Developmental Dislocation of the Hip Successfully Treated by Preoperative Traction and Medial Open Reduction: A 22-year Mean Followup
|
|
|
- Shanon Dalton
- 5 years ago
- Views:
Transcription
1 Clin Orthop Relat Res (2015) 473: DOI /s Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Developmental Dislocation of the Hip Successfully Treated by Preoperative Traction and Medial Open Reduction: A 22-year Mean Followup P. Farsetti MD, R. Caterini MD, V. Potenza MD, E. Ippolito MD Received: 14 October 2014 / Accepted: 13 March 2015 / Published online: 1 April 2015 The Association of Bone and Joint Surgeons Abstract Background During the last 35 years, the medial approach has been reported more frequently than the anterior approach for open reduction of developmental dislocation of the hip (DDH), however, few studies have followed children treated by medial open reduction to adulthood. Questions/purposes The purposes of our study were: (1) to assess the development of 71 completely dislocated hips after medial open reduction, the incidence of additional surgery and avascular necrosis during the followup period, and the long-term radiographic and functional results; and (2) to compare our results with those obtained by others who performed open reduction either by the medial or anterior approach. Patients and Methods We retrospectively evaluated, after the end of growth, 71 hips in 52 patients who underwent open reduction by the medial approach. The mean age of the patients was 16 months (range, 3 36 months). After surgery, the hips were immobilized in 100 flexion, 60 abduction, and neutral rotation for an average of 6 months. All patients had staged clinical and radiographic followups until skeletal maturity. The length of followup averaged 22 years (range, years). Results In all the surgically treated hips, the acetabular index normalized by the end of growth, the incidence of avascular necrosis was 18%, and additional surgery was required in 15% of our cases. At the last followup, 93% of the hips were classified as Severin Classes I or II and 7% as Class III; 76% of the hips had an excellent result, 17% had a good result, and 7% had a fair result according to the McKay scale as modified by Barrett and colleagues. Conclusions Open reduction of DDH through a medial approach provided good long-term radiographic and functional results in patients 3 to 36 months old and it was the only surgery performed in 85% of our cases. Future comparative studies are needed to confirm our results, especially in older children. Level of evidence Level IV, therapeutic study. Each author certifies that he or she, or a member of his or her immediate family, has no funding or commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article. All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research 1 editors and board members are on file with the publication and can be viewed on request. Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained. P. Farsetti, R. Caterini, V. Potenza, E. Ippolito (&) Department of Orthopaedic Surgery, University of Tor Vergata, Viale Oxford, 81, Rome, Italy ippolito@med.uniroma2.it Introduction The incidence of complete dislocation of the hip as the final step of developmental dysplasia of the hip (DDH) has decreased attributable mostly to early diagnosis and treatment [8, 15, 19, 28, 29, 55, 87]; however, cases of complete dislocation, requiring open reduction still occur. Open reduction for treatment of a complete dislocation of the hip may be performed either by an anterior or medial approach. During the last 36 years, the anterior approach has been reported less frequently [1, 10, 17, 18, 20, 23, 25, 30, 31, 47, 58, 70, 71, 73, 79, 80] than the medial approach [4, 6, 7, 11, 16, 21, 22, 33, 36, 37, 39, 40, 46, 48 50, 52 54, 60, 69, 77, 78, 85, 88], especially in younger children.
2 Volume 473, Number 8, August 2015 DDH Treated by Medial Open Reduction 2659 Independently of the approach, various complications have been reported and in some of the previously cited series, the incidence of complications is high. It is known that the final result of DDH after open reduction can be evaluated only when musculoskeletal growth is completed [81], but to our knowledge, there is a paucity of studies including skeletally mature patients [5, 18, 30, 33, 39, 52, 71, 78 80]. The purposes of our study were: (1) to assess the development of completely dislocated hips after medial open reduction, the incidence of additional surgery and avascular necrosis during the followup period, and the long-term radiographic and functional results; and (2) to compare our results with those obtained by others who used either medial or anterior open reduction. Patients and Methods From January 1980 to December 2000, a total of 512 children ranging in age from 2 months to 7 years (mean age, 11 months) underwent treatment for DDH at our institution. Treatment included either bracing, plaster casting, or surgery depending on the evolutive stage of the DDH and its severity. Whenever open reduction of a hip dislocation was required, we used a medial approach in children up to 36 months old and an anterior approach in older children. One-hundred-sixty-nine consecutive patients (234 hips) who had unreducible complete hip dislocation were treated by or under the direct supervision of the four authors in accordance with the directions of the senior author (EI). All patients who had started any treatment elsewhere, including prior bracing or use of a Pavlik harness, and patients with teratologic, neuromuscular, or syndromic dislocation, were not included in our study. Since 1980, the protocol at our institution for managing unreducible, complete developmental hip dislocation consisted of traction in bed for 4 weeks; attempt at closed reduction with gentle maneuvers using general anesthesia; and whenever closed reduction was not achieved or there was concern that it could be unstable in 100 flexion, 60 abduction, and neutral rotation, an open reduction was performed at the same time. Of 169 patients with unreducible hip dislocations, 82 patients (112 hips) had successful closed reduction under general anesthesia. Closed reduction was considered safe when the hip was stable at 100 flexion, 60 abduction, and in neutral rotation [45]. Arthrography was not performed routinely in hips that had closed reduction. The patients ranged from 3 to 21 months old (mean age, 9 months). Eighty-seven patients (122 hips) in whom closed reduction either was not achieved or was thought to be unstable in 100 flexion, 60 abduction, and neutral rotation had open reduction through a medial approach as described by Weinstein and Ponseti [85]. A transverse incision was made parallel and 1 cm distal to the inguinal fold extending from a point just medial to the femoral neurovascular bundle to the medial border of the adductor longus muscle that was isolated and sectioned. The anterior branch of the obturator nerve was identified under the pectineus muscle that was retracted medially. The iliopsoas tendon was identified and sectioned just above the lesser trochanter and the medial circumflex artery and vein were ligated. The articular capsule then was opened along its longitudinal axis and a second perpendicular incision of the capsule was made parallel to the medial border of the acetabulum. The joint was inspected and all the obstacles to the concentric reduction of the femoral head (ligamentum teres, fibrofatty tissue of the pulvinar, transverse acetabular ligament) were removed. The neolimbus (inverted labrum) was never an obstacle to reduction but rather a posterior stabilizer of the femoral head after reduction. Surgery was performed by one of the four authors; residents were part of the surgical team but they did not perform the medial open reduction independently. The 87 patients (122 hips) who had medial open reduction were enrolled in our retrospective study. Twelve patients (16 hips) were lost to followup because they had moved elsewhere and it was not possible to contact them. We were able to locate 75 patients (106 hips), but only 57 (79 hips) agreed to return for clinical and radiographic followups. Eighteen patients (27 hips) contacted by telephone declined our invitation because they lived far from our hospital, but 10 of them (14 hips) agreed to send recent radiographs of their pelvis. Of the 57 patients (79 hips) who came to the hospital, five (eight hips) did not have initial radiographs in their records whereas 52 (71 hips) had a full set of radiographs taken according to our followup schedule and they were included in the statistical analysis of the study. The eight patients (14 hips) who had only telephone interview, the 10 patients who had telephone interview and who mailed recent radiographs, and the five patients who came to the hospital but had an incomplete set of radiographs were included in the final followup but were excluded from the statistical analysis of the study (Fig. 1). The age of the patients at the time of diagnosis ranged from 3 to 36 months (mean age, 16 months). In all cases, medial open reduction was performed after the patient underwent 4 weeks of traction after diagnosis. Forty-two patients were girls and 10 were boys. Forty left hips and 31 right hips were dislocated. Twenty-five patients had bilateral DDH, but in six of the 25, one dislocated hip had successful closed reduction. We divided the 52 patients (71 hips) who underwent medial open reduction into three age groups to evaluate the influence of age at surgery on the
3 2660 Farsetti et al. Clinical Orthopaedics and Related Research 1 87 patients 122 hips Patients with complete DDH treated by medial open reduction 12 patients 16 hips Lost to followup Unable to contact 75 patients 106 hips Located and contacted by phone 13% 18 patients 27 hips Did not return to hospital for followup 57 patients 79 hips Returned to hospital for followup 10 patients 14 hips Telephone interview and radiographic followup; no clinical evaluation 8 patients 13 hips Telephone interview; no clinical and radiographic followups 52 patients 71 hips Full set of radiographs and clinical and radiographic followups 5 patients 8 hips Incomplete set of radiographs and clinical and radiographic followups Not included in the statistics of the study Not included in the statistics of the study Included in the statistics of the study Not included in the statistics of the study 12% 8% 61% 6% Fig. 1 The flow-diagram of the patients enrolled in the study is shown. development of the hip during growth and on the complication rate and long-term results. All the patients underwent 4 weeks of traction before surgery. To obtain valid traction, a hip spica cast was applied to the contralateral hip. Two strings were sealed to the back of the plaster cast that was firmly anchored to the head of the bed [41]. Skin traction then was applied to the dislocated hip in approximately 20 flexion, 20 abduction, and 20 external rotation. Since 1989, owing to increased hospital costs, traction has been an outpatient procedure and it is maintained by the patient afterward at home. Before traction, the height of the dislocation was graded according to Gibson and Benson [27] (Table 1). After surgery, a bilateral hip spica cast was applied in 100 flexion, 60 abduction, and neutral rotation. Six weeks later, radiographs were taken and a second bilateral spica cast, in the same position, was applied for 6 more weeks; thereafter, an abduction brace was applied full time for an average of 4 months. The patient then was allowed to crawl and walk freely, keeping the brace on only at night for 2 more years. Two hips in two patients redislocated while the patients were wearing the plaster cast, and a second medial open reduction stabilized with a 1.8-mm thick K-wire crossing the joint was performed in each patient. After cast removal, patients had clinical and radiographic examinations at regular intervals of 3, 6, 12, 18, and 24 months, then once a year until 7 years of age, and then once every 2 years until menarche in girls and puberty in boys. Families of six patients (nine hips) refused the last followup radiographs that should have been taken at puberty. The senior author (EI) measured the following radiographic parameters once a week for 3 consecutive weeks using a computer metric program: the (1) acetabular index [43]; (2) lateral instability index [68]; (3) Wiberg angle [86]; (4) anterior coverage of the femoral head [42]; (5) Sharp angle [67], and the (6) neck-shaft and femoral anteversion angles [75]. The intraobserver j-score was Avascular necrosis (AVN) of the proximal femoral epiphysis was classified according to the Bucholz and Ogden classification [13] modified by Morcuende et al. [50]. Additional surgery was performed either in symptomatic cases or in cases in which the radiographic parameters were persistently altered, with risk of subluxation [81]. At the last followup, clinical results were graded using the criteria of McKay modified by Barrett et al. [9] and radiographic results were classified according to Severin [66].
