesions (chondroplasty) 44. Athletes who played more games per season were more likely to return to play after chondroplasty of articular cartilage lesions of the knee, but those undergoing a more invasive treatment with a concomitant microfracture were 4.4 times less likely to return to the NFL than were those who did not undergo this procedure 44. To treat cartilage lesions in the athlete, especially in the patellofemoral joint, doctors could use the ideas presented by Mandelbaum et al 45, where the first step is a chondroprotection procedure that aims to prevent loss of existing cartilage. This may include a simple flap debridement plus a synovectomy, combined with rehabilitation including an analysis of how the athlete can optimally biomechanically load his/ her affected joint in order to protect the joint from further cartilage deterioration. Regular follow-ups monitoring the joint is mandatory to ensure we know when to intervene with a more aggressive cartilage restoration. References Available at Mats Brittberg M.D., Ph.D. Consultant Othopaedic Surgeon Cartilage Repair Unit, University of Gothenburg Region Halland Orthopaedics Kungsbacka Hospital Kungsbacka, Sweden Contact: mats.brittberg@regionhalland.se 242 Journal TT Cartilage 10 Final.indd 242
CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS
 CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
Chondral Injuries in the Athlete
 Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS
 ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
MSK Covered Services. Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components
 CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
Knee Preservation and Articular Cartilage Restoration
 Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Disclosures. How to approach cartilage repair. Articular Cartilage Problems: Surface Options
 Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Articular Cartilage Surgical Restoration Options
 Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Hip, Knee and Shoulder Surgery
 Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
Orthopaedic Advances. Abstract
 Orthopaedic Advances Cartilage Restoration Techniques for the Patellofemoral Joint Robert H. Brophy, MD Robert D. Wojahn, MD Joseph D. Lamplot, MD From Washington University Orthopedics, Chesterfield,
Orthopaedic Advances Cartilage Restoration Techniques for the Patellofemoral Joint Robert H. Brophy, MD Robert D. Wojahn, MD Joseph D. Lamplot, MD From Washington University Orthopedics, Chesterfield,
Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular
 Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular Cartilage Lesions Corporate Medical Policy File name: Osteochondral Allograft Transplantation
Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular Cartilage Lesions Corporate Medical Policy File name: Osteochondral Allograft Transplantation
Autologous Chondrocyte Implantation and Other Cell-based Treatments of Focal Articular Cartilage Lesions. Original Policy Date
 MP 7.01.36 Autologous Chondrocyte Implantation and Other Cell-based Treatments of Focal Articular Cartilage Lesions Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.36 Autologous Chondrocyte Implantation and Other Cell-based Treatments of Focal Articular Cartilage Lesions Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review
Horizon Scanning Centre November Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects
 Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Page: 1 of 21. Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Page: 1 of 21 Last Review Status/Date: September 2015 Focal Articular Cartilage Lesions Description A variety of procedures are being developed to resurface articular cartilage defects. Autologous chondrocyte
Page: 1 of 21 Last Review Status/Date: September 2015 Focal Articular Cartilage Lesions Description A variety of procedures are being developed to resurface articular cartilage defects. Autologous chondrocyte
Joint Preservation Clinical Case
 Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions
 Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD
 Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD Harvard Vanguard Medical Associates New England Baptist Hospital Boston, USA Cartilage Repair Marrow Stimulation
Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD Harvard Vanguard Medical Associates New England Baptist Hospital Boston, USA Cartilage Repair Marrow Stimulation
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Corporate Medical Policy
 Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Autologous Chondrocyte Implantation. Gerard Hardisty FRACS
 Autologous Chondrocyte Implantation Gerard Hardisty FRACS Disclosure Orthopaedic Surgeons Strong as an OX and half as bright Orthopaedic Innovation Arthroscopy Joint replacement Trauma management MIS Early
Autologous Chondrocyte Implantation Gerard Hardisty FRACS Disclosure Orthopaedic Surgeons Strong as an OX and half as bright Orthopaedic Innovation Arthroscopy Joint replacement Trauma management MIS Early
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Autografts and Allografts in the Treatment of Focal Page 1 of 30 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Autografts and Allografts in the Treatment of Focal
Autografts and Allografts in the Treatment of Focal Page 1 of 30 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Autografts and Allografts in the Treatment of Focal
