ARTICLE. Effectiveness of Oral or Nebulized Dexamethasone for Children With Mild Croup
|
|
|
- Leon Morgan
- 5 years ago
- Views:
Transcription
1 ARTICLE Effectiveness of Oral or Nebulized Dexamethasone for Children With Mild Croup Joseph W. Luria, MD; Javier A. Gonzalez-del-Rey, MD; Gregg A. DiGiulio, MD; Constance M. McAneney, MD; Jennifer J. Olson, MD; Richard M. Ruddy, MD Objective: To assess the efficacy of oral dexamethasone or nebulized dexamethasone sodium phosphate in children with mild croup. Methods: Double-blind, placebo-controlled study of 264 children between 6 months and 6 years of age with symptoms of croup for fewer than 48 hours. Patients were excluded if they received racemic epinephrine or corticosteroid treatment. Other exclusion criteria included corticosteroid treatment during the 14 days prior to enrollment or complicating medical condition. Subjects randomly received oral dexamethasone (0.6 mg/kg), nebulized dexamethasone sodium phosphate (160 µg), or placebo. Telephone follow-up was obtained on days 1, 2, 3, 4, and 7. Main Outcome Measures: The primary outcome measure was treatment failure, defined as receiving corticosteroid or racemic epinephrine treatment during the 7 days after enrollment in the study. Secondary outcome measures included seeking additional care and the parental assessments of the patients condition obtained during follow-up (worse, same, better, or gone). Results: Eighty-five patients received oral dexamethasone, 91 received nebulized dexamethasone, and 88 received placebo. There were 3 treatment failures in the oral dexamethasone treated group, 12 in the nebulized dexamethasone treated group, and 10 in the placebo-treated group (P=.05). Ten children in the oral dexamethasone treated group sought additional care compared with 27 and 29 in the nebulized dexamethasone treated and placebotreated groups, respectively (P=.002). Parents of children in the oral dexamethasone treated group reported greater improvement on day 1 (P.001) compared with the nebulized dexamethasone treated and placebotreated groups. Conclusions: Children with mild croup who receive oral dexamethasone treatment are less likely to seek subsequent medical care and demonstrate more rapid symptom resolution compared with children who receive nebulized dexamethasone or placebo treatment. Arch Pediatr Adolesc Med. 2001;155: From the Division of Emergency Medicine, Children s Hospital Medical Center, Cincinnati, Ohio (Drs Luria, Gonzalez-del-Rey, DiGiulio, McAneney, and Ruddy); and the Section of Emergency Medicine, Mayo Eugenio Litta Children s Hospital, Mayo Clinic, Rochester, Minn (Dr Olson). CORTICOSTEROIDS are commonly prescribed for the treatment of acute viral laryngotracheobronchitis (croup). Much of the evidence that supports this practice is derived from patients with more severe disease. This includes outpatient investigations in which a substantial number of patients received treatment with nebulized epinephrine 1,2 and inpatient studies. 3-5 Recently, Geelhoed et al 6 reported that patients with mild croup are less likely to seek additional care if treated with a single dose of oral dexamethasone. Despite evidence supporting the use of nebulized budesonide in the treatment of croup, 7-9 we identified only 1 published study examining the effectiveness of nebulized dexamethasone sodium phosphate. 10 The authors reported that patients treated with nebulized dexamethasone demonstrated greater clinical improvement at 4 hours compared with patients receiving placebo. There was no evidence of a sustained clinical effect and 2 patients in the treatment arm developed significant complications. The study herein determined whether administration of oral or nebulized dexamethasone decreases the need for subsequent treatments, shortens symptom duration, or decreases the need for subsequent care in children with croup of mild severity. The study also addresses the need for additional information regarding the effectiveness of corticosteroids for treating patients with mild disease. RESULTS Two hundred sixty-four patients were enrolled in the study. Eighty-five patients were in the oral dexamethasone treated 1340
2 PATIENTS AND METHODS PATIENTS The study population consisted of patients presenting to the emergency departments (EDs) at either Children s Hospital Medical Center, Cincinnati, Ohio, or Children s Hospital, Columbus, Ohio, from September 1, 1995, through December 31, The study institutions are large urban tertiary care centers. Each ED has approximately patient visits annually. Patients eligible for the study were 6 months to 6 years old presenting with a syndrome of barky cough, stridor, and/or hoarseness for fewer than 48 hours. In an attempt to exclude patients with spasmodic croup, the presence of a viral prodrome consisting of fever, cough, or rhinorrhea was required for study participation. Patients were excluded if they had been treated with corticosteroids during the 14 days prior to enrollment or if they had severe disease. Severe disease was defined as any patient who received nebulized racemic epinephrine or corticosteroids at the order of the treating ED physician or had an oxygen saturation rate of less than 94%. Patients were similarly excluded if they had a clinical picture consistent with spasmodic croup, a history of prolonged endotracheal intubation, a history of chronic respiratory illness (ie, asthma or cystic fibrosis), a condition associated with airway abnormalities (ie, Pierre Robin or trisomy 21 syndrome), or did not have a working telephone. Informed written consent was obtained for eligible patients who agreed to participate in the study. Consent was obtained by attending ED physicians or fellows. The ED physicians and fellows were familiarized with the study protocol and consent process prior to initiating the study. After informed consent was obtained, demographic, historical, and family data were recorded. This included the duration of the child s croup symptoms, whether the child had a history of croup, whether the parent had ever cared for a child with croup, if there were smokers in the home, and if the family had access to a humidifier and/or vaporizer. Subsequent to the collection of this information, a croup score (Table 1) was calculated and a nasopharyngeal viral culture was obtained. The croup score used in the study was a modification of the system employed by Westley et al. 11 Specifically, the stridor section of the score was altered to include 1 point if the subject had stridor only with agitation or excitement. The Westley et al 11 scoring system was designed to evaluate patients over a broad range of severity. Since the patients in this study had mild croup, a score of 0 for air entry, cyanosis, and level of consciousness was expected. Croup scores were assigned solely to describe symptom severity at enrollment. After examining the other 2 portions of the score, stridor and retractions, we believe our modification was necessary to more accurately describe disease severity in the study population. Subjects were then block randomized in a doubleblind fashion to 1 of 3 treatment groups. The randomization was performed in blocks of 15 by the study pharmacist at each enrolling site with the use of a random number generator. The study pharmacist then assembled numbered croup kits containing study preparations that reflected the results of the randomization. The kits were sealed to prevent any tampering and were kept in the EDs. The study physician retrieved the lowest numbered kit when enrolling a new subject to maintain the randomization order. Only the study pharmacists knew the results of the randomization. The first treatment group received 0.6 mg/kg of oral dexamethasone (maximum dose, 10 mg) and nebulized placebo. Dexamethasone Intensol (Roxane Laboratories Inc, a subsidary of Boehringer Ingelheim Crop, Ridgefield, Conn), a 1-mg/mL solution, was used as the oral treatment. The second group received oral placebo and 160 µg of nebulized dexamethasone sodium phosphate. The third group received both oral and nebulized placebo. All oral study preparations were mixed 1:1 with a commercially available grape flavoring to minimize taste bias. Nebulized study preparations were delivered via a nebulizer (Airlife, Misty-Neb Nebulizer; Allegiance Healthcare Corp, McGaw Park, Ill) with a fill volume of 3 ml and oxygen flow set at 5 to 6 L/min. Continued on next page group, 91 patients in the nebulized dexamethasone treated group, and 88 in the placebo-treated group. It was discovered that 9 patients did not meet enrollment criteria after entering the study. These patients were included in keeping with the intention-to-treat study design. Six of the 9 patients had croup symptom duration of longer than 48 hours. Two had a history of chronic pulmonary illness (asthma) and 1 had a history of prolonged endotracheal intubation. Two hundred twenty-one patients (84%) were available on day 7 (Table 2). The hospital and outpatient records of the 43 patients who were unavailable 1 week after enrollment were reviewed. The records indicate that 14 of these patients returned to either the ED or their primary care physician s office. Twenty-nine of the 43 children returned to neither the enrolling ED nor their primary care physician. Only data obtained during telephone encounters with these 29 patients data were included. Otherwise these data were considered missing. There was no significant difference between the 3 groups for age, sex, symptom duration, or croup score (Table 3). Similarly, there was no difference in the viral isolates recovered from the patients (Table 4). There were 3 (4%) treatment failures in the oral dexamethasone treated group (Figure). This compares with 12 (16%) and 10 (14%) treatment failures in the nebulized dexamethasone treated and placebo-treated groups, respectively (P=.05). Based on the sample size, the study had 58% power to detect the observed difference in treatment failures. Twenty of the treatment failure patients returnedforadditionalcareandreceivedcorticosteroidswithin 2 days of enrollment. The other 5 treatment failure patients received corticosteroids 3 to 4 days after enrollment. Seventeen of the treatment failure patients presented to the ED for their subsequent care. The other 8 patients received corticosteroids at the primary care physician s office. Based on the treatment failure rates observed in the oral dexamethasone treated and placebo-treated groups, a number needed to treat was calculated. A practitioner 1341
