Paediatric Tonsillectomy Clinical Guidelines. With or without adenoidectomy
|
|
|
- Adele Whitehead
- 6 years ago
- Views:
Transcription
1 Paediatric Tonsillectomy Clinical Guidelines With or without adenoidectomy
2 Table of Contents Pre-procedure recommendations... 3 Risk assessment for post-operative bleeding... 3 Diagnosis for Obstructive Sleep Apnea Syndrome... 3 Indications for paediatric respiratory investigation... 4 Fever... 4 Fasting guidelines... 4 Prescription of intravenous (IV) fluids... 5 Parent/caregiver and patient education... 5 Medication... 5 Nutrition... 5 Parent stressors... 5 Management of anxiety in children... 6 Toys and other distractions... 6 Information and resources... 6 Talking to children about the procedure... 6 Anesthesia consult... 7 Pain management counselling... 8 Intra-operative recommendations... 8 Topical anaesthetics for IV placement... 8 Local anaesthesia... 8 Steroids... 8 Acetaminophen... 8 Ketamine... 9 NSAIDS... 9 Analgesia for patients with known or suspected OSAS... 9 Post-operative recommendations... 9 Pain management... 9 Antibiotics... 9 Discharge planning and complication management...10 Management of post-operative bleeding...10 Management of post-operative fever...10 Guidelines for potential extended observation / hospital admission due to complications postoperatively...10 Information for parents/caregivers with pre- and post-operative instructions...10 References...12 Appendix A...13 Appendix B...14 Appendix C...15 Appendix D...16 Page 2 of 16
3 Pre-procedure recommendations Risk assessment for post-operative bleeding Prior to operative intervention patients should undergo a risk assessment for post-operative hemorrhage. This should include: Both a patient history and family history of bleeding disorders. Patients without a bleeding history do not require routine coagulation screening prior to surgery. Medication history assessment to determine potential risks for increased post-operative hemorrhage in children who are taking over the counter (OTC), and/or natural health products, and/or prescription medications. Diagnosis for Obstructive Sleep Apnea Syndrome Obstructive Sleep Apnea Syndrome (OSAS) is one of the major risk factors contributing to the occurrence of post-operative respiratory complications. An overnight sleep study (polysomnography) is considered to be the gold standard for diagnosis of OSAS. In the absence of a sleep study, patient history and examination using physical markers and overnight oximetry monitoring can be used to determine the presence of risk factors. The Clinical Practice Guideline for diagnosis and management of childhood OSAS from the American Academy of Paediatrics recommends: History Frequent snoring (> 3 nights/week) Laboured breathing during sleep Gasps/snorting noises Observed episodes of apnea Sleep enuresis (especially secondary enuresis after at least 6 months of continence) Sleeping in a seated position or with the neck hyperextended Cyanosis Headaches on awakening Daytime sleepiness Attention deficit/hyperactivity disorder Learning problems Physical Examination Under/over weight Tonsillar hypertrophy Adenoidal facies Micrognathia/retrognathia High-arched palate Failure to thrive Hypertension Page 3 of 16
4 Patients with suspected severe OSAS should be considered for admission to hospital for their surgery. Indications for paediatric respiratory investigation The following indications should be considered for paediatric respiratory investigations such as a sleep study, pulmonary function tests, overnight oximetry monitoring and an arterial blood gas: Diagnosis of OSAS unclear or inconsistent Down syndrome Cerebral palsy Hypotonia or neuromuscular disorders Significant Craniofacial anomalies Mucopolysaccharidosis Obesity (body mass index > 2.5 standard deviation scores or > 99th percentile for age and gender) Significant co-morbidity such as congenital heart disease, chronic lung disease Residual symptoms after adenotonsillectomy Other indications based on the Tonsillectomy QBP Clinical Expert Advisory Group: Age < 2 years Failure to thrive Pulmonary hypertension Sickle cell disease Fever A patient presenting on day of surgery with a new onset of fever is an indication for cancelling the surgery. The decision to go ahead with surgery or not is one that will be made by both the anesthesiologist and surgeon based on the child s medical history and condition. The recommended guidelines for fever are: 37.5 C via axilla reading 38 C via temporal reading Fasting guidelines The pre-operative fasting guidelines for scheduled tonsillectomy surgery are as follows: Water and clear fluids permitted up to 2 hours before induction of anesthesia. Breast milk may be given up to 4 hours before induction of anesthesia. Formula or cow's milk may be given up to 6 hours before induction of anesthesia. Solid food may be given up to 8 hours before induction of anesthesia. Page 4 of 16
5 Clear fluids or any type of liquids that you can see through clearly when poured into a glass. Examples of clear fluids include water, apple juice, Pedialyte and Gatorade. Prescription of intravenous (IV) fluids The use of isotonic fluid (e.g. Lactated Ringer s solution) is recommended in most circumstances to provide IV fluid maintenance requirements. Parent/caregiver and patient education Parental/caregiver anxiety is a common phenomenon and can be a significant predictor of a child s anxiety before surgery. Timely information, tailored to the needs and concerns of parents/caregivers and children, is recommended in order to decrease intraoperative stress for the child, improve patient compliance, improve outcomes and family satisfaction. Medication Discuss with the parent/caregiver which prescribed home medications their child should take on the day of surgery. Be sure to include and discuss any over-the-counter medications as well as any natural health products. These medications will need to be stopped two weeks prior to surgery and two weeks after surgery as these products may affect bleeding. Nutrition Reinforce the above mentioned pre-operative fasting guidelines for their child on day of surgery. Discuss the importance regarding appropriate nutrition for parent/caregivers on the day of surgery. It is important to remember and care for their nutritional needs. Parent stressors Realize that helping their child through the experience of surgery can be exhausting for the parent/caregiver. Help them think about what will assist them to be at their best for their child. Finding out who can support them with tasks like picking other children up from school can be a great stress reducer. Remind the parent/caregiver to bring something they can do for themselves while waiting for their child s surgery to be done or when they get home. Reducing the parent/caregivers stresses and anxieties will go a long way in reducing their child's anxieties. Most children go home after the procedure; however, instruct the parent to bring items the child may need overnight in case the child has to stay. Inform the parent/caregiver that their child will be monitored closely by nurses in the recovery room, but if there is a concern with how their child is breathing or if the child is not taking in enough fluids, then their child may need to stay overnight for observation. Page 5 of 16