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
7 Advanced Course on Knee Surgery. 14 to 18 January 2018 Val d Isère France. Classification of the cartilage lesions.
 7 Advanced Course on Knee Surgery TH Centre of Orthopeadics and Traumatology Hospital Brandenburg th th Fontane Medical School Theodor 14 to 18 January 2018 Val d Isère France Classification of the cartilage
7 Advanced Course on Knee Surgery TH Centre of Orthopeadics and Traumatology Hospital Brandenburg th th Fontane Medical School Theodor 14 to 18 January 2018 Val d Isère France Classification of the cartilage
AN OVERVIEW : Cartilage Treatment. Eric Thiel, MD. WVAM Conference 01/25/2019
 AN OVERVIEW : Cartilage Treatment Eric Thiel, MD WVAM Conference 01/25/2019 No Disclosure The Science of Hyaline Cartilage I. HYALINE CARTILAGE BASIC SCIENCE Normal Anatomy Cartilage is hypocellular, avascular,
AN OVERVIEW : Cartilage Treatment Eric Thiel, MD WVAM Conference 01/25/2019 No Disclosure The Science of Hyaline Cartilage I. HYALINE CARTILAGE BASIC SCIENCE Normal Anatomy Cartilage is hypocellular, avascular,
Cartilage Care in the Mature Female Athlete
 Cartilage Care in the Mature Female Athlete K. Linnea Welton, MD Hip Preservation Fellow Department of Orthopedic Surgery University of Colorado Women in Sports Medicine Conference February 24, 2018 Disclosures
Cartilage Care in the Mature Female Athlete K. Linnea Welton, MD Hip Preservation Fellow Department of Orthopedic Surgery University of Colorado Women in Sports Medicine Conference February 24, 2018 Disclosures
AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement.
 AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement. Dr. Andrea Fontana Istituto Auxologico Italiano Milan - Italy Introduction Chondropathies of
AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement. Dr. Andrea Fontana Istituto Auxologico Italiano Milan - Italy Introduction Chondropathies of
Index. D Delayed gadolinium-enhanced MRI of cartilage (dgemric), 357,
 A ACI. See Autologous chondrocyte implantation (ACI) Anaesthesia carbon dioxide arthroscopy, 352 high tibial osteotomy, 273 injection, 350 knee surgery, 350 regional anaesthesia ambulatory surgery, spinal,
A ACI. See Autologous chondrocyte implantation (ACI) Anaesthesia carbon dioxide arthroscopy, 352 high tibial osteotomy, 273 injection, 350 knee surgery, 350 regional anaesthesia ambulatory surgery, spinal,
St Vincent s SportsMed
 St Vincent s SportsMed Cartilage Transplantation In The Knee INTRODUCTION Normal articular cartilage is characterized by a smooth surface with very low friction and the ability to withstand repeated high
St Vincent s SportsMed Cartilage Transplantation In The Knee INTRODUCTION Normal articular cartilage is characterized by a smooth surface with very low friction and the ability to withstand repeated high
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee
 1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
Cartilage repair update: Indications are being refined and the future is bright
 Cartilage repair update: Indications are being refined and the future is bright ORTHOPEDICS TODAY 2008; 28:46 September 2008 Cartilage is a highly structured tissue with low cellularity and virtually no
Cartilage repair update: Indications are being refined and the future is bright ORTHOPEDICS TODAY 2008; 28:46 September 2008 Cartilage is a highly structured tissue with low cellularity and virtually no
AUTOLOGOUS CHONDROCYTE TRANSPLANTATION IN THE KNEE
 UnitedHealthcare Commercial Medical Policy AUTOLOGOUS CHONDROCYTE TRANSPLANTATION IN THE KNEE Policy Number: 2019T0030Q Effective Date: January 1,2019 Instructions for Use Table of Contents Page COVERAGE
UnitedHealthcare Commercial Medical Policy AUTOLOGOUS CHONDROCYTE TRANSPLANTATION IN THE KNEE Policy Number: 2019T0030Q Effective Date: January 1,2019 Instructions for Use Table of Contents Page COVERAGE