3 After the study treatments were administered, patients were discharged home if the treating ED physician did not believe further treatment or observation was warranted. Prior to discharge, all parents were given preprinted information about croup including strategies for home management. The information sheet also contained a telephone number that caregivers could call if they desired medical advice. Medical advice calls were answered by 1 of the investigators who was available 24 hours a day, 7 days a week. Telephone follow-up was obtained on days 1, 2, 3, 4, and 7 after enrollment. During each follow-up encounter caregivers were asked to provide a global assessment of their child s croup symptoms (ie, worse, same, better, or gone) compared with their condition in the ED. 2 Parents were also asked whether they had called a health care professional for medical advice or sought additional medical evaluation since enrollment or the last follow-up encounter. The office and/or hospital medical records of patients who sought additional care were reviewed to determine the severity of croup symptoms at that time as well as any treatments that were prescribed. The hospital and primary care medical records of all patients who did not complete follow-up were also reviewed to determine if they had returned for subsequent care. These medical records were used to determine the reason these children returned for care, the severity of any croup symptoms, and whether any new treatments were prescribed. The primary outcome measure was treatment failure, defined as a physician reevaluating a patient s condition and prescribing corticosteroids or racemic epinephrine. Secondary outcome measures included whether the child presented for additional medical care and the parental assessments of the patients condition obtained during telephone follow-up. The study design was based on an intention-to-treat model. Data from patients who refused or vomited oral dexamethasone were included in the oral dexamethasone treated group. Similarly, data from patients who were combative during the administration of nebulized dexamethasone were included in the nebulized dexamethasone treated group. The study protocol did not allow for a second dosing of the oral or nebulized dexamethasone treatments. To further quantify the relationship between corticosteroid exposure and subsequent treatment failure, the number needed to treat was calculated. 12 In this study, the number needed to treat estimates the number of children a clinician would have to treat with corticosteroids to prevent 1 patient from returning with clinically significant croup. STATISTICAL ANALYSES The 2 test was used to analyze all categorical data. Analysis of variance was applied to continuous normally distributed data and the Kruskal-Wallis test was used to evaluate nonnormally distributed data. Statistical significance was set at a P.05. Pairwise analyses of outcome measures were also performed. For pairwise comparisons, the 2 test was used to analyze all categorical data and the Mann- Whitney test was applied to continuous nonnormally distributed data. Statistical significance for the pairwise comparisons was set at P.02. SPSS 10.0 software (SPSS, Chicago, Ill) was used for all statistical analyses. The investigational review boards at each of the participating hospitals approved this study. SAMPLE SIZE At the time of the study, we could not identify any published data estimating the percentage of untreated children with mild croup who subsequently require additional follow-up or treatment with corticosteroids. Therefore, we did not use our primary outcome measure to calculate the sample size of the study. Pilot data indicated that croup symptoms generally resolve within 4 days. To detect a 25% reduction in symptom duration between those patients treated with corticosteroids and those not receiving treatment, at least 50 patients were required in each treatment arm assuming an level of.05 and power of 80%. Since the sample size calculation was not based on the study outcome measures, a post hoc power calculation was performed. would need to treat 10 patients (95% confidence interval, 9-11 patients) with oral dexamethasone to prevent 1 from returning with croup severe enough to warrant corticosteroid administration. Ten children (13%) in the oral dexamethasone treated group sought a second medical evaluation during the 7 days following enrollment. This compares with 27 (33%) in the nebulized dexamethasone treated group and 29 (37%) in the placebo-treated group, respectively (P=.002). Of the children who sought additional medical evaluation, 7 (9%) in the oral dexamethasone treated group returned specifically because of concerns regarding croup symptoms. This compares with 19 patients (24%) in the nebulized dexamethasone treated group and 18 patients (24%) in the placebo-treated group (P=.03) (Figure). Parents were asked during each follow-up call if their child s croup symptoms were worse, the same, better, or gone. These responses were assigned a score of 1, 2, 3, or 4, respectively. For each follow-up telephone encounter (days 1, 2, 3, 4, and 7), the scores of individual subjects were ranked. The mean ranks of the children in each treatment arm were then compared. The scores of the children in the oral dexamethasone treated group were significantly better than those in the nebulized dexamethasone treated and placebo-treated groups on day 1 (P.001). There was no difference in the caregiver reports for days 2, 3, 4, or 7. Pairwise comparisons revealed no statistical differences in treatment failure rates between the 3 groups. Statistical differences were noted between the oral dexamethasone treated and placebo-treated groups with respect to seeking subsequent care and returning for care specifically owing to croup symptoms (P=.001 and P=.014, respectively). Similar differences were found between the oral and nebulized dexamethasone treated groups (P=.003 and P=.01, respectively). Caregivers of children in the oral dexamethasone treated group reported greater clinical improvement in croup symptoms on day 1 (P.001) compared with the placebo-treated group. Children in the oral 1342
4 Table 1. Croup Scoring System Indicator of Disease Severity Score Stridor None 0 Only with agitation or excitement 1 At rest with stethoscope* 2 At rest without stethoscope* 3 Retractions None 0 Mild 1 Moderate 2 Severe 3 Air entry Normal 0 Decreased 1 Severely decreased 2 Cyanosis None 0 With agitation 4 At rest 5 Level of consciousness Normal 0 Altered mental status 5 *At rest with stethoscope indicates stridor can only be heard using a stethoscope; at rest without stethoscope, stridor so loud it can be heard without using a stethoscope. dexamethasone treated group also demonstrated greater clinical improvement on day 1(P =.002) and day 2 (P=.005) compared with the nebulized dexamethasone treated group. There was no difference between the nebulized dexamethasone treated and placebo-treated groups with respect to returning for subsequent care, returning for care specifically owing to croup symptoms, or the caregiver reports. COMMENT In our study, children with mild croup benefited from a single 0.6-mg/kg dose of oral dexamethasone compared with 160 µg of aerosolized dexamethasone sodium phosphate or placebo. In 1996, Geelhoed et al 6 published the results of a study in which patients with mild croup were treated with either oral dexamethasone (0.15 mg/kg) or placebo. In that study, none of the patients who received dexamethasone treatment and 17% of the patients who received placebo subsequently presented for ongoing croup symptoms. By comparison, 9% of those who received oral dexamethasone and 24% of those who received placebo in our study sought additional care because of their croup symptoms. It