The effect of periapatite on the micromotion of total knee arthroplasty tibial components in osteoarthritis
|
|
|
- Christal Cox
- 6 years ago
- Views:
Transcription
1 The effect of periapatite on the micromotion of total knee arthroplasty tibial components in osteoarthritis A controlled prospective, randomized RSA study in 90 patients Mathys J.A. van der Linde 1, Eric H. Garling 2, Edward R. Valstar 2,3, Rob G.H.H. Nelissen 2, Alfons J. Tonino 1 1 Department of Orthopaedic Surgery and Traumatology, Atrium Medisch Centrum Heerlen, The Netherlands 2 Department of Orthopaedics, Leiden University Medical Center, The Netherlands 3 Department of Biomechanical Engineering, Faculty of Mechanical, Maritime and Materials Engineering, Delft University of Technology, The Netherlands
2 Abstract Both cemented and cementless total knee designs produce excellent clinical results. However, for specific patient groups, the cementless knees could have advantages. The way of bonding of the prosthesis to the adjacent bone remains a topic in total knee arthroplasty (TKA), especially in the younger patient population. Furthermore, the question of the value of adding a calciumphosphate coating to the prosthesis surface remains. A controlled randomized prospective study was performed on 90 Duracon TKA, to evaluate the effect of a Periapatite (PA) coating on the fixation of the tibial tray using micromotion (as measured with roentgen stereophotogrammetric analysis) as evaluation method. Twenty-five cemented components were included as the control group. The coated and the non-coated groups matched perfectly well for sex, age, weight, length, BMI and Insall score. Stage of osteoarthritis according to Ahlback, preoperative and postoperative femorotibial angle (FTA) and the mechanical leg axis showed no statistical differences. The non-coated tibial components showed more subsidence at two years 0.5 ± 0.63 mm (range, to 2.07 mm), than the PA coated tibial components: 0.1 ± 0.60 mm (range, to 2.75 mm); (p = 0.047). Also the medial-lateral motion of the non-coated group was significantly larger (p = 0.003). Translation and rotation migration data for the other axes were not significantly different. As expected the control group cemented components showed no subsidence after two-years follow-up: -0.1 ± 0.17 (range, to 0.22 mm). This study shows that periapatite augmentation improves the fixation of the Duracon total knee prosthesis, thus preventing mechanical loosening and subsequent long-term revision. 120
3 Micromotion of periapatite coated tibial components in OA patients 8.1 Introduction Nowadays, total knee arthroplasty is considered a routine procedure for degenerative changes of the knee joint. Cemented fixation of the components is still the most frequently used way of fixation. The advantages of a cemented design are the immediate implant stability, and the fact that the cement will act as a barrier for wear particles migration into the bone-prosthesis interface. Advantages of cementless designs are that more bone is preserved, which is of special importance to younger patients (Hofmann et al., 2002), and that peri-prosthetic fracture treatment can be performed more easily, which is important to the elderly patients. However, studies on the long-term results of cementless designs (Akizuki et al., 2003; Gejo et al., 1988; Nilsson et al., 1999) show the same and sometimes even better favorable clinical results as with cemented designs (Buechel, 2002; Whiteside, 2001). The addition of a calcium phosphate coating might even augment the boneprosthesis fixation and may also act as a barrier for ingress of wear-particles by sealing of the interface through periprosthetic bone ingrowth (Rahbek et al., 2000). Since these cementless designs have to osteointegrate for enduring fixation, this process of bonding between bone and prosthesis is the crucial issue for failure apart from polyethylene failure. Osteointegration is reflected by the absence of progressive micromotion (Nelissen et al., 1998; Ryd et al., 1995), absence of radiolucent lines and bone remodeling next to the prosthesis (Fuiko et al., 2003). The addition of a hydroxyapatite (HA) coating on the tibial tray may reduce micromotion in a cementless design even more (Akizuki et al., 2003; Nelissen, 1995; Onsten et al., 1998; Regnner et al., 2000; Toksvig-Larsen et al., 2000). Early migration as measured with roentgen stereophotogrammetric analysis (RSA) has been shown to be related to long-term implant survival (Grewal et al., 19992; Ryd et al., 1995). The purpose of this study was to examine the amount of three-dimensional micromotion of the tibial component in a prospective randomized RSA study, comparing uncoated tibial components and tibial components coated with periapatite (PA). Cemented tibial components were used as a control group. 121
4 8.2 Materials and Methods Patients Ninety consecutive primary total knee arthroplasties (TKA) (eighty-two patients) were included in this prospective, randomized RSA study. During surgery, a randomization scheme selected the patients for either the PA coated group or the uncoated group (Duracon: Stryker Howmedica Osteonics). Subsequently twenty-five cemented TKA s of the same design were included as a control group to validate the measurements. All patients had osteoarthritis. The PA group consisted of 44 knees and the uncoated group of 46 knees. The institution s ethics committee approved the study, and the patients gave informed consent. Tibial components The Duracon prosthetic design consists of a posterior cruciate retaining, nonconstrained system. All tibial baseplates had a cruciform keel for rotational stability and the same porous coated multiple layer beads ingrowth surface. In general, HA coating is applied with a plasma spraying process (Nelissen et al., 1998; Onsten et al., 1998), but this technique is not appropriate to coat the deeper layers of a porous surfaced prosthesis. The Duracon porous coated surface consists of a multiple layer beads (diameter 0.4 mm) with a porosity of 35%, a mean pore size of 425 micrometer and a thickness of 1.5 mm. During the PA coating technique, the prosthesis is submerged in a watery bath of calcium and phosphate at regulated ph (7.4) and temperature (80 ). As result of this process nucleation of the calcium phosphate as calcium deficient HA (similar to the process of bone mineralization) on the metal surface will take place. The PA technique reveals a pure single crystallized precipitated HA coating with a thickness of 20 micrometer in all layers of the porous surfaced prosthesis. No other calcium phosphate phases are present with this type of coating technique. In all knee replacements a PA porous coated femoral component and a full polyethylene cemented patellar prosthesis was used. The femorotibial design is a biconcave polyaxial radiated design with elongated posterior condyles and is medial-lateral stabilized with two pegs. The anatomically shaped patella component 122
5 Micromotion of periapatite coated tibial components in OA patients articulates in a proximal elongated trochlear groove. The exchangeable UHMW polyethylene insert, minimal thickness 11 mm, is fixed with an anterior and posterior lipping mechanism on the tibial tray (Figure 1). Figure 1. Radiograph of Duracon total knee prosthesis. Six tantalum markers are visible in the polyethylene inlay and in the tibia bone. Operative technique and after-treatment In all knee replacements, the same standard surgical procedure under tourniquet control was used. After a straight midline incision the knee was opened with a medial Payer approach. The tibial cutting surface was extramedullary aligned (classical prosthetic alignment perpendicular to the talocrural joint) and the distal femoral cut intra medullary aligned and was adjusted to the femoral anatomy both based on long standing X-rays. Soft tissue releases were performed when necessary. In the implants were bone cement (Genta Palacos, Biomet-Merck, Sjöbo, Sweden) was used, the bone surfaces were cleaned with a pulse lavage system. During operation three to eight tantalum beads (1 millimeter diameter) were inserted in preselected places in the metaphysial bone of the tibia. The insert of the tibial tray was manufactured with six tantalum balls (Howmedica Inc., Rutherford, USA). The locking mechanism between the insert and the tibial tray was pre-tested and showed no movement between the two parts. 123
