Dr. Laith M. Jazrawi Chief, Division of Sports Medicine Associate Professor Department of Orthopaedic Surgery
|
|
|
- Darren McGee
- 5 years ago
- Views:
Transcription
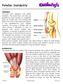
1 Dr. Laith M. Jazrawi Chief, Division of Sports Medicine Associate Professor Department of Orthopaedic Surgery Rehabilita)on Protocol Following Microfracture Procedures to the Knee There are two types of car/lage in the knee: meniscus and ar/cular. One type of car/lage is the meniscus. The knee has a medial meniscus and a lateral meniscus which together are called menisci. Menisci are semi lunar wedges that sit between the femur (thigh bone) and /bia (shin bone). The menisci are primarily composed of fibrocar/lage, with about 75% of the dry weight being type I collagen. The func/on of the menisci is to protect the other type of car/lage in the knee the ar/cular car/lage. The ar/cular car/lage is a layer of hyaline car/lage that covers the end of bones that ar/culate with other bones. In the knee there is ar/cular car/lage on the end of the femur (femoral condyles), the top of the /bia (/bial plateau) and the back of the knee cap (patella). The ar/cular car/lage has a fric/onal coefficient approximately 1/5 of ice on ice i.e. rubbing ar/cular car/lage on ar/cular car/lage would be 5x smoother than rubbing ice on ice. This allows for a very smooth gliding surface. A large por/on of ar/cular car/lage is fluid, which provides significant resistance to compressive forces.1 During athle/c trauma or injury, focal areas of the ar/cular car/lage can be damaged or torn. This is referred to as an ar/cular car/lage lesion (Figure 12). When this happens the ar/cular car/lage loses its normal smooth gliding ar/cula/on and the ability to resist compressive forces at the joint. These changes can cause pain, swelling, loss of mo/on, weakness and reduced func/on or performance. One op/on for trea/ng ar/cular car/lage lesions is a microfracture procedure. When performing a microfracture procedure, the surgeon will start by debriding any frayed /ssue or aps at the margin of the lesion (Figure 22). ARer this, the calcified chondral layer is debrided to expose the underlying subchondral bone (Figure 32). Removing this layer allows the surgeon to pick holes into the subchondral bone with an awl. (Figure 42) By picking holes in the subchondral bone, blood and fat droplets are given a pathway to flow into the defect or lesion. This develops in to a mesenchymal clot, which will mature and form in to fibrocar/lage (Figure 52) th St. New York, NY (646) newyorkortho.com!
2 Rehabilita)on Protocol Following Microfracture Procedures to the Knee The rehabilita/on process is crucial for the success of the microfracture procedure. Avoiding weight bearing exercises and engaging in frequent range of mo/on ac/vi/es are the hallmarks of the early rehabilita/on process. Ar/cular car/lage lesions are more accurately iden/fied thanks to improved imaging techniques and awareness. Many professional athletes have suffered ar/cular car/lage injuries to the knee. Greg Oden was the first selec/on in the 2007 NBA drar and was diagnosed with an ar/cular car/lage injury 4 months later. He then went on to have a microfracture procedure. This procedure has become so common in the NBA that a website has been developed that tracks the outcome of these players. The NFL also has a similar list. The return to high impact sports arer a microfracture procedure is more difficult than the return to non-impact sports and ac/vi/es of daily living.3 A successful outcome and the /me it takes to return to ac/vity is dependent on the pa/ent s age, pa/ent s body mass, lesion size, dura/on of symptoms prior to surgery, presence of arthri/s, previous surgery and post-opera/ve rehabilita/on program.2-4 Because of this, there are some pa/ents that may not be candidates for the microfracture procedure. Post-opera/ve rehabilita/on is an important factor in achieving a successful outcome from a microfracture procedure.5 The UW Health Sports Medicine rehabilita/on guidelines are presented in a criterion based progression. Specific /me frames, restric/ons and precau/ons are given to protect healing /ssues and the surgical repair/reconstruc/on. General /me frames are also given to reference the average rehabilita/on /me, but individual pa/ents will progress at different rates depending on their age, associated injuries, pre-injury health status, rehabilita/on compliance and injury severity. Injury severity refers to the size and loca/on of the ar/cular car/lage lesion. Individuals with lesions that are larger or are in predominantly weight bearing loca/ons will progress more slowly than those with smaller or non- weight bearing lesions.5 Specific aden/on must be given to impairments that caused the ini/al injury. For example if the pa/ent is status post medial compartment microfracture procedure with a varus alignment, postopera/ve rehabilita/on should include correc/ng muscle imbalances or postures that contribute to medial compartment stress th St. New York, NY (646) newyorkortho.com!
