Although nontraumatic osteonecrosis (ON) is most
|
|
|
- Doris Watts
- 5 years ago
- Views:
Transcription
1 Techniques in Shoulder & Elbow Surgery 9(1):23 30, 2008 T E C H N I Q U E Technique and Early Results of Intramedullary Pressure-Guided Core Decompression of the Humeral Head for Nontraumatic Osteonecrosis Milford H. Marchant Jr, MD Division of Orthopaedic Surgery Duke University Medical Center Durham, NC Allston J. Stubbs, MD North Carolina Sports Medicine Institute Winston-Salem, NC Carl J. Basamania, MD Triangle Orthopaedic Associates, P.A. Durham, NC Ó 2008 Lippincott Williams & Wilkins, Philadelphia ABSTRACT The purpose of this study was to describe a modified technique for humeral head core decompression using biplanar fluoroscopy and intraosseous pressure monitoring to identify osteonecrotic regions for targeted decompression. A bone marrow biopsy needle and arterial pressure monitoring equipment were used to locate the region of maximum pressure, and then acorn-style reamers decompressed the osteonecrotic bone. In 12 shoulders (11 patients) evaluated, the peak intramedullary lesion pressure was, on average, 6 times higher than the entry pressure. At 6 months, Visual Analog Scale pain scores had decreased in all shoulders by 70.3% (P G ) on average. Nine of 12 shoulders, with an average follow-up of 44.2 months (range, 12Y72.5 months), were evaluated for pain relief, disease progression, and need for arthroplasty. In that group, Visual Analog Scale pain scores had decreased by 56.8% (P G 0.008) on average. Only 1 patient, despite excellent initial results, had progression of symptoms and required arthroplasty at 12 months. Pressure-guided core decompression provides a technique for directly localizing the osteonecrotic bone and potentially improving decompression outcomes. Keywords: osteonecrosis, avascular necrosis, core decompression, intraosseous pressure monitoring, humeral head, humerus Reprints: Carl J. Basamania, MD, Triangle Orthopaedic Associates, P.A., 120 William Penn Plaza, Independence Park, Durham, NC ( cbasam@surgical.net). Although nontraumatic osteonecrosis (ON) is most frequently found in the femoral head, the humeral head is the second most common location. 1Y7 Initially described in the humeral head by Heimann and Freiberger 8 in 1960, most of our subsequent knowledge regarding the disease process has been extrapolated from femoral head disease. Although the 2 disease locations share the same etiologies and underlying pathology, humeral head ON is a different clinical entity. The functional capacity of the shoulder is more forgiving largely because of the fact that it is a nonweightbearing joint and is less constrained, and significant additional motion is afforded by the scapulothoracic articulation. 9 In addition, the shoulder is thought to have a greater vascular watershed. 6 Therefore, the treatment algorithm for humeral head ON is slightly different; often incorporating more conservative management. Core decompression for nontraumatic ON has been advocated for use in both the femoral and humeral heads. 3,5,9Y21 For accurate core decompression, several methods have been used to identify and confirm the area of necrotic bone. Preoperative evaluation uses imaging modalities including plain radiography, bone scans, and magnetic resonance imaging (MRI). Arthroscopy and/or biplanar fluoroscopy have been used intraoperatively to confirm lesion location. 11,19,22 Other studies have confirmed adequate decompression by using postoperative histology. 19,22 The goal of core decompression is to reduce the intraosseous/extravascular pressure to reestablish blood flow to the subchondral bone. Larsen 23 first observed Volume 9, Issue 1 23
2 Marchant et al TABLE 1. Demographic Data Shoulder Sex Age, y Diagnosis Etiology Shoulder Cruess stage Follow-up, mo Arthroplasty 1 F 45 Intra-articular injection CS L 1 2 NA 2 F 34 Intracerebral hemorrhage CS R 2 72 No 3 F 30 Sickle cell disease SCD L No 4 F 28 Sickle cell disease CS/SCD L 2 68 No 5 M 27 Autoimmune pericarditis CS L 3 60 No 6 F 43 Anaplastic ependymoma CS L 5 12 Yes 7* M 43 Leukemia CS R No 8* M 46 Leukemia CS L NA 9 F 44 Asthma CS L No 10 F 35 Hemolytic anemia CS R No 11 M 27 Meningioma CS L 2 44 No 12 M 42 Acoustic neuroma CS R 2 5 NA *Same patient. F indicates female; M, male; CS, corticosteroid use; SCD, sickle cell disease; L, left; R, right; NA, follow-up data less than 12 months. the relationship between bone ischemia and increased intramedullary pressure in Corticosteroid usey, alcohol abusey, Sickle cell diseasey, and Gaucher diseasey related ON have elevated intraosseous pressure as part of their proposed pathophysiologies. 2 Measurement of intramedullary pressure to identify ON has been demonstrated in the proximal femur but not in the humeral head. 9Y13,17 By identifying the region of maximum pressure within the bone, the accuracy of lesion identification and decompression could increase. The purpose of this study is to describe and evaluate the method of a modified technique for humeral head core decompression using combined biplanar fluoroscopy and intraosseous pressure monitoring to more accurately identify the regions of ON for targeted decompression. METHODS Patient records from November 2000 to October 2006 were retrospectively reviewed to identify patients who underwent pressure-guided core decompression for nontraumatic humeral head ON. Institutional review board approval was obtained to perform the chart and radiographic review. Twelve shoulders (11 patients) were identified as being treated with pressure-guided core decompression, and the intramedullary pressure data were available. Patient demographic data are summarized in Table 1. Evaluation All patients were evaluated preoperatively by plain radiography, and most patients had an MRI study. The most common reported risk factor for developing nontraumatic ON was corticosteroid use (11 of 12 shoulders). Core decompression had been advocated previously for patients with Cruess 1 modified stage 1, 2, and 3 disease of the humeral head. 2,3,5,19Y22 Stage 2 ON was the most common disease severity (7 shoulders) in our cohort, but all stages of disease were treated. The patient with stage 5 disease had multifocal ON with glenoid involvement but no collapse of the humeral head. FIGURE 1. Jamshidi bone marrow biopsy needle (top) and acorn-style reamer (bottom). FIGURE 2. Arterial pressure tubing connected to the bone biopsy needle. 24 Techniques in Shoulder & Elbow Surgery