6 After one day of bed rest patients were mobilized with two crutches and partial weight bearing during 6 weeks. Anti-trombotic profylaxis was performed using acenocoumarol (6 weeks), peri operatively patients received three doses of Cefamandol intravenously for infection prevention Radiographs and RSA The patients were evaluated preoperatively, and at one week before mobilization, three months, six months, one year, and two years postoperatively. At each evaluation the clinical status was assessed and radiographs for RSA were made. Immediately after the operation, at the one-year, and at the two-year follow-up, standard anterior/ posterior (AP) were taken with the patient standing. Lateral radiographs as well as axial radiographs of the patella were made supine. The femorotibial angle, the lateral and AP position of the tibial and femoral component were measured as well as the leg axis (Ewald, 1989). The RSA set-up consisted of two synchronized roentgen tubes positioned approximately 1.5 meter above a roentgen cassette (35x43 cm) at a 20 angle to the vertical. Both roentgen tubes simultaneously exposed the roentgen film. A calibration box made of Perspex was used to define the three-dimensional (laboratory) coordinate system. For this purpose 38 tantalum 1-mm markers were positioned in the lower plane of the box (fiducial markers). In order to calculate the focus position, 20 1-mm tantalum markers were positioned in the upper plane of the box (control markers). With a Vidar VXR-12 scanner (Vidar, Lund, Sweden), the radiographs were scanned at 150 dots per inch resolution and eight-bit gray scale resolution. The measurement of marker coordinates in the digitized radiographs, the threedimensional reconstruction of the marker positions, and the micromotion analysis was done with RSA-CMS (Medis, Leiden, The Netherlands), a software package that performs the RSA procedure automatically in digitized or digital radiographs (Valstar, 2001; Vrooman et al., 1998). In order to assess the micromotion of the implant with a high accuracy, the bone markers need to be well fixated in the bone. Bone markers were defined unstable when they moved more than 0.3 mm with respect to the other bone markers. Unstable markers were excluded from analysis. 124
7 Micromotion of periapatite coated tibial components in OA patients The first RSA examination served as the reference baseline. All subsequent evaluations of micromotion were related to the relative position of the prosthesis with respect to the bone at that the time of the evaluation. In 30 knees (16 PA and 14 uncoated) the first RSA radiograph was not made within 5 days after operation but at six weeks. As a consequence this radiograph was used as the reference baseline. Micromotion of the components was expressed as translation of the center of gravity of the prosthesis makers and rotation of the rigid body defined by the prosthesis markers about this center of gravity. Positive directions for translations along the orthogonal axes were: transverse (medial-lateral), longitudinal (caudal-cranial), and sagittal (posterior-anterior). Positive directions for rotations about the coordinate axes were anterior tilt (transverse axis), internal rotation (longitudinal axis), and varus (sagittal axis). When an integrated bone-prosthesis interface exists, the implant should be stable and a stable implant would not be at risk for aseptic loosening. In an RSA study of Ryd et al. (1995), a micromotion rate of 0.2 mm or more during the second postoperative year was identified to be a predictor for loosening of total knee implants at ten-year follow-up with a predictive power of about 85%. In this study, implants were defined to be at risk for aseptic loosening when the translation rate during the second postoperative year was larger than 0.5 mm along one or more coordinate axes (Ryd et al., 1995) and/or the rotation rate was larger than one degree about one or more coordinate axes. The reproducibility of the RSA measurements was determined by means of double examination of twenty patients (Table 1). Double examination consists of two RSA examinations of the same patient exposed within a time interval of about ten minutes. Because of the short time-interval between these two radiographs, the assumption is made that the implant did not migrate between these two exposures relative to the surrounding bone. By comparing these two radiographs, the accuracy of the micromotion parameters can be assessed (Ranstam et al., 2000). In some cases problems occurred with respect to the marking of the tibia. In six cases, the bone was either marked with less than three markers, or the markers were positioned so that they were occluded by the component. These cases were excluded from the analysis. 125
8 Table 1. Accuracy of the RSA measurements based on double examinations. Presented numbers are the upper limits of the 95%-confidence interval (N = 20). Translation (mm) Rotation ( ) Trans Long Sag Trans Long Sag Stem Statistical methods Mean values and standard deviations were calculated for all variables. For comparison of the mean values of the two groups, a Kruskall-Wallis test was used. In order to explore the effects of the two types of fixation on the amount of micromotion after two-years a linear regression was used with migration at the two years follow-up as the dependent variable and the fixation type and the base-line examination (directly postoperative or 6 weeks post operative) as co-variables. Levene s test for homogeneity of variance was used to determine the differences of the group variances in the micromotion data. For all analyses, significance was determined by a p-value of less than Results Clinical results The two groups and the cemented control group matched perfectly well for sex, age, weight, length, BMI and Insall score. Stage of osteoarthritis according to Ahlback, preoperative and postoperative femorotibial angle (FTA) and the mechanical leg axis showed no statistical differences (Table 2). The average operating time was 79 minutes (SD 18) for the uncemented knees and 81 minutes (SD 15) for cemented knees. During follow-up 5 PA coated, 3 uncoated and 1 cemented knee (9 patients) were lost to follow-up (not knee related). In the PA group 3 patients died, all after one year follow-up, one other patient had a cerebrovascular accident within two weeks after operation and the fifth patient moved abroad after 6 month follow-up. Based on the RSA results at the last follow-up, these knees were judged as stable. 126
9 Micromotion of periapatite coated tibial components in OA patients In the uncoated group one patient died and one moved after one year follow-up. Both knees were stable based on RSA examination. The third patient underwent an upper limb amputation because of vascular problems in another hospital. For this patient, RSA follow-up was too short for defining stability, which was the same for the patient in the cemented group who died after 6 month follow-up. Otherwise there was no evidence of clinical or radiographic failure in any of these patients. Clinical results by means of Insall score, active knee flexion and active extension lag showed no statistical difference among the two groups and the cemented control group during follow-up (Table 3). Table 2. Preoperative patient data (mean and standard deviations). PA coated Uncoated Cemented Sex F/M 33/10 31/12 14/11 Age 71 (± 7.8) 71 (± 7.27) 72 (± 6.6) Weight (kg) 78 (± 13.3) 79 (± 12.57) 79 (± 11.4) Length (cm) 165 (± 8.6) 166 (± 8.53) 168 (± 7.8) BMI 29 (± 4.7) 30 (± 4.9) 29 (± 4.9) Insall 53 (± 14.9) 49 (± 14.6) 60 (± 13.8) Ahlbäck 1-5 (N) 6/18/10/6/2 9/13/13/5/3 4/15/4/2 FTA 184 (± 8.9) 183 (± 8.6) 181 (± 4.9) Leg axis 177 (± 8.6) 177 (± 8.4) 174 (± 4.5) Table 3. Clinical results during follow-up (mean and standard deviations). Insall 81.8 (± 11.76) Flexion 98.5 (± 13,82) Extension 1.5 (± 3,62) PA coated Uncoated Cemented Post 2 yrs Post 2 yrs Post 2 yrs 88.5 (± 8.35) (± 12.67) 0.2 (± 0.93) 83.0 (± 8.80) (± 10.74) 2.5 (± 5.04) 88.5 (± 9.02) (± 12.66) 0.6 (± 2.00) 82.2 (± 13.04) 97.0 (± 10.10) 2.4 (± 5.42) 90.6 (± 6.98) (± 12.59) 0.6 (± 2.24) 127
10 8.3.2 Radiographic results Routine radiographs of the knee revealed no radiolucent lines of two millimeters or more around the tibial, femoral or patellar component in any knees of the three groups at the two-year follow-up evaluation. Sclerotic lines around the keel of the tibia tray were seen in 8 knees, 1 in the PA group and 7 in the uncoated group (P < 0.05; Pearson Chi Square test). Table 4. Radiographic results (mean and standard deviations) or number of knees. FTA (± 4.37) Hip-knee-ankle axis (± 4.66) Hip-knee-ankle axis <177 (n) Hip-knee-ankle axis >183 (n) PA coated Uncoated Cemented Post 2 yrs Post 2 yrs Post 2 yrs (± 3.98) (± 3.77) (± 3.59) (± 3.28) (± 3.81) (± 3.77) (± 2.85) (± 2.58) (± 2.75) (± 2.75) Table 5. Component position on AP and lateral radiographs (mean and standard deviation). Femur AP ( ) 98 (± 2.6) Femur lat ( ) 2 (± 2.5) Tibia AP ( ) 88 (± 2.6) Tibia lat ( ) 87 (± 2.8) PA coated Uncoated Cemented Post 2 yrs Post 2 yrs Post 2 yrs 98 (± 2.4) 1 (± 2.0) 88 (± 2.5) 86 (± 2.9) 99 (± 2.6) 2 (± 2.4) 89 (± 2.2) 87 (± 2.7) 99 (± 2.7) 2 (± 2.7) 89 (± 1.8) 86 (± 2.4) 99 (± 2.3) 10 (± 2.3) 89 (± 3.2) 85 (± 2.5) 98 (± 2.1) 1.3 (± 2.2) 89 (± 2.7) 86 (± 2.5) 128
