First-time anterior shoulder dislocation natural history and epidemiology: immobilization versus early surgical repair
|
|
|
- Jessica Green
- 5 years ago
- Views:
Transcription
1 Review Article Page 1 of 7 First-time anterior shoulder dislocation natural history and epidemiology: immobilization versus early surgical repair Tanner Gurney-Dunlop, Ahmed Shawky Eid, Jason Old, James Dubberley, Peter MacDonald Section of Orthopaedics, Department of Surgery, Pan Am Clinic/University of Manitoba, Winnipeg, Manitoba, Canada Contributions: (I) Conception and design: T Gurney-Dunlop; (II) Administrative support: All authors; (III) Provision of study materials or patients: T Gurney-Dunlop; (IV) Collection and assembly of data: T Gurney-Dunlop; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Tanner Gurney-Dunlop. Section of Orthopaedics, Department of Surgery, Pan Am Clinic/University of Manitoba, Winnipeg, Manitoba R3M 3E4, Canada. tannerdunlop@gmail.com. Abstract: Traumatic anterior shoulder dislocations are a common problem. There is a high rate of recurrent instability, especially in patients <30 years of age that are involved in high level sports. The purpose of this review is to discuss the natural history after a first-time shoulder dislocation and provide a brief overview of management options. Initial nonoperative management consists of immobilization in internal rotation for 1 3 weeks. The current evidence does not support immobilization in external rotation or for longer periods of time. For those patients who are at a high risk of recurrent instability, the evidence suggests that early surgical repair to address the pathology can be undertaken. This has shown to be clinically and fiscally effective while improving patient outcomes. Keywords: Shoulder; instability; anterior dislocation; arthroscopic stabilization Received: 01 June 2017; Accepted: 18 September 2017; Published: 22 November doi: /aoj View this article at: Introduction The glenohumeral joint is the most frequently dislocated major joint in the body due to the large arc of motion. The majority of dislocations are anterior following traumatic events with the shoulder in the at risk position of abduction and external rotation. Anterior shoulder dislocations have an estimated general population prevalence of 2% to 8% (1-3) and overall incidence rate in the United States of 23.9 per 100,000 person-years (4). Despite traumatic first-time anterior dislocations being a common injury, there remains controversies over the best management strategy for these patients. Certain situations warrant special considerations such as dislocation in the elderly and the mid-season instability event in the young athlete. The purpose of this review is to summarize and present the current literature on the first-time traumatic anterior shoulder dislocation focusing on the natural history, epidemiology, and current treatment recommendations. Natural history Given the common nature of this injury, the orthopaedic surgeon needs a thorough understanding of the natural history to be able to engage in a discussion with the patient to optimize treatment and patient outcomes. The overall goal of treatment should be to minimize the risk of recurrent instability and improve the patient s quality of life. The incidence of recurrent instability ranges from 14% to 100% in the literature (5). There are many factors that influence the risk of recurrent dislocations following a patient s first traumatic anterior shoulder dislocation. Traditionally, age and gender have been identified as key factors in determining the possibility of recurrent dislocations, however, several other factors have been found to influence the rate of recurrence. Recurrent instability has been considered the main outcome measure but it is
2 Page 2 of 7 Annals of Joint, 2017 prudent to consider others, such as continued apprehension, failure to return to work or sport, quality of life outcomes, and the development of post-traumatic osteoarthritis. Age and gender Young males, who are at a high risk of having a first-time dislocation, are known to be at an increased risk of recurrent instability. Robinson et al. (6) reported a survival analysis to predict recurrent instability at 1, 2, and 5 years in patient age groups years, years, years and years, and found at 5 years they were 86.6%, 73.8%, 48.8%, and 30.7%, respectively. In gender comparison at 5 years, men had a higher percent of recurrent instability when compared to women (70.4% vs. 37.5%). Hovelius et al. (7) reported one of the longest prospective studies, a 25-year follow-up study of patients who were treated non-operatively following a primary traumatic anterior shoulder dislocation. They found a recurrence rate of 72% among patients aged years, 56% of those years and 27% in patients older than 30 years and noted 38% of patients aged years underwent surgical stabilization at some point. Level and types of sports Contact or overhead sports were found to be associated with a higher risk for recurrence compared to non-contact or no sport participation. In a prognostic level I study, Sachs et al. (8) noted a higher re-dislocation rate (55%) following a primary traumatic anterior shoulder dislocation in patients who played contact or collision sports compared with those who did not (38%). Robinson et al. (6) found the recurrence rates for patients who played contact or overhead sports, non-contact sports, or no sports were 63.3%, 73.3%, and 46.0% at 2 years and 62.8%, 33.9%, and 43.9% at 5 years, respectively. Bony factors Significant bone defects of the glenoid, humeral head or both are known risk factors for recurrent instability. Isolated anterior glenoid fractures (bony Bankart lesions) involving >20% of the glenoid width are associated with a high recurrence rate even following a Bankart repair (9). Associated Hill-Sachs lesions should not be ignored, as there is risk of engagement and dislocation of the humeral head if it extends medially over the medial margin of the glenoid track. The size of these lesions should be considered in addition to a co-existing anterior glenoid defect (10). Soft tissue factors Generalized ligamentous laxity has been shown as a risk factor for primary traumatic anterior shoulder dislocation and subsequent recurrences. In a prospective study on 38 patients with a primary traumatic anterior shoulder dislocation, Muhammad et al. (11) reported a higher incidence of recurrence in hypermobile patients compared to patients who did not have hypermobility (60% vs. 39%). Thirty percent of patients fulfilled the Beighton score criteria for hypermobility and 60% had a family history of laxity. Similarly, Cameron et al. (12) observed an association between generalized hypermobility and glenohumeral instability. Military cadets with hypermobility, defined as a score of 2 on the Beighton scale, were 2.5 times more likely to report a history of glenohumeral joint instability. Anterior labral-periosteal sleeve avulsion (ALPSA) lesions was reported to occur in 30% of patients with primary anterior dislocation (13). Patients with ALPSA lesions present with a higher number of recurrent dislocations than those with discrete Bankart lesions. Accordingly, surgical stabilization is recommended to prevent further capsulolabral damage (14,15). Patients presenting with a primary traumatic anterior shoulder dislocation, should be counseled about the natural history and the relevant risk factors of recurrence following surgical stabilization and non-operative management, so that an informed decision can be made. Dislocation in patients older than 40 years Patients older than 40 years old at the time of their initial traumatic anterior shoulder dislocation require special consideration as they can present with pathology likely not seen in younger individuals. These individuals are more likely to sustain injuries to the rotator cuff, axillary nerve or brachial plexus. Rotator cuff pathologies following a dislocation is more common than nerve palsies and are more frequent with advancing age (16). Rotator cuff tears can be mistaken for nerve palsies. Therefore, when evaluating these patients, a thorough evaluation for rotator cuff lesions is mandatory. Patients older than 40 years of age have a 35% prevalence of rotator cuff tears, which increases to over 80% at 60 years and older (16). Though rotator cuff pathology is common, the lesions vary widely and