3 Pressure-Guided Humeral Core Decompression FIGURE 3. Intramedullary pressure recordings. Entry pressure wave (A) and lesion pressure wave (B). Arrows mark the period of equilibrium. The primary chief complaint was pain. Patients were maximized with nonoperative treatment before consideration for core decompression. All patients were educated regarding risk factors. Patient symptoms were generally managed with a nonsteroidal anti-inflammatory and activity modification for 6 to 12 weeks. Because the superior central portion of the humeral head is the most common region affected, patients are advised to avoid overhead activities. Exercises to help patients maintain motion were used when necessary, with or without physical therapy assistance. Corticosteroid injections were generally avoided in patients with early stage disease to avoid the potential of disease progression. OPERATIVE TECHNIQUE The operative procedure was modified from a technique described by Ficat and Arlet 9 in the evaluation of femoral head ON and Downey et al 24 in a biomechanical study evaluating femoral head pressure during variable joint loading. Specific instruments used are shown in Figure 1; the operative sequence is shown in Figures 2 to 5. All patients received either general or regional anesthesia with sedation. Patients were placed in a beach-chair position. The fluoroscopy C-arm was positioned before preparing and draping to allow for intraoperative imaging. During positioning of the fluoroscopy machine, the C- arm was inverted, so that the ring was facing the ceiling, and the open portion was facing the floor. The shoulder was positioned within the radiographic field, so that the humeral head was easily visualized. Anteroposterior and lateral views of the humeral head could then be obtained simply by internally and externally rotating the arm. Once the shoulder and extremity were prepared in the standard sterile fashion, sterile U-drapes were placed on the shoulder, with the superior U-drape arranged over the top of the C-arm. Therefore, the entire case could proceed without having to move the patient or the C-arm machine to obtain fluoroscopic imaging. Before decompression, a diagnostic shoulder arthroscopy was performed to rule out significant intraarticular FIGURE 4. Guidance of the bone biopsy needle using fluoroscopic guidance. FIGURE 5. Acorn-style reamer used to decompress the lesion under fluoroscopic guidance. Volume 9, Issue 1 25
4 Marchant et al FIGURE 6. Preoperative MRI study showing region of ON. pathology including unstable cartilage flaps or articular collapse. No cartilage flaps or loose fragments were removed before proceeding with the decompression. Although the purpose of the arthroscopy was not for lesion identification, the cartilage overlying the suspected lesion was observed to be abnormal in several patients. Instead of its typical smooth appearance, the articular cartilage demonstrated macroscopic changes consistent with Outerbridge grade 1 chondromalacia. More specifically, it had a dimpled texture similar to peau d orange skin changes seen in thyroid disease and certain types of breast carcinoma. A 1-cm longitudinal incision was then made over the lateral humerus, 4 cm from the lateral edge of the acromion to avoid injury to the axillary nerve. With most lesions located on the superior aspect of the articular surface,thisstartingpointallowedforgoodaccesstothe lesion while staying within the safe area of the deltoid. 25 Through this incision, under fluoroscopic guidance, a Jamshidi bone marrow biopsy needle with a FIGURE 7. Postoperative MRI at 2 years, demonstrating resolution of ON and core decompression tract. stylus (Cardinal Health, Toronto, Ontario, Canada) was introduced through the lateral cortex. The stylus was removed, and an arterial pressure transducer was connected to the needle (Fig. 2). An intramedullary sinusoidal pressure wave was observed at the entry point and allowed to achieve equilibrium (Fig. 3A). Pressure readings were recorded from the arterial pressure monitor during the equilibrium period. The stylus was then reinserted. Under biplanar fluoroscopic guidance, a small mallet was used to slowly advance the needle to within 2 to 4 mm of the articular surface. Fluoroscopy was used to both assist with needle positioning within the osteonecrotic lesion and to monitor the advancement of the needle to avoid penetration of the articular surface. Several passes into the lesion were made with intermittent pressure monitoring at several sites within the subchondral bone (Fig. 4). Areas of increased intramedullary pressure within the lesion were located. On the pressure monitor, the intralesional pressure wave rose substantially and TABLE 2. Operative Data Shoulder No. Entry pressure, mm Hg Lesion pressure, mm Hg Pressure difference, mm Hg Lesion/entry ratio * * Average Maximum Minimum *Same patient. 26 Techniques in Shoulder & Elbow Surgery
5 Pressure-Guided Humeral Core Decompression FIGURE 8. Postoperative radiograph at 6 years demonstrating no articular collapse. remained high after achieving equilibrium (Fig. 3B). Once the area of peak pressure was identified, the arterial line was disconnected, and a guide wire was passed through the needle to the area of greatest pressure. Fluoroscopy was used additionally to ensure that the bone biopsy needle and the guide wire did not violate the glenohumeral joint. Subsequently, the bone biopsy needle was removed, and 2 passes with an acorn-style reamer (5Y7.5 mm) were performed to decompress the area of intramedullary hypertension (Fig. 5). The size of the reamer was determined based on the size of the lesion. Reamers greater than 7.5 mm were not used so as to avoid creating a large hole on the lateral cortex of the humerus. For that same reason, we avoided more than 1 entry site for the decompression. In 3 patients with large areas of ON, the needle and guide wire were redirected to another part of the lesion, and a second reaming occurred. This was easily performed through the initial lateral entry hole. The decision to make a second reaming was subjectively determined by the surgeon (C.J.B.). Generally, a second reaming was used if the size of the lesion was particularly large or if the first reamer selected was too small. Upon completion of the decompression, the instruments were then removed, and the wound was irrigated and closed in a standard layered fashion. Postoperative Care All patients were placed in a sling initially and instructed to wear it for 3 to 5 days postoperatively. Pendulum exercises were initiated on postoperative day 1 or 2. Patients were then instructed to