4 Volume 473, Number 8, August 2015 DDH Treated by Medial Open Reduction 2661 Table 1. Three patient age groups Dislocation height according to Gibson and Benson classification [27] Group 1 Age 3 12 months 22 patients*/26 hips (9 bilateral; 13 unilateral) Group 2 Age months 19 patients /27 hips (9 bilateral; 10 unilateral) Group 3 Age months 11 patients/18 hips (7 bilateral; 4 unilateral) High Intermediate Low * One hip in each of five patients with bilateral DDH had successful closed reduction; one hip in one patient with bilateral DDH had successful closed reduction; DDH = developmental dislocation of the hip. Statistical analysis was performed using SPSS Version 15.0 (SPSS Inc, Chicago, IL, USA). Descriptive statistics consisted of the mean ± SD for parameters with Gaussian distributions (after confirmation with the Kolmogorov- Smirnov test) or median and range (minimum-maximum) for non-gaussian parameters. Comparison among groups of Gaussian parameters was performed with one-way plus multiple-comparison ANOVA using the Bonferroni and Kruskal-Wallis tests for non-gaussian parameters. For numbers, frequencies (%), or categoric variables, comparisons among groups were performed with the chi-square test or Fisher s exact test (in a contingency table with cell frequencies less than 5). A p value less than 0.05 was considered statistically significant. The length of followup ranged from 13 to 32 years, with an average of 22 years. At final followup, all patients were skeletally mature. The study was approved by our institutional ethical board. Results At diagnosis, the acetabular index averaged 40. It improved rapidly during the first year after open reduction and then slowly, reaching a standard value on average 4 years after open reduction (range, years) (Fig. 2). Improvement in the acetabular index occurred more quickly in patients in Group 1 who were 3 to 12 months old than in the other two groups (Fig. 3). In 28 children with DDH who were 14 months and older, several small centers of ossification developed in the acetabular cartilage which became fully ossified by gradual coalescence of the ossification centers (Fig. 4). The lateral stability index of Smith et al. [68] always scored within normal limits ( ), even when the acetabular index remained abnormal (Fig. 4). All the children had limited ROM of the hip after weaning from the brace, but all recovered a normal gait. No patient reported any limitations of activities of daily life and 35 patients had become involved in sport activities. During the followup, 10 patients (11 hips) had additional surgery for a total of 13 procedures (15%): seven Tönnis periacetabular osteotomies [76], five varus derotation femoral osteotomies, and one distal transfer of the greater trochanter. Before surgery, four patients were symptomatic. Three patients ranging in age from 14 to 15 years with acetabular insufficiency (Wiberg \ 20 ) had a painful limp after prolonged walking or sporting activities. One 13-yearold patient was limping owing to 2.5-cm femoral shortening attributable to Grade III AVN. No statistically significant differences were found between age group and additional surgeries (p = 0.229). Three patients had a transient mild limp after the varus derotation femoral osteotomy. No patient required an arthroplasty at the time of the last followup (Table 2). AVN Grades II to V developed in 13 hips (18.3%) (Figs. 3, 4). AVN was significantly different among the three groups of patients (p = 0.002) and three levels of dislocation (p = 0.001) [27]. AVN developed in one of 22 hips without the ossification center of the femoral head and in 12 of 49 hips with the ossification center. One patient with Grade III AVN had 2 cm lower limb shortening and he started to limp when he was 10 years old (Table 3). At the last followup three patients with Grade II AVN who underwent varus derotation femoral osteotomy had a lower limb length discrepancy ranging from 1 cm to 2 cm; the discrepancy measured 2.5 cm in the patient with Grade III AVN. In patients with shortening of 2 to 2.5 cm, the limb length discrepancy was well compensated with an insole. No patient reported pain. All patients were fully satisfied with the surgical scar resulting from the medial approach, which in many cases was barely visible. At clinical evaluation [9], 44 hips (76%) had an excellent result, 24 (17%) had a good result, and three (7%) had a fair result (Table 4). There was a statistically significant difference between age group and clinical results (p = ). At radiographic evaluation, the Sharp angle was normal in all the hips, with a mean measure of 40 (range, ); 39 hips (63%) were ranked as Severin Class I and 64% of them were in patients in age Group 1 including the youngest patient at surgery; 27 hips (30%)
5 2662 Farsetti et al. Clinical Orthopaedics and Related Research 1 Fig. 2A E (A) An AP view radiograph shows bilateral high developmental dislocation of the hip in a 13-month-old girl. (B) After 4 weeks in traction, both hips were pulled to a low position. (C) Both hips were well developed, and the acetabular index and Wiberg angle were normal when the patient was 9 years old. (D) At age 15 years, 6 months after menarche, both hips became painful and the Wiberg angle was abnormal bilaterally. A Tönnis triple pelvic osteotomy was performed with normalization of the Wiberg angle. (E) At the last followup, the patient was 28 years old and both of her hips had an excellent clinical result, with Severin Class I on the right and Class II on the left.
6 Volume 473, Number 8, August 2015 DDH Treated by Medial Open Reduction 2663 Fig. 3A C (A) An AP view radiograph shows high developmental dislocation of the left hip and subluxation of the right hip in a 32- month-old girl. (B) At age 5 years, 3 years after she underwent medial open reduction of the left hip, Grade III avascular necrosis was evident. (C) At the last followup, the patient was 17 years old. The avascular necrosis was classified as Grade V but the hip had a good clinical result and was scored Severin Class II. were ranked as Severin Class II whereas five (7%) were Class III. Three of the six patients who missed the scheduled radiographic followup had their hips ranked as Severin Class III at the last followup (Table 4). There was a statistically significant difference between age group and radiographic results (p = ). At the last followup, 20 of 34 hips reduced in patients after 16 months of age (88.2%) showed minor radiographic abnormalities of the femoral head consisting of asymmetry and size and shape alteration. In the same cases, moderate deformity of the ossific nucleus of the femoral head was present before open reduction. Fig. 4A D (A) An AP view radiograph shows bilateral developmental dislocation of the hip, which was high on the right and intermediate on the left, in a 36-month-old girl with bilateral DDH. (B) When the patient was 5 years old, 2 years after bilateral medial open reduction, her right hip showed Grade IV avascular necrosis and the acetabular index was abnormal bilaterally, although both hips were clinically and radiographically stable. (C) At age 11 years, the patient s acetabular index had become normal bilaterally. (D) At the last followup, the patient was 32 years old and both of her hips had an excellent clinical result, with Severin Class I on the left and Class II on the right.
7 2664 Farsetti et al. Clinical Orthopaedics and Related Research 1 Table 2. Additional surgeries Case Age of patient at surgery (years) Diagnosis Clinical aspects before surgery Type of surgery 1 9 Grade II avascular necrosis Asymptomatic Varus derotation femoral osteotomy 2 9 Grade II avascular necrosis Asymptomatic Varus derotation femoral osteotomy 3 9 Coxa valga antetorta Asymptomatic Varus derotation femoral osteotomy 4 10 Grade II avascular necrosis Asymptomatic Varus derotation femoral osteotomy, Tönnis osteotomy 5 11 Grade II avascular necrosis Asymptomatic Tönnis osteotomy 6 13 Grade III avascular necrosis Limp Distal transfer of the greater trochanter 7 14 Acetabular insufficiency (Wiberg angle \ 20 ) Asymptomatic Tönnis osteotomy 8 14 Acetabular insufficiency (Wiberg angle \ 20 ) coxa valga antetorta 9 15 Acetabular insufficiency (Wiberg angle \ 20 ) 10 15* Acetabular insufficiency (Wiberg angle \ 20 ) 11 15* Acetabular insufficiency (Wiberg angle \ 20 ) Pain Pain Pain Pain Varus derotation femoral osteotomy, Tönnis osteotomy Tönnis osteotomy Tönnis osteotomy Tönnis osteotomy No significant difference between age groups and additional surgery (p = 0.229); 13 procedures in 11 hips (10 patients). In Cases 4 and 8, varus derotation femoral osteotomy and Tönnis periacetabular osteotomy were performed during the same operative session; *same patient had bilateral procedures. Table 3. Avascular necrosis Age of patient (years) at radiographic diagnosis Grade* Age of patient at surgery (months) Height of dislocation 9 II 10 High 9 II 18 Intermediate 10 II 19 High 11 II 28 Intermediate 3 III 29 High 2.5 IV 22 High 3 IV 24 High 3.5 IV 27 High 3.5 IV 27 High 4 IV 32 High 4 IV 32 High 4 IV 36 High 4.5 V 34 Intermediate * Statistically significant difference with patient age at surgery (p = 0.002) and height of dislocation (p = 0.001); Bucholz and Ogden [13] grade modified by Morcuende et al. [50], observed in 13 of 71 hips; six hips with Grade I avascular necrosis not included because avascular necrosis resolved without any long-term sequelae; same patient with bilateral developmental dislocation of the hip. Of the 23 patients included in the followup but excluded from the statistics of the study, 18 patients who had a telephone interview affirmed they were doing well without pain or restrictions of physical activity. Ten also mailed recent radiographs of their hips: six hips were ranked Severin Class I, seven were Class II, and one was Class III. The five patients (eight hips) who came to the hospital whose initial radiographs were missing from their records also were asymptomatic and at clinical evaluation, three hips had an excellent result; three had a good result, and two had a fair result. Three hips were ranked Severin Class I, three were Class II, and two were Class III. Discussion This retrospective study shows our 20-year-experience with open medial reduction of complete DDH in patients ranging from 3 to 36 months old. Although medial versus anterior open reduction is debated with complete dislocations [11, 16, 21, 40, 46, 49, 50, 52, 53, 64, 77, 84, 85, 88], open medial reduction after preliminary traction gave us good results. All hips in our patients remained stable after completion of treatment and the acetabular index normalized in all of them. The prevalence of AVN and additional surgery was reasonably low, and the majority of the hips had a high radiographic Severin class at the end of growth. Our study has several limitations. First, as in all retrospective studies, there is partial patient selection bias. We have statistically evaluated only 61% of the original cohort
