Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D.
|
|
|
- Tracy Townsend
- 6 years ago
- Views:
Transcription
1 Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion of any joint in the body and as a result is particularly susceptible to dislocation and subluxation. Recurrent instability is a common complication after traumatic shoulder dislocation in young people, with rates as high as 100% in skeletally immature patients and 96% in for adolescents. Treatment for shoulder dislocation has traditionally involved immobilization followed by a rehabilitation program. Recent studies have reported decreased rates of recurrent instability and improved outcomes in patients treated with surgical stabilization of acute, traumatic shoulder dislocation. The purpose of this review is to review recent publications concerning the treatment of traumatic shoulder dislocations in adolescents. Recent findings Lawton et al. retrospectively reviewed 70 shoulders in 66 patients 16 years old or younger treated for shoulder instability with follow-up more than 2 years. Forty-two shoulders were successfully treated with physical therapy, whereas 28 eventually required surgery. Subsequently, Deitch et al. retrospectively identified 32 patients between 11 and 18 years of age with radiographically documented traumatic anterior shoulder dislocation. Instability recurred in 75% of patients and 50% eventually required surgical stabilization. Bottoni et al. reported results of a prospective randomized trial comparing arthroscopic stabilization to nonoperative treatment of acute, traumatic shoulder dislocations in patients aged 18 to 26 years. Recurrent instability developed in 75% of patients treated conservatively versus 11% in those treated with surgery. DeBerardino et al. prospectively evaluated arthroscopic stabilization of acute shoulder dislocations in 48 young athletes with an average follow-up of 37 months and reported a 12% rate of recurrent instability. All patients with stable shoulders were able to return to their previous levels of activity. Summary Conservative management of traumatic shoulder dislocations in young patients is associated with high rates of recurrent instability. Recent studies have demonstrated improved results and significant reduction in recurrent instability in patients treated with surgical stabilization when compared with nonoperative treatment. Keywords shoulder dislocation, adolescent athletes, surgical stabilization, arthroscopy Curr Opin Pediatr 17: Lippincott Williams & Wilkins. Sports Medicine/Shoulder Service, Hospital for Special Surgery, New York, New York, USA Correspondence to John D. MacGillivray, MD, Sports Medicine/Shoulder Service, Hospital for Special Surgery, 535 East 70th Street, New York, NY 10021, USA Tel: ; fax: ; macgillivrayj@hss.edu Current Opinion in Pediatrics 2005, 17: Lippincott Williams & Wilkins Introduction The glenohumeral joint is a ball and socket joint with three degrees of freedom of motion. Because of this great range of motion, the shoulder is susceptible to dislocation and subluxation in the setting of trauma and high demand sporting activities. Most studies involving shoulder dislocation in children have reported this injury to be very rare. Shoulder trauma in the skeletally immature child more commonly results in fracture through the proximal humeral physis rather than shoulder dislocation [5,6]. Adolescents, however, are much more commonly affected by instability after similar traumatic episodes. This recurrent instability and dislocation may lead to permanent articular damage and long-term shoulder joint degeneration. Historical treatment has consisted of immobilization followed by a period of rehabilitation; however, recent data suggest that surgical stabilization or acute shoulder dislocations may be more beneficial for some patients. Anatomy The shoulder consists of three bones and four joints. The glenohumeral joint is the ball and socket joint in which the humeral head articulates with the glenoid cavity. The glenoid cavity is a widening of the lateral scapula and is surrounded by a fibrocartilaginous ring called the labrum. This labrum acts to anchor the glenoid to the humeral head as well as to deepen the socket of the shoulder joint. The glenohumeral joint is stabilized by static restraints including the labrum, ligaments, and joint capsule, as well as by dynamic restraints including the rotator cuff muscles and scapular stabilizers. Shoulder dislocation Dislocation of the glenohumeral joint is a complete disassociation between the glenoid cavity and the humeral 25
2 26 Orthopedics head. The separation is commonly observed after a traumatic event and usually requires manipulation to reduce the humeral head back into the glenoid. Subluxation, on the other hand, involves instability and translation across the glenohumeral joint without complete dislocation. Instability may involve the humeral head traveling in an anterior, posterior, or inferior direction in relation to the glenoid cavity. Instability may also occur in multiple directions within the same patient and has been associated with generalized joint laxity in young patients [7]. Shoulder dislocation may or may not occur in the setting of trauma. Traumatic dislocations occur with an acute onset and an appropriate mechanism of injury is present. Conversely, atraumatic dislocations may present with a questionable onset and may lack an appropriate mechanism of injury. Atraumatic dislocations are seen in patients with multidirectional instability and ligamentous laxity, and the presence of these factors should be recognized to maximize further treatment. Traumatic anterior dislocation Anterior dislocation represents more than 90% of traumatic dislocations. These injuries are commonly seen in adolescents participating in contact sports. The dislocation occurs after