The Copeland resurfacing humeral head implant does not restore humeral head anatomy. A retrospective study
|
|
|
- Myron Shaw
- 5 years ago
- Views:
Transcription
1 Arch Orthop Trauma Surg (2013) 133: DOI /s ORTHOPAEDIC SURGERY The Copeland resurfacing humeral head implant does not restore humeral head anatomy. A retrospective study Inger Mechlenburg Anders Amstrup Thomas Klebe Stig Storgaard Jacobsen Gerhardt Teichert Maiken Stilling Received: 20 July 2012 / Published online: 14 March 2013 Ó Springer-Verlag Berlin Heidelberg 2013 Abstract Purpose Recently, there has been concern that the Copeland resurfacing humeral head implant (RHHI) leaves the shoulder joint overstuffed. The purpose of this study was in a selected cohort of patients operated with a Copeland RHHI (1) to evaluate the Length of the Gleno- Humeral Offset (LGHO), (2) to assess the patient-reported quality of life and functional outcome measured by Western Ontario Osteoarthritis of the Shoulder Index (WOOS) and (3) to determine the number of revisions in the cohort. Methods Pre- and postoperative radiographs were retrieved from 71 of 91 possible patients operated with a Copeland RHHI from 2005 to The cohort consisted of 30 males and 41 females at a mean age of 61 (38 89) years. One radiologist measured the LGHO and performed double measurements. The WOOS score 1 year after surgery and the number of revisions from all patients operated with a Copeland RHHI in Denmark was requested from the Danish Shoulder Arthroplasty Registry. I. Mechlenburg (&) M. Stilling Department of Orthopaedics, Aarhus University Hospital, Tage-Hansens Gade 2, Building 10 A, Office 13, 8000 Aarhus C, Denmark inger.mechlenburg@ki.au.dk A. Amstrup Department of Radiology, Holstebro Regional Hospital, Holstebro, Denmark T. Klebe Department of Orthopedic Surgery, Silkeborg Regional Hospital, Silkeborg, Denmark S. S. Jacobsen G. Teichert Department of Orthopaedics, Horsens Regional Hospital, Horsens, Denmark Results The mean LGHO was 4.99 ± 0.53 cm before surgery and 5.39 ± 0.58 cm after surgery, (p \ 0.001). 95 % limits of agreement for measurements of LGHO were ± 0.11 cm. One year after surgery, the WOOS score was 67 for the cohort and 64 for all patients operated with a Copeland RHHI in Denmark. 13 of 71 RHHI in the cohort were revised. Conclusion The Copeland RHHI causes significantly increased LGHO and leads to overstuffing in the shoulder joint. The WOOS score in the cohort was comparable to that for all other Danish patients operated with a Copeland RHHI. Keywords Resurfacing humeral head implant Overstuffing WOOS Shoulder Introduction The number of patients presenting with symptoms attributable to glenohumeral arthritis has increased tremendously over the past decade [1]. The reasons are multifactorial, and include the aging of the population as well as an increased awareness of arthritis in the shoulder joint. Cementless resurfacing humeral head implants (RHHI) is a viable treatment option for glenohumeral arthritis with acceptable clinical results for young [2, 3] as well as older [4] patients and with results comparable to those obtained with a modern stemmed shoulder implants [5, 6]. RHHI necessitate minimal bone resection compared to conventional stemmed shoulder implants and problems with humeral stress fracture in proximity of the diaphyseal stem are avoided. The Copeland RHHI (Biomet) has been in clinical use for more than 20 years and in Denmark the treatment
2 616 Arch Orthop Trauma Surg (2013) 133: indication for this RHHI is primarily osteoarthritis and to a lesser degree rheumatoid arthritis in the shoulder joint [7]. There has been concern that the Copeland RHHI leaves the shoulder joint overstuffed because the reaming process only removes 2 mm of the humeral surface, while the average thickness of the prosthesis is 4 mm. The design of the Copeland HHRI was in 2010 changed by the manufacturer (Copeland thin shell) to comply with concerns of overstuffing. The purpose of this study was (1) to evaluate the Length of the Gleno-Humeral Offset (LGHO) in a selected cohort of patients operated with a Copeland RHHI, (2) to assess the patient-reported quality of life and functional outcome measured by Western Ontario Osteoarthritis of the Shoulder Index (WOOS) in the cohort and in all Danish patients operated with the Copeland RHHI in the same time period and (3) to determine the number of revisions in the cohort and in the Danish population operated with the Copeland RHHI in the same time period. Patients and methods Between 2005 and 2009, 91 patients were operated with a Copeland RHHI at two Regional Hospitals in Denmark. Digital pre- and 6 months post-operative radiographs were retrieved from 71 of the patients (Table 1). The cohort consisted of 30 males and 41 females with a mean age of 61 (38 89) years. The patients in the cohort were operated by three senior orthopaedic surgeons. The operations were performed via the deltopectoral approach and the RHHI were inserted after the surgeons had validated that the osteoarthritis was primarily visible on the humeral head and that there was no need for a glenoid component. The Copeland RHHI has a Closed Pore, Porous Coating and Table 1 Summary of demographics for the cohort of patients operated with a Copeland RHHI, presented for females and males Copeland RHHI Females (n = 41) Males (n = 30) Age (range) years 66 (45 89) 58 (38 79) Diagnose OA/RA 32/9 27/3 Size of resurfacing implant Operated side (right/left) 30/11 20/10 Prior shoulder surgery a (yes/no) 29/12 23/7 Additional surgery b at time of insertion of RHHI (yes/no) 22/19 19/11 OA osteoarthritis, RA rheumatoid arthritis a Synovectomy, cuff reconstruction, subacromial decompression, acromioclavicular joint resection, arthroscopic surgery b Cuff reconstruction, subacromial decompression, acromioclavicular joint resection, biceps tenotomy, biceps tenodesis hydroxyapatite for cementless fixation, and further the implant design features an extended skirted rim for a circumferential press-fit and a tapered cruciform peg to provide rotational