progress slowly in terms of their range of motion with no overhead activity or strenuous activity for at least 6 weeks. At the 6-week mark, patients could transition to activity as tolerated. Analysis Entry and maximum intralesional intraosseous pressures were recorded for each patient. All patients were evaluated for pain relief, disease progression, and the need for arthroplasty. Preoperative and postoperative Visual Analog Scale (VAS) pain scores were recorded to evaluate pain relief. Progression to arthroplasty was considered to be the end point of the clinical course and conservative treatment strategies in previous studies evaluating core decompression 15,19,20,22 and subsequently was the final outcome measure. All 12 shoulders were evaluated at 6 months, and 9 of the 12 shoulders, received longterm follow-up for an average of 44.2 months (range, 12Y72.5 months) postoperative. Using a paired t test (GraphPad Software, San Diego, Calif), pressure differences and pain scores were compared preoperatively and postoperatively. A P G 0.05 was determined to be statistically significant. RESULTS There were no complications noted with the operative technique. Operative data, including pressure recordings, are displayed in Table 2. The average difference between thepeaklesionpressureandtheentrypressureswas mm Hg, with a 95% confidence interval (CI) from to mm Hg, and was found to be statistically significant (P G ). The average ratio of FIGURE 9. Postoperative MRI at 6 years confirming no articular incongruity. Volume 9, Issue 1 27
6 Marchant et al intramedullary lesion pressure to intramedullary entry pressure was 6.1, with a 95% CI ranging from 4.0 to 8.2. Patients generally reported good subjective clinical resultsinregardtopainrelief,oftenwithindaysofsurgery. The average preoperative and postoperative VAS pain scores at 6 months for all 12 patients were 7.4 (range, 5Y10; 95% CI, 6.5Y8.3) and 2.2 (range, 0Y8; 95% CI, 0.8Y3.6), respectively. At 6 months, pressureguided core decompression provided an average reduction in VAS pain score of 70.3% (P G ). The average postoperative pain score in 9 patients with follow-up of 1 year or more was 3.2 (range, 0Y10; 95% CI, 1.2Y6), which provided an average reduction of pain scores of 56.8% (P G 0.008). Of the 9 shoulders with long-term follow-up, only 2 patients have reported significant pain returning after surgery. One patient did very well for 4 years, with VAS pain scores remaining less than 4. At 5 years postsurgery, his radiographs did not demonstrate collapse but did show changes consistent with osteoarthritis. The other patient whose symptoms returned had complete pain relief for 11 months postsurgery. She eventually progressed to shoulder arthroplasty at exactly 1 year after the core decompression. The overall incidence of progression to arthroplasty was 11.1%, with 95% CI of to Although not all of the patients in our cohort received postoperative MRI studies, Figures 6 and 7 demonstrate the effect of targeted decompression. The preoperative lesion seen in Figure 6 has improved or, at the very least, has not progressed at the 2-year follow-up point shown in Figure 7. One can also identify the tracts from the core decompression hitting the osteonecrotic target site within the humeral head. Figures 8 and 9 show the radiographic and MRI image of another patient 6 years postsurgery. No appreciable collapse or articular damage can be identified. DISCUSSION The purpose of this report was to describe a means of identifying the region of ON during core decompression of the humeral head. Specifically, in regard to ON of the humeral head, localization of the osteonecrotic lesion has been previously accomplished via indirect methods such as preoperative MRI and intraoperative fluoroscopy. 19,22 Mont et al, 19 in 1993, first described the use of core decompression for nontraumatic humeral ON. The technique was performed using a modified deltopectoral approach through the anterior axillary fold using fluoroscopy as the primary means of lesion identification. Since that time, arthroscopy has been used to assist with lesion identification. 11,15 Arthroscopic debridement has also been described as an alternate treatment modality. 26 In review of the literature, this marks the first attempt at intraosseous pressure monitoring through a small lateral incision for humeral head during core decompression. The use of intramedullary pressure monitoring, however, is not new. Several authors have used varying techniques of pressure monitoring in regard to ON of the proximal femur. 10,12Y14 Authors including Ficat, 12 Ficat and Arlet, 9 and Hungerford 14 have demonstrated a high correlation between elevated intramedullary pressures and biopsy-confirmed ON. Only Ficat and Arlet 9 have evaluated the pressure differential between entry and intralesional intramedullary pressure as a means to identify the osteonecrotic lesion. Our technique takes advantage of radiographic diagnosis using plain radiograph, scintigraphy, and MRI for initial lesion localization and further exploits the pressure differential between normal and diseased bone for targeted decompression. Our data from 12 shoulders undergoing core decompression demonstrates a direct and reproducible technique for intraoperative localization of necrotic bone within the humeral head. A statistically significant increase in intraoperative intramedullary pressure can be appreciated between the diseased bone and the normal bone of the proximal humerus. Furthermore, our data suggest that the osteonecrotic lesion within the humeral head would be identified by an approximate 4-fold rise in the intramedullary pressure. These findings compare with the data collected by Ficat and Arlet, 9 which show an approximate 2-fold increase in intramedullary pressures between normal and osteonecrotic bone of the proximal femur. When evaluating outcomes from core decompression, similar to the results seen in ON of the hip, core decompression of the proximal humerus has had mixed results. Results from the initial study by Mont et al 19 found overall 73% good-to-excellent results in 30 shoulders at 5 or more years, with the best outcomes seen in patients with precollapse disease. Eight of the 30 patients required arthroplasty, with 5 of 8 requiring replacement within 1 year after core decompression. L Insalata et al 15 performed core decompressions on 5 stage 3 patients with progressive disease, and progression was not altered. Four of the 5 patients required arthroplasty, and the fifth was a candidate for the procedure at the time of publication. LaPorte et al 22 reported expanded results from the cohort of Mont et al 19 to include 63 shoulders (43 patients) with 2- to 18-year follow-up. A result pattern similar to the initial study was seen. Good-to-excellent University of CaliforniaYLos Angeles shoulder scores reported in 46 of 56 shoulders with stage 1 to 3 disease. Of the 16 patients that failed, the average time to arthroplasty was 24 months. In evaluating our cohort of patients, it is easy to see that the procedure afforded significant pain relief. It is 28 Techniques in Shoulder & Elbow Surgery