8 Volume 473, Number 8, August 2015 DDH Treated by Medial Open Reduction 2665 Table 4. Clinical and radiographic results at the last followup Group months old 22 patient/26 hips Group months old 19 patients /27 hips Group months old 11 patients/18 hips Clinical* and radiographic results Clinical results 26 hips 13 hips 5 hips Excellent (76%) 0 13 hips 11 hips Good (17%) 0 1 hip 2 hips Fair (7%) Radiographic results 25 hips 10 hips 4 hips Class I (63%) 1 hip 15 hips 11 hips Class II (30%) 0 2 hips 3 hips Class III (7%) Clinical results, p = ; radiographic, p = ; *evaluated using McKay scale modified by Barrett et al. [9], and Severin radiographic class [66]. of patients. However, the overall number of patients who had followups with satisfactory long-term results is 87% of the original cohort if we include patients who had either telephone interview or partial clinical and radiographic evaluations, although not fulfilling all the criteria to be included in the statistics of the study. The second limitation is an assessment bias because only the senior author (EI) made the radiographic measurements. However, his intraobserver j score was which makes his assessment error acceptable. The third limitation is the lack of a control series. However, none of the previously reported long-term followup series after medial open reduction has a control series [33, 39, 50, 78]. The fourth limitation is the lack of homogeneity between the three age groups, with the third group including almost 30% less cases than the other two. However, a similar discrepancy was present in other series of patients with DDH treated by medial open reduction in which the number of children older than 24 months was relatively low [33, 39, 50, 78]. All the hips with DDH in our series were not reducible in flexion and abduction at the time of diagnosis, even in children 3 to 10 months old. For this reason, a more conservative treatment, such as the Pavlik harness or other braces, was not used [15, 29]. In our institution, traction has been part of DDH treatment since the early 1960s. Since then, we have continued to use preliminary traction to decrease the risk of complications in case of closed reduction, as reported by others [24, 51, 57]. The effect of preoperative traction has been questioned for surgical treatment of DDH since all the anatomic obstacles to hip reduction are surgically eliminated [35, 59, 64, 82]. Although the percentage of our excellent and good long-term radiographic results, according to the Severin classification, is higher than in other series in which traction was not used [18, 30, 33, 39, 50, 71, 78 80], it is difficult to determine whether preoperative traction served to decrease the complication rate. Inpatient traction is costly [35, 59, 82]; however, more than 1/2 of our patients successfully completed home traction before surgery. The hip spica cast was firmly anchored to the bed ensuring the child s compliance with the traction. The patient s compliance and the amount of traction were supervised twice a week at home by one of our residents. Early hip subluxation after open reduction and/or redislocation while wearing the plaster cast has been reported in a range of 0% to 11% with a mean of 2.4% for anterior and medial open reductions [7, 10, 11, 16, 18, 20, 21, 23, 31, 37, 40, 46, 50, 52, 69, 70, 77 79, 88]. Our patients had a redislocation rate of 2.8%. Since then, hips that were not fully stable at surgery at 100 flexion, 60 abduction, and neutral rotation had K-wire fixation [3] to prevent redislocation. Additional surgery after open reduction is important, and it is related to hip development after open reduction [2]. Its prevalence in patients with DDH who had open reduction by either the anterior or medial approach ranges from 0% to 100% [1, 4, 6, 7, 10, 11, 16, 18, 20, 21, 23, 25, 30, 31, 33, 36, 37, 39, 46 50, 52 54, 58, 60, 69, 71, 73, 77 80, 88], and its prevalence in our series was 15%. We believe that a high acetabular index during the years after open reduction is not an indication for a mandatory acetabular procedure like a Pemberton acetabuloplasty or Salter osteotomy if the hip is stable. All our patients hips showed stable concentric reduction clinically and radiographically, according to the lateral instability index of Smith et al. [68]. Cartilaginous and labral coverage, as evaluated by MRI, may be normal even in cases with delayed acetabular cartilage ossification [34]. The acetabular index improved slowly, especially in our older patients, and took several years to become normal in many children
9 2666 Farsetti et al. Clinical Orthopaedics and Related Research 1 who underwent surgery after 14 months old, as reported by others [1, 32, 38, 43]. Moreover, acetabular procedures performed early do not fully guarantee the persistence of normal acetabular coverage to the end of growth, as shown in a long-term followup study by Thomas et al. [74], in which 15% of the hips were scored Severin Class III and 2% were Class IV despite the Salter procedure being performed after open reduction. We performed the Tönnis osteotomy on patients ranging from 10 to 15 years old whose hips had an abnormal Wiberg angle. In some of the cases, acetabular coverage was normal before puberty, and we might speculate that acetabular depth failed to increase in proportion to femoral head enlargement owing to the lack of development of the secondary centers of ossification of the acetabulum at puberty [56, 81]. We believe patients with dislocated hips should be followed up radiographically after open reduction until puberty to avoid missing late acetabular insufficiency. In our series, the incidence of AVN was 18%. Numerous authors have reported an incidence of AVN in patients who had open reduction either by the medial or anterior approach [10, 21, 31, 37, 60, 77, 88] that was lower than the incidence in our series. However, the followups were too short in those series to include all possible cases of AVN since many, especially type 2, may show up when the patient is 9 to 10 years or older [13, 39, 50, 69, 81]. In some studies, the AVN rate was high when the ossific nucleus of the femoral head was absent [17, 65]. In our study and others [44, 62], an opposite correlation was found (p = 0.002). The proper approach (anterior versus medial) for open reduction of complete DDH continues to be debated. Many authors recommend the medial approach as a procedure that can be performed safely in children younger than 18 to 24 months [24, 27, 28, 30, 32, 34, 35, 37, 41, 43, 44, 84]. We agree with those authors because in patients younger than 24 months, AVN and additional surgery have been reported in patients treated by anterior open reduction at a similar or higher rate than patients treated by medial open reduction [12]. In a recent prospective study of two cohorts of patients with an upper age limit of 24 months [72], one cohort had the medial approach and the other had the anterior approach, and the AVN rate was significantly lower in the medial approach cohort at an average followup of 7 years (12% versus 18%). In our series, the prevalence of AVN in patients younger than 24 months was 9.4%, although in a recent meta-analysis of open reduction by the medial approach, the average prevalence of AVN was 20% [26]. Anterior open reduction has been recommended in children with complete hip dislocation who are older than 24 months [84]. This same recommendation was made by many authors who advocated medial open reduction in children younger than 24 months [11, 16, 21, 40, 46, 49, 50, 52, 53, 77, 85, 88]. Although we were aware of this general trend in favor of anterior open reduction that provides capsulorrhaphy and avoids medial circumflex vessels, the good preliminary results we obtained in children older than 24 months encouraged us to increase the upper age limit for medial open reduction to 36 months. Moreover, according to the literature, even open reduction by the anterior approach may provide unsatisfactory results in children older than 24 months [17, 18, 25, 30, 33, 47, 58, 73, 79, 80]. Schoenecker and Strecker [64] reported two series of patients older than 24 months who had open reduction by the anterior approach. One series of patients had preliminary traction while the others underwent femoral shortening osteotomy. In the first series, AVN developed in 53.8% of the patients, whereas it was absent in the second series, although in the latter, three of four hips in patients 38 to 40 months old ultimately were ranked as Severin Class III or IV. Galpin et al. [25] reported 14 hips in patients with similar ages who had open reduction by the anterior approach with femoral shortening osteotomy. The AVN rate was only 10%, but 42.8% of the hips were ranked as Severin Class III. The conclusions that may be drawn from the studies by Schoenecker and Strecker [64] and Galpin et al. [25] are that (1) in children older than 24 months, the anterior approach reduces the AVN rate only if it is associated with femoral shortening osteotomy; and (2) in children older than 24 months, the anterior approach does not prevent unsatisfactory final results according to the Severin classification. We observed a 40% rate of AVN in children 25 to 36 months old but the final radiographic results, according to the Severin classification, were good in 80% of cases. However, patients with sequelae of AVN do not show early significant physical disability, although their good function tends to decline with age [61, 81]. According to Schoenecker and Strecker [64] and Galpin et al. [25], we might perform an associated femoral shortening osteotomy with medial open reduction to further reduce the rate of AVN in patients 25 to 36 months old. Long-term followup studies at skeletal maturity are rare in DDH series where patients underwent open reduction either by the anterior [5, 18, 30, 33, 39, 50, 71] or medial approach [78 80]. The Severin classification has been used to evaluate final radiographic results owing to its reliability [14]. In anterior approach series, the average prevalence of AVN is 24% (range, 7.6% 47%); the average prevalence of additional surgery is 68.9% (range, 22.4% 100%), while the average prevalence of excellent and good radiographic results according to the Severin classification is 73.8% (range, 33% 96%). In medial approach series, the average prevalence of AVN is 28.7% (range, 9% 43%); the average prevalence of additional surgery is 35.5% (range, 17.2% 50%), while the average prevalence of excellent