11 Micromotion of periapatite coated tibial components in OA patients The average femoral-tibial angle was not different for the two groups and did not change substantially during follow-up (Table 4). The radiographic results of the components, evaluating the surgical technique for all groups individually by component position on standardized plain radiographs showed no differences between the three groups. In the cemented control group the FTA, legaxis and component positioning did not significantly differ from the other two groups (Table 5) RSA results The migration of the tibial components in millimeters at the two years follow-up is presented in Table 6. The graphs of the migration data showing the patterns of how the components in the two randomized groups and the control group migrated during the two-year follow-up are presented in Figures 2 7. At two year follow-up the non-coated tibial components showed more subsidence 0.5 ± 0.63 mm (range, to 2.07 mm), than the PA coated tibial components: 0.1 ± 0.60 mm (range, to 2.75 mm); (p = 0.047). In the first six weeks after implantation the uncoated implants already subsided 0.3 mm, while the PA coated group subsided only 0.1 mm. Also the medial-lateral motion between the two groups was significantly different (p = 0.003). Figure 2. Medial-lateral translations of the PA coated, uncoated and cemented tibial components (mean and standard deviation). 129
12 Figure 3. Caudal-cranial translations of the PA coated, uncoated and cemented tibial components (mean and standard deviation). Figure 4. Posterior-anterior translations of the PA coated, uncoated and cemented tibial components (mean and standard deviation). 130
13 Micromotion of periapatite coated tibial components in OA patients Figure 5. Anterior tilt of the PA coated, uncoated and cemented tibial components (mean and standard deviation). Figure 6. Internal rotations of the PA coated, uncoated and cemented tibial components (mean and standard deviation). 131
14 Figure 7. Varus rotation of the PA coated, uncoated and cemented tibial components (mean and standard deviation). Translation along the other 2 axis and rotation around all three axis migration data along the other axes were not significantly different among the groups. The effect of the other co-variable base-line examination was not significant (p>0.2) for all directions. This indicates that there was no difference between the delayed base-line examination group on the total amount of micromotion from 6 weeks post operatively up to the two year examination compared with the completely examined group. As in the group with the baseline within 5 days post operatively as in the group with the baseline at six weeks, it was possible to identify the stable tibial trays and the migrating tibial trays at risk for late aseptic loosening. The two groups showed no differences in the rotational migration data. However, the uncoated group showed a significant higher variance in anterior tilt compared to the PA coated components (Levene s test: p = 0.01). The tibial slope was not of influence on the amount of tilting of the components. The PA coated group showed also a high variance in varus rotation. This could be explained by one of the components in that group showing a high varus (7.7 degrees) tilt at the two years follow-up. This varus rotation of that tibial tray was also clearly visible on the plain 132
15 Micromotion of periapatite coated tibial components in OA patients radiographs. However, clinically there were no signs of failure of this component at two year follow-up. No relation between the femoral-tibial angle and varus/valgus rotation of the components could be found. The significant difference in the micromotion data between the two groups in medial-lateral direction can also be explained by the varus/valgus rotations of the components. These rotations are expressed by a medial-lateral motion of the center point of gravity of the markers in the polyethylene. Therefore it is very important to present three-dimensional micromotion data, not limited to in-plane translations that are actually caused by rotations of the components. As expected the control group showed no subsidence after two-years follow-up: -0.1 ± 0.17 mm (range, to 0.22 mm). Only a small posterior tilt of 0.3 degrees was observed. Four of the cemented components showed a posterior tilting of the component and three components an anterior tilt. The results of the control group validated the RSA measurements in this study. A total of 11 tibial trays from the PA group (26%), and 29 tibial trays from the uncoated group (63%) could be identified as at risk according to the definition given in the Materials and Methods section of this paper. Table 6. Migration (mean and standard deviation) of the PA coated, uncoated and cemented tibial components at the 2-year follow-up evaluation. PA coated Uncoated Cemented Translations medial-lateral ± ± ± 0.34 caudal-cranial 0.15 ± ± ± 0.17 posterior-anterior 0.07 ± ± ± 0.52 Rotations anterior tilt ± ± ± 0.60 internal rotation 0.07 ± ± ± 0.75 varus rotation ± ± ±
16 8.4 Discussion The loosening process of total knee implants seems to start with the tibial component. Continuous micromotion during the first two years after implantation in one or more directions detected by RSA, a validated tool to measure micromotion in vivo, reflects the start of this process (Grewal et al., 1992; Kärrholm et al., 1994; Ryd et al., 1995). General requirements for good fixation are close apposition of bone to the porous surface and a lack of movement at the developing interface between bone and implant. Optimization of the interface between bone and implant is therefore of paramount importance. In a cemented design, suboptimal conditions of both surfaces are corrected by the cement, but in cementless designs, apart from the type of ingrowth surface (calciumphosphate and/or metal pore diameter) the status of the prepared bone surfaces, bone quality and the gap between bone and implant are of high importance. In a comparative study of human cancellous bone remodeling to titanium and hydroxylapatite (HA) coated implants, Hofman showed that HA increases the percentage of the implant surface with ingrowth of bone (Hofmann et al., 1993). Ongrowth or ingrowth of human cancellous bone is possible in gaps smaller than 50 μm while HA had no metabolic influence on bone mineral apposition rate. In another study, Bloebaum showed the same maximum gap healing properties (max 50 μm) of surrounding human cancellous bone in the absence of HA on the titanium implants and found that bone apposition on non coated titanium implants needed a minimal time of 12 weeks (Bloebaum et al., 1971). Taking the assumption that HA coating accelerates bone ingrowth or ongrowth in time, it will create a higher area percentage bone-prosthesis contact. This could be an explanation for the higher level of migration of the uncoated implants observed in our RSA results and the faster stabilisation of the periapatite implants after an initial period of subsidence. From animal experiment it was already known that a thin lining of bone is present on the implant surface at three weeks, while at 6 weeks the implant is histologically osteointegrated (Geesink et al., 1988). In human, Hardy (Hardy et al., 1991) and Frayssinet (Frayssinet et al., 1993) showed intimate contact between woven bone and the hydroxyapatite coated hip prosthesis before six weeks after implantation. This study is in agreement with an earlier study by Nelissen on RSA measurement 134
17 Micromotion of periapatite coated tibial components in OA patients in TKA which also showed favorable results of adding a calcium-phosphate coating to the surface of uncemented tibial trays in TKA. In that study the noncoated components subsided significantly more than the coated and cemented components (Nelissen et al., 1998). In our study and the study by Nelissen the coated implants show stabilization after a short initial period of subsidence projecting the ingrowth phase, where as the uncoated implants show ongoing subsidence. Major difference between that study and the current study is the amount of subsidence observed in the uncoated groups, 0.73 mm vs 0.5 mm respectively at two years follow-up. One explanation for this difference could be the non-homogenous patient selection in the study by Nelissen. They included a mix of patients with rheumatoid arthritis and osteoarthritis. In generally patients with rheumatoid arthritis have more osteoporosis inducted by the use of corticosteroids resulting in a weaker foundation for the tibial tray. Li and Nilsson acknowledged this observation by showing a significant relationship between lower average BMD and more migration of the tibial component in TKA (Li and Nilsson, 2000). The greater variability in the migration profile of the uncemented tibial trays as found in this study stresses more the individual differences in bone ongrowth to the prosthesis, a factor not only determined by the available bone mass, but also dependent on the distance between bone and prosthesis immediate after implantation as well the intrinsic mechanical stability. Technically optimized instrumentation is necessary especially in uncemented TKA not only for creating correct alignement but also for exact bone cuts to create immediate implant stability without gaps. So, addition of the calcium phosphate PA did enhance initial component stability comparable to cemented TKA. Several other studies also acknowledge the beneficial effect of calcium phosphates (Akizuki et al., 2003; Fuiko et al., 2003; Nelissen et al., 1998; Nilsson et al., 1999; Onsten et al., 1998; Toksvig-Larsen et al., 2000). Looking at the different migration profiles of the cementless TKA designs described in these studies, the profile of the porous surface of the TKA seems also to be a factor related with migration. The titanium PFC design described by Önsten et al. had a porous surface with a pore diameter of micrometer (Onsten et al., 1998), while the vitallium Interax total knee described by Nelissen et al. had a fiber mesh surface with pore diameter of 1690 micrometer. The first mentioned 135