3 Annals of Joint, 2017 when there is extension of the tear anterosuperior into the subscapularis tendon, the prognosis is very poor. As over 20% of all dislocations occur in those over 60 years, an early MRI has been recommended for the above reasons (17). Early diagnosis and repair of the traumatic rotator cuff tear yields optimal outcomes (18). Arthropathy following dislocation Hovelius and Saeboe (19) looked at the presence of arthropathy after a primary anterior traumatic dislocation 25 years later. Those who experienced recurrent dislocations had a significantly higher proportion of arthropathy (40%) compared to those without recurrence (18%). They concluded that risk factors found to correlate with the development of arthropathy (moderate/severe) included age >25 years at time of initial dislocation, high energy sports activities as the dislocation etiology, recurrence and alcohol abuse. Similar results were previously reported by Buscayret et al. (20). Page 3 of 7 Patients were split into two groups, <30 years and 30 years. The recurrence rate was 89% in the <30 years group and 26% in the 30 years group (P<0.05). A relationship between the immobilization period and the recurrence rate could not be found (P=0.8). Simonet et al. (23) concluded that duration of immobilization had no effect on the risk of recurrent instability within 124 patients who suffered a traumatic anterior shoulder dislocation and were immobilized from 1 to 6 weeks. There was a positive difference noted in regards to satisfaction when patients refraining from sports, or full activities, for a longer duration of time ( 6 weeks) compared to those who returned at <6 weeks. Currently, there is a level I study (24) and multiple level II studies that have been unable to demonstrate that longer periods of immobilization reduce the risk of recurrent instability episodes. However, it is possible that longer immobilization may improve pain and patient satisfaction in the acute setting. Currently it is recommended to immobilize patients for 1 to 3 weeks. Nonoperative management Traditionally, nonoperative management has been carried out for patients suffering from a primary traumatic anterior shoulder dislocation. This starts in the emergency room with a closed reduction. This can be done with premedication with intra-articular lidocaine or intravenous sedation. There are many described reduction techniques that may be used. Simple traction-counter traction is most commonly used, however, no one technique can be recommended and the physician should use whichever technique they are most comfortable with. Following a closed reduction, the arm is immobilized for two reasons, pain control and patient satisfaction. However, immobilization has not been shown to decrease the rate of recurrence. Consideration of the length and position of immobilization are important. Length of immobilization Following a meta-analysis, Paterson et al. (21) reported no significant differences in recurrence rates in patients aged <30 years who were immobilized for 1 week (41%) compared to those patients who were immobilized for 3 weeks (37%). Lill et al. (22) noted length of immobilization was dependent on patient age at time of dislocation within 175 patients treated conservatively. Position of immobilization The concept of immobilizing the arm in external rotation for nonoperative management of a first-time shoulder dislocation was developed in the late 1990s. The rationale behind this position was to put tension on the subscapularis, thereby positioning the soft tissues in a more favorable position on the glenoid. Proponents of positioning the arm in external rotation cite both cadaveric and MRI studies that show a better positioning of soft tissues in relation to the glenoid (25-27). Itoi et al. (28) showed immobilization in external rotation for 3 weeks to be associated with significantly less re-dislocation than when immobilized in an internal rotation position for the same length of time (29). However, subsequent studies were not able to reproduce these results and found no difference in the re-dislocation rate between immobilization in internal and external rotation (30). Following a meta-analysis, Paterson et al. (21) reported a non-statistically significant difference in the rate of recurrent instability for those immobilized in internal rotation (40%) compared to those managed in external rotation (35%). Jordan et al. (31) performed a systematic review looking at external rotation bracing for anterior shoulder dislocation. Of the six studies assessed, five looked at labral reduction on MRI and one arthroscopically. Each study reported overall improvement in labral reduction
4 Page 4 of 7 Annals of Joint, 2017 with external rotation, but anatomic reduction was only achieved 35% of the time. They concluded failure to reduce the labrum may be a contraindication to external rotation bracing. A recent Cochrane review (32) also noted a lack of good evidence to make any strong recommendations to immobilize in external rotation. To date, there are multiple level I studies, including randomized control trials (RCTs) and meta-analyses that exist, however, a significant amount of inconsistency has been found among these studies. The majority do not show a benefit to immobilization in external rotation, and most physicians continue to immobilize in internal rotation for ease and practicality. Failure of nonoperative management is usually manifested by recurrent symptoms of instability such as dislocations, subluxations or pain despite nonoperative management. Failure to return to sport or work could be considered failure as well. Surgical management Surgical management for a first-time anterior shoulder dislocation has increased in frequency. Historically, stabilization was reserved for patients who had recurrently instability, with the goal of surgical stabilization to restore normal soft tissue anatomy and re-tensioning of the inferior glenohumeral ligament. As some populations, such as the young, active athlete have a high rate of recurrent instability, there has been an increasing role for immediate surgical stabilization. Indications for arthroscopic anterior soft tissue stabilization after primary anterior shoulder dislocation include young patients, high demand patients, recurrent traumatic anterior instability without bone loss, and overhead athletes, especially throwing athletes where preserving motion is preferred. Open bony procedures may be considered when there are large engaging Hill-Sachs lesions or significant bony deficiencies of the glenoid (>20%). Arciero et al. (33) and Deberardino et al. (34) showed a