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Recommendations and Treatment Outcomes for Patellofemoral Articular Cartilage Defects With Autologous Chondrocyte Implantation Cecilia Pascual-Garrido,
The American Journal of Sports Medicine http://ajs.sagepub.com/ Recommendations and Treatment Outcomes for Patellofemoral Articular Cartilage Defects With Autologous Chondrocyte Implantation Cecilia Pascual-Garrido,
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Origins of PF Pain. Genesis of Iatrogenic Patellofemoral Pain
 Origins of PF Pain Genesis of Iatrogenic Patellofemoral Pain ISAKOS: DonJoy Consensus Meeting: Understanding Patellofemoral Pain Saturday, May 26, 2007 8:00-12:30 Talk: 7 minutes Improper Techniques Iatrogenic:
Origins of PF Pain Genesis of Iatrogenic Patellofemoral Pain ISAKOS: DonJoy Consensus Meeting: Understanding Patellofemoral Pain Saturday, May 26, 2007 8:00-12:30 Talk: 7 minutes Improper Techniques Iatrogenic:
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Knee Articular Cartilage Restoration: From cells to the patient. Professor Lars Engebretsen, University of Oslo, Norway
 Knee Articular Cartilage Restoration: From cells to the patient Professor Lars Engebretsen, University of Oslo, Norway Much of this started in 1994: I 1989 Grande et al -cartilage cell transplantation
Knee Articular Cartilage Restoration: From cells to the patient Professor Lars Engebretsen, University of Oslo, Norway Much of this started in 1994: I 1989 Grande et al -cartilage cell transplantation
CARTILAGE REPAIR INTRODUCTION. M. BERRUTO and G.M. PERETTI 1,2. Received January 6, Accepted January 8, 2013
 CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
The Aging Athletes Knee
 The Aging Athletes Knee Douglas P Tewes Orthopedic Sports Medicine Lincoln Orthopedic Center 1 Common Sports Knee Injuries Cartilage defects/chondromalacia Meniscal tears ACL tear Articular Cartilage injury/chondromalacia
The Aging Athletes Knee Douglas P Tewes Orthopedic Sports Medicine Lincoln Orthopedic Center 1 Common Sports Knee Injuries Cartilage defects/chondromalacia Meniscal tears ACL tear Articular Cartilage injury/chondromalacia
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
How to Manage a Failed Cartilage Repair: A Systematic Literature Review
 THIEME Review Article 93 How to Manage a Failed Cartilage Repair: A Systematic Literature Review Donato Rosa 1 Sigismondo Luca Di Donato 1 Giovanni Balato 1 Alessio D Addona 1 Francesco Smeraglia 1 Gaetano
THIEME Review Article 93 How to Manage a Failed Cartilage Repair: A Systematic Literature Review Donato Rosa 1 Sigismondo Luca Di Donato 1 Giovanni Balato 1 Alessio D Addona 1 Francesco Smeraglia 1 Gaetano
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation for the Repair of Chondral Defects of the Knee
 International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
Osteochondral allografting for all other joints is not covered as the evidence is insufficient to determine the
 Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Increased Failure Rate of Autologous Chondrocyte Implantation After Previous Treatment With Marrow Stimulation Techniques
 Increased Failure Rate of Autologous Chondrocyte Implantation After Previous Treatment With Marrow Stimulation Techniques Tom Minas,* MD, MS, Andreas H. Gomoll, MD, Ralf Rosenberger, MD, Ronald O. Royce,
Increased Failure Rate of Autologous Chondrocyte Implantation After Previous Treatment With Marrow Stimulation Techniques Tom Minas,* MD, MS, Andreas H. Gomoll, MD, Ralf Rosenberger, MD, Ronald O. Royce,
ARTICULAR CARTILAGE INJURY: EVALUATION AND WORK-UP ISMF Carlsbad Ca.
 ARTICULAR CARTILAGE INJURY: EVALUATION AND WORK-UP IMF 2018- Carlsbad Ca. Ken Zaslav MD Director: Cartilage Restoration Center ORTHO VIRGINIA: Richmond Virginia Clinical Prof. of Orthopedic urgery: V.C.U.