stability. The postoperative course after insertion of Copeland RHHI was immobilization with an arm sling on the first postoperative day. Hereafter, un-weighted, passive movement supervised by a physiotherapist was allowed to maximum 60 outward rotation, whereas only pain limited the motion in abduction and flexion. After 6 weeks, free, active movement, respecting the pain threshold, was encouraged under supervision of a physiotherapist. One radiologist measured the LGHO [8, 9] using a modified method on the 71 pre- and postoperative radiographs. The X-ray technique of the two hospitals was standardized; the patients were positioned standing with the back against the image receptor and the non-affected side was turned away from the image receptor. The affected arm was flexed 90 in the elbow and the underarm was internally rotated. The angle of the beam was tilted in cranial caudal direction and was centered towards the shoulder joint (Fig. 1). First a line from the top to the bottom of the glenoid cavity was drawn. Then the centre axis of the humeral bone was drawn and a parallel line was shifted till it touched the most lateral part of the major tubercle. This point was marked and the perpendicular distance from the glenoid line to this point was noted as the modified measure of LGHO (Fig. 2). In theory, LGHO after surgery should be identical to LGHO before the shoulder morphology changed due to arthritis if no soft tissue is changed in that period. But as osteoarthritis progresses with narrowing of the joint space, loss of the articular cartilage, destruction of the humeral head and capsule tightening, the soft tissue adapts to the changed morphology by shrinking and the LGHO should not be wider after surgery than before. Classically, the measure of LGHO is performed by measuring from the base of the coracoid process to the greater tubercle [8, 10]. But this measure shows systematic errors in inter-tester reliability [10] because it is difficult to locate the base of the coracoid process and thus one tester is likely to locate it more medially than the other tester. Due to the reported problems with inter-tester reliability of the standard LGHO measurements, we chose to apply the modified LGHO in this study and the radiologist performed repeated measurements using the modified LGHO method on preoperative and postoperative AP radiographs from 15 patients (60 radiographs) to estimate the intra-tester reliability of the method. The WOOS score 1 year after surgery and the number of revisions from all patients operated with a Copeland RHHI in Denmark from primo 2005 to ultimo 2009 were requested from the Danish Shoulder Arthroplasty Registry (662
3 Arch Orthop Trauma Surg (2013) 133: Fig. 1 X-ray of the left shoulder before and 6 months after implantation of shoulder humeral head resurfacing implant. Length of Gleno Humeral Offset is measured by a modified method in which the first step is drawing a line from the top to the bottom of the glenoid cavity (A). Then the centre axis of the humeral bone was drawn and a parallel line was shifted till it touched the most lateral part of the major tubercle (B). This point was marked and the perpendicular distance from the glenoid-line A to this point was noted (C) patients). From the data set, we could calculate the WOOS score and the number of revisions for the population and for our cohort (n = 71). In 2011 (2 5 years after surgery) we asked the patients in the cohort to fill out the WOOS questionnaire once again to obtain a more recent follow-up and 62 patients returned their answers. The WOOS is used in this study because the data are already collected in the Danish Shoulder Arthroplasty Registry and thus we had access to these patient-reported data on quality of life and functional outcome after RHHI. The WOOS contains 19 items, each with a visual analog scale response option for the four domains (six questions for pain and physical symptoms, five questions for sport, recreation and work, five questions for lifestyle function and three questions for emotional function). The instrument is proven to be valid by demonstrating predicted correlations with previously published shoulder measures, global health status measure and range of motion [11]. In the WOOS the range of points goes from 1900 (the worst possible outcome) to 0 (asymptomatic shoulder). In orthopaedic studies, there is a tradition to report scores out of 100 and present a percentage of normal score (100). Thus in this study, the aggregate score is subtracted from 1900 and divided by 19. Data for LGHO per- and postoperatively was tested by a paired t test. The 95 % limits of agreement were calculated as described by Bland and Altman [12]. The systematic variation (bias) between the double measurements was estimated as the mean difference between the two measurements. The difference between the two measurements followed a normal distribution (Shapiro Wilk test) and was tested by a paired t test. The variance (random variation) between double examinations was tested by Pitmans test. Results Fig. 2 Standardized X-ray projection. Patients were positioned standing with the back against the image receptor and the nonaffected side was turned away from the image receptor. The affected arm was flexed 90 in the elbow and the underarm was internally rotated. The angle of the beam was tilted in cranial caudal direction and was centered towards the shoulder joint The mean LGHO increased from 4.99 ± 0.53 cm before surgery to mean 5.39 ± 0.58 cm after surgery, (p \ 0.001). In the two hospitals LGHO was 4.96 and 5.08 cm preoperative and 5.39 and 5.40 cm postoperative. 95 % limits of agreement for measurements of LGHO were ± 0.11 cm indicating a high intra-tester reliability of the method. No systematic variation between the first and second measurement was found, the difference being (95 % CI to 0.01). One year after surgery, the WOOS score was mean 67 (20 100) for the cohort and mean 64 (5 100) for all