7 Pressure-Guided Humeral Core Decompression also worth noting that patients with stage 1 to 5 disease were all represented in our cohort, and only 1 patient with stage 5 disease went on to require arthroplasty. Furthermore, the 1 patient who did fail decompression was on chronic corticosteroid therapy for a malignant brain tumor and had multifocal ON with progressive glenoid disease. Therefore, it is difficult to determine the origin of her shoulder pain at 1 year and if she truly failed because of humeral pathology. Core decompression of humeral head ON has been shown to offer patients relief of symptoms, particularly those with precollapse disease. The benefits of a pressure-guided technique for localizing osteonecrotic lesions are greater confidence in decompressing diseased versus normal bone, thereby improving the decompression yields; small incisions; and a reduced need for additional indirect studies including the use of excessive fluoroscopy. It is still uncertain whether core decompression alters the natural history of ON, but this technique does not seem to negatively affect the clinical course or patient outcomes. Early clinical results from our study group suggest that this technique is successful in reducing pain symptoms at both short- and long-term follow-up. The incidence of conversion to arthroplasty was comparable to, if not lower than, other case series reported in the literature. Disadvantages of the procedure seem to be limited to the risks of surgery and the possible violation of the articular cartilage with the bone marrow biopsy needle. We did not encounter any of these complications in our study group. Further study will be needed to determine the accuracy and precision of this technique and whether pressureguided core decompression will delay or reduce the need for shoulder arthroplasty, resulting in significantly better clinical outcomes. ACKNOWLEDGMENT The authors thank Robin M. Queen, PhD, for assistance with our statistical evaluation. REFERENCES 1. Cruess RL. Experience with steroid-induced avascular necrosis of the shoulder and etiologic considerations regarding osteonecrosis of the hip. Clin Orthop Relat Res. 1978;130:86Y Cushner MA, Friedman RJ. Osteonecrosis of the humeral head. J Am Acad Orthop Surg. 1997;5:339Y Hasan SS, Romeo AA. Nontraumatic osteonecrosis of the humeral head. J Shoulder Elbow Surg. 2002;11:281Y Rutherford C, Cofield RH. Osteonecrosis of the shoulder. Orthop Trans. 1987;11: Sarris I, Weiser R, Sotereanos DG, et al. Pathogenesis and treatment of osteonecrosis of the shoulder. Orthop Clin North Am. 2004;35:397Y Usher BW Jr, Friedman RJ. Steroid-induced osteonecrosis of the humeral head. Orthopedics. 1995;18:47Y Hattrup SJ, Cofield RH. Osteonecrosis of the humeral head: relationship of disease stage, extent, and cause to natural history. J Shoulder Elbow Surg. 1999;8: 559Y Heimann WG, Freiberger RH. Avascular necrosis of the femoral and humeral heads after high-dosage corticosteroid therapy. N Engl J Med. 1960;263:672Y Ficat RP, Arlet J. Treatment of bone ischemia and necrosis. In: Hungerford DS, ed. Ischemia and Necrosis of Bone. Baltimore: Williams and Wilkins; 1980:171Y Camp JF, Colwell CW. Core decompression of the femoral head for osteonecrosis. J Bone Joint Surg Am. 1986;68A: 1313Y Chapman C, Mattern C, Levine WN. Arthroscopically assisted core decompression of the proximal humerus for avascular necrosis. Arthroscopy. 2004;20:1003Y Ficat RP. Idiopathic bone necrosis of the femoral head: early diagnosis and treatment. J Bone Joint Surg Br. 1985; 67:3Y Hopson CN, Silverhus SW. Ischemic necrosis of the femoral head: treatment by core decompression. J Bone Joint Surg Am. 1988;70:1048Y Hungerford DS. Bone marrow pressure, venography, and core decompression in ischemic necrosis of the femoral head. In: Sledge CB, ed. The Hip: Proceedings of the Seventh Open Scientific Meeting of the Hip Society. St. Louis: C.V. Mosby; 1979:218Y L Insalata JC, Pagnani MJ, Dines DM, et al. Humeral head osteonecrosis: clinical course and radiographic predictors of outcome. J Shoulder Elbow Surg. 1996;5:355Y Loebenberg MI, Plate AM, Zuckerman JD. Osteonecrosis of the humeral head. Instr Course Lect. 1999;48: 349Y Meyers MH. Osteonecrosis of the femoral head: pathogenesis and long-term results of treatment. Clin Orthop Relat Res. 1988;231:51Y Mont MA, Hungerford DS. Non-traumatic avascular necrosis of the femoral headvcurrent concepts review. J Bone Joint Surg Am. 1995;77:459Y Mont MA, Maar DC, Urquhart M, et al. Avascular necrosis of the humeral head treated by core decompressionva retrospective review. J Bone Joint Surg Br. 1993;75B: 785Y Mont MA, Jacque HP, Mohan V, et al. The results of core decompression for avascular necrosis of the humeral head. Specialty Society Day, American Shoulder and Elbow Society, American Academy of Orthopaedic Surgeons 1997 Annual Meeting; February 1997; San Francisco, CA. 21. Urquart MW, Mont MA, Maar DC, et al. Results of core Volume 9, Issue 1 29
8 Marchant et al decompression for avascular necrosis of the humeral head. Orthop Trans. 1992;16: LaPorte DM, Mont MA, Mohan V, et al. Osteonecrosis of the humeral head treated by core decompression. Clin Orthop Relat Res. 1998;355:254Y Larsen RM. Intramedullary pressure with particular reference to massive diaphyseal bone necrosis: experimental observations. Ann Surg. 1938;108: Downey DJ, Simkin PA, Taggart R. The effect of compressive loading on intraosseous pressure in the femoral head in vitro. J Bone Joint Surg Am. 1988;70A: 871Y Cetik O, Murad U, Halil IA, et al. Is there a safe area for the axillary nerve in the deltoid muscle? A cadaveric study. J Bone Joint Surg Am. 2006;88:2395Y Hardy P, Decrette E, Jeanrot C, et al. Arthroscopic treatment of bilateral humeral head osteonecrosis. Arthroscopy. 2000;16:332Y Techniques in Shoulder & Elbow Surgery
Atraumatic Osteonecrosis of the Humeral Head. Vascular Anatomy