18 uncoated design showed a mean subsidence of 0.71 ± 0.56 mm (coated 0.87 ± 0.56), while the components in the latter study subsided 0.73 ± 0.92 mm at the two-year follow-up (coated 0.06 ± 0.17 mm) in a rheumatoid arthritis patient group. In our series with a homogenous osteoarthritic patient group, the uncoated tibial trays, (pore size 425 micrometer) subsided 0.5 mm ± 0.63 mm (range to 2.07 mm) while the coated subsided 0.1 mm ± 0.60 mm (range to 2.75). One reason for this difference might be their patient selection but another reason may be the quality of the pore size. In experiments with calcium aluminate, Klawitter showed that a minimal pore diameter of 100 μm is necessary for the ingrowth of bone (Klawitter et al., 1971). A minimal pore diameter of 50 μm is needed for ingrowth of osteoid and smaller pore sizes of about 5 μm to 15 μm result in ingrowth of fibrous tissue. If coatings are added to the porous surface more open structures may be required to keep the structure open. The Duracon prosthesis in this study has a porous surface with a pore diameter of 425 μm and after adding the 20 μm periapatite layer a remaining pore size diameter of 385 μm, which should be enough for ingrowth of bone according to the results of Klawitter. The small remaining pore size diameter ( micrometer) in the PFC study by Önsten could be the explanation for the high amount of subsidence in their coated group (0.87mm ± 0.56 mm). It must be emphasized that for all surface gap sizes reported in the literature, the addition of a calciumphosphate coating improved fixation, independent of the initial migration. A randomized RSA study comparing calciumphosphate coated tibial components with different gap sizes should further prove this effect. It is expected that when calciumphosphate coated implants sustain the forces that threaten the fixation in the early period after implantation, a strong and enduring fixation will be obtained. The influence of the local BMD on migration patterns of cemented and non cemented tibial trays is another subject of further analysis. 8.5 Conclusion This study shows that periapatite augmentation improves the fixation of the Duracon total knee prosthesis, thus preventing mechanical loosening and subsequent longterm revision. Uncemented non coated tibial trays in TKA are not advised to use. 136
19 Micromotion of periapatite coated tibial components in OA patients References Ahlback S. Osteoarthrosis of the knee. A radiographic investigation. Acta Radiol Diagn 1968; Suppl-72. Akizuki S, Takizawa T, Horiuchi H. Fixation of a hydroxyapatite-tricalcium phosphate-coated cementless knee prosthesis. Clinical and radiographic evaluation seven years after surgery. J Bone Joint Surg [Br] 2003; 85(8): Bloebaum R, Bachus K, Momberger N, Hofmann A. Miniral apposition rates of human cancellous bone at the interface of porous coated implants. J Biomed Mater Res Sympos 1971; 2: Buechel FF Sr. Long-term follow-up after mobile-bearing total knee replacement. Clin Orthop 2002; 404: Buechel FF Sr, Buechel FF Jr, Pappas MJ, Dalessio J. Twenty-year evaluation of the New Jersey LCS Rotating Platform Knee Replacement. J Knee Surg 2002; 15(2): Ewald F. The knee society total knee arthroplasty roentgenographic evaluation and scoring system. Clin Orthop 1989; 248: Frayssinet P, Hardy D, Conte P, Delince P. Histological analysis of the bone/prosthesis interface in man after implantation of a hip prosthesis coated with plasma sprayed hydroxyapatite. Rev chir. Orthop.Reparatrice Appar Mat 1993; 79(3): Fuiko R, Zembsch A, Loyoddin M, Ritschl P. Osteointegration and implant position after cementless total knee replacement. Clin Orthop 2003; 408: Geesink RGT, de Groot K, Klein CPAT. Bonding of Bone to Apatite-Coated Implants. J Bone Joint Surg 1988; 70(B): Gejo R, Akizuki S, Takizawa T. Fixation of the NexGen HA-TCP-coated cementless, screwless total knee arthroplasty: comparison with conventional cementless total knee arthroplasty of the same type. J Arthroplasty 2002; 17(4): Grewal R, Rimmer MG, Freeman MA. Early migration of prostheses related to long-term survivorship. Comparison of tibial components in knee replacement. J Bone Joint Surg [Br] 1992; 74(2): Hardy D, Fraysssinet P, Guithem A, Lafontaine M, Delince P. Bonding of hydroxyapatite-coated femoral prosthesis. J Bone Joint Surg [Br] 1991; 73(5): Hofmann A, Bachus K, Bloebaum R. Comparitive study of human cancellous bone remodeling to titanium and hydroxyapatite-coated implants. J Arthroplasty 1993; 2: Hofmann AA, Heithoff SM, Camargo M. Cementless total knee arthroplasty in patients 50 years or younger. Clin Orthop 2002; 404: Kärrholm J, Borssen B, Lowenhielm G, Snorrason F. Does early micromotion of femoral stem prostheses matter? 4-7-year stereoradiographic follow-up of 84 cemented prostheses. J Bone Joint Surg [Br] 1994; 76(6): Klawitter J, Hubert S. Application of porous ceramics for the attachment of load bearing internal orthopaedic applications. J Biomed Mater Res Sympos 1971; 2:
20 Li M,Nilsson K. The effect of the preoperative bone quality on the fixation of the tibial component in total knee arthroplasty. J. Arthoplasty 2000; 15(6): Nelissen RGHH. Fundamental aspects of the clinical evaluation of total joint prostheses. The total condylar knee prosthesis. 1995; Thesis Leiden University. ISBN : Groen, Leiden. Nelissen RG, Valstar ER, Rozing PM. The effect of hydroxyapatite on the micromotion of total knee prostheses. A prospective, randomized, double-blind study. J Bone Joint Surg 1998; 80: Nilsson KG, Kärrholm J, Carlsson L, Dalen T. Hydroxyapatite coating versus cemented fixation of the tibial component in total knee arthroplasty: prospective randomized comparison of hydroxyapatitecoated and cemented tibial components with 5-year follow-up using radiostereometry. J Arthroplasty 1999; 14(1): Nilsson KG, Kärrholm J, Linder L. Femoral component migration in total knee arthroplasty: randomized study comparing cemented and uncemented fixation of the Miller-Galante I design. J Orthop Res 1995; 13(3): Onsten I, Nordqvist A, Carlsson AS, Besjakov J, Shott S. Hydroxyapatite augmentation of the porous coating improves fixation of tibial components. A randomised RSA study in 116 patients. J Bone Joint Surg [Br] 1998; 80(3): Rahbek O, Overgaard S, Lind M, Bendix K, Bürger C, Söballe K. Sealing effect of hydroxyapatite coating on peri-implent migration of particles. Journal of Bone and Joint surgery [Br] 2001; 83(3): Rahbek O, Overgaard S, Jensen T, Bendix K, Söballe K. Sealing of hydroxyapatite coating. Acta Orthop Scand 2000; 71; Ranstam J, Ryd L, Onsten I. Accurate accuracy assessment: review of basic principles. Acta Orthop Scand 2000; 71: Regner L, Carlsson L, Kärrholm J, Herberts P. Tibial component fixation in porous- and hydroxyapatite-coated total knee arthroplasty: a radiostereo metric evaluation of migration and inducible displacement after 5 years. J Arthroplasty 2000; 15(6): Ryd L, Albrektsson BE, Carlsson L, Dansgard F, Herberts P, Lindstrand A, Regner L, Toksvig- Larsen S. Roentgen stereophotogrammetric analysis as a predictor of mechanical loosening of knee prostheses. J Bone Joint Surg [Br] 1995; 77: Toksvig-Larsen S, Jorn LP, Ryd L, Lindstrand A. Hydroxyapatite-enhanced tibial prosthetic fixation. Clin Orthop 2000; 370: Valstar ER. Digital Roentgen Stereophotogrammetry. Development, validation, and clinical application. 2001; Thesis, Leiden University. ISBN : Pasmans BV, Den Haag. Vrooman HA, Valstar ER, Brand GJ, Admiraal DR, Rozing PM, Reiber JH. Fast and accurate automated measurements in digitized stereophotogrammetric radiographs. J Biomech 1998; 31: Whiteside LA. Long-term follow-up of the bone-ingrowth Ortholoc knee system without a metalbacked patella. Clin Orthop 2001; 388:
Micromotion of mobile bearing versus posterior stabilized total knee prostheses. Randomized RSA study of 40 knees followed for 2 years
 Micromotion of mobile bearing versus posterior stabilized total knee prostheses Randomized RSA study of 40 knees followed for 2 years Eric H. Garling 1, Edward R. Valstar 1,2, Rob G.H.H. Nelissen 1 1 Department
Micromotion of mobile bearing versus posterior stabilized total knee prostheses Randomized RSA study of 40 knees followed for 2 years Eric H. Garling 1, Edward R. Valstar 1,2, Rob G.H.H. Nelissen 1 1 Department
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Triathlon Tritanium Knee System
 Triathlon Tritanium Knee System Table of Contents Cementless TKA... 4 Why Cementless TKA?... 4 Cementless TKA - Clinical History... 4 Published RSA Results Comparing Fixation Methods... 5 Biologic Fixation...