4 618 Arch Orthop Trauma Surg (2013) 133: patients operated with a Copeland RHHI in Denmark in the same period of time. Two to five years later, the WOOS score for the cohort was mean 66 (7 100). One to five years after RHHI, 13 of 71 implants (14 %) in the cohort were revised, eight due to persistent pain. In those cases, overstuffing of the shoulder joint was suspected to cause the pain. Figure 3 shows an example of one of the cases observed. One patient had the RHHI revised due rotator cuff problems, one due to glenoid attrition, one had a technically failed primary operation, one due to luxation and one due to infection in shoulder joint. In the Danish population of Copeland RHHI operated in the same period, 25 of 662 implants (4 %) were revised. The causes for revision were luxation (2), loosening (3), glenoid attrition (12), infection (3), rotator cuff problems (2), and persistent pain (8). Discussion We evaluated the LGHO in a selected cohort of patients operated with a Copeland RHHI and found the mean LGHO to be significantly 4 mm wider after surgery compared to before. The measurements were precise with a high intratester reliability. The design of the RHHI is sought to recreate the normal anatomic relationships and contours of the humeral head but we consider the Copeland RHHI to potentially overstuff the shoulder joint caused by the reaming process that removes only 2 mm of the humeral Fig. 3 An example of too large offset and overstuffing of left shoulder joint in one of the included patients. The Copeland RHHI does not allow the surgeon to reame the humeral head smaller and thus the offset becomes too large and the joint overstuffed surface while the average thickness of the prosthesis is 4 mm. Due to these design parameters, the RHHI may result in overstuffing and pain when the shoulder capsule is tight. There may be differences in the laxity of the joint capsule between patients so that some patients can adapt to the added offset with the Copeland RHHI while others cannot. The problem the surgeons experienced when using the Copeland RHHI was that the reamer for the Copeland RHHI did not allow the surgeon to reame the humeral head smaller. Then, the surgeon had the option of using an implant with a small diameter which resulted in an implant that looked like a hat put on the humeral head. Or the surgeon could use an implant that fitted the diameter of the humeral head but ended up with overstuffing the joint. Recently, the design of the Copeland HHRI was altered by the manufacturer to comply with concerns of overstuffing. The measurements of LGHO were easy to perform in a standardized manner and the results of the measurements turned out to be very informative in relation to show a difference in shoulder geometry after Copeland RHHI. We applied the modified LGHO and we recommend others to use that also because it is easy to identify the relevant anatomical landmarks used to perform the measurements. We used the 6-months radiographs for post-operative measurements and therefore we do not believe that intraarticular oedema or blood falsely increased the LGHO measurements. We set out to assess the patient-reported quality of life and functional outcome measured by WOOS and found the score to be comparable in the cohort to the Danish population of patients operated with the Copeland RHHI in the same time period. This indicates that there was nothing unusual about the functional results for the cohort. Two to five years later, the WOOS score for the cohort was unchanged (WOOS score 66) for those patients not revised. Does a WOOS score of 66 out of possible 100 represent an acceptable functional capacity? Thomas et al. [5] applied the Constant Score [13] to evaluate the outcome 34 months after Copeland RHHI and reported a mean score of 54 out of possible 100. In Copeland s own series [14], the Constant Score at 5 10 year follow-up was 73. The results from the WOOS and the Constant Score are based on very different measurements and cannot be compared; however, the level of the scores after RHHI indicates that rehabilitation should be granted a higher focus after HHRI surgery. Early postoperative range of motion exercises and progressive strengthening exercises, have been shown to result in decreased pain, improved range of motion, and fast return to work following hemiarthroplasty [15]. Usually, rehabilitation after RHHI focuses on range of motion and functional exercise but it is plausible that a protocol of progressive strengthening as used after total hip and knee arthroplasty would be more effective in re-gaining functional capacity and coping with activities of daily living for these patients.
5 Arch Orthop Trauma Surg (2013) 133: The rate of revisions in the cohort 1 year after RHHI was 14 %, for eight patients due to persistent pain and possible overstuffing and for five patients due to rotator cuff problems, glenoid attrition, technically failed primary operation, luxation and infection in the shoulder joint. In the Danish population operated with the Copeland RHHI in the same time period, only 4 % were revised. Although, a cohort of 71 patients is a small sample, questions arise on why the rate of revisions was higher in the cohort, compared to the population operated in the same time interval. A number of revisions can happen if inexperienced surgeons perform few procedures with a new prosthesis. However, the surgeons who operated this cohort are specialized shoulder surgeons with vast experience from shoulder replacement surgery and fracture osteosynthesis and therefore we believe that the design of the Copeland RHHI may lead to overstuffing and eventually revision. Another explanation could be that the patient selection has been different in the cohort compared to the population and that some of the patients in the cohort had been better off with a total shoulder arthroplasty. Attention on overstuffing and discussions of the subject among the surgeons who operated the cohort may theoretically have affected the rate of revision for these patients but it is not very likely as the primary cause of revision was persistent pain in both the cohort and