6 Parents/caregivers may be anxious about what happens to their child during surgery. Let parents/caregivers know that the health care team (surgeon, anaesthetist, nurses) are focused on their child, at all times, to ensure the best possible outcome of the procedure. They can expect a visit from the surgeon in the waiting area directly following the operation. Management of anxiety in children Surgery has been shown to cause anxiety in children, which in turn may result in short and long term negative outcomes. The surgical team will provide resources to facilitate patient comfort and to reduce perceived and actual psychological anxiety and behavioural issues in children preparing for surgery. Toys and other distractions Instruct the parent/caregiver to bring the child's favourite toy. Familiar objects help children feel more comfortable in a strange place. These items can serve as a security blanket and can accompany the child into surgery and the recovery room. A favorite pillow or blanket may also offer comfort. Grace's Place Paediatric Surgery Waiting Room is upgraded and has a television and video games to play, but as there are many children using them, let the parent/caregiver know that they are welcome to bring in ipads or other hand-held gaming devices to use while waiting for surgery. Information and resources Direct the parent/caregiver to North York General Hospital s (NYGH) external website ( for information pertaining to our pre, intra and post-operative care for tonsillectomy with/out adenoidectomy. Give the parents the one page handout that includes preoperative instructions (Appendix A). From the NYGH website, families will have access to other external links i.e. SickKids Hospital and Children s Hospital of Eastern Ontario for more information. Talking to children about the procedure It s important to prepare children and youth for the anesthetic and upcoming surgery. Knowing what to expect on the day of surgery will help the child or teen cope. Encourage the parent/caregiver to tell the truth about what will happen and provide information based on the child's age. Talking to pre-school children (3-6 years) Preschool children may not fully understand why surgery is needed. The parent/caregiver can help by: Page 6 of 16
7 Talking about the surgery 2-3 days ahead of time using a calm and relaxed voice Talking about the hospital and explaining that it is a safe place and the staff are there to help Using play to help the child understand the surgery (toy medical kits or books) Avoiding bribes or negative feedback. Talking to school aged children (6-12 years) School aged children have a basic understanding of how their bodies work. Start preparing your child a week or more ahead of time. They need time to ask questions and talk about their feelings. The parent/caregiver can help by: Encouraging the child to ask questions and express feelings. Avoiding bribes or negative feedback. Talking to youth (12-18 years) Youth are more independent and should become involved in their health care. They may ask for detailed explanations. They are often worried about privacy. The parent/caregiver can help by: Being honest. Teens have a right to know about everything that will happen. Encouraging the teen to ask questions of you or hospital staff. Giving space so the teen can speak to the doctor or nurse alone. Reminding the teen that it s OK to feel angry or worried. Children with special needs It is important to find out how best to communicate and interact with a child with special needs. Discuss this with the parent/caregiver so that this can be added to the patient s history. Then those caring for the child day of surgery will understand how the child reacts and the health care team will be better able to respond to whatever fears or worries the child may have. If the child wears hearing aids or glasses, etc., let the parent/caregiver know that these items can stay with the child and accompany them into the operating room. These items will be returned soon after the operation. Anaesthesia consult Pediatric patients identified as requiring an anesthetic consult prior to surgery will receive their consult in the Pre-Operative Clinic at a scheduled time before the day of surgery. All other patients will receive their consultation with the anaesthesiologist on the day of surgery. The parent/caregiver and child will meet the anesthesiologist in Grace's Place Pediatric Surgery Waiting Room before surgery. This time will be used to talk about the child's medical history, condition, and to provide suggestions for helping the child through surgery. The anesthesiologist will discuss the anesthesia plan with the parent/caregiver. This is also the time when there will be discussion about the post-operative plan of care including, but not limited to, possibility for hospitalization and pain management at home. Page 7 of 16
8 Pain management counselling Examine the parent/caregiver's level of anxiety in relation to post-operative pain their child will experience. It is recommended to reinforce the guidelines for type, dosing and timing of postoperative medications mentioned later in this booklet. Intra-operative recommendations Topical anaesthetics for IV placement Topical anesthetic is recommended for IV placement prior to anesthesia induction in patients where an inhalational induction is not planned in order to minimize pain associated with line insertion. The use of anesthetic cream/ vapocoolant spray before IV insertion has been shown to be both safe and effective in decreasing pain during IV placement. Local anaesthesia Topical Application of: Bupivacaine 0.5% plain applied directly on the Tonsillar/adenoid bed. Steroids Based on available evidence, a single intra-operative dose of IV steroids (Dexamethasone) is strongly recommended as a safe and effective treatment for reducing morbidity from paediatric tonsillectomy/adenoidectomy. Based on available literature, Dexamethasone 0.1mg/kg dose IV is recommended, up to a maximum of 8mg/dose. Acetaminophen Administration of Acetaminophen is strongly recommended for management of post-operative pain. The intraoperative dose of Acetaminophen is 40 mg/kg suppository dose per rectum. The next dose will be 15 mg/kg PO q6h around the clock for 24 hours (the maximum dose in the first 24hrs is 90 mg/kg including the intra-operative dose). After the first 24 hours, the maximum dose per day is 75 mg/kg. EXCLUSION criteria for a maximum of 90 mg/kg/ 24 hour dosing: Hepatic impairment, underlying metabolic problems. Concomitant drugs that induce CYP450 enzymes (e.g. Phenobarbital, phenytoin, rifampin, isoniazid, dexamethasone). Chronic malnutrition. Page 8 of 16
9 Ketamine Ketamine is not recommended for intraoperative pain control in paediatric tonsillectomy/ adenoidectomy patients. NSAIDS Ketorolac is safe to use and will be used intraoperative after hemostasis has been attained. The recommended IV dose is 0.5 mg/kg up to a maximum 30 mg/kg. Analgesia for patients with known or suspected OSAS Evidence indicates increased sensitivity to narcotics and other anesthetic drugs with central respiratory and sedating effects, among patient with OSAS and obesity. An individualized anesthesia plan may involve a reduction in opioid analgesic dose e.g. Morphine or 0.03 mg/kg IV, reducing doses or avoiding Gravol or other sedation medications, and relying on nonsedating methods of pain control such as Acetaminophen, NSAIDs, and other topical local anaesthetics. Post-operative recommendations Pain management Acetaminophen and Morphine are recommended as primary pharmacologic agents for treatment of post-operative pain. Ibuprofen may be used if there are intolerance issues with Morphine or if pain control is inadequate with Acetaminophen and Morphine. Morphine: Start low and titrate up with small increments. Intravenous: Suggested maximum starting dose is 0.05 mg/kg/dose IV q 2-4 hours as needed with a usual maximum starting dose of 2.5 to 5 mg/dose. **For patients with OSAS the suggested maximum starting dose is mg/kg/dose. Oral: Maximum starting dose is 0.1 to 0.2 mg/kg/dose PO q4-6h as needed with a maximum starting dose of 10 mg/dose. Acetaminophen: 15 mg/kg/dose PO or PR every 4 to 6 hours as needed (not to exceed 90 mg/kg/ day or 4 grams / day, whichever is less). Ibuprofen: 5-10 mg/kg/ dose PO every 6 to 8 hours as needed (not to exceed 40 mg/kg/ day or 2.4 grams / day, whichever is less). Antibiotics: Antibiotics will not be given in paediatric tonsillectomy / adenoidectomy patients. Individual consideration should be taken into account in instances where other co-morbidities may require the use of antibiotics in facilitating post-tonsillectomy recovery. Page 9 of 16