ARTICULAR CARTILAGE INJURY: EVALUATION AND WORK-UP IMF 2018- Carlsbad Ca. Ken Zaslav MD Director: Cartilage Restoration Center ORTHO VIRGINIA: Richmond Virginia Clinical Prof. of Orthopedic urgery: V.C.U.
NEW DEVELOPMENTS IN MENISCAL SURGERY
 NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
ACI < > < > +/- MSC MSC MASS
 Articular Cartilage Injury Natural History Management of Small Articular Cartilage Lesions Kai Mithoefer, MD Harvard Vanguard Medical Associates Harvard Medical School New England Baptist Hospital Boston,
Articular Cartilage Injury Natural History Management of Small Articular Cartilage Lesions Kai Mithoefer, MD Harvard Vanguard Medical Associates Harvard Medical School New England Baptist Hospital Boston,
Failed Cartilage Repair
 Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Articular cartilage repair using collagen type I hydrogels Clincal results
 Articular cartilage repair using collagen type I hydrogels Clincal results Ulrich Nöth, MD Department of Orthopaedic Surgery, König-Ludwig-Haus University of Würzburg, Germany Orthopädisches Zentrum für
Articular cartilage repair using collagen type I hydrogels Clincal results Ulrich Nöth, MD Department of Orthopaedic Surgery, König-Ludwig-Haus University of Würzburg, Germany Orthopädisches Zentrum für
Knee Cartilage Transplants
 Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Osteo-chondral Transplantation (OATS) The Unhappy ACL. Dr Ivan Popoff Knee, Elbow & Shoulder Surgery
 Osteo-chondral Transplantation (OATS) The Unhappy ACL The Unhappy ACL ACL reconstruction highly successful surgery for restoring stability and return to pre-injury levels of sporting activity? Return to
Osteo-chondral Transplantation (OATS) The Unhappy ACL The Unhappy ACL ACL reconstruction highly successful surgery for restoring stability and return to pre-injury levels of sporting activity? Return to
Why do they fail?? TOM MINAS MD MS. The Management of Failed Cartilage Repair Procedures PALM BEACH FL
 The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
Osteochondral Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions. Original Policy Date
 MP 7.01.61 Osteochondral Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date
MP 7.01.61 Osteochondral Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date
Retrospective study of cell-free collagen matrix for cartilage repair
 SCIENCE / RESEARCH Survey / Review 515 Andreas Breil-Wirth 1, Lars von Engelhardt 1,2, Stefan Lobner 1, Jörg Jerosch 1 Retrospective study of cell-free collagen matrix for cartilage repair n Study objective:
SCIENCE / RESEARCH Survey / Review 515 Andreas Breil-Wirth 1, Lars von Engelhardt 1,2, Stefan Lobner 1, Jörg Jerosch 1 Retrospective study of cell-free collagen matrix for cartilage repair n Study objective:
Disclosures 8/11/2017. ACI 2 Stage Technique Generation 1. Technical Improvements and Expansion of Indications based on evidence for ACI
 Technical Improvements and Expansion of Indications based on evidence for ACI Tom Minas MD MS Director, Cartilage Repair Center, Brigham and Women s, Hospital, Professor, Harvard Medical School, Boston
Technical Improvements and Expansion of Indications based on evidence for ACI Tom Minas MD MS Director, Cartilage Repair Center, Brigham and Women s, Hospital, Professor, Harvard Medical School, Boston
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review
 Techniques in Knee Surgery 5(1):47 52, 2006 T E C H N I Q U E Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review Shane J. Nho, MD, Christopher C.
Techniques in Knee Surgery 5(1):47 52, 2006 T E C H N I Q U E Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review Shane J. Nho, MD, Christopher C.