 6 Atraumatic Osteonecrosis of the Humeral Head Konrad I. Gruson, M.D., and Young W. Kwon, M.D., Ph.D. Abstract While much literature has focused on the management of osteonecrosis of the femoral head,
6 Atraumatic Osteonecrosis of the Humeral Head Konrad I. Gruson, M.D., and Young W. Kwon, M.D., Ph.D. Abstract While much literature has focused on the management of osteonecrosis of the femoral head,
Materials and methods. Table I. 2 J.W. Uribe, A.B.-van Bemden
 2 J.W. Uribe, A.B.-van Bemden Table I Stage I Stage II Stage III Stage IV Stage V Cruess classification for osteonecrosis of humeral head Preradiographic, requires magnetic resonance imaging, bone scan,
2 J.W. Uribe, A.B.-van Bemden Table I Stage I Stage II Stage III Stage IV Stage V Cruess classification for osteonecrosis of humeral head Preradiographic, requires magnetic resonance imaging, bone scan,
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
A Patient s Guide to Osteonecrosis of the Humeral Head
 A Patient s Guide to Osteonecrosis of the Humeral Head 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
A Patient s Guide to Osteonecrosis of the Humeral Head 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Osteonecrosis of the humeral head
 Review Article Osteonecrosis of the Humeral Head Kevin L. Harreld, MD* David R. Marker, BS* Ethan R. Wiesler, MD Babar Shafiq, MD Michael A. Mont, MD * Dr. Harreld and Mr. Marker contributed equally as
Review Article Osteonecrosis of the Humeral Head Kevin L. Harreld, MD* David R. Marker, BS* Ethan R. Wiesler, MD Babar Shafiq, MD Michael A. Mont, MD * Dr. Harreld and Mr. Marker contributed equally as
Osteochondritis dissecans (OCD) lesions of the knee
 Extra-articular, Intraepiphyseal Drilling for Osteochondritis Dissecans of the Knee Andrew T. Pennock, M.D., James D. Bomar, M.P.H., and Henry G. Chambers, M.D. Abstract: Symptomatic osteochondritis dissecans
Extra-articular, Intraepiphyseal Drilling for Osteochondritis Dissecans of the Knee Andrew T. Pennock, M.D., James D. Bomar, M.P.H., and Henry G. Chambers, M.D. Abstract: Symptomatic osteochondritis dissecans
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Idiopathic osteonecrosis of the medial tibial plateau
 Idiopathic osteonecrosis of the medial tibial plateau J. R. Valenti J. A. Illescas A. Barriga R. Dölz ABSTRACT Osteonecrosis of the medial tibial plateau is characterized by acute pain on the medial aspect
Idiopathic osteonecrosis of the medial tibial plateau J. R. Valenti J. A. Illescas A. Barriga R. Dölz ABSTRACT Osteonecrosis of the medial tibial plateau is characterized by acute pain on the medial aspect
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study
 Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Correspondence should be addressed to Takeshi Makihara;
 Hindawi Case Reports in Orthopedics Volume 2017, Article ID 4898057, 8 pages https://doi.org/10.1155/2017/4898057 Case Report Autologous Concentrated Bone Marrow Grafting for the Treatment of Osteonecrosis
Hindawi Case Reports in Orthopedics Volume 2017, Article ID 4898057, 8 pages https://doi.org/10.1155/2017/4898057 Case Report Autologous Concentrated Bone Marrow Grafting for the Treatment of Osteonecrosis
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Index. orthopedic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acetabular fractures pediatric, 494 498 classification of, 494 diagnostic imaging of, 494, 496 497 epidemiology of, 494 treatment of, 494 498
Note: Page numbers of article titles are in boldface type. A Acetabular fractures pediatric, 494 498 classification of, 494 diagnostic imaging of, 494, 496 497 epidemiology of, 494 treatment of, 494 498
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure)
 Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Not relevant to this presentation.
 Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy
 The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Arthritis of the Shoulder
 Page 1 of 7 Arthritis of the Shoulder This article is also available in Spanish: Artritis del hombro (Arthritis of the Shoulder) (topic.cfm?topic=a00723). In 2011, more than 50 million people in the United
Page 1 of 7 Arthritis of the Shoulder This article is also available in Spanish: Artritis del hombro (Arthritis of the Shoulder) (topic.cfm?topic=a00723). In 2011, more than 50 million people in the United
Osteonecrosis - Spectrum of imaging findings
 Osteonecrosis - Spectrum of imaging findings Poster No.: C-1861 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Ninitas, A. L. Amado Costa, A. Duarte, I. Távora ; Lisbon/ 1 1 2 1 1 2 PT, Costa
Osteonecrosis - Spectrum of imaging findings Poster No.: C-1861 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Ninitas, A. L. Amado Costa, A. Duarte, I. Távora ; Lisbon/ 1 1 2 1 1 2 PT, Costa
URSA HEMI-SHOULDER ARTHROPLASTY B I O T E K
 URSA HEMI-SHOULDER ARTHROPLASTY SURGICAL TECHNIQUE B I O T E K 2 Surgical Position Once general anesthesia has been satisfactorily induced, or a supraclavicular nerve block has been given, the patient
URSA HEMI-SHOULDER ARTHROPLASTY SURGICAL TECHNIQUE B I O T E K 2 Surgical Position Once general anesthesia has been satisfactorily induced, or a supraclavicular nerve block has been given, the patient
Part II: Rotator Cuff Repair, Day of Surgery and Postoperative Course
 Part II: Rotator Cuff Repair, Day of Surgery and Postoperative Course Benjamin W. Sears, MD 303-321-1333 western-ortho.com denvershoulder.com Day of Surgery Most patients will undergo outpatient surgery
Part II: Rotator Cuff Repair, Day of Surgery and Postoperative Course Benjamin W. Sears, MD 303-321-1333 western-ortho.com denvershoulder.com Day of Surgery Most patients will undergo outpatient surgery
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
The Kienböck disease and scaphoid fractures. Mariusz Bonczar
 The Kienböck disease and scaphoid fractures Mariusz Bonczar The Kienböck disease and scaphoid fractures Mariusz Bonczar Kienböck disease personal experience My special interest for almost 25 years Thesis
The Kienböck disease and scaphoid fractures Mariusz Bonczar The Kienböck disease and scaphoid fractures Mariusz Bonczar Kienböck disease personal experience My special interest for almost 25 years Thesis
A Patient s Guide to Adult Proximal Humerus (Shoulder) Fractures
 A Patient s Guide to Adult Proximal Humerus (Shoulder) Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER:
A Patient s Guide to Adult Proximal Humerus (Shoulder) Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER:
Case Study: David. Conditions Treated Femoral Neck Fracture with Avascular Necrosis of the Hip. Age Range During Treatment 16 Years