is difficult to ascertain the reason we observed a modestly higher rate of return among dexamethasone-treated patients. Our larger sample size, younger study population, intention-to-treat model, and the fact our study population presented with somewhat more severe symptoms may have contributed to this. In another outpatient study, Cruz et al 2 administered intramuscular dexamethasone (0.6 mg/kg) or placebo to patients with moderate croup. They reported that 84% of the dexamethasone-treated patients and 42% of those in the placebo group reported improvement in croup symptoms 24 hours after enrollment. Our results were Table 2. Summary of Patient * Day Oral (n = 85) Nebulized (n = 91) Placebo (n = 88) 1 80 (94) 81 (89) 79 (90) 2 80 (94) 80 (88) 76 (86) 3 77 (91) 78 (86) 75 (85) 4 75 (88) 74 (81) 73 (83) 7 73 (86) 77 (85) 71 (81) *Oral treatment group indicates those who received 0.6 mg/kg of oral dexamethasone and nebulized placebo (ie, a 1-mg/mL solution of Dexamethasone Intensol; Roxane Laboratories Inc, subsidiary of Boehringer Ingelheim Corp, Ridgefield, Conn); nebulized treatment group, those who received oral placebo and 160 µg of nebulized dexamethasone sodium phosphate; placebo treatment group, those who received oral and nebulized placebo. All data are given as number (percentage) of patients. similar despite our subjects having less severe disease. In our study, 83% of the patients treated with oral dexamethasone and 56% of the subjects in the placebo group reported improvement 24 hours after enrollment. When assessing the validity of this study, a number of factors require consideration. The first is our choice of outcome measures. In evaluating response to therapy, we monitored whether individual subjects received additional therapy, how home caregivers described disease severity, and whether home caregivers sought additional medical evaluation. Each of these outcome measures is subjective and, therefore, may not accurately reflect true disease severity. The double-blind, randomized, placebocontrolled study design should have minimized this effect. After enrolling patients for 12 months, it was discovered that, due to an error in the randomization process at 1 institution, too few patients were being assigned to the placebo group. The initial randomization ratio of 1:1:1 (oralnebulized-placebo) was changed to 1:1:3 at both institutions and enrollment continued. The pharmacists performing the randomization and 4 of us (J.W.L., J.A.G., G.A.D., and R.M.R.) were notified of the randomization error. No one involved with data collection was informed to avoid any potential bias. There was no difference in the age, sex, symptom duration, or croup scores of patients enrolled during the first year of the study and those enrolled subsequently. Therefore, we believe the change in the randomization procedure did not affect the results of the study. Our sample size calculation was not based on the primary outcome measure. At the time the study was initiated, however, we could not identify any published data estimating the percentage of untreated ED patients with mild croup who subsequently required treatment with corticosteroids. Based on available data, we planned to enroll 150 patients. After discovering the randomization error, it was necessary to enroll more patients than the original estimation to ensure near-equal numbers of subjects in each group. This is why the study group included more than 80 patients per group. We observed a P value of.05 for our primary outcome measure, treatment failure. A post hoc power calculation revealed that the study had 58% power to detect the observed difference in treatment failures. In the 1343
5 Table 3. Patient Characteristics at Study Enrollment* Variable Oral Nebulized Placebo P Value Age, mean (range), mo 28 (6-70) 31 (6-71) 26 (6-71).16 Sex, No. (%) of males 61 (72) 58 (64) 57 (65).48 Race, No. (%) of white patients 55 (65) 74 (81) 64 (72).06 Symptom duration, mean, h Mean/median croup score (range) 1.6/1 (0-6) 1.6/1 (0-5) 1.7/1 (0-5).94 Patients with access to a humidifier, No. (%) 52 (66) 59 (68) 58 (69).91 Patients with a history of croup, No. (%) 22 (26) 21 (24) 11 (13).07 Caregivers with experience with croup, No. (%) 37 (45) 34 (40) 29 (35).45 Patients with a smoker in the home, No. (%) 41 (52) 37 (44) 33 (42).42 *Oral treatment group indicates those who received 0.6 mg/kg of oral dexamethasone and nebulized placebo (ie, a 1-mg/mL solution of Dexamethasone Intensol; Roxane Laboratories Inc, subsidiary of Boehringer Ingelheim Corp, Ridgefield, Conn); nebulized treatment group, those who received oral placebo and 160 µg of nebulized dexamethasone sodium phosphate; placebo treatment group, those who received oral and nebulized placebo. P.05. Table 4. Viral Isolates From Nasopharyngeal Cultures* Culture Result Oral Nebulized Placebo No growth Parainfluenza Type Type Type Type Influenza type A RSV Other Oral n = 85 Patients 76 Patients Completed Study Patients N = 264 R Nebulized n = 91 Patients 81 Patients Completed Placebo n = 88 Patients 78 Patients Completed *Oral treatment group indicates those who received 0.6 mg/kg of oral dexamethasone and nebulized placebo (ie, a 1-mg/mL solution of Dexamethasone Intensol; Roxane Laboratories Inc, subsidiary of Boehringer Ingelheim Corp, Ridgefield, Conn); nebulized treatment group, those who received oral placebo and 160 µg of nebulized dexamethasone sodium phosphate; placebo treatment group, those who received oral and nebulized placebo. RSV indicates respiratory syncytial virus. 10 Patients Sought Additional Medical Care 7 Patients Returned for Concerns Regarding Croup Symptoms 27 Patients Sought Additional Medical Care 19 Patients Returned for Concerns Regarding Croup Symptoms 29 Patients Sought Additional Medical Care 18 Patients Returned for Concerns Regarding Croup Symptoms 3 Patients Were Failures 12 Patients Were Failures 10 Patients Were Failures Study flowchart. R indicates randomization; oral treatment group, those who received 0.6 mg/kg of oral dexamethasone and nebulized placebo (ie, a 1-mg/mL solution of Dexamethasone Intensol; Roxane Laboratories Inc, a subsidary of Boehringer Ingelheim Corp, Ridgefield, Conn); nebulized treatment group, those who received oral placebo and 160 µg of nebulized dexamethasone sodium phosphate; and placebo treatment group, those who received oral and nebulized placebo. For a description of how patients were randomized to 1 of the 3 study arms, see the Patients subsection of the Patients and Methods section. context of the clinical data and number-needed-to-treat calculation, we believe the observed P value represents a type II error. It is also important to consider the enrollment criteria of the study. Patients were eligible for the study if the responsible ED physician did not believe they required corticosteroids and/or racemic epinephrine. At the time of the project, this was a practical criterion because we were interested in knowing if patients with croup who were not receiving corticosteroids would benefit from their administration. Some might argue that the administration of oral corticosteroids to every ED patient with croup constitutes an overly aggressive approach to this clinical process. A selective approach to corticosteroid administration would likely focus on patients who present without stridor. To our knowledge, there are no studies that specifically address the use of corticocorticosteroids in this patient population. Fifty-four patients (21%) in this study presented without stridor. Three of these subjects sought additional care due to concerns regarding their croup symptoms. Two were in the placebo-treated group and 1 was in the nebulized dexamethasone treated group. Unfortunately, this is too little data to draw any meaningful conclusions about this subgroup of patients. There are some facts that support prescribing oral dexamethasone to all patients with croup who present to the ED. In our study population of patients with mild disease, a clinician would have to treat only 10 patients with oral dexamethasone to prevent 1 child from coming back with clinically significant croup symptoms. In addition, this medication has an excellent safety profile and is inexpensive. The hospital cost of a 10-mg dose of dexamethasone (Dexamethasone Intensol) is approximately $4. The oral administration of the parenteral form of dexamethasone is even less expensive. Since