10 Discharge planning and complication management Management of post-operative bleeding If patient presents to the Emergency Department for bleeding, they will be seen by the emergency physician who will then consult with the ENT surgeon. The ENT surgeon will then consult the paediatrician if required. (Appendix D). Management of post-operative fever If patient presents to the Emergency Department for fever/dehydration, they will be seen by the emergency physician who will then consult with the paediatrician if required. (Appendix D). Guidelines for potential extended observation / hospital admission due to complications postoperatively Age < 2 Obesity (body mass index > 2.5 standard deviation scores or > 99 th percentile for age or gender) OSAS without pulmonary hypertension or co-morbidities If a patient continuously desaturates without O 2 Signs and symptoms of stridor, noisy breathing or apneas during sleep Periods of shallow breathing Uncontrolled pain Post-op bleeding Information for parents/caregivers with pre- and post-operative instructions Pamphlets and a one page, easy to read handout have been created with input by both the Tonsillectomy Quality Based Procedures Committee, including review by a Patient and Family Advisor. (Appendix A, B & C). The handout/ pamphlet can be given to parents/caregivers at the physician s office, Day Surgery Unit, Child and Teen Unit or by accessing the electronic version on North York General Hospital website. Information in the Pre-operative Pamphlet includes: Talking to children about the procedure Importance of bringing a toy or other distractions Child presenting day of surgery with a fever Fasting guidelines prior to surgery It is important that the parent/caregiver take care themselves Information on location and parking at NYGH Page 10 of 16
11 The pre-operative one page handout includes much of the same information as on the preoperative pamphlet but has been designed with pictures and is intended for families where English is not their first language. Information on the Post-operative Pamphlet includes: Nutrition and fluids Nausea and vomiting Mouth care Bleeding Activity Fever Pain Medications and side effects Next dose of medication once they arrive home Page 11 of 16
12 References Anderson, B., Kanagasundarum, S., & Woollard, G. (1996). Analgesic efficacy of paracetamol in children using tonsillectomy as a pain model. Anaesthesia and Intensive Care, 24: Anderson, B.J., Holford, N.H.G., Woollard, G.A., et al. (1999). Perioperative pharmacodynamics of acetaminophen analgesia in children. Anesthesiology, 90: Association of Paediatric Anaesthetists of Great Britain and Ireland. (2013). Codeine and paracetamol in paediatric use. 4 th November; updated version. Retrieved on December 18, 2014 from: ember%202013%20.pdf Association of Paediatric Anaesthetists of Great Britain and Ireland. (2012). Pediatric anesthesia good practice. Postoperative and Procedural Pain Management, 2nd ed. (2, Suppl 1): Birmingham, P.K., Tobin, M.J., Henthorn, T.K., et al. (1997). Twenty-four-hour pharmacokinetics of rectal acetaminophen in children: An old drug with new recommendations. Anesthesiology, 87: Baugh, R., Archer, S., Mitchell, R., Rosenfeld, R., Amin, R., Burns, J., & Patel, M. (2011). Clinical practice guideline: Tonsillectomy in children. Otolaryngology - Head and Neck Surgery, 144(1 Suppl):S1-30. Provincial Council for Maternal and Child Health. (2014, Feb). Quality based procedure tonsillectomy with or without adenoidectomy toolkit. Riggin, L., Ramakrishna, J., Sommer, D.D., & Koren, G. (2013). A 2013 updated systematic review & meta-analysis 36 randomized controlled trials of non-steroidal antiinflammatory agents on the risk of bleeding after tonsillectomy. Clinical Otolaryngology, 38: Sullivan, J.E., & Farrar, H.C. (2011). The Section on Clinical Pharmacology and Therapeutics and Committee on Drugs. Fever and antipyretic use in children. Pediatrics, 127: St-Onge, A. (2012, Dec). Reducing paediatric anxiety preoperatively: strategies for nurses. ORNAC Journal, 30(4): The Children s Hospital of Eastern Ontario. (n.d.). Getting ready for surgery: Talking about the surgery with your child. Retrieved on December 5, 2014 from: The Hospital for Sick Children. (n.d.). Talking to my children about surgery. Retrieved on December 5, 2014 from: Page 12 of 16
13 Appendix A Page 13 of 16
14 Appendix B Page 14 of 16
15 Appendix C Page 15 of 16
16 Appendix D POST-OP TONSILLECTOMY PEDIATRIC PATIENT PRESENTS TO EMERGENCY DEPARTMENT at NYGH Patient presents with FEVER and/or DEHYDRATION Patient presents with BLEEDING Patient seen by Emergency Physician Patient seen by Emergency Physician Consult with ENT Surgeon Pediatric MD Consult needed? NO YES Physician/Surgeon manages patient care Physician/Surgeon collaborates with PEDIATRICIAN regarding patient care Page 16 of 16
Paediatric Quality-Based Procedures Tonsillectomy with and without Adenoidectomy
 Paediatric Quality-Based Procedures Tonsillectomy with and without Adenoidectomy Webinar #1 (Feb 19 th, 2014) and Webinar #2 (Mar 27 th, 2014) Questions & Answers Q 1 Is the webinar presentation being
Paediatric Quality-Based Procedures Tonsillectomy with and without Adenoidectomy Webinar #1 (Feb 19 th, 2014) and Webinar #2 (Mar 27 th, 2014) Questions & Answers Q 1 Is the webinar presentation being
Frequently Asked Questions
 Page 1 Frequently Asked Questions Codeine and all multiple-ingredient products containing codeine are restricted on the AHS Provincial Drug Formulary to patients 18 years of age and older. 1. What does
Page 1 Frequently Asked Questions Codeine and all multiple-ingredient products containing codeine are restricted on the AHS Provincial Drug Formulary to patients 18 years of age and older. 1. What does
Pediatric Sleep Disorders
 Pediatric Sleep Disorders S. SHAHZEIDI, MD, FAAP, FCCP, FAASM GRAND HEALTH INSTITUTE Objectives Discuss the importance of screening for snoring Explain the signs and symptoms of parasomnias and sleep apnea
Pediatric Sleep Disorders S. SHAHZEIDI, MD, FAAP, FCCP, FAASM GRAND HEALTH INSTITUTE Objectives Discuss the importance of screening for snoring Explain the signs and symptoms of parasomnias and sleep apnea
Day care adenotonsillectomy in sleep apnoea
 Day care adenotonsillectomy in sleep apnoea Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Day care adenotonsillectomy in presence of sleep apnoea 1a 2a 2b Contact
Day care adenotonsillectomy in sleep apnoea Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Day care adenotonsillectomy in presence of sleep apnoea 1a 2a 2b Contact
Anesthetic Risks of Obstructive Sleep Apnea in Children
 Anesthetic Risks of Obstructive Sleep Apnea in Children Dawn M. Sweeney, M.D. Associate Professor of Anesthesiology and Pediatrics University of Rochester Medical Center Risk Factors for OSA in Children
Anesthetic Risks of Obstructive Sleep Apnea in Children Dawn M. Sweeney, M.D. Associate Professor of Anesthesiology and Pediatrics University of Rochester Medical Center Risk Factors for OSA in Children
Clinical Practice Guideline: Tonsillectomy in Children, Baugh et al Otolaryngology Head and Neck Surgery, 2011 J and: 144 (1 supplement) S1 30.
 Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Codeine and Paracetamol in Paediatric use, an Update 5 th October 2013
 Codeine and Paracetamol in Paediatric use, an Update 5 th October 2013 This guidance should be read in parallel to the detailed guidelines on pain management in children (APA guidelines) 2 nd edition.
Codeine and Paracetamol in Paediatric use, an Update 5 th October 2013 This guidance should be read in parallel to the detailed guidelines on pain management in children (APA guidelines) 2 nd edition.
Colonic (Large Intestine) Manometry
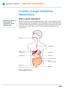 Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Post Tonsillectomy Pain Presented by: Dr.Z.Sarafraz Otolaryngologist
 Post Tonsillectomy Pain Presented by: Dr.Z.Sarafraz Otolaryngologist Tonsillectomy is a common surgery in children Post tonsillectomy pain is an important concern. Duration &severity of pain depend on:
Post Tonsillectomy Pain Presented by: Dr.Z.Sarafraz Otolaryngologist Tonsillectomy is a common surgery in children Post tonsillectomy pain is an important concern. Duration &severity of pain depend on:
Sleep-Disordered Breathing in Children and a Critical Review of T&A. Objectives. No disclosures
 Sleep-Disordered Breathing in Children and a Critical Review of T&A No disclosures Anna Meyer, MD, FAAP Pediatric Otolaryngology Otolaryngology-Head & Neck Surgery UCSF February 2014 1 Objectives Summarize
Sleep-Disordered Breathing in Children and a Critical Review of T&A No disclosures Anna Meyer, MD, FAAP Pediatric Otolaryngology Otolaryngology-Head & Neck Surgery UCSF February 2014 1 Objectives Summarize
New Guidelines for Tonsillectomy Daniel C. Chelius, Jr., MD Pediatric Otolaryngolo Pediatric Otolary gy--head Head and Neck S and Neck u S rgery
 New Guidelines for Tonsillectomy Daniel C. Chelius, Jr., MD Pediatric Otolaryngology-Head and Neck Surgery November 16, 2011 EXIT Procedures Sinus surgery/skull base surgery Head and Neck Cancers Thyroid/Parathyroid
New Guidelines for Tonsillectomy Daniel C. Chelius, Jr., MD Pediatric Otolaryngology-Head and Neck Surgery November 16, 2011 EXIT Procedures Sinus surgery/skull base surgery Head and Neck Cancers Thyroid/Parathyroid
The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions
 The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions Pain control is a key part of your care after surgery. It can help speed recovery and improve the results of your surgery. This handout
The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions Pain control is a key part of your care after surgery. It can help speed recovery and improve the results of your surgery. This handout
TONSILLECTOMY WHAT ARE THE TONSILS?
 WHAT ARE THE TONSILS? The tonsils are two pads of tissue located on either side of the back of the throat. Tonsils can become enlarged in response to recurrent tonsil infections or strep throat. They can
WHAT ARE THE TONSILS? The tonsils are two pads of tissue located on either side of the back of the throat. Tonsils can become enlarged in response to recurrent tonsil infections or strep throat. They can
Pediatric Patient Selection for Ambulatory Surgery Centers
 Pediatric Patient Selection for Ambulatory Surgery Centers 2017 Dr. Alan Jay Schwartz: Hello. This is Alan Jay Schwartz, Editor-in-Chief of the American Society of Anesthesiologists 2017 Refresher Courses
Pediatric Patient Selection for Ambulatory Surgery Centers 2017 Dr. Alan Jay Schwartz: Hello. This is Alan Jay Schwartz, Editor-in-Chief of the American Society of Anesthesiologists 2017 Refresher Courses
POST-OP PAIN MANAGEMENT
 POST-OP PAIN MANAGEMENT You re Part of the Team Pain Management After Surgery Having a procedure or surgery to address a health issue can result in post-op (postoperative) pain. This pain can and should
POST-OP PAIN MANAGEMENT You re Part of the Team Pain Management After Surgery Having a procedure or surgery to address a health issue can result in post-op (postoperative) pain. This pain can and should
 Content provided by and used with permission from the Children s Hospital Boston Department of Otolaryngology and Communication Disorders www.napervillekidsent.com 630-761-5531 Page 1 Tonsillectomy &
Content provided by and used with permission from the Children s Hospital Boston Department of Otolaryngology and Communication Disorders www.napervillekidsent.com 630-761-5531 Page 1 Tonsillectomy &
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy
 Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Problem Based Learning Discussion: Perioperative management of the child with obstructive sleep apnea
 Problem Based Learning Discussion: Perioperative management of the child with obstructive sleep apnea Moderators: Allison Fernandez MBA MD and Deborah Schwengel MD Institution: Johns Hopkins School of
Problem Based Learning Discussion: Perioperative management of the child with obstructive sleep apnea Moderators: Allison Fernandez MBA MD and Deborah Schwengel MD Institution: Johns Hopkins School of
Your visit to theatre
 Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Parents, thank you for visiting this site. Below, we have outlined some questions that are frequently
 F r e q u e n t ly A s k e d Q u e s t i o n s SPS SOCIETY FOR PEDIATRIC SEDATION safe and sound Parents, thank you for visiting this site. Below, we have outlined some questions that are frequently asked
F r e q u e n t ly A s k e d Q u e s t i o n s SPS SOCIETY FOR PEDIATRIC SEDATION safe and sound Parents, thank you for visiting this site. Below, we have outlined some questions that are frequently asked
CLINICAL GUIDELINES ID TAG
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Guideline for the management of pain in children Kieran O Connor Anaesthetics ATICS Date Uploaded: 1 September 2016 Review
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Guideline for the management of pain in children Kieran O Connor Anaesthetics ATICS Date Uploaded: 1 September 2016 Review
Pain relief for your child after surgery
 Great Ormond Street Hospital for Children NHS Trust: Information for Families Pain relief for your child after surgery When coming into hospital, children and their families are often worried that they
Great Ormond Street Hospital for Children NHS Trust: Information for Families Pain relief for your child after surgery When coming into hospital, children and their families are often worried that they
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
POLICY All patients will be assessed for risk factors associated with OSA prior to any surgical procedures.
 Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Concerned. Surgery? About Pain After. Talk to Your Doctor About Reducing Postsurgical Pain
 Concerned About Pain After Surgery? Talk to Your Doctor About Reducing Postsurgical Pain Will it Hurt? How Will Pain After Surgery Be Treated? If you re about to have surgery or if you re thinking about
Concerned About Pain After Surgery? Talk to Your Doctor About Reducing Postsurgical Pain Will it Hurt? How Will Pain After Surgery Be Treated? If you re about to have surgery or if you re thinking about
Using Questionnaire Tools to Predict Pediatric OSA outcomes. Vidya T. Raman, MD Nationwide Children s Hospital October 201
 Using Questionnaire Tools to Predict Pediatric OSA outcomes Vidya T. Raman, MD Nationwide Children s Hospital October 201 NCH Conflict of Interest SASM $10,000 Grant NCH intramural/interdepartmental $38,000
Using Questionnaire Tools to Predict Pediatric OSA outcomes Vidya T. Raman, MD Nationwide Children s Hospital October 201 NCH Conflict of Interest SASM $10,000 Grant NCH intramural/interdepartmental $38,000
WRHA Surgery Program. Obstructive Sleep Apnea (OSA)
 WRHA Surgery Program Obstructive Sleep Apnea (OSA) March 2010 Prepared by WRHA Surgery & Anesthesiology Programs Objectives 1. Define obstructive sleep apnea (OSA). 2. Purpose of the guidelines. 3. Identify
WRHA Surgery Program Obstructive Sleep Apnea (OSA) March 2010 Prepared by WRHA Surgery & Anesthesiology Programs Objectives 1. Define obstructive sleep apnea (OSA). 2. Purpose of the guidelines. 3. Identify
Postoperative Analgesia for Children After Tonsillectomy
 Postoperative Analgesia for Children After Tonsillectomy A/Prof George Chalkiadis Pain Medicine Physician, Anaesthetist Head, Children s Pain Management Service, RCH Clinical Associate Professor, University
Postoperative Analgesia for Children After Tonsillectomy A/Prof George Chalkiadis Pain Medicine Physician, Anaesthetist Head, Children s Pain Management Service, RCH Clinical Associate Professor, University
Digital RIC. Rhode Island College. Linda M. Green Rhode Island College
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2013 The Relationship
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2013 The Relationship
Sedation in Children
 CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
The Children s Hospital, Oxford Sedation for clinical procedures Information for parents and carers
 The Children s Hospital, Oxford Sedation for clinical procedures Information for parents and carers What is sedation? Sedation can help your child by reducing anxiety before and during a clinical procedure,
The Children s Hospital, Oxford Sedation for clinical procedures Information for parents and carers What is sedation? Sedation can help your child by reducing anxiety before and during a clinical procedure,
Neck Mass Surgery Perioperative Instructions
 Neck Mass Surgery Perioperative Instructions We would like to make sure all your questions are answered before your procedure. We previously discussed the risks, benefits and alternatives to having the
Neck Mass Surgery Perioperative Instructions We would like to make sure all your questions are answered before your procedure. We previously discussed the risks, benefits and alternatives to having the
POSTOPERATIVE PAIN MANAGEMENT IN PEDIATRICS
 POSTOPERATIVE PAIN MANAGEMENT IN PEDIATRICS PRESENTED BY: JENIFER LICHTENFELS, M.D. PHARMACISTS OBJECTIVES Identify risk factors for narcotic induced respiratory depression in children with OSA State the
POSTOPERATIVE PAIN MANAGEMENT IN PEDIATRICS PRESENTED BY: JENIFER LICHTENFELS, M.D. PHARMACISTS OBJECTIVES Identify risk factors for narcotic induced respiratory depression in children with OSA State the
Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1
 Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1 Fast onset of pain relief with 7% reduction in visual analog scale (VAS) scores
Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1 Fast onset of pain relief with 7% reduction in visual analog scale (VAS) scores
You and your anaesthetic Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia explained and www.youranaesthetic.info This leaflet gives basic information to help
Information for patients, families and carers. General Tonsillectomy Information An e-book
 General Tonsillectomy Information An e-book Key Points The tonsils are a collection of cells in the back of the throat that fight infection. When there is inflammation of the tonsils, this is called tonsillitis.
General Tonsillectomy Information An e-book Key Points The tonsils are a collection of cells in the back of the throat that fight infection. When there is inflammation of the tonsils, this is called tonsillitis.
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Your child s general anaesthetic for dental treatment
 Questions you may like to ask your anaesthetist Q Who will give my child s anaesthetic? Q Is this the only type of anaesthetic possible for dental treatment? Q Have you often used this type of anaesthetic?
Questions you may like to ask your anaesthetist Q Who will give my child s anaesthetic? Q Is this the only type of anaesthetic possible for dental treatment? Q Have you often used this type of anaesthetic?
Dear patient and family,
 The Johns Hopkins Hospital, Division of Interventional Neuroradiology Dear patient and family, Welcome to Johns Hopkins Medicine! Your doctor has referred you to Johns Hopkins Pediatric Interventional
The Johns Hopkins Hospital, Division of Interventional Neuroradiology Dear patient and family, Welcome to Johns Hopkins Medicine! Your doctor has referred you to Johns Hopkins Pediatric Interventional
Wellness along the Cancer Journey: Palliative Care Revised October 2015
 Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
Pain Control After Surgery. Patient Information
 Pain Control After Surgery Patient Information What is Pain? Pain is an uncomfortable feeling that tells you something may be wrong in your body. Pain is your body s way of sending a warning to your brain.