in the general Danish population of Cope RHHI. In a 5 10 year follow-up of the Copeland RHHI, the rate of revision was 7.7 % [14]. Studies on outcome with hemiarthroplasty to glenohumeral arthritis have reported results ranging from no revisions at 2 year [16] and at 5 year [17] to 28 % revision at 10 year follow-up [18]. In conclusion, the LGHO was significantly increased after Copeland RHHI and the high rate of revisions points to a problem with overstuffing associated with this prosthesis design. The design of the Copeland HHRI has been changed by the manufacturer to comply with the concerns of overstuffing and therefore this version of the Copeland HHRI will not be further used. Shoulder surgeons should be aware of potential overstuffing when they see a patient with persistent pain after RHHI. Acknowledgments This study has been financially supported by the Danish Rheumatism Association and The Aase And Ejnar Danielsen Foundation. None of the participants have any economic association with the providers of the economic support. Conflict of interest of interest. The authors declare that they have no conflict 2. Raiss P, Pape G, Becker S, Rickert M, Loew M (2010) Cementless humeral surface replacement arthroplasty in patients less than 55 years of age. Orthopade 39(2): Buchner M, Eschbach N, Loew M (2008) Comparison of the short-term functional results after surface replacement and total shoulder arthroplasty for osteoarthritis of the shoulder: a matched-pair analysis. Arch Orthop Trauma Surg 128(4): Mullett H, Levy O, Raj D, Even T, Abraham R, Copeland SA (2007) Copeland surface replacement of the shoulder. Results of an hydroxyapatite-coated cementless implant in patients over 80 years of age. J Bone Joint Surg Br 89(11): Thomas SR, Wilson AJ, Chambler A, Harding I, Thomas M (2005) Outcome of Copeland surface replacement shoulder arthroplasty. J Shoulder Elbow Surg 14(5): Gordiev K, Seitz WH Jr (2004) Surface arthroplasty in shoulder arthritis. Semin Arthroplasty 15(4): Rasmussen JV, Jakobsen J, Brorson S, Olsen BS (2012) The Danish Shoulder Arthroplasty Registry: clinical outcome and short-term survival of 2,137 primary shoulder replacements. Acta Orthop 83: Lehtinen JT, Belt EA, Kauppi MJ, Kaarela K, Kuusela PP, Kautiainen HJ, Lehto MU (2001) Bone destruction, upward migration, and medialisation of rheumatoid shoulder: a 15 year follow up study. Ann Rheum Dis 60(4): Stilling M, Mechlenburg I, Amstrup A, Soballe K, Klebe T (2012) Precision of novel radiological methods in relation to resurfacing humeral head implants: assessment by radiostereometric analysis, DXA, and geometrical analysis. Arch Orthop Trauma Surg 132: Thomas SR, Sforza G, Levy O, Copeland SA (2005) Geometrical analysis of Copeland surface replacement shoulder arthroplasty in relation to normal anatomy. J Shoulder Elbow Surg 14(2): Lo IK, Griffin S, Kirkley A (2001) The development of a diseasespecific quality of life measurement tool for osteoarthritis of the shoulder: the Western Ontario Osteoarthritis of the Shoulder (WOOS) index. Osteoarthritis Cartilage 9(8): Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1(8476): Constant CR, Murley AH (1987) A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res (214): Levy O, Copeland SA (2001) Cementless surface replacement arthroplasty of the shoulder. 5- to 10-year results with the Copeland mark-2 prosthesis. J Bone Joint Surg Br 83(2): Ellenbecker TS, Bailie DS, Lamprecht D (2008) Humeral resurfacing hemiarthroplasty with meniscal allograft in a young patient with glenohumeral osteoarthritis. J Orthop Sports Phys Ther 38(5): Lynch JR, Franta AK, Montgomery WH Jr, Lenters TR, Mounce D, Matsen FA III (2007) Self-assessed outcome at two to four years after shoulder hemiarthroplasty with concentric glenoid reaming. J Bone Joint Surg Am 89(6): Wirth MA, Tapscott RS, Southworth C, Rockwood CA Jr (2006) Treatment of glenohumeral arthritis with a hemiarthroplasty: a minimum five-year follow-up outcome study. J Bone Joint Surg Am 88(5): Bartelt R, Sperling JW, Schleck CD, Cofield RH (2011) Shoulder arthroplasty in patients aged fifty-five years or younger with osteoarthritis. J Shoulder Elbow Surg 20(1): References 1. Norris TR, Iannotti JP (2002) Functional outcome after shoulder arthroplasty for primary osteoarthritis: a multicenter study. J Shoulder Elbow Surg 11(2):130
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Name of Policy: Shoulder Resurfacing
 Name of Policy: Shoulder Resurfacing Policy #: 366 Latest Review Date: November 2010 Category: Surgery Policy Grade: Active policy but no longer scheduled for regular literature reviews and update. Background/Definitions:
Name of Policy: Shoulder Resurfacing Policy #: 366 Latest Review Date: November 2010 Category: Surgery Policy Grade: Active policy but no longer scheduled for regular literature reviews and update. Background/Definitions:
Inger Mechlenburg, PhD a, *, Thomas M. Klebe, MD b, Kaj V. Døssing, MD c, Anders Amstrup, MD d, Kjeld Søballe, DMSc a, Maiken Stilling, PhD a
 J Shoulder Elbow Surg (2014) 23, 1427-1436 www.elsevier.com/locate/ymse Evaluation of periprosthetic bone mineral density and postoperative migration of humeral head resurfacing implants: two-year results
J Shoulder Elbow Surg (2014) 23, 1427-1436 www.elsevier.com/locate/ymse Evaluation of periprosthetic bone mineral density and postoperative migration of humeral head resurfacing implants: two-year results
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Fixed and Variable Geometry Total Shoulder Arthroplasty
 Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Technical difficulty in component sizing and positioning in humeral resurfacing: Relationship to clinical outcomes
 Page 32 SA Orthopaedic Journal Spring 2015 Vol 14 No 3 Technical difficulty in component sizing and positioning in humeral resurfacing: Relationship to clinical outcomes P Ryan MBChB (UCT), FC(Orth) (SA),
Page 32 SA Orthopaedic Journal Spring 2015 Vol 14 No 3 Technical difficulty in component sizing and positioning in humeral resurfacing: Relationship to clinical outcomes P Ryan MBChB (UCT), FC(Orth) (SA),