statistically significant difference in recurrence following primary traumatic anterior shoulder dislocation in those treated with surgical stabilization vs. conservative treatment management in a young, high demand, active population. A prospective randomized control trial performed by Kirkley et al. (1) found a significant difference between recurrent dislocations between the surgical group (19%) and the conservative group (60%) within 40 patients aged <30 years old randomized to early surgical stabilization with rehabilitation or immobilization with rehabilitation. Thus, they suggest early surgical stabilization in patients <30 years and high-level athletes is the treatment of choice. Risk of arthropathy A commonly cited reason for early surgical stabilization is prevention of future arthritis. Hovelius et al. (7) reported 11% of the primary anterior shoulder dislocations treated nonoperatively developed mild arthritis. Eighteen percent developed moderate or severe, regardless of whether there was recurrence and regardless of treatment the patient received. Ogawa et al. (35) looked at radiographs and computed tomography (CT) evidence of preoperative arthritis in patients with scheduled surgery for primary anterior shoulder dislocation. Two hundred and eightytwo shoulders were evaluated in patients younger than 40 years without previous surgery. Osteoarthritis was found in 32 joints (11.3%) (mild in 30 and moderate in 2) on the radiographs. CT revealed arthritic changes in 88 shoulders (31.2%), including all 32 radiographically osteoarthritic joints. They concluded that the development of preoperative osteoarthritis in cases with traumatic anterior instability is closely related to the total number and frequency of repeated trauma. Further long-term studies are needed to examine the effect and incidence of osteoarthritis after primary anterior shoulder dislocation and whether initial stabilization decreases the risk of osteoarthritis from recurrent instability. Cost effectiveness Crall et al. (36) examined the cost effectiveness of early surgical stabilization specifically for first-time dislocations, comparing age groups, and gender in patients aged 15 vs. 25 vs. 35 years. Primary surgery was less costly and more clinically effective for 15-year-old males, females and 25-year-old males. For the remaining scenarios, primary surgery was more effective and costly, however, it was noted to still be very cost-effective (cost per quality-adjusted life year, <$25,000). In all scenarios, surgery was less costly and more effective, even after recurrent dislocations. Open vs. arthroscopic Today, the most common procedure in North America for managing anterior shoulder instability without significant glenoid or humeral head bone loss is arthroscopic
5 Annals of Joint, 2017 stabilization. This is due to the continued improvements and advancements in both arthroscopic techniques and implant advancements. Analysis of data from the American Board of Orthopedic Surgery Certification Examination shows a significant trend towards arthroscopic stabilization with nearly 90% of the procedures being done arthroscopically in 2008 (37). Fabbriciani et al. (38) were among the first to show equivalent outcomes between arthroscopic stabilization with suture anchors and open repair. Quality of Life As previously mentioned, Kirkley et al. (1) evaluated recurrent instability as well as quality of life and functional outcomes. Forty patients <30 years of age were randomized to immediate anterior stabilization plus rehabilitation or immobilization followed by rehabilitation. The Western Ontario Shoulder Instability (WOSI) index scores were followed for each patient. The surgical group showed improvements in four components of the WOSI: physical symptoms, sport function, lifestyle and social function, and emotional wellbeing. This supports the notion that early surgery not only decreased recurrence rate but also improved quality of life in patients who are younger than 30 years and are high level athletes. Treatment should be individualized with consideration of all factors affecting recurrence. Current evidence supports initial surgical stabilization in younger patients aged <30 years who participate in collision or contact sports to reduce the rate of recurrences. This can be accomplished with arthroscopic stabilization when no significant bone loss is present. Mid-season anterior instability in athletes Competitive and overhead athletes are at risk for a glenohumeral instability event, which frequently occurs during the competitive season. Returning the athlete to competition needs to be done safely and efficiently. Minimizing the time away from competition, prevention of further injury and restoring function should be the goals of treatment (38). Generally, it is possible for athletes with an in-season instability event to have an attempt at nonoperative management and rehabilitation carried out with a return to competition that season. Nonsurgical management recommendations are similar to nonathletes and consists Page 5 of 7 of immobilization (3 to 10 days) with early rehabilitation focusing on range of motion (ROM), strengthening, scapular stabilization, and sport-specific exercises. When deciding when on treating an athlete nonoperatively we can look to certain player and sport-specific characteristics described by Owens et al. (39) to help guide management. Injury characteristics include initial shoulder dislocation, osseous defects in the glenoid <25%, and absence of fracture or soft tissue that requires surgery. Player- and sport-specific characteristics include the athlete desires to return to sports during the same season, non-overhead or non-throwing athlete, noncontact sport, and the athletes ability to complete sport-specific drills without instability. The athlete may be able to return to sport in 7 to 21 days if they demonstrate symmetric pain-free shoulder ROM and strength, the ability to perform sport-specific skills, with the absence of subjective or objective instability. The decision to proceed with in-season surgical stabilization is made following failure of nonoperative management. Usually this presents as a failure to perform sport-specific drills. Other indications include recurrent instability episodes, athlete s eligibility for future playing time, and the timing of the instability event during the season. Early surgical stabilization can be considered in those with large bony defects, recurrent instability, inability to perform sport-specific drills and where nonsurgical management may place limitations on shoulder function that would prevent the athlete from returning to competition, such as a throwing athlete. Conclusions Following primary traumatic anterior shoulder dislocation, there is a high likelihood of recurrent instability with age, gender, level and type of sport, soft-tissue and bony factors each playing a role. Currently, nonoperative management is most often attempted, with immobilization in internal rotation for 1 3 weeks to assist in pain control and patient comfort, followed by rehabilitation focused on shoulder ROM, strengthening +/ sport-specific exercises. There is currently no evidence to suggest a clinical advantage of immobilization in external rotation nor longer duration of immobilization. Early surgical management should be considered in patients under age of 30 who are higher level athletes. It has shown to be cost-effective resulting in decreased recurrence rates and improved quality of life. However, treatment should be tailored to the individual patient, with careful consideration of the natural history,
