Acromioplasty. Surgical Indications and Considerations
|
|
|
- Augusta Knight
- 5 years ago
- Views:
Transcription
1 1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic (intratendinous) and extrinsic (extratendinous) factors have been implicated as etiologies of the impingement process. The unique anatomy of the shoulder joint sandwiches the soft tissue structures of the subacromial space (rotator cuff tendons, coracoacromial ligament, long head of biceps, bursa) between the overlying anterior acromion, acromioclavicular joint, coracoid process, underlying greater tuberosity of the humeral head and the superior glenoid rim. Pathogenesis: When subacromial impingement is suspected it is necessary to differentiate primary from secondary impingement. This is essential for successful treatment. Primary subacromial impingement is the result of an abnormal mechanical relationship between the rotator cuff and the coracoacromial arch. Secondary impingement is a clinical phenomenon that results in relative narrowing of the subacomial space. This often results from glenohumeral or scapulothoracic joint instability. The loss of the stabilizing function of the rotator cuff also leads to an abnormal superior translation of the humeral head (decreased depression of the humeral head during overhead activity and less clearance ) and mechanical impingement of the rotator cuff on the coracoacromial arch. In patients who have scapular instability, impingement results from improper positioning of the scapula with relation to the humerus. The instability leads to the insufficient retraction of the scapula, which allows for earlier contact of the coracoacromial arch on the underlying rotator cuff. Epidemiology: Patients with primary impingement are usually older than 40 years, complain of anterior shoulder and lateral upper arm pain, with an inability to sleep on the affected side. They have complaints of shoulder weakness, and difficulty performing overhead activities. Patients with secondary impingement are usually younger and often participate in overhead sporting activities such as baseball, swimming, volleyball, or tennis. They complain of pain and weakness with overhead motions and may even describe a feeling of the arm going dead. Diagnosis History and physical examination are crucial in diagnosing subacromial impingement syndrome because findings may be subtle and symptoms may overlap with various differential diagnoses Physical examination focuses on shoulder and cervical spine. Cervical spine must be cleared to rule out cervical radiculopathy, degenerative joint disease, and other disorders of the neck contributing to referred pain in the shoulder. Primary impingement: o (+) Hawkins sign o (+) Neer impingement sign o Possible associated AC joint arthritis (tenderness to palpation and increased pain with horizontal adduction)
2 2 Secondary impingement: look for associated pathology o GH instability: (+) apprehension and relocation test, load and shift o Abnormal scapular function: scapular winging, scapular dyskinesia o Posterior capsule tightness: leads to an obligatory translation of the humeral head and rotator cuff in an anterior and superior direction, which contributes to impingement problem. Radiographs are helpful in demonstrating acromial anatomy types, hypertrophic coracoacromial ligament spurring, acromioclavicular joint osteoarthritis, and calcific tendonitis. MRI can be helpful in revealing relationships in impingement syndrome, especially if rotator cuff tear and other internal derangement pathologies are suspected. Nonoperative Versus Operative Management: Nonoperative treatment is very successful and the comprehensive rehabilitative protocols for primary and secondary impingement syndrome are similar and follow the postoperative rehabilitation plan for patients who have had a subacromial decompression with a normal rotator cuff. Initial goals of the rehabilitation process are to obtain pain relief and regain range of motion. Various modalities, oral medications and corticosteroid subacromial injections are helpful in the early stages to decrease the inflammatory process allowing for more successful advances in motion and strengthening. Strengthening exercises begin by avoiding impingement positions while performing the exercises. The focus is on closed kinetic chain exercises initially with open chain exercises to follow without aggravating shoulder discomfort. These exercises help to restore the ability of the rotator cuff to dynamically depress and stabilize the humeral head, resulting in a gradual relative increase in the subacromial space. Nonoperative treatment should be considered unsuccessful if the patient shows no improvement after 3 months of a comprehensive and coordinated