a high-energy injury, commonly involving a fall on the outstretched hand. This mechanism of injury abducts and externally rotates the shoulder, pushing the humeral head out the front of the glenoid cavity, with resultant injury to the anterior glenohumeral ligaments. The anteriorly dislocating humeral head and joint capsule may tear the labrum from the rim of the glenoid as it dislocates, and this common injury is termed a Bankart lesion (Fig. 1). After the dislocation, the posterior humeral head is snapped back against the anterior glenoid rim. This impaction may lead to a fracture on the Figure 1. Arthroscopic photograph of a Bankart lesion Arthroscopic photograph of a Bankart lesion demonstrating the separation of the glenoid labrum (right) from the rim of the glenoid cavity. posterior superior humeral head (called a Hill-Sachs lesion) and may be visible on plain radiographs. Traumatic posterior dislocation Traumatic posterior shoulder dislocation is an uncommon injury representing less than 5% of all traumatic shoulder dislocations [8,9]. Most cases of posterior dislocation in young patients are associated with multidirectional instability. Few statistics are available for children and adolescents, but some authors have estimated the incidence of posterior dislocations to be nearer to 10% in this group because of the increased ligamentous laxity associated with youth. Posterior dislocation may occur as the result of a fall on the outstretched hand with the shoulder in adduction and internal rotation, which may force the humeral head out the back of the glenoid cavity. Posterior dislocations may also result from a direct anterior blow to the shoulder, which pushes the humeral head posteriorly out of the glenoid. Finally, it is important to remember that posterior dislocations may occur as the result of an electrical shock or seizure. The mechanism of dislocation in these cases is sustained contraction of the internal rotator musculature, which may lever the humeral head out of the glenoid cavity posteriorly. Clinical evaluation Patients with traumatic shoulder dislocation often present with obvious deformity and pain with range of motion. The humeral head may be visible with an obvious deformity. The acromion may be prominent with a cavity inferiorly where the humeral head usually sits. Patients commonly present with the arm internally rotated and supported by their other hand. Initial evaluation should also include a careful neurovascular examination. Radial and ulnar pulses should be documented in addition to individual nerve testing. The axillary nerve is the most commonly injured structure and has been reported in 5 to 35% of traumatic anterior shoulder dislocations. Radiographic evaluation Plain radiographs are the best routine imaging studies for the evaluation of acute shoulder dislocation and should include three specific views: the anteroposterior view, axillary view, and scapular Y view. These views allow the location of the humeral head to be visualized in threedimensional space in relation to the glenoid cavity. Single anteroposterior views and oblique views are commonly obtained secondary to patient discomfort, but are not sufficient to determine the location and nature of dislocation and should never be accepted. These same three views should also be obtained to confirm shoulder reduction after manipulation. Postreduction views commonly reveal the posterolateral humeral head impaction fracture (or Hill-Sachs lesion) mentioned earlier. Although of little use in the emergency room, MRI scans have the ability to provide very specific details regarding soft tissue injuries after shoulder dislocation. MRI is the modality of choice for evaluating capsular and labral in-
3 Shoulder dislocation in teen athlete Good and MacGillivray 27 jures including the previously described Bankart lesion (Fig. 2). MRI also allows visualization of the ligaments and muscles responsible for shoulder stabilization and motion. The anatomic detail provided by an MRI scan provides much information in regard to surgical planning and rehabilitation. Initial management of shoulder dislocation After physical examination and standard radiography, closed reduction is the initial treatment for shoulder dislocation. A number of effective techniques have been described, and the reduction of an acute shoulder dislocation can commonly be accomplished without the use of anesthesia. Shoulders that have been dislocated for a number of hours or patients experiencing significant pain and muscle spasm may require anesthesia, including intraarticular injection and intravenous sedation. Once reduction is achieved, repeat neurologic examination and postreduction radiographs must be performed. After reduction, the shoulder is immobilized in a sling for protection. Nonoperative management after shoulder dislocation Patients with acute, traumatic shoulder dislocation have traditionally been treated with conservative means, including a brief period of immobilization followed by a rehabilitation program with a delayed return to full activities. The duration of immobilization and the type and length of rehabilitation after shoulder dislocation are Figure 2. Arthroscopic photograph of a Bankart lesionmri of the shoulder revealing the presence of a bony Bankart lesion (arrow) This bony avulsion fracture is created as the anteriorly dislocating humeral head and joint capsule tear the labrum from the rim of the glenoid. controversial. As has previously been stated, recurrent dislocation is the most common complication after traumatic shoulder dislocation. Rehabilitation after immobilization includes muscle strengthening including the rotator cuff, deltoid, and shoulder stabilizers. Historical studies Historically, a large number of studies examining shoulder instability have been conducted; however, details specific