Accuracy of Humeral Articular Surface Restoration in a Novel Anatomic Shoulder Arthroplasty Technique and Design: A Cadaveric Study
 Original Scientific Research Accuracy of Humeral Articular Surface Restoration in a Novel Anatomic Shoulder Arthroplasty Technique and Design: A Cadaveric Study Journal of Shoulder and Elbow Arthroplasty
Original Scientific Research Accuracy of Humeral Articular Surface Restoration in a Novel Anatomic Shoulder Arthroplasty Technique and Design: A Cadaveric Study Journal of Shoulder and Elbow Arthroplasty
Surface Replacement for the Active Patient with GH DJD. Disclosures. Popularized by Copeland 3/1/2018
 Surface Replacement for the Active Patient with GH DJD E. Rhett Hobgood, M.D. MS Sports Medicine Jackson, MS Disclosures Consultant for Exactech No royalties from any company Fellowship support from Mitek,
Surface Replacement for the Active Patient with GH DJD E. Rhett Hobgood, M.D. MS Sports Medicine Jackson, MS Disclosures Consultant for Exactech No royalties from any company Fellowship support from Mitek,
TORNIER AEQUALIS FX. Shoulder System SYSTEM OVERVIEW
 TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
Materials and methods. Table I. 2 J.W. Uribe, A.B.-van Bemden
 2 J.W. Uribe, A.B.-van Bemden Table I Stage I Stage II Stage III Stage IV Stage V Cruess classification for osteonecrosis of humeral head Preradiographic, requires magnetic resonance imaging, bone scan,
2 J.W. Uribe, A.B.-van Bemden Table I Stage I Stage II Stage III Stage IV Stage V Cruess classification for osteonecrosis of humeral head Preradiographic, requires magnetic resonance imaging, bone scan,
Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty
 S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
S5 Biomechanical Impact of Posterior Glenoid Wear on Anatomic Total Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Sean G. Grey, M.D., and Pierre-Henri Flurin, M.D. Abstract
Integra. Titan Modular Shoulder System, 2.5
 Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review
 Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Humeral surface replacement for the sequelae of fractures of the proximal humerus
 Humeral surface replacement for the sequelae of fractures of the proximal humerus G. Pape, F. Zeifang, T. Bruckner, P. Raiss, M. Rickert, M. Loew From University of Heidelberg, Heidelberg, Germany G. Pape,
Humeral surface replacement for the sequelae of fractures of the proximal humerus G. Pape, F. Zeifang, T. Bruckner, P. Raiss, M. Rickert, M. Loew From University of Heidelberg, Heidelberg, Germany G. Pape,
Not relevant to this presentation.
 Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
DESIGN RATIONALE AND SURGICAL TECHNIQUE
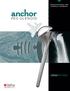 DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
DESIGN RATIONALE AND SURGICAL TECHNIQUE ANCHOR PEG GLENOID DESIGN RATIONALE In total shoulder arthroplasty, most cases of clinical and radiographic loosening involve failure of the fixation of the glenoid
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease
 Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Early To Medium Term Results of the Anatomical Total Shoulder Replacement
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 13 Number 2 Early To Medium Term Results of the Anatomical Total Shoulder Replacement R Sloan, J Young, N Parker, I Nwachukwu Citation R Sloan,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 13 Number 2 Early To Medium Term Results of the Anatomical Total Shoulder Replacement R Sloan, J Young, N Parker, I Nwachukwu Citation R Sloan,
comprehensive Design Rationale shoulder system Knees Hips Extremities Cement and Accessories PMI TEchnology
 comprehensive shoulder system Design Rationale Knees Hips Extremities Cement and Accessories PMI TEchnology . INTRODUCTION The Comprehensive Shoulder System is an evolutionary design based on the successful
comprehensive shoulder system Design Rationale Knees Hips Extremities Cement and Accessories PMI TEchnology . INTRODUCTION The Comprehensive Shoulder System is an evolutionary design based on the successful
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Surgical. Technique. AEQUALIS Spherical Base Glenoid. Shoulder Prosthesis.
 Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Stemless shoulder prosthesis versus conventional anatomic shoulder prosthesis in patients with osteoarthritis
 J Orthopaed Traumatol (2013) 14:31 37 DOI 10.1007/s10195-012-0216-9 ORIGINAL ARTICLE Stemless shoulder prosthesis versus conventional anatomic shoulder prosthesis in patients with osteoarthritis A comparison
J Orthopaed Traumatol (2013) 14:31 37 DOI 10.1007/s10195-012-0216-9 ORIGINAL ARTICLE Stemless shoulder prosthesis versus conventional anatomic shoulder prosthesis in patients with osteoarthritis A comparison
Results of a new stemless shoulder prosthesis: Radiologic proof of maintained fixation and stability after a minimum of three years follow-up
 J Shoulder Elbow Surg (2010) 19, 847-852 www.elsevier.com/locate/ymse Results of a new stemless shoulder prosthesis: Radiologic proof of maintained fixation and stability after a minimum of three years
J Shoulder Elbow Surg (2010) 19, 847-852 www.elsevier.com/locate/ymse Results of a new stemless shoulder prosthesis: Radiologic proof of maintained fixation and stability after a minimum of three years
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Long-term results and patient satisfaction after shoulder resurfacing
 J Shoulder Elbow Surg (2011) 20, 771-777 www.elsevier.com/locate/ymse Long-term results and patient satisfaction after shoulder resurfacing James W. Pritchett, MD* Orthopedics International, Seattle, WA,
J Shoulder Elbow Surg (2011) 20, 771-777 www.elsevier.com/locate/ymse Long-term results and patient satisfaction after shoulder resurfacing James W. Pritchett, MD* Orthopedics International, Seattle, WA,
Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty
 J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
P V S MEMORIAL HOSPITAL LTD.
 SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 6
 Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
S h o u l d e r Solutions by Tornier C o n v e r T i b l e S h o u l d e r S y S T e m
 S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
Shoulder Replacement Commonly Asked Questions
 Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Making sense of all our measures-inclination, version, subluxation, reaming depth & implant seating
 Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis
 Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
The Bio-Modular Choice Shoulder System,
 Surgical Technique The Bio-Modular Choice Shoulder System, designed for both total and hemiarthroplasty of the shoulder, has enjoyed nearly two decades of clinical success. The variety of head types and
Surgical Technique The Bio-Modular Choice Shoulder System, designed for both total and hemiarthroplasty of the shoulder, has enjoyed nearly two decades of clinical success. The variety of head types and
ANATOMIC TOTAL SHOULDER REPLACEMENT:
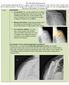 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
Technique. Aequalis Resurfacing Humeral Head
 S u r g i c a l Technique Aequalis Resurfacing Humeral Head 1 The Aequalis Resurfacing Humeral Head has been developed in conjunction with Drew Miller, MD - Atlanta, GA. The Aequalis Resurfacing Humeral
S u r g i c a l Technique Aequalis Resurfacing Humeral Head 1 The Aequalis Resurfacing Humeral Head has been developed in conjunction with Drew Miller, MD - Atlanta, GA. The Aequalis Resurfacing Humeral
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder
 Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Resurfacing Arthroplasty of the Humerus: Indications, Surgical Technique, and Clinical Results
 8(3):152 160, 2007 Ó 2007 Lippincott Williams & Wilkins, Philadelphia R E V I E W Resurfacing Arthroplasty of the Humerus: Indications, Surgical Technique, and Clinical Results Jason J. Scalise, MD, Anthony
8(3):152 160, 2007 Ó 2007 Lippincott Williams & Wilkins, Philadelphia R E V I E W Resurfacing Arthroplasty of the Humerus: Indications, Surgical Technique, and Clinical Results Jason J. Scalise, MD, Anthony
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Both anatomic (atsa) and reverse (rtsa) total
 S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
Shoulder hemiarthroplasty in the management of humeral head fractures
 Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
MSK Covered Services. Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components
 CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
CPT CODE S2118 MSK Covered Services Musculoskeletal: Joint Metal-on-metal total hip resurfacing, including acetabular and femoral components 23000 Removal of subdeltoid calcareous deposits, open 23020
Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty
 Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty Jessica Ottow, Student Physical Therapist Suzanne Ryer, MPT Faculty Mentor Abstract Background: Treatment of glenohumeral arthritis
Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty Jessica Ottow, Student Physical Therapist Suzanne Ryer, MPT Faculty Mentor Abstract Background: Treatment of glenohumeral arthritis
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY
 E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
E C H E L O N P R I M A R Y H I P S Y S T E M P R O D U C T R A T I O N A L E ADDRESSING CLINICAL ISSUES OF CEMENTLESS HIP ARTHROPLASTY Echelon Primary Total Hip System HIGH OFFSET STANDARD OFFSET Cementless
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Approach Patients with Confidence
 Surgical Technique Approach Patients with Confidence The ACTIS Total Hip System is the first DePuy Synthes stem specifically designed to be utilized with tissue sparing approaches, such as the anterior
Surgical Technique Approach Patients with Confidence The ACTIS Total Hip System is the first DePuy Synthes stem specifically designed to be utilized with tissue sparing approaches, such as the anterior
Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease
 Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease Gregory P. Nicholson, MD, Jordan L. Goldstein, MD, Anthony A.
Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease Gregory P. Nicholson, MD, Jordan L. Goldstein, MD, Anthony A.