6 What This Study Adds While the effectiveness of dexamethasone as a treatment for patients with moderate to severe croup is well established, few studies have examined the use of this treatment for mild croup. Little data are related to the use of nebulized dexamethasone as a treatment for croup. This study addresses the need for additional information regarding the effectiveness of oral and inhaled dexamethasone for treating patients with mild disease. The results indicate that patients with mild croup treated with oral dexamethasone are less likely to seek subsequent care and demonstrate more rapid clinical improvement compared with those who receive nebulized dexamethasone or placebo. dose is needed to complete treatment, compliance is not an issue. Smaller doses of oral dexamethasone may also be effective. In a study of patients with moderate to severe croup, oral dexamethasone doses of 0.6 mg/kg, 0.3 mg/ kg, and 0.15 mg/kg were shown to be equally effective for abating croup symptoms. 13 Geelhoed 14 also reported that the introduction of corticosteroid treatment at his hospital resulted in a decrease in the number of intubations, intensive care unit days, and length of stay for patients with croup. These effects have been maintained even as the routine dexamethasone dose has decreased from 0.6 mg/kg to 0.15 mg/kg. The dose and method of drug provision for the nebulized dexamethasone treated arm are also important limitations of this study. When we initiated the project, we identified no published reports examining the effectiveness of nebulized dexamethasone for treating croup. We selected 160 µg because it was equivalent to 2 puffs of a commercially available dexamethasone metered-dose inhaler. We subsequently identified 1 study that examined the use of aerosolized dexamethasone for croup. 10 In that report, children with moderately severe disease were given 10 to 20 mg of nebulized dexamethasone sodium phosphate or placebo. Dexamethasone-treated patients showed improvement in their croup scores at 4 hours compared with controls. There was no statistical difference between the 2 groups with regard to hospitalization rates and 2 patients in the treatment group developed bacterial tracheitis. In our study, aerosolized dexamethasone was delivered via an updraft nebulizer. Consequently, much of the drug may have been lost through the ventilation holes in the mask. This may be especially true for children who are not used to receiving aerosols since they often cry or scream during the treatment. The small dose and use of an updraft nebulizer probably resulted in little actual drug delivery to the patients and may account for the similarity between the nebulized dexamethasone treated and placebo-treated groups. CONCLUSIONS Children who present to the ED during the first 2 days of viral croup benefit from a single dose of oral dexamethasone. Further studies may help with specific dosing questions and whether inhaled dexamethasone is of any value. Accepted for publication July 16, This study was partially funded through a grant from the Bremer Foundation at The Ohio State University, Columbus. Presented at the annual meeting of the Pediatric Academic Societies, San Francisco, Calif, May 1, We thank all of the ED nurses and physicians at the participating institutions. We would like to specifically note the efforts of Kathy Montefiore, RPh, Marijo Martin, RPh, and Kathy Mack. We would also like to thank Jackie Grupp- Phelan, MD, for her review of the manuscript. Corresponding author and reprints: Joseph Luria, MD, Division of Emergency Medicine, Children s Hospital Medical Center, 3333 Burnet Ave OSB-4, Cincinnati, OH ( joe.luria@chmcc.org). REFERENCES 1. Johnson DW, Jacobson S, Edney PC, Hadfield P, Mundy ME, Schuh S. A comparison of nebulized budesonide, intramuscular dexamethasone, and placebo for moderately severe croup. N Engl J Med. 1998;339: Cruz MN, Stewart G, Rosenberg N. Use of dexamethasone in the outpatient management of acute laryngotracheitis. Pediatrics. 1995;96: Super DM, Cartelli NA, Brooks LJ, Lembo RM, Kumar ML. A prospective randomized double-blind study to evaluate the effect of dexamethasone in acute laryngotracheitis. J Pediatr. 1989;115: Kairys SW, Olmstead EM, O Connor GT. Steroid treatment of larygotracheitis: a meta-analysis of the evidence from randomized trials. Pediatrics. 1989;83: Tibballs J, Shann FA, Landau LI. Placebo-controlled trial of prednisolone in children intubated for croup. Lancet. 1992;340: Geelhoed GC, Turner J, Macdonald WB. Efficacy of a small single dose of oral dexamethasone for outpatient croup: a double blind placebo controlled clinical trial. BMJ. 1996;313: Husby S, Agertoft L, Mortensen S, Pedersen S. of croup with nebulised steroid (budesonide): a double blind, placebo controlled study. Arch Dis Child. 1993;68: Klassen TP, Feldman ME, Watters LK, Sutcliffe T, Rowe PC. Nebulized budesonide for children with mild-to-moderate croup. N Engl J Med. 1994;331: Godden CW, Campbell MJ, Hussey M, Cogswell JJ. Double blind placebo controlled trial of nebulised budesonide for croup. Arch Dis Child. 1997;76: Johnson DW, Schuh S, Koren G, Jaffee DM. Outpatient treatment of croup with nebulized dexamethasone. Arch Pediatr Adolesc Med. 1996;150: Westley CR, Cotton EK, Brooks JG. Nebulized racemic epinephrine by IPPB for the treatment of croup: a double-blind study. AJDC. 1978;132: Sackett DL, Richardson WS, Rosenberg W, Haynes RB. Evidence-Based Medicine: How to Practice and Teach EBM. New York, NY: Churchill Livingstone Inc; Geelhoed GC, Macdonald WB. Oral dexamethasone in the treatment of croup: 0.15 mg/kg versus 0.3 mg/kg versus 0.6 mg/kg. Pediatr Pulmonol. 1995;20: Geelhoed GC. Sixteen years of croup in a Western Australian teaching hospital: effects of routine steroid treatment. Ann Emerg Med. 1996;28:
PAEDIATRIC ACUTE CARE GUIDELINE. Croup. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Croup Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Croup Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Oral Dexamethasone in the Treatment of Croup: 0.15 mglkg Versus 0.3 mglkg Versus 0.6 mglkg
 Pediatric Pulmonology 20:362-368 (1995) Oral Dexamethasone in the Treatment of Croup: 0.15 mglkg Versus 0.3 mglkg Versus 0.6 mglkg G.C. Geelhoed, FRACP, and W.B.G. Macdonald, FRACP Summary. The objective
Pediatric Pulmonology 20:362-368 (1995) Oral Dexamethasone in the Treatment of Croup: 0.15 mglkg Versus 0.3 mglkg Versus 0.6 mglkg G.C. Geelhoed, FRACP, and W.B.G. Macdonald, FRACP Summary. The objective
The New England Journal of Medicine A COMPARISON OF NEBULIZED BUDESONIDE, INTRAMUSCULAR DEXAMETHASONE, AND PLACEBO FOR MODERATELY SEVERE CROUP
 A COMPARISON OF NEBULIZED, INTRAMUSCULAR, AND PLACEBO FOR MODERATELY SEVERE CROUP DAVID W. JOHNSON, M.D., SHEILA JACOBSON, M.B., B.CH., PETER C. EDNEY, B.SC., PAT HADFIELD, R.N., MARIANNE E. MUNDY, R.N.,
A COMPARISON OF NEBULIZED, INTRAMUSCULAR, AND PLACEBO FOR MODERATELY SEVERE CROUP DAVID W. JOHNSON, M.D., SHEILA JACOBSON, M.B., B.CH., PETER C. EDNEY, B.SC., PAT HADFIELD, R.N., MARIANNE E. MUNDY, R.N.,
A Randomized Trial of a Single Dose of Oral Dexamethasone for Mild Croup
 The new england journal of medicine original article A Randomized Trial of a Single Dose of Oral Dexamethasone for Mild Croup Candice L. Bjornson, M.D., Terry P. Klassen, M.D., Janielee Williamson, R.N.,
The new england journal of medicine original article A Randomized Trial of a Single Dose of Oral Dexamethasone for Mild Croup Candice L. Bjornson, M.D., Terry P. Klassen, M.D., Janielee Williamson, R.N.,
Acute Laryngitis in Childhood
 Acute Laryngitis in Childhood Hany Simon Junior Viral croup Definition The term croup syndrome characterizes a group of diseases with variable anatomic involvement and etiology, and is clinically manifested
Acute Laryngitis in Childhood Hany Simon Junior Viral croup Definition The term croup syndrome characterizes a group of diseases with variable anatomic involvement and etiology, and is clinically manifested
Nebulized Budesonide Is as Effective as Nebulized Adrenaline in Moderately Severe Croup
 Nebulized Budesonide Is as Effective as Nebulized Adrenaline in Moderately Severe Croup Dominic Fitzgerald, MBBS, FRACP*; Craig Mellis, MBBS, MPH, FRACP*; Mark Johnson, MBBS; Hugh Allen, MBBS, FRACPII;
Nebulized Budesonide Is as Effective as Nebulized Adrenaline in Moderately Severe Croup Dominic Fitzgerald, MBBS, FRACP*; Craig Mellis, MBBS, MPH, FRACP*; Mark Johnson, MBBS; Hugh Allen, MBBS, FRACPII;
Croup (Laryngo-tracheo-bronchitis)
 Croup (Laryngo-tracheo-bronchitis) 1a 2a 2b Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Date of
Croup (Laryngo-tracheo-bronchitis) 1a 2a 2b Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Date of
Clinical Guideline. Clinical Guideline on Management of Viral Croup D NG, PY CHOW, YL WONG, D LAU, KT SO, G CHAN, NS TSOI, HW LIU
 HK J Paediatr (new series) 2002;7:68-75 Clinical Guideline Clinical Guideline on Management of Viral Croup D NG, PY CHOW, YL WONG, D LAU, KT SO, G CHAN, NS TSOI, HW LIU Guideline Development Member Guideline
HK J Paediatr (new series) 2002;7:68-75 Clinical Guideline Clinical Guideline on Management of Viral Croup D NG, PY CHOW, YL WONG, D LAU, KT SO, G CHAN, NS TSOI, HW LIU Guideline Development Member Guideline
Key points. and available across the world. L-adrenalin is used because it is safe, cheap
 Key points The term "croup" refers to a clinical syndrome characterised by barking cough, inspiratory stridor and hoarseness of voice. The standard work-up for clinical diagnosis includes the assessment
Key points The term "croup" refers to a clinical syndrome characterised by barking cough, inspiratory stridor and hoarseness of voice. The standard work-up for clinical diagnosis includes the assessment
Simulation 01: Two Year-Old Child in Respiratory Distress (Croup)