to children and adolescents have been sparse. In 1956, Rowe et al. [10,11] published a review of 500 shoulder dislocations. Of these patients, only eight patients were younger than 10 years old, whereas 99 were between the ages of 10 and 20. Rowe reported a recurrence rate of 100% in patients younger than 10 and a 94% recurrence rate in patients between 10 and 20 years of age. More recent studies have focused on the younger population in particular. In 1983, Wagner et al. [12] presented the first series with data specific to shoulder dislocation in children, taken from a large series of traumatic anterior shoulder dislocations. Nine cases of dislocation reportedly occurred in children with open physes (4.7% incidence); all of them were treated with immobilization and physical therapy. Among these nine patients, a recurrence rate of 80% was reported, with all recurrences requiring operative intervention. In 1992, Marans et al. [13] reviewed the outcomes of 21 patients with traumatic anterior shoulder dislocation treated with sling and swathe immobilization and reported a recurrence rate of 100%. Hovelius et al. [14,15] have also published 2, 5, and 10-year follow-up data for patients between 12 and 40 years of age after anterior shoulder dislocation. Seventy percent of patients from 12 to 16 years old had recurrent dislocations at the time of final follow-up (this includes patients treated with conservative therapy and those treated with surgery). Recent publications addressing incidence and recurrence Recent data have also supported the high rates of shoulder instability reported after traumatic shoulder dislocation in children and adolescents. Lawton et al. [2] retrospectively reviewed 70 shoulders in 66 patients 16 years old or younger with a history of shoulder instability. They associated trauma with the initial episode of instability in 86% of patients, with 50% of patients actually experiencing a dislocation with this primary event. Instability was associated with male sex, adolescence, and a history of trauma. Sixty-seven percent of patients were treated with therapy and 40% eventually underwent surgery. At more than 2-year follow-up, 70% described their shoulders as better and 90% were performing at preinjury levels at sports and work. Surgically treated patients were less likely to have recurrent stability or report limitations, and factor analysis found that older boys with traumatic onset, no history of voluntary instability, and who were
4 28 Orthopedics treated surgically did better than patients with other factors. Deitch et al. [5] recently reported on 32 patients from 8 to 11 years of age with radiographically documented anterior shoulder dislocation. Follow-up at an average of 4 years via telephone revealed that 23 (71%) experienced at least one episode of recurrence and 16 were treated with surgery for recurrent dislocation. Outcomes analysis performed with the data from these interviews found no significant differences in outcomes between patients treated nonoperatively compared with those who underwent surgical stabilization. Surgical treatment A number of surgical alternatives have been investigated for the treatment of acute traumatic shoulder dislocation in young patients [1,2 4,16,17,18]. Operative management may consist of formal open surgery, arthroscopic surgery, or arthroscopically assisted open surgery. Arthroscopic findings have documented the presence of hemarthrosis and Bankart repair after acute traumatic anterior shoulder dislocation. Repair of a Bankart lesion is of paramount importance when surgically addressing traumatic anterior shoulder instability. Formal open repair has been the gold standard for performing this repair and is commonly carried out via an incision lying in the axillary crease lateral to the coracoid process. Arthroscopic repair has previously been associated with higher rates of postoperative stability, but the use of newer techniques, sutures, and anchors has produced promising results. In addition, the presence of hemarthrosis in the setting of the healing response may provide a favorable setting in which to perform arthroscopic stabilization. Recent publications concerning surgery In 2000, Bottoni et al. [3] published a prospective randomized evaluation of arthroscopic stabilization versus nonoperative treatment in patients with acute, traumatic first-time shoulder dislocations. This study included 24 US active duty military personnel between 18 and 26 years of age. Patients were randomized to nonoperative management consisting of 4 weeks immobilization followed by physical therapy versus arthroscopic stabilization using a bioabsorbable tack. At average follow-up of 36 months, the recurrence rate in the nonoperative group was 75% versus 11% in the surgical group. The data supporting arthroscopic stabilization is also supported by the work of DeBerardino et al. in 2001 [4], who performed a prospective evaluation of arthroscopic stabilization for treatment of acute, initial shoulder dislocations in young athletes at the US military academy. Forty-nine patients were treated with arthroscopic stabilization using bioabsorbable tacks. Eighty-eight shoulders were found to remain stable after stabilization with all of these patients returning to their preinjury level of functioning at 5-year follow-up. Outcomes assessment performed at follow-up revealed significantly better results than patients treated nonoperatively. Additional support was recently published by Swung-Ho et al. [17 ], who published results evaluating arthroscopic Bankart repair with suture anchors and nonabsorbable sutures in 167 patients with a mean age of 25 years. All shoulder scores improved significantly after surgery, and the incidence of postoperative instability was only 4% at mean follow-up of 44 months. Conclusion Patients with acute, traumatic