medical and rehabilitative program. In addition, after 6 months of appropriate treatment, most patients have achieved maximal improvement from the nonoperative treatment program. The success of operative treatment is determined by the choice of an appropriate operative procedure and the skills of the surgeon. It is imperative to determine whether the patient has a primary or secondary impingement. For primary impingement the procedure of choice presently is arthroscopic subacromial decompression, although comparable long-term results can be obtained with a traditional open acromioplasty. Arthroscopic subacromial decompression has many advantages including the ability to evaluate the glenohumeral joint for associated labral, rotator cuff, and biceps pathology, as well as assessment of the acromioclavicular joint. Second, this technique produces less postoperative morbidity and is relatively noninvasive, minimizing deltoid muscle fiber detachment. However, arthroscopic subacromial decompression is a technically demanding procedure and the surgeon must be very skilled. When glenohumeral joint instability is the reason for secondary impingement, surgical treatment is a stabilization procedure. Surgical Procedure: Many different arthroscopic techniques have been described, but one that is often recommended is the modified technique initially described by Caspari and Thaw. Using standard posterior portal, the surgeon inserts the arthroscope into the glenohumeral joint and evaluates for pathology including biceps tendon, labrum and rotator cuff. Any incidental pathology can be addressed arthroscopically at this time prior to subacromial space arthroscopy being performed. Starting from the posterior portal and using an aggressive synovial resector with the inflow in the anterior portal, the surgeon uses the lateral portal to perform a bursectomy
3 3 and debride the soft tissues of the subacromial space. This is done in a sequential manner, working from the lateral bursal area to the anterior and medial acromioclavicular regions. After the subacromial bursectomy and denudement of the undersurface of the acromion, the superior rotator cuff can be visualized along the acromioclavicular joint and anterior acromial anatomy is more easily defined. The surgeon must be careful not to disturb the coracoacromial ligament during the initial bursectomy procedure. Next the surgeon performs sequential acromioplasty with an acromionizer instrument with the therapeutic goal of a flat type I acromion and removal of the coracoacromial ligament from its bony attachment. In addition, the acromioclavicular joint may be assessed at this point and minimal inferior osteophytes may be excised. Lastly, dependent on preoperative evaluation the surgeon may choose to perform a distal clavicle excision (usually cm). Surgical outcomes for arthroscopic subacromial decompression, partial acromioplasties, and distal clavical excisions have been favorable. Most surgical failures are associated with incomplete bone resection and not addressing acromioclavicular joint arthropathy. POSTOPERATIVE REHABILITATION Note: The following rehabilitation progression is a summary of the guidelines provided by Phillips and Tippet. Refer to their publication to obtain further information regarding criteria to progress from one phase to the next, anticipated impairments and functional limitations, interventions, goals, and rationales. Postoperative rehabilitation can be divided into three phases: 1. Phase one emphasizes a return of range of motion 2. Phase two stresses regaining muscle strength 3. Phase three stresses endurance and functional progression Phase I: Return of range of motion: Weeks 0-3 Goals: Days: 1-10 Control normal postoperative inflammation and pain Prevent infection Protect healing soft tissues Minimize effects of immobilization and activity restriction Days: Flexion PROM to 150º External/internal rotation PROM to functional levels Supine AROM flexion to 120º
4 4 Phase I a & b (first 10 days post op) Cryotherapy Grip strengthing exercises Passive range of motion as indicated Isometrics (Submaximal to maximal internal and external rotation) Active range of motion (scapular retraction/protraction) Joint mobilizations (sternoclavicular and acromioclavicular joints as indicated) Phase I c (11-21 days post op) Active range of motion: o External rotation (at 60º-90º abduction) o Supine flexion, scapular protraction o Sidelying external rotation o Prone scapular retraction Cardiovascular exercise, pool therapy Return to limited work duties (depending on job tasks) Phase II: Regaining muscle strength: Weeks 3-8 Goals: Control any residual symptoms of inflammation and pain Full PROM in all ranges Symmetric flexion AROM AROM flexion in standing to shoulder height without substitution Emphasis on muscle strengthening with continued work on rotator cuff musculature and scapula stabilizer strengthening Continue range of motion efforts if limited capsular extensibility detrimentally affects physiologic motion Restoration of normal arm strength ratios (involved/uninvolved) Return to previous levels of activities/sport Prevention of poor throwing mechanics Progressive resistance exercises for rotator cuff musculature and scapular stabilizers Joint mobilizations as indicated Proprioceptive neuromuscular retraining Towards end of phase 2 begin progressive throwing program and gentle plyometrics