Pain Control After Surgery Patient Information What is Pain? Pain is an uncomfortable feeling that tells you something may be wrong in your body. Pain is your body s way of sending a warning to your brain.
ACUTE ADENOIDITIS -An infection & enlargement of the adenoid A disease causing nasal obstruction CHRONIC ADENOIDITIS when adenoid hypertrophied it
 ACUTE ADENOIDITIS -An infection & enlargement of the adenoid A disease causing nasal obstruction CHRONIC ADENOIDITIS when adenoid hypertrophied it obstruct posterior nose or Eustachian tube extension of
ACUTE ADENOIDITIS -An infection & enlargement of the adenoid A disease causing nasal obstruction CHRONIC ADENOIDITIS when adenoid hypertrophied it obstruct posterior nose or Eustachian tube extension of
Epidural Infusions for Pain Relief Including Discharge Advice
 Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
MANAGING POST-OP PAIN AT HOME
 MANAGING POST-OP PAIN AT HOME Medicines and Self-Care After Surgery Managing Pain at Home Pain is expected after surgery. Know that you have a right to have this pain controlled. Managing pain helps you
MANAGING POST-OP PAIN AT HOME Medicines and Self-Care After Surgery Managing Pain at Home Pain is expected after surgery. Know that you have a right to have this pain controlled. Managing pain helps you
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain
 Index No: MMG43 PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain Version: 3.1 (Includes anti-emetics and naloxone) Date ratified: July 2013 Ratified by: (Name of Committee) Name
Index No: MMG43 PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain Version: 3.1 (Includes anti-emetics and naloxone) Date ratified: July 2013 Ratified by: (Name of Committee) Name
Radiation Therapy for Prostate Cancer: Gold Seed Implant Procedure
 R.S. McLaughlin Durham Regional Cancer Centre 1 Hospital Court Oshawa, ONT L1G 2B9 905-576-8711, ext. 3856 www.lakeridgehealth.on.ca Radiation Therapy for Prostate Cancer: Gold Seed Implant Procedure You
R.S. McLaughlin Durham Regional Cancer Centre 1 Hospital Court Oshawa, ONT L1G 2B9 905-576-8711, ext. 3856 www.lakeridgehealth.on.ca Radiation Therapy for Prostate Cancer: Gold Seed Implant Procedure You
The Participant will be able to: All Better!: Pediatric Adenotonsillectomy Pain Management
 All Better!: Pediatric Adenotonsillectomy Pain Management Deborah Scalford, RN, MSN The Children s Hospital of Philadelphia Objectives The Participant will be able to: Identify reasons why pain is unrelieved.
All Better!: Pediatric Adenotonsillectomy Pain Management Deborah Scalford, RN, MSN The Children s Hospital of Philadelphia Objectives The Participant will be able to: Identify reasons why pain is unrelieved.
Patient Information. A guide to your anaesthetic
 Patient Information A guide to your anaesthetic This booklet has been produced to answer your questions and to help ease your mind about the anaesthetic you are to have. Contents Page 1. What is anaesthesia?
Patient Information A guide to your anaesthetic This booklet has been produced to answer your questions and to help ease your mind about the anaesthetic you are to have. Contents Page 1. What is anaesthesia?
Satisfactory Analgesia Minimal Emesis in Day Surgeries. (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone
 Satisfactory Analgesia Minimal Emesis in Day Surgeries (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone HARSHA SHANTHANNA ASSISTANT PROFESSOR ANESTHESIOLOGY MCMASTER UNIVERSITY
Satisfactory Analgesia Minimal Emesis in Day Surgeries (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone HARSHA SHANTHANNA ASSISTANT PROFESSOR ANESTHESIOLOGY MCMASTER UNIVERSITY
History taking in paediatrics PROF. DR STANISŁAW POPOWSKI REGIONAL SPECIALIZED CHILDREN S HOSPITAL IN OLSZTYN
 History taking in paediatrics PROF. DR STANISŁAW POPOWSKI REGIONAL SPECIALIZED CHILDREN S HOSPITAL IN OLSZTYN Paediatric history taking- Introduction Obtaining an accurate history is the critical first
History taking in paediatrics PROF. DR STANISŁAW POPOWSKI REGIONAL SPECIALIZED CHILDREN S HOSPITAL IN OLSZTYN Paediatric history taking- Introduction Obtaining an accurate history is the critical first
PEDIATRIC SLEEP GUIDELINES Version 1.0; Effective
 MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
Pain management following your operation
 INFORMATION FOR PATIENTS Pain management following your operation Following your operation we want you to be as comfortable as possible. While we cannot guarantee you will be absolutely pain-free, painkillers
INFORMATION FOR PATIENTS Pain management following your operation Following your operation we want you to be as comfortable as possible. While we cannot guarantee you will be absolutely pain-free, painkillers
OSA in children. About this information. What is obstructive sleep apnoea (OSA)?
 About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
You and your anaesthetic Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia Explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia Explained and www.youranaesthetic.info This leaflet gives basic information to help
An Anaesthetist is a highly trained doctor
 This information sheet has been prepared by the Australian Society of Anaesthetists. toassist those people who are about to have an anaesthetic. It is an introduction to the basis of anaesthesia and the
This information sheet has been prepared by the Australian Society of Anaesthetists. toassist those people who are about to have an anaesthetic. It is an introduction to the basis of anaesthesia and the
Lumbar Fusion. Reference Guide for PACU CLINICAL PATHWAY. All patient variances to the pathway are to be circled and addressed in the progress notes.
 Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Davy the Detective. Finding out about anaesthetics
 Davy the Detective Finding out about anaesthetics When Davy wants to know about something, he becomes a detective (with a little help from his friends). Information about anaesthesia for young people This
Davy the Detective Finding out about anaesthetics When Davy wants to know about something, he becomes a detective (with a little help from his friends). Information about anaesthesia for young people This
You and your anaesthetic
 Questions you may like to ask your anaesthetist Q Who will give my anaesthetic? Q Do I have to have a general anaesthetic? Q What type of anaesthetic do you recommend? Q Have you often used this type of
Questions you may like to ask your anaesthetist Q Who will give my anaesthetic? Q Do I have to have a general anaesthetic? Q What type of anaesthetic do you recommend? Q Have you often used this type of
Pre-op Clinical Triad - Pulmonary. Sammy Pedram, MD FCCP Assistant Professor of Medicine Pulmonary & Critical Care Medicine March 16, 2018
 Pre-op Clinical Triad - Pulmonary Sammy Pedram, MD FCCP Assistant Professor of Medicine Pulmonary & Critical Care Medicine March 16, 2018 Disclosures none Case Mr. G is a 64 year-old man who presents to
Pre-op Clinical Triad - Pulmonary Sammy Pedram, MD FCCP Assistant Professor of Medicine Pulmonary & Critical Care Medicine March 16, 2018 Disclosures none Case Mr. G is a 64 year-old man who presents to
Taking opioid pain medicine safely
 Taking opioid pain medicine safely Information for patients taking opioid pain medicine Read this booklet to learn about: why you need to wean off your pain medicine how to wean off slowly how to control
Taking opioid pain medicine safely Information for patients taking opioid pain medicine Read this booklet to learn about: why you need to wean off your pain medicine how to wean off slowly how to control
The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery
 + The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery Elif GEZGINCI Gulhane Military Medical Academy School of Nursing Ankara 1 + 2 PREOPERATİVE + Preoperative (Patient
+ The Roles and Responsibilities of Nurse Before and After Laparoscopic Urologic Surgery Elif GEZGINCI Gulhane Military Medical Academy School of Nursing Ankara 1 + 2 PREOPERATİVE + Preoperative (Patient
TYMPANOPLASTY WITH OR WITHOUT MASTOIDECTOMY SURGICAL INSTRUCTIONS
 Head and Neck Associates of Orange County, Inc. An Incorporated Medical Group Head & Neck Surgery Pediatric & Adult Otolaryngology Facial Reconstructive Surgery TYMPANOPLASTY WITH OR WITHOUT MASTOIDECTOMY
Head and Neck Associates of Orange County, Inc. An Incorporated Medical Group Head & Neck Surgery Pediatric & Adult Otolaryngology Facial Reconstructive Surgery TYMPANOPLASTY WITH OR WITHOUT MASTOIDECTOMY
Final FRCA Written PAEDIATRICS Past Paper Questions November March 2014
 Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Pain Relief During Labor
 UW MEDICINE PATIENT EDUCATION Pain Relief During Labor Common pain relief options This chapter explains common pain relief options used during labor and delivery, when and how they are used, and what the
UW MEDICINE PATIENT EDUCATION Pain Relief During Labor Common pain relief options This chapter explains common pain relief options used during labor and delivery, when and how they are used, and what the
Maria Tracey, Director-Perioperative and Elaine Warren, Directory-Surgery Level. III (Three)
 PAGE 1/6 MANAGEMENT OF ADULT SURGICAL CLIENTS WITH KNOWN OR SUSPECTED OBSTRUCTIVE SLEEP APNEA (OSA) Patient Care Issuing Authority Dr. James Flynn, Clinical Chief Surgical Services (Perioperative) Signed
PAGE 1/6 MANAGEMENT OF ADULT SURGICAL CLIENTS WITH KNOWN OR SUSPECTED OBSTRUCTIVE SLEEP APNEA (OSA) Patient Care Issuing Authority Dr. James Flynn, Clinical Chief Surgical Services (Perioperative) Signed
How things work at our surgical wards
 How things work at our surgical wards ALL ABOUT OUR SURGICAL WARDS Here is a little brochure to help you know what to expect while you are here. It s normal to be uneasy at the prospect of surgery and
How things work at our surgical wards ALL ABOUT OUR SURGICAL WARDS Here is a little brochure to help you know what to expect while you are here. It s normal to be uneasy at the prospect of surgery and
Factors Predictive of Adverse Postoperative Events Following Tonsillectomy. A thesis submitted to the. Graduate School
 Factors Predictive of Adverse Postoperative Events Following Tonsillectomy A thesis submitted to the Graduate School of the University of Cincinnati in partial fulfillment of the requirements for the degree
Factors Predictive of Adverse Postoperative Events Following Tonsillectomy A thesis submitted to the Graduate School of the University of Cincinnati in partial fulfillment of the requirements for the degree
Pediatric Obstructive Sleep apnea An update What else is there to know?
 Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Preoperative Anxiety
 Alyssa Brzenski Case You are called by a parent of a child who you took care of a week and a half ago. The child, a 4 year old boy, came to IR for the first of many sclerotherapy of a Venous Malformation
Alyssa Brzenski Case You are called by a parent of a child who you took care of a week and a half ago. The child, a 4 year old boy, came to IR for the first of many sclerotherapy of a Venous Malformation
Screening - inclusion criteria
 A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Patient code (local): Room number: Screening - inclusion criteria
A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Patient code (local): Room number: Screening - inclusion criteria
Anaesthetic choices for hip or knee replacement
 Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Managing Pain and Sickness after Surgery
 Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Pediatric Sedation Pocket Reference
 Pediatric Sedation Pocket Reference No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopy, recording,
Pediatric Sedation Pocket Reference No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopy, recording,
Questions: What tests are available to diagnose sleep disordered breathing? How do you calculate overall AHI vs obstructive AHI?
 Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Information leaflet for parents and Carers. Pain Relief after Surgery
 Information leaflet for parents and Carers Pain Relief after Surgery This leaflet gives important information about your child s pain relief medicines and how to give them safely after surgery. It is important
Information leaflet for parents and Carers Pain Relief after Surgery This leaflet gives important information about your child s pain relief medicines and how to give them safely after surgery. It is important
Screening - inclusion criteria
 PAIN OUT Community research EU ROP EAN COMMISSION A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Room number: Screening
PAIN OUT Community research EU ROP EAN COMMISSION A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Room number: Screening
Pain and Ways to Manage It
 Pain and Ways to Manage It FM.850.M311.PHC (R.Jul-15) 1 Contents This page intentionally left blank. What the words mean............................. 2 Why is it important to manage your pain?............
Pain and Ways to Manage It FM.850.M311.PHC (R.Jul-15) 1 Contents This page intentionally left blank. What the words mean............................. 2 Why is it important to manage your pain?............