Triathlon Tritanium Knee System Table of Contents Cementless TKA... 4 Why Cementless TKA?... 4 Cementless TKA - Clinical History... 4 Published RSA Results Comparing Fixation Methods... 5 Biologic Fixation...
Guidelines for standardization of radiostereometry (RSA) of implants
 Acta Orthopaedica ISSN: 1745-3674 (Print) 1745-3682 (Online) Journal homepage: http://www.tandfonline.com/loi/iort20 Guidelines for standardization of radiostereometry (RSA) of implants Edward R Valstar,
Acta Orthopaedica ISSN: 1745-3674 (Print) 1745-3682 (Online) Journal homepage: http://www.tandfonline.com/loi/iort20 Guidelines for standardization of radiostereometry (RSA) of implants Edward R Valstar,
Does a new knee design perform as well as the design it replaces?
 Freely available online KNEE Does a new knee design perform as well as the design it replaces? M. Molt, P. Ljung, S. Toksvig-Larsen From Hässlehom Hospital, Hässleholm, Sweden Objectives The objective
Freely available online KNEE Does a new knee design perform as well as the design it replaces? M. Molt, P. Ljung, S. Toksvig-Larsen From Hässlehom Hospital, Hässleholm, Sweden Objectives The objective
Early migration of tibial components is associated with late revision
 Acta Orthopaedica 2012; 83 (Id.no 5477) Early migration of tibial components is associated with late revision A systematic review and meta-analysis of 21,000 knee arthroplasties Bart G Pijls 1, Edward
Acta Orthopaedica 2012; 83 (Id.no 5477) Early migration of tibial components is associated with late revision A systematic review and meta-analysis of 21,000 knee arthroplasties Bart G Pijls 1, Edward
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Integrated assessment techniques for linking kinematics, kinetics and muscle activation to early migration: A pilot study
 Integrated assessment techniques for linking kinematics, kinetics and muscle activation to early migration: A pilot study Nienke Wolterbeek 1, Eric H. Garling 1, Henrica M.J. van der Linden 1, Rob G.H.H.
Integrated assessment techniques for linking kinematics, kinetics and muscle activation to early migration: A pilot study Nienke Wolterbeek 1, Eric H. Garling 1, Henrica M.J. van der Linden 1, Rob G.H.H.
Insert mobility in a high congruent mobile-bearing total knee prosthesis
 Insert mobility in a high congruent mobile-bearing total knee prosthesis Nienke Wolterbeek 1, Eric H. Garling 1, Bart J.A. Mertens 2, Henrica M.J. van der Linden 1, Rob G.H.H. Nelissen 1, Edward R. Valstar
Insert mobility in a high congruent mobile-bearing total knee prosthesis Nienke Wolterbeek 1, Eric H. Garling 1, Bart J.A. Mertens 2, Henrica M.J. van der Linden 1, Rob G.H.H. Nelissen 1, Edward R. Valstar
Total Knee Replacement
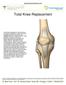 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
The optimal timing of baseline radiostereometric analysis of uncemented press fit cups
 Scandinavian Journal of Surgery 99: 244 249, 2010 The optimal timing of baseline radiostereometric analysis of uncemented press fit cups O. Wolf, J. Milbrink, S. Larsson, P. Mattsson, H. Mallmin Department
Scandinavian Journal of Surgery 99: 244 249, 2010 The optimal timing of baseline radiostereometric analysis of uncemented press fit cups O. Wolf, J. Milbrink, S. Larsson, P. Mattsson, H. Mallmin Department
Hydroxyapatite (HA) coating appears to be of benefit for implant durability of tibial components in primary total knee arthroplasty
 Acta Orthopaedica 2011; 82 (Id. no. 4437) Supplementary article data 1 Supplementary article data Hydroxyapatite (HA) coating appears to be of benefit for implant durability of tibial components in primary
Acta Orthopaedica 2011; 82 (Id. no. 4437) Supplementary article data 1 Supplementary article data Hydroxyapatite (HA) coating appears to be of benefit for implant durability of tibial components in primary
Knee Revision. Portfolio
 Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Optimum implant geometry
 Design Rationale Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Design Rationale Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Evolution. Medial-Pivot Knee System The Bi-Cruciate-Substituting Knee. Key Aspects
 Evolution Medial-Pivot Knee System The Bi-Cruciate-Substituting Knee Key Aspects MicroPort s EVOLUTION Medial-Pivot Knee System was designed to recreate the natural anatomy that is lost during a total
Evolution Medial-Pivot Knee System The Bi-Cruciate-Substituting Knee Key Aspects MicroPort s EVOLUTION Medial-Pivot Knee System was designed to recreate the natural anatomy that is lost during a total
BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS IN TOTAL KNEE REPLACEMENTS
 Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
ARTICLE IN PRESS. Journal of Biomechanics
 Journal of Biomechanics 42 (2009) 2387 2393 Contents lists available at ScienceDirect Journal of Biomechanics journal homepage: www.elsevier.com/locate/jbiomech www.jbiomech.com Implementation and validation
Journal of Biomechanics 42 (2009) 2387 2393 Contents lists available at ScienceDirect Journal of Biomechanics journal homepage: www.elsevier.com/locate/jbiomech www.jbiomech.com Implementation and validation
Optimum implant geometry
 Design Rationale Optimum implant geometry Extending the proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Design Rationale Optimum implant geometry Extending the proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
J. Uvehammer *, J. Karrholm. Accepted 21 February 2001
 ELSEVIER Journal of Orthopaedic Research 19 (2001) 1168-1 177 Journal of Orthopaedic Research www.elsevier.com/locate/orthres Inducible displacements of cemented tibial components during weight-bearing
ELSEVIER Journal of Orthopaedic Research 19 (2001) 1168-1 177 Journal of Orthopaedic Research www.elsevier.com/locate/orthres Inducible displacements of cemented tibial components during weight-bearing
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Frontal Plane Kinematics After Mobile- Bearing Total Knee Arthroplasty
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 392, pp. 56 61 2001 Lippincott Williams & Wilkins, Inc. Frontal Plane Kinematics After Mobile- Bearing Total Knee Arthroplasty James B. Stiehl, MD*; Richard
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 392, pp. 56 61 2001 Lippincott Williams & Wilkins, Inc. Frontal Plane Kinematics After Mobile- Bearing Total Knee Arthroplasty James B. Stiehl, MD*; Richard
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year
 Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Zimmer Segmental System
 Zimmer Segmental System Simple solutions for solving complex salvage cases A Step Forward The Zimmer Segmental System is designed to address patients with severe bone loss associated with disease, trauma
Zimmer Segmental System Simple solutions for solving complex salvage cases A Step Forward The Zimmer Segmental System is designed to address patients with severe bone loss associated with disease, trauma
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Preoperative gait patterns and BMI are associated with tibial component migration
 478 Acta Orthopaedica 2010; 81 (4): 478 486 Preoperative gait patterns and BMI are associated with tibial component migration Janie L Astephen Wilson 1, David A J Wilson 1, Michael J Dunbar 1,2, and Kevin
478 Acta Orthopaedica 2010; 81 (4): 478 486 Preoperative gait patterns and BMI are associated with tibial component migration Janie L Astephen Wilson 1, David A J Wilson 1, Michael J Dunbar 1,2, and Kevin