6 Page 6 of 7 Annals of Joint, 2017 relevant risk factors of recurrence and evaluation of patient specific goals and outcome measures. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Kirkley A, Werstine R, Ratjek A, et al. Prospective randomized clinical trial comparing the effectiveness of immediate arthroscopic stabilization versus immobilization and rehabilitation in first traumatic anterior dislocations of the shoulder: long-term evaluation. Arthroscopy 2005;21: Brophy RH, Marx RG. The treatment of traumatic anterior instability of the shoulder: nonoperative and surgical treatment. Arthroscopy 2009;25: Kirkley A, Griffin S, McLintock H, et al. The development and evaluation of a disease-specific quality of life measurement tool for shoulder instability. The Western Ontario Shoulder Instability Index (WOSI). Am J Sports Med 1998;26: Zacchilli MA, Owens BD. Epidemiology of shoulder dislocations presenting to emergency departments in the United States. J Bone Joint Surg Am 2010;92: Boone JL, Arciero RA. First-time anterior shoulder dislocations: has the standard changed? Br J Sports Med 2010;44: Robinson CM, Howes J, Murdoch H, et al. Functional outcome and risk of recurrent instability after primary traumatic anterior shoulder dislocation in young patients. J Bone Joint Surg Am 2006;88: Hovelius L, Olofsson A, Sandström B, et al. Nonoperative treatment of primary anterior shoulder dislocation in patients forty years of age and younger. a prospective twenty-five-year follow-up. J Bone Joint Surg Am 2008;90: Sachs RA, Lin D, Stone ML, et al. Can the need for future surgery for acute traumatic anterior shoulder dislocation be predicted? J Bone Joint Surg Am 2007;89: Itoi E, Lee SB, Berglund LJ, et al. The effect of a glenoid defect on anteroinferior stability of the shoulder after Bankart repair: a cadaveric study. J Bone Joint Surg Am 2000;82: Provencher MT, Bhatia S, Ghodadra NS, et al. Recurrent shoulder instability: current concepts for evaluation and management of glenoid bone loss. J Bone Joint Surg Am 2010;92 Suppl 2: Akhtar Muhammad A, Jenkins P, Ashton F, et al. Hypermobility- a risk factor for recurrent shoulder dislocations. Br J Sports Med 2013;47:e Cameron KL, Duffey ML, DeBerardino TM, et al. Association of generalized joint hypermobility with a history of glenohumeral joint instability. J Athl Train 2010;45: Kim DS, Yoon YS, Yi CH. Prevalence comparison of accompanying lesions between primary and recurrent anterior dislocation in the shoulder. Am J Sports Med 2010;38: Ozbaydar M, Elhassan B, Diller D, et al. Results of arthroscopic capsulolabral repair: Bankart lesion versus anterior labroligamentous periosteal sleeve avulsion lesion. Arthroscopy 2008;24: Lee BG, Cho NS, Rhee YG. Anterior labroligamentous periosteal sleeve avulsion lesion in arthroscopic capsulolabral repair for anterior shoulder instability. Knee Surg Sports Traumatol Arthrosc 2011;19: Rapariz JM, Martin-Martin S, Pareja-Bezares A, et al. Shoulder dislocation in patients older than 60 years of age. Int J Shoulder Surg 2010;4: Rumian A, Coffey D, Fogerty S, et al. Acute first-time shoulder dislocation. Orthop Trauma 2011;25: Pevny T, Hunter RE, Freeman JR. Primary traumatic anterior shoulder dislocation in patients 40 years of age and older. Arthroscopy 1998;14: Hovelius L, Saeboe M. Neer Award 2008: Arthropathy after primary anterior shoulder dislocation--223 shoulders prospectively followed up for twenty-five years. J Shoulder Elbow Surg 2009;18: Buscayret F, Edwards TB, Szabo I, et al. Glenohumeral arthrosis in anterior instability before and after surgical treatment: incidence and contributing factors. Am J Sports Med 2004;32: Paterson WH, Throckmorton TW, Koester M, et al. Position and duration of immobilization after primary anterior shoulder dislocation: a systematic review and meta-analysis of the literature. J Bone Joint Surg Am 2010;92: Lill H, Korner J, Hepp P, et al. Age-Dependent Prognosis Following Conservative Treatment of Traumatic Anterior
7 Annals of Joint, 2017 Page 7 of 7 Shoulder Dislocation. Eur J Trauma 2001;27: Simonet WT, Melton LJ 3rd, Cofield RH, et al. Incidence of anterior shoulder dislocation in Olmsted County, Minnesota. Clin Orthop Relat Res 1984;(186): Kuhn JE. Treating the initial anterior shoulder dislocation- -an evidence-based medicine approach. Sports Med Arthrosc 2006;14: Itoi E, Sashi R, Minagawa H, et al. Position of immobilization after dislocation of the glenohumeral joint. A study with use of magnetic resonance imaging. J Bone Joint Surg Am 2001;83-A: Seybold D, Schliemann B, Heyer CM, et al. Which labral lesion can be best reduced with external rotation of the shoulder after a first-time traumatic anterior shoulder dislocation? Arch Orthop Trauma Surg 2009;129: Miller BS, Sonnabend DH, Hatrick C, et al. Should acute anterior dislocations of the shoulder be immobilized in external rotation? A cadaveric study. J Shoulder Elbow Surg 2004;13: Itoi E, Hatakeyama Y, Sato T, et al. Immobilization in external rotation after shoulder dislocation reduces the risk of recurrence. A randomized controlled trial. J Bone Joint Surg Am 2007;89: Itoi E, Hatakeyama Y, Kido T, et al. A new method of immobilization after traumatic anterior dislocation of the shoulder: a preliminary study. J Shoulder Elbow Surg 2003;12: Liavaag S, Brox JI, Pripp AH, et al. Immobilization in external rotation after primary shoulder dislocation did not reduce the risk of recurrence: a randomized controlled trial. J Bone Joint Surg Am 2011;93: Jordan RW, Saithna A, Old J, et al. Does external rotation bracing for anterior shoulder dislocation actually result in reduction of the labrum? A systematic review. Am J Sports Med 2015;43: Hanchard NC, Goodchild LM, Kottam L. Conservative management following closed reduction of traumatic anterior dislocation of the shoulder. Cochrane Database Syst Rev 2014;(4):CD Arciero RA, Wheeler JH, Ryan JB, et al. Arthroscopic Bankart repair versus nonoperative treatment for acute, initial anterior shoulder dislocations. Am J Sports Med 1994;22: DeBerardino TM, Arciero RA, Taylor DC, et al. Prospective evaluation of arthroscopic stabilization of acute, initial anterior shoulder dislocations in young athletes. Two- to five-year follow-up. Am J Sports Med 2001;29: Ogawa K, Yoshida A, Ikegami H. Osteoarthritis in shoulders with traumatic anterior instability: preoperative survey using radiography and computed tomography. J Shoulder Elbow Surg 2006;15: Crall TS, Bishop JA, Guttman D, et al. Costeffectiveness analysis of primary arthroscopic stabilization versus nonoperative treatment for first-time anterior glenohumeral dislocations. Arthroscopy 2012;28: Owens BD, Harrast JJ, Hurwitz SR, et al. Surgical trends in Bankart repair: an analysis of data from the American Board of Orthopaedic Surgery certification examination. Am J Sports Med 2011;39: Fabbriciani C, Milano G, Demontis A, et al. Arthroscopic versus open treatment of Bankart lesion of the shoulder: a prospective randomized study. Arthroscopy 2004;20: Owens BD, Dickens JF, Kilcoyne KG, et al. Management of mid-season traumatic anterior shoulder instability in athletes. J Am Acad Orthop Surg 2012;20: doi: /aoj Cite this article as: Gurney-Dunlop T, Eid AS, Old J, Dubberley J, MacDonald P. First-time anterior shoulder dislocation natural history and epidemiology: immobilization versus early surgical repair..
First-Time Anterior Shoulder Dislocation: Is it time to take a stand?
 Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Surgical versus conservative treatment for acute first-time anterior shoulder dislocation: the evidence
 J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years
 Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years Elisabeth C. Robinson,* MD, Vijay B. Thangamani, MD, Michael A. Kuhn, MD, and Glen Ross, MD Investigation performed
Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years Elisabeth C. Robinson,* MD, Vijay B. Thangamani, MD, Michael A. Kuhn, MD, and Glen Ross, MD Investigation performed
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Patient ID. Case Conference. Physical Examination. Image examination. Treatment 2011/6/16
 Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
SHOULDER AND ELBOW. M. Bouliane, D. Saliken, L. A. Beaupre, A. Silveira, M. K. Saraswat, D. M. Sheps
 M. Bouliane, D. Saliken, L. A. Beaupre, A. Silveira, M. K. Saraswat, D. M. Sheps From University of Alberta, Edmonton, Alberta, Canada M. Bouliane, MD, FRCS(C), Orthopaedic Surgeon D. Saliken, MD, Orthopaedic
M. Bouliane, D. Saliken, L. A. Beaupre, A. Silveira, M. K. Saraswat, D. M. Sheps From University of Alberta, Edmonton, Alberta, Canada M. Bouliane, MD, FRCS(C), Orthopaedic Surgeon D. Saliken, MD, Orthopaedic
Management of Anterior Shoulder Instability
 Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; a 2 Year Follow Up
 External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; a 2 Year Follow Up 2010 Bi-Annual SESA Closed Conference DISCLAIMER None of the authors have
External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; a 2 Year Follow Up 2010 Bi-Annual SESA Closed Conference DISCLAIMER None of the authors have
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior Shoulder Instability
 Original Article DOI 10.3349/ymj.2010.51.3.421 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 421-426, 2010 The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior
Original Article DOI 10.3349/ymj.2010.51.3.421 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 421-426, 2010 The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior
Disclosure. Traumatic Anterior Shoulder Instability 7/23/2018. Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist
 Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist Christopher E. Baker M.D. Sports Medicine Shoulder Reconstruction Traumatic Anterior Shoulder Instability Disclosure Speaking/Consulting
Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist Christopher E. Baker M.D. Sports Medicine Shoulder Reconstruction Traumatic Anterior Shoulder Instability Disclosure Speaking/Consulting
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
The Open Orthopaedics Journal
 Send Orders for Reprints to reprints@benthamscience.ae The Open Orthopaedics Journal, 2017, 11, (Suppl-6, M17) 1001-1010 1001 The Open Orthopaedics Journal Content list available at: www.benthamopen.com/toorthj/
Send Orders for Reprints to reprints@benthamscience.ae The Open Orthopaedics Journal, 2017, 11, (Suppl-6, M17) 1001-1010 1001 The Open Orthopaedics Journal Content list available at: www.benthamopen.com/toorthj/
My shoulder popped out what now?
 My shoulder popped out what now? Richard Dallalana Epworth Shoulder Symposium June 2017 Shoulder Dislocation First event Best approach? Manual Reduction Should it be put back on field? - YES Prone lying
My shoulder popped out what now? Richard Dallalana Epworth Shoulder Symposium June 2017 Shoulder Dislocation First event Best approach? Manual Reduction Should it be put back on field? - YES Prone lying
Watson et al Jul Aug A Clinical Review of Return-to-Play Considerations After Anterior Shoulder Dislocation
 651956SPHXXX10.1177/1941738116651956Watson et alsports Health research-article2016 Watson et al Jul Aug 2016 [ Orthopaedic Surgery ] A Clinical Review of Return-to-Play Considerations After Anterior Shoulder
651956SPHXXX10.1177/1941738116651956Watson et alsports Health research-article2016 Watson et al Jul Aug 2016 [ Orthopaedic Surgery ] A Clinical Review of Return-to-Play Considerations After Anterior Shoulder
Shoulder Instability Disclosures
 Bony Deficiency and the Latarjet Procedure Detroit, MI July 13, 2017 Shariff K. Bishai, D.O., M.S., FAOAO Associated Orthopedists of Detroit, PC Sports Medicine, Shoulder Surgery and Hip Arthroscopy Assistant
Bony Deficiency and the Latarjet Procedure Detroit, MI July 13, 2017 Shariff K. Bishai, D.O., M.S., FAOAO Associated Orthopedists of Detroit, PC Sports Medicine, Shoulder Surgery and Hip Arthroscopy Assistant
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai
 POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
Glenoid Track Concept vs Humeral Head Engagement in Recurrent Anterior Shoulder Instability with Glenoid Bone Loss Less Than 25%
 Med. J. Cairo Univ., Vol. 85, No. 6, September: 2407-2412, 2017 www.medicaljournalofcairouniversity.net Glenoid Track Concept vs Humeral Head Engagement in Recurrent Anterior Shoulder Instability with
Med. J. Cairo Univ., Vol. 85, No. 6, September: 2407-2412, 2017 www.medicaljournalofcairouniversity.net Glenoid Track Concept vs Humeral Head Engagement in Recurrent Anterior Shoulder Instability with
Shoulder Arthroscopy. Dr. J.J.A.M. van Raaij. NOV Jaarvergadering Den Bosch 25 jan 2018
 Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Shoulder Instability and Tendon Injuries
 Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D.
 Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM
 RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; A 2 year Follow-up
 External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; A 2 year Follow-up Moxon A.P., Walker T., Rando A. Gold Coast Hospital, Nerang Rd, Southport,
External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; A 2 year Follow-up Moxon A.P., Walker T., Rando A. Gold Coast Hospital, Nerang Rd, Southport,
Sports Medicine: Shoulder Arthrography. Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System
 Sports Medicine: Shoulder Arthrography Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Disclosure Off-label use for gadolinium Pediatric Sports Injuries
Sports Medicine: Shoulder Arthrography Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Disclosure Off-label use for gadolinium Pediatric Sports Injuries
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Glenohumeral Joint Instability: An Athlete s Perspective
 Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Shoulder Instability
 J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
Review Article International Journal of Basic and Clinical Studies (IJBCS) 2016; 5(2): Celik D et al.
 Traumatic Anterior Shoulder Instability: A Review of Pathoanatomy Diagnosis and Evaluation Derya Celik 1 Buket Akinci 2 Saime Nilay Arman 3 1 Assoc.Prof, PT, PhD, Istanbul University, Faculty of Health
Traumatic Anterior Shoulder Instability: A Review of Pathoanatomy Diagnosis and Evaluation Derya Celik 1 Buket Akinci 2 Saime Nilay Arman 3 1 Assoc.Prof, PT, PhD, Istanbul University, Faculty of Health
Glenohumeral Joint Instability. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ
 1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
Anterior shoulder instability: Evaluation using MR arthrography.