 Simulation 01: Two Year-Old Child in Respiratory Distress (Croup) Flow Chart Opening Scenario 2 year-old child in respiratory distress - assess Section 1 Type: IG audible stridor with insp + exp wheezing;
Simulation 01: Two Year-Old Child in Respiratory Distress (Croup) Flow Chart Opening Scenario 2 year-old child in respiratory distress - assess Section 1 Type: IG audible stridor with insp + exp wheezing;
CLINICAL GUIDELINE FOR THE MANAGEMENT OF VIRAL LARYNGO-TRACHEOBRONCHITIS (CROUP) V3.0
 CLINICAL GUIDELINE FOR THE MANAGEMENT OF VIRAL LARYNGO-TRACHEOBRONCHITIS (CROUP) V3.0 Clinical Guideline Template Page 1 of 13 1. Aim/Purpose of this Guideline 1.1. This guideline applies to all nursing
CLINICAL GUIDELINE FOR THE MANAGEMENT OF VIRAL LARYNGO-TRACHEOBRONCHITIS (CROUP) V3.0 Clinical Guideline Template Page 1 of 13 1. Aim/Purpose of this Guideline 1.1. This guideline applies to all nursing
STRIDOR. Respiratory system. Lecture
 STRIDOR Stridor is a continuous inspiratory harsh sound produced by partial obstruction in the region of the larynx or trachea. Total obstruction cyanosis & death. Etiology Acute stridor Infectious croup
STRIDOR Stridor is a continuous inspiratory harsh sound produced by partial obstruction in the region of the larynx or trachea. Total obstruction cyanosis & death. Etiology Acute stridor Infectious croup
Management of croup in children
 Management of croup in children Mncengeli Sibanda, BPharm, MPharm, MSc Pharmacology, MBA Zandile Gumede, BPharm School of Pharmacy, Sefako Makgatho Health Sciences University Correspondence to: Mncengeli
Management of croup in children Mncengeli Sibanda, BPharm, MPharm, MSc Pharmacology, MBA Zandile Gumede, BPharm School of Pharmacy, Sefako Makgatho Health Sciences University Correspondence to: Mncengeli
Video Cases in Pediatrics. Ran Goldman, MD BC Children s Hospital University of British
 Video Cases in Pediatrics Ran Goldman, MD BC Children s Hospital University of British Columbia @Dr_R_Goldman Bronchiolitis Viral infection of the lower respiratory tract characterized by acute inflammation,
Video Cases in Pediatrics Ran Goldman, MD BC Children s Hospital University of British Columbia @Dr_R_Goldman Bronchiolitis Viral infection of the lower respiratory tract characterized by acute inflammation,
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
PEDIATRIC ACUTE ASTHMA SCORE (P.A.A.S.) GUIDELINES. >97% 94% to 96% 91%-93% <90% Moderate to severe expiratory wheeze
 Inclusion: Children experiencing acute asthma exacerbation 24 months to 18 years of age with a diagnosis of asthma Patients with a previous history of asthma (Consider differential diagnosis for infants
Inclusion: Children experiencing acute asthma exacerbation 24 months to 18 years of age with a diagnosis of asthma Patients with a previous history of asthma (Consider differential diagnosis for infants
Children suffering from asthma symptoms present
 Original Article Single-Dose Oral Dexamethasone in the Emergency Management of Children With Exacerbations of Mild to Moderate Asthma Saleh Altamimi, MD, FRCP(C), FAAP, Glenn Robertson, MD, FRCP(C), UBC,
Original Article Single-Dose Oral Dexamethasone in the Emergency Management of Children With Exacerbations of Mild to Moderate Asthma Saleh Altamimi, MD, FRCP(C), FAAP, Glenn Robertson, MD, FRCP(C), UBC,
Trust Guideline for Acute Stridor in Children
 A Clinical Guideline For Use in: By: For: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported by: Children
A Clinical Guideline For Use in: By: For: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported by: Children
Simulation 1: Two Year-Old Child in Respiratory Distress
 Simulation 1: Two Year-Old Child in Respiratory Distress Opening Scenario (Links to Section 1) You are the respiratory therapist in a 300 bed community hospital working the evening shift. At 8:30 PM you
Simulation 1: Two Year-Old Child in Respiratory Distress Opening Scenario (Links to Section 1) You are the respiratory therapist in a 300 bed community hospital working the evening shift. At 8:30 PM you
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
Steroid Storms: Controversies and Considerations in PEM
 Steroid Storms: Controversies and Considerations in PEM Kimball Prentiss, MD, FAAP Division of Pediatric Emergency Medicine September 19, 2018 CCEM Conference, Northampton Objectives Develop an understanding
Steroid Storms: Controversies and Considerations in PEM Kimball Prentiss, MD, FAAP Division of Pediatric Emergency Medicine September 19, 2018 CCEM Conference, Northampton Objectives Develop an understanding
Humidified air inhalation for treating croup: a systematic review and meta-analysis
 Published by Oxford University Press. doi:10.1093/fampra/cmm022 Family Practice Advance Access published on 29 June 2007 Humidified air inhalation for treating croup: a systematic review and meta-analysis
Published by Oxford University Press. doi:10.1093/fampra/cmm022 Family Practice Advance Access published on 29 June 2007 Humidified air inhalation for treating croup: a systematic review and meta-analysis
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Is There a Treatment for BPD?
 Is There a Treatment for BPD? Amir Kugelman, Pediatric Pulmonary Unit and Department of Neonatology Bnai Zion Medical Center, Rappaport Faculty of Medicine Haifa, Israel Conflict of Interest Our study
Is There a Treatment for BPD? Amir Kugelman, Pediatric Pulmonary Unit and Department of Neonatology Bnai Zion Medical Center, Rappaport Faculty of Medicine Haifa, Israel Conflict of Interest Our study
AT TRIAGE. Alberta Acute Childhood Asthma Pathway: Evidence based* recommendations For Emergency / Urgent Care
 1 1 Should the child be placed into the Pathway? Asthma Clinical Score (PRAM) Inclusion Children 1 year and 18 years of age who present with wheezing and respiratory distress, and have been diagnosed by
1 1 Should the child be placed into the Pathway? Asthma Clinical Score (PRAM) Inclusion Children 1 year and 18 years of age who present with wheezing and respiratory distress, and have been diagnosed by
trust clinical guideline
 CG26 VERSION 1.0 1/8 Guideline ID CG26 Version 1.0 Title Approved by Management of Croup Clinical Effectiveness Group Date Issued 01/10/2014 Review Date 31/09/2017 Directorate Authorised Staff Medical
CG26 VERSION 1.0 1/8 Guideline ID CG26 Version 1.0 Title Approved by Management of Croup Clinical Effectiveness Group Date Issued 01/10/2014 Review Date 31/09/2017 Directorate Authorised Staff Medical
The assessment and management of croup
 PAEDIATRIC RESPIRATORY REVIEWS (2006) 7, 73 81 REVIEW The assessment and management of croup Dominic A. Fitzgerald* University of Sydney, Department of Respiratory Medicine, The Children s Hospital at
PAEDIATRIC RESPIRATORY REVIEWS (2006) 7, 73 81 REVIEW The assessment and management of croup Dominic A. Fitzgerald* University of Sydney, Department of Respiratory Medicine, The Children s Hospital at
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
Management of acute asthma in children in emergency department. Moderate asthma
 152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
The New England Journal of Medicine EFFECT OF NEBULIZED IPRATROPIUM ON THE HOSPITALIZATION RATES OF CHILDREN WITH ASTHMA. Subjects
 EFFECT OF NEBULIZED IPRATROPIUM ON THE HOSPITALIZATION RATES OF CHILDREN WITH FAIQA QURESHI, M.D., JOHN PESTIAN, PH.D., PARIS DAVIS, B.A., AND ARNO ZARITSKY, M.D. ABSTRACT Background Anticholinergic medications
EFFECT OF NEBULIZED IPRATROPIUM ON THE HOSPITALIZATION RATES OF CHILDREN WITH FAIQA QURESHI, M.D., JOHN PESTIAN, PH.D., PARIS DAVIS, B.A., AND ARNO ZARITSKY, M.D. ABSTRACT Background Anticholinergic medications
Primary Care practice clinics within the Edmonton Southside Primary Care Network.
 Allergy/Immunotherapy Injections Last Review: November 2016 Intervention(s) and/or Procedure: Administration of allergen injections throughout immunotherapy treatment. Immunotherapy for allergic disease
Allergy/Immunotherapy Injections Last Review: November 2016 Intervention(s) and/or Procedure: Administration of allergen injections throughout immunotherapy treatment. Immunotherapy for allergic disease
Croup develops in more than Can -
 CMAJ Review CME Croup in children Candice L. Bjornson MD, David W. Johnson MD Croup develops in more than 80 000 Can - adian children each year, making it the second most common cause of respiratory distress
CMAJ Review CME Croup in children Candice L. Bjornson MD, David W. Johnson MD Croup develops in more than 80 000 Can - adian children each year, making it the second most common cause of respiratory distress
Surveillance report Published: 6 April 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Pediatric Respiratory Disease: A Model for the Future of Emergency Medicine Research
 Pediatric Respiratory Disease: A Model for the Future of Emergency Medicine Research Joseph J. Zorc, MD, MSCE Mark Fishman Professor, Department of Pediatrics Perelman School of Medicine, University of
Pediatric Respiratory Disease: A Model for the Future of Emergency Medicine Research Joseph J. Zorc, MD, MSCE Mark Fishman Professor, Department of Pediatrics Perelman School of Medicine, University of
SYNOPSIS. Study center(s) This study was conducted in the United States (128 centers).