5 5 Phase III: Endurance and Functional Progression: Weeks 9-12 Goals: Unrestricted overhead work and sporting activity Focus on enhancing kinesthesia and joint position sense Muscular endurance Performing work-specific and sport-specific tasks Exercises to improve both passive detection of shoulder movement and active joint repositioning for enhanced kinethesia and joint positioning sense Decreased weight with increased repetitions during strengthening exercises of rotator cuff and scapular stabilizers. Emphasis on timing of muscle contraction and movement without substitution (proprioceptive neuromuscular facilitation) Functional progression program involving a series of sport or work-specific basic movement patterns graduated according to the difficulty of the skill and the patient s tolerance. Selected References: Caspari R: A technique for arthroscopic S.A.D., Arthroscopy. 1992;8:23. Gartsman GM et al: Arthroscopic subacromial decompression. an anatomical study, Am J Sports Med. 1988;16:48. Jobe FW: Impingement problems in the athlete. In Nicholas JA, Hershamann EB, eds. The Upper Extremity in Sports Medicine. St Louis, Mosby, Jobe FW, Jobe CM: Painful athletic injuries of the shoulder. Clin orthop., 1989; 173: Paulos LE, Franklin JC: Arthroscopic S.A.D. Development and application: a 5 year experience. Am J Sports Med. 1990; 18:235. Phillips P, Tippett S. Acromioplasty. In Maxey L, Magnusson J, eds, Rehabilitation for the Postsurgical Orthopedic Patient. St. Louis, Mosby, Wilk KE, Meister K, Andrews JR: Current concepts in the rehabilitation of the overhead throwing athlete. Am J Sports Med. 2002; 30: Wilk KE: The shoulder. In Malone TR, McPoil T, Nitz AJ, editors: Orthopaedic and sports physical therapy, ed 3, St Louis, Mosby, 1997.
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy
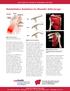 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
Rehabilitation Guidelines for Large Rotator Cuff Repair
 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE
 ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative
ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) BENJAMIN J. DAVIS, MD
 I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative effects of immobilization Promote dynamic stability Diminish pain and inflammation
I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative effects of immobilization Promote dynamic stability Diminish pain and inflammation
Rehabilitation of Overhead Shoulder Injuries
 Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Chronic Shoulder Disorders
 Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
Shoulder joint Assessment and General View
 Shoulder joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The shoulder contains
Shoulder joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The shoulder contains
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR
 REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
The ball-and-socket articulation at the glenohumeral joint is between the convex
 SLAP Lesion Repair Emily Cotey, Emily Hurysz, and Patrick Schroeder Abstract SLAP lesion, which stands for Superior Labrum Anterior and Posterior, is a detachment tear of the superior labrum that originates
SLAP Lesion Repair Emily Cotey, Emily Hurysz, and Patrick Schroeder Abstract SLAP lesion, which stands for Superior Labrum Anterior and Posterior, is a detachment tear of the superior labrum that originates
Nonoperative Treatment of Subacromial Impingement Rehabilitation Protocol
 Therapist Nonoperative Treatment of Subacromial Impingement Rehabilitation Protocol Subacromial impingement is a chronic inflammatory process produced as one of the Rotator Cuff Muscle the and the Subdeltoid
Therapist Nonoperative Treatment of Subacromial Impingement Rehabilitation Protocol Subacromial impingement is a chronic inflammatory process produced as one of the Rotator Cuff Muscle the and the Subdeltoid
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
DK7215-Levine-ch12_R2_211106
 12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
The shoulder that won t get better.