3 Phase I (Surgery to 8 weeks after surgery) Microfracture of Microfracture of Trochlea/ Patellar Defect Weightbearing: Touchdown weightbearing (20-30% of body weight max) for 6-8 weeks No Bracing Required Range of Mo)on Con/nuous Passive Mo/on (CPM) Machine for 6-8 hours per day for 6-8 weeks o Set CPM to 1 cycle per minute star/ng at level of flexion that is comfortable o Advance 10 per day un/l full flexion is achieved o Passive Range of Mo/on and stretching under guidance of PT o Quadriceps/Hamstring isometrics o Heel slides Weightbearing: Weightbearing as tolerated in hinged knee brace locked in extension Hinged Knee Brace: Locked in extension for ambula/on opened up 0-40 for ROM exercises Range of Mo)on Con/nuous Passive Mo/on (CPM) Machine for 6-8 hours per day for 6-8 weeks o Set CPM to 1 cycle per minute range from 0-40 o Passive Range of Mo/on and stretching under guidance of PT o Quadriceps/Hamstring isometrics
4 Phase II (8 weeks to 12 weeks following surgery) Trochlea/Patellar Defect Weightbearing: Advance to full weightbearing as tolerated -- discon/nue crutch use Range of Mo)on Advance to full/painless ROM o Closed chain extension exercises o Hamstring curls o Toe raises o Balance exercises o Begin use of the sta/onary bicycle/ellip/cal Weightbearing: Advance to full weightbearing as tolerated -- discon/nue crutch use Discon)nue Use of Hinged Knee Brace Range of Mo)on Advance to full/painless ROM (PROM/AAROM/AROM) o Emphasize Patellofemoral Program o Closed chain extension exercises o Hamstring curls o Toe raises o Balance exercises o Begin use of the sta/onary bicycle/ellip/cal Phase III (3 months to 6 months following surgery) Weightbearing: Full weightbearing Range of Mo)on Full/Painless ROM o Advance closed chain strengthening exercises, propriocep/on ac/vi/es o Sport-specific rehabilita/on Gradual return to athle/c ac/vity as tolerated including jumping/culng/ pivo/ng sports Maintenance program for strength and endurance Trochlea/Patellar Defect Weightbearing: Full weightbearing Range of Mo)on Full/Painless ROM o Advance closed chain strengthening exercises, propriocep/on ac/vi/es o Sport-specific rehabilita/on Gradual return to athle/c ac/vity as tolerated including jumping/culng/ pivo/ng sports Maintenance program for strength and endurance
5 References
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
MICROFRACTURE LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Rehabilitation Guidelines for Meniscal Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Athletic Preparation ACL Reconstruction - Accelerated Rehabilitation. Autologous Bone-Tendon-Bone, Patella Tendon Graft
 Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Knee Arthroscopy
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
Microfracture of Knee Joint
 Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION
 REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY
 MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
ACL Reconstruction with Hamstring Autograft Rehabilitation Protocol
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 316-631-1600 Fax: (316) 631-1674 2778 N. Webb Rd. Wichita, KS 67226 www.aoaortho.com ACL Reconstruction with Hamstring Autograft Rehabilitation Protocol
Brennen Lucas, M.D. Advanced Orthopaedic Associates 316-631-1600 Fax: (316) 631-1674 2778 N. Webb Rd. Wichita, KS 67226 www.aoaortho.com ACL Reconstruction with Hamstring Autograft Rehabilitation Protocol
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
Sheena Black, MD PHYSICAL THERAPY PRESCRIPTION MCL RECONSTRUCTION. Orthopaedic Surgery, Sports Medicine.
 PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Rehabilitation Following Unilateral Patellar Tendon Repair
 Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ACL Patella Tendon Autograft Reconstruction Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE
 KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at if you have any questions.
 OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
ACL AUTOGRAFT PATELLAR TENDON RECONSTRUCTION PLUS MENISCUS REPAIR PROTOCOL
 Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL
 ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GENERAL GUIDELINES GUIDELINES FOR REHABILITATION FOLLOWING DISTAL
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GENERAL GUIDELINES GUIDELINES FOR REHABILITATION FOLLOWING DISTAL
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL REHABILITATION FOLLOWING UNILATERAL PETELLAR TENDON REPAIR BENJAMIN J.
 I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
OSCELL MICROFRACTURE OR DRILLING OPERATION (FEMORAL CONDYLE SITES) PATIENT ADVICE.
 OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a femoral condyle articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove
OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a femoral condyle articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
Patient Information & Exercise Folder
 MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Freedom and safety in treatment
 medi GmbH & Co. KG Medicusstraße 1 95448 Bayreuth Germany T +49 921 912-0 F +49 921 912 780 ortho@medi.de www.medi.de 97E37/09.2012 Freedom and safety in treatment An informative brochure with an individual
medi GmbH & Co. KG Medicusstraße 1 95448 Bayreuth Germany T +49 921 912-0 F +49 921 912 780 ortho@medi.de www.medi.de 97E37/09.2012 Freedom and safety in treatment An informative brochure with an individual
Ellipse Rehab Phase 2 Strengthening
 Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
High Tibial Osteotomy
 High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
Rehabilitation Following ACL with Semitendinosus Reconstruction
 Page 1 of 5 Rehabilitation Following ACL with Semitendinosus Reconstruction I. IMMEDIATE POSTOPERATIVE PHASE : Goals: 1) Protect ACL reconstruction 2) Reduce swelling & inflammation 3) Restore & maintain
Page 1 of 5 Rehabilitation Following ACL with Semitendinosus Reconstruction I. IMMEDIATE POSTOPERATIVE PHASE : Goals: 1) Protect ACL reconstruction 2) Reduce swelling & inflammation 3) Restore & maintain
NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY ( Program)
 Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Medial Patellofemoral Ligament Repair/Reconstruction
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Meniscus Repair Rehabilitation Protocol
 Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Address correspondence to Michael M. Reinold, Boston Red Sox Baseball Club, Fenway Park, 4 Yawkey Way, Boston, MA
 Current Concepts in the Rehabilitation Following Articular Cartilage Repair Procedures in the Knee Journal of Orthopaedic & Sports Physical Therapy Michael M. Reinold, PT, DPT, ATC, CSCS 1 Kevin E. Wilk,
Current Concepts in the Rehabilitation Following Articular Cartilage Repair Procedures in the Knee Journal of Orthopaedic & Sports Physical Therapy Michael M. Reinold, PT, DPT, ATC, CSCS 1 Kevin E. Wilk,
Patellofemoral Osteoarthritis
 Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Common Knee Injuries
 Common Knee Injuries In 2010, there were roughly 10.4 million patient visits to doctors' offices because of common knee injuries such as fractures, dislocations, sprains, and ligament tears. Knee injury
Common Knee Injuries In 2010, there were roughly 10.4 million patient visits to doctors' offices because of common knee injuries such as fractures, dislocations, sprains, and ligament tears. Knee injury
PATELLA INSTABILITY AND REALIGNMENT
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
ACL PATELLAR TENDON AUTOGRAFT RECONSTRUCTION PROTOCOL
 Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
first four postoperative
 STEVEN K. BELOW, MD POSTOPERATIVE REHABILITATION INFORMATION AND PROTOCOL FOR ANTERIOR CRUCIATE LIGAMENT (ACL) ALLOGRA AFT/AUTOGRAFT RECONSTRUCTION This information and protocol is a guideline, individual
STEVEN K. BELOW, MD POSTOPERATIVE REHABILITATION INFORMATION AND PROTOCOL FOR ANTERIOR CRUCIATE LIGAMENT (ACL) ALLOGRA AFT/AUTOGRAFT RECONSTRUCTION This information and protocol is a guideline, individual
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis
What is Medial Plica Syndrome?