10 Volume 473, Number 8, August 2015 DDH Treated by Medial Open Reduction 2667 and good radiographic results according to the Severin classification is 62.9% (range, 45.7% 79%). In our series, the AVN rate was 8%, additional surgery was 15%, and excellent and good results were 93% according to the Severin classification. We believe the anterior and medial approaches are comparable; in long-term followups, the rate of AVN is lower in patients who had the anterior approach, mainly with femoral shortening osteotomy, whereas the number of additional surgeries is much lower in patients who had the medial approach. At the last radiographic followup, minor deformities of the femoral head were observed in 88.2% of the hips in patients who had open reduction after 16 months of age [53]. We might speculate that mild deformity of the femoral head may be caused by minor degrees of AVN not described in any of the current AVN classifications [50, 63]. We also might speculate that overpressure to the epiphyseal cartilage, exerted by the acetabulum or pelvis owing to the position of the dislocated hip, may cause damage to the femoral epiphysis mainly in older dislocations before any treatment is provided [83]. We report satisfactory long-term results at an average followup of 22 years in a cohort of patients ranging from 3 to 36 months old who had complete DDH reduced by a medial approach. On the basis of the results obtained in our fully grown patients, we believe that open reduction of DDH through a medial approach after preliminary traction can be considered a safe surgical procedure in patients up to the age of 36 months. References 1. Akagi S, Tanabe T, Ogawa R. Acetabular development after open reduction for developmental dislocation of the hip: 15-year follow-up of 22 hips without additional surgery. Acta Orthop Scand. 1998;69: Albinana J, Dolan LA, Spratt KF, Morcuende J, Meyer MD, Weinstein SL. Acetabular dysplasia after treatment of developmental dysplasia of the hip: implications for secondary procedures. J Bone Joint Surg Br. 2004;86: Alsiddiky AM, Bakarman KA, Alzain KO, Aljassir FF, Al- Ahaideb AS, Kremli MK, Zanzam MM, Letts RM. The early detection and management of unstable concentric closed reduction of DDH with percutaneous K-wire fixation in infants 6 to 12 months of age. J Pediatr Orthop. 2012;32: Altay M, Demirkale I, Senturk F, Firat A, Kapicioglu S. Results of medial open reduction of developmental dysplasia of the hip, with regard to walking age. J Pediatr Orthop B. 2013;22: Angliss R, Fuji G, Pickvance E, Wainwright AM, Benson MK. Surgical treatment of late developmental displacement of the hip: results after 33 years. J.Bone Joint Surg Br. 2005;87: Bache CE, Graham HK, Dickens RV, Donnan L, Johnson MB, Natrass G, O Sullivan M, Torode IP. Ligamentum teres tenodesis in medial approach open reduction for developmental dislocation of the hip. J Pediatr Orthop. 2008;28: Baki C, Sener M, Aydin H, Yildiz M, Sahuran S. Single-stage open reduction through a medial approach and innominate osteotomy in developmental dysplasia of the hip. J Bone Joint Surg Br. 2005;87: Barlow TG. Early diagnosis and treatment of congenital dislocation of the hip. J Bone Joint Surg Br. 1962;44: Barrett WP, Staheli LT, Chew DE. The effectiveness of the Salter innominate osteotomy in the treatment of congenital dislocation of the hip. J Bone Joint Surg Am. 1986;68: Berkeley ME, Dickinson JH, Cain TE, Donovar MM. Surgical therapy for congenital dislocation of the hip in patients who are twelve to thirty-six months old. J Bone Joint Surg Am. 1984;66: Bicimoglu A, Agus H, Omeroglu H, Tumer Y. Posteromedial limited surgery in developmental dysplasia of the hip. Clin Orthop Relat Res. 2008;466: Broughton NS, Graham HK, Nattrass GR, Torode IP, Marshall PD, O Sullivan M. Comment on: Ludloff s medial approach for open reduction of congenital dislocation of the hip. J Bone Joint Surg Br. 1997;79: Bucholz RW, Ogden JA. Patterns of ischemic necrosis of the proximal femur in nonoperatively treated congenital hip disease. The Hip: Proceedings of the Sixth Open Scientific Meeting of the Hip Society. St Louis, MO: CV Mosby; 1978: Carroll KL, Murray KA, MacLeod LM, Hennessey TA, Woiczik MR, Roach JW. Measurement of the center edge angle and determination of the Severin classification using digital radiography, computer-assisted measurement tools, and a Severin algorithm: Intraobserver reliability revisited. J Pediatr Orthop. 2011;31:e Cashman JP, Round J, Taylor G, Clarke NM. The natural history of developmental dysplasia of the hip after early supervised treatment in the Pavlik harness: a prospective, longitudinal follow-up. J Bone Joint Surg Br. 2002;84: Castillo R, Sherman FC. Medial adductor open reduction for congenital dislocation of the hip. J Pediatr Orthop. 1990;10: Clarke NM, Jowett AJ, Parker L. The surgical treatment of established congenital dislocation of the hip: results of surgery after planned delayed intervention following the appearance of the capital femoral ossific nucleus. J Pediatr Orthop. 2005; 25: Cordier W, Tönnis D, Kalchschmidt K, Storch KJ, Katthagen BD. Long-term results after reduction of developmental hip dislocation by an anterior approach lateral and medial of the iliopsoas muscle. J Pediatr Orthop Br. 2005;14: Dezateux C, Godward S. A national survey of screening for congenital dislocation of the hip. Arch Dis Child. 1996;74: Dhar S, Taylor JF, Jones WA, Owen R. Early open reduction for congenital dislocation of the hip. J Bone Joint Surg Br. 1990;72: Di Mascio L, Carey-Smith R, Tucker K. Open reduction of developmental hip dysplasia using a medial approach: a review of 24 hips. Acta Orthop Belg. 2008;74: Diepstraten AF. Open reduction of congenital hip dislocation: advantages of the Ferguson medial approach. Acta Orthop Scand. 1985;56: Doudoulakis JK, Cavadias A. Open reduction of CDH before one year of age: 69 hips followed for 13 (10 19) years. Acta Orthop Scand. 1993:64: Gage JR, Winter RB. Avascular necrosis of the capital femoral epiphysis as a complication of closed reduction of congenital dislocation of the hip: a critical review of twenty years experience at Gillette Children s Hospital. J Bone Joint Surg Am. 1972;54: Galpin RD, Roach JW, Wenger DR, Herring JA, Birch JG. Onestage treatment of congenital dislocation of the hip in older
11 2668 Farsetti et al. Clinical Orthopaedics and Related Research 1 children, including femoral shortening. J Bone Joint Surg Am. 1989;71: Gardner RO, Bradley CS, Howard A, Narayanan UG, Wedge JH, Kelley SP. The incidence of avascular necrosis and the radiographic outcome following medial open reduction in children with developmental dislocation of the hip: a systematic review. Bone Joint J. 2014;96: Gibson PH, Benson MK. Congenital dislocation of the hip: review at maturity of 147 hips treated by excision of the limbus and derotation osteotomy. J Bone Joint Surg Br. 1982;64: Graf R, Tschauner C, Klapsch W. Progress in prevention of late developmental dislocation of the hip by sonographic newborn hip screening : results of a comparative follow-up study. J Pediatr Orthop. 1993;2: Grill F, Bensahel H, Canadell J, Dungl P, Matasovic T, Vizkelety T. The Pavlik harness in the treatment of congenital dislocating hip: report on a multicenter study of the European Pediatric Orthopaedic Society. J Pediatr Orthop. 1988;8: Gulman B, Tunkay IC, Dobak N, Karaismailoglu N. Salter s innominate osteotomy in the treatment of congenital hip dislocation: a long-term study. J Pediatr Orthop. 1994;14: Haidar RK, Jones RS, Vergroesen DA, Evans GA. Simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip. J Bone Joint Surg Br. 1996;78: Harris NH. Acetabular growth potential in congenital dislocation of the hip and some factors upon which it may depend. Clin Orthop Relat Res. 1976;119: Holman J, Carroll KL, Murray KA, Macleod LM, Roach JW. Long-term follow-up of open reduction surgery for developmental dislocation of the hip. JPediatrOrthop. 2012;32: Huber H, Mainard-Simard L, Lascombes P, Renaud F, Jean- Baptiste M, Journeau P. Normal values of bony, cartilaginous, and labral coverage of the infant hip in MR imaging. J Pediatr Orthop. 2014;34: Kahle WK, Anderson MB, Alpert J, Stevens P, Coleman SS. The value of preliminary traction in the treatment of congenital dislocation of the hip. J Bone Joint Surg Am. 1990;72: Kalamchi A, Schmidt TL, MacEwen GD. Congenital dislocation of the hip: open reduction by the medial approach. Clin Orthop Relat Res. 1982;169: Kiely N, Younis U, Day JB, Meadows TM. The Ferguson medial approach for open reduction of developmental dysplasia of the hip: a clinical and radiological review of 49 hips. J Bone Joint Surg Br. 2004;86: Kim HW, Morcuende JA, Dolan LA, Weinstein SL. Acetabular development in developmental dysplasia of the hip complicated by lateral growth disturbance of the capital femoral epiphysis. J Bone Joint Surg Am. 2000;82: Koizumi W, Moriya H, Tsuchiya K, Takeuchi T, Kamegaya M, Akita T. Ludloff s medial approach for open reduction of congenital dislocation of the hip: a 20-year follow-up. J Bone Joint Surg Br. 1996;78: Konigsberg DE, Karol LA, Colby S, O Brian S. Results of medial open reduction of the hip in infants with developmental dislocation of the hip. J Pediatr Orthop. 2003;23: Lehman WB, Grant AD, Nelson J, Robbins H, Milgram J. Hospital for Joint Diseases traction system for preliminary treatment of congenital dislocation of the hip. J Pediatr Orthop. 1983;3: Lequesne M, de Sèze S. [False profile of the pelvis: a new radiographic incidence for the study of the hip. Its use in dysplasias and different coxopathies][in French]. Rev Rhum Mal Osteoartic. 1961;28: Lindstrom JR, Ponseti IV, Wenger DR. Acetabular development after reduction in congenital dislocation of the hip. J Bone Joint Surg Am. 1979;61: Luhmann SJ, Schoenecker PL, Anderson AM, Bassett GS. The prognostic importance of the ossific nucleus in the treatment of congenital dysplasia of the hip. J Bone Joint Surg Am. 1998; 80: Madhu TS, Akula M, Scott BW, Templeton PA. Treatment of developmental dislocation of hip: does changing the hip abduction angle in the hip spica affect the rate of avascular necrosis of the femoral head? J Pediatr Orthop Br. 2013;22: Mankey MG, Arntz GT, Staheli LT. Open reduction through a medial approach for congenital dislocation of the hip: a critical review of the Ludloff approach in sixty-six hips. J Bone Joint Surg Am. 1993;75: Mardam-Bey TH, MacEwen GD. Congenital hip dislocation after walking age. J Pediatr Orthop. 1982;2: Matsushita T, Miyake Y, Akazawa H, Eguchi S, Takahashi Y. Open reduction for congenital dislocation of the hip: comparison of the long-term results of the wide exposure method and Ludloff s method. J Orthop Sci. 1999;4: Mergen E, Adyaman S, Omeroglu H, Erdemli B, Isiklar U. Medial approach open reduction for congenital dislocation of the hip using the Ferguson procedure: a review of 31 hips. Arch Orthop Trauma Surg. 1991;110: Morcuende JA, Meyer MD, Dolan LA, Weinstein SL. Long-term outcome after open reduction through an anteromedial approach for congenital dislocation of the hip. J Bone Joint Surg Am. 1997;79: Morin C, Bisogno J, Kulkarni S, Morel G. Treatment of latepresenting developmental dislocation of the hip by progressive orthopaedic reduction and innominate osteotomy: our results with more than 30 years of follow up. JChildOrthop. 2011;5: O Hara JN, Bernard AA, Dwyer NS. Early results of medial approach open reduction in congenital dislocation of the hip: use before walking age. J Pediatr Orthop. 1988;8: Okano K, Enomoto H, Osaki M, Takahashi K, Shindo H. Femoral head deformity after open reduction by Ludloff s medial approach. Clin Orthop Relat Res. 2008;466: Okano K, Yamada K, Takahashi K, Enomoto H, Osaki M, Shindo H. Long-term outcome of Ludloff s medial approach for open reduction of developmental dislocation of the hip in relation to the age at operation. Int Orthop. 2009;33: Ortolani M. Un segno poco noto e sua importanza per la diagnosi precoce di prelussazione congenita dell anca. Pediatria. 1937;45: Ponseti IV. Morphology of the acetabulum in congenital dislocation of the hip: gross, histological and roentgenographic studies. J Bone Joint Surg Am. 1978;60: Pospischill R, Weninger J, Ganger R, Altenhuber J, Grill F. Does open reduction of the developmental dislocated hip increase the risk of osteonecrosis? Clin Orthop Relat Res. 2012;470: Powell EN, Gerratana FJ, Gage JR. Open reduction for congenital hip dislocation: the risk of avascular necrosis with three different approaches. J Pediatr Orthop. 1986;6: Quinn RH, Renshaw TS, DeLuca P. Preliminary traction in the treatment of developmental dislocation of the hip. J Pediatr Orthop. 1994;14: Roose PE, Chingren GL, Klaaren HE, Broock G. Open reduction for congenital dislocation of the hip using the Ferguson procedure: a review of twenty-six cases. J Bone Joint Surg Am. 1979;61: Roposch A, Liu LQ, Offiah AC, Wedge JH. Functional outcomes in children with osteonecrosis secondary to treatment of developmental dysplasia of the hip. J Bone Joint Surg Am. 2011; 93:e Roposch A, Stöhr KK, Dobson M. The effect of the femoral head ossific nucleus in the treatment of developmental dysplasia of the hip: a meta-analysis. J Bone Joint Surg Am. 2009;91:
12 Volume 473, Number 8, August 2015 DDH Treated by Medial Open Reduction Roposch A, Wedge JH, Riedl G. Reliability of Bucholz and Hodgen classification for osteonecrosis secondary to developmental dysplasia of the hip. Clin Orthop Relat Res. 2012;470: Schoenecker PL, Strecker WB. Congenital dislocation of the hip in children: comparison of the effects of femoral shortening and of skeletal traction in treatment. J Bone Joint Surg Am. 1984;66: Segal LS, Boal AK, Borthwick L, Clark MW, Localio AR, Schwentker EP. Avascular necrosis after treatment of DDH: the prospective influence of the ossific nucleus. J Pediatr Orthop. 1999;19: Severin E. Contribution to the knowledge of congenital dislocation of the hip joint: late results of closed reduction and arthrographic studies of recent cases. Acta Chir Scand. 1941;84(suppl 63): Sharp IK. Acetabular dysplasia: the acetabular angle. J Bone Joint Surg Br. 1961;43: Smith WS, Badgley CE, Orwing JB, Harper JM. Correlation of post-reduction roentgenograms and thirty-one-year follow-up in congenital dislocation of the hip. J Bone Joint Surg Am. 1968;50: Sosna A, Rejholec M. Ludloff s open reduction of the hip: longterm results. J Pediatr Orthop. 1992;12: Szepesi K, Biro B, Fazekas K, Szucs G. Preliminary results of early open reduction by an anterior approach for congenital dislocation of the hip. J Pediatr Orthop B. 1995;4: Szepesi K, Szucs G, Szeverenyi C, Csernatony Z. Long-term followup of DDH patients who underwent open reduction without a postoperative cast. J Pediatr Orthop B. 2013;22: Tarassoli P, Gargan MF, Atherton WG, Thomas SR. The medial approach for the treatment of children with developmental dysplasia of the hip. Bone Joint J. 2014;96: Thomas IH, Dunin AJ, Cole WG, Menelaus MB. Avascular necrosis after open reduction for congenital dislocation of the hip: analysis of causative factors and natural history. J Pediatr Orthop. 1989;9: Thomas SR, Wedge JH, Salter RB. Outcome at forty-five years after open reduction and innominate osteotomy for late-presenting developmental dislocation of the hip. J Bone Joint Surg Am. 2007;89: Tönnis D. Congenital Dysplasia and Dislocation of the Hip in Children and Adults. Legal H, Graf R, collaborators; Telger TC, translator. Berlin, Germany: Springer-Verlag; Tönnis D, Behrens K, Tscharani F. A modified technique of the triple pelvic osteotomy: early results. J Pediatr Orthop. 1981; 1: Tumer Y, Ward T, Grudziak J. Medial open reduction in the treatment of developmental dislocation of the hip. J Pediatr Orthop. 1997;17: Ucar DH, Isiklar ZU, Stanitski CL, Kandemir U, Tumer Y. Open reduction through a medial approach in developmental dislocation of the hip: a follow-up study to skeletal maturity. J Pediatr Orthop. 2004;24: Varner KE, Incavo SJ, Haynes RJ Dickson JH. Surgical treatment of developmental hip dislocation in children aged 1 to 3 years: a mean 18-years, 9-month follow-up study. Orthopedics. 2010;10: Wang TM, Wu KW, Shih SF, Huang SC, Kuo KN. Outcomes of open reduction for developmental dysplasia of the hip: does bilateral dysplasia have a poorer outcome? J Bone Joint Surg Am. 2013;95: Weinstein SL. Congenital hip dislocation: long-range problems, residual signs, and symptoms after successful treatment. Clin Orthop Relat Res. 1992;281: Weinstein SL. Traction in developmental dislocation of the hip: is its use justified? Clin Orthop Relat Res. 1997;338: Weinstein SL. CORR insights: Reliability of Bucholz and Ogden classification for osteonecrosis secondary to developmental dysplasia of the hip. Clin Orthop Relat Res. 2012;470; Weinstein SL. Developmental hip dysplasia and dislocation. In: Weinstein SL, Flynn JM, eds. Lovell and Winter s Pediatric Orthopaedics. 7th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2014: Weinstein SL, Ponseti IV. Congenital dislocation of the hip. J Bone Joint Surg Am. 1979;61: Wiberg G. Studies on dysplastic acetabula and congenital subluxation of the hip joint with special reference to the complication of osteoarthritis. Acta Chir Scand. 1939;83(suppl 58): Wirth T, Stratmann L, Hinrichs F. Evolution of late presenting developmental dysplasia of the hip and associated surgical procedures after 14 years of neonatal ultrasound screening. J Bone Joint Surg Br. 2004;86: Zamzam MM, Khoshhal KI, Abak AA, Bakarman KA, Alsiddiky AM, AlZain KO, Kremli MK. One-stage bilateral open reduction through a medial approach in developmental dysplasia of the hip. J Bone Joint Surg Br. 2009;91:
Long-term outcome following medial open reduction in developmental dysplasia of the hip: a retrospective cohort study
 J Child Orthop (2016) 10:179 184 DOI 10.1007/s11832-016-0729-5 ORIGINAL CLINICAL ARTICLE Long-term outcome following medial open reduction in developmental dysplasia of the hip: a retrospective cohort
J Child Orthop (2016) 10:179 184 DOI 10.1007/s11832-016-0729-5 ORIGINAL CLINICAL ARTICLE Long-term outcome following medial open reduction in developmental dysplasia of the hip: a retrospective cohort
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH)
 The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future surgery
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2-1-2003 Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2-1-2003 Reduction of a dislocation of the hip due to developmental dysplasia: Implications for the need for future
Does Open Reduction of the Developmental Dislocated Hip Increase the Risk of Osteonecrosis?
 Clin Orthop Relat Res (2012) 470:250 260 DOI 10.1007/s11999-011-1929-4 CLINICAL RESEARCH Does Open Reduction of the Developmental Dislocated Hip Increase the Risk of Osteonecrosis? Renata Pospischill MD,
Clin Orthop Relat Res (2012) 470:250 260 DOI 10.1007/s11999-011-1929-4 CLINICAL RESEARCH Does Open Reduction of the Developmental Dislocated Hip Increase the Risk of Osteonecrosis? Renata Pospischill MD,
EVALUATION OF MEDIAL APPROACH (LUDLLOF) FOR OPEN REDUCTION OF DEVELOPMENTAL DYSPLASIA OF THE HIP IN CHILDREN
 Basrah Journal Original Article Of Surgery EVALUATION OF MEDIAL APPROACH (LUDLLOF) FOR OPEN REDUCTION OF DEVELOPMENTAL DYSPLASIA OF THE HIP IN CHILDREN Haider R Majeed *, Ali A Ahmed Al-Iedan @ & Haider
Basrah Journal Original Article Of Surgery EVALUATION OF MEDIAL APPROACH (LUDLLOF) FOR OPEN REDUCTION OF DEVELOPMENTAL DYSPLASIA OF THE HIP IN CHILDREN Haider R Majeed *, Ali A Ahmed Al-Iedan @ & Haider
Subluxation of the hip presenting for the first time
 The treatment of subluxation of the hip in children over the age of four years John A. Fixsen, Patrick L. S. Li From the Hospitals for Sick Children, Great Ormond Street, London, England Subluxation of
The treatment of subluxation of the hip in children over the age of four years John A. Fixsen, Patrick L. S. Li From the Hospitals for Sick Children, Great Ormond Street, London, England Subluxation of
Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip
 Med. J. Cairo Univ., Vol. 84, No. 2, March: 287-291, 2016 www.medicaljournalofcairouniversity.net Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip MOHAMED M. HEGAZY, M.D.; MOHAMED
Med. J. Cairo Univ., Vol. 84, No. 2, March: 287-291, 2016 www.medicaljournalofcairouniversity.net Subsartorial Approach in Open Reduction of Developmental Dysplasia of Hip MOHAMED M. HEGAZY, M.D.; MOHAMED
Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip
 Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 6-10 Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip Banskota
Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 6-10 Original Article Results of simultaneous open reduction and Salter innominate osteotomy for developmental dysplasia of the hip Banskota
ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING
 Basrah Journal Original Article Of Surgery Bas J Surg, March, 17, 2011 ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING MBChB,
Basrah Journal Original Article Of Surgery Bas J Surg, March, 17, 2011 ONE STAGE COMBINED SURGICAL TREATMENT FOR DEVELOPMENTAL DISLOCATION OF THE HIP IN OLDER CHILDREN INCLUDING FEMORAL SHORTENING MBChB,
The surgical treatment of developmental dislocation of the hip in older children : A comparative study
 Acta Orthop. Belg., 2005, 71, 678-685 ORIGINAL STUDY The surgical treatment of developmental dislocation of the hip in older children : A comparative study Gunduz TEZEREN, Mehmet TUKENMEZ, Okay BULUT,
Acta Orthop. Belg., 2005, 71, 678-685 ORIGINAL STUDY The surgical treatment of developmental dislocation of the hip in older children : A comparative study Gunduz TEZEREN, Mehmet TUKENMEZ, Okay BULUT,
Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study
 Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP
 EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP SUNIL DHAR, J. F. TAYLOR, W. A. JONES, R. OWEN From Alder Hey Children s Hospital, Liverpool We have reviewed 82 children with congenital dislocation
EARLY OPEN REDUCFION FOR CONGENITAL DISLOCATION OF THE HIP SUNIL DHAR, J. F. TAYLOR, W. A. JONES, R. OWEN From Alder Hey Children s Hospital, Liverpool We have reviewed 82 children with congenital dislocation
Abstract. Introduction
 Outcome of Triple Procedure in Older Children with Developmental Dysplasia of Hip (DDH) Masood Umer, Haq Nawaz 2, Pashtoon Murtaza Kasi 2, Mahmood Ahmed 3, Syed Sohail Ali 2 Department of Surgery, Medical
Outcome of Triple Procedure in Older Children with Developmental Dysplasia of Hip (DDH) Masood Umer, Haq Nawaz 2, Pashtoon Murtaza Kasi 2, Mahmood Ahmed 3, Syed Sohail Ali 2 Department of Surgery, Medical
After open reduction for developmental dysplasia of
 Test of stability as an aid to decide the need for osteotomy in association with open reduction in developmental dysplasia of the hip A LONG-TERM REVIEW H. G. Zadeh, A. Catterall, A. Hashemi-Nejad, R.
Test of stability as an aid to decide the need for osteotomy in association with open reduction in developmental dysplasia of the hip A LONG-TERM REVIEW H. G. Zadeh, A. Catterall, A. Hashemi-Nejad, R.
Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies
 Original Research Article DOI: 10.18231/2395-1362.2018.0012 Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies G. Jagadesh 1, Venugopal
Original Research Article DOI: 10.18231/2395-1362.2018.0012 Outcome of surgical management of late presenting developmental dysplasia of hip with pelvic and femoral osteotomies G. Jagadesh 1, Venugopal
Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age
 ORIGINAL ARTICLE Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age MUHAMMAD KAMRAN SIDDIQUI, MUHAMMAD KAMRAN SHAFI, BASHIR QAISRANI ABSTRACT Background:
ORIGINAL ARTICLE Evaluation of the Results of Operative Treatment of Hip Dysplasia in Children after the walking age MUHAMMAD KAMRAN SIDDIQUI, MUHAMMAD KAMRAN SHAFI, BASHIR QAISRANI ABSTRACT Background:
TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE
 TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE INDICATIONS FROM TWO-DIRECTIONAL ARTHROGRAPHY SHIGERU MITANI, YOICHI NAKATSUKA, HIROFUMI AKAZAWA, KIYOSHI AOKI, HAJIME INOUE
TREATMENT OF DEVELOPMENTAL DISLOCATION OF THE HIP IN CHILDREN AFTER WALKING AGE INDICATIONS FROM TWO-DIRECTIONAL ARTHROGRAPHY SHIGERU MITANI, YOICHI NAKATSUKA, HIROFUMI AKAZAWA, KIYOSHI AOKI, HAJIME INOUE
Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip
 International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
Evaluation of the results of operative treatment of hip dysplasia in children after the walking age
 Alexandria Journal of Medicine (2012) 48, 115 122 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Evaluation of the results of operative
Alexandria Journal of Medicine (2012) 48, 115 122 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Evaluation of the results of operative
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip
 The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia Of The Hip
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 1 Number 2 A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 1 Number 2 A One Stage Open Reduction With Salter's Innominate Osteotomy And Corrective Femoral Osteotomy For The Treatment Of Congenital Dysplasia
What is a Hip Dysplasia?
 What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year mean follow up
 754 Acta Orthop. Belg., 2016, 82, j. 754-761 mcfarlane, j. h. kuiper, n. kiely ORIGINAL STUDY Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year
754 Acta Orthop. Belg., 2016, 82, j. 754-761 mcfarlane, j. h. kuiper, n. kiely ORIGINAL STUDY Surgical treatment for developmental dysplasia of the hip- a single surgeon series of 47 hips with a 7 year
Treatment of DDH before Walking Age 고려대학안암병원
 Treatment of DDH before Walking Age 이 순혁 고려대학안암병원 Subluxated Hip Always to deg. hip The more, the earlier Even in 2nd Decade Dysplastic Hip Eventually to osteoarthritis but later Etiology of end-stage
Treatment of DDH before Walking Age 이 순혁 고려대학안암병원 Subluxated Hip Always to deg. hip The more, the earlier Even in 2nd Decade Dysplastic Hip Eventually to osteoarthritis but later Etiology of end-stage
Mohamed El-Sayed Tarek Ahmed Sameh Fathy Hosam Zyton. Introduction
 J Child Orthop (2012) 6:471 477 DOI 10.1007/s11832-012-0451-x ORIGINAL CLINICAL ARTICLE The effect of Dega acetabuloplasty and Salter innominate on acetabular remodeling monitored by the acetabular index
J Child Orthop (2012) 6:471 477 DOI 10.1007/s11832-012-0451-x ORIGINAL CLINICAL ARTICLE The effect of Dega acetabuloplasty and Salter innominate on acetabular remodeling monitored by the acetabular index
REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP
 Original Article REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP Saeid Tabatabaei 1, Ahmad Dashtbozorg 2, Sharareh Shalamzari 3 ABSTRACT Objectives:
Original Article REDISLOCATION FOLLOWING OPERATIONS TO REDUCE HIP OR TREATING DYSPLASIA IN DEVELOPMENTAL DYSPLASIA OF THE HIP Saeid Tabatabaei 1, Ahmad Dashtbozorg 2, Sharareh Shalamzari 3 ABSTRACT Objectives:
Childhood hip conditions. Belen Carsi Paediatric Orthopaedic Consultant
 Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
DDH: Pathology Diagnosis, and Treatment before Walking Age
 DDH: Pathology Diagnosis, and Treatment before Walking Age 영남의대 김세동 Ⅰ. Terminology of hip dysplasia a. Congenital dysplasia or dislocation of the hip(cdh): Hippocrates Congenital -Existing at Birth but
DDH: Pathology Diagnosis, and Treatment before Walking Age 영남의대 김세동 Ⅰ. Terminology of hip dysplasia a. Congenital dysplasia or dislocation of the hip(cdh): Hippocrates Congenital -Existing at Birth but
ED: Nirmala Op: sree BPB: lww_bpb_0322
 ED: Nirmala Op: sree BPB: lww_bpb_0322 Original article 1 Long-term results after open reduction of developmental hip dislocation by an anterior approach lateral and medial of the iliopsoas muscle Wolfgang
ED: Nirmala Op: sree BPB: lww_bpb_0322 Original article 1 Long-term results after open reduction of developmental hip dislocation by an anterior approach lateral and medial of the iliopsoas muscle Wolfgang
Downloaded from:
 Niziol, R; Elvey, M; Protopapa, E; Roposch, A (2017) Association between the ossific nucleus and osteonecrosis in treating developmental dysplasia of the Hip: updated meta-analysis. BMC Musculoskelet Disord,
Niziol, R; Elvey, M; Protopapa, E; Roposch, A (2017) Association between the ossific nucleus and osteonecrosis in treating developmental dysplasia of the Hip: updated meta-analysis. BMC Musculoskelet Disord,
Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD. November 4, 2017
 Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD November 4, 2017 Introduction Developmental Dysplasia of the Hip DDH - preferred term Teratologic hips Subluxation Dislocation-usually
Hip Dysplasia for the Primary Care Physician George Gantsoudes, MD November 4, 2017 Introduction Developmental Dysplasia of the Hip DDH - preferred term Teratologic hips Subluxation Dislocation-usually
A modified surgical approach of the hip in children: is it safe and reliable in patients with developmental hip dysplasia?
 J Child Orthop (2015) 9:199 207 DOI 10.1007/s11832-015-0659-7 ORIGINAL CLINICAL ARTICLE A modified surgical approach of the hip in children: is it safe and reliable in patients with developmental hip dysplasia?
J Child Orthop (2015) 9:199 207 DOI 10.1007/s11832-015-0659-7 ORIGINAL CLINICAL ARTICLE A modified surgical approach of the hip in children: is it safe and reliable in patients with developmental hip dysplasia?
Acta Medica Okayama JUNE 2009
 Acta Medica Okayama Volume 63, Issue 3 29 Article 1 JUNE 29 Radiographic Prediction of the Results of Long-term Treatment with the Pavlik Harness for Developmental Dislocation of the Hip Takao Ohmori Hirosuke
Acta Medica Okayama Volume 63, Issue 3 29 Article 1 JUNE 29 Radiographic Prediction of the Results of Long-term Treatment with the Pavlik Harness for Developmental Dislocation of the Hip Takao Ohmori Hirosuke
Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old
 Copyright 984 by The Journal of Bone and Joint Surgers. Incorporated Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old BY MICHAEL E. BERKELEY, M.D.*,
Copyright 984 by The Journal of Bone and Joint Surgers. Incorporated Surgical Therapy for Congenital Dislocation of the Hip in Patients Who Are Twelve to Thirty-six Months Old BY MICHAEL E. BERKELEY, M.D.*,
Ultrasound-guided gradual reduction using flexion and abduction continuous traction for developmental dysplasia of the hip
 K. Fukiage, T. Futami, Y. Ogi, Y. Harada, F. Shimozono, N. Kashiwagi, T. Takase, S. Suzuki From Shiga Medical Center for Children, Japan K. Fukiage, MD, PhD, Paediatric Orthopaedic Surgeon T. Futami, MD,
K. Fukiage, T. Futami, Y. Ogi, Y. Harada, F. Shimozono, N. Kashiwagi, T. Takase, S. Suzuki From Shiga Medical Center for Children, Japan K. Fukiage, MD, PhD, Paediatric Orthopaedic Surgeon T. Futami, MD,
L side 65% Torticollis, Plagiocephaly, Metatarsus varus Flat foot.
 DEVELOPMENTAL DISLOCATION OF THE HIP [DDH] Older terminology was Congenital dislocation of the hip. DDH means developmental dysplasia of the hip. DDH is better than CDH as dislocation is not always congenital.
DEVELOPMENTAL DISLOCATION OF THE HIP [DDH] Older terminology was Congenital dislocation of the hip. DDH means developmental dysplasia of the hip. DDH is better than CDH as dislocation is not always congenital.
DDH New Developments and Timeless Classics. DDH Define Treatment Group. (by age) DDH Imaging Choice in 6wk old Infant?
 The 59 th Annual Edward T. Smith Orthopaedic Lectureship Emerging Concepts in the Surgical Management of the Hip: Deformity, Impingement and Fracture DDH New Developments and Timeless Classics Perry L.
The 59 th Annual Edward T. Smith Orthopaedic Lectureship Emerging Concepts in the Surgical Management of the Hip: Deformity, Impingement and Fracture DDH New Developments and Timeless Classics Perry L.
Avascular necrosis following closed reduction for treatment of developmental dysplasia of the hip: a systematic review
 J Child Orthop (2016) 10:627 632 DOI 10.1007/s11832-016-0776-y ORIGINAL CLINICAL ARTICLE Avascular necrosis following closed reduction for treatment of developmental dysplasia of the hip: a systematic
J Child Orthop (2016) 10:627 632 DOI 10.1007/s11832-016-0776-y ORIGINAL CLINICAL ARTICLE Avascular necrosis following closed reduction for treatment of developmental dysplasia of the hip: a systematic
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation
 Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
Results of Surgical Treatment of Coxa Vara in Children: Valgus Osteotomy with Angle Blade Plate Fixation Chatupon Chotigavanichaya MD*, Duangjai Leeprakobboon MD*, Perajit Eamsobhana MD*, Kamolporn Kaewpornsawan
Surgical Treatment of Developmental Dysplasia of the Hip in Children Three to Five Years of Age
 ISSN: 2572-2964 Volume 2, Issue 1, 8 Pages Research Article Introduction The neglected DDH with adaptive changes in bone and soft tissue is difficult to treat and can lead to permanent disability. [1].
ISSN: 2572-2964 Volume 2, Issue 1, 8 Pages Research Article Introduction The neglected DDH with adaptive changes in bone and soft tissue is difficult to treat and can lead to permanent disability. [1].
Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip
 J Child Orthop (2016) 10:185 192 DOI 10.1007/s11832-016-0743-7 ORIGINAL CLINICAL ARTICLE Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip Mathew D. Schur
J Child Orthop (2016) 10:185 192 DOI 10.1007/s11832-016-0743-7 ORIGINAL CLINICAL ARTICLE Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip Mathew D. Schur
DDH: Pathology, Diagnosis & Treatment before Walking Age 고려대학안암병원
 DDH: Pathology, Diagnosis & Treatment before Walking Age 이 순혁 고려대학안암병원 Developmental Hip Dysplasia (DDH) Klisic 1988 AAOS 1991 Congenital Hip Dislocation Not always congenital or dislocated Causes, Risk
DDH: Pathology, Diagnosis & Treatment before Walking Age 이 순혁 고려대학안암병원 Developmental Hip Dysplasia (DDH) Klisic 1988 AAOS 1991 Congenital Hip Dislocation Not always congenital or dislocated Causes, Risk
A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip
 J Child Orthop (2014) 8:319 324 DOI 10.1007/s11832-014-0600-5 ORIGINAL CLINICAL ARTICLE A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip Anthony Cooper
J Child Orthop (2014) 8:319 324 DOI 10.1007/s11832-014-0600-5 ORIGINAL CLINICAL ARTICLE A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip Anthony Cooper
Acetabular dysplasia after treatment for developmental dysplasia of the hip
 Children s orthopaedics Acetabular dysplasia after treatment for developmental dysplasia of the hip IMPLICATIONS FOR SECONDARY PROCEDURES J. Albinana, L. A. Dolan, K. F. Spratt, J. Morcuende, M. D. Meyer,
Children s orthopaedics Acetabular dysplasia after treatment for developmental dysplasia of the hip IMPLICATIONS FOR SECONDARY PROCEDURES J. Albinana, L. A. Dolan, K. F. Spratt, J. Morcuende, M. D. Meyer,
Bo Ning, Yi Yuan, Jie Yao, Sichng Zhang and Jun Sun *
 Ning et al. BMC Musculoskeletal Disorders 2014, 15:401 RESEARCH ARTICLE Open Access Analyses of outcomes of one-stage operation for treatment of late-diagnosed developmental dislocation of the hip: 864
Ning et al. BMC Musculoskeletal Disorders 2014, 15:401 RESEARCH ARTICLE Open Access Analyses of outcomes of one-stage operation for treatment of late-diagnosed developmental dislocation of the hip: 864
Hip Dysplasia David S. Feldman, MD
 Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Joints of the lower limb
 Joints of the lower limb 1-Type: Hip joint Synovial ball-and-socket joint 2-Articular surfaces: a- head of femur b- lunate surface of acetabulum Which is deepened by the fibrocartilaginous labrum acetabulare
Joints of the lower limb 1-Type: Hip joint Synovial ball-and-socket joint 2-Articular surfaces: a- head of femur b- lunate surface of acetabulum Which is deepened by the fibrocartilaginous labrum acetabulare
DDH. Abnormal hip development Traditionally CDH (congenital dysplasia of the hip) Today DDH(developmental dysplasia of the hip)
 DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
Surgical treatment of developmental dysplasia of the hip in the periadolescent period
 J Orthop Sci (2005) 10:15 21 DOI 10.1007/s00776-004-0850-z Original article Surgical treatment of developmental dysplasia of the hip in the periadolescent period Vasilios A. Papavasiliou 1 and Athanasios
J Orthop Sci (2005) 10:15 21 DOI 10.1007/s00776-004-0850-z Original article Surgical treatment of developmental dysplasia of the hip in the periadolescent period Vasilios A. Papavasiliou 1 and Athanasios
Classifications in Brief
 Clin Orthop Relat Res (2013) 471:2068 2072 DOI 10.1007/s11999-013-2992-9 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons IN BRIEF Classifications
Clin Orthop Relat Res (2013) 471:2068 2072 DOI 10.1007/s11999-013-2992-9 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons IN BRIEF Classifications
Radiological Sequelae of developmental dysplasia of the hip: a Review
 Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
Developmental dysplasia of the hip: What has changed in the last 20 years?
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v6.i11.886 World J Orthop 2015 December 18; 6(11): 886-901 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v6.i11.886 World J Orthop 2015 December 18; 6(11): 886-901 ISSN 2218-5836 (online)
Is ultrasound screening for DDH in babies born breech sufficient?
 J Child Orthop (2010) 4:3 8 DOI 10.1007/s11832-009-0217-2 ORIGINAL CLINICAL ARTICLE Is ultrasound screening for DDH in babies born breech sufficient? Meghan Imrie Vanessa Scott Philip Stearns Tracey Bastrom
J Child Orthop (2010) 4:3 8 DOI 10.1007/s11832-009-0217-2 ORIGINAL CLINICAL ARTICLE Is ultrasound screening for DDH in babies born breech sufficient? Meghan Imrie Vanessa Scott Philip Stearns Tracey Bastrom
Society for Pediatric Radiology 2015 Hands on Session. DDH: Pitfalls and Practical Tips
 Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
The Hip Baby?? Baby Hippie??
 In Need of a Title? The Hip Baby?? Baby Hippie?? Review of Developmental Dysplasia of the Hip in the Newborn OCR Symposium 2018 Ryan L. Hartman, MD Specialty: Pediatric and Sports Orthopaedics 23 month
In Need of a Title? The Hip Baby?? Baby Hippie?? Review of Developmental Dysplasia of the Hip in the Newborn OCR Symposium 2018 Ryan L. Hartman, MD Specialty: Pediatric and Sports Orthopaedics 23 month
Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View
 Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View Ryo Mori 1, Yuji Yasunaga 2, Takuma Yamasaki 1, Michio Hamanishi 1, Takeshi Shoji 1, Sotaro Izumi 1, Susumu Hachisuka
Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View Ryo Mori 1, Yuji Yasunaga 2, Takuma Yamasaki 1, Michio Hamanishi 1, Takeshi Shoji 1, Sotaro Izumi 1, Susumu Hachisuka
)318( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )318( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Outcome of Salter Innominate Osteotomy for Developmental Hip Dysplasia before and after 3 Years Old Taghi Baghdadi, MD;
)318( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Outcome of Salter Innominate Osteotomy for Developmental Hip Dysplasia before and after 3 Years Old Taghi Baghdadi, MD;
A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip
 Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Copyright Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited.
 Original article 222 Legg Calvé Perthes disease in patients under 5 years of age does not always result in a good outcome. Personal experience and meta-analysis of the literature Kristof Fabry, Guy Fabry
Original article 222 Legg Calvé Perthes disease in patients under 5 years of age does not always result in a good outcome. Personal experience and meta-analysis of the literature Kristof Fabry, Guy Fabry
Developmental dysplasia of the hip angle trends after operation in different age groups
 Clinical research Developmental dysplasia of the hip angle trends after operation in different age groups Sonja Milasinovic 1, Radivoj Brdar 2, Ivana Petronic 3, Dejan Nikolic 3, Dragana Cirovic 3 1Institute
Clinical research Developmental dysplasia of the hip angle trends after operation in different age groups Sonja Milasinovic 1, Radivoj Brdar 2, Ivana Petronic 3, Dejan Nikolic 3, Dragana Cirovic 3 1Institute
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Does Salter Innominate Osteotomy Predispose the Patient to Acetabular Retroversion in Adulthood?
 Clin Orthop Relat Res (2015) 473:1755 1762 DOI 10.1007/s11999-014-4053-4 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Salter
Clin Orthop Relat Res (2015) 473:1755 1762 DOI 10.1007/s11999-014-4053-4 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Does Salter
Developmental Dysplasia of the Hip
 Developmental Dysplasia of the Hip Abnormal relationship of femoral head to the acetabulum Formerly known as congenital hip dislocation Believed to be developmental Most dislocations are evident at births
Developmental Dysplasia of the Hip Abnormal relationship of femoral head to the acetabulum Formerly known as congenital hip dislocation Believed to be developmental Most dislocations are evident at births
How Does Bony Surgery Affect Results of Anterior Open Reduction in Walking-age Children With Developmental Hip Dysplasia?
 Clin Orthop Relat Res (2016) 474:1199 1208 DOI 10.1007/s11999-015-4598-x Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: THE HIP FROM CHILDHOOD
Clin Orthop Relat Res (2016) 474:1199 1208 DOI 10.1007/s11999-015-4598-x Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: THE HIP FROM CHILDHOOD
DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES. Dr G B Firth
 DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES Dr G B Firth A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,
DEVELOPMENTAL HIP DYSPLASIA PREDICTING OUTCOME AND IMPLICATIONS FOR SECONDARY PROCEDURES Dr G B Firth A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,
Hip ultrasound for developmental dysplasia: the 50% rule
 Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip.
 Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip. Item Type Article Authors Molony, Diarmuid C;Harty, James A;Burke, Thomas E;D'Souza, Lester G Citation
Popliteal angle as an indicator for successful closed reduction of developmental dysplasia of the hip. Item Type Article Authors Molony, Diarmuid C;Harty, James A;Burke, Thomas E;D'Souza, Lester G Citation
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes
 The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (4), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (4), Page 64466451 Outcome of delayed surgery in developmental hip dysplasia in a tertiary care setting Mohammad Khabti Alnamshan, Ayman
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (4), Page 64466451 Outcome of delayed surgery in developmental hip dysplasia in a tertiary care setting Mohammad Khabti Alnamshan, Ayman
One-stage Hip Reconstruction for Developmental Hip Dysplasia in Children over 8 Years of Age
 ORIGINAL ARTICLE http://dx.doi.org/10.5371/hp.2018.30.4.260 Print ISSN 2287-3260 Online ISSN 2287-3279 One-stage Hip Reconstruction for Developmental Hip Dysplasia in Children over 8 Years of Age Irfan
ORIGINAL ARTICLE http://dx.doi.org/10.5371/hp.2018.30.4.260 Print ISSN 2287-3260 Online ISSN 2287-3279 One-stage Hip Reconstruction for Developmental Hip Dysplasia in Children over 8 Years of Age Irfan
Treatment of congenital subluxation and dislocation of the hip by knee splint harness
 Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Hip Biomechanics and Osteotomies
 Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia
 Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia, MBChB, D Orth, MSc. Abstract: The aim of the study to determine the benefit of delaying appearance
Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia, MBChB, D Orth, MSc. Abstract: The aim of the study to determine the benefit of delaying appearance
RESULTS OF THE EARLY TREATMENT OF DEVELOPMENTAL DYSPLASIA OF THE HIP
 RESULTS OF THE EARLY TREATMENT OF DEVELOPMENTAL DYSPLASIA OF THE HIP Dana Vasilescu, Dan Cosma University of Medicine and Pharmacy Iuliu Haţieganu Cluj-Napoca 13, E. Isac st., 400023 Cluj-Napoca, România
RESULTS OF THE EARLY TREATMENT OF DEVELOPMENTAL DYSPLASIA OF THE HIP Dana Vasilescu, Dan Cosma University of Medicine and Pharmacy Iuliu Haţieganu Cluj-Napoca 13, E. Isac st., 400023 Cluj-Napoca, România
Developmental Dysplasia of the Hip From Birth to Six Months
 From Birth to Six Months James T. Guille, MD, Peter D. Pizzutillo, MD, and G. Dean MacEwen, MD Abstract The term developmental dysplasia or dislocation of the hip (DDH) refers to the complete spectrum
From Birth to Six Months James T. Guille, MD, Peter D. Pizzutillo, MD, and G. Dean MacEwen, MD Abstract The term developmental dysplasia or dislocation of the hip (DDH) refers to the complete spectrum
The surgical treatment of Perthes disease by
 Lateral shelf acetabuloplasty in Perthes disease A REVIEW AT THE END OF GROWTH K. Daly, C. Bruce, A. Catterall From the Royal National Orthopaedic Hospital, Stanmore, England The surgical treatment of
Lateral shelf acetabuloplasty in Perthes disease A REVIEW AT THE END OF GROWTH K. Daly, C. Bruce, A. Catterall From the Royal National Orthopaedic Hospital, Stanmore, England The surgical treatment of
Medial circumflex artery Lateral circumflex artery
 Femoral Head Fractures: A Critical But Frequently Missed Injury Susanna C. Spence MD Manickam Kumaravel MBBS University of Texas Health Science Center at Houston Background Femoral head fractures: A complication
Femoral Head Fractures: A Critical But Frequently Missed Injury Susanna C. Spence MD Manickam Kumaravel MBBS University of Texas Health Science Center at Houston Background Femoral head fractures: A complication
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip
 Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
OPEN REDUCTION OF HIP DISLOCATION IN PATIENTS WITH ARTHROGRYPOSIS MULTIPLEX CONGENITA - AN ANTEROMEDIAL APPROACH
 ARTIGO ORIGINAL OPEN REDUCTION OF HIP DISLOCATION IN PATIENTS WITH ARTHROGRYPOSIS MULTIPLEX CONGENITA - AN ANTEROMEDIAL APPROACH Luis Eduardo Munhoz da Rocha 2, Fábio Koiti Nishimori 3, Daniel Carvalho
ARTIGO ORIGINAL OPEN REDUCTION OF HIP DISLOCATION IN PATIENTS WITH ARTHROGRYPOSIS MULTIPLEX CONGENITA - AN ANTEROMEDIAL APPROACH Luis Eduardo Munhoz da Rocha 2, Fábio Koiti Nishimori 3, Daniel Carvalho
CLINICAL AND RADIOLOGICAL EVALUATION ON DEVELOPMENTAL HIP DYSPLASIA AFTER SALTER AND OMBRÉDANNE PROCEDURE
 ORIGINAL ARTICLE CLINICAL AND RADIOLOGICAL EVALUATION ON DEVELOPMENTAL HIP DYSPLASIA AFTER SALTER Válney Luiz da Rocha 1, André Luiz Coelho Thomé 2, Daniel Labres da Silva Castro 2, Leandro Zica de Oliveira
ORIGINAL ARTICLE CLINICAL AND RADIOLOGICAL EVALUATION ON DEVELOPMENTAL HIP DYSPLASIA AFTER SALTER Válney Luiz da Rocha 1, André Luiz Coelho Thomé 2, Daniel Labres da Silva Castro 2, Leandro Zica de Oliveira
ORIGINAL ARTICLE. Anisuddin Bhatti, Jagdesh Kumar, Siraj Ahmed Butt
 1015 ORIGINAL ARTICLE Outcome of one stage combined open reduction, pelvic and derotation femoral osteotomy in congenital dislocated hips of children younger than three years age Anisuddin Bhatti, Jagdesh
1015 ORIGINAL ARTICLE Outcome of one stage combined open reduction, pelvic and derotation femoral osteotomy in congenital dislocated hips of children younger than three years age Anisuddin Bhatti, Jagdesh
Lower Extremity Fracture Management. Fractures of the Hip. Lower Extremity Fractures. Vascular Anatomy. Lower Extremity Fractures in Children
 Lower Extremity Fracture Management Brian Brighton, MD, MPH Levine Children s s Hospital Carolinas Medical Center Charlotte, NC Oscar Miller Day October 16, 2009 Lower Extremity Fractures in Children Anatomic
Lower Extremity Fracture Management Brian Brighton, MD, MPH Levine Children s s Hospital Carolinas Medical Center Charlotte, NC Oscar Miller Day October 16, 2009 Lower Extremity Fractures in Children Anatomic
Acta Medica Okayama AUGUST 2009
 Acta Medica Okayama Volume 63, Issue 4 2009 Article 2 AUGUST 2009 Radiological and clinical results of rotational acetabular osteotomy combined with femoral intertrochanteric osteotomy for avascular necrosis
Acta Medica Okayama Volume 63, Issue 4 2009 Article 2 AUGUST 2009 Radiological and clinical results of rotational acetabular osteotomy combined with femoral intertrochanteric osteotomy for avascular necrosis
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS
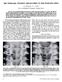 HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
Valgus extension femoral osteotomy to treat hinge abduction in Perthes disease
 J Child Orthop (2012) 6:463 469 DOI 10.1007/s11832-012-0453-8 ORIGINAL CLINICAL ARTICLE Valgus extension femoral osteotomy to treat hinge abduction in Perthes disease Pasquale Farsetti Matteo Benedetti-Valentini
J Child Orthop (2012) 6:463 469 DOI 10.1007/s11832-012-0453-8 ORIGINAL CLINICAL ARTICLE Valgus extension femoral osteotomy to treat hinge abduction in Perthes disease Pasquale Farsetti Matteo Benedetti-Valentini
Friday Teaching. Bones
 Friday Teaching Bones Regarding slipped femoral capital epiphysis It represents Salter Harris type V injury 20% are bilateral There is slight widening of the joint space Slip is typically posteromedial
Friday Teaching Bones Regarding slipped femoral capital epiphysis It represents Salter Harris type V injury 20% are bilateral There is slight widening of the joint space Slip is typically posteromedial
The costs of late detection of developmental dysplasia of the hip
 J Child Orthop (2014) 8:325 332 DOI 10.1007/s11832-014-0599-7 ORIGINAL CLINICAL ARTICLE The costs of late detection of developmental dysplasia of the hip Timothy Woodacre A. Dhadwal T. Ball C. Edwards
J Child Orthop (2014) 8:325 332 DOI 10.1007/s11832-014-0599-7 ORIGINAL CLINICAL ARTICLE The costs of late detection of developmental dysplasia of the hip Timothy Woodacre A. Dhadwal T. Ball C. Edwards
SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW
 SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW Dr. Upendra Yadav *1, 3, Dr. Zhu Xiao Fang 3, Dr. Ajit Kumar Yadav 1, 2, Dr. Sudhir Kumar Yadav 4 and Dr. Jeetendra Yadav 4 1 Yangtze
SCREENING THE NEWBORN FOR DEVELOPMENTAL DYSPLASIA OF THE HIP: REVIEW Dr. Upendra Yadav *1, 3, Dr. Zhu Xiao Fang 3, Dr. Ajit Kumar Yadav 1, 2, Dr. Sudhir Kumar Yadav 4 and Dr. Jeetendra Yadav 4 1 Yangtze
ORDER OF VERBAL EXAMS
 ORDER OF VERBAL EXAMS The students are able to register for the exam on the NEPTUN system. The students pick two titles, from the title list available at the beginning of the Semester. This list can be
ORDER OF VERBAL EXAMS The students are able to register for the exam on the NEPTUN system. The students pick two titles, from the title list available at the beginning of the Semester. This list can be
Bilateral hip pain with right proximal femoral lesion
 Bilateral hip pain with right proximal femoral lesion Legg-Calve-Perthes Idiopathic osteonecrosis of the femoral head epiphysis during childhood First described by Arthur Thorton Legg in 1909 and published
Bilateral hip pain with right proximal femoral lesion Legg-Calve-Perthes Idiopathic osteonecrosis of the femoral head epiphysis during childhood First described by Arthur Thorton Legg in 1909 and published
Percutaneous medial hemi-epiphysiodesis using a transphyseal screw for caput valgum associated with developmental dysplasia of the hip
 Shin et al. BMC Musculoskeletal Disorders (2017) 18:451 DOI 10.1186/s12891-017-1833-5 RESEARCH ARTICLE Percutaneous medial hemi-epiphysiodesis using a transphyseal screw for caput valgum associated with
Shin et al. BMC Musculoskeletal Disorders (2017) 18:451 DOI 10.1186/s12891-017-1833-5 RESEARCH ARTICLE Percutaneous medial hemi-epiphysiodesis using a transphyseal screw for caput valgum associated with
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ
 Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Preoperative Planning for DDH Revision Surgery Tips and Tricks
 Review Article Preoperative Planning for DDH Revision Surgery Tips and Tricks Mousa M. Alhaosawi MD 1, Amir Shahryar Ariamanesh MD 2* 1- King Fahad Hospital, Almadinah Almunawwarah, Saudi Arabia 2- Mashhad
Review Article Preoperative Planning for DDH Revision Surgery Tips and Tricks Mousa M. Alhaosawi MD 1, Amir Shahryar Ariamanesh MD 2* 1- King Fahad Hospital, Almadinah Almunawwarah, Saudi Arabia 2- Mashhad
Ultrasound Scanning of Neonatal Hips
 Ultrasound Scanning of Neonatal Hips Dr. Dickson S F Tsang Associate Consultant Queen Mary Hospital Why? How? What? Outline IAAHS 2nd April, 2011 Outline Why? Why performing hip ultrasound (USG)? Why USG?
Ultrasound Scanning of Neonatal Hips Dr. Dickson S F Tsang Associate Consultant Queen Mary Hospital Why? How? What? Outline IAAHS 2nd April, 2011 Outline Why? Why performing hip ultrasound (USG)? Why USG?
The Pavlik harness is a positioning device commonly
 RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Developmental dysplasia of the hip
 Developmental dysplasia of the hip Shahryar Noordin, Masood Umer, Kamran Hafeez, Haq Nawaz Section of Orthopedics, Dept. of Surgery, Aga Khan University, Karachi, Pakistan Abstract Developmental dysplasia
Developmental dysplasia of the hip Shahryar Noordin, Masood Umer, Kamran Hafeez, Haq Nawaz Section of Orthopedics, Dept. of Surgery, Aga Khan University, Karachi, Pakistan Abstract Developmental dysplasia
Peggers Super Summaries: Paediatric Hip
 EMBRYOLOGY Development o Mesenchymal stem cells cartilage blood supply bone Dates o 6/40 Limb development o 8-11/40 hip development (acetabulum and hip formed from one bone splitting by apoptosis) o 16/40
EMBRYOLOGY Development o Mesenchymal stem cells cartilage blood supply bone Dates o 6/40 Limb development o 8-11/40 hip development (acetabulum and hip formed from one bone splitting by apoptosis) o 16/40