 The shoulder that won t get better. www.fisiokinesiterapia.biz Shoulder Injuries Acute Chronic Acute shoulder injuries Instability Labral pathology (SLAP lesions) Fractures (clavicle, scapula, humerus)
The shoulder that won t get better. www.fisiokinesiterapia.biz Shoulder Injuries Acute Chronic Acute shoulder injuries Instability Labral pathology (SLAP lesions) Fractures (clavicle, scapula, humerus)
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Recurrent Shoulder Dislocation.
 Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
PHASE I (Begin PT 3-5 days post-op) DOS:
 REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
2015 OPSC Annual Convention. syllabus. February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California
 2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California THURSDAY, FEBRUARY 5, 2015: 3:30pm - 4:30pm The Shoulder: 2 View or Not 2 View * Presented by Alexandra
2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California THURSDAY, FEBRUARY 5, 2015: 3:30pm - 4:30pm The Shoulder: 2 View or Not 2 View * Presented by Alexandra
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Stefan C Muzin, MD PM&R Attending Physician, Beth Israel Deaconess Medical Center, Harvard Medical School Onsite Physiatrist, GE Aviation, Lynn, MA
 Stefan C Muzin, MD PM&R Attending Physician, Beth Israel Deaconess Medical Center, Harvard Medical School Onsite Physiatrist, GE Aviation, Lynn, MA Consultant, OEHN (Occupational and Environmental Network)
Stefan C Muzin, MD PM&R Attending Physician, Beth Israel Deaconess Medical Center, Harvard Medical School Onsite Physiatrist, GE Aviation, Lynn, MA Consultant, OEHN (Occupational and Environmental Network)
Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SLAP Lesions Assessment & Treatment
 SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
SLAP Lesion Type II Repair Rehabilitation Program
 SLAP Lesion Type II Repair Rehabilitation Program The GLSM SLAP Type II Repair Rehabilitation Program is an evidence-based and soft tissue healing dependent program allowing patients to progress to vocational
SLAP Lesion Type II Repair Rehabilitation Program The GLSM SLAP Type II Repair Rehabilitation Program is an evidence-based and soft tissue healing dependent program allowing patients to progress to vocational
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
WEEKEND 2 Shoulder. Shoulder Active Range of Motion Assessment
 Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Shoulder Shoulder Active Range of Motion Assessment - Patient Positioning: Standing, appropriately undressed so that
Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Shoulder Shoulder Active Range of Motion Assessment - Patient Positioning: Standing, appropriately undressed so that
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Joint G*H. Joint S*C. Joint A*C. Labrum. Humerus. Sternum. Scapula. Clavicle. Thorax. Articulation. Scapulo- Thoracic
 A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
Increase referrals and revenue by incorporating diagnosis and conservative management of subacromial impingement syndrome
 IN THIS ISSUE Issue: July 2002 Rubbing Shoulders by Craig D. Cook, DC, CCSP, QME Normal Version Increase referrals and revenue by incorporating diagnosis and conservative management of subacromial impingement
IN THIS ISSUE Issue: July 2002 Rubbing Shoulders by Craig D. Cook, DC, CCSP, QME Normal Version Increase referrals and revenue by incorporating diagnosis and conservative management of subacromial impingement
Arthroscopic Anterior Capsulolabral Repair Protocol
 PHASE I: POST-OP WEEKS 0-6 Goals: Arthroscopic Anterior Capsulolabral Repair Protocol Bart Eastwood D.O. 250 South Main St. Suite 224A Blacksburg, VA 24060 540-552-7133 Maximally protect the surgical repair
PHASE I: POST-OP WEEKS 0-6 Goals: Arthroscopic Anterior Capsulolabral Repair Protocol Bart Eastwood D.O. 250 South Main St. Suite 224A Blacksburg, VA 24060 540-552-7133 Maximally protect the surgical repair