Case Report. Byung Ill Lee, MD and Byoung Min Kim, MD Department of Orthopedic Surgery, Soonchunhyang University Hospital, Seoul, Korea
 Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Cartilage OnlineFirst, published on February 13, 2012 as doi: /
 428222CARXXX10.1177/1947603511 428222Schüttler and AndjelkovCartilage The Author(s) 2010 Reprints and permission: http://www. sagepub.com/journalspermissions.nav Cartilage OnlineFirst, published on February
428222CARXXX10.1177/1947603511 428222Schüttler and AndjelkovCartilage The Author(s) 2010 Reprints and permission: http://www. sagepub.com/journalspermissions.nav Cartilage OnlineFirst, published on February
3/13/2018. Cartilage Cases. Case. Physical exam
 Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Tibial Cartilage Defects
 Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Autologous Chondrocyte Implantation Improves Patellofemoral Cartilage Treatment Outcomes
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 000, pp. 000 000 2007 Lippincott Williams & Wilkins Autologous Chondrocyte Implantation Improves Patellofemoral Cartilage Treatment Outcomes Jack Farr,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 000, pp. 000 000 2007 Lippincott Williams & Wilkins Autologous Chondrocyte Implantation Improves Patellofemoral Cartilage Treatment Outcomes Jack Farr,
8/10/2016. Treatment of Articular Cartilage Injuries: Osteochondral autograft Osteochondral allograft DISCLOSURES CONSIDERATIONS:
 Treatment of Articular Cartilage Injuries: Center for Cartilage Repair and Restoration University of Kentucky Osteochondral autograft Osteochondral allograft Christian Lattermann, MD Professor for Orthopaedics
Treatment of Articular Cartilage Injuries: Center for Cartilage Repair and Restoration University of Kentucky Osteochondral autograft Osteochondral allograft Christian Lattermann, MD Professor for Orthopaedics
Treatment Options for Articular Cartilage Defects of the Knee
 Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
The management of articular cartilage injuries in the
 1 2 3 4 5 6 7 8 Q1 Osteochondral Allograft Transplantation and Osteochondral Autograft Transfer D12XXAustin V. Stone, D13XXMD, PhD, D14XXDavid R. Christian, D15XXBS, D16XXMichael L. Redondo, D17XXMA, BS,
1 2 3 4 5 6 7 8 Q1 Osteochondral Allograft Transplantation and Osteochondral Autograft Transfer D12XXAustin V. Stone, D13XXMD, PhD, D14XXDavid R. Christian, D15XXBS, D16XXMichael L. Redondo, D17XXMA, BS,
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Autologous Chondrocyte Implantation
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Page 1 of 19 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Autologous Chondrocyte Implantation
Bipolar Articular Chondral Lesions of the Knee
 Bipolar Articular Chondral Lesions of the Knee Brian Waterman 1 Annabelle Davey 2 Michael L. Redondo 3 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Wake Forest School of Medicine, Winton-Salem,
Bipolar Articular Chondral Lesions of the Knee Brian Waterman 1 Annabelle Davey 2 Michael L. Redondo 3 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Wake Forest School of Medicine, Winton-Salem,
Osteochondral Knee Injuries. Marc N Ialenti, MD PGY-4 8/19/14
 Osteochondral Knee Injuries Marc N Ialenti, MD PGY-4 8/19/14 Articular Cartilage Complex, layered structure Viscoelastic material Resist shear forces Variable loadbearing Range of motion Position Essential
Osteochondral Knee Injuries Marc N Ialenti, MD PGY-4 8/19/14 Articular Cartilage Complex, layered structure Viscoelastic material Resist shear forces Variable loadbearing Range of motion Position Essential
Treatment of Full-Thickness Chondral Defects in the Knee With Autologous Chondrocyte Implantation
 Treatment of Full-Thickness Chondral Defects in the Knee With Autologous Chondrocyte Implantation Scott D. Gillogly, MD 1 Thomas H. Myers, MD 2 Michael M. Reinold, PT, DPT, ATC, CSCS 3 Autologous chondrocyte
Treatment of Full-Thickness Chondral Defects in the Knee With Autologous Chondrocyte Implantation Scott D. Gillogly, MD 1 Thomas H. Myers, MD 2 Michael M. Reinold, PT, DPT, ATC, CSCS 3 Autologous chondrocyte
POSITION STATEMENT The Use of Osteochondral Transplantation for the Treatment of Osteochondral Lesions of the Talus