 Case Study: David Conditions Treated Femoral Neck Fracture with Avascular Necrosis of the Hip Age Range During Treatment 16 Years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of
Case Study: David Conditions Treated Femoral Neck Fracture with Avascular Necrosis of the Hip Age Range During Treatment 16 Years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of
Noncemented Total Hip Arthroplasty for Osteonecrosis of the Femoral Head in Elderly Patients
 Noncemented Total Hip Arthroplasty for Osteonecrosis of the Femoral Head in Elderly Patients Ta-I Wang, MD; Shih-Hsin Hung, RN, MSN; Yu-Ping Su, MD; Chi-Quang Feng, MD; Fang-Yao Chiu, MD; Chien-Lin Liu,
Noncemented Total Hip Arthroplasty for Osteonecrosis of the Femoral Head in Elderly Patients Ta-I Wang, MD; Shih-Hsin Hung, RN, MSN; Yu-Ping Su, MD; Chi-Quang Feng, MD; Fang-Yao Chiu, MD; Chien-Lin Liu,
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
A Patient s Guide to Quadrilateral Space Syndrome
 A Patient s Guide to Quadrilateral Space Syndrome Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this
A Patient s Guide to Quadrilateral Space Syndrome Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
DK7215-Levine-ch12_R2_211106
 12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
Synovial Chondromatosis Associated with Polyarteritis Nodosa
 Synovial Chondromatosis Associated with Polyarteritis Nodosa Hywel Davies BSc ( ),Andrew J Unwin BSc, Nick P H Morgan BSc Windsor Knee Clinic, Windsor, United Kingdom Correspondence: Hywel Davies, Windsor
Synovial Chondromatosis Associated with Polyarteritis Nodosa Hywel Davies BSc ( ),Andrew J Unwin BSc, Nick P H Morgan BSc Windsor Knee Clinic, Windsor, United Kingdom Correspondence: Hywel Davies, Windsor
Anatomy Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
 Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints combined with tendons and muscles that allow a great
Introduction & Question 1
 Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
A Patient s Guide to Anatomic Total Shoulder Replacement (Standard Shoulder Shoulder)
 A Patient s Guide to Anatomic Total Shoulder Replacement (Standard Shoulder Shoulder) Introduction Yearly, there are approximately 50,000 shoulder replacements performed annually in the USA. Anatomic shoulder
A Patient s Guide to Anatomic Total Shoulder Replacement (Standard Shoulder Shoulder) Introduction Yearly, there are approximately 50,000 shoulder replacements performed annually in the USA. Anatomic shoulder
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
A Technique To Retrieve A Broken Probe During Shoulder Arthroscopy: A Technical Tip
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 22 Number 1 A Technique To Retrieve A Broken Probe During Shoulder Arthroscopy: A Technical Tip A Yewlett, A Bhattacharjee, H Mehta, R Kulkarni
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 22 Number 1 A Technique To Retrieve A Broken Probe During Shoulder Arthroscopy: A Technical Tip A Yewlett, A Bhattacharjee, H Mehta, R Kulkarni
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Interesting Case Series. Simultaneous Avascular Necrosis of the Lunate and Scaphoid
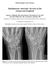 Interesting Case Series Simultaneous Avascular Necrosis of the Lunate and Scaphoid Benson J. Pulikkottil, MD, Edward Ruane, MD, Michael E. Scott, DO, Alexandre Philipp Sater, BS, and Joseph E. Imbriglia,
Interesting Case Series Simultaneous Avascular Necrosis of the Lunate and Scaphoid Benson J. Pulikkottil, MD, Edward Ruane, MD, Michael E. Scott, DO, Alexandre Philipp Sater, BS, and Joseph E. Imbriglia,
MRI Evaluation of Post Core Decompression Changes in Avascular Necrosis of Hip
 Original Article MRI Evaluation of Post Core Decompression Changes in Avascular Necrosis of Hip DOI: 10.7860/JCDR/2015/13995.6967 Radiology Section Madhavi Nori 1, Sravan Kumar Marupaka 2, Swathi Alluri
Original Article MRI Evaluation of Post Core Decompression Changes in Avascular Necrosis of Hip DOI: 10.7860/JCDR/2015/13995.6967 Radiology Section Madhavi Nori 1, Sravan Kumar Marupaka 2, Swathi Alluri
Common Shoulder Problems and Treatment Options. Benjamin W. Szerlip D.O. Austin Shoulder Institute
 Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Mid-term Outcomes of Arthroscopic-Assisted Core Decompression of Pre-collapse Osteonecrosis of Femoral Head Minimum of 5 Year Follow-up
 Arthroscopic-Assisted Core Decompression of Pre-collapse Osteonecrosis of Femoral Head Minimum of 5 Year Follow-up Mark R. Nazal*, Ali Parsa, Scott D. Martin Sports Medicine, Department of Orthopaedic
Arthroscopic-Assisted Core Decompression of Pre-collapse Osteonecrosis of Femoral Head Minimum of 5 Year Follow-up Mark R. Nazal*, Ali Parsa, Scott D. Martin Sports Medicine, Department of Orthopaedic
Arthritis of the Shoulder
 Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
The utility of hip arthroscopy has certainly increased
 Hip Arthroscopy and the Anterolateral Portal: Avoiding Labral Penetration and Femoral Articular Injuries Stephen Kenji Aoki, M.D., James Thomas Beckmann, M.D., and James Derek Wylie, M.D. Abstract: Establishing
Hip Arthroscopy and the Anterolateral Portal: Avoiding Labral Penetration and Femoral Articular Injuries Stephen Kenji Aoki, M.D., James Thomas Beckmann, M.D., and James Derek Wylie, M.D. Abstract: Establishing
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease
 Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Speaker s Disclosure Statement. Starvation, Death and Destruction: The Battlefield of AVN. Objectives. Risk Factors
 Starvation, Death and Destruction: The Battlefield of AVN Speaker s Disclosure Statement I have no industry relationships to disclose I will discuss off-label use of medications Dana-Farber/Boston Children
Starvation, Death and Destruction: The Battlefield of AVN Speaker s Disclosure Statement I have no industry relationships to disclose I will discuss off-label use of medications Dana-Farber/Boston Children
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D.
 Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
A Patient s Guide to Adult Proximal Humerus (Shoulder) Fractures
 A Patient s Guide to Adult Proximal Humerus (Shoulder) Fractures 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com 1 DISCLAIMER: The information in this booklet
A Patient s Guide to Adult Proximal Humerus (Shoulder) Fractures 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com 1 DISCLAIMER: The information in this booklet
Does the self-centering mechanism of bipolar hip endoprosthesis really work in vivo?