 Anterior shoulder instability: Evaluation using MR arthrography. Poster No.: C-2407 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Lord, I. Katsimilis, N. Purohit, V. T. Skiadas; Southampton/UK
Anterior shoulder instability: Evaluation using MR arthrography. Poster No.: C-2407 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Lord, I. Katsimilis, N. Purohit, V. T. Skiadas; Southampton/UK
Acute Versus Delayed Magnetic Resonance Imaging and Associated Abnormalities in Traumatic Anterior Shoulder Dislocations
 Original Research Acute Versus Delayed Magnetic Resonance Imaging and Associated Abnormalities in Traumatic Anterior Shoulder Dislocations Nathan D. Orvets,* MD, Robert L. Parisien,* MD, Emily J. Curry,*
Original Research Acute Versus Delayed Magnetic Resonance Imaging and Associated Abnormalities in Traumatic Anterior Shoulder Dislocations Nathan D. Orvets,* MD, Robert L. Parisien,* MD, Emily J. Curry,*
The Athlete s Shoulder
 The Athlete s Shoulder Lennard Funk lenfunk@shoulderdoc.co.uk Decision Making NORMATIVE evidence base COGNITIVE environmental PSYCHOLOGICAL individual needs, bias, preferences, values Three P s 1. Major
The Athlete s Shoulder Lennard Funk lenfunk@shoulderdoc.co.uk Decision Making NORMATIVE evidence base COGNITIVE environmental PSYCHOLOGICAL individual needs, bias, preferences, values Three P s 1. Major
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
HAGL lesion of the shoulder
 HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Anatomy GH Joint. Glenohumeral Instability. Components of Stability. Components of Stability 7/7/2017. AllinaHealthSystem
 Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Current Concepts in the Diagnosis and Management of Traumatic, Anterior Glenohumeral Subluxations
 Review Current Concepts in the Diagnosis and Management of Traumatic, Anterior Glenohumeral Subluxations Joseph A. Gil,* MD, Steven DeFroda,* MD, and Brett D. Owens,* MD Investigation performed at the
Review Current Concepts in the Diagnosis and Management of Traumatic, Anterior Glenohumeral Subluxations Joseph A. Gil,* MD, Steven DeFroda,* MD, and Brett D. Owens,* MD Investigation performed at the
Arthroscopic Treatment of the First Anterior Shoulder Dislocation in Young Skiers
 Journal of ASTM International, March 2006, Vol. 3, No. 3 Paper ID JAI14199 Available online at www.astm.org Christos K. Yiannakopoulos, 1 Athanassios N. Zacharopoulos, 2 and Emmanuel Antonogiannakis 1
Journal of ASTM International, March 2006, Vol. 3, No. 3 Paper ID JAI14199 Available online at www.astm.org Christos K. Yiannakopoulos, 1 Athanassios N. Zacharopoulos, 2 and Emmanuel Antonogiannakis 1
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury.
 Biomedical Research 2017; 28 (19): 8295-8299 ISSN 0970-938X www.biomedres.info Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury. Zonghao
Biomedical Research 2017; 28 (19): 8295-8299 ISSN 0970-938X www.biomedres.info Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury. Zonghao
Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder
 Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder WWW.FISIOKINESITERAPIA.BIZ Overview To be able to quickly categorize shoulder injuries To take appropriate history and conduct
Acute Orthopaedic Injuries Developing a Diagnostic Approach to the Shoulder WWW.FISIOKINESITERAPIA.BIZ Overview To be able to quickly categorize shoulder injuries To take appropriate history and conduct
Objectives. Coracoid Fractures in Football: Evaluation and Management. Objectives. Introduction 5/8/2017
 Objectives Coracoid Fractures in Football: Evaluation and Management Discuss operative and non-operative management of coracoid fractures Chris Warrell, M.D. Orthopaedic Sports Medicine Fellow Andrews
Objectives Coracoid Fractures in Football: Evaluation and Management Discuss operative and non-operative management of coracoid fractures Chris Warrell, M.D. Orthopaedic Sports Medicine Fellow Andrews
My Disclosures. Engaging Hill- Sachs. Engaging Hill- Sachs. Non Engaging Hill-Sachs. Non Engaging Hill-Sachs 5/8/2014
 3-D Modeling of Humeral Head Defects: Jaicharan J. Iyengar, MD May 8, 2014 35 th Annual Inman Lectureship My Disclosures 1. Financial - None 2. Scientific - Peer Reviewer, Journal of Shoulder and Elbow
3-D Modeling of Humeral Head Defects: Jaicharan J. Iyengar, MD May 8, 2014 35 th Annual Inman Lectureship My Disclosures 1. Financial - None 2. Scientific - Peer Reviewer, Journal of Shoulder and Elbow
Incidence and Characteristics of Traumatic Shoulder Instability in Japanese Military Cadets
 MILITARY MEDICINE, 181, 6:577, 2016 Incidence and Characteristics of Traumatic Shoulder Instability in Japanese Military Cadets LTC Masatoshi Amako, MC JGSDF (Ret.)*; MAJ Hiroshi Sasao, MC JGSDF*; CPT
MILITARY MEDICINE, 181, 6:577, 2016 Incidence and Characteristics of Traumatic Shoulder Instability in Japanese Military Cadets LTC Masatoshi Amako, MC JGSDF (Ret.)*; MAJ Hiroshi Sasao, MC JGSDF*; CPT
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
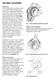 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
P.O. Box Sierra Park Road Mammoth Lakes, CA Orthopedic Surgery & Sports Medicine
 P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
Page 1. Shoulder Injuries in Sports.