 Position Statement POSITION STATEMENT The Use of Osteochondral Transplantation for the Treatment of Osteochondral Lesions of the Talus The American Orthopaedic Foot & Ankle Society (AOFAS) endorses the
Position Statement POSITION STATEMENT The Use of Osteochondral Transplantation for the Treatment of Osteochondral Lesions of the Talus The American Orthopaedic Foot & Ankle Society (AOFAS) endorses the
Clinical Policy Title: Autologous chondrocyte implantation
 Clinical Policy Title: Autologous chondrocyte implantation Clinical Policy Number: 14.03.07 Effective Date: March 1, 2017 Initial Review Date: February 15, 2017 Most Recent Review Date: February 6, 2018
Clinical Policy Title: Autologous chondrocyte implantation Clinical Policy Number: 14.03.07 Effective Date: March 1, 2017 Initial Review Date: February 15, 2017 Most Recent Review Date: February 6, 2018
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Policy Number: Original Effective Date: MM.06.002 8/1/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 12/01/2017
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Policy Number: Original Effective Date: MM.06.002 8/1/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 12/01/2017
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Osteochondral Problems of the Knee
 Arthroscopy: The Journal of Arthroscopic & Related Surgery Online October 1999, Supplement 1 Volume 15 Number 7
Arthroscopy: The Journal of Arthroscopic & Related Surgery Online October 1999, Supplement 1 Volume 15 Number 7
Theoretical Background Cartilage
 Theoretical Background Cartilage NEW TECHNIQUES FOR CARTILAGE REPAIR AND REPLACEMENT Kevin R. Stone, M.D. Michael J. Mullin, ATC, PTA Injury to the cartilage of the knee joint is one of the most common
Theoretical Background Cartilage NEW TECHNIQUES FOR CARTILAGE REPAIR AND REPLACEMENT Kevin R. Stone, M.D. Michael J. Mullin, ATC, PTA Injury to the cartilage of the knee joint is one of the most common
Greetings From SCOI. Richard D. Ferkel, M.D
 Greetings From SCOI Richard D. Ferkel, M.D OLT In the Athlete Operative Treatment and Return to Play The Following relationships exist: Royalties and stock options Smith and Nephew Consulting income
Greetings From SCOI Richard D. Ferkel, M.D OLT In the Athlete Operative Treatment and Return to Play The Following relationships exist: Royalties and stock options Smith and Nephew Consulting income
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
MEDICAL POLICY SUBJECT: OSTEOCHONDRAL GRAFTING
 MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
AUTOLOGOUS CHONDROCYTE TRANSPLANTATION IN THE KNEE
 UnitedHealthcare Community Plan Medical Policy AUTOLOGOUS CHONDROCYTE TRANSPLANTATION IN THE KNEE Policy Number: CS006.E Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1
UnitedHealthcare Community Plan Medical Policy AUTOLOGOUS CHONDROCYTE TRANSPLANTATION IN THE KNEE Policy Number: CS006.E Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1
AUTOLOGOUS CHONDROCYTE TRANSPLANTS & COLLAGEN MENISCUS IMPLANTS IN THE KNEE
 AUTOLOGOUS CHONDROCYTE TRANSPLANTS & COLLAGEN MENISCUS IMPLANTS IN THE KNEE Protocol: SUR048 Effective Date: September 1, 2016 Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE...
AUTOLOGOUS CHONDROCYTE TRANSPLANTS & COLLAGEN MENISCUS IMPLANTS IN THE KNEE Protocol: SUR048 Effective Date: September 1, 2016 Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE...
Anterior knee pain is a common complaint of patients. Considerations in Evaluating Treatment Options for Patellofemoral Cartilage Pathology
 REVIEW ARTICLE Considerations in Evaluating Treatment Options for Patellofemoral Cartilage Pathology Gregory J. Pinkowsky, MD* and Jack Farr, MDwz Abstract: Patellofemoral (PF) pain, a subset of anterior
REVIEW ARTICLE Considerations in Evaluating Treatment Options for Patellofemoral Cartilage Pathology Gregory J. Pinkowsky, MD* and Jack Farr, MDwz Abstract: Patellofemoral (PF) pain, a subset of anterior
Clinical Policy: Articular Cartilage Defect Repairs Reference Number: CP.MP.26
 Clinical Policy: Reference Number: CP.MP.26 Effective Date: 10/08 Last Review Date: 05/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.26 Effective Date: 10/08 Last Review Date: 05/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