National Joint Replacement Registry. Lay Summary 2015 Annual Report Hip and Knee Replacement
 National Joint Replacement Registry Lay Summary 2015 Annual Report Hip and Knee Replacement SUPPLEMENTARY REPORT 2015 TABLE OF CONTENTS Introduction... 1 A brief history of the Registry origins... 1 The
National Joint Replacement Registry Lay Summary 2015 Annual Report Hip and Knee Replacement SUPPLEMENTARY REPORT 2015 TABLE OF CONTENTS Introduction... 1 A brief history of the Registry origins... 1 The
Comparison of tibial bone coverage of 6 knee prostheses: a magnetic resonance imaging study with controlled rotation
 Journal of Orthopaedic Surgery 2012;20(2):143-7 Comparison of tibial bone coverage of 6 knee prostheses: a magnetic resonance imaging study with controlled rotation Gregory C Wernecke, 1 Ian A Harris,
Journal of Orthopaedic Surgery 2012;20(2):143-7 Comparison of tibial bone coverage of 6 knee prostheses: a magnetic resonance imaging study with controlled rotation Gregory C Wernecke, 1 Ian A Harris,
Clinical Biomechanics
 Clinical Biomechanics 27 (2012) 398 402 Contents lists available at SciVerse ScienceDirect Clinical Biomechanics journal homepage: www.elsevier.com/locate/clinbiomech Kinematics and early migration in
Clinical Biomechanics 27 (2012) 398 402 Contents lists available at SciVerse ScienceDirect Clinical Biomechanics journal homepage: www.elsevier.com/locate/clinbiomech Kinematics and early migration in
Excellent Fixation Achieved With Cementless Posteriorly Stabilized Total Knee Arthroplasty
 The Journal of Arthroplasty Vol. 28 No. 1 2013 Excellent Fixation Achieved With Cementless Posteriorly Stabilized Total Knee Arthroplasty Steven F. Harwin, MD, FACS,* Mark A. Kester, PhD,y Arthur L. Malkani,
The Journal of Arthroplasty Vol. 28 No. 1 2013 Excellent Fixation Achieved With Cementless Posteriorly Stabilized Total Knee Arthroplasty Steven F. Harwin, MD, FACS,* Mark A. Kester, PhD,y Arthur L. Malkani,
Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty
 Tsukada et al. Journal of Orthopaedic Surgery and Research 2013, 8:36 RESEARCH ARTICLE Open Access Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty Sachiyuki
Tsukada et al. Journal of Orthopaedic Surgery and Research 2013, 8:36 RESEARCH ARTICLE Open Access Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty Sachiyuki
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Masterclass. Tips and tricks for a successful outcome. E. Verhaven, M. Thaeter. September 15th, 2012, Brussels
 Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
ANATOMIC SURGICAL TECHNIQUE. 5 in 1. Conventional instrumentation 07/11/2013
 ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
Biomechanics of. Knee Replacement. Mujda Hakime, Paul Malcolm
 Biomechanics of Knee Replacement Mujda Hakime, Paul Malcolm 1 Table of contents Knee Anatomy Movements of the Knee Knee conditions leading to knee replacement Materials Alignment and Joint Loading Knee
Biomechanics of Knee Replacement Mujda Hakime, Paul Malcolm 1 Table of contents Knee Anatomy Movements of the Knee Knee conditions leading to knee replacement Materials Alignment and Joint Loading Knee
NexGen Legacy LPS-Flex Knee. Brochure
 NexGen Legacy LPS-Flex Knee Brochure What postoperative range of motion can your TKA patients expect? For patients with the ability and desire to perform For patients with the ability high-flexion activities,
NexGen Legacy LPS-Flex Knee Brochure What postoperative range of motion can your TKA patients expect? For patients with the ability and desire to perform For patients with the ability high-flexion activities,
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
VARIABILITY OF THE POSTERIOR CONDYLAR ANGLE
 VARIABILITY OF THE POSTERIOR CONDYLAR ANGLE Łukasz Cieliński, Damian Kusz, Michał Wójcik Department of Orthopedics Medical University of Silesia in Katowice Introduction Correct positioning of implants
VARIABILITY OF THE POSTERIOR CONDYLAR ANGLE Łukasz Cieliński, Damian Kusz, Michał Wójcik Department of Orthopedics Medical University of Silesia in Katowice Introduction Correct positioning of implants
Partial Knee Replacement
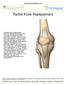 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Clinical Results of Bone Ingrowth TKA in Patients with Rheumatoid Arthritis
 Clin Orthop Relat Res (2008) 466:3071 3077 DOI 10.1007/s11999-008-0394-1 ORIGINAL ARTICLE Clinical Results of Bone Ingrowth TKA in Patients with Rheumatoid Arthritis Roberto Viganó MD, Leo A. Whiteside
Clin Orthop Relat Res (2008) 466:3071 3077 DOI 10.1007/s11999-008-0394-1 ORIGINAL ARTICLE Clinical Results of Bone Ingrowth TKA in Patients with Rheumatoid Arthritis Roberto Viganó MD, Leo A. Whiteside
Correlation of Femoral Component Micromotion to a Physical Test Using an FEA Model.
 Correlation of Femoral Component Micromotion to a Physical Test Using an FEA Model. Robert Davignon, Ananthkrishnan Gopalakrishnan. Stryker Corporation, Parsippany, NJ, USA. Disclosures: R. Davignon: 3A;
Correlation of Femoral Component Micromotion to a Physical Test Using an FEA Model. Robert Davignon, Ananthkrishnan Gopalakrishnan. Stryker Corporation, Parsippany, NJ, USA. Disclosures: R. Davignon: 3A;
Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W.
 University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
Axial alignment of the lower extremity in Chinese adults. Journal Of Bone And Joint Surgery - Series A, 2000, v. 82 n. 11, p.
 Title Axial alignment of the lower extremity in Chinese adults Author(s) Tang, WM; Zhu, YH; Chiu, KY Citation Journal Of Bone And Joint Surgery - Series A, 2000, v. 82 n. 11, p. 1603-1608 Issued Date 2000
Title Axial alignment of the lower extremity in Chinese adults Author(s) Tang, WM; Zhu, YH; Chiu, KY Citation Journal Of Bone And Joint Surgery - Series A, 2000, v. 82 n. 11, p. 1603-1608 Issued Date 2000
Over 20 Years of Proven Clinical Success. Zimmer Natural-Knee II System
 Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Featuring. Technology. Product Rationale
 Featuring Technology Product Rationale 2 Optimum implant geometry Extending proven TRI-LOCK heritage The original TRI-LOCK Stem was introduced in 1981. This implant was the first proximally coated tapered-wedge
Featuring Technology Product Rationale 2 Optimum implant geometry Extending proven TRI-LOCK heritage The original TRI-LOCK Stem was introduced in 1981. This implant was the first proximally coated tapered-wedge
TOTAL KNEE ARTHROPLASTY (TKA)
 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
Metha Short Hip Stem System
 Metha Short Hip Stem System Accuracy That Stands Alone Aesculap Orthopaedics Metha Short Hip Stem System Designed For Anatomic Accuracy The Metha Short Hip Stem is designed for anatomic accuracy to restore
Metha Short Hip Stem System Accuracy That Stands Alone Aesculap Orthopaedics Metha Short Hip Stem System Designed For Anatomic Accuracy The Metha Short Hip Stem is designed for anatomic accuracy to restore
Knee arthroplasty: What radiologists should know.
 Knee arthroplasty: What radiologists should know. Poster No.: C-2174 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Araújo 1, J. Pires 2, J. Oliveira 3, C. Macedo 1, S. Magalhães 1, I. Ferreira
Knee arthroplasty: What radiologists should know. Poster No.: C-2174 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Araújo 1, J. Pires 2, J. Oliveira 3, C. Macedo 1, S. Magalhães 1, I. Ferreira
Kinematic vs. mechanical alignment: What is the difference?
 Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
Total ankle replacement
 Total ankle replacement THE RESULTS IN 200 ANKLES P. L. R. Wood, S. Deakin From Wrightington Hospital, Wigan, England B etween 1993 and 2000 we implanted 200 cementless, mobile-bearing STAR total ankle
Total ankle replacement THE RESULTS IN 200 ANKLES P. L. R. Wood, S. Deakin From Wrightington Hospital, Wigan, England B etween 1993 and 2000 we implanted 200 cementless, mobile-bearing STAR total ankle
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Complications of Total Knee Arthroplasty
 Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Examination of Porous-Coated Patellar Components and Analysis of the Reasons for Their Retrieval
 Examination of Porous-Coated Patellar Components and Analysis of the Reasons for Their Retrieval J. P. Collier,* M. B. Mayor,+ V. A. Surprenant,* H. P. Surprenant,* and R.E. Jensen* *Dartmouth Biomedical
Examination of Porous-Coated Patellar Components and Analysis of the Reasons for Their Retrieval J. P. Collier,* M. B. Mayor,+ V. A. Surprenant,* H. P. Surprenant,* and R.E. Jensen* *Dartmouth Biomedical
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
A Kinematic Assessment of Knee Prosthesis from Fluoroscopy Images
 Memoirs of the Faculty of Engineering, Kyushu University, Vol. 68, No. 1, March 2008 A Kinematic Assessment of Knee Prosthesis from Fluoroscopy Images by Mohammad Abrar HOSSAIN *, Michihiko FUKUNAGA and
Memoirs of the Faculty of Engineering, Kyushu University, Vol. 68, No. 1, March 2008 A Kinematic Assessment of Knee Prosthesis from Fluoroscopy Images by Mohammad Abrar HOSSAIN *, Michihiko FUKUNAGA and
Aseptic Revision Total Knee Surgical Techniques. Andrew Ehmke, DO Chicago, IL May 5, 2018
 Aseptic Revision Total Knee Surgical Techniques Andrew Ehmke, DO Chicago, IL May 5, 2018 I have no disclosures relevant to this talk 3 Phases of Revision 1. Exposure Key to the case!! 2. Component Removal
Aseptic Revision Total Knee Surgical Techniques Andrew Ehmke, DO Chicago, IL May 5, 2018 I have no disclosures relevant to this talk 3 Phases of Revision 1. Exposure Key to the case!! 2. Component Removal
Early Results of Total Knee Replacements:
 Early Results of Total Knee Replacements: "A Clinical and Radiological Evaluation" K.S. Dhillon, FRCS* Jamal, MS* S. Bhupinderjeet, MBBS** * Dept. of Orthopaedic Surgery University of Malaya, Kuala Lumpur
Early Results of Total Knee Replacements: "A Clinical and Radiological Evaluation" K.S. Dhillon, FRCS* Jamal, MS* S. Bhupinderjeet, MBBS** * Dept. of Orthopaedic Surgery University of Malaya, Kuala Lumpur
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
*smith&nephew SL-PLUS Cementless Femoral Hip System. Product Information
 Product Information *smith&nephew SL-PLUS Cementless Femoral Hip System First Came the Philosophy to develop a universal hip system that could be used in almost every indication, immaterial to the patient
Product Information *smith&nephew SL-PLUS Cementless Femoral Hip System First Came the Philosophy to develop a universal hip system that could be used in almost every indication, immaterial to the patient
Bicruciate-Retaining or Medial Pivot Total Knee Prosthesis Pritchett 225 Fig. 3. The MP total knee prosthesis. Fig. 1. An anteroposterior radiograph o
 The Journal of Arthroplasty Vol. 26 No. 2 2011 Patients Prefer A Bicruciate-Retaining or the Medial Pivot Total Knee Prosthesis James W. Pritchett, MD, FACS Abstract: Four-hundred forty patients underwent
The Journal of Arthroplasty Vol. 26 No. 2 2011 Patients Prefer A Bicruciate-Retaining or the Medial Pivot Total Knee Prosthesis James W. Pritchett, MD, FACS Abstract: Four-hundred forty patients underwent
Analysis of an Early Intervention Tibial Component for Medial Osteoarthritis
 Analysis of an Early Intervention Tibial Component for Medial Osteoarthritis Miriam Chaudhary, M.Sc. 1, Peter S. Walker, PhD 2. 1 NYU Hospital for Joint Diseases, New York City, NY, USA, 2 NYU-Hospital
Analysis of an Early Intervention Tibial Component for Medial Osteoarthritis Miriam Chaudhary, M.Sc. 1, Peter S. Walker, PhD 2. 1 NYU Hospital for Joint Diseases, New York City, NY, USA, 2 NYU-Hospital
Gold standard of a TKA. Conflicting goals? POLYETHYLENE WEAR THE SOLUTION: MOBILE BEARING KNEES. MOBILE BEARING A totally new approach (1977)
 Changing designs : the case against mobile bearing? Gold standard of a TKA Goal of a TKA: 1. Pain 2. Motion 3. Longevity Stress Guy BELLIER M.D. PARIS France Conformity = Durability w/o constraints = non
Changing designs : the case against mobile bearing? Gold standard of a TKA Goal of a TKA: 1. Pain 2. Motion 3. Longevity Stress Guy BELLIER M.D. PARIS France Conformity = Durability w/o constraints = non
SPECT/CT Imaging. Knee & Hip Prosthesis
 SPECT/CT Imaging Knee & Hip Prosthesis Helmut Rasch, Michael T. Hirschmann Institute of Radiology and Nuclear Medicine, Dept. Orthopaedic Surgery and Traumatology, -Bruderholz, Switzerland helmut.rasch@unibas.ch
SPECT/CT Imaging Knee & Hip Prosthesis Helmut Rasch, Michael T. Hirschmann Institute of Radiology and Nuclear Medicine, Dept. Orthopaedic Surgery and Traumatology, -Bruderholz, Switzerland helmut.rasch@unibas.ch
Knee Replacement Implants
 Knee Replacement Implants During knee replacement surgery, an orthopaedic surgeon will resurface your damaged knee with artificial components, called implants. There are many different types of implants.
Knee Replacement Implants During knee replacement surgery, an orthopaedic surgeon will resurface your damaged knee with artificial components, called implants. There are many different types of implants.