 Drug product: Drug substance(s): Document No.: Edition No.: Study code: Date: SYMBICORT pmdi 160/4.5 µg Budesonide/formoterol SD-039-0725 17 February 2005 SYNOPSIS A Twelve-Week, Randomized, Double-blind,
Drug product: Drug substance(s): Document No.: Edition No.: Study code: Date: SYMBICORT pmdi 160/4.5 µg Budesonide/formoterol SD-039-0725 17 February 2005 SYNOPSIS A Twelve-Week, Randomized, Double-blind,
Nguyen Tien Dung A/Prof. PhD. MD Head of Pediatric Department - Bach Mai Hospital
 Nguyen Tien Dung A/Prof. PhD. MD Head of Pediatric Department - Bach Mai Hospital A girl patient 11 years old admitted to Bach mai Hospital at 4h15, 12nd November because of difficult breathing She has
Nguyen Tien Dung A/Prof. PhD. MD Head of Pediatric Department - Bach Mai Hospital A girl patient 11 years old admitted to Bach mai Hospital at 4h15, 12nd November because of difficult breathing She has
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Edwards KM, Zhu Y, Griffin MR, et al. Burden of human metapneumovirus
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Edwards KM, Zhu Y, Griffin MR, et al. Burden of human metapneumovirus
Asthma Care in the Emergency Department Clinical Practice Guideline
 Asthma Care in the Emergency Department Clinical Practice Guideline Inclusion: 1) Children 2 years of age or older with a prior history of wheezing, and 2) Children less than 2 years of age with likely
Asthma Care in the Emergency Department Clinical Practice Guideline Inclusion: 1) Children 2 years of age or older with a prior history of wheezing, and 2) Children less than 2 years of age with likely
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Metered Dose Inhalers with Valved Holding Chamber: A Pediatric Hospital Experience
 Metered Dose Inhalers with Valved Holding Chamber: A Pediatric Hospital Experience 8th Annual North Regional Respiratory Care Conference Minnesota & Wisconsin Societies for Respiratory Care Mayo Civic
Metered Dose Inhalers with Valved Holding Chamber: A Pediatric Hospital Experience 8th Annual North Regional Respiratory Care Conference Minnesota & Wisconsin Societies for Respiratory Care Mayo Civic
Croup. Guideline for the Diagnosis and Management of. Definitions. Recommendations (see Algorithm) 2008 Update
 Guideline for the Diagnosis and Management of Croup Administered by the Alberta Medical Association 2008 Update This clinical practice guideline was developed by an Alberta Clinical Practice Guideline
Guideline for the Diagnosis and Management of Croup Administered by the Alberta Medical Association 2008 Update This clinical practice guideline was developed by an Alberta Clinical Practice Guideline
Dex single dose Pred- 5 day course Mean Difference Mean Difference Mean 3.5. Weight 100.0% IV, Fixed, 95% CI [-1.97, 0.37] 100.
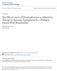
![Dex single dose Pred- 5 day course Mean Difference Mean Difference Mean 3.5. Weight 100.0% IV, Fixed, 95% CI [-1.97, 0.37] 100. Dex single dose Pred- 5 day course Mean Difference Mean Difference Mean 3.5. Weight 100.0% IV, Fixed, 95% CI [-1.97, 0.37] 100.](/thumbs/90/101418001.jpg) Question : In the child with asthma exacerbation in the ED should prednisolone/prednisone vs. dexamethasone be used to prevent hospitalization, decrease time in the ED or improve pulmonary function? Forest
Question : In the child with asthma exacerbation in the ED should prednisolone/prednisone vs. dexamethasone be used to prevent hospitalization, decrease time in the ED or improve pulmonary function? Forest
Acute Wheezing Emergencies: From Young to Old! Little Wheezers in the ED: Managing Acute Pediatric Asthma
 Acute Wheezing Emergencies: From Young to Old! Little Wheezers in the ED: Managing Acute Pediatric Asthma Talk Outline Case Delivery of bronchodilators Meter-dose inhalers and spacers Continuous nebulization
Acute Wheezing Emergencies: From Young to Old! Little Wheezers in the ED: Managing Acute Pediatric Asthma Talk Outline Case Delivery of bronchodilators Meter-dose inhalers and spacers Continuous nebulization
Infectious Upper Airway Obstruction
 Infectious Upper Airway Obstruction Prof. Muhi K. Al-Janabi MRCPCH; DCH; FICMS Consultant Pediatric Pulmonologist Objectives Viral croup Objectives 1. Know and understand the aetiology and natural history
Infectious Upper Airway Obstruction Prof. Muhi K. Al-Janabi MRCPCH; DCH; FICMS Consultant Pediatric Pulmonologist Objectives Viral croup Objectives 1. Know and understand the aetiology and natural history
ARTICLE. Annette Delgado, MD; Katherine J. Chou, MD; Ellen Johnson Silver, PhD; Ellen F. Crain, MD, PhD
 ARTICLE Nebulizers vs Metered-Dose Inhalers With Spacers for Bronchodilator Therapy to Treat Wheezing in Children Aged 2 to 24 Months in a Pediatric Emergency Department Annette Delgado, MD; Katherine
ARTICLE Nebulizers vs Metered-Dose Inhalers With Spacers for Bronchodilator Therapy to Treat Wheezing in Children Aged 2 to 24 Months in a Pediatric Emergency Department Annette Delgado, MD; Katherine
Croup v.2.0: ED Management
 Croup v.2.0: ED Executive Summary Test Your Knowledge Citation Information Inclusion Criteria Previously healthy children Age 6 months to 6 years Explanation of Evidence Ratings Summary of Version Changes
Croup v.2.0: ED Executive Summary Test Your Knowledge Citation Information Inclusion Criteria Previously healthy children Age 6 months to 6 years Explanation of Evidence Ratings Summary of Version Changes
Management of wheeze in pre-school children. Prof Colin Robertson, Respiratory Medicine, Royal Children s Hospital, Melbourne
 Management of wheeze in pre-school children Prof Colin Robertson, Respiratory Medicine, Royal Children s Hospital, Melbourne General Practitioner encounters for asthma Asthma in Australia, 2003 Emergency
Management of wheeze in pre-school children Prof Colin Robertson, Respiratory Medicine, Royal Children s Hospital, Melbourne General Practitioner encounters for asthma Asthma in Australia, 2003 Emergency
County of San Diego HEALTH AND HUMAN SERVICES AGENCY
 NICK MACCHIONE, FACHE DIRECTOR WILMA J. WOOTEN, M.D., M.P.H. PUBLIC HEALTH OFFICER Bruce E. Haynes, M.D. Medical Director Division of Emergency Medical Services 6255 Mission Gorge Road San Diego, CA 9212-3599
NICK MACCHIONE, FACHE DIRECTOR WILMA J. WOOTEN, M.D., M.P.H. PUBLIC HEALTH OFFICER Bruce E. Haynes, M.D. Medical Director Division of Emergency Medical Services 6255 Mission Gorge Road San Diego, CA 9212-3599
The Effectiveness of Dexamethasone as Adjunctive Therapy to Racemic Epinephrine for a Pediatric Patient With Bronchiolitis
 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-14-2010 The Effectiveness of Dexamethasone as Adjunctive Therapy to Racemic Epinephrine
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-14-2010 The Effectiveness of Dexamethasone as Adjunctive Therapy to Racemic Epinephrine
Severity Assessment. Can be given Q2 hours
 VIRAL CROUP ALGORITHM: Outpatient/ED Management Mild Severity Stridor only with activity/ agitation Suprasternal retractions only Normoxia, no tachypnea, no tachycardia Normal mental status Able to talk
VIRAL CROUP ALGORITHM: Outpatient/ED Management Mild Severity Stridor only with activity/ agitation Suprasternal retractions only Normoxia, no tachypnea, no tachycardia Normal mental status Able to talk
ADASUVE (LOXAPINE) INHALATION POWDER. EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS
 ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
T h e n e w e ng l a nd j o u r na l o f m e dic i n e
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e clinical practice Croup James D. Cherry, M.D., M.Sc. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
T h e n e w e ng l a nd j o u r na l o f m e dic i n e clinical practice Croup James D. Cherry, M.D., M.Sc. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
NOVEL INFLUENZA A (H1N1) Swine Flu
 Introduction Definitions Influenza-like Illness Emergency Department Assessment Anitiviral Medication Oseltamivir (Tamiflu) Dosing Infection Control Issues Staff Exposure References Introduction This guideline
Introduction Definitions Influenza-like Illness Emergency Department Assessment Anitiviral Medication Oseltamivir (Tamiflu) Dosing Infection Control Issues Staff Exposure References Introduction This guideline