shoulder dislocation have traditionally been treated with conservative therapy including immobilization, therapy, and restricted activities. The most common complication of nonoperative therapy after traumatic shoulder dislocation is recurrent instability. This is a particular concern in the adolescent and pediatric population because the single greatest prognostic factor determining rate of recurrence is patient age at time of initial injury. Recent studies have shown rates of recurrence to be between 70 and 100% in the adolescent population, with a great number of patients eventually requiring surgery for unacceptable instability. The patients at greatest risk of recurrence are commonly males with a history of traumatic dislocations who are involved in high demand sporting activities. Recent studies have shown that in this patient population, acute, primary arthroscopic stabilization is an effective treatment that may decrease recurrence rates, rehabilitation time, and improve overall outcomes. It is currently our practice to offer acute stabilization to young athletes after acute traumatic shoulder dislocation. Further followup data are necessary to compare results of open stabilization to that performed arthroscopically and to better predict which patients will succeed with different surgical techniques. References and recommended reading Papers of particular interest, published within the annual period of review, have been highlighted as: Of special interest Of outstanding interest 1 Deitch J, Mehlman CT, Foad SL, et al. Traumatic anterior shoulder dislocation in adolescents. Am J Sports Med 2003; 31: A retrospective cohort study documenting instability rates and functional outcome in adolescents after dislocation. 2 Lawton RL, Choudhury S, Mansat P, et al. Pediatric shoulder instability: presentation, findings, treatment, and outcomes. J Pediatr Orthop 2002; 22: Bottoni CR, Wilckens JH, DeBardino TM, et al. A prospective, randomized evaluation of arthroscopic stabilization versus nonoperative treatment in patients with acute, traumatic, first-time shoulder dislocations. Am J Sports Med 2000; 30: DeBerardino TM, Arciero RA, Taylor DC, et al. Prospective evaluation of arthroscopic stabilization of acute, initial anterior shoulder dislocations in young athletes. Am J Sports Med 2001; 29:
5 Shoulder dislocation in teen athlete Good and MacGillivray 29 5 Dameron TB, Reibel DB: Fractures involving the proximal humeral epiphyseal plate. J Bone Joint Surg 1969; 51: Gregg-Smith SJ, White SH: Salter-Harris III fracture-dislocation of the proximal humeral epiphysis. Injury 1992; 23: Mallon WJ, Speer KP: Multidirectional instability: current concepts. J Shoulder Elbow Surg 1995; 4: Boyd HB, Sisk TD: Recurrent posterior dislocation of the shoulder. J Bone Joint Surg 1972; 54A: Kawam M, Sinclair J, Letts M: Recurrent posterior shoulder dislocation in children: the results of surgical management. J Pediatr Orthop 1997; 17: Rowe C: Prognosis in dislocation of the shoulder. J Bone Joint Surg [Am] 1956; 38: Rowe C, Sakellarides H: Factors related to recurrences of anterior dislocations of the shoulder. Clin Orthop 1961; 20: Wagner KT, Lyne ED: Adolescent traumatic dislocations of the shoulder with open epiphyses. J Pediatr Orthop 1983; 3: Marans HJ, Angel KR, Schemitsch EH, Wedge JH: The fate of traumatic anterior dislocation of the shoulder in children. J Bone Joint Surg 1992; 74A: Hovelius L: Gavle: anterior dislocation of the shoulder in teen-agers and young adults. J Bone Joint Surg 1987; 69A: Hovelius L: The natural history of primary anterior dislocation of the shoulder in the young. J Orthop Sci 1999; 4: Pagnani MJ, Dome DC: Surgical treatment of traumatic anterior shoulder instability in American football players. J Bone Joint Surg 2002; 84A: Seung-Ho K, Kwon-Ick H, Yang-Bum C, et al. Arthroscopic anterior stabilization of the shoulder. J Bone Joint Surg 85A: A report demonstrating satisfactory outcomes after arthroscopic stabilization with suture anchors. 18 Warner JJP, Warren RF: Arthroscopic Bankart repair using a cannulated, absorbable fixation device. Oper Tech Orthop 1991; 1:
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai
 POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Anterior Shoulder Instability
 Anterior Shoulder Instability Anterior shoulder instability typically results from a dislocation injury to the shoulder joint when the humeral head (ball) of the humerus (upper arm bone) is displaced from
Anterior Shoulder Instability Anterior shoulder instability typically results from a dislocation injury to the shoulder joint when the humeral head (ball) of the humerus (upper arm bone) is displaced from
Glenohumeral Joint Instability: An Athlete s Perspective
 Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Patient ID. Case Conference. Physical Examination. Image examination. Treatment 2011/6/16
 Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Disclosure. Traumatic Anterior Shoulder Instability 7/23/2018. Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist
 Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist Christopher E. Baker M.D. Sports Medicine Shoulder Reconstruction Traumatic Anterior Shoulder Instability Disclosure Speaking/Consulting
Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist Christopher E. Baker M.D. Sports Medicine Shoulder Reconstruction Traumatic Anterior Shoulder Instability Disclosure Speaking/Consulting
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Shoulder Instability
 J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The suction cup mechanism is enhanced by the slightly negative intra articular pressure within the joint.
 SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Management of Anterior Shoulder Instability
 Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Recurrent Shoulder Dislocation.
 Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Anatomy GH Joint. Glenohumeral Instability. Components of Stability. Components of Stability 7/7/2017. AllinaHealthSystem
 Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Shoulder Trauma (Fractures and Dislocations)
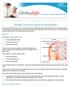 Shoulder Trauma (Fractures and Dislocations) Trauma to the shoulder is common. Injuries range from a separated shoulder resulting from a fall onto the shoulder to a high-speed car accident that fractures
Shoulder Trauma (Fractures and Dislocations) Trauma to the shoulder is common. Injuries range from a separated shoulder resulting from a fall onto the shoulder to a high-speed car accident that fractures
 www.fisiokinesiterapia.biz Shoulder Problems Fractures Instability Impingement Miscellaneous Anatomy Bones Joints / Ligaments Muscles Neurovascular Anatomy Anatomy Supraspinatus Anterior Posterior Anatomy
www.fisiokinesiterapia.biz Shoulder Problems Fractures Instability Impingement Miscellaneous Anatomy Bones Joints / Ligaments Muscles Neurovascular Anatomy Anatomy Supraspinatus Anterior Posterior Anatomy
DK7215-Levine-ch12_R2_211106
 12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
First-Time Anterior Shoulder Dislocation: Is it time to take a stand?
 Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
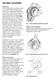 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Latarjet Procedure (coracoid transfer) Shoulder Stabilisation Surgery Ms. Ruth Delaney Consultant Orthopaedic Surgeon
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Latarjet Procedure (coracoid transfer) Shoulder Stabilisation Surgery Ms. Ruth Delaney Consultant Orthopaedic Surgeon
The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior Shoulder Instability
 Original Article DOI 10.3349/ymj.2010.51.3.421 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 421-426, 2010 The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior
Original Article DOI 10.3349/ymj.2010.51.3.421 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 421-426, 2010 The Spectrum of Lesions and Clinical Results of Arthroscopic Stabilization of Acute Anterior
My shoulder popped out what now?
 My shoulder popped out what now? Richard Dallalana Epworth Shoulder Symposium June 2017 Shoulder Dislocation First event Best approach? Manual Reduction Should it be put back on field? - YES Prone lying
My shoulder popped out what now? Richard Dallalana Epworth Shoulder Symposium June 2017 Shoulder Dislocation First event Best approach? Manual Reduction Should it be put back on field? - YES Prone lying
Glenohumeral Joint Instability. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ
 1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012
 Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
Posterior Shoulder Instability
 Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
P.O. Box Sierra Park Road Mammoth Lakes, CA Orthopedic Surgery & Sports Medicine
 P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
The Shoulder Complex. Anatomy. Articulations 12/11/2017. Oak Ridge High School Conroe, Texas. Clavicle Collar Bone Scapula Shoulder Blade Humerus
 The Shoulder Complex Oak Ridge High School Conroe, Texas Anatomy Clavicle Collar Bone Scapula Shoulder Blade Humerus Articulations Sternoclavicular SC joint. Sternum and Clavicle. Acromioclavicular AC
The Shoulder Complex Oak Ridge High School Conroe, Texas Anatomy Clavicle Collar Bone Scapula Shoulder Blade Humerus Articulations Sternoclavicular SC joint. Sternum and Clavicle. Acromioclavicular AC
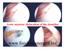 Acute anterior dislocation of the shoulder www.fisiokinesiterapia.biz Anatomy Stability: - ball & socket = compression in concavity effect Bone - big head small cup = unstable Menisci - labium = depth
Acute anterior dislocation of the shoulder www.fisiokinesiterapia.biz Anatomy Stability: - ball & socket = compression in concavity effect Bone - big head small cup = unstable Menisci - labium = depth
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
SHOULDER JOINT ANATOMY AND KINESIOLOGY
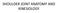 SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
Surgical versus conservative treatment for acute first-time anterior shoulder dislocation: the evidence
 J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
J Orthopaed Traumatol (2007) 8:207 213 DOI 10.1007/s10195-007-0095-7 EVIDENCE-BASED MEDICINE SECTION R. Padua R. Bondì L. Bondì A. Campi Surgical versus conservative treatment for acute first-time anterior
Common Surgical Shoulder Injury Repairs
 Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Sports Medicine: Shoulder Arthrography. Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System
 Sports Medicine: Shoulder Arthrography Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Disclosure Off-label use for gadolinium Pediatric Sports Injuries
Sports Medicine: Shoulder Arthrography Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Disclosure Off-label use for gadolinium Pediatric Sports Injuries
Arthroscopic Treatment of the First Anterior Shoulder Dislocation in Young Skiers
 Journal of ASTM International, March 2006, Vol. 3, No. 3 Paper ID JAI14199 Available online at www.astm.org Christos K. Yiannakopoulos, 1 Athanassios N. Zacharopoulos, 2 and Emmanuel Antonogiannakis 1
Journal of ASTM International, March 2006, Vol. 3, No. 3 Paper ID JAI14199 Available online at www.astm.org Christos K. Yiannakopoulos, 1 Athanassios N. Zacharopoulos, 2 and Emmanuel Antonogiannakis 1
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum
 Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years
 Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years Elisabeth C. Robinson,* MD, Vijay B. Thangamani, MD, Michael A. Kuhn, MD, and Glen Ross, MD Investigation performed
Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years Elisabeth C. Robinson,* MD, Vijay B. Thangamani, MD, Michael A. Kuhn, MD, and Glen Ross, MD Investigation performed
Football and netball season A review of the apophysis and the acute shoulder: assessment. Simon Locke Sport and Exercise Physician
 Football and netball season A review of the apophysis and the acute shoulder: assessment Simon Locke Sport and Exercise Physician Apophyseal injuries; How to diagnose and manage? Goals for tonight Recognise
Football and netball season A review of the apophysis and the acute shoulder: assessment Simon Locke Sport and Exercise Physician Apophyseal injuries; How to diagnose and manage? Goals for tonight Recognise
Shoulder Arthroscopy. Dr. J.J.A.M. van Raaij. NOV Jaarvergadering Den Bosch 25 jan 2018
 Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
Shoulder Instability and Tendon Injuries
 Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM
 RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?)
 Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
A Patient s Guide to Shoulder Dislocations
 A Patient s Guide to Shoulder Dislocations 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Shoulder Dislocations 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
Shoulder Injuries. Glenoid labrum injuries. SLAP Lesions
 Shoulder Injuries functional anatomy clinical perspective impingement rotator cuff injuries glenoid labrum injuries dislocation Glenoid labrum injuries SLAP lesions stable or unstable traction/compression
Shoulder Injuries functional anatomy clinical perspective impingement rotator cuff injuries glenoid labrum injuries dislocation Glenoid labrum injuries SLAP lesions stable or unstable traction/compression
The ball-and-socket articulation at the glenohumeral joint is between the convex
 SLAP Lesion Repair Emily Cotey, Emily Hurysz, and Patrick Schroeder Abstract SLAP lesion, which stands for Superior Labrum Anterior and Posterior, is a detachment tear of the superior labrum that originates
SLAP Lesion Repair Emily Cotey, Emily Hurysz, and Patrick Schroeder Abstract SLAP lesion, which stands for Superior Labrum Anterior and Posterior, is a detachment tear of the superior labrum that originates
HAGL lesion of the shoulder
 HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
SHOULDER INSTABILITY
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of Shoulder Instability must be made in conjunction with your
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of Shoulder Instability must be made in conjunction with your
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Introduction & Question 1
 Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Chronic Shoulder Instability
 Chronic Shoulder Instability The shoulder is the most moveable joint in your body. It helps you to lift your arm, to rotate it, and to reach up over your head. It is able to turn in many directions. This
Chronic Shoulder Instability The shoulder is the most moveable joint in your body. It helps you to lift your arm, to rotate it, and to reach up over your head. It is able to turn in many directions. This
Throwing Injuries and Prevention: The Physical Therapy Perspective
 Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Shoulder Instability and Stabilisation
 Shoulder Instability and Stabilisation The benefit of the huge range of movements at the shoulder is that we are able to position the hand as required, the cost is that the shoulder is more likely to dislocate
Shoulder Instability and Stabilisation The benefit of the huge range of movements at the shoulder is that we are able to position the hand as required, the cost is that the shoulder is more likely to dislocate
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
R. Frank Henn III, MD. Associate Professor Chief of Sports Medicine Residency Program Director
 R. Frank Henn III, MD Associate Professor Chief of Sports Medicine Residency Program Director Disclosures No financial relationships to disclose 1. Labral anatomy 2. Adaptations of the throwing shoulder
R. Frank Henn III, MD Associate Professor Chief of Sports Medicine Residency Program Director Disclosures No financial relationships to disclose 1. Labral anatomy 2. Adaptations of the throwing shoulder
Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury.
 Biomedical Research 2017; 28 (19): 8295-8299 ISSN 0970-938X www.biomedres.info Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury. Zonghao
Biomedical Research 2017; 28 (19): 8295-8299 ISSN 0970-938X www.biomedres.info Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury. Zonghao
From the Sports Medicine Section, Orthopaedic Surgery Service, Tripler Army Medical Center, Honolulu, Hawaii
 0363-5465/102/3030-0576$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 30, No. 4 A Prospective, Randomized Evaluation of Arthroscopic Stabilization Versus Nonoperative Treatment in Patients with
0363-5465/102/3030-0576$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 30, No. 4 A Prospective, Randomized Evaluation of Arthroscopic Stabilization Versus Nonoperative Treatment in Patients with
Anterior shoulder instability in weight lifters
 Anterior shoulder instability in weight lifters MICHAEL L. GROSS,* MD, STEPHEN L. BRENNER, MD, IRA ESFORMES, AND JOHN J. SONZOGNI, MD From Orthopaedic and Sports Medicine Associates, Emerson, New Jersey
Anterior shoulder instability in weight lifters MICHAEL L. GROSS,* MD, STEPHEN L. BRENNER, MD, IRA ESFORMES, AND JOHN J. SONZOGNI, MD From Orthopaedic and Sports Medicine Associates, Emerson, New Jersey
Shoulder Labral Tear and Shoulder Dislocation
 Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Body Planes. (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal
 Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Superior Labrum, Anterior to Posterior (SLAP) Surgical Repair
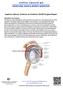 Superior Labrum, Anterior to Posterior (SLAP) Surgical Repair Indications for Surgery The labrum is a fibrocartilaginous soft tissue that encircles the rim of the glenoid (socket of the shoulder). The
Superior Labrum, Anterior to Posterior (SLAP) Surgical Repair Indications for Surgery The labrum is a fibrocartilaginous soft tissue that encircles the rim of the glenoid (socket of the shoulder). The
Surgical Treatment of Traumatic Anterior Shoulder Instability in American Football Players BY MICHAEL J. PAGNANI, MD, AND DAVID C.