Hip, Knee and Shoulder Surgery
 Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
Hip, Knee and Shoulder Surgery Policy Number: MM.06.030 Lines of Business: HMO; PPO; QUEST Integration; Medicare Advantage Section: Surgery Place(s) of Service: Outpatient; Inpatient Original Effective
RESURFACING HUMERAL HEAD IMPLANT TRAUMA & EXTREMITIES GROUP
 S U R G I C A L T E C H N I Q U E RESURFACING HUMERAL HEAD IMPLANT TRAUMA & EXTREMITIES GROUP TABLE OF CONTENTS SYSTEM OVERVIEW ANATOMIC SIZING AND DESIGN FEATURES INSTRUMENTATION INDICATIONS AND CONTRAINDICATIONS
S U R G I C A L T E C H N I Q U E RESURFACING HUMERAL HEAD IMPLANT TRAUMA & EXTREMITIES GROUP TABLE OF CONTENTS SYSTEM OVERVIEW ANATOMIC SIZING AND DESIGN FEATURES INSTRUMENTATION INDICATIONS AND CONTRAINDICATIONS
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
System Overview 3. Anatomic Sizing And Design Features 4. Instrumentation 6. Indications And Contraindications 7. Surgical Technique 8
 Surgical Technique Table of Contents System Overview 3 Anatomic Sizing And Design Features 4 Instrumentation 6 Indications And Contraindications 7 Surgical Technique 8 Implant Information 22 Instrumentation
Surgical Technique Table of Contents System Overview 3 Anatomic Sizing And Design Features 4 Instrumentation 6 Indications And Contraindications 7 Surgical Technique 8 Implant Information 22 Instrumentation
Balgrist Shoulder Course 2017
 My approach to failed hemiprosthesis Ernst Wiedemann OCM Clinic Munich Consultant to Arthrex Royalties from Arthrex Consultant to Zimmer Disclosures Pathways Hemi-prosthesis Anatomical prosthesis (HSA
My approach to failed hemiprosthesis Ernst Wiedemann OCM Clinic Munich Consultant to Arthrex Royalties from Arthrex Consultant to Zimmer Disclosures Pathways Hemi-prosthesis Anatomical prosthesis (HSA
Patient-Specific Implants in Severe Glenoid Bone Loss
 Patient-Specific Implants in Severe Glenoid Bone Loss Publish date: February 8, 2018 Authors: Ivan De Martino, MD David M. Dines, MD Russell F. Warren, MD Edward V. Craig, MD, MPH Lawrence V. Gulotta,
Patient-Specific Implants in Severe Glenoid Bone Loss Publish date: February 8, 2018 Authors: Ivan De Martino, MD David M. Dines, MD Russell F. Warren, MD Edward V. Craig, MD, MPH Lawrence V. Gulotta,
Bone Preservation Stem
 TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Arthroplasty Of The Shoulder
 Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Shoulder & Elbow Service, University of Washington Department of Orthopaedics and Sports Medicine
 Reverse Total Shoulder or Delta Shoulder for Shoulder Arthritis Combined with Massive Rotator Cuff Tear and for Failed Conventional Total Shoulder Replacement Follow: shoulderarthritis.blogspot.com For
Reverse Total Shoulder or Delta Shoulder for Shoulder Arthritis Combined with Massive Rotator Cuff Tear and for Failed Conventional Total Shoulder Replacement Follow: shoulderarthritis.blogspot.com For
Shoulder Arthroplasty
 Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Assessment of rotation in proximal humeral osteotomy
 Acta Radiologica ISSN: 024-11 (Print) 1600-04 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Assessment of rotation in proximal humeral osteotomy Veli Söderlund, M. Kronberg & L.-Å.
Acta Radiologica ISSN: 024-11 (Print) 1600-04 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Assessment of rotation in proximal humeral osteotomy Veli Söderlund, M. Kronberg & L.-Å.
Common Shoulder Problems and Treatment Options. Benjamin W. Szerlip D.O. Austin Shoulder Institute
 Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
The Shoulder. By Patrick Ryan, Bobby Law, Jack Beaty, Alex Newhouse and Chuck Nelson
 The Shoulder By Patrick Ryan, Bobby Law, Jack Beaty, Alex Newhouse and Chuck Nelson Learning Objectives/Agenda Review the anatomy of the shoulder Describe the main diseases of the shoulder Describe the
The Shoulder By Patrick Ryan, Bobby Law, Jack Beaty, Alex Newhouse and Chuck Nelson Learning Objectives/Agenda Review the anatomy of the shoulder Describe the main diseases of the shoulder Describe the
Predicting the Position of the Femoral Head Center
 The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
Acromioplasty. Surgical Indications and Considerations
 1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic
1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic
Developments in Shoulder Arthroplasty
 Developments in Shoulder Arthroplasty Andrew L. Wallace PhD MFSEM FRCS FRACS Consultant Shoulder Surgeon Glenohumeral Joint Arthritis Relatively uncommon Not as common as hip/knee/hand UK National Joint
Developments in Shoulder Arthroplasty Andrew L. Wallace PhD MFSEM FRCS FRACS Consultant Shoulder Surgeon Glenohumeral Joint Arthritis Relatively uncommon Not as common as hip/knee/hand UK National Joint
Disclosure. General. Total Shoulder Arthroplasty : Results, Outcomes and Expectations 2/8/2016. Consultant for Tornier/Wright, DJO, and Conventus
 Total Shoulder Arthroplasty : Results, Outcomes and Expectations Edwin E Spencer Jr MD Knoxville Orthopaedic Clinic Disclosure Consultant for Tornier/Wright, DJO, and Conventus General The literature is
Total Shoulder Arthroplasty : Results, Outcomes and Expectations Edwin E Spencer Jr MD Knoxville Orthopaedic Clinic Disclosure Consultant for Tornier/Wright, DJO, and Conventus General The literature is
Management of Glenoid and Humeral Bone Loss in Shoulder Instability
 Short Stem and Long Stem Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics Today Short Stem
Short Stem and Long Stem Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics Today Short Stem
Musculoskeletal Ultrasound. Technical Guidelines SHOULDER
 Musculoskeletal Ultrasound Technical Guidelines SHOULDER 1 Although patient s positioning for shoulder US varies widely across different Countries and Institutions reflecting multifaceted opinions and
Musculoskeletal Ultrasound Technical Guidelines SHOULDER 1 Although patient s positioning for shoulder US varies widely across different Countries and Institutions reflecting multifaceted opinions and
DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS
 DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS Lyndon B. Gross M.D. Ph.D. The Orthopedic Center of St. Louis SHOULDER PAIN Third most common musculoskeletal
DISTINGUISHING BETWEEN ACUTE AND CHRONIC ROTATOR CUFF INJURIES IN WORKERS COMPENSATION PATIENTS Lyndon B. Gross M.D. Ph.D. The Orthopedic Center of St. Louis SHOULDER PAIN Third most common musculoskeletal
Hip Resurfacing System
 Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid
 The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid David R. J. Gill, MB, ChB, FRACS, a Robert H. Cofield, MD, b and Charles Rowland, MS, c Joondalup, Australia,
The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid David R. J. Gill, MB, ChB, FRACS, a Robert H. Cofield, MD, b and Charles Rowland, MS, c Joondalup, Australia,
The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study
 4edwards.qxd 4/6/04 3:53 PM Page 401 The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study GIUSEPPE FAMA, MD*; T. BRADLEY EDWARDS,
4edwards.qxd 4/6/04 3:53 PM Page 401 The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study GIUSEPPE FAMA, MD*; T. BRADLEY EDWARDS,
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Design Rationale. ECHELON Primary Hip System
 Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
Design Rationale ECHELON Primary Hip System ECHELON Primary Total Hip System Addressing clinical issues of cementless hip arthroplasty Cementless total hip arthroplasty has provided a proven method of
Instability of the Shoulder after Arthroplasty*
 Copyright 1993 by The Journal ofbone and Joint Surgery, Incorporated Instability of the Shoulder after Arthroplasty* BY BRUCE H. MOECKEL. M.D.t. DAVID w. ALTCHEK. M.D3. RUSSELL F. WARREN. M.D4, THOMAS
Copyright 1993 by The Journal ofbone and Joint Surgery, Incorporated Instability of the Shoulder after Arthroplasty* BY BRUCE H. MOECKEL. M.D.t. DAVID w. ALTCHEK. M.D3. RUSSELL F. WARREN. M.D4, THOMAS
AML Hip System. Design Rationale/ Surgical Technique
 AML Hip System Design Rationale/ Surgical Technique Design Rationale Evolution In 1977, DePuy Synthes Companies introduced the original cementless total hip. The AML Hip launched in order to solve one
AML Hip System Design Rationale/ Surgical Technique Design Rationale Evolution In 1977, DePuy Synthes Companies introduced the original cementless total hip. The AML Hip launched in order to solve one
Optimizing function Maximizing survivorship Accelerating recovery
 Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Surgical Technique r5.indd 1 12/8/10 10:36 AM
 Surgical Technique The science of simplicity With more than 700,000 implantations and two and a half decades of clinical success, the Corail Total Hip System now has the most extensive experience with
Surgical Technique The science of simplicity With more than 700,000 implantations and two and a half decades of clinical success, the Corail Total Hip System now has the most extensive experience with
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Conflicts of Interest Consulting (C), Royalty (R)
 Principles of Anatomic Total Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflicts of Interest Consulting
Principles of Anatomic Total Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflicts of Interest Consulting
TABLE OF CONTENTS SURGICAL TECHNIQUE 1 POST-OPERATIVE REHABILITATION 18. pages 1 RADIOLOGICAL ASSESSMENT 1 2 PATIENT POSITIONING 1
 TABLE OF CONTENTS SURGICAL TECHNIQUE 1 1 RADIOLOGICAL ASSESSMENT 1 2 PATIENT POSITIONING 1 3 DELTO-PECTORAL APPROACH 2 4 HUMERAL HEAD OSTEOTOMY 6 5 CHOICE OF HUMERAL INCLINATION AND RETROVERSION 7 pages
TABLE OF CONTENTS SURGICAL TECHNIQUE 1 1 RADIOLOGICAL ASSESSMENT 1 2 PATIENT POSITIONING 1 3 DELTO-PECTORAL APPROACH 2 4 HUMERAL HEAD OSTEOTOMY 6 5 CHOICE OF HUMERAL INCLINATION AND RETROVERSION 7 pages
Shoulder DJD in Athletic patient. What is Athletic? McCarty University of Colorado Fall Sports Medicine Symposium. Oct. 3, 2008
 Indications for Shoulder Arthroplasty in Athletic Patients Eric C. McCarty, M.D. Associate Professor, Dept. of Orthopaedics Chief, Sports Medicine and Shoulder Surgery Head Team Physician, University of
Indications for Shoulder Arthroplasty in Athletic Patients Eric C. McCarty, M.D. Associate Professor, Dept. of Orthopaedics Chief, Sports Medicine and Shoulder Surgery Head Team Physician, University of
SSSR. 1. Nov Shoulder Prosthesis. Postoperative Imaging. Florian M. Buck, MD
 Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Arthritis of the Shoulder
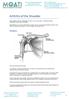 Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Approach Patients with Confidence
 Approach Patients with Confidence The is the first stem specifically designed to be utilized with tissue sparing approaches, such as the anterior approach, as well as traditional approaches. The implant
Approach Patients with Confidence The is the first stem specifically designed to be utilized with tissue sparing approaches, such as the anterior approach, as well as traditional approaches. The implant
Scholars Journal of Medical Case Reports
 DOI: 10.21276/sjmcr Scholars Journal of Medical Case Reports Sch J Med Case Rep 2017; 5(7):422-426 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic
DOI: 10.21276/sjmcr Scholars Journal of Medical Case Reports Sch J Med Case Rep 2017; 5(7):422-426 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic
HIP SYSTEM SURGICAL TECHNIQUE
 HIP SYSTEM SURGICAL TECHNIQUE Introduction...2 Preoperative Planning...3 Preoperative Planning...3 Templating and Radiographs...4 Determination of Leg Length Discrepancy...5 Determining Acetabular Cup
HIP SYSTEM SURGICAL TECHNIQUE Introduction...2 Preoperative Planning...3 Preoperative Planning...3 Templating and Radiographs...4 Determination of Leg Length Discrepancy...5 Determining Acetabular Cup
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