Clinical Director for Women s and Children s Division
 UPPER AIRWAY OBSTRUCTION (UAO) (INCLUDING CROUP) CHILDREN & YOUNG PEOPLE 0-16 CLINICAL GUIDELINES Register No: 10097 Status: Public Developed in response to: Guideline Review CQC Fundamental Standard:
UPPER AIRWAY OBSTRUCTION (UAO) (INCLUDING CROUP) CHILDREN & YOUNG PEOPLE 0-16 CLINICAL GUIDELINES Register No: 10097 Status: Public Developed in response to: Guideline Review CQC Fundamental Standard:
Is Oral Dexamethasone Safe and Effective for Treating Asthma Exacerbations In Pediatric Patients?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Oral Dexamethasone Safe and Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Oral Dexamethasone Safe and Effective
Provincial Clinical Knowledge Topic Croup, Pediatric Emergency and Inpatient V 1.0
 Provincial Clinical Knowledge Topic Croup, Pediatric Emergency and Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
Provincial Clinical Knowledge Topic Croup, Pediatric Emergency and Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Asthma Coding Fact Sheet for Primary Care Pediatricians
 01/01/2017 Asthma Coding Fact Sheet for Primary Care Pediatricians Physician Evaluation & Management Services Outpatient 99201 99202 99203 99204 99205 Office or other outpatient visit, new patient; self
01/01/2017 Asthma Coding Fact Sheet for Primary Care Pediatricians Physician Evaluation & Management Services Outpatient 99201 99202 99203 99204 99205 Office or other outpatient visit, new patient; self
Respiratory infection what works Professor Terence Stephenson President Royal College of Paediatrics & Child Health
 Respiratory infection what works Professor Terence Stephenson President Royal College of Paediatrics & Child Health Nuffield Professor, Institute of Child Health, University College London & Great Ormond
Respiratory infection what works Professor Terence Stephenson President Royal College of Paediatrics & Child Health Nuffield Professor, Institute of Child Health, University College London & Great Ormond
ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS
 R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
Emergency Department Guideline. Asthma
 Emergency Department Guideline Inclusion criteria: Patients 2 years old with: o Known history of asthma or wheezing responsive to bronchodilators presenting to the ED with cough, wheeze, shortness of breath,
Emergency Department Guideline Inclusion criteria: Patients 2 years old with: o Known history of asthma or wheezing responsive to bronchodilators presenting to the ED with cough, wheeze, shortness of breath,
Asthma: Evaluate and Improve Your Practice
 Potential Barriers and Suggested Ideas for Change Key Activity: Initial assessment and management Rationale: The history and physical examination obtained from the patient and family interviews form the
Potential Barriers and Suggested Ideas for Change Key Activity: Initial assessment and management Rationale: The history and physical examination obtained from the patient and family interviews form the
INFORMATION FOR THE CONSUMER IMPORTANT INFORMATION YOU SHOULD KNOW ABOUT
 - 1 - INFORMATION FOR THE CONSUMER IMPORTANT INFORMATION YOU SHOULD KNOW ABOUT PULMICORT NEBUAMP (budesonide suspension for inhalation) Before using PULMICORT NEBUAMP, read this leaflet carefully. It contains
- 1 - INFORMATION FOR THE CONSUMER IMPORTANT INFORMATION YOU SHOULD KNOW ABOUT PULMICORT NEBUAMP (budesonide suspension for inhalation) Before using PULMICORT NEBUAMP, read this leaflet carefully. It contains
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant. Tara Brennan, MD 2,3
 Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Rapid Effects of Inhaled Corticosteroids in Acute Asthma Gustavo J. Rodrigo, MD.
 Rapid Effects of Inhaled Corticosteroids in Acute Asthma Gustavo J. Rodrigo, MD WWW.chestjournal.org Background: Current reviews on the use of inhaled corticosteroids (ICS) for acute asthma underestimated
Rapid Effects of Inhaled Corticosteroids in Acute Asthma Gustavo J. Rodrigo, MD WWW.chestjournal.org Background: Current reviews on the use of inhaled corticosteroids (ICS) for acute asthma underestimated
McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis. Optional #2 2017
 McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis Optional #2 2017 The tones go out at 3 am for a child with difficulty breathing. As it is a kid
McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis Optional #2 2017 The tones go out at 3 am for a child with difficulty breathing. As it is a kid
An Audit on Hospital Management of Bronchial Asthma
 An Audit on Hospital Management of Bronchial Asthma Pages with reference to book, From 298 To 300 Javaid A. Khan, Shehryar Saghir, Ghazala Tabassum, S. Fayyaz Husain ( Department of Medicine, The Aga Khan
An Audit on Hospital Management of Bronchial Asthma Pages with reference to book, From 298 To 300 Javaid A. Khan, Shehryar Saghir, Ghazala Tabassum, S. Fayyaz Husain ( Department of Medicine, The Aga Khan
Treatment of Acute Asthma Exacerbations in Adults in the Primary Care or Urgent Care Setting Clinical Practice Guideline MedStar Health.
 Treatment of Acute Asthma Exacerbations in Adults in the Primary Care or Urgent Care Setting Clinical Practice Guideline MedStar Health Background: These guidelines are provided to assist physicians and
Treatment of Acute Asthma Exacerbations in Adults in the Primary Care or Urgent Care Setting Clinical Practice Guideline MedStar Health Background: These guidelines are provided to assist physicians and
TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Croup Evidence-Based Guideline
 TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Croup Evidence-Based Guideline Definition: Croup, also known as laryngotracheobronchitis, is a respiratory illness that results in inflammation
TEXAS CHILDREN S HOSPITAL EVIDENCE-BASED OUTCOMES CENTER Croup Evidence-Based Guideline Definition: Croup, also known as laryngotracheobronchitis, is a respiratory illness that results in inflammation
Nebulized hypertonic saline treatment in hospitalized children with moderate to severe viral bronchiolitis
 ORIGINAL ARTICLE INFECTIOUS DISEASES Nebulized hypertonic saline treatment in hospitalized children with moderate to severe viral bronchiolitis Z. Luo, Z. Fu, E. Liu, X. Xu, X. Fu, D. Peng, Y. Liu, S.
ORIGINAL ARTICLE INFECTIOUS DISEASES Nebulized hypertonic saline treatment in hospitalized children with moderate to severe viral bronchiolitis Z. Luo, Z. Fu, E. Liu, X. Xu, X. Fu, D. Peng, Y. Liu, S.
beclometasone 100 MDI 2 puffs twice a day (recently changed to non CFC (Clenil Modulite))
 Case 1 Mr Thomson, a 32 year old asthmatic who is well known to you comes into your pharmacy. He is known to have a best peak flow of 640 L/min. He tells you that over the last few weeks he has been wakening
Case 1 Mr Thomson, a 32 year old asthmatic who is well known to you comes into your pharmacy. He is known to have a best peak flow of 640 L/min. He tells you that over the last few weeks he has been wakening
Appendix D Clinical specialist statement template
 Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Practical Approach to Managing Paediatric Asthma
 Practical Approach to Managing Paediatric Asthma Dr Andrew Tai FRACP, PhD Paediatric Respiratory and Sleep Specialist Women's and Children's Hospital, Adelaide Approaching the patient Check the diagnosis
Practical Approach to Managing Paediatric Asthma Dr Andrew Tai FRACP, PhD Paediatric Respiratory and Sleep Specialist Women's and Children's Hospital, Adelaide Approaching the patient Check the diagnosis
Budesonide treatment of moderate and severe asthma in children: A doseresponse
 Budesonide treatment of moderate and severe asthma in children: A doseresponse study Soren Pedersen, MD, PhD, and Ove Ramsgaard Hansen, MD Kolding, Denmark Objective: The purpose of the study was to evaluate
Budesonide treatment of moderate and severe asthma in children: A doseresponse study Soren Pedersen, MD, PhD, and Ove Ramsgaard Hansen, MD Kolding, Denmark Objective: The purpose of the study was to evaluate
A preliminary assessment of nurses asthma education needs and the effect of a training. programme in an urban tertiary healthcare facility.