 Journal of Orthopaedic Surgery 2005;13(1):46-51 Does the self-centering mechanism of bipolar hip endoprosthesis really work in vivo? H Tsumura, N Kaku, T Torisu Department of Orthopedic Surgery, Oita University,
Journal of Orthopaedic Surgery 2005;13(1):46-51 Does the self-centering mechanism of bipolar hip endoprosthesis really work in vivo? H Tsumura, N Kaku, T Torisu Department of Orthopedic Surgery, Oita University,
Unicameral bone cysts are benign, fluid-filled cavities
 Endoscopic Surgery for Symptomatic Unicameral Bone Cyst of the Proximal Femur Wataru Miyamoto, M.D., Masato Takao, M.D., Youichi Yasui, M.D., Shinya Miki, M.D., and Takashi Matsushita, M.D. Abstract: Recently,
Endoscopic Surgery for Symptomatic Unicameral Bone Cyst of the Proximal Femur Wataru Miyamoto, M.D., Masato Takao, M.D., Youichi Yasui, M.D., Shinya Miki, M.D., and Takashi Matsushita, M.D. Abstract: Recently,
Screening for and Assessment of Osteonecrosis in Oncology Patients. Sue C. Kaste, DO SPR Postgraduate Course 2015
 Screening for and Assessment of Osteonecrosis in Oncology Patients Sue C. Kaste, DO SPR Postgraduate Course 2015 The author declares no potential conflicts of interest or financial disclosures Osteonecrosis
Screening for and Assessment of Osteonecrosis in Oncology Patients Sue C. Kaste, DO SPR Postgraduate Course 2015 The author declares no potential conflicts of interest or financial disclosures Osteonecrosis
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Shoulder Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Compiled by Rob Liddell,
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Shoulder Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Compiled by Rob Liddell,
A Patient s Guide to Avascular Necrosis of the Hip
 A Patient s Guide to Avascular Necrosis of the Hip 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Avascular Necrosis of the Hip 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
EVIDENCE BASED MEDICINE VOICE
 EVIDENCE BASED MEDICINE VOICE Orthofix approach to Evidence Based Medicine: For years, clinical decision-making was based primarily on physician knowledge and expert opinion. Now, the medical community
EVIDENCE BASED MEDICINE VOICE Orthofix approach to Evidence Based Medicine: For years, clinical decision-making was based primarily on physician knowledge and expert opinion. Now, the medical community
AcUMEDr. LoCKING CLAVICLE PLATE SYSTEM
 AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
Rotator Cuff Tears: Surgical Treatment Options
 Rotator Cuff Tears: Surgical Treatment Options The following article provides in depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article "Rotator Cuff
Rotator Cuff Tears: Surgical Treatment Options The following article provides in depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article "Rotator Cuff
Locked Plating of 3- and 4-Part Proximal Humerus Fractures in Older Patients: The Effect of Initial Fracture Pattern on Outcome
 ORIGINAL ARTICLE Locked Plating of 3- and 4-Part Proximal Humerus Fractures in Older Patients: The Effect of Initial Fracture Pattern on Outcome Brian D. Solberg, MD,* Charles N. Moon, MD, Dennis P. Franco,
ORIGINAL ARTICLE Locked Plating of 3- and 4-Part Proximal Humerus Fractures in Older Patients: The Effect of Initial Fracture Pattern on Outcome Brian D. Solberg, MD,* Charles N. Moon, MD, Dennis P. Franco,
Femoral Head Osteonecrosis in Military Training Recruits: A Report of Two Cases
 MILITARY MEDICINE, 174, 11:1231, 2009 Femoral Head Osteonecrosis in Military Training Recruits: A Report of Two Cases Capt Susan M. Eckert, USAF MC * ; Maj Meredith Warner, USAF MC ; Lt Col James A. Keeney,
MILITARY MEDICINE, 174, 11:1231, 2009 Femoral Head Osteonecrosis in Military Training Recruits: A Report of Two Cases Capt Susan M. Eckert, USAF MC * ; Maj Meredith Warner, USAF MC ; Lt Col James A. Keeney,
Samuel A. Dubrow, MD Division of Shoulder & Elbow Surgery Department of Orthopaedics Alegent Creighton Clinic Creighton University School of Medicine
 Samuel A. Dubrow, MD Division of Shoulder & Elbow Surgery Department of Orthopaedics Alegent Creighton Clinic Creighton University School of Medicine Education 8/2003 5/2007 (M.D) Creighton University
Samuel A. Dubrow, MD Division of Shoulder & Elbow Surgery Department of Orthopaedics Alegent Creighton Clinic Creighton University School of Medicine Education 8/2003 5/2007 (M.D) Creighton University
A Patient s Guide to Rotator Cuff Tendinitis or Shoulder Impingement
 A Patient s Guide to Rotator Cuff Tendinitis or Shoulder Impingement Introduction Shoulder pain is a common condition whether due to aging, overuse, trauma or a sports injury. Shoulder pain and injuries
A Patient s Guide to Rotator Cuff Tendinitis or Shoulder Impingement Introduction Shoulder pain is a common condition whether due to aging, overuse, trauma or a sports injury. Shoulder pain and injuries
Percutaneous Humeral Fracture Repair Surgical Technique
 Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Massive Rotator Cuff Tears. Rafael M. Williams, MD
 Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
A Patient s Guide to Rotator Cuff Repair Surgery
 NewYork-Presbyterian Columbia ORTHOPAEDICS A Patient s Guide to Rotator Cuff Repair Surgery NewYork-Presbyterian Columbia ORTHOPAEDICS The Rotator Cuff At Columbia Orthopaedics, patients find nationally
NewYork-Presbyterian Columbia ORTHOPAEDICS A Patient s Guide to Rotator Cuff Repair Surgery NewYork-Presbyterian Columbia ORTHOPAEDICS The Rotator Cuff At Columbia Orthopaedics, patients find nationally
Biceps Tendon Rupture
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about Biceps Tendon Rupture must be made in conjunction with your Physician or a
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about Biceps Tendon Rupture must be made in conjunction with your Physician or a
Case Dysbaric osteonecrosis of the humerus