Enhanced Recovery Patient Diary
 Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Tonsillectomy - Referral for Assessment Criteria Based Access and Prior Approval Policy Date Adopted: 04 November 2016 Version: 1617.1.01 Individual Funding
Commissioning Policy Individual Funding Request Tonsillectomy - Referral for Assessment Criteria Based Access and Prior Approval Policy Date Adopted: 04 November 2016 Version: 1617.1.01 Individual Funding
BRITISH ASSOCIATION FOR EMERGENCY MEDICINE Registered Charity No
 BRITISH ASSOCIATION FOR EMERGENCY MEDICINE Registered Charity No 273876 AT THE ROYAL COLLEGE OF SURGEONS OF ENGLAND 35-43 LINCOLN'S INN FIELDS, LONDON, WC2A 3PE, UNITED KINGDOM Telephone: +44 (0)20 7831
BRITISH ASSOCIATION FOR EMERGENCY MEDICINE Registered Charity No 273876 AT THE ROYAL COLLEGE OF SURGEONS OF ENGLAND 35-43 LINCOLN'S INN FIELDS, LONDON, WC2A 3PE, UNITED KINGDOM Telephone: +44 (0)20 7831
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
STARTER PACK: Webinar #1 ADE4 - OPIOIDS
 STARTER PACK: Webinar #1 ADE4 - OPIOIDS Welcome to the Starter Pack Webinar #1 Why this is important Establishing a Team Best practices Understanding the Measures Completing a gap analysis First Steps
STARTER PACK: Webinar #1 ADE4 - OPIOIDS Welcome to the Starter Pack Webinar #1 Why this is important Establishing a Team Best practices Understanding the Measures Completing a gap analysis First Steps
PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older)
 Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Section 8: Accidental awareness during general anaesthesia
 Risks associated with your anaesthetic Section 8: Accidental awareness during general anaesthesia Summary This leaflet explains what accidental awareness is during an anaesthetic. During a general anaesthetic
Risks associated with your anaesthetic Section 8: Accidental awareness during general anaesthesia Summary This leaflet explains what accidental awareness is during an anaesthetic. During a general anaesthetic
NSAIDs and Tonsillectomy: Efficacy for Pain Relief
 NSAIDs and Tonsillectomy: Efficacy for Pain Relief Natasha Cohen, Sarah Lapner, Jayant Ramakrishna, Lehana Thabane, Doron Sommer, Gideon Koren McMaster OTL HNS Resident Research Day October 25 th 2013
NSAIDs and Tonsillectomy: Efficacy for Pain Relief Natasha Cohen, Sarah Lapner, Jayant Ramakrishna, Lehana Thabane, Doron Sommer, Gideon Koren McMaster OTL HNS Resident Research Day October 25 th 2013
Grade 7 School Immunization Program
 Grade 7 School Immunization Program Information for Parents/Guardians 1 READ the information booklet about Grade 7 vaccines. 2 COMPLETE the consent form in this package. 3 RETURN the signed form to your
Grade 7 School Immunization Program Information for Parents/Guardians 1 READ the information booklet about Grade 7 vaccines. 2 COMPLETE the consent form in this package. 3 RETURN the signed form to your
ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment
 ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment This booklet was created to help you learn about tapering. You probably have lots
ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment This booklet was created to help you learn about tapering. You probably have lots
ENDOSCOPIC SINUS SURGERY A Pre-Operative and Post-Operative Guide for Parents and Patients
 Jacqueline E. Jones, MD 1175 Park Avenue Suite 1A New York, NY 10128 ENDOSCOPIC SINUS SURGERY A Pre-Operative and Post-Operative Guide for Parents and Patients SOME BACKGROUND INFORMATION 1. What are sinuses?
Jacqueline E. Jones, MD 1175 Park Avenue Suite 1A New York, NY 10128 ENDOSCOPIC SINUS SURGERY A Pre-Operative and Post-Operative Guide for Parents and Patients SOME BACKGROUND INFORMATION 1. What are sinuses?
TONSILLECTOMY AND ADENOIDECTOMY SURGICAL INSTRUCTIONS
 John S. Supance, M.D., F.A.C.S. Mark A. Wohlgemuth, M.D., F.A.C.S. James K. Bredenkamp, M.D., F.A.C.S. Michael K. Jakobsen, M.D., F.A.C.S. Michael Cho, M.D., F.A.C.S. Phillip R. Wells, M.D. Dennis M. Crockett,
John S. Supance, M.D., F.A.C.S. Mark A. Wohlgemuth, M.D., F.A.C.S. James K. Bredenkamp, M.D., F.A.C.S. Michael K. Jakobsen, M.D., F.A.C.S. Michael Cho, M.D., F.A.C.S. Phillip R. Wells, M.D. Dennis M. Crockett,
Quality-Based Procedure
 Quality-Based Procedure Tonsillectomy with or without Adenoidectomy TOOLKIT February 2014 Introduction Quality-Based Procedures (QBPs) are an integral part of Ontario s Health System Funding Reform (HSFR)
Quality-Based Procedure Tonsillectomy with or without Adenoidectomy TOOLKIT February 2014 Introduction Quality-Based Procedures (QBPs) are an integral part of Ontario s Health System Funding Reform (HSFR)
Appendix Surgery. (Appendectomy) Your surgery and recovery at home. This booklet belongs to: Royal Columbian Hospital Eagle Ridge Hospital
 Appendix Surgery (Appendectomy) Royal Columbian Hospital Eagle Ridge Hospital Your surgery and recovery at home This booklet belongs to: We also give you Preparing for Your Surgery booklet. Read both booklets
Appendix Surgery (Appendectomy) Royal Columbian Hospital Eagle Ridge Hospital Your surgery and recovery at home This booklet belongs to: We also give you Preparing for Your Surgery booklet. Read both booklets
About general anaesthesia Day Surgery Unit Patient Information Leaflet
 About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction
 Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Improving Health, Enriching Life. Pain Management. Altru HEALTH SYSTEM
 Improving Health, Enriching Life altru.org Pain Management Altru HEALTH SYSTEM There are many different causes and kinds of pain. Pain can be caused by injury, illness, sickness, disease or surgery. Treating
Improving Health, Enriching Life altru.org Pain Management Altru HEALTH SYSTEM There are many different causes and kinds of pain. Pain can be caused by injury, illness, sickness, disease or surgery. Treating
Colonoscopy Bowel Prep Instructions SUPREP
 Colonoscopy Bowel Prep Instructions SUPREP Refer to this instruction sheet for the entire week before your colonoscopy. Colonoscopy prep instructions are extremely important for a successful colonoscopy.
Colonoscopy Bowel Prep Instructions SUPREP Refer to this instruction sheet for the entire week before your colonoscopy. Colonoscopy prep instructions are extremely important for a successful colonoscopy.
disease or in clients who consume alcohol on a regular basis. bilirubin
 NON-OPIOID Acetaminophen(Tylenol) Therapeutic class: Analgesic, antipyretic Aspirin (ASA, Acetylsalicylic Acid) Analgesic, NSAID, antipyretic Non-Opioid Analgesics COMMON USES WHAT I NEED TO KNOW AS A
NON-OPIOID Acetaminophen(Tylenol) Therapeutic class: Analgesic, antipyretic Aspirin (ASA, Acetylsalicylic Acid) Analgesic, NSAID, antipyretic Non-Opioid Analgesics COMMON USES WHAT I NEED TO KNOW AS A