Optimizing function Maximizing survivorship Accelerating recovery
 Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design. Adam I. Harris, M.D. & Michelle Ammerman
 Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design Adam I. Harris, M.D. & Michelle Ammerman History: The Total Condylar knee represented a significant advance in
Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design Adam I. Harris, M.D. & Michelle Ammerman History: The Total Condylar knee represented a significant advance in
PARTIAL KNEE REPLACEMENT
 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis
 The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
The Journal of Arthroplasty Vol. 18 No. 8 2003 15-Year Follow-up Study of Total Knee Arthroplasty in Patients With Rheumatoid Arthritis Jun Ito, MD, PhD, Tomihisa Koshino, MD, PhD, Renzo Okamoto, MD, PhD,
Radiostereometric analysis of hip implants: a critical review of methodology and future directions
 Page 1 of 5 Diagnosis Radiostereometric analysis of hip implants: a critical review of methodology and future directions S Sesselmann *, R Forst, F Tschunko Abstract Introduction Early migration of endoprostheses
Page 1 of 5 Diagnosis Radiostereometric analysis of hip implants: a critical review of methodology and future directions S Sesselmann *, R Forst, F Tschunko Abstract Introduction Early migration of endoprostheses
MODEL-BASED RADIOSTEREOMETRIC ANALYSIS OF AN UNCEMENTED MOBILE-BEARING TOTAL ANKLE ARTHROPLASTY SYSTEM. Jason W. Fong
 MODEL-BASED RADIOSTEREOMETRIC ANALYSIS OF AN UNCEMENTED MOBILE-BEARING TOTAL ANKLE ARTHROPLASTY SYSTEM by Jason W. Fong Submitted in partial fulfilment of the requirements for the degree of Master of Applied
MODEL-BASED RADIOSTEREOMETRIC ANALYSIS OF AN UNCEMENTED MOBILE-BEARING TOTAL ANKLE ARTHROPLASTY SYSTEM by Jason W. Fong Submitted in partial fulfilment of the requirements for the degree of Master of Applied
Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system
 Journal of Orthopaedic Surgery 2005:13(3):280-284 Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system S Asif, DSK Choon Department of Orthopaedic Surgery, University of
Journal of Orthopaedic Surgery 2005:13(3):280-284 Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system S Asif, DSK Choon Department of Orthopaedic Surgery, University of
LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS
 6 LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS J.C.T. van der Lugt R.B. Geskus P.M. Rozing Acta Orthop. 2005;76(5):654-61 Chapter 6 Abstract
6 LIMITED INFLUENCE OF PROSTHETIC POSITION ON ASEPTIC LOOSENING OF THE SOUTER-STRATHCLYDE TOTAL ELBOW PROSTHESIS J.C.T. van der Lugt R.B. Geskus P.M. Rozing Acta Orthop. 2005;76(5):654-61 Chapter 6 Abstract
Triathlon Knee System
 Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique
 ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
R/F. Can T-smart Tomosynthesis Improve Diagnostic Accuracy on THA Component Stability? 1. Abstract
 R/F Can T-smart Tomosynthesis Improve Diagnostic Accuracy on THA Component Stability? Professor and Chair Dept. of Adult Reconstructive Surgery Beijing Jishuitan Hospital, the 4th Clinical College of PKU
R/F Can T-smart Tomosynthesis Improve Diagnostic Accuracy on THA Component Stability? Professor and Chair Dept. of Adult Reconstructive Surgery Beijing Jishuitan Hospital, the 4th Clinical College of PKU
Section of total knee replacement. Total Knee Replacement System. Knieendoprothesen System. Système de prothèse totale de genou
 Section of total knee replacement Total Knee Replacement System Knieendoprothesen System Système de prothèse totale de genou Introduction: This knee system features great versality with its modular component
Section of total knee replacement Total Knee Replacement System Knieendoprothesen System Système de prothèse totale de genou Introduction: This knee system features great versality with its modular component
Bone Preservation Stem
 TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Consistency in U2 Knee System over Time
 U2 TM Knee System Consistency in U2 Knee System over Time Share the same femoral profile of all types allow inter-changibility Uniform AP/ML dimensions in all tibial components enhance intraoperative flexibility
U2 TM Knee System Consistency in U2 Knee System over Time Share the same femoral profile of all types allow inter-changibility Uniform AP/ML dimensions in all tibial components enhance intraoperative flexibility
EXPERIENCE GPS FOR TOTAL KNEE ARTHROPLASTY DETERMINE YOUR OWN COURSE.
 EXPERIENCE GPS FOR TOTAL KNEE ARTHROPLASTY DETERMINE YOUR OWN COURSE. The year 2010 marked Exactech s silver aiversary and 25 years of mobility. As a company founded by an orthopaedic surgeon and a biomedical
EXPERIENCE GPS FOR TOTAL KNEE ARTHROPLASTY DETERMINE YOUR OWN COURSE. The year 2010 marked Exactech s silver aiversary and 25 years of mobility. As a company founded by an orthopaedic surgeon and a biomedical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Range of Motion of Standard and High-Flexion Posterior Stabilized Total Knee Prostheses A PROSPECTIVE, RANDOMIZED STUDY
 1470 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Range of Motion of Standard and High-Flexion Posterior Stabilized Total Knee Prostheses A PROSPECTIVE, RANDOMIZED STUDY BY YOUNG-HOO
1470 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Range of Motion of Standard and High-Flexion Posterior Stabilized Total Knee Prostheses A PROSPECTIVE, RANDOMIZED STUDY BY YOUNG-HOO
A cementless, elastic press-fit socket with and without screws
 Acta Orthopaedica 2012; 83 (5): 481 487 481 A cementless, elastic press-fit socket with and without screws A 2-year randomized controlled radiostereometric analysis of 37 hips Dean Pakvis 1, Joan Luites
Acta Orthopaedica 2012; 83 (5): 481 487 481 A cementless, elastic press-fit socket with and without screws A 2-year randomized controlled radiostereometric analysis of 37 hips Dean Pakvis 1, Joan Luites
Avenir Femoral Hip System
 Avenir Femoral Hip System Avenir Hip System Intuitive and Reproducible During its decade of experience in the bone compaction stem market, the Avenir Hip System has helped surgeons experience flexible,
Avenir Femoral Hip System Avenir Hip System Intuitive and Reproducible During its decade of experience in the bone compaction stem market, the Avenir Hip System has helped surgeons experience flexible,
Saiph Knee System. Technical Dossier
 Saiph Knee System Technical Dossier Developed in collaboration with an international surgical team Professor Justin P Cobb Chair in Orthopaedic Surgery Imperial College Hospital, London Professor Fares
Saiph Knee System Technical Dossier Developed in collaboration with an international surgical team Professor Justin P Cobb Chair in Orthopaedic Surgery Imperial College Hospital, London Professor Fares
Foot and ankle radiographic parameters: validity and reproducibility of biplane imaging system versus conventional radiography
 Foot and ankle radiographic parameters: validity and reproducibility of biplane imaging system versus conventional radiography Chamnanni Rungpai, MD; Jessica E. Goetz, PhD; Marut Arunakul, MD; Yubo, Gao,
Foot and ankle radiographic parameters: validity and reproducibility of biplane imaging system versus conventional radiography Chamnanni Rungpai, MD; Jessica E. Goetz, PhD; Marut Arunakul, MD; Yubo, Gao,
Uniglide. Unicompartmental Knee Replacement Product overview
 Uniglide Unicompartmental Knee Replacement Product overview Uniglide History Technology Versatility Uniglide is a clinically proven highly congruent, triple radius unicompartmental knee system, offering
Uniglide Unicompartmental Knee Replacement Product overview Uniglide History Technology Versatility Uniglide is a clinically proven highly congruent, triple radius unicompartmental knee system, offering
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray
 Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Stephen R Smith Northeast Nebraska Orthopaedics PC. Ligament Preserving Techniques in Total Knee Arthroplasty
 Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Appendix E-1 (Figures and Tables) Fig. E-1
 Page 1 Appendix E-1 (Figures and Tables) Fig. E-1 Survival curves (Kaplan-Meier) for revised knees (failed primary TKAs revised to TKAs [TKA TKA] and failed primary UKAs revised to TKAs [UKA TKA]) according
Page 1 Appendix E-1 (Figures and Tables) Fig. E-1 Survival curves (Kaplan-Meier) for revised knees (failed primary TKAs revised to TKAs [TKA TKA] and failed primary UKAs revised to TKAs [UKA TKA]) according
Approach Patients with CONFIDENCE
 Design Rationale Approach Patients with CONFIDENCE The ACTIS Total Hip System is the first DePuy Synthes stem specifically designed to be utilized with tissue sparing approaches, such as the anterior
Design Rationale Approach Patients with CONFIDENCE The ACTIS Total Hip System is the first DePuy Synthes stem specifically designed to be utilized with tissue sparing approaches, such as the anterior
Total Knee Arthroplasty in a Patient with an Ankylosing Knee after Previous Patellectomy
 Case Report Knee Surg Relat Res 2014;26(3):182-186 http://dx.doi.org/10.5792/ksrr.2014.26.3.182 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Total Knee Arthroplasty in a Patient with
Case Report Knee Surg Relat Res 2014;26(3):182-186 http://dx.doi.org/10.5792/ksrr.2014.26.3.182 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Total Knee Arthroplasty in a Patient with
Tibial Base Design Factors Affecting Tibial Coverage After Total Knee Arthroplasty: Symmetric Versus Asymmetric Bases
 Tibial Base Design Factors Affecting Tibial Coverage After Total Knee Arthroplasty: Symmetric Versus Asymmetric Bases Chadd Clary, PhD I Staff Engineer I DePuy Synthes Joint Reconstruction Daren Deffenbaugh,
Tibial Base Design Factors Affecting Tibial Coverage After Total Knee Arthroplasty: Symmetric Versus Asymmetric Bases Chadd Clary, PhD I Staff Engineer I DePuy Synthes Joint Reconstruction Daren Deffenbaugh,