 What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
ACL Hamstring Tendon Autograft Reconstruction Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Hamstring Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Hamstring Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the
REHABILITATION PROTOCOL
 GEOFFREY S. VAN THIEL, MD/MBA Assistant Professor - Rush University Medical Center Team Physician - US National Soccer Teams Team Physician - Chicago Blackhawks Medical Network - Ice Hogs www.vanthielmd.com
GEOFFREY S. VAN THIEL, MD/MBA Assistant Professor - Rush University Medical Center Team Physician - US National Soccer Teams Team Physician - Chicago Blackhawks Medical Network - Ice Hogs www.vanthielmd.com
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
Patellar Instability. OrthoInfo Patella Instability Page 1 of 5
 Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Hip Arthroscopy Labral Repair Protocol
 Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
OSCELL MICROFRACTURE OR DRILLING OPERATION (PATELLOFEMORAL SITES) PATIENT ADVICE.
 OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a trochlea articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove on
OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a trochlea articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove on
Week 1 Orthotics- 1. Knee brace locked in full extension at all times except for rehab exercises 2. Elastic bandage as needed to control swelling
 General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
Neofitos Stefanides, M.D., P.C.
 Name: Date: Diagnosis: Date of Surgery: ACL REHAB PROTOCOL I. IMMEDIATE POSTO-OPERATIVE PHASE POD 1 Brace-brace locked at zero degrees extension for ambulation Weight bearing-weight bearing as tolerated
Name: Date: Diagnosis: Date of Surgery: ACL REHAB PROTOCOL I. IMMEDIATE POSTO-OPERATIVE PHASE POD 1 Brace-brace locked at zero degrees extension for ambulation Weight bearing-weight bearing as tolerated
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ORIF PATELLA BENJAMIN J. DAVIS, MD
 I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
Patellofemoral Replacement
 Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
l. Initiate early proprioceptive activity and progress by means of distraction techniques: i. eyes open to eyes closed ii. stable to unstable m.
 Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
MENISCAL REPAIR LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Personalized Blood Flow Restriction Rehabilitation. Anterior Cruciate Reconstruction with Meniscal Repair
 Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
REHABILITATION GUIDELINES
 REHABILITATION GUIDELINES Autologous Chondrocyte Implantation using Carticel (autologous cultured chondrocytes) Michael M. Reinold, PT, ATC* Kevin E. Wilk, PT* Jeffrey R. Dugas, MD* E. Lyle Cain, MD* Scott
REHABILITATION GUIDELINES Autologous Chondrocyte Implantation using Carticel (autologous cultured chondrocytes) Michael M. Reinold, PT, ATC* Kevin E. Wilk, PT* Jeffrey R. Dugas, MD* E. Lyle Cain, MD* Scott
Therapy following DRF Yes or No?
 Distal Radius Fractures Rehabilita6on & Ortho6c Selec6on Do you think outcomes will be the same? 1 2 Therapy following DRF Yes or No? Evidence for Therapy following DRF Level I: Systema6c Review (Handoll,
Distal Radius Fractures Rehabilita6on & Ortho6c Selec6on Do you think outcomes will be the same? 1 2 Therapy following DRF Yes or No? Evidence for Therapy following DRF Level I: Systema6c Review (Handoll,
Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Knee Injuries. PSK 4U Mr. S. Kelly North Grenville DHS. Medial Collateral Ligament Sprain
 Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Knee Injuries PSK 4U Mr. S. Kelly North Grenville DHS Medial Collateral Ligament Sprain Result from either a direct blow from the lateral side in a medial direction or a severe outward twist Greater injury
Posterior Cruciate Ligament Rehabilitation
 Posterior Cruciate Ligament Rehabilitation Phase 6: Running program for Return to Sports : 24 Weeks after surgery onward Goals: 1. Safely recondition the injured area for the demands of sports activity.
Posterior Cruciate Ligament Rehabilitation Phase 6: Running program for Return to Sports : 24 Weeks after surgery onward Goals: 1. Safely recondition the injured area for the demands of sports activity.
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