 A preliminary assessment of nurses asthma education needs and the effect of a training programme in an urban tertiary healthcare facility O O Adeyeye, Y A Kuyinu, R T Bamisile, and C I Oghama Abstract
A preliminary assessment of nurses asthma education needs and the effect of a training programme in an urban tertiary healthcare facility O O Adeyeye, Y A Kuyinu, R T Bamisile, and C I Oghama Abstract
IDPH ESF-8 Plan: Pediatric and Neonatal Surge Annex Sample Pediatric Admission Orders 2015
 Purpose: To provide guidance to practitioners caring for pediatric patients who need inpatient hospital care during a disaster. Disclaimer: This guideline is not meant to be all inclusive, replace an existing
Purpose: To provide guidance to practitioners caring for pediatric patients who need inpatient hospital care during a disaster. Disclaimer: This guideline is not meant to be all inclusive, replace an existing
Common Pediatric Respiratory Illness and Emergencies
 Common Pediatric Respiratory Illness and Emergencies Rob Cloutier, MD Assistant Professor Emergency Medicine & Pediatrics Oregon Health & Science University Overview Review key differences between pediatric
Common Pediatric Respiratory Illness and Emergencies Rob Cloutier, MD Assistant Professor Emergency Medicine & Pediatrics Oregon Health & Science University Overview Review key differences between pediatric
Secondary Outcome/Efficacy Variable(s):
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Recommended Component: Assure Immediate Access to Medications as Prescribed
 Recommended Component: Assure Immediate Access to Medications as Prescribed Students must have immediate access to all medications as approved by healthcare providers and parents, regardless of the availability
Recommended Component: Assure Immediate Access to Medications as Prescribed Students must have immediate access to all medications as approved by healthcare providers and parents, regardless of the availability
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
2/12/2015. ASTHMA & COPD The Yin &Yang. Asthma General Information. Asthma General Information
 ASTHMA & COPD The Yin &Yang Arizona State Association of Physician Assistants March 6, 2015 Sedona, Arizona Randy D. Danielsen, PhD, PA-C, DFAAPA Dean & Professor A.T. Still University Asthma General Information
ASTHMA & COPD The Yin &Yang Arizona State Association of Physician Assistants March 6, 2015 Sedona, Arizona Randy D. Danielsen, PhD, PA-C, DFAAPA Dean & Professor A.T. Still University Asthma General Information
Setting The setting was outpatient departments of referral hospitals. The economic analysis was conducted in India.
 Three day versus five day treatment with amoxicillin for non-severe pneumonia in young children: a multicentre randomised controlled trial ISCAP study group Record Status This is a critical abstract of
Three day versus five day treatment with amoxicillin for non-severe pneumonia in young children: a multicentre randomised controlled trial ISCAP study group Record Status This is a critical abstract of
INFLUENZA VACCINATION AND MANAGEMENT SUMMARY
 INFLUENZA VACCINATION AND MANAGEMENT SUMMARY Morbidity and mortality related to influenza occur at a higher rate in people over 65 and those with underlying chronic medical conditions. Annual influenza
INFLUENZA VACCINATION AND MANAGEMENT SUMMARY Morbidity and mortality related to influenza occur at a higher rate in people over 65 and those with underlying chronic medical conditions. Annual influenza
PEDIATRIC ASTHMA INPATIENT CARE MAP
 DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
Supplementary Medications during asthma attack. Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus
 Supplementary Medications during asthma attack Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus Conflicts of Interest None Definition of Asthma Airway narrowing that is
Supplementary Medications during asthma attack Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus Conflicts of Interest None Definition of Asthma Airway narrowing that is
Title Protocol for the Management of Asthma
 Document Control Title Protocol for the Management of Asthma Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and Resilience Department Version
Document Control Title Protocol for the Management of Asthma Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and Resilience Department Version
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
Critical Appraisal. Dave Abbott Senior Medicines Information Pharmacist
 Critical Appraisal Dave Abbott Senior Medicines Information Pharmacist Aims Identify key components of clinical trial design and apply these to a critical appraisal of the literature Be able to work out
Critical Appraisal Dave Abbott Senior Medicines Information Pharmacist Aims Identify key components of clinical trial design and apply these to a critical appraisal of the literature Be able to work out
Pediatric Respiratory Distress. Dr. Karen Forward Dr. Mike Peddle
 Pediatric Respiratory Distress Dr. Karen Forward Dr. Mike Peddle Objectives Discuss epidemiology & causes of respiratory distress in pediatric patients Identify differences between the pediatric and adult
Pediatric Respiratory Distress Dr. Karen Forward Dr. Mike Peddle Objectives Discuss epidemiology & causes of respiratory distress in pediatric patients Identify differences between the pediatric and adult
Oxygen and Oxygen Equipment
 Oxygen and Oxygen Equipment I. Policy University Health Alliance (UHA) will reimburse for home oxygen and oxygen equipment when it is determined to be medically necessary and when it meets the medical
Oxygen and Oxygen Equipment I. Policy University Health Alliance (UHA) will reimburse for home oxygen and oxygen equipment when it is determined to be medically necessary and when it meets the medical
INPATIENT ASTHMA CARE PROTOCOL
 INPATIENT ASTHMA CARE PROTOCOL When ordered by a physician, an eligible child 2 years of age or older who is admitted to the General Pediatric Inpatient Unit at the Children s Hospital of Georgia with
INPATIENT ASTHMA CARE PROTOCOL When ordered by a physician, an eligible child 2 years of age or older who is admitted to the General Pediatric Inpatient Unit at the Children s Hospital of Georgia with
The treatment of postnatal depression: a comprehensive literature review Boath E, Henshaw C
 The treatment of postnatal depression: a comprehensive literature review Boath E, Henshaw C Authors' objectives To evalute treatments of postnatal depression. Searching MEDLINE, PsycLIT, Sociofile, CINAHL
The treatment of postnatal depression: a comprehensive literature review Boath E, Henshaw C Authors' objectives To evalute treatments of postnatal depression. Searching MEDLINE, PsycLIT, Sociofile, CINAHL
Croup: Emergency Department Clinical Practice Guideline
 Croup: Emergency Department Clinical Practice Guideline Clinical Practice Guideline Approved by: Division of Pediatric Emergency Medicine and Otolaryngology Date(s) of Approval: January 219 Date Created:
Croup: Emergency Department Clinical Practice Guideline Clinical Practice Guideline Approved by: Division of Pediatric Emergency Medicine and Otolaryngology Date(s) of Approval: January 219 Date Created:
Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet
 1 Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet 1 Name of Guideline / Policy/ Procedure MANAGEMENT OF ACUTE PAEDIATRIC ASTHMA Purpose of Procedure/
1 Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet 1 Name of Guideline / Policy/ Procedure MANAGEMENT OF ACUTE PAEDIATRIC ASTHMA Purpose of Procedure/
Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis. Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine
 Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine Asthma Defined National Asthma Education and Prevention
Wheezy? Easy Peasy! The Emergent Management of Asthma & Bronchiolitis Maneesha Agarwal MD Assistant Professor of Pediatrics & Emergency Medicine Asthma Defined National Asthma Education and Prevention
Discuss the benefits for developing an outpatient bronchiolitis clinic.
 Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Medical Center Discuss the benefits for developing an outpatient bronchiolitis clinic. 1 Definition Inflammation of the bronchioles
Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Medical Center Discuss the benefits for developing an outpatient bronchiolitis clinic. 1 Definition Inflammation of the bronchioles
SYNOPSIS. First subject enrolled 15 August 2003 Therapeutic confirmatory (III) Last subject completed 03 February 2005
 Drug product: SYMBICORT pmdi 160/4.5 μg Drug substance(s): Budesonide/formoterol Study code: SD-039-0728 Edition No.: FINAL Date: 27 February 2006 SYNOPSIS A 52-week, randomized, double-blind, single-dummy,
Drug product: SYMBICORT pmdi 160/4.5 μg Drug substance(s): Budesonide/formoterol Study code: SD-039-0728 Edition No.: FINAL Date: 27 February 2006 SYNOPSIS A 52-week, randomized, double-blind, single-dummy,