Shoulder Arthroscopy Curriculum
 ARTHRO Mentor 1 Description All those with an interest in the shoulder should develop a basic level of proficiency and should be able to perform a thorough diagnostic exam, looking from both the anterior
ARTHRO Mentor 1 Description All those with an interest in the shoulder should develop a basic level of proficiency and should be able to perform a thorough diagnostic exam, looking from both the anterior
Management of Massive/Revision Rotator Cuff Tears
 Management of Massive/Revision Rotator Cuff Tears Nikhil N. Verma MD, Director Sports Medicine, Rush University Medical Center, Midwest Orthopedics at Rush, Chicago, IL nverma@rushortho.com I. Anatomy
Management of Massive/Revision Rotator Cuff Tears Nikhil N. Verma MD, Director Sports Medicine, Rush University Medical Center, Midwest Orthopedics at Rush, Chicago, IL nverma@rushortho.com I. Anatomy
Shoulder Impingement Rehabilitation Recommendations
 Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder: Clinical Anatomy, Kinematics & Biomechanics
 Shoulder: Clinical Anatomy, Kinematics & Biomechanics Dr. Alex K C Poon Department of Orthopaedics & Traumatology Pamela Youde Nethersole Eastern Hospital Clinical Anatomy the application of anatomy to
Shoulder: Clinical Anatomy, Kinematics & Biomechanics Dr. Alex K C Poon Department of Orthopaedics & Traumatology Pamela Youde Nethersole Eastern Hospital Clinical Anatomy the application of anatomy to
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Work-related shoulder pain
 Work-related shoulder pain Stadler Kirsten M.B., Ch.B. (1987) (Pret), M. Med. (Orthop) (1998) (Stell.), Orthopaedic Surgeon, Room 333, Louis Leipoldt Medical Centre, Broadway Street, Bellville Cape Town
Work-related shoulder pain Stadler Kirsten M.B., Ch.B. (1987) (Pret), M. Med. (Orthop) (1998) (Stell.), Orthopaedic Surgeon, Room 333, Louis Leipoldt Medical Centre, Broadway Street, Bellville Cape Town
The Shoulder. Jill Inouye Primary Care Sports Medicine Family Medicine Resident School February 26, 2014
 The Shoulder Jill Inouye Primary Care Sports Medicine Family Medicine Resident School February 26, 2014 Objectives Review shoulder anatomy Explain and demonstrate shoulder physical exam Diagnosis and management
The Shoulder Jill Inouye Primary Care Sports Medicine Family Medicine Resident School February 26, 2014 Objectives Review shoulder anatomy Explain and demonstrate shoulder physical exam Diagnosis and management
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Reverse Total Shoulder
 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Throwing Injuries and Prevention: The Physical Therapy Perspective
 Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Common Surgical Shoulder Injury Repairs
 Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Diagnostic and Management Approach to the Painful Shoulder
 Diagnostic and Management Approach to the Painful Shoulder Introduction What conditions causing shoulder pain commonly present in General Practice? Subacromial impingement Rotator cuff tears AC joint pathology
Diagnostic and Management Approach to the Painful Shoulder Introduction What conditions causing shoulder pain commonly present in General Practice? Subacromial impingement Rotator cuff tears AC joint pathology
Returning the Shoulder Back to Optimal Function. Scapula. Clavicle. Humerus. Bones of the Shoulder (Osteology) Joints of the Shoulder (Arthrology)
 Returning the Shoulder Back to Optimal Function Sternum Clavicle Ribs Scapula Humerus Bones of the Shoulder (Osteology) By Rick Kaselj Clavicle Scapula Medial Left Anterior Clavicle Inferior View 20 degree
Returning the Shoulder Back to Optimal Function Sternum Clavicle Ribs Scapula Humerus Bones of the Shoulder (Osteology) By Rick Kaselj Clavicle Scapula Medial Left Anterior Clavicle Inferior View 20 degree
Structure and Function of the Bones and Joints of the Shoulder Girdle
 Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Shoulder Labral Tear and Shoulder Dislocation
 Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
AC reconstruction Protocol: Dr. Rolf
 AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete)
 ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete) This rehabilitation program's goal is to return the patient/athlete to their activity/sport as quickly and safely as
ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete) This rehabilitation program's goal is to return the patient/athlete to their activity/sport as quickly and safely as
REMINDER. an exercise program. Senior Fitness Obtain medical clearance and physician s release prior to beginning
 Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Continuing Education: Shoulder Stability
 Continuing Education: Shoulder Stability Anatomy & Kinesiology: The GHJ consists of the articulation of three bones: the scapula, clavicle and humerus. The scapula has three protrusions: the coracoid,
Continuing Education: Shoulder Stability Anatomy & Kinesiology: The GHJ consists of the articulation of three bones: the scapula, clavicle and humerus. The scapula has three protrusions: the coracoid,
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Vol 3, 2008 CEC ARTICLE: Special Medical Conditions Part 2: Shoulder Maintenance and Rehab C. Eggers
 Vol 3, 2008 CEC ARTICLE: Special Medical Conditions Part 2: Shoulder Maintenance and Rehab C. Eggers SHOULDER GIRDLE STABILIZATION Knowledge of the anatomy and biomechanics of the shoulder girdle is essential
Vol 3, 2008 CEC ARTICLE: Special Medical Conditions Part 2: Shoulder Maintenance and Rehab C. Eggers SHOULDER GIRDLE STABILIZATION Knowledge of the anatomy and biomechanics of the shoulder girdle is essential
ARTHROSCOPIC DECOMPRESSION PROTOCOL Dr. Steven Flores
 ARTHROSCOPIC DECOMPRESSION PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following an arthroscopic decompression surgical procedure. The arthroscopic decompression
ARTHROSCOPIC DECOMPRESSION PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following an arthroscopic decompression surgical procedure. The arthroscopic decompression
Large/Massive Rotator Cuff Repair
 Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Shoulder examination. P Sripathi Rao Arthroscopy & Sports Injuries Unit Dean, Kasturba Medical College
 Shoulder examination P Sripathi Rao Arthroscopy & Sports Injuries Unit Dean, Kasturba Medical College Manipal University, Manipal Common symptoms Tingling Numbness Pain Loss of movements Weakness Approach
Shoulder examination P Sripathi Rao Arthroscopy & Sports Injuries Unit Dean, Kasturba Medical College Manipal University, Manipal Common symptoms Tingling Numbness Pain Loss of movements Weakness Approach
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
 www.simonmoyes.com+ www.shoulder-arthroscopy.co.uk Impingement)and)Rotator)Cuff) Tears) Presented+by+Mr+Simon+Moyes+ Shoulder)Experience) RNOH)shoulder)unit) Visi7ng)fellow)Royal)North)Shore,)Sydney) RNOH)shoulder)fellow)
www.simonmoyes.com+ www.shoulder-arthroscopy.co.uk Impingement)and)Rotator)Cuff) Tears) Presented+by+Mr+Simon+Moyes+ Shoulder)Experience) RNOH)shoulder)unit) Visi7ng)fellow)Royal)North)Shore,)Sydney) RNOH)shoulder)fellow)
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Rehabilitation Guidelines for Biceps Tenodesis with Hardware Fixation
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Biceps Tenodesis with Hardware Fixation The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Biceps Tenodesis with Hardware Fixation The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms
Mercer County Community College Donna Doulong March 8, 2013
 Mercer County Community College Donna Doulong March 8, 2013 Why strengthen the scapular muscles? The scapular thoracic articulation is the true core of the upper extremity. (Shankman & Manske, 2011, p.
Mercer County Community College Donna Doulong March 8, 2013 Why strengthen the scapular muscles? The scapular thoracic articulation is the true core of the upper extremity. (Shankman & Manske, 2011, p.