 www.schulterteam.ch Shoulder Injuries in Sports Matthias A Zumstein Shoulder, Elbow and Orthopaedic Sports Medicine Department of Orthopedic Surgery and Traumatology University of Berne, Switzerland matthias.zumstein@insel.ch
www.schulterteam.ch Shoulder Injuries in Sports Matthias A Zumstein Shoulder, Elbow and Orthopaedic Sports Medicine Department of Orthopedic Surgery and Traumatology University of Berne, Switzerland matthias.zumstein@insel.ch
SLAP Lesions Assessment & Treatment
 SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
MRI of the Shoulder What to look for and how to find it? Dr. Eric Handley Musculoskeletal Radiologist Cherry Creek Imaging
 MRI of the Shoulder What to look for and how to find it? Dr. Eric Handley Musculoskeletal Radiologist Cherry Creek Imaging MRI of the Shoulder Benefits of Ultrasound: * Dynamic * Interactive real time
MRI of the Shoulder What to look for and how to find it? Dr. Eric Handley Musculoskeletal Radiologist Cherry Creek Imaging MRI of the Shoulder Benefits of Ultrasound: * Dynamic * Interactive real time
DK7215-Levine-ch12_R2_211106
 12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
Christopher A Brown, MD Sports Medicine Orthopedist. Duke Orthopedic Residency Sports Medicine Fellowship Stanford
 Christopher A Brown, MD Sports Medicine Orthopedist Duke Orthopedic Residency Sports Medicine Fellowship Stanford Office Geneva Newark Opening Canandaigua and Penfield Topics Of Discussion Shoulder dislocation
Christopher A Brown, MD Sports Medicine Orthopedist Duke Orthopedic Residency Sports Medicine Fellowship Stanford Office Geneva Newark Opening Canandaigua and Penfield Topics Of Discussion Shoulder dislocation
GOAL. Open Bankart: Why and How? 2/16/2017. Richard J. Hawkins, MD. Convince You That Open Bankart should be in our toolbox
 Current Solutions in Shoulder & Elbow Surgery Tampa, Florida February 9 12, 2017 Open Bankart: Why and How? Richard J. Hawkins, MD Steadman Hawkins Clinic of the Carolinas Hawkins Foundation Greenville,
Current Solutions in Shoulder & Elbow Surgery Tampa, Florida February 9 12, 2017 Open Bankart: Why and How? Richard J. Hawkins, MD Steadman Hawkins Clinic of the Carolinas Hawkins Foundation Greenville,
Introduction & Question 1
 Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
MRI of Shoulder Instabilities
 MRI of Shoulder Instabilities Anna Hirschmann, MD Musculoskeletal Division Clinic of Radiology and Nuclear Medicine University of Basel Hospital Glenohumeral Articulation Centering of the humeral head
MRI of Shoulder Instabilities Anna Hirschmann, MD Musculoskeletal Division Clinic of Radiology and Nuclear Medicine University of Basel Hospital Glenohumeral Articulation Centering of the humeral head
Posterior Shoulder Instability
 Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
Football and netball season A review of the apophysis and the acute shoulder: assessment. Simon Locke Sport and Exercise Physician
 Football and netball season A review of the apophysis and the acute shoulder: assessment Simon Locke Sport and Exercise Physician Apophyseal injuries; How to diagnose and manage? Goals for tonight Recognise
Football and netball season A review of the apophysis and the acute shoulder: assessment Simon Locke Sport and Exercise Physician Apophyseal injuries; How to diagnose and manage? Goals for tonight Recognise
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
A modification of Bristow Latarjet procedure and results at 2 years follow-up
 2017; 1(3): 26-30 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(3): 26-30 Received: 06-08-2017 Accepted: 07-09-2017 Dr. Raja Shekhar K Assistant Professor,
2017; 1(3): 26-30 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(3): 26-30 Received: 06-08-2017 Accepted: 07-09-2017 Dr. Raja Shekhar K Assistant Professor,
The shoulder joint is the most frequently dislocated
 Primary Repair Versus Conservative Treatment of First-Time Traumatic Anterior Dislocation of the Shoulder: A Randomized Study With 10-Year Follow-up Bent Wulff Jakobsen, M.D., Hans Viggo Johannsen, M.D.,
Primary Repair Versus Conservative Treatment of First-Time Traumatic Anterior Dislocation of the Shoulder: A Randomized Study With 10-Year Follow-up Bent Wulff Jakobsen, M.D., Hans Viggo Johannsen, M.D.,
Learning Curve of Arthroscopic Anatomic Glenoid Reconstruction: Comparison to the Arthroscopic Bristow Latarjet
 Learning Curve of Arthroscopic Anatomic Glenoid Reconstruction: Comparison to the Arthroscopic Bristow Latarjet Iustin Moga MD George Konstantinidis MD, PhD Cathy Coady MD, FRCS(C) Ivan Wong MD, FRCS(C)
Learning Curve of Arthroscopic Anatomic Glenoid Reconstruction: Comparison to the Arthroscopic Bristow Latarjet Iustin Moga MD George Konstantinidis MD, PhD Cathy Coady MD, FRCS(C) Ivan Wong MD, FRCS(C)
Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report
 Case Reports in Orthopedics Volume 2012, Article ID 789418, 4 pages doi:10.1155/2012/789418 Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report Takeshi Kokubu,
Case Reports in Orthopedics Volume 2012, Article ID 789418, 4 pages doi:10.1155/2012/789418 Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report Takeshi Kokubu,
Shoulder Instability in the Contact Athlete - I do it arthroscopically Brian J. Cole, MD, MBA
 Shoulder Instability in the Contact Athlete - I do it arthroscopically Brian J. Cole, MD, MBA bcole@rushortho.com Key points: o Greater incidence of anterior shoulder instability in contact and collision
Shoulder Instability in the Contact Athlete - I do it arthroscopically Brian J. Cole, MD, MBA bcole@rushortho.com Key points: o Greater incidence of anterior shoulder instability in contact and collision
Fumiaki Takase, Atsuyuki Inui, Yutaka Mifune, Tomoyuki Muto, Yoshifumi Harada, Takeshi Kokubu, and Masahiro Kurosaka
 Case Reports in Orthopedics, Article ID 312968, 4 pages http://dx.doi.org/10.1155/2014/312968 Case Report Concurrent Rotator Cuff Tear and Axillary Nerve Palsy Associated with Anterior Dislocation of the
Case Reports in Orthopedics, Article ID 312968, 4 pages http://dx.doi.org/10.1155/2014/312968 Case Report Concurrent Rotator Cuff Tear and Axillary Nerve Palsy Associated with Anterior Dislocation of the
Outcome analysis of management of recurrent shoulder dislocation by latarjet procedure
 2018; 4(3): 82-86 ISSN: 2395-1958 IJOS 2018; 4(3): 82-86 2018 IJOS www.orthopaper.com Received: 17-05-2018 Accepted: 18-06-2018 Dr. AN Sarath Babu Senior Assistant Professor, Institute of Orthopaedics
2018; 4(3): 82-86 ISSN: 2395-1958 IJOS 2018; 4(3): 82-86 2018 IJOS www.orthopaper.com Received: 17-05-2018 Accepted: 18-06-2018 Dr. AN Sarath Babu Senior Assistant Professor, Institute of Orthopaedics
Revision Instability Repair
 Revision Instability Repair Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics
Revision Instability Repair Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics
Preface. Functional Anatomy and Biomechanics of Shoulder Stability in the Athlete 607
 Shoulder Instability in the Athlete Foreword Mark D. Miller xiii Preface Stephen R. Thompson xv Functional Anatomy and Biomechanics of Shoulder Stability in the Athlete 607 Iain R. Murray, Ewan B. Goudie,
Shoulder Instability in the Athlete Foreword Mark D. Miller xiii Preface Stephen R. Thompson xv Functional Anatomy and Biomechanics of Shoulder Stability in the Athlete 607 Iain R. Murray, Ewan B. Goudie,
Common Surgical Shoulder Injury Repairs
 Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Management of Massive/Revision Rotator Cuff Tears
 Management of Massive/Revision Rotator Cuff Tears Nikhil N. Verma MD, Director Sports Medicine, Rush University Medical Center, Midwest Orthopedics at Rush, Chicago, IL nverma@rushortho.com I. Anatomy
Management of Massive/Revision Rotator Cuff Tears Nikhil N. Verma MD, Director Sports Medicine, Rush University Medical Center, Midwest Orthopedics at Rush, Chicago, IL nverma@rushortho.com I. Anatomy
Recurrent Shoulder Dislocation.
 Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012
 Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
Osteochondral augmentation of glenoid bone loss distal tibia allograft
 Review Article Page 1 of 9 Osteochondral augmentation of glenoid bone loss distal tibia allograft Colin P. Murphy 1, Anthony Sanchez 1, Mitchell I. Kennedy 1, Rachel M. Frank 2, Matthew T. Provencher 1,3
Review Article Page 1 of 9 Osteochondral augmentation of glenoid bone loss distal tibia allograft Colin P. Murphy 1, Anthony Sanchez 1, Mitchell I. Kennedy 1, Rachel M. Frank 2, Matthew T. Provencher 1,3
The suction cup mechanism is enhanced by the slightly negative intra articular pressure within the joint.
 SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum
 Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Anterior Shoulder Instability
 Anterior Shoulder Instability Anterior shoulder instability typically results from a dislocation injury to the shoulder joint when the humeral head (ball) of the humerus (upper arm bone) is displaced from
Anterior Shoulder Instability Anterior shoulder instability typically results from a dislocation injury to the shoulder joint when the humeral head (ball) of the humerus (upper arm bone) is displaced from
Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
Introduction. Omid Reza Momenzadeh 1 Masoome Pourmokhtari. Amir Reza Vosoughi 1
 DOI 10.1007/s10195-015-0348-9 ORIGINAL ARTICLE Does the position of shoulder immobilization after reduced anterior glenohumeral dislocation affect coaptation of a Bankart lesion? An arthrographic comparison
DOI 10.1007/s10195-015-0348-9 ORIGINAL ARTICLE Does the position of shoulder immobilization after reduced anterior glenohumeral dislocation affect coaptation of a Bankart lesion? An arthrographic comparison
Hugo C. van der Veen James P. M. Collins Paul C. Rijk
 DOI 10.1007/s00402-011-1423-1 ARTHROSCOPY AND SPORTS MEDICINE Value of magnetic resonance arthrography in post-traumatic anterior shoulder instability prior to arthroscopy: a prospective evaluation of
DOI 10.1007/s00402-011-1423-1 ARTHROSCOPY AND SPORTS MEDICINE Value of magnetic resonance arthrography in post-traumatic anterior shoulder instability prior to arthroscopy: a prospective evaluation of
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Body Planes. (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal
 Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?)
 Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Acute traumatic posterior shoulder instability is
 Arthroscopic Treatment of a Reverse Hill-Sachs Lesion Richard E. Duey, M.D., and Stephen S. Burkhart, M.D. Abstract: Acute traumatic posterior shoulder instability is a rare injury. Such injuries can result
Arthroscopic Treatment of a Reverse Hill-Sachs Lesion Richard E. Duey, M.D., and Stephen S. Burkhart, M.D. Abstract: Acute traumatic posterior shoulder instability is a rare injury. Such injuries can result
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Study of bipolar bone defects in unstable shoulder: From "engaging / non-engaging" to "on-track / off-track".
 Study of bipolar bone defects in unstable shoulder: From "engaging / non-engaging" to "on-track / off-track". Poster No.: C-2219 Congress: ECR 2017 Type: Educational Exhibit Authors: E. Jose Salgado Ribeiro,
Study of bipolar bone defects in unstable shoulder: From "engaging / non-engaging" to "on-track / off-track". Poster No.: C-2219 Congress: ECR 2017 Type: Educational Exhibit Authors: E. Jose Salgado Ribeiro,
Chronic Shoulder Disorders
 Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Don t forget the open Bankart Look at the evidence
 Review Article Page 1 of 7 Don t forget the open Bankart Look at the evidence Luke Sanborn 1, Robert A. Arciero 2, Justin S. Yang 3 1 Drexel University College of Medicine, Philadelphia, USA; 2 Department
Review Article Page 1 of 7 Don t forget the open Bankart Look at the evidence Luke Sanborn 1, Robert A. Arciero 2, Justin S. Yang 3 1 Drexel University College of Medicine, Philadelphia, USA; 2 Department
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Shoulder Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Compiled by Rob Liddell,
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Shoulder Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Compiled by Rob Liddell,
Chronic Shoulder Instability
 Chronic Shoulder Instability The shoulder is the most moveable joint in your body. It helps you to lift your arm, to rotate it, and to reach up over your head. It is able to turn in many directions. This
Chronic Shoulder Instability The shoulder is the most moveable joint in your body. It helps you to lift your arm, to rotate it, and to reach up over your head. It is able to turn in many directions. This
Management of Humeral Bone Loss in Anterior Shoulder Instability. Scott D. Mair, MD University of Kentucky Sports Medicine
 Management of Humeral Bone Loss in Anterior Shoulder Instability Scott D. Mair, MD University of Kentucky Sports Medicine Disclosure Smith and Nephew Endoscopy fellowship support Importance Bone loss (glenoid
Management of Humeral Bone Loss in Anterior Shoulder Instability Scott D. Mair, MD University of Kentucky Sports Medicine Disclosure Smith and Nephew Endoscopy fellowship support Importance Bone loss (glenoid
A Patient s Guide to Shoulder Dislocations
 A Patient s Guide to Shoulder Dislocations 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Shoulder Dislocations 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE
 ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
Current Controversies in Shoulder Surgery:
 Current Controversies in Shoulder Surgery: Shoulder Instability Rotator Cuff Injury and Repair Reverse Shoulder Arthroplasty Brian Feeley, MD UC San Francisco Sports Medicine and Shoulder Surgery Disclosures
Current Controversies in Shoulder Surgery: Shoulder Instability Rotator Cuff Injury and Repair Reverse Shoulder Arthroplasty Brian Feeley, MD UC San Francisco Sports Medicine and Shoulder Surgery Disclosures
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