 711 COPYRIGHT 2002 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Surgical Treatment of Traumatic Anterior Shoulder Instability in American Football Players BY MICHAEL J. PAGNANI, MD, AND DAVID
711 COPYRIGHT 2002 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Surgical Treatment of Traumatic Anterior Shoulder Instability in American Football Players BY MICHAEL J. PAGNANI, MD, AND DAVID
The Bankart repair illustrated in crosssection
 The Bankart repair illustrated in crosssection Some anatomical considerations RALPH B. BLASIER,* MD, JAMES D. BRUCKNER, LT, MC, USNR, DAVID H. JANDA,* MD, AND A. HERBERT ALEXANDER, CAPT, MC, USN From the
The Bankart repair illustrated in crosssection Some anatomical considerations RALPH B. BLASIER,* MD, JAMES D. BRUCKNER, LT, MC, USNR, DAVID H. JANDA,* MD, AND A. HERBERT ALEXANDER, CAPT, MC, USN From the
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Upper Extremity Injuries in Youth Baseball: Causes and Prevention
 Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Acute Management of Shoulder Dislocation. Mr. Paul Halliwell Royal Surrey County Hospital, Guildford.
 Acute Management of Shoulder Dislocation Mr. Paul Halliwell Royal Surrey County Hospital, Guildford. Acute: Injury to rehab. Management: Hx, O/E, x-ray, Rx Shoulder: Glenohumeral Dislocation: Complete
Acute Management of Shoulder Dislocation Mr. Paul Halliwell Royal Surrey County Hospital, Guildford. Acute: Injury to rehab. Management: Hx, O/E, x-ray, Rx Shoulder: Glenohumeral Dislocation: Complete
Treatment of Primary Anterior Shoulder Dislocation: Conflicting Study Outcomes. Prof. C. Milgrom Hadassah University Hospital Jerusalem, Israel
 Treatment of Primary Anterior Shoulder Dislocation: Conflicting Study Outcomes Prof. C. Milgrom Hadassah University Hospital Jerusalem, Israel I. Natural history of shoulder dislocation and traditional
Treatment of Primary Anterior Shoulder Dislocation: Conflicting Study Outcomes Prof. C. Milgrom Hadassah University Hospital Jerusalem, Israel I. Natural history of shoulder dislocation and traditional
Instability of the shoulder Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Instability of the shoulder Orthopaedic Department Patient Information Leaflet Page 1 Shoulder instability There is a balance between movements in the shoulder whilst maintaining stability. When the shoulder
Instability of the shoulder Orthopaedic Department Patient Information Leaflet Page 1 Shoulder instability There is a balance between movements in the shoulder whilst maintaining stability. When the shoulder
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
Types of shoulder Dislocation: Shoulder dislocation. 1. Anterior 2. Posterior 3. Luxatio erecta (inferior dislocation)
 Types of shoulder Dislocation: Shoulder dislocation 1. Anterior 2. Posterior 3. Luxatio erecta (inferior dislocation) Anterior Dislocation: head is dislocated anterior to the glenoid Most common among
Types of shoulder Dislocation: Shoulder dislocation 1. Anterior 2. Posterior 3. Luxatio erecta (inferior dislocation) Anterior Dislocation: head is dislocated anterior to the glenoid Most common among
COMMON KNEE AND SHOULDER INJURIES IN THE YOUNG ATHLETE. Outline 5/11/2017
 COMMON KNEE AND SHOULDER INJURIES IN THE YOUNG ATHLETE IRVING RAPHAEL MD Syracuse Orthopedic Specialists Former S.U. Head Team Physician May 19, 2017 Meniscal Injuries anatomy Exam Treatment ACL Injuries
COMMON KNEE AND SHOULDER INJURIES IN THE YOUNG ATHLETE IRVING RAPHAEL MD Syracuse Orthopedic Specialists Former S.U. Head Team Physician May 19, 2017 Meniscal Injuries anatomy Exam Treatment ACL Injuries
Management of the unstable shoulder
 Link to this article online for CPD/CME credits Management of the unstable shoulder Tanujan Thangarajah, 1 Simon Lambert 2 1 John Scales Centre for Biomedical Engineering, Institute of Orthopaedics and
Link to this article online for CPD/CME credits Management of the unstable shoulder Tanujan Thangarajah, 1 Simon Lambert 2 1 John Scales Centre for Biomedical Engineering, Institute of Orthopaedics and
Chronic Shoulder Disorders
 Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
Chronic Shoulder Disorders Dr. Mustafa Elsingergy Consultant orthopedic surgeon Dallah Hospita Prof. Mamoun Kremli Almaarefa Medical College Contents INTRINSIC Shoulder Pain Due to causes in the shoulder
GOAL. Open Bankart: Why and How? 2/16/2017. Richard J. Hawkins, MD. Convince You That Open Bankart should be in our toolbox
 Current Solutions in Shoulder & Elbow Surgery Tampa, Florida February 9 12, 2017 Open Bankart: Why and How? Richard J. Hawkins, MD Steadman Hawkins Clinic of the Carolinas Hawkins Foundation Greenville,
Current Solutions in Shoulder & Elbow Surgery Tampa, Florida February 9 12, 2017 Open Bankart: Why and How? Richard J. Hawkins, MD Steadman Hawkins Clinic of the Carolinas Hawkins Foundation Greenville,
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
Pediatric Fractures. Objectives. Epiphyseal Complex. Anatomy and Physiology. Ligaments. Bony matrix
 1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patien
 The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
( 1 ) Ball and socket. Shoulder capsule. Rotator cuff.
 Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, "arthro" (joint)
Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, "arthro" (joint)
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
An analysis of 140 injuries to the superior glenoid labrum
 ORIGINAL ARTICLES An analysis of 140 injuries to the superior glenoid labrum Stephen J. Snyder, MD, Michael P. Banas, MD, and Ronald P. Karzel, MD, Van Nuys, Calif. Between 1985 and 1993 140 injuries of
ORIGINAL ARTICLES An analysis of 140 injuries to the superior glenoid labrum Stephen J. Snyder, MD, Michael P. Banas, MD, and Ronald P. Karzel, MD, Van Nuys, Calif. Between 1985 and 1993 140 injuries of
External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; a 2 Year Follow Up
 External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; a 2 Year Follow Up 2010 Bi-Annual SESA Closed Conference DISCLAIMER None of the authors have
External Rotation Brace Combined with a Physiotherapy Program for First Time Anterior Shoulder Dislocators; a 2 Year Follow Up 2010 Bi-Annual SESA Closed Conference DISCLAIMER None of the authors have
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Labral Tears. Fig 1: Intact labrum and biceps tendon
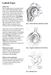 Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Proximal Humerus Fractures/Dislocations.
 Proximal Humerus Fractures/Dislocations www.fisiokinesiterapia.biz History/Demographics Bimodal: young-high energy, elderly-low energy(osteoporosis) 45% of all humerus fx. elderly females 4:1 over males
Proximal Humerus Fractures/Dislocations www.fisiokinesiterapia.biz History/Demographics Bimodal: young-high energy, elderly-low energy(osteoporosis) 45% of all humerus fx. elderly females 4:1 over males
Treatment of reverse Hill-Sachs lesion by autograft reconstruction
 CASE REPORT Acta Orthop Traumatol Turc 2012;46(5):398-402 doi:10.3944/aott.2012.2506 Treatment of reverse Hill-Sachs lesion by autograft reconstruction Gökhan TOKER 1, F rat OZAN 2, Osman Arslan BORA 3
CASE REPORT Acta Orthop Traumatol Turc 2012;46(5):398-402 doi:10.3944/aott.2012.2506 Treatment of reverse Hill-Sachs lesion by autograft reconstruction Gökhan TOKER 1, F rat OZAN 2, Osman Arslan BORA 3
Christopher A Brown, MD Sports Medicine Orthopedist. Duke Orthopedic Residency Sports Medicine Fellowship Stanford
 Christopher A Brown, MD Sports Medicine Orthopedist Duke Orthopedic Residency Sports Medicine Fellowship Stanford Office Geneva Newark Opening Canandaigua and Penfield Topics Of Discussion Shoulder dislocation
Christopher A Brown, MD Sports Medicine Orthopedist Duke Orthopedic Residency Sports Medicine Fellowship Stanford Office Geneva Newark Opening Canandaigua and Penfield Topics Of Discussion Shoulder dislocation
Management of Humeral Bone Loss in Anterior Shoulder Instability. Scott D. Mair, MD University of Kentucky Sports Medicine
 Management of Humeral Bone Loss in Anterior Shoulder Instability Scott D. Mair, MD University of Kentucky Sports Medicine Disclosure Smith and Nephew Endoscopy fellowship support Importance Bone loss (glenoid
Management of Humeral Bone Loss in Anterior Shoulder Instability Scott D. Mair, MD University of Kentucky Sports Medicine Disclosure Smith and Nephew Endoscopy fellowship support Importance Bone loss (glenoid
Shoulder Arthroscopy Lab Manual
 Shoulder Arthroscopy Lab Manual Dalhousie University Orthopaedic Program May 5, 2017 Skills Centre OBJECTIVES 1. Demonstrate a competent understanding of the arthroscopic anatomy and biomechanics of the
Shoulder Arthroscopy Lab Manual Dalhousie University Orthopaedic Program May 5, 2017 Skills Centre OBJECTIVES 1. Demonstrate a competent understanding of the arthroscopic anatomy and biomechanics of the