 Case 14398 Dysbaric osteonecrosis of the humerus Magdalena Posadzy 1, Nicolas De Vos 2, 3, Filip Vanhoenacker2, 3, 4 1. W. Dega Orthopaedic and Rehabilitation University Hospital, Karol Marcinkowski University
Case 14398 Dysbaric osteonecrosis of the humerus Magdalena Posadzy 1, Nicolas De Vos 2, 3, Filip Vanhoenacker2, 3, 4 1. W. Dega Orthopaedic and Rehabilitation University Hospital, Karol Marcinkowski University
Asymptomatic acromioclavicular joint arthritis in arthroscopic rotator cuff tendon repair: a prospective randomized comparison study
 Arch Orthop Trauma Surg (2011) 131:363 369 DOI 10.1007/s00402-010-1216-y ARTHROSCOPY AND SPORTS MEDICINE Asymptomatic acromioclavicular joint arthritis in arthroscopic rotator cuff tendon repair: a prospective
Arch Orthop Trauma Surg (2011) 131:363 369 DOI 10.1007/s00402-010-1216-y ARTHROSCOPY AND SPORTS MEDICINE Asymptomatic acromioclavicular joint arthritis in arthroscopic rotator cuff tendon repair: a prospective
Shoulder hemiarthroplasty in the management of humeral head fractures
 Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS
 SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
SHOULDER IMPINGEMENT / ROTATOR CUFF TENDONITIS / SUBACROMIAL BURSITIS The terms impingement, rotator cuff tendonitis, and subacromial bursitis, all refer to a spectrum of the same condition. Anatomy The
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
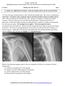 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 9/22/2012 Radiology Quiz of the Week # 91 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 9/22/2012 Radiology Quiz of the Week # 91 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6
 Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid
 The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid David R. J. Gill, MB, ChB, FRACS, a Robert H. Cofield, MD, b and Charles Rowland, MS, c Joondalup, Australia,
The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid David R. J. Gill, MB, ChB, FRACS, a Robert H. Cofield, MD, b and Charles Rowland, MS, c Joondalup, Australia,
Surgical Technique. Intramedullary locked Nailing With Screws for Humerus Fractures Solid/Cannulated. Humeral Interlocking Nail.
 Screws for Humerus Fractures Surgical Technique Humeral Interlocking Nail Approved by Humerus Nail Kit Code 08050001 Contents Introduction Implant design Indications Pre-operative planning Patient positioning
Screws for Humerus Fractures Surgical Technique Humeral Interlocking Nail Approved by Humerus Nail Kit Code 08050001 Contents Introduction Implant design Indications Pre-operative planning Patient positioning
Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty
 texas orthopaedic journal CASE REPORT Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty Gaurav S. Sharma, BA; Ronald W. Lindsey, MD Department of Orthopaedic Surgery
texas orthopaedic journal CASE REPORT Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty Gaurav S. Sharma, BA; Ronald W. Lindsey, MD Department of Orthopaedic Surgery
( 1 ) Ball and socket. Shoulder capsule. Rotator cuff.
 Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Shoulder Arthroscopy Page ( 1 ) Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, arthro
Shoulder Joint Replacement
 TREATMENT Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
TREATMENT Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
DOJ ABSTRACT. MATERIALS AND METHODS Following approval by our Institutional Review Board, we performed a search of our institution s perioperative
 10.5005/jp-journals-10017-1038 ORIGINAL Restoration RESEARCH of Shoulder Abduction after Radial to Axillary Nerve Transfer following Trauma or Shoulder Arthroplasty Restoration of Shoulder Abduction after
10.5005/jp-journals-10017-1038 ORIGINAL Restoration RESEARCH of Shoulder Abduction after Radial to Axillary Nerve Transfer following Trauma or Shoulder Arthroplasty Restoration of Shoulder Abduction after
Anatomical Shoulder Glenoid. Surgical Technique
 Anatomical Shoulder Glenoid Surgical Technique Anatomical Shoulder Glenoid Surgical Technique 3 Table of Contents Glenoid Preparation Surgical Steps 4 Anatomical Shoulder Glenoid 4 Glenoid Components
Anatomical Shoulder Glenoid Surgical Technique Anatomical Shoulder Glenoid Surgical Technique 3 Table of Contents Glenoid Preparation Surgical Steps 4 Anatomical Shoulder Glenoid 4 Glenoid Components
OPERATIVE TECHNIQUE GALAXY FIXATION SHOULDER
 OPERATIVE TECHNIQUE GALAXY FIXATION SHOULDER cop2 OPERATIVE TECHNIQUE INTRODUCTION 1 FEATURES OF SHOULDER COMPONENTS 2 EQUIPMENT REQUIRED 5 PREOPERATIVE PLANNING 6 SURGICAL PROCEDURE 8 POST OPERATIVE MANAGEMENT
OPERATIVE TECHNIQUE GALAXY FIXATION SHOULDER cop2 OPERATIVE TECHNIQUE INTRODUCTION 1 FEATURES OF SHOULDER COMPONENTS 2 EQUIPMENT REQUIRED 5 PREOPERATIVE PLANNING 6 SURGICAL PROCEDURE 8 POST OPERATIVE MANAGEMENT
STATE OF CONNECTICUT ETHICS BOARD NONE ARTHREX INC ARTHREX INC
 Rationale, Biomechanics,Early Results after Superior Capsular Reconstruction Augustus D Mazzocca MS, MD Director of the New England Musculoskeletal Institute Chairman Department of Orthopaedic Surgery
Rationale, Biomechanics,Early Results after Superior Capsular Reconstruction Augustus D Mazzocca MS, MD Director of the New England Musculoskeletal Institute Chairman Department of Orthopaedic Surgery
EXTENDED TROCHANTERIC OSTEOTOMY SURGICAL TECHNIQUE FPO EXTENSIVELY COATED FIXATION
 EXTENDED TROCHANTERIC OSTEOTOMY SURGICAL TECHNIQUE FPO EXTENSIVELY COATED FIXATION SINCE 1983 PREOPERATIVE PLANNING EXPLANTATION OPTIONS the cement from inside the cement canal until the bone/ cement bond
EXTENDED TROCHANTERIC OSTEOTOMY SURGICAL TECHNIQUE FPO EXTENSIVELY COATED FIXATION SINCE 1983 PREOPERATIVE PLANNING EXPLANTATION OPTIONS the cement from inside the cement canal until the bone/ cement bond
System. Humeral Nail. Surgical Technique
 System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
